ENGLISH-MEDICAL SURGICAL NURSING – 1 (12/09/2025) PAPER SOLUTION NO 14(UPLOAD)


Q-1
a) Define Cerebro Vascular Accident (CVA). Define CVA.03
Definition:
Cerebrovascular accident is also called stroke. Stroke is also often called brain attack. Cerebrovascular accident is a condition in which the brain cells, tissues and any particular brain part are not supplied with sufficient amount of oxygen due to insufficient amount of blood supply. Due to this, the brain cells, tissues and parts of the brain are not supplied with sufficient amount of oxygen. Therefore, the part of the brain cannot function properly and it is called brain damage. The body function performed by the part is also impaired.
1) Ischemic stroke:
This type of stroke occurs due to interruption of blood supply to the brain.
Thrombotic Stroke:
This type of stroke arises due to the formation of a blood clot in one or more blood vessels of the brain, a condition called thrombotic stroke.
Embolic Stroke:
In this stroke, a blood clot forms in any of the blood vessels of the body and that blood clot travels to the blood vessels of the brain and then the blood clot that has traveled gets stuck in the vessels of the brain, then embolic stroke occurs.
2) Heamorraagic Stroke:
Hemorrhagic stroke occurs when any cerebral vessel ruptures due to any reason, causing bleeding in the brain and due to this, the condition of hemorrhagic stroke arises.
b) Write down signs and symptoms of CVA. Write the signs and symptoms of CVA.04
1.Motor (Motor Related)
- Hemiplegia – Complete paralysis on one side of the body
- Hemiparesis – Weakness on one side of the body
- Facial paralysis (facial drooping) Face drooping on one side
- Difficulty in walking
- Loss of coordination
2. Speech and Language Problems
- Aphasia – Inability to speak
- Dysarthria – Difficulty in understanding speech
- Difficulty in understanding speech
3.Sensory Symptoms (Sensation Related)
- Loss of sensation on one side of body
- Numbness or tingling
- Pain on affected side
4.Visual Symptoms (Vision Related)
- Sudden loss of vision in one or both eyes
- Blurred vision
- Double vision (Diplopia)
- Visual field defect
5.Cognitive and Mental Changes
- Confusion
- Memory loss
- Difficulty in concentration
- Altered level of consciousness
6.Headache and Associated Symptoms
- Sudden severe headache
- Nausea and vomiting
- Dizziness
7.Balance and Coordination
- Loss of balance
- Ataxia
8.Swallowing and Autonomic Symptoms
- Dysphagia – difficulty in swallowing
- Drooling of saliva
- Loss of bladder and bowel control
9.Severe / Late Symptoms
- Loss of consciousness
- Coma
- Seizures
- Respiratory difficulty
FAST Warning Signs (Important for emergency)
- F – Face drooping → Face drooping
- A – Arm weakness → Arm weakness
- S – Speech difficulty → Speech difficulty
- T – Time → Get treatment immediately
c) Write down nursing management of CVA patient. Write the nursing management of a patient with CVA.05
1) Ineffective Cerebral tissues percussion related to interruption of blood supply.
2) Impaired physical mobility related to Neuromuscular Impairment.
3) Impaired Verbal communication related to loss of facial muscles tone.
4) knowledge deficit related to disease condition and treatment.
Nursing management:
- Assess the patient’s neurological status.
- Advise the patient to take proper rest.
- Properly provide oxygen to the patient.
- Properly monitor the patient’s vital signs.
- Frequently change the patient’s position.
- Keep the patient in a comfortable position.
- Keep the patient in a comfortable position.
- Advise the patient to speak slowly. Advise the patient to limit activity.
- Advise the patient to take medication properly.
- Maintain the patient’s hydration status properly.
- Maintain the patient’s nutritional status properly.
- Give the patient small amounts of fluids daily. Advise on routine activities.
- Provide analgesic medicine if the patient is in pain.
- Properly collaborate with other health care personnel for proper care of the patient.
- Provide occupational therapy, physical therapy, speech therapy to the patient.
- Advise the patient to avoid fatty foods.
- Advise the patient to avoid smoking and alcohol.
- Advise the patient to exercise regularly.
- Advise the patient to maintain their blood cholesterol level in the normal range.
- Assess the patient’s proper glass go-come scale.
- Advise the patient to exercise properly.
- Advise the patient to speak in small amounts.
- Advise the patient to reduce weight if he is obese.
- Advise the patient to take proper medication.
- Advise the patient to take proper follow-up.
OR
a) What is Pneumonia? What is Pneumonia? 03
Pneumonia is an infection and inflammation of the lung parenchyma (alveoli) caused by bacterial, viral or fungal infections. In which the air sacs fill with fluid or pus and become solid. Alveoli normally work to exchange gases but in the condition of pneumonia, due to infection and inflammation and accumulation of pus, gas exchange gets interfered with.
b) Write down types of pneumonia. Write down types of pneumonia.04
On the basis of etiological factors
- Bacterial pneumonia:
Pneumonia caused by bacterial infection is known as bacterial pneumonia. Pneumonia is caused by Streptococcus pneumoniae, Mycoplasma pneumoniae, and Haemophilus influenzae bacteria. - Viral pneumonia:
Pneumonia caused by viral infection is known as viral pneumonia. Viruses such as influenza, coronavirus, adenovirus and respiratory syncytial virus are responsible for causing pneumonia. - Fungal pneumonia:
Pneumonia caused by fungal infection is known as fungal pneumonia.
On the basis of anatomical structure:
Pneumonia is classified as follows on the basis of anatomical structure
- Lobar pneumonia:
In lobar pneumonia, infection is seen in one or more lobes of the lungs. - Broncho pneumonia:
In broncho pneumonia, infection is seen in multiple lobes as well as the bronchi. - Interstitial pneumonia:
In interstitial pneumonia, the interstitial tissue and alveolar septa become infected.
On the basis of broad classification:
- Community acquired pneumonia: Pneumonia that occurs in the community is called community acquired pneumonia.
