ENGLISH-MSN-1-UNIT-11-RENAL AND UROLOGICAL DISORSER-DEEPALI-PART-2
1)Define/explain the Acute glomerulonephritis. (Define acute glomerulonephritis).
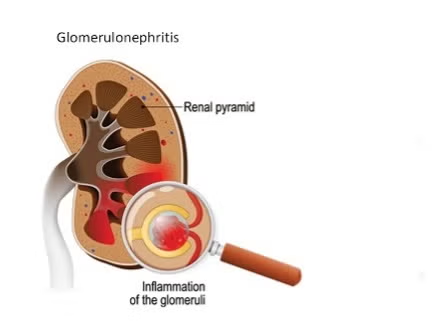
- In acute glomerulonephritis, the glomerular capillaries in the kidney The inflammation is called glomerulonephritis.
- Acute glomerulonephritis is mainly caused by streptococcal bacteria.
- The most common symptoms of acute glomerulonephritis include swelling, increased blood pressure, and changes in urine output.
Glomeruli :=
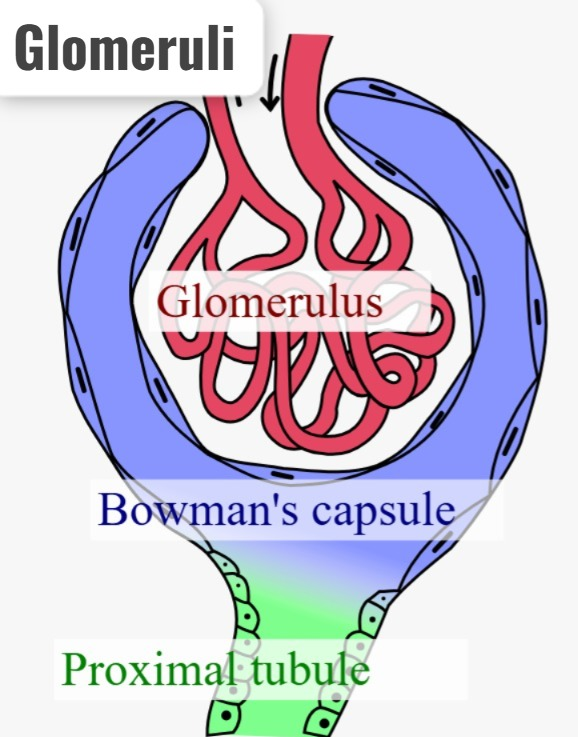
- Glomerulae are tiny ball-shaped structures located in the kidneys that play an important role in the filtration of blood and the formation of urine. Responsible for doing. A kidney has thousands of filtration units, which are surrounded by a membrane and contain capillaries. Their main function is to filter waste products, excess water and electrolytes.}
- { Inflammation of the glomerular and its capillaries its called as a glomerulonephritis.}
2)Explain the Etiology/ cause of the glomerulonephritis .
- Due to streptococcal infection.
- Due to heavy doses of nonsteroidal anti-inflammatory drugs.
- Due to bacterial, viral and parasitic infections.
3) Explain the Clinical manifestation of the patient with the acute glomerulonephritis. (Symptoms and signs of acute glomerulonephritis.)
- => Hematuria (blood in urine).
- => In ED.
- => Proteinuria (increased protein level in urine).
- => Fever,
- =>Feeling cold,
- => Weakness,
- => Loss of appetite,
- => Tiredness,
- =>Nausea,
- => vomiting,
- =>Generalized facial,
- => Periorbital swelling,
- => headache.
4)Explain the diagnostic evaluation of the patient with the acute glomerulonephritis .(Write the diagnostic evaluation of the patient with acute glomerulonephritis.)
- => history taking and physical examination.
- => Urine Analysis.
- =>24 hour urine for protein and creatinine clearance outline the degree of renal function.
- =>Assess the blood urea nitrogen level.
- =>Needle biopsy of the kidney.
- => Antistreptolycin o titers.
- => Erythrocyte sedimentation rate test.
- => Complete blood count.
- => KUB abdominal x rays.
- => Kidney scan.
5) Explain the management of the patient with the acute glomerulonephritis.
Medical management
- Provide antihypertensive medicine to the patient To do.
- Provide antibiotic medicine to the patient.
- Provide corticosteroid medicine to the patient.
- Provide diuretic medicine to the patient.
- Provide corticosteroid medicine to the patient.
- Provide immunosuppressive agent to the patient.
6)Explain the Nursing management of patients with the Acute glomerulonephritis (Explain the Nursing Management of Patients with Acute Glomerulonephritis.)
- Advise the patient to take a salt and fluid restriction diet.
- Ask the patient to avoid excessive fluid intake.
- Monitor the patient’s vital signs.
- Monitor the patient’s intake output chart.
- Advise the patient to take proper rest.
- Monitor the patient’s blood urea nitrogen, creatinine and blood pressure.
- Properly monitor the patient’s fluid balance.
- Advise the patient to take proper rest. Advise the patient to take antihypertensive and diuretic medicines properly.
- Advise the patient to avoid a protein-rich diet.
- Advise the patient to take adequate amounts of carbohydrates.
- Advise the patient to restrict potassium and sodium intake.
- Carefully monitor the patient’s fluid balance.
- Monitor the patient for any signs and symptoms of heart failure.
- Treat the patient immediately if he has any type of infection.
- Monitor the patient’s daily weight.
- Advise the patient to have regular follow-up
1)Explain/Define chronic glomerulonephritis. (Define chronic glomerulonephritis.)
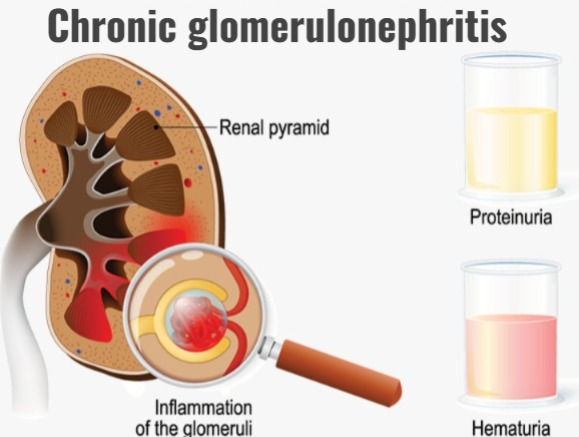
- Chronic glomerulonephritis is a condition in which there is long-term inflammation of the glomeruli (kidney filtering unit). This causes damage to the kidneys and the function of the kidneys becomes impaired over time.
- Chronic glomerulonephritis occurs due to repeated episodes of acute glomerulitis.
- In chronic glomerulonephritis, the size of the kidneys is reduced and due to this, end-stage renal disease (ESRD) occurs.
2) Explain the Etiology of the patient with the cronic glomerulonephritis. ( Explain the reason for chronic glomerulonephritis.)
- Due to immune system disorders.
- Due to autoimmune disorders.
- Due to infection.
- Due to chronic viral infections.
- Due to hypertension.
- Due to diabetes.
- Due to genetic factors.
- Due to exposure to toxins.
- Due to streptococcal infection.
- Due to bacterial, viral and parasitic infections.
3) Explain the Clinical manifestation of the patient with the chronic glomerulonephritis.
- Proteinuria.
- Hematuria.
- Hypertension.
- In AD.
- Fatigue.
- Weakness.
- Decreased urine output.
- Electrolyte imbalance.
- Renal insufficiency.
- Nosebleeds.
- Weight and strength loss.
- Irritability.
- Nocturia.
- Headache.
- Dizziness.
- Digestive problems.
- Peripheral edema.
- Anemia.
- Cardiomegaly.
- Neck veins become distended.
- Congestive heart failure.
- Crackling sounds are heard from the lungs.
- Tendon reflexes become diminished.
- Neurosensory changes.
4) Explain the diagnostic evaluation of the chronic glomerulonephritis.
- History taking and physical examination.
- Creatinine test.
- Blood urea nitrogen test (BUN).
- Electrolyte test.
- Complete blood count.
- Urinalysis.
- Ultrasound.
- CT scan.
- MRI.
- Kidney biopsy.
- Autoimmune infection test.
- Renal function test.
- 24 hour urine test.
- Blood pressure monitoring.
5)Explain the management of the patient with the chronic glomerulonephritis. (Write the management of the patient with chronic glomerulonephritis.)
- Give the patient antihypertensive medication.
- Provide the patient with immunosuppressive therapy.
- Give the patient corticosteroid medicine.
- Give the patient diuretic medicine.
- Monitor the patient’s daily weight.
- Advise the patient to avoid protein.
- Advise the patient to have adequate calorie intake.
- Start dialysis to prevent any further complications.
- Provide antibiotic medicine to the patient.
- Provide anti-inflammatory medicine to the patient.
- Provide anticoagulant agent to the patient.
- Provide erythropoietin injection to the patient.
- Monitor the patient’s condition regularly.
- Advise the patient to exercise regularly.
- Advise the patient to have a balanced diet, regular exercise, and avoid smoking.
6) Explain the Nursing management of patients with the chronic glomerulonephritis.
- Provide comprehensive care and support to the patient.
- Monitor the patient’s vital signs regularly.
- Monitor the patient’s fluid intake output.
- Monitor the patient’s nutritional status properly.
- Advise the patient to avoid sodium-rich foods.
- Advise the patient to consume proper calories.
- Provide oral care to the patient.
- Advise the patient to take proper bed rest.
- Change the patient’s position every two hours.
- Administer medication properly to the patient.
- Advise the patient to take medication properly as per the schedule.
- Provide the patient with complete information about his disease condition, its causes, and its symptoms.
- Manage the patient’s pain properly.
- Provide analgesic medicine to reduce the patient’s pain.
- Advise the patient to maintain proper aseptic technique to prevent infection.
- Monitor the patient’s blood urea nitrogen (BUN) regularly.
- Monitor the patient’s electrolyte levels properly.
- Provide proper psychological support to the patient.
- Advise the patient to do proper physical exercise.
- Advise the patient to maintain proper good hygienic technique.
- Administer immunosuppressive medicine to the patient.
- Provide the patient with proper compatible devices.
- Provide proper psychological support to the patient.
- Provide a calm and comfortable environment for the patient.
- Advise the patient to take proper follow-up.
1)Define/Explain urolithiasis. (Define urolithiasis.)
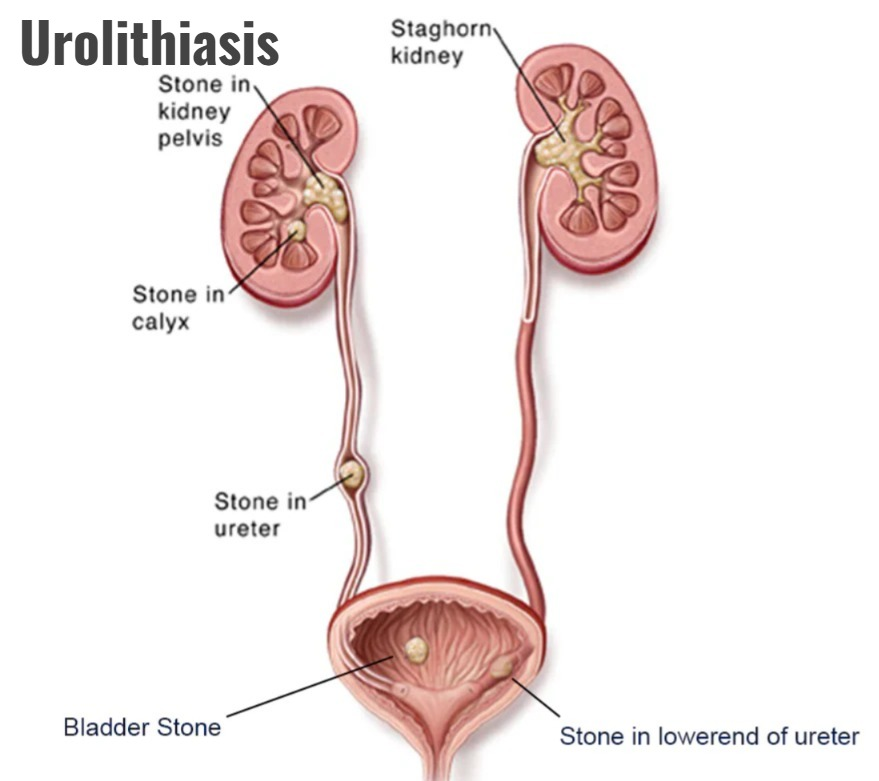
- Urolithiasis is the formation of urinary calculi (stones) and they are mainly located anywhere in the urinary system. These stones are mainly formed due to an increase in the concentration of substances present in the urine, such as calcium and uric acid. Stone formation in the urinary tract occurs when urinary concentrations of substances such as calcium oxalate, calcium phosphate, and uric acid increase.
- If stone formation occurs in the kidneys, it is called (nephrolithiasis)
- If stone formation occurs in the ureters, it is called (ureterolithiasis), and if stone formation occurs in the bladder, it is called (cystolithiasis). Urolithiasis is a condition in which minute deposits of different sizes, called sand and gravel, are formed. Large stones such as orange stones are formed.
- Urolithiasis has a nucleus and a concentric layer of urinary salts is deposited around it.
2) Explain the Etiology/ cause of the urolithiasis.
- Due to dehydration.
- Due to hyperparathyroidism.
- Due to obstruction of urine flow.
- Due to infection in the urinary tract.
- Due to renal tubular acidosis.
- Cancer Due to.
- Granulomatous disease.
- Intake of excessive amounts of vitamin D.
- Intake of excessive amounts of milk.
- Due to a genetic defect in cysteine metabolism.
- Use of certain types of medicine in excessive amounts Because of.
- Ex:=
- ~diuretic,
- ~Some chemotherapy medicine for cancer.
- ~Some medication used to treat HIV.
- Due to chronic illness.
- Due to cystic fibrosis.
- Due to renal tubular acidosis.
- Due to inflammatory bowel disease.
- Due to dietary factors.
- Due to salt and animal protein diet.
- Due to excessive intake of certain minerals such as calcium oxalate, uric acid etc.
- Due to metabolic factors.
- Due to genetic conditions.
- Due to certain medical conditions.
- Due to anatomical abnormalities.
- Due to urinary stasis.
- Due to obesity.
- Due to inadequate fluid intake.
- Due to a family history of kidney stones.
- Due to a diet high in protein, high in sodium, and high in sugar.
- Due to neurogenic bladder.
- Pregnancy Due to related changes.
- Due to high amount of calcium in urine.
- Due to obesity, diabetes, and high blood pressure.
- Due to inflammatory bowel disease.
- Due to prolonged immobilization.
3)Explain the sign and symptoms/clinical manifestation of the urolithiasis.
- Renal colic (sudden and severe pain at abdomen which should be radiating towards the groin area).
- Camping pain in the lower back.
- Hemangiuria.
- Urinary frequency and urgency.
- Dysuria (pain or discomfort during urination).
- Cloudy and foul smelling urine.
- Fever.
- Chills.
- Painful urination.
- Burning sensation during urination.
- Oliguria and Anuria.
- Pyuria (pus in urine).
- Post renal azotemia.
- Abdominal distension.
- Nausea and vomiting.
- Incontinence of urine emptying.
4)Explain the diagnostic evaluation of the patient with the urolithiasis.
- History tacking and physical examination.
- Blood test.
- Urine test.
- Analysis of passed stones.
- Imaging test.
- X rays.
- CT scan.
- MRI.
- Ultrasonography examination.
- Retrograde pyelography.
- 24 hour urine test.
- Blood chemistry study.
5)Explain the medical management of the patient with the urolithiasis.
- Provide analgesic medicine to relieve the patient’s pain.
- Provide hot bath to the patient.
- Advise the patient to take adequate amounts of fluid.
- Provide nutritional therapy to the patient.
- If there is calcium stone, provide calcipotriene to the patient to increase calcium absorption.
- If there is oxalate stone, advise the patient to avoid chocolate, tea, spinach.
- Advise the patient to restrict protein-rich diet.
- Provide intravenous fluids to maintain the patient’s hydration status.
- Provide antiemetic medicine if the patient is vomiting.
- Provide opioid analgesic medicine if the patient is experiencing severe pain.
- Provide antispasmodic agent if the patient is experiencing colic pain.
- Provide the patient with anti-inflammatory drugs.
- Provide the patient with calcium channel blocker medicine.
- Provide the patient with antacid medicine.
1) calcium stones:=
- To prevent calcium formation, provide the patient with a thiazide diuretic and a phosphate-containing preparation.
- To prevent calcium stones, provide cellulose sodium phosphate.
2) Uric acid stone :=
- To prevent the formation of uric acid stones, provide allopurinol medicine, which is used to reduce the level of uric acid in the blood.
3)struvite stone : =
- To prevent the formation of struvite stones, provide the patient with antibiotic medicine, which keeps the urine free of bacteria and prevents infection. Can be.
4) Cystine stone:=
- Treating stones is difficult, so some medications are provided to alkalize the urine, which can prevent stone formation.
6) Explain the surgical management of patients with urolithiasis. (Write the surgical management of a patient with urolithiasis.)
1) Ureteroscopy
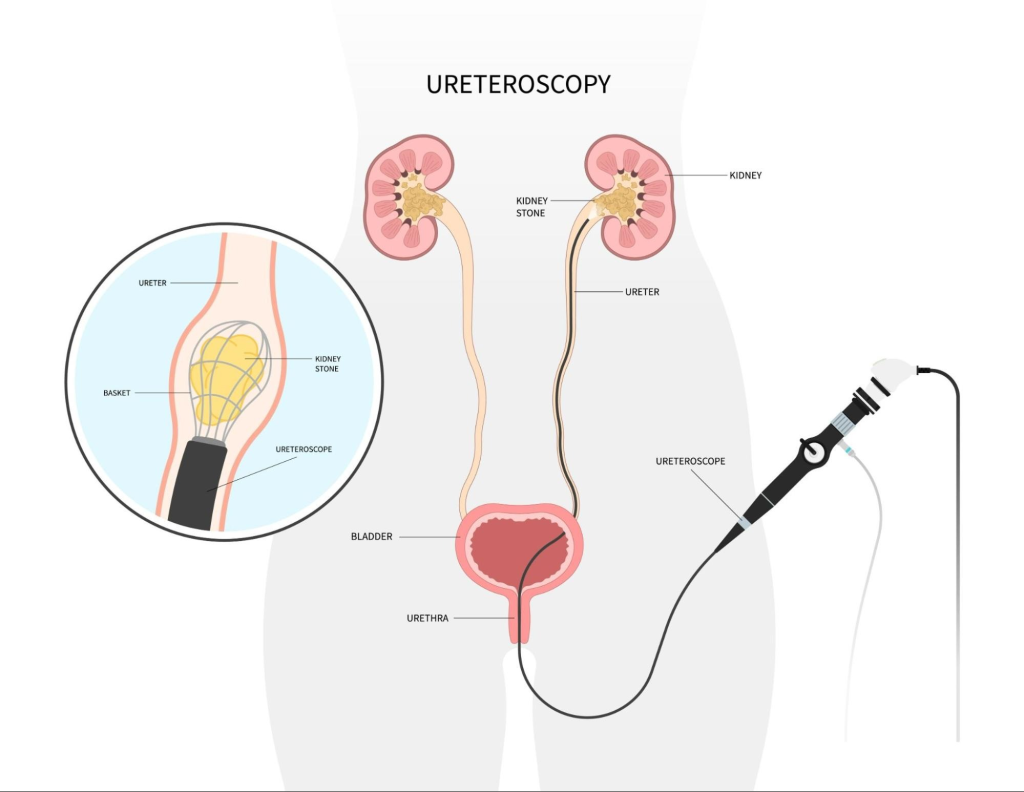
- Ureteroscopy is mainly used when there is stone formation in the lower urinary tract.
