Anatomy-Unit-10-B.sc-The Nervous system
🧠 STRUCTURE OF NEURONS
📌 Introduction
Neurons are the structural and functional units of the nervous system. These specialized cells are responsible for receiving, processing, and transmitting electrical and chemical signals throughout the body.
A typical human body contains over 86 billion neurons, working in networks to regulate every action—from reflexes to thoughts, movement, memory, and emotions.
🔬 I. Definition
A neuron is an excitable cell designed to transmit information through electrical impulses (action potentials) and chemical signals (neurotransmitters).
🧩 II. Basic Structure of a Neuron
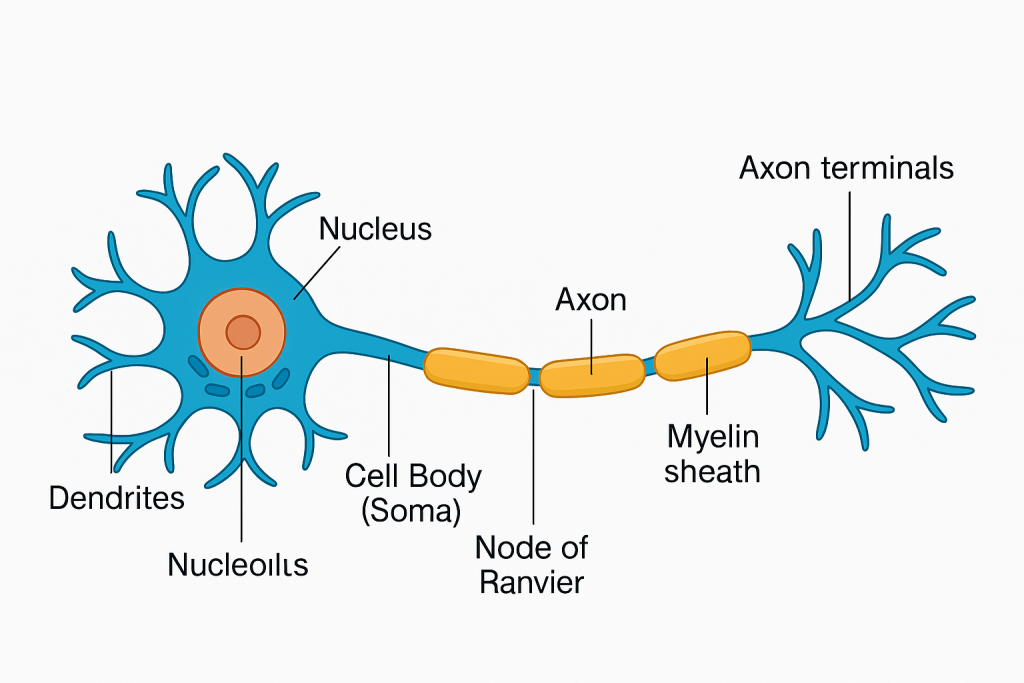
All neurons share a basic structure composed of three main parts:
1. Cell Body (Soma or Perikaryon)
- The central part of the neuron that contains:
- A large, round nucleus with a prominent nucleolus.
- Nissl bodies (or Nissl substance): Rough endoplasmic reticulum rich in ribosomes, involved in protein synthesis.
- Mitochondria, Golgi apparatus, and other organelles for cellular metabolism.
Functions:
- Maintains cell function.
- Synthesizes proteins, enzymes, and neurotransmitters.
- Integrates incoming signals from dendrites.
2. Dendrites
- Short, branching projections extending from the soma.
- Highly branched to increase surface area for receiving signals.
Functions:
- Receive incoming signals from other neurons or sensory receptors.
- Conduct impulses toward the cell body.
- Play a key role in neuroplasticity (learning and memory).
3. Axon
- A single, long process extending from the cell body (can be up to 1 meter in humans).
- Starts at the axon hillock (specialized part of the soma) and ends in axon terminals (telodendria).
- May have collateral branches.
Functions:
- Conducts nerve impulses away from the soma toward other neurons, muscles, or glands.
- Facilitates action potential propagation.
Special Features:
- Axoplasm: Cytoplasm of axon.
- Axolemma: Plasma membrane of the axon.
- Terminal boutons (axon terminals): Release neurotransmitters at synapses.
🌐 III. Myelin Sheath and Nodes of Ranvier
Many axons are covered by an insulating layer called the myelin sheath, formed by:
- Schwann cells in the Peripheral Nervous System (PNS)
- Oligodendrocytes in the Central Nervous System (CNS)
🛡️ Myelin Sheath:
- Lipid-rich, white-colored sheath that increases the speed of impulse conduction.
- Provides electrical insulation.
⚡ Nodes of Ranvier:
- Gaps between adjacent myelin segments.
- Saltatory conduction occurs here—action potentials jump from node to node, increasing speed.
🔁 IV. Synapse
The synapse is the junction between:
- Two neurons (neuron-neuron synapse),
- Or a neuron and muscle/gland cell (neuromuscular/neuroglandular junction).
Components of a Synapse:
- Presynaptic terminal – contains synaptic vesicles filled with neurotransmitters.
- Synaptic cleft – the small gap between the two cells.
- Postsynaptic membrane – contains receptors that bind neurotransmitters.
Neurotransmitters:
- Examples: Acetylcholine, dopamine, serotonin, GABA, glutamate, norepinephrine
- They modulate, excite, or inhibit the postsynaptic cell.
🧬 V. Types of Neurons (Based on Structure)
1. Multipolar Neurons:
- One axon, many dendrites.
- Most common type (e.g., motor neurons, interneurons).
2. Bipolar Neurons:
- One axon and one dendrite.
- Found in special senses (e.g., retina, olfactory epithelium).
3. Unipolar (Pseudounipolar) Neurons:
- One process that splits into an axon and dendrite.
- Found in sensory neurons of spinal ganglia.
🧠 VI. Types of Neurons (Based on Function)
1. Sensory (Afferent) Neurons:
- Transmit impulses from sensory receptors to CNS.
2. Motor (Efferent) Neurons:
- Transmit impulses from CNS to muscles/glands.
3. Interneurons (Association Neurons):
- Located entirely in the CNS.
- Process information, connect sensory and motor neurons.
🩺 VII. Clinical Relevance in Nursing and Health Sciences
Understanding neuron structure is critical in managing conditions like:
- Stroke – damage to neurons due to interrupted blood flow.
- Multiple Sclerosis (MS) – demyelination in the CNS leading to impaired conduction.
- Parkinson’s Disease – loss of dopamine-producing neurons.
- Peripheral Neuropathy – damage to peripheral nerves due to diabetes or trauma.
- Spinal Cord Injuries – disrupt signal transmission below the injury level.
- Seizures/Epilepsy – abnormal neuronal firing.
- Neurotoxic Drug Reactions – some medications (e.g., chemotherapy) can affect neurons.
✅
A neuron is a dynamic and specialized cell responsible for rapid communication in the body. Its structure—soma, dendrites, axon, and synapse—is finely tuned to process and transmit signals. Nurses and healthcare providers must understand the anatomy and physiology of neurons to comprehend neurological diseases, medications’ effects, and recovery after nervous system injuries.
🧠 CENTRAL NERVOUS SYSTEM (CNS) – STRUCTURE AND FUNCTION
📌 Introduction
The Central Nervous System (CNS) is the control center of the entire nervous system. It processes sensory input, initiates motor output, and is responsible for higher mental functions such as thought, memory, emotion, and learning. The CNS consists of the brain and spinal cord, both protected by bones, meninges, and cerebrospinal fluid (CSF).
🧠 CENTRAL NERVOUS SYSTEM – BRAIN ANATOMY
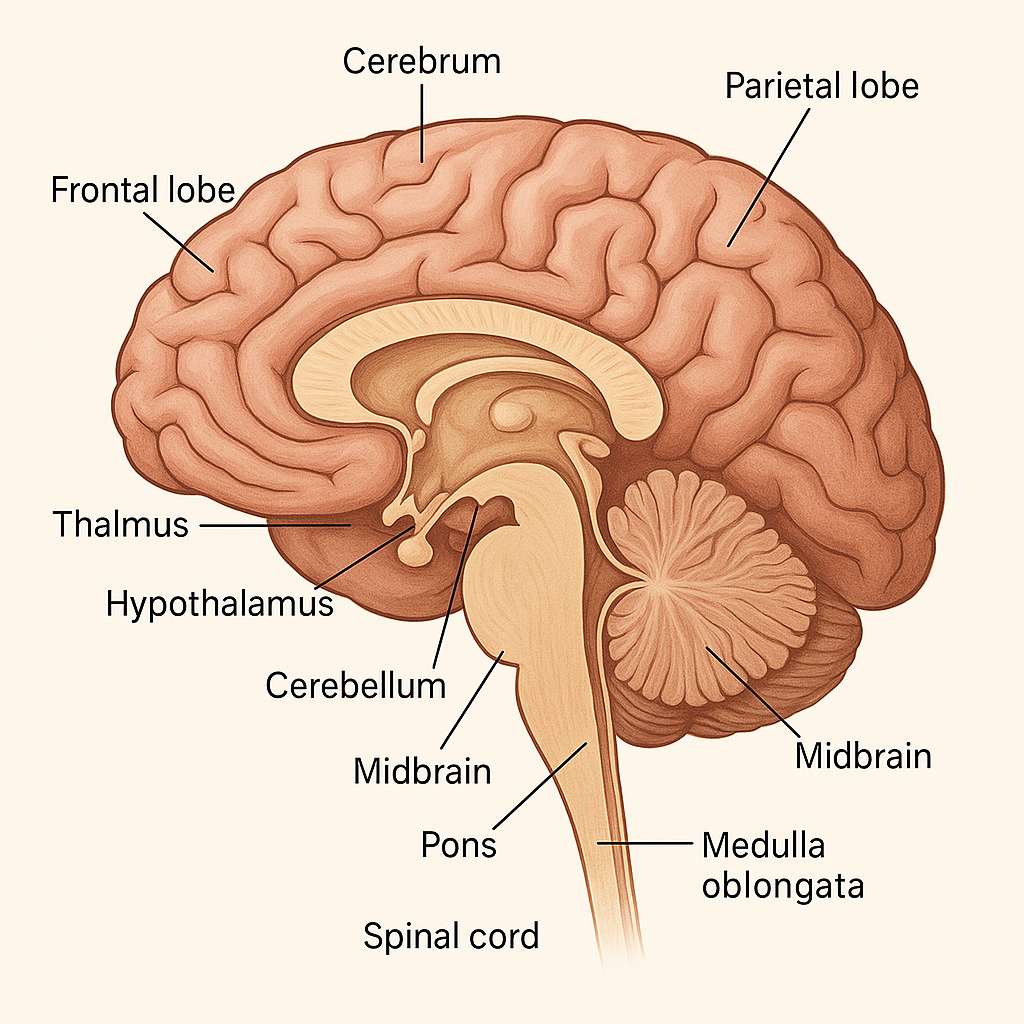
📌 Introduction
The brain is the most complex organ in the human body, comprising billions of interconnected neurons. It is the command center of the Central Nervous System (CNS), responsible for sensory interpretation, motor control, cognitive functions, emotion, and autonomic regulation. It is housed in the cranial cavity, protected by the skull, meninges, and cerebrospinal fluid (CSF).
🧠 GROSS ANATOMY OF THE BRAIN
The brain is divided into three main regions:
I. Forebrain (Prosencephalon)
II. Midbrain (Mesencephalon)
III. Hindbrain (Rhombencephalon)
Let’s explore each in detail:
I. FOREBRAIN
A. Cerebrum (Telencephalon)
- Largest part of the brain (~80% of brain mass)
- Divided into two cerebral hemispheres (left and right), connected by the corpus callosum
- Each hemisphere is divided into four lobes:
🔹 Frontal Lobe
- Located at the front of the brain
- Functions:
- Voluntary motor control (primary motor cortex)
- Speech production (Broca’s area – usually in the left hemisphere)
- Personality, behavior, planning, decision-making
🔹 Parietal Lobe
- Located behind the frontal lobe
- Functions:
- Somatosensory perception (touch, temperature, pain)
- Spatial orientation
- Interpretation of language and mathematics
🔹 Temporal Lobe
- Located on the sides near the ears
- Functions:
- Auditory processing (hearing)
- Memory formation
- Language comprehension (Wernicke’s area – usually in left hemisphere)
🔹 Occipital Lobe
- Located at the back of the brain
- Function:
- Visual processing (primary visual cortex)
➕ Additional Structures:
- Insula (deep within the lateral sulcus): Involved in emotion, taste, and visceral sensation
🧠 Cerebral Cortex:
- Gray matter: outermost layer; contains neuron cell bodies
- White matter: inner layer; contains myelinated axons
B. Diencephalon
Deep brain structure made of:
🔹 Thalamus
- Major relay center for all sensory information (except smell)
- Sends information to appropriate areas of the cerebral cortex
🔹 Hypothalamus
- Located below the thalamus
- Regulates:
- Body temperature
- Hunger and thirst
- Autonomic nervous system (ANS)
- Endocrine functions via pituitary gland
- Sleep-wake cycles and emotional behavior
🔹 Epithalamus
- Contains pineal gland, which secretes melatonin for circadian rhythm regulation
II. MIDBRAIN (MESENCEPHALON)
Part of the brainstem, located between the diencephalon and pons.