- Hospital Acquired Pneumonia:
Pneumonia that occurs after 48 hours of hospitalization is called hospital acquired pneumonia. - Ventilator Associated Pneumonia:
Pneumonia that occurs due to endotracheal intubation or mechanical ventilation is called ventilator associated pneumonia. - Aspiration Pneumonia:
Endogenous or exogenous Pneumonia caused by aspirating substances is called aspiration pneumonia.
c) Write down management of pneumonia. Write the management of pneumonia.05
Management:
Antibiotics:
- Provide antibiotic drugs to treat bacterial pneumonia.
Antiviral drugs:
- Giving antiviral drugs to treat viral pneumonia.
Antipyretics:
- Provide antipyretic medicine to reduce fever.
Pain Relievers:
- Provide analgesic drugs to reduce chest pain.
Oxygen therapy:
- Provide supplemental oxygen to maintain oxygen levels.
Expectorants & mucolytics (cough expectorants):
- Provide expectorants to thin and expel phlegm.
Bronchodilators:
- To keep the airway open.
Rest And Fluid :
- Provide adequate rest to the patient. Also maintain hydration levels.
Nursing Management of Pneumonia:
Ineffective airway clearance related to broncho constriction and increased mucus production
Maintain a patent airway.
- Monitor vital signs.
- Assess respiratory rate, rhythm, and breathing pattern.
- Assess breath sounds and chest movement.
- Monitor pulse oximetry and arterial blood gas values.
- Provide the patient with a Fowler position and restrict his/her activity.
- Explain and encourage the patient to do deep breathing and cuffing exercises.
- Provide knowledge about pursed lip breathing and diaphragmatic breathing to the patient.
- Encourage the patient to expectorate phlegm if secretions are present.
- Provide oxygen therapy if the SpO2 level is low.
- Provide nebulization to the patient.
- Medicine prescribed by the doctor (Bronchodilator) administration.
- Maintain records and reports.
Impaired gas exchange related to decrease ventilation
Improve gas exchange
- Monitor vital signs.
- Assess respiratory rate, rhythm, and breathing pattern.
- Assess breath sounds and chest movement.
- Monitor pulse oximetry and arterial blood gas values.
- Provide the patient with a Fowler position and restrict their activity. To do.
- Explain and encourage the patient about deep breathing and cuffing exercises.
- Provide the patient with knowledge about pursed lip breathing and diaphragmatic breathing.
- Encourage the patient to expectorate phlegm if secretions are present.
- Provide oxygen therapy if the SpO2 level is low.
- Provide nebulization to the patient.
- Administer the medicine (bronchodilator) prescribed by the doctor.
- Maintain records and reports.
Infective breathing pattern related to chest pain
- Monitor vital signs.
- Assess respiratory rate, rhythm, and breathing pattern.
- Assess breath sounds and chest movement.
- Monitor pulse oximetry and arterial blood gas values.
- Provide the patient with a Fowler position and restrict his/her activity.
- Explain deep breathing and cuffing exercises to the patient and provide anchorage To do.
- Provide knowledge about pursed lip breathing and diaphragmatic breathing to the patient.
- Encourage the patient to expectorate phlegm if secretions are present.
- Provide oxygen therapy if the SpO2 level is low.
- Provide nebulization to the patient.
- Administering medicine (bronchodilator) prescribed by the doctor.
- Maintaining records and reports.
Q-2
a) Define suture. Enlist & describe types of suture. Define suture. List its types and explain them in detail. 08
Definition:
Suture material is a surgical thread that is used to close a patient’s wound or incision. Its main purpose is to connect the tissues of the body and keep them in place until the natural healing process.
Need for Sutures:
- For Hemostasis
- For Tissue Approximation
- To Prevent Infection
- For the wound to heal quickly and properly
- To maintain the stability of the organ or bone
Main Types of Suture Material:
1.According to Absorbability
A. Absorbable Sutures:
This material is absorbed by the body within a few days after it is inserted.
Use: Internal organs, gastrointestinal tract, gynecological surgeries
Examples:
- Plain Catgut (from animal intestine)
- Chromic Catgut (treated for time-delay)
- Polyglactin 910 (Vicryl)
- Polyglycolic acid (Dexon)
- Polydioxanone (PDS)
Absorption Time:
Vicryl: ~60-90 days
Catgut: ~7-10 days
PDS: ~120-180 days
B. Non-Absorbable Sutures:
This material is not absorbed by the body and often has to be surgically removed.
Use: Skin, cardiovascular, neurological, and orthopedic surgeries
Examples:
- Silk
- Nylon (Ethilon)
- Polypropylene (Prolene)
- Polyester (Ethibond)
- Stainless Steel wire
2.According to Structure:
A. Monofilament Sutures:
Made of a single fiber → Less abrasion → Less risk of infection
Example: Nylon, Prolene, PDS
B. Multifilament Sutures:
Made of many fibers → Stronger → More knot security
Example: Silk, Vicryl, Polyester
3.According to Origin
A. Natural Sutures:
Obtained from natural sources
Example: Catgut (sheep intestine), Silk (silkworm)
B. Synthetic Sutures:
Manmade polymer based materials
Example: Vicryl, Nylon, PDS, Prolene
4.According to Usage Site :
Site Preferred Sutures
Skin Nylon, Prolene
Internal Organs Vicryl, PDS
Cardiovascular Prolene
Orthopedic Stainless steel wire
Neurosurgery Silk, Prolene
Suture Sizes:
Larger number → thinner thread
0 to 7 = thick sutures (for orthopedic or fascia)
4-0 to 10-0 = finer sutures (for blood vessels, nerves, eyes)
Example:
6-0 Nylon → Used for facial/cosmetic suturing
0 Vicryl → For muscle closure
Suture Needles (Types of Suture Needles):
Cutting Needle – Hard tissue (Skin)
Reverse Cutting – Plastic surgery
Tapered Needle – Soft tissue (intestine, bladder)
Blunt Needle – Friable tissues (liver)
Role of Nurse (Role of Nurse with Suture Materials):
- Maintain sterile field
- Choosing the right type – Absorbable vs Non-absorbable
- Suture expiry date & Check labeling
- Prepare instruments and sutures in OT set-up
- Assist/handle sutures as per doctor’s order
- Assess sutures for post-op wound inspection
- Follow aseptic technique for suture removal
- Documentation – Suture type, size, site, date of removal
Suture materials are a basic surgical material for the safe wound of the patient. Their proper selection, use and management are very important for a skilled nurse.
b) Write down causes of hyperkalemia. Write the causes of hyperkalemia.04
Causes of Hyperkalemia (causes)
1) Renal causes (kidney related causes):
- Acute renal failure (acute renal failure)
- Chronic renal failure (chronic kidney failure)
- Decreased potassium excretion
If the kidneys are not working properly, potassium accumulates in the body.
