ENGLISH-MSN-UNIT- 4-ALTERED IMMUNE RESPONSE-UPLOAD
ALTERED IMMUNE RESPONSE:

Definition:
1) Define/explain immunity:

Immunity is a type of resistance that is provided by the host’s body. When any foreign body or antigen enters the body, the host’s immune system is activated and fights against the antigen and produces antibodies, which is called immunity.
2) Define/explain allergy (Define allergy):

Allergy is an inappropriate and harmful immune response of the body’s immune system against a harmless substance.
3) Define/explain allergens:

Allergens are substances that are responsible for activating the condition of allergy in the body and act as a foreign body in the body.
4) Define/explain antibody (Define antibody) :
Antibody is a type of protein substance. When the body comes into contact with any specific allergen, antibodies are produced in the body to fight against it.
5) Define/explain hypersensitivity. (Define Hypersensitivity) :

Hypersensitivity is when the immune system overactivates to provide a response against an antigen that enters the body. (overactivation of immune response against allergens its called hypersensitivity).
6) Define/explain histamine. (Define histamine) :

Histamine is a substance in the body that increases the level of histamine when any allergic condition is created in the body. Histamine increases gastric secretion, dilates capillaries, and constricts bronchial smooth muscles.
7) Define/explain Anaphylaxis. (Define Anaphylaxis) :

When the human body is exposed to any antigen, an immediate allergic reaction starts in the human body and it provides a hyperactive immune response and within a minute the allergic reaction starts and signs and symptoms are seen in the body, it is called anaphylaxis.
8)Define/explain immunoglobulin. (Define immunoglobulin):
Immunoglobulin is a type of protein substance that works like an antibody. is.
9) Define/explain lymphocytes:
These are a type of cell that plays an important role in producing circulating antibodies.
10) Define/explain Atopic dermatitis. (Define atopic dermatitis):
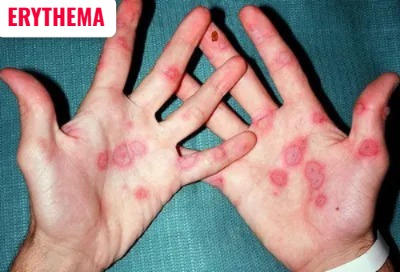
Atopic dermatitis is a type I hypersensitivity reaction and its signs and symptoms are primarily seen in the skin. Such as itching, redness and skin lesions.
11) Diffuse Redness of skin its called … ERYTHEMA (erythema).
12) Define/explain mast cells:
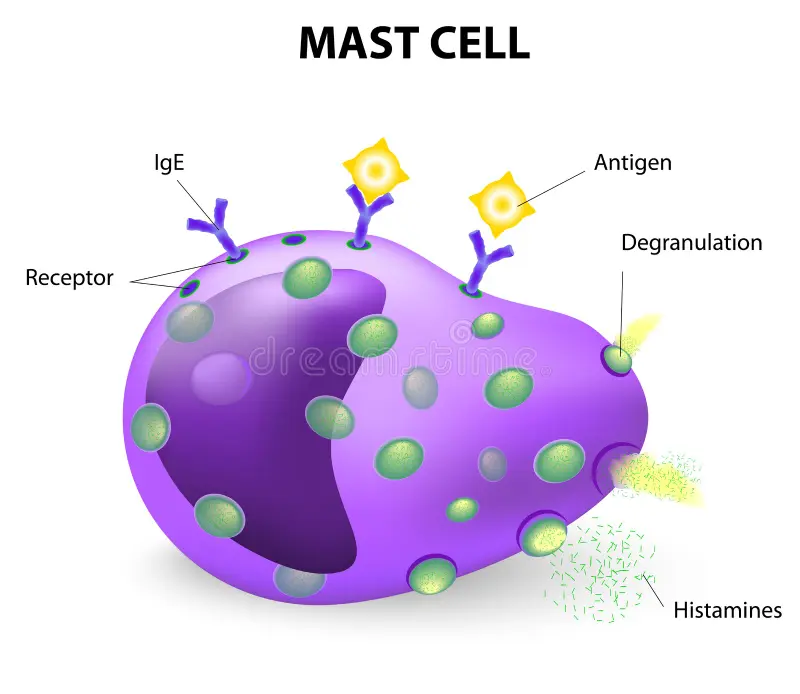
Mast cells are cells of connective tissues, whose granules contain heparin and histamine.
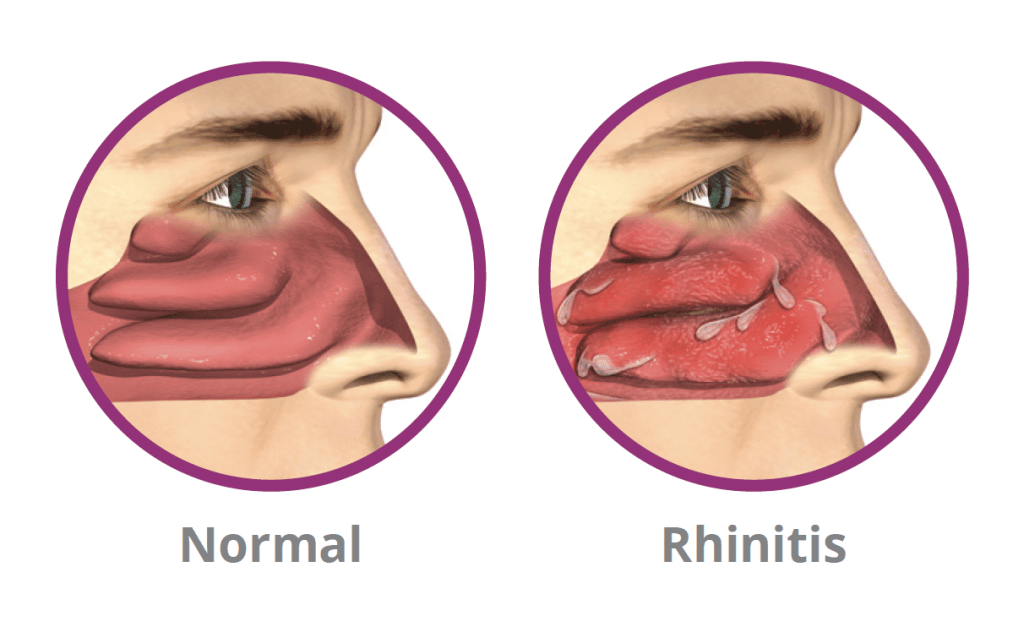
13) Inflammation of the nasal mucosa it’s called… RHINITIS (Rhinitis).
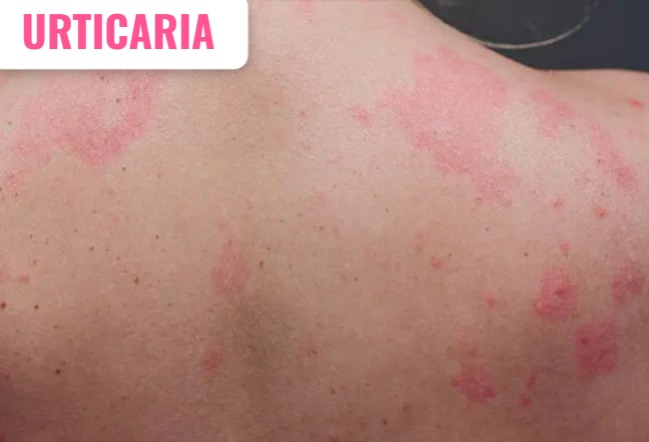
14) Give other name of HIVES (Hives)… URTICARIA (URTICARIA).
Explain/define immunity:

- Immunity is a type of resistance that is activated by the host’s body.
- When any foreign body / antigen enters the host’s body The antibody that fights against the antigen when it enters is called immunity.
- When an antigen/infection enters the body, the body’s ability to fight against it is called immunity.
Factors affecting immunity:

1)Nutritional Factores (Nutritional Factores).
2)Hormons (Hormones).
3)sex (Sex).
4)General health (General Health).
5)Age (Age).
6)Defence mechanisms (Defence mechanisms) Mechanism).
7)mechanical barriers and surface secretion.
8)stress.
1)Nutritional Factores (Nutritional Factores).

- BALANCED DIET increases the body’s immune system.
- The immune system is impaired due to NUTRITIONAL DEFICIENCY.
- Thus nutritional factors affect the immune system is.
- Ex: PEM: (PROTIEN ENERGY MALNUTRITION) ,
- BLINDNESS (DUE TO DEFICIENCY OF VITAMIN A)
2)Hormones (Hormones):

When the hormones in the body increase or decrease too much, the immune system becomes disturbed.
Ex:
- cortisol,
- Thyroid,
- Estrogen,
- Progesterone,
- Testosterone etc.
3) sex:

- Some diseases are seen according to the caste.
- Ex: hemophilia (Hemophilia: Hemophilia is a disease condition in which blood does not clot properly, due to which excessive bleeding occurs when an injury occurs).
-> Sickle cell Anemia (Sickle cell anemia is a genetic disorder in which the red blood cells are shaped like a sickle) - This is a disease that is more common in males and less common in females and females act as carriers.
4)General health:

A person’s general well-being and health condition also affect immunity.
If a person
-> Adopt healthy habits (by adopting healthy habits),
-> maintain personal hygiene (by maintaining personal hygiene),
-> tack a balanced diet (by taking a balanced diet) …. then the person’s immune system becomes strong.
5)Age:
- Different types of immunity are seen in different people.
- old age: The immunity of an old person is less than that of an adult because the immune system of an old person declines.
- neonates (from 0 to 28 day baby): The immune system in neonates is underdeveloped, so infections in neonates occur very quickly.
- Thus, the immune system is also affected in the same way.
6) Defence mechanisms:

- If the body produces humoral and cellular immunity ( humoral immunity ( B lymphocytes)/cellular immunity (T lymphocytes)) properly, then the body can defend itself properly.
7) mechanical barriers and surface secretion (mechanical Barrier and Surface Sikrisan) :
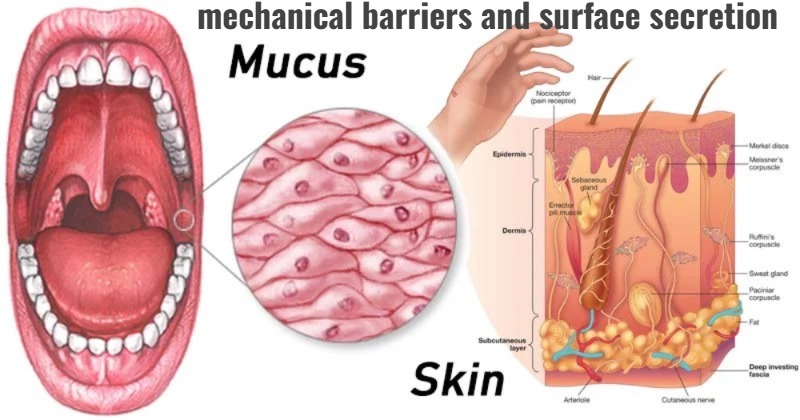
- Provides high degree of protection if there is skin intake in the body.
- (Intact skin has an outer horny layer, which contains keratin. This keratin provides a shield to the epidermis layer.)
surface secretion:
- Our skin secretes sebaceous secretion and sweat.
- This secretion works as a bactericide and fungicide.
- [Bactericidal:= kill the bacteria],
- [fungicide:= kill the fungi], thus providing strength to immunity.
8) Stress:

- If a person is under stress for a long time, then the level of cortisol hormone increases in that person due to stress and if there is an increase in cortisol hormone in the body, then his immune system is affected.
- Thus, immunity is also affected due to stress.
- All these factors affect immunity.
=> Immunity:

Immunity is a type of resistance that is activated by the host’s body .
When any foreign body (antigen) enters the host’s body, the antibodies of the host’s body that fight against that antigen are called immunity. When an antigen (foreign body) enters the body, the body’s ability to fight against it is called immunity.
There are two types of immunity:
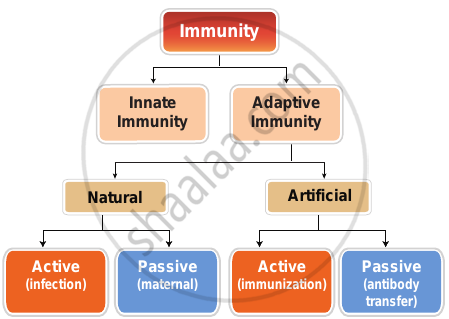
1) Innate immunity
2) Acquired immunity
(1) Innate immunity (innate immunity/( IN BORN)):

Innate immunity is the immunity that a person has by birth. This is a type of natural immunity.
(2) Acquired immunity (Acquired immunity/(AFTER BORN)):
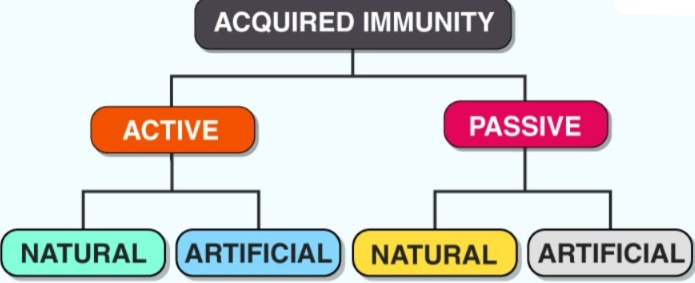
The immunity that the body gets during the life after birth is called acquired immunity.
TYPES OF INNATE IMMUNITY :
1)SPECIES IMMUNITY
2)RACIAL IMMUNITY
3)INDIVIDUAL IMMUNITY
1)species immunity
(Species immunity: Different species have different immunities)
2)Racial immunity
(Racial immunity: Different immunities are found according to different races.)
3)individual immunity
(Individual immunity: Each individual has different have immunity).
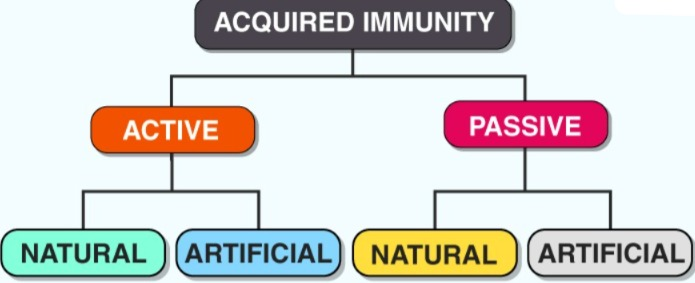
TYPES OF ACQUIRED IMMUNITY :

1)ACTIVE IMMUNITY
(Active Immunity),
2) PASSIVE IMMUNITY
(Passive Immunity)
1)Active immunity Immunity):
(Active immunity: The immunity that is produced by the body itself is called active immunity)
There are also two types of active immunity:
A)Active natural immunity:
(Active natural immunity: When a person is exposed to an infection, immunity is seen in that person.)
B)Active artificial immunity (Active artificial immunity):
(Active artificial immunity: When a person is immunized and immunity develops in that person, it is called active artificial immunity.)
2) PASSIVE IMMUNITY:
(Passive Immunity: The immunity that is developed by others is called passive immunity. This immunity does not develop in the own body.
There are also two types of active immunity:
A) passive natural immunity (Passive Natural Immunity) :
(Passive natural immunity: When the fetus is in the mother’s womb and the immunity that the fetus gets from the mother is called passive natural immunity.)
B) passive artificial immunity (Passive artificial immunity):
(Passive artificial immunity: When antibodies are made from someone else and transferred to someone else’s body, it is called passive artificial immunity. है).
Full information of Classification of innate immunity
1)INNATE IMMUNITY:
Other 3 types of innate immunity
1)species immunity
( species immunity),
2)Racial immunity
( Racial Immunity),
3) Individual immunity
(Individual immunity)
1)INNATE IMMUNITY:

Innate immunity is the immunity that a person has by birth. This is a type of natural immunity.
there are 3 types of innate immunity

1) species immunity:
This type of immunity is found only in a particular species.
- Ex: human beings ,
- Plants ,
- Animals .
All of these have different immunities, which are called species immunity.
This immunity is found in all members of a particular species.
Ex:
1) Human beings have total resistance to pathogens present in plants and animals, so even if they come in contact with plants and animals that have diseases, they do not get the disease because human beings are totally resistant to it.
2) Rats have immunity against diphtheria. But humans do not have immunity against diphtheria, so humans are becomes infected or susceptible to diphtheria.
3) The cholera microorganism cannot infect birds. But humans can become infected or susceptible to it.
4) Dogs, sheep, and horses do not get tuberculosis. But tuberculosis is found in human beings. Thus, different types of immunity are found according to each species.
2) Racial immunity:
There are different species, different types of immunity are found in all the species.
Ex:
- 1)South Indian people,
- 2)North Indian people
Different types of immunity are found in different races.
1) Algerian sheep have immunity against anthrax. But European sheep do not have resistance against anthrax, so anthrax disease is found in them.
2) Black people’s (negros) are more susceptible than white people Immunity is observed.
3) White people have a higher chance of getting tuberculosis, while black people have a lower chance of getting tuberculosis. Thus, different types of immunity are found in people of every caste.
3) Individual immunity:
- Individual immunity is found in different types in different people.
- Ex: If four people live in a house, three of them have common cold and one person does not, then the immunity of that one person is more for common cold. Thus, the immunity of each person is of different types. is.
The mechanisms of innate immunity:
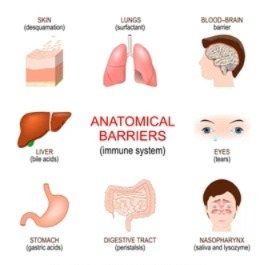
1)SKIN (Skin) :
- The skin has a mechanical barrier.
- The skin has a horny layer (keratin) which shields the epidermis layer of the skin and works as a shield.
- Due to which pathogenic bacteria, viruses, and microorganisms enter the body No.
- Skin sweat contains a high concentration of salts which are responsible for killing pathogens.
- Skin contains sebaceous secretions and these sebaceous secretions have a bacteriocidal effect which is necessary to kill bacteria.
2)Respiratory track (Respiratory track):
- The respiratory track has a nasal mucosal layer and if any microorganism enters this mucosal layer, it gets stuck there.
- If microorganisms get stuck in the nose, they get out of the body through sneezing.
- The nasal cavity has hairs like cilia that trap the pathogenic microorganisms in the air and do not allow them to enter the body.
Thus, the respiratory track also boosts immunity.
3) Gastrointestinal track:
- Our mouth has saliva. This saliva contains lysosomes which work to kill pathogens.
- The pH of the stomach is acidic due to the hydrochloric acid (HCL) present in the stomach.
- If any pathogenic bacteria enters the stomach, then due to the acidic pH present there Microorganisms are killed and immunity is boosted.
4) Conjunctiva (Conjunctiva):
- There are tears in the eyes and these tears contain lysosomes which work as bactericidal and kill bacteria.
- Tears flush the eyes when any microorganism enters the eyes. If it goes, it gets flushed through tears and it works to boost immunity.
5)Genitourinary track:
- Urine flushes and cleans the urethra. When any microorganism reaches the urethra, it is flushed out through urine and it boosts immunity.
- Thus, immunity is boosted due to this mechanism in the body.
Full information about AQUIRED IMMUNITY (Full information about Acquired Immunity):
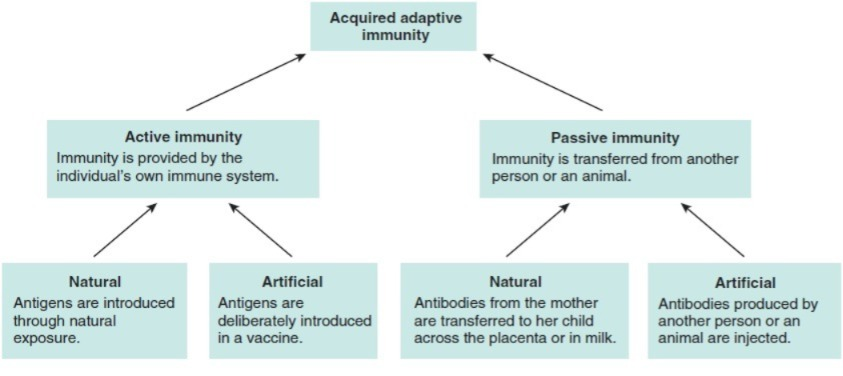
The immunity that the body gets after birth during whole life is called acquired immunity.
There are two types of acquired immunity.
1)ACTIVE IMMUNITY
2)PASSIVE IMMUNITY
1) ACTIVE IMMUNITY,
When any antigen enters the body, the body In the same way, antibodies are produced against the antigen and it is called active immunity. (active immunity develops after entry of antigen)
There are 2 types of active immunity.
1) Active natural immunity (Active natural immunity),
This immunity is natural and active, so it is called active natural immunity. This immunity arises when an antigen enters the body and antibodies are produced in the body against that antigen, then immunity is seen in the body and this immunity life is long.
A) humoral immunity,
Humoral immunity develops from the body’s plasma.
B) cell-mediated immunity (Cell Mediated Immunity)
Cell mediated immunity is mainly developed from T- lymphocytes.
T- lymphocytes provide defense against any antigen in the body, against any microorganism that causes chronic bacterial infections.
2)Active artificial immunity (Active artificial immunity)
Artificial means (man made) is artificially made and is not related to nature.
When an immunity is provided by a vaccine and the body produces antibodies against it, it is called Artificial Active Immunity.
- Ex: BCG (Baccilus callmate guarine),
- hepatitis,
- DPT (Deptheria, Pertussis, Tetanus),
- DT (Deptharia, Tetanus),
- pentavelent etc.
2) PASSIVE IMMUNITY:
Passive Immunity: The immunity that is developed by others is called passive Immunity. It does not develop in the body itself.
There are 2 types of passive immunity:
1) Passive natural immunity.
2) Passive Artificial immunity immunity).
1) Passive natural immunity:
- This immunity that the fetus gets from the mother is called passive natural immunity.
- This immunity is also called congenital immunity.
- Ex: 1) IgG (immunoglobulin G) is passed from the placenta to the fetus.
- 2)IgA (immunoglobulin A) is obtained by the fetus from breast milk.
- These two antibodies IgG and IgA are obtained from the mother by the fetus, hence it is called passive natural immunity.
2) Passive Artificial immunity (Passive Artificial Immunity):
This immunity is Artificial (man made).
In this, antibodies are administered directly into the body of the recipients.
Given by:
1)antitoxin,
2)antibacterial,
3)antiviral,
- Ex: Tetanus toxoid ( TT),
- Gas gangrene antitoxin,
- Anti venom sera,
- Anti lymphatic serum.
These antibodies provide immediate protection and are temporary.
use of passive immunization
1) Passive immunization provides immediate immunity in the body.
2) Suppresses active immunity.
3) Provides immediate immunity to treat serious infections.
ALTERED IMMUNE RESPONSE:

Immune Response:
Immune response is a type of reactivity that is stimulated by antigens, i.e. when an antigen enters the human body, the body’s immune system is activated and it produces antibodies against the antigen and an antigen – antibody reaction is seen, which is called immune response.
There are two types of immune response:
The human body activates its immune system against infectious pathogens such as bacteria, viruses, fungi, and parasites. Two main types of immune responses are seen for this protection:
1) Humoral Immune Response
2) Cell Mediated Immune Response
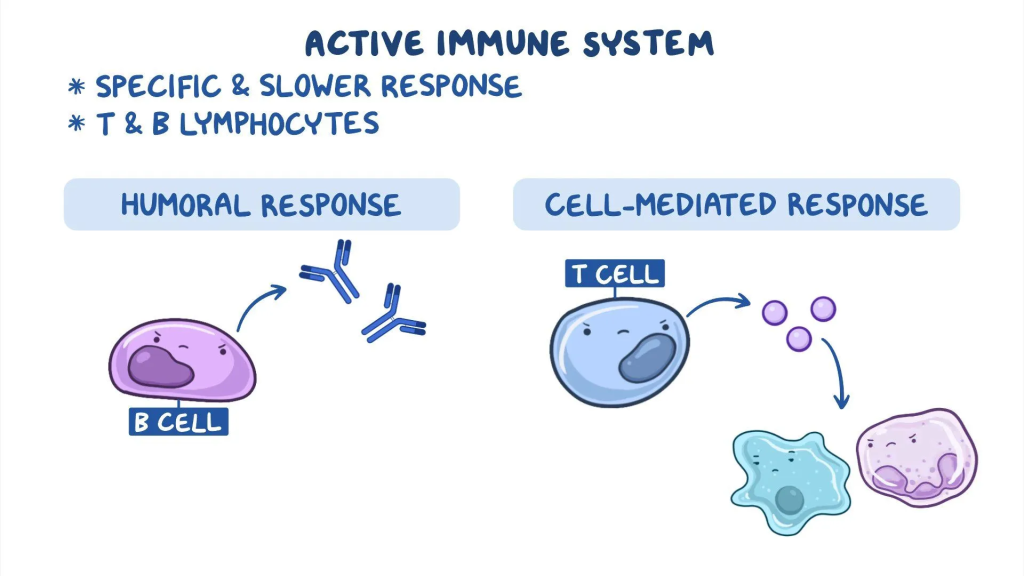
1) Humoral Immune Response:
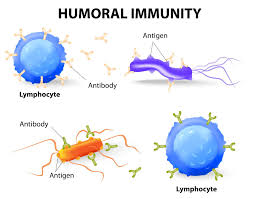
Humoral immune response is a reaction in which B lymphocytes or B cells produce antibodies. When an antigen enters the body, B cells identify it and make antibodies against it. This antibody then diffuses into the blood plasma and lymph and binds to the antigen, eliminating it or preparing it for phagocytosis.
Characteristics of this reaction:
- Processed by B cells
- Produces antibody antibodies)
- Mainly active in fluids such as blood and lymph
- Especially effective against bacteria and foreign viruses
2) Cell Mediated Immune Response:
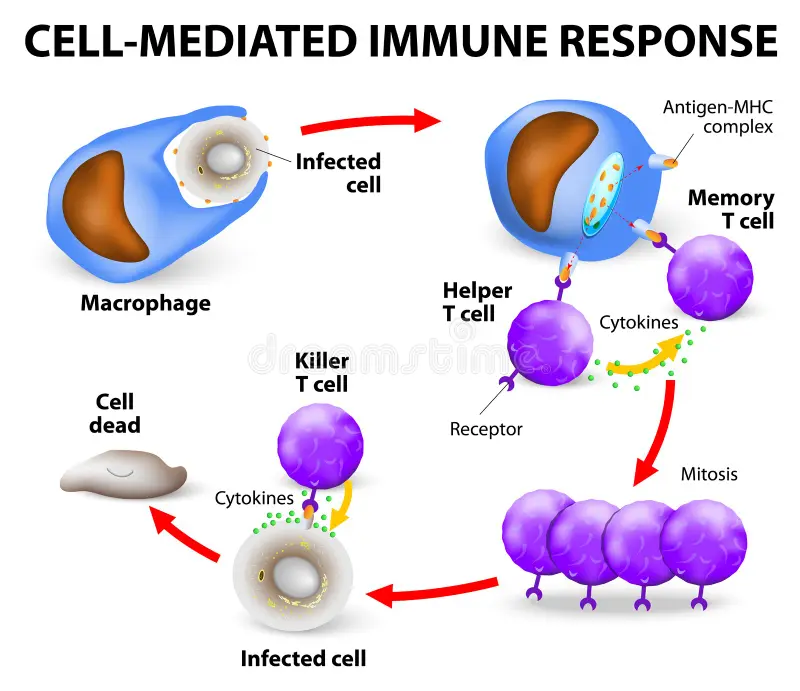
A cell-mediated immune response is a reaction that is controlled by T lymphocytes or T cells. This response does not depend on antibodies. T cells directly destroy infected cells, cancer cells, or transplanted cells in the body. Also, T cells produce various cytokines that activate other immune cells.
Characteristics of this response:
- Operated by T cells
- Direct cell-based response, not antibodies
- Effective against virus-infected cells, cancer cells, and other non-self cells
- Produces cytokines
Health history and laboratory investigations of Allergic disorders.

Health history:
- Collection of the patient’s history and physical examination can help determine whether the patient has any allergic disorders.
Laboratory evaluation:
1)CBC : complete blood count:
- Check the WBC level (usually white blood is normal but if there is an infection condition then the WBC count increases).
- Check the level of eosinophil count (check the level of eosinophil count).
2)Total serum immunoglobulin levels:
- for assessment of ig E level in blood.
3)Skin test:
- intradermal injection, superficial application of solutions,
- prick test,
- Scratch test,
Intradermal testing (intradermal testing):
- 0.5.ml or 1ml sterile syringe which Using a 26 to 27 gauge needle, insert 0.02 to 0.03 ml of allergen intradermally.
- Introduce a small amount of allergens by inserting the needle intradermally, which creates a bleb (a raised area) on the injected site and it should be about five millimeters in diameter and this test is considered positive when symptoms like redness, itching, wheal are seen on the injected side.
- So, skin test is done to assess the allergen.
4)Provoking testing:
Provoking testing is a test in which the body is deliberately exposed to a suspected allergen, so that it can be known whether the body gives an immune response or a hypersensitive reaction to it or not.
Purpose:
- A person is exposed to a specific allergen To determine whether there is sensitivity to (the substance causing the allergy).
- To determine the severity and type of allergic reaction.
- To confirm the diagnosis when other tests do not give a clear result.
Method:
In this test, the suspected allergen is administered to the Target Organ of the body – such as Nose, Eye, Lungs or Oral Route and the Immediate or Delayed Reaction of the body is observed.
Types:
1. Nasal Provoking Test:
In the nose Allergens are administered to test for rhinitis or nasal allergy.
2. Bronchial Provoking Test: Breathing difficulty or asthma is tested by inhaling allergens.
3. Conjunctival Provoking Test: Allergic Conjunctivitis is tested by injecting allergens into the eye.
4. Oral Food/Drug Provoking Test:
The body is tested for Allergy through food or medicine.
Result:
- Positive Result: If symptoms like hives, runny nose, difficulty breathing appear on the skin, it is considered positive for allergy.
- Negative Result: If no symptoms are observed, then the substance is not the cause of the allergy.
Provoking testing is a test in which the body is exposed to the suspected allergen producing substance (Allergen) to see if an allergic reaction occurs.
This test should always be performed by a trained medical professional.
5) Full form of RAST test is (RADIO ALLERGO SORBENT TEST) (રેડીઓ એલેરોગો સોર્બંટ Test):
This test is used to assess the allergen.
Hypersensitivity:
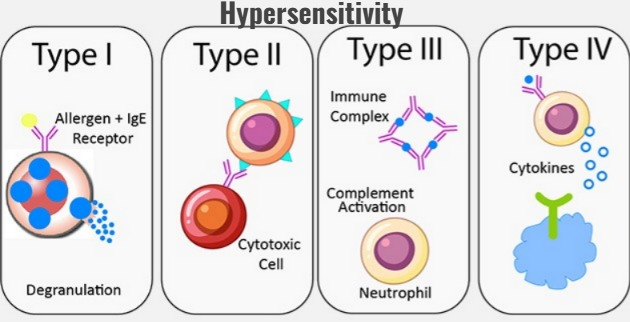
Hypersensitivity is an altered stage of our body’s immunity in which when any antigen enters the human body, the human body’s immune system becomes hyperactive and provides a response to it and creates unacceptable symptoms in the body. This is called Hypersensitivity.
Four types of hypersensitivity (four types of hypersensitivity):