Major Structures:
🔹 Tectum (posterior part)
- Contains:
- Superior colliculi – visual reflexes
- Inferior colliculi – auditory reflexes
🔹 Cerebral peduncles (anterior)
- Contain motor tracts from cerebral cortex to spinal cord
🔹 Substantia nigra
- Involved in dopamine production
- Degenerates in Parkinson’s disease
III. HINDBRAIN (RHOMBENCEPHALON)
A. Pons
- Bridge between cerebrum and cerebellum
- Contains respiratory centers
- Relays signals for hearing, equilibrium, and facial sensations
B. Medulla Oblongata
- Extends into the spinal cord
- Controls vital autonomic functions:
- Heart rate
- Breathing
- Blood pressure
- Reflexes: coughing, swallowing, vomiting
- Site of decussation of pyramids (crossing over of motor fibers)
C. Cerebellum
- Located posterior to the pons and medulla
- Two hemispheres, separated by the vermis
- Functions:
- Coordination of voluntary movements
- Balance and posture
- Muscle tone regulation
- Motor learning
🔁 VENTRICULAR SYSTEM
- Consists of 4 interconnected ventricles:
- 2 Lateral ventricles
- Third ventricle (in diencephalon)
- Fourth ventricle (between pons and cerebellum)
- Filled with cerebrospinal fluid (CSF) produced by choroid plexus
- CSF flows into subarachnoid space and central canal of spinal cord
🔬 MICROSTRUCTURE
- Gray Matter: Contains neuron cell bodies (outer cerebral cortex and deep nuclei)
- White Matter: Contains myelinated axons for communication between regions
🛡️ PROTECTION OF THE BRAIN
- Cranium (skull) – Bony protection
- Meninges:
- Dura mater – tough outer layer
- Arachnoid mater – web-like middle layer
- Pia mater – thin inner layer adheres to brain surface
- Cerebrospinal Fluid (CSF) – Cushions and nourishes brain
- Blood-Brain Barrier (BBB) – Regulates passage of substances into the brain tissue
🧠 BLOOD SUPPLY
- Anterior circulation: Internal carotid arteries
- Posterior circulation: Vertebral arteries → Basilar artery
- Together form the Circle of Willis, which ensures collateral blood flow
- Brain is extremely sensitive to hypoxia (oxygen deprivation)
🧠 BRAIN FUNCTIONAL AREAS (BY CORTEX)
| Area | Location | Function |
|---|---|---|
| Primary motor cortex | Precentral gyrus (frontal lobe) | Voluntary movement |
| Primary sensory cortex | Postcentral gyrus (parietal lobe) | Sensory perception |
| Broca’s area | Left frontal lobe | Speech production |
| Wernicke’s area | Left temporal lobe | Language comprehension |
| Visual cortex | Occipital lobe | Vision |
| Auditory cortex | Temporal lobe | Hearing |
🩺 CLINICAL SIGNIFICANCE IN NURSING
🧠 Common Conditions:
- Stroke (CVA): Disruption of cerebral blood flow
- Traumatic brain injury (TBI)
- Epilepsy: Abnormal electrical discharges
- Meningitis: Inflammation of meninges
- Hydrocephalus: CSF buildup
- Parkinson’s disease: Dopamine neuron degeneration
- Brain tumors
- Alzheimer’s disease: Neurodegeneration of cortex and hippocampus
🩺 Nursing Role:
- Monitor neurological status (LOC, GCS, pupil size, limb movement)
- Prepare for imaging (CT, MRI)
- Administer anticonvulsants, mannitol, steroids, etc.
- Provide education and support for neurological rehab
✅
The brain is a sophisticated organ composed of several distinct regions with specialized functions. From coordinating movement to interpreting sensory data and regulating vital processes, it is the epicenter of bodily control. A thorough understanding of brain anatomy is essential for diagnosing, treating, and caring for patients with neurological disorders.
🧠 AUTONOMIC NERVOUS SYSTEM (ANS) – STRUCTURE
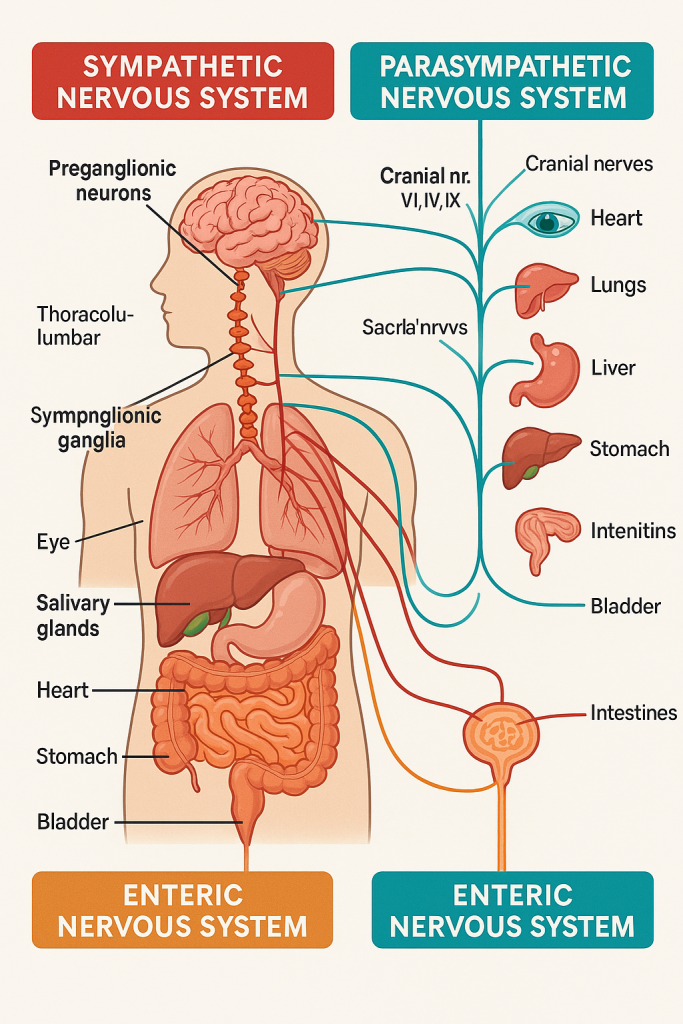
📌 Introduction
The Autonomic Nervous System (ANS) is a subdivision of the peripheral nervous system (PNS) that controls involuntary functions of the body. It regulates the activity of smooth muscle, cardiac muscle, and glands—controlling essential functions like heart rate, digestion, respiration, pupil dilation, and blood pressure.
🔍 Key Feature: The ANS functions unconsciously, maintaining homeostasis and responding to internal and external stimuli.
🧠 I. Divisions of the ANS
The ANS is divided into three functional components:
1. Sympathetic Nervous System (SNS)
2. Parasympathetic Nervous System (PNS)
3. Enteric Nervous System (ENS)
Let’s break down each component:
⚡️ II. Sympathetic Nervous System (SNS) – “Fight or Flight”
🔹 Function:
- Prepares the body for emergency, stress, or vigorous activity.
- Increases heart rate, blood pressure, respiration, and glucose release.
- Dilates pupils, inhibits digestion, and redirects blood to muscles.
🔹 Origin:
- Arises from thoracolumbar region of the spinal cord (T1 to L2)
🔹 Structure:
a) Preganglionic Neurons:
- Originate in the lateral horns of spinal cord (T1–L2)
- Axons are short and synapse in sympathetic ganglia
b) Sympathetic Ganglia:
- Paravertebral ganglia: form the sympathetic chain on both sides of the vertebral column.
- Prevertebral ganglia: located anterior to the vertebrae (e.g., celiac, superior mesenteric, inferior mesenteric)
c) Postganglionic Neurons:
- Long axons that travel to target organs (e.g., heart, lungs, blood vessels)
🔹 Neurotransmitters:
- Preganglionic: Acetylcholine (ACh)
- Postganglionic: Norepinephrine (NE) (except sweat glands – ACh)
🌿 III. Parasympathetic Nervous System (PNS) – “Rest and Digest”
🔹 Function:
- Promotes relaxation, digestion, energy conservation, and waste elimination.
- Decreases heart rate, increases digestive secretions, contracts bladder.
🔹 Origin:
- Arises from craniosacral regions:
- Cranial nerves III, VII, IX, X
- Sacral spinal cord (S2–S4)
🔹 Structure:
a) Preganglionic Neurons:
- Originate in brainstem and sacral spinal cord
- Axons are long, synapsing near or within target organs
b) Ganglia:
- Located close to or within target organs (terminal or intramural ganglia)
c) Postganglionic Neurons:
- Short axons that innervate smooth muscle, cardiac muscle, and glands
🔹 Neurotransmitters:
- Both preganglionic and postganglionic neurons release Acetylcholine (ACh)
🍽️ IV. Enteric Nervous System (ENS) – “Gut Brain”
🔹 Function:
- Controls the gastrointestinal system independently or under modulation by SNS/PNS.
- Regulates:
- Peristalsis
- Secretion
- Blood flow to the gut
🔹 Structure:
- Composed of two major plexuses in the walls of the GI tract:
- Myenteric (Auerbach’s) plexus – controls GI motility
- Submucosal (Meissner’s) plexus – controls GI secretion and blood flow
🔀 V. Comparison of Sympathetic vs Parasympathetic
| Feature | Sympathetic | Parasympathetic |
|---|---|---|
| Origin | Thoracolumbar (T1–L2) | Craniosacral (CN III, VII, IX, X; S2–S4) |
| Preganglionic fibers | Short | Long |
| Postganglionic fibers | Long | Short |
| Ganglia location | Near spinal cord | Near/in target organ |
| NT at effector | Norepinephrine (mostly) | Acetylcholine |
| Action | Fight or flight | Rest and digest |
🧠 VI. Key Autonomic Reflexes
- Baroreceptor reflex – regulates blood pressure
- Pupillary light reflex – constriction/dilation of pupils
- Micturition reflex – bladder control
- Gastrocolic reflex – promotes defecation post-meal
These are coordinated by autonomic centers in the hypothalamus, brainstem, and spinal cord.
🩺 VII. Clinical Importance in Nursing & Medicine
🧠 Common ANS-related Conditions:
- Orthostatic hypotension – failure of sympathetic system to constrict blood vessels on standing
- Autonomic neuropathy – seen in diabetes, Parkinson’s, multiple system atrophy
- Pheochromocytoma – adrenal tumor causing excessive catecholamine release
- Neurogenic bladder – impaired bladder control due to nerve damage
- Horner’s syndrome – sympathetic nerve disruption (ptosis, miosis, anhidrosis)
🩺 Nursing Role:
- Monitor vital signs, especially in patients on ANS-affecting drugs (e.g., beta-blockers, anticholinergics)
- Educate on postural hypotension precautions
- Recognize autonomic warning signs: dizziness, excessive sweating, dry mouth, GI issues
- Support patients with temperature dysregulation or urinary incontinence
✅
The Autonomic Nervous System (ANS) is a vital part of the peripheral nervous system that regulates automatic, unconscious bodily functions. Comprising the sympathetic, parasympathetic, and enteric systems, the ANS ensures internal balance (homeostasis) through rapid, involuntary responses. Its dysfunction is central to many medical conditions, and understanding its structure and role is crucial for nurses, clinicians, and students alike.
🧠 PERIPHERAL NERVOUS SYSTEM (PNS)
📌 Introduction
The Peripheral Nervous System (PNS) is the part of the nervous system outside the brain and spinal cord. It serves as a communication line between the Central Nervous System (CNS) and the rest of the body, including organs, limbs, skin, and muscles.
The PNS is essential for sensation, movement, autonomic regulation, and reflexes. It carries sensory (afferent) information to the CNS and motor (efferent) commands from the CNS to the body.
🧠 I. DIVISIONS OF THE PNS
The PNS is divided into two major functional components:
1. Somatic Nervous System (SNS)
- Controls voluntary actions (skeletal muscle movement)
- Transmits sensory information from skin, muscles, joints to the CNS
2. Autonomic Nervous System (ANS)
- Controls involuntary actions (cardiac, smooth muscles, glands)
- Further divided into:
- Sympathetic nervous system (fight or flight)
- Parasympathetic nervous system (rest and digest)
- Enteric nervous system (gut brain)
🔍 II. STRUCTURAL COMPONENTS OF THE PNS
1. Cranial Nerves (12 pairs)
Arise from the brain and brainstem, innervate the head, neck, and some thoracic/abdominal structures.
🧠 The 12 Cranial Nerves:
| Nerve | Name | Function |
|---|---|---|
| I | Olfactory | Smell (sensory) |
| II | Optic | Vision (sensory) |
| III | Oculomotor | Eye movement, pupil constriction (motor) |
| IV | Trochlear | Eye movement (superior oblique) (motor) |
| V | Trigeminal | Facial sensation & chewing (mixed) |
| VI | Abducens | Eye movement (lateral rectus) (motor) |
| VII | Facial | Facial expression, taste, tear/saliva (mixed) |
| VIII | Vestibulocochlear | Hearing and balance (sensory) |
| IX | Glossopharyngeal | Taste, swallowing, salivation (mixed) |
| X | Vagus | Parasympathetic control of thoracic/abdominal organs (mixed) |
| XI | Accessory | Neck and shoulder movement (motor) |
| XII | Hypoglossal | Tongue movement (motor) |
2. Spinal Nerves (31 pairs)
Arise from the spinal cord and are connected to specific body regions (dermatomes & myotomes).
📍 Classification:
- 8 Cervical (C1–C8)
- 12 Thoracic (T1–T12)
- 5 Lumbar (L1–L5)
- 5 Sacral (S1–S5)
- 1 Coccygeal (Co1)
Each spinal nerve has:
- Dorsal (posterior) root – carries sensory (afferent) fibers
- Ventral (anterior) root – carries motor (efferent) fibers
- These unite to form a mixed spinal nerve
🕸️ III. NERVE PLEXUSES OF THE PNS
Plexuses are networks of interconnected spinal nerves that redistribute fibers to different body regions.
