ENGLISH-diges disor part 2
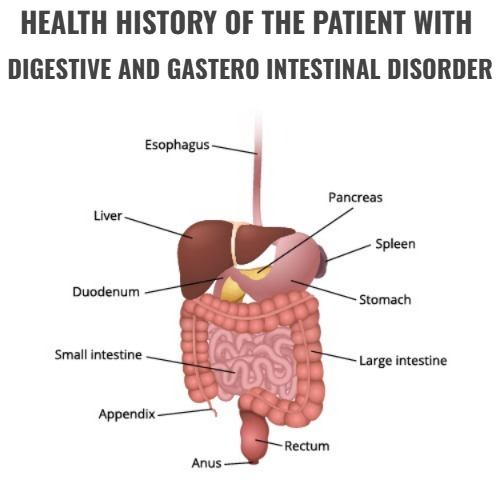
History and Physical Assessment of the patient with the Digestive and gastero intestinal Disorder.
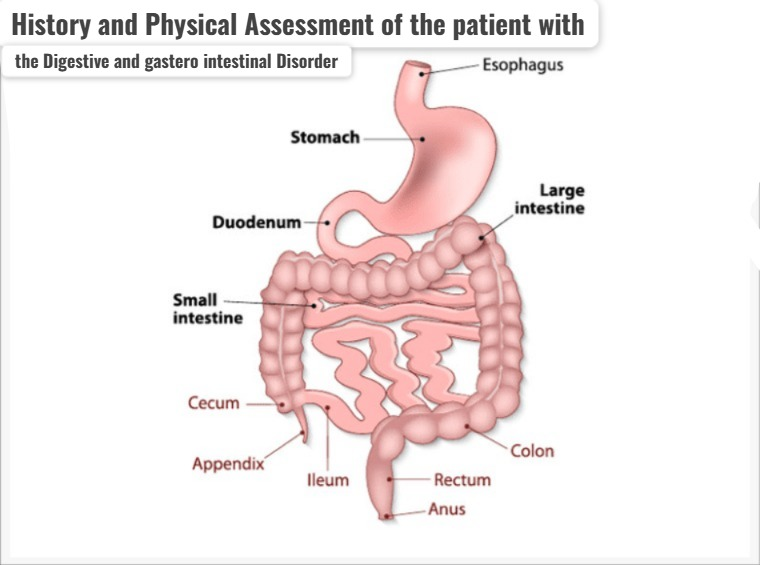
HEALTH HISTORY OF THE PATIENT WITH DIGESTIVE AND GASTERO INTESTINAL DISORDER (Write the health history of the patient with digestive and gastrointestinal disorder):
- To know the health status of a person, it is very important to take his/her proper health history.
- Health history includes information about the patient, which includes the patient’s diet, his/her lifestyle, his/her habits, if any previous medication is being taken, if any previous medical reports have been made, and if he/she has any such family history, all this information is included in the health history.
1)Assess the patient presenting complaint:
- In this history, information is obtained about the patient’s present abdominal pain, abdominal bloating, gastroesophageal reflux, nausea, and changes in bowel habits.
2)Symptomatology:
- In this symptomatology, the onset of the signs and symptoms, their period, their frequency, their duration, and which factors increase the signs and symptoms, and which factors decrease the signs and symptoms, are obtained from the patient.
3)Tacking Dietary history of the patient. (Take the patient’s dietary history.)
- In this history, get information about the patient’s dietary habit and what kind of diet the patient has taken, the patient’s dietary pattern.
4) Assess the Bowel habit of the patient (ask for information about the patient’s bowel habit).
- Get information about the patient’s normal bowel habits and any changes in them. Get information from the patient about the stool, its frequency, and its consistency.
5) Explain the Medical history of the patient. (Get a complete medical history from the patient.)
- Get complete information from the patient about past and current medical conditions and any medications and any surgeries if any.
- Ask the patient whether he has had any diseases of the gastrointestinal system in the past and whether he is taking any medications for any diseases, get complete information from the patient.
6) Explain about the medication history. (Collect information about the patient’s medication history.)
- In this, if the patient is taking any medication, and if the patient is taking any over the counter (over the counter) medication, if the patient is taking any vitamin supplements, then get complete information about it.
7) Obtain the family medical history:
- This Ask the patient’s family members about any gastro intestinal track related diseases in the history and get complete information about whether any person has had gastro intestinal track diseases in the past.
- Get complete information about whether any person has genetic diseases.
8) Assess the social history:
- Assess the patient’s lifestyle factors. Such as getting information about stress level, physical activity, and sleep pattern.
- Get complete information about whether the patient smokes and consumes alcohol or not because smoking and alcohol consumption greatly affect the digestive system.
9) Psychosocial factor (getting complete information about the patient’s psychosocial factor):
- Get complete information about the patient’s stress level and emotional well-being.
10) Assess the Allergies and sensitivity of patients. (Getting information about the patient’s allergies and sensitivities.)
- Getting information about whether the patient has allergies and sensitivities to any food and medication.
11) Screening of Risk Factors. (Screening for risk factors)
- Getting information about the patient’s risk factors, including age, sex, and any other health history, and getting them screened.
- By getting this comprehensive information about the patient, the patient’s present complaint and problem can be identified and information about what type of risk factor is there and what type of treatment the patient needs to be provided.
- While taking the patient’s health history, the patient To provide complete information so that the patient can be provided with complete medical treatment for whatever disease condition he/she may have.
Physical examination of the patient with digestive and gastero intestinal Disorder. (Write the physical examination of the patient with digestive and gastero intestinal Disorder.)
- A physical examination involves examining the patient’s mouth, abdomen, and rectum.
- A physical examination can help determine the patient’s health status and provide information about what type of treatment should be provided to the patient.
- The patient’s oral cavity is assessed through the inspection method.
- In which the patient’s mouth, tongue, teeth, and gums are examined for any ulcers, nodules, swelling, Inspection is done to assess for conditions such as discoloration and inflammation.
The gastrointestinal tract is physically examined using four methods.
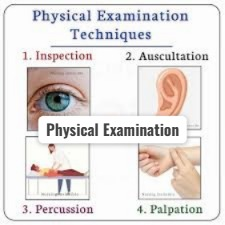
- 1) INSPECTION (inspection: by eyes (visual examination)),
- 2) AUSCULTATION ( by the stethoscope),
- 3) PERCUSSION ( Percussion : percussion with the use of finger tips ),
- 4) PALPATION (palpation: by the palpate the organ by the finger pad)
1) INSPECTION (Inspection: by eyes (Visual examination)),

- Assessment of the intestinal system starts with the oral cavity.
- The lips are examined to assess whether there is any lesion, abnormal colour, and any abnormality in the lips.
- The oral cavity is inspected for any inflammation, tenderness, ulceration, swelling, bleeding, and discoloration.
- The patient’s breathing is assessed to determine whether there is any abnormal order.
- If there is any foul order (foul odor) coming from the patient’s oral cavity, it is an indication of infection and impaired Oral care is indicated.
- The tongue is examined to assess for any signs of dehydration.
- The patient’s gums are assessed for any swelling or redness.
- The patient is placed in the supine position and then the patient’s abdominal cavity is inspected to assess for any redness, irregularities, scars, cracks, or other abnormalities in the skin.
2) AUSCULTATION (Auscultation : By the stethoscope),
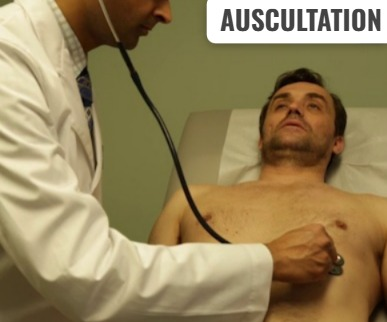
- When a patient’s abdomen is auscultated, first place the stethoscope in the upper right quadrant of the patient’s abdomen and then listen to the sounds of the patient’s abdomen in a clockwise direction.
- To listen to the patient’s bowel sounds, the stethoscope is placed lightly on the abdomen.
- Bowel sounds are soft clicks and gurgles that are heard over the abdomen every 5 to 15 seconds.
- Bowel sounds are assessed in all four quadrants of the abdomen using the diaphragm of the stethoscope.
- When bowel sounds are heard through a stethoscope, a high pitch gurgling sound is most often heard.
- Bowel sounds are mainly heard due to peristalsis movement in the bowel.
Types of the bowel sound are (Type of the Bowel Sound Is) :
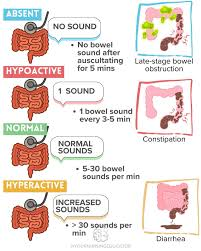
1) Normal bowel sound,
- Normal bowel sounds are heard every 5 to 20 seconds.
2) Hyperactive bowel sound,
- Hyperactive bowel sound is heard five to six sounds in less than 30 seconds.
3) Hypoactive bowel sound,
- One to two sounds are heard every two minutes.
4) Absent bowel sound.
- Not a single sound is heard every three to five minutes.
Hyperactive bowel sounds ( Hyperactive Bowel Sounds) :

- Hyperactive bowel sound is a rapid, high-pitched, bowel sound that is mainly heard when there is gastroenteritis.
Hypoactive bowel sound ( Hypoactive Bowel Sound) :

- Hypoactive bowel sound is mainly seen when there is paralytic ilius and It is mainly infrequent, as it is heard after any abdominal surgery.
3) PERCUSSION ( Percussion : by the percussion with the use of finger tips. )

- Percussion is performed to identify the density of an organ.
- Percussion is primarily performed to detect any fluid, air, and masses present and is used to identify the size and location of organs in the abdominal cavity.
4) PALPATION ( Palpation: by the palpate the organ by the finger pad ),
- Lightly palpating the body with the finger pads can assess whether there is any tenderness and swelling in the abdominal area.
Diagnostic evaluation of the patient with Digestive and Gastrointestinal Disorder. (Diagnostic Evaluation of a Patient with Gastrointestinal Disorders)

1)Endoscopy (Endoscopy) :
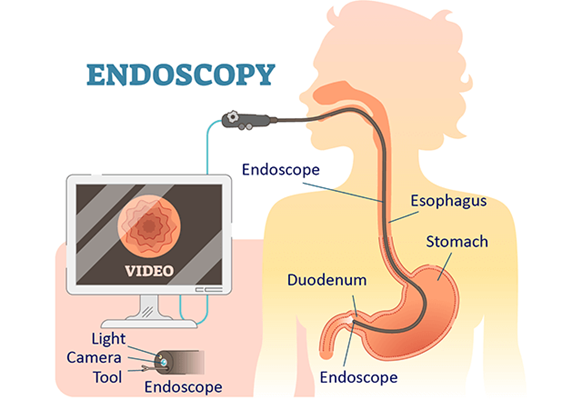
- Direct visualization of the lumen of the gastro intestinal tract in endoscopy Examination is performed.
- The endoscope consists of a flexible tube and a light at its front side through which proper visualization of the gastrointestinal tract can be done.
- The length of the endoscope is 140 centimeters.
- The upper gastrointestinal tract is examined through the endoscope.
2)Gastrocopy :
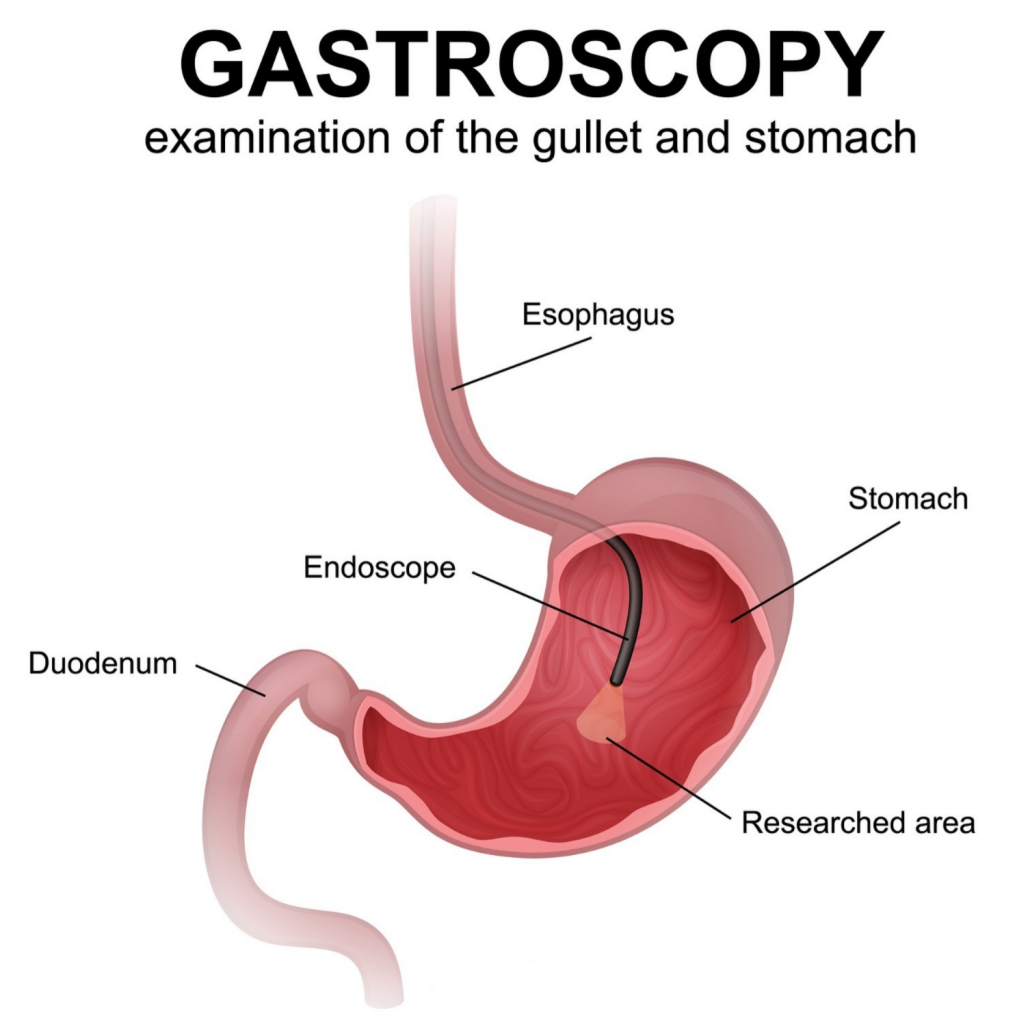
- Gastroscopy or esophago-gastro-duodenoscopy is a diagnostic test that involves visual examination of the inside of the esophagus, stomach, and duodenum.
- Gastroscopy involves passing a flexible endoscope, less than 10 mm in diameter, directly into the upper gastrointestinal tract and then visualizing the proximal duodenum. In this, the entire esophagus, stomach, and proximal duodenum can be directly visualized.
3) Colonoscopy :
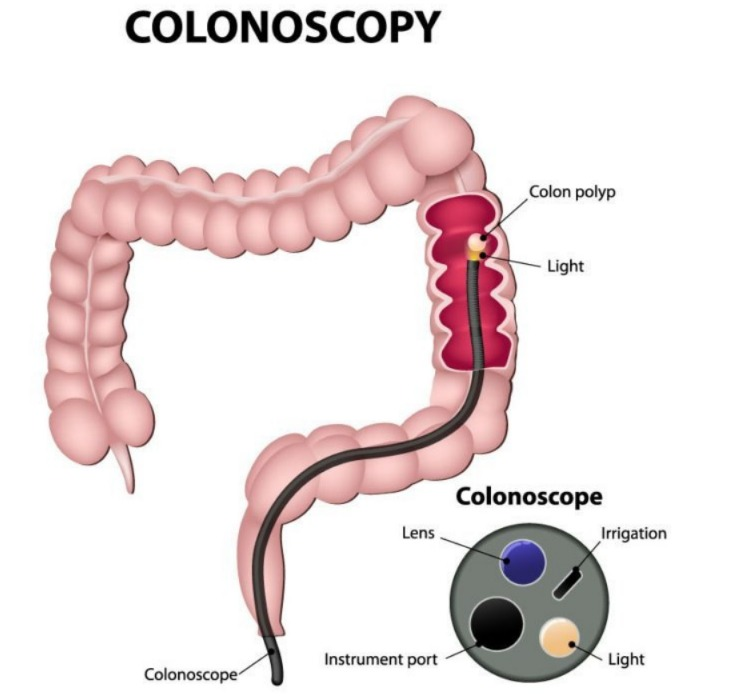
- A colonoscopy is an examination of the lower gastrointestinal tract, which includes the entire colon and rectum.
- A colonoscope is a 1.2 to 1.8 m long instrument. Nu has.
4) Procto Sigmoidoscopy:
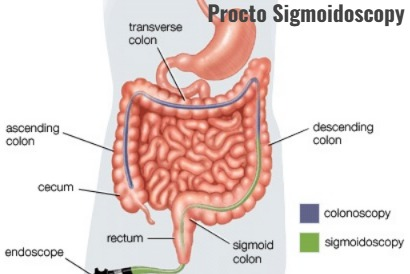
- In proctosigmoidoscopy, the rectum and sigmoid colon are examined using a proctoscope.
- The proctoscope is 25 to 30 centimeters long and has a diameter of 1.5 cm.
- In proctosigmoidoscopy, a visual examination of the anal canal can be performed.
- Proctosigmoidoscopy is performed to detect melaena, persistent diarrhea, and passage of mucous. Bacteriological and histological studies are performed.
5) Flexible sigmoidoscopy:
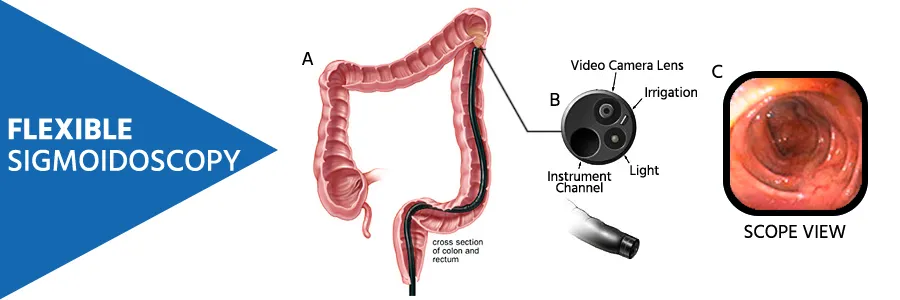
- Flexible sigmoidoscopy uses a flexible instrument to visualize the rectum, sigmoid, and proximal colon.
- The length of the flexible sigmoidoscope is 65 centimeters.
- Flexible sigmoidoscopy is more tolerant than protosigmoidoscopy.
Radiological investigation of patient with digestive and gastro intestinal Disorder. (Write a radiological investigation of a patient with digestive and gastrointestinal disorders):

Radiological investigation includes (Radiological Investigation) :
1)Barrium swallow,
2)Barrium enema,
3)Upper gastero intestinal series.
4)Abdominal Ultrasound ( Abdominal Ultrasound).
5) CT (Computed Tomography) scan ( Computed Tomography Scan)
- All of these radiological investigations are used to assess abnormalities of the gastrointestinal tract.
- Barium studies are better tolerated than endoscopic investigations.
- Radiological studies use barium as a contrast medium.
- Barrium is a chalky, non-allergic substance that is used to visualize the esophagus, stomach, and lower gastrointestinal tract. examination can be done.
- Barium preparations are mainly administered orally or rectally, but their use is contraindicated in patients with suspected gastro intestinal obstruction or perforation.
- If the patient does not pass the barium within 48 hours of barium administration, the nurse should provide the patient with appropriate enema and laxatives to relieve the patient’s constipation and obstruction.
1) Barium swallow:
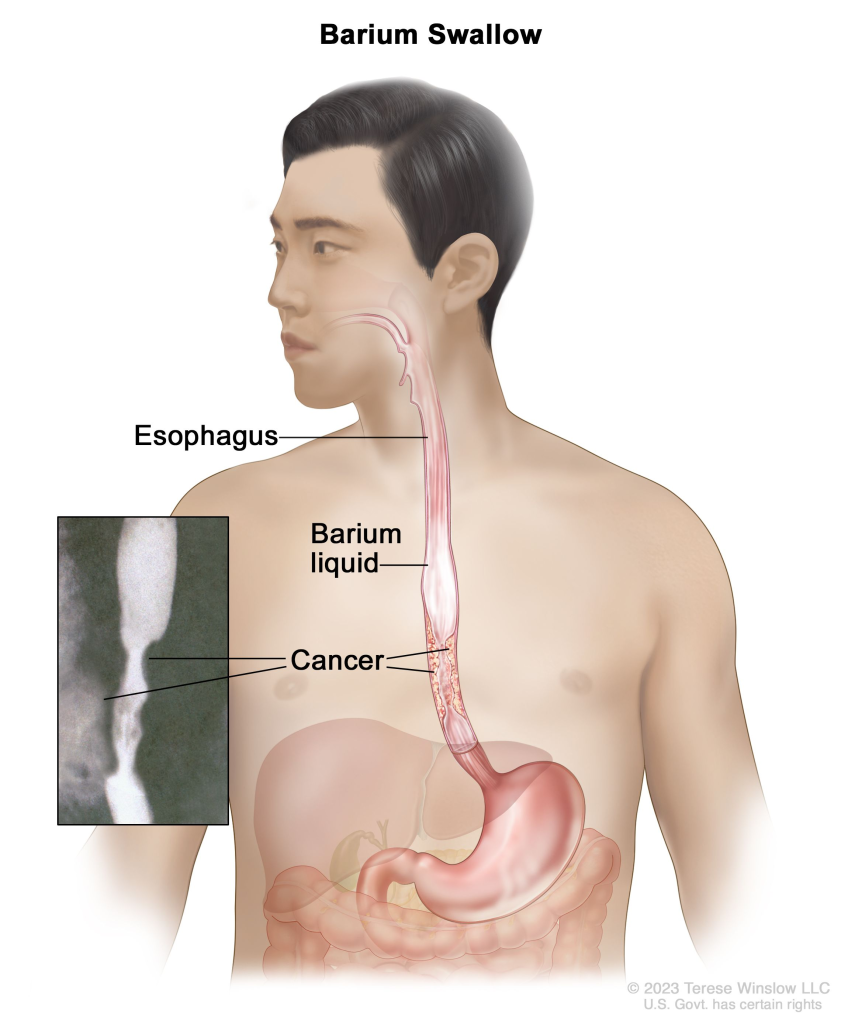
- Radiological of esophagus in barium swallow Examination is performed
- This procedure is used to diagnose whether there is any stricture present in the esophagus, any motility disorder, any ulceration, and whether there is a foreign body present.
- Barium swallow is less sensitive than endoscopy for making any diagnosis.
- Barium swallow should be avoided in people who have a condition called dysphagia (difficulty in swallowing).
2) Barium enema (in barium enema),
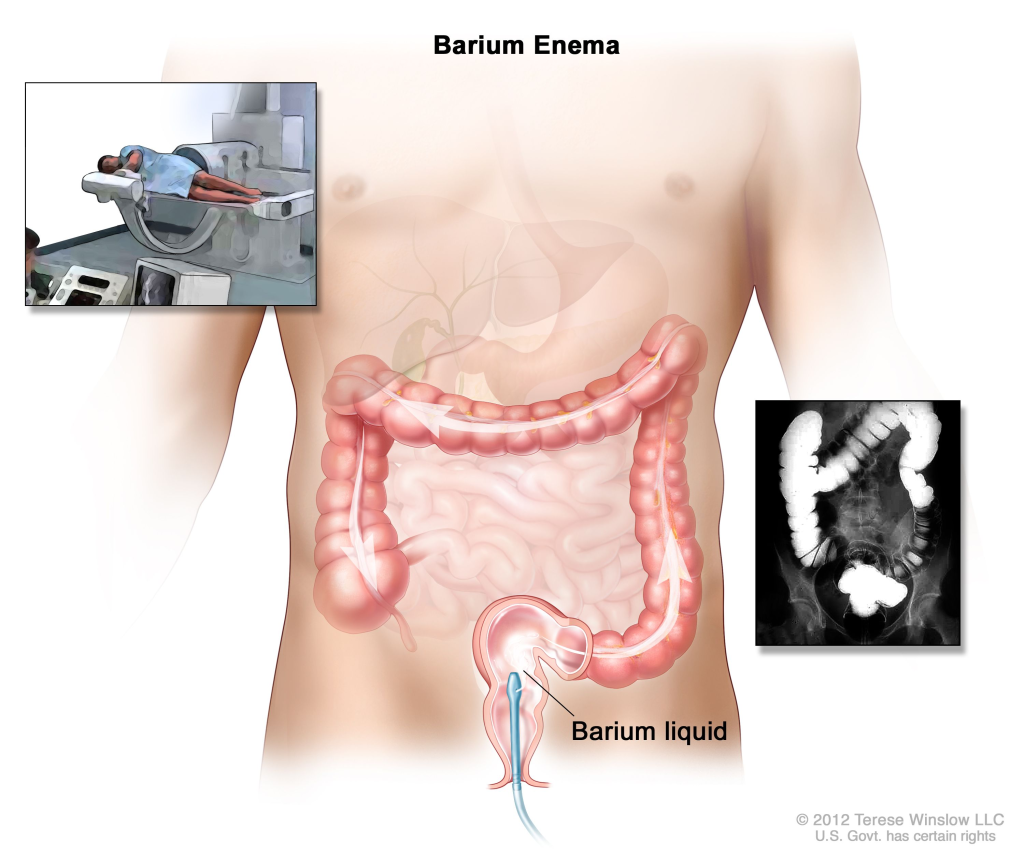
- A barium enema is a radiological examination of the colon (large intestine).
- A barium enema is primarily used to diagnose any
- polyps,
- diverticula,
- any structural abnormality of the colon,
- colorectal cancer and inflammatory bowel disease. It is used to detect bowel disease.
3)Upper gastro intestinal series. (Upper Gastrointestinal Series).
- Upper gastrointestinal series mainly involves radiological examination of the stomach and small intestine, in which A barium solution is injected.
- This procedure is used to examine any diverticula, strictures, hiatus hernias, obesity disorders, tumors, Crohn’s disease, and malabsorption syndrome.
4) Abdominal Ultrasound. (Abdominal Ultrasound).
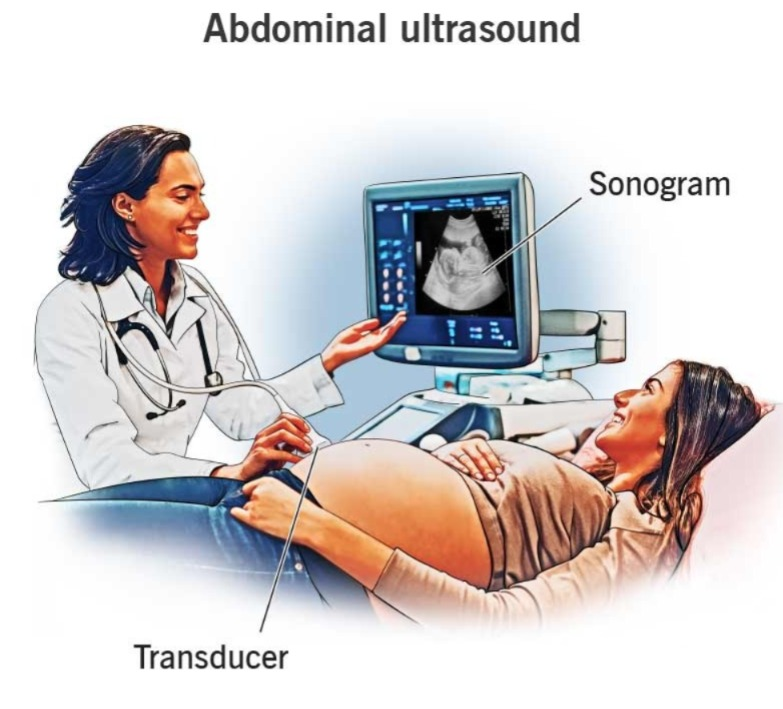
- Abdominal ultrasound is a procedure that is used to indicate the size and shape of the body’s organs. It is used.
- It is used to diagnose any abnormality of the abdominal cavity.
- The investigation is done using sound waves.
- It is mainly used to diagnose any stone present in the abdominal cavity, and the condition of cholecystitis.
5) CT (Computed Tomography) scan:
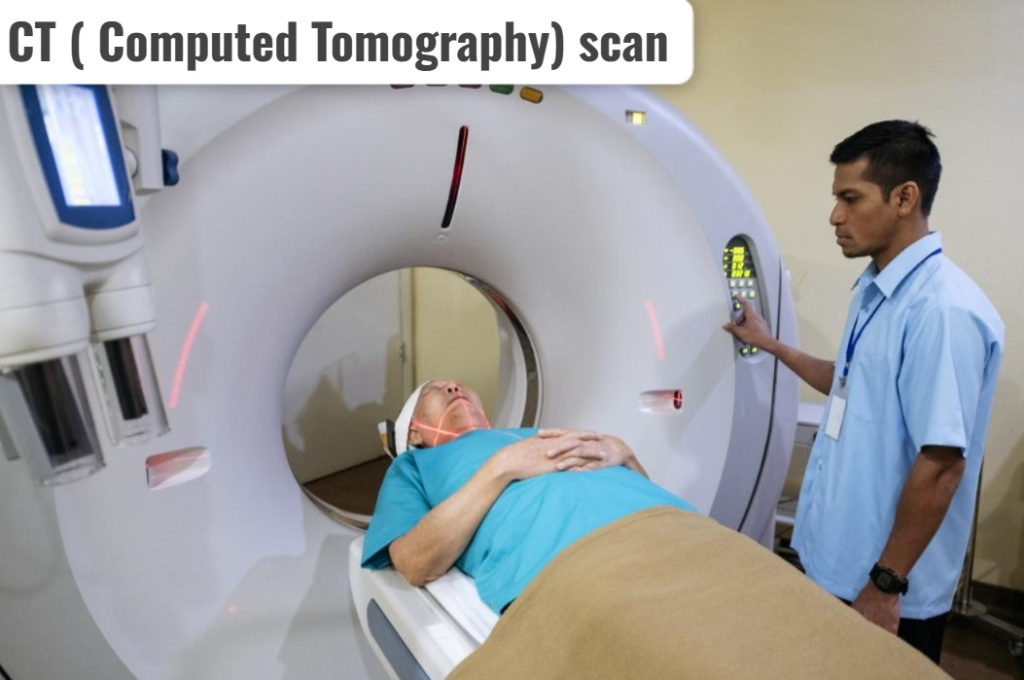
- CT scan is a non-invasive radiological scan.
- It provides more accurate images of body tissues than ultrasound and is mainly used to detect any disease condition of the liver, spleen, kidney, pancreas, and pelvic cavity.
- CT scan is mainly used to detect inflammatory conditions of the colon, such as,
- Appendicitis,
- Regional enteritis,
- Ulcerative colitis is also used to diagnose the condition.
Other investigation includes (Other Investigations Include):
1) Hematological and Biochemical test:
- Mainly in this test
- RBC (red blood cell),
- Hb, serum iron test,
- Iron binding capacity,
- Serum B12,
- Mcv (mean corpuscular volume),
- Serum albumin,
- Serum Electrilyte
- etc tests are done.
2) Stool examination:
- Stool examination assesses the consistency of the stool, whether there is blood present in the stool, whether there is any abscess, and the color of the stool.
- When the stool is examined under a microscope and if pus is seen in the stool, then any condition of Bacillary dysentery or inflammatory bowel disease is detected.
3) Gastric Acid Secretion (Gastric Acid Secretion) Secretion):

