ENGLISH-endocrine disorder (part-3)(deepali)
1)define/explain the goiter. (Describe goiter.)
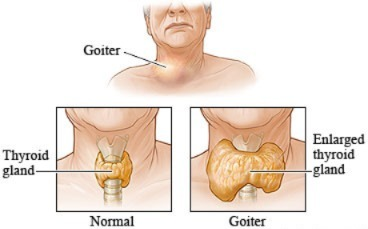
- => Goiter is a disease of the thyroid gland in which the size of the thyroid gland increases.
- =>( goiter is a condition in which enlargement of the thyroid gland is seen)
- => Goiter can be found in any person but is mainly seen in women.
- => Goiter alters the normal function of the thyroid gland.
2) Explain the Etiology/ cause of goiter. (Tell the cause of goiter)
- Due to iodine deficiency.
- (Iodine helps the thyroid gland to produce thyroid hormone, but if there is no adequate amount of iodine in the body, the thyroid gland has to work extra hard to produce thyroid hormone, so the size of the thyroid gland increases)
- Hyperthyroidism ( due to hyperthyroidism),
- Grave’s disease (Grave’s disease := autoantibody that activates TSH Receptor),
- Hashimoto’s thyroiditis (Hashimoto’s thyroiditis := autoimmune disease)
- goitrogen ingestion(lithium tablets, prophyle lithavracil, Sulphonamides, salicylates, amiodarone)
- critinism,
- nodules ( Nodules:= Nodules are solid and filled with fluid. These nodules look like hard structures from the outside but are filled with fluid inside. They are called nodules. These nodules are non-cancerous but they enlarge the thyroid.
- thyroid cancer.
3)explain sign and symptoms/clinical manifestation of goiter.
In goiter clinical manifestation include hyperthyroidism +hypothyroidism
- in hyperthyroidism:=
- tachycardia ( tachycardia),
- palpitations,
- nervousness,
- weight loss,
- Increased blood pressure,
- Heat intolerance,
in hypothyroidism:=
- Bradycardia
- Weight gain,
- Cold intolerance,
- Constipation,
- Lethargy,
Other symptoms:=
- hoarseness of voice,
- dysphagia (= difficulties in swallowing),
- coughing,
- dyspnea (= difficulty breathing),
- Swelling in the neck,
- Nodules are seen on the side of the neck.
- Dizziness.
3)explain the risk factor (Explain the risk factor)
- Hereditary,
- A family history of thyroid cancer,
- Inadequate iodine intake,
- Iodine deficiency,
- Women’s are at high risk,
- If any radiation therapy,
4) Explain the diagnostic evaluation. (Type diagnostic evaluation)
- History taking and physical examination (visible enlargement of thyroid gland),
- assess the TSH, T3,T4 hormone level,
- blood test,
- thyroid scan,
- ultrasound,
- Biopsy
5) Explain the management of goiter. (Write management of goiter.)
medical management
1)if hyperthyroidism:=
- radioactive iodine therapy.
- methimazole,
- propylthiouracil.
2)if hypothyroidism:=
- provide levothyroxin (levothyroxine),
3)if iodine deficiency:=
- Provide lugol’s iodine (Lugol’s iodine),
- provide potassium iodine (potassium iodine).
6)explain the nursing management of patients with goiter. Write the nursing management of patients with goiter.
- Maintain the patient’s proper airway.
- Assess the patient for any signs of airway obstruction.
- Properly suction the patient.
- Properly intubate the patient and take appropriate care of him.
- Provide the patient with high fowler’s position while eating and after meals atlist 30 minutes Provide high fowler position to patient. To prevent patient from aspirating.
- Ask patient to wear loose cloth on neck side.
- Ask patient not to wear tight cloth on neck side.
- Ask patient to take iodized. at least 30 micrograms.
- Ask the patient to take the medicine regularly.
- Assess the patient for any signs and symptoms of thyrotoxicosis crisis like:=neck swelling, weight loss,difficulty in breathing and swallowing.
Disorder of Adrenal gland (A gland which should be present above the renal/kidney it’s called adrenal gland. )
1)Explain/define Addition disease. Define Addison’s disease.)
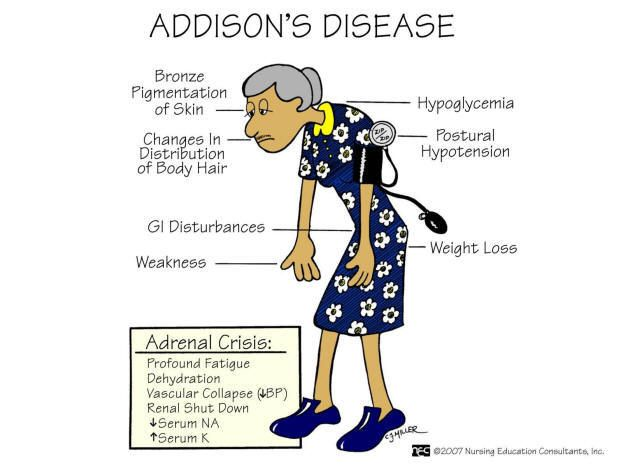
- => Addison’s disease is a rare and chronic disease.
- => Addison’s disease occurs when the adrenal gland does not produce its own hormone in an adequate amount.
- => Therefore, Addison’s disease is also called adrenal insufficiency and hypocortisolism.
- => Therefore, there is a deficiency of hormones such as glucocorticoids and mineralocorticoids of the cortex part (outer part) of the adrenal gland.
- => This condition was named after Dr. Addition in 1855.
- => Addison’s disease is mainly seen between the ages of 30 – 50 years.
2)explain the Etiology/cause of addition’s disease. (Write the causes of Addison’s disease.)
1)primary adrenal insufficiency
- := This is mainly due to a problem in the adrenal gland itself, so the hormone is not secreted.
- ( Due to disorder of the adrenal gland themselves. )
2)secondary adrenal insufficiency (Secondary adrenal insufficiency):=
- =>Due to inadequate secretion of ACTH by the pituitary gland.
1)primary adrenal insufficiency (Primary adrenal insufficiency)
- := This is mainly due to a problem in the adrenal gland itself, due to which the hormone is not secreted.
- ( Due to disorder of the adrenal gland themselves. )
- => This is mainly seen due to damage to the outer layer of the adrenal gland.
- => It is mainly damaged due to autoimmune diseases.
Other cause :=
- Due to infection,
- cancer of adrenal gland,
- tuberculosis,
- bleeding into adrenal gland,
- due to the use of anticoagulant.
2)secondary adrenal insufficiency:=
- =>Due to inadequate secretion of ACTH by the pitutary gland.
- => This is mainly due to some other reasons where the adrenal gland is not able to secrete the hormone in adequate amount.
- => Due to any disease of the pituitary gland.
- => Due to taking some kind of medication.
- => Due to radiation,
- => Due to infection,
- => Due to decreased blood flow,
- => Due to any neurosurgery.
- => Due to stress.
- => Due to an accident.
- => Due to nausea and vomiting due to dehydration.
other cause :=
- => Due to industrialized world.
- => Due to cushing syndrome.
- => hypopitutarysam,
- => due to myasthenia gravis.
- => due to pernicious anemia.
3)explain the Clinical manifestation/sign and symptoms of addition diseases. (Write the clinical manifestations/signs and symptoms of addition diseases.)
- Low blood pressure,
- tachycardia,
- Muscle weakness,
- Weight loss,
- nausea,
- vomiting,
- diarrhoea,
- hyperpigmentation (dark colours in some place).
- extreme weakness,
- fatigue,
- hyponatremia ( low level of sodium in blood stream)
- hypercalcemia ( Increase level of calcium in blood)
- hypoglycemia (low blood glucose level)
- hyperkalemia ( high level of potassium in blood. )
- slow, sluggish movement,
- Not feeling hungry,
- Lesion on the side of cheek,
- Loss of weight,
- Addison’s crisis,
- Kidney failure,
- Loss of consciousness.
- Low blood pressure.
4)explain the diagnostic evaluation of addition diseases. Write diagnostic evaluation of addition diseases
- History taking and physical examination,
- assess the laboratory investigation,
- Evaluate the sodium, potassium, and cortisol levels.
- X Ray,
- ct scan,
- MRI TEST,
- CRH stimulating test (corticotrophin releasing hormone),
- ACTH stimulating test.(Adrenocorticotrophins releasing hormone),
- insulin induce hypoglycemia test,
- 17-hydroxycorticosteroid test,
- 17-ketosteroids,
- blood eosinophil count,
- 24-hour urinary aldosterone excretion rate,
- Aldosterone test,
5) Explain the management of additions disease
medical management
- Provide Hormonal replacement therapy to the patient,
- Provide hydrocortisol to the patient,
- provide prednisolone to the patient,
- Provide glucocorticosteroids and mineralocorticoid to the patient.
- If patient has adrenal crisis (symptoms like low blood pressure, low sugar level, high potassium level) so provide intra venous glucocorticoids and provide large volume of saline dextrose.