1. Cervical Plexus (C1–C4)
- Innervates neck and diaphragm (phrenic nerve – C3, C4, C5)
2. Brachial Plexus (C5–T1)
- Innervates upper limbs
- Major nerves: axillary, radial, ulnar, median, musculocutaneous
3. Lumbar Plexus (L1–L4)
- Innervates anterior and medial thigh
- Major nerves: femoral, obturator
4. Sacral Plexus (L4–S4)
- Innervates posterior thigh, lower leg, foot
- Major nerves: sciatic nerve (largest in body), tibial, peroneal
💡 IV. FUNCTIONAL CLASSIFICATION OF PNS FIBERS
A. Sensory (Afferent) Fibers
- Carry information from the body to the CNS
- Include:
- Somatic sensory fibers – skin, muscles, joints
- Visceral sensory fibers – organs (e.g., stretch, chemical changes)
B. Motor (Efferent) Fibers
- Carry commands from CNS to muscles/glands
- Include:
- Somatic motor fibers – skeletal muscles (voluntary)
- Autonomic motor fibers – cardiac/smooth muscle, glands (involuntary)
🔁 V. REFLEX ARC – Basic Unit of PNS Response
A reflex arc is the simplest pathway of neural control, involving:
- Receptor – detects stimulus
- Sensory neuron – sends info to CNS
- Integration center – spinal cord (sometimes brain)
- Motor neuron – sends command to effector
- Effector – muscle or gland responds
⚡ Example: Patellar (knee-jerk) reflex
🧠 VI. Neurotransmitters in the PNS
- Acetylcholine (ACh): Used by motor neurons at neuromuscular junctions, and parasympathetic fibers
- Norepinephrine (NE): Used by sympathetic postganglionic neurons
🩺 VII. Clinical Relevance in Nursing and Healthcare
✨ Common PNS Disorders:
- Peripheral neuropathy – due to diabetes, toxins, infections
- Guillain-Barré syndrome – autoimmune demyelination of peripheral nerves
- Bell’s palsy – facial nerve (CN VII) paralysis
- Carpal tunnel syndrome – median nerve compression
- Sciatica – compression of sciatic nerve
🩺 Nursing Role:
- Conduct neurovascular assessments (sensation, strength, reflexes)
- Monitor effects of nerve injury, surgery, or compression
- Educate patients on nerve protection, pain management, and rehabilitation
- Administer and monitor medications that affect the neuromuscular junction or autonomic system
✅
The Peripheral Nervous System is the link between the CNS and the rest of the body. It is structurally made up of cranial and spinal nerves, and functionally classified into somatic and autonomic divisions. The PNS plays a vital role in sensation, motor function, reflexes, and autonomic regulation, making it a critical focus in neurological assessment, nursing care, and patient management.
🧠 STRUCTURE OF THE BRAIN
📌 Introduction
The brain is the central organ of the central nervous system (CNS) and serves as the body’s command center. It is responsible for consciousness, coordination, emotion, memory, sensory processing, movement, and vital autonomic functions. It is housed within the cranial cavity, protected by the skull, meninges, and cerebrospinal fluid (CSF).
The adult human brain weighs approximately 1.3 to 1.4 kg, and is composed of gray matter (neuronal cell bodies) and white matter (myelinated axons).
🧠 Main Divisions of the Brain
The brain is anatomically and functionally divided into three major parts:
1. Cerebrum (Forebrain)
2. Cerebellum
3. Brainstem
🧠 STRUCTURE OF THE CEREBRUM (FOREBRAIN)
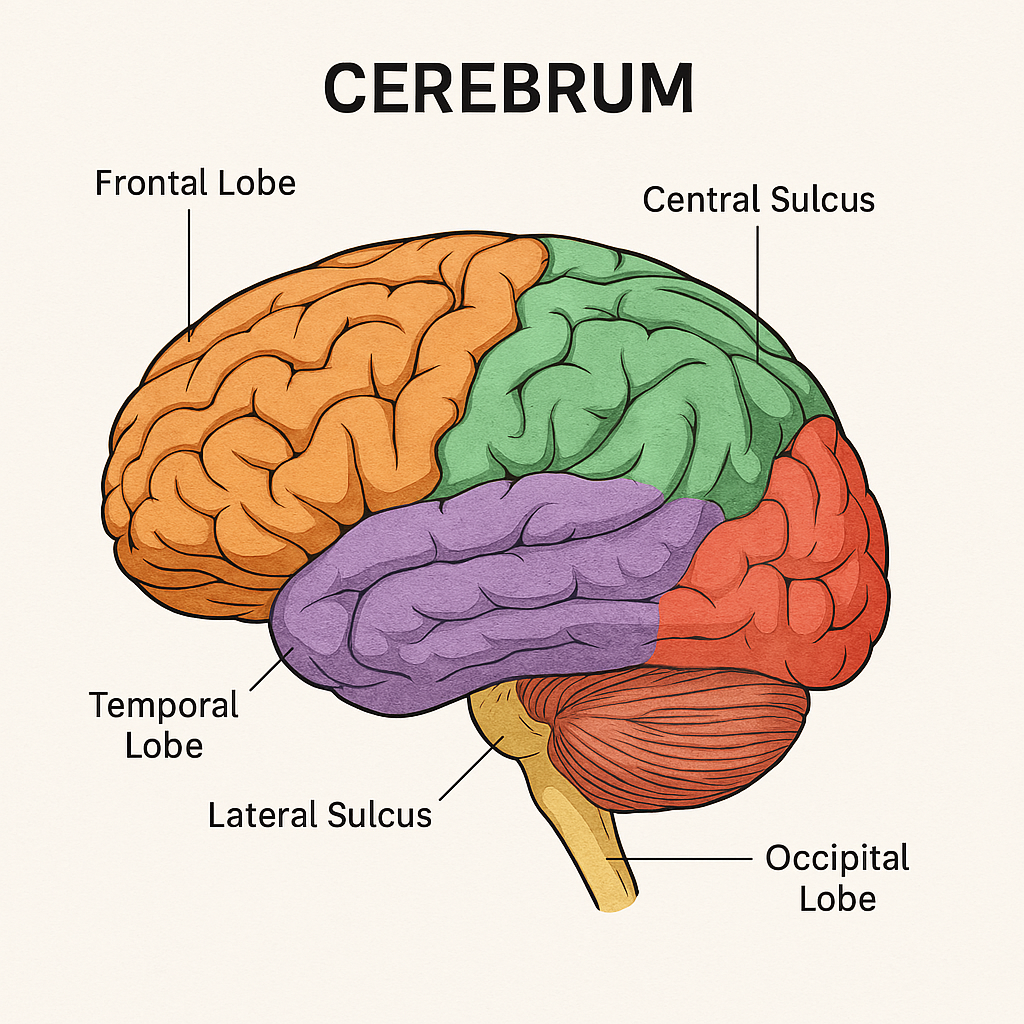
The cerebrum is the largest and most prominent part of the human brain, forming the major portion of the forebrain (prosencephalon). It is responsible for voluntary motor activity, sensory perception, intelligence, memory, language, emotions, and consciousness.
The cerebrum makes up ~85% of the brain’s mass and is divided into two cerebral hemispheres, each controlling the opposite side of the body.
🧠 I. Gross Anatomy of the Cerebrum
1. Cerebral Hemispheres
- The cerebrum is divided into left and right hemispheres, separated by a deep groove called the longitudinal fissure.
- The two hemispheres are connected internally by a thick band of white matter called the corpus callosum, allowing communication between them.
2. Lobes of the Cerebrum
Each hemisphere is divided into four lobes, named after the overlying cranial bones:
🔹 A. Frontal Lobe
- Located in the front part of the cerebrum
- Functions:
- Voluntary motor control (via primary motor cortex)
- Personality, reasoning, judgment, decision-making
- Speech production (Broca’s area in the dominant hemisphere)
- Emotional expression and social behavior
🔹 B. Parietal Lobe
- Located behind the frontal lobe and above the temporal lobe
- Functions:
- Sensory perception (via primary somatosensory cortex)
- Touch, pressure, pain, temperature
- Spatial orientation, body awareness
- Integration of sensory input from various systems
🔹 C. Temporal Lobe
- Located beneath the frontal and parietal lobes, near the temples
- Functions:
- Hearing and auditory processing
- Language comprehension (Wernicke’s area in the dominant hemisphere)
- Olfactory perception (smell)
- Memory and learning
🔹 D. Occipital Lobe
- Located at the back of the cerebrum
- Functions:
- Visual processing (primary visual cortex)
- Interpretation of color, shape, and motion
🔹 E. Insular Lobe (Insula)
- Located deep within the lateral sulcus
- Functions:
- Taste perception
- Visceral sensations
- Emotion, empathy, self-awareness
🧩 II. Surface Features of the Cerebrum
1. Gyri (singular: gyrus)
- Elevated ridges or folds on the cerebral surface
- Increase surface area for more neurons
2. Sulci (singular: sulcus)
- Shallow grooves between gyri
- Important sulci:
- Central sulcus – separates frontal and parietal lobes
- Lateral sulcus – separates temporal lobe from frontal and parietal
- Parieto-occipital sulcus – separates parietal and occipital lobes
3. Fissures
- Deep grooves dividing large brain regions
- Longitudinal fissure – divides left and right hemispheres
- Transverse fissure – separates cerebrum from cerebellum
🧬 III. Internal Structure of the Cerebrum
1. Cerebral Cortex
- Outer layer of the cerebrum
- Composed of gray matter (neuronal cell bodies)
- Responsible for conscious thought, sensory perception, and voluntary movement
Cortex Regions:
- Motor areas – control voluntary muscle movements
- Sensory areas – interpret incoming sensory information
- Association areas – integrate motor and sensory functions for complex actions
2. White Matter
- Lies beneath the cortex
- Made of myelinated axons
- Functions to connect different parts of the cerebrum and brain
Types of Fibers:
- Commissural fibers: connect left and right hemispheres (e.g., corpus callosum)
- Association fibers: connect regions within the same hemisphere
- Projection fibers: connect the cerebrum to the lower brain and spinal cord
🧠 IV. Deep Structures of the Cerebrum
1. Basal Ganglia (Basal Nuclei)
- A group of deep gray matter nuclei
- Includes: caudate nucleus, putamen, globus pallidus
- Functions:
- Regulation of voluntary motor movements
- Control of posture, muscle tone, and movement precision
- Involved in Parkinson’s disease and Huntington’s disease
2. Limbic System
- A ring-like structure deep in the cerebrum
- Includes: hippocampus, amygdala, cingulate gyrus
- Functions:
- Emotion, behavior, motivation
- Memory formation
- Emotional response to stimuli
🧪 V. Blood Supply of the Cerebrum
- Supplied by:
- Internal carotid arteries
- Vertebral arteries
- These form the Circle of Willis at the base of the brain
- Main cerebral arteries:
- Anterior cerebral artery – supplies medial frontal and parietal lobes
- Middle cerebral artery – supplies lateral surface of cerebrum (most common site of stroke)
- Posterior cerebral artery – supplies occipital lobe and part of temporal lobe
🧠 VI. Functional Areas of the Cerebral Cortex
| Functional Area | Location | Function |
|---|---|---|
| Primary Motor Cortex | Precentral gyrus (frontal) | Voluntary skeletal muscle movement |
| Primary Somatosensory Cortex | Postcentral gyrus (parietal) | Touch, pain, temperature sensation |
| Broca’s Area | Left frontal lobe | Speech production |
| Wernicke’s Area | Left temporal lobe | Language comprehension |
| Primary Visual Cortex | Occipital lobe | Visual perception |
| Primary Auditory Cortex | Temporal lobe | Hearing |
| Prefrontal Cortex | Anterior frontal lobe | Personality, planning, judgment |
🩺 VII. Clinical Relevance of the Cerebrum
Common Cerebral Disorders:
- Stroke – blockage or rupture of cerebral arteries
- Epilepsy – abnormal electrical discharges in the cortex
- Alzheimer’s Disease – degeneration of cerebral cortex and hippocampus
- Parkinson’s Disease – basal ganglia dysfunction
- Brain tumors – often affect specific lobes and functions
- Traumatic Brain Injury (TBI) – damage to specific cortical areas can cause motor, sensory, or behavioral deficits
🧠 STRUCTURE OF THE CEREBELLUM
📌 Introduction
The cerebellum is a vital part of the hindbrain, located in the posterior cranial fossa, beneath the occipital lobes of the cerebrum and behind the brainstem. Though only about 10% of the brain’s weight, it contains over 50% of the brain’s neurons.