2) Excess potassium intake:
- Excess potassium rich diet
- Excess IV potassium
- Potassium supplements overdose
Excessive potassium intake in the body causes hyperkalemia.
3) Tissue destruction:
Severe burns
- Trauma
- Hemolysis (RBC breakdown)
- Crush injury
The potassium inside the cell is released into the blood due to cell breakdown.
4) Metabolic causes:
- Metabolic acidosis
- Diabetic ketoacidosis (DKA)
Potassium is released from the cell in acidosis.
5) Drug induced causes:
- Potassium sparing diuretics
- ACE inhibitors
- NSAIDs
- Heparin
Some drugs increase potassium.
6) Endocrine causes (hormonal causes):
- Addison’s disease
- Hypoaldosteronism
If aldosterone is low, potassium is not released.
OR
a) What is cirrhosis of liver? Write down types of it. What is cirrhosis of liver? Write down types of it. 08
Definition:
Cirrhosis of the liver is a chronic, degenerative disease in which normal liver cells are damaged and fibrous scar tissues form in the liver. Scar tissues form instead of healthy liver tissues, which blocks blood flow to the liver and prevents the liver from functioning properly, leading to liver failure. The liver becomes distorted, hardened and lumpy.
Classification of liver cirrhosis:
1) Alcoholic cirrhosis
2) Post necrotic cirrhosis
3) Biliary cirrhosis
1) Alcoholic cirrhosis
Alcoholic cirrhosis is also called Laennec’s cirrhosis and is the most common type of cirrhosis.
This cirrhosis is mainly caused by hepatitis – C and chronic alcohol use.
In this, the liver is damaged mainly due to malnutrition and chronic alcohol consumption.
In this type of cirrhosis, fibrous tissues form around the portal area and central veins.
2) Post necrotic cirrhosis:
Post necrotic cirrhosis is mainly caused by any toxic agent and viral hepatitis.
Due to which liver cells are damaged, it is called post necrotic cirrhosis.
Post necrotic cirrhosis occurs in 10-30% of patients. is.
3)Billiary cirrhosis:
Biliary cirrhosis is a chronic disease that occurs mainly due to inflammation and damage to the bile ducts in the liver.
In biliary cirrhosis, fibrous tissue and scar formation occur around the bile ducts of the liver. This causes chronic obstruction of the bile duct
b) Write down complications of cirrhosis of liver. Write down complications of cirrhosis of liver. 04
1) Portal Hypertension
- Obstructions in blood flow in the liver increase pressure in the portal vein.
- This causes ascites, varicose veins, and enlargement of the spleen.
2) Ascites
- Fluid accumulation in the abdomen.
- The stomach feels bloated, there is difficulty in breathing and walking.
3) Esophageal Varices
- The veins of the esophagus become swollen.
- If it ruptures, it causes heavy bleeding and bloody vomiting.
4) Hemorrhage
- The liver does not produce clotting factors, so bleeding occurs easily.
- Bleeding may occur through the nose, mouth, or stool.
5) Hepatic Encephalopathy
- The liver cannot remove toxins Therefore, the brain is affected.
- The patient may experience confusion, drowsiness, fainting and coma.
6) Jaundice
- The eyes and skin become yellow due to increased bilirubin.
- The urine becomes yellow and the appetite decreases.
7) Hepatorenal Syndrome
- Liver failure also causes kidney function to stop.
- Urine output may decrease and kidney failure may occur.
8) Splenomegaly
- The spleen becomes enlarged.
- It causes anemia and low platelets.
9) Infection
- The body’s immune system decreases. The patient gets frequent infections.
10) Anemia
- There is a deficiency of blood. Weakness, fatigue and dizziness occur.
11) Liver Failure
- The liver stops working completely.
- It becomes a life-threatening condition.
12) Hepatocellular carcinoma (liver cancer)
- Long-term cirrhosis can lead to liver cancer.
Q-3 Write short answer (any two) Write a short answer. (Any two) 6+6=12
a) What is pancreatitis. Write sign and symptoms of acute pancreatitis. What is pancreatitis? Write the signs and symptoms of acute pancreatitis.
Definition:
=>Infection and inflammation of the pancreas is called pancreatitis.
=> The pancreas is a gland located behind the stomach that releases insulin, glucagon, and many digestive enzymes that help in the digestion and absorption of food.
=> There are two types of the pancreatitis.
1)Acute pancreatitis.
2) chronic pancreatitis
1) Acute pancreatitis. (Acute Pancreatitis)
- =>Acute pancreatitis is a condition in which there is infection and inflammation of the pancreas and it resolves within a few days and it creates serious complications.
- => Acute pancreatitis is an infection and inflammation of the pancreas that occurs within a week.
- => Acute pancreatitis is a life-threatening condition and can cause severe complications.
2) Chronic pancreatitis. (Chronic pancreatitis)
- => Chronic pancreatitis is a gradual and long-term infection and inflammation of the pancreas, which causes permanent damage to the pancreas.
- => This condition of the pancreas develops gradually, in which ••> there is ongoing inflammation of the pancreas, ••> there is scarring of the pancreatic tissue, and ••> there is impairment in the function of the pancreas.
- => Chronic pancreatitis is a condition in which the pancreas gradually becomes infected and inflamed, and it does not heal and reaches a state of permanent pancreas damage. It is called chronic pancreatitis.
