ENGLISH-Bacterial infection of skin disease Part : 5 (UPLOADED)
Bacterial infection of skin
- Bacterial skin infection is known as pyoderma.
- Pyoderma means ‘pus in the skin’.
- Cutaneous infections caused by pus-forming bacteria are known as pyoderma. This pus is not always visible to the naked eye.
- This infection can be primary or secondary.
- Primary skin infection occurs due to a break in the skin integrity and direct contact with an organism.
- While secondary skin infection occurs due to a primary skin infection or due to trauma, injury or surgery on the skin.
- Bacterial skin infections are mainly caused by gram-positive Staphylococcus aureus and beta-hemolytic streptococci bacteria.
Write a Factors associated with bacterial skin disease
- Moisture, perspiration, friction
- Obesity
- Poor hygiene and poor nutrition
- Systemic diseases such as diabetes
- Immunosuppression
Pathophysiology of bacterial skin infection
Bacteria enter the body through a cut, hair follicle, or other opening in the skin.
|
When bacteria find a favorable environment, they multiply and increase in number
|
Due to which primary (localized) infection is seen.
|
If the primary infection is not treated, it reaches the deep tissues and blood.
|
Due to which systemic infection or secondary infection is seen.
Explain Sign & symptoms seen in bacterial skin disease
- Papules and pustules
- Nodules and bumps
- Erythema
- Redness
- Swelling
- Abcess
- Pain
- Tenderness
- Itching
- Fever
- Chills
- Malaise
Diagnosis of bacterial skin infection
- History collection (to know if any systemic disease or immunosuppression therapy is ongoing)
- Physical examination (to know the characteristics of the lesion and wound)
- Complete blood count (especially to know the white blood cell count)
- Culture and sensitivity test (to know what type of infection (to know if there is an abscess present in the soft tissue and to know which type of medicine is more effective)
- Ultrasonography (to know if there is an abscess present in the soft tissue)
Medical management of bacterial skin infection
- Apply a topical antibiotic to the lesion or wound.
- Use systemic antibiotics such as penicillin, cloxacillin, dicloxacillin, erythromycin, and cephalosporin drugs to treat bacterial infections.
- Apply a warm moist compress.
- Clean the wound thoroughly with antistaphylococcal soap.
- Use an antipyretic drug to reduce fever.
- Use analgesic medicine to relieve pain. Surgical management of bacterial skin infection
- Incision and drainage procedures are used to remove skin abscesses.
Nursing management of bacterial skin infection
Assess vital signs.
Note the color and type of lesion.
Educate the patient on the importance of hygiene and hand washing.
Advise the patient to clean the wound with antistaphylococcal soap and antiseptic solution.
Apply regular dressings to the wound.
Educate the patient on wound care.
Advise the patient not to touch the wound frequently.
Advise the patient’s family members to use separate towels and washcloths for each member.
Wear gloves when dealing with the wound or lesion.
Advise the patient to use an electric razor while shaving. Apply lotion to the area after shaving.
Change the patient’s position every two hours to prevent bedsores.
Explain the procedure to the patient before the procedure.
Administer the medicine prescribed by the doctor.
Maintain records and reports.
- Impetigo (Define Impetigo)

- Impetigo is also known as ‘school sore’ because impetigo is more common in children and spreads from one person to another, and sores are seen in it.
- Impetigo is a contagious superficial skin infection caused by Gram-positive Staphylococcus aureus and group A beta-hemolytic streptococcus and other bacteria.
- Impetigo can occur at any age but is more common in children (two to five years).
- Impetigo is most commonly seen on the face, hands, neck and extremities.
write Types of impetigo
There are three types of impetigo based on clinical presentation.