🧠 Primary Functions:
- Coordination of voluntary movements
- Balance and posture
- Muscle tone regulation
- Motor learning and fine-tuning
🧠 I. Location and External Anatomy
🔹 Location:
- Posterior to the pons and medulla oblongata
- Inferior to the occipital lobes of the cerebrum
- Separated from the cerebrum by the tentorium cerebelli (a dural fold)
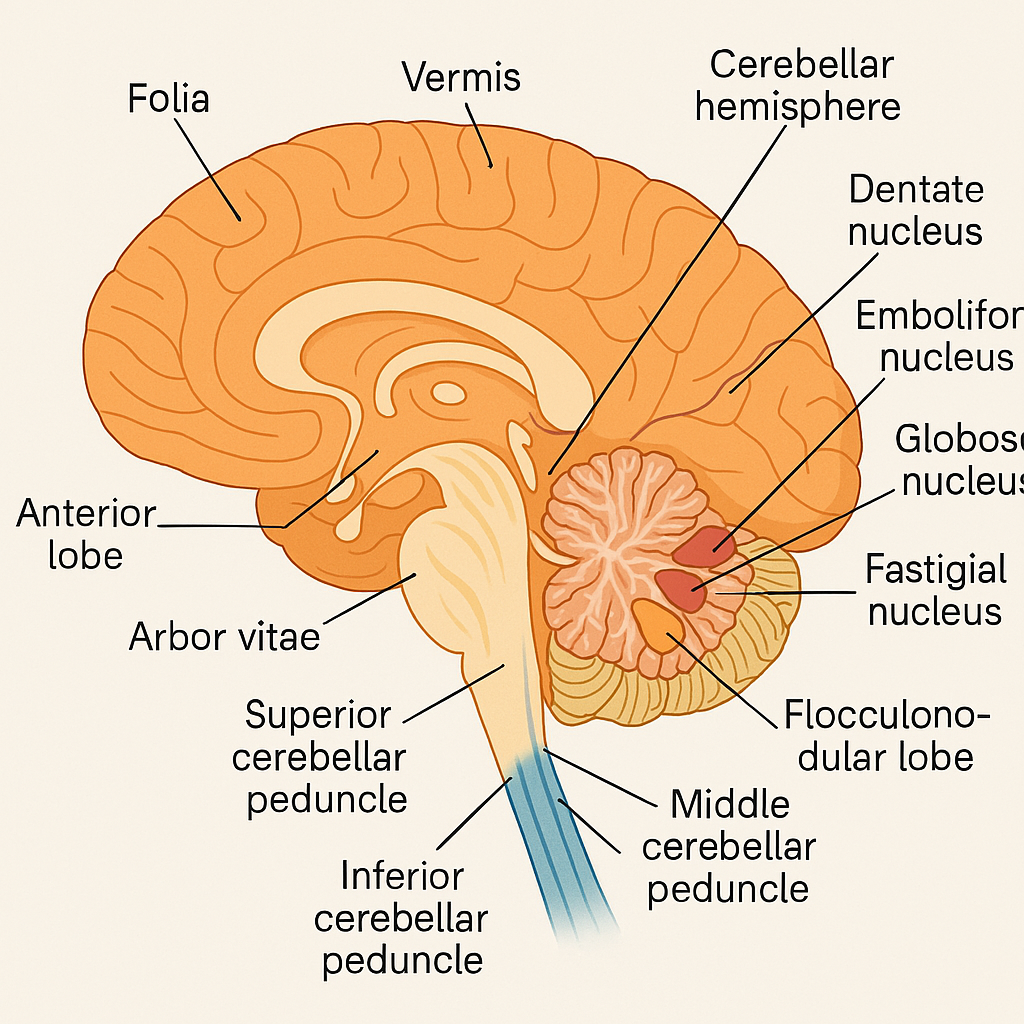
🔹 External Features:
- The cerebellum has two hemispheres (right and left)
- A central narrow midline structure called the vermis connects the hemispheres
- The surface is folded into numerous narrow parallel grooves called folia, increasing surface area
- Divided into anterior, posterior, and flocculonodular lobes
🧩 II. Lobes and Functional Divisions
The cerebellum is divided both anatomically and functionally:
🔹 A. Anatomical Lobes:
- Anterior Lobe: Primarily involved in limb movement coordination
- Posterior Lobe: Involved in fine motor coordination and planning
- Flocculonodular Lobe: Controls balance and eye movements
🔹 B. Functional Zones:
- Vestibulocerebellum:
- Comprises the flocculonodular lobe
- Maintains balance and controls eye movements
- Spinocerebellum:
- Comprises the vermis and intermediate parts
- Coordinates posture, muscle tone, and gross limb movements
- Cerebrocerebellum:
- Lateral hemispheres
- Involved in planning and initiation of voluntary movement, motor learning
🧬 III. Internal Structure
🔹 1. Cerebellar Cortex
- The outer gray matter arranged in three layers:
- Molecular Layer – contains dendrites and interneurons
- Purkinje Cell Layer – single layer of large Purkinje neurons, which send inhibitory signals
- Granular Layer – densely packed with small neurons
🔹 2. White Matter (Arbor Vitae)
- Underlying white matter appears like a tree in cross-section (Latin: “tree of life”)
- Carries afferent and efferent signals to/from the cerebellar cortex
🔹 3. Cerebellar Nuclei (Deep nuclei embedded in white matter)
These are the output centers of the cerebellum:
- Dentate nucleus: Largest; involved in planning and initiation of voluntary movement
- Emboliform and Globose nuclei (interposed nuclei): Regulate limb movement
- Fastigial nucleus: Maintains balance and posture
🔁 IV. Cerebellar Peduncles
The cerebellum connects to the brainstem through three paired cerebellar peduncles, which carry afferent and efferent fibers:
| Peduncle | Connects To | Function |
|---|---|---|
| Superior | Midbrain | Sends output from cerebellum to cerebral cortex |
| Middle | Pons | Receives input from cerebrum (largest input pathway) |
| Inferior | Medulla | Receives input from spinal cord and brainstem |
🧠 V. Blood Supply of the Cerebellum
Supplied by three main arteries:
- Superior cerebellar artery (SCA)
- Anterior inferior cerebellar artery (AICA)
- Posterior inferior cerebellar artery (PICA)
These branches arise from the basilar and vertebral arteries.
💬 VI. Functions of the Cerebellum
Although the cerebellum does not initiate movement, it fine-tunes and coordinates it. Key functions include:
- Balance and posture regulation
- Coordination of voluntary movement
- Muscle tone maintenance
- Motor learning (e.g., learning to ride a bicycle)
- Smooth execution of complex movements
- Correcting errors in motor commands by comparing intended vs. actual movement
⚠️ VII. Clinical Importance in Nursing and Medicine
Damage to the cerebellum can result in ataxia, or uncoordinated movement.
🩺 Common Cerebellar Disorders:
- Cerebellar ataxia: Gait and movement disorders
- Intention tremor: Tremor during voluntary movement
- Dysmetria: Inability to judge distance (overshooting/undershooting)
- Dysdiadochokinesia: Difficulty with rapid alternating movements
- Nystagmus: Involuntary eye movements
- Vertigo and balance problems
- Cerebellar stroke or tumor
👩⚕️ Nursing Assessment Tips:
- Observe gait and coordination
- Perform finger-to-nose or heel-to-shin tests
- Assess speech clarity (may be slow or slurred in cerebellar lesions)
- Monitor for dizziness, nausea, or nystagmus
✅
The cerebellum is a vital motor coordination center, involved in ensuring that movements are smooth, precise, and well-timed. Though it works subconsciously, its influence on posture, gait, balance, and fine motor skills is indispensable. A solid understanding of cerebellar structure and function is crucial for diagnosing neurological deficits, guiding rehabilitation, and ensuring patient safety.
🧠 STRUCTURE OF THE BRAINSTEM
📌 Introduction
The brainstem is the lowest part of the brain, connecting the cerebrum and cerebellum with the spinal cord. It is vital for life-sustaining functions such as breathing, heartbeat, blood pressure regulation, and consciousness. The brainstem also houses cranial nerve nuclei, ascending sensory and descending motor pathways, and reflex centers.
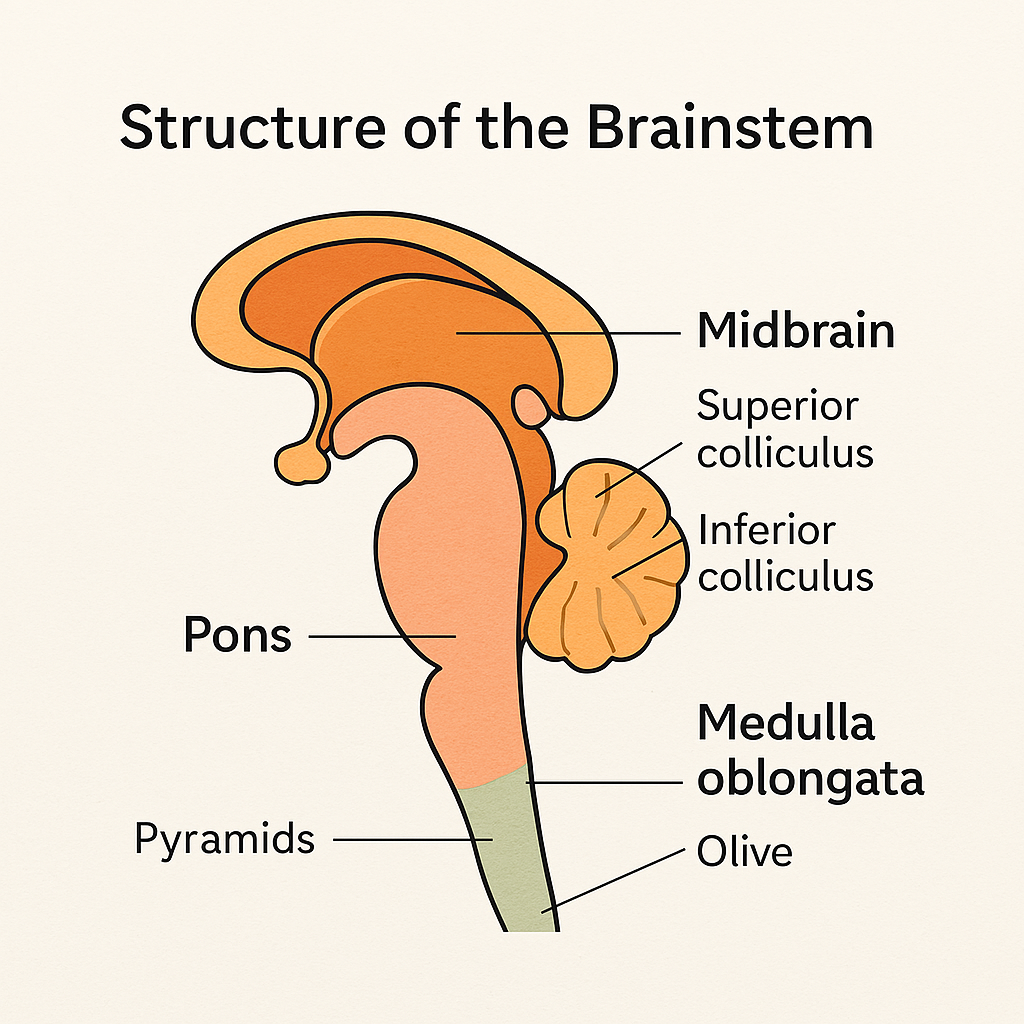
🧠 I. Main Parts of the Brainstem
The brainstem is anatomically divided into three major parts, from top to bottom:
- Midbrain (Mesencephalon)
- Pons
- Medulla Oblongata
1️⃣ MIDBRAIN (MESENCEPHALON)
🔹 Location:
- Uppermost part of the brainstem
- Connects the diencephalon (thalamus) to the pons
🔹 Key Structures:
- Cerebral Peduncles (anterior side):
- Bundles of descending motor fibers from the cerebral cortex to the brainstem and spinal cord
- Tectum (posterior side):
- Contains four colliculi forming the corpora quadrigemina:
- Superior colliculi: Visual reflex centers (e.g., tracking moving objects)
- Inferior colliculi: Auditory reflex centers (e.g., startle response)
- Contains four colliculi forming the corpora quadrigemina:
- Substantia Nigra:
- Produces dopamine; degeneration here leads to Parkinson’s disease
- Red Nucleus:
- Involved in motor coordination
- Cerebral Aqueduct:
- Connects the third and fourth ventricles, allowing CSF flow
🔹 Cranial Nerves:
- CN III (Oculomotor)
- CN IV (Trochlear)
2️⃣ PONS
🔹 Location:
- Lies between the midbrain and medulla oblongata
- Appears as a rounded bulge on the anterior surface of the brainstem
🔹 Functions:
- Acts as a bridge between the cerebrum, cerebellum, and spinal cord
- Assists in respiratory control via the pneumotaxic and apneustic centers
- Plays a role in sleep, facial expressions, bladder control
🔹 Key Features:
- Contains transverse fibers connecting to the cerebellum via the middle cerebellar peduncles
- Contains ascending sensory and descending motor tracts
- Houses several cranial nerve nuclei
🔹 Cranial Nerves:
- CN V (Trigeminal)
- CN VI (Abducens)
- CN VII (Facial)
- CN VIII (Vestibulocochlear) – partly in pons and medulla
3️⃣ MEDULLA OBLONGATA
🔹 Location:
- Lowest part of the brainstem
- Continuous with the spinal cord at the foramen magnum
- Lies anterior to the cerebellum
🔹 Key Features:
- Pyramids:
- Contain corticospinal (motor) tracts
- Site of decussation of pyramids – ~90% of motor fibers cross to the opposite side
- Olives:
- Swellings lateral to pyramids
- Relay sensory and motor signals, especially for coordination
🔹 Vital Centers (Autonomic Nuclei):
- Cardiac center: Regulates heart rate
- Vasomotor center: Regulates blood pressure
- Respiratory center: Controls breathing rhythm (works with pons)
- Reflex centers: For coughing, sneezing, vomiting, swallowing
🔹 Cranial Nerves:
- CN IX (Glossopharyngeal)
- CN X (Vagus)
- CN XI (Accessory)
- CN XII (Hypoglossal)
🧠 II. Functions of the Brainstem
The brainstem acts as a relay center and reflex integrator, playing essential roles in:
- Consciousness and arousal (via Reticular Activating System – RAS)
- Autonomic control of heart rate, respiration, and blood pressure
- Cranial nerve function (nuclei of 10 out of 12 cranial nerves lie here)
- Motor and sensory pathway transmission between the body and brain
- Coordination of balance and movement via connections to the cerebellum
🧬 III. Reticular Formation
- A network of interconnected neurons spanning the entire brainstem
- Involved in:
- Arousal and consciousness (Reticular Activating System)
- Regulation of sleep-wake cycles
- Pain modulation
- Posture and motor control
🩺 IV. Clinical Significance of Brainstem
Damage to the brainstem can be life-threatening due to its control over vital functions.
Common Conditions:
- Brainstem stroke – may cause locked-in syndrome
- Multiple sclerosis (MS) – demyelination affects brainstem pathways
- Tumors or trauma – compress brainstem structures
- Brainstem herniation – can result in coma or death
- Decerebrate/decorticate posturing – signs of severe brainstem injury
Nursing Considerations:
- Monitor vital signs, especially respiratory and cardiovascular status
- Assess cranial nerve function regularly
- Use Glasgow Coma Scale (GCS) to track changes in consciousness
- Prepare for ventilator support if respiratory centers are compromised
- Watch for pupil changes, motor deficits, dysphagia, or gag reflex loss
🧠 STRUCTURE OF THE SPINAL CORD –
📌 Introduction
The spinal cord is a long, cylindrical structure that serves as a vital communication highway between the brain and the body. It is part of the Central Nervous System (CNS) and is responsible for transmitting sensory and motor information, as well as coordinating reflexes.
🧠 I. Location and Extent
- The spinal cord is located within the vertebral canal of the vertebral column.
- It extends from the medulla oblongata (brainstem) at the level of the foramen magnum down to the L1–L2 vertebral level in adults.
- Below this level, it continues as the cauda equina (a bundle of nerve roots).
🔢 II. Length and Segmentation
- Average length: 42–45 cm in adults
- The spinal cord is divided into 31 segments, each giving rise to a pair of spinal nerves:
- 8 cervical (C1–C8)
- 12 thoracic (T1–T12)
- 5 lumbar (L1–L5)
- 5 sacral (S1–S5)
- 1 coccygeal (Co1)
Each segment connects to the body through dorsal (sensory) and ventral (motor) nerve roots.