1) type : 1 hypersensitivity is called ANAPHYLACTIC HYPERSENSITIVITY (anaphylactic hypersensitivity),
2) type : 2 hypersensitivity is called CYTOTOXIC HYPERSENSITIVITY (Cytotoxic Hypersensitivity),
3) type: 3 hypersensitivity is called IMMUNE COMPLEX HYPERSENSITIVITY( Immune Complex Hypersensitivity),
4) Type : 4 hypersensitivity is called DELAYED HYPERSENSITIVITY (Delayed sensitivity)

1) types: 1 hypersensitivity (Anaphylactic hypersensitivity : anaphylactic hyper Sensitivity)
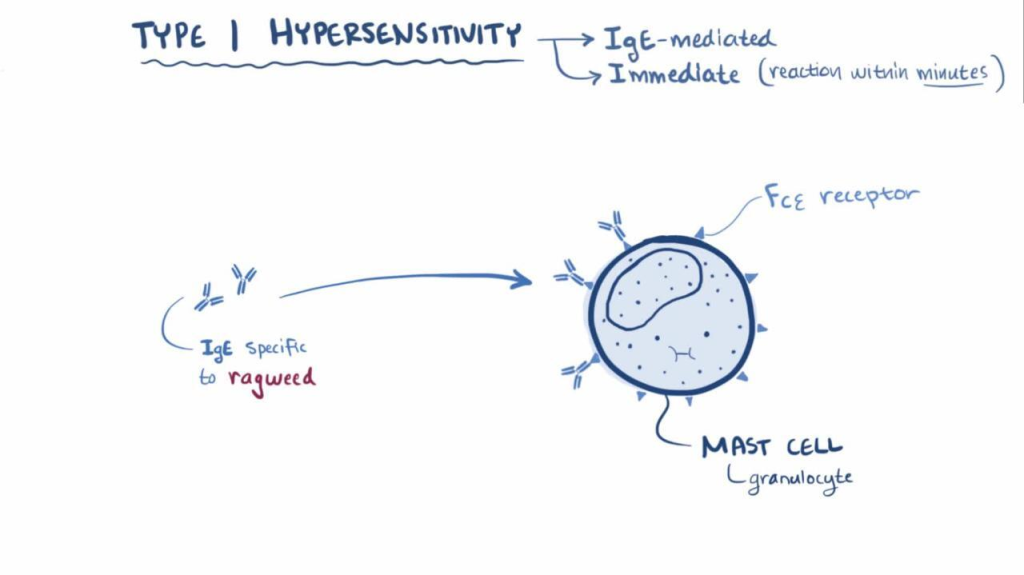
- Type 1 hypersensitivity is called the most severe type of hypersensitivity. is.
- In type one hypersensitivity, an immediate reaction is seen when a reaction is seen within a minute after exposure to an antigen.
- In type one hypersensitivity, edema is seen in many tissues of the body such as the larynx and hypotension is also seen.
- Type 1 hypersensitivity mediated by Ig-E antibody.
- And helper is T -lymphocytes .
Symptoms :
- Hypotension,
- Excessive mucus secretion,
- Itching,
- Allergic rhinitis,
- Hay fever,
- Allergic conjunctivitis,
- Hives,
- Anaphylactic shock (Anaphylactic shock) it’s a common symptom in type 1 hypersensitivity.
2) type : 2 hypersensitivity (Cytotoxic hypersensitivity):
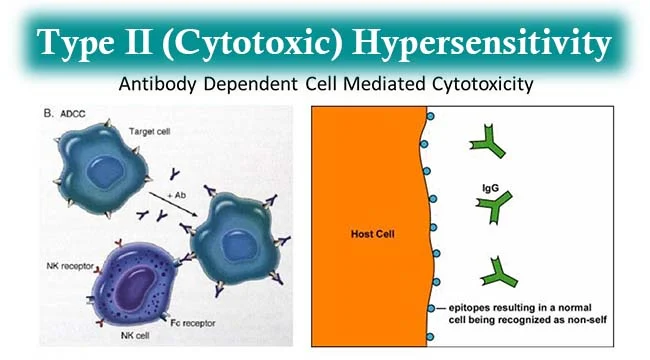
- When this type of hypersensitivity occurs, the body treats its own normal cells as antigens and creates an antibody reaction.
- Type 2 reactions stimulated by exogenous antigen ex: foreign tissues, cells or drug reactions.
- type 2 hypersensitivity mediated by IgG and Igm antibody
- Ex: Autoimmune hemolytic anemia (In this, our own body’s immune system destroys our own red blood cells and blood deficiency is seen in it Autoimmune hemolytic anemia is called).
3) Type : 3 hypersensitivity (immune complex hypersensitivity (immune complex hypersensitivity) :
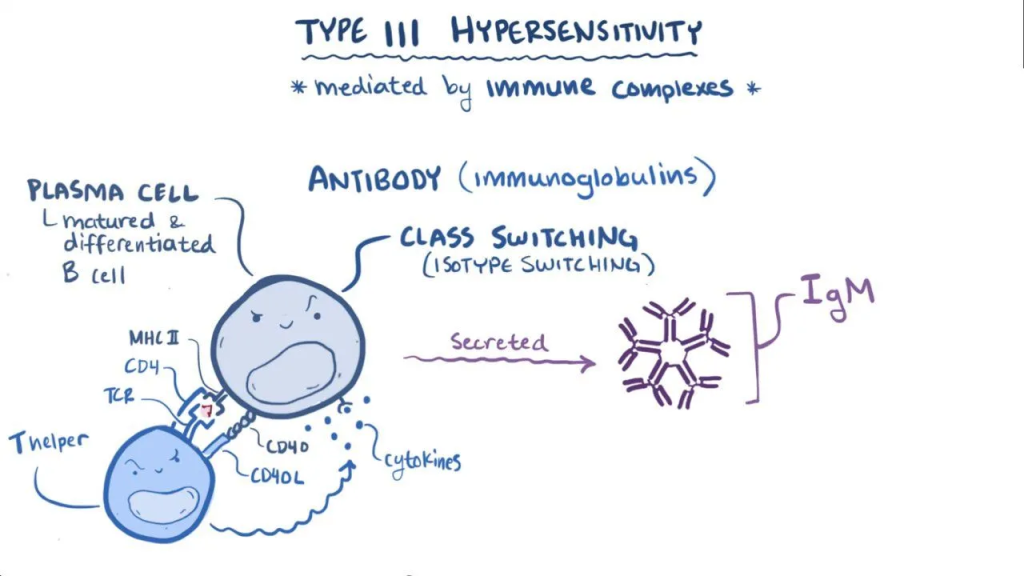
In this type of hypersensitivity, when an antigen binds with an antibody, an immune complex is formed.
Ex:
- SLE (Systemic lupus erythematous) ,
- RA (Rheumatoid arthritis) ,
- Nephritis,
- Certain type of Bacterial endocarditis.
4) type : 4 Delayed hypersensitivity:
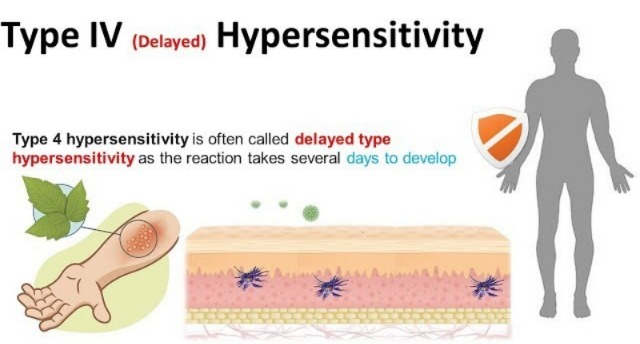
- This type of hypersensitivity is known as cellular hypersensitivity.
- This type of hypersensitivity is known as delayed hypersensitivity because its signs and symptoms appear 24 to 48 hours after coming into contact with any allergen. That is why it is called delayed hypersensitivity.
- this Hypersensitivity is mediated by T cells and macrophages.
- Ex:
intradermal injection of tuberculin (intradermal injection of tuberculin),
PPD (Purified protein derivatives),
contact dermatitis (contact dermatitis).
ALLERGIC REACTIONS (allergic reaction):

Explain the Allergic disorders:

Define/explain Allergy :

Allergy is a Hypersensitive Reaction in which when there is a harmless substance in the body, the body’s immune system (Immune System) has an inappropriate and harmful response against that harmless substance. It is called allergy.
Define/Explain Allergens:

Allergens act as foreign bodies in the body.
Allergens are substances that are responsible for activating allergic conditions in the body. When an antigen is environmental or exogenous (external) and triggers an immune response, it is called an allergy. The antigen that initiates the immune response is called an allergen.
Types:
There are two types of allergic reactions:
Atopic and Non-Atopic allergic reactions:
1) Atopic :
Atopic disorders involve a hereditary predisposition to local IgE reactions and antibody production.
- For example (Ex) :
- Anaphylaxis,
- Allergic Rhinitis,
- Allergic asthma,
- Atopic dermatitis .
2) Non Atopic :
- Ex: Latex allergy. There are two types of hypersensitivity reactions: Type 1 and Type 4.
Define /Explain Anaphylaxis:
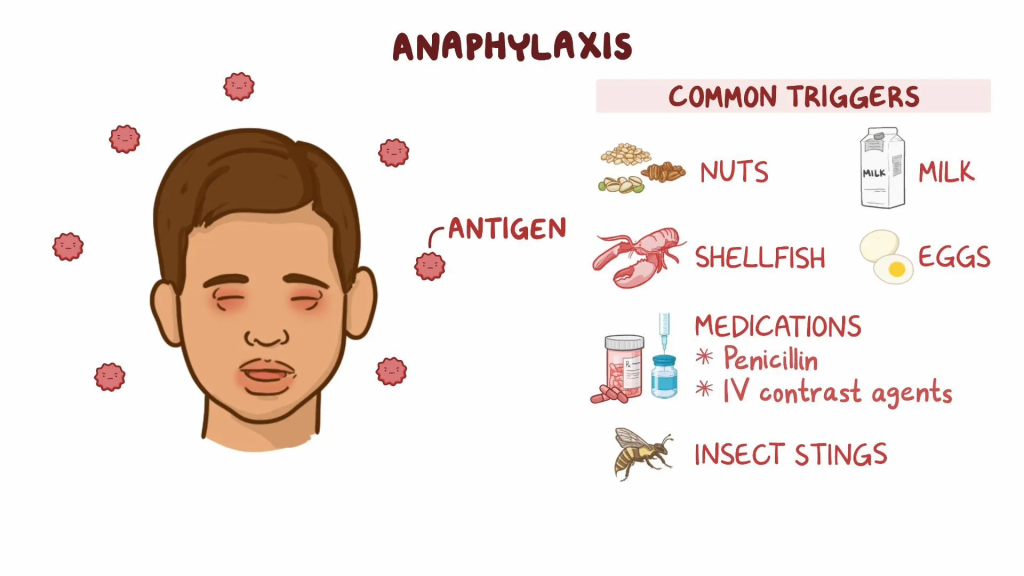
- Anaphylaxis is an immediate immunologic reaction (hypersensitivity) between any specific type of antigen and antibody. Anaphylaxis reaction occurs when mediators of a specific type of reaction are released. (Mediators – Histamine, Proteases are mediators produced by mast cells. Mediators are activated when antigens enter the body). This is a life-threatening allergic reaction (Anaphylaxis reaction is a severe life threatening condition) and it can happen within a few minutes. (For example: after a drug injection, after a fly bite).
- Anaphylaxis reaction results from IgE antibody. Anaphylactic reaction is triggered when any antigen is inhaled,
- Inhalation,
- Ingestion,
- Injection or
- Body exposure through skin contact.
PATHOPHYSIOLOGY:
Anaphylaxis is a severe allergic reaction of rapid onset that affects multiple body systems. The process is mediated by an immunologic reaction involving inflammatory mediators and cytokines released from mast cells and basophils, but often by non-immunologic mechanisms.
IMMUNOLOGIC :
In the immunologic mechanism, immunoglobulin E (IgE) binds to antigen. Foreign material activates an allergic reaction; foreign material is an antigen introduced into the body from outside). IgE bound to the antigen activates the FcαRI receptor on mast cells and basophils, which releases inflammatory mediators such as histamine. These mediators then increase the contraction of bronchial smooth muscles, further promote vasodilation, increase fluid leakage from blood vessels, and depress cardiac muscle. This is also an immunologic mechanism that does not rely on IgE, but it is not known whether it occurs in humans.
NON – IMMUNOLOGIC (Non-immunologic):
Non-immunologic mechanisms include substances that directly cause degranulation of mast cells and basophils. (Degranulation – This is a cellular process in which substances such as histamine are released when an allergen enters the body). These include factors such as different media, opioids, temperature (hot or cold) and vibration.
Foreign antigen
⬇️
Certain types of antibodies are present on mast cells and basophils
⬇️
This will release histamine and other bioactive mediators
⬇️
Now platelets, eosinophils and neutrophils will be activated
⬇️
Vascular permeability will change and due to this flushing, urticaria, angioedema and hypotension and bronchoconstriction will be seen
⬇️
Bronchospasm, mucosal edema and inflammation will be present.
Explain Etiology:
1)Food 🍛: It is a main common cause in children.
- Ex:
- 🥜 peanuts,
- 🌾Wheat,
- Shell fish ,
- 🐟 fishes,
- Chick pea,
- 🥛 milk ,
- 🥚 egg ,
- 🍚 Rice .
2) Medication 💊: The most common bigger factor in adults is medication.
- antibiotics ( like : penicillin),
- NSAID group drug
- ( Aspirine),
- Chemotherapy,
- herbal preparations,
- vaccines.
3) venom: Insect stings or biting.
- Ex: Honey bee🐝
4) less common cause is ( लेस कोमन कोज ) :
- Physical factors ,
- Biological agent,
- Latex ,
- Hormonal changes,
- Food additives ,
- Food colour , etc.
Explain risk factore:
Atopic disease (Atopic disease)
Ex:
- Atopic asthma (Atopic asthma),
- Atopic eczema (Atopic eczema),
- Atopic Rhinitis (Atopic rhinitis).
ExplainClinical manifestation/sign and symptoms:
The symptoms of an anaphylaxis reaction occur within 5 – 30 minutes of exposure to the allergen that causes you to be allergic. In some cases, symptoms of anaphylaxis appear more than an hour later.
Mild reaction:
- Itching,
- Tingling sensation in peripheral areas.
- Warmth sensation Sensation),
- Feeling of fullness in the mouth and throat.
- Nasal congestion.
- Swelling in the periorbital area.
- Tears in the eyes.
Moderate reaction (Moderate reaction) :
- flushing,
- warmthness,
- Itching ,
- anxiety,
- Bronchial Spasm
- Difficulty in breathing.
- Oedema in airway.
- dyspnea.
- Cough.
- wheezing sound ( high pitch music sound).
Severe systemic reaction:
- Severe Broncho Spasm,
- Severe Laryngeal Oedema,
- Severe Dyspnoea,
- Severe Dysphagia,
- Cyanosis ( bluish discolouration of skin, nails, around the eyes and lips )
- hypotension (hypotension),
- Abdominal cramps (abdominal cramps),
- Diarrhoea (diarrhea),
- nausea ( nausea),
- vomiting (vomiting),
- shock ,
- Cardiac arrest ,
- Coma.
Explain the Diagnostic Evaluation ( History Taking and Physical Examination ),
- history tacking and physical examination (History Taking and Physical Examination),
- allergy testing (Allergy Testing),
- wbc count (WBC Count).
- RAST TEST (Radio Allergo Sorbate Test).
- measures the blood pressure (Blood Pressure Measurement).
Explain the management of Anaphylaxis Reaction:
Medical management:
Management depends on the severity of the systemic reaction. It evaluates respiratory and circulatory functions.
Mild symptoms :
1) Apinephrine dose: 0.2-0.5 ml 1:1000 diluted
- Route : Subcutaneous/intramuscular
- time: within 10-15 minutes.
- 0.5 ml epinephrine diluted 1 : 1000 subcutaneously or intramuscularly every 10 – 15 minutes is given to the patient as per the physician’s order.
2)provide antihistamine,
3)provide corticosteroids.
Moderate and Severe reaction:
- increase the amount of epinephrine
- dose: 0.5ml (1:10,000) ,
- Route: intravenously,
- Time: within 5-10 minutes.
- Maintain the patient’s airway patency.
- Provide oxygen to the patient Provide therapy.
- Check the patient’s vital signs. (blood pressure, temperature,
Pulse, Respiration). - Keep the patient warm.
- Provide the patient with an anti-histamine (benadryl, diphenhydramine)
- Maintain the patient’s blood pressure by providing adequate amounts of fluid/volume expander.
- Provide the patient with corticosteroids (prednisone, methyle prednisone).
- Monitor the patient’s respiratory status.
- Check the patient’s level of consciousness.
- Intubate the patient if there is respiratory distress.
- Provide ventilatory support to the patient.
Nursing Management:
- Monitor the patient’s airway, breathing, and circulation (ABC).
- Assess the patient’s vital signs (blood pressure, pulse, respiration, temperature, and SpO2).
- Maintain patency of the patient’s intravenous (IV) line for administration of fluids and medications.
- Prepare any intubation equipment if needed. Keep.
- Provide oxygen support to the patient if needed.
- Instruct the patient to avoid allergen contact.
- Provide antibiotic medicine to the patient.
- Instruct the patient to avoid allergens to prevent anaphylaxis reactions (for example: perform an allergic test for the medicine or antibiotic to be given).
ATOPIC ALLERGIC REACTIONS:

Atopic Allergic reactions include Allergic Rhinitis, Allergic Asthma, Atopic Dermatitis, Urticaria, and Angioedema.
ALLERGIC RHINITIS :
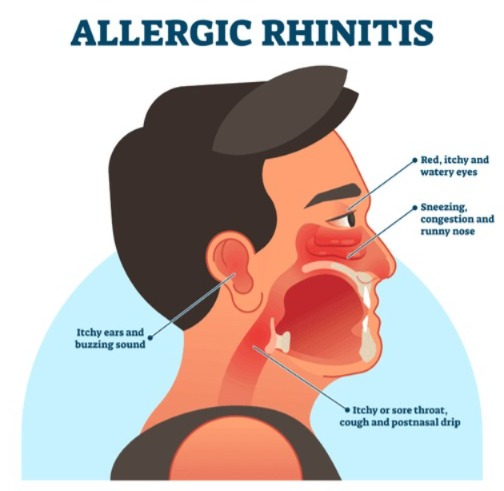
Allergic Rhinitis is also known as hay fever or Seasonal Allergic Rhinitis. It is a type 1 hypersensitivity reaction. Allergic rhinitis is caused by airborne particles, dust, pollen, weeds, grass, mold. It mainly affects the conjunctiva of the eye and the mucosa of the upper respiratory tract.
(Allergic rhinitis is a hypersensitive reaction of the nasal mucus membrane,
in which the body’s immune system gives a hypersensitive reaction to the allergen in the air through IgE antibodies, which results in symptoms like sneezing, runny nose and swelling inside the nose).
Symptoms =>
- Sneezing
- Nasal congestion
- Clear, watery discharge from the nose
- Itchy nose
- Itchy throat
- Soft palate and eyes
Often, the activation of inflammatory mediators in the patient leads to contraction of the smooth muscles of the airways, causing the patient to experience shortness of breath, cough, thick sputum, wheezing (this is an abnormal respiratory sound) and tightness in the chest.
Explain the cause/Etiology (Write the reason):
- Air born,
- pollens,
- dust,
- molds( mold),
- weeds,
- grasses,
Explain sign and symptoms/clinical manifestation (Write symptoms and signs):
- sneezing,
- nasal congestion,
- watery nasal discharge,
- nasal itching,
- Itching in the throat, soft palate and eyes,
- Wheezing sound,
- Dyspnea,
- coughing,
- tightness in chest,
- thick sputum,
- Headache,
- Fatigue,
- Loss of consciousness.
- Loss if sleep.
Explain the Diagnostic Evaluation (Write a diagnostic evaluation)
- History taking and physical examination.
- total serum IgE test,
- peripheral blood count,
- nasal smear,
- nasal provocation test.
Explain the management of Allergic Rhinitis (Write the management of allergic rhinitis):
1)Avoidance therapy,
2)pharmacological therapy,
1)Avoidance therapy,
Allergic therapy involves providing therapy that asks the person to stay away from the thing that causes the allergy and asks the person to avoid the thing that does not cause the allergy.
2)pharmacological therapy,
- provide antihistamine,
- provide adrenergic agents,
- provide mast cell stabilizer,
- Provide corticosteroids.
Explain the Dermatitis:
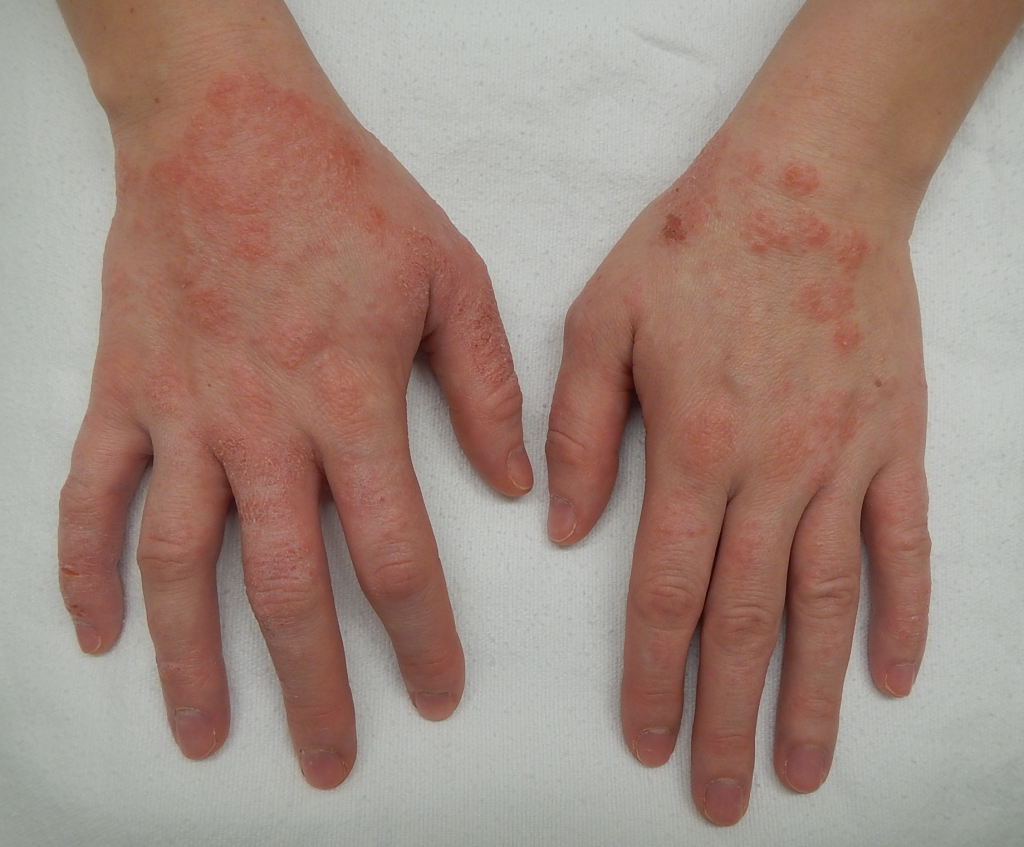
1) Define Ddermatitis (Define dermatitis):
- Inflammation of the Dermis layer of the skin its called dermatitis. (Inflammation in the dermis layer of the skin is called dermatitis).
2) Explain the type of Dermatitis:
1)ATOPIC DERMATITIS,
2)CONTECT DERMATITIS,
3)DERMATITIS MEDICAMENTOSA ( Dermatitis Medicamentosa).
1)ATOPIC DERMATITIS:
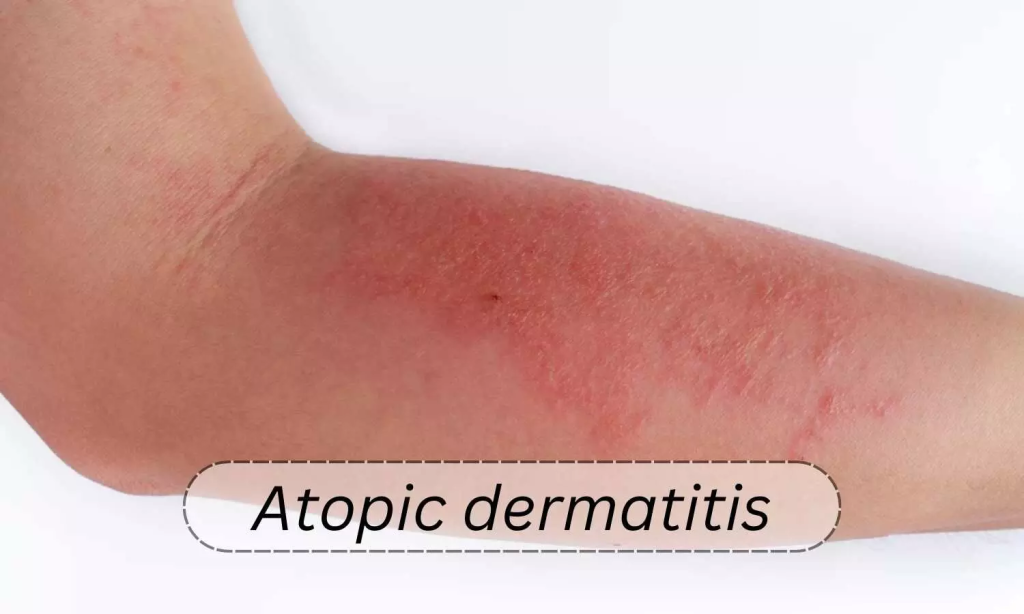
- Atopic dermatitis is a type 1 immediate hypersensitivity reaction. Atopic dermatitis is due to IgE antibody (it is an atopic allergic reaction caused by IgE antibody). Atopic dermatitis is mainly seen in infants and children. In atopic dermatitis, pruritus and irritability are seen in the skin due to high levels of histamine in the skin layer.
- The patient has a family history of hypersensitivity. Its symptoms include vasodilation of blood vessels leading to interstitial edema and vesicle formation. The patient experiences itching, excessive skin irritation, skin dryness, and sweating. If the skin is repeatedly touched or scratched, there is immediate redness.
2) CONTACT DERMATITIS:
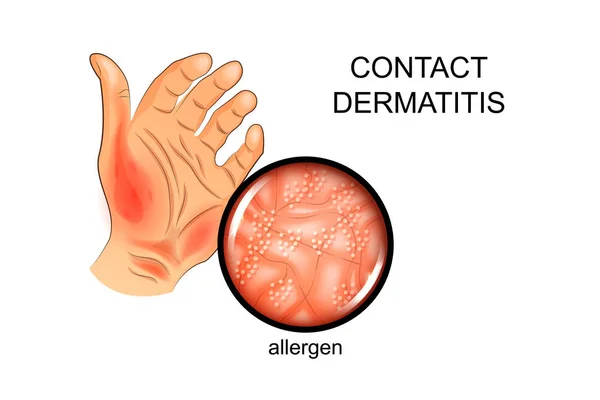
- Contact dermatitis is a type 4 delayed hypersensitivity reaction.( Contact dermatitis is a type 4 delayed hypersensitivity reaction). Contact dermatitis is mainly caused by direct contact of the skin with chemicals and allergens. For example; Metals containing mercury or nickel, cosmetics, poisons, oak, rubber, etc.).
- Its symptoms include itching, redness, burning sensation, skin lesions (papules, vesicles and bullae) and swelling. It can also cause crusting, drying and eventually peeling of the skin. Due to this repeated occurrence, the skin becomes thick and pigmentary changes are seen.
3) DERMATITIS MEDICAMENTOSA (Drug reaction):
- Dermatitis medicamentosa is a type 1 immediate hypersensitivity reaction. This dermatitis occurs due to direct skin contact with a medication. This dermatitis is seen in a person who is allergic to medications, so he should be asked to stop taking that medication.
3)Explain Etiology /cause (explain the cause):
- Due to contact with any allergic substance.
- Any irritating material Due to contact with.
- 💊 Due to medications.
4)Explain sign and symptoms/clinical manifestation (write symptoms and signs):
- Itching,
- Burning,
- Redness in the skin,
- Lesions in the skin,
- Happening in the heels,
- Wheeling, crusting and finally dring of skin,
5) Explain the Diagnostic Evaluation:
- History taking and physical examination.
- complete blood count (Complete Blood Count (CBC)),
- assessment of WBC count,
- RAST TEST ( radio allergo sorbate test / Radioallergio sorbant test ( RAST )),
- sputum of nasal and bronchial secretion test for present of eosinophil (To check for the presence of Eosinophils in the nose and bronchial secretions)
- assess the 🫁 Pulmonary function test (Pulmonary function test).
- patch test on the skin .
Explain Management of Dermatitis :
Medical management:
- provide antihistamine medicine to the patient
- provide corticosteroids medicines to the patient
- provide decongestant drug (to provide decongestant drug to the patient).
- provide mast cell stabilising drug (cromolin/ nedocromil this drug inhibit the release of histamine).
- provide leuckoterine recepter antagonist to the patient.
- provide immunotherapy to the patient.
- Wash the clothes with mild detergent.
- Humidify the dry air in winter.
- Keep the room temperature between 20°c to 22°c.
- Stay away from things that cause allergic conditions such as animals, dust, sprays, perfumes, etc.
- Keep the skin moisturized.
Explain the Nursing Management:
Nursing Assessment:
- Patient’s eyes, skin, mouth etc. Assess.
- Take a complete health history of the patient.
- Assess the patient for any rashes, breathing difficulties.
- Perform a complete physical examination of the patient.
- Frequently check vital signs (temperature, pulse, respiration and blood pressure) and check for hypotension, tachycardia and tachypnea.
- Check the skin for color, capillary refill, temperature, and swelling.
- Check the level of concentration.
Nursing Management:
- Assess the patient’s vital signs.
- Assess the patient’s skin color.
- Assess the patient’s level of consciousness.
- Assess the patient’s allergic condition before giving a blood transfusion Ask whether or not.
- Advise the patient to identify allergens (foods, insects, environmental allergens).
- Advise the patient to avoid exposure to mold or pollen.
- Identify the food to which the patient is allergic.
- Advise the patient to remove dust from their home.
- Early identify the patient’s allergies and provide them with appropriate treatment.
- Provide the patient with prescribed medicine.
Urticaria
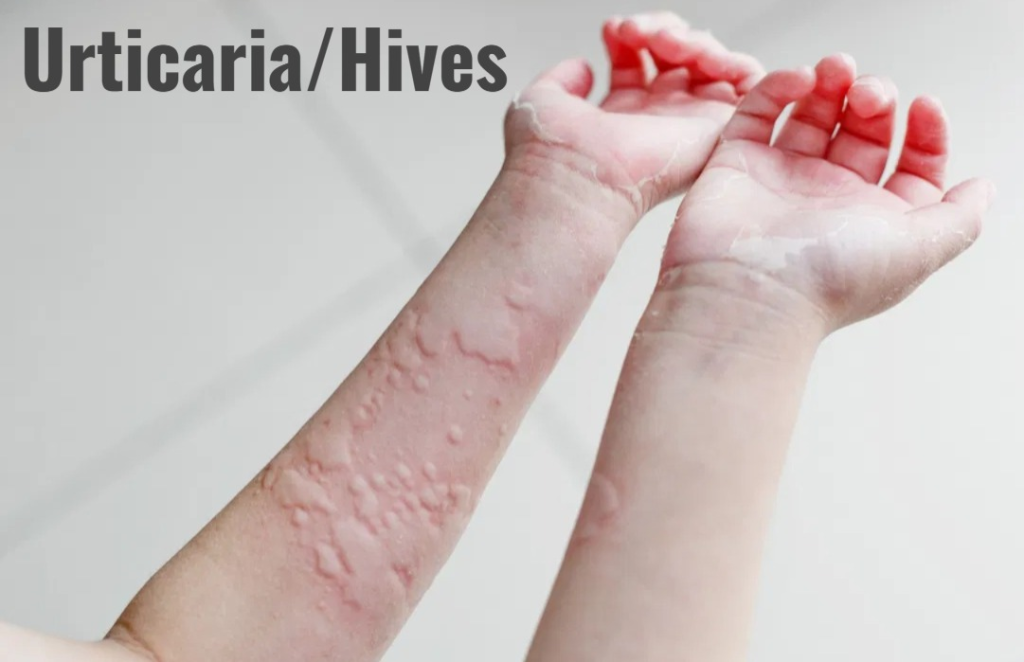
- Urticaria is a type 1 hypersensitivity allergic reaction characterized by transient wheals (pinkish, raised, swollen, and pus-filled areas), itching, and local discomfort. They can be found in any organ of the body and vary in size and shape.
- They develop after exposure to an allergen and last for a few minutes or hours. Histamine is released and causes localized vasodilation, wheezing and flaring, which can also affect other organs of the body such as the larynx, gastrointestinal tract and urticaria. Its signs and symptoms appear within minutes or hours after exposure to any allergen.
ANGIONEUROTIC EDEMA :
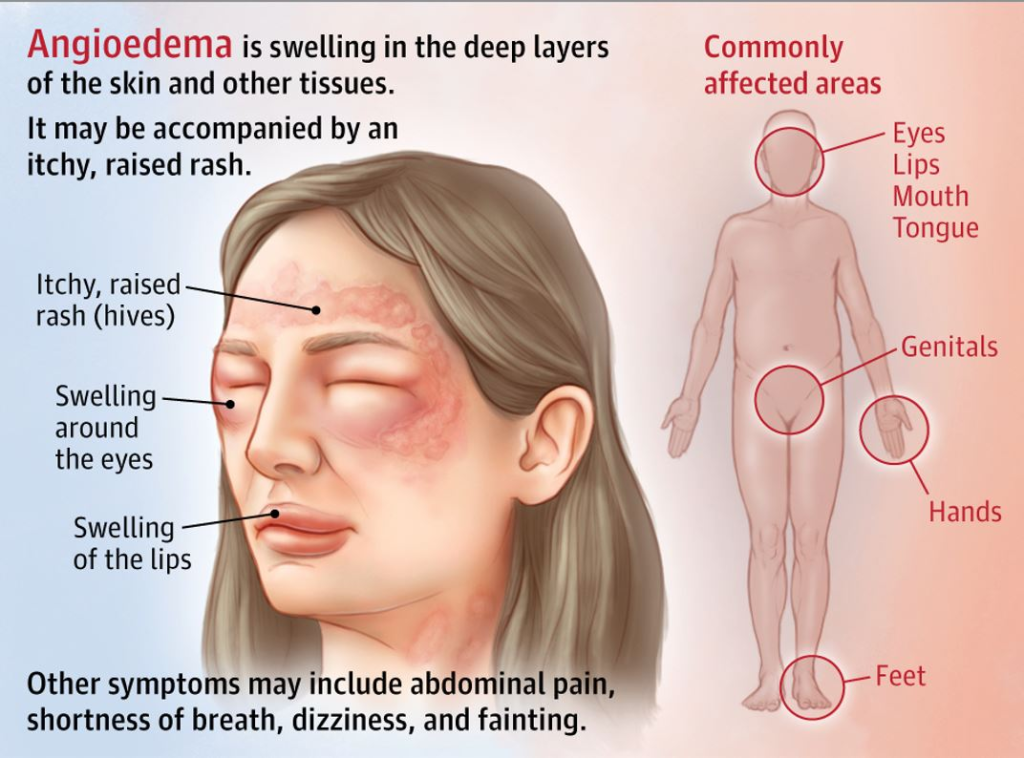
- It is a type of local skin lesion. It also involves the deep layers of the skin and therefore is more inflamed than a discrete lesion (a lesion that has a distinct border). These lesions mainly involve the eyelids, lips, tongue, larynx, hands, feet, gastrointestinal tract, and genital area. The swelling mainly starts from the face and then progresses to different areas of the airway and body.
- There is a burning sensation or itching in the area and if it is in the Gastrointestinal Tract, it can also cause abdominal pain.
FOOD ALLERGY:

- A food allergy occurs when the body’s immune system overreacts to a food or food substance. A hypersensitivity reaction occurs within a minute of exposure to a food allergen. It is dangerous and can be treated immediately with an injection of epinephrine (adrenaline). The most severe allergic reaction is anaphylaxis – a life-threatening reaction to the whole body that causes difficulty breathing, a drop in blood pressure (hypotension) and a decrease in heart rate.
Foods that can cause allergies:-

- (Egg) Egg,
- (Milk) milk,
- (Peanut) Mahali,
- (Tree nuts) Tree nuts,
- (Seeds) Sesame and mustard seeds,
- (Fish) Fish,
- (Shellfish) Shellfish,
- (Wheat) Wheat,
- (Soy products) Soy products,
Explain sign and symptoms / Clinical manifestation (Write signs and symptoms):
- Local reactions may include diarrhea or vomiting.
- Urticaria (systemic response to food absorption).
- Shortness of breath (shortness of breath, difficulty breathing)
- Wheezing Sound
- Repetitive Cough
- Shock or circulatory collapse (blood circulation does not reach properly)
- Angioedema (swelling of local tissue) is seen in the tongue, lips, hands, feet, etc…
- Angioedema (swelling of tongue, lips, hands, feet, etc…) in the tongue, lips, hands, feet, etc…
- Sore throat and difficulty swallowing
- Skin turns pale or blue
All these symptoms occur within about two hours of eating the food or they may appear within minutes. A delayed reaction (after 4-6 hours) may also occur. Eczema is most commonly seen in children.
Explain the Diagnostic Evaluation:
History tacking and physical examination:
- How much and what has he eaten?
- How long did it take for the symptoms to appear?
- What symptoms have you experienced and how long did they last?
Skin test :
- For food allergens, a small amount of the food in liquid form is placed on the skin or back, then the skin is pricked with a needle and the liquid is allowed to flow down. If a raised bump is seen at that place, it is a positive test, meaning that food is considered an allergen.
Blood test:
This test is done to find out the amount of antibody IgE in any particular food.
TREATMENT (ट्रात्मन) :
- The main aim of treatment is to advise the patient to avoid the food that causes the allergic reaction.
- Advise the patient to carefully check the labels on food products.
- Tell the patient to be careful when eating at any hotel Keep.
- Epinephrine is a safe drug.
- Steroids (for example: cortisone) can be given in an emergency.
- Antihistamines: diphenhydramine (Benadryl) and cetirizine can be given.
- Short-acting bronchodilators can also be given.
SERUM SICKNESS:
- Serum sickness is a type 3 hypersensitivity reaction that can occur in response to the injection of heterologous or foreign proteins or to certain drugs such as penicillins and sulfonamides. It results in the formation of IgG or IgM antigen-antibody immune complexes in the circulation. This complex is deposited on the walls of small blood vessels, on the walls of the kidneys and on the walls of the joints.
ETIOLOGY (Causes):
DRUGS:
Antitoxins (tetanum antitoxin), antivenoms, streptokinase, vaccine, antibiotic (Cephalosporin, Ciprofloxacine Antibiotics (cephalosporin, ciprofloxacine) , Furoxane , Metronidazole , Penicillin , Streptomycine , Tetracycline , Sulphonamides , Allopurinol , Barbiturates , Carbamazapine , Iodides .
Antibodies :
Monoclonal antibodies. For example: Infliximab (Crohn’s disease and Used in rheumatoid arthritis, omalizumab is used in the treatment of allergic asthma, rituximab is used to treat many diseases such as rheumatoid disorders, lymphoma.
Explain sign and symptoms/clinical manifestation (Write signs and symptoms):
- Fever (temperature 104°F), usually appears before the rash.
- Urticaria or itching and rash
- Joint pain (arthralgia) mainly in the joints of the fingers and toes.
- Lymphadenopathy (swelling of the lymph nodes, mainly near the injection site, in the neck and head).
- Fatigue
- Hypotension
- Glomerulonephritis (glomerulonephritis)
- Proteinuria ( proteinuria : presence of protein in the urine )
- Hematuria ( hematuria , : presence of blood in the urine )
- Shock
Explain the Diagnostic Evaluation:
- A diagnosis can be made based on a sufficient history from the patient and the medications currently being given.
TREATMENT (Treatment) :
- Symptoms usually disappear within 4 – 5 days after stopping the drug that caused the allergic reaction.
- Corticosteroids. For example: Hydrocortisone and antihistamines and analgesics (ibuprofen) are the main line of treatment.
- Plasmapheresis (removal of harmful components in plasma) can also be done.
PREVENTION:
- Avoid antitoxins that induce serum sickness. This is the best way to prevent it.
- A skin test should be done before giving antibiotics (penicillin).
latex Allergy:
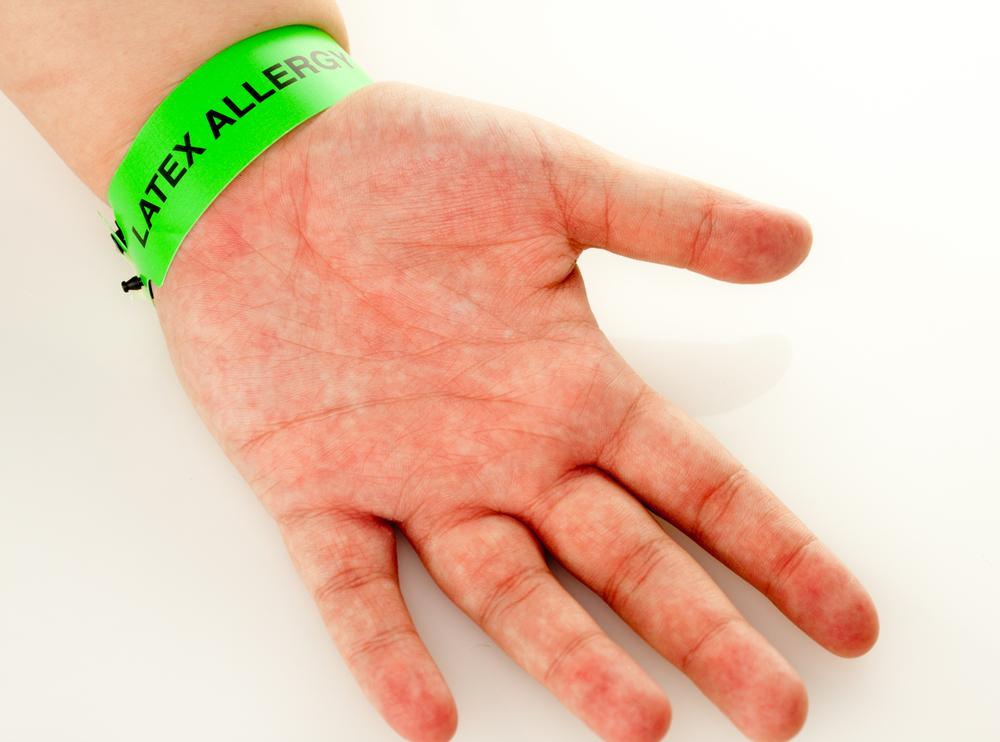
- Latex allergy is a medical term that refers to an allergic reaction to natural rubber and synthetic (man-made) rubber. Latex allergy is a reaction to certain proteins found in latex, which is a natural rubber, a milky liquid that comes from the rubber tree.
- Healthcare facilities use gloves and many other latex-containing products. For example: IV tubing, syringes, oxygen masks, urinary catheters, and adhesive tape. Gloves are powdered with cornstarch, and when removed, these particles are released into the air. Due to this, both the Respiratory System and Skin come into contact with latex.
- Natural rubber is made from the sap of the latex rubber tree. Latex surgical gloves, balloons, condoms, rubber bands, rubber balls, baby feeding bottles – all of these contain natural rubber. The protein found in fruits such as bananas (🍌 banana), avocados (🥑evocado), chestnuts (🌰 chestnuts), kiwis (🥝kiwis) and tomatoes (🍅 tomato) is similar to the protein found in natural rubber. All these foods increase the risk of latex allergy.
TYPES OF LATEX ALLERGY:
there are two types of latex allergy
1)type :1 IgE mediated immediate hypersensitivity reaction,
2)type :4 Delayed hypersensitivity reaction.
Latex protein is the allergen that causes latex allergy. The more a person is exposed to latex protein, the more likely they are to develop a latex allergy.
Explain sign and symptoms/clinical manifestation (write symptoms and signs):
- itching,
- dryness,
- cracking of the skin followed by redness,
- Swelling and crusting occur within 24-48 hours. These symptoms are most often seen on the back of the hand.
- Prolonged exposure can cause lichenification (thickening and hardening of the skin), scaling (roughness), and hyperpigmentation.
- Type 1 hypersensitivity includes rhinitis,
- asthma,
- conjunctivitis, and anaphylaxis.
- The patient may have urticaria,
- wheezing,
- shortness of breath,
- laryngeal edema,
- increased heart rate,
- Angioedema, hypotension, and cardiac arrest may occur in ANGIOD.
Explain the Diagnostic Evaluation:
- The doctor will ask about the history and symptoms of latex allergy. Along with this, the doctor will do a complete physical examination to determine if there are any other medical problems.
- He may also recommend two other tests:
1 – Skin Test:
- In this test, a hole is made in the skin and it is exposed to latex and the reaction to latex is identified. In this test, a small amount of latex is placed on the front or back of the skin of the hand. Then the skin is pricked with a needle and a small amount of latex is allowed to go under the skin. If you are allergic to this particular substance, then a welt will appear on the skin at that place (allergic reaction). Thus, a skin test is done to assess latex allergy.
2 – Blood Test:
- A blood test checks the immune system’s response to latex, which is checked by allergy antibodies in the blood called immunoglobulin E antibodies. The blood sample is sent to a medical laboratory where it is checked for latex sensitivity.
MEDICAL MANAGEMENT:
- Avoid using products that contain latex.
- Use antihistamines and epinephrine.
- Advise healthcare providers to use non-latex products.
- Advise hand washing after removing gloves to reduce latex exposure.
Nursing Management:

- Collect a complete history from a health care provider to identify workers who are sensitive to latex.
- Assess risk factors in people with hay fever, asthma, and certain food allergies.
- Advise people to use powder-free gloves.
- Use latex-free gloves
- Wash hands after removing gloves Wash
- Keep areas that have latex dust clean.
PREVENTING LATEX ALLERGY:
Avoid using powdered gloves
Latex gloves are often coated with a fine latex powder that helps them stick together. However, this powder can release latex proteins into the air, which can be inhaled. Powder-free gloves help prevent the spread of latex proteins into the air, which reduces the risk of developing latex allergies. So provide your workers with powder-free and low-protein latex gloves.
Choose gloves carefully
- If there are enough latex-free gloves, choose them.
- Use thick rubber gloves instead of latex surgical gloves for housework.
- Don’t wear gloves unless necessary. For example, gloves are not required when taking blood pressure or pulse.
- If gloves are required when preparing food, choose plastic or non-latex gloves.
Use latex gloves properly
- Wash and dry hands thoroughly before putting on and taking off gloves.
- Avoid using oily hand creams or lotions. It breaks down latex and makes the protein stick more to the hands.
- Do not pull the gloves while putting them on or removing them.
IMMUNOTHERAPY (Immunotherapy):

In immunotherapy, desensitization/hyposensitization is done to the allergen. Immunotherapy is mainly used for IgE (immunoglobulin E) mediated diseases. Time and compliance are essential for successful treatment of this therapy.
INDICATION (Indications):
- Allergic rhinitis
- Conjunctivitis
- Allergic Asthma
- A sting allergy that is not controlled by avoidance of the allergen.
GOAL OF IMMUNOTHERAPY:
- The goal of immunotherapy is to reduce the level of IgE in the circulation, along with increasing the level of the antibody IgG, which can reduce cell mediator sensitivity.
MECHANISM OF ACTION:
- When an allergic patient is exposed to an allergen, the level of IgE immunoglobulin increases and the antibody combines with the allergen and histamine is produced.
- Allergens are easily bound to IgG immunoglobulins. In immunotherapy, an external injection of the allergen is given that is high in IgG. The allergen bound to IgG prevents IgE from binding to mast cells, which prevents mast cell degranulation and reduces the number of tissue-damaging processes. Immunotherapy reduces the levels of IgG and allergen-specific T suppressors.
METHOD OF ADMINISTRATION:
- The specific allergen is identified through a skin test or blood test.
- Injections of the identified allergen (allergy vaccine) are initiated.
- Initially, a small amount of diluted allergy vaccine is given at weekly intervals.
- The amount and concentration are gradually increased and the dose is given until the maximum tolerated dose is achieved.
- Maintenance doses are given at 2-4 week intervals for several years to maximize benefit.
- Many allergens are now standardized (dust mites, cat grass and ragweed pollen, Hymenoptera venom [yellow jackets, Yellow and white-faced hornets, bees, wasps ] ).
NURSING MANAGEMENT ( Nursing Management):
- Phlebitis after injection is rare but is a risk.
- Health care facilities such as epinephrine, trained personnel, and emergency equipment should be available when administering the injection.
- Ask the patient to stay in the office for 30 minutes after the injection, during this time there is a risk of anaphylaxis.
- If there is excessive local reaction (redness, induration) after the injection, check the next dose and reduce it; This can reduce the risk of systemic reactions.
- If injections are missed for several weeks, the dose may need to be reduced to prevent reactions.
- Medications, such as antihistamines and decongestants, should be continued until symptoms are relieved (12 – 24 months).
- Environmental controls should be maintained to maximize the effects of immunotherapy.
Define autoimmune disease:
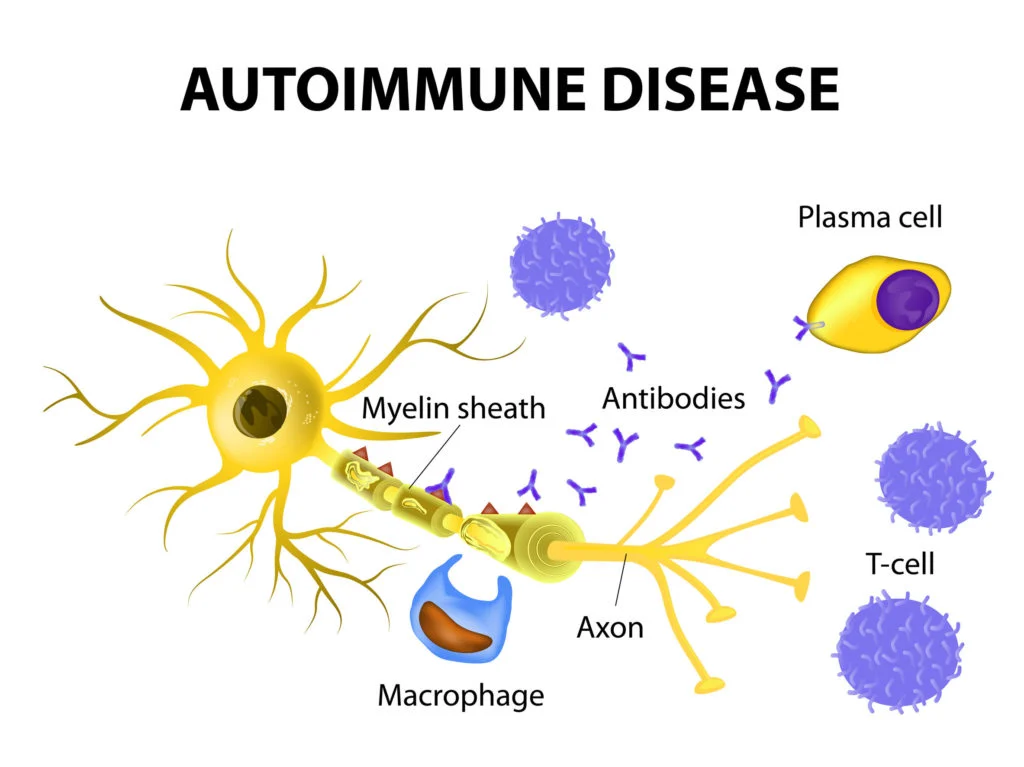
- Normally the body’s immune system does not produce any antibodies against the body’s own cells, but in Autoimmune Disease, the body’s immune system produces antibodies against normal cells and damages normal cells, which is called autoimmune disease.
Define Rheumatoid Arthritis.
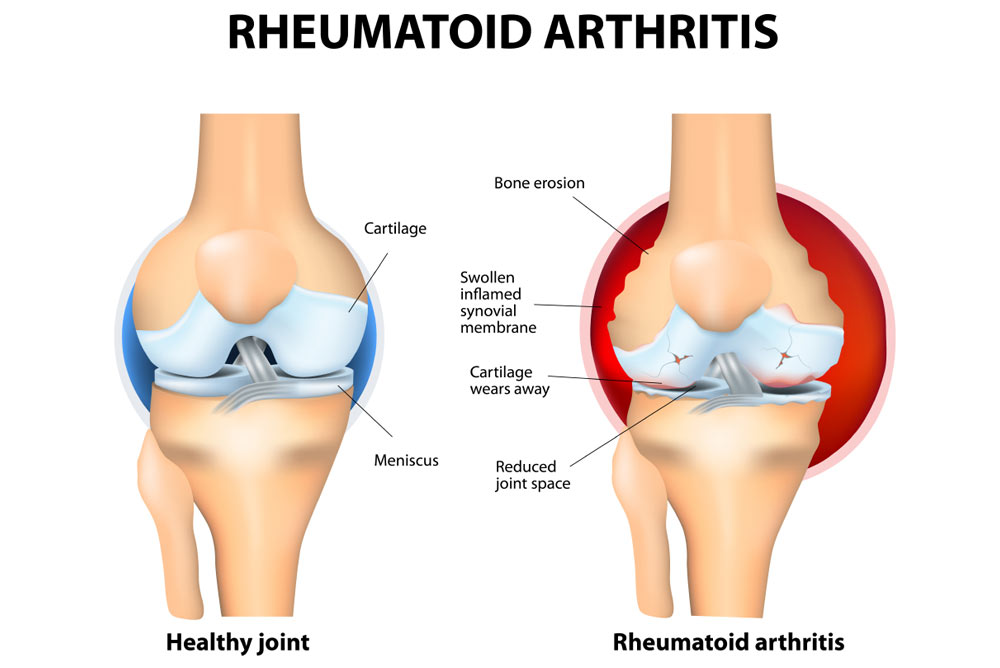
- Rheumatoid Arthritis is a chronic, systemic, autoimmune connective tissue disorder that causes inflammation of the tissues surrounding the joints, including the synovial membrane, and destruction and proliferation of synovial members, resulting in joint destruction, ankylosis (stiffness of the joint) and deformity (physical deformity).
- In autoimmune disease, the body’s immune system produces antibodies against normal cells and damages normal cells. This is called autoimmune disease. Joint pain, stiffness, and immobility occur.
- Rheumatoid arthritis also affects other organs of the body, including the skin, eyes, lungs, and blood vessels.
Explain Etiology of Rheumatoid Arthritis (Causes of Rheumatoid Arthritis):
- Rheumatoid The exact cause of arthritis is unknown.
- Due to genetic factors (if a parent has this disease, there is a possibility of it in their child),
- Due to stress.
- Sex: women are more likely to develop Rheumatoid Arthritis.
- Due to any infectious agent.
- Age mainly between 30 and 60 years In age.
- Due to environmental factors.
- Due to family history.
- Due to hormonal effects.
- Due to long-term smoking.
- Due to metabolic and biochemical abnormalities.
- Any bacteria, Due to fungal, viral infection.
- Due to immunological response.
Explain the Stages of Rheumatoid Arthritis (Explain the Stages of Rheumatoid Arthritis).
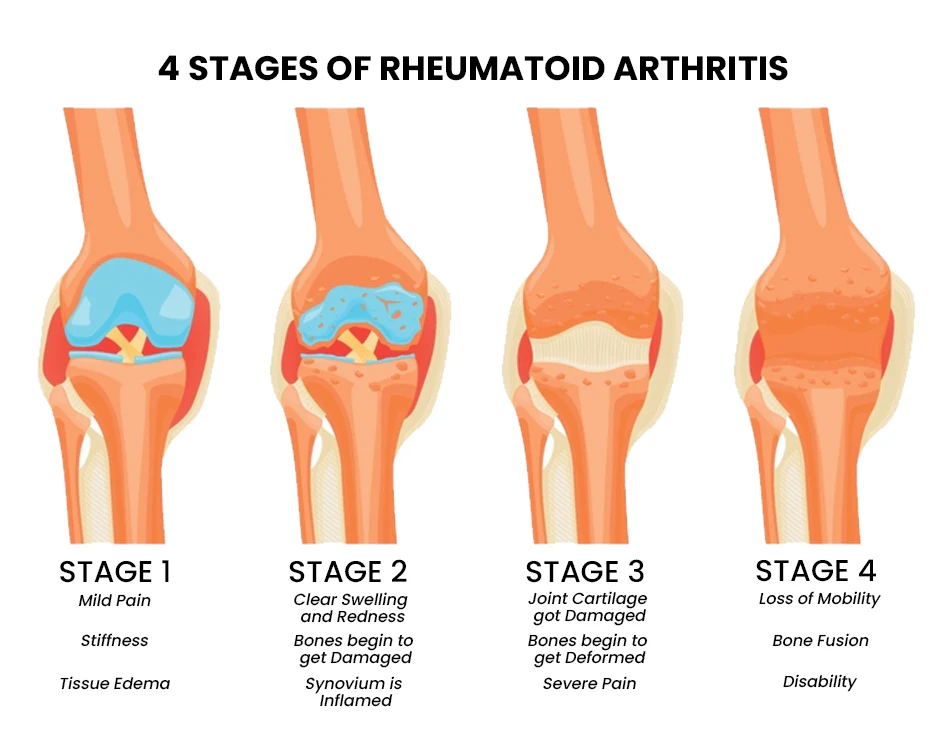
1) Synovitis,
2) Pannus formation,
3) Fibrous tissues Ankylosis,
4) Bony Ankylosis.
1) Synovitis:
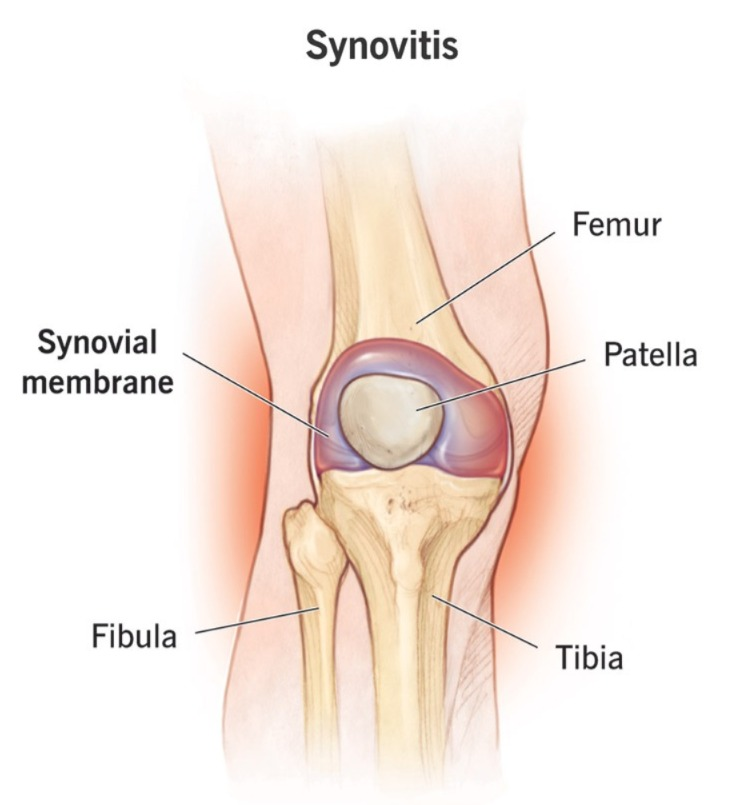
- In the synovitis stage, when there is an infection in the body, that infection affects the synovial membrane of the joint and due to this, the synovial members become infected and inflamed and due to this, synovitis occurs and synovial fluid increases.
2) Pannus formation:
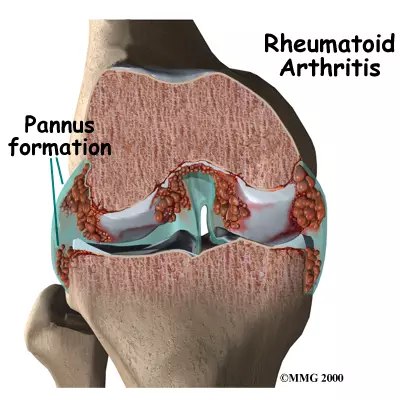
- In this, the synovial fluid gets invaded and becomes very thick and this fluid increases around the capsule of the joint.
3) Fibrous tissues Ankylosis:
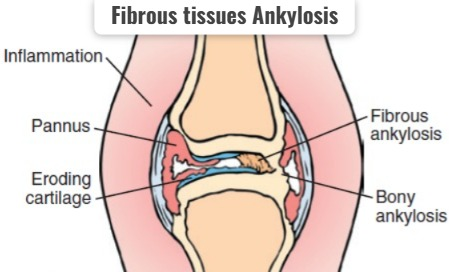
- In this, the synovial fluid increases a lot and it becomes stiff and it gets stuck around the joint and forms a hard structure.
4)Bony Ankylosis (Bony Ankylosis):
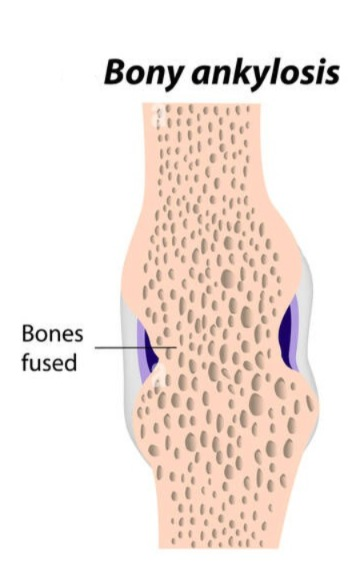
- In this, the fibrous tissue forms a very hard structure and forms a bone-like formation and due to this the joint becomes immobilized And stiffness occurs in it.
Due to any etiological factor.
|
\/
Infection of synovial membrane occurs.
|
\/
Inflammation of synovial members occurs.
|
\/
Synovial fluid is secreted from synovial members.
|
\/
This fluid progresses and accumulates in the bone.
|
\/
Then the bone becomes very hard and stiff Which is an immobilized bone.
|
\/
Rheumatoid arthritis .
Explain Clinical Manifestation/ sign and symptoms :
- The affected joint becomes red, warm.
- The joints become swollen and stiff and tender.
- Morning stiffness in the joints.
- Arthritis occurs in more than three bones.
- The joint becomes swollen (sponge like).
- Arthritis occurs in the joints of the hands.
- firm bumps of tissues under the skin on Arms.
- Rheumatoid nodules form.
- Rh factor positive.
- Fluid accumulation occurs in the ankles.
- The joint loses its range of motion and becomes deformed.
- Muscular atrophy around the affected joint.
Ulnar Deviation:
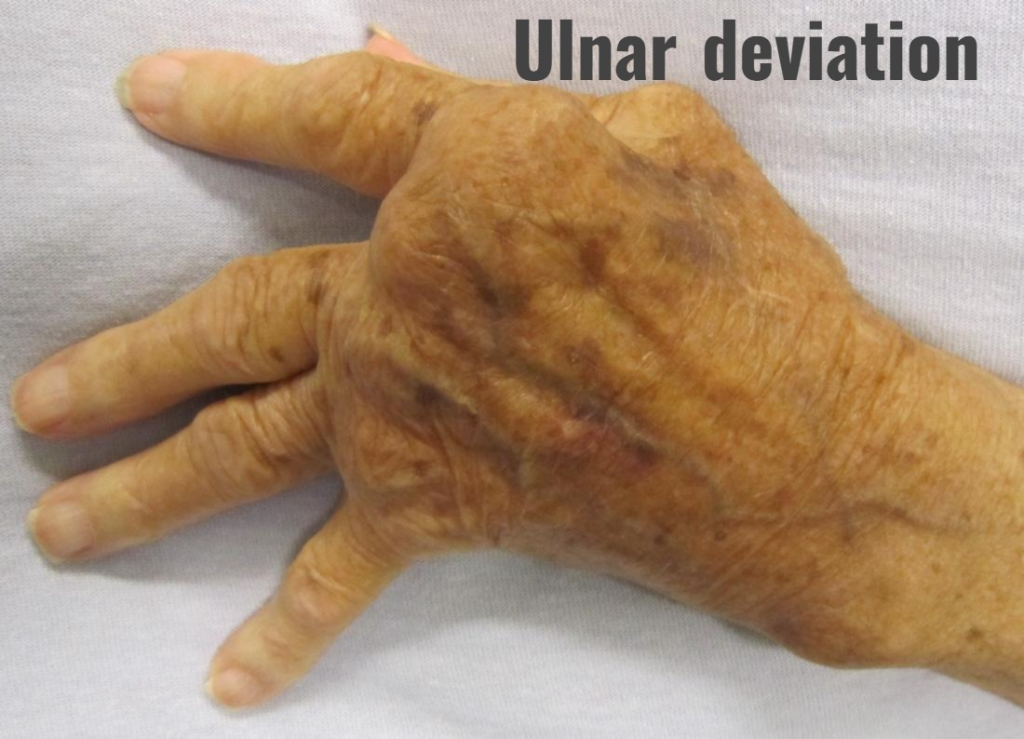
In this, the finger deviates towards the ulnar surface.
Swan Neck Deformity:
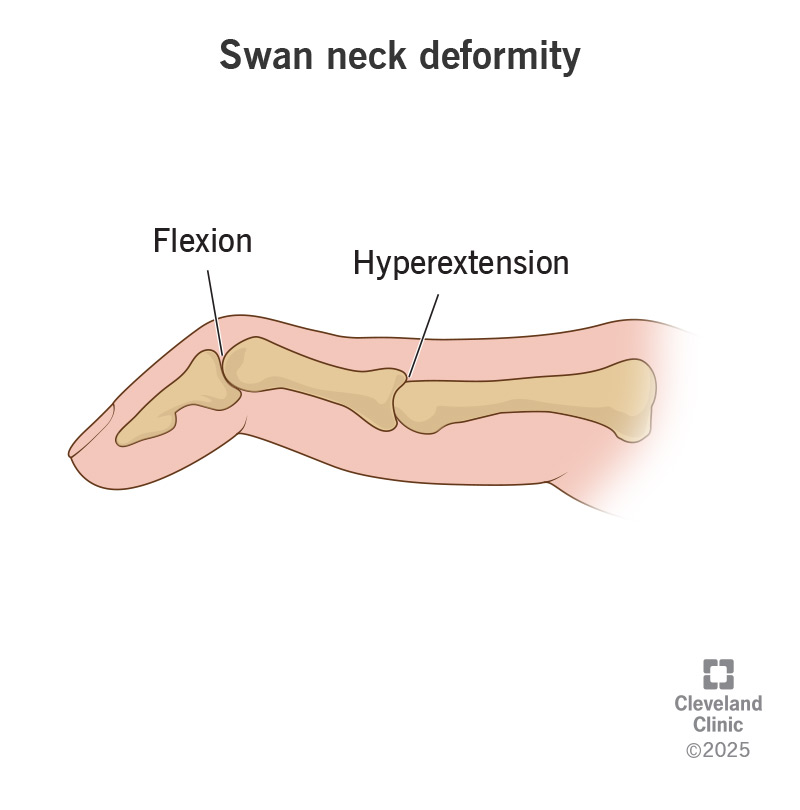
In this, the finger becomes a swan’s head.
Bouterine Deformity:
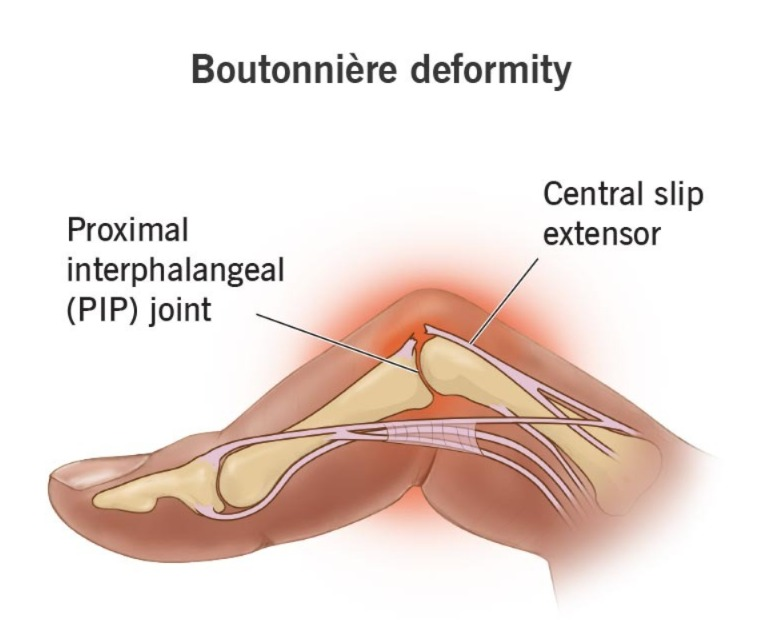
Ama, finger is bent.
- knock knee.
- Difficulty in Sleep .
- Numbness and tingling sensation.
- Burning sensation in hand and foot.
- Module formation within the skin.
- Burning sensation in the eyes.
- Itching and discharge.
- Dry mouth and eyes.
- Chest pain.
- Weakness.
- Difficulty breathing.
- Fatigue.
- Loss of appetite.
- Weight loss.
- Low grade fever.
- Malaise.
- Depression.
- Lymphadenopathy.
- Inflammation of blood vessels.
- Multiple organ involvement (pericarditis, Osteoporosis, Anemia, subcutaneous nodules, vasculities, neuropathy, fibrotic lungs disease).
Explain Diagnostic Evaluation (Write diagnostic evaluation):
- history tacking and physical examination (History Taking and Physical Examination).
- Rheumatoid factor test: RA positive (Rheumatoid Factor Test).
- Antinuclear Antibody test (Antinuclear Antibody Test).
- Erythrocyte sedimentation rate (ESR – Erythrocyte Sedimentation Rate ).
- C-reactive protein ( crp test C ).
- complete Blood count test .
- comprehensive metabolic panel ( to monitor kidney and liver function).
- synovial fluid analysis (synovial fluid changes from transparent to milky ,cloudy, and dark yellow fluid).
- Arthroscopic examination .
- X Ray .
- joint Ultrasound .
- MRI.
Explain the management of rheumatoid arthritis (Write the management of rheumatoid arthritis):
Medical Management (Medical Management):
1) NSAID (NON STEROIDAL ANTI INFLAMMATORY DRUG):
This medicine is used to relieve pain and inflammation.
Ex: ibuprofen,
Naproxen sodium.
2) DMARDs ( Disease modifying Antirheumatic Drugs):
These are mainly given in conditions such as moderate to severe Rheumatoid Arthritis.
Ex: imuran,
Anti malarial medication,
Panicillamine and mithotrexate.
3) Antimalarial medication :
