Unit-7-B.sc-TheMusculoskeletal system:-
🦴 Introduction to the Skeletal System
The skeletal system is the framework of the human body. Made up of 206 bones in adults, it provides structure, support, and protection to vital organs and also enables movement in coordination with the muscular system.
From the skull that protects the brain, to the rib cage that shields the heart and lungs, and the spine that supports the body and houses the spinal cord — every bone plays a critical role. This system is more than just a hard structure — it’s living tissue that grows, repairs, and produces blood cells within the bone marrow.
🧍♂️✨ Anatomical Position – The Foundation of Human Anatomy
Imagine you’re looking at a statue designed to show every detail of the human body clearly. The way that statue stands—upright, facing forward, with arms relaxed at the sides and palms turned outward—is the anatomical position.
This position may seem simple, but it’s one of the most important reference points in anatomy. It forms the universal starting line from which all descriptions of direction, position, and movement begin.
🔷 What is the Anatomical Position?
The anatomical position is a standardized posture used in medicine and anatomy to describe the location of body parts. This standard prevents confusion when health professionals communicate about the human body—because everyone refers to the same orientation.
🧍 Key Characteristics of the Anatomical Position:
When a body is in the anatomical position:
- It stands erect and upright.
- The head faces forward, looking straight ahead.
- The eyes gaze directly forward, level with the ground.
- The arms hang loosely at the sides of the body.
- The palms face forward, with the thumbs pointing away from the body.
- The legs are straight, with the feet slightly apart.
- The toes point forward, not out to the sides.
🧠 Note: Even if a person is lying down during surgery or a scan, doctors still describe the body parts as if the person is in the anatomical position. This helps maintain consistency.
📍 Why is Anatomical Position So Important?
Anatomical position acts like a GPS system for the body. Without it, doctors, nurses, and anatomists would easily get confused when talking about the location of a wound, organ, or bone.
Think of it like giving directions in a city. If everyone uses the same map, they won’t get lost. The anatomical position is that map of the human body.
🧭 Understanding Directional Terms in Relation to Anatomical Position
Once we place the body in anatomical position, we can describe where one structure is in relation to another. These directional terms are used in surgeries, X-rays, anatomy classes, and clinical documentation.
For example:
- “The heart is posterior to the sternum” means the heart lies behind the breastbone.
- “The stomach is inferior to the lungs” means it’s below the lungs.
These terms are based entirely on the anatomical position.
🧭 Detailed Directional Terms in Human Anatomy
All of the terms below are explained assuming the body is in the standard anatomical position—standing upright, facing forward, arms at the sides, and palms facing forward.
🔹 1. Anterior (Ventral)
Definition:
Refers to the front side of the body.
Details:
The term “anterior” is commonly used to describe structures that are located toward the front of the body. In humans, since we stand upright, the face, chest, abdomen, and front of the arms and legs are considered anterior structures.
Example:
- The breastbone (sternum) is anterior to the heart.
- The toes are anterior to the heel.
🧠 “Ventral” is more commonly used in animals, but in humans, “anterior” and “ventral” are often used interchangeably.
🔹 2. Posterior (Dorsal)
Definition:
Refers to the back side of the body.
Details:
“Posterior” is used to describe structures located toward the rear of the body. This includes the back of the head, back, buttocks, and the backs of the arms and legs.
Example:
- The vertebral column (spine) is posterior to the stomach.
- The scapula (shoulder blade) is posterior to the ribs.
🧠 In four-legged animals, “dorsal” refers to the upper side (back), and is used more often than “posterior.”
🔹 3. Superior (Cranial)
Definition:
Means above, or toward the head or upper part of the body.
Details:
“Superior” is used when comparing the vertical position of body parts. If one structure is higher than another, it is said to be superior.
Example:
- The brain is superior to the lungs.
- The eyes are superior to the mouth.
🧠 “Cranial” is more commonly used in animal anatomy, referring to the head end.
🔹 4. Inferior (Caudal)
Definition:
Means below, or toward the feet/lower part of the body.
Details:
Used when comparing parts of the body vertically. If one structure is lower than another, it is described as inferior.
Example:
- The stomach is inferior to the heart.
- The knees are inferior to the hips.
🧠 “Caudal” means “toward the tail”—more applicable in animals.
🔹 5. Medial
Definition:
Refers to a structure that is closer to the midline of the body.
Details:
The midline is an imaginary vertical line that divides the body into equal right and left halves. Structures closer to this line are medial.
Example:
- The nose is medial to the ears.
- The big toe is medial compared to the little toe.
🔹 6. Lateral
Definition:
Refers to a structure that is farther from the midline of the body.
Details:
Lateral is the opposite of medial. Structures located away from the center of the body are considered lateral.
Example:
- The ears are lateral to the nose.
- The lungs are lateral to the heart.
🔹 7. Proximal
Definition:
Means closer to the point of attachment or origin of a limb or structure.
Details:
Mostly used in reference to limbs (arms and legs). The point of attachment is typically the shoulder (for the upper limb) or the hip (for the lower limb).
Example:
- The elbow is proximal to the wrist (closer to the shoulder).
- The thigh is proximal to the foot.
🔹 8. Distal
Definition:
Means farther from the point of attachment or origin of a limb.
Details:
Distal is the opposite of proximal. It is used to describe parts farther away from the trunk or root of a limb.
Example:
- The fingers are distal to the elbow.
- The foot is distal to the knee.
🔹 9. Superficial
Definition:
Located toward or on the surface of the body.
Details:
Used to describe structures that are close to the body’s surface.
Example:
- The skin is superficial to the muscles.
- A superficial wound is one that affects the surface only.
🔹 10. Deep
Definition:
Located away from the surface, more internal.
Details:
This term is used to describe structures beneath other layers.
Example:
- The bones are deep to the skin.
- The heart is deep to the rib cage.
🌟 Clinical Tip:
In documentation, these terms help prevent errors. For example:
Instead of writing “wound on front leg,” a nurse will write:
“A 3 cm superficial laceration is present on the anterior aspect of the right thigh, lateral to the patella.”
🧠 Bonus Insight: Anatomical Planes
To study the body in sections, we also refer to planes:
- Sagittal Plane: Divides the body into left and right sides.
- Midsagittal (Median) Plane: Divides it into equal left and right halves.
- Frontal (Coronal) Plane: Splits the body into front and back parts.
- Transverse (Horizontal) Plane: Cuts the body into top and bottom halves.
These planes help when viewing imaging like MRI, CT scans, or in surgery.
🛏️ Clinical Body Positions – Beyond the Anatomical
In clinical practice, patients may be placed in various positions depending on the procedure or condition. These include:
- Supine: Lying flat on the back, face up.
- Prone: Lying flat on the stomach, face down.
- Fowler’s Position: Semi-sitting position, often used in respiratory distress.
- Lithotomy Position: Lying on the back with legs raised (used in gynecological exams).
- Trendelenburg Position: Body is flat but feet are elevated higher than the head (used in shock).
🧩 Real-World Example:
Imagine a nurse is documenting a wound as being on the left lateral thigh. This means it’s on the outer side of the left upper leg, based on anatomical position—even if the patient is lying sideways or upside down.
🎯
The anatomical position is more than a pose—it’s a global language in healthcare and anatomy. It creates a shared understanding so that everyone, from surgeons to students, speaks the same language when describing the human body.
🦴 Structure of Bone (Detailed Explanation)
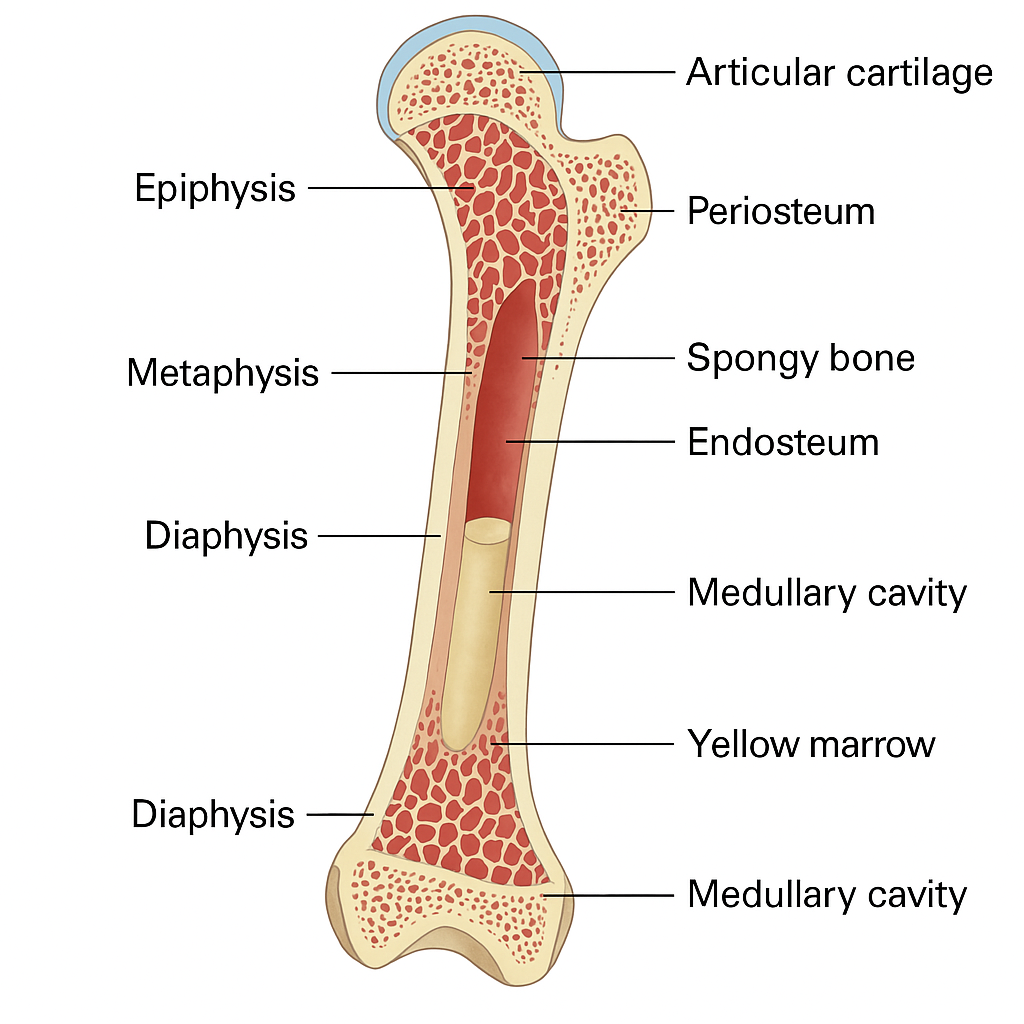
🔷 A. Gross (Macroscopic) Structure of Bone
To understand the structure of a typical long bone (like the femur or humerus), we divide it into major visible parts:
1. Diaphysis (Shaft)
- It is the long, cylindrical middle portion of a long bone.
- Composed mainly of compact (cortical) bone, which gives strength.
- Contains the medullary cavity (marrow cavity) filled with yellow marrow in adults (fat storage).
- The walls are thick and strong to bear weight.
2. Epiphysis (Ends)
- These are the expanded ends of the bone.
- Consist mostly of spongy (cancellous) bone containing red bone marrow (site of blood cell formation).
- Covered by a thin layer of compact bone on the outside.
- At joint surfaces, the epiphysis is covered by articular (hyaline) cartilage to reduce friction and absorb shock.
3. Metaphysis
- The transitional area between diaphysis and epiphysis.
- In growing bones, it includes the epiphyseal plate (growth plate)—made of cartilage that allows bones to grow in length.
- After puberty, the plate becomes a bony line (epiphyseal line).
4. Periosteum
- A tough, double-layered membrane covering the outer surface of the bone (except at joint surfaces).
- Outer fibrous layer: made of dense connective tissue; attachment site for muscles, ligaments, and tendons.
- Inner osteogenic layer: contains osteoblasts and osteoclasts (for bone growth and repair).
- Rich in blood vessels and nerves; plays a major role in nourishment, protection, and healing.
5. Endosteum
- A thin vascular membrane that lines the inner surface of the bone (medullary cavity and spaces in spongy bone).
- Contains bone-forming and bone-destroying cells.
- Involved in bone remodeling and healing.
6. Medullary (Marrow) Cavity
- A hollow space inside the diaphysis.
- In children: filled with red bone marrow (produces blood cells).
- In adults: contains mostly yellow marrow (fat storage), which can revert to red marrow if needed during severe blood loss.
🔷 B. Microscopic Structure of Bone
There are two types of bone tissue visible under a microscope:
1. Compact (Cortical) Bone
- Dense and strong, forming the outer layer of all bones.
- Made up of repeating structural units called osteons (Haversian systems).
📌 Components of an Osteon:
- Central (Haversian) Canal
– Runs longitudinally; contains blood vessels, lymph vessels, and nerves. - Lamellae
– Concentric rings of calcified matrix around the central canal. - Lacunae
– Small spaces between lamellae that house osteocytes (mature bone cells). - Canaliculi
– Tiny channels that connect lacunae to each other and to the central canal.
– Allows nutrient and waste exchange between osteocytes.
Think of an osteon like a tree trunk: the rings are lamellae, the small holes are lacunae, and the canals are blood vessel pathways.
2. Spongy (Cancellous) Bone
- Found mainly in the epiphyses of long bones and inside flat and irregular bones (like the skull and vertebrae).
- Composed of a network of thin plates called trabeculae.
📌 Features:
- Trabeculae are aligned along lines of stress to resist pressure.
- Spaces between trabeculae are filled with red bone marrow (hematopoietic tissue).
- No osteons in spongy bone, but it contains lamellae and osteocytes within lacunae.
- Lightweight but strong—reduces bone weight while maintaining support.
🔷 C. Bone Cells Involved in Structure and Function
- Osteoblasts
- Build new bone matrix.
- Found in periosteum and endosteum.
- Active during growth and healing.
- Osteocytes
- Mature bone cells that maintain the bone matrix.
- Found in lacunae.
- Communicate through canaliculi.
- Osteoclasts
- Break down bone matrix (resorption).
- Important in remodeling, calcium release, and repair.
🧠 Bonus: Bone Matrix Composition
- Organic part (35%)
- Mainly collagen fibers – gives bones flexibility and tensile strength.
- Inorganic part (65%)
- Mainly calcium phosphate crystals (hydroxyapatite) – gives bones hardness and strength.