- => Chronic pancreatitis takes many years to develop but is estimated to last 10 years or more.
Sign And Symptoms:
Pain related symptoms:
- Severe epigastric pain
- Pain radiating to back
- Sudden onset pain
- Pain increases after fatty meals
- Pain relieved by bending forward
Gastrointestinal symptoms Symptoms):
- Nausea
- Vomiting
- Loss of appetite
- Abdominal distension
- Constipation
- Diarrhea
- Indigestion
General symptoms:
- Fever
- Weakness
- Restlessness
- Anxiety
- Sweating
- Dehydration
Cardiovascular symptoms:
- Tachycardia
- Hypotension
- Shock
Respiratory symptoms:
- Dyspnea (difficulty breathing)
- Rapid breathing
- Cyanosis
Abdominal signs:
- Abdominal tenderness
- Guarding and rigidity
- Decreased bowel sounds
Specific signs:
- Cullen’s sign (blue color around the umbilicus)
- Grey Turner’s sign (blue color on the back/flank) Color)
- Jaundice – severe case
- Ascites (accumulation of water in the abdomen)
b) Enlist steps of physical examinations and write down any two types in detail. Write the steps of physical examination and explain any two types in detail.
Physical examination uses systemic assessment techniques and visual, auditory, tactile, and olfactory senses. All these senses will be used in specific assessment techniques.
For example.. Often, it is detected by its changes in body fluids.
Four specific techniques are used in physical examination. In which..
Steps of Physical Examination
- Inspection – Inspection
- Palpation – Examination by touch
- Percussion – Examination by tapping
- Auscultation – Examination by listening
1.Inspection:
Inspection is a visual examination of the patient. And it is a visual examination of the body. In which the patient’s general appearance, body size, gait, height, shape, posture, etc. are carefully observed. This begins as soon as the nurse makes contact with the patient.
During the inspection phase of the physical assessment, the nurse uses observation skills to systematically collect observable data.
This includes measuring the patient’s respiratory effort, skin color, and wounds.
General Appearance
Status of Consciousness Personal Grooming
Expression: Concerned, Comfortable, Alert, Nervous. Body build: Thin, Fatty, Moderate. In this, the patient’s words are also combined with body language. For example, the patient’s pain experience is related to his body language. During inspection, visualize the maximum area of the body and then compare it with the side of the other body. Compare the width of the right hand with the width of the left hand. Adequate exposure of the body area is very important. Which includes observing color, texture, mobility, symmetry, nutritional status, etc.
2.Palpation:
Palpation means using the hands and fingers to feel the texture, size, shape, placement, location, etc. of the organ. In which the temperature, pulse, texture, moisture, mass, tenderness and pain of the skin are assessed using the finger tips of the hands.
Assess skin, pulse, palpation, and tenderness by pressing 1 cm deep.
Then press 4 cm deep with both hands, which is deep palpation. Use it to determine the size of the organ and the deep organ (liver).
What should be kept in mind while palpating?
- It is always very important to explain to the patient before palpation because in our culture, touch is very important. It is important to keep the hands warm and nails short before palpation. The palmar surface of the fingers is more sensitive than the finger tips, with the ulnar surface being more sensitive to vibration, and the dorsal surface being used for temperature. Palpation also helps to determine the size of the lymph node. Always proceed with gentle palpation first, followed by deep palpation. Because it can cause tenderness or disruption of fluid.
- The size and shape of the kidneys and uterus are assessed using both hands between the finger tips and the organ.
3. Percussion:
In simple words, it is called tapping. To get the quality of the sound, the sound is heard against the patient’s body by tapping with the finger. Which is used to reflect the density of internal organs. Sound, vibration and resistance which are produced with different densities and vary from organ to organ and are used to know the size, shape, position, and also to detect fluid field organs.
Percussion is a technique that physicians practice to determine the consistency of tissues.
Percussion involves tapping on the body surface with short or sharp strokes to produce various palpable vibration sounds.
Percussion is used to detect the sound, location, size, shape, and size of many organs of the body. In which the examiner taps on the patient. To produce sound, usually place the middle finger of the non-dominant hand on the percussion area. And place the middle finger of the dominant hand on the non-dominant.
In which percussion is done in two ways.
1.Direct percussion
This is used for the chest of infants and the sinuses of adults. With the help of finger tips, specific parts of the body are struck.
In the tenderness of the kidneys. Listen to the vibrations created.
It is necessary to select the same point two or three times before moving on to another. It is done to get an accurate reading. Fatty patient needs strong percussion.
_Percussion tone: Air la ute, fluid dull and solid area soft.
2. Indirect percussion
This varies according to the area in which the non-dominant hand is placed palm down and the fingers of the dominant hand are gently struck on the CVA e.g. T.. In the kidney….
_Thorax: The middle finger of the dominant hand strikes the interphalangeal joint of the non-dominant hand which lies against the patient’s skin.
Percussion produces a sound which has many sounds and different characteristics.
Characteristics of the sound
Tympanic It is usually heard over the abdomen.
Resonance in normal lung tissue.
Hyper resonance in inflamed lungs.
Dullness in the lungs.
Flatness in the muscles.
4. Auscultation
Auscultation is usually performed with a stethoscope. A stethoscope is used to block out extraneous sounds while assessing the condition of the heart, blood vessels, lungs, pleura, and intestines.
This includes breath sounds, heart vascular sounds, and bowel sounds, etc.
It is commonly used to detect the presence of abdominal sounds and assess their loudness, pitch, quality, frequency, and duration.
The most common sounds heard include those of the lungs, heart, and abdomen and blood vessels.
The chest is auscultated to hear heart sounds. Lung sounds are auscultated anteriorly and posteriorly for normal and abnormal lung sounds. The abdomen is auscultated for bowel sounds.
Characteristics of the sound:
Intensity: Loud, Medium, Soft.
Pitch: Low, High, Medium.
Duration: Short, Long, Medium.
Quality: Booming, Hollow, Dull and Drum-like.
c) What is hypersensitivity reaction? Enlist its types in detail. What is Hypersensitivity Reaction? Explain its types in detail.
