ENGLISH-fluid-part-3-UPLOAD
Fluid and Electrolyte Acid-Base imbalance and its management:
What is fluid and electrolyte imbalance?

- Excessive amounts of fluid and electrolytes from the body can cause fluid and electrolyte imbalance in the body due to diaphoresis (sweating) in the skin or burns.
- Fluid imbalance is an abnormality in the level of fluid in the body.
- Fluid-related complications are mainly seen in the elderly.
- Excessive amounts of fluid or fluid overload can cause dehydration or fluid overload. It is seen in the elderly.
- Fluid volume imbalance is seen due to hypovolemia, hypervolemia.
- Trauma is one of the main reasons for any dehydration because due to trauma, excessive amount of fluid is lost from the body and due to this, the condition of dehydration is created and the other main reason for dehydration is excessive amount of sweating from the body due to which the fluid from the body is also reduced.
- Continuous dehydration leads to a decrease in blood volume, and destruction The return (venus return) also decreases and due to this, a condition of hypotension is created.
- The normal osmolarity of body fluid is 300 mol/liter (mol per liter).
If the osmolarity of a solution is the same as the osmolarity of body fluid (300 mol/liter), then it is called an isotonic fluid.
- ( isotonic solutions: osmolarity is equal to 300 mol/liter)
If the osmolarity of a fluid is greater than the body fluid osmolarity, it is called a hypertonic solution.
- ( hypertonic solutions: osmolarity is greater than 300 mol/ liter).
If the osmolarity of a fluid is less than that of body fluid, it is called a hypotonic solution.
- ( hypotonic solutions: osmolarity is less than 300 mol/liter)
1)Explain the fluid volume deficit ( hypovolemia):

- When too much fluid is lost from the body, a condition of dehydration occurs in the body.
- For a normal person, its sign is that the person feels very thirsty.
- If a person is not able to take fluids on his own, then he activates antidiuretic hormone, due to which the osmotic pressure and extracellular fluid in the body are regulated.
- The condition of dehydration occurs when there is not enough fluid in the body. There is no amount of.
- In hypovolemia, if the amount of fluid excreted from the body is not taken in in the same amount, then the condition of dehydration or hypovolemia occurs in the body.
Etiology/cause (reasons for dehydration):
- The most important reason is that the body loses more fluid than it loses. Excessive fluid excretion.
- Prolonged NPO (Non-purgeive nutrition):
- Internal bleeding or hemorrhage.
- Profuse sweating.
- Ectopic pregnancy,
- Due to taking any diuretic therapy.
- Due to drainage from the wound.
- Diarrhea,
- suctioning,
- Vomiting,
- Difficulty swallowing,
- Systemic infection,
- renal failure ,
- fever,
- diabetic acidosis,
- burns,
- frequent enemas,
- ileostomy (opening in the ileum),
- Chronic illness,
- cecostomy,
- Low fluid intake.
- Diabetes insipidus.
- Certain types of medicine,
- Accident or trauma,
- cirrhosis of liver
Explain clinical manifestation/sign and symptoms:
- Extreme thirst,
- Weight loss,
- rapid, weak pulse,
- Low blood pressure,
- decrease tear formation,
- dry skin,
- dry mucous membrane,
- poor skin turgur,
- increase body temperature,
- Decreased urine output,
- Dehydration,
- dark urine,
- Constipation,
- Dry mouth,
- Changes in mental status,
- Weakness,
- Sunken eye balls,
- Restlessness,
- Dry eyes,
- Decrease jugular venous pressure.
Diagnostic evaluation:
- history taking and physical examination.
- blood uria nitrogen ( BUN) level
- increase hematocrit level
- increase the specific gravity of urine greater than 1.030
medical management:
- The main priority of a patient with dehydration is to Replacing fluid in the body
- Therefore, provide intravenous fluid to the patient.
- If the patient has suffered an injury or trauma and is losing a lot of fluid, apply pressure to the area where the blood is being lost so that excessive amounts of blood can be prevented.
- Give the patient isotonic fluid. (ex: ringer lactate, 0.9% normal saline).
- Assess the patient for any signs and symptoms of dehydration.
- Assess the patient’s skin integrity.
- Check the patient’s weight daily. To do.
- Check the patient’s intake output every eight hours.