✅ Summary of Bone Structure
| Part | Description |
|---|---|
| Diaphysis | Shaft, compact bone with marrow cavity |
| Epiphysis | Ends, spongy bone with red marrow |
| Metaphysis | Growth area in growing bones |
| Periosteum | Outer membrane with blood supply and osteoblasts |
| Endosteum | Inner membrane, active in remodeling |
| Compact Bone | Dense, organized in osteons |
| Spongy Bone | Light, mesh-like trabeculae with red marrow |
| Bone Marrow | Red (hematopoiesis), Yellow (fat storage) |
🦴 Types of Bones – Detailed Explanation
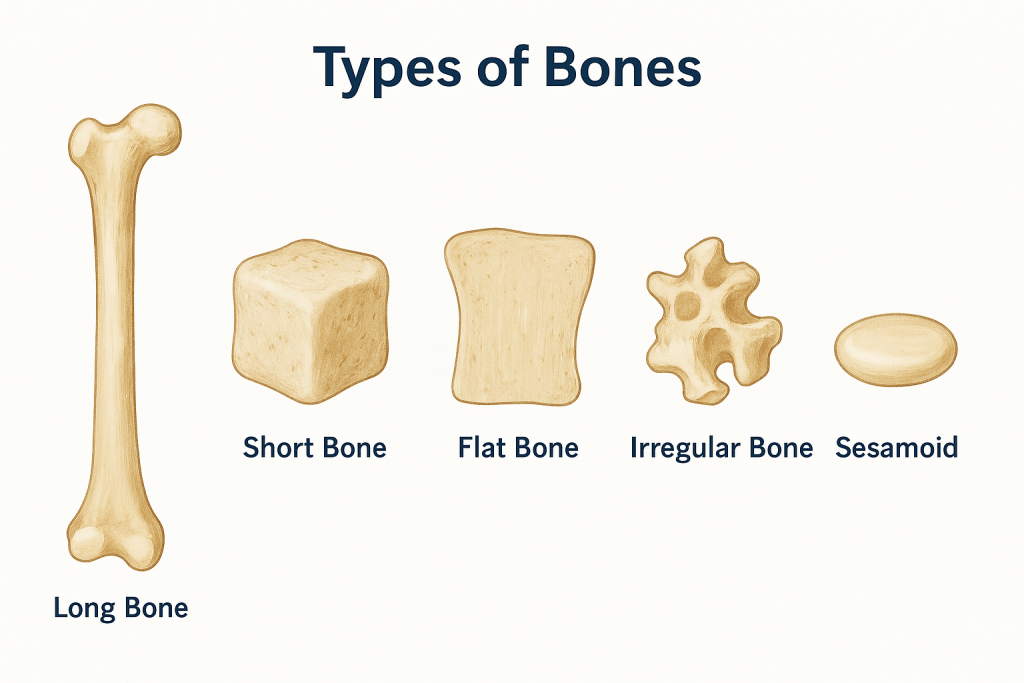
The human body contains 206 bones, which are classified into five main types based on their shape and function. These categories help us understand how bones support movement, protect organs, and contribute to the structure of the body.
🔷 1. Long Bones
📌 Description:
- These bones are longer than they are wide.
- They have a shaft (diaphysis) and two ends (epiphyses).
- Mainly composed of compact bone with spongy bone at the ends.
- Designed to support weight and facilitate movement.
📌 Functions:
- Act as levers for muscles.
- Support and movement of limbs.
- Site for red marrow (blood cell production) in children.
📌 Examples:
- Upper limb: Humerus, Radius, Ulna
- Lower limb: Femur, Tibia, Fibula
- Others: Metacarpals, Metatarsals, Phalanges
🧠 Fun fact: The femur is the longest and strongest bone in the human body!
🔷 2. Short Bones
📌 Description:
- Roughly cube-shaped, as long as they are wide.
- Thin layer of compact bone surrounds a spongy interior.
- No shaft or prominent ends.
- Designed for strength and stability with limited movement.
📌 Functions:
- Provide support and stability.
- Absorb compressive forces.
📌 Examples:
- Carpals (wrist bones)
- Tarsals (ankle bones)
These bones are often found in clusters in areas requiring flexibility and shock absorption.
🔷 3. Flat Bones
📌 Description:
- Thin, usually curved, and have broad surfaces.
- Made up of two parallel layers of compact bone with spongy bone (diploë) in between.
- Provide protection and surface area for muscle attachment.
📌 Functions:
- Protect vital organs.
- Serve as attachment points for muscles.
📌 Examples:
- Skull bones: Frontal, Parietal, Occipital
- Thoracic bones: Sternum, Ribs
- Shoulder bones: Scapula
The cranial bones protect the brain, and the ribs protect the heart and lungs.
🔷 4. Irregular Bones
📌 Description:
- Have complex shapes that don’t fit into the other categories.
- Made of compact bone outside and spongy bone inside.
- Often specialized for protection or anchoring muscles.
📌 Functions:
- Protect organs (e.g., spinal cord, brain).
- Provide attachment for muscles.
📌 Examples:
- Vertebrae (spinal bones)
- Facial bones: Maxilla, Mandible, Zygomatic
- Pelvic bones: Ischium, Pubis, Ilium
- Sphenoid and Ethmoid bones of the skull
These bones are structurally unique and often perform multiple functions.
🔷 5. Sesamoid Bones
📌 Description:
- Small, round bones embedded within tendons.
- Usually found where a tendon passes over a joint.
- Can vary in number and size among individuals.
📌 Functions:
- Protect tendons from wear and tear.
- Improve mechanical efficiency of muscles.
📌 Examples:
- Patella (kneecap) – the largest sesamoid bone
- Other small sesamoid bones in hands and feet
The patella enhances the leverage of the quadriceps muscle in the knee.
🔷 Bonus: Accessory (Supernumerary) Bones
Sometimes, people have extra bones, such as:
- Sutural bones: tiny bones found between skull sutures.
- Accessory navicular: an extra bone in the foot.
These are normal variants and may be asymptomatic or occasionally cause issues.
✅ Summary at a Glance:
| Bone Type | Shape & Feature | Function | Examples |
|---|---|---|---|
| Long Bones | Longer than wide, shaft + ends | Movement, strength | Femur, Humerus, Tibia |
| Short Bones | Cube-shaped, spongy inside | Support with limited movement | Carpals, Tarsals |
| Flat Bones | Thin, flat, often curved | Protection, muscle attachment | Skull, Ribs, Sternum, Scapula |
| Irregular Bones | Irregular, complex shapes | Protection, multiple muscle attachments | Vertebrae, Facial bones, Pelvis |
| Sesamoid Bones | Small, round, in tendons | Reduce friction, improve force | Patella, small sesamoids in feet |
📘 Clinical Tip:
- Fractures of long bones often lead to significant blood loss due to rich vascular supply.
- Flat bones (like the sternum) are common sites for bone marrow biopsies.
- Osteoporosis affects all bones, but vertebrae (irregular bones) and femur neck (long bone) are especially prone to fractures.
🦴 Bone Growth and Ossification – Detailed Explanation
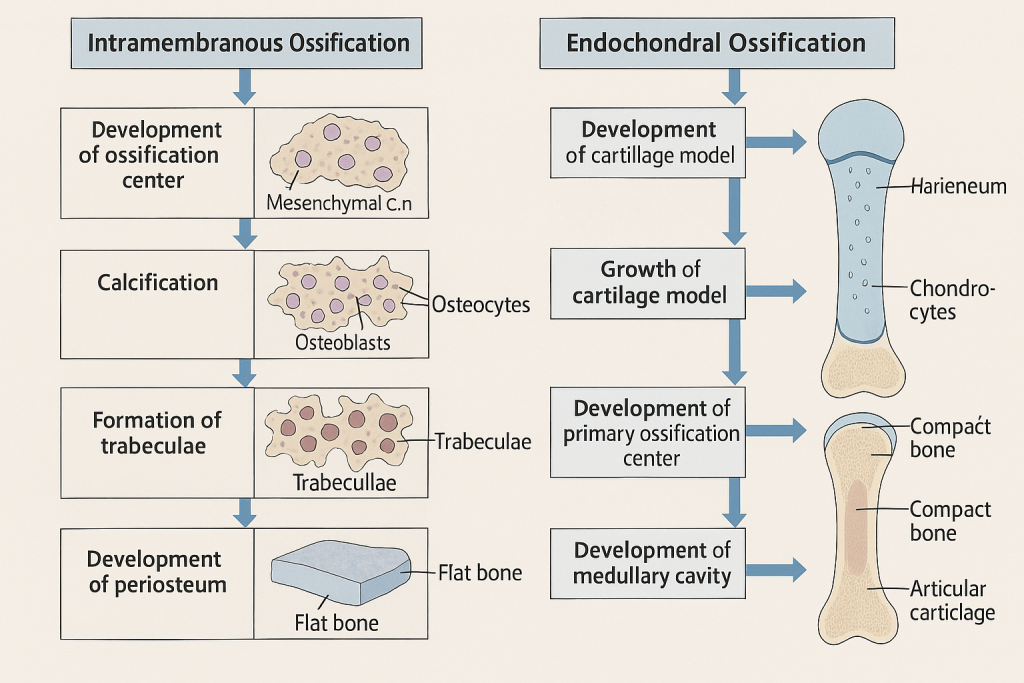
🔷 What is Ossification?
Ossification (also called osteogenesis) is the process of bone formation. It begins during embryonic development and continues throughout childhood, adolescence, and even adulthood during healing and remodeling.
There are two main types of ossification processes based on how bone is formed:
🔹 1. Intramembranous Ossification
📌 Definition:
Bone develops directly from mesenchymal tissue (embryonic connective tissue), without a cartilage stage.
📌 Where it occurs:
- Mostly in flat bones of the skull, mandible (lower jaw), and clavicle (collarbone).
📌 Process:
- Mesenchymal cells group together and differentiate into osteoblasts.
- Osteoblasts begin to secrete bone matrix (osteoid).
- The matrix hardens by calcification, trapping osteoblasts that become osteocytes.
- The bone forms into trabeculae (spongy bone).
- The outer surface forms a periosteum, and compact bone develops on the outside.
🧠 Think of it like a bone forming inside a membrane—hence “intramembranous.”
🔹 2. Endochondral Ossification
📌 Definition:
Bone forms by replacing hyaline cartilage with bone tissue.
📌 Where it occurs:
- Most bones of the body, especially long bones (femur, humerus), vertebrae, and pelvis.
📌 Process:
- Mesenchymal cells first form a cartilage model of the future bone.
- The cartilage grows in size.
- A bone collar forms around the cartilage shaft.
- Chondrocytes (cartilage cells) die in the center, forming cavities.
- Blood vessels invade the center → bringing osteoblasts.
- Primary ossification center forms in the diaphysis.
- Later, secondary ossification centers develop in the epiphyses (bone ends).
- Cartilage remains only in the epiphyseal plate (growth plate) and articular cartilage.
🧠 This process takes longer and is how most bones in the body are formed.
🔷 Growth in Length – Epiphyseal Plate Activity
Bones grow in length at the epiphyseal (growth) plate, a layer of hyaline cartilage between the epiphysis and diaphysis in growing bones.
📌 Zones of the Epiphyseal Plate (from epiphysis to diaphysis):
- Resting Zone – Small, inactive cartilage cells.
- Proliferation Zone – Chondrocytes divide rapidly and form columns.
- Hypertrophic Zone – Chondrocytes enlarge and mature.
- Calcification Zone – Matrix calcifies; chondrocytes die.
- Ossification Zone – Osteoblasts replace calcified cartilage with bone.
📌 As long as the epiphyseal plate is active, the bone can grow in length. 📌 Around age 18–25, the growth plate closes (becomes epiphyseal line), and growth in length stops.
🔷 Growth in Thickness – Appositional Growth
Bones also grow in diameter (thickness) through a process called appositional growth.
📌 How it works:
- Osteoblasts in the periosteum lay down new bone layers on the outer surface.
- Osteoclasts in the endosteum dissolve bone on the inside, enlarging the medullary cavity.
- This allows the bone to become thicker and stronger without becoming heavy.
🧠 This type of growth continues even after length growth stops—especially in response to physical activity or stress.
🔷 Bone Remodeling (Lifelong Process)
Even after bones stop growing, they constantly remodel to maintain strength and balance minerals.
- Osteoblasts form new bone.
- Osteoclasts resorb (break down) old bone.
- Remodeling is regulated by hormones (e.g., parathyroid hormone, calcitonin) and mechanical stress (exercise).
🔷 Factors Affecting Bone Growth and Ossification
✅ Essential Nutrients:
- Calcium and phosphorus – bone mineralization.
- Vitamin D – calcium absorption.
- Vitamin C – collagen synthesis.
- Vitamin A – osteoblast activity.
✅ Hormones:
- Growth hormone (GH) – stimulates epiphyseal plate activity.
- Thyroid hormone – regulates GH.
- Sex hormones (estrogen & testosterone) – promote growth spurt and then plate closure.
✅ Physical Activity:
- Weight-bearing exercise stimulates bone deposition and thickness.
- Lack of exercise leads to bone weakening (osteopenia/osteoporosis).
🔷 Clinical Relevance
- Fracture Healing involves reactivation of the ossification process.
- Rickets (children) and osteomalacia (adults) result from defective mineralization due to Vitamin D deficiency.
- Achondroplasia: a genetic disorder where endochondral ossification is impaired, leading to dwarfism.
- Osteoporosis: bone resorption exceeds formation; bones become fragile.