- Ureteroscopymainly involves visualizing the stone first and then destroying it.
2) Extracorporeal shock wave lithotripsy ( Extracorporeal Shockwave Lithotripsy)
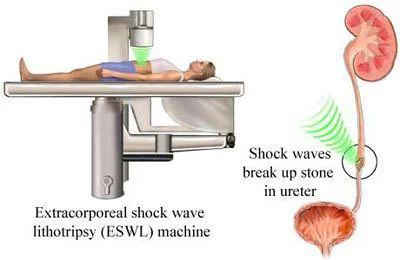
- Extracorporeal shockwave lithotripsy is a procedure that is mainly performed on half and inch It is used to remove smaller stones that are locked near the calycx of the kidney.
- In this procedure, ultrasonic waves or shock waves are used to break the stone, after which the stone is removed from the body through urine.
3) Percutaneous stone dissolution / chemolysis
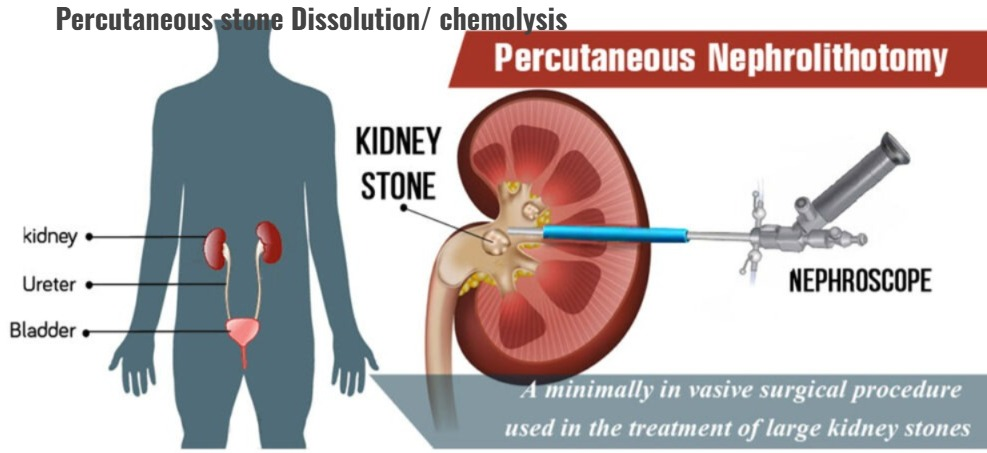
- Percutaneous stone dissolution involves infusion of an alkalizing agent and an acidifying agent to dissolve the stone.
4) Percutaneous Nephrolithotomy
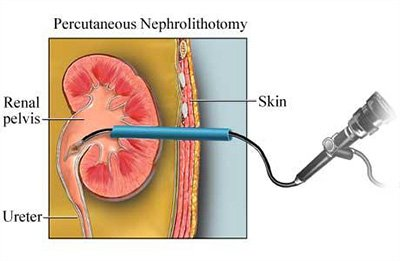
- Percutaneous nephrolithotomy is mainly used to remove large stones near the kidney.
- In this procedure, an endoscope is inserted to remove the stone.
5) Cystolithotomy
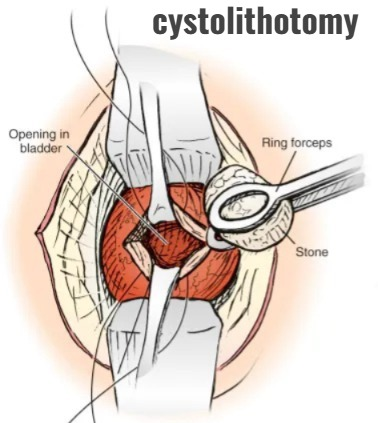
- Cystolithotomy is mainly used to remove bladder calculi through a suprapubic incision, but this procedure is used only when the stone is not crushed and can be removed transurethrally. is.
6) partial Total Nephrecromy (partial total nephrectomy)
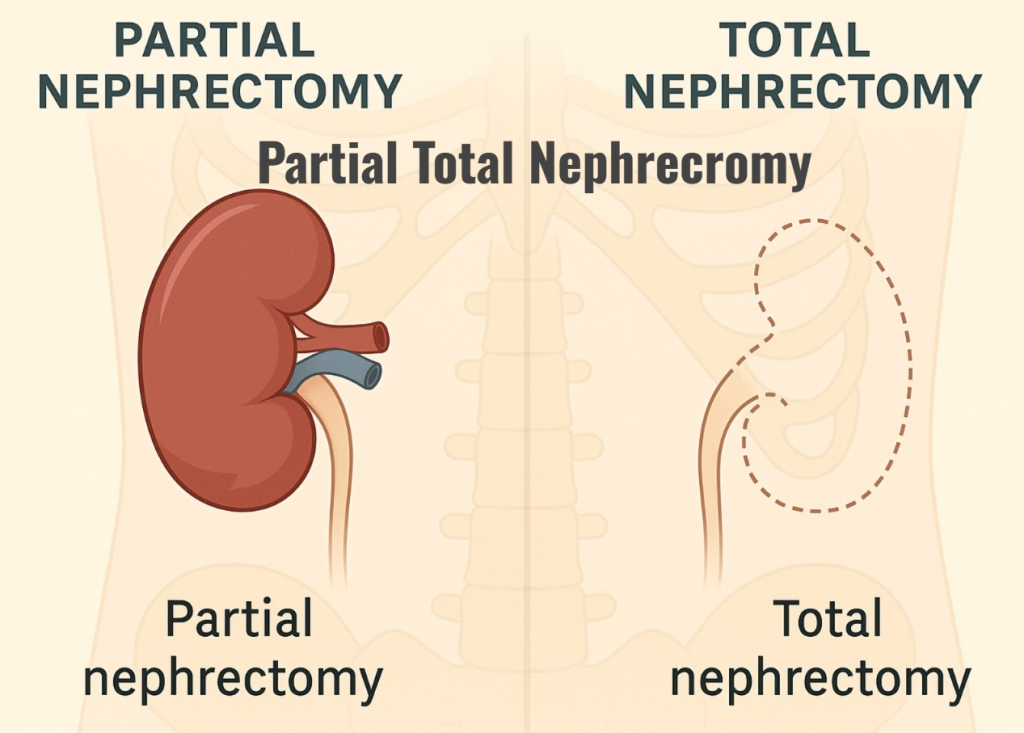
- Partial total nephrectomy is mainly performed when the kidney is damaged and there is an overwhelming renal infection.
7) Explain the Nursing management of patients with the renal calculi.
Nursing assessment
Take a complete health history of the patient and perform a physical examination.
Find out if the patient has any family history of tonsillitis.
Assess the patient for dehydration.
Assess the patient for urinary tract infection.
Assess the patient’s pain level.
Assess the patient for any other signs such as nausea, vomiting, abdominal distention, diarrhea.
Assess the patient for signs and symptoms of urinary tract infection such as urinary urgency and frequency, pyuria, fever, chills.
Assess the patient for conditions such as oliguria, anuria.
Nursing interventions
1) controlling pain
- => Assessing the patient’s pain level.
- => Use opioid analgesics to relieve the patient’s pain.
- => Provide the patient with nonsteroidal anti-inflammatory medicine.
- => Advise the patient to apply moist heat to relieve pain.
- => Provide the patient with allopurinol medicine to decrease uric acid production.
2) Maintaining urinary elimination.
- => Monitor the patient for any signs and symptoms of urinary obstruction.
- => Provide the patient with oral and intravenous fluids.
- => Monitor the patient’s intake output chart.
3) Control infection:=
- => Provide the patient with oral antibiotic medicine.
- => Monitor the patient’s vital signs.
4)Prevention of Recurrent stone formation:=
- => Advise the patient to avoid excess calcium and phosphorus in their access account.
- => Advise the patient to follow a low sodium diet.
- => Provide the patient with a low protein diet.
- => Advise the patient to have urine pH testing.
- => Assess the patient for any signs and symptoms of urinary tract infection.
- => Advise the patient to avoid sugar and animal protein diet.
- => Provide adequate amount of fluids to the patient.
5) Improving knowledge:=
- => Advise the patient to consume adequate amounts of fluid.
- => Advise the patient to avoid high purine rich foods.
- => Advise the patient to avoid high oxalate rich foods.
- => Advise the patient to limit intake of milk and dairy products.
- => Advise the patient to follow a modified diet. Advise patients with calcium, oxalate, and uric acid stone formation to follow a slow-release diet.
1)Define/ Explain the renal calculi.
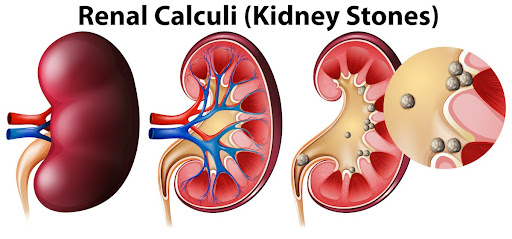
- Renal calculi are also called kidney stones. Kidney stones are hard deposits of salt and minerals that form mainly in the kidneys.
- These stones mainly vary in size.
- Renal stones, calculi, and lithiasis are the most common diseases of the urinary tract.
- These are mainly seen more in men than women.
2) Explain the Etiology/ cause of the renal calculi.
- Due to dehydration.
- Due to dietary factors.
- Due to excessive amounts of calcium, oxalate and uric acid.
- Excessive intake of sodium and animal protein Due to intake in large amounts.
- Due to genetic abnormalities.
- Due to metabolic disorders.
- Due to urinary tract infections.
- Due to certain types of medications.
- Due to excessive amounts of diuretics and antacids.
- Due to vitamin A deficiency.
- Due to urinary tract infection.
- Due to hyperparathyroidism.
- Low urine volume.
- Due to low fluid intake.
- Due to high protein intake.
- Due to high sodium intake and low calcium intake.
3)Explain the type of renal calculus.
1) Primary stone (Primary stone)
- => Primary stones are mainly found in a healthy urinary tract without any inflammation.
2) Secondary stone (Secondary stone)
- => Secondary stones are mainly found due to inflammation in the urinary tract.
4)Explain the Clinical manifestation/ sign and symptoms of the Urinary calculi .
- Severe pain.
- Hemanchuria.
- Increase in urinary frequency and urgency.
- Dysuria (pain and burning sensation during urination).
- Nausea.
- Vomiting.
- Cloamy and foul-smelling urine.
- Hydronephrosis.
- Pyuria.
- Tenderness occur.
- Muscles become stiff.
- Abdominal distension occurs.
- Peristalsis moment becomes diminished.
5)Explain the Diagnostic evaluation of the renal calculus. (Write the diagnostic evaluation of the renal calculus.)
- history taking and physical examination.
- Blood examination.
- Urine analysis.
- Radiography
- Straight X-ray
- Excretory urogram
- Ultrasonography.
- Computed tomography.
- Renal scan.
- Cytoscopy.
- Stone analysis.
- Blood urea nitrogen test.
- Intravenous Pyelogram.
- Urography.
5) Explain the medical management of the renal calculi.
- Provide nonsteroidal anti-inflammatory drugs (NSAIDs) and analgesic medicines if the patient is in pain.
- Advise the patient to take adequate amounts of fluid to maintain hydration status.
- Advise the patient to take prescribed medications in adequate amounts.
- Provide thiazide diuretic medications to increase the patient’s urine flow.
- Advise the patient to make dietary modifications.
- Advise the patient to avoid oxalate-rich foods and purine-rich foods.
- Advise the patient to make lifestyle modifications.
- If the patient has any other metabolic disorders, treat them immediately.
- Advise the patient to avoid things like milk, cheese.
6) Explain the Nursing management of patients with the renal calculi.
- Properly assess the patient.
- Properly monitor the patient’s vital signs.
- Maintain the patient’s intake output chart.
- Assess the patient’s pain level.
- Provide analgesic medicine if the patient is in pain.
- Provide the patient with mind diversional therapy.
- Provide the patient with a comfortable position.
- Advise the patient to take adequate amounts of fluid.
- Monitor the patient’s fluid balance.
- Monitor the patient’s intake output chart.
- Advise the patient to make dietary modifications.
- Apply hot compresses to the patient’s body part where there is discomfort.
- Provide emotional support and reassurance to the patient.
- Provide proper medicine to the patient.
- Collaborate with other health care personnel to provide effective care to the patient.
- Advise the patient to make lifestyle modifications.
- Advise the patient to follow up properly.
- Properly document the care provided to the patient.
- Properly provide reassurance to the patient.
- Clear all doubts of the patient and his family members To do.
- Advise the patient to follow up regularly.
1)Explain/ define trauma of genitourinary trauma (renal, bladder, urethra , and ureters.)
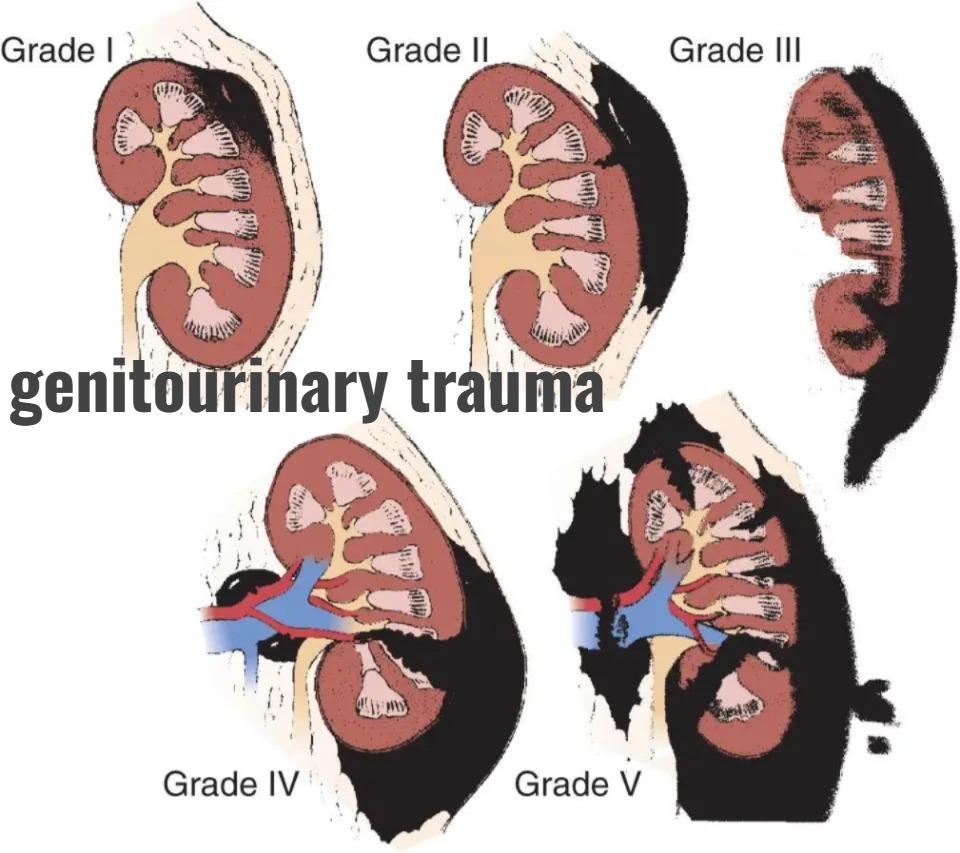
- Trauma occurs mainly in the urinary system. Injuries to the urinary system affect the kidneys, bladder, ureters, and urethra.
- Blunt and penetrating injuries can also cause trauma to the kidneys, ureters, urethra, and bladder. है.
2) Explain the Etiology/ cause of the genitourinary trauma.
- Due to road traffic accident.
- Due to sports injury.
- Due to blunt force.
- Due to pelvic fracture.
- Due to urethral injury.
- Due to motor vehicle accident.
- Due to sports injury.
- Due to fall down.
- Due to certain medical procedures.
- Assault.
- Due to occupational injury.
- Due to contusion.
- Due to intraperitoneal rupture.
- Due to extraperitoneal rupture.
- Due to certain surgical procedures.
3) Explain the Clinical manifestation/ sign and symptoms of the patient with the genitourinary system trauma.
- Hemanturia,
- Abdominal pain,
- Lower abdominal pain,
- Difficulty urinating.
- Oliguria (secretion of less amount of urine).
- Anuria (absence of urine output).
- Swelling.
- Tenderness.
- Retroperitoneal bleeding.
- Difficulty urinating.
- Perineal pain.
- Ecchymosis.
- Shock symptoms.
- Hypotension.
- Tachycardia.
- Tachypnea.
- Pale skin.
- Altered level of consciousness.
- nausea.
- vomiting.
- pyelonephritis.
4) Explain the diagnostic evaluation of the patient with the genitourinary system trauma.
- history taking and physical examination.
- complete hemograme to check the hemoglobin level.
- ultrasound.
- CT scan.
- laboratory tests.
- urine analysis.
- renal arteriography.
- aspartate aminotransferase.
- intravenous pyelography.
- kidney, ureters, bladder ( KUB ) test.
- cytogram.
5) Explain the management of the genitourinary system trauma.
- Keep the patient’s airway, breathing and circulation properly patent.
- Provide analgesic medicine if the patient is in pain.
- Provide comfort measures to the patient.
- Conduct investigations like ultrasound, X-ray CT scan etc. to assess whether the patient has any further injury.
- Monitor the patient’s vital signs properly.
- Administer blood transfusion to the patient.
- Catheterize the patient properly.
- Provide broad spectrum antibiotic medicine if the patient has an infection.
- Close observation and monitoring of the patient properly.
- If the patient is in shock, administer intravenous fluid.
- Monitor the patient’s intake-output chart properly.
- Advise the patient to take proper bed rest.
- Advise the patient to take regular follow-up.
6) Explain the Nursing management of patients with the genitourinary system trauma.
- Properly assess the patient.
- Monitor the patient’s vital signs properly.
- Properly assess the patient’s pain level.
- Properly evaluate the patient’s urinary output.
- Assess the patient for any signs and symptoms of bleeding infection.
- If the patient is in pain, provide analgesic medicine.
- Monitor the patient’s urinary output.
- Catheterize the patient properly.
- Monitor the patient’s fluid and electrolytes properly.
- Provide intravenous fluids to the patient.
- Provide the patient with a comfortable position.
- Provide comfort devices to relieve the patient’s pain.
- Assess the patient for any further injuries.
- Advise the patient to maintain aseptic technique to prevent infection.
- Provide the patient with proper emotional support.
- Advise the patient to eat a nutritious diet.
- Advise the patient to take adequate amounts of fluid.
- If the patient is in pain, provide a comfortable position.
- Advise the patient to take plenty of fluid.
- Provide reassurance to the patient and his family members.
1)Define/Explain ureteral stricture.
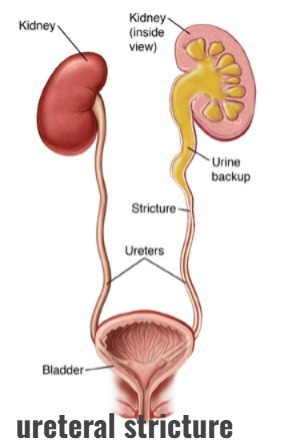
- In urethral stricture, there is a narrowing of the urethral lumen (the structure that helps carry urine from the kidney to the bladder), due to which functional obstruction is seen.
- The most common cause of urethral stricture is ureteropelvic junction.
2) Explain the etiology/cause of the ureteral stricture. (Give reasons for urethral stricture.)
- Due to trauma.
- Due to infection.
- Due to inflammation.