- Gastric acid secretion is a condition that determines whether there is any ulcer formation in the stomach and any malignancy. It is used to assess.
1) Explain/Define the Cheilitis. (Define cheilitis).
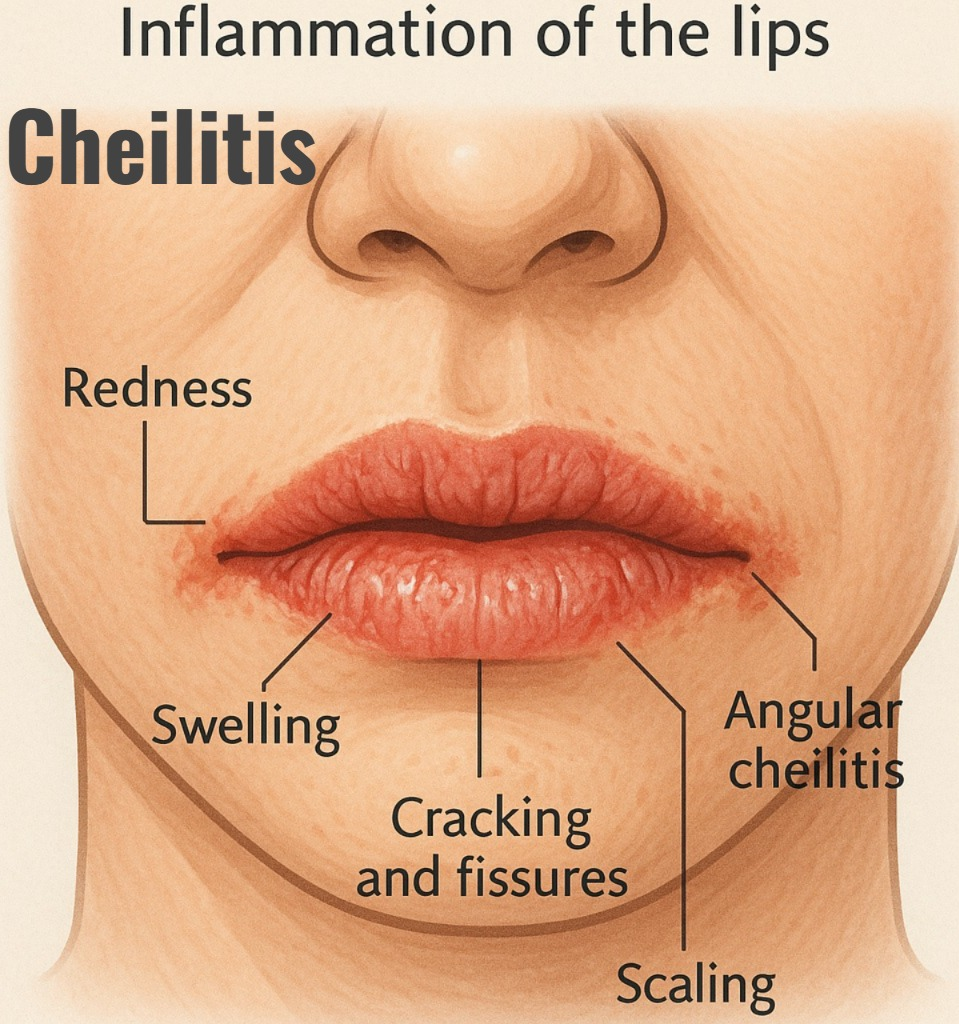
- Chilitis is a medical condition in which the lips become infected and inflamed.
- Chilitis is caused by dryness due to any infection, allergic condition, and any disease condition.
- Cheilitis causes redness, swelling, dryness, and cracks in the lips.
There are 6 (Six) Different types of cheilitis:
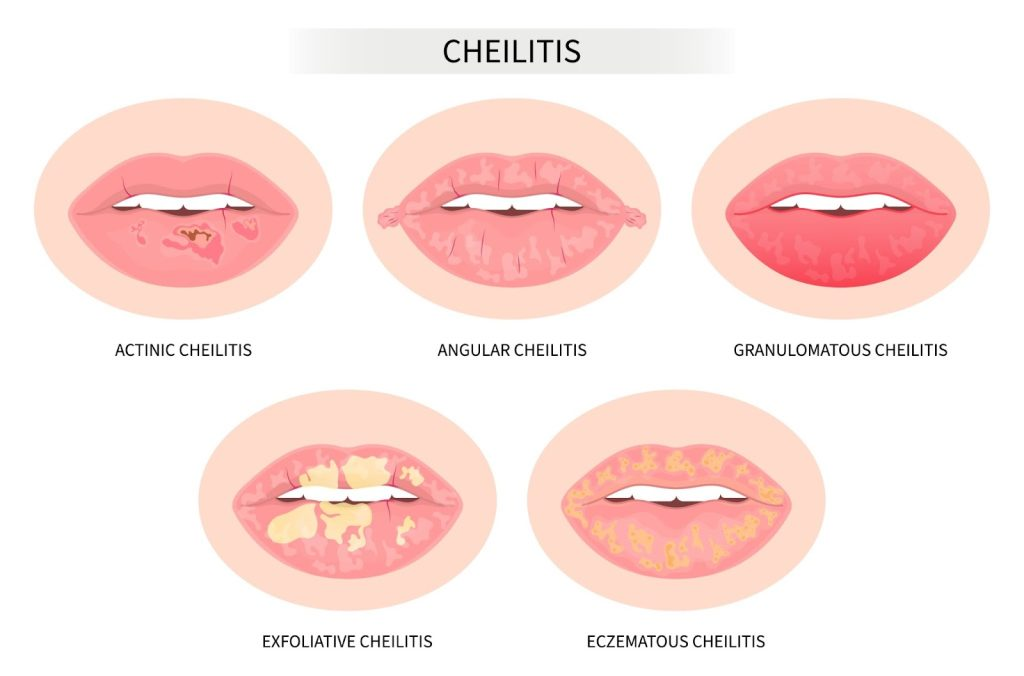
1) cheilitis exfoliative,
2)Allergic contact cheilitis ,
3)Actinic cheilitis ,
4)Cheilitis Grandularis ,
5)Angular chelitis ,
6)plasma cell chelitis ,
1) explain/define cheilitis exfoliative,
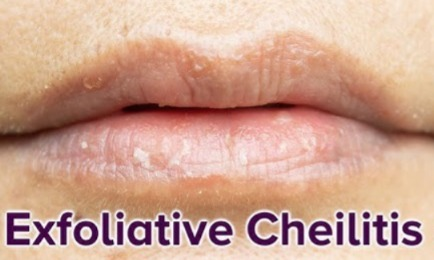
- Exfoliative cheilitis is an inflammatory condition of the lips in which the lips are covered by a crust.
- Exfoliative cheilitis involves continuous peeling and shedding of the outer part (vermillions) of the lips.
- This only affects the one lip (mainly lower lip).
2) Explain the etiology of exfoliative cheilitis. (Explain the causes of exfoliative cheilitis)
- Due to infection.
- Due to bacterial infection.
- Due to fungal infection.
- Lip licking or biting.
- Due to psychological factors.
- Due to anxiety.
- Due to stress.
- Due to psychological conditions.
- Due to exposure to allergens.
- Due to irritating substances.
- Due to autoimmune disease conditions.
- Due to deficiency of certain vitamins and minerals.
3)explain the Clinical manifestation / sign and symptoms of exfoliative cheilitis.
- The skin of the lips is continuously peeling and shedding.
- Redness and inflammation are seen in the lips,
- Lips become dry,
- cracking of the lip’s skin,
- Burning sensation in the lips.
- Discomfort.
- Pain in the lips,
- Difficulty in eating.
- Difficulty in speaking.
- Tingling sensation in the lips.
- Itching and dryness in the lips is.
- fissuring ,
- ulceration,
- unplesant appearance is seen.
4)explain the Diagnostic evaluation of exfoliative chelitis. (Write the diagnostic evaluation of exfoliative chelitis)
- History taking and physical examination,
- swab of the infection,
- biopsy,
- Patch test if any Allergic condition to the patient.
- Psychological assessment of patient.
5) Explain the treatment of exfoliative chelitis. (Write the treatment of exfoliative cheilitis)
- Tell the patient to apply keratolytic lip balm to the lips.
- Tell the patient to apply sunscreen.
- Tell the patient to apply antifungal cream.
- Tell the patient to apply topical and systemic steroids. Tell.
- Tell the patient to apply antibiotics.
- Tell the patient to undergo cryotherapy.
- Tell the patient to apply topical tacrolimus and calendula officinalis (marigold) ointment 10%.
- If the patient has cheilitis due to a fungal infection, provide antifungal treatment.
- If the patient If there is any psychological disorder, provide antipsychotic medication.
1) Explain/define Allergic contact cheilitis
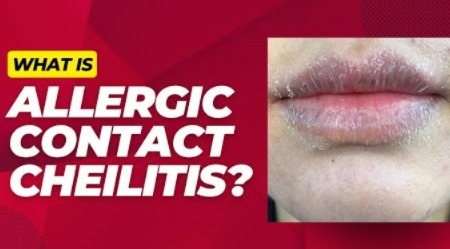
- Allergic contact cheilitis is an infection and inflammation of the lips caused by contact with any allergic substance. It is called allergic contact cheilitis.
- Allergic contact cheilitis is a type 4 hypersensitivity reaction that occurs after contact with any allergen.
2) Explain the Etiology/cause of Allergic contact cheilitis. (Explain the cause of allergic contact cheilitis).
- Allergic contact cheilitis is more common in women than in men.
- Anyone can develop allergic contact cheilitis after coming into contact with an allergen.
- Due to lipstick and lip cosmetics.
- Certain types of toothpaste.
- Certain types of dental Due to the use of care products such as mouthwash, denture cleaner, etc.
- Due to contact with certain types of metal objects.
- Due to food,
- Due to medication,
- Due to rubber and latex,
- Nail varnishes,
- Due to medication.
3) Explain the clinical manifestation/sign and symptoms of Allergic contact cheilitis. (Write the signs and symptoms of allergic contact cheilitis)
- eczema-like changes on the vermilion margin or skin around the mouth.
- Redness in the lips.
- Swelling in the lips.
- itching on lips.
- Dry lips to happen.
- Burning sensation in the lips.
- craking on the lips.
- scaling,
- Burning sensation in the lips,
- pain in the lips,
- lip pigmentation,
4) Explain the diagnostic evaluation of Allergic contact cheilitis. (Write a diagnostic evaluation of allergic contact cheilitis).
- history tacking and physical examination.
- patch test.
- (ROAT : Reapeated open application test).
- blood test.
5)explain the treatment of the patient with Allergic contact cheilitis. (Write the treatment of the patient with Allergic contact cheilitis).
- Avoid the things the patient is allergic to.
- Ask the patient to use corticosteroid ointment.
- Provide the patient with antihistamine medication.
- Ask the patient to apply a moisturizer.
- The patient Ask for proper follow-up.
1)Explain/Define Actinic cheilitis.

- Actinic chelitis is known as
- “farmer’s lip ” (farmer’s lip)”
- or “sailor’s lip” (sailor’s lip)”.
- Actinic chelitis is a sun exposure (sun exposure).
- Actinic cheilitis mainly affects the lips, causing thickening whitish discolouration.
- Actinic cheilitis mainly affects the lover lips.
2)explain the Etiology/cause of Actinic cheilitis. (Explain the etiology of Actinic cheilitis).
- Actinic cheilitis is mainly seen after the age of 50.
- Mainly due to exposure to ultraviolet radiation.
- Due to the use of tobacco.
- Due to the use of lip balm.
- Due to poor oral hygienic conditions.
- Due to dentures.
- Due to prosthesis.
- Due to fair skin.
- Due to geographic location (speciall in high level of sun exposure area).
- Age.
- Due to weak immune system.
3)explain the Clinical manifestation/sign and symptoms of the patient with Actinic cheilitis. (Write the clinical manifestations/signs and symptoms of the patient with Actinic cheilitis)
- Actinic cheilitis mainly affects the lower lips.
- Redness.
- Scaling.
- chapping.
- Dryness and scaling of lips.
- Cracking and fissure in lips.
- Swelling of lips.
- White and grayish colour change in the lips.
- Burning sensation.
- Sensitivity to sunlight To be done.
4)explain the treatment of the patient with the Actinic cheilitis .(Write the treatment of the patient with the actinic cheilitis).
- Tell the patient to use a chemotherapeutic agent (5- flurouracil).
- Tell the patient to use a topical immunomodulator.
- Advise the patient for cryotherapy.
- If the condition is very severe, surgically remove the affected tissues.
- Laser therapy is used to destroy abnormal cells.
- The patient should avoid sun exposure.
1) explain / define cheilitis grandularis.
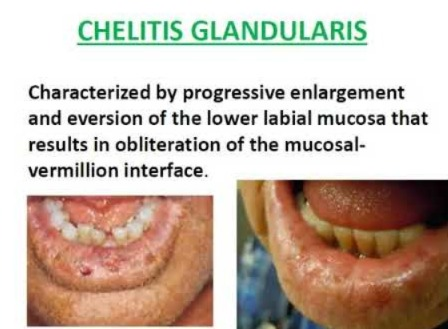
- Cheilitis glandularis is a condition in which there is swelling and eversion of the lower lips.
- Cheilitis glandularis mainly affects the lips and sometimes the face as well.
- Cheilitis glandularis is a chronic inflammatory condition of the lips.
- Cheilitis glandularis is a primarily acquired disorder of unknown cause, characterized by swelling, ulceration, crusting, mucous gland hyperplasia, and sinusitis of the lips. Abscess formation occurs in the tract.
2)explain the Etiology/cause of cheilitis Grandularis. (चेलितिस ग्लेडुलारिस ना कर्नो कर्नो).
- the exact causes are unknown.
- Due to chronic irritation (Due to contact with the cronic irritant materials from the environment).
- Due to obstruction of the salivary gland.
- Due to any bacterial and viral infection.
- Due to genetic factors.
- Due to any autoimmune disease.
- Due to chronic sun exposure.
3)explain the Clinical manifestation/sign and symptoms of the patient with cheilitis Grandularis .(Write the clinical manifestation/sign and symptoms of the patient with cheilitis grandularis)
- Swelling of the lips
- Gradual cheilitis mainly involves swelling of the foreskin, eye lids and scalp.
- excessive dryness of lips,
- cracking and fissuring on the lips,
- pain in the lips.
- inflammation in the lips.
- scallening and peeling of the lips.
- burning sensation in the lips.
- ulceration in the lips.
4)explain the Diagnostic evaluation of the patient with cheilitis Grandularis. (Write the Diagnostic Evaluation of Cheilitis Grandularis).
- History taking and physical examination.
- Assessment of the skin appearance.
- biopsy.
- blood test.
- culture or swab.
- patch test.
5)explain the management of the patient with cheilitis Grandularis. (Explain the management of the patient with cheilitis grandularis).
- If the patient has chelitis grandularis due to any allergic condition, then avoid that allergen.
- Provide the patient with topical corticosteroids.
- Provide the patient with antibiotics.
- Provide the patient with anti-inflammatory medicine.
- Apply topical corticosteroids to the affected area. Administer corticosteroid injections (sulfasalazine, clofazimine).
- Surgically reduce the affected area.
- Instruct the patient to apply a topical moisturizer.
- Provide topical corticosteroids to reduce inflammation.
- Avoid irritating substances such as toothpaste, mouthwash.
- Instruct the patient to maintain good oral hygiene.
- Instruct the patient to drink plenty of fluids to maintain hydration status.
- Instruct the patient to avoid spicy and acidic foods.
- Provide education to the patient to have regular follow-up.
1)explain/define Angular cheilitis.
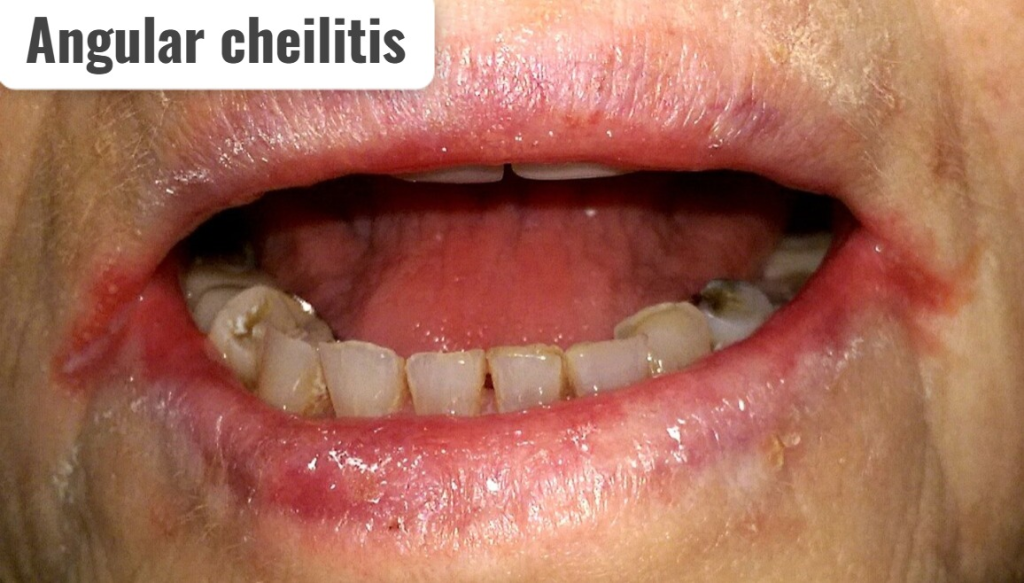
- Angular cheilitis ne ” PERLECHE (Perleche) is called “ .
- Angular cheilitis is an inflammatory condition that mainly occurs in the labial commissure or corner of the mouth, on or above both sides.
- Angular cheilitis causes deep cracks and splints.
- If there is a severe condition, bleeding occurs from these splints.
2) Explain the Etiology/cause of Angular chelitis. (Give reasons for angular cheilitis).
- Due to bacterial infection.
- Due to fungal infection.
- Due to immunocompromise.
- Due to any head and neck radiation exposure.
- Ion deficiency Due to.
- Due to vitamin B12 deficiency.
- Due to folate deficiency.
3) Explain the Clinical manifestation/sign and symptoms of patient with Angular cheilitis. (Explain the Clinical manifestation/sign and symptoms of patient with Angular cheilitis).
- Cracking or fissuring at the corner of the mouth.
- Redness.
- ulceration.
- drainage of pus.
- tissues softness and tenderness.
4)explain the management of the patient with Angular cheilitis
- Tell the patient to apply a topical antibiotic.
- Tell the patient to apply a topical antifungal.
6) Define/explain plasma cell cheilitis
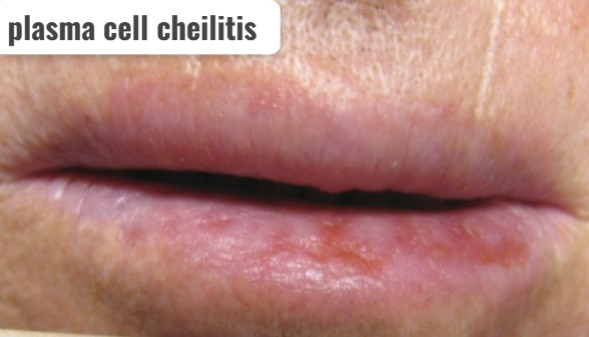
- Plasma cell cheilitis is a condition in which the lips become infected and inflamed.
- It causes Signs and symptoms like erosive, ulcerative, fissuring, bleeding, crusting, and erythematous are seen in the lips.
1) Define/explain parotitis. (Define parotitis).
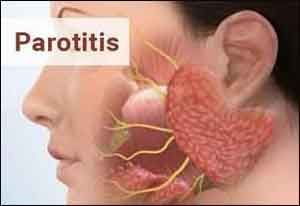
- The parotid gland is the largest salivary gland.
- The parotid gland is located below the ear and near the jaw.
- The parotid gland plays an important role in the production of saliva in the mouth, which plays an important role in the cleansing of the mouth.
- Parotitis is an infection and inflammation of the salivary gland (salivary gland / parotid gland). parotitis).
- Inflammation occurs in one or both parotid glands.
- Due to inflammation, redness, soreness, and swelling are also seen in the tissues surrounding the salivary gland.
- Due to inflammation in the salivary gland, the functional ability of the salivary gland is reduced, which creates an infection in the mouth.
- Thus, When the salivary gland (parotid gland) in the mouth becomes infected and inflamed, it is called “parotitis”.
2)Explain the type of parotitis. (Write the type of parotitis).
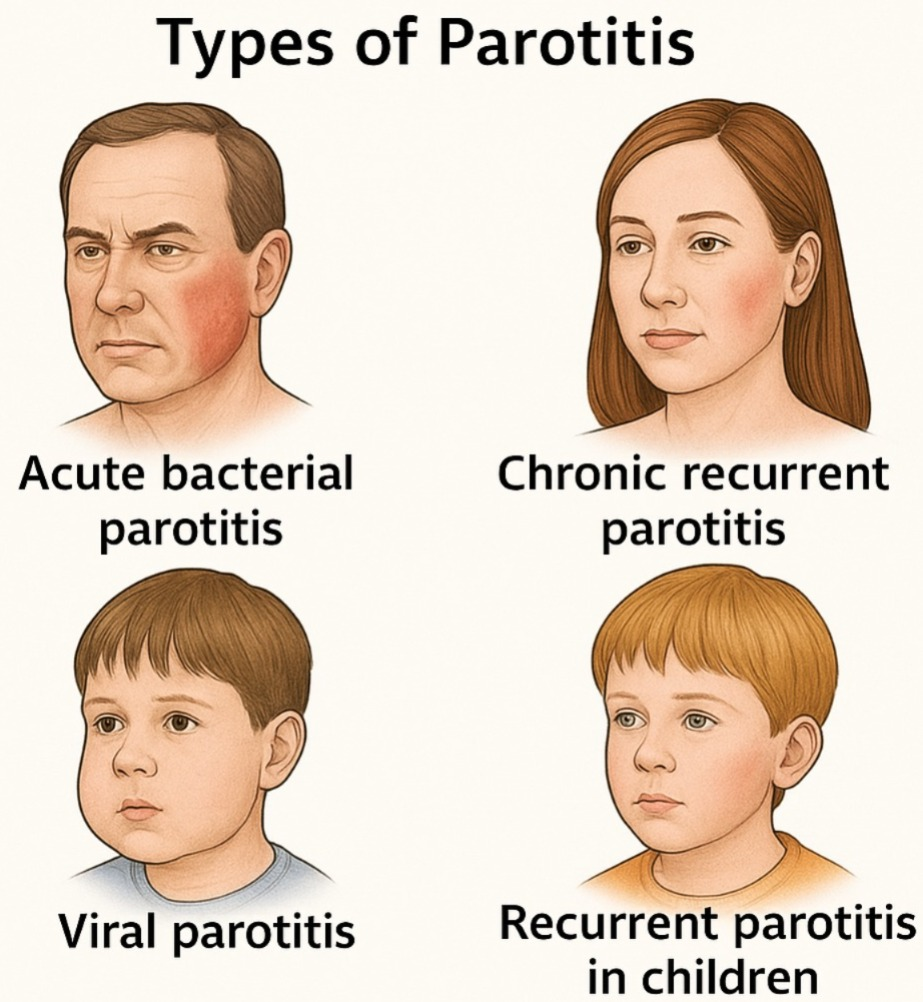
1)Acute bacterial parotitis.
2)chronic Recurrent parotitis.
3)viral parotitis
4)Recurrent parotitis in children
1)Acute bacterial parotitis. (Acute Bacterial Parotitis)
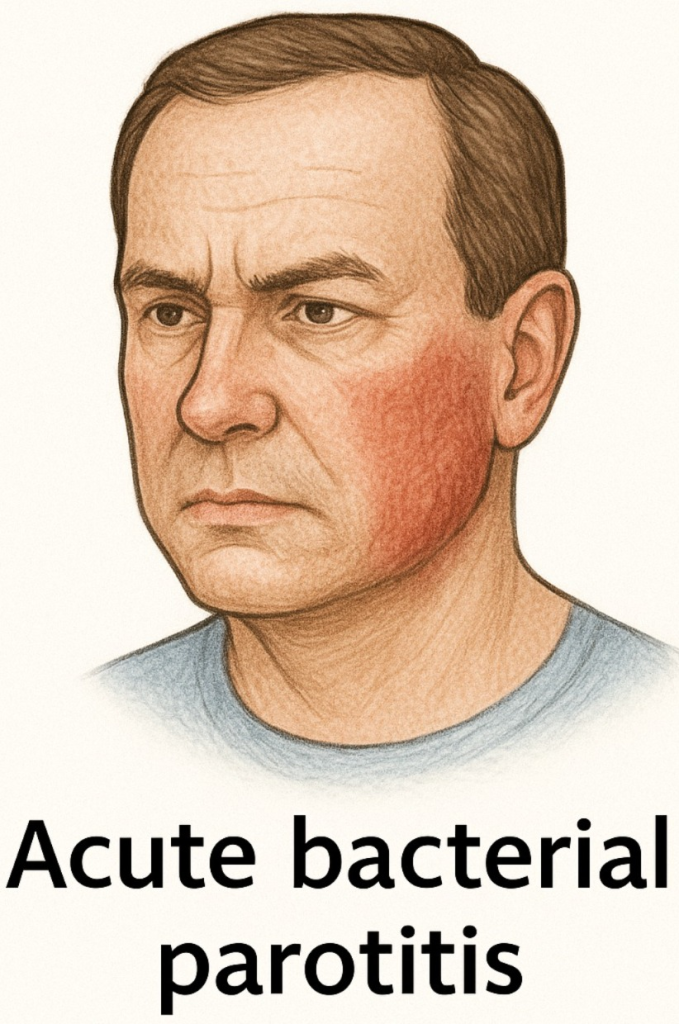
- Acute bacterial parotitis is a sudden and painful swelling of one or both parotid glands. Inflammation of the gland occurs.
- It causes redness, pain, swelling, and tenderness.
- Acute bacterial parotitis is mainly seen in any •>dehydrated patient, •>any postoperative patient, •>after any radiotherapy, and •>a person whose immune system is compromised.
2)Chronic Recurrent parotitis. (Chronic Recurrent Parotitis)
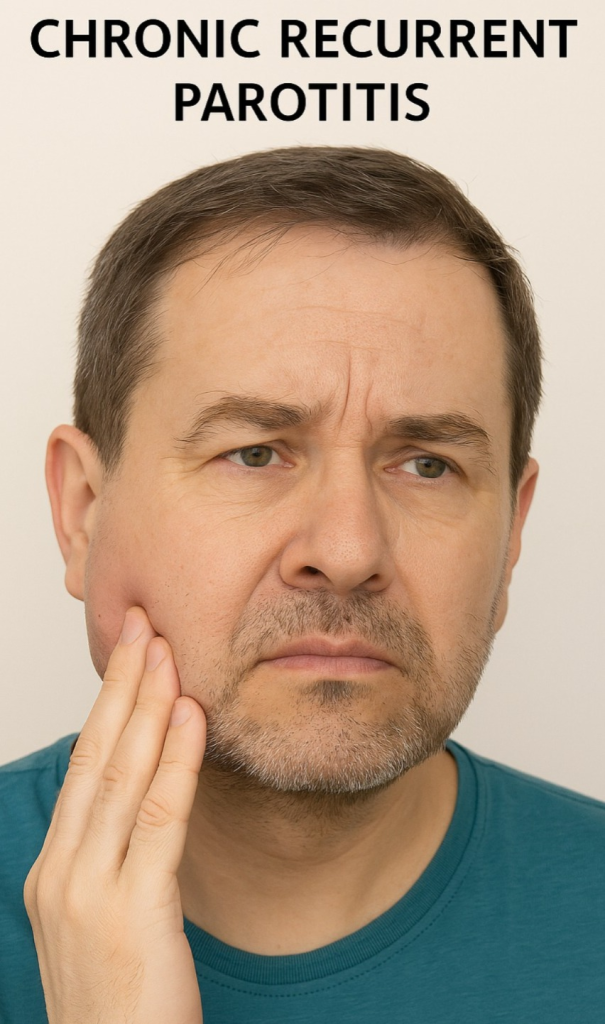
- Parotid gland swelling after eating in chronic recurrent parotitis Repeated episodes of swelling occur.
- Chronic recurrent parotitis is a condition caused by blockage or stricture of any of the salivary glands.
3)Viral parotitis
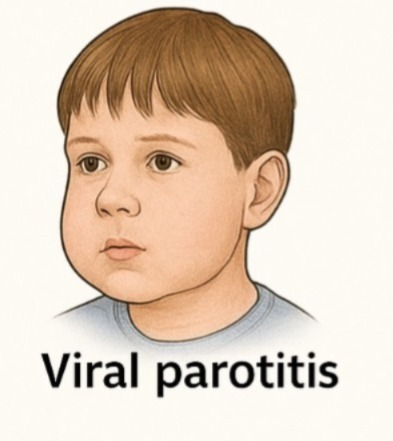
- Viral parotitis is an infection and inflammation of one or both parotid glands caused by any viral infection.
- The most common viral parotitis is caused by mumps.
- ( Mumps is a highly contagious It is an infection that comes from the paramyxovirous family. )
- Viral parotitis causes inflammation of both parotid glands.
4) Recurrent parotitis in children

- Recurrent parotitis in children is mainly caused by Streptococcus bacteria.
- This condition is mainly caused by duct distension and ballooning (ectacia: dilatation and distance of the hollow organ).
- It is mainly self-limiting and does not require surgery. Sometimes there is a need.
2)explain the Etiology/cause of parotitis.
- Due to bacterial infection.
- Due to poor oral hygiene.
- Due to infection.
- Due to certain types of medication.
- Due to radiation.
- Due to any viral infection.
- Obstruction in the salivary glands
- (obstruction)
- Some medications that cause dry mouth, such as antihistamines and cancer treatments.
- Sjogren’s syndrome: Sjogren’s syndrome is an autoimmune degenerative disorder in which the lacrimal gland and salivary gland produce secretions. (due to which there is dryness in the oral cavity and eyes)
- Due to close contact with a person who has mumps infection.
- Due to dehydration.
- If a person has not taken the MMR (mumps, measles and rubella) vaccine.
- Due to dehydration.
- Autoimmune diseases Due to.
- Traumatic and ductal abnormality.
- Due to ductal obstruction.
3)explain the Clinical manifestation/sign and symptoms of parotid gland.
- Swelling,
- Pain,
- Bad taste,
- Dry mouth.
- Bad taste in the mouth.
- Opening the mouth Difficulty occurs.
- Face pain.
- Fever.
- Mouth pain.
- Redness on the side of the mouth.
- Difficulty in breathing.
- Difficulty in swallowing.
- sore throat.
- high fever.
- difficulty swallowing.
- swelling.
- redness and warmth.
- dry mouth.
5) Explain the diagnostic evaluation of the patient with parotitis. Write a diagnostic evaluation of a patient with parotitis.
- history taking and physical examination.
- assess the salivary gland fluid.
- assess the blood test.
- x rays.
- Computed Tomography.
- MRI (Magnetic resonance imaging).
6) Explain the management of the patient with parotitis. Write the management of a patient with parotitis.
medical management
- Provide antibiotic medicine to the patient.
- If the patient has parotitis due to a viral infection, then provide him with antiviral medication.
- If there is an abscess (absence) in the parotid side, then it is surgically aspirated.
- Rinse the mouth with salt water to moisten the mouth (1/2 teaspoon of salt in 1 cup of water).
- Instruct the patient to drink lots of fluids.
- Instruct the patient to use sugar-free lemon drops to increase saliva flow.
- Instruct the patient to maintain good oral hygiene.
- Instruct the patient to brush properly twice a day.
Explain the nursing management of patients with parotitis. Write the nursing management of a patient with parotitis.
- Advise the patient to take food in small amounts.
- Advise the patient to take soft food in frequent amounts.
- Advise the patient to take liquid food.
- Ask the patient to take plenty of water.
- Ask the patient to avoid smoking.
- Ask the patient to maintain oral hygiene.
- Properly immunize the patient with mumps, measles, and rubella (MMR).
- Ask the patient to perform proper hand hygiene before and after defecation.
- Irritant foods such as coffee, spicy foods Advise the patient to avoid spicy foods, as well as hot drinks and hot foods.
- Advise the patient to avoid spicy foods.
- Use lukewarm saline solution to moisten the patient’s mouth.
- Advise the patient to use sugar-free lemon drops to increase saliva production.
- Advise the patient to take a semi-solid diet.
1)Define/explain stomatitis. Define stomatitis.