✅ Summary: Differences Between Intramembranous and Endochondral Ossification
| Feature | Intramembranous Ossification | Endochondral Ossification |
|---|---|---|
| Starts from | Mesenchymal cells | Cartilage model |
| Type of bones | Flat bones (skull, clavicle) | Long bones, vertebrae, pelvis |
| Cartilage involved? | No | Yes (hyaline cartilage) |
| Speed | Faster | Slower |
| Example | Skull bones | Femur, Tibia, Vertebrae |
🦴 Human Skeleton – Axial vs Appendicular Skeleton
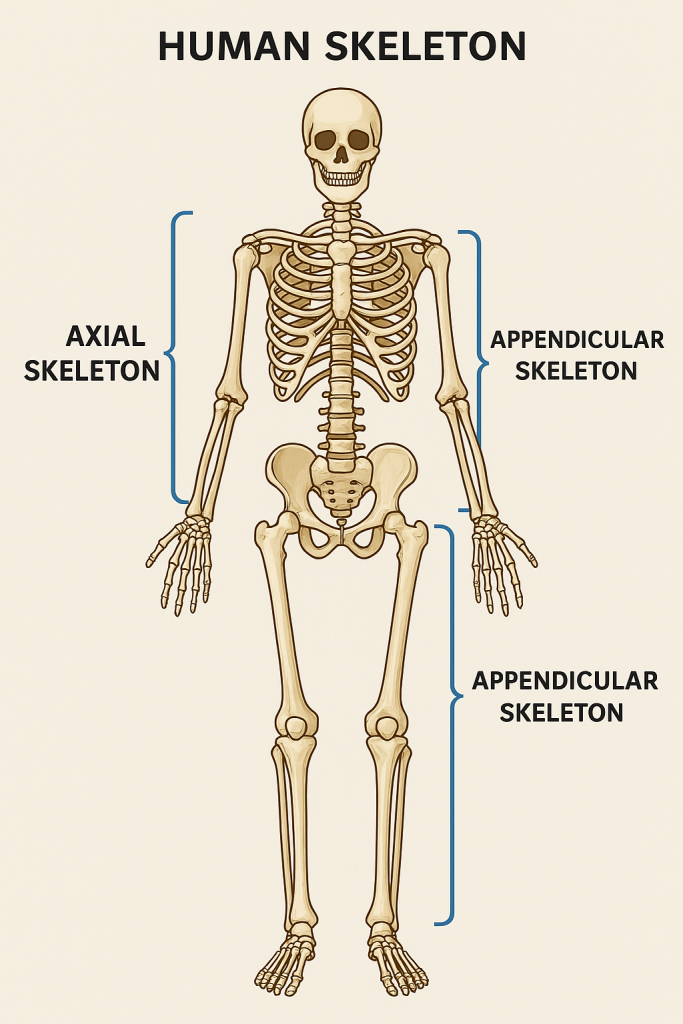
The human skeleton is a strong yet flexible framework of 206 bones (in adults). It is divided into two main parts:
- Axial Skeleton – the central core of the body
- Appendicular Skeleton – the limbs and girdles that attach to the axial skeleton
🔷 1. Axial Skeleton
📌 Definition:
The axial skeleton forms the central axis of the body and supports and protects vital organs like the brain, spinal cord, heart, and lungs.
📌 Total Bones: 80 bones
📌 Major Parts of Axial Skeleton:
🟢 A. Skull (Cranium and Facial Bones) – 22 bones
▪️ Cranium – 8 bones
Protects the brain
- Frontal (1)
- Parietal (2)
- Temporal (2)
- Occipital (1)
- Sphenoid (1)
- Ethmoid (1)
▪️ Facial Bones – 14 bones
Forms the face, holds teeth, and protects sensory organs
- Maxilla (2)
- Mandible (1)
- Zygomatic (2)
- Nasal (2)
- Lacrimal (2)
- Palatine (2)
- Inferior nasal conchae (2)
- Vomer (1)
▪️ Middle Ear Bones (Auditory Ossicles) – 6 bones (3 pairs)
- Malleus (2)
- Incus (2)
- Stapes (2)
These transmit sound vibrations.
▪️ Hyoid Bone – 1 bone
- U-shaped bone in the neck.
- Supports the tongue and aids swallowing.
- Not connected to any other bone.
🟢 B. Vertebral Column (Spine) – 26 bones
Provides support, protects the spinal cord, and allows flexibility.
- Cervical vertebrae – 7 (neck)
- Thoracic vertebrae – 12 (upper back)
- Lumbar vertebrae – 5 (lower back)
- Sacrum – 1 (formed by fusion of 5 sacral vertebrae)
- Coccyx – 1 (tailbone, fusion of 4 coccygeal vertebrae)
🟢 C. Thoracic Cage (Rib Cage) – 25 bones
Protects the heart and lungs and assists in breathing.
- Ribs – 24 (12 pairs)
- True ribs (1–7): directly attached to sternum
- False ribs (8–10): indirectly attached
- Floating ribs (11–12): no anterior attachment
- Sternum – 1 (Breastbone)
- Made up of manubrium, body, and xiphoid process
✅ Summary of Axial Skeleton:
| Part | No. of Bones | Function |
|---|---|---|
| Skull | 22 | Protects brain, supports face |
| Ear Ossicles | 6 | Transmit sound |
| Hyoid Bone | 1 | Supports tongue and throat muscles |
| Vertebral Column | 26 | Protects spinal cord, supports head |
| Rib Cage | 25 | Protects thoracic organs, respiration |
| Total | 80 bones |
🔷 2. Appendicular Skeleton
📌 Definition:
The appendicular skeleton includes all bones of the limbs and the girdles (shoulder and pelvic) that attach them to the axial skeleton.
📌 Total Bones: 126 bones
📌 Major Parts of Appendicular Skeleton
🟢 A. Pectoral (Shoulder) Girdle – 4 bones
Connects the upper limb to the axial skeleton and allows wide range of motion.
- Clavicles (Collarbones) – 2
- Scapulae (Shoulder blades) – 2
🟢 B. Upper Limbs (Arms) – 60 bones (30 per limb)
Each arm includes:
- Humerus – 1 (upper arm)
- Radius and Ulna – 2 (forearm)
- Carpals – 8 (wrist bones)
- Metacarpals – 5 (palm bones)
- Phalanges – 14 (finger bones)
🟢 C. Pelvic Girdle (Hip Bones) – 2 bones
- Composed of 2 hip bones (coxal bones).
- Each hip bone is formed by the fusion of 3 bones:
- Ilium
- Ischium
- Pubis
- Connects the lower limb to the axial skeleton.
- Supports the weight of the upper body and protects pelvic organs.
🟢 D. Lower Limbs (Legs) – 60 bones (30 per limb)
Each leg includes:
- Femur – 1 (thigh bone, longest bone)
- Patella – 1 (kneecap, a sesamoid bone)
- Tibia and Fibula – 2 (lower leg)
- Tarsals – 7 (ankle bones)
- Metatarsals – 5 (foot bones)
- Phalanges – 14 (toe bones)
✅ Summary of Appendicular Skeleton:
| Part | No. of Bones | Function |
|---|---|---|
| Shoulder Girdle | 4 | Connects arms to trunk |
| Upper Limbs | 60 | Enables arm and hand movement |
| Pelvic Girdle | 2 | Connects legs to trunk, supports pelvic organs |
| Lower Limbs | 60 | Enables leg and foot movement, weight-bearing |
| Total | 126 bones |
🔷 Comparison Table: Axial vs Appendicular Skeleton
| Feature | Axial Skeleton | Appendicular Skeleton |
|---|---|---|
| Total bones | 80 | 126 |
| Main regions | Skull, spine, rib cage | Limbs, shoulder and pelvic girdles |
| Primary functions | Protection and support | Movement and mobility |
| Bone types included | Mostly flat and irregular | Mostly long, short, and irregular bones |
| Connection to limbs | No | Yes (via girdles) |
🧠 Clinical Tip:
- Fractures of appendicular bones (e.g., femur, humerus) are common in trauma and sports injuries.
- Spinal abnormalities like scoliosis affect the axial skeleton.
- Osteoarthritis often affects appendicular joints like the knee and hip.
🤝 Joints (Articulations) – Classification
🔷 What is a Joint?
A joint is a point where two or more bones meet. Joints are essential for providing mobility, flexibility, and support to the skeletal system. Some joints allow movement, while others are designed for stability and protection.
🔷 Functions of Joints:
- Allow movement (e.g., elbow, knee)
- Provide support and structure
- Protect internal organs (e.g., joints in the rib cage)
- Hold the skeleton together
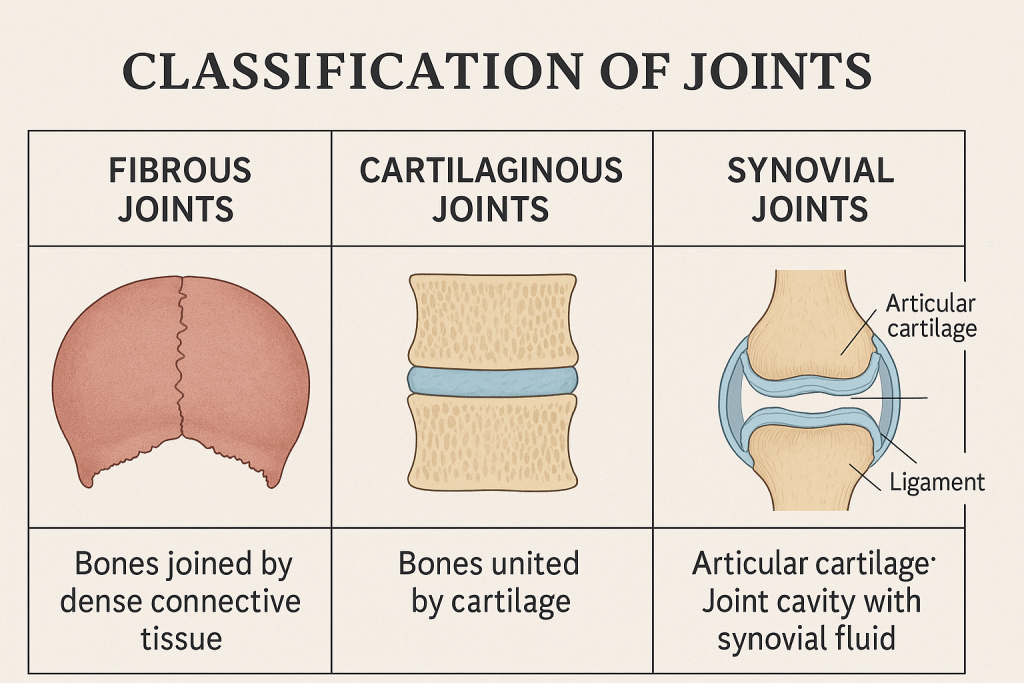
🔷 Classification of Joints
Joints can be classified in two ways:
- Structural Classification – based on the type of tissue binding bones together and whether there is a joint cavity
- Functional Classification – based on the degree of movement permitted
🧱 1. Structural Classification of Joints
There are three main types:
🔹 A. Fibrous Joints
📌 Characteristics:
- Bones are joined by dense fibrous connective tissue
- No joint cavity
- Mostly immovable (synarthrosis)
📌 Subtypes:
- Sutures – Found only in the skull; interlocking joints (e.g., coronal suture)
- Syndesmoses – Bones connected by ligaments (e.g., between radius and ulna)
- Gomphoses – Peg-in-socket joints (e.g., teeth in alveolar sockets)
📌 Function: Stability and protection
🔹 B. Cartilaginous Joints
📌 Characteristics:
- Bones connected by cartilage
- No joint cavity
- Allow limited movement (amphiarthrosis)
📌 Subtypes:
- Synchondroses – Bones united by hyaline cartilage
👉 Example: Epiphyseal plate in growing bones, first rib and sternum - Symphyses – Bones united by fibrocartilage
👉 Example: Pubic symphysis, intervertebral discs
📌 Function: Shock absorption and slight movement
🔹 C. Synovial Joints
📌 Characteristics:
- Bones are separated by a joint cavity
- Cavity filled with synovial fluid
- Most freely movable joints (diarthroses)
📌 Essential Structures of Synovial Joints:
- Articular cartilage – Covers bone ends, reduces friction
- Joint (synovial) cavity – Space filled with fluid
- Articular capsule – Double-layered; fibrous outside, synovial membrane inside
- Synovial fluid – Lubricates and nourishes cartilage
- Ligaments – Strengthen and stabilize joint
- Nerves and blood vessels – Supply nutrients and feedback
📌 Function: Free movement and flexibility
🔹 Subtypes of Synovial Joints (Based on Shape and Movement):
| Type | Description | Example |
|---|---|---|
| Plane (Gliding) | Flat surfaces glide over each other | Intercarpal joints (wrist) |
| Hinge | Flexion and extension (like a door hinge) | Elbow, knee, ankle |
| Pivot | Rotation around a single axis | Atlas-axis (neck), radioulnar joint |
| Condyloid (Ellipsoid) | Movement in two planes (flexion, extension, etc.) | Wrist joint (radiocarpal) |
| Saddle | Biaxial movement with concave-convex surfaces | Thumb joint (carpometacarpal) |
| Ball-and-Socket | Multiaxial movement in all directions | Shoulder, hip |
🔄 2. Functional Classification of Joints
Based on movement, joints are classified into:
🔹 A. Synarthroses – Immovable joints
- No movement
- Bones tightly joined
- Often fibrous joints
🦴 Examples:
- Skull sutures
- Teeth in sockets (gomphoses)
🔹 B. Amphiarthroses – Slightly movable joints
- Limited movement
- Cartilaginous joints
🦴 Examples:
- Pubic symphysis
- Intervertebral joints
🔹 C. Diarthroses – Freely movable joints
- Most common type
- Always synovial joints
🦴 Examples:
- Knee, elbow, shoulder, fingers
🔶 Clinical Relevance of Joints
- Arthritis – Inflammation of joints, causing pain and stiffness
- Osteoarthritis: Degenerative wear and tear
- Rheumatoid arthritis: Autoimmune inflammatory disease
- Dislocation – Bone slips out of the joint cavity
- Sprain – Ligament injury
- Meniscus tear – Common in knees (especially in athletes)
- Gout – Uric acid crystals in joints, causing pain
✅
| Classification | Types | Movement |
|---|---|---|
| Structural | Fibrous, Cartilaginous, Synovial | Based on tissue & cavity |
| Functional | Synarthrosis, Amphiarthrosis, Diarthrosis | Based on mobility |
🤝 Major Joints of the Human Body – Structure in Detail
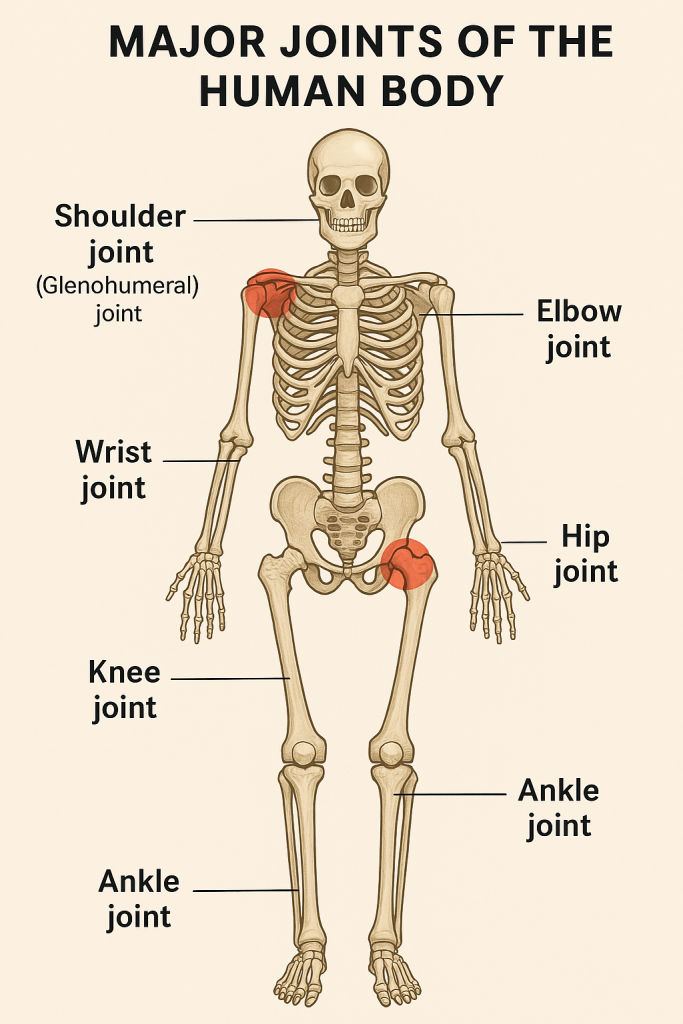
The body has many joints, but some are classified as major joints due to their complexity, size, range of motion, and clinical importance.