- Due to medical procedures.
- Due to congenital factors.
- Idiopathic.
- Due to scar tissue formation.
- Due to congenital defect.
- Due to other treatment of urogenic conditions.
- Due to stone and tumor formation.
- Due to pelvic radiation therapy.
- Due to any gynecological procedure.
- Due to any external traumatic injury.
3)Explain the Classification of ureteral stricture. (Explain the classification of urethral stricture.)
There are six classifications of urethral stricture.
- 1) intrinsic,
- 2) extrinsic,
- 3) benign,
- 4) malignant ( malignant),
- 5) Iatrogenic ( iatrogenic),
- 6) Noniatrogenic ( noniatrogenic).
1) intrinsic ( इंत्रिन्त्रिन्सिक ),
- Intrinsic urethral stricture is seen due to any problem in the urethra itself.
2) Extrinsic (Extrinsic),
- Extrinsic urethral stricture is a stricture of the ureters that occurs due to any outside factor.
3) benign,
- Benign urethral strictures are caused by non-cancerous causes such as inflammation, infection, scarring, or congenital anomalies.
4) malignant,
- Malignant tissue is seen due to cancerous growth.
5) Iatrogenic,
- Iatrogenic strictures are seen unintentionally. Occurs due to any medical procedure or intervention.
6) Noniatrogenic.
- Noniatrogenic urethral strictures occur without the direct involvement of any medical procedure.
4) Explain the Clinical manifestation/ sign and symptoms of the ureteral stricture.
- Urinary flow decrease.
- Urinary urgency.
- Unilateral pain.
- Urinary tract infection.
- Hematuria ( blood in urine ) .
- Hydronephrosis.
- Swelling in the kidneys.
- Impaired kidney function.
- Blood in semen.
- Passing bloody and dark urine.
- Decreased urine output.
- Difficulty urinating.
- Discharge from the urethra.
- Difficulty urinating.
- Bladder enlargement.
- Urinary incontinence.
- Painful urination.
- Pain in the lower abdomen.
- Pelvic pain.
- Slow urine stream.
- Lymph nodes enlarge.
- Enlarged and tender prostate gland.
- Slow urine stream.
5) Explain the Diagnostic evaluation of the ureteral stricture.
- history taking and physical examination.
- ct scan.
- MRI.
- Direct visualization.
- Intravenous pyelogram.
- Renal ultrasound.
- Bladder examination.
- Urine analysis.
- Urine culture and sensitivity test.
- serum electrolyte test.
- Assess the Blood uria nitrogen level.
- Ureteroscopy.
- Renal ultrasonography.
- Retrograde pyelography.
6) Explain the medical management of the ureteral stricture.
- If the patient has a condition of infection, then provide antibiotic medicine.
- To relax the muscles of the ureters, provide alpha blocker medicine to the patient.
- If the patient is in pain, then provide nonsteroidal anti-inflammatory medicine (NSAID).
7) Explain the surgical management of patients with the ureteral stricture.
1) Ballon Dilation
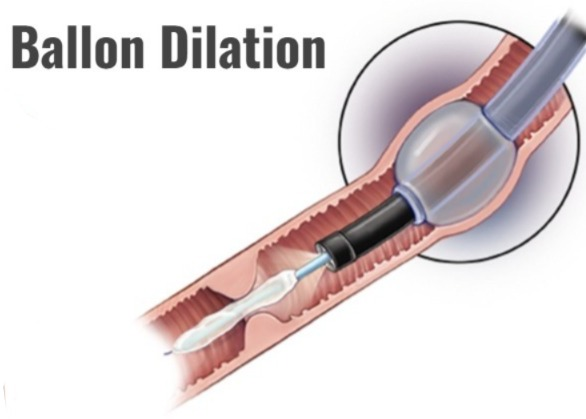
- The most common initial management of benign ureteral stricture is balloon dilation.
2) Endoureterotomy
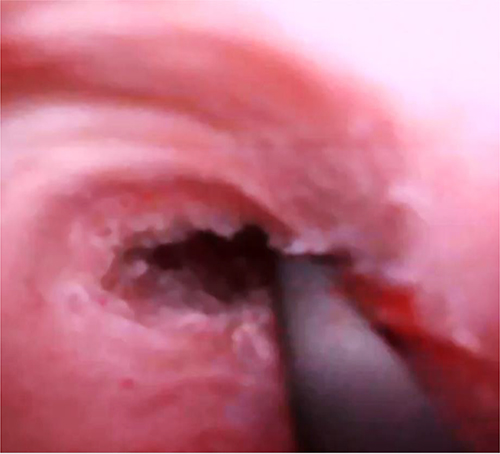
- In endoscopic surgery, the stricture in the ureters is opened.
3) Ureteral Metal stents
- Metal stents are mainly used in end-stage malignant diseases.
4) Transureterostomy
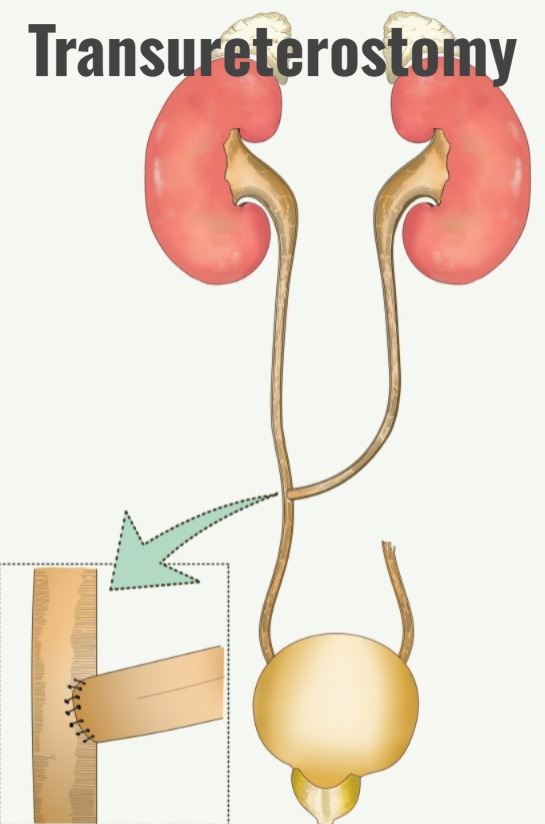
- Transureterostomy is a primary urinary reconstruction technique in which one ureter is joined to another ureter.
8) Explain the Nursing management of patients with the ureteral stricture.
- Properly assess the patient.
- Properly monitor the patient’s vital signs.
- Properly provide fluids to the patient.
- Provide analgesic medicine if the patient is in pain.
- Provide adequate fluids to maintain the patient’s hydration status.
- Provide antibiotic medicine if the patient has a urinary tract infection.
- Provide education to the patient about their disease, its causes, and its symptoms and signs.
- Patient Provide proper psychological support.
- Advise the patient to take proper follow up care.
1)explain/ Define the definition of neurogenic bladder .
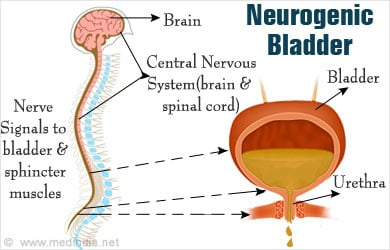
- Neurogenic bladder is a type of neurogenic dysfunction.
- Neurogenic bladder is a dysfunction of the urinary bladder, which is mainly caused by problems in the central and peripheral nervous system.
- Neurogenic bladder is mainly caused by impairment in the normal nerve path. Conditions like urinary retention, incontinence of urine, urinary tract infection, stone formation, renal failure arise due to neurogenic bladder.
2) Explain the type of neurogenic bladder.
- 1) flassid neurogenic bladder ( flassid neurogenic bladder).
- 2)spastic neurogenic bladder ( spastic neurogenic bladder.)
1) Flaccid neurogenic bladder.
- Flaccid bladder is mainly seen due to motor neuron lesion and any trauma.
- Due to the decrease in the sensation of bladder feeling, the bladder does not concentrate forcefully and due to this the bladder becomes full and the bladder becomes distended, due to which urinary incontinence is seen.
2) Spastic neurogenic bladder
- Spastic bladder is mainly characterized by uncontrolled and frequent bladder expulsion of urine.
- This is mainly seen due to brain damage and spinal cord damage.
- Due to this, urine emptying becomes incomplete. है.
3) Explain the cause/Etiology of the neurogenic bladder
- Neurogenic bladder is seen at any age.
- Alzheimer’s disease.
- Alcohol Neuropathy.
- Stroke.
- Meningomyelocele.
- Aids.
- Parkinson’s disease.
- Brain or spinal cord tumor.
- Diabetic neuropathy.
- Spina bifida.
- Multiple sclerosis.
- Nerve damage.
- Due to any diabetes or alcoholic disorder.
- Injury to the spinal cord.
- Due to new damage.
- Vitamin B12 deficiency.
4)explain the Clinical manifestation/sign and symptoms ( Explain the Clinical manifestation/sign and symptoms of neurogenic bladder)
- Excessive urine production.
- Bladder overactivity.
- Urinary incontinence.
- Frequent urination.
- Urinary retention.
- Urinary frequency and urgency Occurrence.
- Problem in expelling the entire urine from the bladder.
- The bladder becomes full and urine leaks due to this.
- Loss of bladder control.
- Loss of sensation of bladder fullness.
- Pain and burning during urination.
- Erectile dysfunction.
- Urinary tract infection.
5)explain the diagnostic evaluation (Write the diagnostic evaluation of neurogenic bladder.)
history taking and physical examination
- complete Neurological examination.
- post void residual volume.
- renal ultrasonography.
- Serum creatinine.
- cytography.
- cytoscopy.
- cytometrography.
- urodynamic testing.
6) Explain the treatment of neurogenic bladder
- Provide medications that relax the bladder.
- Urinary tract infection and Control.
- Ask the patient to take a lot of water intake, which will reduce urinary tract infections.
- Ambulate the patient frequently.
- Change the patient’s position frequently.
- Ask the patient to take calcium in small amounts.
- Change the patient’s position frequently.
7) explain specific treatment
- 1) physical-psychological therapy.
- 2) Bladder evacuation.
- 3) electrical stimulatory therapy.
explain surgery
- 1) Transurethral resection of the bladder neck.
- 2)urethral dilatation.
- 3)External sphincterotomy.
- 4)urinary diversional procedure.
- 5)implantation of artificial sphincture.
- 6)urethral stent.
8) Explain the nursing management of neurogenic bladder.
- Monitor residual urine.
- Monitor for signs and symptoms of any renal calculi.
- Assess urinary stasis.
- Check for signs and symptoms of any urinary tract infection, including urine color, order, volume, frequency, urgency.
- Check the patient’s intake output.
- Administer vitamin C to the patient to produce acidic urine and prevent bacterial growth.
- Assess the patient’s voiding pattern.
- Ask the patient to do kiggle exercises.
- Provide different methods to empty the patient’s bladder like crede’s method, valsalva’s maneuver etc.
- Use aseptic technique and sterile method when catheterizing the patient.
- Prescribe drugs to maintain continence.
- Ask the patient for regular follow-up.
- Monitor the patient’s urine intake output chart.
- Assess the patient for any signs and symptoms of urinary tract infection. To do.
- Provide the patient with a diet rich in vitamin C.
- Provide the patient with education to do Kegel exercises.
- Advise the patient to maintain personal hygiene.
- Assess the patient for any signs and symptoms of urinary incontinence.
- The patient Advise to take medication regularly.
1) Define /Explain renal cyst.
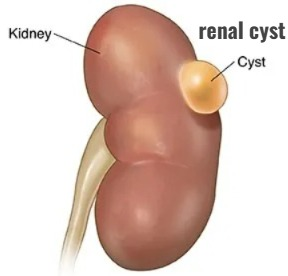
- A renal cyst is a fluid-filled sac that forms in the kidney.
- These cysts are non-cancerous and come in different sizes.
- If there is a single cyst, it occurs on the surface of the kidney, but when multiple cysts form, it affects one or both kidneys.
2) Explain the Etiology/ cause of the renal cyst.
- Due to age related changes.
- Due to genetic factors
- Due to acquired cystic kidney disease.
- Obstruction of the tubules Due to.
- Due to vascular factors.
- Due to inflammatory conditions.
- Due to weakening of the kidney layer.
3) Explain the Clinical manifestation/ sign and symptoms of the patient with the renal cyst.
- Abdominal pain.
- Feeling cold.
- Fever.
- Renal function is impaired.
- Hemanchuria.
- Flank pain.
- Urinary tract infection.
- High blood pressure.
- Palpable mass-like structure filling.
4) Explain the diagnostic evaluation of the patient with the renal cyst.
- history taking and physical examination.
- ultrasound.
- ct scan.
- MRI.
- kidney function test.
- laboratory test.
5) Explain the medical management of the patient with the renal cyst.
- Surgery to remove the cyst.
- Sclerotherapy to block blood flow to the cyst.
- Provide analgesic medicine if the patient is in pain.
- If the patient has any infection, then administer antibiotic medicine.
- If the patient has hypertension, then do lifestyle modification.
- Provide genetic counseling to the patient.
6) Explain the Nursing management of patients with the renal cyst.
- Properly inform the patient about his disease condition.
- Assess the patient for pain infection and any other signs and symptoms.
- Provide analgesic medicine if the patient is in pain.
- Provide mind diversional therapy to the patient To do.
- Monitor the patient’s vital signs regularly.
- Advise the patient to take adequate amounts of fluid.
- Collaborate with other health care personnel for the patient’s treatment.
- Provide psychological support to the patient.
- Advise the patient to make lifestyle modifications to his/her condition. Advise the patient to avoid hot and spicy foods. Advise the patient to follow a low-protein diet to prevent cyst growth. Advise the patient to limit salt intake. Advise the patient to have regular follow-up. –>
1) Explain/ define Renal Abscess.
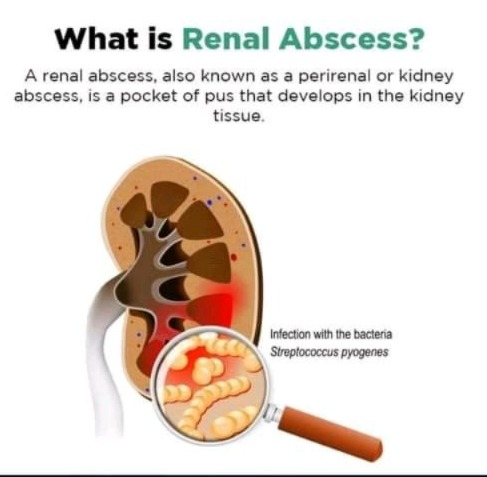
- Renal abscess is a condition in which pus forms in the tissues of the kidney.
- Renal abscess is mainly a complication of kidney infection.
- Pus develops in the tissues of the kidney and then forms an abscess.
2) Explain the Etiology/ cause of the renal Abscess.
- Due to urinary tract infection.
- Due to hematogenous spread.
- Due to urinary tract obstruction.
- Due to structural abnormality.
- Kidney Due to infection.
- Due to immunocompromise.
- Due to impaired immunity of diabetic patients.
- In pregnant women.
- In people with chronic kidney disease.
- In elderly people.
3)Explain the Clinical manifestation/sign and symptoms of the patient with the renal Abssess.
- Increase in body temperature.
- Abdominal pain.
- Decreased appetite.
- Pain while passing urine.
- Hematuria.
- Hypotension.
- Fever.
- Chills.
- Abdominal pain.
- Frequent urination.
- Nausea.
- Vomiting.
- Generalized weakness.
- Fatigue.
- Hypotension.
- Pale skin.
- Tachycardia.
4) Explain the diagnostic evaluation of the patient with the renal abscess.
- History taking and physical examination.
- CT scan.
- MRI.
- Urine examination.
- Blood investigation.
- Urine culture.
- Blood culture.
- Complete blood count test.
5) Explain the medical management of the patient with the renal abscess.
- If the patient has any infectious condition, provide antibiotic medicine.
- If the abscess is not treated with antibiotics, perform drainage procedure.
- If the patient is in pain, provide analgesic medicine.
- Maintain the patient’s fluid and electrolyte balance.
- Provide antipyretic medicine to the patient for management of fever.
- Advise the patient to have regular follow-up.
6) Explain the Nursing management of patients with the renal Abssess.
- If the patient has a fever, administer antipyretic medicine.
- If the patient is in pain, provide analgesic medicine to relieve it.
- Monitor the patient’s intake output chart.
- Advise the patient to maintain aseptic technique.
- Advise the patient to take adequate fluids.
1) Explain / Define Nephrotic syndrome.

Nephrotic syndrome is a combination of two words.
- 1) Nephron Meaning kidney.
- 2) syndrome denoting group of symptoms.
Nephrotic syndrome is a collection of symptoms that are mainly caused by damage to the glomeruli in the kidneys.
There are four main symptoms seen in nephrotic syndrome.
- 1) High levels of protein excreted from the body in the urine (proteinuria).
- 2) Decrease in the amount of protein in the blood (hypoalbuminemia).
- 3) Increase in the amount of lipids in the blood (hyperlipidemia).
- 4) In the body part Swelling (called edema).
These four main symptoms are seen in nephrotic syndrome.
Nephrotic syndrome affects people of any age.
It is mainly seen in children between the ages of two and six.
2) Explain the Etiology/cause of the Nephrotic syndrome. (Tell the cause of nephrotic syndrome.)
- Due to damage to the small blood vessels of the kidney.
- Due to some type of disease condition.
- Mainly seen in children.
- Due to abnormal kidney function.
- Due to diabetic kidney disease.
- Due to certain types of infections.
- Due to medications.
- Focal segmental glomerulosclerosis (FSGS).
- Scattered scarring of glomeruli.
- Membranous nephropathy.
- Due to heart failure.
- Due to certain types of infections such as Hepatitis B, Hepatitis C, Malaria etc.
3) Explain the Clinical manifestation/ sign and symptoms of the patient with the Nephrotic syndrome. (Describe the symptoms and signs of a patient with nephrotic syndrome)
- Swelling.
- Swelling is mainly seen in the lining of the eye socket and around the eye.
- Swelling is mainly seen in the feet and ankles due to sitting or standing for a long time.
- Swelling is often seen in the whole body, which is called Anasarca. is.
- Oliguria (decreased urine output).
- Weight gain.
- Hematuria (blood in urine).
- Respiratory distress.
- Increased blood pressure.
- Kidney failure To be.
- Increase in cholesterol levels in the body.
- Feeling tired.
- Getting an infection immediately.
- Not feeling hungry.
- Feeling tired.
4) Explain the diagnostic evaluation of the patient with the Nephrotic syndrome.Write the diagnostic evaluation of the patient with Nephrotic syndrome.
- History taking and physical examination.
- Urine test.
- Blood test.
- Kidney Biopsy.
- Blood pressure monitoring.
- Blood chemistry.
- Imaging study.
- Ultrasound.
- CT scan.
5) Explain the medical management of the patient with the Nephrotic syndrome.
- Provide the patient with corticosteroids medicine to treat inflammation.
- Provide the patient with immunosuppressive medicine.
- Provide the patient with diuretic medicine.
- Provide antihypertensive medicine to the patient.
- Provide ACE inhibitor medicine to the patient.
- Provide statin group medicine to decrease the patient’s cholesterol level.
- Advise the patient to restrict salt.
- Advise the patient to reduce fluid intake.
- Provide anticoagulant medicine to the patient.
6) Explain the Nursing management of patients with the Nephrotic syndrome. (Explain the nursing management of a patient with nephrotic syndrome)
- Properly assess the patient.
- Monitor the patient’s vital signs.
- Monitor the patient’s fluid balance.