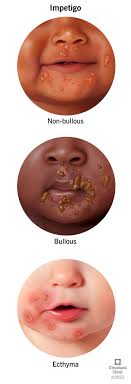
i) Non bullous impetigo
- Non bullous impetigo is the most common form of impetigo. It presents as red, itchy sores around the mouth and nose. When these sores break down, a brownish yellow crust forms.
ii) Bullous impetigo
- In bullous impetigo, large fluid-filled blisters develop from the original vesicle. These blisters are painless. When these blisters break down, a raw and red area is seen there.
iii) Ecthyma
- Ecthyma is a severe form of impetigo. When impetigo is not treated, ecthyma occurs. In which painful blisters are seen deep in the skin. These blisters turn into pus-filled sores and crusts.
Write Sign & symptoms seen in impetigo
- In the beginning, small and red colored macules are seen.
- Then they turn into thin-walled vesicles.
- These vesicles are painless.
- When these vesicles rupture, a honey yellow colored crust is seen in them.
- Removing this crust reveals a smooth red moist surface.
- If left untreated, the blister becomes painful and a pus-filled sore is seen.
Diagnosis of impetigo
- History collection
- Physical examination
- Complete blood count
- Culture and sensitivity test
Write Medical management of impetigo
- Provide systemic antibiotics.
- Provide benzathine penicillin in non-bullous impetigo.
- Use cloxacillin and dicloxacillin in bullous impetigo.
- Use erythromycin medicine for people who are allergic to penicillin.
- Topical antibiotic – Mupirocin ointment applied two to three times a day.
- Wash the lesion thoroughly with antiseptic solution or soap and remove the crust.
Write Nursing management of impetigo
- Note the location and type of skin lesion.
- Assess vital signs.
- Advise the patient to maintain personal hygiene.
- Advise the patient to bathe with antistaphylococcal soap and clean the lesion thoroughly with antiseptic solution.
- Educate the patient about wound care.
- Apply topical medicine to the sore.
- Advise the patient not to touch the lesion frequently and to wash hands before touching it.
- Advise the patient’s family members to use separate towels and washcloths for each member.
- Avoid sharing items used by the patient and avoid contact with others.
- Administer medications prescribed by the doctor.
- Maintain records and reports.
2.Folliculitis
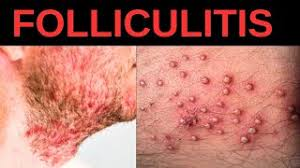
Folliculitis is the name given to the infection and inflammation of the hair follicle.
The infection starts at the opening of the hair follicle and extends down into the follicle.
The bacteria Staphylococcus aureus is responsible for causing folliculitis.
Folliculitis is more common in areas where there is excessive friction, moisture and rubbing.
Folliculitis is mainly seen in the beard area where it shaves, in addition to the armpits, groin, buttocks and trunk areas.
Folliculitis is more common in people who have poor hygiene and wear tight, heavy fabric clothes.
write short notes on Type of folliculitis
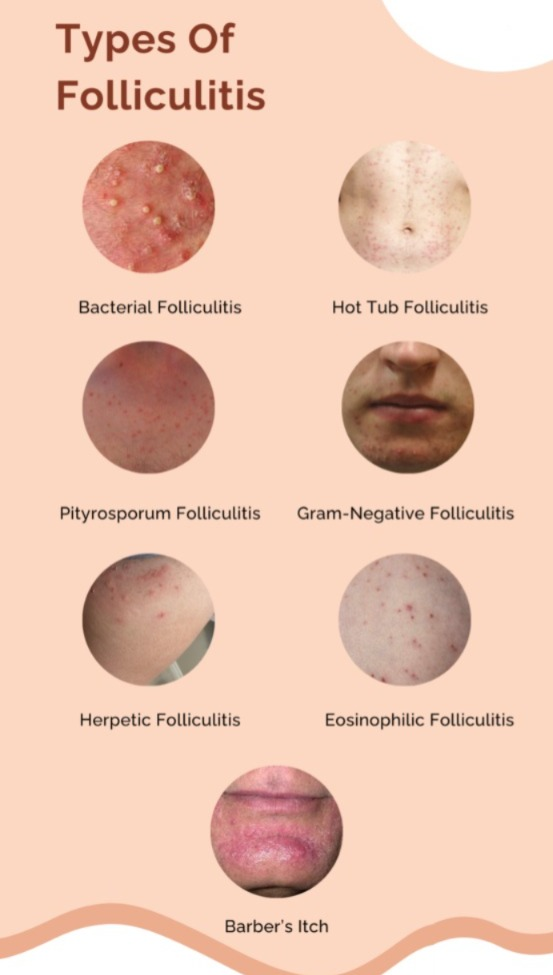
Folliculitis is of the following types.