6)surgery like: =
- Adrenalectomy
7) Explain the nursing management of patients with additional diseases.
nursing assessment
- Take a complete history of the patient and perform a physical examination.
- Check the patient’s vital signs.
- Maintain the patient’s intake output chart.
- Assess the patient’s sleeping pattern To do.
- Monitor the patient’s daily weight.
- Assess the patient for any signs and symptoms of Addison’s disease.
nursing diagnosis
1)Risk for nutritional imbalance related to decrease gastro intestinal enzyme and decrease gastric acid production.
maintain nutritional needs of patients
- Assess the nutritional status of the patient.
- Monitor the patient’s daily weight.
- Monitor the patient’s serum glucose level.
- Provide the patient with a high protein, low carbohydrate and low fat diet. Provide a low sodium diet.
- Instruct the patient to eat small and frequent amounts of food.
- Instruct the patient to rest after eating to increase digestion.
2)Risk for fluid volume deficit related to disease condition.
- maintain fluid and electrolyte balance of patients
- Assess the patient’s fluid level.
- Assess the patient’s skin turgor.
- Assess the patient’s mucous membrane.
- Monitor the patient’s vital signs.
- Assess the patient’s urine color and amount.
- Ask the patient to take adequate amount of fluid.
- Provide parenteral fluid to the patient.
- Assess the patient for any signs of petechiae in the body.
3)Risk for decrease cardiac output related to disease condition.
maintain ediquate cardiac output of patients
- Monitor the patient’s vital signs.
- Assess the patient’s peripheral pulse.
- Maintain the patient’s intake output chart.
- Advise the patient to take adequate rest.
- Provide intravenous fluid to the patient.
4)Knowledge deficit related to self administration of steroid medication.
Improve the knowledge of patients
- Provide the patient with adequate information about his/her situation.
- Discuss drug therapy with the patient including action regarding prescribed hormone.
- Inform the patient of the principles of medication.
- Tell the patient that an intramuscular self-injection administration kit is available for the client.
- Demonstrate the procedure to the patient To show by doing.
1)define/explain cushing syndrome. (Define Cushing’s syndrome.)
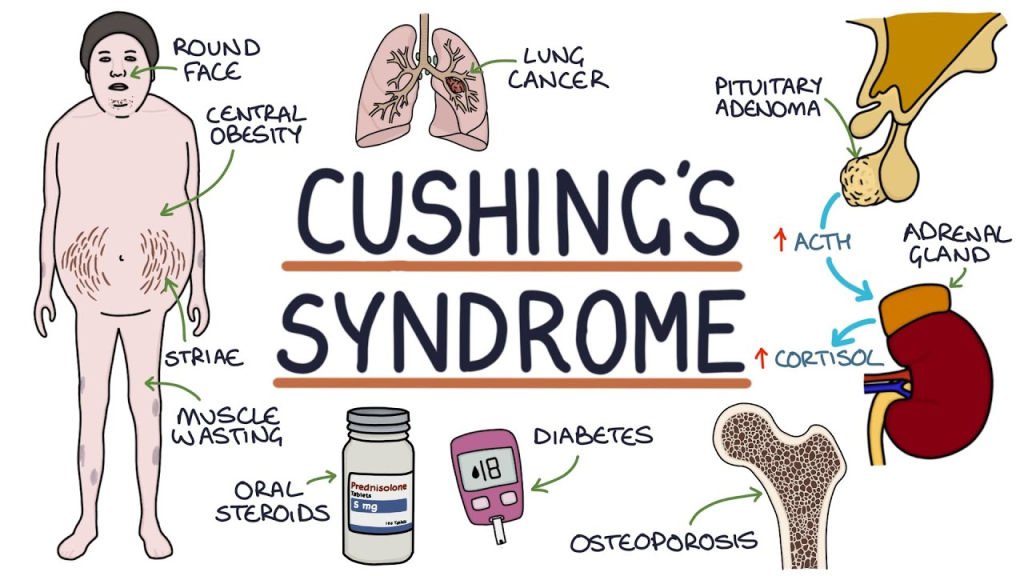
- => Cushing’s syndrome is an endocrine disorder.
- => Cushing’s syndrome is primarily caused by prolonged exposure of body tissues to high levels of the hormone cortisol.
- => Cushing’s syndrome is primarily caused by excessive secretion of adrenocorticotropic hormone (ACTH) from the pituitary gland and cortisol from the cortex of the adrenal gland.
- => Cushing’s syndrome is also called hypercortisolism.
- =>Hypercortisolism is a condition described by Harvey Cushing in 1922.
- => Cushing’s syndrome is most common between the ages of 20 and 50.
- => ( Cushing syndrome occurs due to excessive secretion of cortisol hormone from the adrenal gland cortex. )
2)explain the Etiology/cause of cushing syndrome. (Explain the cause of cushing syndrome.)
- Excess secretion of cortisol hormone from the adrenal gland cortex.
- Excess secretion of adrenocorticotrophin releasing hormone (ACTH) from the pituitary gland Due to decreased secretion.
- Due to excessive corticosteroid medication (ex:= prednisone and prednisolone).
- Due to a tumor in the pituitary gland.
- Adrenal hyperplasia.
- Due to a tumor in another part of the body (ex:= pancreas, lung, thyroid).
- Pseudo cushing syndrome (temporary over production of cortisol) is due to( depression, anorexia nervosa, alcoholism ) etc.
3)explain the Clinical manifestation/sign and symptoms of cushing syndrome. (Write the symptoms and signs of Cushing’s syndrome.)
- Increase in body weight.
- Upper body obesity and thin arms and legs.
- The patient’s face becomes round and red.
- Fatty buffalo hump in the neck region.
- Its growth in children is also Slow is observed.
# skin changes are:=
- Skin infection is seen.
- Acne is seen in the body.
- Stretch marks (white colour stretch marks on the abdominal skin) are seen on the skin of the abdomen, thigh, and breast.
- skin with easy brushing (bruising of the skin).
- Skin becomes thin, fragile.
##muscles and bone change includes:=
- Backache while doing routine activities.
- Pain and tenderness in the bones.
- Proximal muscles weakness leading to difficulty climbing stairs.
- Collection of fat between the two shoulders (buffalo hump).
- Fractures in the ribs and spinal cord due to thinning of the bones.
- Muscle weakness.
##Women with cushing syndrome often have:=
- Cushing’s syndrome in women causes excessive hair growth (hirsutism) on the face, neck, chest, and thighs.
- Irregular menstrual cycle.
##man may have :=
- decrease or no desire for sexual activity.
- impotency (ejaculatory failure).
##other symptoms of cushing syndrome are:=
- psychological problems:= Depression, anxiety and behavioural changes are seen.
- Blood pressure increases.
- Bone a week.
- Sleep disturbances are observed.
- Excessive catabolism of protein occurs.
- Muscle wasting occurs.
- Sodium and water retention occurs.
- The patient has a moon face appearance.
- In the patient A condition of hyperglycemia is seen.
- Polyuria (increased frequency of urination).
- Polydypsia (Increase thirst).
4) Explain the diagnostic evaluation of cushing syndrome .
- History tacking and physical examination.
- assess serum sodium level.
- assess blood glucose level.
- urinary cortisole level is monitored.
- ACTH production is testing.
# assess 24 hour urinary free cortisole level:=
- => In this test, the patient’s 24-hour urine is collected and tested for cortisol.
- => If the cortisol level is more than 50 to 100 micrograms, it suggests Cushing’s syndrome.
overnight 1mg dexamethasone suppression test:=
- => In this test, 1 mg dexamethasone is administered to the patient at 11 pm.
- => The next morning, serum cortisol is monitored at 8 am.
- => If a healthy individual has a cortisol level of less than 2-3 mcg/dl, but if a person has Cushing’s syndrome, the cortisol level is greater than 1.8 mcg/dl.
- assess the CRH stimulating test.
- ct scan.
- MRI.
5)explain the management of Cushing syndrome.
## Write the management of Cushing’s syndrome##
#medical management #
- If the cause of Cushing’s syndrome is a tumor in the pituitary gland, then the tumor should be removed.
- Provide radiation therapy to remove the tumor in the pituitary gland.
- If there is hyperplasia of the adrenal cortex, then adrenalectomy (surgical removal of one or both adrenal glands) should be performed.
- Provide the patient with a cortisol inhibiting drug.
- If Cushing’s syndrome is caused by corticosteroid medicine, then the dose of the medicine should be gradually reduced.
- use of drug which should be reduce the synthesis of corticosteroids like,
- Mitotane,
Ketoconazole,
Metyrapone,
Aminoglutethimide,
Trilostane and etomidate etc.
6) Explain the nursing management of patients with cushing syndrome.
nursing assessment
- Patient’s vitals To assess the sign.
- Monitor the patient’s daily weight.
- Maintain the patient’s intake output chart.
- Assess the patient’s abdominal girth.
- Inquire about the patient’s dietary habits.
- Assess the patient’s sleeping pattern.