- Monitor the patient’s weight regularly.
- Monitor the patient’s intake output chart.
- If the patient has a condition of edema, elevate the extremities.
- If the patient has a condition of edema, apply compression stockings and monitor fluid levels.
- Continuously maintain the patient’s nutritional status.
- Advise the patient to avoid protein and salt.
- Provide proper meditation to the patient.
- Provide complete information to the patient about his disease condition, its causes, his symptoms and signs and diagnostic evaluation.
- Advise the patient to maintain personal hygiene to prevent infection.
- Provide emotional support to the patient.
- Proper care of the patient To collaborate with other health care personnel.
- Provide complete education to the patient and his family members.
- To clear all doubts of the patient and his family members.
1) Explain/Define Renal failure. (Define Renal Failure)
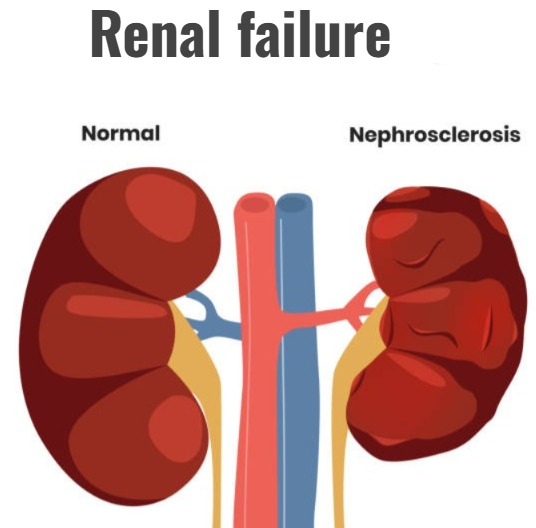
- Renal failure is also known as kidney failure.
- Renal failure is a condition in which the kidneys lose their ability to remove waste products and filter them from the body.
- This condition causes toxic materials to accumulate in the body and electrolyte imbalances in the body. Renal failure is a condition in which the kidneys fail to function adequately.
There are two types of renal failure.
1) Acute Renal failure
2) Chronic Renal failure
1) Define/ Explain the Acute Renal failure.
- Acute renal failure is also known as acute kidney injury (AKI). In which kidney function declines suddenly and rapidly.
- Acute kidney failure is a condition in which the functional ability of the kidneys is suddenly impaired, due to which the kidneys cannot filter properly and cannot maintain electrolyte balance and fluid balance in the body. Acute kidney failure occurs within 7 to 90 days.
- In acute kidney failure, the glomerular filtration rate mainly decreases, the concentration of blood urea nitrogen increases, the amount of creatinine increases, and the urine output is reduced. If it is less than 400ml per day, the condition of hyperkalemia arises and sodium retention is observed in the body.
2) Explain the Etiology/ cause of the Acute Renal failure.
1) Pre Renal cause
- Due to impaired blood supply to the kidneys.
- Due to dehydration.
- Diarrhea.
- vomiting.
- hemorrhage.
- burn.
- diuretic medicine Due to excessive use of.
- Due to decrease in cardiac output.
- Due to congestive heart failure.
- Due to cardiogenic shock.
- Due to acute pulmonary embolism.
- Due to constriction of the blood vessels supplying blood to the kidneys.
- Due to dilation of blood vessels supplying blood to the kidney.
2) Intrarenal (Intra Renal)
- Intrarenal failure is mainly caused by structural damage to the glomeruli, renal tubules, and nephrons.
- Prolonged renal ischemia.
- Blood clots, cholesterol deposits around the veins and arteries.
- Infection.
- Hemolytic uremic syndrome.
- Severe transfusion reaction.
- Exposure to any nephrotoxic agent.
- Like:=
NSAID Drug,
ACE inhibitor,
Aminoglycoside Lupus,
Multiple myeloma,
3) Postrenal
- Obstructed urine flow.
- Kidney stones.
- Cancer of the urinary tract organs.
- Due to some types of medication.
- Due to bladder stones.
- Due to enlarged prostate gland.
- Due to bladder cancer.
- Due to neurological disorders.
3) Explain the Risk factore of the Acute Renal failure.
- Due to advanced age.
- Due to blood vessel blockage.
- Due to diabetes.
- Due to high blood pressure.
- Due to kidney disease.
- Due to heart failure.
- Due to liver disease.
4) Explain the Clinical manifestation/ sign and symptoms of the patient with the Acute Renal failure.
- Oliguria (decreased urine output),
- Anuria (no urine output),
- Fluid retention.
- ED.
- Electrolyte imbalance.
- Muscle weakness.
- Uremic symptoms.
- Hypertension.
- Bruising and bleeding.
- Respiratory distress.
- Neurological symptoms.
- Cardiovascular complications.
- Patient is critically ill and lethargic.
- Passing dark colored urine.
- Foamy or bubbly urine.
- Dry skin and mucous membranes.
- Azotemia.
- Rapid heart rate.
- Flank pain.
- Shortness of breath.
- Metabolic acidosis.
- Anemia and platelet dysfunction.
- Increased susceptibility to secondary infections.
- Generalized malaise.
- Fatigue.
- Cardiac problems.
- Increased susceptibility to secondary infections.
- Fluid and electrolyte imbalance.
- Fluid overload.
- Hyperkalemia.
- Hyponatremia.
- Hypocalcemia.
- Hypermagnesemia.
- Loss of appetite.
- Nausea.
- Vomiting.
- Diarrhea.
- Constipation.
- Dry mucous membranes.
- Metallic taste from the mouth.
- Abdominal pain.
- Headache.
- Drowsiness.
- Irritability.
- Confusion.
- Peripheral neuropathy.
- Stunting.
- Coma.
5) Explain the diagnostic evaluation of the patient with Acute renal failure.
- History taking and physical examination.
- Blood test.
- Potassium test.
- Electrolyte test.
- Urine test.
- ECG.
- Kidney biopsy.
- Imaging test.
- Kidney biopsy.
6) Explain the medical management of the patient with the renal failure.
- Identify the specific cause of the patient with the renal failure.
- Assess whether the patient has a urinary tract infection.
- Assess the patient’s fluid level.
- Provide the patient with proper diuretic medicine.
- Monitor the patient’s electrolyte level.
- If the patient has severe renal failure, perform dialysis.
- Provide the patient with proper medicine.
- Provide nutritional support to the patient.
- Provide antihypertensive medicine to the patient.
- Provide medication to control anemia.
- Continuously monitor the patient’s renal function.
- Continuously monitor the patient’s electrolyte levels.
- Advise the patient to make lifestyle modifications.
7) Explain the Nursing management of patients with Acute renal failure.
- Properly assess the patient.
- Properly monitor the patient’s vital signs.
- Properly monitor the patient’s fluid balance.
- Properly monitor the patient’s intake output chart.
- Monitor the patient’s blood urea nitrogen level.
- Assess the patient for any signs and symptoms of fluid overload.
- Collaborate with the health care team.
- Monitor the patient’s electrolyte levels.
- Provide the patient with appropriate medication.
- Provide the patient with antihypertensive medication.
- Provide proper nutritional support to the patient.
- Advise the patient for fluid restriction.
- Provide proper dialysis care to the patient.
- Provide proper skin care to the patient.
- Properly monitor the patient’s skin integrity.
- Advise the patient to follow dietary restrictions.
- Provide psychological support to the patient.
- Advise the patient to maintain proper hygienic conditions.
- Properly collaborate with the patient’s health care team.
- Monitor the patient’s intake output chart.
- Monitor the patient’s daily weight.
- Properly monitor the patient’s blood pressure.
- Monitor the patient’s blood urea nitrogen level, creatinine and electrolyte levels.
- Monitor the patient’s nutritional status.
- Provide the patient with a high-calorie, low-protein, low-sodium, low-potassium diet and vitamin supplementation.
- Provide the patient with small and frequent amounts of food.
- Advise the patient to maintain strict aseptic technique.
- Provide good mouth care to the patient.
- Properly monitor the patient’s heart activity.
1) Explain/ define the chronic renal failure. (Define Chronic Renal Failure)
- Chronic renal failure is also known as chronic kidney disease ( CKD ). Comes.
- In chronic kidney failure, kidney function rapidly and progressively deteriorates, causing electrolyte imbalance and fluid imbalance, which causes conditions such as uremia and azotemia to arise over a period of months or years.
- In chronic renal failure, renal excretory and regulatory function is slowly, insidiously, and irreversibly impaired.
- The final stage of chronic kidney disease is called end-stage renal disease (ESRD).
- Chronic kidney disease is a condition in which the kidneys are gradually unable to filter waste products and fluids from the body, resulting in the accumulation of toxic substances in the body. This condition is mainly caused by various reasons such as diabetes, hypertension, glomerulonephritis, polycystic kidney disease, etc.
2) Explain the Etiology/cause of the chronic renal failure. (Give reasons for chronic renal failure)
- Due to diabetes mellitus.
- Due to hypertension.
- Due to a family history of kidney disease.
- Due to frequent episodes of acute renal failure.
- Due to long-term infections such as chronic pyelonephritis and tuberculosis.
- Due to autoimmune disorders.
- Due to polycystic kidney disease.
- Due to nephrotoxic agents.
- Due to certain types of chemicals.
- Due to reflux nephropathy.
- Due to any injury or trauma.
- Due to kidney stones and infection.
3) Explain the Clinical manifestation/ sign and symptoms of the patient with the chronic kidney disease. (Tell the symptoms and signs of chronic kidney disease)
- Fatigue.
- Weakness.
- Fluid retention.
- Erectile dysfunction.
- Changes in urination.
- Increased urinary frequency.
- Hypertension.
- Electrolyte imbalance.
- Anemia.
- Bone pain.
- Fracture.
- Mineral imbalance Itching (pruritus).
- Difficulty breathing.
- Neuropathy.
- Numbness.
- Weakness.
- Vomiting.
- Loss of appetite.
- Weight loss.
- Cognitive impairment.
- Personality changes.
- Confusion.
- Inability to concentrate.
- Disorientation.
- Flapping hands.
- Restlessness.
- Burning sensation in feet.
- Chest pain.
- Hyperlipidemia.
- Hyperkalemia.
4) Explain the diagnostic evaluation of the patient with the chronic kidney disease. (Explain the diagnostic evaluation of the patient with chronic kidney disease)
- history taking and physical examination.
- Blood test.
- Serum creatinine test.
- Blood urea nitrogen test.
- Urine test.
- Albumin to creatinine ratio.
- Imaging study.
- Ultrasound.
- CT scan.
- MRI.
- Kidney biopsy.
- Glomerular filtration rate.
- Assess the electrolyte Level.
- Assess the hemoglobin level.
- Assess the hematocrit level.
- Blood pressure monitoring.
5) Explain the medical management of the patient with the chronic kidney disease. (Describe the medical management of a patient with chronic kidney disease)
- If the patient has a condition of high blood pressure, then provide antihypertensive medicine.
- If the patient has a condition of diabetes, then provide antidiabetic medicine.
- Provide the patient with A.C.E inhibitor medication.
- The patient’s blood cholesterol Provide statin group medicine to reduce.
- Provide iron supplement to the patient for the treatment of anemia.
- Provide phosphate binder medicine if the patient has a condition of hyperphosphatemia.
- Provide calcium and vitamin D supplement to the patient.
- Provide diuretic medication to prevent the patient from fluid retention. To do.
- Provide the patient with properly nutritious food.
- Properly monitor the patient.
- Advise the patient to modify his/her lifestyle.
- Advise the patient to quit smoking.
- Advise the patient to maintain a healthy weight.
- Advise the patient to exercise regularly.
- Advise the patient to limit alcohol.
- Properly refer the patient for specialized care.
- Provide proper care to the patient to prevent any other complications.
6) Explain the Nursing management of patients with the chronic kidney disease. Explain the nursing management of patients with the chronic kidney disease.
- Properly assess the patient.
- Properly monitor the patient’s vital signs.
- Properly monitor the patient’s fluid balance.
- Assess the patient for any other complications.
- Provide the patient with the prescribed medicine.
- Monitor the patient’s fluid and electrolyte levels.
- Properly provide nutritional counseling to the patient.
- Properly monitor the patient’s hemoglobin level.
- Properly monitor the patient’s blood pressure.
- Properly provide education to the patient.
- Assess the patient for any other signs or symptoms.
- Provide appropriate psychological support to the patient.
- Advise the patient on lifestyle modifications to prevent other complications.
- Collaborate with other health care personnel for proper care of the patient.
- Provide appropriate support to the patient and their family members. Provide psychological support.
1) Explain/ Define the Dialysis. Dialysis.

- Dialysis is a medical procedure. Dialysis is done when the kidney function is impaired.
- Dialysis is done when the kidneys are not able to perform their function and therefore are not able to remove toxic substances from the body. Dialysis is done to filter the blood, remove toxic substances and fluids from the body and maintain electrolyte balance.
- Dialysis is a procedure in which fluid and molecules are transferred from one compartment to another through a semipermeable membrane.
2) Explain the Goal of the Dialysis. State the goal of dialysis.
- To remove the end products of protein metabolism such as urea and creatinine from the body.
- To maintain a safe concentration of serum electrolytes.
- To correct acidosis.
- To remove excess fluid from the body.
- To prevent the accumulation of toxin substances in the body.
3) Explain the indication of the Dialysis. State the indications for dialysis.
- In patients with irreversible kidney disease.
- To control uremia.
- In patients with impaired kidney function.
- In patients with end stage renal disease (ESRD).
- In the condition of acute renal failure.
- In the condition of chronic renal failure.
4) Explain the three principles of the Dialysis. Describe the principles of dialysis.
There are three main principles of dialysis.
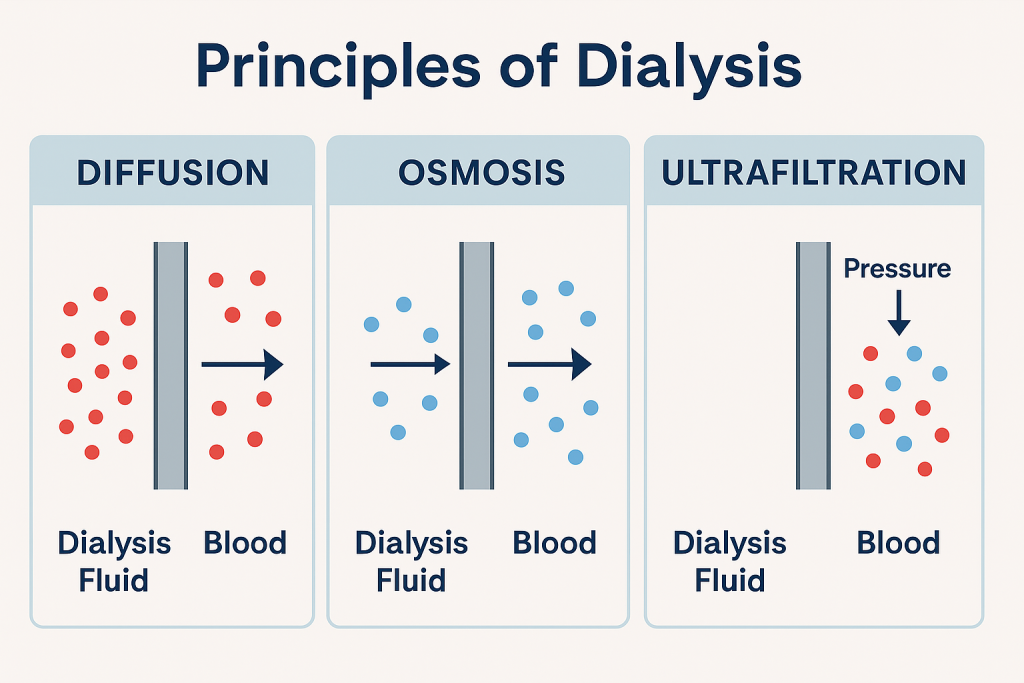
- 1) Diffusion (diffusion),
- 2) Osmosis (Osmosis),
- 3) Ultrafiltration (Ultrafiltration)
1) Diffusion,
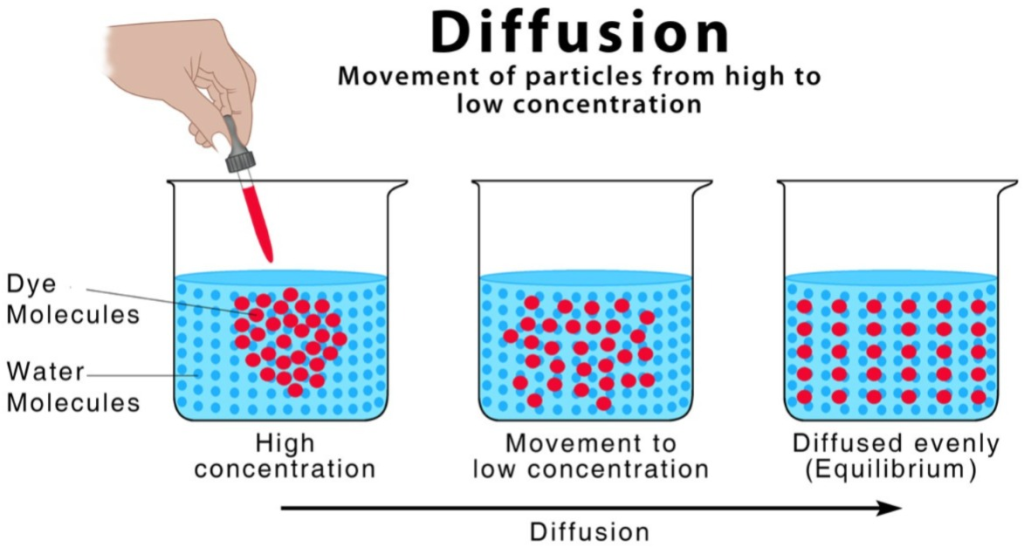
- In diffusion, solutes move from high concentration to low concentration across a semipermeable membrane.
2) Osmosis,
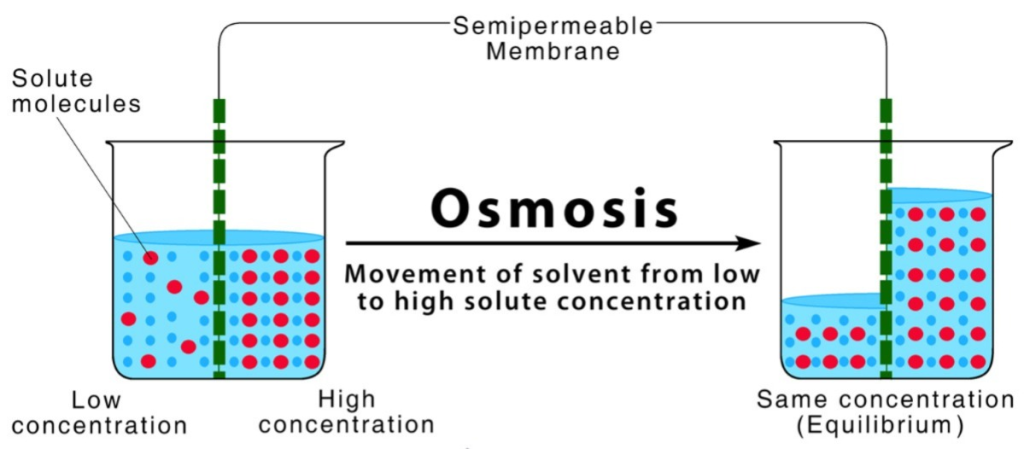
- Osmosis is the process in which fluid (water) moves from a lower solute concentration to a higher solute concentration through a semipermeable membrane and continues to move until the concentration on both sides of the semipermeable membrane is equal.