- Stomatitis is an infection and inflammation of the mucous membrane of the mouth.
- This infection can also extend to the buccal mucosa, lips and palate.
- Stomatitis causes discomfort, pain and soreness in the mouth.
2)explain the types/classification of stomatitis. Explain the classification of stomatitis.
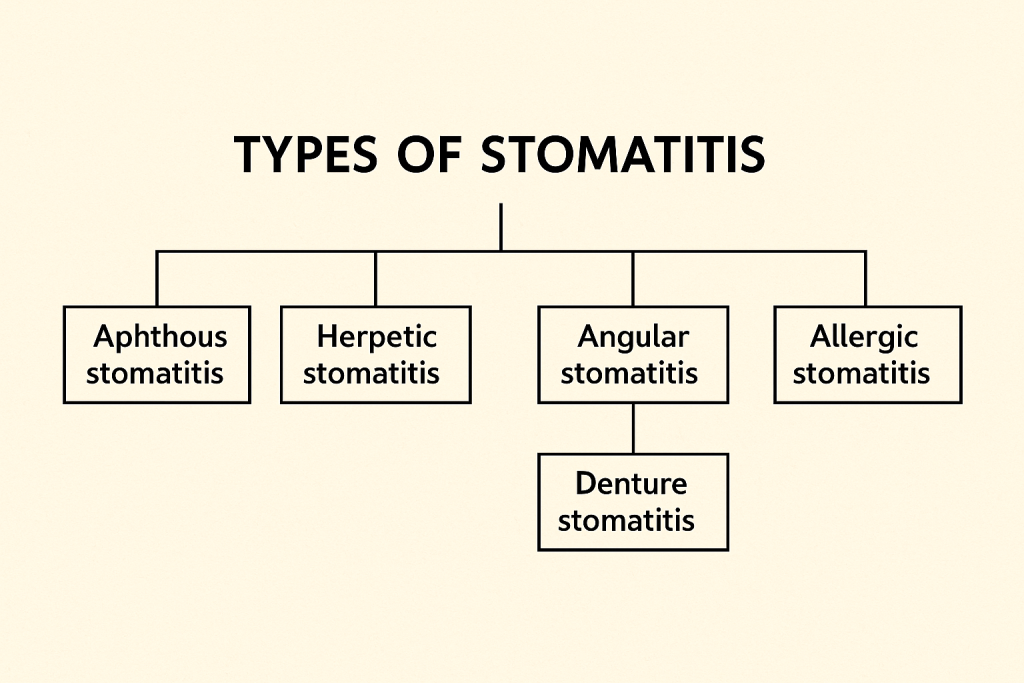
There are a total of five types of stomatitis. are:
1)Acute herpetic stomatitis
2)Aphthous stomatitis
3)Angular stomatitis
4)Nicotic stomatitis
5)Eosinophilic stomatitis
1 ) Acute herpetic stomatitis.
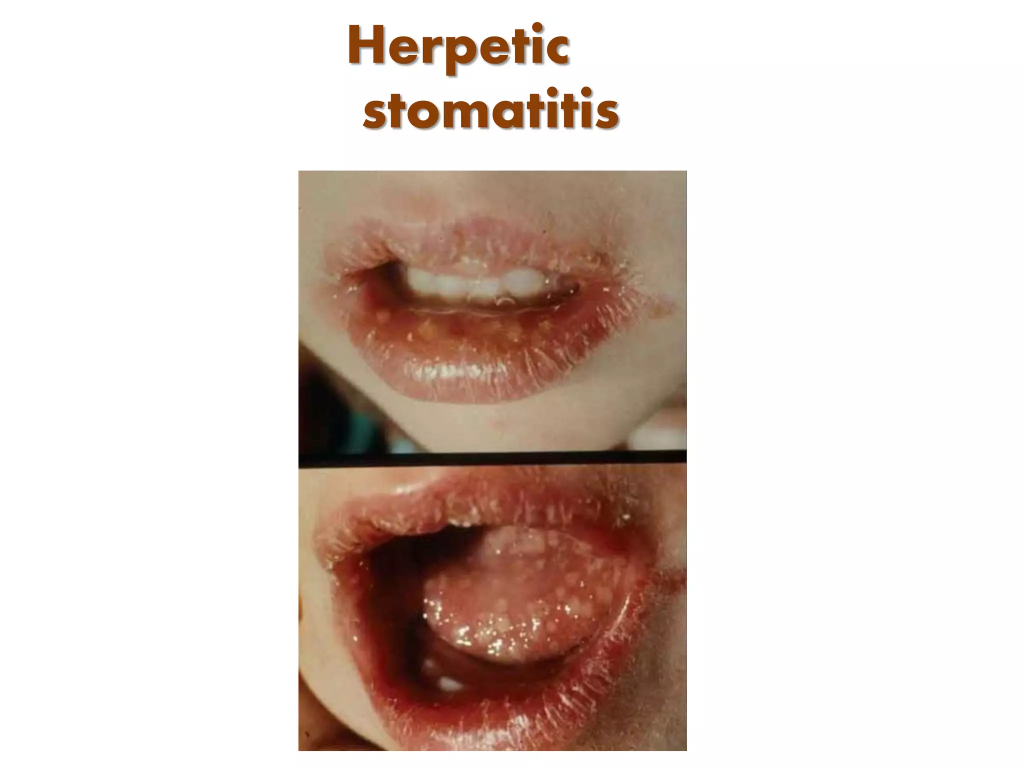
- Acute herpetic stomatitis is caused by the herpes simplex virus.
- Acute herpetic stomatitis Painful sores and ulcers occur in the mother’s mouth.
- Acute herpetic stomatitis is short lived and easily recognised and is severe and is generalised and foetal in the neonate.
2)Aphthous stomatitis.
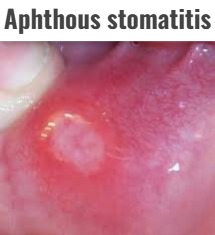
- The cause of aphthous stomatitis is unknown. It causes recurrent, small, painful ulcers in the mouth.
- Aphthous Stomatitis It heals spontaneously and does not form a scar. It heals within 10 to 14 days.
3)Angular stomatitis
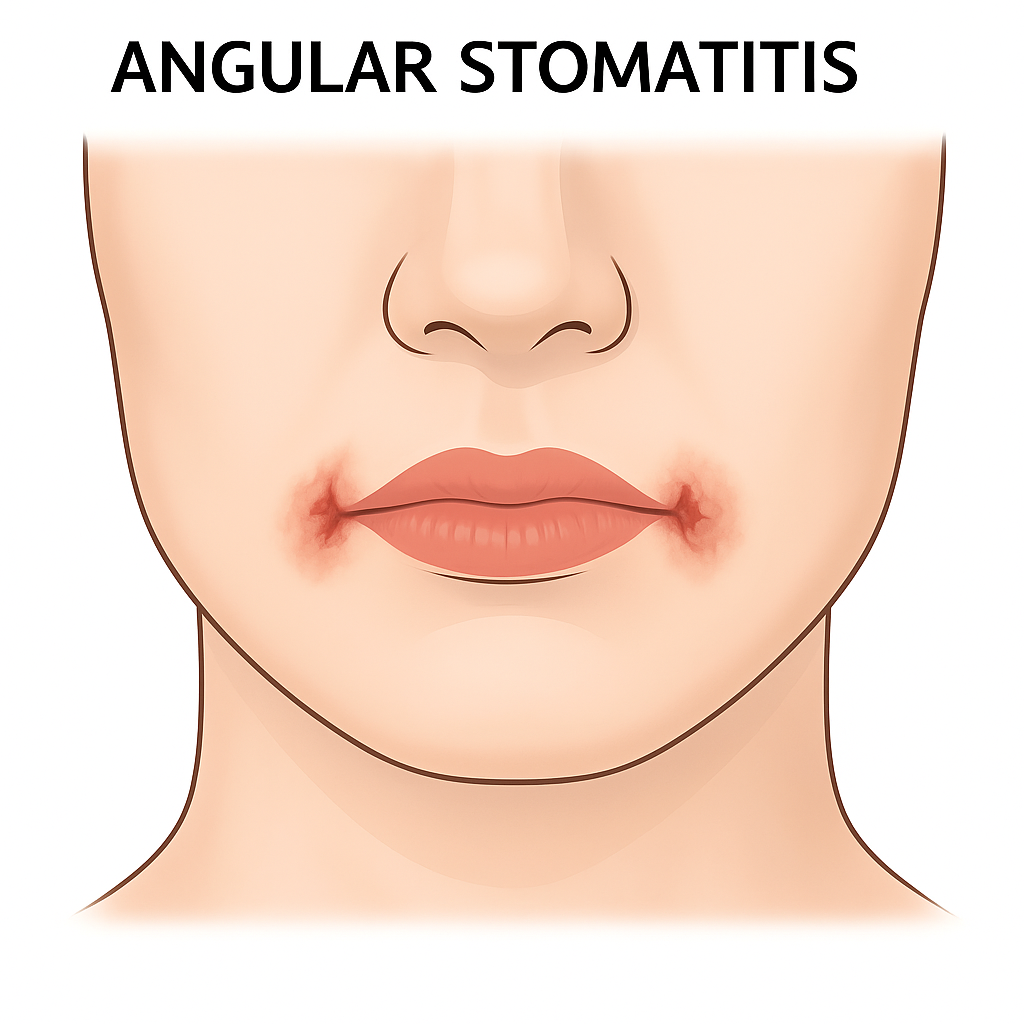
- Angular stomatitis is inflammation and soreness at the corners of the mouth.
- Angular stomatitis is caused by nutritional deficiency and fungal infection.
4)Nicotic stomatitis.
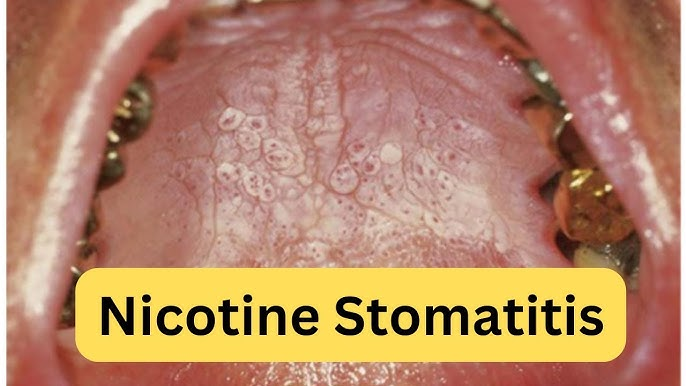
- Nicotine stomatitis is caused by the consumption of tobacco.
- It causes inflammation in the mouth and changes in the appearance of the palate.
5) Eosinophilic stomatitis
- Eosinophilic stomatitis is seen due to an increase in eosinophil count.
- It can be caused by any allergic reaction and Some diseases are caused by conditions.
3)explain the Etiology/cause of the stomatitis. Explain the causes of stomatitis.
- Due to medication.
- Due to poor nutritional habits.
- Due to stress.
- Due to bacterial and viral infections.
- Due to lack of sleep.
- Due to sudden weight loss.
- Due to certain types of food such as potatoes, citrus fruits, coffee, chocolate, cheese and nuts etc.
- Due to immune system weakness.
- Due to hormonal changes.
- Due to low levels of B12, iron and folate.
- Due to genetic abnormalities.
- Due to autoimmune diseases.
- Due to herpes simplex virus.
- Due to any injury in the mouth cavity.
- Due to certain types of allergies (sensitivity to food, fluid, and certain medication).
- Due to chemotherapy.
- Due to radiation therapy.
- Due to tobacco use.
- Due to alcohol use.
4)explain the Clinical manifestation/sign and symptoms of stomatitis. Explain the symptoms and signs of stomatitis.
- The sore is painful.
- There is a burning sensation in the mouth.
- There is a tingling sensation in the mouth.
- The gums become swollen.
- Bleeding from the gums.
- Tenderness in the mucous membrane.
- Papulovesicular ulcer appears in the mouth.
- Redness appears in the mouth.
- Lesion appear into the mouth.
- Single or multiple small, round ulcer with whitish center and red border.
- Inflammation occurs in the mouth.
- Difficulty in eating and drinking.
- Bad breath (halitosis).
- Fever.
- Lymph node swelling.
- Cracking and dryness in the mouth.
5)Explain the Diagnostic evaluation of stomatitis. Write the diagnostic evaluation of stomatitis.
- History taking and physical examination.
- Biopsy.
- Blood test.
- Cultures.
- Imaging studies.
- X rays.
- CT scan.
- Patch test.
- Assess the stomatitis is related to the food.
6)Explain the treatment of stomatitis. Write the treatment of stomatitis.
- Tell the patient to avoid hot beverages.
- Tell the patient to avoid hot food.
- Advise the patient to avoid spicy and salty food.
- If the patient is in pain, provide analgesic medicine.
- Advise the patient to gargle with cold water.
- Advise the patient to drink plenty of water.
- Advise the patient to rinse the mouth with salt water.
- Advise the patient to maintain proper dental hygiene.
- Advise the patient to apply topical anesthetics such as ligbocaine and xylocaine (not provide to the children under 6 years of age.).
- Advise the patient to apply topical corticosteroids such as triamcinolone.
- Advise the patient to apply lidex gel.
- Advise the patient to apply Aphthasole anti-inflammatory paste.
- Advise the patient to apply Peridex mouthwash.
- If the patient has a sore mouth, provide folate and vitamin B12.
- Provide the patient with an anti-inflammatory drug such as a corticosteroid.
- Provide the patient with an antiviral agent (5% acyclovir ointment).
- Advise the patient to apply ice to the lesion.
Explain the Nursing management of patients with the stomatitis. Write the nursing management of a patient with stomatitis:
- Advise the patient to consume citrus fruits and fresh fruits such as apples, grapes, pineapple, peaches, papaya etc.
- Advise the patient to rinse the mouth properly with warm water.
- Advise the patient to avoid alcoholic mouthwash.
- Advise the patient to take a liquid diet, clear liquids, and a bland diet.
- Advise the patient to take whole grains, cereals, raw and lightly cooked vegetables, and seeds.
- Advise the patient to take a high fiber diet such as fruits, vegetables, salads without salt.
- Advise the patient to take a diet rich in vitamin C such as lemon water daily.
- Advise the patient to avoid tea, coffee, junk food, ice cream, hot diet, breakfast, spicy food or things that irritate the mouth.
- Advise the patient to avoid pickles, refined processed food, condiments,
- Meat and soft drinks.
- Advise the patient to gargle properly to prevent infection.
- Advise the patient to maintain proper oral hygiene.
- Advise the patient to get proper rest and sleep.
- Advise the patient on multivitamin medication such as vitamin B complex and becasole capsule.
- Advise the patient to brush the teeth softly to prevent bleeding from the gums.
- Take proper care to avoid swallowing the medicine applied on the ulcer.
- Advise the patient to maintain proper oral hygiene.
1)explain/define Glossitis. Define glossitis.
- Glossitis is an infection and inflammation of the tongue.
- Infection and inflammation of the tongue causes the tongue to become swollen and its color to change.
- Glossitis causes the finger-like projections on the tongue, called papillae, to be lost from the surface of the tongue, making the tongue appear smooth.
2) Explain the type of Glossitis. Write the types of glossitis.
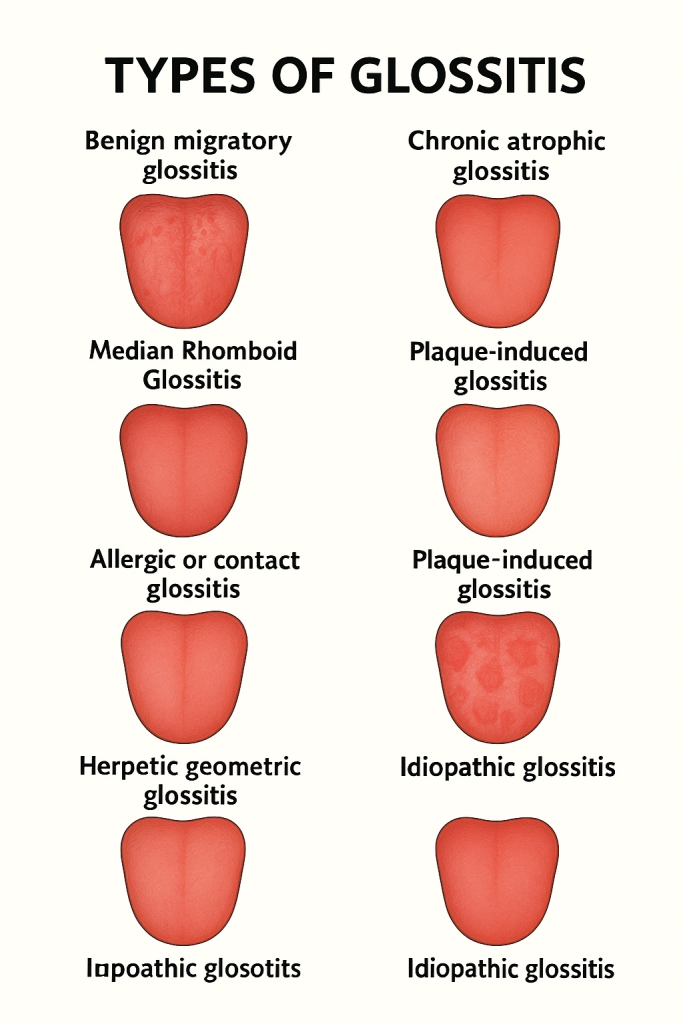
There are 9 types of glossitis. There are:
1)Benign migratory glossitis.
2)Acute infective glossitis.
3)chronic atrophic glossitis/hunter glossitis
4)median Rhomboid Glossitis
5)Allergic or contact Glossitis.
6)plaque -induced Glossitis.
7)papillary Atrophy Glossitis.
8)Herpetic geometric Glossitis
9) Idiopathic Glossitis
1)Benign migratory glossitis. (Benign Migratory Glossitis) ,
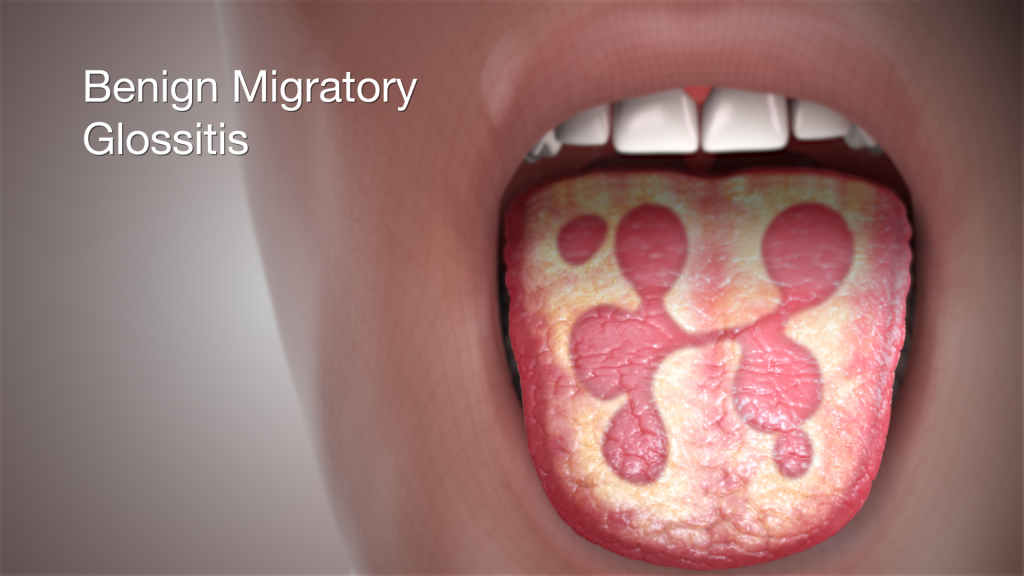
- Filiform papillae in Benign Migratory Glossitis ( filliform papillae) on the dorsal part of the tongue.
- It has a pinkish-red central lesion and yellowish lines or bands that change over a few days.
- Because this glossitis changes over a few days, it is called
- Erythema migrans
(migraine in erythema), - Glossitis migrans
(migraine in erythema) , - Glossitis areata exfoliativa
( Glossitis areata exfoliativa) , - pityriasis linguae ( Pityriasis linguis)
is called.
2)Acute infective glossitis. (Acute Infective Glossitis) ,
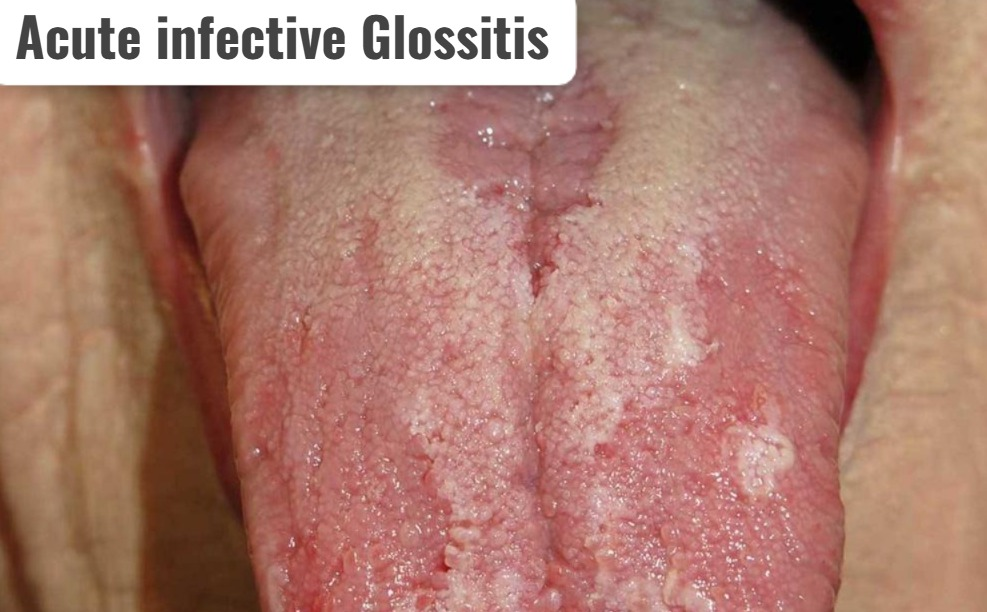
- Acute Infective Glossitis is caused by a bacterial infection.
- Acute infectious glossitis is seen due to poor oral hygiene and compromised immunity.
- Its onset is rapid.
- Symptoms of acute infectious glossitis include pain, swelling, and difficulty swallowing.
3)Chronic Atrophic Glossitis/Hunter Glossitis.
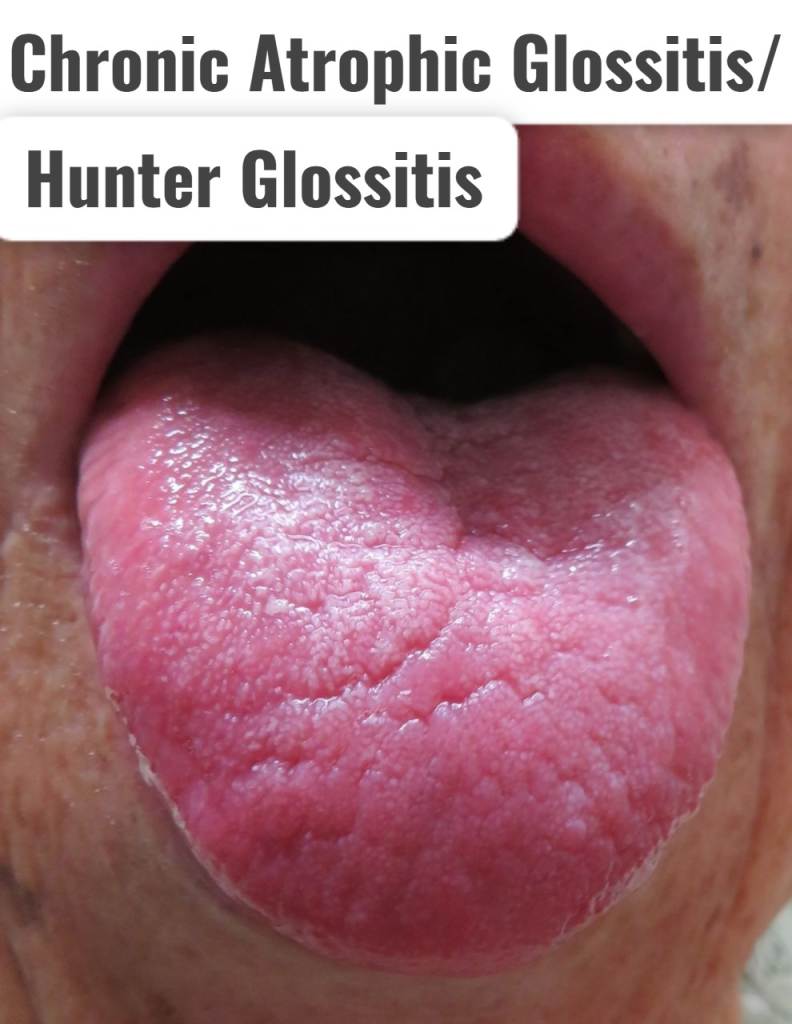
- Chronic Atrophic Glossitis It is also called Hunter Glossitis.
- In Hunter Glossitis, the papillae of the tongue are lost, giving the tongue a smooth and shiny appearance.
- Hunter Glossitis is caused by iron and vitamin B12 deficiency.
- Hunter Glossitis causes pain and burning sensation.
- Hunter Glossitis can also spread to other parts of the oral cavity. is.
- In Hunter Glossitis, the tongue has a beefy red color and shiny appearance.
- In Hunter Glossitis, small ulcers spread over the surface, hence it is also called Atrophic Glossitis.
4)Median Rhomboid Glossitis,
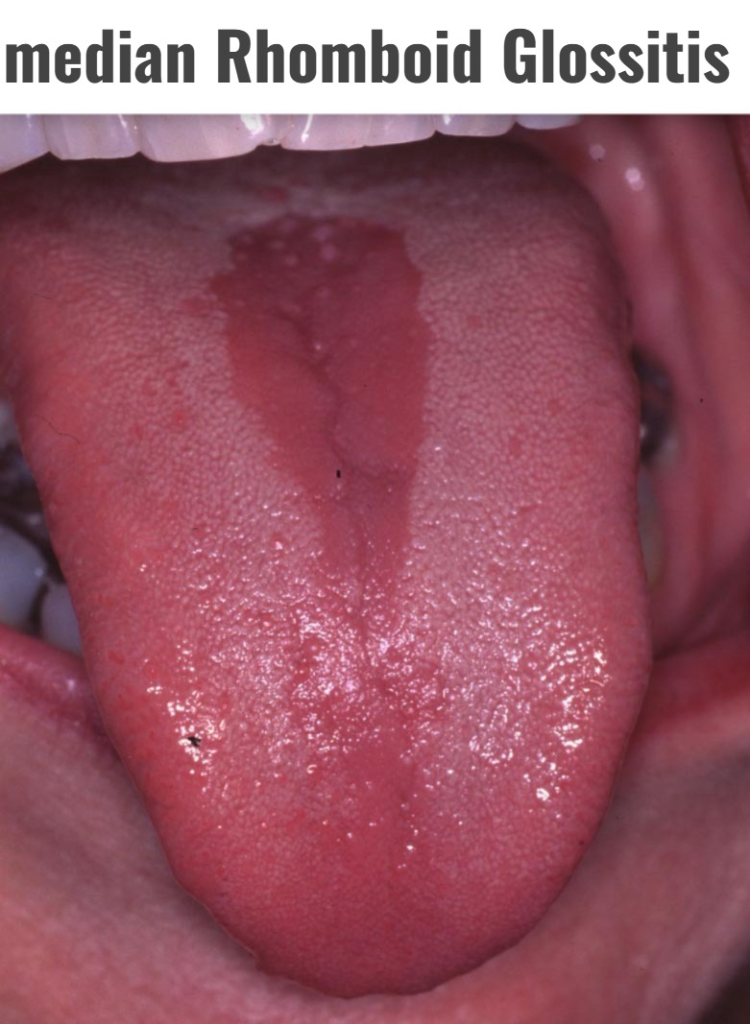
- Diamond-shaped reddish lesion is seen in the center of the tongue in median rhomboid glossitis.
- Median rhomboid glossitis is caused by yeast (candida) infection.
- Median rhomboid glossitis is a congenital disorder.
- It is characterized by a rhomboid reddish, smooth and shiny lesion along with some opalescent spots on the central part of the tongue.
5)Allergic or contact Glossitis. (Allergic or Contact Glossitis),
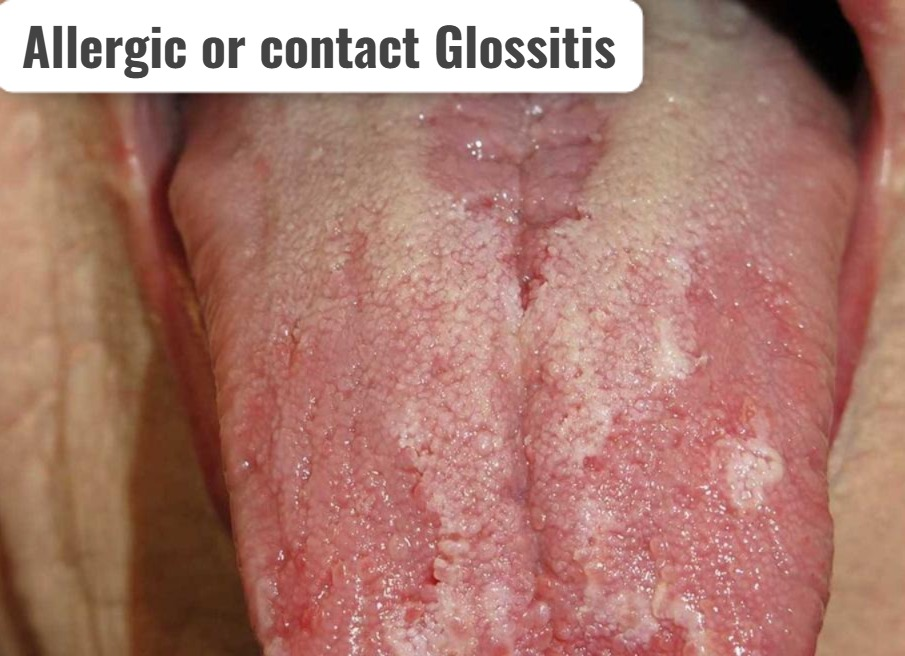
- Allergic contact glossitis is an allergic reaction to certain foods, medications, and oral care products. Due to this, the condition of glossitis is seen.
6) Plaque-induced glossitis. (Plaque Induced Glossitis) ,
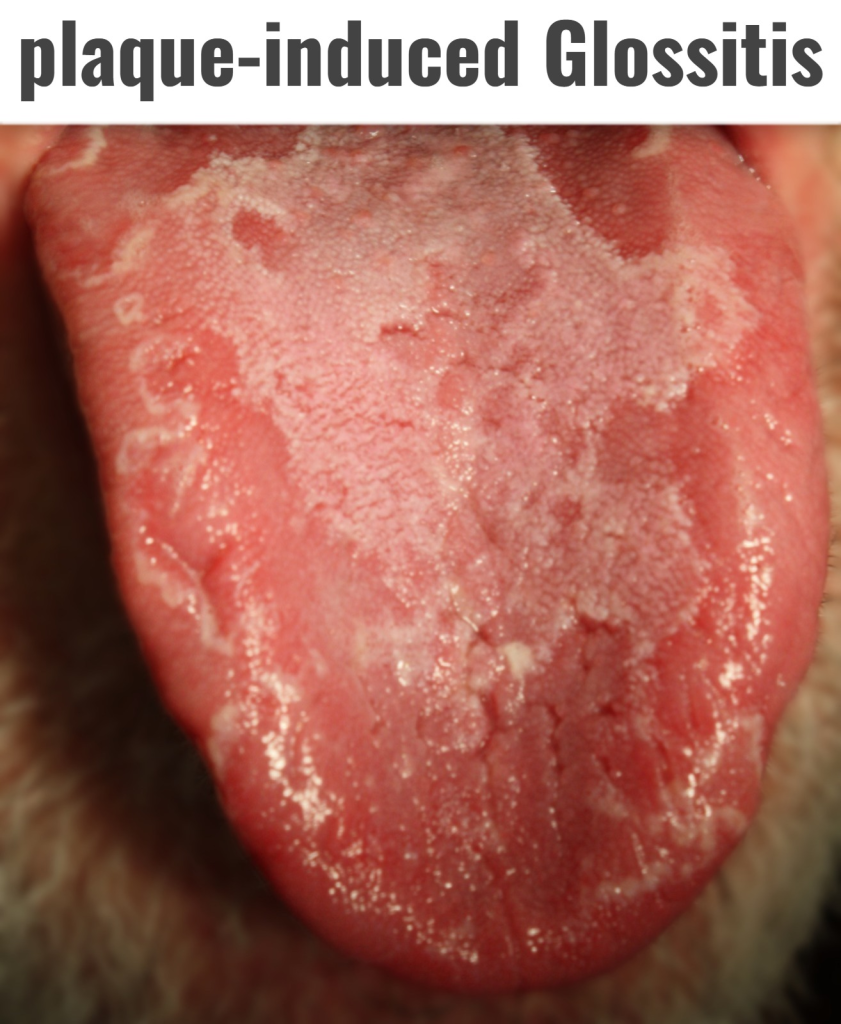
- Plaque Induced Glossitis It is caused by inadequate oral hygiene.
- Plaque induced Glossitis is caused by the accumulation of plaque on the tongue.
7)Papillary Atrophy Glossitis. (Papillary Atrophy Glossitis) ,
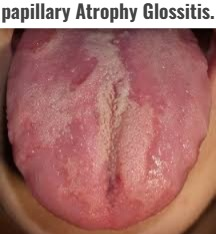
- Papillary Atrophy Glossitis is a condition in which the filiform papillae on the surface of the tongue are removed. (filliform papillae) is seen due to loss.
- Therefore, the tongue has a bald (smooth) and depapillated appearance.
8)Herpetic geometric Glossitis (Herpetic geometric glossitis),
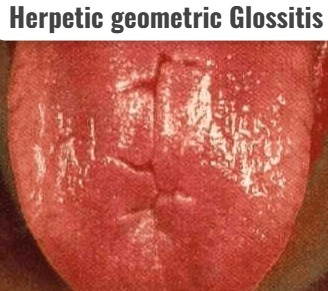
- Herpetic geometric glossitis is characterized by painful, longitudinal, crossed, and branched fissures on the dorsum (posterior) surface of the tongue.
9) Idiopathic Glossitis ( Idiopathic Glossitis)