- Assess the patient’s mood and mental activity.
nursing diagnosis
1)altered nutritional pattern related to disease condition.
meet nutritional need of patient :=
- Assess the nutritional status of the patient.
- Ask the patient about their food likes and dislikes.
- Instruct the patient to eat small and frequent amounts of food.
- Serve the food to the patient in an attractive manner.
- Instruct the patient to eat high-fiber, low-potassium, and calcium-rich foods.
- Maintain the patient’s intake output chart.
2)fluid volume excess related to sodium and water retention.
maintain fluid and electrolyte balance of patients:=
- Monitor the patient’s vital signs.
- Maintain the patient’s intake output chart.
- Record the patient’s body weight daily.
- Provide the patient with prescribed medicine.
3)Altered sleeping pattern related to disease condition.
improve sleeping pattern of patients: =
- Assess the patient’s sleeping pattern.
- Provide a calm and comfortable environment to the patient.
- The patient Involve the patient in daily routine activities to some extent during the day.
- Maintain the patient’s hygiene.
- Ask the patient to read a book.
- Ask the patient to pray and meditate before sleeping time.
4)Anxiety related to disturbed body image.
relieve anxiety of the patient:=
- Assess the patient’s anxiety level.
- Listen actively to the patient.
- Clear all the patient’s doubts.
- Involve family members in the patient’s care.
5)risk for infection related to disease condition.
improve the health of the patient and prevent from the infection:=
- Monitor the patient’s vital signs.
- Maintain the client’s personal hygiene.
- Provide the patient with a clean and ventilated room.
- Ask the patient to wear clean cotton clothes.
- Maintain aseptic technique before performing any invasive procedure.
- Wash hands properly before and after taking the patient’s medication.
- Ask the patient to take a well-balanced diet.
1)explain/define pheochromocytoma. Describe pheochromocytoma.
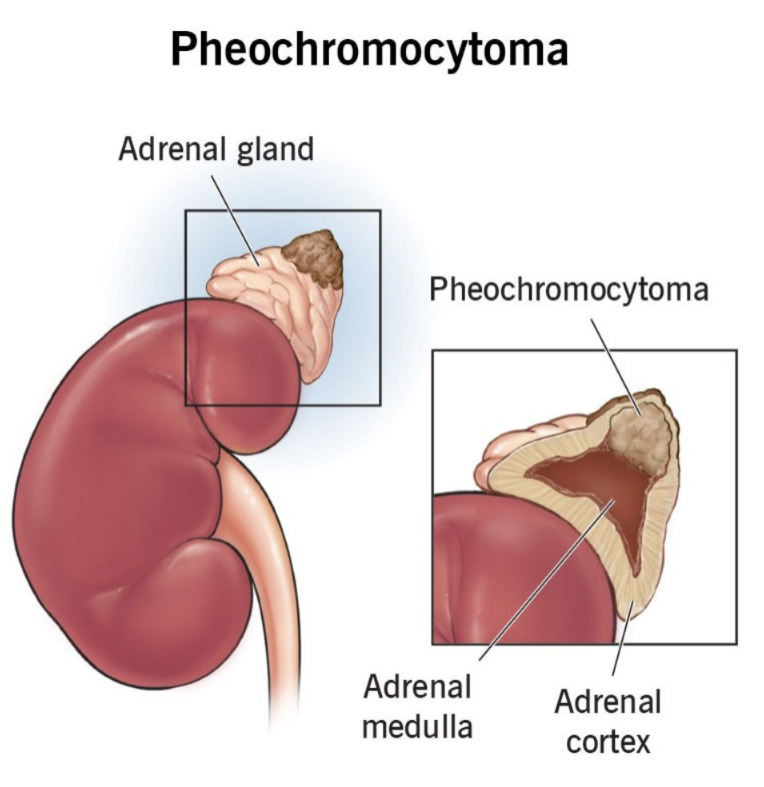
- => Pheochromocytoma is a tumor of the adrenal gland.
- => Pheochromocytoma causes the release of large amounts of the hormones epinephrine and norepinephrine, which play an important role in maintaining heart rate, metabolism, and blood pressure.
- => Pheochromocytoma can become a life-threatening condition if not diagnosed and treated.
- => Pheochromocytoma can occur at any age but is most common in middle age (40 to 60).
2)explain Etiology/cause of pheocromocytoma.
- Because of family history.
- Because of genetic disease.
- von hipple -Lindu disease.
- Multiple endocrine neoplasia.
- Neurofibromatosis type 1.
3) Explain the clinical manifestation of pheochromocytoma. Describe the symptoms and signs of pheochromocytoma.
- abdominal pain.
- chest pain.
- headache.
- sweating.
- palpitation.
- Irritability.
- Appetite increase.
- nausea.
- vomiting.
- constipation.
- difficulty breathing.
- fatigue.
- Weight loss.
- sleeping difficulty.
- difficulty seeing.
- seizures.
- tingling, burning and numbness in legs.
- pallor.
- rapid heart rate.
- Severe headache.
- Sweating.
- Hand tremor.
- Sleeping difficulty.
4)explain the diagnostic evaluation of pheochromocytoma .
Diagnostic Evaluation of Pheochromocytoma Write.
- 24-hour urine testing,
- clonodine suppression test,
- ultrasound,
- ct scan,
- MRI,
- Adrenal Biopsy,
- catecholamines blood test,
- glucose test,
- meta iodobenzylguanidine(MIBG)scanning,
- fluorodopamine PET scan,
- urin catecholamines,
- urine menephrines.
5)explain the management of pheochromocytoma. Write the management of pheochromocytoma.
medical management
- To remove the tumor through surgery.
- To monitor the patient’s vital signs properly.
- Radiation therapy.
- chemotherapy.
6)explain the nursing management of patients with pheochromocytoma. Write the nursing management of pheochromocytoma.
- Monitor the patient’s vital signs.
- Provide antihypertensive medicine to the patient.
- Instruct the patient to take continuous rest.
- Assess the patient’s urine test.
- Tell the patient not to do prolonged exercise.
- Provide the patient with a high-calorie and well-balanced diet.
- Tell the patient not to smoke.
- Provide intravenous fluids to the patient.
- Tell the patient to take adequate rest.
- Tell the patient to take medicine properly.
- To follow up the patient properly Saying.
1)explain/define diabetes ketoacidosis( DKA).Define diabetic ketoacidosis.

- => Diabetic ketoacidosis (DKA:= diabetes ketoacidosis) is a life-threatening complication of diabetes mellitus (DM:= Diabetes malitus).
- => Diabetic ketoacidosis occurs when the body produces an inadequate amount of insulin or lacks insulin.
- •••{ Insulin :=-> Insulin is a hormone.->It is released from the beta cells of the pancreas and plays an important role in transporting glucose from the blood to the cells and converting glucose into energy.
- => Diabetic ketoacidosis occurs mainly when there is an inadequate amount of insulin in the body and due to insulin deficiency.
- => When there is a deficiency of insulin in the body, glucose is not transported from the blood to the cells, so the cells do not convert glucose into energy.
- => Therefore, the body’s cells use fat for energy and break down fat.
- => Due to the breakdown of this fat, ketone bodies are released in the body as a byproduct.
- => The condition of diabetic ketoacidosis is seen due to the build up of these ketone bodies in the body.
2) Explain Etiology of diabetes ketoacidosis. Explain the cause of diabetes ketoacidosis.:=
- Insulin in the body is in an inadequate amount or due to insulin deficiency.
- Infection in the body (like diarrhea, vomiting, high fever).
- Undetected diabetes mellitus (DM).
- Due to stress.
- Some types of medication such as Corticosteroids
- ( corticosteroids), sympathomimetics, alpha and beta blockers, and diuretic medicines.
- Pancreatitis (infection and inflammation of the pancreas).
- Urinary tract infection.
- Missed insulin injection or inadequate insulin dose.
- Due to pneumonia.
- Due to surgery.
- Due to any physical or emotional trauma.
3) Explain pathophysiology of diabetic ketoacidosis. Write the pathophysiology of diabetic ketoacidosis
1)due to insulin deficiency (due to lack of insulin in the body)
-
- => Due to lack of insulin in the body, glucose is not transported from the blood to the cells.
-
- => Therefore, the cell does not get enough energy source, (because glucose works as an energy source for the cell, but when glucose is not transported from the blood to the cell, the cell does not get a source of energy).
2)increase glucose production
-
- => When there is a deficiency of allele in the body, the production of glucose by the liver increases and the condition of hyperglycemia is observed in the body.
3)break down of fats
-
- => Due to insulin deficiency, the body cannot use glucose as a source of energy,
-
- Then the body breaks down fat to get energy and fatty acids are released due to the breakdown of fat.
4)ketogenesis
-
- => Fatty acids are converted into ketone bodies and ketone bodies are acidic in nature.
5) Ketosis
-
- => Ketone bodies build up in the blood stream. And turns into ketosis.
6) Osmosis diuresis
-
- => Due to the increase in the amount of glucose in the body, osmotic diuresis is seen, due to which excessive excretion of urine is seen from the body, due to which dehydration and electrolyte imbalance are also seen in the body. Mainly potassium (pottasium) imbalance is more common.