i) Bacterial folliculitis
Bacterial folliculitis is caused by a bacteria called Staphylococcus aureus, hence bacterial folliculitis is also called ‘Staphylococcus aureus folliculitis’. In bacterial folliculitis, infection is seen in the hair follicle. In which small red and white colored pus filled pimples are seen around the hair follicle.
ii) Hot tube folliculitis
Hot tube folliculitis is caused by a bacteria called Pseudomonas aeruginosa. These bacteria are found in hot tubs, hot pools and water slides. Hence, round itchy bumps appear on the skin one to four days after bathing in such places.
iii) Pseudofolliculitis barbae
Pseudofolliculitis barbae is also known as ‘razor bumps’. Pseudo means fake. In pseudofolliculitis, there is no infection in the hair follicle but signs of infection are seen. Pseudofolliculitis barbae is mainly seen in the bearded area. In which irritation is seen in that area after shaving with a razor. Pseudofolliculitis barbae is more common in people with curly hair and black color.
iv) Sycosis barbae
- Sycosis Barbe is a more severe type of folliculitis caused by saving related folliculitis. In sycosis barbe, the entire hair follicle is infected due to which a large red colored pustule is seen.
v) Pityrosporum folliculitis
- Pterosporum folliculitis is also known as ‘Malassezia folliculitis’. Pterosporum folliculitis is caused by a yeast infection. Due to which itchy pus filled bumps are seen. Which is mostly seen in upper chest and back.
vi) Eosinophilic folliculitis
- Eosinophilic folliculitis occurs in immunosuppressed patients such as those with human immunodeficiency virus (HIV). In which there is an itching pustule bump in the neck, upper arm, solder, fore head.
vii) Gram negative folliculitis
- Gram negative folliculitis occurs as a result of prolonged use of antibiotics used to treat one. Overuse of this medicine causes bacteria to become resistant to it and these resistant bacteria grow and multiply thus creating the condition of folliculitis. In which pus filled bumps are seen around the nose and mouth.
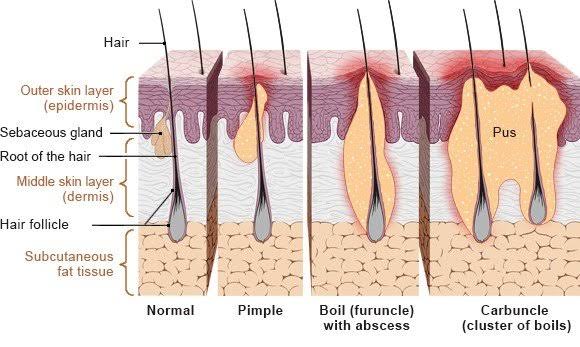
viii) Furuncle (boil) & Carbuncle (furuncle and carbuncle)
- Furuncles and carbuncles are infections caused by Staphylococcus aureus bacteria deep into the hair follicle. A painful inflamed bump is seen in a furuncle. When a cluster of boils is found in a carbuncle.
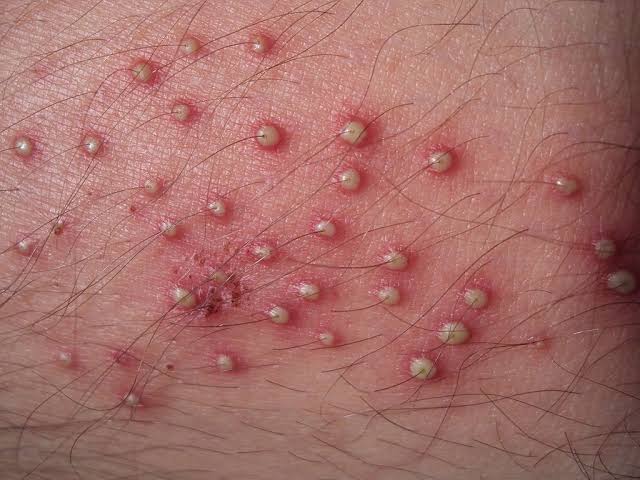
Sign & symptoms seen in folliculitis (sign and symptoms seen in folliculitis)
- One or more papules and pustules are seen near the hair follicle.