- Idiopathic glossitis is an infection and inflammation of the tongue, but the cause is unknown. It is called idiopathic. It is called glossitis.
- In idiopathic glossitis, there is redness, swelling and changes in the color of the tongue.
3)explain the Etiology/cause of Glossitis. Explain the cause of glossitis:
- Due to any bacterial or viral infection (including oral herpes simplex).
- Due to poor hydration.
- Due to low amount of saliva in the mouth.
- Any injury in the mouth such as a burn.
- Due to any trauma in the mouth.
- Rough edges of the teeth.
- Due to exposure to any irritant such as tobacco, alcohol,
- Hot food and spicy food etc.
- Due to continuous colonization of the tongue by any microorganism.
- Due to allergic reaction to any toothpaste, mouthwash, breath freshener, dyes in candy, plastic dentures,
- Due to medication.
- Due to some disorders like
- Iron deficiency Anemia,
- Pernicious Anemia,
- Vitamin B deficiency,
- Oral lichen planus,
- Erythema multiform,
- Aphthous ulcer,
- Pemphigus vulgaris,
- Syphillus,
- And
- other yeast infections.
- Due to dry mouth.
- Inherited
- Due to poor oral hygiene.
4)Explain the Clinical manifestation/sign and symptoms of Glossitis. Explain the symptoms and signs of Glossitis.
- Inflammation and swelling of the tongue occurs.
- Smooth appearance of the tongue is seen.
- The color of the tongue is dark “beefy” red color.
- Pale color due to Pernicious Anemia.
- The tongue becomes sore and tender.
- Ulceration is seen in the tongue.
- Difficulty in chewing.
- Difficulty in swallowing.
- Difficulty in speaking.
- Fiery red, due to deficiency of B Vitamin.
- Tongue is sore and tender.
- White patches are seen on the tongue.
5)Explain the Diagnostic evaluation of the patient with Glossitis. Write the diagnostic evaluation of the patient with Glossitis.
- History taking and physical examination.
- Blood test.
- Microbiological test.
- Biopsy.
- Allergic testing.
- Imaging studies.
- CT scan test.
- Salivary gland test.
6)Explain the treatment of the patient with Glossitis. Write the treatment of the patient with Glossitis.
- Advise the patient to maintain good oral hygiene.
- Advise the patient to brush their teeth properly twice a day.
- If the patient has anemia and nutritional deficiency, provide dietary supplements.
- Advise the patient to avoid hot and spicy food, alcohol and tobacco.
- Provide corticosteroids to reduce the inflammation of the patient’s tongue.
- Provide antibiotics to the patient.
- Provide antifungals to the patient.
- Provide iron, vitamin B12 and folate to the patient.
Explain the nursing management of patients with Glossitis. Write the nursing management of a patient with glossitis.
- Provide a balanced diet to the patient to prevent nutritional deficiency.
- Advise the patient to avoid very hot and very cold items.
- Advise the patient to avoid coffee, tea, and spicy and salty foods.
- Advise the patient to avoid cigarette smoking.
- Advise the patient to have adequate fluid intake.
- Advise the patient to avoid allergens.
- Advise the patient to maintain good oral hygiene.
- Advise the patient to use a soft toothbrush.
- Advise the patient to rinse the mouth frequently.
- Minimize irritating products.
- Advise the patient to use a topical emollient (glycerine).
- Advise the patient to brush properly twice a day.
- Advise the patient to apply topical corticosteroids.
- Advise the patient to rinse the mouth properly with a mouthwash.
- Inform the doctor if the patient is allergic to any medication.
- Advise the patient to have regular mouth check-ups.
- Advise the patient to have regular follow-ups.
1)Define/explain the Gingivitis. Define the Gingivitis.
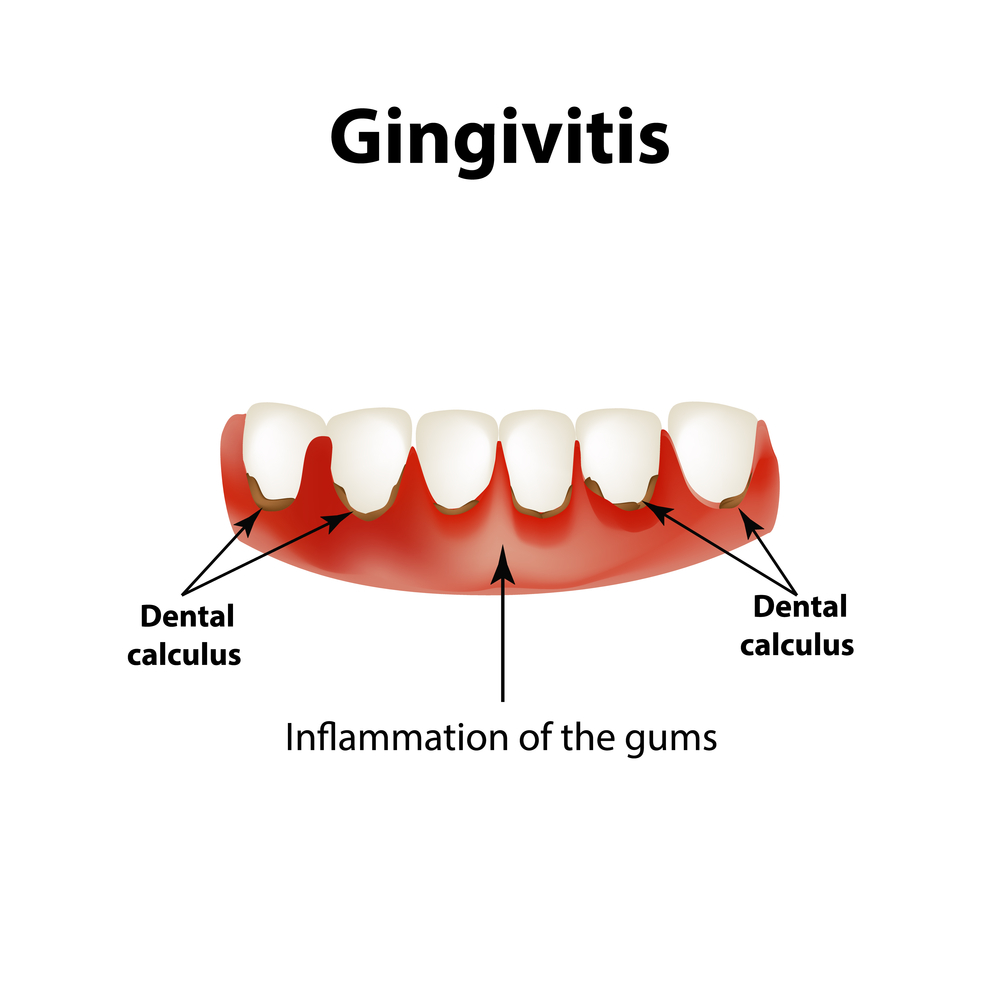
- Gingivitis is a common and mild form of gum disease, in which the
gums/gingiva become infected and inflamed. - Gingivitis is mainly caused by the build-up of plaque.
- Gingivitis causes redness, swelling, pain, and irritation in the gums.
2) Explain the types of Gingivitis. Write the type of gingivitis.
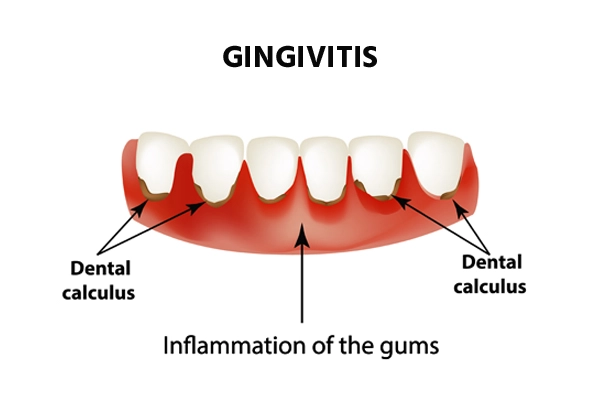
There are four types of gingivitis.
1)Acute Necrotizing Ulcerative Gingivitis (ANUG)
2)Chronic Gingivitis
3)Paque induced Gingivitis. ( Plaque Induced Gingivitis) ,
4)Non plaque induced Gingivitis ( Non plaque induced Gingivitis)
1)Acute Necrotizing ulcerative Gingivitis ( ANUG ) ( Acute necrotizing ulcerative gingivitis)
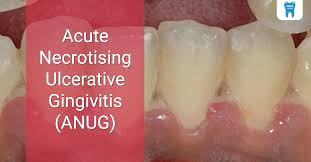
- Acute necrotizing ulcerative gingivitis is a condition that occurs in people with an impaired immune system and malnutrition.
- Acute gingivitis causes foul smelling (halitosis) from the mouth, fever, and painful gums.
- Acute gingivitis is more common in smokers. It is found in lesser proportion in non-smokers.
2)Chronic Gingivitis:
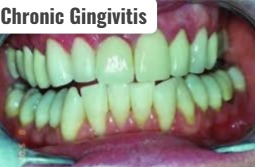
- Chronic Gingivitis is the most common type of gingivitis.
- It is caused by poor oral hygiene.
- Chronic Gingivitis is seen for a long time.
3) Paque induced Gingivitis. ( Plaque Induced Gingivitis) ,
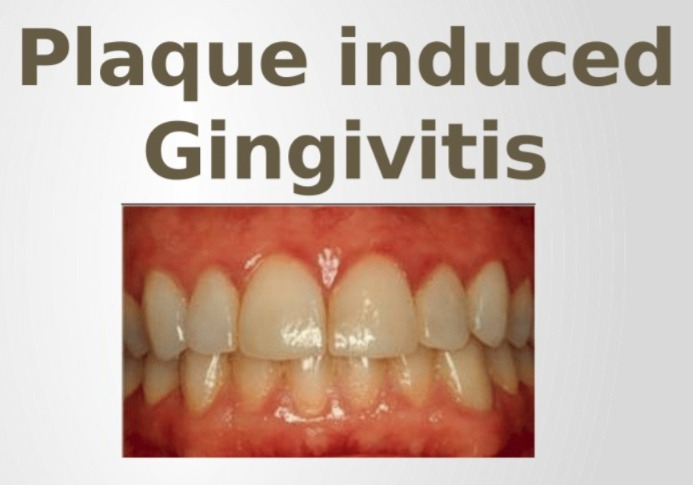
- Plaque induced gingivitis is caused by the formation of plaque in the gums. is.
4) Non plaque induced gingivitis:
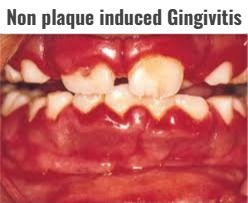
- Non plaque induced gingivitis is caused by any disease condition, hormonal changes, and some disease conditions.
- It is mainly caused by viral infection, fungal infection, or genetic origin.
3)explain the Etiology/cause of Gingivitis. Give the causes of gingivitis.
- Due to plaque deposition.
- Due to injury to the gums.
- Due to vigorous brushing.
- General illness.
- Due to hormonal changes during pregnancy.
- Due to smoking.
- Due to uncontrolled diabetes.
- Due to dentures.
- Due to certain types of medication.
- Ex:phenytoin ,
Calcium channel blocker.
Birth control pills. - Due to taking birth control pills.
- Due to poor oral hygiene.
- Due to bacterial growth.
- Due to smoking.
- Due to tobacco use.
- Due to autoimmune disorders.
- Due to hormonal changes.
4) Explain the clinical manifestation/sign and symptoms of the Gingivitis. Write the symptoms and signs of gingivitis.
- Gums become swollen.
- bright red or purple colour gums.
- Bleeding from the gums.
- Gums that tender when touched.
- Halitosis (halitosis: bed breath).
- Fever.
- Gums are swollen and have a shiny appearance.
- Gingival Edema.
- Ulceration.
- Redness in the gums.
- Gums become tender.
5) Explain the Diagnostic evaluation of Gingivitis. Write the diagnostic evaluation of gingivitis.
- History taking and physical examination.
- x rays.
- Biopsy.
- blood test.
- culture.
- patch testing.
6)explain management of the patient with the Gingivitis. Write the management of the patient with the Gingivitis.
- Advise the patient to maintain proper oral hygiene.
- Advise the patient to gargle with saline solution.
- Provide antibiotics to the patient.
- Provide non-steroidal anti-inflammatory drugs to the patient.
- Provide xylocaine to relieve the patient’s pain.
- Advise the patient to clean the mouth with antibacterial mouthwash.
- Remove plaque if it has formed in the oral cavity.
- Advise the patient for scaling, root planing, and curettage.
- Advise the patient to use chlorhexidine or hydrogen peroxide mouthwash to treat the gingivitis condition.
- Provide antibiotic therapy to the patient.
- Ex: Amoxicillin, cephlexin.
Explain the Nursing management of patients with Gingivitis. Write the nursing management of a patient with gingivitis.
- Advise the patient to maintain oral hygiene.
- Advise the patient to brush teeth daily.
- If plaque has formed in the patient’s oral cavity, remove it.
- If dentures are worn, maintain their proper hygienic condition.
- Blood test the patient Advise to maintain glucose level.
- Avoid use of certain medications.
- Ex: phinytoin,
Calcium channel blocker.
Birth control pills etc. - Advise the patient to use a soft brush for brushing.
- Advise the patient to avoid cigarette smoking.
- Advise the patient to take proper nutrition such as green leafy vegetables, vitamin – E, and vitamin – C.
- Advise the patient to clean the mouth regularly.
- Consult a dentist for proper brushing and flushing technique of the mouth.
1)Define/explain pyorrhea/periodontitis. Define pyorrhea / periodontitis.
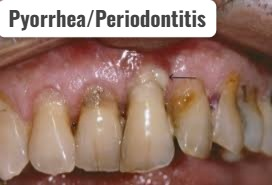
- Pyorrhea is also known as periodontitis.
- Periodontitis is a condition in which the bones and ligaments that support the teeth become infected and inflamed.
- Pyorrhea is a serious gum infection that destroys the soft tissue and bone that support the teeth.
- Periodontitis can lead to tooth loss and other health conditions such as heart attack, stroke, and other serious health problems.
- Periodontitis is caused by poor oral hygiene conditions.
2)explain the types/classification of pyorrhea/periodontitis. Write the type of pyorrhea/periodontitis.
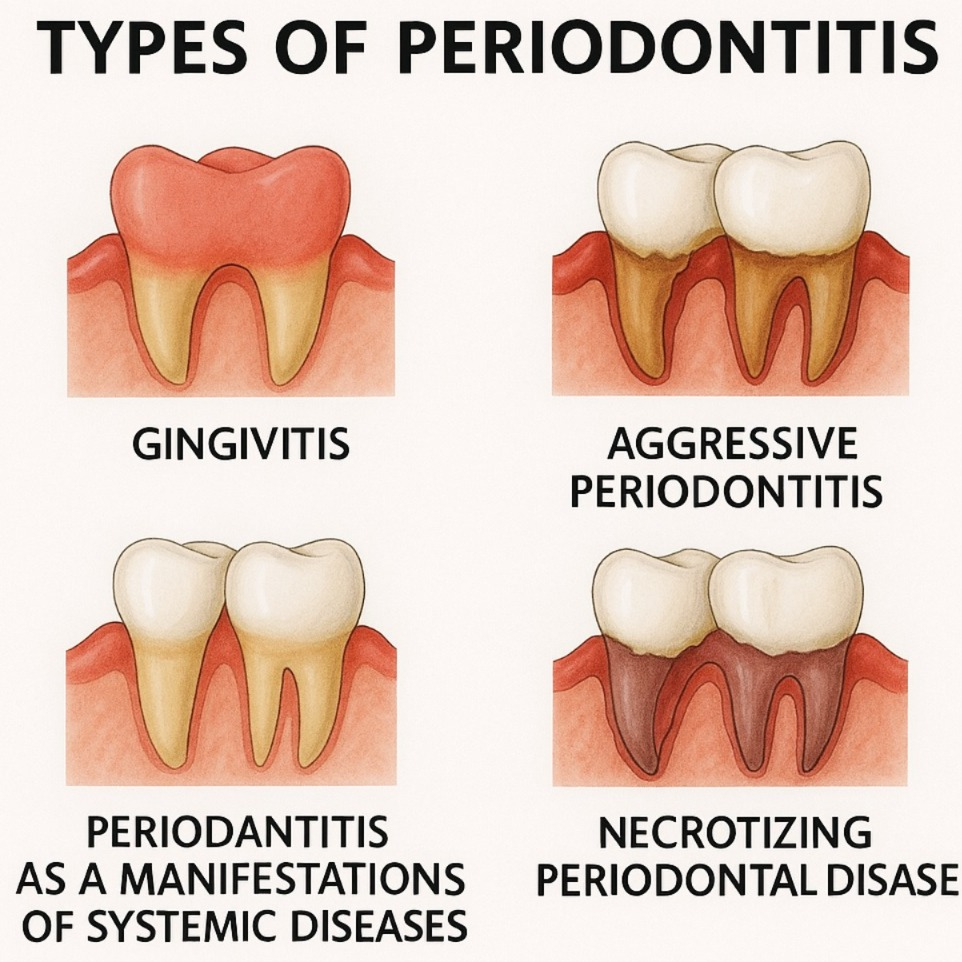
There are five main types of pyorrhea. These types are mainly classified based on the severity of the disease.
1) Gingivitis,
2) Aggressive periodontitis,
3) Chronic periodontitis ,
4) Periodontitis as a manifestation of systemic disease. ( Periodontitis as a manifestation of systemic disease.) ,
5) Necrotizing periodontal disease ( Necrotizing periodontal disease)
1) Gingivitis ( Gingivitis) ,
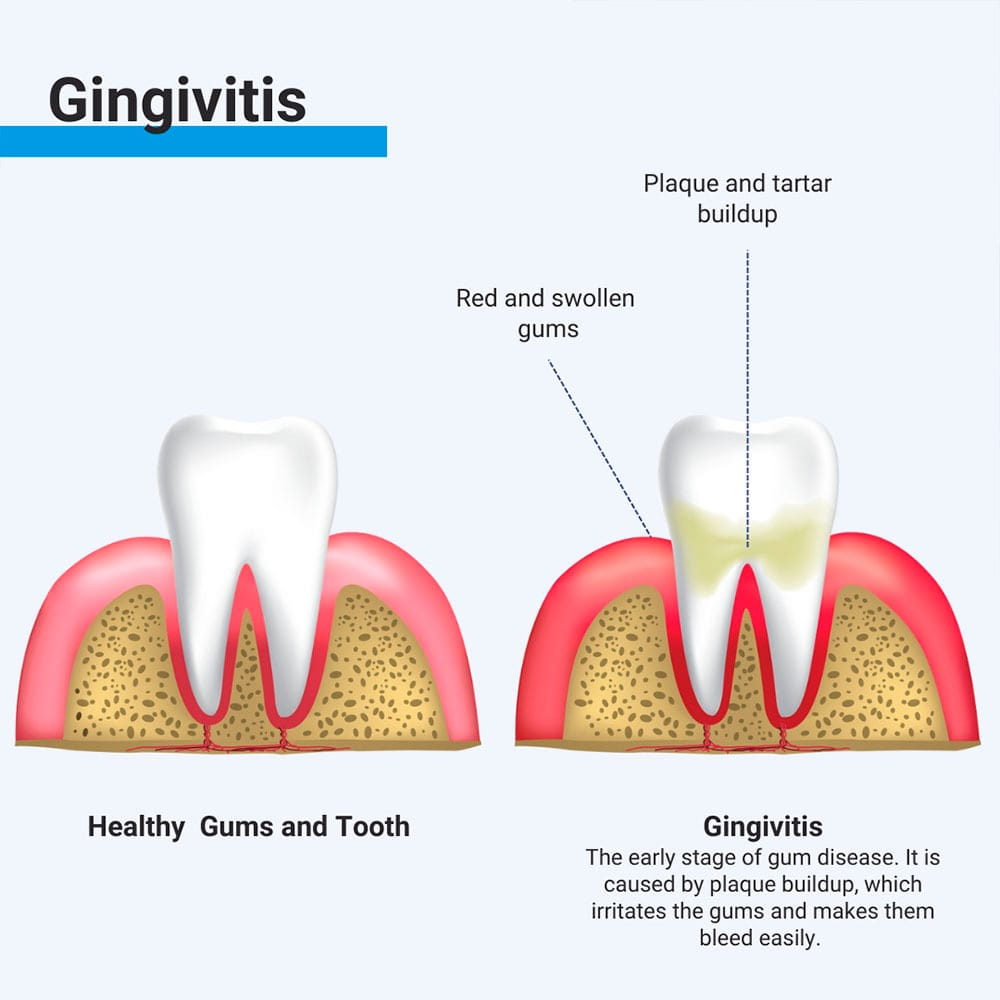
- Gingivitis is the initial stage of gum disease, in which the gums become infected and inflamed.
- Gingivitis is reversible if proper oral hygiene is maintained.
2) Aggressive periodontitis,
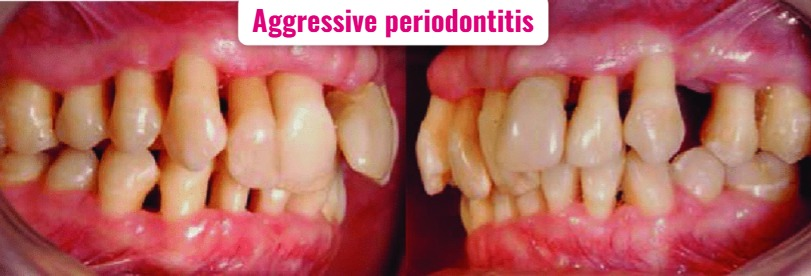
- Aggressive periodontitis develops more rapidly.
- Aggressive periodontitis is a more severe condition.
- In aggressive periodontitis, the bones and tissues that support the teeth are rapidly lost.
3) Chronic periodontitis ( Periodontitis) ,
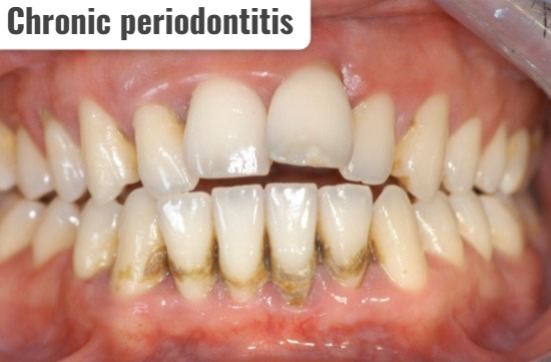
- Chronic periodontitis is the most common type of periodontitis.
- Chronic periodontitis is characterized by the loss of attachment of the bones and tissues that support the teeth to the teeth.
- Chronic periodontitis develops progressively and gradually.
4)Periodontitis as a manifestation of systemic disease. ( Periodontitis as a manifestation of systemic disease) ,
- The condition of periodontitis also arises due to certain types of systemic disease.
- Ex: heart disease ,
Respiratory disease,
Diabetes malitus etc.
5) Necrotizing periodontal disease ( Necrotizing periodontal disease Disease)
- Necrotizing periodontal disease is a condition in which •>gingival tissues, •>periodontal ligaments, and •>alveolar bone are lost.
- This condition is mainly seen in individuals with systemic conditions such as •>HIV infection •>Malnutrition And •>immuno suppresant.
3)explain the Etiology/cause of Pyorrhea/periodontitis. Give the causes of pyorrhea/periodontitis:
- When gingivitis is not treated properly.
- Due to the formation of plaque on the teeth.
- Due to the accumulation of tartar on the teeth.
- Hereditary,
- Due to smoking.
- Poor Due to oral health habits.
- Due to hormonal changes in females.
- Due to diabetes.
- AIDS infection,
- certain drugs ( like:
- •>antidepressant,
•>antihistamine,
•>Anti seizure,
•>Calcium channel blocker,
•>Drugs that suppress the immune system. ), - Due to cancer.
- Due to older age.
- Due to decreased immunity.
- Due to poor nutrition.
- Due to substance abuse.
4) Explain the clinical manifestation/sign and symptoms of the patient with pyorrhea/periodontitis. Describe the symptoms and signs of a patient with pyorrhea.
- Gums are soft and bleed easily.
- Gums are swollen, bright red, and purple in color.
- Large spaces between the gums.
- gums that pull away from the teeth.
- Teeth may appear longer than normal length.
- Pus may appear between the teeth and gums.
- Bad breath (halitosis) from the mouth.
- Loose teeth.
- Bleeding may be seen when brushing the teeth.
- A metallic taste from the mouth.
- Inflammation in gums.
- Gums become red, swollen and tender.
- gums pain .
5) Explain the diagnostic evaluation of the patient with pyorrhea. Write a diagnostic evaluation of a patient with pyorrhea.
- history tacking and physical examination.
- Dental X Ray.
- periodontal probing.
- bite assessment.
- plaque and tartar analysis.
- Gingival crevicular fluid analysis.
6) Explain the management of the patient with pyorrhea/periodontitis. Write the management of a patient with periodontitis.
Medical management :
Advise the patient to maintain daily routine oral hygiene.
1) Scaling:
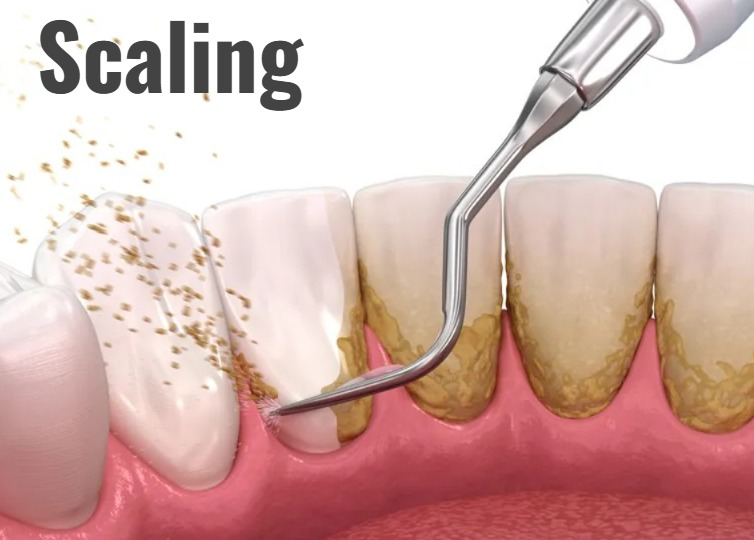
- Scaling removes tartar, plaque and bacteria from the surface of the teeth.
- Scaling is done using an instrument and an ultrasonic device.
2) Root planning:
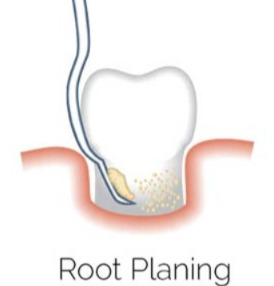
- In root planning, the root surface is smoothed, due to which the buildup of plaque and tartar cannot occur.
3) Antibiotic:

- Provide topical and oral antibiotics to the patient to prevent bacterial infections.
4) Antimicrobial Mouth rinse:
- Provide the patient with an antimicrobial mouth wash to prevent the growth of bacteria in the mouth. (Ex: chlorhexidine).
5) Antiseptic “CHIP”( Antiseptic Chip) :
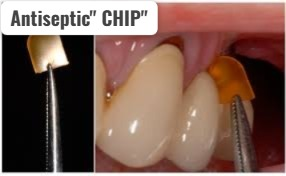
- The antiseptic “chip” consists of a small piece of gelatin, which is filled with chlorhexidine. It is,
- It controls the growth of bacteria, and reduces the size of the periodontal pocket,
- This medicine is mainly placed in the pocket after root planning and this medicine is slowly released.
6)Antibiotic gel
- This gel mainly contains the antibiotic Doxycycline,
- This medicine controls the growth of bacteria,
- This is mainly placed in the pocket after scaling and root planning and slowly releases the medicine from it.
7)Antibiotic microspheres (Antibiotic microspheres) Microspheres)
- Antibiotic microspheres mainly contain minocycline antibiotic which controls the growth of bacteria and also reduces the size of periodontal pockets.
- It is mainly placed in the pocket after scanning and root planning from which the medicine is slowly released.
8) Enzyme suppressant ( Enzyme Suppressant)
- Enzyme suppressants provide a low dose of Doxycycline.
- Some enzymes break down the tissues of the gums. By providing this medicine, the body’s response to that enzyme is held and the breakdown of the tissues of the gums is prevented.
- This is taken orally (as a pill).
9)Oral antibiotics:
- Oral antibiotics are taken in the form of capsules or tablets.
- Oral antibiotics are used for short-term treatment in people with acute and locally persistent periodontal infections.
Surgical management :
- Surgical management is performed if the patient has advanced periodontitis and the gum tissue does not respond to non-surgical treatment and good oral hygiene.
1) Flap surgery (Pocket reduction surgery)
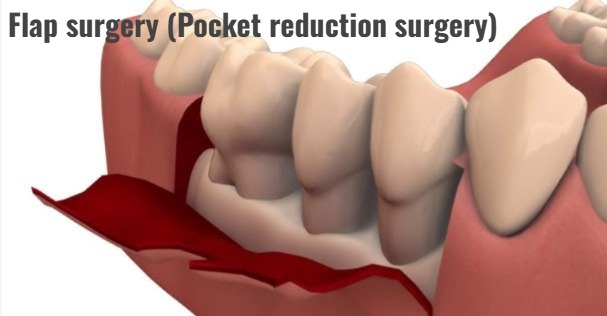
- In this procedure, the periodontist makes a tiny incision at the root of the gums.
- So the gum tissue is pushed back The lift is done and the root is properly exposed, so scaling and root planning can be done more effectively.
- This procedure takes one to three hours and is performed under local anesthesia.
2) Soft tissue graft:
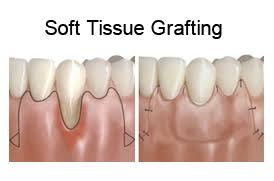
- When a patient’s gums are lost due to any periodontal disease, the teeth appear longer than their normal length, and the damaged ones are replaced.
- In soft tissue grafting, a small amount of tissues is removed from the roof (palate) of the mouth or tissues from a donor are attached to the affected site.
- This procedure mainly reduces further recession of the gums and covers the exposed root. is.
3) Bone grafting:
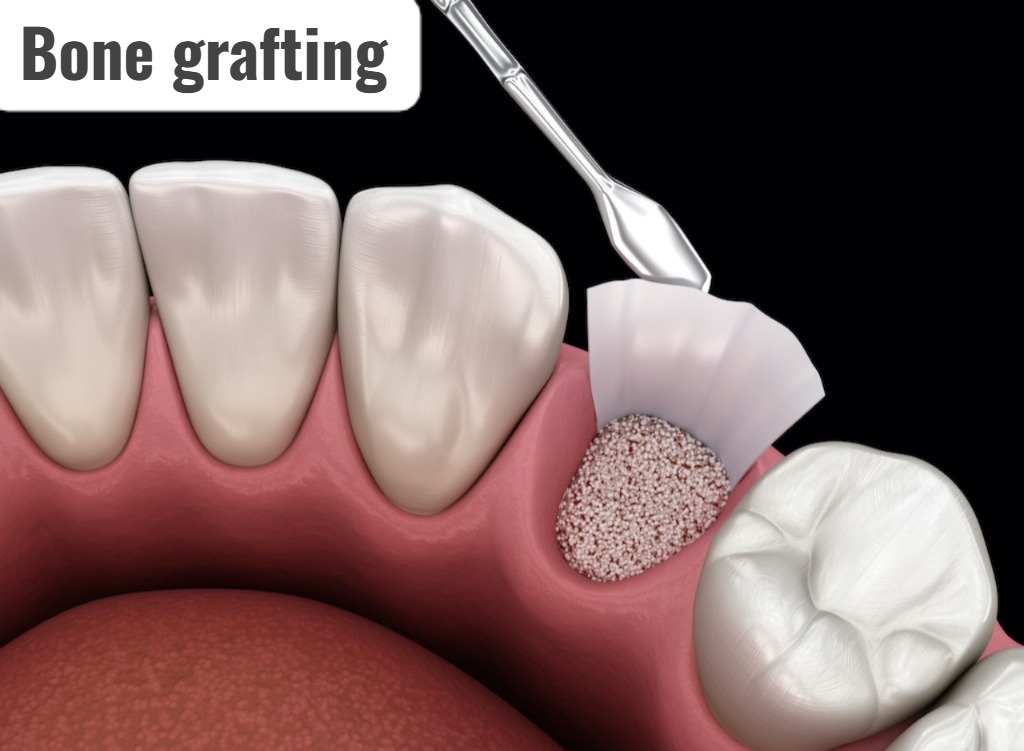
- This procedure is performed when the bone surrounding the teeth has been destroyed due to periodontitis.
- Bone grafting uses the patient’s own bone or synthetic or donated bone.
- Bone grafting can hold the tooth in place, preventing tooth loss.
- Bone grafting stimulates the growth of natural bone The platform is provided for.
4) Guided tissues regeneration:
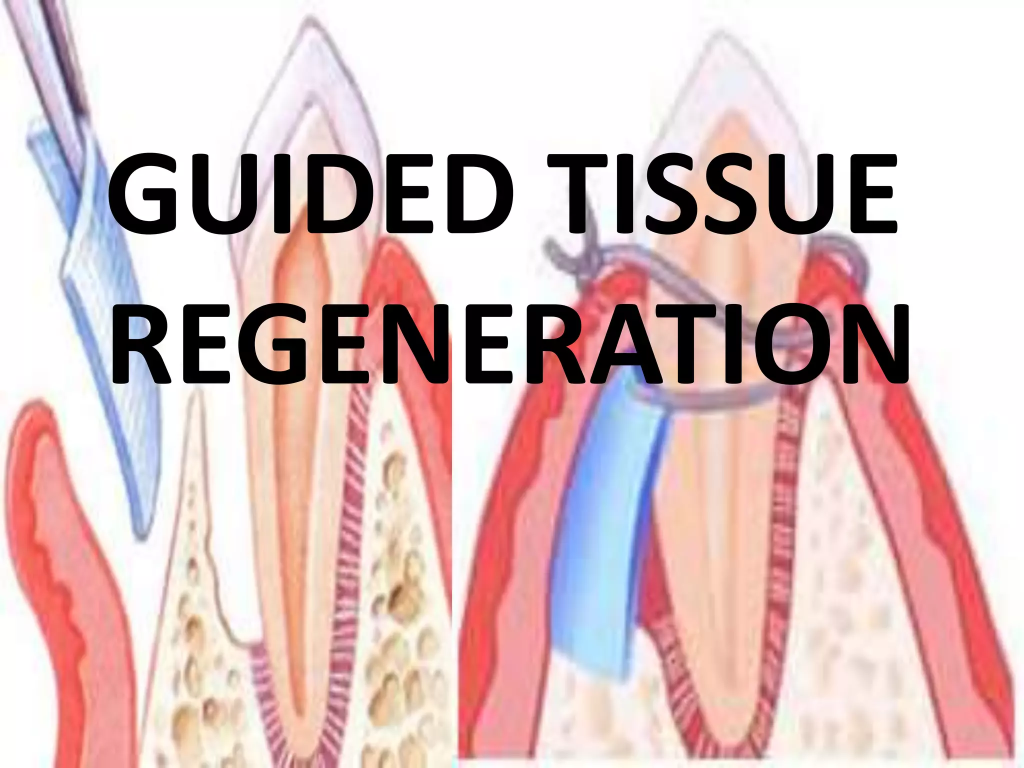
- This procedure provides a platform for the regrowth of bone that has been destroyed by bacteria.
- In this procedure, the dentist places special pieces of biocompatible fabric between the bone and the teeth.
- This material prevents unwanted tissue from moving into the healing area, allowing the bone to grow properly.
5) Enamel matrix derivative application (Enamel matrix derivative application)
- In enamel matrix derivative application, a specialized gel is applied to the root of the diseased tooth.
- This gel contains the same proteins that are present in the enamel of the tooth, which are responsible for stimulating the growth of healthy bone and tissue.
Explain the nursing management of the patient with the pyorrhea
- Advise the patient to maintain proper oral hygiene.
- Advise the patient to brush properly at least twice a day.
- Advise the patient to wash the mouth properly with an antiseptic mouthwash, Chlorhexidine glucomate.
- Advise the patient to have regular dental checkups.
- Advise the patient to brush properly after meals.
- Advise the patient to use a soft toothbrush.
- Advise the patient to take a well-balanced diet.
- Advise the patient to take a diet rich in calcium and vitamin C.
1) Define/explain dental caries.
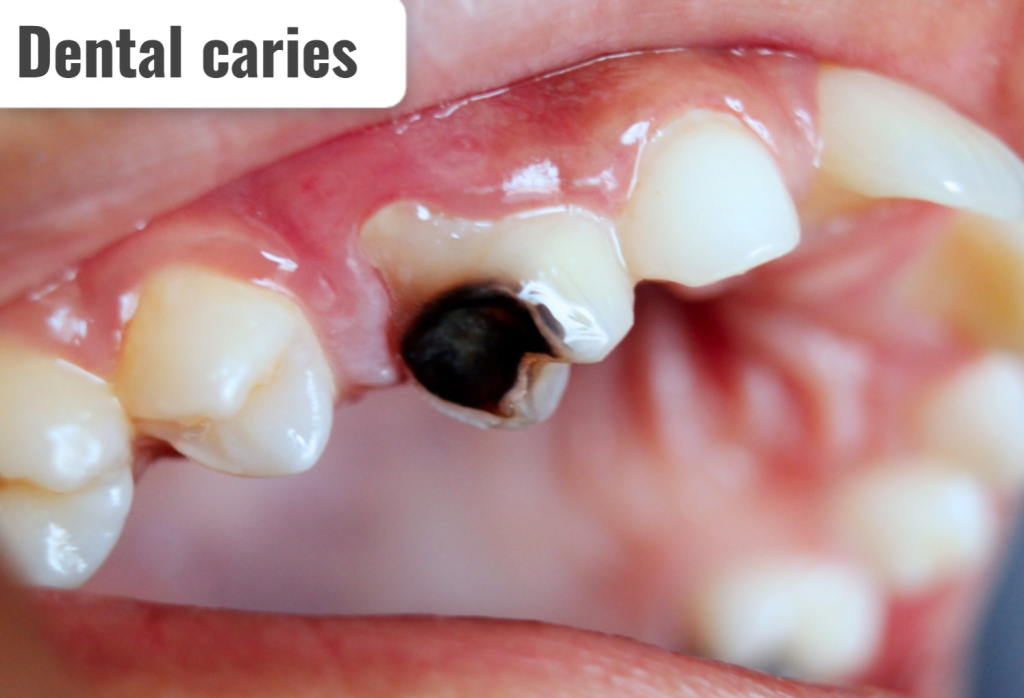
- Dental caries is an infectious microbiological disease that causes the dissolution and destruction of the calcified tissue of the teeth.
- Dental caries causes the formation of small shallow holes in the teeth.
- Dental caries causes tooth decay and the formation of cavities.
- Dental caries is caused by the growth of bacteria in the mouth, which causes acid in the mouth cavity. Formation occurs which destroys/breaks down the hard tissues surrounding the teeth.
- Due to this, cavities form in the teeth.
2) Explain the Etiology/cause of dental caries. Explain the causes of dental caries.
1) Due to bacterial infection.
Streptococcus mutans
2) Due to excessive intake of sugar and carbohydrates in the diet.
Due to excessive intake of carbohydrates.
3) Due to poor oral hygiene Due to
Not brushing properly.
4) Due to reduced salivary flow.
Due to reduced salivary flow in the mouth.
5) Due to genetic factors
The condition of dental caries is seen due to genetic abnormality.
6) Due to poor fluoridated water
Fluoride strengthens teeth excessively. When the amount of fluoride is low, cavities form in the teeth.
7)Lack of Dental care
Dental caries can also occur due to lack of proper care of teeth.
8) Accumulation of food particles in the mouth Due to.
9) Due to bacterial infection.
10) Due to plaque formation in the mouth.
11) Due to poor oral hygiene.
12) Due to autoimmune disorder.
13) Due to dehydration of the mouth.
14) Due to taking some types of cancer medication.
3) Explain the Clinical manifestation/sign and symptoms of the patient with the Dental caries.
1) Tooth Sensitivity:
- When sensitivity to any hot, cold, acidic, spicy beverages or food is caused, it is an early sign of dental caries.
2) Toothache or Pain:
- Pain in the tooth is observed due to the formation of cavities in the tooth.
3) Visible cavities:
- Small cavities form in the mouth. Which is visible.
4) Tooth discoloration:
- Tooth discoloration occurs in white, brown and black.
5) Bad breath (halitosis):
- Persistent bed breath is seen due to bacterial activity.
6) Pain when chewing :
- Pain is seen in the teeth when chewing on the affected side.
7) Pus (Abscess) Formation:
- When a severe condition occurs, pus accumulates around the teeth, causing pain and swelling in the teeth.
8) Visible holes and breaks in the teeth:
- The formation of teeth caries causes the breakdown of the teeth structure, which leads to the formation of holes in the teeth.
4)explain the Diagnostic evaluation of the patient with the Dental caries.
- history taking and physical examination.
- Dental X-rays.
- cavity detection tools.
- tooth sensitivity evaluation.
- Dye or staining agent.
- visual or tactile examination.
- assessment of the symptoms.
5) Explain the treatment of the patient with the dental caries. Write the treatment of a patient with dental caries.
Treatment can prevent tooth damage.
1)Fluide medication:

- Fluoride is a mineral that prevents the formation of hollow cavities in the teeth.
- Therefore, fluoride medication should be provided.
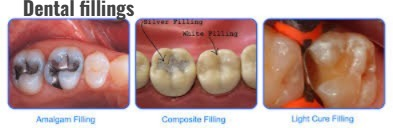
2)Dental fillings:
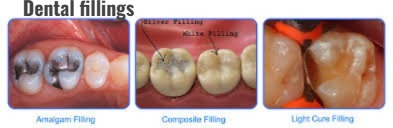
- If a cavity has formed in a small and moderate mount, the dentist removes the decayed part of the tooth and fills the teeth with some materials.
- Material like:
- Ex: Amalgume ,
- Composite resine ,
- Glass ionometer
3) Crowns:
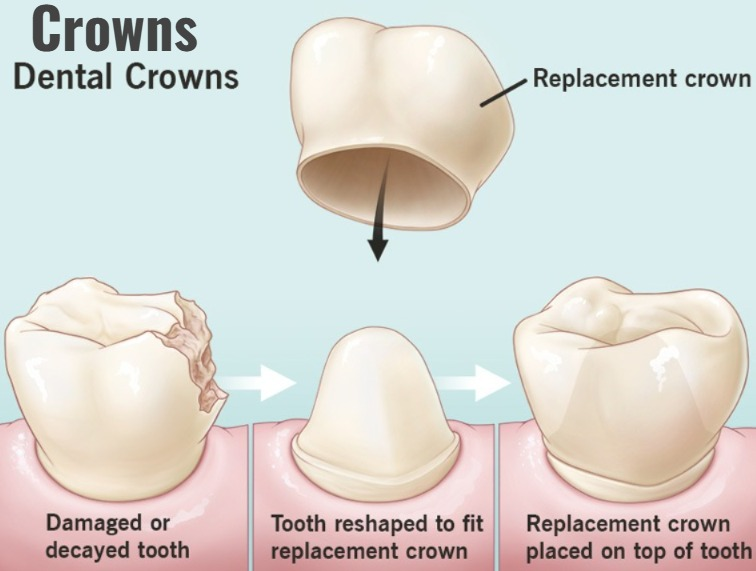
- If a large cavity has formed in the teeth, a crown is placed on the teeth.
- By placing a crown on the teeth, the structure of the remaining teeth can be prevented from being destroyed.
4) Root canal therapy (root canal) Therapy):
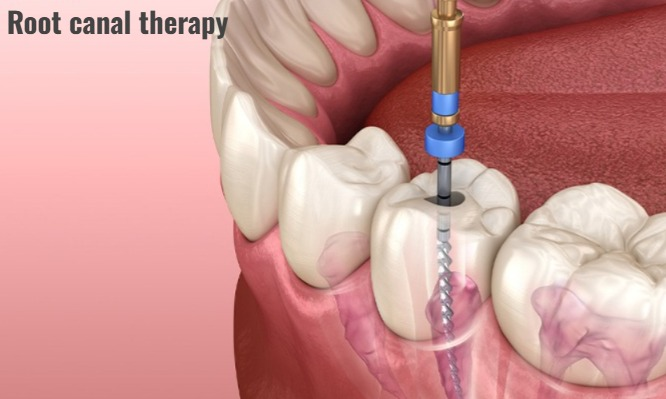
- A root canal is performed when tooth decay has reached the nerve of the tooth.
- This mainly involves removing the infected pulp (nerve) and cleaning the root canal. And it is sealed to prevent further infection.
5)Dental bonding:
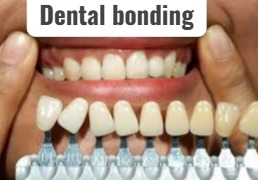
- Dental bonding is used to treat minor cavities that have formed in the teeth.
- In this, a tooth-colored resin material is applied.
- It is given a shape and made hard by a special light.
6)Preventing treatment
- Fluoride treatment and dental sealants primarily prevent further decay of teeth.
7)Dental extraction
- Teeth extraction is done when the teeth have suffered severe decay.
8) Education for nutritional diet and oral hygiene.
- Advise the patient to maintain proper oral hygiene.
- Advise the patient to brush properly.
- Advise the patient to avoid sugary foods, acidic foods and beverages.
9)Regular dental check up :
- Advise the patient to get their teeth checked regularly.
1)explain/Define Halitosis. Define halitosis.