7)dehydration
- => Dehydration is a condition caused by excessive fluid loss from the body.
8)Acidosis:=
- => Due to accumulation of ketone bodies in the body, hydrogen ions are released and metabolic acidosis is observed in the body and blood pH is less than 7.35.
4)explain clinical manifestation/sign and symptoms of diabetes ketoacidosis. Write the signs and symptoms of diabetic ketoacidosis
- Polyuria ( polyuria := increase frequency of urination)
- Polydipsia ( polydypsia := excessive thirst)
- Hyperglycemia ( hyperglycemia := due to deficiency of insuline hormone)
- Increase in the level of ketones in the body.
- kussmaul’s breathing ( Kussmaul’s breathing :=rapid and deep breathing)
- Abdominal pain.
- nausea.
- vomiting.
- Weakness.
- Fatigue.
- Alteration of mental status.
- Confusion.
- Dry skin and mouth.
- Acetone breath (fruity odor),
- Muscle stiffness.
- Anorexia (loss of appetite).
- Blurred vision.
- Blood pressure decreases.
- Orthostatic hypotension (orthostatic hypotension: = sudden low blood pressure when sitting or supine and standing. )
- Weak and rapid pulse.
- Lower level of consciousness.
- Headache.
4) Explain diagnostic evaluation of diabetic ketoacidosis. # Write a diagnostic evaluation of diabetic ketoacidosis##
- history tacking and physical examination.
- assess the blood glucose level.
- In the condition of diabetic ketoacidosis, the blood glucose level exceeds
250 mg. - assess the blood for the presence of ketone bodies in blood.
- assess the urine for presence of ketone in urine.
- arterial blood gas analysis (for assessment of metabolic acidosis).
- assess the electrolyte level of body like :=
- Sodium,
Potassium,
And other electrolyte. - complete blood count test .
- Assess the blood urea nitrogen level (BUN) (for assessing the kidney function).
- CRP (C-reactive protein for assessment of any infection).
- urinanalysis.
- ECG (electro cardiogram for assessing the heart Abnormalities).
- assess the blood pH level is less than < 7.35.
- assess the serum creatinine level.
5) Explain the management of diabetic ketoacidosis. Write the management of diabetic ketoacidosis.
6)medical management
- In the management of diabetic ketoacidosis, an attempt should be made to correct the insulin deficiency.
1)insulin therapy :=
- => Provide regular insulin intravenously to the patient.
- => The dose of insulin should be provided based on the blood glucose level and ketone bodies.
2)Fluid replacement:=
- => To correct the patient’s dehydration, administer
- 0.9% normal saline intravenously.
- 0.5 to 1 liter/hour.
- => Fluid infusion should be continued until the dehydration condition is treated or for 24 – 36 hours.
- => Continuously monitor the patient’s blood glucose level. When the blood glucose level falls below 300mg/dl, provide 5% dextrose to prevent the blood glucose level from declining.
3)Maintain electrolyte level:=
- => Monitor the patient’s electrolyte level.
- => Specially assess the level of potassium because in the best amount potassium is transported from extracellular place to intracellular place.
- => Provide potassium replacement therapy to the patient. Check urine output before potassium replacement.
4)correct of acidosis :=
- => The patient can be treated with insulin therapy and fluid resuscitation to correct metabolic acidosis.
Other :=
- => Continuously monitor the patient’s blood glucose and ketone levels.
- => If the condition of diabetic ketoacidosis has occurred in the body due to any other reason, then it should be treated, just like if there is any infection in the body, then it should be treated.
- => Provide bicarbonate therapy to the patient.
- => Monitor the patient’s vital signs regularly.
- => Perform laboratory tests on the patient.
- => When the condition of diabetic ketoacidosis is under control, insulin should be provided through subcutaneous route while keeping the patient under observation.
7)Explain complication of diabetic ketoacidosis. Write the complications of diabetic ketoacidosis. Cerebral edema, fluid and electrolyte imbalances are seen. Hypoglycemia. Acute kidney problems. Respiratory distress. .
- cerebral oedema,
- Fluid and electrolyte imbalances are seen.
- Hypoglycemia.
- Acute kidney problems.
- Respiratory distress.
- Cardiac Complications.
- Pulmonary oedema.
- Hypokalemia (hypokalemia := deficiency of pottasium in blood stream) Diabetic retinopathy.
8)Explain the nursing management of patients with diabetes ketoacidosis.(Write the nursing management of patients with diabetes ketoacidosis.)
1.assessment
- Properly assess the patient.
- Properly check the patient’s vital signs.
- Assess the patient’s neurological status.
- Assess the patient’s respiratory status.
- Assess the patient’s intake output chart.
- Check the patient for any signs of dehydration.
- Check the patient’s electrolyte levels.
2)Continuously monitoring of patient
- Patient’s blood glucose Monitor the level continuously.
- Assess the amount of ketone bodies present in the patient’s blood.
- Check the patient’s vital signs, including respiratory rate, heart rate, and pulse.
- Continuously monitor the patient’s blood pressure.
- Assess the patient for any complications such as respiratory distress, cardiac arrhythmias, and mental status.
3)Fluid and electrolyte balance:=
- Provide intravenous fluid to treat the patient’s dehydration condition.
- Check the patient’s electrolyte levels, especially the potassium level.
4)Insulin therapy:=
- Provide intravenous fluids to the patient.
- Continuously monitor the patient’s blood glucose level.
5)Neurological status:=
- Check the patient’s neurological status and level of consciousness.
- Assess the patient for cerebral edema, headache, and any changes in mental status.
6)Patient Education:=
- Provide education to the patient and their family members about the signs and symptoms of diabetic ketoacidosis and its treatment.
- Advise the patient to take a proper diet.
- Collaborate with other health care professionals for the patient’s treatment.
- Provide emotional support to the patient and their family members.
- Ask the patient’s family members to clear all doubts.
- Continuously monitor the patient when transitioning from intravenous insulin to subcutaneous injection.
1)explain/define the diabetes incipidus. (Describe diabetes incipidus)
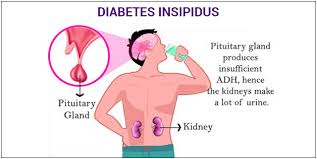
- Diabetes insipidus is caused by a deficiency or inadequate amount of antidiuretic hormone (Due to deficiency or inadequate amount of ANTIDIURETIC HORMONE). is.
- ••{ ANTIDIURETIC HORMONE:= Antidiuretic hormone regulates the body’s water balance. This hormone is produced by the hypothalamus and secreted by the posterior pituitary gland. }••
- => Diabetes insipidus is a condition in which antidiuretic hormone is secreted in inadequate amounts or there is a deficiency of antidiuretic hormone.
- => Due to this, the body water level is impaired and urine output from the body increases.
Two main symptoms are seen in diabetes insipidus.
- 1) Polyuria (excessive urination := due to deficiency of antidiuretic hormone),
- 2)Polydypsia (excessive thirst := due to the excretion of excess urine from the body.)
2)Explain the causes and types of diabetes incipidus Explain the causes and types of diabetes incipidus.
There are four main types of diabetes incipidus.
- 1)NEUROGENIC DIABETES INCIPIDUS OR CENTRAL DIABETES INCIPIDUS ( Neurogenic Diabetes Insipidus or Central Diabetes).
- 2)NEPHROGENIC DIABETES INCIPIDUS ( Nephrogenic Diabetes Insipidus)
- 3)PSYCOGENIC DIABETES INCIPIDUS ( Psychogenic Diabetes Insipidus)
- 4)GESTATIONAL DIABETES INCIPIDUS ( Gestational Diabetes Insipidus)
1)NEUROGENIC DIABETES INCIPIDUS OR CENTRAL DIABETES INCIPIDUS ( Neurogenic Diabetes Insipidus or Central Diabetes Insipidus).
- => Central diabetes insipidus is mainly caused by the production and release of inadequate amounts of antidiuretic hormone (ADH).
- =>Antidiuretic hormone plays an important role in regulating the body’s water.
etiology/cause of central diabetes insipidus:=
- => Due to any lesion in the hypothalamus and pituitary gland.
- => Due to any head injury.
- => Due to any surgery of the head.
- => Due to infection and inflammation of the central nervous system.
- => Due to any genetic condition.
- => Due to developmental abnormality.
- => Due to aneurysm in the head. (Aneurism:= Aneurism is a bulge or balloon-like structure formed from the area due to weakening of the wall of the blood vessels. It is called aneurysm.
- => Due to skull fracture.
- => Thus, central diabetes insipidus is seen due to deficiency or inadequate amount of antidiuretic hormone in the body.
2) NEPHROGENIC DIABETES INCIPIDUS (Nephrogenic Diabetes Insipidus)
=> Nephrogenic diabetes insipidus occurs when the antidiuretic hormone (ADH) is present in the body in adequate amounts but the kidneys/renals do not respond to the antidiuretic hormone for any reason.