- In this process, mainly excess water is removed from the blood.
3) Ultrafiltration
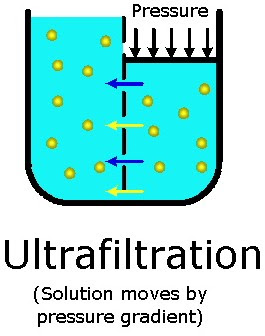
- In the ultrafiltration process, water moves from high pressure to low pressure.
- Ultrafiltration is mainly Dialysis is done by applying negative pressure to the membrane.
- This process is mainly more efficient in removing water from the body.
- Dialysis is mainly of two types.
- 1) Peritoneal Dialysis ( Peritoneal Dialysis)
- 2) Hemodialysis ( hemodiasis).
1) Explain/Define the Hemodialysis. Describe Hemodialysis.
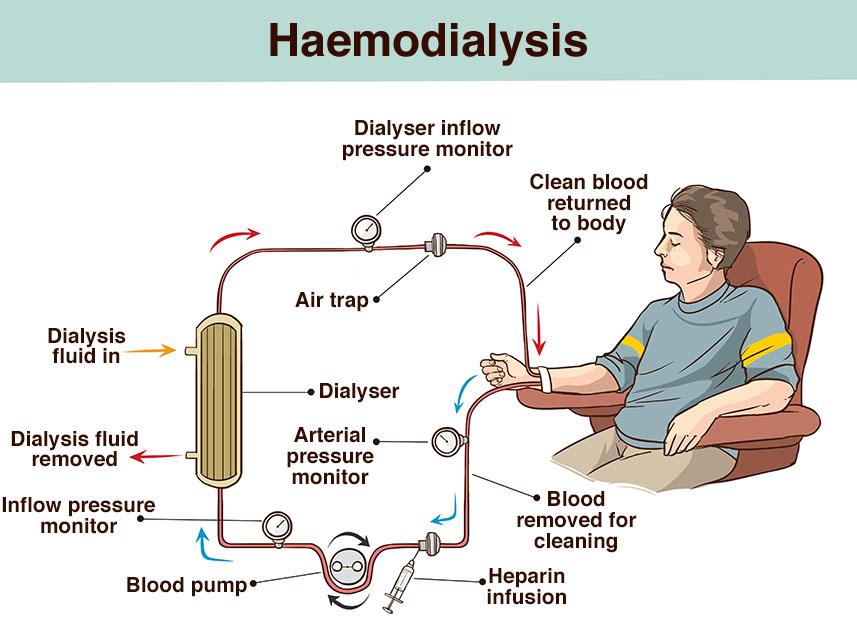
- Hemodialysis removes waste, toxic materials and extra fluid from the body and balances electrolytes (sodium, potassium bicarbonate, chloride, calcium, magnesium and phosphate).
- Hemodialysis is a medical procedure in which the blood of a person with kidney failure is filtered and toxic materials and waste products are removed from it.
- Hemodialysis is a procedure in which blood is continuously removed from the body and passed through an artificial kidney to be cleaned.
- A dialysis machine pumps the blood through a dialyzer.
- The cleaned blood is then returned to the patient’s body.
- Hemodialysis is a process in which blood is continuously removed from the body and is passed through an artificial kidney to be cleaned. It is continuously removed from the.
- This filter, which is known as a dialyzer or artificial kidney, has 10 to 12 pints of blood in the average person.
- During dialysis, only one pint of blood passes through the dialyzer.
2) Explain/ Define the Dialyzer. Connect the dialyzer.

- The dialyzer is known as the key to hemodialysis.
- A dialyzer is a man-made membrane and acts as an artificial kidney.
- A dialyzer consists of a semipermeable hollow fiber membrane that contains thousands of tiny cellophane tubules that act as a semipermeable membrane made of cellulose and other synthetic materials.
- A dialyzer consists of two sections.
- One section is for the dialysate and the other section is for the blood and they are divided from each other by a semipermeable membrane which Therefore, they can be prevented from mixing with each other.
- The semipermeable membrane has some microscopic holes that only allow certain substances to cross.
- This dialyzer removes the toxic substances present in the blood.
- Only water, waste products such as urea, potassium and extra fluid pass through the semipermeable membrane in the dialyzer, but blood cells and proteins do not pass through it because they are bigger than the holes in the semipermeable membrane.
3) Explain the Dialysate. Describe the dialysate.
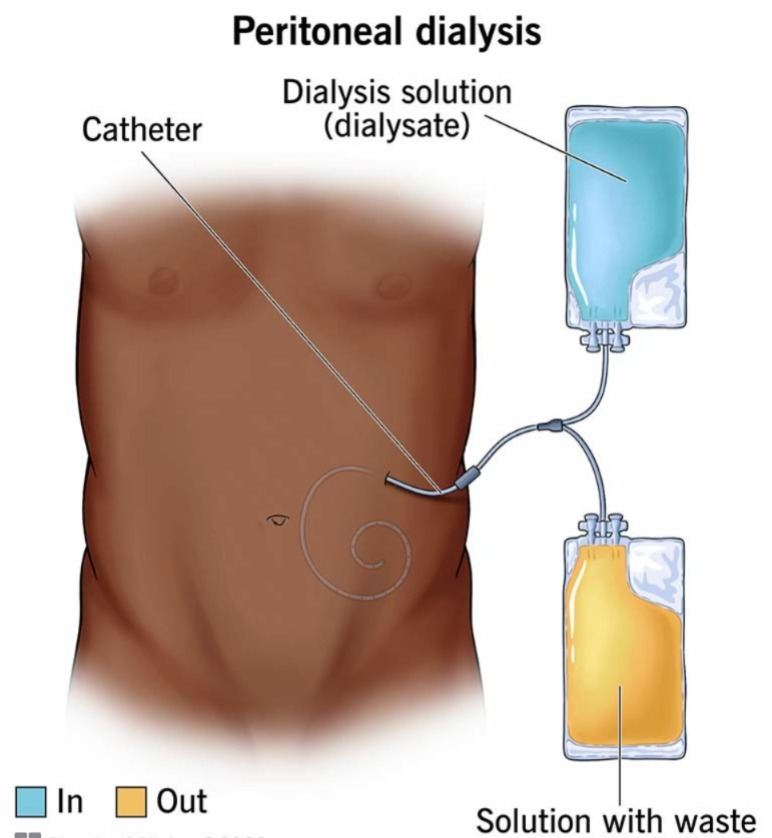
- Dialysate is also called dialysis fluid, dialysis solution, or bath.
- Dialysate solution is made up of pure water, electrolytes, and salts such as bicarbonate and sodium.
- The purpose of dialysate is primarily to remove toxic substances from the blood and pull them into the dialysate.
- The toxic materials present in the blood are removed through a diffusion process in the dialysate.
4) Explain the vascular access. Describe vascular access.
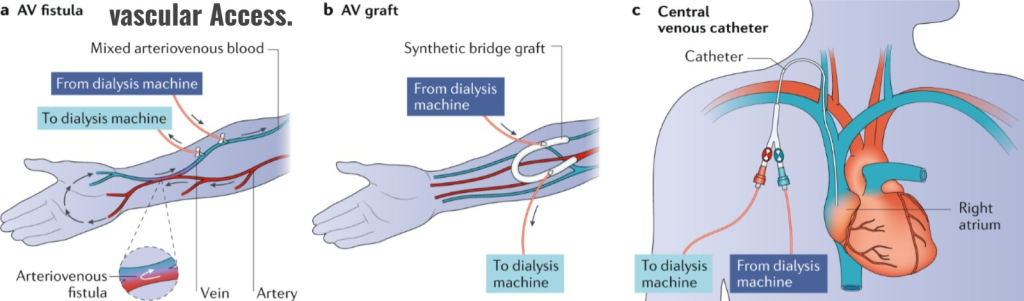
An important step before starting dialysis is to prepare the vascular access.
Access is done so that the blood in which toxic material is present is removed from the body and circulated through the dialysis machine and the blood with the removed toxic material is returned to the body through the access.
After the access is healed, two needles are connected to the tubing and inserted into the access, out of which the toxic blood present in the body is removed through one needle and that blood enters the dialysis machine and is filtered, after which the filtered blood is returned to the body through the other needle.
A week or a month before starting dialysis Vascular access is formed.
There are three types of access formation in hemodialysis.
- 1) AV FISTULA ( Atriovenous fistula) ,
- 2) AV GRAFT ( Arteriovenous Graft) ,
- 3) Central venous catheter ( Central venous catheter) .
•••>
1) AV FISTULA (Atriovenous fistula),
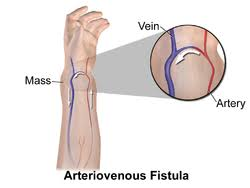
- Atriovenous fistula is the preferred type of vascular access.
- This is a type of surgical procedure that is mainly used to make a connection between an artery and a vein.
- •> In this atriovenous fistula, a connection is mainly made between the site of the artery and the site of the vein.
Or
•> A connection is made between the site of the artery and the end of the vein.
Or
•> A connection is made between the end of the artery and the site of the vein.
Or
•> And a connection is made between the end of the artery and the end of the vein. - Atriovenous fistula is mainly done in the upper arm and lower arm.
- This fistula takes about four to six weeks to mature.
- Atriovenous fistula is the best access for dialysis because it has fewer complications and lasts longer.
2) AV GRAFT (Arteriovenous Graft),
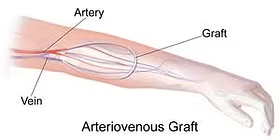
- Many times, the vein in the patient’s arm is not suitable for creating a fistula.
- In such cases, the surgeon uses a flexible rubber tube to create a path between the artery and the vein, which is called a synthetic bridge graft.
- This graft is mainly surgically anastomosised between an artery (brachial) and a vein (antecubital).
- This graft is mainly used in the forearm, It is performed in the upperarm and thigh.
- Atriovenous grafts mature faster than atriovenous fistulas. But an atriovenous graft is artificial, narrow and more infected.
3) Central venous catheter (Central venous catheter) .
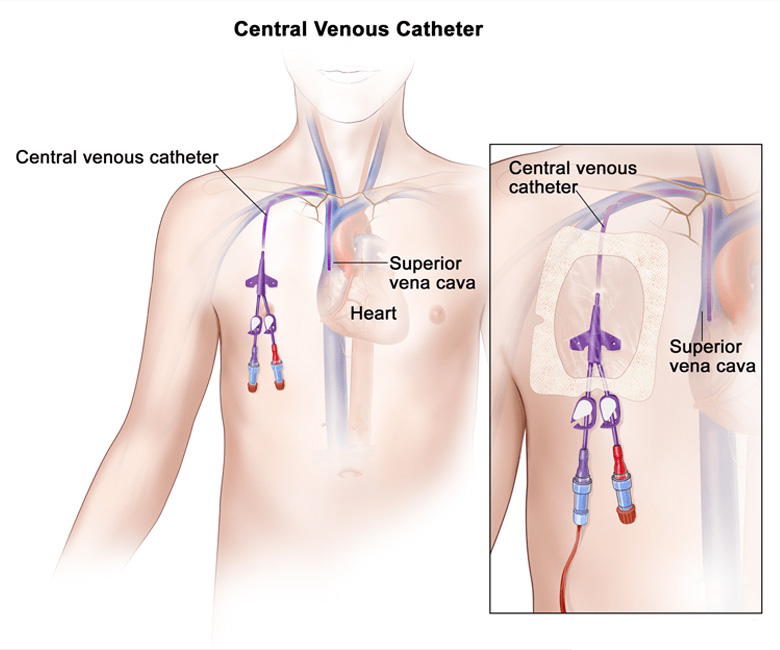
- Central venous catheter is mainly used when dialysis needs to be started immediately and when the patient has an atriovenous fistula and atriovenous graft.
- A central venous catheter is a thin flexible tube placed in a large vein to perform dialysis.
5) Explain the Hemodialysis procedure. Describe the procedure of hemodialysis.
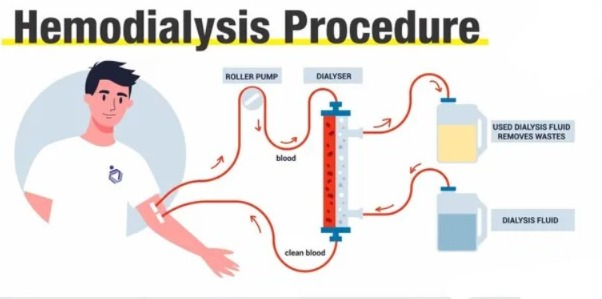
- When a patient is admitted for dialysis, his vital signs should be checked.
- Assess the patient’s weight.
- The patient is then “put on the machine”
- Two needles are inserted into the patient’s vascular access site, one to withdraw blood from the body and the other to return the blood. Helps to enter the body.
- The dialyzer has two compartments that are separated by a semipermeable membrane.
- Blood flows mainly in one direction from the blood compartment. 200-500ml/min and dialysate flows in the opposite direction from the dialysate compartment. 300-900ml/min.
- A dialysis session takes 2 to 6 hours.
- This Continuously monitor the patient’s heart rate, blood pressure, and respiration during dialysis sessions.
- Blood samples are collected before and after the dialysis procedure to assess changes in blood pressure.
- People who need dialysis need dialysis three times a week, and one dialysis session takes 3 to 5 hours to complete. During dialysis, the patient is given medication to replace the hormones that the kidneys are unable to produce.
6) Explain the care for excess . Explain the care for excess.
- It is important to take care of the access to prevent complications.
- The area where the access has formed should be washed with soap and water daily and washed properly before dialysis.
- Do not scratch the access area.
- Assess the patient for any signs and symptoms of infection at the access area.
- Check whether there is proper blood flow at the accessed site.
- Vibrate the access side, if absent, notify the health care provider immediately.
- Take proper care to avoid any kind of trauma to the accessed site.
- Do not wear any kind of tight clothes, jewelry and do not lift any heavy items.
- The arm above Do not provide blood samples, blood pressure measurements, or any type of injection from the arm where the access was formed.
- When removing the needle inserted at the access site, apply gentle pressure to the needle site for a short time to stop bleeding.
- If bleeding at the access site does not stop within 30 minutes, inform the health care provider immediately.
6) Explain the complications of the Hemodialysis. Explain the complications of the Hemodialysis.
- Infection,
- Aneurysm,
- Stenosis,
- Blood loss,
- Heart failure,
- Chest pain.
7) Explain the Risk of the Hemodialysis. Explain the risks of hemodialysis.
- Anemia,
- Nausea,
- Infection,
- Infectious diseases,
- Vomiting.
8) Explain the Nursing interventions of the patient with the Hemodialysis. Explain the nursing management of the patient with hemodialysis.
- Properly assess the patient.
- Regularly assess the patient’s vital signs.
- Properly assess the patient’s fluid status.
- Properly monitor the patient’s weight before and after dialysis.
- Properly assess the access site to determine if any infection is present. Assess.
- Properly monitor the patient’s fluid intake to prevent fluid overload.
- Weigh the patient daily to ensure proper fluid provision.
- Provide the patient with prescribed medication.
- Monitor the patient for any side effects of the drug.
- Access the site to any type Advise the patient to maintain proper hygiene to prevent infection.
- Advise the patient not to perform any heavy procedures on the access site.
- Advise the patient to control the diet rich in potassium, phosphorus and sodium.
- Provide proper psychological support to the patient.
- Laboratory values of the patient such as serum creatinine, electrolytes, hemoglobin levels Continuously monitor.
- Advise the patient to maintain proper hygienic conditions to prevent infection.
- Properly collaborate with other health care personnel to provide proper care to the patient.
- Keep emergency medications and treatments ready while on dialysis so that immediate care can be provided to the patient in case of an emergency during dialysis.
- Advise the patient to take medication and follow up regularly.
1) Explain the peritonial Dialysis. Describe peritoneal dialysis.
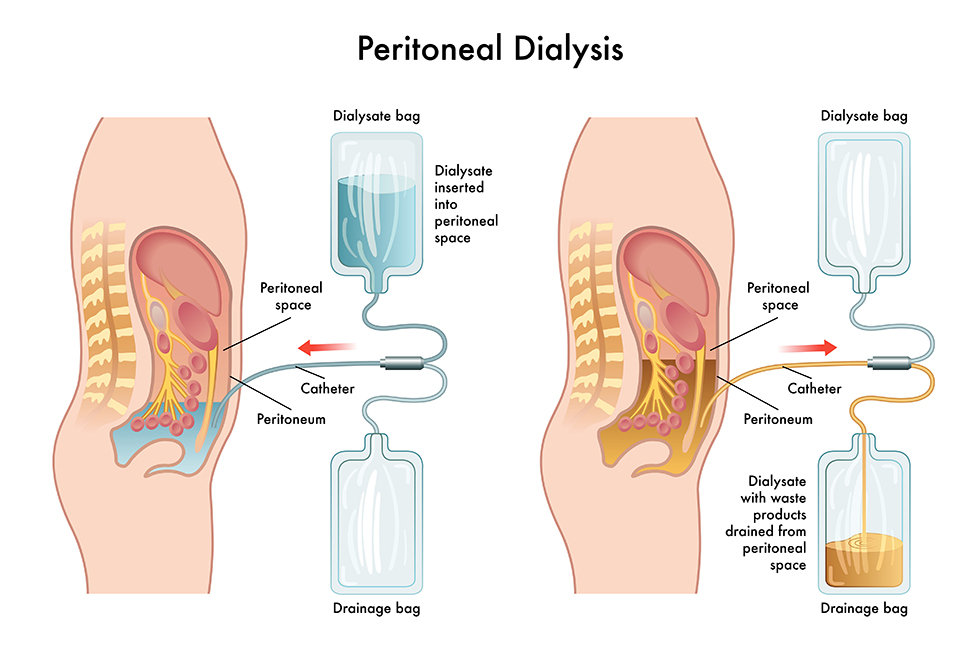
- Peritoneal dialysis is a form of dialysis.
- In peritoneal dialysis, a special fluid called dialysate is infused into the peritoneal cavity. A container in the peritoneal cavity that is surrounded by arteries and veins, which allows blood to flow and remove waste products from the peritoneal cavity.
- In peritoneal dialysis, the peritoneal cavity acts as a semipermeable membrane and helps remove waste materials from the body.
- In peritoneal dialysis, the dialysate solution is instilled into the peritoneal cavity.
{ Dwell time (dwell time) := The period of time for which the cleansing solution (Dialysate) is introduced into the peritoneal cavity, the period of time for which the solution remains in the peritoneal cavity is known as Dwell time.}
- In peritoneal dialysis, the dialysate solution is repeatedly instilled into the cavity and then the excess waste products and toxic substances present in the body are removed.
- The dwell time of the dialysate solution is 30 to 40 minutes. (Dwell time is the period of time for which the dialysate solution instilled into the peritoneal cavity remains in the peritoneal cavity.)
- Maximum exchange occurs in the first 5 minutes.
- Equilibrium between blood and dialysate solution occurs in 15 to 30 minutes.
- Peritoneal dialysis is mainly used to remove toxic substances and metabolic waste products from the body and to reestablish normal fluid and electrolyte balance.
2) Explain the types of peritonial Dialysis. State the type of peritoneal dialysis.