- Halitosis is also called bed breath.
- In halitosis, an unpleasant odour is present when the breath is exhaled.
- Halitosis is mainly caused by dental decay, poor dental care, any gum disease, and bacterial infection.
2)explain the Etiology of the patient with the halitosis. Explain the causes of halitosis in patients.
1) Due to consumption of certain types of food.
- Ex: Due to onion, garlic, fish, cheese, spices etc.
2) Due to tobacco products:
- Due to smoking Gum disease causes bad breath to come out of the mouth.
3) Poor dental hygiene:
- If the mouth is not cleaned properly, bad breath can come out of the mouth.
4) Oral disease:
- Halitosis is also seen due to gingivitis, dental decay, ulceration etc.
5)other cause:
- Chronic rhinosinusitis.
- Tonsillitis.
- Gastroesophageal reflux disease (GERD),
- Due to lower respiratory tract infection.
- Due to renal failure.
- Due to nasal infection.
- Due to renal infection.
- Due to diabetes mellitus (smell of acetone breath).
3)explain the diagnostic evaluation of the halitosis. Write the diagnostic evaluation of a person with halitosis.
- History taking and physical examination.
- halimeter test.
- gas chromatography.
4) Explain the management of the patient with the halitosis. Write the management of a patient with halitosis.
- Advise the patient to maintain daily oral hygiene.
- Advise the patient to have a proper diet.
- Advise the patient to chew sugar free gum.
- Advise the patient to stop smoking and alcohol.
- Advise the patient to visit the dentist regularly.
- Advise the patient to clean the tongue properly.
- Advise the patient to brush twice a day.
- Advise the patient to maintain proper oral hygiene after meals.
- Advise the patient to properly rinse the mouth with mouthwash. Advise gargling.
- If the patient has dentures, advise them to clean them properly.
- Advise the patient to have plenty of fluid intake.
- Advise the patient to have high fiber fruits and citrus foods.
- Advise the patient to have a diet low in carbohydrates and high fat and high protein.
1) Explain/define Dysphagia.
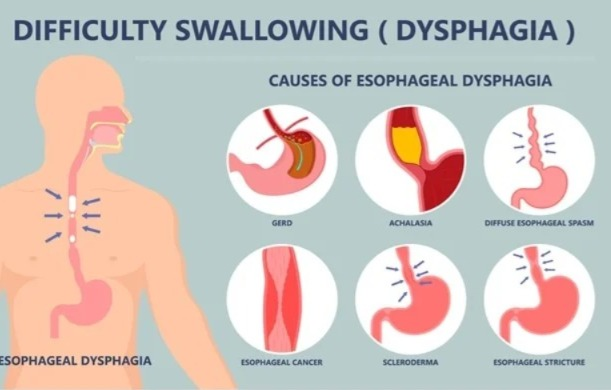
- Dysphagia is a medical term for difficulty swallowing.
- Dysphagia can also be caused by a primary oesophageal disorder.
specific causes of dysphagia including:
1)Neuromotor malfunction
2)Mechanical obstruction
3)Cardiovascular Abnormality
4)Neurological disease
2) Explain the Classification of the Dysphagia. Explain the classification of dysphagia
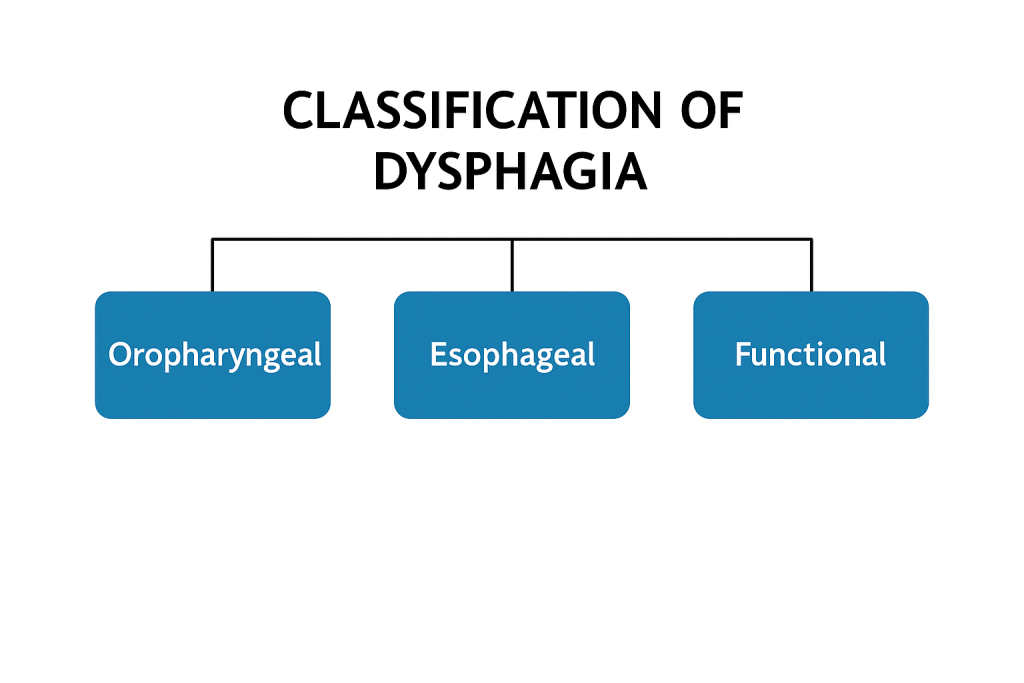
Three classifications of dysphagia It falls.
1) Oropharyngial dysphagia,
2) Esophagial dysphagia,
3) Functional dysphagia.
1) Oropharyngeal dysphagia:
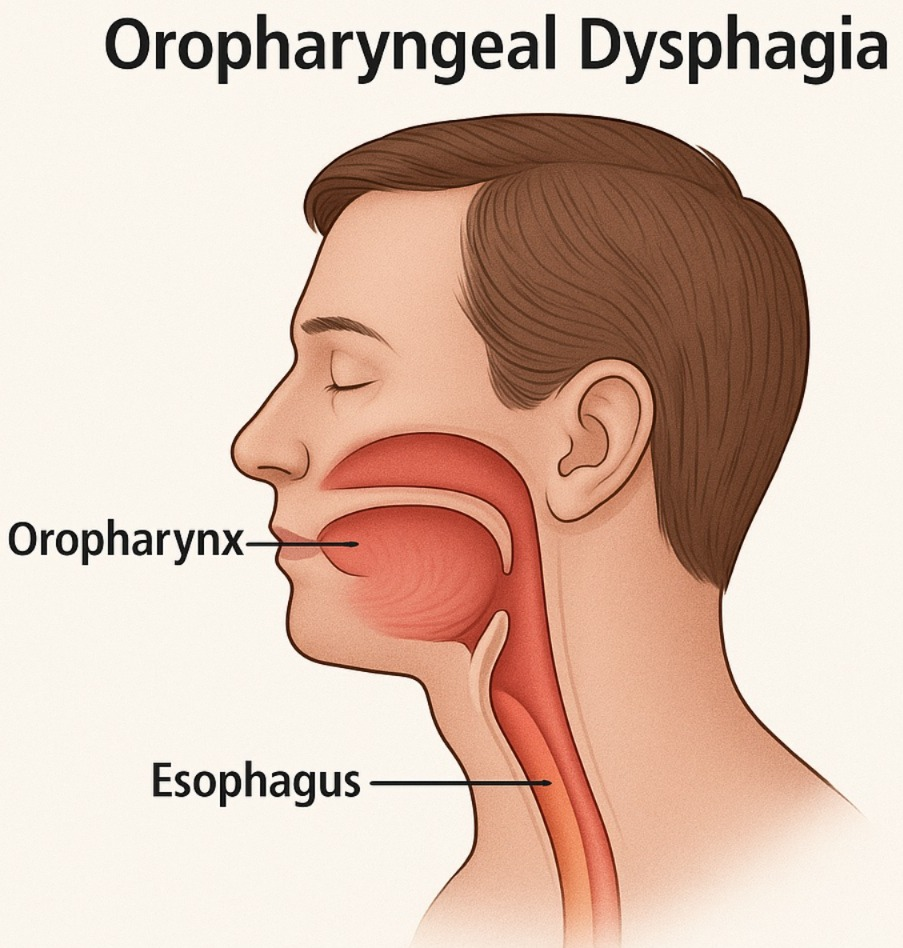
- The condition is mainly seen in the oral cavity and pharynx due to any obstruction.
- The condition of dysphagia is also seen due to problems in the tongue and throat.
- Oropharyngial dysphagia can also be due to the following reasons
- Tonsillitis (Tonsillitis),
- Peritonsill abscess (Peritonsillar abscess) Abscess),
- Stomatitis,
- Tongue cancer
2)Esophageal dysphagia:
- Esophageal dysphagia occurs due to a problem in the structure of the esophagus (food pipe) or due to any disease condition of the esophagus.
like:
1)Narrowing of the esophagus.
( Due to narrowing of the esophagus) ,
2)obstruction of the esophagus
( Due to obstruction in the esophagus) ,
3) weak muscles contraction
( Due to weak muscles contraction)
3) functional dysphagia ( Functional Dysphagia)
Functional dysphagia is mainly characterized by dysphagia that is not due to any organic cause. But it is mainly seen due to any neurological disorder due to impaired muscle contraction.
3)explain the Etiology/cause of dysphagia. Give the causes of dysphagia.
- Achalasia (Achalasia is a condition in which the peristalsis (a wave like movement) of the smooth muscles of the esophagus is impaired and the relaxation of the lower sphincter in the esophagus is impeded.).
- Esophageal tumor.
- Esophageal stricture (narrowing).
- Gastroesophageal reflux disease (GERD).
- Foreign body.
- Any allergy (eosinophilic esophagitis).
- scleroderma (scar tissues formed and cause hardening and stiffening of the tissues).
- Neurological disorders (stroke, Parkinson’s disease, Alzheimer’s disease).
4)explain the Clinical manifestation/sign and symptoms of the patient with the dysphagia. Explain the Clinical manifestation/sign and symptoms of the patient with dysphagia.
- Pain in swallowing.
- Difficulty in swallowing.
- Pulmonary aspiration.
- A sensation of food being stuck in the throat.
- Coughing.
- Choking.
- drooling of the saliva.
- Weight loss.
- Regurgitation of food
- (back flow of food) to happen.
- Frequent heart burn.
- Hoarseness of voice.
- gagging while swallowing.
5) Explain the diagnostic evaluation of the patient with the dysphagia. Write the diagnostic evolution of a patient with dysphagia.
- history tacking and physical examination.
- barrium swallow.
- fluoroscopy.
- X Ray.
- ct scan.
- MRI.
- Endoscopy.
- Ultrasonography.
- Esophageal muscle test (monometry).
6)explain the treatment of the patient with the dysphagia. Write the treatment of a patient with dysphagia.
- Dysphagia causes difficulty in swallowing, so advise the patient about swallowing therapy, exercise, and dietary changes.
- If the patient has esophageal stricture, educate him about dilatation.
- Insert a feeding tube for the patient to take food.
- Balloon dilation of the patient’s esophagus.
- If there is a problem with the esophageal sphincter, laparoscopic myotomy (making an incision on the lower sphincter of the esophagus to reduce pressure) should be performed.
- If the patient has gastroesophageal reflux disease (GERD), provide antacid medicine.
Nursing management of patients with the dysphagia Nursing management of patients with the dysphagia Write.
- If the patient has a condition of dysphagia, then all emergency equipment such as suction, oxygen and face mask should be kept at the patient’s bedside.
- Advise the patient to change the eating habit. Provide the patient with small amounts of food at frequent intervals and advise him to eat slowly.
- Provide the patient with a high Fowler position in the sitting position with the support of a chair or pillow.
- Advise the patient to identify the foods that cause the patient to have a condition of dysphagia and advise him to avoid those foods such as coffee, butter, spicy food etc.
- Provide proper mouth care to the patient before and after meals. If there is secretion present in the mouth, remove it by suction.
- Advise the patient to avoid tea, coffee, soft drinks, tobacco, alcohol, which are foods that form acid and cause heart burn.
- Provide a calm and comfortable environment to the patient.
- Advise the patient to avoid sticky foods such as peanut butter, chocolate, milk.
- Advise the patient to use a straw to ingest any liquid.
- Ask the patient to avoid talking while taking meals.
- Advise the patient to ingest semi-solid foods so that the patient does not have difficulty swallowing.
1)define/explain Achalasia. Define Achalasia.
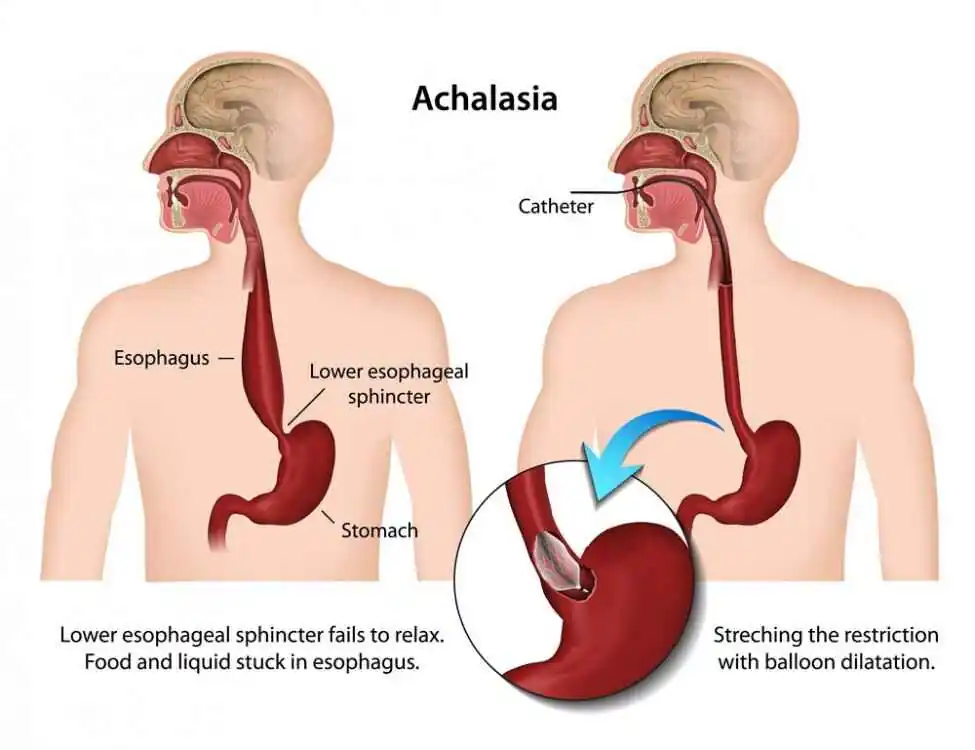
- Achalasia is a type of medical condition.
- Achalasia is a medical condition in which there is an inability of the lower oesophageal sphincter (lower oesophageal sphincter) to relax, due to which liquid and food cannot be transferred properly from the esophagus to the stomach.
- In Achalasia, the peristalsis movement (a wave like movement) of the esophagus is impaired.
- In Achalasia, the esophagus narrows just above the stomach, resulting in incomplete emptying of the esophagus and food not being transferred properly to the stomach.
2) Explain the Etiology/cause of the patient with Achalasia. Explain the causes of achalasia in patients.
- nerve damage (due to new damage).
- autoummune factore( autoimmune factor).
- genetic predisposition ( genetic predisposition).
- viral infection ( viral infection).
- autoimmune disease (autoimmune disease).
3) Explain the clinical manifestation/sign and symptoms of the patient with the Achalasia. Write the symptoms and signs of a patient with achalasia.
- Difficulty in swallowing.
- Chest pain.
- Heartburn.
- Discomfort while taking liquid and solid food.
- Gastric contents aspiration.
- Regurgitation (back flow of stomach contents).
- Having chest pain.
4) Explain the diagnostic evaluation of the patient with the Achalasia. Write the diagnostic evaluation of achalasia vada patient.
- History taking and physical examination.
- X rays.
- gastrointestinal examination.
- barium swallow.
- Endoscopy.
- Esophageal monometry.
5) Explain the management of the patient with the Achalasia. Write the management of a patient with achalasia.
medical management
1)calcium channel blocker and nitrates.
- Calcium channel blockers help relax the lower oesophageal sphincter, allowing food to pass properly into the stomach.
2)Botulinum toxin injection
- Botulinum toxin injection is given directly into the lower esophageal sphincter, which causes temporary relaxation of the lower oesophageal sphincter.
- But its effect is short-lived, so it needs to be repeated.
3)Dilatation (pneumatic balloon dilatation)
- In this procedure, a balloon is inflated in the narrowed esophagus.
- Due to this, the esophagus dilates and the food container empties into the stomach.
- But this procedure is also temporary and the esophagus needs to be dilated repeatedly.
surgery
- Surgical management involves cutting the lower oesophageal sphincter and removing the narrowing of the esophagus to relieve the obstruction.
Heller’s myotomy
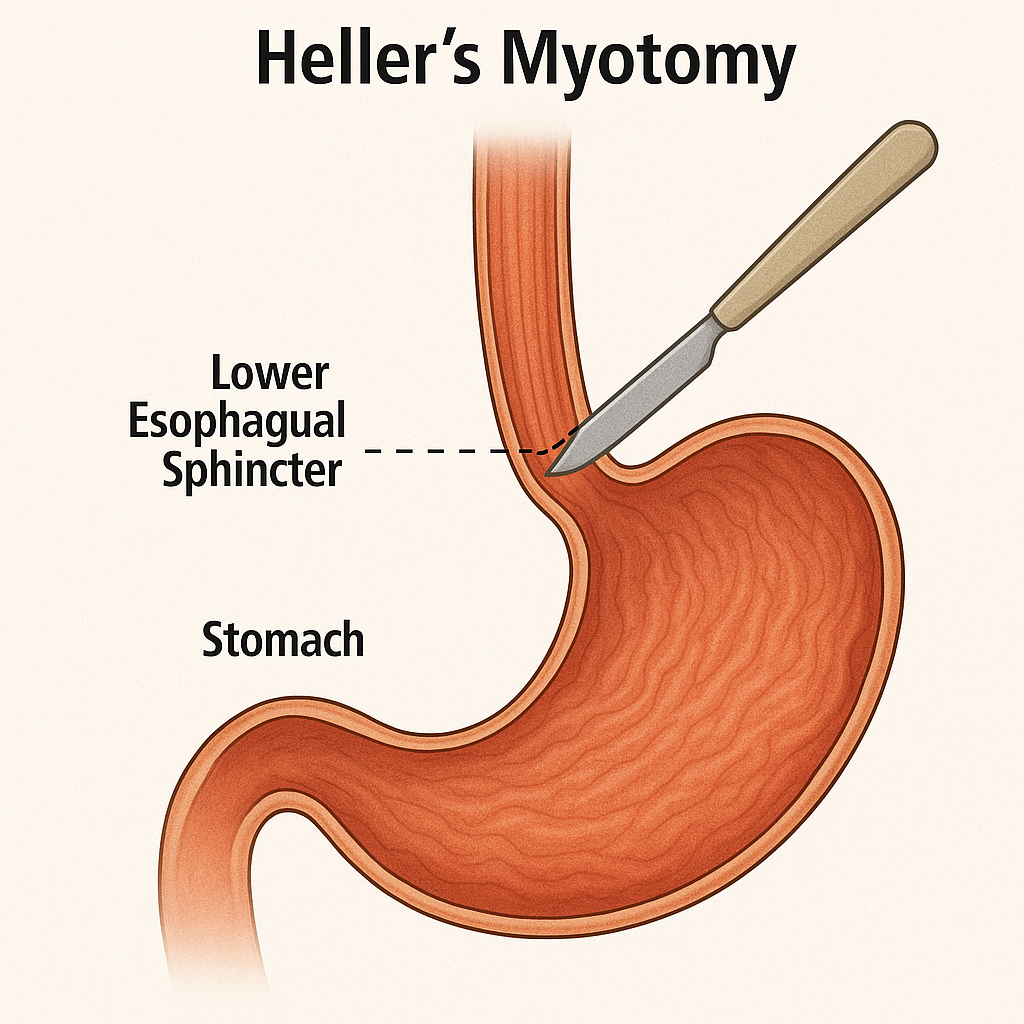
- In this procedure, the lower esophageal sphincter is surgically cut.
- An antireflux procedure (fundoplication) is also performed to prevent gastroesophageal reflux.
Explain the nursing management of patients with the Achalasia. Write the nursing management of a patient with Achalasia.
- Advise the patient to take a clear fluid, soft diet that is easy to swallow.
- Advise the patient to take high fiber food.
- Advise the patient to take a liquid diet and a bland diet.
- Advise the patient to take high fiber food such as fruits and vegetables.
- Advise the patient to take a diet rich in vitamin C.
- Advise the patient to avoid spicy food and pickles and spices.
- Advise the patient to avoid tea, coffee, junk food, ice cream, and hot diet.
- Encourage the patient to take plenty of fluids to prevent dehydration.
- Advise the patient to take proper rest and sleep to relieve pain and discomfort.
- Provide antibiotic medicine to prevent infection.
- Monitor the patient’s daily weight.
- Provide calcium channel blocker medicine to relieve muscle contraction.
- Provide analgesic medicine to relieve the patient’s pain level.
- Advise the patient to have regular follow-up.
1)explain/define the Gastroesophageal reflux disorder. Describe the gastroesophageal reflux disorder.
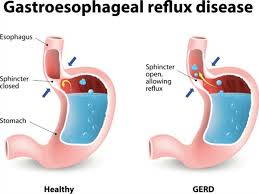
- In gastroesophageal reflux disorder, excessive amount of gastric and duodenal contents flow back into the esophagus.
- Because of incompetent •>oesophageal sphincture / •>pyloric stenosis/ •>esophageal motor disorder, stomach contents (acid) flow back into the esophagus. This causes a condition of irritation and inflammation.
2)explain the Etiology/cause of gastro esophageal reflux disorder. Explain the causes of gastroesophageal reflux disease.
- Due to neuromuscular development delay.
- Hyatal hernia (This is a condition in which part of the stomach crosses the diaphragm and comes upwards. ) .
- Due to cerebral defect.
- Due to loss of esophageal sphincter.
- Abdominal pressure is increased due to obesity, constipation.
- Due to fatty food intake.
- Smoking, chocolate, caffeine, alcohol, obesity, pregnancy, stomach emptying delay.
- Bronchopulmonary
- Dysphasia.
- Because of some type of medication. ( like: theophylline).
- Due to lower esophageal sphincter dysfunction.
- Due to delayed gastric emptying.
- Due to pregnancy.
- Due to certain food and lifestyle changes.
3) Explain the clinical manifestation/sign and symptoms of the patient with the gastro esophageal reflux disease. Describe the signs and symptoms of a patient with gastroesophageal reflux disease.
- Burning sensation.
- Heartburn.
- Regurgitation (back flow of food into the esophagus).
- Indigestion (dyspepsia).
- Abdominal Bloating.
- Odynophagia (pain on swallowing).
- Passing bloody and black stools.
- Burping.
- Hyper salivation.
- Chest pain.
- Difficulty swallowing ( dysphagia).
- Hiccups that don’t let up.
- nausea.
- hoarseness.
- Esophagitis (oesophagitis).
- Not feeling hungry.
- Weight loss.
- Discomfort in the upper abdominal area.
- Nausea.
- Hoarseness.
- Whistling sound,
- Dry cough,
- chronic sore throat.
4)explain the Diagnostic evaluation of the patient with the gastero esophageal reflux disease. Write the diagnostic evaluation of the patient with gastroesophageal reflux disease.
- history tacking and physical examination.
- Barrium swallow.
- Endoscopy.
- Bilirubin monitoring.
- Esophageal histology finding.
- Esophagogastroduodenoscopy
(EGD) . - Esophageal monometry.
- PH monitoring of the esophagus.
- biopsy.
5) Explain the management of the patient with the gastroesophageal reflux disease. Write the management of a patient with gastroesophageal reflux disease.
- provide antacid to the patient.
- Ex:=antacids such as maalox,
Mylanta,
Gelusil,
Rolaids,
Tums. - provide proton pump inhibitor to the patient.
- Proton pump inhibitor medicine is given when the patient has severe symptoms. To provide.
- Ex:=proton pump inhibitor drugs are:
•>omeprazole ( prilosec),
•>lansoprazole
( prevacid),
•>Rabeprazole
( Aciphex),
•>pantoprazole
( protonix),
•>Ex omeprazole (Nexium). - Provide Acid suppressants to the patient.
- Provide prokinetic agents to the patient.
surgery and other procedures.
fundoplication:
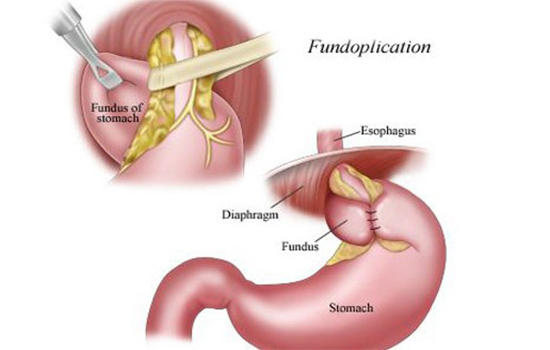
1)procedures:
- In this surgical intervention, the surgeon wraps the upper part of the stomach and the lower part of the esophagus.
- This creates a valve-like structure.
- This procedure prevents the contents of the stomach from coming into the esophagus.
2)Approaches:
1)Laparoscopic fundoplication
- This procedure is a minimally invasive procedure in which a small incision is made. And a camera and special instruments are placed.
- This mainly results in faster recovery and fewer post-operative complications than open surgery.
2)Open fundoplication:
- Open surgery is also performed in certain types of cases.
3)Types of fundoplication ( Type of Fundoplication
A)Nissan fundoplication
- This is the most common type of fundoplication in which the fundus part of the stomach is completely wrapped around the esophagus.
B)Partial fundoplication
- In this procedure, part of the stomach is partially wrapped.
Antroplasty /pyloroplasty
- This is a procedure in which the lower part of the stomach (pylorus) is widened so that the contents of the stomach can completely empty into the duodenum.
- do a gasrotomy (surgically opening into the stomach).
explain the Nursing management of patients with the gastroesophageal reflux disease. Write the nursing management of patients with the gastroesophageal reflux disease.
- Take a complete medical history and physical examination of the patient.
- Provide the patient with complete information about the gastroesophageal reflux disease, its causes, its signs and symptoms and its treatment.
- Advise the patient to make proper dietary modifications such as avoiding fatty and spicy foods. Advise the patient to avoid food.
- Advise the patient to maintain proper body weight.
- Advise the patient to consume soft drinks such as tea, coffee, alcohol in small quantities.
- Advise the patient to avoid smoking, cigarettes, fatty and spicy food, milk, onion, garlic.
- Advise the patient not to lie down directly after eating.
- Advise the patient to eat a diet low in fat, high in protein, high in fiber, and green leafy vegetables.
- Advise the patient to make lifestyle modifications, including maintaining a proper weight and avoiding smoking and tobacco.
- Advise the patient to take medications such as antacids and proton pump inhibitor medicines properly.
- Advise the patient to take medications properly, such as antacids and proton pump inhibitor medicines.
- Advise the patient to take Advise the patient to lie down only after two hours after eating.
- Advise the patient to take food three hours before lying down so that acid reflux can be prevented.
- Advise the patient to take proper fluid intake.
- Advise the patient to take small and frequent amounts of food.
- As some medications cause acid reflux, advise the patient to drink water properly before taking the medicine. Drink.
- Advise the patient to walk after every meal.
- Advise the patient to take medicine properly.
- Provide proper emotional support to the patient.
- Provide proper health education to the patient.
1) explain/define Esophagus cancer. Define Esophageal Cancer
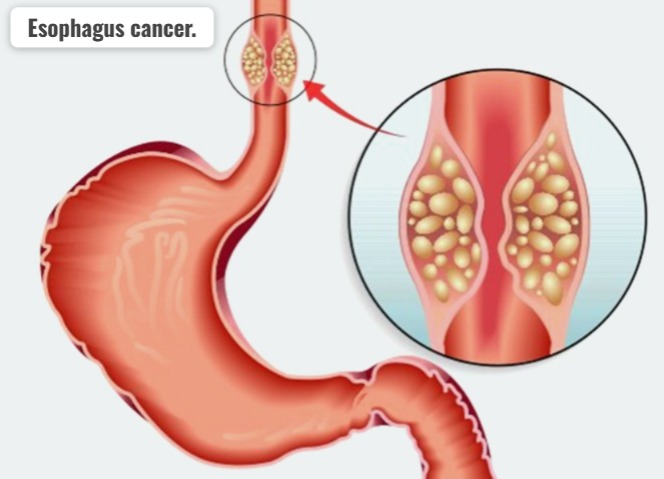
- This is cancer of the esophagus and it involves the lining of the esophagus and its muscles and lymph nodes and the development of cancer.
- In esophageal cancer, there is abnormal and uncontrolled growth of epithelial cells in the esophagus
and formation of tumors and it creates cancer of the esophagus.
2) explain the types of esophageal cancer. Name the types of esophageal cancer.
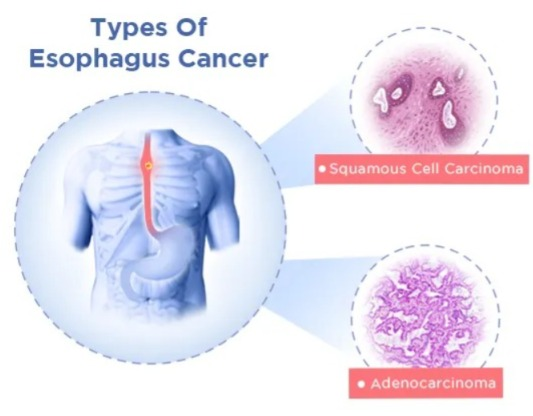
There are two main types of esophageal cancer.
1)Adenocarcinoma of the esophagus
2)squamous cell carcinoma of the esophagus
1)Adenocarcinoma of the esophagus.
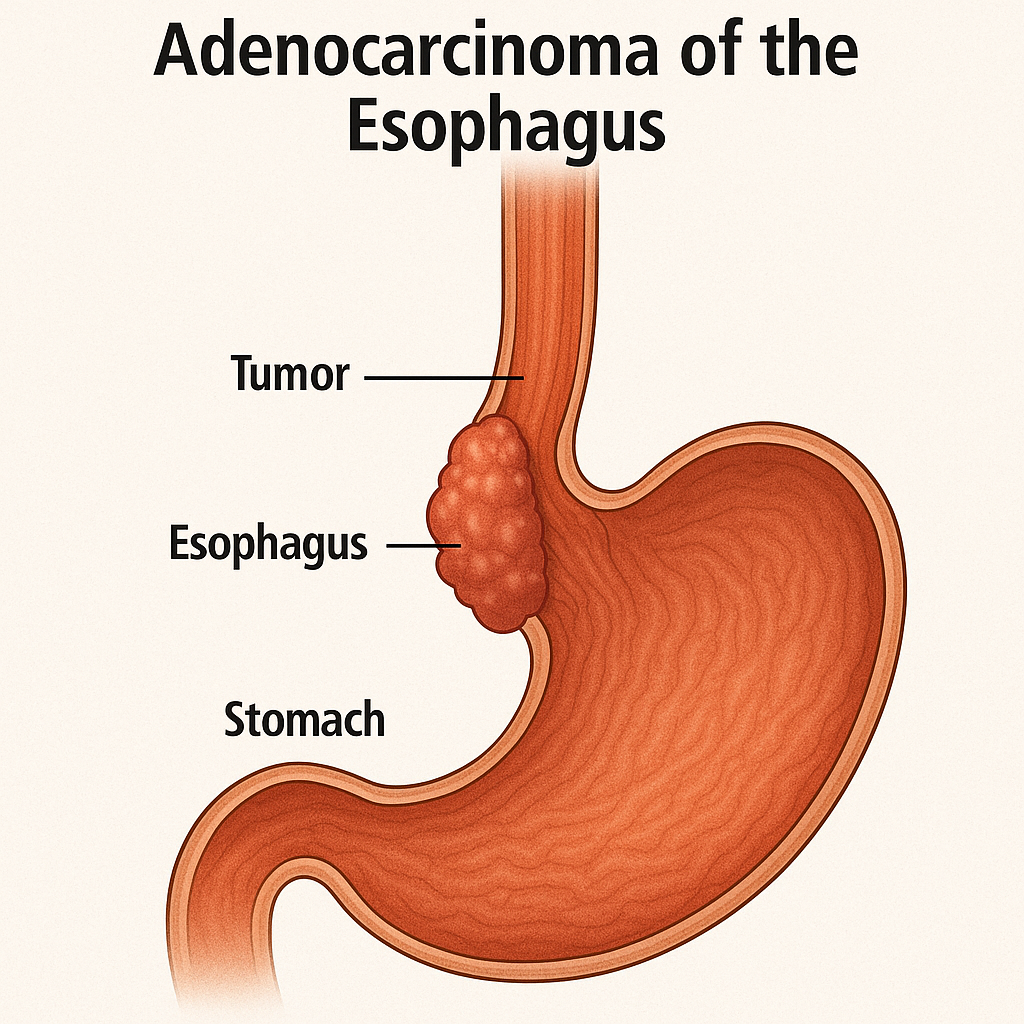
- Adenocarcinoma is found in the lower part of the esophagus and near the stomach.
- United States (United Adenocarcinoma is the most common type of esophageal cancer in the United States.
2) Squamous cell carcinoma of the esophagus
This type of cancer is mainly found in the upper 2/3 of the esophagus.
Squamous cell carcinoma is mainly found in the United States, but is less common in Americans.
But the most common type of cancer in the world is esophageal cancer.
3) Explain Etiology/cause of the patient with the esophageal cancer.
- 1)Gender more in men ,👨🦼
- 2)Race (race) Esophageal cancer occurs more in African and American races.
- 3)Age: It occurs more in people after the age of 50.
- 4)use of Alcohol and tobacco,
- 5)GERD( Gastero esophageal reflux disease : Gastero esophagitis Dizziness),
- 6)hot,spicy dietary intake (due to excessive spicy fried food),
- 7)Exposure to niterosomine in food/Environments.
- 8) Obesity.
- 9) Due to acid reflux.
- 10)chronic peptic sore.
- 11) Diet low in fruits and vegetables.
- 12) Human papillomavirus.
- 13) Iron deficiency.
- 14) Barrett esophagus.
- 15) Medical history of head and neck cancer.
- 16) Any radiation therapy.
- 17) coeliac disease.
- 18) Due to thermal injury.
- 19) Achalasia.
4) explain the clinical manifestation/sign and symptoms of the patient with the esophageal cancer.
- Dysphagia (severe difficulty swallowing),
- feeling of lump in throat. (lump in throat),
- painfully and difficulty in swallowing (difficulty swallowing),
- regurgitation of undigested food (undigested food comes back into the mouth),
- loss of appetite (loss of appetite),
- loss of weight (loss of weight),
- food gets stuck in the esophagus Going.
- Losing a lot of weight.
- Pain in the throat and pain in the part behind the breastbone and between the shoulder blades.
- Hoarseness and chronic cough.
- Coughing up blood.
- Heartburn.
- Nausea.
- vomiting.
- Regurgitation of food (back flow of the food).
5) Explain the diagnostic evaluation of the patient with the esophageal cancer. Write the diagnostic evaluation of a patient with esophageal cancer.
- History tacking and physical examination ,
- X Ray,
- Ct scan,
- MRI,
- PET (Positron Emissive Tomography),
- barrium swallow.
- gastro esophagoscopy.
- biopsy.
6) explain Management of the patient with the esophageal cancer. Write the management of the patient with esophageal cancer.
- Radiation therapy,
- chemotherapy,
- De bulking surgery,
- chemotherapy and radiation therapy combination
- laser therapy.
- photodynamic therapy
7) Explain the nursing management of the patient with the esophageal cancer. Write the nursing management of a patient with esophageal cancer.
- Check the patient’s vital signs.
- Provide emotional support to the patient.
- Maintain hygienic conditions.
- Feed the patient with high calorie and high protein rich food.
- Meet all the needs of the patient To do.
- While giving chemotherapy and radiation therapy to the patient, check whether he is experiencing any side effects.
- To check if the patient is experiencing any adverse effects.
- To maintain the nutritional status of the patient.
- To maintain the patient’s fluid level.
- To monitor any side effects of the patient and his family members. Clear all doubts.
- Provide psychological support to the patient and his family members.
- Provide total parenteral nutrition if the patient is unable to take food orally.
- If the patient is unable to swallow, insert an esophageal stent to keep the esophagus patent.
- Provide intravenous fluid to the patient.
- Monitor the patient’s arterial blood gas level.
- Advise the patient to avoid overeating. Advise the patient to take food in small amounts.
- Advise the patient to report immediately if nausea, vomiting, cough, difficulty in swallowing occurs.
- Provide a calm and comfortable environment to the patient.
1)Explain/define Esophageal stricture. Define esophageal stricture.
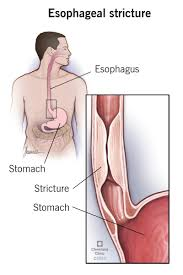
- In esophageal stricture, the esophagus gradually narrows or tightens. This causes difficulty in swallowing.
- Esophageal stricture is caused by the build up of scar tissues in the esophagus.
- When the lining of the esophagus is damaged, scarring develops in the esophagus.
- When this scarring develops, the esophagus becomes stiff. When there is a build up of continuous stiffness in the esophagus, difficulty in swallowing also occurs.
2)explain the Etiology/cause of the patient with the esophageal stricture. Explain the etiology/cause of the patient with the esophageal stricture.
- Due to gastroesophageal reflux disease.
- caustic ingestion ( acid or alkali).
- due to prolonged use of a nasogastric tube.
- malignancy.
- due to injection of any toxic chemical.
- Due to ingestion of any corrosive substance (household cleaning agents).
- Chronic and severe viral and bacterial infections.
- •>candida.
•>herpes simplex virus (HSV).
•>cytomegaloviral (CMV).
•>Human immunodeficiency virus (HIV). - Injury caused by use of endoscope Due to.
- In an immunosuppressed patient or a transplant recipient.
- Due to scar formation from previous surgery.
- Due to esophageal cancer.
- Medication induced stricture.
- •>Non steroidal anti inflammatory drug ( NSAID).
- •>phynytoin.
- •>potassium chloride.
- •>quinidine.
- •>tetracycline.
- •>Acorbic acid.
- Idiopathic
- Eosinophilic Esophagitis (idiopathic eosinophilic esophagitis).
- due to extrinsic compression.
- due to squamous cell carcinoma.
3)explain the Clinical manifestation/sign and symptoms of the patient with the esophageal stricture. Describe the symptoms and signs of a patient with esophageal stricture.
- Difficulty in swallowing.
- Discomfort with swallowing.
- Feeling that food is stuck in the esophagus.
- Regurgitation of food.
- Weight loss.
- Heartburn.
- Bitter and acidic taste in the mouth.
- Choking.
- Coughing.
- Shortness of breath.
- Frequent burping or hiccups.
- Pain on swallowing.
4)explain the Diagnostic evaluation of the patient with the esophageal stricture . Write the diagnostic evaluation of the patient with esophageal stricture.
- history tacking and physical examination.
- Barrium swallow.
- Endoscopy examination.
- Complete blood cell count.
- liver profile.
- complete metabolic panel.
- Imaging studies.
- Barium esophagram.
- Chest radiograph (posterior anterior and lateral).
- X rays.
- ct scan.
- Endoscopic ultrasound.
5) Explain the management of the patient with the esophageal stricture. Write the management of a patient with esophageal stricture.
- Properly provide antibiotic medicine to the patient.
- Perform esophageal dilation (pneumatic dilatore).
- Provide proton pump inhibitor medicine to the patient.
- Ex:= omeprazole,
Lansoprazole,
Rabeprazole.
Explain the nursing management of patients with the esophageal stricture. Write the nursing management of a patient with esophageal stricture.
- Advise the patient to make lifestyle modifications.
- Advise the patient to avoid fatty food, spicy food, alcohol, chocolate, and peppermint.
- Advise the patient to eat small amounts of food frequently.
- Advise the patient to avoid eating in a hurried manner.
- Advise the patient to eat two to three hours before bedtime.
- Advise the patient to lose weight.
1)explain/define Esophageal varices. Define esophageal varices.
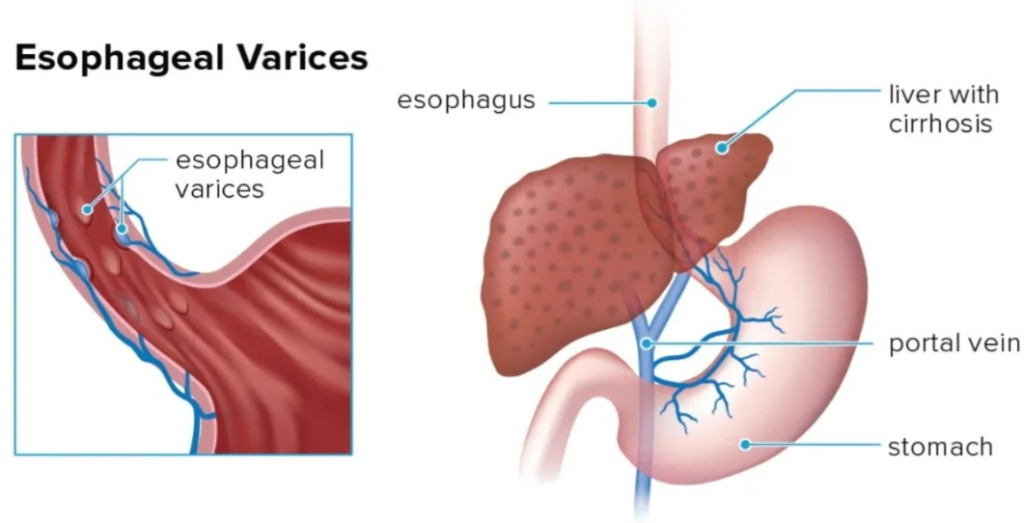
- Esophageal varices are abnormally enlarged veins in the lower part of the esophagus. enlarges.
- Esophageal varices are most common in patients with liver cirrhosis.
- Esophageal varices develop when the normal blood flow in the liver slows down.
- This causes blood flow to back up into nearby smaller blood vessels.
- It mainly occurs in the vessels of the esophagus, causing the blood vessels to dilate.
Esophageal varices develop - Many times esophageal varices rupture. This creates life threatening bleeding.
2)explain the Etiology/cause of esophageal varices . State the cause of esophageal varices.
- Liver failure.
- Liver cirrhosis.
- Portal hypertension.
pre hepatic cause:
- Portal vein thrombosis.
- Increased portal blood flow fistula.
- Portal vein obstruction.
Intra hepatic:
- cirrhosis due to varices cause.
- idiopathic portal hypertension.
- acute hepatitis.
- schistosomiasis.
- congenital hepatic Fibrosis.
- Myelosclerosis.
post- hepatic :
- Budd chiary syndrome.
- Constrictive pericarditis.
other cause:
- Liver disease.
- Malnutrition.
- Due to alcohol ingestion.
- Physical exercise.
- Circadian rhythm.
- Increases intra-abdominal pressure.
- Aspirin intake.
- Non steroidal anti inflammatory drug ( NSAID).
- Bacterial infection.
3) Explain the clinical manifestation of the patient with the clinical manifestation/sign and symptoms of the patient with the esophageal varices. Write the symptoms and signs of esophageal varices.
- Gastrointestinal bleeding.
- Hematemesis (blood in vomit).
- Abdominal pain.
- Dysphagia (dysphagia: difficulty in swallowing).
- Odynophagia (odynophagia:= pain in swallowing).
- Confusion.
- Symptom of Anemia and shock.
- Blood in vomiting.
- Abdominal pain.
- Ascites (Acities: accumulation of fluid in to the stomach).
- Hepatic encephalopathy.
- Pallor
- Hypotension/shock.
- Reduced urine output.
- Malena.
- Reduced Glasgow Coma Scale.
- sign of sepsis .
4)explain the diagnostic evaluation of the patient with the esophageal varices. Write the diagnostic evaluation of the patient with the esophageal varices.
- History taking and physical examination.
- Complete blood count (CBC).
- hemoglobin level assessment.
- assess the platelet count.
- assess the international normalized ratio (INR).
- renal function test
- liver function test.
- Computerized Tomography (ct scan assessment).
7) Explain the management of the patient with the digestive and gastro intestinal disorder. Write the management of a patient with gastro intestinal disorder.
1)Endoscopic band ligation
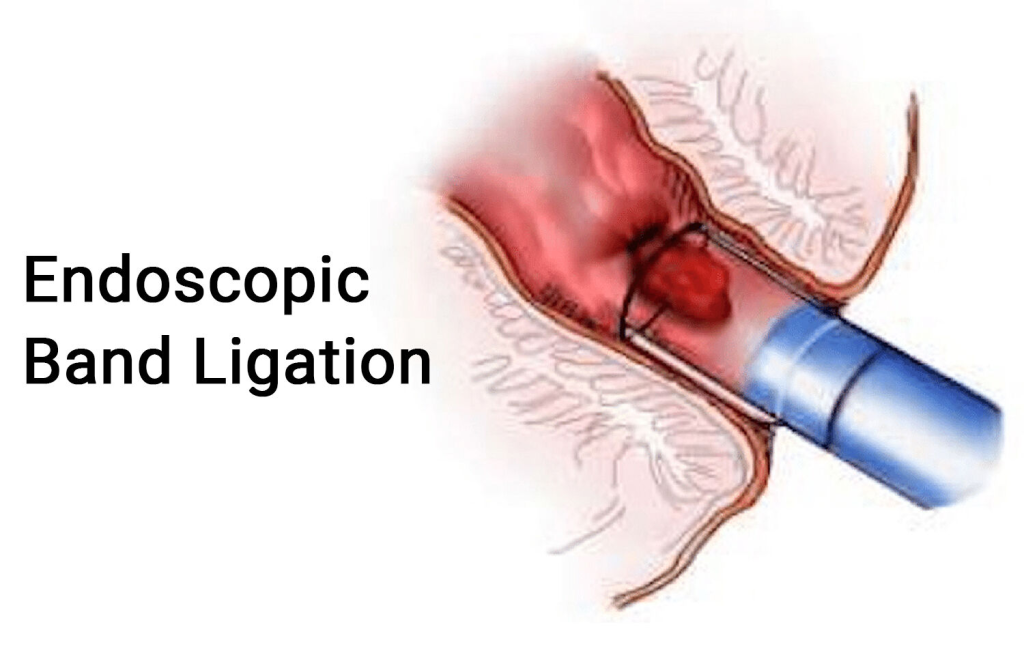
- In endoscopic ligation, a rubber band is tied around the bulging vein and the bleeding is stopped.
- Endoscopic band ligation is considered the first line treatment for esophageal varices.
2) Balloon tamponade ( Balloon Tamponade)
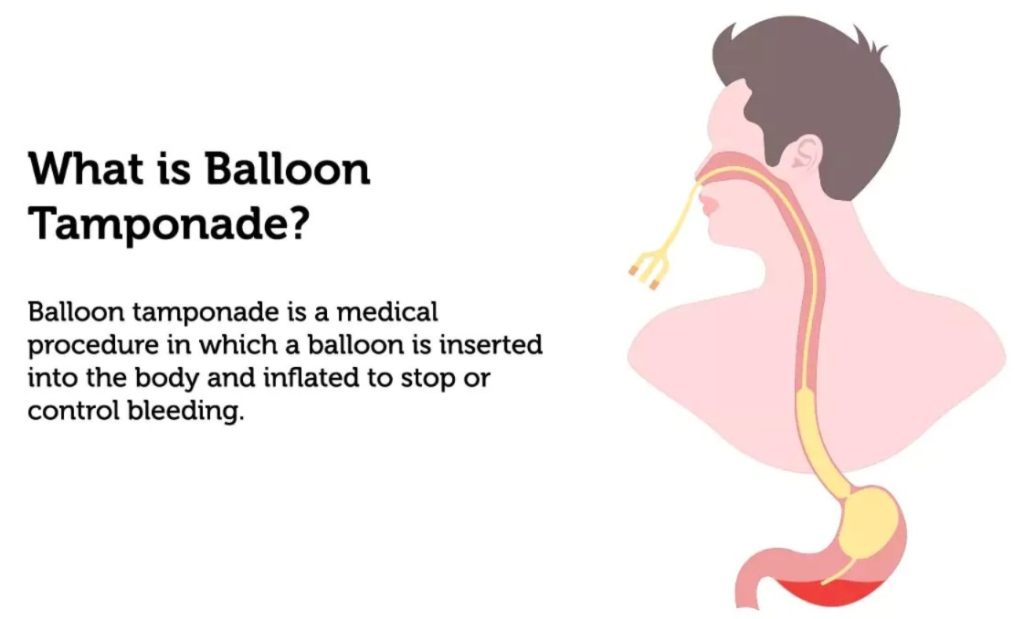
- In the balloon tamponade procedure, a balloon is inserted through the nose and The bleeding that occurs is stopped.
3) Sclerotherapy
- In sclerotherapy, an injection is introduced into the building site and due to this, the blood clots and the bleeding also stops.
4)Drug therapy
In drug therapy, drugs are provided to reduce blood pressure.
Ex:= terlipressin,
Vasopressin,
NIitroglycerine,
Octerotides.
Somatostatin.
5)Transjugular intrahepatic portosystemic shunting (TIPS)
6) Distal splenorenal shunt (DSRS). ,
7)Esophagial Transection.
8)Liver transplantation.
explain the nursing management of patients with the esophagial varices. Write the nursing management of a patient with esophagial varices.
- Advise the patient to stop drinking alcohol.
- Advise the patient to eat a healthy diet.
- Advise the patient to eat fruits and vegetables.
- Advise the patient to avoid fatty and spicy foods.
- Advise the patient to maintain his body weight. Give.
- Advise the patient to maintain proper hygiene.
1)define/explain hiatus hernia . Define hiatus hernia.
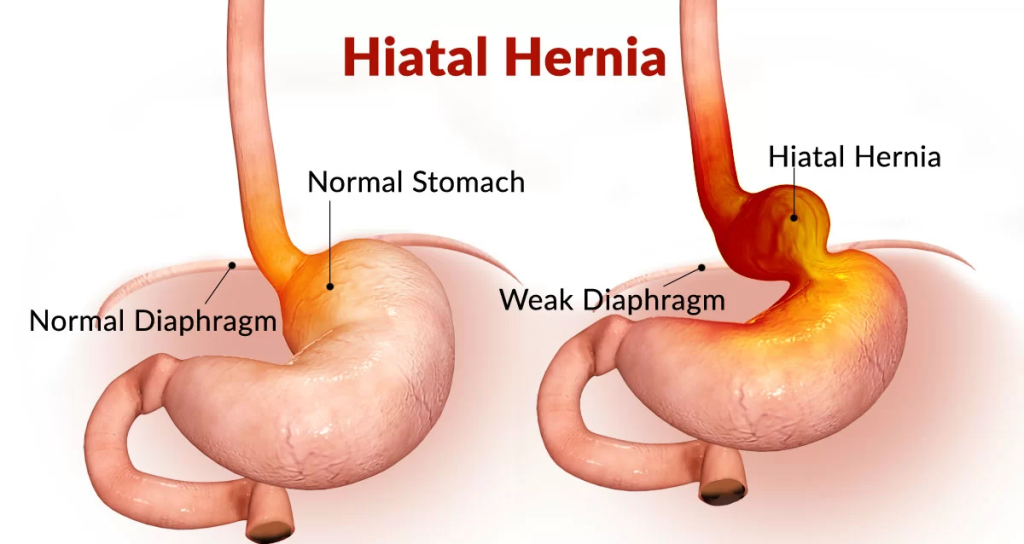
- Hiatus hernia is a condition in which the esophagus protrudes through an opening in the diaphragm (its called hiatus) A part of the stomach protrudes from the abdominal cavity into the chest cavity through the space (hiatus) where the stomach enters the abdominal cavity. This is called a hiatus hernia.
- Hiiatus hernia is a more common disease of the gastro intestinal track.
2)Explain the types of hiatus hernia. Write the type of hiatus hernia.
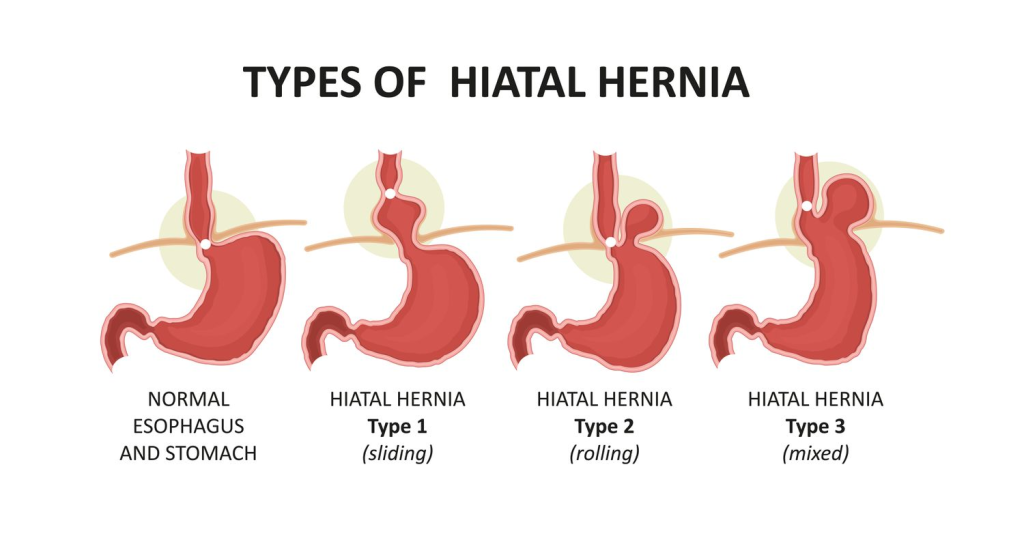
There are a total of four types of hiatus hernia.
1) sliding hiatus hernia,
2)fixed hiatus hernia,
3)complecated hiatus hernia,
4)Rolling/para esophageal hernia
1) Sliding hiatus hernia,
- In sliding hiatus hernia, the upper most part of the stomach, the gastroesophageal sphincter, protrudes into the chest cavity.
2) Fixed hiatus hernia (Fixed hiatus hernia),
- In fixed hernia, the uppermost part of the stomach protrudes into the chest cavity.
- This type of hernia is not serious and has few symptoms.
3) Complicated hiatus hernia ( Complicated hiatus hernia),
- Complicated hiatus hernia is the most complex form of hernia.
- In this hernia, the entire stomach protrudes into the chest cavity.
- This type of hernia has many symptoms and causes great difficulty for the patient.
- This type of hernia is not common.
4)Rolling/para esophageal hernia (Rolling or Paraesophageal Hernia)
- In rolling/paraesophageal hernia, the junction where the esophagus and stomach are connected remains normal.
- But parts of the stomach protrude into the chest cavity.
3) Explain the classification of the hiatus hernia. Write the classification of hiatus hernia
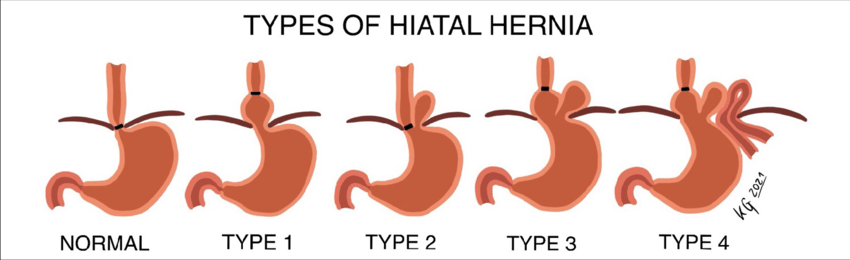
- type:=1 hiatus hernia,
- type:=2 hiatus hernia,
- type:=3 hiatus hernia,
- type:=4 hiatus hernia .
type:=1 hiatus hernia,
- This type of hernia involves the gastroesophageal junction and the chest of the stomach. Displacement occurs in the cavity.
- This type of hernia is symptomatic and asymptomatic.
- This type of hernia mainly requires surgical intervention to place the hernia in the abdominal cavity.
type:=2 hiatus hernia,
- In this type of hernia, the stomach protrudes into the chest cavity and the gastroesophageal junction is in its normal position.
- This type of hernia is mainly caused by the tissue of the diaphragm muscles becoming loose.
type:=3 hiatus hernia,
- This is mainly a type one and type two type of hernia Combination
( its a combination of type 1 and type 2 hernia ) is. - In this type of hernia, the gastroesophageal junction and the fundus part of the stomach protrude into the chest cavity.
- This type of hernia is massive, so it is called a giantesophageal hernia.
type:=4 hiatus hernia .
- In this type of hernia, other organs of the abdomen are also displaced.
- Ex:=•> omentum,
- •> Transverse colon,
- •>Mesocolon,
- •>Spleen.
4) Explain the etiology/cause of the patient with the hiatus hernia. State the cause of hiatus hernia.
- Due to excessive consumption of white flour (mandan flour), and its products such as cakes, pastries, biscuits,
white bread. - Aging. (Mainly seen in old age people due to diaphragm muscles.).
- Refined sugar.
- Due to trauma and surgery.
- Due to obesity.
- Poor nutrition.
- Due to genetic abnormalities.
- Due to pregnancy.
- chronic straining.
- Connective tissue disorder.
5)explain the Clinical manifestation/sign and symptoms of the hiatus hernia. Write the symptoms and signs of hiatus hernia.
- Heartburn.
- Sense of fullness after eating.
- Indigestion.
- Retrosternal pain.
- Nausea.
- vomiting.
- Regurgitation (back flow of food).
- Anemia.
- Difficulty swallowing.
- Chest pain.
- belching or hiccups.
6) Explain the diagnostic evaluation of the patient with the hiatus hernia. Write the diagnostic evaluation of a patient with hiatus hernia.
- history tacking and physical examination.
- upper GI barium.
- chest x rays studies.
- gasteroscopy.
- Barrium swallow.
- Fluoroscopy.
- Upper intestinal endoscopy.
7)explain the management of the patient with the hiatus hernia. Write the management of a patient with hiatus hernia.
- Provide antacid medicine to the patient.
- Ex:=
•> maalox,
•>Mylanta,
•>Gelusil,
•>Tums. - Advise the patient to avoid alcohol and smoking.
- Give the patient prokinetic medication.
- Ex:=
•>reeglan,
•>Bethanacol, - Provide the patient with proton pump inhibitor medicine.
- Ex:=
•>prilosec
( omeprazole),
•>Prevacid
( esomeprazole), - Give the patient histamime blocker medicine.
- Ex:=
zantac
( ranitidine),
Tagmet
( cimetidine),
Pepcid
( famotidine).
surgical management
1)Nyssen fundoplication
- This is a laparoscopic procedure in which the upper part of the stomach is wrapped around the lower esophageal sphincter, which can prevent gastric reflux.
2) Laparoscopic hiatal hernia repair,
- This is a minimally invasive procedure in which the upper part of the stomach is wrapped around the lower esophageal sphincter, which can prevent gastric reflux. The hernia is replaced using stitches and mesh.
- This surgery mainly has a shorter healing time than traditional open surgery.
3) Toupet fundoplication
- Troupet fundoplication is mainly similar to Nissen fundoplication but only partially The fundus is wrapped around the esophagus.
- In paraesophageal hernia, the stomach, which has protruded into the chest cavity, is placed back in its normal position in the abdominal cavity.
- Hill procedure is used to fix the lower esophagus in place (diaphragm) to prevent its upward moment and hernia.
4) Paraesophageal hernia
5)Hill procedures
Explain the nursing management of patients with the hiatus hernia. Write the nursing management of a patient with hiatus hernia.
- Collect the patient’s history properly.
- Properly monitor the patient’s vital signs.
- Advise the patient to eat soft diet like porridge, khichdi etc.
- Serve food to the patient in an attractive manner.
- Advise the patient to eat food in small and frequent amounts Give.
- Advise the patient to take a bland diet.
- Provide antacid medicine to the patient.
- Assess the patient’s skin color and turgor.
- Advise the patient to take clear fluids, coconut water.
- Advise the patient to maintain oral hygiene.
- Provide the patient with intravenous fluid.
- Provide the patient with antiemetic medicine.
- Assess the patient’s pain level.
- Assess the duration and location of the patient’s pain.
- Provide comfort measures to the patient.
- Properly dispose of the patient And give advice to take sleep.
- Place the patient in a semi-fowler position.
- Provide analgesia if the patient is in pain.
- Assess the patient’s daily routine activity.
- Advise the patient to rest and sleep properly.
- Properly provide the patient with diversional therapy such as Or give advice for music, newspaper, sports etc.
- Give advice to the patient to take a properly balanced diet.
- Provide multi-vitamin medicine to the patient.
1)Define/explain gastritis. Define gastritis.
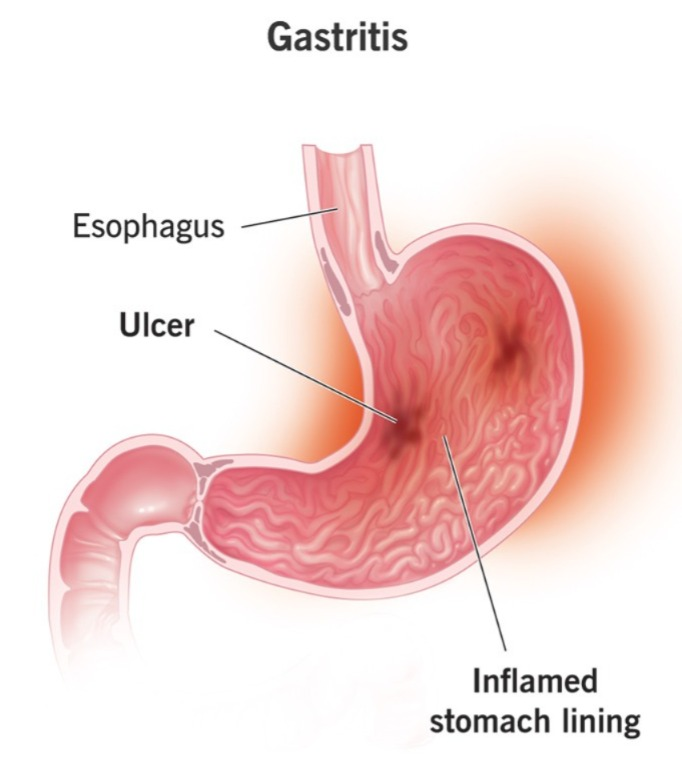
Gastritis is mainly made up of two words.
★ “Gastro” meaning: “stomach “
★ “Itis” meaning : “inflammation”
- Gastritis means inflammation, infection, irritation and erosion of the stomach mucosal lining.
- gastritis means infection and inflammation of the stomach mucosal lining.
2) Explain the types of gastritis. Tell the type of gastritis.
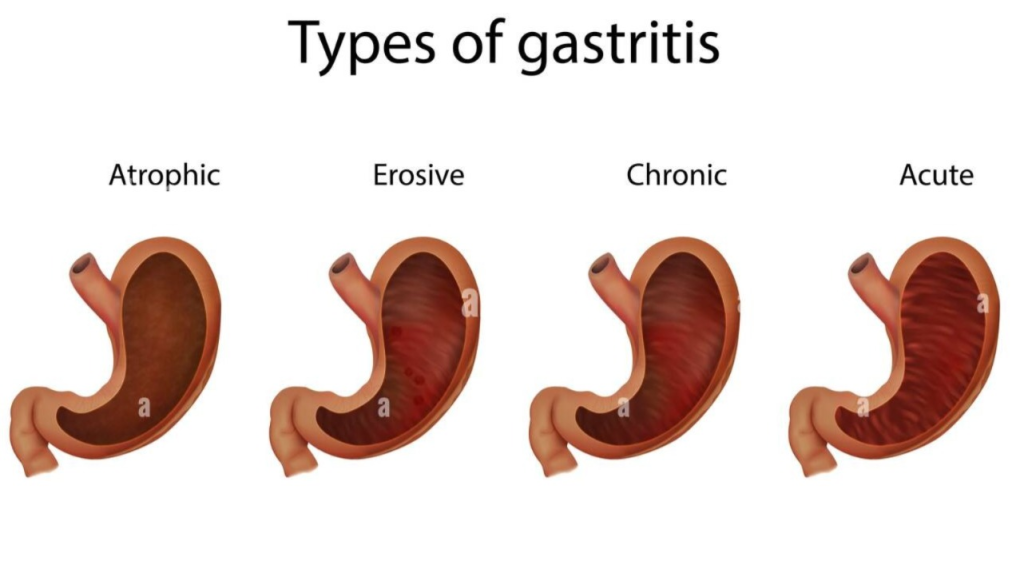
There are a total of seven types of gastritis. :
1)Acute gastritis (Acute gastritis),
2) Chronic gastritis (Chronic gastritis),
Other type of chronic gastritis :
A) Erosive gastritis,
B)Non erosive gastritis,
C)Acute stress gastritis ( acute stress gastritis),
D)Atrophic gastritis ( atrophic gastritis),
E)H.pylori ( heliobacterium pylori ) associated gastritis.
( Helicobacterium pylori associated gastritis),
F)Autoimmune gastritis (autoimmune gastritis),
G)chemical gastritis (chemical gastritis),
1)Acute gastritis (acute gastritis),
- Acute gastritis is the most common type of gastritis condition.
- Acute gastritis mainly develops suddenly and in the short term.
- In acute gastritis, there is inflammation in the stomach lining and it mainly occurs suddenly and due to this, bleeding is also seen in the mucosal lining of the stomach.
- In this, bleeding is mostly seen for less than 24 hours.
- Acute gastritis is caused by the bacteria Helicobacter pylori.
- Acute gastritis is mainly caused by spoiled food, dead fish, animal, bone, plastic, goods, chemicals, drugs, toxic, plants, and viral infections.
- Acute gastritis is mainly caused by non-steroidal anti-inflammatory drugs, alcohol, and viral and bacterial infections.
2) Chronic gastritis,
- Chronic gastritis is mainly seen in older people’s.
- Chronic gastritis is a long-term (gradual) inflammation of the mucous lining of the stomach.
- Chronic gastritis is mainly spread by a bacteria called Helicobacter pylori (H. Pylori).
- Chronic gastritis mainly occurs when the sphincter at the top of the stomach does not function properly, causing the stomach to leak acid. Acid comes into the esophagus, causing conditions like chest pain, heart burn.
- Chronic gastritis is mainly caused by an infection, pernicious anemia, and irritating substances.
Other type of chronic gastritis :
A) Erosive gastritis ,
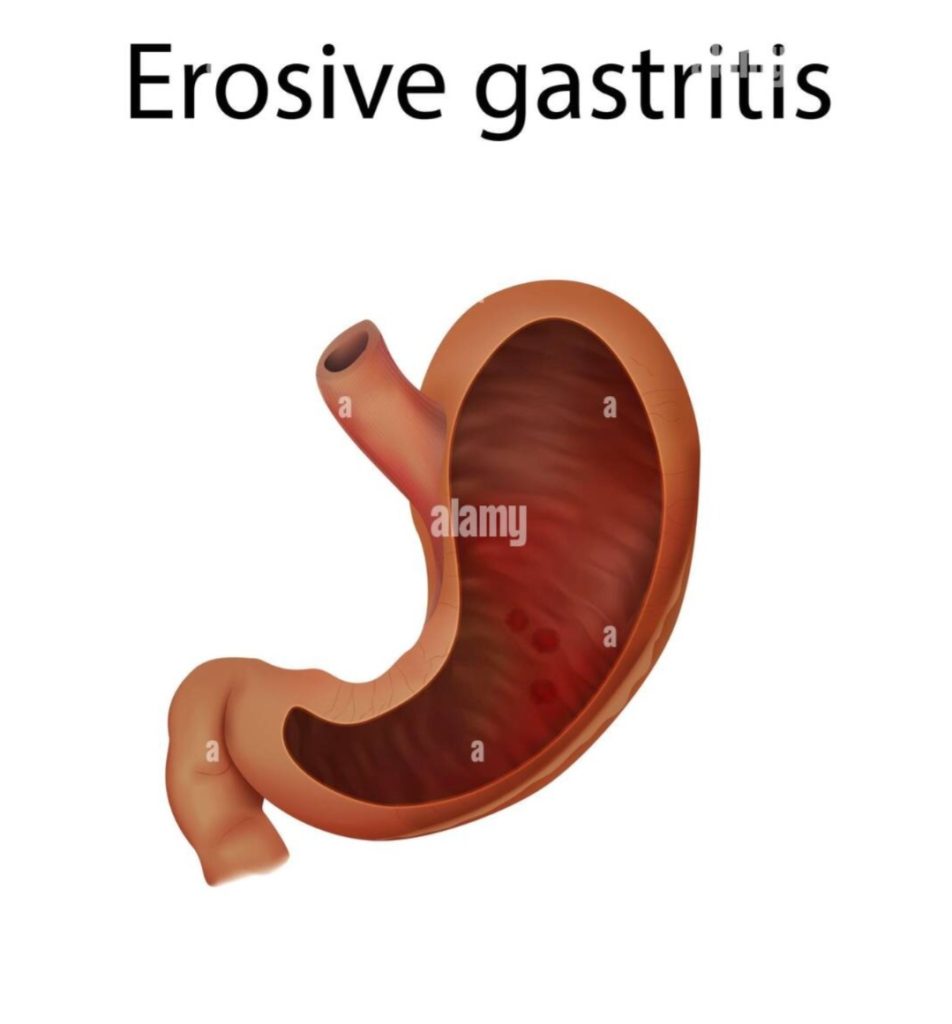
- Erosive gastritis is mainly caused by erosion in the mucosal lining of the stomach.
- Erosive gastritis is caused by any irritating substance
- Such as alcohol, Non steroidal anti inflammatory drug (NSAID) etc.
- In erosive gastritis, weight loss, lesions in the mucosal lining of the stomach, abdominal pain occur.
B) Non Erosive gastritis,
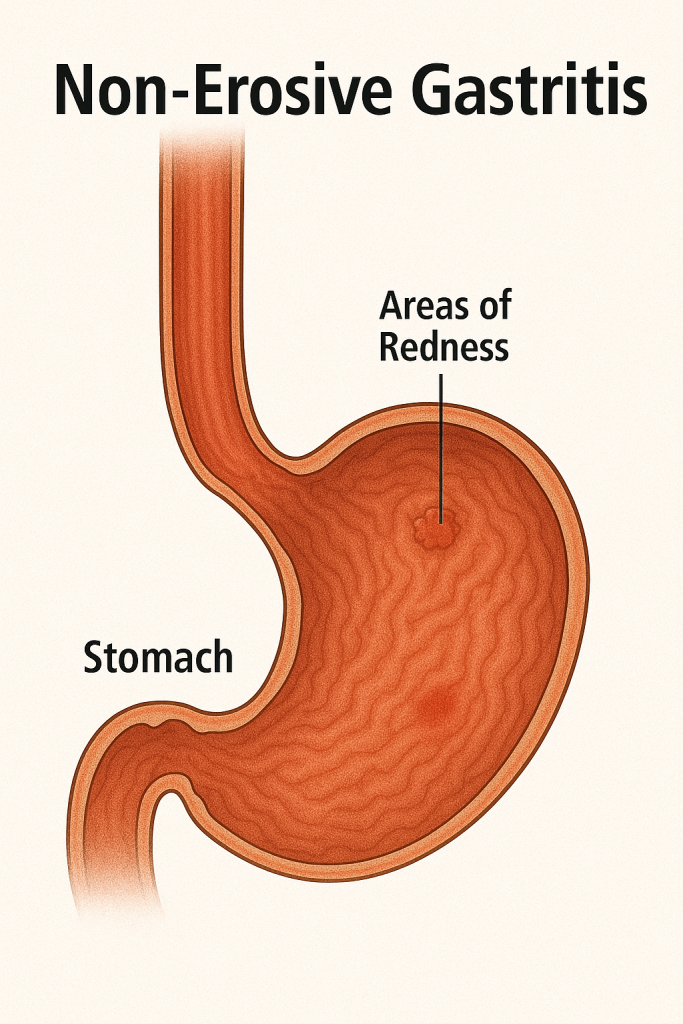
- Non-erosive gastritis is caused by histological abnormalities and is caused by Helicobacter pylori infection (H. Pylori).
- In non-erosive gastritis, the body accidentally identifies the stomach as a foreign protein and infection, due to which antibodies are produced in the body against it and cause severe damage to the mucosal lining of the stomach, due to which the condition of non-erosive gastritis arises.
C) Acute stress gastritis,