=> Therefore, the water balance in the body is impaired.
cause/Etiology of nephrogenic diabetes insipidus:=
- => Due to any defect in the kidney tubules, water is excreted in excess from the body.
- => Due to any impairment in the structure of the kidney.
- => Due to any genetic disorder.
- => Due to taking certain medications such as lithium, diuretics.
- => Due to any kidney disease.
- => Due to general anesthesia.
- => Due to any developmental abnormality.
- => Thus, nephrogenic diabetes insipidus is seen due to an impairment in the structure of the kidney.
3) PSYCOGENIC DIABETES INCIPIDUS (Psychogenic Diabetes Insipidus)
- => Psychogenic diabetes insipidus is also called primary polydypsia.
- =>Psychogenic diabetes insipidus is caused by excessive fluid intake for any reason because antidiuretic hormone is suppressed due to excessive fluid intake.
- => Due to a mental health disorder.
- => Due to the habit of consuming too much fluid.
- => Thus, psychogenic diabetes insipidus is seen due to excessive fluid intake.
4)GESTATIONAL DIABETES INCIPIDUS ( GESTATIONAL DIABETES INCIPIDUS)
- => Gestational diabetes insipidus is mainly seen during pregnancy.
- => Because during pregnancy, the antidiuretic hormone is destroyed due to the release of enzymes from the patient.
3) Explain clinical manifestation of diabetes incipidus. (Explain the symptoms and signs of diabetes incipidus)
1) Polyuria (Polyuria:= Passing excessive urine)
- => A very large amount of diluted urine is passed.
2) Polydypsia (Polydipsia:= Excessive thirst)
- => Due to excessive amount of urine passing from the body, the body loses fluid, so the body feels thirsty to maintain fluid.
- ( fluid intake is 5 to 20 liter/day.)
3) Nocturia
- =>Excessive amount of urine passing during night time causes sleep pattern to be altered.
4) Dehydration
- => Due to excessive loss of water from the body, the body becomes dehydrated, hence conditions like dry mouth, dry skin, impaired skin turgor are seen.
5) Hypernatremia
- => Hypernatremia is an increase in the amount of sodium in the body and this is mainly seen due to excessive fluid loss from the body.
- Due to this, many neurological symptoms such as seizure are also seen in the body.
6)Hypotension
- Hypotension is seen due to excessive fluid loss from the body, due to which conditions like dizziness and fainting are seen. Found.
7) Weight loss
- Due to continuous fluid loss from the body (due to polyuria), body weight decreases.
other symptoms:=
- Fatigue,
- Fever,
- Tachycardia,
- Difficulty seeing ,
- Electrolyte imbalance,
- No appetite (Anorexia),
- Electrolyte imbalance.
- Diarrhea,
- Vomiting.
- Bed wetting.
4) explain diagnostic evaluation of diabetes incipidus. (Write a diagnostic evaluation of diabetes incipidus.)
history taking and physical examination.
1)water dipreviation test.
- => This test is done to assess the cause of diabetes insipidus.
- => In this test, the patient is asked to stop drinking fluids for two to three hours.
- => Then, the changes in the body due to not drinking fluids are assessed, such as changes in body weight, urine output, urine concentration, etc.
- => This test also assesses the amount of antidiuretic hormone present in the blood.
- => When this test is performed on children and pregnant women, close observation is done and it should be kept in mind that the body weight should not lose more than five percent.
2)Antidiuretic hormone ( ADH) Test.
- => Antidiuretic hormone test is done after water deprivation test.
- => In this test, antidiuretic hormone (Desmopressine :=synthetic antidiuretic hormone) is provided in small doses through injection.
- => Then it is observed how the body reacts to this hormone.
- => This test is performed to assess what type of diabetes insipidus the patient has.
- => In this test, when the patient is provided with antidiuretic hormone and the patient’s urine production stops, the patient is found to have a condition of diabetes insipidus due to shortage of antidiuretic hormone.
- => This mainly detects central diabetes insipidus (neurogenic diabetes insipidus) in the patient.
- => If urine production remains at the same level even after providing the patient with antidiuretic hormone, it detects that the body is producing adequate amounts of antidiuretic hormone, but due to some kidney abnormality, the kidneys are not responding to the antidiuretic hormone. Therefore, nephrogenic diabetes insipidus is detected.
3)urin analysis:=
- => In this test, when the amount of water in the urine is high and the amount of salt and waste products is low, it detects the condition of diabetes insipidus.
4)MRI( Magnetic resonance imaging)
- => This test is mainly done to detect any problems in the hypothalamus and pituitary gland.
5)serum osmolality:=
- => This test is mainly done to assess the amount of solutes in the blood.
6)Fluid intake output monitoring:=
- => This test is mainly done to assess how much fluid the patient has ingested and how much urine is output.
7) Genetic testing:=
- => This test is mainly done to assess if there is any genetic abnormality.
8)check the electrolyte level
- => It is done to detect if there is any electrolyte imbalance in the patient’s body.
5)explain the management of diabetes incipidus.
medical management
central diabetes incipidus:
- => Central diabetes insipidus is caused by inadequate levels of antidiuretic hormone.
- => Therefore, the patient should be provided with synthetic antidiuretic hormone (Desmopressin).
- => Synthetic antidiuretic hormone is taken in the form of nasal spray,
- Oral tablets,
- And injection.
- => Providing this synthetic antidiuretic hormone reduces the excessive urine output.
Nephrogenic diabetes incipidus:=
- => If the cause of diabetes incipidus is due to an abnormality of the kidneys, then synthetic Desmopressin is not used as a treatment.
- => If you have diabetes insipidus due to kidney disease, then follow a low salt diet.
- => Do not take any medicine that damages the kidneys.
- => People who have nephrogenic diabetes insipidus should take drugs from the prostaglandin inhibitor group.
3)psychogenic diabetes incipidus:=
- If a person has psychogenic diabetes insipidus, i.e., diabetes insipidus due to any mental illness, then that mental illness should be treated.
4) Gestational diabetes insipidus.
- => If the condition is gestational diabetes insipidus, provide the patient with synthetic desmopressin.
6) Explain the nursing management of patients with diabetes insipidus.
nursing assessment
- Patient’s vital sign monitor To do.
- Ask the patient about any history of head injury.
- Inquire about the patient’s eating habits.
- Assess the patient’s urine output and fluid intake.
- Assess the patient’s skin turgor.
- Ask the patient about signs such as polyuria and polydipsia.
nursing management
nursing diagnosis
- 1) Electrolyte level imbalance related to hypernatremia.
- 2) fluid volume deficit related to polyuria.
- 3) Disturbed sleeping pattern related to disease condition.
- 4) Altered tissue perfusion related to disease condition.
- 5)Risk of complications related to disease condition.
nursing interventions
maintain fluid and electrolyte balance of patients:=
- Monitor the patient’s vital signs.
- Maintain the patient’s intake output chart.
- Provide intravenous fluid to the patient.
- Follow the trick aseptic technique.
maintain tissues perfusion of patient:=
- Assess the patient’s skin integrity.
- Provide skin care to the patient.
- Ask the patient to wear clean, loose clothing.
- Change the patient’s position every two hours.
- Ask the patient to do active and passive exercises.
relief anxiety level of patient
- Assess the patient’s anxiety level.
- Ask the patient to clear all his doubts.
- Provide information about the disease and its symptoms to the patient.
- Involve family members in the client’s care.
maintain hygiene of patient:=
- Ask the client to maintain his personal hygiene.
- Ask the patient to change his clothes daily.
- Ask the patient to wear clean cotton clothes.
- Assess the patient’s discomfort level.
promote comfort and sleep of patient:=
- Assess the patient’s sleeping habits.
- Provide a conductive environment to the patient.
prevent the occurrence of complication to the patient
- Prevent the patient from complications such as dehydration, metabolic acidosis, etc. Monitor the patient if any of the following symptoms are observed.
- If the patient exhibits any of these symptoms, report them to the physician immediately.
- Provide the patient with the prescribed medicine.
- Provide reassurance to the client.
- Monitor the patient for any complications.