- Erythema around hair follicles.
- There is itching and irritation at the site of the infected hair follicle along with a slight burning sensation.
- Tenderness is also seen with it.
Diagnosis of folliculitis
- History Collection
- Physical Examination
- Blood culture
- Culture and sensitivity test
- Potassium Hydroxide Testing
Medical management of folliculitis
- Using topical antibiotics clindamycin and bactroban.
- Using antistaphylococcal soap while bathing.
- Provide warm moist compression on the affected area.
Prevention of folliculitis
- Wash the skin daily.
- Maintain proper hygiene.
- Using a clean towel and washcloth.
- Avoid friction and pressure on the skin.
- Avoid wearing tight heavy fabric clothes.
- Avoid shaving if possible.
- Using another method to remove hair.
- Using an electric shaving laser and taking great care while shaving.
- Apply lotion in that area after saving.
- Using clean hot tubes and heat pools.
3.Furuncle
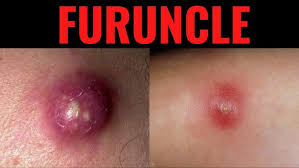
- A furuncle is also known as a ‘boil’.
- In a furuncle one or more hair follicles are infected and these hair follicles are infected deep and the infection extends to the dermis layer.
- That means a furuncle is a deep folliculitis.
- A bacteria called Staphylococcus aureus is responsible for causing the furuncle.
- Furuncles are most commonly found in the neck, axilla, thighs, buttocks and perineum area.
- Multiple and recurrent lesions are known as furunculosis.
Sign & symptoms seen in furuncle (Sign and symptoms seen in furuncle)
- Initially a painful pimple of deep, hard, pink or red color is seen.
- Which is one to five centimeters in diameter.
- After few days this pimple increases in size and cystic nodule is formed. In which pus collection is seen i.e. formation of abscess.
- Tenderness is also seen around the affected area.
Diagnosis of furuncle (Diagnosis of furuncle)
- History Collection
- Physical Examination
- Blood count
- Culture and sensitivity test
Medical management of furuncle (Medical management of furuncle)
- Using systemic antibiotics to treat bacterial infections.
- Apply a topical antibiotic to the affected area.
- Provide warm compresses on the affected area.
- Cleaning the lesion or wound with antistaphylococcal soap.
Surgical management of furuncle
- Using an incision and drainage procedure to remove the abscess.
Nursing management of furuncle
- Note the size and color of the skin nodule.
- To assess vital signs.
- Advise the patient not to prick boils and pimples.
- Advise the patient to clean the wound thoroughly with antistaphylococcal soap and antiseptic solution.
- Explaining wound care to the patient.
- Applying topical medicine on the wound.
- Explaining the patient about home care.
- Educate the patient about hand wash and hygiene.
- To administer the medicine prescribed by the doctor.
- To maintain records and reports.