- 1) CAPD (Continuous Ambulatory Peritoneal Dialysis/ Continuous Ambulatory Peritoneal Dialysis),
- 2) APD ( Automated peritonial Dialysis)
•••>
1) CAPD ( Continuous Ambulatory Peritoneal Dialysis),
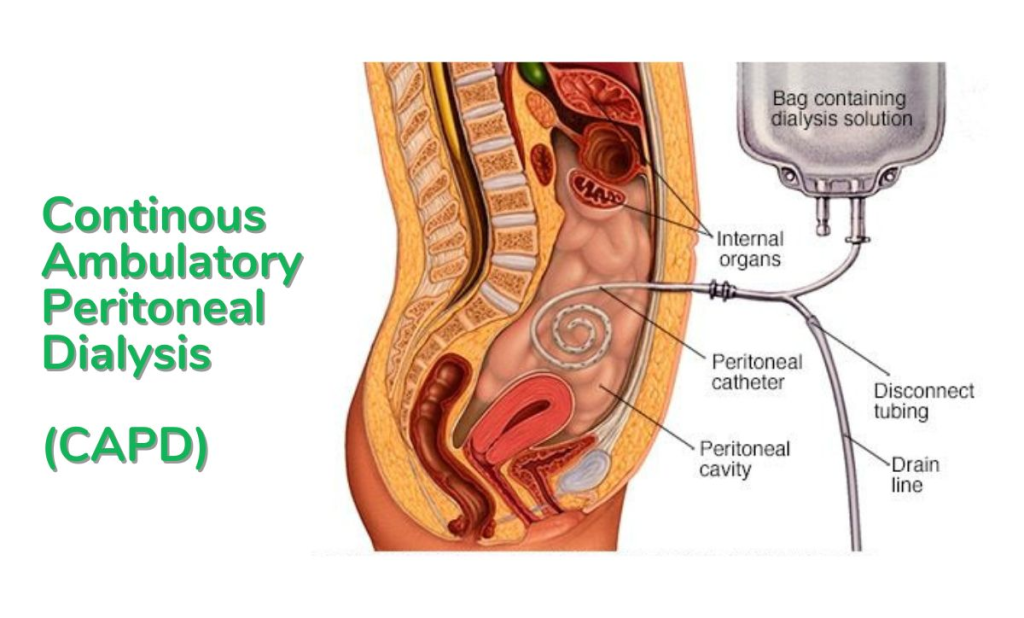
- This type of peritoneal dialysis does not require any machinery.
- This type of dialysis is mainly done by the patient and is performed by a caregiver.
- In continuous ambulatory peritoneal dialysis, 1.5 to 3.0 liters of dialysate is instilled into the abdominal cavity daily.
- Continuous ambulatory peritoneal dialysis is performed four to five times throughout the day.
- Three dialysis sessions are performed during the day.
- A long dialysis session is performed mainly at night and lasts for 8 hours. How long it takes.
- In this procedure, two liters (2 liters) of dialysate solution is instilled into the peritoneal cavity using a plastic tube. Then the tube is attached to one side by a permanent catheter and the other side of the bag is attached to the spike. Then after instilling the dialysate solution into the peritoneal cavity, the bag and tubing are disconnected.
- When the equilibrium period of the dialysate solution and blood is completed, the tubing is reconnected and the dialysate solution remaining in the peritoneal cavity is drained and returned to the peritoneal cavity in two A liter of solution is infused.
- In this way, three dialysis sessions are performed during the day and one long dialysis session during the night.
2) APD (Automated peritonial Dialysis)
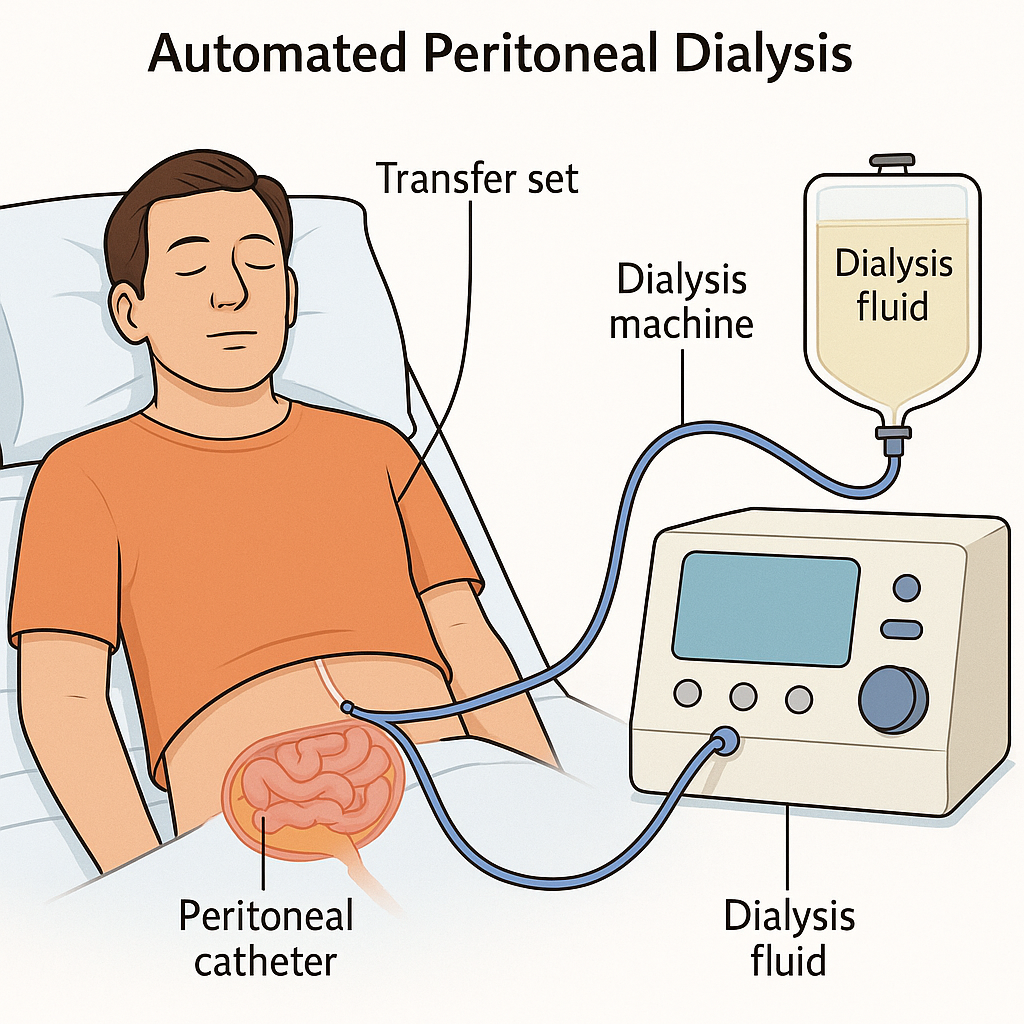
- In automated peritoneal dialysis, cycler equipment is used to instill the dialysate solution into the peritoneal cavity.
- In automated cycler equipment, the filling, dwell and drain times of the dialysate solution are set.
- In automated peritoneal dialysis, fluid is exchanged four to eight times in a night and there is a one to two hour dwell time.
- Many times, medications are also added to the dialysis solution, such as heparin to prevent blood clotting, insulin for diabetic patients, and antibiotic medications to prevent the patient from infection.
There are three types of automated peritoneal dialysis.
- 1) continuous cyclic peritoneal dialysis,
- 2) IPD (Intermittent Peritoneal Dialysis),
- 3) NPD (Nocturnal Peritoneal Dialysis)
•••>
1) continuous Cyclic Peritoneal Dialysis,
- This is the most common type of peritoneal dialysis.
- In continuous cyclic peritoneal dialysis, exchange is mainly done through cycler equipment.
- This type of dialysis is mainly done when the patient is in a sleeping position at night.
- In this dialysis, the dialysate solution is infused by the machine and then removed after two to three hours. is done and then fresh solution is infused again.
- A session (4 cycles) takes 10 to 12 hours to complete.
2) IPD (Intermittent Peritoneal Dialysis),
- Intermittent peritoneal dialysis is not a continuous procedure of dialysis.
- This type of dialysis is performed three to four times in a week.
- In this type of dialysis, a machine administers the same dialysate solution into the peritoneal cavity and the drain is also done by the machine itself. This session takes 12 to 24 hours to complete.
3) NPD (Nocturnal Peritoneal Dialysis)
- This type of dialysis is mainly performed at night.
3) Explain the equipment used for peritoneal dialysis. Please list the equipment for peritoneal dialysis.
- Intraperitoneal dialysis solution.
- Peritoneal dialysis catheter.
- Peritoneal dialysis set (infusion and drainage).
- Dressing tray.
- Emergency Medicine Tray.
- Injection Tray.
- T.P.R And B.p. Tray.
- I.v. Stand.
- Bucket for Discarded Drainage Fluid.
4) Explain the procedure for peritonial Dialysis. Explain the procedure of peritoneal dialysis.
1) Preparation of the patient:=
- To fully prepare the patient for dialysis before catheter insertion.
- To provide information about dialysis to the client who is going to undergo the dialysis procedure.
- Provide the patient with a thorough explanation of dialysis.
- Properly monitor the patient’s vital signs.
- Monitor the patient’s temperature, pulse, respiration, and blood pressure.
- Monitor the patient’s daily weight.
- Monitor the patient’s serum electrolyte levels before dialysis.
- Advise the patient to completely empty the bowel and bladder before performing the dialysis procedure.
- Properly measure the patient’s central venous pressure.
- Properly monitor the patient’s cardiac output.
- Properly provide the patient with a supine position before performing dialysis and wear a mask to prevent air-born infection.
- The dialysate solution is Before instilling into the abdominal cavity, warm the dialysate solution to body temperature and then instill it into the abdominal cavity to prevent discomfort and abdominal pain and to dilate the blood vessels so that urea clearance can occur properly.
- Instill heparin with the solution to prevent blood clotting in the catheter.
- Administer broad-spectrum antibiotic medication to the patient to prevent infection.
2) Peritoneal Dialysis Access.
- In peritoneal dialysis access, a catheter or flexible hollow tube is surgically placed in the lower abdomen.
- This catheter is usually inserted two to five centimeters below the umbilicus.
- This catheter is usually inserted in the operating room under local anesthesia.
- Before the procedure, the skin is prepared with an antiseptic solution to prevent infection. can be done.
- The physician advises the patient to raise his head and then tighten the abdominal muscles, after which a puncture is made in the abdomen with the help of a trochar.
- Then a peritoneal catheter is installed in the peritoneal space.
- This catheter is used to remove toxic materials.
- Then this catheter is properly secured with a purse-string suture.
- Then antimicrobial ointment and sterile dressing are applied to prevent infection.
3) Peritonial Dialysis treatment:=
- In peritoneal dialysis, a catheter is placed through which the exchange process is performed.
- Exchange is a process in which a dialysate solution is instilled into the abdominal cavity, after which the solution is left in the abdominal cavity until the toxic material is exchanged, and then the dialysate solution is drained from the body.
- This exchange procedure usually takes one to four hours.
- Thus, the procedure of peritoneal dialysis is performed in the peritoneal cavity.
1) Explain the KIDNEY CANCER Kidney cancer.
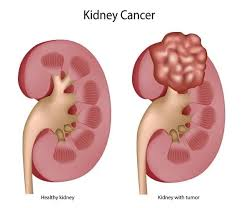
- Kidney Cancer Renal Cancer Also called.
- In this, abnormal and uncomfortable growth occurs in the cells of the kidney and the formation of a tumor.
- These tumors can be both benign and malignant.
- Kidney cancer mainly affects the kidney. The two parts are overproduced.
the Renal tubule, ( Renal cell carcinoma),
The Renal pelvis ( transitional cell carcinoma).
- If a patient has a renal tumor, he complains of blood in the urine (hematuria) or a mass and pain. Does.
2) Explain the Etiology of the renal cancer.
- exact cause is unknown,
- cigarette smoking,
- Obesity,
- High blood pressure,
- long term dialysis,
- occupational exposure to toxic agents,
- certain Analgesic,
- childhood chemotherapy,
- previous radiation therapy.
3) Explain the clinical manifestation of the renal cancer (tell the symptoms and signs of renal cancer.
- Abnormal urine color like :=dark ,rusty, brown.
- back pain,
- hydronephrosis (accumulation of fluid in the kidney),
- Abdominal mass or lump,
- Fever,
- Hypertension,
- malaise,
- weight loss,
- anorexia,
- cold intolerance (inability to tolerate cold),
- chronic fatigue (extreme tiredness),
- leg and ankle swelling (swelling in the legs and ankles),
- profuse sweating at night,
- Difficulty seeing,
- High calcium levels in the body (hypercalcemia).
4) Explain the Diagnostic evaluation of the renal cancer Explain the diagnostic evaluation of renal cancer.
- History taking and physical examination,
- intra venous urography,
- Cytological examination,
- Renal angiogram,
- ultra sonography,
- ct scan.
5) Explain the Management of the renal cancer Explain the management of renal cancer.
- Radiation therapy,
- chemotherapy,
- Hormonal therapy,
surgery, :=
->Nephrectomy
•simple Nephrectomy:= In this only the tumor is removed.
•partial Nephrectomy:= In this, the tumor and some surrounding area are removed.
•Radical Nephrectomy:= In this, the kidney, tumor, adrenal gland, lymph node and surrounding tissue are removed.
6) Explain the Nursing management of the renal cancer Explain the Nursing management of the renal cancer
preoperative and*post operative Nursing management:=
pre operative Nursing management:=
- Provide psychological support to the patient.
- Explain the procedure to the patient and his/her relative.
- Check the patient’s intake output.
- Provide intravenous fluid to the patient.
- Provide blood transfusion to the patient.
- Provide oxygen to the patient.
- Shave the patient on the operative area.
- Provide a comfortable and working environment for the patient and his/her relatives.
Post operative Nursing management :=
- Keep the patient under close observation after the operation.
- Check the patient’s vital signs every 15 minutes.
- Check the patient’s blood pressure every 15 minutes.
- Provide oxygen to the patient if necessary To do.
- Provide intra venous fluid.
- Maintain the nutritional and hydration status of the patient.
- Provide psychological support to the patient and his family members.
- Provide proper antibiotic and analgesia medicine to the patient.
- Properly dress the patient’s operation area.
- To clear all the doubts of the patient and his family members.
1) Explain the BLADDER CANCER Explain the bladder cancer.
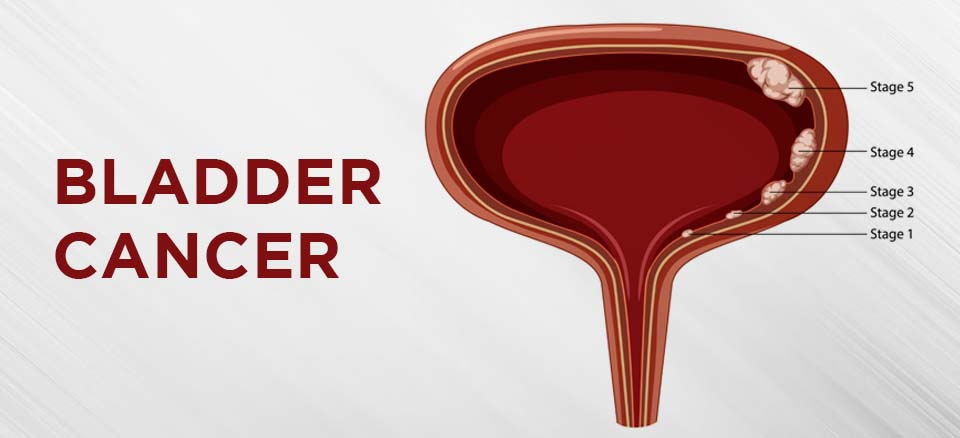
In Bladder Cancer of the Bladder Abnormal and uncontrolled growth of epithelial cells occurs and forms a tumor. These tumors can be benign and malignant.
Bladder cancer accounts for 90% of all cancers of the urinary system.
The types of cancer in the urinary system are classified according to the cells they contain.
- urethelial carcinoma (in urethral carcinoma),
- squamous cell carcinoma,
- Adenocarcinoma (Adenocarcinoma).
2) Explain the Etiology of the bladder cancer Explain the causes of bladder cancer.
- Age := Mainly seen between the ages of 50 and 70.
- sex := Affects men more than women. ( 3 : 1),
- cigarette smoking,
- chemical exposure,
- Diet := more common in people who eat fried meat and animal fats.
- Race := White people are more likely to get bladder cancer.
- person history of bladder cancer,
- family history of bladder cancer,
- chronic bladder inflammation,
- Birth defects,
- External beam radiation.
- Treatment of certain drugs.
3) Explain the clinical manifestation of the bladder cancer Describe the symptoms and signs of bladder cancer.
- blood in urine (hematuria := blood in urine),
- pain during urination,
- frequent urination,
- pelvic pain,
- back pain,
- alteration in voiding .
4) Explain the diagnostic evaluation of the bladder cancer. Explain the diagnostic evaluation of bladder cancer.
- history taking and physical examination
- cytoscopy,
- excretory urography,
- ct scan,
- ultrasonography,
- Biannual examination,
- Tumor Biopsy,
- Cytological examination
5) Explain the medical management of the bladder cancer. State the medical management of bladder cancer.
- Radiation therapy,
- chemotherapy,
- Immunotherapy.
surgery:
- • cystectomy, (removing the bladder)
- • partial cystectomy, (in this, only the affected portion of the bladder is removed).
- • Radical cystectomy. (in this operation, the entire bladder, along with its surrounding lymph nodes and surrounding tissue structures, is removed).
pre operative and post operative nursing management:
- In this pre-operative and post-operative management, the patient’s urine output should be checked every hour.
- Properly hospitalize the patient and keep him under close observation of the nurse and transportation personnel.
- If the patient and any complication arise, immediately inform the health care personnel.
pre operative nursing management:=
- Check the patient’s urine output.
- Insert a catheter into the patient.
- Properly explain the surgery and its complications, benefits and side effects to the patient.
- Vitality of the patient To check the sign.
- Prepare the patient for surgery.
- Obtain consent for surgery from the patient’s family members.
- Remove all the patient’s clothes and jewelry.
- Properly shave the area of the patient’s body where the operation is to be performed.
- Provide psychological support to the patient and his family members. Apply.
- Provide Indra Venus Fluid to the patient.
- Paint the patient’s body area with proper Savlon and Spirit.
post operative nursing management:=
- Keep the patient under close observation after the operation Keep.
- Check the patient’s vital signs every 15 minutes.
- Keep blood transfusion ready for the patient.
- Provide the patient with intravenous fluid.
- Properly dress the patient’s operative area.
- Provide the patient with proper antibiotic and analgesic medicine.
- Maintain aseptic technique while handling the patient.
- Clear all doubts of the patient and his family members.
- Tell the patient not to do hard activities.
- Tell the patient not to eat very spicy and fatty foods.
- Maintain the patient’s intake output chart.
- Ask the patient to maintain personal hygiene.
- Get all the blood investigations done on the patient.
- Provide psychological support to the patient and his family members.
1) Explain/ Define the uremia. Define uremia.

- Uremia is a type of medical condition in which there is an excess of urea and toxic waste in the blood due to kidney failure or inadequate function. Waste material accumulates and due to this the condition of uremia arises.
2) Explain the Etiology/ cause of the uremia. Give the causes of uremia.
- Chronic kidney disease,
- Acute kidney injury.
- Glomerulonephritis.
- Diabetes.
- Hypertension.
- Polycystic kidney disease.
- Caused by autoimmune disorder.
- Caused by obstruction.
3) Explain the Clinical manifestation/ sign and symptoms of the patient with the uremia. Explain the symptoms and signs of the patient with the uremia.
- Fatigue.
- Swelling.
- Changes in urination.
- Nausea and vomiting.
- Loss of appetite.
- Itching.
- Neurological symptoms.
- Hypertension.
- Anemia.
- Bone and joint pain.
- Cardiovascular complications.