Hypersensitivity:
Hypersensitivity is an altered stage of our body’s immunity in which when any antigen enters the human body, the human body’s immune system becomes hyperactive and provides a response to it and creates unacceptable symptoms in the body. This is called Hypersensitivity.
Four types of hypersensitivity:

1) type : 1 hypersensitivity is called ANAPHYLACTIC HYPERSENSITIVITY (anaphylactic hypersensitivity),
2) type : 2 hypersensitivity is called CYTOTOXIC HYPERSENSITIVITY (Cytotoxic Hypersensitivity),
3) type: 3 hypersensitivity is called IMMUNE COMPLEX HYPERSENSITIVITY (Immune Complex Hypersensitivity),
4) Type : 4 hypersensitivity is called DELAYED HYPERSENSITIVITY (Delayed Sensitivity)
1) types: 1 hypersensitivity (Anaphylactic hypersensitivity : Anaphylactic Hypersensitivity)
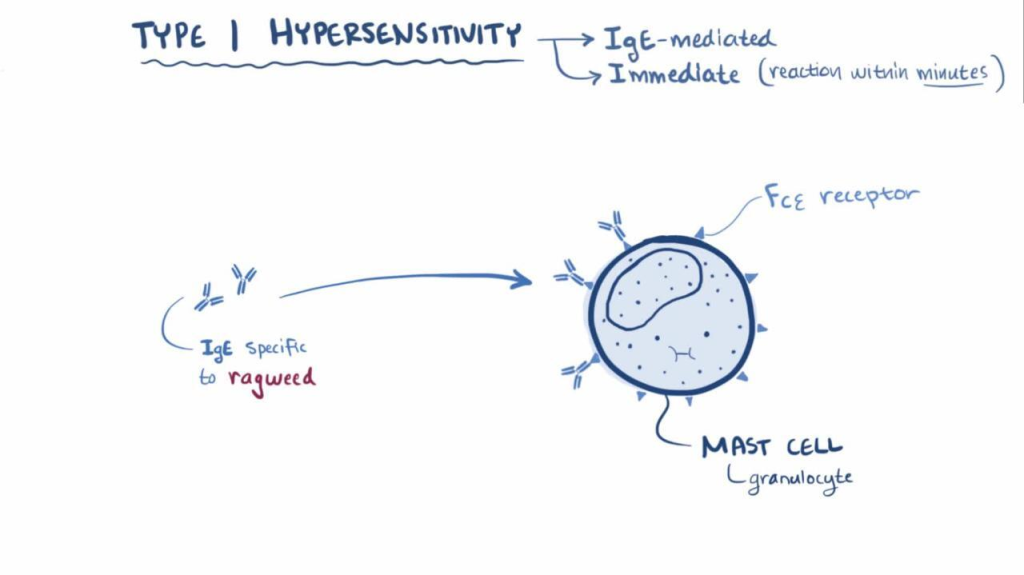
- Type 1 hypersensitivity is called a very severe type of hypersensitivity.
- In type one hypersensitivity, an immediate reaction is seen when a reaction is seen within a minute after exposure to an antigen.
- Type one hypersensitivity is characterized by edema in many tissues of the body, as well as conditions such as bronchospasm and hypotension.
- Type 1 hypersensitivity mediated by Ig-E antibody.
And helper is T -lymphocytes .
Symptoms :
- Hypotension,
- Excessive mucus secretion,
- Itching,
- Allergic rhinitis,
- Hay fever,
- Allergic conjunctivitis,
- Hives,
- Anaphylactic shock (Anaphylactic shock) it’s a common symptom in type 1 hypersensitivity.
2) type : 2 hypersensitivity (Cytotoxic hypersensitivity):
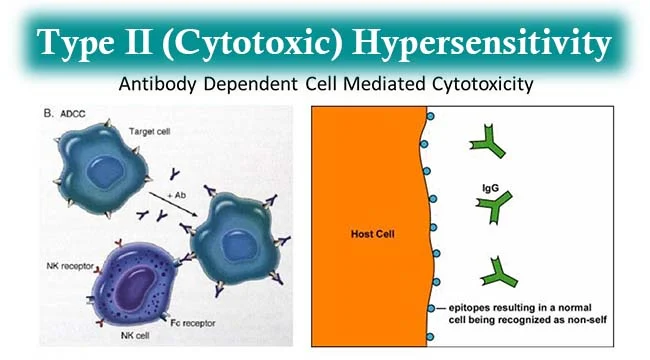
- When this type of hypersensitivity occurs, the body treats its own normal cells as antigens and creates an antibody reaction.
- Type 2 reactions stimulated by exogenous antigen ex: foreign tissues, cells or drug reactions.
- type 2 hypersensitivity mediated by IgG and Igm antibody
- Ex: Autoimmune hemolytic Anemia (In this our own body’s immune system destroys our own body’s red blood cells and blood deficiency is seen, it is called autoimmune hemolytic anemia).
3) Type : 3 hypersensitivity (immune complex hypersensitivity (immune complex hypersensitivity) :
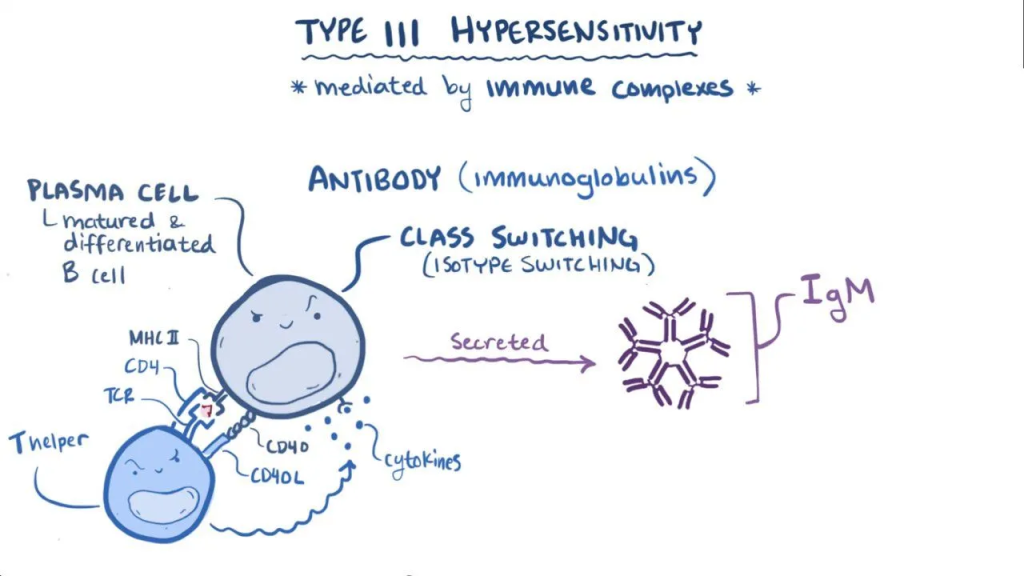
In this type of hypersensitivity, when an antigen binds to an antibody, an immune complex is formed.