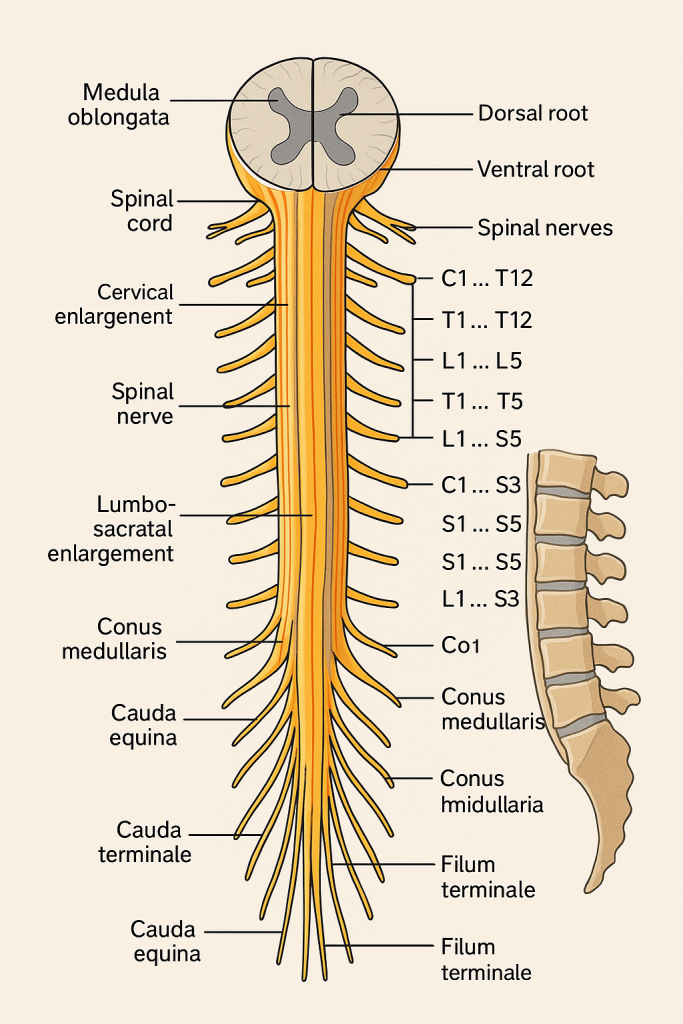
🧬 III. External Structure
🔹 Spinal Cord Enlargements
These are areas where the cord is thicker due to a higher density of neurons:
- Cervical enlargement (C4–T1) – supplies upper limbs
- Lumbosacral enlargement (L2–S3) – supplies lower limbs
🔹 Conus Medullaris
- The tapered terminal end of the spinal cord (~L1–L2)
🔹 Cauda Equina
- “Horse’s tail” of nerve roots extending below the conus medullaris
🔹 Filum Terminale
- A thin filament that anchors the spinal cord to the coccyx
🧩 IV. Internal Structure (Cross-Section)
The spinal cord in cross-section has a butterfly or H-shaped gray matter surrounded by white matter.
🔸 A. Gray Matter
- Located centrally
- Consists of neuron cell bodies
- Divided into:
- Dorsal (posterior) horns – receive sensory input
- Ventral (anterior) horns – send out motor signals
- Lateral horns (T1–L2 only) – contain sympathetic neurons
- Central canal: A small canal running through the center; filled with CSF
🔸 B. White Matter
- Located peripherally
- Contains myelinated axons organized into tracts:
- Ascending tracts – carry sensory info to the brain
- Descending tracts – carry motor commands from the brain
Example Tracts:
- Spinothalamic tract – pain and temperature (ascending)
- Corticospinal tract – voluntary motor control (descending)
- Dorsal column tract – fine touch and proprioception (ascending)
🕸️ V. Spinal Nerves and Roots
Each spinal segment gives rise to a pair of spinal nerves (mixed – sensory + motor):
- Dorsal root: Contains sensory fibers and dorsal root ganglion
- Ventral root: Contains motor fibers
- These unite to form a spinal nerve, which exits the vertebral column via intervertebral foramen
🛡️ VI. Protective Structures
- Vertebrae – bony protection
- Meninges – three layers covering the spinal cord:
- Dura mater (outer, tough)
- Arachnoid mater (middle, web-like)
- Pia mater (inner, delicate)
- Cerebrospinal Fluid (CSF) – circulates in the subarachnoid space; cushions and nourishes
🔄 VII. Functions of the Spinal Cord
- Sensory Relay – Receives input from body and sends to brain
- Motor Relay – Transmits brain signals to muscles and organs
- Reflex Center – Controls involuntary, immediate responses (e.g., withdrawal reflex)
- Autonomic Control – Involved in control of visceral organs (e.g., bladder, bowel)
⚕️ VIII. Clinical Relevance in Nursing and Healthcare
🧠 Common Conditions:
- Spinal cord injury (SCI) – trauma causing paralysis, sensory loss
- Herniated disc – compresses spinal nerves
- Spinal stenosis – narrowing of the spinal canal
- Multiple sclerosis (MS) – demyelination of spinal tracts
- Meningitis – inflammation of the meninges
- Cauda equina syndrome – emergency; loss of bowel/bladder control, saddle anesthesia
🩺 Nursing Considerations:
- Assess motor and sensory function
- Monitor reflexes (Babinski, deep tendon reflexes)
- Prevent pressure ulcers and infections in paralyzed patients
- Support bladder and bowel training in spinal injury patients
- Assist in spinal immobilization, lumbar puncture procedures
✅
The spinal cord is the essential communication link between the brain and the rest of the body. It is involved in reflex activity, sensory integration, motor output, and autonomic control. Its segmental organization and pathway structures make it a critical focus in neurology and emergency care.
🧠 STRUCTURE OF CRANIAL NERVES
📌 Introduction
Cranial nerves are 12 pairs of nerves that arise directly from the brain or brainstem, rather than the spinal cord. They are primarily responsible for motor and sensory functions of the head, neck, and certain internal organs. Some cranial nerves are purely sensory, others purely motor, and several are mixed (both sensory and motor).
🔍 Mnemonic for Names:
Oh Oh Oh To Touch And Feel Very Good Velvet Ah Heaven
(CN I–XII: Olfactory, Optic, Oculomotor, Trochlear, Trigeminal, Abducens, Facial, Vestibulocochlear, Glossopharyngeal, Vagus, Accessory, Hypoglossal)
🔍 Mnemonic for Type (Sensory, Motor, Both):
Some Say Marry Money But My Brother Says Big **Brains Matter More
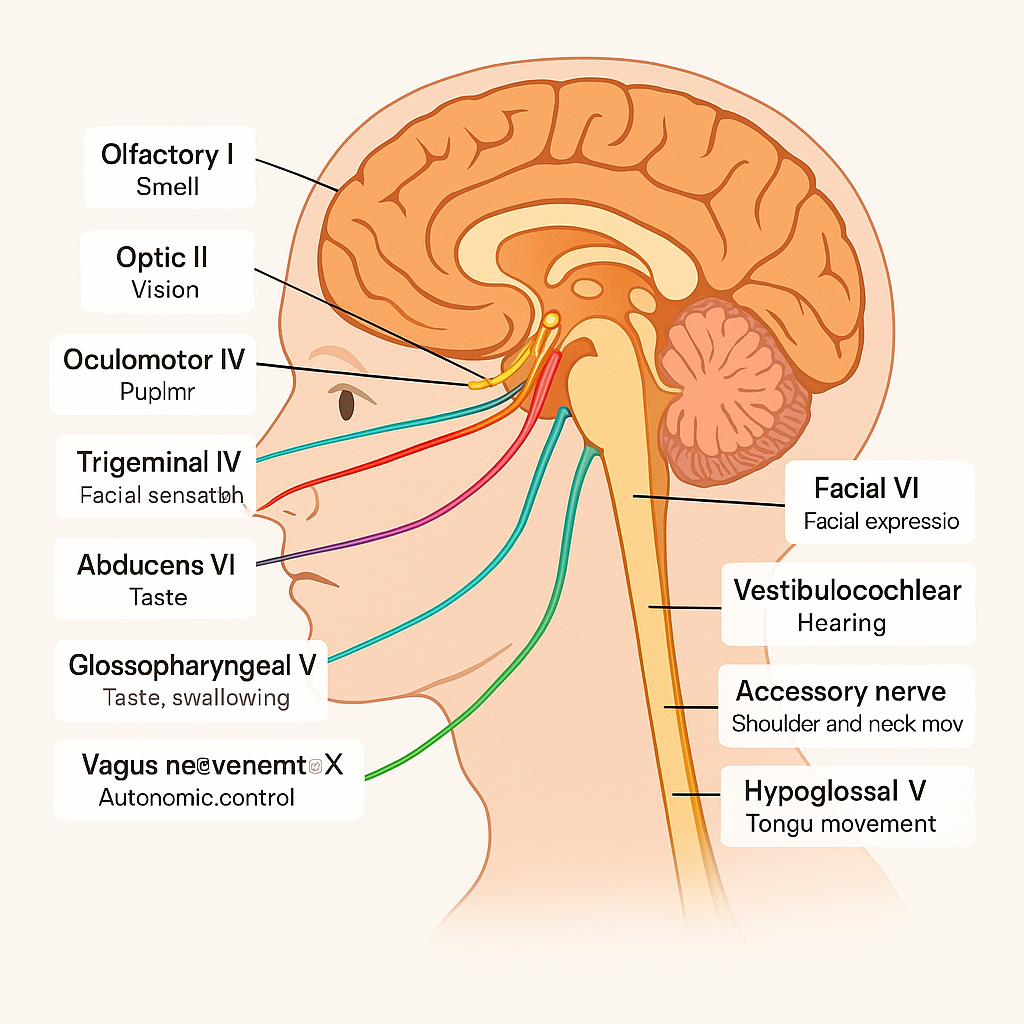
🧠 I. List and Structure of the 12 Cranial Nerves
| CN | Name | Type | Main Functions |
|---|---|---|---|
| I | Olfactory | Sensory | Smell |
| II | Optic | Sensory | Vision |
| III | Oculomotor | Motor | Eye movement, pupil constriction, eyelid elevation |
| IV | Trochlear | Motor | Eye movement (superior oblique muscle) |
| V | Trigeminal | Mixed | Facial sensation, chewing |
| VI | Abducens | Motor | Eye movement (lateral rectus muscle) |
| VII | Facial | Mixed | Facial expression, taste (anterior 2/3 of tongue), salivation, lacrimation |
| VIII | Vestibulocochlear | Sensory | Hearing and balance |
| IX | Glossopharyngeal | Mixed | Taste (posterior 1/3), swallowing, salivation (parotid), carotid body reflex |
| X | Vagus | Mixed | Autonomic control of heart, lungs, GI tract, swallowing, voice |
| XI | Accessory | Motor | Shoulder and neck movement (trapezius, sternocleidomastoid) |
| XII | Hypoglossal | Motor | Tongue movement |
🧬 II. Origin and Pathways
| CN | Brain Origin | Foramina of Exit |
|---|---|---|
| I | Olfactory bulb | Cribriform plate (ethmoid bone) |
| II | Diencephalon | Optic canal |
| III | Midbrain | Superior orbital fissure |
| IV | Midbrain (dorsal side) | Superior orbital fissure |
| V | Pons | V1 – Superior orbital fissure; V2 – Foramen rotundum; V3 – Foramen ovale |
| VI | Pons | Superior orbital fissure |
| VII | Pons-medulla junction | Internal acoustic meatus → stylomastoid foramen |
| VIII | Pons-medulla junction | Internal acoustic meatus |
| IX | Medulla | Jugular foramen |
| X | Medulla | Jugular foramen |
| XI | Medulla + spinal cord | Jugular foramen |
| XII | Medulla | Hypoglossal canal |
🔍 III. Detailed Functional Overview
🔹 CN I – Olfactory Nerve (Sensory)
- Function: Smell
- Pathway: Nasal mucosa → olfactory bulb → olfactory tract → brain
- Clinical test: Smell test with non-irritating substances
🔹 CN II – Optic Nerve (Sensory)
- Function: Vision
- Pathway: Retina → optic nerve → optic chiasm → optic tract → visual cortex
- Clinical test: Visual acuity, visual fields, fundoscopy
🔹 CN III – Oculomotor Nerve (Motor)
- Controls 4 of 6 extraocular muscles
- Function: Eye movement, eyelid elevation (levator palpebrae), pupil constriction
- Lesion signs: Ptosis, diplopia, dilated pupil, “down and out” eye
🔹 CN IV – Trochlear Nerve (Motor)
- Innervates superior oblique muscle (eye)
- Function: Downward and lateral eye movement
- Lesion signs: Vertical diplopia, worse on downward gaze
🔹 CN V – Trigeminal Nerve (Mixed)
- 3 branches:
- V1 (Ophthalmic) – sensory (forehead, scalp, cornea)
- V2 (Maxillary) – sensory (cheek, upper lip, upper teeth)
- V3 (Mandibular) – sensory + motor (jaw, lower lip, mastication muscles)
- Clinical test: Corneal reflex, jaw clench, facial sensation
🔹 CN VI – Abducens Nerve (Motor)
- Controls lateral rectus muscle
- Function: Eye abduction
- Lesion signs: Inability to move eye laterally, diplopia
🔹 CN VII – Facial Nerve (Mixed)
- Functions:
- Motor: Facial expression
- Sensory: Taste (anterior 2/3 of tongue)
- Parasympathetic: Lacrimal and salivary glands
- Clinical test: Facial movement, taste test, tear production
- Lesion: Bell’s Palsy – ipsilateral facial paralysis
🔹 CN VIII – Vestibulocochlear Nerve (Sensory)
- Two divisions:
- Cochlear – hearing
- Vestibular – balance
- Clinical test: Hearing tests (Rinne, Weber), balance exams
🔹 CN IX – Glossopharyngeal Nerve (Mixed)
- Functions:
- Taste (posterior 1/3 tongue)
- Gag reflex
- Salivation (parotid gland)
- Carotid body/baroreceptor reflex
- Lesion: Loss of taste, impaired swallowing
🔹 CN X – Vagus Nerve (Mixed)
- Longest cranial nerve
- Functions:
- Motor: Pharynx, larynx, soft palate
- Parasympathetic: Heart, lungs, GI tract
- Sensory: Thoracic and abdominal viscera
- Lesion signs: Hoarseness, dysphagia, loss of gag reflex
🔹 CN XI – Accessory Nerve (Motor)
- Motor innervation to:
- Trapezius – shoulder elevation
- Sternocleidomastoid – head rotation
- Test: Shrug shoulders, turn head against resistance
🔹 CN XII – Hypoglossal Nerve (Motor)
- Controls tongue muscles
- Test: Stick out tongue → deviates toward affected side if paralyzed
🩺 Clinical Relevance in Nursing and Healthcare
💡 Cranial Nerve Assessments Are Vital In:
- Neurological examination (stroke, trauma, brain tumors)
- ICU/critical care monitoring (brainstem function)
- Conditions like:
- Bell’s palsy (CN VII)
- Trigeminal neuralgia (CN V)
- Vestibular neuritis (CN VIII)
- Dysphagia and aspiration risk (CN IX, X)
- Brainstem lesions (multiple CN involvement)
🩺 Nursing Considerations:
- Perform routine cranial nerve exams
- Monitor for speech, swallowing, hearing, facial symmetry
- Document findings in detail
- Support with feeding modifications, eye care, speech therapy referrals when needed
✅
The cranial nerves are a crucial set of 12 paired nerves that arise from the brain and brainstem. Each has specific roles in sensation, motor control, or autonomic regulation, especially in the head, face, and visceral organs. Accurate understanding and assessment of cranial nerves are vital for early diagnosis and care of neurological conditions.