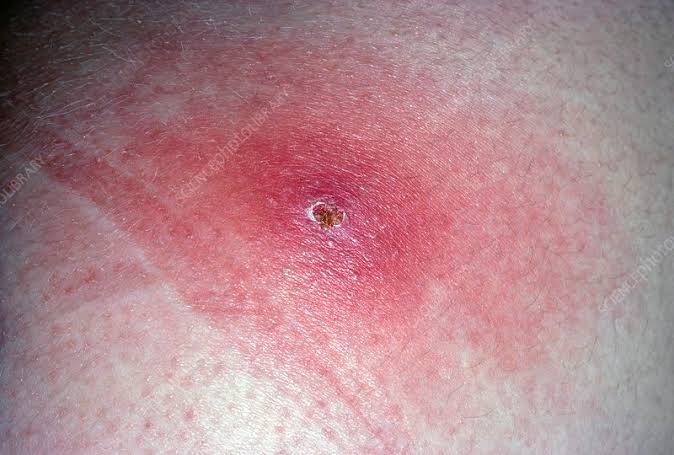
4.Carbuncle
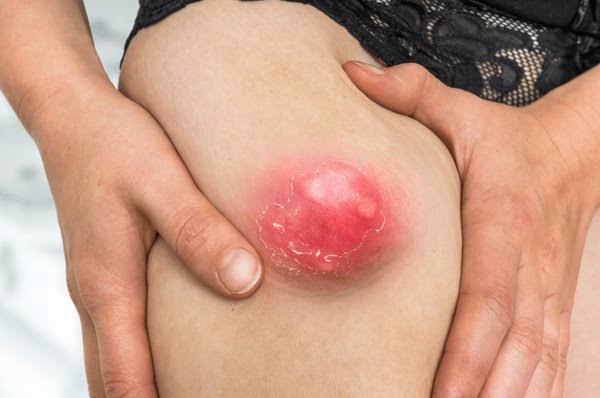
- A cluster of boils is known as a carbuncle.
- A carbuncle involves simultaneous infection of many hair follicles and the infection extends to the surrounding skin and subcutaneous tissue and abscess formation is seen.
- Carbuncle is caused by Staphylococcus aureus bacteria.
- Carbuncles are mainly found in thick and inelastic areas.
- Carbuncle is mostly found in neck, upper arm, buttock, lateral.
- Carbuncles and furuncles are more common in people with immunosuppression, diabetes and systemic diseases.
Sign & symptoms seen in carbuncle (Sign and symptoms seen in carbuncle)
- Painful pus filled bump of red color is seen in the affected area.
- These bumps range in size from a pea to a golf ball.
- Due to the collection of pus, the central part appears white or yellow in color.
- Leukocytosis, fever, chills and fatigue are also seen.
- Scar formation is seen.
Diagnosis of carbuncle (Diagnosis of carbuncle)
- History Collection
- Physical Examination
- Complete Blood Count
- Culture and sensitivity test
- Ultra sonography
Medical management of carbuncle (Medical management of carbuncle)
- Apply a topical antibiotic to the affected area.
- Using the systemic antibiotic dicloxacillin or cloxacillin.
- Take analgesic medicine to relieve pain.
- Using antipyretic drug to remove fever. Surgical management of carbuncle (Surgical management of carbuncle)
- Incision and drainage to drain the abscess.
- Regular dressing on incision and drained area.
Home care of carbuncle (Home care of carbuncle)
- Apply a clean, warm, moist cloth to the affected area.
- Clean the affected area with antibacterial soap.
- Regular dressing changes.
- Wash hands before touching the affected area.
- Maintain proper hygiene.
- Take regular medicine and get checkups done.