🔷 1. Shoulder Joint (Glenohumeral Joint)
📌 Type:
- Ball-and-socket synovial joint
📌 Bones Involved:
- Humerus (head)
- Scapula (glenoid cavity)
📌 Structure:
- Joint capsule: Thin and loose → allows wide movement
- Glenoid labrum: Fibrocartilage ring that deepens the socket
- Ligaments: Coracohumeral and glenohumeral ligaments
- Rotator cuff muscles: Provide dynamic stability (SITS – Supraspinatus, Infraspinatus, Teres minor, Subscapularis)
📌 Movements:
- Flexion, extension, abduction, adduction, rotation, circumduction
🩺 Clinical Note:
- Most mobile and most dislocated joint in the body due to shallow socket
🔷 2. Elbow Joint
📌 Type:
- Hinge synovial joint
📌 Bones Involved:
- Humerus, Ulna, Radius
📌 Structure:
- Humeroulnar joint: True hinge joint
- Joint capsule: Thick and reinforced by ligaments
- Ligaments: Ulnar and radial collateral ligaments
- Annular ligament: Holds head of radius for rotation
📌 Movements:
- Flexion, extension; (forearm rotation occurs at radioulnar joint)
🩺 Clinical Note:
- Tennis elbow (lateral epicondylitis) affects tendons near the elbow
🔷 3. Wrist Joint (Radiocarpal Joint)
📌 Type:
- Condyloid (ellipsoid) synovial joint
📌 Bones Involved:
- Radius, Scaphoid, Lunate (not ulna directly)
📌 Structure:
- Joint capsule: Surrounds the wrist
- Ligaments: Palmar, dorsal, and collateral ligaments
- Disc: Separates ulna from wrist bones
📌 Movements:
- Flexion, extension, abduction (radial deviation), adduction (ulnar deviation), circumduction
🩺 Clinical Note:
- Common site for fractures (e.g., Colles’ fracture)
🔷 4. Hip Joint (Acetabulofemoral Joint)
📌 Type:
- Ball-and-socket synovial joint
📌 Bones Involved:
- Femoral head, Acetabulum of the pelvis
📌 Structure:
- Deep socket compared to shoulder
- Acetabular labrum: Fibrocartilage ring for socket depth
- Strong ligaments: Iliofemoral (Y-shaped), pubofemoral, ischiofemoral
- Joint capsule: Thick and strong
- Muscles: Gluteals, hip flexors, adductors
📌 Movements:
- Flexion, extension, abduction, adduction, rotation, circumduction
🩺 Clinical Note:
- Fracture neck of femur is common in elderly (can cause avascular necrosis)
- Site for hip replacements
🔷 5. Knee Joint (Tibiofemoral Joint)
📌 Type:
- Modified hinge synovial joint
📌 Bones Involved:
- Femur, Tibia, and Patella
📌 Structure:
- Menisci (medial and lateral): C-shaped cartilage that cushions the joint
- Ligaments:
- ACL (Anterior Cruciate Ligament)
- PCL (Posterior Cruciate Ligament)
- MCL (Medial Collateral Ligament)
- LCL (Lateral Collateral Ligament)
- Patellar ligament: Connects patella to tibia
- Joint capsule and synovial membrane
📌 Movements:
- Flexion, extension, slight rotation when flexed
🩺 Clinical Note:
- Common site for sports injuries, especially ACL tears
- Meniscus tears, arthritis, and bursitis are also frequent
🔷 6. Ankle Joint (Talocrural Joint)
📌 Type:
- Hinge synovial joint
📌 Bones Involved:
- Tibia, Fibula, Talus
📌 Structure:
- Joint capsule: Thin but reinforced
- Ligaments:
- Deltoid ligament (medial)
- Lateral ligaments (anterior/posterior talofibular, calcaneofibular)
📌 Movements:
- Dorsiflexion (toes up)
- Plantarflexion (toes down)
🩺 Clinical Note:
- Common site for sprains, especially lateral ligament injury
🔷 7. Temporomandibular Joint (TMJ)
📌 Type:
- Modified hinge synovial joint
📌 Bones Involved:
- Mandible (condylar process)
- Temporal bone
📌 Structure:
- Articular disc between bones
- Ligaments: Lateral ligament, sphenomandibular, stylomandibular
- Muscles: Masseter, temporalis, pterygoids
📌 Movements:
- Elevation, depression (open/close jaw)
- Protraction, retraction
- Lateral movement (chewing)
🩺 Clinical Note:
- TMJ disorders can cause jaw pain, clicking, and headache
✅
| Joint | Type | Bones Involved | Main Movements |
|---|---|---|---|
| Shoulder | Ball-and-socket | Humerus, Scapula | All directions |
| Elbow | Hinge | Humerus, Ulna, Radius | Flexion, extension |
| Wrist | Condyloid | Radius, Carpal bones | Flexion, extension, deviation |
| Hip | Ball-and-socket | Femur, Pelvis | All directions |
| Knee | Modified hinge | Femur, Tibia, Patella | Flexion, extension, rotation |
| Ankle | Hinge | Tibia, Fibula, Talus | Dorsiflexion, plantarflexion |
| TMJ | Modified hinge | Mandible, Temporal bone | Jaw movements |
🦴🧠 Musculoskeletal System – Applications and Implications in Nursing
🔷 What is the Musculoskeletal System?
The musculoskeletal system is composed of:
- Bones
- Joints
- Muscles
- Tendons
- Ligaments
- Cartilage
Together, they enable movement, stability, posture, and protection of vital organs. It also contributes to blood cell production and mineral storage (especially calcium and phosphorus).
🔶 Applications of Musculoskeletal Knowledge in Nursing
Understanding the musculoskeletal system is critical in many aspects of nursing care, such as:
🟢 1. Patient Assessment
Nurses must assess:
- Posture and gait
- Muscle strength
- Joint mobility and alignment
- Presence of pain, swelling, or deformity
🔍 Tools:
- Goniometers for joint angle
- Pain scale assessments
- Manual Muscle Testing (MMT)
🟢 2. Immobilization and Mobility Care
Nurses often deal with:
- Patients on bed rest
- Use of splints, traction, braces, plasters, or orthopedic devices
🔑 Nursing Role:
- Prevent complications of immobility (e.g., pressure sores, deep vein thrombosis)
- Assist with ROM (Range of Motion) exercises
- Turn and reposition patients regularly
🟢 3. Orthopedic Nursing Care
Conditions include:
- Fractures, dislocations
- Arthritis
- Osteoporosis
- Back injuries
- Joint replacements (hip/knee)
👩⚕️ Nursing responsibilities:
- Pain management
- Wound care and monitoring for infection
- Neurovascular assessments (CMS check: Circulation, Movement, Sensation)
- Assisting in mobility aids and rehabilitation
🟢 4. Medication Administration
Nurses administer:
- Analgesics (e.g., NSAIDs for pain)
- Muscle relaxants
- Calcium and Vitamin D supplements
- Steroids in inflammatory conditions
- Anti-resorptives for osteoporosis
⚠️ Caution:
- Monitor for side effects like GI irritation (NSAIDs)
- Educate about compliance and timing
🟢 5. Patient Education & Rehabilitation
🧑🏫 Nurses educate patients and families on:
- Safe use of mobility aids (crutches, walkers)
- Fall prevention at home
- Diet rich in calcium and protein
- Exercise routines for strengthening muscles and joints
- Post-surgery care (especially after joint replacements)
🔶 B. Common Nursing Diagnoses Related to the Musculoskeletal System
- Impaired physical mobility related to pain or injury
- Risk for falls due to weak muscles or poor balance
- Acute or chronic pain related to inflammation or trauma
- Self-care deficit due to joint stiffness or muscle weakness
- Impaired skin integrity due to immobility
- Risk of infection in post-op orthopedic patients
🔶 C. Complications Nurses Help Prevent
| 🔴 Complication | 🧑⚕️ Nursing Intervention |
|---|---|
| Pressure ulcers | Regular turning, pressure-relieving surfaces |
| Muscle atrophy | ROM exercises, active/passive mobilization |
| Joint contractures | Splinting, repositioning, ROM |
| Deep vein thrombosis (DVT) | Early ambulation, compression stockings |
| Constipation | High-fiber diet, hydration, mobility |
| Respiratory issues | Deep breathing exercises, incentive spirometry |
🔶 D. Emergency Musculoskeletal Situations Nurses Face
- Fractures with bleeding or deformity
- Spinal cord injury with paralysis
- Compartment syndrome (pain, pallor, pulselessness – surgical emergency!)
- Dislocations or trauma
- Sudden loss of movement or sensation
🆘 Nurses must:
- Quickly assess circulation and neurological function
- Immobilize the area
- Prepare for emergency interventions
✅ Summary: Role of Nursing in Musculoskeletal System
| 🏥 Area | 💡 Nursing Role |
|---|---|
| Assessment | Observe posture, joint movement, muscle strength |
| Mobility | Prevent complications, assist with transfers |
| Pain Management | Monitor and manage pain levels |
| Education | Teach exercises, fall safety, medication adherence |
| Rehabilitation | Encourage independence, use of assistive devices |
| Surgical Care | Wound care, neurovascular checks, infection signs |
🧠 Clinical Tip:
When caring for an orthopedic or immobilized patient, remember the “6 P’s of Neurovascular Assessment”:
- Pain
- Pallor
- Pulselessness
- Paresthesia (tingling)
- Paralysis
- Poikilothermia (temperature changes)
💪 Structure of Muscles
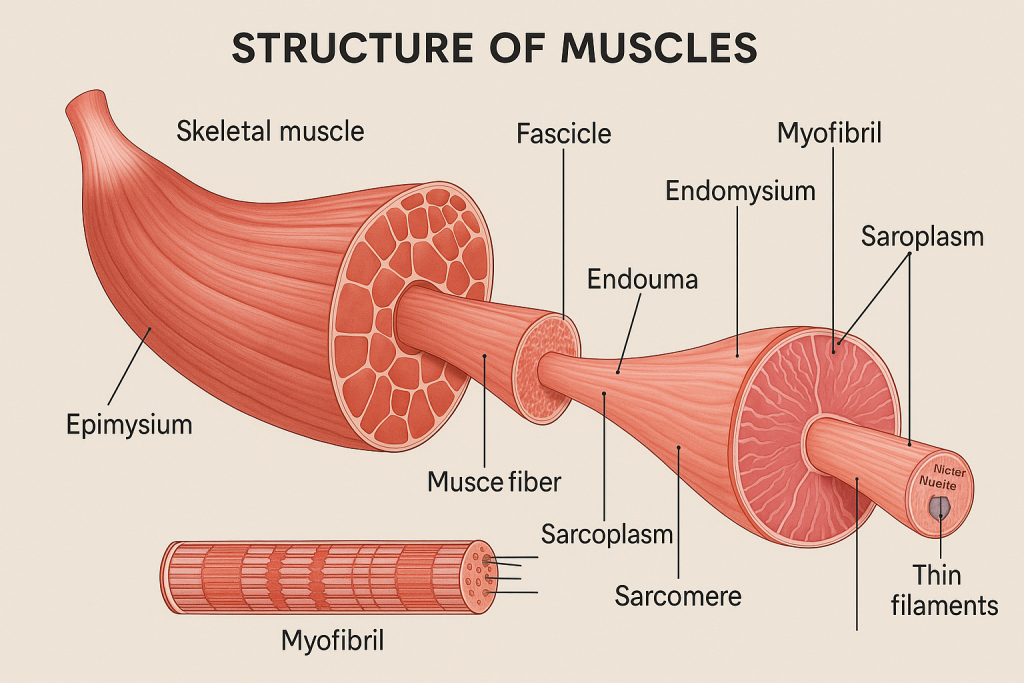
🔷 What are Muscles?
Muscles are specialized contractile tissues that allow movement, posture, and heat production in the body. They are made of muscle fibers (cells) bundled together and attached to bones, skin, or other muscles.
🔶 Types of Muscles in the Body:
- Skeletal Muscle – Voluntary, striated, attached to bones
- Cardiac Muscle – Involuntary, striated, found only in the heart
- Smooth Muscle – Involuntary, non-striated, found in organs (e.g., intestines, blood vessels)
💡 This explanation focuses mainly on skeletal muscle structure, which is most relevant in the musculoskeletal system.
🔷 A. Gross Structure of Skeletal Muscle (Macroscopic)
From outside to inside, skeletal muscles are arranged in layers:
🟣 1. Muscle (Organ Level)
- Surrounded by a connective tissue sheath called epimysium
- Contains bundles of muscle fascicles
🟣 2. Fascicle
- A bundle of muscle fibers (cells)
- Surrounded by perimysium (connective tissue)
🟣 3. Muscle Fiber (Muscle Cell)
- Long, cylindrical, multinucleated cell
- Surrounded by endomysium
- Contain multiple myofibrils
📌 All three layers (epimysium, perimysium, endomysium) merge at the ends to form tendons, which attach muscle to bone.