🧠 STRUCTURE OF SPINAL NERVES
📌 Introduction
The spinal nerves are part of the Peripheral Nervous System (PNS). They arise from the spinal cord and serve as vital communication links between the central nervous system (CNS) and the rest of the body. Each spinal nerve carries motor, sensory, and autonomic fibers that supply specific parts of the body.
🔹 Humans have 31 pairs of spinal nerves, each emerging from the spinal cord via nerve roots.
🧠 I. Number and Distribution of Spinal Nerves
There are 31 pairs of spinal nerves, categorized by the spinal cord region from which they emerge:
| Region | Number of Pairs | Nerve Pairs |
|---|---|---|
| Cervical | 8 (C1–C8) | 8 |
| Thoracic | 12 (T1–T12) | 12 |
| Lumbar | 5 (L1–L5) | 5 |
| Sacral | 5 (S1–S5) | 5 |
| Coccygeal | 1 (Co1) | 1 |
🧠 Note: Despite having only 7 cervical vertebrae, there are 8 cervical spinal nerves because C1 exits above the first vertebra, and C8 exits below the seventh.
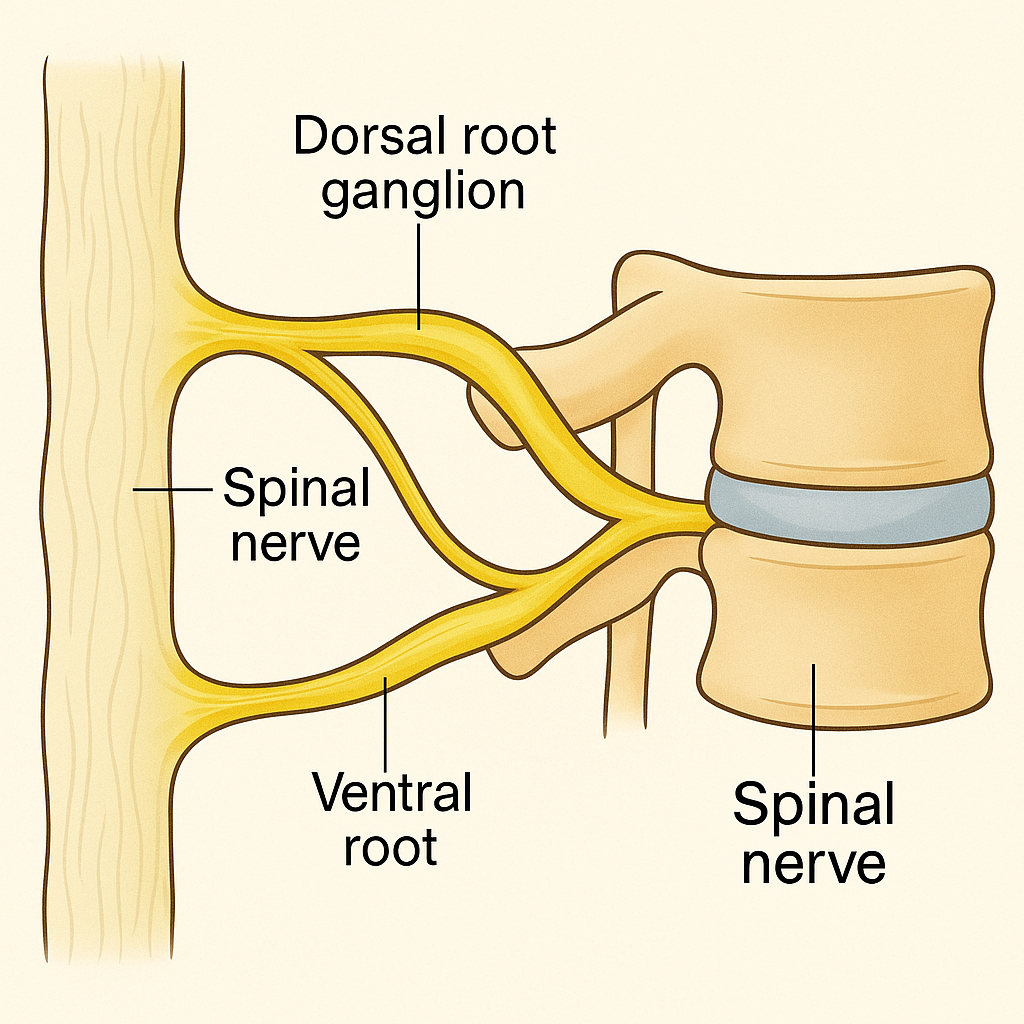
🧬 II. Basic Structure of a Spinal Nerve
Each spinal nerve is formed by the union of two nerve roots:
🔹 1. Dorsal (Posterior) Root
- Carries sensory (afferent) fibers from the body to the spinal cord
- Contains a dorsal root ganglion, which houses the cell bodies of sensory neurons
🔹 2. Ventral (Anterior) Root
- Carries motor (efferent) fibers from the spinal cord to muscles and glands
🔹 3. Mixed Spinal Nerve
- After the dorsal and ventral roots unite, they form a short mixed spinal nerve that carries both motor and sensory fibers
🧠 III. Spinal Nerve Branches (Rami)
After emerging from the intervertebral foramen, the spinal nerve divides into four branches:
1. Dorsal (Posterior) Ramus
- Supplies muscles and skin of the back
2. Ventral (Anterior) Ramus
- Supplies limbs and the anterior/lateral parts of the trunk
- Forms plexuses in cervical, brachial, lumbar, and sacral regions
3. Meningeal Branch
- Reenters vertebral canal to innervate meninges, vertebrae, and blood vessels
4. Rami Communicantes
- Connect spinal nerves to the sympathetic chain of the autonomic nervous system
- White ramus (preganglionic fibers)
- Gray ramus (postganglionic fibers)
🕸️ IV. Spinal Nerve Plexuses
A plexus is a network of intersecting nerves formed by ventral rami.
🔹 1. Cervical Plexus (C1–C4)
- Innervates neck, head, shoulders, diaphragm
- Phrenic nerve: Supplies the diaphragm (C3–C5)
🔹 2. Brachial Plexus (C5–T1)
- Supplies upper limbs
- Major branches: Axillary, Radial, Median, Ulnar, Musculocutaneous
🔹 3. Lumbar Plexus (L1–L4)
- Supplies anterior and medial thigh
- Major nerves: Femoral, Obturator
🔹 4. Sacral Plexus (L4–S4)
- Supplies lower limb and pelvic organs
- Major nerves: Sciatic, Tibial, Common peroneal
🔹 5. Coccygeal Plexus (S4–Co1)
- Supplies skin around the coccyx
🧠 V. Functional Components of Spinal Nerve Fibers
Each spinal nerve contains four functional fiber types:
| Type | Direction | Function |
|---|---|---|
| Somatic Afferent | Sensory | Skin, muscles, joints to CNS |
| Somatic Efferent | Motor | CNS to skeletal muscles |
| Visceral Afferent | Sensory | Organs to CNS |
| Visceral Efferent | Motor | CNS to smooth/cardiac muscle & glands (ANS) |
🔄 VI. Dermatomes and Myotomes
🔹 Dermatomes:
- Areas of skin innervated by sensory fibers from a single spinal nerve
- Useful in diagnosing nerve root or spinal cord injuries
🔹 Myotomes:
- Groups of muscles innervated by motor fibers from a single spinal nerve
🩺 Clinical Note:
- Shingles (Herpes zoster) follows a dermatomal pattern
- Testing muscle strength and reflexes helps localize spinal nerve damage
🩺 VII. Clinical Significance in Nursing and Medicine
🔹 Common Disorders:
- Herniated Disc – compresses spinal nerves → pain, numbness
- Spinal Cord Injury – leads to paralysis or sensory loss below the level
- Radiculopathy – inflammation/compression of a spinal nerve root
- Cauda Equina Syndrome – emergency involving lower spinal nerves
👩⚕️ Nursing Responsibilities:
- Perform neurological assessments (motor, sensory, reflexes)
- Educate on nerve injury precautions
- Support mobility, bowel/bladder care, and skin integrity
- Monitor for dermatomal pain or weakness
🧠 STRUCTURE OF PERIPHERAL NERVES
📌 Introduction
Peripheral nerves are the communication lines of the Peripheral Nervous System (PNS) that connect the Central Nervous System (CNS) to limbs, organs, muscles, and skin. These nerves carry sensory (afferent) information to the CNS and motor (efferent) commands from the CNS to the body.
They include:
- Cranial nerves (arising from the brain/brainstem)
- Spinal nerves (arising from the spinal cord)
- Autonomic nerves (sympathetic and parasympathetic fibers)
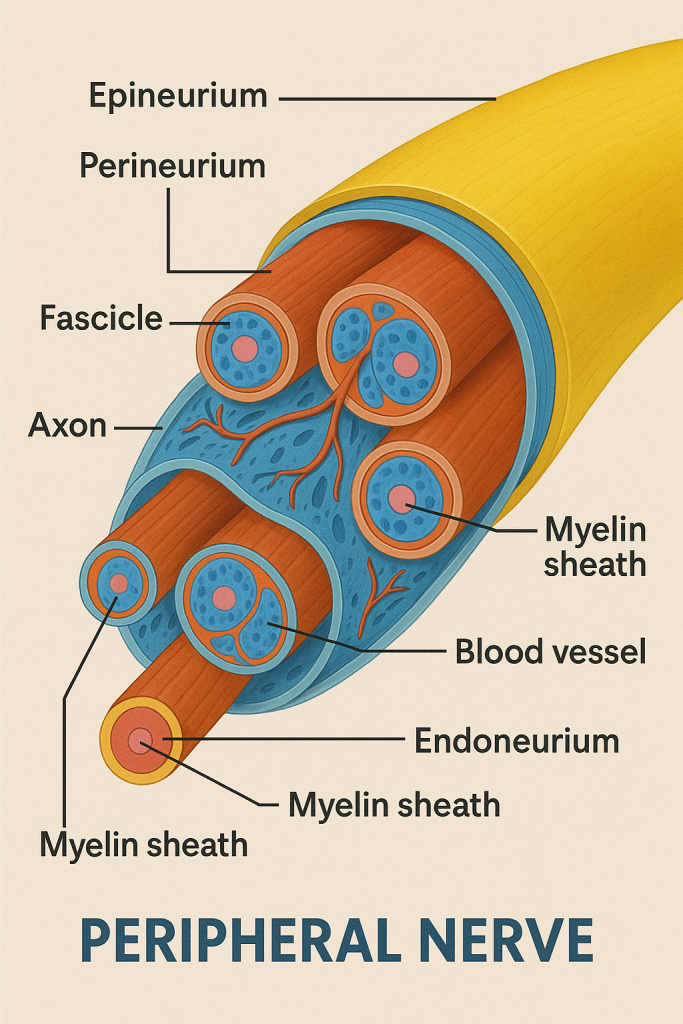
🧬 I. Composition of a Peripheral Nerve
A peripheral nerve is a bundle of nerve fibers (axons) wrapped in several layers of connective tissue, organized much like electrical cables.
🔹 1. Nerve Fibers
- Axons: Long projections of neurons that transmit electrical signals
- May be myelinated (fast conduction) or unmyelinated (slower conduction)
- Surrounded by Schwann cells (in the PNS) which:
- Produce myelin sheath (in myelinated fibers)
- Support and insulate the axon
📦 II. Connective Tissue Layers (Protective Sheaths)
- Endoneurium:
- Surrounds individual axons
- Delicate layer of connective tissue containing capillaries
- Perineurium:
- Surrounds a bundle of axons (fascicle)
- Provides a protective barrier against toxins and pathogens
- Epineurium:
- Outermost thick layer
- Encloses multiple fascicles and blood vessels
- Provides mechanical strength to the whole nerve
🧠 Vasa nervorum: Small blood vessels that supply the nerve within the epineurium and perineurium.
🧠 III. Types of Peripheral Nerve Fibers
🔸 Based on Function:
| Fiber Type | Direction | Function |
|---|---|---|
| Somatic Afferent | Sensory | From skin, muscles, joints → CNS |
| Somatic Efferent | Motor | From CNS → skeletal muscles |
| Visceral Afferent | Sensory | From internal organs → CNS |
| Visceral Efferent | Motor | From CNS → smooth muscles, glands (ANS) |
🔸 Based on Conduction:
- A fibers: Large, myelinated, fast (motor and sensory)
- B fibers: Small, lightly myelinated (autonomic)
- C fibers: Smallest, unmyelinated, slow (pain, temperature)
🧠 IV. Peripheral Nerve Organization
🔹 A. Sensory Nerves
- Carry afferent impulses from receptors in the skin, muscles, and organs to the CNS
- Examples: Touch, temperature, pain, proprioception
🔹 B. Motor Nerves
- Carry efferent impulses from CNS to muscles and glands
- Control voluntary movement and autonomic responses
🔹 C. Mixed Nerves
- Contain both motor and sensory fibers
- Most spinal nerves are mixed nerves
📌 V. Neurolemma (Sheath of Schwann)
- The outermost membrane of Schwann cells
- Important for nerve fiber regeneration in the PNS
- CNS neurons lack this sheath, so regeneration is limited in the brain/spinal cord
🧠 VI. Nerve Regeneration in PNS
- PNS nerves can regenerate if the cell body is intact
- Process involves:
- Wallerian degeneration (distal axon dies)
- Axonal sprouting
- Guidance by Schwann cells and endoneurial tubes
⚠️ CNS neurons lack this capability due to absence of Schwann cells and presence of inhibitory factors.