Ex:
- SLE (Systemic lupus erythematous) ,
- RA (Rheumatoid arthritis),
- Nephritis,
- Certain type of Bacterial endocarditis.
4) type : 4 Delayed hypersensitivity:
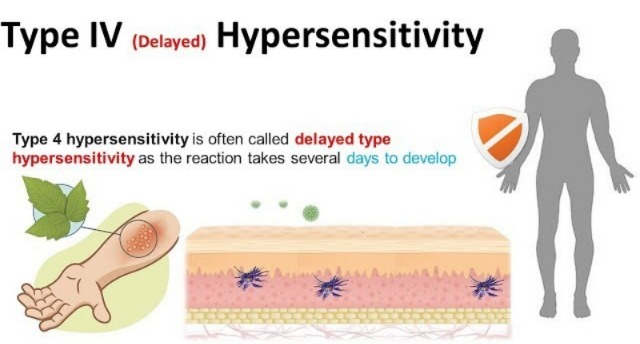
- This type of hypersensitivity is known as cellular hypersensitivity.
- This type of hypersensitivity occurs within 24 hours of exposure to an allergen. Its signs and symptoms appear after 48 hours, hence it is called Delayed Hypersensitivity.
- this Hypersensitivity is mediated by T cells and macrophages.
- Ex:
intradermal injection of tuberculin (Intradermal Injection of Tuberculin),
PPD (Purified protein derivatives),
contact dermatitis (Contact Dermatitis).
Q-4 Write short notes. Write short notes. (Any three) 12
a) Regional Anesthesia. – Regional Anesthesia
1) Definition :
- Regional anesthesia is a method of anesthesia in which Pain and sensation are blocked in a specific part of the body, but the patient remains conscious.
2) Purpose:
- To relieve pain during surgery
- To produce numbness in body part (body part) To numb)
- For safe surgical procedure (to make surgery easier)
3) Types:
- Spinal anesthesia (spinal anesthesia)
- Epidural anesthesia (epidural anesthesia)
- Nerve block (nerve block) Block)
- Field block
4) Advantages:
- Patient remains conscious
- Less risk than general anesthesia
- Good pain relief Relief)
- Less nausea and vomiting
5) Complications:
- Hypotension (low BP)
- Headache
- Infection (Infection)
- Nerve injury
- Urinary retention
6) Nursing Responsibilities:
- Check vital signs
- Explain procedure to patient (explain procedure)
- Maintain sterile technique (sterile technique)
- Monitor BP and pulse (BP and pulse check)
- Observe complications (complications to be observed)
- Provide comfort and safety (patient comfort)
b) Esophageal varices – esophageal varices
1) Definition:
- Esophageal varices are abnormal enlargements of veins in the lower part of the esophagus.
- Esophageal varices are most common in patients with liver cirrhosis.
- Esophageal varices develop when the normal blood flow to the liver slows down.
- This causes blood flow to the nearby smaller blood vessels. The vessel backs up.
- It mainly occurs in the vessels of the esophagus, due to which the blood vessels dilate. Esophageal varices develop
- Many times esophageal varices rupture. Then life threatening bleeding is created.
2)Etiology:
- Liver failure.
- Liver cirrhosis.
- Portal hypertension.
pre hepatic cause:
- Portal vein thrombosis.
- Increased portal blood flow fistula.
- Portal vein obstruction.
Intra hepatic:
- cirrhosis due to varices cause.
- Idiopathic portal hypertension.
- Acute hepatitis.
- Schistosomiasis.
- Congenital hepatic fibrosis.
- Myelosclerosis.
post- hepatic :
- Budd chiary syndrome.
- Constrictive pericarditis.
other cause:
- Liver disease.
- Malnutrition.
- Due to alcohol intake.
- Physical exercise.
- Circadian rhythm.
- Increases intra-abdominal pressure.
- Aspirin intake ( Aspirine intake ).
- Non steroidal anti inflammatory drug ( NSAID).
- Bacterial infection.
3)Sign And Symptoms (Sign And Symptoms):
- Gastrointestinal bleeding.
- Hematemesis (blood in vomit).
- Abdominal pain.
- Dysphagia(dysphagia:: difficulty in swallowing).
- Odynophagia(odynophagia:= pain in swallowing).
- Confusion.
- symptom of Anemia and shock .
- Blood in vomiting.
- Abdominal pain.
- Ascites (Acities: accumulation of fluid in to the stomach).
- Hepatic encephalopathy.
- Pallor
- Hypotension (hypotension/shock).
- Reduced urine output.
- Malena.
- Reduced Glasgow Coma Scale.
- Sign of sepsis .
4) Diagnostic evaluation (Diagnostic evaluation).
- History taking and physical examination.
- Complete blood count (CBC).
- hemoglobin level assessment.
- assess the platelet count.
- assess the international normalized ratio (INR).
- renal function test
- liver function test.
- Computerized Tomography (ct scan assessment).
5) Management (Management):
1) Endoscopic band ligation (endoscopic band ligation)
- In endoscopic ligation, a rubber band is tied around the bulging vein and the bleeding is stopped.