🔷 B. Microscopic Structure of Skeletal Muscle
Now let’s zoom in at the cellular and sub-cellular level:
🟢 1. Muscle Fiber (Cell)
- Long cylindrical cell, up to 30 cm
- Multiple nuclei located at the periphery
- Sarcolemma – Cell membrane
- Sarcoplasm – Cytoplasm, contains mitochondria, glycogen, and myoglobin
🟢 2. Myofibrils
- Thread-like structures that run the length of the fiber
- Contain contractile proteins arranged into repeating units called sarcomeres
🟢 3. Sarcomere – Basic Contractile Unit
- Region between two Z-lines
- Contains thick filaments (myosin) and thin filaments (actin)
- Other proteins: troponin and tropomyosin regulate contraction
✅ Bands of Sarcomere:
- A band – Dark band (myosin + actin overlap)
- I band – Light band (actin only)
- H zone – Center of A band (myosin only)
- M line – Center of sarcomere (holds myosin in place)
🔁 During contraction, the sarcomere shortens, bringing Z-lines closer, causing the entire muscle to contract.
🔷 C. Other Important Structures
🔸 1. Sarcoplasmic Reticulum (SR)
- Specialized smooth ER that stores and releases calcium ions (Ca²⁺) needed for muscle contraction
🔸 2. T-Tubules (Transverse Tubules)
- Invaginations of the sarcolemma that carry the action potential deep into the cell
🔸 3. Mitochondria
- “Powerhouse” organelles that generate ATP, essential for muscle contraction
🔶 Summary Table: Structure of Skeletal Muscle
| Level | Structure | Covering |
|---|---|---|
| Muscle (Organ) | Whole muscle | Epimysium |
| Fascicle | Bundle of fibers | Perimysium |
| Muscle Fiber | Muscle cell | Endomysium |
| Myofibril | Thread within fiber | No covering |
| Sarcomere | Functional unit | Between Z-lines |
| Myofilaments | Actin & Myosin | Inside sarcomere |
🔷 D. Nerve and Blood Supply
- Motor neurons stimulate muscle fibers via neuromuscular junctions
- Each muscle fiber is innervated by a branch of a motor neuron
- Muscles are highly vascular – rich blood supply provides oxygen and nutrients, removes waste
🔷 E. Muscle Contraction (Brief Overview)
- Nerve impulse reaches neuromuscular junction
- Acetylcholine (ACh) is released, depolarizing sarcolemma
- Calcium is released from SR
- Calcium binds to troponin, moving tropomyosin away from actin’s binding sites
- Myosin heads bind to actin → form cross-bridges
- ATP is used → muscle fiber shortens (contracts)
- When stimulation ends → calcium is pumped back, muscle relaxes
🧠 Clinical Relevance for Nurses
| 🩺 Condition | 💡 Muscle Relevance |
|---|---|
| Muscle Atrophy | Due to immobilization or malnutrition |
| Muscle Spasm or Cramp | Electrolyte imbalance (e.g., calcium, potassium) |
| Muscular Dystrophy | Genetic muscle-wasting disorders |
| Myasthenia Gravis | Autoimmune – affects neuromuscular transmission |
| Rhabdomyolysis | Breakdown of muscle tissue → releases myoglobin → kidney damage |
| IM Injections | Knowledge of muscle layers essential for safe administration (e.g., deltoid, gluteus medius) |
✅
- Skeletal muscle is a well-organized tissue made of fibers, fascicles, and functional units (sarcomeres).
- Understanding the layers and function helps in clinical assessment, mobility care, injections, and identifying muscular disorders.
- Muscle health is vital for overall mobility, independence, and recovery.
💪🧠 Types of Muscles in the Human Body
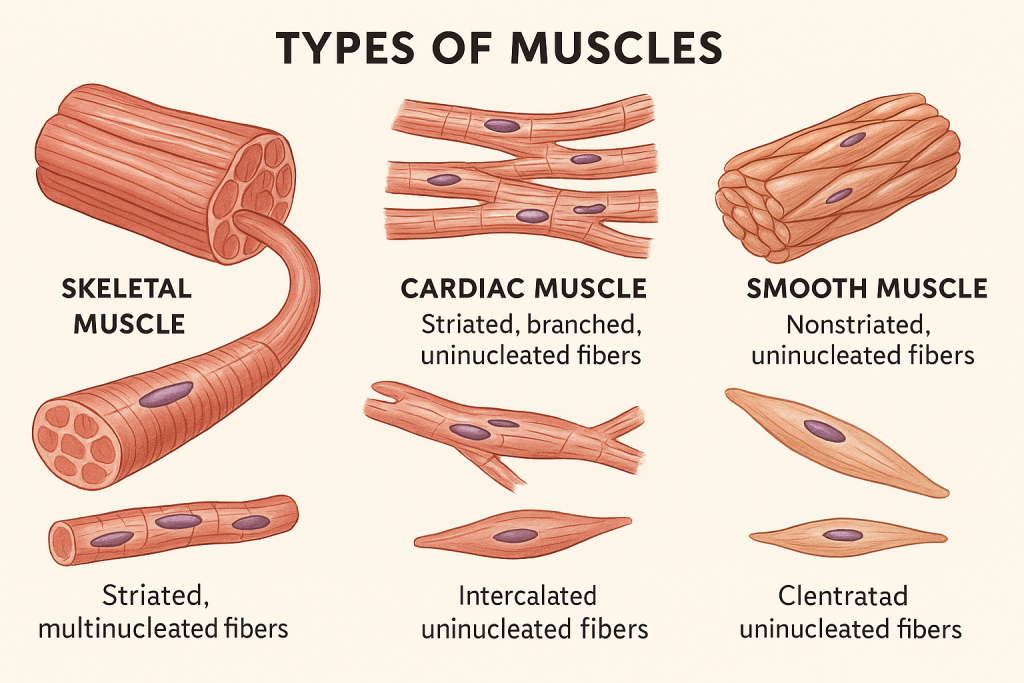
The human body contains three main types of muscle tissue, each with unique features, structure, and function.
🔷 1. Skeletal Muscle
📌 Overview:
- Voluntary, striated muscle
- Controlled by the somatic nervous system
- Attached to bones via tendons
- Responsible for movement, posture, and heat production
🔬 Structure:
- Long, cylindrical, multinucleated fibers
- Striations (alternating dark and light bands) visible under microscope
- Organized into fascicles, surrounded by connective tissue (epimysium, perimysium, endomysium)
⚙️ Function:
- Voluntary movements (walking, lifting)
- Maintains posture
- Produces body heat during contraction
- Supports joints
📍 Location:
- Arms, legs, face, tongue, diaphragm, abdominal wall, etc.
🩺 Clinical Relevance:
- Muscle atrophy (wasting) from inactivity or disease
- Tetanus: uncontrolled contraction due to bacterial toxin
- Myasthenia gravis: autoimmune condition affecting muscle strength
- Injection site for IM injections (e.g., deltoid, gluteus medius)
🔷 2. Cardiac Muscle
📌 Overview:
- Involuntary, striated muscle
- Found only in the heart
- Controlled by the autonomic nervous system and intrinsic pacemaker (SA node)
🔬 Structure:
- Branched, cylindrical fibers
- Single central nucleus
- Striated like skeletal muscle
- Connected by intercalated discs with gap junctions and desmosomes for synchronized contraction
⚙️ Function:
- Pumps blood throughout the body
- Automatic rhythmic contraction (does not fatigue like skeletal muscle)
📍 Location:
- Wall of the heart (myocardium) only
🩺 Clinical Relevance:
- Myocardial infarction (heart attack): death of cardiac muscle cells due to oxygen loss
- Arrhythmias: irregular electrical activity in cardiac muscle
- Cardiomyopathy: disease of cardiac muscle function
🔷 3. Smooth Muscle
📌 Overview:
- Involuntary, non-striated muscle
- Controlled by the autonomic nervous system
- Found in walls of hollow organs and blood vessels
🔬 Structure:
- Spindle-shaped cells
- Single central nucleus
- No striations (smooth appearance)
- Cells arranged in sheets
⚙️ Function:
- Moves substances through organs (peristalsis in GI tract)
- Constricts or dilates blood vessels and airways
- Controls functions like urination, childbirth, and digestion
📍 Location:
- Walls of digestive tract, blood vessels, urinary bladder, uterus, respiratory tract, iris of the eye
🩺 Clinical Relevance:
- Asthma: bronchial smooth muscle spasm
- Hypertension: smooth muscle overactivity in arteries
- Irritable Bowel Syndrome (IBS): abnormal smooth muscle contractions
✅ Summary Comparison Table
| Feature | Skeletal Muscle | Cardiac Muscle | Smooth Muscle |
|---|---|---|---|
| Control | Voluntary | Involuntary | Involuntary |
| Striations | Present | Present | Absent |
| Shape of Cells | Long, cylindrical | Branched | Spindle-shaped |
| Nucleus per Cell | Multiple (peripheral) | Single (central) | Single (central) |
| Location | Attached to bones | Heart wall (myocardium) | Walls of hollow organs and vessels |
| Function | Movement, posture, heat | Pumping blood | Movement of substances (peristalsis) |
| Special Features | Quick to contract, tires easily | Self-exciting, rhythmic contraction | Slow, sustained contraction |
🧠 Mnemonic to Remember Muscle Types:
“SCS” – Skeletal, Cardiac, Smooth
- Skeletal – Strong, Striated, Somatic
- Cardiac – Central nucleus, Conductive, Constant contraction
- Smooth – Slow, Single nucleus, Spindle-shaped
🩺 Nursing Implications:
| Situation | Muscle Type Involved | Nurse’s Role |
|---|---|---|
| IM Injection | Skeletal | Know muscle sites (deltoid, vastus lateralis) |
| Post-op abdominal surgery | Smooth | Monitor for bowel sounds, peristalsis recovery |
| Cardiac monitoring post-MI | Cardiac | Monitor ECG, heart rate, oxygenation |
| Asthma or COPD | Smooth | Administer bronchodilators to relax airways |
| Fracture or immobilization | Skeletal | Prevent atrophy via ROM exercises |
💀💪 Muscle Groups – Muscles of the Head
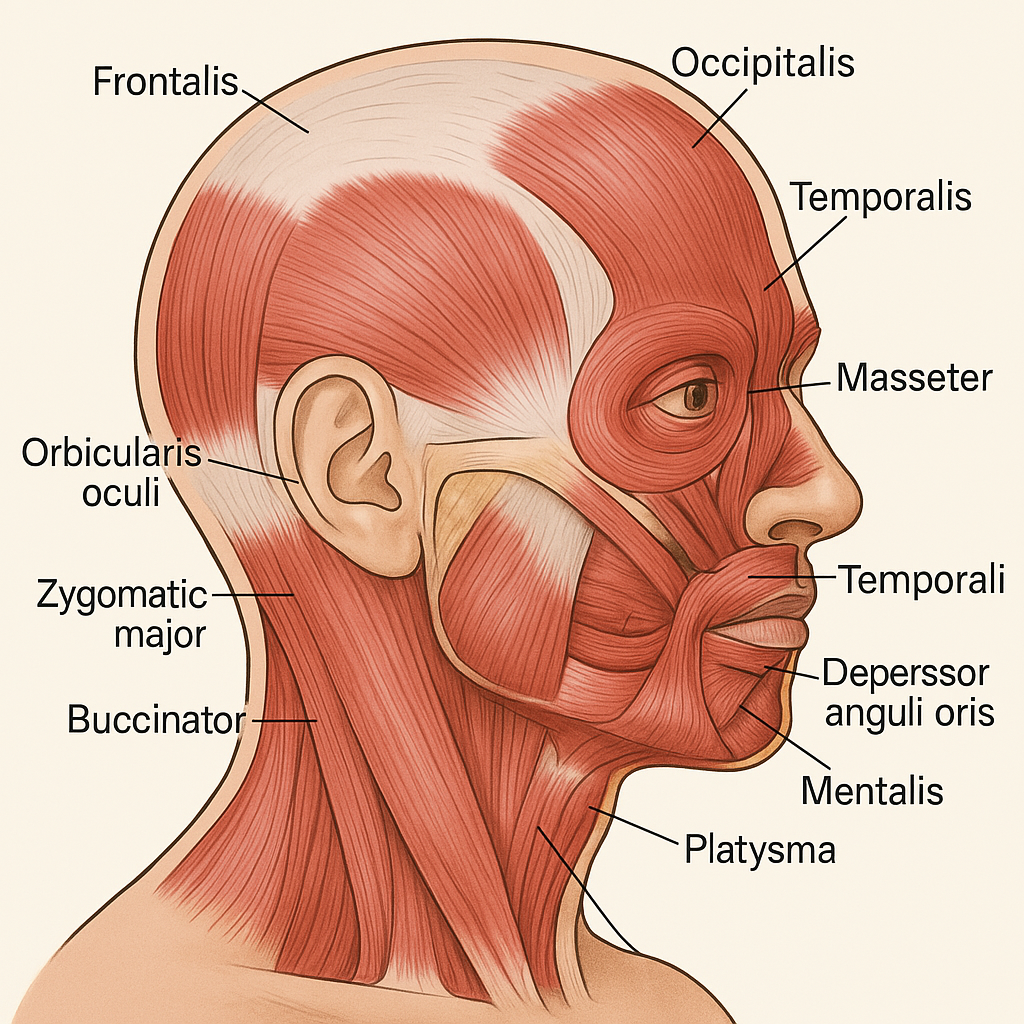
🔷
Muscles of the head are grouped into the following categories:
- Muscles of facial expression
- Muscles of mastication (chewing)
- Extraocular muscles (eye movement)
- Muscles of the tongue
- Muscles of the scalp and ears (minor group)
These muscles are paired, thin, and mostly originate from bone and insert into the skin or other soft tissue—especially for facial expression.
🔶 1. Muscles of Facial Expression
📌 Function:
- Control facial movements: smiling, frowning, blinking, puckering lips
- Innervated by the facial nerve (cranial nerve VII)
| Muscle | Location/Action |
|---|---|
| Frontalis | Forehead; raises eyebrows and wrinkles forehead |
| Occipitalis | Back of skull; pulls scalp backward |
| Orbicularis oculi | Surrounds the eye; closes the eyelids (blinking, squinting) |
| Orbicularis oris | Surrounds the mouth; closes and puckers lips (kissing) |
| Zygomaticus major/minor | Cheek; pulls mouth upward and laterally (smiling) |
| Buccinator | Cheek; compresses cheek (blowing, sucking) |
| Levator labii superioris | Raises upper lip |
| Depressor anguli oris | Pulls corner of mouth downward (frowning) |
| Mentalis | Chin; protrudes lower lip (pouting) |
| Platysma | Neck; tenses skin of neck and lowers jaw slightly |
💡 Damage to the facial nerve (e.g., Bell’s palsy) causes facial asymmetry and inability to move facial muscles on one side.