- Assess the patient’s vital signs.
- Assess the patient’s mucous membrane.
Nursing management:
Assessment:
Nursing diagnosis:
1) fluid Volume deficit related to fluid loss or inadequate fluid intake.
2) decrease cardiac output related to insufficient blood volume.
3) Impaired oral mucous membrane related to inadequate oral secretion.
4) ineffective tissue perfusion related to insufficient blood volume.
5) Constipation related to decrease body fluid.
Nursing interventions:
- Check the patient’s vital signs.
- Instruct the patient to take fluids.
- Check the patient’s intake output.
- If the patient is able to take fluids orally, give them orally. Provide fluids.
- Ask the patient to take fluids at regular intervals.
- If the patient is unable to take fluids orally, provide fluids through the parenteral route.
- Provide fluids such as Ringer’s lactate, 0.9 normal saline, and dextrose 5%, etc. to the patient.
- If the patient is dehydrated due to severe diarrhea, provide antidiarrheal medicine to the patient. To do.
- If the patient is dehydrated due to vomiting, then provide him with antiemetic medicine.
- If the patient has any kind of infection, then provide him with antibiotic medicine.
- Check the patient’s level of consciousness such as anxiety, restlessness, confusion, etc.
- Check the patient’s skin integrity.
- Change the patient’s position every two hours.
- If the patient has mild dehydration, he can be treated at home and dehydration can be eliminated.
- If the patient has severe dehydration, he needs immediate hospitalization.
complications:
- If dehydration is not treated immediately, the blood amount in the body can decrease and due to this, the functions of the main organs of the body can also be altered. Such as the brain, kidneys, heart, these organs cannot function properly.
prevention:
- To prevent dehydration, the patient should be given proper fluid intake to do, and patients who are at high risk, such as infants, should be advised to take in larger amounts of fluid.
patient education:
- Provide health education to patients and their family members about the signs and symptoms of dehydration.
- Advise patients to take adequate fluids. Ask the patient to take fluid in the amount.
- Provide health education to the patient or to take fluid in frequent amounts.
- Provide education to the patient or to take fluid in small amounts in between when doing excessive hard work so that the condition of dehydration can be prevented.
Define hypervolemia (Define hypervolemia):

INTRODUCTION :
- Hypervolemia is also called fluid overload or overhydration.
- This is a condition in which an excess amount of fluid collects in the body.
- People have fluid overload, which causes an excess amount of fluid to remain in the body, which dilutes electrolytes and red blood cells.
- The condition of hypervolemia occurs when the amount of sodium and water in the body increases. and due to this, the condition of hypervolemia is created.
Etiology/cause of hypervolemia ( Give the cause of hypervolemia):
- Due to excessive IV fluid being provided.
- Heart failure condition.
- Corticosteroid therapy.
- Low protein intake in the diet.
- Syndrome of inappropriate antidiuretic hormone.
- Renal failure.
- Cirrhosis of the liver,
- Cushing’s syndrome,
- Due to excessive fluid intake.
Explain the clinical manifestation/sign and symptoms of the hypervolemia:
- Changes in vital signs,
- Ascites,
- Increased blood pressure,
- Increased pulse rate,
- Increased respiration,
- Distended neck veins,
- Edema in feet and legs,
- Diluted urine,
- Difficulty breathing,
- Weight gain,
- Increased urine output.
- History taking,
- Physical examination,
- Low blood urea nitrogen (BUN) level,
- Low hematocrit level,
- Low urine specific gravity.
- Heart failure,
- Pulmonary edema,
- Organ failure.
Explain the Diagnostic evaluation of hypervolemia:
Explain the complication of the hypervolemia:
Explain the medical management of the hypervolemia
Drug therapy ,
Diet therapy ,
Drug therapy :
- Provide diuretic drug (Frusemide),
Diet therapy:
- Advise patient to take low-salt diet.
- Advise patient to take low-salt diet Give.
- Ask the patient to take less fluid.
- Provide proper oxygen if the patient is having difficulty breathing.
- Provide the patient with a Fowler’s position to help him breathe more easily.
Explain the nursing management of the hypervolemia ( Nursing Management of Hypervolemia Explain):
assessment:
- Assess the patient’s fluid amount.
- Assess the patient’s intake output.