This medicine mainly uses hydroxychloroquine along with methotrexate.
4)Corticosteroid:
Corticosteroid is used to relieve inflammation.
5)Biological agent:
Tnf-a antagonist targets B cells and T cells.
- Actemra in biological agent,
- Rituxan,
- Remicade,
- Enbrel,
- Includes Kindred.
6) Immunosuppressants (Immunosuppressants):
The immune system is out of control in rheumatoid arthritis. This medication weakens the immune system.
Ex: Azathioprine (imuran, azasan),
Cyclosporine.
7) Tumor necrosis factor a:
This medicine inhibits the inflammatory chemical that is tumor necrosis factor.
This medicine inhibits the inflammatory chemical that is tumor necrosis factor.
Explain Surgical management (Explain Surgical Management):
1) Joint fusion:
In this, the joint is surgically fused to stabilize the joint.
2) Synovectomy:
In this, the joint lining is removed is removed.
This is mainly used to remove the inflamed tissues that are creating pain.
Synovectomy is mainly used to reduce swelling and slow down joint damage.
3) Tendon repairs:
The surgeon repairs the tendons around the joint that are inflamed and damaged, causing loss of tendons. and keeps it stable.
4) Total joint replacement:
In joint replacement, the surgeon removes the damaged joint part and inserts a prosthesis made of metal or plastic in its place.
Explain nursing management:
- Assess the patient’s pain level.
- Assess whether the patient has morning stiffness.
- Provide the patient with a comfortable position.
- Encourage the patient to engage in non-pharmacological management, such as yoga, relaxation techniques, guided imagery, and rhythmic breathing.
- Advise the patient for hot and cold applications.
- Provide the patient with prescribed medicine.
- Instruct the patient to rest between activities.
- Instruct the patient to rest frequently.
- Instruct the patient to engage in physical activities such as walking, swimming, etc.
- Instruct the patient to Ask for the use of assistive devices.
- Ask the patient to verbalize his/her feelings.
- Provide the patient with complete education about the disease and its treatment.
- Ask the patient to maintain strict aseptic technique.
- Provide the patient with education to participate in self care activities.
- Encourage the patient to join self-help groups and support groups.
1) Explain SLE (SYSTEMIC LUPUS ERYTHEMATOUS) DISEASE (SYSTEMIC LUPUS ERYTHEMATOUS) :
Full form of SLE IS SYSTEMIC LUPUS ERYTHEMATOUS. SLE is a type of autoimmune disease that affects the connective tissues of the body.
SLE is commonly seen between the ages of 15 and 40. But it can occur at any age. SLE has a multisystem affect on the body.
- Affected organs are:
- Skin (skin) ,
- Joint (joint) ,
- Kidney (kidney),
- Heart (heart),
- Lungs,
- Blood vessels,
- And Brain are also affected.
2) Explain the Etiology/cause:
- The exact causes are unknown means Idiopathic disease .
- Genetic cause,
- Ultraviolet light,
- Drugs/medication
( ex:isoniazid/procanamide/quinidine also cause the SLE. )
3)Explain the type of SLE (Systemic Lupus Write the type of erythematous):
There are a total of five types of SLE.
1)Discoid lupus erythematous:
- This type mainly affects the skin of the body.
- This is a chronic skin disorder.
- In this, raised rashes are seen on the skin. Which is commonly seen on the face, scalp or elsewhere in the body.
- In this, rashes can last for a few days or even years.
2) Subacute cutaneous lupus erythematous (Subacute cutaneous lupus erythematous):
- In this, lesions are mainly seen on the body but are only seen when exposed to sunlight (Due to ultraviolet light).
- Lesions are formed in this but no scar formation occurs.
3) Drug induced lupus erythematous:
This is mainly seen due to medications.
- Ex: isoniazid,
- Quinidine etc.
4) Neonatal lupus erythematous:
- In this, mainly neonate (0 to 28 days) systemic lupus erythematous is seen.
- When a woman has the condition of systemic lupus erythematous and that woman gives birth to a child, then there is a chance of systemic lupus erythematous in that child too, hence it is called neonatal systemic lupus erythematous.
5) Sjograne syndrome:
In Sjograne syndrome, the body’s immune system destroys the exocrine glands (that secret tears and saliva).
- Tear:lacrimal gland,
- saliva:salivary gland .
When the immune system destroys this gland, inflammation occurs. Therefore, less saliva and tears are secreted.
Due to this, the moisturisation of the oral cavity and eyes decreases. result in dry oral mucosa (xerostomia) and dry eyes (xeropthelmia).
4) Explain the sign and symptoms/clinical manifestations:
- General Discomfort,
- Feel tired,
- fever,
- weight loss,
- Arthralgia (joint pain),
- myalgia (muscle pain),
- Race (commonly seen on the face),
- chest pain,
- Alopecia (hair loss),
- skin is sensitive to sun,
- oedema/swelling legs,
- oedema around the eyes.
specific sign of systemic lupus erythematous :
1) Malar rash/Butterfly Rash :
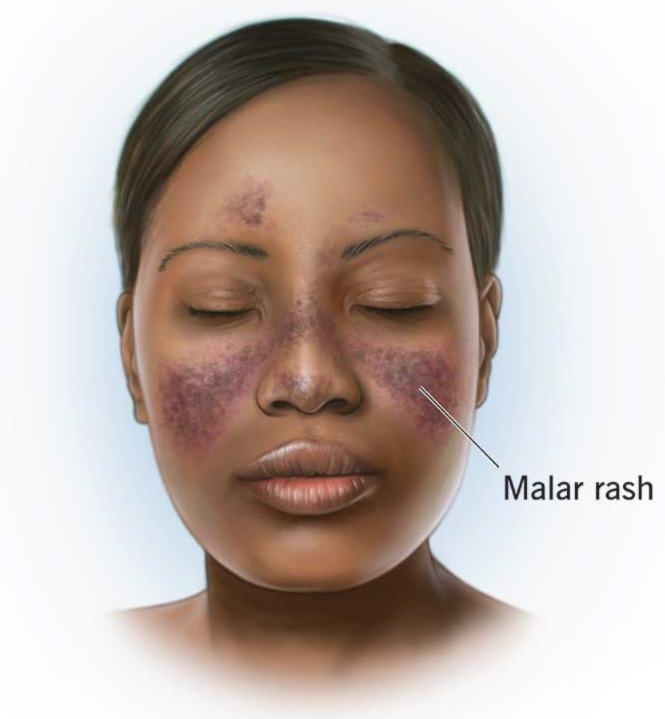
- Butterfly shape red colour rash on face.Rash is flate, raised and rashes are worse by sun exposure.
2) Reynoad ‘s phenomena :
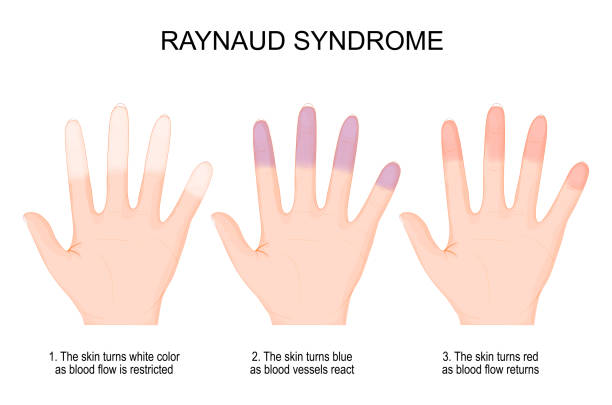
- fingers become white due to lack of blood supply Than bluish,Than due to return blood supply colour is red (Fingers become white due to lack of blood supply Than bluish,Than due to return blood supply colour is red).
3) Mouth ulcer :
- Painless sore in mouth/nose (painless sore is seen in the mouth and nose).
5) Explain the Diagnostic evaluation of SLE (Write the diagnostic evolution of SLE):
- History taking and physical examination.
- complete blood count.
- complete blood count.
- check the white blood cell count (white blood cell count) .
- check the erythrocyte sedimentation rate ( erythrocyte sedimentation rate check).
- Skin Biopsy ( skin biopsy ).
- kidney Biopsy ( kidney biopsy) .
- X Ray ( X Ray).
6) Complications of SLE :
- Pericarditis ( inflammation of the outer layer of heart. )
- heart attack,
- stroke,
- change in memory (due to lack of blood supply to the brain),
- Seizures (Abnormal impulses generated from the brain)
7) Explain Management of SLE:
Medical management:
1) Provide non-steroidal anti-inflammatory drugs (NSAIDs) to reduce the patient’s pain and inflammation.
EX: IBUPROFEN,
NEPROXEN.
2) Provide corticosteroid drugs to reduce inflammation.
3)provide antimalarial drugs For mild immunosuppressant use with other drugs.
Ex:
hydrochloroquine,
Chloroquine.
Quinacrine.
4)provide immunosuppresant drug to the patient.
Ex: cyclophosphomide( if involve kidney and brain).
5)plasma exchange therapy:
In this, plasma is exchanged.
6)Intravenous immunoglobulin.
7)In severe cases Stem Cell Transplantation.
8) Explain nursing management:
- To reduce lesions.
- To advise the patient not to expose to the sun.
- To reduce the patient’s pain level.
- If the patient is experiencing joint pain, ask him to mobilise.
- Ask the patient to exercise.
- Assess the patient’s vital signs.
- Ask the patient to take rest between exercises.
- Ask the patient to take proper skin care.
- To ensure that the patient takes proper rest to say.
1) Ankylosis Spondylitis:
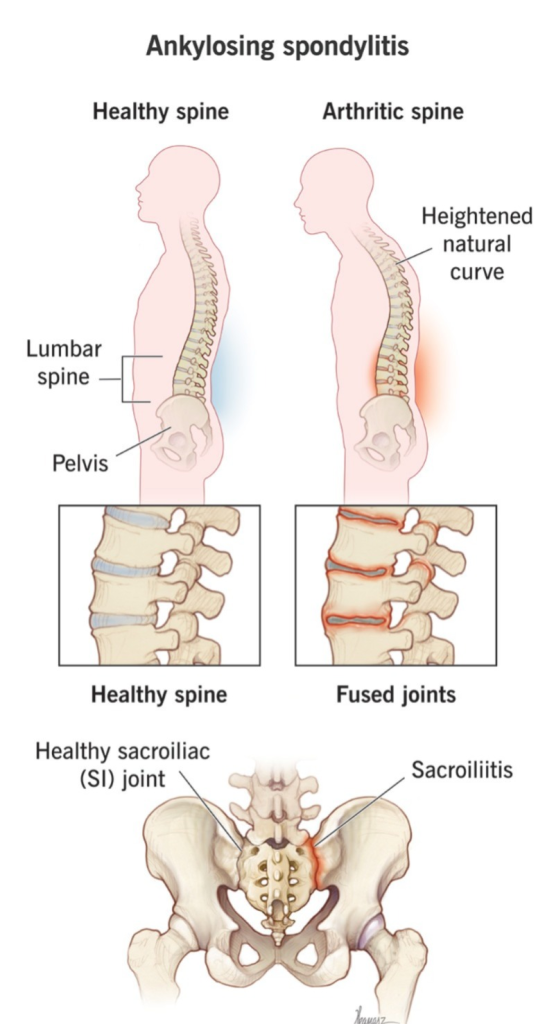
- Ankylosing spondylitis is a chronic inflammatory disorder. This disease first affects the axial skeleton in the body, as well as the spinal cord (vertebral joints and large joints). Pain and stiffness are mainly seen in the vertebral column.
- This disease is more common in males than females and is more common in adults.
2) Etiology/cause of Ankylosis spondylitis (Give cause):
- Idiopathic,
- Due to genetic cause.
- HLA-B27 antigen is the main cause of Ankylosis spondylitis.
- Unhygienic lifestyle
3) Name of the affected organ:
- eyes ,
- lungs ,
- heart ,
- kidney ,
- peripheral nervous system, and
- vertebral joints.
All of these organs are affected in ankylosing spondylitis.
4) Clinical manifestation/sign and symptoms of Ankylosis spondylitis (Write the signs and symptoms of Ankylosis spondylitis):
- Low back pain that radiates to the buttocks and hip area down the leg.
- Stiffness (stiffness).
- Stiffness increases with activity.
- Impaired mobility,
- Impaired movement,
- Systemic infections
- Fever,
- Fatigue,
- Anorexia( loss of appetite)
- Weight loss.
- Inflammation of iris/uveitis
- Hyperkyphosis (Hyperkyphosis is an excessive forward curvature of the upper spine (thoracic region), typically over 40-45 degrees).
- coming to Wickes,
- Neck pain,
- Joint pain,
- Risk of hypertension,
- Risk of heart disease,
- Bowel dysfunction,
- Constipation.
5) Diagnostic Evaluation of Ankylosis Spondylitis (Ankylosis Spondylitis) Diagnostic Evaluation of):
- X Ray ,
- MRI ,
- Blood test ,
- Erythrocyte sedimentation rate is be increase .
- white blood cell count is increased.
- Assess complete blood count
- Genetic test
- assess HLA-B27
6) Management of Ankylosis Spondylitis:
Medical management:
- provide NSAID (Non steroidal Antiinflammatory drug) drug.
- Ex: ibuprofen,
- Provide corticosteroids to the patient,
- Provide physiotherapy to the patient for improving the mobility of patients.
- provide DMARD ( disease modifying anti-rheumatic drugs)
- Ex: sulfasalasine,
- Methotrexate.
Surgical management of patients with Ankylosis spondylitis :
- repair damage joint.
- laminectomy.
Explain the Nursing Management of patients with Ankylosis spondylitis (Nursing Management):
- Provide education to the patient to maintain good spinal posture.
- Ask the patient to maintain a comfortable position.
- Ask the patient to exercise.
- Ask the patient to rest between exercises.
- Ask the patient to do range of motion exercises.
- Tell the patient to stop smoking.
GVHD IS GRAFT VERSUS HOST DISEASE :
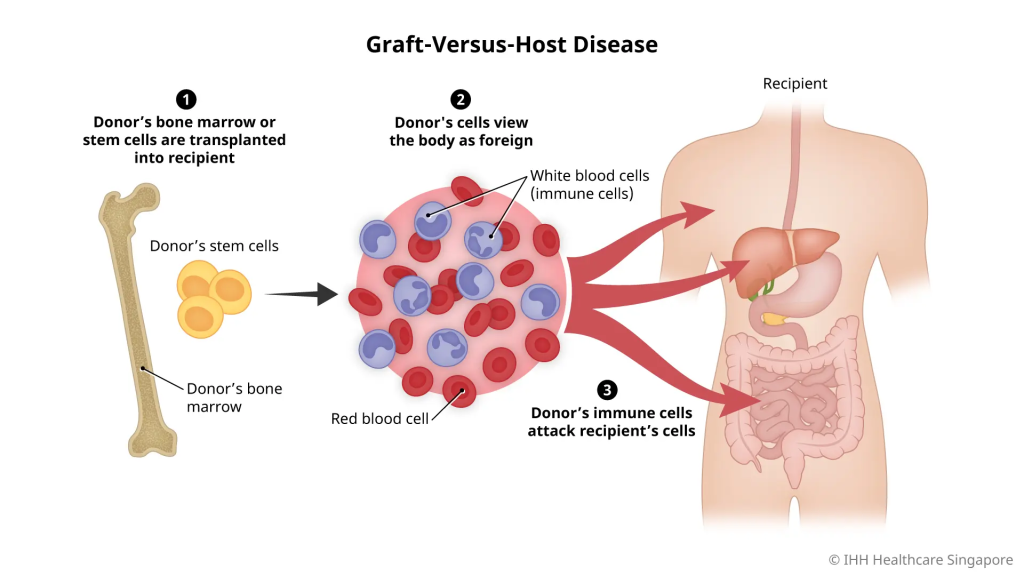
GVHD (GRAFT VERSUS HOST DISEASE) – GRAFT VERSUS HOST DISEASE