🔶 2. Muscles of Mastication (Chewing)
📌 Function:
- Move the mandible (jaw) to allow chewing
- Innervated by the mandibular branch of the trigeminal nerve (cranial nerve V3)
| Muscle | Function |
|---|---|
| Masseter | Elevates mandible (closes jaw); very strong |
| Temporalis | Elevates and retracts mandible |
| Medial pterygoid | Elevates mandible; side-to-side movement |
| Lateral pterygoid | Protrudes mandible; opens jaw slightly; side-to-side movement |
🦷 These muscles are essential for biting, grinding, and speaking.
🔶 3. Extraocular Muscles (Eye Movement)
📌 Function:
- Control precise movements of the eyeball
- Innervated by cranial nerves III (oculomotor), IV (trochlear), and VI (abducens)
| Muscle | Function | Nerve |
|---|---|---|
| Superior rectus | Elevates the eye (looks up) | CN III |
| Inferior rectus | Depresses the eye (looks down) | CN III |
| Medial rectus | Moves eye medially (toward nose) | CN III |
| Lateral rectus | Moves eye laterally (toward ear) | CN VI |
| Superior oblique | Rotates eye down and outward | CN IV |
| Inferior oblique | Rotates eye up and outward | CN III |
🧠 Damage to these nerves can result in double vision (diplopia) or eye misalignment (strabismus).
🔶 4. Muscles of the Tongue (Intrinsic and Extrinsic)
📌 Function:
- Aid in speaking, chewing, and swallowing
- Innervated mainly by hypoglossal nerve (cranial nerve XII)
🔹 Intrinsic Muscles:
- Located within the tongue
- Change shape (lengthen, shorten, curl, flatten)
🔹 Extrinsic Muscles:
| Muscle | Function |
|---|---|
| Genioglossus | Protrudes and depresses tongue |
| Hyoglossus | Depresses and retracts tongue |
| Styloglossus | Elevates and retracts tongue |
| Palatoglossus | Elevates posterior tongue (CN X – vagus) |
👅 Damage to hypoglossal nerve causes the tongue to deviate toward the paralyzed side.
🔶 5. Minor Groups: Scalp and Auricular Muscles
📌 Include:
- Auricular muscles (move ears – mostly non-functional in humans)
- Occipitofrontalis (Frontalis + Occipitalis): raises eyebrows, moves scalp
✅ Summary: Muscle Groups of the Head
| Group | Key Muscles | Main Nerve | Primary Function |
|---|---|---|---|
| Facial Expression | Orbicularis oculi, oris, zygomaticus, buccinator | Facial nerve (VII) | Smile, frown, blink, talk |
| Mastication | Masseter, temporalis, pterygoids | Trigeminal nerve (V3) | Chewing |
| Eye Movement | Rectus and oblique muscles | CN III, IV, VI | Move eyeballs |
| Tongue Muscles | Genioglossus, hyoglossus, etc. | Hypoglossal nerve (XII) | Swallowing, speech |
| Scalp & Ear | Occipitofrontalis, auriculars | Facial nerve (VII) | Raise eyebrows, move scalp |
🩺 Nursing/Clinical Relevance:
- Stroke patients often lose facial muscle control on one side.
- Bell’s palsy affects muscles of facial expression.
- Trigeminal neuralgia causes pain during chewing or touching the face.
- Cranial nerve assessments involve checking eye movements, facial symmetry, and tongue position.
- Speech therapy, facial physiotherapy, and oral hygiene depend on knowledge of head muscles.
🧠💪 Neck and Head-Associated Muscles
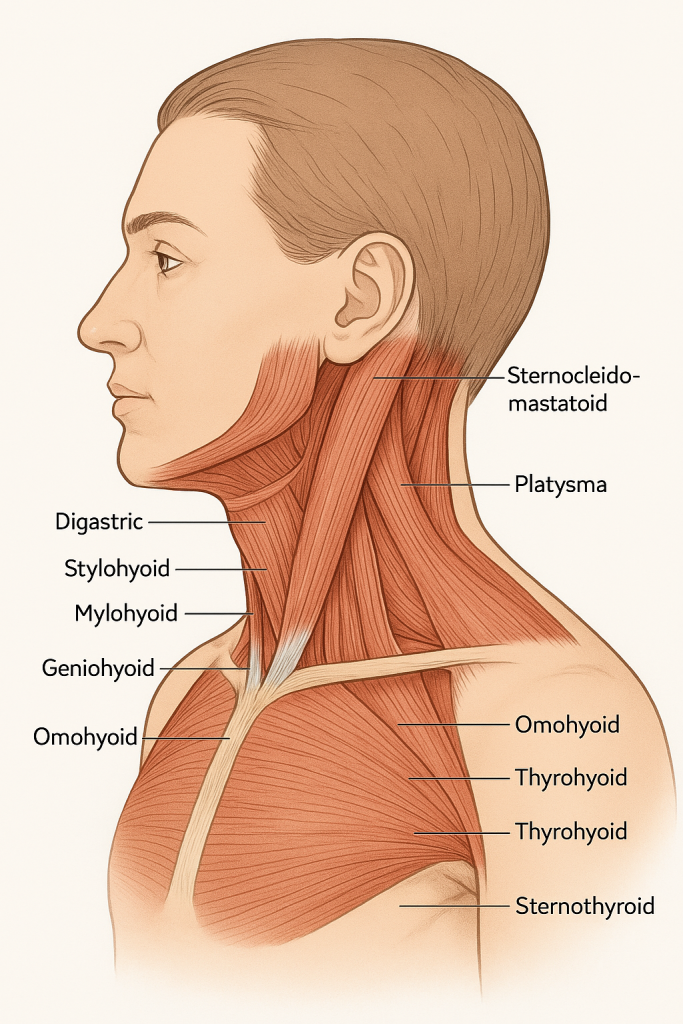
🔷
The neck contains superficial and deep muscles, organized into functional groups based on their actions and locations:
- Superficial Neck Muscles
- Muscles of the Anterior Triangle
- Muscles of the Posterior Triangle
- Suprahyoid Muscles
- Infrahyoid Muscles
- Deep Neck Flexors
- Suboccipital Muscles (connect head to upper cervical spine)
🔶 1. Superficial Neck Muscles
🔹 A. Sternocleidomastoid (SCM)
- Origin: Manubrium of sternum & clavicle
- Insertion: Mastoid process of the temporal bone
- Function:
- Unilateral: Turns head to opposite side
- Bilateral: Flexes the neck forward
- Innervation: Accessory nerve (CN XI)
📌 Clinically visible; palpated during neck movement exams
🔹 B. Platysma
- Thin, sheet-like muscle in superficial fascia of neck
- Origin: Chest and shoulder fascia
- Insertion: Lower jaw and skin around mouth
- Function: Tenses neck skin, depresses lower jaw and lip (expression of horror/fear)
- Innervation: Facial nerve (CN VII)
🔶 2. Muscles of the Anterior Triangle of the Neck
This triangle contains hyoid-related muscles important for swallowing and speech.
🔷 A. Suprahyoid Muscles (Above the hyoid bone)
| Muscle | Function | Innervation |
|---|---|---|
| Digastric | Elevates hyoid and depresses mandible | Anterior belly: CN V3; Posterior belly: CN VII |
| Mylohyoid | Elevates hyoid and floor of mouth | Mandibular nerve (CN V3) |
| Stylohyoid | Elevates and retracts hyoid | Facial nerve (CN VII) |
| Geniohyoid | Pulls hyoid forward | Cervical nerve C1 (via CN XII) |
📌 Help in initiating swallowing, stabilizing hyoid during speech.
🔷 B. Infrahyoid Muscles (Below the hyoid bone)
Also called “strap muscles“; depress the hyoid and larynx after swallowing.
| Muscle | Function | Innervation |
|---|---|---|
| Sternohyoid | Depresses hyoid | Ansa cervicalis (C1-C3) |
| Omohyoid | Depresses and stabilizes hyoid | Ansa cervicalis |
| Sternothyroid | Depresses larynx | Ansa cervicalis |
| Thyrohyoid | Depresses hyoid or elevates larynx | C1 via hypoglossal nerve (CN XII) |
📌 Vital for voice modulation, breathing, airway protection.
🔶 3. Muscles of the Posterior Triangle of the Neck
These muscles assist in neck rotation, lateral flexion, and shoulder movement.
| Muscle | Function |
|---|---|
| Trapezius | Elevates, retracts scapula; extends neck |
| Splenius capitis | Rotates and extends head |
| Levator scapulae | Elevates scapula, bends neck laterally |
| Scalenes (anterior, middle, posterior) | Flex and rotate neck; assist in inspiration by elevating ribs |
🧠 The brachial plexus and subclavian artery pass between anterior and middle scalene muscles.
🔶 4. Deep Neck Flexors (Prevertebral Muscles)
These muscles are deep to the trachea and vertebral column.
| Muscle | Function |
|---|---|
| Longus colli | Flexes neck and rotates head |
| Longus capitis | Flexes head |
| Rectus capitis anterior/lateralis | Fine head movements; stabilization |
Important in posture and cervical spine stability
🔶 5. Suboccipital Muscles (at base of skull)
| Muscle | Function |
|---|---|
| Rectus capitis posterior major/minor | Extends and rotates head |
| Obliquus capitis superior/inferior | Tilts and rotates head |
Involved in head posture, proprioception, and headache patterns.
✅ Summary Table: Neck Muscles by Function
| Function | Muscle Groups |
|---|---|
| Neck flexion | SCM (bilateral), scalene anterior, longus colli |
| Neck extension | Splenius capitis, trapezius, suboccipitals |
| Neck rotation | SCM (unilateral), scalenes, splenius |
| Larynx & hyoid control | Suprahyoid and infrahyoid muscles |
| Swallowing/speech | Mylohyoid, digastric, geniohyoid, thyrohyoid |
| Breathing support | Scalenes (elevate ribs) |
| Facial expression | Platysma |
🩺 Clinical Relevance for Nursing and Medicine:
- Neck muscle spasm → Torticollis (wry neck)
- Neck surgery or trauma may injure CN XI → shoulder droop (trapezius)
- Difficulty swallowing (dysphagia) → suggests suprahyoid/infrahyoid dysfunction
- Whiplash injuries affect deep neck flexors
- Airway management involves knowledge of neck anatomy for intubation and tracheostomy
🫁 Muscle Groups of the Thorax
The thorax, or chest region, is not only a protective cage for vital organs like the heart and lungs but also a dynamic structure involved in breathing and upper body movement. The muscles of the thorax are categorized based on their location, function, and role in respiration. These muscles work in perfect harmony to enable essential actions like inspiration, expiration, and movement of the trunk and upper limbs.
1️⃣ Muscles of the Thoracic Wall
These muscles are located between and around the ribs, forming the chest wall. They play a crucial role in stabilizing the ribs and facilitating the movement of the ribcage during respiration.
🔹 External Intercostal Muscles
These are situated between the ribs and run obliquely downward and forward from the rib above to the rib below. Their primary function is to elevate the ribs during inspiration, increasing the volume of the thoracic cavity. These muscles are active mainly during quiet and deep breathing.
🔹 Internal Intercostal Muscles
Lying just deep to the external intercostals, these fibers run in the opposite direction – downward and backward. They help to depress the ribs during forced expiration, such as during exercise or coughing.
🔹 Innermost Intercostals
These are the deepest intercostal muscles and act similarly to the internal intercostals. They also aid in forced expiration, though their contribution is relatively minor.
🔹 Subcostal Muscles
These are found mostly on the lower part of the posterior thoracic wall. They span more than one intercostal space and assist in depressing the ribs, contributing to expiration.
🔹 Transversus Thoracis
This thin muscle lies on the inner surface of the anterior thoracic wall. It extends from the sternum to the costal cartilages of the ribs and helps to pull the rib cartilages downward, aiding in expiration.
2️⃣ Muscles of Respiration
Breathing is a mechanical process that requires the coordinated contraction of muscles. These are divided into primary and accessory respiratory muscles.
🔹 Primary Muscle of Respiration – The Diaphragm
The diaphragm is the most important muscle for breathing. It is a dome-shaped muscular partition between the thoracic and abdominal cavities. Upon contraction, it flattens and moves downward, increasing thoracic volume and drawing air into the lungs. It is innervated by the phrenic nerve (C3–C5).
🔹 Accessory Muscles of Inspiration
These muscles are recruited during labored or deep breathing, such as during exercise, respiratory distress, or illness:
- Sternocleidomastoid (SCM): Elevates the sternum, thus increasing thoracic volume.
- Scalenes (anterior, middle, posterior): Elevate the first and second ribs.
- Pectoralis Major and Minor: Help elevate the chest when the arms are fixed.
- Serratus Anterior: Aids in rib elevation, especially when the scapula is stabilized.
- Latissimus Dorsi: Assists in deep expiration and stabilization of the back.
These muscles are not active during normal, quiet breathing but are essential in forced breathing.
3️⃣ Posterior Thoracic Muscles Influencing Respiration
Although primarily back muscles, some of them assist with thoracic movement and breathing:
- Serratus Posterior Superior: Helps elevate the upper ribs during deep inspiration.
- Serratus Posterior Inferior: Assists in pulling the lower ribs downward, aiding forced expiration.
- Erector Spinae Group (Iliocostalis, Longissimus, Spinalis): These long muscles of the back help extend the spine and maintain posture. They indirectly support respiration by stabilizing the thoracic cage.
4️⃣ Summary of Muscle Roles in Respiration
| Phase of Breathing | Muscles Involved |
|---|---|
| Quiet Inspiration | Diaphragm, External Intercostals |
| Forced Inspiration | SCM, Scalenes, Pectorals, Serratus Anterior |
| Quiet Expiration | Passive (elastic recoil of lungs) |
| Forced Expiration | Internal Intercostals, Abdominals, Serratus Posterior Inferior |
🩺 Clinical Relevance
- Damage to the phrenic nerve (e.g., during surgery or trauma) can cause diaphragmatic paralysis, leading to difficulty in breathing.
- Overuse of accessory muscles is often seen in patients with asthma, COPD, or during a panic attack.
- Weakness or injury to the intercostal muscles may impair the ability to expand the rib cage properly, reducing ventilation.
🌟
The muscles of the thorax are more than just anatomical structures—they are vital for life-sustaining functions like breathing and movement. Understanding their location, action, and coordination not only helps in anatomy but also in diagnosing and managing respiratory and musculoskeletal conditions in clinical practice.