4) Explain the Diagnostic evaluation of the patient with the uremia. Explain the diagnostic evaluation of the patient with the uremia.
- History taking and physical examination.
- Blood test.
- Assess calcium level.
- Assess the phosphorus level.
- Assess the glomerular filtration rate (GFR).
- Assess the blood urea nitrogen level.
- Assess the creatinine level.
- Assess the calcium, potassium, and phosphorus level.
- Urine test.
- Radioisotope test.
- Assess complete blood count test.
- Urine analysis.
- Imaging test.
- Ultrasound.
- CT scan.
- MRI.
- Renal biopsy.
- Medical imaging test.
5) Explain the management of the patient with the uremia. Explain the management of the patient with uremia.
- Treat the condition that caused the uremia.
- Assess the patient’s fluid intake so that fluid intake can be prevented.
- Assess the patient’s electrolyte level.
- Dialyze the patient properly.
- Provide proper medication to the patient.
- Provide phosphate binder medicine to the patient to control hyperphosphatemia.
- Provide erythropoietin stimulating agent to the patient to treat the condition of anemia.
- Provide vitamin D analog medicine to the patient.
- Provide antihypertensive medicine to the patient.
- Advise the patient to consume nutritious food.
- Monitor the nutritional status of the patient properly.
- Provide erythropoietin therapy to the patient to treat the condition of anemia and improve the production of red blood cells.
- Treat the patient for any other complications.
- Monitor the patient’s renal function and electrolyte levels properly.
- Prepare the patient’s treatment plan properly.
- Provide education to the patient about medication and lifestyle modification.
- Provide the patient with complete information about his disease condition, its causes, its symptoms and signs, and its treatment.
- Provide education to the patient about renal transplantation.
6) Explain the Nursing management of patients with the uremia. Explain the nursing management of patients with uremia.
- Provide comprehensive care and support to the patient.
- Properly assess the patient.
- Properly assess the patient’s vital signs.
- Properly assess the patient’s fluid levels.
- Properly assess the patient’s neurological status.
- Properly assess the patient’s laboratory values.
- Properly assess the patient’s blood urea nitrogen (BUN) level, electrolyte levels, and complete blood count (CBC).
- Properly assess the patient’s fluid and electrolyte levels.
- Properly monitor the patient’s intake output chart.
- Collaborate with other health care team members for the patient’s treatment.
- Provide complete information about dialysis to the patient.
- Properly assess the patient’s vascular access for signs and symptoms of infection.
- Provide the prescribed medication to the patient.
- Provide proper nutritional support to the patient.
- Properly treat the patient for any other signs and symptoms.
- Provide proper emotional support to the patient.
- Provide complete information to the patient about his disease condition, its causes, its symptoms and signs and its treatment.
- Provide proper care to the patient if he is undergoing dialysis.
- Provide proper psychological support to the patient.
- Collaborate with other health care personnel for proper care of the patient.
- Provide proper psychological support to the patient.
- Advise the patient to take proper follow-up.
1) Explain the care of patient with the KIDNEY transplantation. (Kidney transplantation patient care).
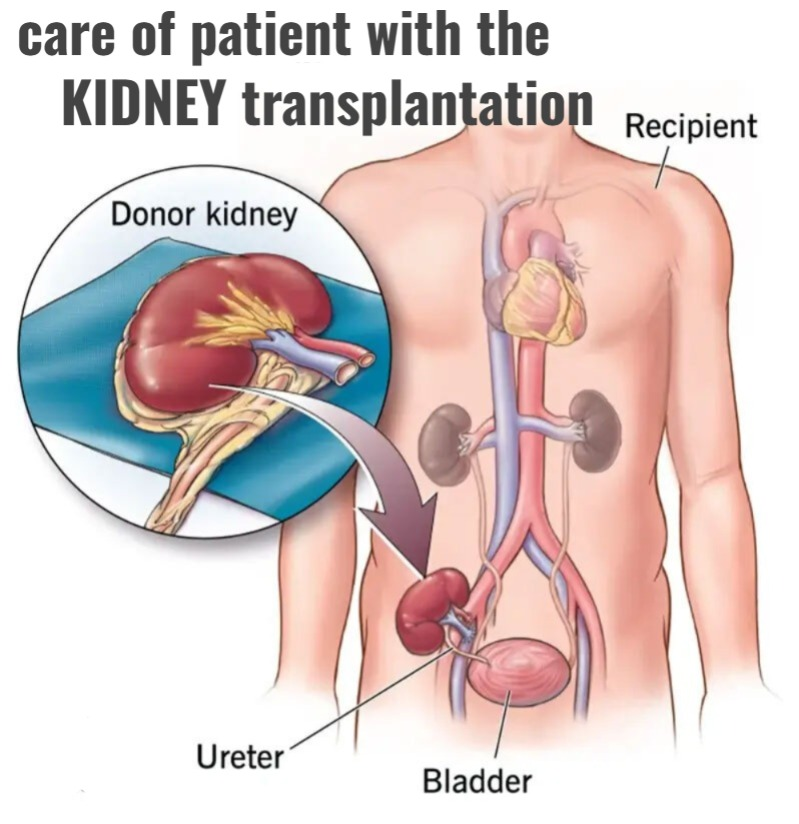
- Kidney transplantation is a surgical procedure and a permanent medical procedure.
- In kidney transplantation, a kidney is obtained from a living or dead person and then transplanted into a person whose kidneys cannot function properly or who has end stage renal disease, which is called kidney transplantation.
2) Explain the Etiology/ cause of KIDNEY transplantation. Explain the reason for kidney transplantation.
- Due to chronic kidney disease.
- Due to any type of genetic disease.
- Due to polycystic kidney disease.
- Due to any type of autoimmune disease.
- Due to malignant hypertension.
- Due to any type of infection.
- Due to diabetes mellitus.
- Due to the condition of glomerulonephritis.
3) Explain the source of KIDNEY transplantation. State the source of kidney transplantation.
1) Living Related Donor
- In a living related donor, the very close relatives such as parents, siblings, children, grandparents or those who are close relatives can donate a kidney. This is called a living related donor.
- This is mainly because in normal A person has two kidneys and if both of them are working properly, then any person can survive life properly on one of his kidneys, so he can donate one kidney. Donating this one kidney does not change the physical capacity and lifestyle of that person and he can survive properly on one kidney too.
2) Cadever Donors (Cadever Donors)
- Cadever donors are those people who have died due to any kidney related reason. If the person is brain dead due to any kind of accident or stroke and the kidney is obtained from such a person, it is known as a cadaver donor.
3) Emotionally Related recipient donor
- In situations where a cadaver donor is not possible and a living related donor is unfit, any emotionally related donor such as husband/wife, cousin, uncle , Aunty-in-law, etc. can donate a kidney which is known as an emotionally related kidney donor.
4) Unrelated kidney Donors (Unrelated kidney donor)
- When cadaver donor, living related donor and emotionally related donor are impossible, then the kidney is obtained from unrelated kidney donors which is called unrelated kidney donor but there is a risk of rejection in unrelated kidney donors. The chances are high, so costly medication such as cyclosporine is provided.
4) Explain the types of kidney transplantation.
There are 3 types of kidney transplantation.
1) Diseased donor kidney transplantation ( Diseased donor kidney transplantation) Donor Kidney Transplantation)
- If a person who has died recently and the kidney of that person is taken and transplanted into the recipient, it is called a diseased donor kidney transplant.
2) Living donor kidney transplantation (Living donor kidney transplantation)
- The person who is a relative If both their kidneys are functioning properly and that person donates one kidney and provides it to the recipient, it is called a living donor kidney transplant.
3) Primitive kidney transplantation
- Primitive kidney transplantation is mainly done in developed countries.
- In this type of kidney transplantation, if the patient’s kidneys are functioning to a lesser extent or has any type of chronic kidney disease and that person already undergoes kidney transplantation, it is called primitive kidney transplantation.
5) Explain the donor recipient match for the kidney transplantation. Describe donor-recipient match for kidney transplantation.
1) Blood group:=
- The blood group of both the person who is the donor and the recipient should match.
2) HLA (Human leukocytes Antigen)
- These are the types of antigens that are present on the surface of white blood cells. Every person has six human leukocyte antigens (HLA) present, three from the father and three from the mother, thus a person has a total of six types of human leukocyte antigens.
- For kidney transplantation, these antigens should match as much as possible between the donor and the recipient, only then kidney transplantation becomes accessible.
3) Negative cross match
- In this, the blood of the donor and the recipient are mixed in a test tube and if no reaction is seen between the two bloods, then the kidney transplantation is done properly.
6) Explain the Risk or complications of the kidney transplantation. Explain the risks and complications of kidney transplantation.
- Bleeding.
- Post-operative infection.
- Trauma and injury.
- Organ rejection.
7) Explain the important facts of kidney transplantation. Tell the important facts of kidney transplantation.
- Kidney transplantation takes about four hours.
- In kidney transplantation, the patient is discharged from the hospital within 1 week.
- If the kidney is taken from a living donor, then it functions quickly.
- If the kidney is taken from a deceased person, then it takes a little more time to work. Is.
- After kidney transplantation, the kidney is removed only if it causes infection in the body, otherwise it is not removed.
8) information about kidney:=
- The first successful kidney transplantation was performed on 23 December 1954 by Dr. Joseph E. Murrey and his colleagues. It was performed between two identical twins (Merrick brothers) at Peter Bent Brigham Hospital, which is present in the US (Boston).
9) Explain the nursing management of patients with renal transplantation. Explain the nursing management of a patient undergoing renal transplantation.
pre operative management:=
- Take a complete history of the patient and perform a physical examination.
- Provide immunosuppressive medicine to the patient before kidney transplantation.
- Provide antibiotic medicine to the patient.
- Provide antiemetic medicine to the patient.
- Provide psychological support to the patient. To do.
- To monitor the patient’s vital signs properly.
- To explain the procedure completely to the patient.
- To properly clear all the doubts of the patient.
post operative management:=
- Assess the patient for any signs and symptoms of kidney rejection.
- Provide proper aseptic technique to prevent infection.
- Properly monitor the patient’s vital signs.
- Assess the patient for any other complications.
- Monitor the patient’s intake output.
- Monitor the patient’s renal function.
- Monitor the patient’s blood urea nitrogen level.
- Assess the patient’s serum creatinine level.
- Provide the patient with a semi-Fowler’s position.
- Advise the patient to maintain good hygienic conditions.
- Advise the patient to take proper care of the wound.
- Provide proper psychological support to the patient.
- Provide proper medication to the patient.
- Advise the patient to take proper follow-up.
- Advise the patient to report any complications to the health care personnel immediately if any. giving.
Disorder of the male genitourinary track :
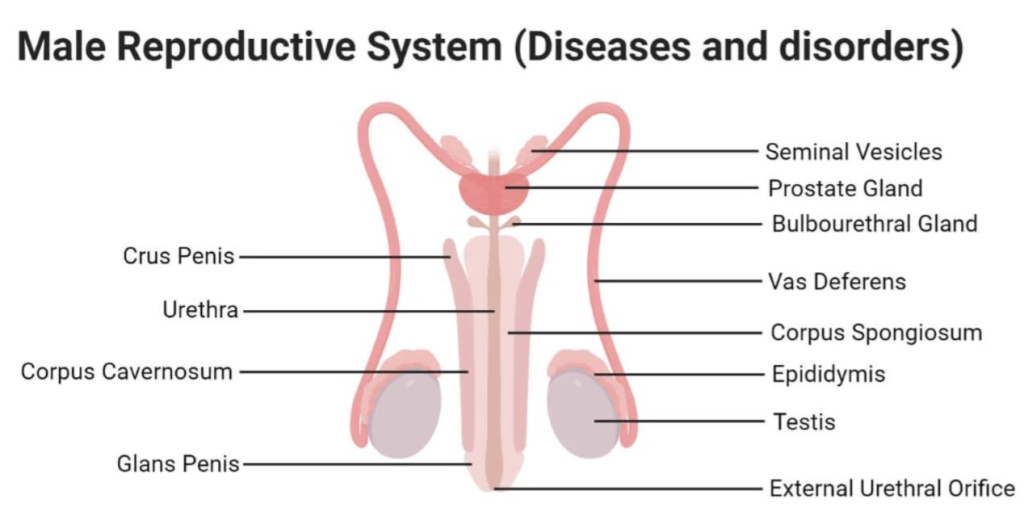
1) Explain/ Define the Hydrocele.
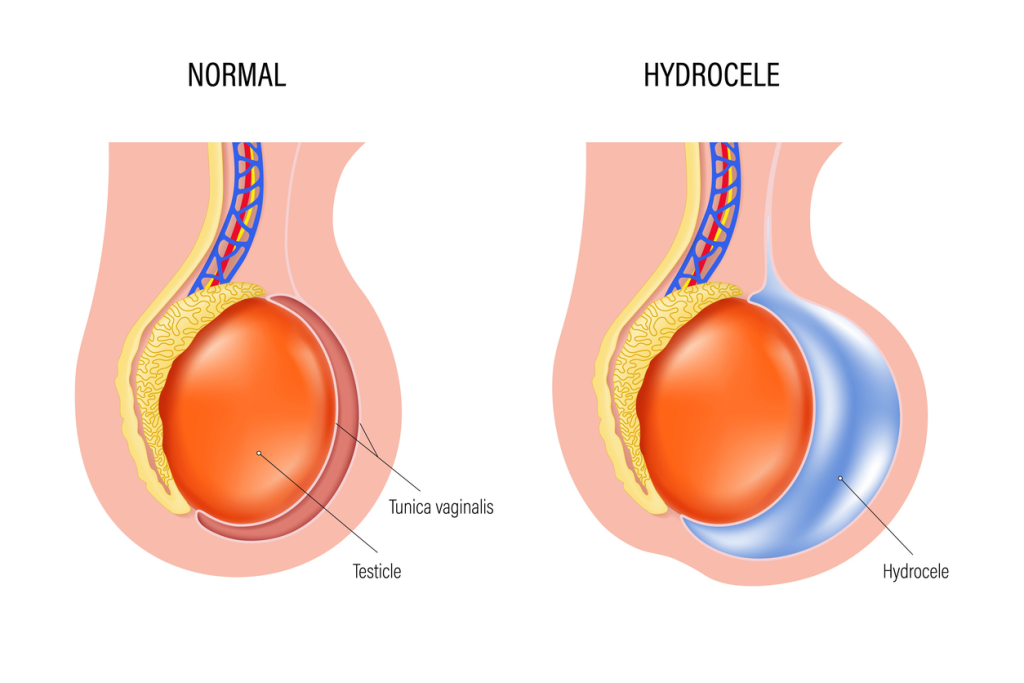
- Hydrocele is a condition in which fluid collects around the testicles, causing swelling in the scrotum and groin area. This fluid collection is called hydrocele.
- The condition of hydrocele arises when the fluid around the testicles is naturally absorbed into the body. When this absorption does not occur, the fluid builds up around the testicles and the condition of hydrocele arises.
2) Explain the Etiology/ cause of the Hydrocele. Give the reasons for hydrocele.
- Excect cause is unknown.
- This is mainly due to any kind of injury in the scrotum and surgery in the groin area.
- Due to infection.
- Due to inflammation.
- Testicular cancer Due to.
- Any type of injury and trauma.
3) Explain the Clinical manifestation/ sign and symptoms of the patient with the Hydrocele. Describe the symptoms and signs of a patient with hydrocele.
- Swelling in the scrotum.
- Heaviness and discomfort.
- Pain.
- Redness in the scrotum.
- Tenderness.
- Difficulty in palpating the testicles.
- Enlargement of the scrotum.
- Filling of fullness.
- Overnight size reduction of the testicles.
4) Explain the Diagnostic evaluation of the Hydrocele. Write an evaluation.
- history taking and physical examination.
- Transillumination test.
- Ultrasound of scrotum.
- Blood test.
- Laboratory investigation.
5) Explain the medical management of the patient with the Hydrocele. Explain the medical management of the patient with the Hydrocele.
Fine Needle Aspiration.
- In this procedure, the fluid accumulated around the testicles is aspirated.
Sclerotherapy
- In this procedure, after aspirating the fluid around the testicles, a scarring agent is inserted around the testicles to prevent fluid buildup.
- Surgery is performed if the hydrocele is causing discomfort.
Anti-inflammatory medication
- Provide the patient with non-steroidal anti-inflammatory drugs to reduce the inflammation and discomfort caused by the hydrocele.
6) Explain the Nursing management of patients with the Hydrocele.
- Proper assessment of the patient To do.
- Assess the patient’s pain level.
- Provide analgesic medicine to reduce the patient’s pain.
- Provide mind diversional therapy to reduce the patient’s discomfort.
- Advise on aseptic wound care techniques if the patient has had surgery or fluid aspirated.
- Collaborate with other health care personnel for proper care of the patient.
- Advise the patient to take medication properly.
- Advise the patient to avoid riding a bike for at least three weeks.
- Advise the patient to avoid strenuous activity.
- To prevent the patient from infection Advise the patient to maintain hygienic conditions.
- Advise the patient to apply ice packs if there is scrotal pain.
- Advise the patient to follow up properly.
1) Explain/ Define the Phimosis. Define phimosis.
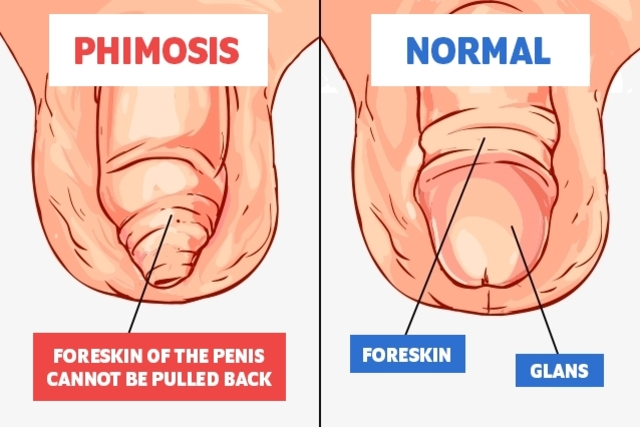
- Phimosis is a condition in which the foreskin over the penis tightens and does not retract properly. retract) and it becomes tight on the gland penis. This condition is called phimosis.
- This condition is mainly congenital but it can also be seen due to any infection.
- Phimosis is a disease condition that causes pain and discomfort during urination and sexual activity.
2) Explain the Etiology/ cause of the Phimosis. Give the reasons for phimosis.
- Due to congenital deformity.
- Due to any infection and inflammation.
- Due to trauma and injury.
- Due to some type of medical condition.
- Balanitis xerotica obliterans (this is a type of chronic and is a progressive condition in which infection, inflammation and scarring are seen in the foreskin over the glans penis.
- Repeated foreskin infection.
- Due to improper hygienic conditions.
- Due to catheterization.
3) Explain the Clinical manifestation/ sign and symptoms of the Phimosis. Explain the symptoms and signs of Phimosis.
- Swelling.
- Redness.
- Tenderness.
- Purulent discharge.
- Tight foreskin.
- Pain and discomfort.
- Inflammation.
- Recurrent infection.
4) Explain the Diagnostic evaluation of the patient with the Phimosis. Explain the diagnostic evaluation of a patient with phimosis.
- history taking and physical examination.
- Urine analysis.
- Blood analysis.
- Swab culture.
- Biopsy.
5) Explain the medical management of the patient with the Phimosis. Explain the medical management of the patient with Phimosis.
- Provide topical corticosteroid application cream to reduce the patient’s inflammation.
- Advise the patient to do gentle foreskin stretching.
- Provide the patient with topical antifungal cream.
- Provide the patient with topical antibiotic cream.