- Explain the disorder of pituitary gland
1)define/explain hypopitutarisam. Define hypopituitarism
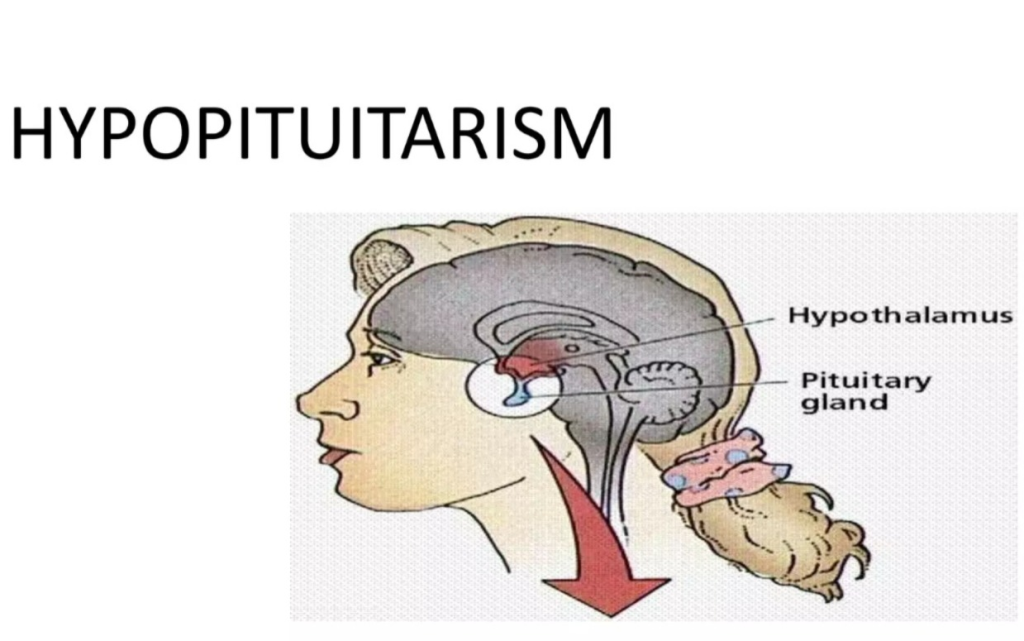
- => Hypopituitarism is a disorder of the pituitary gland in which the pituitary gland is underactive.
- { Pitutary gland ( Pitutary gland) :=> Pitutary gland is called the master endocrine gland ( master endocrine gland ) which is present at the base of the brain. ( Pitutary gland present at the base of the brain) Pitutary gland secretes many hormones of the body and works to regulate body functions (growth, metabolism, regulations, and many other vital functions).}
- => Hypopituitarism is a condition in which the secretion of one or more hormones of the pituitary gland occurs in an inadequate amount (low amount).
- => This is a condition that mainly affects the anterior lobe of the pituitary gland.
- => the hormone that are produced by the pituitary gland may be affected in hypopitutarism are:=
- 1) ADRENO CORTICOTROPHIN HORMONE ( ACTH ),
- 2)ANTIDIURETIC HORMONE (ADH) ,
- 3)FOLLICAL STIMULATING HORMONE (FSH) ,
- 4) THYROID STIMULATING HORMONE ( TSH) ,
- 5)LEUTENIZING HORMONE (LH) ,
- 6)GROWTH HORMONE (GH) ,
- 7)PROLECTINE ..
2) Explain the Etiology/cause of hypopituitarysam. Give the causes of hypopituitarism.)
1) Due to tumor of pituitary gland
- Pituitary gland tumor (benign:= non cancerous) or malignant (malignant:= cancerous) causes suppression of pituitary gland and impaired hormone production.
2) Pituitary infraction (pitutary infraction/sheehans syndrome) :=
- => This is caused by insufficient blood supply to the pituitary gland.
- => This is mainly seen during childbirth and is caused by excessive blood loss.
- => This causes pituitary necrosis and hormone deficiency.
3) Pituitary trauma:
- => Head injury or trauma can also affect the pituitary gland and cause hormonal deficiency.
4)Infection and inflammation: =
=> Impairment in pituitary gland hormones is also seen due to any brain infection.
- 5) Due to any autoimmune disease condition.
- 6) Due to radiation therapy.
- 7) Due to surgery.
- 8) Due to genetic abnormality.
- 9) Due to some types of medication (like := corticosteroids).
- 10) Due to pituitary ED.
- 11) Due to postpartum hypopituitarism (due to severe blood loss during childbirth, the pituitary gland is damaged.
3)explain the Clinical manifestation of hypopitutarisam. Describe the symptoms and signs of hypopituitarism
1)due to thyroid stimulating hormone deficiency:=
- weight gain,
- Bradycardia,
- Hypotension,
- sensitivity to cold,
- Depletion of energy,
- muscles weakness,
- Hair loss,
- Dry skin,
- Hoarseness,
- Growth retardation is seen in children.
2) due to ACTH Deficiency:=
- Feel tired,
- pallor ,
- Not feeling hungry,
- Weight less To be,
- Dizziness,
- Weakness,
- Depression,
- nausea,
- vomiting,
- shock,
- Hypoglycemia,
- Anemia,
- Hyponatremia,
3)due to gonadotrophin deficiency:=
- Irregular menstrual periods,
- dyspareunia,
- infertility,
- osteoporosis (fragile bone),
- delayed puberty in children.
4) due to growth hormone deficiency:=
- Fatigue,
- Shortening of height,
- Low energy,
- Growth retardation,
- visceral obesity,
- decrease muscles mass and strength,
5)due to deficiency of prolectin hormone.
- Decreased milk production,
- Feel tired,
- loss of underarm and pubic hair,
6)due to deficiency of ADH( anti diuretic hormone) :=
- 2p syndrome:=
- =>Polyuria ,
=>Polydypsia . - Decreased urine osmolarity.
- Hypernatremia.
4) Explain the diagnostic evaluation of hypopituitarism. Write a diagnostic evaluation of hypopituitarism.
- history tacking and physical examination,
- serum ACTH test,
- Serum cortisole test,
- serum Estrogen test,
- serum folicule stimulating hormone test,
- serum folicule stimulating hormone test,
- serum luteinizing hormone test,
- X Ray,
- ct scan,
- MRI,
- blood test,
- vision test,
- stimulating or dynamic testing.
5) Explain the management of hypopituitarism. (Write the management of hypopituitarism.)
- If there is adrenocorticotropic hormone deficiency (ACTH Deficiency) in the body, then corticosteroid (ex:=prednisone, hydrocortisone) medicine should be provided to the patient.
- If there is a decrease in thyroid stimulating hormone (TSH deficiency) in the body, then levothyroxin (Levothyroxine) medicine should be provided to the patient.
- If the patient If there is antidiuretic hormone deficiency ( deficiency of ADH ), then provide Desmopressin medicine.
- Desmopressin is available in the form of nasal spray, oral tablet and injection.
- If the patient has growth hormone deficiency ( deficiency of GH ), then provide Genotropin and Humatrope medicine.
- If the patient has sex hormone deficiency ( deficiency of sex hormone), then testosterone replacement therapy (Testosterone replacement therapy) and Estrogen replacement therapy should be provided.
explain the nursing management of patients with hypopitutarisam Write the nursing management of patients with hypopituitarism
1)Disturbed body image related to changes in to the hormones of the body.
- Ask the client to explain his feelings.
- Provide psychological support to the client.
- Ask the patient to describe any issues he is facing.
- Ask the client to improve his coping abilities.
2)Anxiety related to changes in to the health status of patients.
- Provide comfort to the client.
- Ask the client to do some moderate activity.
- Provide education to the patient on relaxation techniques.
3)Impaired skin integrity related to declining hormone level.
- Provide education to the patient for regular skin care.
- Instruct the client to use a moisturizing lotion.
- Instruct the client not to scratch the skin.
- Ensure the patient has plenty of fluids Tell.
- Ask the patient to do range of motion exercises.
- Provide education to the patient on regular skin care.
4)ineffective individual coping related to the disease condition .
- Ask the client to explain his feelings.
- Provide education on how the patient can solve his problem.
- Provide education on relaxation techniques to the client.
5)low self esteem related to changes in to the body apperience.
- Building a proper nurse-patient relationship with the patient.
- Providing psychological support to the client.
- Involving the client’s family members in their care.
- Asking the patient to explain his feelings.
- Tell the patient to improve his coping abilities.
1)explain Acromegaly. Define acromegaly
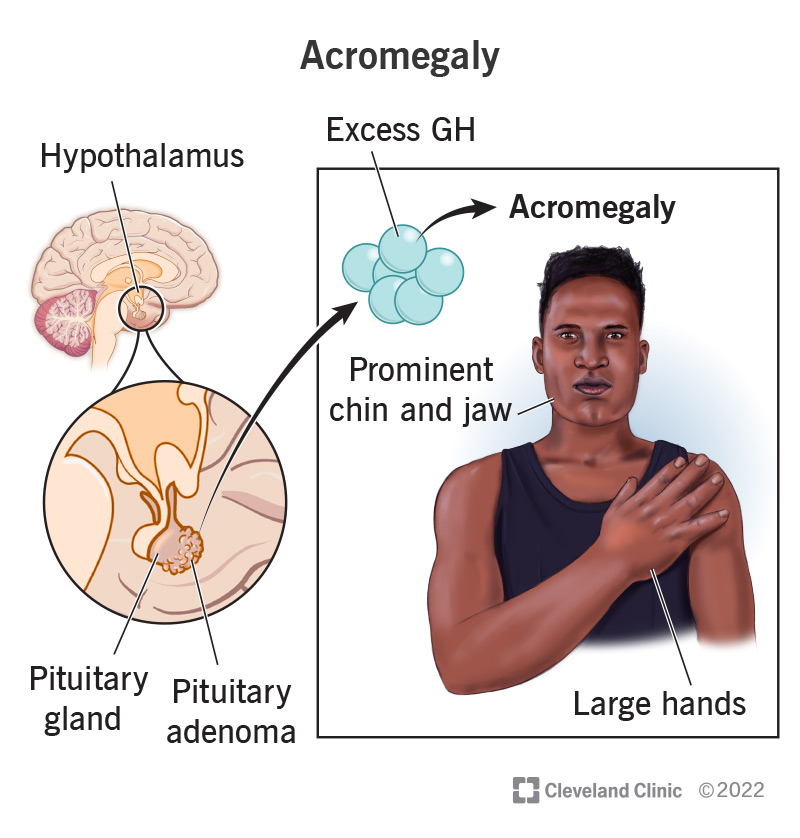
- => Acromegaly is a word derived from the Greek word vada.