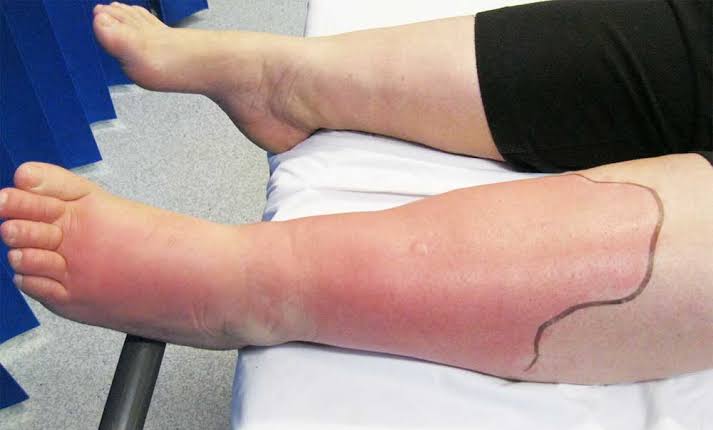
5. Cellulitis
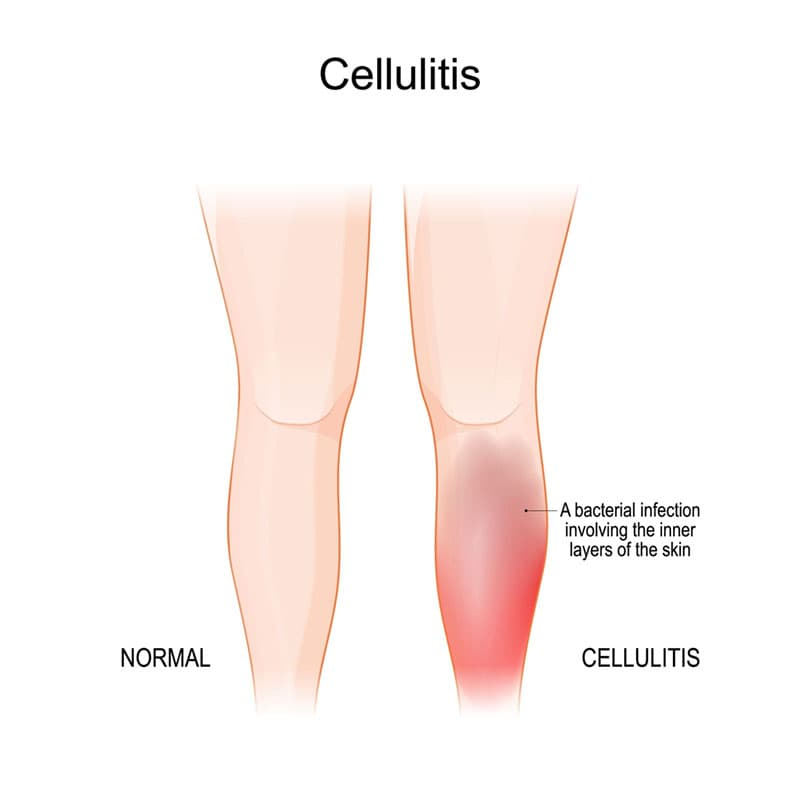
- Cellulitis is a common and serious bacterial infection.
- Cellulitis is a secondary skin infection.
- In which infection occurs in the skin and subcutaneous tissue.
- Bacteria called Staphylococcus and Streptococci are responsible for causing cellulitis.
- Cellulitis is most often seen in the lower leg. Apart from this, it is also seen in the face, arm and other areas.
- If cellulitis is not treated, the infection spreads to the blood and lymph nodes and a life-threatening condition occurs.
Sign & symptoms seen in Cellulitis (Signs and symptoms seen in Cellulitis)
- Signs and symptoms found on any one side of the body.
- Redness and swelling is observed in the affected area.
- Infected area is found hot and tender.
- spots and blisters are seen in the infected area.
- Swelling is seen in the lymph nodes.
- Fever, chills and fatigue are also seen.
Diagnosis of Cellulitis (Diagnosis of Cellulitis)
- History Collection
- Physical Examination
- Blood count
- Culture and sensitivity test
- C-reactive protein
Medical management of Cellulitis
- Using systemic antibiotics to treat bacterial infections.
- Apply topical medicine on the affected area.
- Providing warm moist compression.
- Cleaning the infected area with antiseptic solution.
- Provide analgesic medicine to relieve pain.
- Giving antipyretic drug to remove fever.
Nursing management of Cellulitis
- Perform vital sign assays.
- Checking the infected area for tenderness and swelling.
- Keep skin dry and clean.
- Immobilize and elevate the part with cellulitis.
- Change the patient’s position every two hours.
- Clean the infected area with an antiseptic solution and then apply topical medicine.
- Giving advice to the patient to maintain proper hygiene.
- To administer medicine prescribed by a doctor.
- To maintain records and reports.