- See if there is any fluid in the patient’s body.
- Assess the patient’s vital signs to do.
- Checking the patient’s weight daily.
Nursing management:
1) Excess fluid volume related to excessive fluid intake or inadequate excretion of body fluid.
2) Decrease cardiac output related to excess work on the heart from fluid retention.
3)ineffective tissue percussion related to dependent oedema.
4)risk for Impaired gas exchange related to fluid in the lungs.
nursing interventions:
- Provide treatment as per the patient’s needs.
- Check the patient’s weight daily.
- Check the patient’s intake output.
- Check the patient’s vital signs.
- Provide the patient with a semi-Fowler position.
- Change the patient’s position every two hours.
- Provide the patient with skin care as needed. Avoid massaging the skin with excessive force.
- Tell the patient to take less sodium.
- Elevate the extremities that are in ED.
- Provide the patient with the prescribed diuretic medicine.
- Check the patient’s intake output.
prevention (Prevention):
- The easiest way to prevent the condition of fluid overload is to avoid excessive fluid intake.
- Check the patient’s fluid amount when providing IV fluids.
patient education:
- Eat a low-sodium diet.
- Provide diuretic therapy.
- Provide education to the patient to reduce fluid intake.
- Check the patient’s weight daily.
Electrolyte Balance:
- Electrolyte is a charge that has They have a positive (+) or negative (-) charge and conduct electrical impulses.
- In addition, body fluids and water contain solid substances that dissolve in body fluids and blood and form solutes.
- Some solutes are electrolytes and some solutes are non-electrolytes.
- An electrolyte is a chemical that dissolves in water and conducts electricity.
- Some of them are intracellular and some are extracellular. Extracellular.
- Electrolyte is measured in (millieqivevallent/liter)meq/liter and Millieqivevalents/dl.
There are two types of Electrolyte:
1)Cation (it has a positive electric charge +),
2)Anion (it has a negative electric charge -).
And they are dissolved in water.
1) Cation (positive charge electrolyte) are :
- sodium,
- Potassium,
- Magnesium,
- And hydrogen ion.
2) Anion (negative charge electrolyte) are :
- chloride,
- Bicarbonate,
- Phosphate,
- Sulphate,
- And protein ion.
Na+ is found in the extracellular fluid.
K+ is found in the intracellular fluid.
It is important to have a proper balance of fluids and electrolytes in the body.
Acid-base coordination maintains muscle regulation, heart function,
Fluid absorption and excretion,
Nerve function and concentration, etc.
Define Electrolyte Imbalance :
- Sodium, potassium and calcium play an important role in the passage of nerve impulses.
- If any of these substances increases or decreases, it causes muscle stimulation and imbalance.
Sodium imbalance:
Sodium imbalance occurs when the concentration of sodium in the plasma is either too low or too high.
Normal sodium concentration is 135 to 145 meq/liter.
1) Define sodium deficit (hyponatremia).

- Sodium is an extracellular electrolyte.
- It plays an important role in water distribution.
- Sodium plays an important role in muscle contraction and the transmission of nerve impulses.
- The normal concentration of sodium in the blood is 135 to 145 meq/liter.
- Hyponatremia is a metabolic condition in which the level of sodium in the blood is lower than the normal sodium level.
( in hyponatremia sodium concentration is (less than )<135 meq/liter).
Three types of hyponatremia:
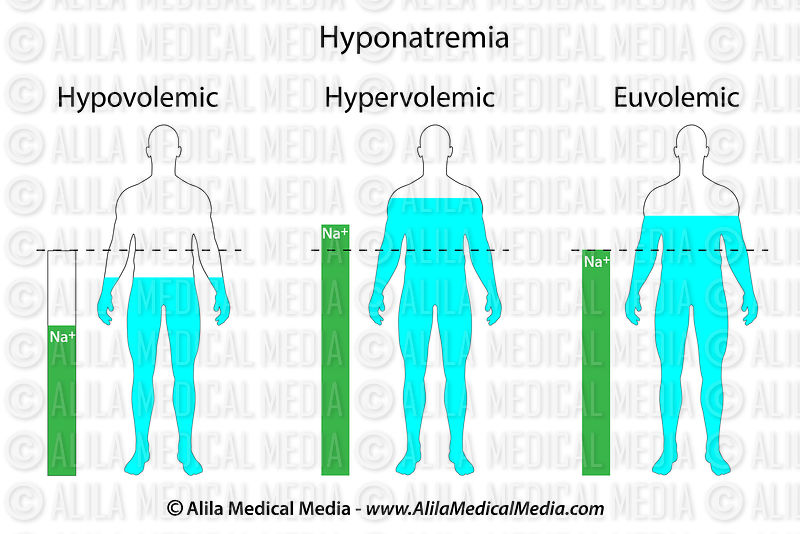
- 1) Euvolemic hyponatremia.