🤍 Muscle Groups of the Abdomen
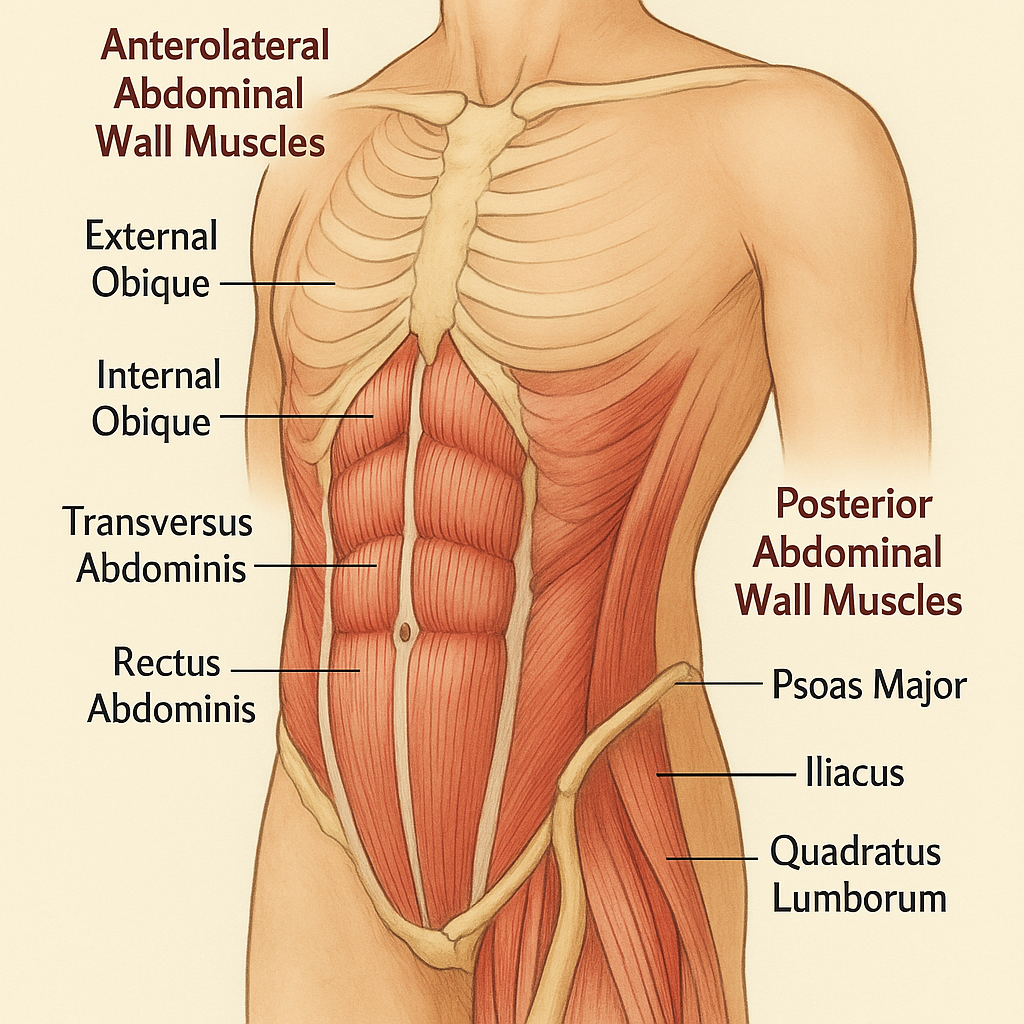
The abdominal muscles form the muscular wall of the anterior and lateral abdomen. These muscles are essential for maintaining posture, protecting internal organs, and performing functions like breathing, coughing, vomiting, childbirth, urination, and defecation. They are grouped based on their location and function into anterior-lateral and posterior abdominal muscles.
🧩 1️⃣ Anterolateral Abdominal Wall Muscles
These include four paired muscles that wrap around the abdominal cavity. Three of them are flat muscles and one is vertical.
🔹 1. External Oblique
- Location: Outermost muscle layer, fibers run downward and medially (like putting hands in your pockets).
- Function:
- Compresses the abdominal contents.
- Flexes and rotates the trunk.
- Supports abdominal wall.
- Clinical note: Forms part of the inguinal ligament.
🔹 2. Internal Oblique
- Location: Just beneath the external oblique; fibers run upward and medially.
- Function:
- Supports abdominal wall.
- Aids in trunk flexion and rotation.
- Compresses the abdomen.
- Fun fact: Acts synergistically with the external oblique on the opposite side for rotation.
🔹 3. Transversus Abdominis
- Location: Deepest of the flat muscles; fibers run horizontally.
- Function:
- Main muscle for abdominal compression.
- Stabilizes the trunk and pelvis.
- Clinical importance: Plays a major role in core stability; targeted in physiotherapy for low back pain.
🔹 4. Rectus Abdominis
- Location: Paired vertical muscles on the front of the abdomen; separated by the linea alba.
- Appearance: Gives rise to the “six-pack” look.
- Function:
- Flexes the vertebral column (especially lumbar region).
- Compresses abdominal contents.
- Tendinous intersections give it the segmented look.
🛡️ 2️⃣ Posterior Abdominal Wall Muscles
These muscles lie deep in the back portion of the abdomen and are crucial for posture and supporting internal organs.
🔸 1. Psoas Major
- Location: Runs from lumbar vertebrae to femur.
- Function:
- Flexes the thigh at the hip joint.
- Helps with trunk flexion when legs are fixed.
🔸 2. Iliacus
- Location: Fills the iliac fossa; joins with the psoas major to form the iliopsoas.
- Function: Strong hip flexor.
🔸 3. Quadratus Lumborum
- Location: Between the iliac crest and the lower ribs/lumbar vertebrae.
- Function:
- Lateral flexion of the spine.
- Stabilizes the pelvis and lumbar spine.
- Clinical note: Can be a source of low back pain if strained.
🌬️ 3️⃣ Role in Respiration and Intra-abdominal Pressure
All abdominal muscles assist in forced expiration by:
- Compressing abdominal organs upward against the diaphragm.
- Engaging during coughing, sneezing, vomiting, and straining (Valsalva maneuver).
They also contribute to maintaining intra-abdominal pressure, which:
- Stabilizes the spine.
- Helps in lifting, bending, and pregnancy-related activities.
📊 Summary Table: Abdominal Muscles at a Glance
| Muscle | Layer | Fiber Direction | Main Function |
|---|---|---|---|
| External Oblique | Superficial | Downward & medially | Trunk rotation, abdominal compression |
| Internal Oblique | Intermediate | Upward & medially | Trunk rotation, abdominal support |
| Transversus Abdominis | Deepest | Horizontal | Core stabilization, compression |
| Rectus Abdominis | Vertical | Vertical | Trunk flexion, abdominal pressure |
| Psoas Major | Posterior | Vertical | Hip flexion |
| Iliacus | Posterior | Fan-shaped | Hip flexion |
| Quadratus Lumborum | Posterior | Vertical | Lateral trunk flexion |
🩺 Clinical Relevance
- Abdominal hernias can occur if muscles or fascia are weak.
- Core instability due to weak transversus abdominis can lead to low back pain.
- Post-surgical complications like abdominal wall separation (diastasis recti) are seen in pregnancy or after surgeries.
- Abdominal exercises like planks and crunches target these muscles for strength and tone.
🧠 Mnemonic for Flat Abdominal Muscles (Superficial to Deep):
“Eat In Tummy” → External, Internal, Transversus
🩻 Pelvic Floor Muscle Groups – An Organized Narrative
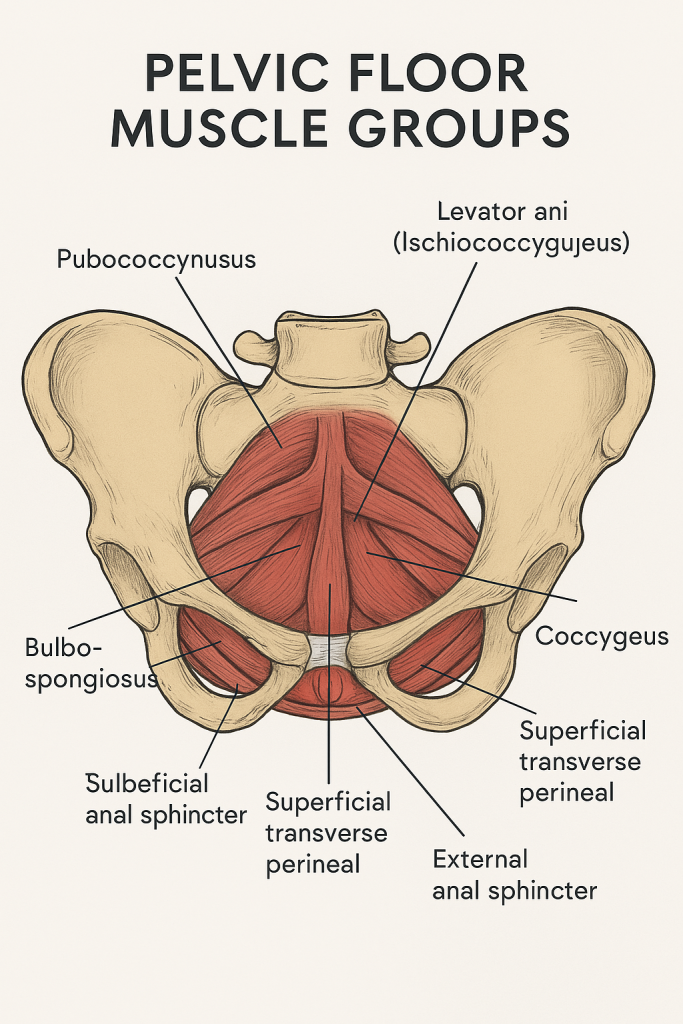
The pelvic floor is a remarkable muscular structure that forms the base of the pelvis. Often described as a muscular hammock or bowl, it stretches from the pubic bone in the front to the tailbone (coccyx) at the back, and between the sitting bones (ischial tuberosities) on either side. These muscles work silently and constantly to support our internal organs, control continence, assist in childbirth, and stabilize our posture.
🌟 Layers of the Pelvic Floor
The muscles of the pelvic floor are arranged in two main layers:
🔹 1. Superficial Perineal Layer (Outer Layer)
This outermost layer lies just under the skin of the perineum. Though relatively small, these muscles play a vital role in sexual function, stabilization, and external sphincter control.
- The ischiocavernosus muscle surrounds the roots of the clitoris or penis and helps maintain erection by compressing veins and limiting blood outflow.
- The bulbospongiosus muscle wraps around the vaginal or penile bulb. In females, it tightens the vaginal orifice and contributes to sexual arousal; in males, it helps with ejaculation and clears the urethra after urination.
- The superficial transverse perineal muscle runs across the perineum and helps stabilize the perineal body—a key connective tissue node anchoring multiple pelvic floor muscles.
- Finally, the external anal sphincter, although not always grouped here anatomically, works closely with this layer. It provides voluntary control over defecation.
🔸 2. Deep Pelvic Floor Layer (Pelvic Diaphragm)
Beneath the superficial layer lies the strong and vital pelvic diaphragm, which forms the true base of the pelvic floor. It supports the weight of the abdominal and pelvic organs, particularly when we stand, cough, or lift heavy objects.
This layer is primarily made up of a group of muscles collectively called the levator ani, and it also includes the coccygeus muscle.
🔶 Levator Ani Group
The levator ani is a broad, thin sheet of muscle made of three parts:
- Pubococcygeus, which stretches from the pubic bone to the coccyx, forms the central part. It helps elevate the pelvic floor and supports pelvic organs like the bladder, uterus, and rectum.
- Puborectalis, a muscular sling looping around the rectum, is crucial for maintaining fecal continence. It creates the angle between the rectum and the anus, which tightens during rest and relaxes during defecation.
- Iliococcygeus arises from the inner side of the pelvis (the ischial spine and fascia) and inserts on the coccyx. Though thinner, it reinforces the pelvic floor and provides additional support.
Together, these muscles lift and support the pelvic organs, particularly during activities that increase abdominal pressure, like sneezing, laughing, or childbirth.
🔷 Coccygeus Muscle
Also known as ischiococcygeus, this smaller muscle lies just behind the levator ani and connects the ischial spine to the coccyx and sacrum. It helps support the posterior pelvic floor and assists in moving the tailbone forward after defecation or labor.
🌬️ Key Functions of the Pelvic Floor Muscles
Despite their deep and hidden location, pelvic floor muscles perform many visible and vital functions:
- 🛡️ Support: They hold the pelvic organs—including the bladder, uterus (in females), prostate (in males), and rectum—in their proper place, preventing prolapse or downward displacement.
- 🚽 Continence Control: These muscles form the foundation of both the urethral and anal sphincters, allowing us to voluntarily hold and release urine and stool.
- ❤️ Sexual Function: In both men and women, they contract rhythmically during orgasm and contribute to erection, arousal, and satisfaction.
- 🤰 Childbirth: The pelvic floor stretches dramatically during vaginal delivery and then helps recoil and heal postpartum. Strong muscles can assist in easier labor and recovery.
- 🧘 Core Stability: Along with the diaphragm, abdominal, and back muscles, the pelvic floor helps stabilize the spine and pelvis, especially during movement or lifting.
🩺 Clinical Significance
Weakness, tightness, or injury in the pelvic floor can lead to a range of issues:
- Pelvic floor dysfunction may cause urinary incontinence, fecal incontinence, or pelvic organ prolapse.
- Overuse or spasm of these muscles can result in pelvic pain, dyspareunia (painful intercourse), or constipation.
- Childbirth trauma, surgeries, obesity, or aging can affect pelvic floor strength and coordination.
- Fortunately, with guidance, targeted exercises—like Kegels—can effectively strengthen or relax these muscles, leading to significant improvement in function and quality of life.
✨ Final Thought
Though often overlooked, the pelvic floor is the powerhouse of the core—it balances strength, stability, and sensitivity. Whether you’re learning anatomy, treating patients, or enhancing personal health, understanding these muscles is key to supporting one of the most essential areas of the body.
🍑 Gluteal Muscles – A Detailed Overview
The gluteal region, or buttock area, contains some of the strongest muscles in the human body. These muscles are essential for hip movement, postural support, and locomotion like walking, running, and climbing.
🔹 The gluteal muscles are divided into superficial and deep layers:
🧩 1️⃣ Superficial Gluteal Muscles
These are the larger, more powerful muscles responsible for gross movements of the hip and thigh.
✅ Gluteus Maximus
- Largest and most superficial muscle of the gluteal region.
- Origin: Posterior ilium, sacrum, coccyx, and sacrotuberous ligament.
- Insertion: Iliotibial tract and gluteal tuberosity of femur.
- Function:
- Primary extensor of the hip.
- Helps with external rotation, rising from a sitting position, and climbing stairs.