- =>Acromegaly means := “extrimities ” And “enlargement “
- => Acromegaly is a chronic metabolic disorder in which too much growth hormone is secreted from the pituitary gland.
- ( Acromegaly:= means secretion of too much growth hormone from the pituitary gland. )
- => Acromegaly occurs after the epiphyseal plate has closed.
- => Acromegaly is characterized by bone thickening and transverse growth.
- => It is mainly seen in men and women between the ages of 30 and 50.
- => Acromegaly is a pituitary gland disorder, which is caused by the secretion of excessive amounts of growth hormone from the pituitary gland. And the body’s extremities grow in an excessive amount.
2)explain the Etiology of Acromegaly.
=> Give the causes of acromegaly.
1) Pituitary tumor :=
- => Due to the presence of a tumor in the pituitary gland, the pituitary gland is pressurized, due to which the hormone of the gland is secreted in excessive amounts.
2)Non pituitary gland tumor :=
- => In many people, Acromegaly is mainly caused by benign and non-cancerous tumors that spread from other parts of the body.
- => Such as lungs, pancreas and adrenal glands.
3) Excessive production of growth hormone from the pituitary gland.
4) Due to genetic abnormalities.
3) Explain the Clinical manifestation/sign and symptoms of Acromegaly. (Write the clinical manifestations/signs and symptoms of Acromegaly)
- => finger swelling occurs.
- => 👞 shoe size increases.
- => Special features include swelling.
- =>The prominence of the jaw and forehead increases.
- =>The skin of the palms and soles thickens.
- => The tongue swells.
- => Pain occurs in the joint (artheritis := infection and inflammation of joint).
- =>Swelling occurs in the neck.
- =>Appearance of large number of skin tags.
- => Breathing difficulty occurs during sleep time.
- => Pain, numbness and tingling sensation in the hand and wrist (carpal tunnel syndrome).
- => Thirst and urination increase.
- => Body odor.
- => Weakness appears.
- => Height increases significantly.
- => Sweat a lot.
- => Headache.
- =>joint pain.
- =>Increase the size of hand and foot.
4) Explain the diagnostic evaluation of Acromegaly.
- History taking and physical examination.
- X Ray.
- CT scan.
- MRI.
- Echocardiogram.
- IGF-1 and growth hormone level assessment.
- genetic testing.
- visual field testing.
5) Explain the management of Acromegaly. (Write the management of acromegaly.)
surgical management
- The main primary cause of acromegaly is a tumor, so the tumor should be surgically removed.
- Transphenoidal hypophysectomy: In this, the tumor is removed through an incision made through the nasal sinus.
5)Medical management:=
=> When surgery is not possible, it is treated with medication.
1) Somatostatin analoge ( Somatostatin Analog ) :=
=>Octerotide ( Octerotide)
=> Somatostatin analogs reduce growth hormone.
2)pegvisomant (Pegvisomant) Pegvisomant blocks the action of growth hormone.
3)radiotherapy := Radiotherapy is used to reduce the size of the tumor.
4)Dopamine agonist (Dopamine agonist) => Dopamine agonist medicines prevent the release of growth hormone from tumor cells.
Ex:= carbagoline,
lanreotide
6) Explain the nursing management of patients with Acromegaly. Write the nursing management of acromegaly patient.
1) disturbed body image related to enlargement of body part.
- Assess the patient’s body image.
- Provide psychological support to the patient.
2) Fluid volume efficient related to polyuria.
- Assess the patient’s fluid and electrolyte status.
- Provide the patient with oral fluids.
- Provide the patient with intravenous fluids.
3)Disturbed sleeping pattern related to soft tissue swelling.
- Assess the patient’s sleeping pattern.
- Provide the patient with a comfortable position
- Provide the patient with a quiet and comfortable environment to work in.
4) Ineffective coping related to changes in appearance.
- Assess the patient’s coping ability.
- Provide psychological support to the patient.
5) Anxiety related to changes in appearance and treatment.
- Assess the patient’s anxiety level.
- Divert the patient’s attention.
- Assess the patient’s coping ability.
- Provide psychological support to the patient.
6)knowledge deficit related to development of disease and treatment.
- Assess the patient’s knowledge level.
- Explain the patient about progressive features of disorder.
- Clarify doubts in the patient.
1)explain/define the Gigantism. (Define gigantism.)
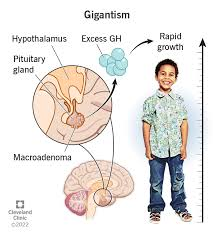
- =>Gigantism is a condition in which the body’s epiphysial plate (bone growth plate) closes. First the body grows abnormally large.
- => It is mainly seen during childhood due to excessive secretion of growth hormone.
2) Explain the Etiology/cause of Gigantism. (Explain the cause of gigantism)
- Due to benign tumor of the pituitary gland.
- Due to excessive secretion of growth hormone.
- Carney complex (Carney complex := This is a hereditary disorder in which pigmentation of the skin is seen.)
- MC cune-albright syndrome (MAS := McCune-albright syndrome is a genetic disorder that mainly affects the bone, skin, and endocrine system. And cafe-au-lait skin pigmentation is seen.)
- multiple endocrine neoplastic type :=1( MEN :=1)
- Multiple endocrine neoplasia is an inherited endocrine disorder in which tumors form in the parathyroid gland, pituitary gland, pancreas ilent.
- Due to exposure to radiation.
3) explain the Clinical manifestation/ sign and symptoms of Gigantism. (Explain the symptoms and signs of Gigantism.)
- Children grow in muscle organ and height.
- Children are seen to grow in height more than their corresponding height.
- Children grow in excessive amount is seen.
- Facial features are seen enlarged.
- Joints are enlarged.
- Enlargement of organs and tissues is seen.
- Puberty is seen delayed.
- Obesity.
- Double vision.
- Frontal bushing and if it becomes prominent.
- Headache.
- Profuse sweating.
- Menstrual periods become irregular.
- Hands and feet become enlarged and fingers and toes become thick.
- Weakness.
4)explain the diagnostic evaluation of Gigantism. Write the diagnostic evaluation of Gigantism.
- history tacking and physical examination.
- ct scan.
- MRI.
- Assessing productin levels.
- Assess the insulin growth factors (igf-1) level.
- assess the cortisole level.
- Assess the estradiol level (in girls). assess the Testosterone level ( in boys).
- Do a thyroid function test.
explain the nursing management of patients with Gigantism
- If there is a tumor in the pituitary gland, it should be surgically removed.
- surgery like:= transphenoidal hypophysectomy. hypophysectomy (hypophysectomy) .
medical management
( somatostatin analoge) Somatostatin analoge
- =>Somatostatin analoge is used to reduce the secretion of growth hormone Dopamine agonist ( dopamine agonist := carbagoline, bromocriptine).
- Used to reduce growth hormone.
growth hormone antagonist ( ex:= pegvisomate ( Peguisomet))
- => This medicine reduces the effect of growth hormone.
- provide Radiation therapy to the patient.
- Providing radiation therapy can cause learning disabilities, obesity, and emotional changes in children, so radiation therapy is provided only if surgery and medication fail.
Nursing management of patients with Gigantism Write the nursing management of patients with Gigantism
1) Health assessment:=
- => Take a comprehensive medical history of the patient.
- => Assess the patient’s physical status, emotional status, and psychological status.
- => Assess the patient’s growth pattern.
2)Psychological support:=
- Provide psychological support to the patient and his family members.
- Improve the patient’s coping ability.
- To clear all the doubts of the patient and his family members.
3)Education
- To provide complete information about the disease to the patient and his family members.
- To provide complete information about the disease, its causes and its treatment to the patient and his family members.
4) Medication management
- Complete information about the medicine, its dose, route and signs and symptoms to the patient and his family members.
5) Monitoring and documentation.
- Continuously monitor the patient’s condition.
- Continuously monitor the signs and symptoms of the patient’s disease condition.
6)Nutritional counselling:=
- Patient’s Continuously monitor nutritional status.
- Collaborate with dietitian to provide education on healthy diet habits for the patient.
7) Joint care:=
- Ask the patient to take continuous care of the joint.
- If the patient is in pain, provide medicine to relieve the pain.
8) Coordination of other health care provider:=
- Collaborate with other health care personnel for the care of the patient and provide adequate treatment to the patient.
9)for health promotion:=
- To promote the health of the patient, ask him to do regular exercise.