- 2) Hypervolemic hyponatremia.
- 3) Hypovomic hyponatremia.
1)Euvomic hyponatremia :
- In this, the water content of the body increases.
- But the sodium level remains constant.
- And this condition is caused by chronic heath conditions, cancer and some medications.
2)hypervolemic hyponatremia :
- In this, both water and sodium content in the body increases.
- But the amount of water is more.
- Excess water dilutes sodium and reduces sodium levels.
- This is mainly due to kidney failure, heart failure or liver failure.
3) hypovomic hyponatremia :
- In this, the level of water and sodium from the body decreases.
- But the level of sodium is lost more than water.
Etiology/cause (cause)
- Drinking too much water during exercise Due to.
- vomiting.
- Hormonal imbalance.
- Diarrhea.
- hypothyroidism ((due to low thyroid amount))
- syndrome of inappropriate antidiuretic hormone (SIADH).
- g.i. billiary drainage.
- Due to excessive thirst.
- nothing by mouth (NPO).
- lithium therapy .
- Diuretic.
- certain medicine like diuretic, anti depression, pain medication.
- chronic or severe dehydration.
- a low sodium. High water diet.
- cirrhosis of liver.
- kidney failure.
- kidney disease.
- congestive heart failure (congestive heart failure).
- burns.
- age.
- If a person is on a low sodium diet, they may develop hyponatremia.
- Drinking too much water during exercise.
- climate.
Clinical manifestation (signs and symptoms):
- Headache,
- muscles weakness.
- Fatigue.
- Restlessness.
- Irritation.
- Loss of interest.
- Muscle twitching and weakness To happen.
- tachycardia (increase heart rate moe than 100 beats/min).
- nausea.
- vomiting.
- abdominal cramps.
- decrease in urine output.
- postural hypotension.
- Not feeling hungry.
- mental confusion.
- delirium.
- coma.
- shock.
- Confusion.
- To be startled.
- coma .
- cellular swelling with cerebral edema leading to headache.
Diagnostic evaluation:
- History taking and physical examination.
- Serum electrolyte level ex: sodium, potassium, chloride.
- serum sodium <135meq/liter.
- decrease urine specific gravity.
- decrease serum osmolarity.
- urin sodium >100meq/24 hours.
medical management:
- Some hyponatremia conditions are caused by cancer.
- So radiation, chemotherapy, and surgery should be provided to remove it.
- So that the sodium imbalance can be corrected.
- If there is a condition of mild hyponatremia, then it can be treated through diet, lifestyle, and medication.
- If there is a condition of severe hyponatremia, then the treatment includes electrolyte and fluid administration to the patient.
- Administer a solution such as 0.9% normal saline fluid to the patient.
- Provide steroid therapy to reduce intracranial swelling.
- Check the patient’s intake output and check weight daily.
- Provide supplementary oxygen if the patient is lethargic.
- Provide IV fluids to the patient as needed.
Nursing management:
- Take a proper health history of the patient to know the cause of the patient’s condition.
- Tell the patient to eat sodium-rich food.
- Provide education to the patient to include sodium-rich fluids in the diet. To do.
- If the patient’s sodium level does not increase by 12 meq/liter in 24 hours, administer Ringer’s lactate and isotonic solution intravenously to the patient.
- Maintain the patient’s intake output chart every 24 hours.
- Check the patient’s weight daily.
- Administer hypertonic normal saline to the patient.
- If the patient has fluid restriction, ask the patient to take small amounts of fluid.
- Check the patient’s level of consciousness.
- See if the patient is in a state of confusion, lethargy, or not.
- Assess whether the patient is oriented to time, place, and person.