- Advise the patient to maintain proper hygienic conditions.
- Advise the patient to have regular follow-up.
- Advise the patient to take medication properly.
6) Explain the Nursing management of patients with the Phimosis. Explain the nursing management of patients with the Phimosis.
- Provide proper medication to the patient.
- Advise the patient to maintain proper hygienic conditions.
- Properly apply topical medication to the patient. Give advice.
- Advise the patient to follow up regularly.
- Provide analgesic medicine if the patient is in pain.
- Provide mind diversional therapy if the patient is uncomfortable.
- Provide proper emotional support to the patient.
- Patient’s Communicate properly with other health care personnel for proper care.
- Provide complete information to the patient about his disease, its causes, its symptoms and signs, and its treatment.
- Provide proper psychological support to the patient and his family members.
1) Define/ Explain prostate cancer Define prostate cancer.
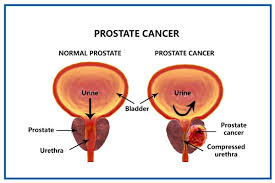
- Prostate cancer occurs in the prostate gland.
- Prostate cancer is caused by abnormal and uncontrolled growth of prostate cells in the prostate gland, which leads to the formation of tumors, which can become cancerous and cause cancer.
- Prostate cancer can also spread to surrounding tissue. And this cancer can spread to all parts of the body like liver bone lungs etc.
2) Explain the Etiology/ cause of the prostate cancer Explain the cause of prostate cancer.
- advance age
- hereditary,
- Hormonal influence,
- Environment Factor,
- cigarette smoking,
- toxins, chemicals.
- industrial products.
- diet high in saturated fat,
- increase age
3) Explain the clinical manifestation/ sign and symptoms of the prostate cancer Explain the symptoms and signs of prostate cancer.
- burning or pain during urination,
- inability to urinate,
- a sensation of incomplete emptying of the bladder even after passing urination,
- Frequent nocturnal urination.
- weak or interrupted flow of urine,
- blood in urine,
- blood in semen, (hematospermia),
- Pelvic pain,
- back or hip pain,
- abdominal pain,
- chest pain,
- weight loss.
4) Explain the Diagnostic evaluation of the prostate cancer. Explain the diagnostic evolution of prostate cancer.
- History taking and physical examination
- Biopsy,
- blood test,
- urine test,
- X Ray,
- ct scan,
- MRI
5) Explain the management of the management of the prostate cancer.
- Radiation therapy,
- chemotherapy,
- biotherapy,
- gene therapy,
- immuno therapy,
- Hormonal therapy,
- cryotherapy
6) Explain the nursing management of the prostate cancer Explain the nursing management of prostate cancer.
assessment
- Perform a head to toe examination of the patient.
- Check the patient’s vital signs.
- Maintain the patient’s intake output chart.
- Assess the patient’s pain level.
- Assess the patient’s skin integrity.
- Assess the patient’s bowel and bladder habits.
- Maintain the patient’s oral hygiene.
- Check if the patient has hair loss or any side effects due to chemotherapy and radiation therapy.
Nursing diagnosis
1)pain related to disease condition
Nursing interventions:=
Reliving pain level:=
- Assess the patient’s pain level.
- Give the patient a comfortable position.
- Give the patient mind diversionary therapy Provide.
- Provide the patient with his/her prescribed medications.
- Provide the patient with a comfortable and functional environment.
2) self care deficit related to disease condition.
Nursing interventions
provide hygiene conditions to the patient
- Provide clean clothes and bedsheets to the patient.
- Provide bed bath and sponge bath to the patient.
- Provide clean and wrinkle-free bedsheets to the patient.
- Maintain oral care for the patient.
- Instruct the patient to wash their hands properly.
3)Impaired skin integrity related to cancerous condition .
Nursing interventions:=
mainten skin integrity.
- Assess the patient’s skin integrity.
- Check the patient’s skin turgor.
- Check the patient for any bleeding from the body.
- Ask the patient to drink two to three liters of water.
- Ask the patient to apply lotion to the body.
- Tell the patient not to rub or scratch the skin.
- Tell the patient to wear cotton clothes.
- Do not let the patient wear tight clothes.
4)Impaired nutrition status of patient less than body requirement related to diarrhea and vomiting.
Nursing interventions:=
improve nutritional status:=
- Assess the nutritional status of the patient.
- Provide a comfortable environment for the patient.
- Instruct the patient to wash their hands before eating.
- Provide the patient with an appetizer.
- Remove any items in bad order around the patient while he is eating.
- Keep the patient’s likes and dislikes in mind.
- Feed the patient at regular intervals.
- Feed the patient only what he likes to eat.
- While the patient is eating, Keep the environment very clean.
5) Disturbed body image ( hair loss) related to radiotherapy and chemotherapy .
Nursing interventions:=
improve body image*of patient:
- Good interpersonal relationship with the patient To maintain.
- Maintain a good rapport with the patient.
- Tell the patient that hair loss is temporary.
- Tell the patient that hair loss is normal when undergoing chemotherapy and radiation therapy.
- Provide psychological support to the patient.
6) Activity intolerance related to the weakness.
Nursing interventions:=
Improve the activities of the client.
- Assess the patient’s activity level.
- Maintain a good interpersonal relationship with the patient.
- Tell the patient to do daily routine activities in small amounts.
- Tell the patient to take some rest between activities.
- Tell the patient to do proper exercise and yoga.
7) High risk of infection related to hospitalizations.
Nursing interventions
Reduce the risk of infection:=
- To assess the infection side of the patient.
- Handling the patient Maintain aseptic technique while dressing the patient’s body parts.
- Maintain aseptic technique while dressing the patient’s body parts.
- Provide proper clean and hygienic conditions to the patient.
- Give the patient a clean cloth to wear.
- Give the patient a high protein rich food that helps the patient fight infection.
- Provide proper antibiotic medicine to the patient.
8)depression and fear related to treatment of cancer .
Nursing interventions:=
Reduce the fear level of client.
- Check the patient’s anxiety and fear level To do.
- Maintain a good interpersonal relationship with the patient.
- Help the patient to solve his doubts and problems.
- Listen to the patient and his family members in a proper manner.
- Answer all the patient’s questions.
- Provide psychological support to the patient. To do.
- Provide coping skills on how the patient can cope with such a bad situation.
1)Explain/Define the orchitis. Define orchitis.
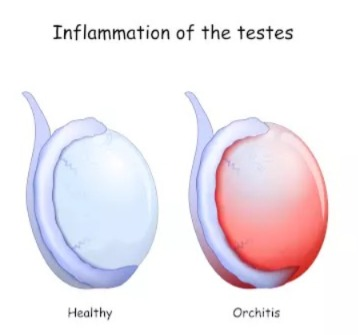
- Orchitis is an inflammation of the testicles in the male reproductive system caused by infection.
- In the condition of orchitis, inflammation occurs due to infection in one or both testicles.
- ( orchitis := infection or inflammation of the one or both testicles it’s called as a orchitis. )
2) Explain the Etiology/ cause of the orchitis. Give the causes of orchitis.
- Due to bacterial infection.
- Due to viral infection.
- Due to trauma.
- Due to autoimmune conditions.
- Due to urinary tract infection.
- Due to autoimmune disease.
- Due to recurrent urinary tract infection.
- Due to insertion of a follicular catheter.
- Due to a weakened immune system.
3) Explain the Clinical manifestation/ sign and symptoms of the orchitis. Explain the clinical manifestations/ signs and symptoms of the orchitis.
- Testicular pain.
- Testicular swelling.
- Tenderness.
- Nausea.
- Fever.
- Discharge from the penis.
- Blood in the semen.
- Passing blood in the urine (hematuria).
- Pain in the groin area.
- Pain during urination.
- Inflammation of the epididymis.
- Swelling in the inguinal lymph nodes.
- Swelling at the affected site.
4) Explain the Diagnostic evaluation of the orchitis. Explain the diagnostic evaluation of orchitis.
- History taking and physical examination.
- Complete blood count.
- Testicular ultrasound.
- Sexually transmitted disease screening.
- Urine analysis.
- Nuclear scan of the testicles.
- Blood test.
- Imaging test.
5) Explain the medical management of the patient with orchitis. Explain the medical management of the patient with orchitis.
- If the patient’s condition of orchitis is caused by bacteria, then provide antibiotic medicine to the patient.
- Provide antiviral medication to the patient.
- If the patient has a condition of pain, then provide analgesic medicine.
- If the patient is uncomfortable, then apply ice.
- Advise the patient to take adequate rest.
- Provide supportive care to the patient.
- Advise the patient to take proper follow-up.
6) Explain the Nursing management of patients with the orchitis. Explain the nursing management of the patient with orchitis.
- If the patient is in pain, then provide analgesic medicine.
- Provide proper comfort measures to the patient.
- Advise the patient to take proper fluids to maintain hydration status.
- Advise the patient to take proper rest.
- Provide education to the patient to make modifications in his daily routine activities.
- Monitor the patient for any other complications.
- Provide proper emotional support to the patient.
- Advise the patient to maintain proper hygienic conditions to prevent infection.
- Collaborate with other health care personnel for proper care of the patient.
- Provide proper psychological support to the patient.
- Provide the patient with complete information about his disease, its causes, its symptoms and signs, and its treatment.
1) Explain/ Define the Epididymitis. Define Epididymitis.
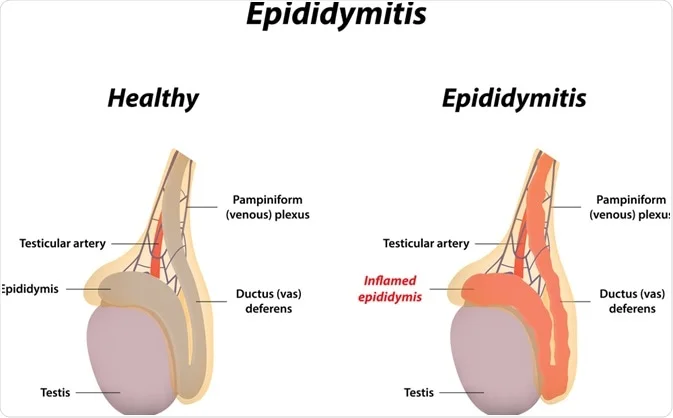
- Epididymitis: The epididymis is a coiled tube that lies above and behind the testicles and plays an important role in storing and transporting sperm.
- Infection and inflammation of the epididymis is called epididymitis.
- The condition of epididymitis is mainly seen due to any infection and inflammation due to which redness, warmth, swelling is seen in the scrotum (sac containing testicles).
- If the condition of epididymitis (inflammation) spreads to the testicles, then it is called epididymo-orchitis.
2) Explain the Etiology/ cause of the Epididymitis.
- Due to bacterial infection.
- Due to sexually transmitted infection.
- Due to urinary tract infection.
- Due to trauma.
- Due to urinary reflux.
- Epididymitis is mainly seen in young men (men between 19- 35 years).
- Due to Mycobacterium tuberculosis.
- Due to any structural problem in the urinary tract.
- Due to catheterization.
- Due to multiple sex partners.
- Due to enlargement of the prostate.
3) Explain the Clinical manifestation/ sign and symptoms of the patient with the Epididymitis. Explain the clinical manifestation/ sign and symptoms of the patient with Epididymitis.
- Groin pain.
- Swelling.
- Redness and warmth.
- Fever.
- Urethral discharge.
- Pain during urination.
- Lump and mass like structure.
- Blood in semen.
- Discharge from urethra.
- Discomfort in lower abdomen and pelvis.
- Frequent urination.
- Pain during ejaculation.
- Pain and burning sensation during urination.
- Tenderness in affected side.
4) Explain the diagnostic evaluation of the patient with the Epididymitis. Explain the diagnostic evaluation of the patient with Epididymitis.
- History taking and physical examination.
- Laboratory tests.
- Ultrasound.
- Blood tests.
- Sexually transmitted infection screening.
- Complete blood count test.
- Testicular scan.
- Urinalysis .
- Urine culture.
5) Explain the management of the patient with the Epididymitis. Explain the management of the patient with the Epididymitis.
- If the patient has an infection caused by bacteria, provide antibiotic medicine.
- If the patient is in pain, provide analgesic medicine.
- Advise the patient to take proper bed rest.
- Elevation of the scrotum to reduce swelling and discomfort.
- Advise the patient to take proper water intake. So that the patient’s hydration status can be properly maintained.
- Apply ice to reduce the patient’s pain.
- If the patient has severe inflammation, provide non-steroidal anti-inflammatory drugs (NSAIDs).
- Regularly screen any sexual partners who may have an infection.
- Advise the patient to have regular follow-up.
6) Explain the Nursing management of patients with the Epididymitis. Explain the nursing management of the patient with epididymitis.
- Properly assess the patient.
- Properly monitor the patient’s vital signs.
- Properly provide comfort measures to manage the patient’s pain.
- Properly provide education to the patient.
- Advise the patient to consume fluids to maintain proper hydration status.
- Provide proper emotional support to the patient.
- Provide antibiotic medicine if the patient has an infection.
- Collaborate with other health care personnel for proper care of the patient.
- Advise the patient to adopt safe sexual activity.
- Advise the patient to have regular follow-up.
1) Explain/ define the penile cancer. Define penile cancer.
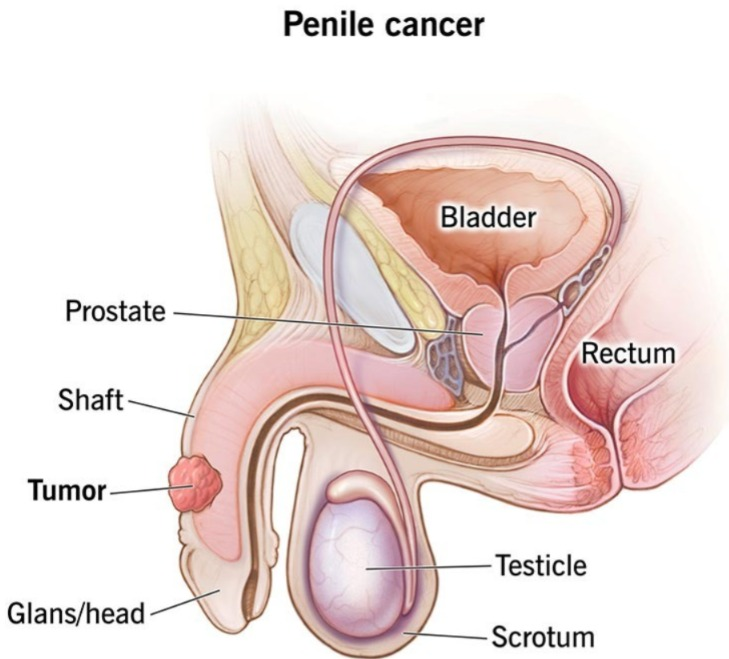
- Penile cancer is a rare type of cancer that mainly arises in the male reproductive organ penis.
- In penile cancer, there is abnormal and uncontrolled growth of cells in the penis and formation of malignant cells and it results in cancer.
- Penile cancer is more common in men after the age of 50.
- If penile cancer is not detected and treated early, it can spread to other parts of the body.
2) Explain the types of penile cancer. Explain the types of penile cancer.
There are a total of four types of penile cancer.
- 1) Epidermoid/ squamous cell carcinoma,
- 2) Basal cell penile cancer,
- 3) Melanoma,
- 4) Sarcoma,
•••>
1) Epidermoid/ squamous cell carcinoma (in epidermoid or squamous cell carcinoma),
- 95% of pineal cancers are epidermoid or squamous cell carcinoma.
- Squamous cell carcinoma develops primarily within the foreskin.
2) Basal cell penile cancer,
- If the cancer in the penis arises mainly from basal cells, it is called basal cell carcinoma.
- Less than 2% of cancers are basal cell carcinomas.
3) Melanoma,
- Melino cancer arises primarily from melanocytes, the cells responsible for skin color.
4) Sarcoma
- 1% of penile cancers are sarcomas.
- Sarcomas are cancers that arise primarily in tissues that support and connect the body, such as blood vessels, smooth vessels, and fat.
2 ) Explain the Etiology/ cause of the penile cancer. Give the causes of penile cancer.
- Due to human papilloma virus ( HPV ).
- Due to smoking.
- Age related.
- Phimosis (tightening of the foreskin).
- Due to chronic inflammation.
- Due to poor hygienic conditions.
- Due to infection with human immunodeficiency virus (HIV).
4) Explain the Clinical manifestation/ sign and symptoms of the patient with the penile cancer..
- Changes in the skin of the penis.
- Feeling of lumps and mass-like structures.
- Formation of ulcers and sores.
- Changes in the shape and size of the penis.
- Discharge from the penis.
- Pain.
- Swelling of the penis.
- Genital lesions on the penis.
- Changes in the color of the penis.
- Thickening of the skin of the penis.
- Foul-odor discharge from the foreskin of the penis.
- Blood coming out of the tip of the foreskin of the penis.
- Irregular or growing bluish brown flat lesions.
- Swollen lymph nodes in the groin.
5) Explain the diagnostic evaluation of the penile cancer. Explain the diagnostic evolution of penile cancer.
- history tacking and physical examination.
- biopsy.
- fine needle aspiration.
- sentinel lymph node biopsy.
- inguinal lymph node dissection.
- X-ray.
- Computed Tomography ( computed Tomography).
- Magnetic Resonance Imaging ( MRI).
- Positron Emission Tomography ( PET).
- Lymph Node Biopsy.
- Cytoscopy.
- Blood test.
- Human papilloma virus test ( HPV ).
6) Explain the stages of the penile cancer. State the stages of penile cancer.
stage :=0
- In stage zero, abnormal cells are mainly found on the surface of the skin of the penis.
- These abnormal cells mainly develop into cancer and spread to nearby tissues.
- Stage 0 is called This is called carcinoma in situ.
Stage :=1
- In Stage 1, the cancer has spread to nearby connective tissue and just under the skin of the penis.
stage:=2
- In stage 2, the cancer has spread from the connective tissue just under the skin of the penis to the lymph nodes on one side of the groin area.
stage:= 3
- In stage 3, the cancer is in the connective tissue, under the skin of the penis, from the lymph node on one side of the groin area to the lymph node on the other side of the groin area, i.e. in stage 3, more than one lymph node is involved.
stage := 4
- In stage four, the cancer has spread to the groin area, pelvis, and distant parts of the body.
7) Explain the management of penile cancer. (Explain the management of penile cancer.)
The management of penile cancer mainly depends on its spread and the size of the tumor.
1) Surgery :=
- Surgery is the most common treatment for penile cancer.
- The goal of surgery is to remove the cancer cells in the penile cancer. Cells and tissues are removed.
- Laser surgery.
- Cryosurgery.
- Lymphnode dissection.
- Radiation therapy.
- Chemotherapy.
- Biological therapy.
8) Explain the Nursing management of patients with the penile cancer. Explain the nursing management of patients with the penile cancer.
- Properly assess the patient with cancer.
- If surgery is to be performed, explain it properly to the patient.
- If the patient has undergone surgery, then provide him with postoperative care. Assess for any complications.
- Provide analgesic medicine if the patient is in pain.
- Provide relaxation techniques if the patient is uncomfortable.
- If the patient has any side effects of the treatment, immediately collaborate with the health care provider.
- Provide proper wound care and hygienic conditions to the patient.
- Provide proper psychological support to the patient.
- Provide complete information to the patient about his disease, its causes, its symptoms and signs, and its treatment.
- Provide psychological support to the patient to cope with his disease.
- Provide education to the patient to take a properly nutritious diet.
- Assess the patient for any other complications.
- Advise the patient to take proper medication.
- Advise the patient to take regular follow-up.