- Endoscopic band ligation is considered the first line treatment for esophageal varices.
2) Balloon tamponade
- In the balloon tamponade procedure, a balloon is inserted through the nose is inserted and the bleeding from the varicose veins is stopped.
3) Sclerotherapy
- In sclerotherapy, an injection is introduced into the building side and due to this, the blood clots and the bleeding also stops.
4) Drug therapy
Drug therapy provides drugs to reduce blood pressure.
Ex:= terlipressin,
Vasopressin,
NItroglycerine,
Octerotides.
Somatostatin.
5)Transjugular intrahepatic portosystemic shunting ( TIPS)
6)Distal spleenorenal shunt ( DSRS). ,
7)Esophagial Transection.
8)Liver transplantation.
6) Nursing Management:
- Advise the patient to stop drinking alcohol.
- Advise the patient to eat a healthy diet.
- Advise the patient to eat fruits and vegetables.
- Advise the patient to eat fruits and vegetables.
- Advise the patient to avoid fatty and spicy food.
- Advise the patient to maintain his body weight.
- Advise the patient to maintain proper weight.
c) Ideal O.T setup – Ideal O.T setup
- The operation theatre should be in style
- The room should be comfortable
- There should be a system in place to control infection
- Modern equipment should be used
- The operation theatre should be separate from other rooms in the hospital
- Separate rooms for different operations Arrangements should be made
- There should be an arrangement of artificial ventilation to maintain the temperature of the operation theater
- There should be an arrangement to ensure 24-hour electricity supply
- Each door of the operation theater should have a hydraulic system
- There should be an arrangement of mobile X-ray
- All the rooms in the operation theater should be arranged as per the requirement
- The Operation Theater should be connected to the hospital by a road.
- The light fittings and sewer lines of the Operation Theater should be underground.
- The ground flooring of the Operation Theater should be made of marble or cobblestone.
- The windows and doors of the O.T. should be of one-way glass and should be covered with curtains.
- The O.T. The floors, walls and furniture of the OT should be washable.
- After entering the OT, the patient should not be able to easily see other patients, the operation or the staff members.
- There should also be a mobile light and shadowless light.
- The staff and servants working in the OT should be well trained.
The following units should be present in the Idle Operation Theatre. To prevent infection, there should be a facility where the patient enters from one side and exits from the other.
Reception room :-
When the patient enters the operation theater, there should be a separate room to receive him.
The patient area should be comfortable. The walls of this room should be colorful and posters should be posted.
There should be a reception room for adults and children. And the room should have a telephone system. This room should be away from the operation theatre room. Nursing staff should be on duty in this room.
Changing room :-
This room should be away from the operation theatre room. Every staff wears OT dress in this room.
Anesthesia room :-
This room should be attached to the main operation room. This room should have a bed, anesthesia trolley and related equipment. There should be a cupboard arrangement in this room to keep anesthetic equipment. This room should be equipped with sufficient supplies of oxygen, suction machine, BP apparatus, anesthetic drugs, and emergency drugs in trays. This room should be out of sight of the patient.
Scrub room :-
The surgeon and staff are scrubbed in this room. For this, necessary things like antiseptic liquid, soap, towels, mirrors should be arranged and for hand washing procedure, there should be a large size sink and a tap with a handle and there should be a provision for 24 hours water supply and this room should have sterilized aprons and gloves.
Main operation room :-
The main part of the OT is where operations are performed. This room should be air conditioned. This room should have all the modern equipment like suction machine, mobile light, mobile X-ray, cautery machine, oxygen, anesthesia trolley, emergency injection tray, ventilator etc.
There should be tables according to the operation to give the position. And there should be shadowless light on the operation table.
Preparation room :-
There should be separate arrangement of tables and ranks for making sets and drums according to different operations
Sterile supply room :-
This room should be arranged for keeping sterilized items and for their supply
Central sterilization supply unit :-
This room should be away from the operation room where all the items are sterilized. For this, there should be an autoclave machine. This room should have proper ventilation.
Minor operating room :-
There should be a separate room for minor procedures
Utility room :-
This room should be arranged to clean and separate the instruments, linen, gloves, etc. used and damaged during the operation
Infectious disease operating room:-
If there is a patient with infectious disease, then there should be a separate room for them to operate so that it should be separate from the main operation room so that the spread of infection can be prevented and timely Regular fumigation should be done
Recovery room :-
The main purpose of the recovery room is to provide total nursing care to the operated patient. The staff working in this room should have knowledge of post-operative and post-anesthetic complications.
This room should be equipped with resuscitation equipment, suction machine, emergency drugs, and oxygen. There should be a modern bed for the patient so that the patient can be given the right position and post The operative should have the necessary equipment.
d) Graves disease – Graves disease
1) Definition:
- Graves disease is an autoimmune disease in which the thyroid gland becomes overactive, causing the thyroid gland to produce too much hormone (hyperthyroidism). Due to this, the body’s metabolism increases and symptoms like weight loss, increased heart rate, anxiety, sweating and bulging eyes (exophthalmos) are seen.
2) Etiology:
- Autoimmune reaction
- Genetic factors
- Genetic factors
- Emotional stress
- Infection
- Excess iodine intake
- Hormonal imbalance
3) Risk Factors:
- Female gender
- Age 20–40 years
- Family history
- Smoking
- Stress
- Pregnancy
- Autoimmune diseases
4) Signs and Symptoms:
- Weight loss
- Increased appetite (Increased appetite)
- Heat intolerance
- Tachycardia
- Palpitation
- Nervousness
- Irritability
- Tremors
- Goiter (Goiter)
- Exophthalmos (exophthalmos)
- Fatigue
- Diarrhea
5) Diagnostic Evaluation:
- Thyroid function test – T3, T4 ↑, TSH ↓
- Thyroid antibody test
- Radioactive iodine uptake test
- Radioactive iodine uptake test
- Thyroid scan
- Ultrasound
- ECG
6) Management:
Medical management:
- Antithyroid drugs – Carbimazole, PTU
- Beta blockers
- Radioactive iodine therapy
- Sedatives
Surgical management:
- Thyroidectomy
7) Nursing Management:
- Monitor vital signs
- Provide calm environment
- Provide calm environment
- High calorie diet
- Administer medications
- Eye care
- Encourage rest
- Monitor weight
8) Complications:
- Thyroid storm
- Heart failure
- Arrhythmias
- Severe weight loss
- Vision problems
9) Prevention:
- Regular check-up
- Stress control
- Avoid smoking Avoid)
- Proper iodine intake
- Follow treatment
Q-5 Define following (any six) Write the following definition. (Any six) 12
a) Colostomy – Colostomy
- A colostomy is a surgical procedure in which a part of the large intestine (colon) is removed to create a stoma (opening) in the abdominal wall. This opening is called a colostomy.