- Tell the patient to have healthy dietary habits.
- Tell the patient to take a well-balanced diet.
- Tell the patient to make changes in lifestyle.
1)Explain/define pituitary gland tumor. (Define Pituitary Gland Tumor.)
- => Pituitary gland tumor is an abnormality of the pituitary gland, in which abnormal growth and uncontrollable mass (abnormal growth and uncontrollable mass)
like structures develop in the pituitary gland and form a tumor. - => Many types of tumors cause excessive production of pituitary hormones. And the pituitary gland hormone is produced in greater quantities.
- =>While many types of tumors restrict the pituitary gland hormone and due to this, the pituitary gland hormone is produced in lesser quantities.
2) Explain the division of pituitary gland tumor. (Write the division of pituitary gland tumor)
=>Tumor of pituitary gland is divided into three parts ##
=> 1)benign pituitary adenomas (benign pituitary adenomas)
=> 2) Invasive pituitary adenomas
=>3)pitutary carcinomas
=> 1)benign pituitary adenomas
- => This tumor is not cancerous.
- => This tumor grows slowly, and does not spread from the pituitary gland to other parts of the body.
- there are other two types of benign pituitary adenomas
- There are two other types of benign pituitary adenomas:=
A)secreting pituitary adenoumas (secreting pituitary adenomas)
- ==> Secretory adenomas are tumors in which the pituitary gland produces excessive amounts of hormones than normal.
B)Non-secretory pituitary adenomas (non-secreting pituitary adenomas)
- ==> In non-secreting adenomas, the pituitary gland does not produce hormones in excess of the normal amount.
( don’t produce excessive amount of pituitary gland hormone).
=> 2) Invasive pituitary adenomas
- => In this, the benign tumor in the invasive pituitary adenomas tumor spreads to the skull bone.
=>3)pitutary carcinomas (pituitary carcinomas)
- => Pituitary carcinoma tumors are cancerous/malignant tumors.
- => These tumors spread to other parts of the central nervous system (brain and spinal cord) and can also spread to other parts of the body outside the central nervous system.
- => Many pituitary tumors are malignant. Pituitary gland tumors are nonfunctioning and functioning.
=> 1)functioning
- => A functioning pituitary tumor is a tumor that produces excessive amounts of pituitary hormones compared to the normal amount.
=>2) Non-functioning pituitary tumor
- => A non-functioning pituitary tumor produces an inadequate amount of hormone compared to normal production.
3) Explain the Etiology/cause of pitutary gland tumor. Explain the causes of pituitary gland tumor
- Idiopathic (actually cause is unknown).
- Due to genetic abnormality.
- Due to family history.
- Multiple endocrine neoplasia type-1
- Carney complex
- somatic mutation
- => Somatic mutations are seen due to any abnormality.
- due to Hormonal imbalance.
- Radiation exposure
- There is a chance of developing a pituitary tumor due to exposure to ionizing radiation in childhood.
- due to Age and gender.
3)explain the sign and symptoms/clinical manifestation of pitutary gland tumor. (Explain the sign and symptoms/clinical manifestation of pitutary gland tumor.)
- => Pituitary gland tumor damages the surrounding parts of the pituitary gland tumor due to its formation, so its function is impaired.
- Headache,
- Difficulty seeing,
- Body hair loss occurs.
in women :=
- =>Menstruation cycle becomes irregular.
- => Milk production decreases.
in man :=
- => Facial hair is lost.
- => Breast tissue growth occurs.
- in women and men lower sex drive.
- => Growth and development in children are reduced.
★To much ACTH (Adreno Corticotrophin Releasing Hormone) may cause:=
- Headache.
- Loss of vision.
- cushing syndrome: =
- • Round face (moon face),
- • Weight gain,
- • Facial hair increase,
- • Trunk enlargement,
- • Extremity thinning,
- •buffelo hump ( बुफेलो हुम्प:= collection of fat between the two shoulder blades),
- Skin becomes thin, purple and pink stretch marks appear on the abdomen and chest.
- Anxiety.
- Irritability.
- Depression.
★ too much Growth Hormone ( GH)
- Gigantism,
- Acromegaly,
- Enlargement of the extremities,
- Headache,
- Loss of vision,
- Hands and Tingling sensation in the feet,
- Joint pain,
- Profuse sweating.
★ To much Hyperthyroidism
- Irregular heartbeat,
- Sweating Vomiting,
- Sleep disturbance,
- Weight loss.
★To much prolectin may cause:=
- Headache,
- Vision loss,
- Lower flow of milk.
- Menstruation cycle stops and secretion of breast milk occurs.
- in man have impotency ( loss of ability to have erection).
- Infertility ( infertility).
★ Other anterior pitutary gland tumor:=
- Leutenising hormone and folical stimulating hormone are secreted in small amounts.
- It causes infertility.
★Posterior pitutary gland tumor:=
- diabetes incipidus,
★Other general signs and symptoms are:=
- nausea,
- Vomiting,
- confusion,
- dizziness,
- Seizures,
- “runny” and” drippy” nose.
4)explain the diagnostic evaluation of pituitary gland tumor. (Write the diagnostic evaluation of pituitary gland tumor.)
- health history and physical examination,
- X Ray,
- ct scan,
- MRI,
- Biopsy,
- visual field examination,
- 24 hour Urine test
- Neurological Examination,
- Complete Endocrinological Evaluation,
- Blood Chemistry Study,
- Venous Sampling for Pituitary Gland Tumor,
- Visual Field Examination,
- Electrocardiogram,
- Radiological examination,
- 24 hour urine test,
- lumber puncture ( spinal tap),
5)explain the management of pitutary gland tumor. Management of Pituitary Gland Tumor Write
surgical management
- To remove the tumor through surgery in pituitary gland tumors.
- Transphenoidal hypophysectomy
if small tumor := perform endoscopy
if large tumor : =perform craniotomy
medical management
Active surveillance:=
- => A person with a pituitary tumor needs to be provided with active treatment.
- => Close observation of a person with a pituitary tumor.
Radiation therapy:=
- In radiation therapy, high energy x rays are used to kill the tumor.
- External beam radiation therapy is used in radiation therapy.
- chemotherapy (chemotherapy) Chemotherapy uses medicine to remove cancerous tumors.
- When chemotherapy is provided through medication and injections, it is called systemic chemotherapy.
- Chemotherapy provided directly into the cerebrospinal fluid, abdomen, and body cavity is called regional chemotherapy.
medication (medication)
- Provide hormonal replacement therapy to the patient.
- Replacement of thyroid hormone,
- Replacement of adrenal hormone,
- Growth hormone Replacement,
- Testosterone in men,
- Estrogen in women,
- bromocriptine and carbegoline medicine should be provided to the patient.
octeripeptide :=
should be used for the patient with pituitary tumor that secretes thyroid stimulating hormone.
6) Explain the nursing management of patients with pituitary gland tumor
1)provide education to the patient :=
- Ask the patient to limit their activity temporarily.
- Explain to the patient the need for follow-up visits.
- Provide education to the patient about radiation therapy and follow-up after surgery.
- Provide education to notify the health care provider immediately if the patient has a condition of thyroid and cortisol imbalance.
2)therapeutic regiments:=
- Provide education to the patient about hormonal replacement therapy.
- Educate the patient Provide information on the signs and symptoms of thyroid and cortisol hormone deficiency and, if present, notify the health care provider immediately.
- Demonstrate the correct method of administering the prescribed medication to the patient.
3) Care of patients after resection of pituitary tumor:=
1)maintain Airway of patients
- => The patient’s airway should be kept properly patent.
- => Suction the patient’s mouth and throat to keep the airway patent.
- => Gently percuss the patient’s chest.
- => Administer oxygen to the patient.
2)Neurological status:=
- => Continuously monitor the neurological status of the patient.
- => To monitor the patient’s vital signs.
3)monitor intracranial pressure:=
- => Continuously monitor the patient’s intracranial pressure.
- => Provide the patient with a neutral position.
- => Assess the patient for any signs and symptoms of increased intracranial pressure.
Such as
• Restlessness,
• Visual disturbances,
• Headache,
• Vomiting,
• Seizures,
• Palpitations.
- Administer minitol if intracranial pressure is increased.
4) Continuously monitor the patient’s glucose level Do.
5) Assess the patient for any signs and symptoms of meningitis.
- • Headache,
- • Stiff neck,
- • Fatigue,
- • Confusion.
6) Assess the patient’s serum electrolyte level.
7) Continuously monitor the patient’s urine output.
8) Continuously monitor the patient’s serum sodium level.
9) Provide intravenous fluid to the patient.
10) Continuously monitor the patient’s intake output chart Monitor.
11) Monitor the patient’s laboratory investigations.
- hypokalemia,
- hypophosphatemia,
- hypoalbuminemia,
12) Assess the patient’s cerebrospinal fluid To do.
13) Assess the patient’s protein level.
14) Monitor the patient’s glucose level.
15) Perform arterial blood gas analysis (ABG testing) of the patient. To assess respiratory parameters in it.