- Acute stress gastritis is caused by any severe illness, and injury.
- Acute stress gastritis is mainly seen in patients who are,
•> in the intensive care unit (ICU),
•> in patients who have respiratory failure, •> neurological trauma,
•> severe burn, ,
•> Peritonitis (infection and inflammation of the peritonium layer of the stomach), - Due to all these reasons, the condition of acute stress gastritis arises.
D) Atrophic gastritis (atrophic gastritis),
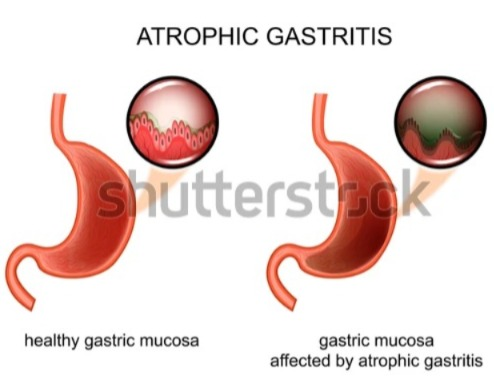
- Atrophic gastritis is a chronic form of gastritis in which the gastric mucosal lining becomes very thin (thin/atrophy) and the cells in the stomach that produce digestive acid and enzymes are lost.
- This type is mainly caused by an autoimmune disorder. is.
E) H. pylori ( helicobacterium pylori ) associated gastritis. ( Helicobacter pylori Associated Gastritis),
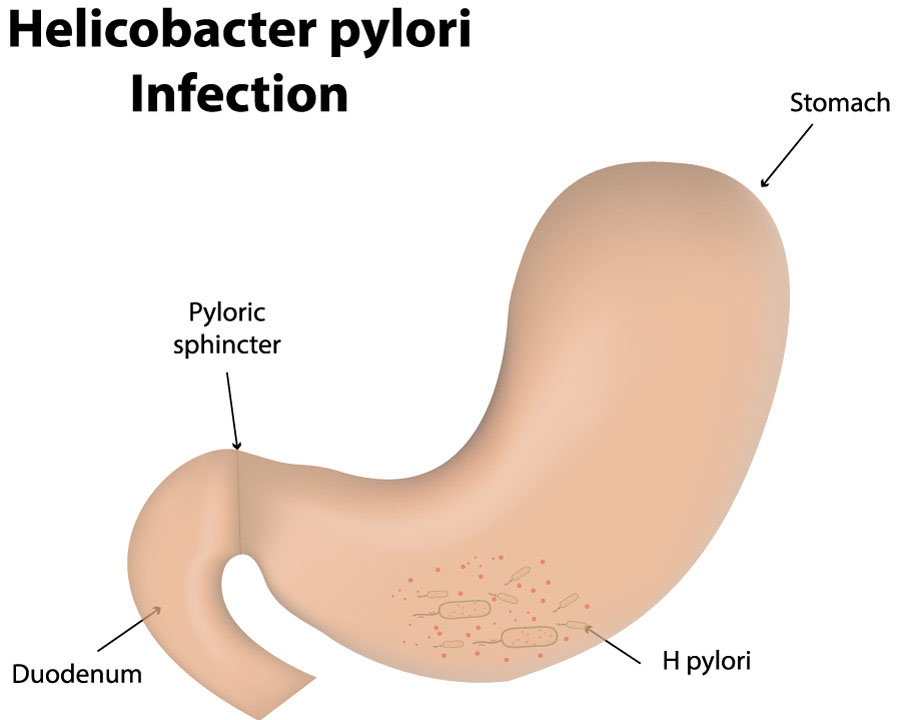
- This type of gastritis is caused by Helicobacter pylori ( ) is caused by a bacteria called Helicobacter pylori.
- Acute gastritis and chronic gastritis are both types of gastritis caused by a bacteria called Helicobacter pylori.
F) Autoimmune gastritis,
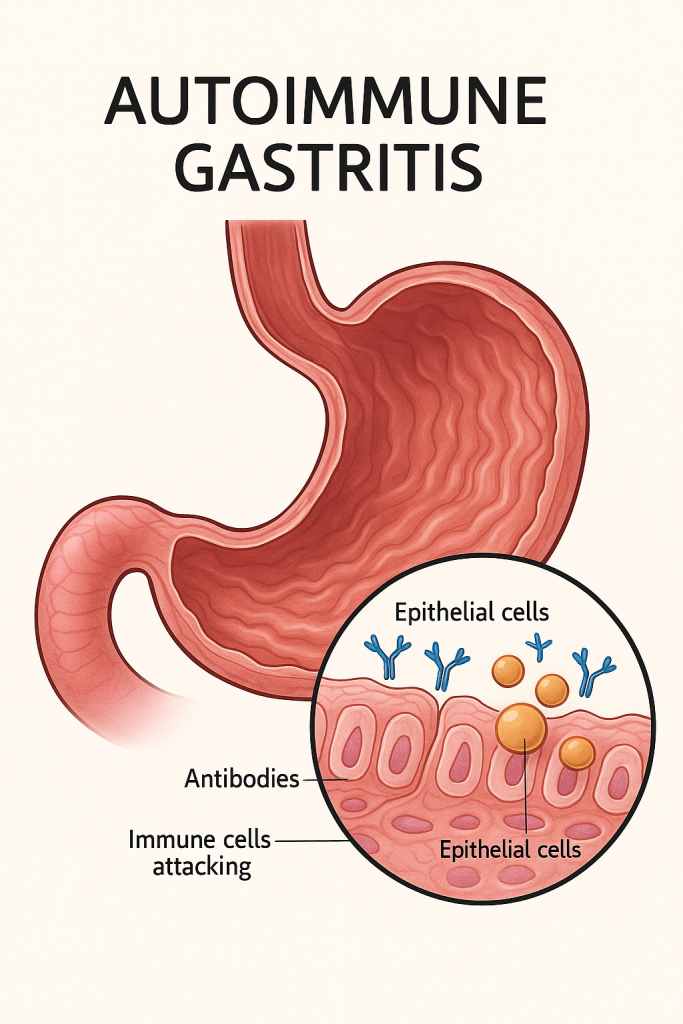
- Autoimmune gastritis is an autoimmune disease in which the body’s own immune system attacks the body’s normal/healthy cells, causing the condition of gastritis.
G) Chemical gastritis,
- Chemical gastritis is caused by prolonged use of any irritant substance.
- Chemical gastritis is caused by taking alcohol, corrosive chemicals, non-steroidal anti-inflammatory drugs (NSAIDs).
3) Explain the etiology/cause of the patient with the gastritis. Explain the causes of gastritis in patients.
- The condition of gastritis arises when the protective layer of the stomach is damaged.
- Due to benign and malignant ulcers in the stomach.
- Due to any medication, medical and surgical condition.
- Due to social habits,
- Due to chemicals,
- Due to infection,
- Pernicious anemia (Anemia is occurs Due to deficiency of vitamin B12) due to.
- Due to bacterial infection such as Helicobacterium pylori bacteria.
- Due to regular use of certain types of medicines.
- Ex: NSAID Drug,
Ibuprofen,
Naproxen, - Due to alcohol and smoking.
- Due to older age.
- Due to hot drinks and spicy food.
- Due to injury,
- Due to infection,
- Due to any major surgery,
- Due to excessive intake of cocaine.
- Due to bile reflux disease.
- Due to other disease conditions such as •>HIV, •{Crohn’s disease)
- •>Parasitic infection
- •{due to stomach cancer etc.
4)explain the Clinical manifestation/sign and symptoms of the patient with the gastritis. Explain the Clinical manifestation/sign and symptoms of the patient with gastritis.
- Abdominal discomfort.
- Burning sensation.
- Headache.
- Indigestion.
- Nausea,
- Vomiting,
- Feeling of fullness in the upper abdomen after eating.
- Not feeling hungry.
- Abdominal bloating.
- Heartburn.
- Sour taste in the mouth.
- hiccups,
- Vitamins Symptoms of B12 deficiency include: Passing black, tarry stools. Fever. Weakness. Stomach cramping. Pallor, sweating, and rapid heartbeat. Difficulty breathing. To be.
- Vomiting with large amounts of blood.
5)explain the diagnostic evaluation of the patient with the gastritis. Write a diagnostic evaluation of a patient with gastritis.
- history tacking and physical examination.
- Complete Blood Count Test (CBC Test).
- Helico Bacterium Pylori Test (H. Pylori Test).
- Liver and Kidney Function Test.
- Urine Analysis (urine analysis).
- Esophagogastro duodenoscopy.
- Fecal occult blood test.
- Double contrast barium study.
- X-ray of the upper digestive system.
- Gallbladder and pancreas test.
- Double contrast barium study.
- Endoscopy.
- Histological examination of tissues obtained by biopsy.
6) Explain the medical management of the patient with the gastritis. Write the medical management of a patient with gastritis.
1)provide Antibiotic medication to the patient.
- Antibiotic medication is mainly used to treat infection caused by bacteria called Helicobacter pylori.
- Ex:=
•> Amoxicillin,
•>Tetracycline,
•>Metronidazole,
•>Clarithromycin.
2)provide antacid medicine to the patient.
- Antacid medicine mainly neutralizes the acid content of the stomach, so antacid medicine should be provided to the patient.
- Ex:=
•>Aspirin,
•>Sodium bicarbonate and magnesia.
3)provide antiemetic medicine to the patient.
- Antiemetic medicine is used to treat the patient’s condition of nausea and vomiting.
- Ex: ondansetron.
4) provide proton pump inhibitor to the patient.
- Proton pump inhibitors mainly reduce the production of acid in the stomach cells that produce acid.
- Ex:
•>Omeprazole
( prilosec),
•>Lansoprazole
( prevacid),
•>Rabeprazole
( Acifex),
•>Esomeprazole
( Nexium),
•>Pantoprazole
( protonix).
5)provide histamine 2 ( H2 )blocker to the patient.
- Histamine blockers mainly help in reducing the amount of acid released in the digestive tract and it relieves gastric pain and helps in healing.
- Ex:=
•>Ranitidine ( Zantac),
•>Famotidine ( Pepcid),
•>Cimetidine ( Tagamet),
•>Nizatidine( Axid).
6) Provide cytoprotective agent to the patient.
- Cytoprotective agent medications mainly help in protecting the tissues of the stomach and small intestine.
- Ex:
•>sucralfate
( carafate),
•>Subsalicylate
( pepto Bismol).
7)explain the nursing management of patients with the gastritis. Write the nursing management of a patient with gastritis.
Assessment
- Complete assessment of the patient and his physical examination.
- Assess the patient’s signs and symptoms of the disease condition.
- Assess the patient’s vital signs To do.
- Auscultate the patient’s bowel sounds.
- Palpate the abdomen.
Nursing management
1)Impaired nutritional status less than body requirement related to acid regurgitation as evidence by intake output chart.
maintain nutritional status of the patient:
- Collect complete history of the patient.
- Monitor vital signs of the patient every hour.
- Advise the patient to take soft diet like porridge, khichdi etc.
- Serve food to the patient in an attractive manner.
- Advise the patient to take small, frequent and non-irritating meals.
- Encourage the patient to maintain daily body weight.
- Advise the patient to take a bland diet.
- Provide antacid medicine to the patient.
2)imbalance fluid level less than body requirement related to vomiting as evidence by assessing the skin turgor of the patient.
maintenance fluid volume of the patient:
- To monitor patient’s vital signs.
- of the patient Assess skin color and turgor.
- Advise the patient to drink clear liquids, juices, and coconut water.
- Advise the patient to maintain oral hygiene.
- Provide intravenous fluids to the patient.
- Provide antiemetic medication such as ondansetron to the patient.
3) Disturbed sleeping pattern related to abdominal pain as evidence by observing the restlessness condition of the patient.
Improve the sleep pattern of the patient:
- Assess the patient’s sleep pattern.
- Provide the patient with a calm and comfortable environment.
- Advise the patient to do daily routine activities in small amounts.
- Provide the patient with a quiet environment.
- Instruct the patient to read a book and pray at bedtime Advise for.
4)Acute pain related to disease condition as evidenced by verbalizing with the patient.
Relieve the pain level of the client:
- Assessing the patient’s pain level.
- Assess the duration and location of the patient’s pain.
- Advise the patient to do comfort measures such as deep breathing exercises.
- Advise the patient to rest and sleep in a quiet environment.
- Provide the patient with a semi-fowler position.
- Advise the patient to do some daily routine activities.
- Provide analgesic medicine to the patient.
5)Activity intolerance related to Anemia as evidenced by weakness.
improve the activities level of the patient
- Assess the patient’s daily routine activity.
- Advise the patient to exercise in small amounts.
- Advise the patient to take proper rest.
- The patient Advise on mind diversional therapy such as music, magazine reading.
- Advise the patient to take a balanced diet.
- Provide vitamin supplements to the patient.
1)define/explain peptic ulcer. Define Peptic/Duodenal Ulcer .
“Peptic ulcer” is a compound word of two words.
1)”peptic”
2)”Ulcer”
1)”peptic”
- “peptic” come from the Latin word “pepticus” (peptics),
- “pepticus” Which comes from the Greek word “peptikus”,
- “peptikus” which comes from the Greek word “peptein”
2) “ulcer” which comes from the Latin word “ulcus”.
- ” ulcus” meaning a sore or a wound , an ulcer.
- Peptic ulcer is an erosion or excavation ( hollow area ) that forms in the mucosal lining of the stomach and the first part of the small intestine (duodenum) and is called a peptic or duodenal ulcer.
- Peptic ulcer is a sore or open sore that develops in the mucosal lining of the stomach and the first part of the small intestine (duodenam) It occurs mainly due to excessive secretion of acidic contents in the stomach and is called peptic and duodenal ulcers.
- If the peptic ulcer is in the “stomach”, it is called “gastric ulcer”.
- If the peptic ulcer is in the “first part of the small intestine (duodenum)”, it is called “duodenal ulcer”.
- If the peptic ulcer is in the just upper part of the stomach, i.e. in the “esophagus”, it is called ” It is called “esophageal ulcer.”
2)explain the types of peptic ulcer. Write the type of peptic ulcer.