🩺 VII. Clinical Importance in Nursing and Medicine
✨ Common Disorders:
- Peripheral neuropathy (e.g., diabetic neuropathy)
- Radial, ulnar, or peroneal nerve palsy
- Carpal tunnel syndrome (median nerve compression)
- Bell’s palsy (facial nerve inflammation)
- Guillain-Barré syndrome (autoimmune demyelination)
- Nerve injury or trauma (from fractures or surgery)
🩺 Nursing Responsibilities:
- Assess motor strength, reflexes, and sensory deficits
- Monitor for nerve injury post-surgery or trauma
- Assist with nerve conduction studies or EMG
- Support rehabilitation and prevent pressure ulcers in affected areas
- Educate on nerve protection, posture, splint use, etc.
✅
Peripheral nerves are bundles of axons encased in protective layers, responsible for transmitting sensory and motor information between the body and CNS. Their structure—consisting of axons, Schwann cells, and connective tissue (endoneurium, perineurium, epineurium)—ensures signal efficiency, protection, and potential for regeneration in case of injury. Understanding this helps in diagnosing and managing nerve disorders effectively.
🧠 FUNCTIONAL AREAS OF THE CEREBRAL CORTEX

📌 Introduction
The cerebral cortex is the outermost layer of the cerebrum, composed of gray matter (neuronal cell bodies). It is responsible for conscious thought, voluntary movement, sensory perception, language, memory, and decision-making.
The cerebral cortex is divided into lobes (frontal, parietal, temporal, occipital), each with specialized functional areas classified into:
- Motor areas
- Sensory areas
- Association areas
🧠 I. MOTOR AREAS – Control Voluntary Movements
🔹 1. Primary Motor Cortex
- Location: Precentral gyrus of the frontal lobe
- Function: Initiates voluntary muscle movements
- Somatotopic organization: Represented by the motor homunculus
- Large area devoted to face, hands, tongue (fine motor control)
🔹 2. Premotor Cortex
- Location: Anterior to primary motor cortex
- Function: Plans and coordinates complex movements, like writing or playing piano
🔹 3. Supplementary Motor Area
- Location: Medial frontal lobe
- Function: Coordinates bilateral movements and motor memory
🔹 4. Broca’s Area (usually in left hemisphere)
- Location: Inferior frontal gyrus
- Function: Controls speech production, facial muscles
- Damage → Broca’s aphasia (non-fluent, expressive aphasia)
🧠 II. SENSORY AREAS – Perceive Sensory Input
🔹 1. Primary Somatosensory Cortex
- Location: Postcentral gyrus (parietal lobe)
- Function: Receives tactile information (touch, pressure, pain, temperature, proprioception)
- Organized into a sensory homunculus
🔹 2. Somatosensory Association Area
- Location: Posterior to primary somatosensory cortex
- Function: Interprets sensory input (e.g., recognizing an object by touch)
🔹 3. Primary Visual Cortex
- Location: Occipital lobe
- Function: Processes basic visual information (light, shape, color)
🔹 4. Visual Association Area
- Location: Surrounding the primary visual cortex
- Function: Interprets and recognizes images (faces, reading)
🔹 5. Primary Auditory Cortex
- Location: Superior temporal gyrus
- Function: Detects pitch, loudness, rhythm of sound
🔹 6. Auditory Association Area
- Location: Posterior to auditory cortex
- Function: Recognizes and interprets sounds (words, music)
🔹 7. Wernicke’s Area (usually in left hemisphere)
- Location: Posterior superior temporal gyrus
- Function: Language comprehension (spoken & written)
- Damage → Wernicke’s aphasia (fluent but nonsensical speech)
🔹 8. Primary Olfactory Cortex
- Location: Temporal lobe (uncus)
- Function: Smell perception
🔹 9. Primary Gustatory Cortex
- Location: Insula and frontal operculum
- Function: Taste perception
🔹 10. Vestibular Cortex
- Location: Insula and parietal lobe
- Function: Perception of balance and spatial orientation
🧠 III. ASSOCIATION AREAS – Integrate and Process Information
🔹 1. Prefrontal Cortex
- Location: Anterior portion of frontal lobe
- Function: Higher cognitive functions:
- Judgment, reasoning, planning, personality, decision-making
- Fully matures in adulthood
🔹 2. Parietal Association Area
- Function: Spatial awareness, body image, attention
- Damage can lead to neglect syndrome
🔹 3. Temporal Association Area
- Function: Memory, recognition of language and faces
🔹 4. Occipital Association Area
- Function: Complex visual processing and object recognition
🧠 IV. Language Areas (Usually in Dominant Hemisphere)
| Area | Location | Function |
|---|---|---|
| Broca’s Area | Inferior frontal gyrus | Speech production |
| Wernicke’s Area | Superior temporal gyrus | Language comprehension |
| Angular gyrus | Parietal lobe near temporal/occipital | Reading and writing interpretation |
🧠 V. Hemispheric Specialization
- Left hemisphere: Language, logic, analytical thinking
- Right hemisphere: Creativity, spatial ability, facial recognition, music
🩺 VI. Clinical Correlation
| Area Affected | Disorder |
|---|---|
| Broca’s Area | Non-fluent (expressive) aphasia |
| Wernicke’s Area | Fluent (receptive) aphasia |
| Prefrontal Cortex | Personality change, poor judgment |
| Motor Cortex | Paralysis on opposite body side |
| Sensory Cortex | Loss of sensation on opposite side |
| Visual Cortex | Blindness or visual field loss |
| Auditory Cortex | Impaired sound perception |
| Parietal Lobe | Spatial neglect (especially right side damage) |
🧠 VENTRICULAR SYSTEM – FORMATION & STRUCTURE
📌 Introduction
The ventricular system is a network of interconnected, fluid-filled cavities within the brain. It is lined by ependymal cells and filled with cerebrospinal fluid (CSF), which cushions and nourishes the central nervous system.
The ventricular system develops from the neural tube during embryogenesis and plays a critical role in CSF production, circulation, and absorption.
🧬 I. Embryological Formation
- Originates from the central canal of the neural tube
- As the brain develops, the lumen (central canal) enlarges and forms the ventricles
- Different parts of the neural tube give rise to different ventricles:
- Telencephalon → Lateral ventricles
- Diencephalon → Third ventricle
- Mesencephalon → Cerebral aqueduct
- Metencephalon & Myelencephalon → Fourth ventricle
- Central canal continues into the spinal cord
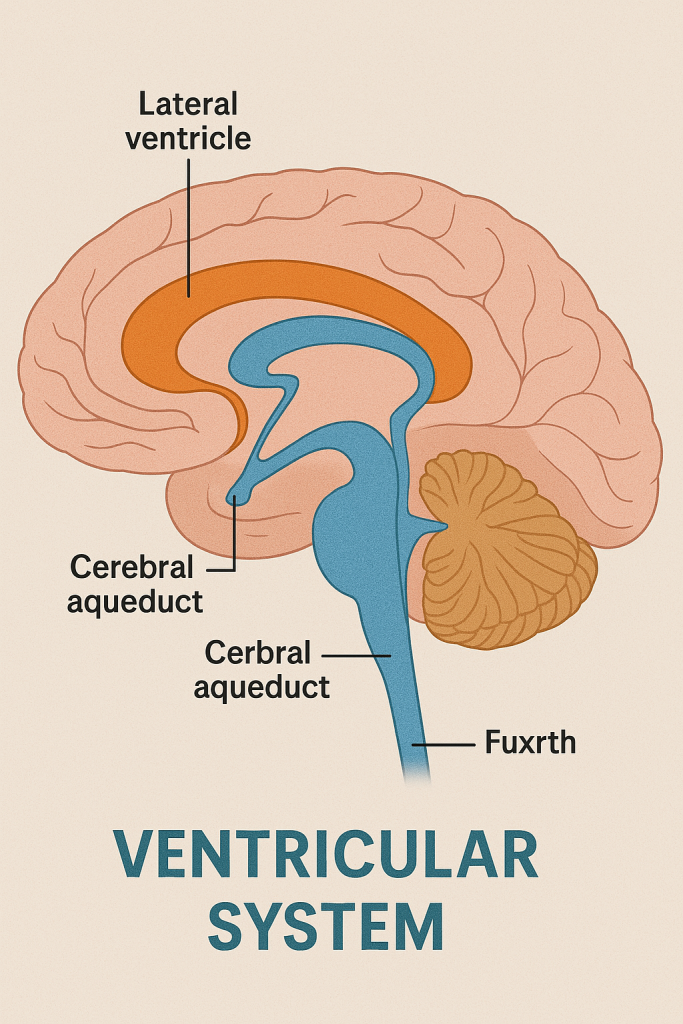
🧠 II. Structure of the Ventricular System
There are four major ventricles and associated channels:
🔹 1. Lateral Ventricles (Right and Left)
- Located within the cerebral hemispheres
- Each has anterior (frontal), posterior (occipital), inferior (temporal) horns, and a body
- Connected to the third ventricle via the interventricular foramina (of Monro)
🔹 2. Third Ventricle
- A narrow, slit-like cavity located in the diencephalon, between the right and left thalamus
- Communicates:
- Anteriorly with the lateral ventricles (via foramina of Monro)
- Posteriorly with the fourth ventricle via the cerebral aqueduct (aqueduct of Sylvius)
🔹 3. Cerebral Aqueduct
- A slender canal in the midbrain
- Connects the third ventricle to the fourth ventricle
- Common site for obstruction → hydrocephalus
🔹 4. Fourth Ventricle
- Located between the pons and medulla (anterior) and the cerebellum (posterior)
- Has three openings for CSF to exit into the subarachnoid space:
- 2 Lateral apertures (foramina of Luschka)
- 1 Median aperture (foramen of Magendie)
- Continues downward as the central canal of the spinal cord
💧 III. Cerebrospinal Fluid (CSF)
🔹 Production:
- CSF is primarily produced by the choroid plexus found in:
- Lateral ventricles
- Third ventricle
- Fourth ventricle
- Volume: ~150 mL in adults
- Daily production: ~500 mL (continuous turnover)
🔹 Circulation of CSF:
- Lateral ventricles
- → Interventricular foramina (of Monro)
- → Third ventricle
- → Cerebral aqueduct
- → Fourth ventricle
- → Subarachnoid space (via Luschka and Magendie foramina)
- → Cerebral and spinal subarachnoid space
- → Arachnoid granulations (villi)
- → Drained into dural venous sinuses, especially the superior sagittal sinus
🧠 IV. Functions of the Ventricular System and CSF
- Protects the brain and spinal cord from trauma (acts as a cushion)
- Maintains chemical stability
- Removes waste products from the brain
- Provides buoyancy – reduces brain weight by ~95%
- Aids in intracranial pressure regulation
🩺 V. Clinical Relevance
✨ Disorders Related to Ventricular System:
| Condition | Description |
|---|---|
| Hydrocephalus | Accumulation of CSF due to obstruction or impaired absorption (can be congenital or acquired) |
| Obstructive (Non-communicating) Hydrocephalus | Blockage within ventricular system (e.g., aqueductal stenosis) |
| Communicating Hydrocephalus | Impaired CSF reabsorption (e.g., due to meningitis, subarachnoid hemorrhage) |
| Normal Pressure Hydrocephalus (NPH) | Ventricular enlargement with normal CSF pressure (classic triad: gait disturbance, dementia, urinary incontinence) |
| Intraventricular Hemorrhage | Bleeding into ventricles, common in premature infants |
| Colloid Cyst of Foramen of Monro | Can obstruct CSF flow and cause sudden hydrocephalus |
🩺 Nursing & Medical Interventions:
- Ventriculoperitoneal (VP) shunt – used to drain excess CSF
- Monitoring of intracranial pressure (ICP)
- Support during lumbar puncture
- Observing for signs of increased ICP: headache, vomiting, altered consciousness, papilledema
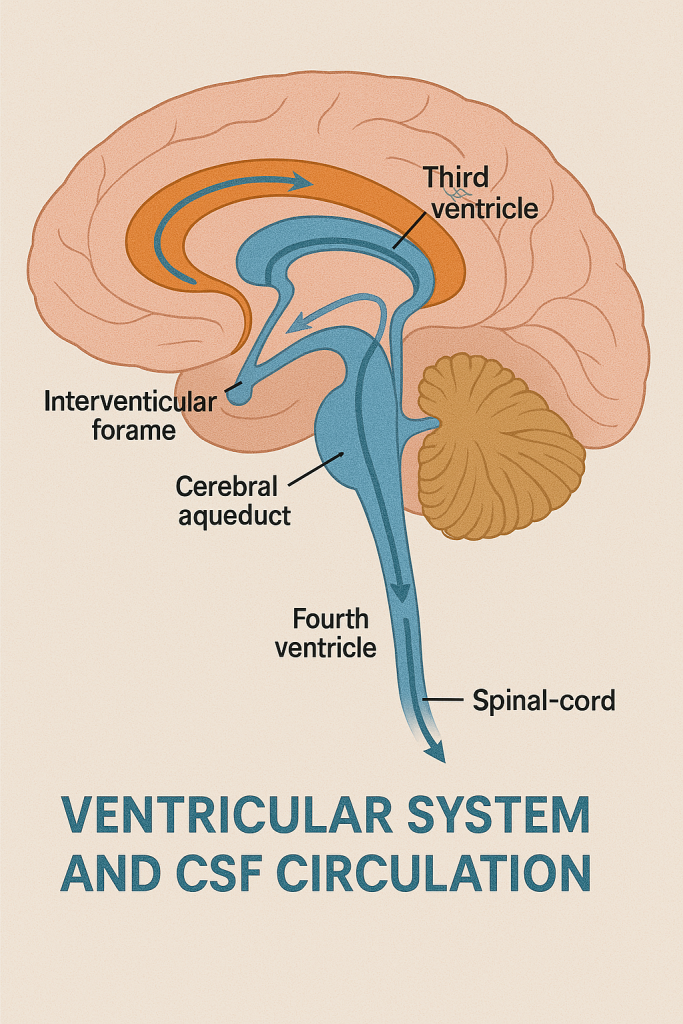
💧 VENTRICULAR SYSTEM – CIRCULATION OF CEREBROSPINAL FLUID (CSF)
📌 Introduction
The ventricular system is a series of connected, fluid-filled cavities in the brain through which cerebrospinal fluid (CSF) flows. This fluid is essential for protecting the brain and spinal cord, regulating pressure, and removing metabolic waste.