- Assess the patient’s deep tendon reflexes, muscle tone, and strength.
prevention:
- Treat the condition that caused the sodium level to be low early.
- Inform the person taking diuretic medicine about the adverse signs and symptoms of taking diuretic medicine, e.g. hyponatremia.
- A person who is exercising excessively should drink water only as needed to replace what has been lost from the body through sweating and should not drink more than one liter of water in an hour.
- The patient’s Ask the patient to drink enough water.
- Tell the patient to drink enough water but be careful not to get fluid overload. And tell the patient to take a sodium replacement diet.
1) Define sodium excess (hypernatremia).
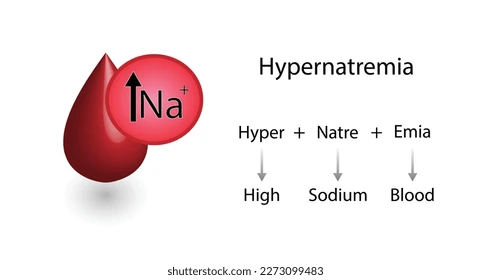
-
- Hypernatremia is an electrolyte imbalance in which the amount of sodium in the blood increases.
-
- When the amount of fluid in our body is low If salt is in excess and renal function is poor, the amount of sodium in the body increases.
-
- Normal sodium level in body is 135 to 145 meq/liter.
-
- If the value of sodium in the body exceeds the normal value, it is called hypernatremia.
-
- ( in hypernatremia the level of sodium is (more than )>145 meq/liter).
Etiology/ cause :
-
- Due to fluid loss from the body,
-
- vomiting,
-
- diarrhea,
-
- sweating,
-
- high fever,
-
- dehydration,
-
- not drinking enough water,
-
- some medications such as steroids, licorice and certain blood pressure lowering drugs.
-
- certain endocrine diseases such as diabetes and aldosteronism.
-
- excessive salt intake.
-
- hyperventilaton.
-
- due to excessive use of sodium bicarbonate.
-
- uncontrolled diabetes.
-
- due to heavy exercise.
-
- renal dysphagia.
-
- obstructive uropathy.
-
- osmotic diuretic.
Clinical manifestation/sign and symptoms:
- Feeling thirsty.
- Mucous membranes dry and sticky.
- Restlessness and agitation.
- Decreased urine output.
- Weight loss.
- Weakness.
- Tissue becomes firm.
- Disorientation.
- Dilutions and hallucinations.
- Tachycardia.
- Confusion and personality changes.
- Lower level of consciousness.
- Loss of appetite.
- nausea.
- vomiting.
- Fluid and electrolyte imbalance.
- Pulmonary edema.
- Pitting in the heel.
- Skin turgor becomes abnormal.
- postural hypotension.
- difficulty breathing.
Diagnostic evaluation:
- history taking and physical examination.
- serum electrolyte:serum sodium level >145meq/liter.
- urin sodium <40meq/liter.
- high serum osmolarity.
- increase urine specific gravity.
Management:
- Infuse the patient with a hypotonic electronic solution intravenously.
- Instruct the patient to drink adequate amounts of water.
- Provide the patient with diuretic medicine.
- Maintain the patient’s intake output chart.
- Monitor fluid loss or gain in patients at risk of increased sodium levels in the body. To do.
- Maintain and assess the patient’s intake output chart.
- Instruct the patient to follow a low sodium diet.
- Notice how much thirst the patient feels.
- Check whether the patient’s body temperature is elevated.
- The patient’s vital signs are altered. or not.
- Check the patient’s level of consciousness.
- Check the patient for headache, nausea, vomiting, and any changes in the patient’s vital signs.
- Monitor the patient’s intake output chart and assess the sodium level.
- If the patient is having seizures, keep his bed down and raise the side rails on the bed.
- Tell the patient with diabetes incipidus to drink plenty of water.
- Tell the patient to avoid salty foods, sugary drinks, and sodas.
- Educate the patient to drink plenty of water during exercise.
- Tell the patient to drink plenty of water when taking diuretic medications.
- The patient’s sodium levels increase or Assess for decrease.
- Maintain aseptic technique when providing intravenous fluid.
- Carefully monitor the patient for flu or uncontrollable vomiting.
- Check whether the patient is oriented to time, place, and person.
- Give the patient reassurance.