- This opening is used to drain fecal matter, i.e. stool, into a pouch connected to the stoma.
b) Enuresis – Enuresis
- Enuresis is also called bedwetting.
- Enuresis is a condition in which a child involuntarily urinates at night, even after the age of five or when the child has had time to achieve adequate bladder control. Enuresis is called. Enuresis (bedwetting) is also called nighttime incontinence.
c) Pheochromocytoma – Pheochromocytoma
- Pheochromocytoma is a rare tumor of the adrenal gland. Pheochromocytoma causes the release of large amounts of epinephrine and norepinephrine hormones, which play an important role in maintaining heart rate, metabolism, and blood pressure. Pheochromocytoma can be a life-threatening condition if not diagnosed and treated.
- Pheochromocytoma can occur at any age, but is most common in middle age (40 to 60).
d) Hypokalemia – Hypokalemia
- Hypokalemia is a metabolic condition in which the concentration of potassium is lower than the normal potassium concentration. It is called hypokalemia. The normal potassium level is 3.5 to 5.5 meq/liter.
- In the condition of hypokalemia, the potassium level is less than 3.5 meq/liter.
- ( In hypokalemia the potassium level is less than < 3.5meq/liter)
e) Osteoporosis
- Osteoporosis is a skeletal disorder in which bone density decreases and the bones become weak and fragile. In this condition, the loss of minerals from the bones puts them at risk of breaking down: especially in the hip, spine, and wrist.
- How are bones affected?
- Normally, bones are under a process of continuous remodeling – in which old bone breaks down and new bone is formed. But in Osteoporosis:
- Bone resorption > Bone formation
This means that old bones are breaking down but new ones are not being formed as quickly, causing bones to become thin and brittle.
f) Cheyne stoke respiration – Cheyne stoke respiration
- Cheyne-Stokes respiration is an abnormal breathing pattern in which the depth and rate of breathing gradually increases, then gradually decreases, and then breathing stops (apnea) for a short period of time. This cycle repeats regularly and is usually seen in heart failure, brain injury, or severe illness.
g) Autoclave – Autoclave
- An autoclave is a sterilization machine used in hospitals and laboratories, which destroys all types of microorganisms by using high temperature and high pressure steam.
- This machine works on the principle of moist heat sterilization. It typically uses steam at 121°C (250°F) temperature and 15 pounds of pressure for 15–30 minutes. This hot steam penetrates the equipment and completely destroys bacteria, viruses, fungi and spores and makes the material sterile.
Autoclaves are used in the following places:
- Hospital
- Operation theater
- Laboratory
- Dental Clinic
To sterilize:
- Surgical instruments
- Dressing material
- Gloves
- Glassware
- Culture Media
h) Pulmonary edema – Pulmonary edema
Pulmonary edema is a condition in which there is an accumulation of excess fluid or fluid build-up in the lungs, around the alveoli of the lungs, and in the interstitial space, and this fluid collects in the air sacs (alveoli) causing breathing difficulty, coughing, wheezing, and feeding difficulties.
Q-6(A) Fill in the blanks – Fill in the blanks. 05
1.Glossitis is an inflammation of _ . Glossitis is an inflammation of _ . tongue.
2.Diabetes insipidus is caused by _ deficiency. Diabetes insipidus is caused by a deficiency of _. ADH (Antidiuretic hormone) ADH hormone
3.GVHD full form is _. The full name of GVHD is _. Graft Versus Host Disease.
4._ position is given after liver biopsy. __ Position is given after liver biopsy. Right lateral position
5.SLE full form is _ SLE full name _. Systemic Lupus Erythematosus.
B) True or False – Tell me the truth. 05
1.Steps of abdominal physical examination are…. Inspection, Percussion, Auscultation and palpation. Abdominal Examination Steps are… Inspection, Percussion, Auscultation and Palpation. 👉 False
✔ Correct order: Inspection → Auscultation → Percussion → Palpation
2.Types II DM is called insulin dependent diabetes mellitus. Type II DM is called insulin dependent diabetes mellitus. class=”has-inline-color”>Type-II DM = Non-insulin dependent
3. Laennec’s cirrhosis is also called alcoholic cirrhosis. Laennec’s cirrhosis is also called alcoholic cirrhosis. 👉 True
4.ANA test is done to diagnose SLE. ANA is reported to diagnose SLE.👉 True
5.Paradoxical breathing is a normal breathing pattern. Paradoxical breathing is a normal breathing pattern.👉 False
✔ Paradoxical breathing = Abnormal breathing pattern
(C) Match the following –
A B
1.Appendicitis – A.Meningitis – Meningitis
2.Nuchal rigidity – Nuchal rigidity B.Mcburney’s point – McBurney’s point
3.Renal stone – Renal stone C.Inj. Mannitol – Mannitol Injection
4.Cerebral edema – Cerebral edema D.Blood in pleura – Blood in pleura
5.Hemothorax – Hemothorax E.Urolithiasis – Urolithiasis
Correct Answer :
| A | Correct Match (B) |
|---|---|
| 1. Appendicitis | B. McBurney’s point |
| 2. Nuchal rigidity | A. Meningitis |
| 3. Renal stone | E. Urolithiasis |
| 4. Cerebral edema | C. Inj. Mannitol |
| 5. Hemothorax | D. Blood in pleura |