- Nerve Supply: Inferior gluteal nerve (L5, S1, S2).
✅ Gluteus Medius
- Lies beneath gluteus maximus, fan-shaped.
- Origin: Outer surface of ilium.
- Insertion: Greater trochanter of femur.
- Function:
- Abducts the thigh.
- Stabilizes pelvis during walking.
- Nerve Supply: Superior gluteal nerve (L4, L5, S1).
- 🩺 Clinical Relevance: Weakness causes Trendelenburg gait (pelvic drop on opposite side).
✅ Gluteus Minimus
- Smallest and deepest of the gluteal muscles.
- Origin: Outer surface of ilium (below gluteus medius).
- Insertion: Greater trochanter of femur.
- Function:
- Assists abduction and medial rotation of the thigh.
- Nerve Supply: Superior gluteal nerve.
🔍 2️⃣ Deep Gluteal Muscles (Lateral Rotators of Hip)
These small, deep muscles are primarily involved in external rotation of the thigh.
- Piriformis
- Superior Gemellus
- Obturator Internus
- Inferior Gemellus
- Quadratus Femoris
🔄 Mnemonic: “PGOGOQ”
These form a muscular layer deep to gluteus maximus and help stabilize the femoral head in the acetabulum.
💪 Vastus Lateralis – A Key Quadriceps Muscle
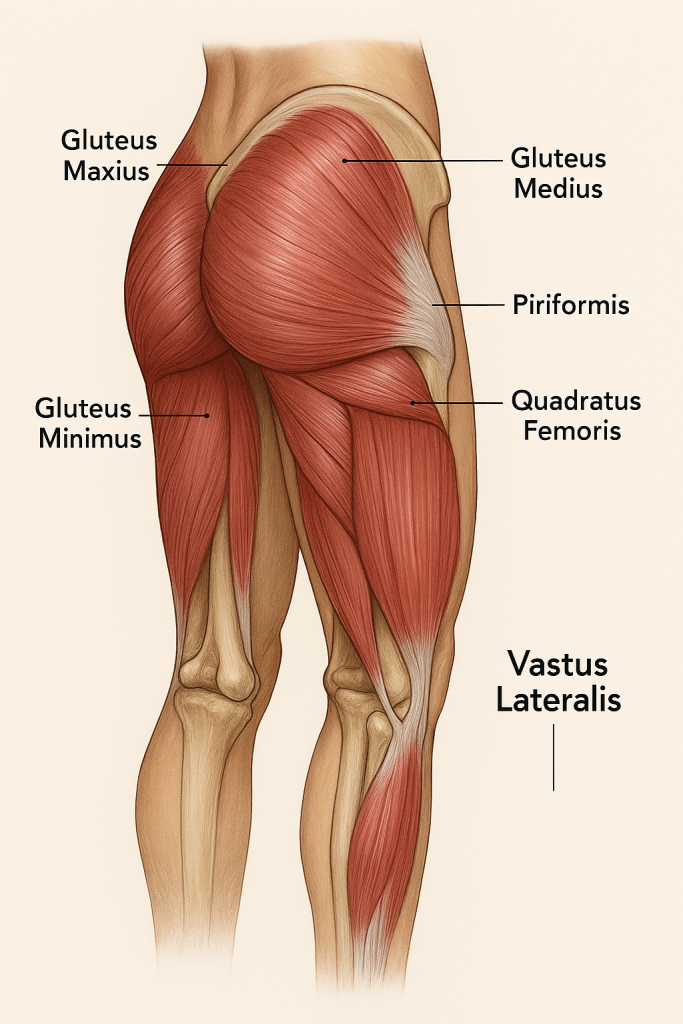
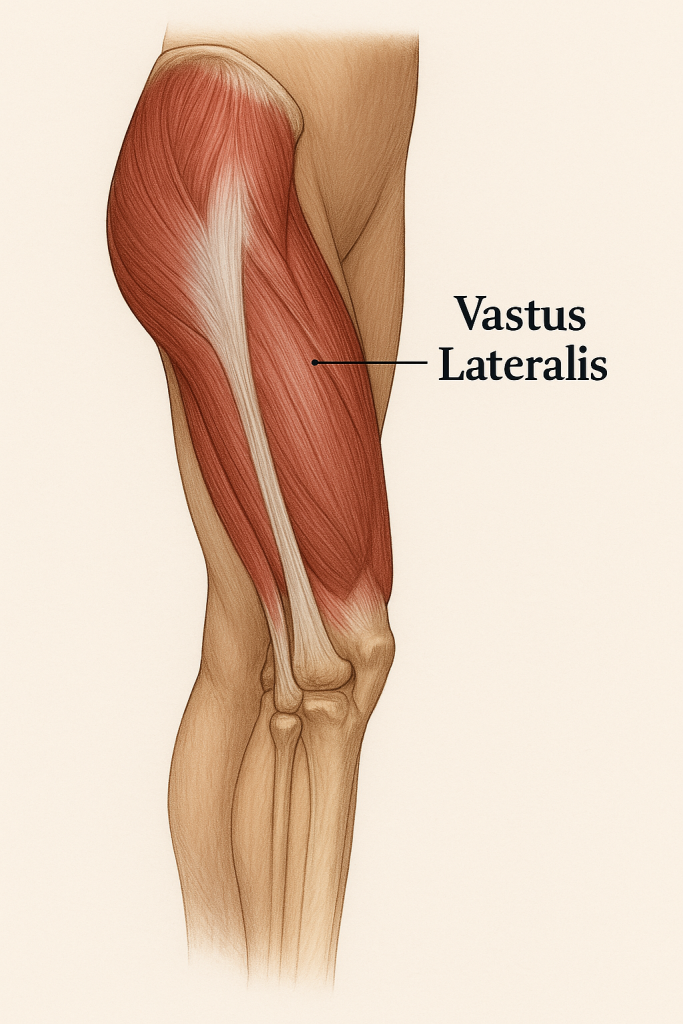
The Vastus Lateralis is one of the four quadriceps muscles, located on the lateral side of the thigh. It is the largest of the quadriceps and plays a major role in knee extension.
✅ Anatomy of Vastus Lateralis
- Origin:
- Greater trochanter.
- Lateral lip of the linea aspera on the femur.
- Insertion:
- Merges with the quadriceps tendon to insert on the patella, which continues as the patellar ligament to insert on the tibial tuberosity.
- Function:
- Extends the knee joint.
- Helps maintain posture and stabilizes the knee during standing, walking, and squatting.
- Nerve Supply: Femoral nerve (L2, L3, L4).
🩺 Clinical Importance of Vastus Lateralis
- 📍 IM Injection Site (Intramuscular):
- It is a preferred site for intramuscular injections in infants and children, especially in the anterolateral thigh, due to its size and thickness.
- ⚠️ Muscle Imbalance or Weakness:
- Weakness can cause knee instability and patellar tracking issues.
- Overdominance can lead to lateral patellar displacement, especially in runners.
⚖️ Gluteal vs. Vastus Lateralis – Functional Contrast
| Gluteal Muscles | Vastus Lateralis |
|---|---|
| Act on the hip joint (extension, rotation, abduction) | Acts on the knee joint (extension) |
| Stabilize pelvis and trunk | Stabilizes the knee during movement |
| Supplied by gluteal nerves | Supplied by femoral nerve |
| Key in posture, gait, and climbing | Key in walking, squatting, and standing up |
✨ Summary Insight
- The gluteal muscles form the powerhouse of the hip and pelvis, essential for upright posture and powerful leg movements.
- The vastus lateralis contributes to the strength and mobility of the knee, making it vital in locomotion.
- Both groups are clinically significant, not just in movement but in patient care—especially for safe IM injection, rehabilitation, and surgical positioning.
🩺 Major Muscles Involved in Nursing Procedures – A Clinical Perspective
Nursing procedures often require physical activity, manual support, and precise movements that engage a range of muscles across the upper limb, lower limb, back, and core. Understanding which muscles are involved helps prevent injury, improves ergonomics, and enhances clinical skills like lifting, injections, positioning, and range-of-motion exercises.
1️⃣ Muscles Involved in Patient Lifting, Transferring, and Positioning
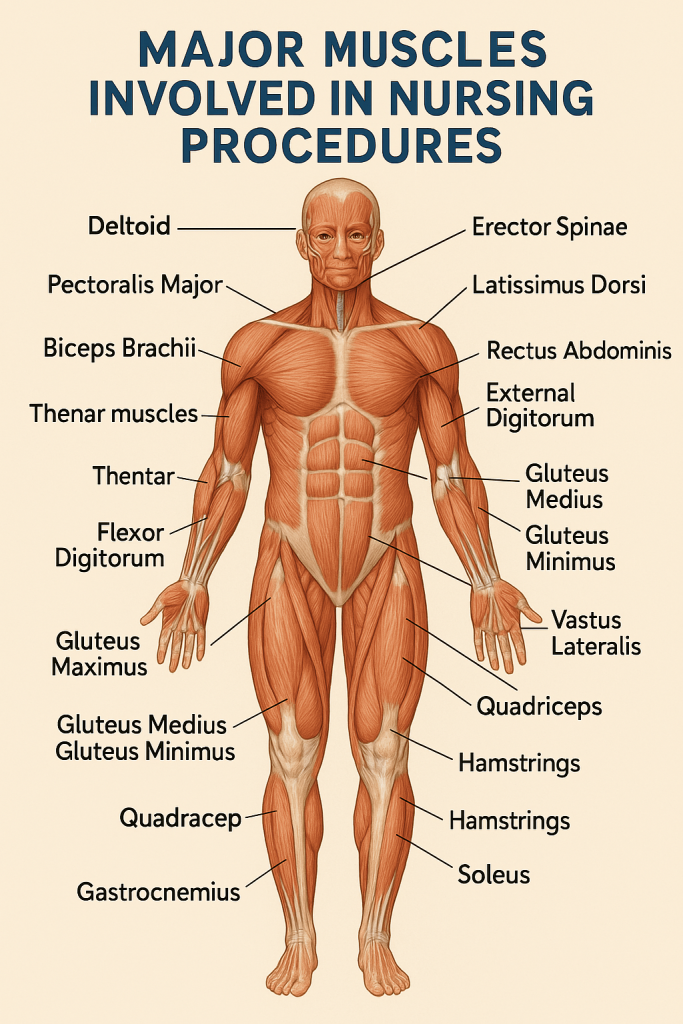
Nurses often assist with turning, lifting, or transferring patients. These actions rely heavily on large muscle groups of the back, legs, and core for strength and stability.
🔹 Back and Core Muscles
- Erector Spinae: Extends and stabilizes the spine during lifting and standing.
- Latissimus Dorsi: Assists in pulling and supporting the torso.
- Rectus Abdominis & Transversus Abdominis: Help stabilize the trunk and prevent spinal injury.
- Obliques (internal & external): Aid in twisting and lateral bending while repositioning patients.
🔹 Lower Limb Muscles
- Gluteus Maximus: Powerful hip extensor, essential for rising from a squatting position.
- Quadriceps (esp. Vastus Lateralis): Extend the knee while standing, squatting, or transferring weight.
- Hamstrings: Assist in hip extension and knee flexion during lifting motions.
- Gastrocnemius & Soleus (calf muscles): Stabilize the ankle and assist in weight-bearing stance.
⚠️ Nursing Tip:
Always bend at the hips and knees (not the waist), engage the core, and use the legs to lift with proper body mechanics.
2️⃣ Muscles Involved in Administering Injections
🔹 Intramuscular (IM) Injection Sites and Muscles
- Deltoid Muscle (upper arm)
- Site: 2.5–5 cm below the acromion process.
- Common for small-volume IM injections (e.g., vaccines).
- Nerve proximity: Avoid the radial nerve.
- Vastus Lateralis (anterolateral thigh)
- Preferred site in infants and children.
- Thick, well-developed muscle with minimal nerve proximity.
- Ventrogluteal Site (Gluteus Medius and Minimus)
- Safest site for larger volumes in adults.
- Avoids major nerves and blood vessels.
- Dorsogluteal Site (Gluteus Maximus)
- Traditionally used but now less favored due to sciatic nerve proximity.
🔹 Subcutaneous Injections
- Engage the fatty tissue and superficial muscles like the triceps or abdomen over the rectus abdominis.
3️⃣ Muscles Used During CPR (Cardiopulmonary Resuscitation)
Administering effective chest compressions during CPR requires strength and endurance.
- Pectoralis Major & Minor: Engage when pressing on the chest.
- Deltoid and Triceps Brachii: Control downward force and elbow extension.
- Biceps Brachii: Stabilize the arm during compressions.
- Core muscles (Rectus Abdominis, Obliques, Transversus Abdominis): Stabilize trunk.
- Erector Spinae: Maintain posture and balance during prolonged compressions.
4️⃣ Muscles Engaged in Range-of-Motion (ROM) Exercises
While performing passive or active ROM exercises, nurses facilitate joint movement by activating or supporting specific muscle groups.
🔹 Upper Limb
- Shoulder flexion/extension: Deltoid, Pectoralis major, Latissimus dorsi.
- Elbow flexion/extension: Biceps and Triceps.
- Wrist movements: Flexor and extensor muscles of the forearm.
🔹 Lower Limb
- Hip movements: Gluteals, Iliopsoas, Adductors.
- Knee flexion/extension: Quadriceps and Hamstrings.
- Ankle movements: Tibialis anterior, Gastrocnemius, Soleus.
5️⃣ Muscles Involved in Ambulation Assistance and Gait Training
When helping patients walk or using assistive devices:
- Core Muscles: Maintain balance and posture.
- Gluteals and Quadriceps: Power hip and knee extension.
- Hamstrings and Calves: Control walking rhythm and foot placement.
- Deltoids and Triceps: Involved when supporting patients with walking aids (e.g., walker, cane).
6️⃣ Fine Motor Muscles in Nursing Skills
Precision-based skills like wound dressing, catheter insertion, IV cannulation, and BP measurement engage small muscles:
- Thenar and Hypothenar Muscles: Control thumb and pinky finger for gripping tools.
- Flexor and Extensor Digitorum: Move fingers for accurate hand control.
- Brachioradialis and Biceps Brachii: Aid in forearm rotation and positioning.
🩺 Summary Insight
Nursing is physically and anatomically demanding. Whether you’re:
- Administering an injection,
- Repositioning a patient,
- Assisting with ambulation, or
- Performing CPR —
You’re engaging multiple muscle groups simultaneously. Awareness of muscle anatomy helps ensure: ✔️ Proper technique
✔️ Prevention of injury
✔️ Increased efficiency
✔️ Better patient outcomes