CSF is produced continuously, circulates through the ventricles, enters the subarachnoid space, and is eventually reabsorbed into the venous blood.
🧬 I. CSF Production
- CSF is produced mainly by the choroid plexus, a specialized vascular structure located within:
- Lateral ventricles
- Third ventricle
- Fourth ventricle
- Daily production: ~500 mL/day
- Total volume in adults: ~150 mL
- CSF is clear, colorless, and contains:
- Glucose, proteins, electrolytes, very few cells
🔄 II. Step-by-Step CSF Circulation Pathway
🔹 1. Lateral Ventricles (Right and Left)
- Located in each cerebral hemisphere
- CSF is first produced here by the choroid plexus
🔹 2. Interventricular Foramina (Foramina of Monro)
- Narrow channels connecting the lateral ventricles to the third ventricle
🔹 3. Third Ventricle
- Located in the diencephalon (between the thalamus and hypothalamus)
- More CSF is added here from its own choroid plexus
🔹 4. Cerebral Aqueduct (Aqueduct of Sylvius)
- A narrow passage through the midbrain
- Connects the third ventricle to the fourth ventricle
🧠 Common site of blockage in hydrocephalus
🔹 5. Fourth Ventricle
- Located between the pons and medulla anteriorly and cerebellum posteriorly
- CSF from the fourth ventricle can exit into the subarachnoid space via:
- Median aperture (Foramen of Magendie)
- Two lateral apertures (Foramina of Luschka)
🔹 6. Subarachnoid Space
- Surrounds the brain and spinal cord
- CSF flows upward around the brain and downward around the spinal cord
- Acts as a shock absorber, and provides nutrients & waste removal
🔹 7. Arachnoid Villi (Granulations)
- Finger-like projections of arachnoid membrane into the dural venous sinuses, especially the superior sagittal sinus
- CSF is absorbed into the bloodstream here, maintaining fluid balance
📈 III. Diagrammatic Summary of CSF Flow
Choroid Plexus → Lateral Ventricles
↓
Interventricular Foramina(Monro)
↓
Third Ventricle
↓
Cerebral Aqueduct (Sylvius)
↓
Fourth Ventricle
↙ ↓ ↘
Lateral Apertures (Luschka)
Median Aperture (Magendie)
↓
Subarachnoid Space(Brain & Spinal Cord)
↓
Arachnoid Villi →Dural Venous Sinuses(e.g., Superior Sagittal Sinus)
↓
Venous Circulation
🧠 IV. Functions of CSF Circulation
- Protects CNS from trauma (cushion effect)
- Maintains chemical stability of the environment
- Facilitates waste removal
- Provides buoyancy (reduces effective weight of the brain)
- Distributes neuroendocrine signals
🩺 V. Clinical Relevance
| Condition | Cause | Impact |
|---|---|---|
| Hydrocephalus | Obstructed CSF flow or poor absorption | Increased intracranial pressure |
| Aqueductal Stenosis | Blockage of cerebral aqueduct | Non-communicating hydrocephalus |
| Meningitis | Inflammation of meninges | Impaired CSF absorption |
| Subarachnoid Hemorrhage | Blood in subarachnoid space | Blocks CSF absorption |
| Lumbar Puncture (LP) | CSF collection from lower spine | Used for diagnostic or therapeutic purposes |
🩺 Nursing Role:
- Monitor signs of increased intracranial pressure (ICP): headache, vomiting, drowsiness
- Assist in CSF collection and care post-lumbar puncture
- Care for patients with VP shunts (ventriculoperitoneal) to drain excess CSF
- Observe neurological status closely in brain injury or infection
🧠 VENTRICULAR SYSTEM – DRAINAGE OF CEREBROSPINAL FLUID (CSF)
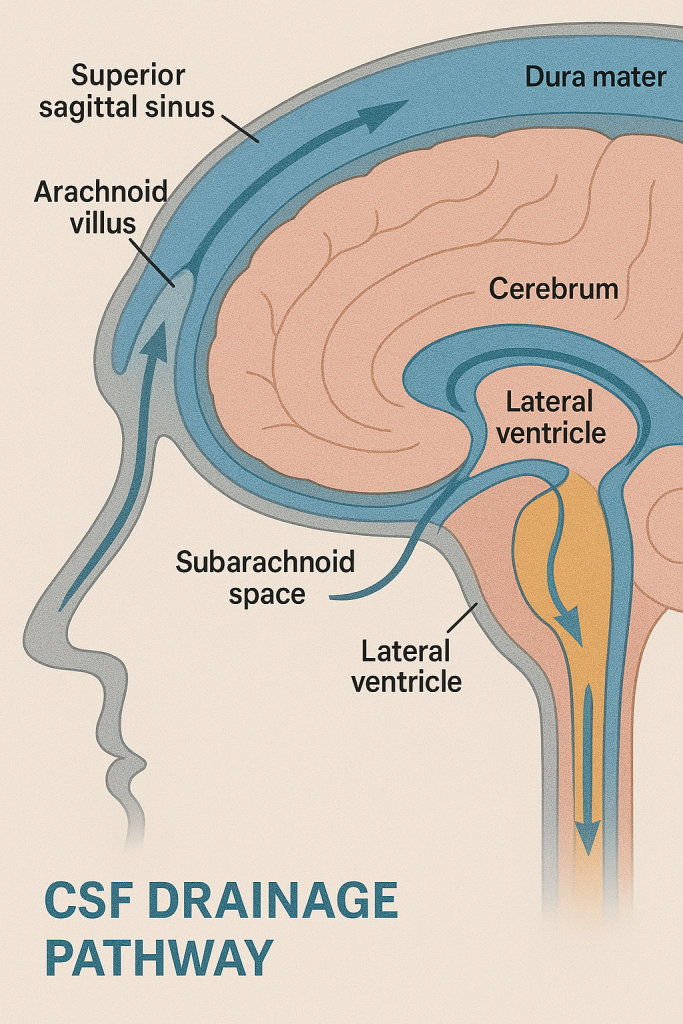
📌 Overview
After CSF is produced in the ventricles, it must be drained from the ventricular system into the venous circulation to maintain intracranial pressure (ICP) and fluid balance. This drainage occurs through specialized pathways, involving the ventricular system, subarachnoid space, and arachnoid granulations.
💧 I. Pathway of CSF Drainage from the Ventricular System
🔹 1. CSF Formation
- Produced mainly by the choroid plexus in:
- Lateral ventricles
- Third ventricle
- Fourth ventricle
🔹 2. Ventricular Circulation
- CSF flows from:
- Lateral ventricles
- → Interventricular foramina (of Monro)
- → Third ventricle
- → Cerebral aqueduct (of Sylvius)
- → Fourth ventricle
🔹 3. Exit from the Fourth Ventricle
CSF leaves the ventricular system and enters the subarachnoid space through:
- One median aperture (Foramen of Magendie) – drains CSF into the cisterna magna
- Two lateral apertures (Foramina of Luschka) – drain CSF into the pontine cistern
These apertures are key exit points for CSF to reach the brain’s surface and the spinal cord.
🌊 II. Circulation in the Subarachnoid Space
- Once in the subarachnoid space, CSF circulates freely around:
- The brain (in cisterns like cisterna magna and ambient cistern)
- The spinal cord (through the spinal subarachnoid space)
- CSF also flows upward and over the cerebral hemispheres, especially into the superior sagittal sinus region, preparing for reabsorption.
🧬 III. CSF Drainage and Absorption into Venous Blood
🔹 1. Arachnoid Villi (Granulations)
- Tiny, finger-like projections of arachnoid mater
- Extend into dural venous sinuses, especially the superior sagittal sinus
- Function as one-way valves:
- Allow CSF to flow into venous blood
- Prevent backflow of blood into CSF
These structures regulate CSF pressure and volume, ensuring drainage keeps pace with production.
🔹 2. Dural Venous Sinuses
- Venous channels between layers of dura mater
- Main ones involved in CSF drainage:
- Superior sagittal sinus
- Transverse sinus
- Straight sinus
🔹 3. Final Drainage into Circulation
- From venous sinuses → internal jugular veins → systemic circulation
🧠 IV. Regulation of CSF Drainage
- Normal CSF pressure: 10–20 cm H₂O (when lying)
- Arachnoid granulations open in response to pressure:
- CSF drains when intracranial pressure exceeds venous pressure
- Balance of production and absorption is critical:
- Increased production or impaired absorption → hydrocephalus
⚠️ V. Clinical Significance of CSF Drainage
| Condition | Cause | Impact |
|---|---|---|
| Communicating Hydrocephalus | Impaired absorption by arachnoid villi (e.g., meningitis, hemorrhage) | Ventricles enlarge; pressure may rise |
| Non-communicating Hydrocephalus | Obstruction within ventricles (e.g., aqueductal stenosis, tumor) | CSF can’t reach subarachnoid space |
| Normal Pressure Hydrocephalus (NPH) | Poor drainage despite normal CSF pressure | Gait disturbance, dementia, urinary incontinence |
| Pseudotumor Cerebri | Increased ICP with normal imaging | Often in obese women, can cause vision loss |
🩺 Nursing & Medical Roles:
- Monitor for signs of increased ICP:
- Headache, nausea, vomiting, altered consciousness
- Support neuroimaging (CT/MRI) for hydrocephalus
- Care for patients with:
- CSF shunts (e.g., ventriculoperitoneal – VP shunt)
- External ventricular drains (EVD)
- Assist with lumbar puncture to assess pressure or drain excess CSF
🧠 THE NERVOUS SYSTEM – APPLICATION AND IMPLICATION IN NURSING
The nervous system is the body’s command and control system, responsible for sensation, movement, coordination, cognition, and autonomic regulation. As nurses, a solid understanding of the structure and function of the nervous system is essential for:
- Accurate patient assessment
- Early identification of neurological changes
- Safe administration of medications
- Providing effective care for neurological disorders
🧠 I. Relevance of the Nervous System in Nursing Practice
🔹 1. Assessment of Neurological Function
Nurses routinely perform neurological assessments to detect changes in brain, spinal cord, or peripheral nerve function.
Key Components:
- Level of consciousness (LOC) – using tools like Glasgow Coma Scale (GCS)
- Pupil reaction – size, symmetry, light response (CN II & III)
- Motor strength – hand grips, limb movement
- Sensory function – touch, pain, temperature
- Speech and cognition – clarity, orientation, memory
- Reflexes – deep tendon reflexes, Babinski’s sign
🔍 Implication: Early detection of conditions like stroke, increased intracranial pressure, spinal cord injury, or infections such as meningitis.
🔹 2. Monitoring and Managing Neurological Disorders
Nurses care for patients with various neurological conditions, including:
- Stroke (CVA)
- Seizures/Epilepsy
- Parkinson’s Disease
- Multiple Sclerosis
- Spinal cord injury
- Peripheral neuropathy
- Meningitis/Encephalitis
Nursing Responsibilities:
- Regular neuro-vital signs monitoring
- Fall precautions and seizure safety
- Bowel and bladder care in spinal cord injuries
- Mobility support, passive ROM exercises
- Skin care to prevent pressure ulcers in immobile patients
🔹 3. Pain Management
The nervous system plays a central role in pain transmission and perception.
Nursing Actions:
- Pain assessment using standardized scales (e.g., Numeric, Wong-Baker)
- Non-pharmacological interventions: heat/cold, positioning, relaxation
- Medication administration:
- Analgesics (NSAIDs, opioids)
- Anticonvulsants (e.g., gabapentin for neuropathic pain)
🧠 Understanding neurological pain pathways helps in choosing effective interventions.
🔹 4. Administration of Neurological Medications
Many drugs act on the nervous system. Nurses must understand drug actions, side effects, and monitoring needs.
Common Classes:
- Antiepileptics (e.g., phenytoin, levetiracetam)
- Antiparkinsonian drugs (e.g., levodopa-carbidopa)
- CNS depressants (e.g., benzodiazepines)
- CNS stimulants
- Anesthetics
- Antidepressants & antipsychotics
❗ Nurses must watch for sedation, confusion, respiratory depression, altered mental status.
🔹 5. Patient and Family Education
Educating patients with neurological disorders is key to self-care, adherence, and safety.
Key Topics:
- Medication usage and side effects
- Signs of worsening condition (e.g., stroke symptoms: FAST)
- Seizure precautions
- Strategies for memory or speech problems
- Need for rehabilitation therapy
🔹 6. Care of Unconscious or Brain-Injured Patients
In ICU or emergency settings, nurses manage patients with traumatic brain injury, coma, or stroke.
Interventions:
- Airway management and suctioning
- Monitoring ICP (if equipment available)
- Eye care, oral hygiene, pressure injury prevention
- Nutrition via NG tube or parenteral route
- Emotional support for families facing poor prognosis
🔹 7. Autonomic Nervous System Monitoring
The ANS controls heart rate, BP, temperature, and digestion.
In Critical Situations:
- Neurogenic shock after spinal injury → bradycardia, hypotension
- Dysautonomia in diseases like Parkinson’s
- Bladder/bowel dysfunction in spinal cord injuries
Nurses must monitor vitals closely, ensure bowel/bladder care, and avoid autonomic dysreflexia.
📈 II. Nursing Applications Based on Nervous System Divisions
| Nervous System Division | Nursing Application |
|---|---|
| Central Nervous System (CNS) | Neurological exams, seizure care, stroke management |
| Peripheral Nervous System (PNS) | Managing peripheral neuropathy, nerve compression, reflex testing |
| Autonomic Nervous System (ANS) | Monitoring vital signs, temperature regulation, bowel/bladder function |
| Somatic Nervous System | Muscle tone and movement assessment, rehab planning |
🧠 III. Summary of Nursing Implications
| Key Area | Nursing Implication |
|---|---|
| LOC Changes | Neurological emergency – report immediately |
| Pupil Changes | Monitor for brain herniation or injury |
| Motor/Sensory Loss | Repositioning, fall risk, rehab support |
| Seizures | Safety, medication, suction, airway |
| Pain | Assessment, appropriate interventions |
| Autonomic Signs | BP, HR, bladder – monitor & manage |
| Communication Issues | Use boards, gestures, speech therapy |
| Emotional Effects | Offer support, listen empathetically |