There are two types of peptic ulcer.
1)Acute peptic ulcer,
2)chronic peptic ulcer
1)Acute peptic ulcer,
- Acute peptic ulcer is a superficial ulcer in which there is erosion of the superficial mucosal layer.
- Some of the symptoms of acute peptic ulcer are: Healing occurs in time, but if it is not treated, bleeding and perforation can occur.
2) Chronic peptic ulcer
- Chronic peptic ulcers have deep, sharp edges and a clean base.
- Chronic peptic ulcers also involve the mucosa and submucosa.
- If the ulcer penetrates the stomach, it can also affect the nearby organ (pancreas).
3)explain the Etiology/cause of the patient with the peptic or duodenal ulcer. Explain the etiology/cause of the patient with peptic or duodenal ulcer.
- H.pylri (by Helicobacter pylori bacteria),
- Due to regular use of pain relieving medication.
- Ex:=
- •>Aspirin ,
- •>Ibuprofen,
- •>Non steroidal anti •>inflammatory drug.
- •>Ibuprofen,
- •>Naproxen etc.
- Due to excessive production of stomach acid.
- Due to hereditary factors.
- Due to smoking.
- Due to alcohol consumption.
- Due to excessive stress.
- Due to excessive use of irritating substances like tea, coffee, spices, tobacco, etc.
- Due to old age.
- Because of anxiety, worry.
4) Explain the clinical manifestation/sign and symptoms of the patient with the peptic ulcer. Describe the symptoms and signs of a patient with peptic ulcer.
- Inflammation in the stomach and the first part of the intestine (duodenum).
- Abdominal bloating.
- Abdominal burning.
- Pain in the upper middle part of the abdomen.
- nausea,
- vomiting,
- heart burn,
- abdominal fullness.
- belching (belching).
- weight loss.
- bloody, black, terry stools (hematochazia) to pass.
- bloody vomiting (hemetemesis).
- Gastero intestinal bleeding.
- Severe abdominal pain.
- feeling of abdominal fullness.
5) Explain the diagnostic evaluation of the patient with the peptic or Duodenal ulcer. Write a diagnostic evaluation of a patient with peptic and duodenal ulcers.
- blood test:
- To detect the presence of helicobacterium pylori bacteria in blood.
- stool test.
- Breathe test.
- upper gastro intestinal x rays.
- Barrium swallow.
- Endoscopy.
6) Explain the management of the patient with the peptic or duodenal ulcer. Write the management of a patient with peptic and duodenal ulcers.
medical management
The main goal of treatment is to eradicate the Helicobacter pylori bacteria.
Provide acid suppression medicine to the patient.
1) provide proton pump inhibitor medication to the patient.
- Proton pump inhibitors reduce the production of acid in the stomach and play an important role in the healing of stomach ulcers.
- Ex:=
•>omeprazole ,
•>Lansoprazole,
•>Pantoprazole .
2) Provide H2 receptor antagonist medicine to the patient Do.
- H2 receptor antagonist medicine reduces the production of acid in the stomach.
- Ex:=
- •> Ranitidine,
- •>Famotidine ,
3)Provide Antibiotic medication to the patient.
- If the peptic ulcer is mainly caused by a bacteria called Helicobacter pylori, then provide antibiotic medicine along with proton pump inhibitor medicine to treat it.
- Ex:=
•>Amoxicillin,
•>Clarithromycine .
4)Provide cytoprotective Agent to the patient.
- Cytoprotective agent protects the cells and tissues in the lining of the stomach and intestines.
- Ex:=
•>sucralfate
( Carafate)
•>Subsalicylate ( pepto bismol).
5)provide Antacid medicine to the patient .
- Antacid medicine mainly neutralizes the acid in the stomach and prevents heart burn.
- Ex:=
•>Aspirin,
•>Sodium bicarbonate,
•>Citric acid,
•>Alumina ,
•>Magnesia,
•>Calcium carbonate.
6) Provide education about the life style modifications to the patient.
Dietary changes:
- Spicy food, caffeine and acidic to the patient Advise the patient to avoid food.
smoking cessation:
- Advise the patient to avoid smoking.
Avoid alcohol consumption:
- Advise the patient to avoid alcohol consumption.
stress management:
- Advise the patient to avoid stress levels.
Regular follow up:
- Advise the patient to have regular follow up.
surgical management
1)vagotomy
- Vagotomy involves cutting the vagus nerve, which is responsible for the secretion of stomach acid.
- The aim of this surgery is to reduce the production of stomach acid and improve the healing of ulcers.
2)Antrectomy
- An antrectomy procedure removes the lower part of the stomach (antrum), which is responsible for producing hormones that increase the production of stomach acid.
3) pyloroplasty
- Pyloroplasty involves widening the lower part of the stomach (pylorus) and the beginning of the small intestine (duodenum), which allows the food content in the stomach to pass properly into the intestine and reduces the risk of ulcers.
4)Gastrectomy
- In a gastrectomy procedure, the stomach is partially (partial gastrectomy) and completely
- ( completely gastrectomy) is removed and the esophagus is directly attached to the small intestine.
4) Billroth 1 (gastroduodenostomy)
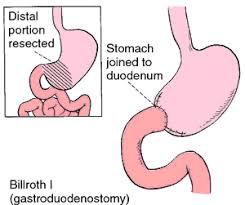
- In this procedure, a new opening is formed between the stomach and the small intestine.
- The lower part of the stomach is removed and the remaining portion of the stomach is anastomosis with the duodenum of the small intestine.
5) Bill Roth 2 ( Billroth to) :
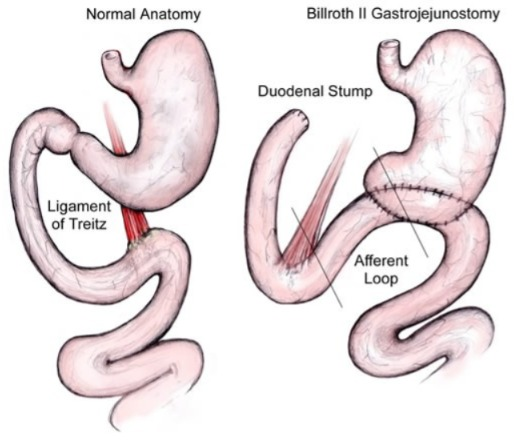
- In this procedure, part of the stomach is anastomosised with the jejunum (middle portion of the small intestine).
7)Nursing management :
1)pain related to gastric mucosa irritation.
Relieve pain of the patient:
- Assess the patient’s pain level.
- Provide the patient with mind diversional therapy.
- Provide the patient with prescribed analgesic medicine.
- Advise the patient to avoid beverages and caffeinated foods.
- Advise the patient on relaxation techniques.
2)Altered nutritional status less than body requirement related to the therapeutic regiments.
maintain nutritional status of the patient.
- Assess the nutritional status of the patient.
- Advise the patient to take liquid and semi-solid food.
- Advise the patient to avoid hot, spicy, and caffeine foods.
- Provide the patient with a bland diet.
- Provide antacid medicine if the patient is experiencing heartburn.
- Provide antiemetic medicine if the patient is vomiting. To do.
3)Anxiety related to the disease condition
Relieve the anxiety level of the client
- Assess the patient’s anxiety level.
- Provide the patient with complete information about his disease condition, its causes and its treatment To do.
- Clear all the doubts of the patient.
- Provide a comfortable environment to the patient and his family members.
- Communicate with the patient properly in simple language.
- Provide psychological support to the patient.
4)Risk for gastro intestinal bleeding related to the surgery.
monitoring the patient for the GI track bleeding.
- Monitor the patient’s vital signs.
- Monitor the patient’s hemoglobin level.
- Assess the patient for any conditions such as dizziness and nausea.
- Monitor the patient’s stool test.
- Monitor the patient’s urine output.
- If the patient is bleeding, take immediate measures to stop it.
- Continue to monitor the patient.
1) Define/explain cancer of stomach.
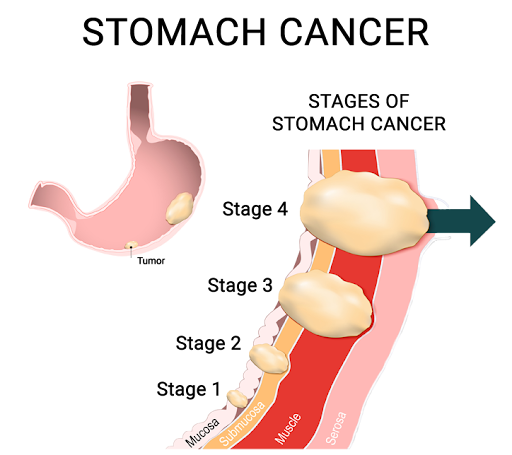
Introduction:
- Stomach cancer is also called gastric cancer.
- It develops in any part of the stomach and in stomach cancer, there is abnormal and uncontrolled growth of stomach cells and formation of tumor and mass-like structures.
- This tumor can be both benign (non-cancerous) and malignant (cancerous).
- About 85% of stomach cancers are adenocarcinomas and develop mainly in the lining (mucosa) of the stomach.
- 40%: = of stomach cancers occur in the lower part of the stomach (pylorus).
- 40%: = of stomach cancers occur in the middle part (body) of the stomach.
- 15%: = of cases occur in the upper part (cardia). And this stomach cancer metastasizes, i.e. transfers and spreads to other parts of the body such as the liver, lungs, bone, and brain.
- It mainly spreads to the periosteum, i.e. the abdominal cavity.
2)explain Etiology/Cause of the patient with stomach cancer.
- Age: It occurs after the age of 40.
- Gender: It is more common in men than in women.
- Region: It is more common in Japanese people.
- Diet: It can also be caused by not eating enough fruits and vegetables.
- Smoking,
- Alcohol,
- Hereditary factors,
- chronic infection in the stomach (due to long-term infection in the stomach),
- Stomach surgery,
- H.pylorus infection( Helicobacterium pylori ),
- High consumption of red meat , (due to eating too much meat),
- Pernicious Anemia (due to vitamin B 12 deficiency),
- Gastric ulcer,
- Hereditary,
- Obecity,
- Hormonal factors,
- Etc.
3)explain clinical manifestation/sign and symptoms of the patient with the stomach cancer stomach cancer Explain the clinical manifestation/sign and symptoms of the patient with stomach cancer.
- Pain in the stomach area.
- Difficulty swallowing.
- Nausea and vomiting occur.
- Weight loss.
- The stomach feels very bloated even after eating a little.
- Blood in vomiting hemetemesis).
- Blood in the stool (hematochezia),
- Gastrointestinal bleeding,
- Conditions such as indigestion (Indiagetion) and gas (heart burn) occur.
- Anorexia (loss of appetite:= loss of appetite),
- Diarrhea (loss watery stool),
- Constipation (difficulty in passing stool),
- fatigue (feels tired)😩.
- Iron deficiency Anemia.
4) Explain the diagnosis evaluation of the patient with stomach cancer. Write the diagnostic evaluation of a patient with stomach cancer.
- History taking and physical examination,
- Biopsy,
- Endoscopy,
- usg ,
- X Ray ,
- ct scan,
- MRI,
5) Explain the management of the patient with stomach cancer. Write the management of a patient with stomach cancer.
- chemotherapy,
- Radiation therapy,
- gastrectomy,
- -> Total gastrectomy,
- ->sub total gastrectomy
- esophageal gastrectomy
- Billiroth :- I (gasteroduodenostomy),
- Billroth:=II
( gastrojejunostomy),
Nursing management :
Emergency management:
- Check the patient’s vital signs every 15 minutes.
- Check the patient’s blood pressure every 15 minutes To do.
- Set up two intravenous lines for the patient and prepare a blood transfusion.
- Give oxygen to the patient.
- Check the patient’s bowel sounds.
- Check whether the patient is vomiting and has diarrhea.
- Catheterize the patient to check urine intake and output.
- Check the patient’s skin color.
- Maintain the patient’s intake output chart.
- Put the patient in the fowler position to prevent aspiration of mucus.
- Insert a naso-gastric tube (N.g tube) into the patient.
- Start feeding the patient with a clear liquid diet.
Preoperative nursing management:
- Provide psychological support to the patient.
- Explain the procedure to the patient and his family member.
- Set up an intravenous line for the patient.
- Catheterize the patient.
- Maintain the patient’s intake output chart.
- Set up blood transfusion for the patient.
- Get the patient’s laboratory investigation done.
- Administer oxygen to the patient.
- On the part of the patient that is the operation part Proper shaving.
- Clean or paint the patient’s operation site with Savlon and spirit.
- Prepare the patient mentally and physically for surgery.
- Check the patient’s vital signs.
- Provide psychological support to the patient and his family members.
post operative nursing management:
- Close observation of the patient after the operation.
- Check the patient’s vital signs every 15 minutes.
- Provide the patient with intravenous fluid through the parenteral route.
- Check the patient’s bowel sound To do.
- Give the patient proper antibiotic medications.
- Provide psychological support to the patient.
- Advise the patient’s family members to ensure that the patient does not do too much hard work.
- Tell the patient to rest.
- Provide the patient with work and a comfortable environment.
- Balance the patient’s nutritional and food status.
- Instruct the patient to do small amounts of activity.
1)explain/Define Gastroenteritis. Define gastroenteritis.
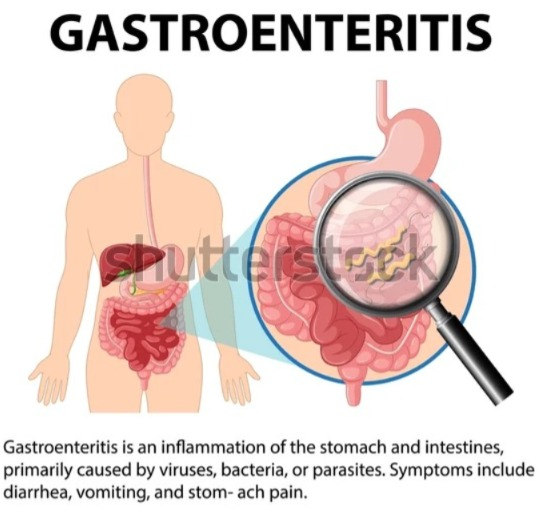
Gastroenteritis
- Gastro meaning:= stomach.
- enter meaning:= intestine.
- itis meaning := inflammation
- In gastroenteritis, there is inflammation of the gastrointestinal tract.
- Which also involves the stomach and small intestine, causing a condition of acute diarrhea.
- Gastroenteritis is a condition that causes infection, irritation and inflammation in the stomach and intestines.
2)explain the Etiology/cause of the patient with the Gastroenteritis Explain the etiology/cause of the patient with the Gastroenteritis.
1) Due to viral infection.
- •>Rotavirus ( ),
- •>Norovirus ( Norovirus) ,
- •>Adenovirus ( adenovirus),
- •>parvovirus ( parvovirus),
- •>Astrovirous ( astrovirus).
2) Due to bacterial infection.
- •>Escherichia coli,
- •>salmonella,
- •>shigella,
- •>campylobacter,
- •>vibrio,
- •>clostridium difficile ( Clostridium difficile ),
3) Due to parasites.
- •> Giardia lamblia,
- •>cryptosporidium,
- •>entamiba histolytica,
4) Due to toxins and chemicals.
- •> Due to ingestion of contaminated food and water.
- •>Due to ingestion of contaminated chemicals.
5)Non-infectious cause
- •> Due to certain types of medication,
- •> Due to food allergy,
- •>reaction to certain substance,
6)poor hygiene factors.
- •> Due to not washing hands properly.
- •> Due to poor hygienic conditions.
3)explain the Clinical manifestation/sign and symptoms of the patient with the Gastroenteritis. Explain the Clinical manifestation/sign and symptoms of the patient with the Gastroenteritis.
- nausea,
- vomiting,
- abdominal discomfort,
- abdominal cramps.
- Diarrhea.
- loss of appetite.
- swollen abdomen .
- Abdominal pain.
- Fever.
- Abdominal bloating (filling about abdomen is full and tight due to the gas ) occurs.
- Diarrhea.
- Blood in vomit (hematemesis).
- Blood in the stool. (hematochezia).
- Dehydration.
- Muscle pain.
- Fatigue.
4)explain the Diagnosis evaluation of the patient with the Gastroenteritis.
- History taking and physical examination.
- Complete blood count.
- Stool Examination.
- Imaging studying.
- Clostridium difficile Testing.
- Electrolyte Testing.
- kidney function test.
5) Explain the management of the patient with the Gastroenteritis. Write the management of a patient with gastroenteritis.
- Maintain the hydration status of the patient.
- Provide intravenous fluid to the patient.
- Provide antibiotic medicine to the patient.
- Provide antidiarrheal medicine to the patient.
- Provide antiemetic medicine to the patient.
- Ex:
- •>promethazine
- ( Phenergan) ,
- •>Prochlorperazine
- ( Compazine),
- •>Ondansetron
- (Zofran),
6) Explain the nursing management of patients with the Gastroenteritis. Write the nursing management of a patient with gastroenteritis.
1)Fluid replacement:
- Advise the patient to take proper fluid intake.
- Advise the patient to take oral rehydration solution if there is electrolyte imbalance.
- The patient’s Maintain hydration status properly.
- Monitor the patient’s vital signs.
2) Maintain nutritional status of the patient.
- The patient can digest easily Advise the patient to take such food.
-
- Ex:
-
- banana,
-
- Rise,
-
- Toast, etc.
- The patient Advise to avoid fatty and spicy food.
- Maintain the patient’s intake output chart.
3)isolation precaution( if Gastroenteritis is infectious) :
- If gastroenteritis is infectious, keep the patient isolated.
- The patient Advise on proper hand hygiene.
4)medication administrations :
- Advise the patient to take the prescribed medicine properly.
- Provide antiemetic medicine to treat the patient’s vomiting.
- Provide antidiarrheal medicine if the patient has a condition of diarrhea.
5)comfort measures:
- Provide comfort measures if the patient is in pain.
- Provide mind diversional therapy to the patient.
6)educational and discharge planning.
- Advise the patient on proper hand washing technique.
- Advise the patient on proper food technique.
- Advise the patient on proper hand washing technique.
- Advise the patient on proper emotional support.
- Provide the patient with a clean and comfortable environment.
1)Define/explain tracheoesophageal fistula. Define esophageal fistula.
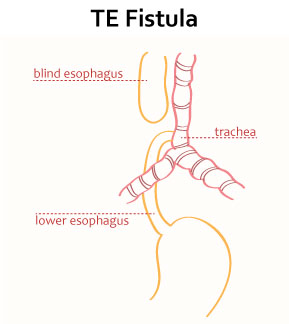
- Fistula is an abnormal connection between any two organs. Tracheoesophageal fistula is an abnormal connection between the trachea (wind pipe) and the esophagus (the tube that carries food from the mouth to the stomach). This is called a tracheoesophageal fistula.
- Tracheoesophageal fistula is mainly a congenital abnormality but if it occurs in late life, it is due to any surgical procedure.
2)explain the Etiology/cause of the patient with the tracheoesophageal fistula. Explain the causes of patients with tracheoesophageal fistula.
- Due to congenital defect.
- Due to traumatic and blunt injury.
- Due to environmental factors.
- Due to tumor.
- due to pressure necrosis by a tracheostomy tube.
- gastric acid regurgitation through Distal fistula.
3)explain the Clinical manifestation of the patient with the tracheoesophageal fistula. Explain the symptoms and signs of the patient with the tracheoesophageal fistula.
- Excessive secretion seen after birth.
- in neonate:
- •>Chocking,
- •>Coughing,
- •>Vomiting,
- •>Cyanosis during •>feeding,
- White frothy bubbles of mucous are present in the mouth and nose of the neonate.
- Cyanosis,
- Abdominal distension occurs.
- coughing.
- poor feeding.
- respiratory distress.
- inability to pass nasogastric tube.
3)explain the diagnostic evaluation of the patient with the esophageal fistula. Write an evaluation .
- History taking and physical examination.
- Ultra Sound,
- chest x rays,
- nasogastric tube insertion,
- Barium Mill,
- Electrocardiogram,
- Echocardiogram,
5) Explain the management of the patient with the tracheoesophageal fistula. Write the management of a patient with truckioesophageal fistula.
management
- Immediate management:
1) Keep the infant at a 30 degree angle to prevent reflux of gastric contents.
2) Place a naso-gastric tube in the esophagus and suction any secretions in the esophagus to prevent aspiration.
3) Wash out the pouch with normal saline to prevent the tube from becoming blocked by mucus.
4) Provide supportive therapy to the patient.
5) Ensure the patient’s nutritional requirements are met.
6) Provide Indra Venors fluid to the patient.
7) Provide antibiotic medicine to the patient.
8) Provide respiratory support to the patient.
9) Advise the patient to maintain a neutral environment.
10) Correct the fistula through surgical intervention in the patient.
Nursing management
- Advise the patient to take more fluid.
- Provide intravenous fluid to the patient.
- Provide respiratory support to the patient.
- Provide oxygen to the patient properly.
- Continuously monitor the patient’s vital signs.
- Provide ventilatory support to the patient.
- Do not give anything by mouth to the patient.
- Keep the agent in a semi-fowler position.
- Provide emotional support to the patient and his family members.
- If the patient develops any complications If it happens, report it immediately.
- Provide all information about the disease to the patient’s family members.
1)explain/define peritonitis. Define peritonitis.
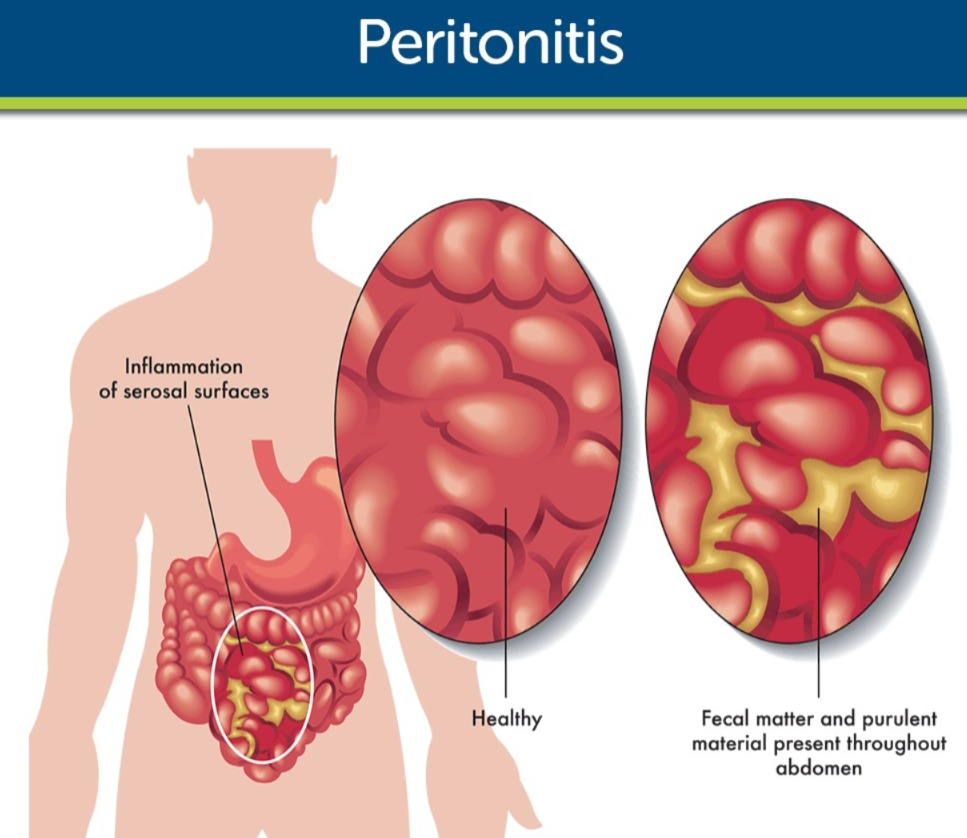
- peritoneum ( Peritoneum: A serous membrane that lines the viscera of the abdominal cavity. Covers and provides support to the abdominal organs)
- Localized and generalized infection and inflammation of the peritoneum is called peritonitis.
- { peritonitis : infection and inflammation of the peritoneum layer of the abdomen its called peritonitis. }
- Peritonitis is mainly caused by any bacterial and fungal infection. Due to this, the most common symptom is severe abdominal pain.
2)explain the Etiology/cause of peritonitis. Give the causes of peritonitis.
- The most common cause of peritonitis is any bacterial or viral infection.
1)Infection (due to infection):
- bacterial infection,
- fungal infection .
2)perforated organ
- In this, when any organ of the abdominal cavity is perforated, infection can also occur.
3) intra abdominal inflammatory condition:
- Diverticulitis,
- Pancreatitis,
- Inflammatory Bowel Disease .
4)Trauma ( Trauma to occur (due to)
- Due to abdominal trauma.
5) Post operative complication
- As a complication of surgery in any abdominal cavity.
6) Ascites (due to ascites)
- Due to accumulation of fluid in the abdominal cavity.
7)other organ inflammation
- Peritonitis occurs due to inflammation in other organs of the body spreading into the abdominal cavity.
8) Intra abdominal Abscess( pus) Due to.
9) Due to peritoneal dialysis.
10) Rupture appendix.
11) Due to peptic ulcer.
12) Due to liver cirrhosis.
13) Due to any pelvic inflammatory disease.
14) Due to inflammation in the fallopian tube.
3)explain the type of peritonitis. Name the types of peritonitis:

There are two types of peritonitis.
1)primary peritonitis (primary peritonitis),
2)secondary peritonitis (secondary peritonitis)
1)primary peritonitis (primary peritonitis),
- When infection and inflammation occurs in the peritoneum due to any blood and lymph infection, it is called primary peritonitis.
- This type of peritonitis is seen only in rare conditions.
2)Secondary peritonitis
- When the peritoneum layer is infected and inflamed by bacteria and enzymes present in the biliary and gastrointestinal tracts, it is called secondary peritonitis.
- This type of peritonitis is the most common.
4)explain the Clinical manifestation/sign and symptoms of the patient with the peritonitis.
- Abdominal pain.
- Abdominal tenderness.
- Abdominal bloating (filling of fullness or tightness in abdomen due to gas accumulate in abdominal cavity).
- fever and chills.
- nausea.
- vomiting.
- loss of appetite.
- Increases in temperature and pulse rate to occur.
- Electrolyte imbalance.
- Leukocytes count increase.
- Breathing difficulty.
- Skin turn pale and cold.
- Heart rate increase.
- Shock.
4) Explain the diagnostic evaluation of the patient with the peritonitis. Write a diagnostic evaluation of a patient with peritonitis.
- history tacking and physical examination.
- Blood test.
- Complete blood count test.
- Blood culture.
- Electrolyte and kidney function test.
- Abdominal ultrasound.
- abdominal x ray.
- abdominal ct scan.
- Laparoscopy.
- peritoneal fluid culture.
- exploratory surgery.
- rectal and pelvic Examination.
5)explain the management of the patient with peritonitis. Write the management of the patient with peritonitis.
medical management
- Identify the cause of peritonitis and treat it immediately.
- Maintain the patient’s fluid and electrolyte balance.
- Provide the patient with isotonic solution to prevent hypovolemia.
- Provide analgesic medicine if the patient is in pain.
- If the patient complains of nausea and vomiting, provide antiemetic medicine.
- If there is a complaint of abdominal distention, perform intestinal intubation and suction, which relieves abdominal distention and promotes intestinal function.
- Provide the patient with adequate amounts of oxygen.
- Provide the patient with broad-spectrum antibiotic medicine.
- Ex:=
- •>Cefoxitin with the aminoglycoside.
- •>Penicillin G.
- •>Clindamycin with aminoglycoside.
- J in Surgery Remove infected tissue.
- Provide the patient with intravenous fluids to normalize electrolyte disturbances if any.
explain the nursing management of patients with the peritonitis. Write the nursing management of a patient with peritonitis.
- Advise the patient to maintain oral hygiene to prevent infection.
- Advise the patient to get proper immunization of mumps, measles and rubella (MMR) during childhood.
- Advise the patient to wash hands properly before and after defecation.
- Advise the patient to avoid irritant foods like caffeine, spicy foods, and hot foods.
- Advise the patient to consume plenty of fluids to reduce dryness of the mouth.
- Advise the patient to stop smoking, alcohol, and cigarettes.
- Advise the patient to use lukewarm saline solution to moisten the mouth.
- Advise the patient to use sugar-free lemon drops. Advise to use helps to increase saliva production and reduce swelling.
- Advise the patient to consume a semi-solid diet.
- Advise to apply heat to the patient’s cheeks to reduce swelling.
- Advise the patient to eat a fiber-rich diet.
- Provide psychological support to the patient.
- Properly inform the patient about the disease, its cause, its treatment.
- Clear all the doubts of the patient and his family members.
- Advise the patient to take medicine regularly.
- Advise the patient to take proper follow up.
1)Explain/define helminthiasis. Define helminthiasis.
- Helminthiasis is also called worm infection.
- When the body is infected by parasitic worms, it is called helminthiasis.
- Helminthiasis is classified as:
- •> Tapeworm
( cestodes), - •> Round worm
( nematodes), - •> Flukes
( trematodes). - These worms mainly live in the gastro intestinal tract but can also spread to other organs of the body and cause physiological changes and damage.
- Helminthiasis mainly affects the intestines, liver, lungs, and blood stream. etc.
- STH ( Soil Transmitted helminthiasis ) and schistosomiasis ( Schistosomiasis) are the most important group of helminthiasis.
2) Explain the types of worm infestation. Name the types of worm infestation.
There are four types of worm infestation.
1)Ascariasis (Round worm infection)

- Roundworm mainly contaminates food and due to this food affects the intestines and lungs.
- Roundworm infections such as lymphatic filariasis are included.
2)Tape worm infection
- Tape worm infection a Mainly caused by eating uncooked food.
- Tape worm infection includes cysticercosis.
3)Enterobiasis (pinworm infection) (pin worm infection)
- Pinworm mainly infects the cecum and its eggs are mainly present on the perianal skin.
4)Hook worm infection ( Hook worm) infection)
Hookworm larvae mainly affect
- •>skin ,
- •>lungs ,
- and
- •>small intestine , •>esophagus.
3)explain the Etiology/cause of helminthiasis. Explain the cause of helminthiasis.
- => Helminthiasis is mainly caused by parasitic worms.
1)contaminated food or water
- => Due to ingestion of food that is infected/contaminated by helminths.
- => Due to poor sanitation.
2)Soil contamination ( Soil contamination.)
- => Due to contact with soil contaminated with helminths and ingestion of contaminated vegetables.
3) Fecal-oral transmission
- => Helminths are spread mainly through the fecal-oral route due to unhygienic conditions.
4) Consumption of undercooked or raw food (due to intake of undercooked and raw food)
- => Some types of helminths such as tapeworms are mainly spread through the ingestion of undercooked or raw food.
5) Contact with the infected animals (due to contact with infected animals)
- => Some types of helminths are spread mainly by direct contact with an infected animal.
6)Vector born transmission
- => Some types of helminths are transmitted mainly by vectors.
4)explain the Clinical manifestation/sign and symptoms of the patient with the helminthiasis. Describe the symptoms and signs of a patient with helminthiasis.
- Low grade fever,
- Blood in sputum,
- Wheezing sound heard.
- Dyspnea (shortness of breath).
- Chest pain.
- Epigastric pain.
- vomiting.
- Abdominal distension.
- perineal itching during night.
- irritability.
- restlessness.
- Insomnia Coming.
- Blood in the stool (hematochezia).
- Anemia.
- Weight loss.
- Fatigue.
5)explain the diagnostic evaluation of the patient with the helminthiasis. Write the diagnostic evaluation of a patient with helminthiasis.
- history tacking and physical examination.
- Microscopical stool examination.
- Complete blood count test.
- Serological testing.
6)explain the medical management of the patient with the helminthiasis. Write the medical management of a patient with helminthiasis.
1) Deforming treatment ( Deforming treatment.)
=> In this treatment, a single dose of tab mebendazole (vermox) is provided to the patient for three days.
=> This dose is repeated every two weeks.
=>provide tab. Albendazole to the patient.
=>provide Oxamniquine to the patient.
=> If the patient has an anemic condition, then tab. Ferrous sulphate 200 mg should be given three times a day.
surgical management
In surgery, the affected part of the intestine is removed.
mass dewarming of children
=> Children in areas with high worm infestation are provided with deworming medication (Albendazole) twice a year.
=> Children are provided with education on proper hand washing.
=> Children are advised to brush properly.
write the Nursing management of the patient with the helminthiasis Write the Nursing management of the patient with helminthiasis.
provide education about the hygiene .
Provide education about proper hand hygiene for the patient.
Provide education to the patient on safe drinking water and safe food preparation.
Advise the patient to maintain cleanliness while preparing food.
Advise the patient to maintain proper environmental sanitation while serving food.
Advise the patient to maintain proper environmental sanitation Provide.
Advise the patient to maintain personal hygiene.
provide education about the proper diet:
- Advise to take a balanced diet to prevent nutritional deficiency.
- Advise to take high protein diet, low carbohydrate and fibrous food.
- Advise the patient to take food in small and frequent amounts.
- Advise to take green leafy vegetables to prevent anemia.
- Advise the patient to drink plenty of fluids.
provide proper medication:
- Properly administer anthelmintic medicine such as albendazole to the patient.
- Advise the patient to have regular check-ups.
- Advise the patient to report any complications immediately.
- Advise the patient to have regular follow-up.
- Advise the patient to take proper medication.
1)Define/explain constipation. Define constipation.
- Constipation is a condition in which •>bowel movements are infrequent or
•>bowel emptying Difficulty in passing stool or •> Difficulty in passing stool, or •> Incomplete bowel evacuation/emptying. - The condition of constipation is mainly caused by •> hardening of the feaceas,
•> inadequate intake of fiber food, and
•> low water intake.
2)explain the Etiology/cause of the constipation. Explain the causes of constipation.
1)Dietary factors
=> Due to low intake of fiber-rich diet.
=> Due to low fluid intake.
=>Due to high intake of processed food.
2)Lack of physical activity (due to low physical activity)
=> Due to sedentary lifestyle and low physical activity.
3) Dehydration
=> Constipation can occur due to reduced fluid intake, which can cause hard stools and difficulty in passing stools.
4) Certain medication (due to certain types of medication)
Ex:=
•>Antihypertensive ,
•>Antidepressant,
•>Antacid,
•>Opioids ( narcotics),
•>Diuretics,
•>Antihistamine,
•>Antispasmodic,
•>Anticonvulsant,
•>Calcium channel blocker,
•>Pain releiver,
All these medications can also cause constipation.
5)Neurological conditions (Neurological conditions)
=> Multiple sclerosis, Parkinson’s disease can also cause constipation.
6) Hormonal changes (due to hormonal changes)
=> Due to hormonal fluctuation due to pregnancy and age.
7)Metabolic or muscular (metabolic and muscular)
•>Hypercalcemia, •>Hypothyroidism, •>Diabetes mellitus, •>Cystic fibrosis,
•> Myotonic dystrophy,
•>Celiac disease,
Constipation can also occur due to other conditions.
8)Structural or functional disorder (due to structural and functional disorder)
=>
•>Colon cancer,
•>Anal fissure,
•>Spinal cord lesion, •>Pregnancy,
•> Descending perineum syndrome,
•>Stroke.
9)Psychological factor (due to psychological factor)
=> Due to stress, anxiety, fear.
10) Due to lead poisoning.
11) Due to connective tissue disorder.
12) Due to appendicitis.
13) Ignorance to the urge of defecation.
14) Due to obstruction.
3) Explain the clinical manifestation/sign and symptoms of the patient with the constipation. Describe the symptoms and signs of a patient with constipation.
- Abdominal discomfort.
- Abdominal distension.
- Abdominal pain.
- Anorexia (loss of appetite).
- straining to pass stool stool.
- Headache.
- Nausea.
- Feeling of fullness.
- Restlessness.
- Indigestion.
- Anismus:= uncoordinated contraction of the anal sphincter during straining to occur.
- fecal impaction:
- feeling a hard mass in the rectum.
- infrequent bowel movements.
- difficulty in passing stool.
- Passing hard and dry stools.
4)Explain the diagnostic evaluation of the patient with the constipation. Write the diagnostic evolution of a patient with constipation.
- history taking and physical examination.
- Barium enema.
- Colonoscopy.
- Sigmoidoscopy.
- Abdominal X-ray.
- Anorectal Manometry.
- Rectal Examination.
5) Explain the complications of the patient with the constipation. Explain the complications of constipation.
- Haemorrhoids.
- Perforation.
- Hypotension.
- Fecal impaction.
- Anal fissure.
- Abdominal pain.
- Diverticulosis.
- Megacolon.
- Bowel perforation.
6) Explain the treatment of the patient with the constipation. Explain the treatment of a patient with constipation.
medical management
- Advise the patient to consume a high-fiber diet.
- Advise the patient to consume fruits and vegetables.
- Advise the patient to drink six to eight glasses of water daily Give.
- If the stool has become impacted, provide the patient with an enema.
- Like:=
- soap water enema,
- Tap water enema,
- Phosphate enema.
- Provide medication therapy to improve the motor function of the intestine.
- Ex:= prokinetic agent( cisatride or metoclopramide).
- provide bulk forming drug to the patient ex:=methyl cellulose psyllium.
- provide stool softner to the patient ex:= Docusate.
- Provide lubricant to the patient.
- Ex:= mineral oil.
- Provide stimulant to the patient.
- Ex:= phenol phthalein.
- Provide saline and osmotic solutions to the patient. To do.
- Ex:=
milk of Magnesia ,
Sodium Phosphate lactulose. - serotonin type a Receptor partial agonist (tegaserod) provide to the patient.
- Advise the patient to take an adequate balanced diet to prevent nutritional deficiency.
- Advise the patient to avoid cigarettes, smoking, and alcohol.
- Advise the patient to avoid irritating foods such as tea, coffee, spicy foods, hot foods.
- Advise the patient to drink adequate amounts of water.
- Advise the patient to eat high-fiber foods.
- Advise the patient to eat fruits and vegetables such as apples, papaya, oranges, etc.
- Ask the patient to avoid sleeping immediately after eating.
Explain the nursing management of patients with constipation. Write the nursing management of a patient with constipation.
1)Advice about taking adequate nutritional diet :
Advice to the patient about the good hygiene :
- Advise the patient to adopt good hand hygiene habits to prevent infection.
- Advise the patient to wash hands properly before and after meals to prevent infection.
- Advise to minimize the use of irritant products and dairy products Give.
- Advise the patient to maintain personal and environmental hygiene.
- Advise the patient to maintain oral hygiene.
educate the patient about the do physical activity and exercise.
- Advise the patient Give that physical activity and exercise increase peristalsis movement so exercise properly.
- Advise the patient to do walking, yoga and meditation which relieves constipation.
Advice about taking adequate medicine.
- Provide laxatives and enemas to the patient properly To do.
- Administer suppositories to the patient to relieve constipation.
- Advise the patient to follow up regularly.
- Advise the patient to take medication properly.
- => Diarrhea is not a disease but a symptom.
- => Diarrhea is a symptom of a disease of the digestive system.
- => In diarrhea, the frequency of stool, its fluid content, and volume increases.
- => Diarrhea is a condition in which liquid and loose stools are passed more than three times a day. It is called diarrhea.
- => Diarrhea is mainly caused by any bacterial, viral, and parasitic infection.
1)Define/explain Diarrhea. Define diarrhea.
2)explain the types of diarrhea. Explain the types of diarrhea.
=> There are a total of seven types of diarrhea.
1)Acute Diarrhea,
=> The onset of acute diarrhea is sudden and of short duration.
=> Acute diarrhea is mainly seen for a few hours or days.
=> Acute diarrhea is mainly caused by •>viral, •>bacterial, and •>parasite infections and food poisoning.
2)Chronic Diarrhea,
=> Chronic or long-lasting diarrhea.
=>If diarrhea persists for more than two weeks, it is called chronic diarrhea.
=> Chronic diarrhea is mainly caused by
•>Irritable bowel syndrome,
•>Inflammatory bowel disease,
•>Malabsorption disorder.
3)Persistent Diarrhea,
=> If the condition of continuous diarrhea lasts for more than a few weeks, it is called persistent diarrhea.
=> Persistent diarrhea is mainly caused by
•>infection
•>inflammatory bowel disease
•>certain medication
.
4)Traveler’s Diarrhea,
=> Traveler’s diarrhea is a condition that occurs mainly when an individual comes into contact with contaminated food and water while traveling.
=> It is mainly caused by bacterial, parasitic infections.
5) Inflammatory Diarrhea,
=> Inflammatory diarrhea is a condition mainly seen in the gastrointestinal tract due to infection and inflammation.
=> This is mainly seen in the conditions of •>Crohn’s disease •>Ulcerative colitis.
6) Osmotic diarrhea,
=> Osmotic diarrhea is mainly caused by poor absorption of water by the intestine.
=> This causes water to enter the bowel. and loose watery stool (loss watery stool) is passed.
=>This condition is mainly seen due to lactose intolerance and malabsorption.
7) Secretory Diarrhea
=> Secretory diarrhea is mainly caused by the secretion of more amount of fluid in the intestine or due to any infection or some type of medication.
3)explain the Etiology/cause of the patient with the Diarrhea. Explain the cause of diarrhea.
1)Infection (due to infection)
=> viral ( virus)
Ex:=Rotavirus.
=>Bacteria ( bacteria)
Ex:=
•>E.coli,
•>Shigellas,
•>Salmonella,
•>Campylobacter species,
•>Clostridium difficile
=>parasitic infection ( parasitic infection)
•>Giardia lamblia,
•>cryptosporidium,
2)Food born illness
=> Due to ingestion of contaminated food and water.
=> Due to lack of cleanliness while preparing food.
3) Certain medication (some types of medication)
=> Some types of antibiotics, antacids and cancer drugs also cause diarrhea.
4)Diatory factors
=> Diarrhea can also be caused by consuming excessive amounts of certain foods and beverages.
Ex:=
•>high fatty food,
•>Spicy food,
•>Caffeinated drinks can also cause diarrhea.
5) Inflammatory bowel disease
=>Crohn’s disease and ulcerative colitis are Infection and inflammation in the digestive tract cause the condition of diarrhea.
6) Irritable bowel syndrome (irritable bowel syndrome)
=>Irritable bowel syndrome also causes the condition of chronic diarrhea.
7) Malabsorption disorder (malabsorption disorder),
celiac disease (Celiac disease)
•>Lactose intolerance (Lactose intolerance)
Due to this, the absorption of nutrition is impaired and the condition of diarrhea arises.
8) Gastro intestinal disorder (Gastrointestinal disorder)
=> Disorders of the gastrointestinal tract such as,
•>Diverticulitis,
•>Colorectal cancer,
•>Gastrointestinal surgery
Diarrhea can occur due to these conditions.
9) Stress and anxiety
=> Emotional factors such as anxiety, and stress also affect bowel habits, which can also cause diarrhea.
10) Exposure to the new environment (due to exposure to a new environment)
=> Diarrhea can also arise due to the intake of any contaminated food and water in a new environment.
11) Due to increased watery content.
=> The use of any stool softener can also increase the water content and cause diarrhea.
12) Due to disturbance of intestinal motility.
4) Explain the Clinical manifestation/sign and symptoms of the patient with the Diarrhea. Explain the symptoms and signs of the patient with diarrhea.
- Frequent bowel movements.
- Passing loose watery stools.
- Abdominal pain.
- Abdominal cramps.
- Dehydration.
- Fluid and electrolyte imbalance.
- Dry mouth.
- Increased thirst.
- Fatigue.
- Fever.
- Abdominal cramping.
- Perianal itching.
- Nausea.
- Vomiting.
- Malaise.
- Weight loss.
- Blood in the stool (hematochezia).
- Weakness.
- Impaired skin turgor.
4) Explain the diagnostic evaluation of the patient with the Diarrhea. Write a diagnostic evaluation of a patient with diarrhea.
- history tacking and physical examination.
- stool analysis.
- blood analysis.
- check the hemoglobin level.
- assess blood uria nitrogen ( BUN Level).
- Colonoscopy (colonoscopy).
- Sigmoidoscopy ( sigmoidoscopy).
- x rays.
- ct scan.
- MRI.
- assess the breath test.
- Endoscopy (endoscopy).
- Allergy or sensitivity test (allergy or sensitivity test).
6) Explain the management of the patient with the Diarrhea. Write the management of a patient with diarrhea.
- Identify the cause of diarrhea and treat it properly.
1)Fluid replacement
- => Provide intravenous fluid to the patient to prevent dehydration and maintain the patient’s hydration status.
- => Provide oral rehydration solution to the patient.
2)Dietary modifications
- => Advise the patient to avoid irritating foods.
- => Advise the patient to take a bland diet.
- => Advise the patient to take food frequently and in small amounts.
- => Advise the patient to avoid fruits, salads, fried foods, spicy foods, coffee and alcohol.
3) Medication
- => If the patient has diarrhea due to any bacterial infection, then antibiotic medicine should be provided.
4)Antidiarrheal medication
- => If the patient has a condition of diarrhea, provide the over-the-counter drug loperamide.
5)Antiviral drugs
- =>If the cause of diarrhea is a viral infection, provide the patient with antiviral medicine.
6)Antiparacitic drug (Antiparasitic drugs)
- => If the patient’s condition of diarrhea is due to any parasitic infection, then the patient should be provided with anti-parasitic medicine.
7)Anti-inflammatory drugs
- => If the patient’s diarrhea is due to any inflammatory condition, then the patient should be provided with anti-inflammatory drugs.
7) Explain the nursing management of patients with the Diarrhea. Write the nursing management of a patient with diarrhea.
1)Assessment
- => Take a complete history of the patient with diarrhea and perform a physical examination.
- => Monitor the patient’s vital signs.
- => Assess the patient for any signs and symptoms of dehydration.
2)Fluid and electrolyte balance
- => Maintain the patient’s intake output chart.
- => Provide the patient with an oral rehydration solution.
- =>Provide intravenous fluid to the patient to maintain the patient’s fluid and electrolyte balance.
3)Provide nutritional support to the patient (Provide nutritional support to the patient)
- => Advise the patient to take a bland diet.
- => Advise the patient to avoid spicy food, fatty food, fried food.
- => Advise the patient to take food in small and frequent amounts.
4)medication administrations (Medication Administration)
- => Provide the patient with prescribed antibiotics and antidiarrheal medicines.
5) Infection control measures
- •> Advise the patient to maintain proper hygienic conditions to control infection.
- •> Advise the patient to wash hands properly.
- •> Advise the patient to maintain hygienic conditions in their home environment.
- •> Advise the patient to consume heated water.
- •> Advise the patient to consume properly cooked food.
- •> Advise the patient to avoid fruits and vegetables.
- •> Advise the patient to maintain proper personal hygiene.