Definition:
- GVHD stands for Graft Versus Host Disease. This is a severe condition in which the live blood cells of the transplanted donor graft, especially T-lymphocytes, identify the recipient’s body, i.e. the host body, as foreign and initiate an immune response against it. As a result, the host’s tissue is damaged.
Causes:
- This disease mainly occurs after Bone Marrow Transplantation and Stem Cell Transplantation.
- When the donor’s immunocompetent T-cells (immunocompetent T-cells) This disease occurs when the donor T-cells recognize the host’s antigen-presenting cells and consider them foreign.
Pathophysiology:
Recognition Phase: The donor T-cells recognize the host’s antigen as foreign.
Activation Phase: Donor T-cells become activated and secrete cytokines.
Effector Phase: These cytokines attack the host’s tissues, especially the skin, liver, and gastrointestinal tract.
Types:
Acute GVHD (Acute Graft Versus Host Disease):
- Occurs within 100 days after transplant.
- Mainly symptoms like skin rash, jaundice, diarrhea are seen.
Chronic GVHD (Chronic Graft GRAFT VERSUS HOST DISEASE:
- Occurs 100 days after transplant.
- Caused by long-term immunological and fibrotic changes.
Sign and symptoms/clinical manifestation of GRAFT VERSUS HOST DISEASE:
In the skin: Erythematous rash, itching, peeling.
In the liver: Jaundice, hepatomegaly, increased bilirubin.
In the gastrointestinal tract: Diarrhea, abdominal pain Pain, nausea
Other Symptoms: weight loss, fatigue, infection susceptibility
If symptoms are limited to the gastrointestinal tract and skin, the prognosis is good, but if multisystem involvement is present, the prognosis is not very good.
Management Of GRAFT VERSUS HOST DISEASE :
Treatment :
- Immunosuppressive Therapy: corticosteroids such as prednisolone, methylprednisolone.
- Calcineurin Inhibitors: Cyclosporine, Tacrolimus.
- Monoclonal Antibodies: Anti-thymocyte globulin.
- Supportive Therapy: Infection control (Infection control), Nutritional support, Hydration.
- Provide corticosteroid medicine to the patient.
- Provide immunosuppressant agent (methotrexate, Cyclosporine) to the patient.
- Proper assessment when blood transfusion is required.
- Assess the patient for any adverse reactions.
- Assess the patient for skin redness, erythema, swelling.
- Provide immunosuppressive therapy to the patient.
- If the patient has any other signs and symptoms, inform the doctor immediately.
Prevention (Prevention):
- Selecting a proper HLA matching donor.
- Using T-cell depletion techniques.
- Prophylactic immunosuppression before and after transplant.
- GVHD is when the donor’s immune cells react against the host’s tissues and attack the host’s organs such as the skin, liver, and intestines. This can be a serious and sometimes life-threatening condition. Timely identification and proper immunosuppressive treatment can save the patient’s life.
