Anatomy B.sc-Unit-6-The Sensory organs
🧴🧬 Structure of the Skin – The Body’s Protective Barrier
The skin is the largest organ of the human body. It covers the entire body and performs multiple essential functions including protection, sensation, temperature regulation, and immune defense. Structurally, the skin is composed of three main layers: epidermis, dermis, and hypodermis (subcutaneous tissue).
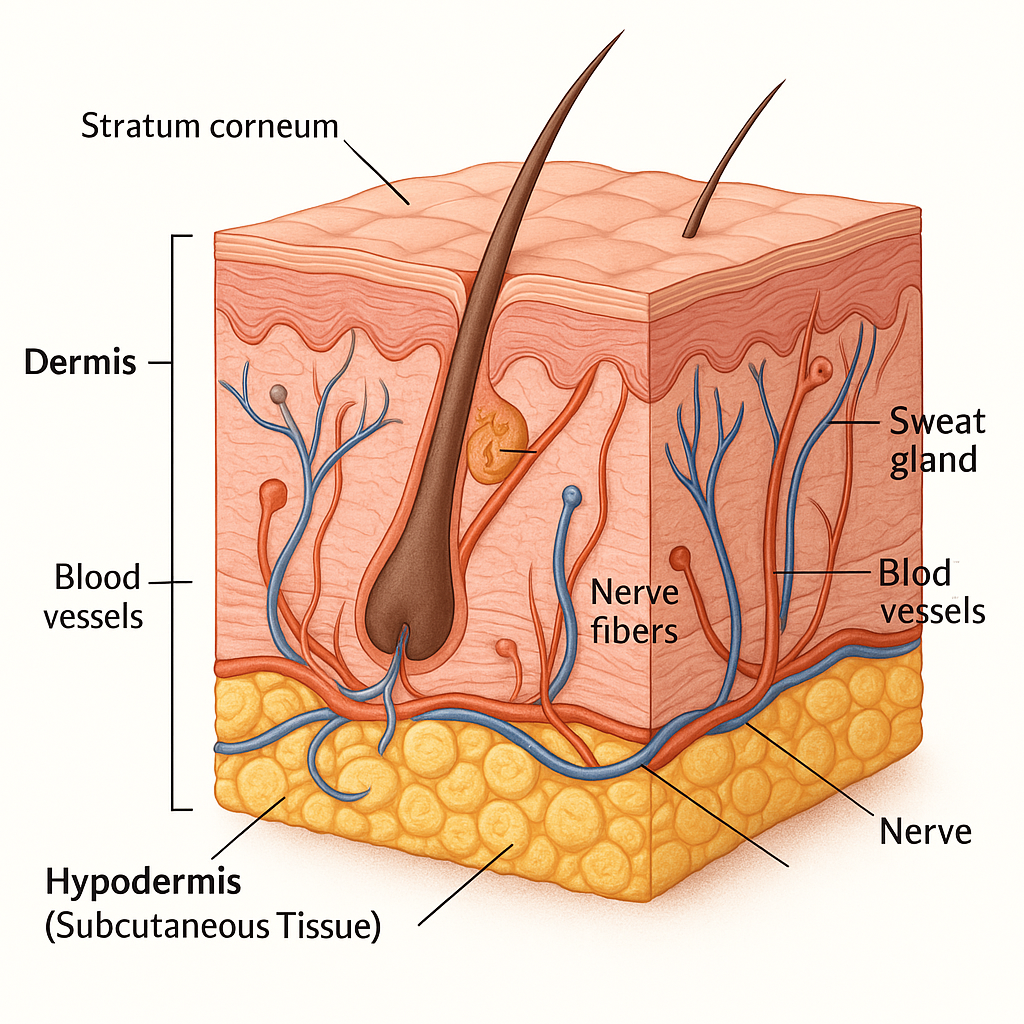
📍 1. Epidermis – The Outer Protective Layer
The epidermis is the superficial, avascular layer made of stratified squamous keratinized epithelium. It provides a barrier against environmental hazards like pathogens, UV radiation, and dehydration.
🧬 Layers of the Epidermis (from deep to superficial):
Remember: “Come Let’s Get Sun Burned”
- Stratum basale (basal layer)
- Deepest layer; single row of stem cells
- Contains melanocytes, keratinocytes, and Merkel cells
- Site of cell division (mitosis)
- Stratum spinosum
- Several layers of keratinocytes
- Contains Langerhans cells (immune function)
- Cells connected by desmosomes
- Stratum granulosum
- 3–5 cell layers with keratohyalin granules
- Cells begin to die and become flat
- Stratum lucidum
- Thin, transparent layer
- Present only in thick skin (palms, soles)
- Stratum corneum
- Outermost layer of dead keratinized cells
- Continuously shed and replaced
- Forms a protective barrier
🧠 Special Cells in the Epidermis
- Keratinocytes: Main cells, produce keratin (waterproof protein)
- Melanocytes: Produce melanin, which gives skin color and protects against UV radiation
- Langerhans cells: Antigen-presenting immune cells
- Merkel cells: Touch-sensitive mechanoreceptors
🧵 2. Dermis – The Strength and Support Layer
The dermis lies beneath the epidermis and is vascularized, thicker, and made of connective tissue, collagen, and elastic fibers. It supports the epidermis and houses sensory structures, blood vessels, and appendages like hair follicles and glands.
🔹 Two Layers of Dermis:
A. Papillary layer (superficial)
- Loose connective tissue
- Contains capillaries, nerve endings, Meissner’s corpuscles (light touch)
- Forms dermal papillae, which interlock with epidermis (fingerprints)
B. Reticular layer (deep)
- Dense irregular connective tissue
- Contains hair follicles, sebaceous (oil) glands, sweat glands, blood vessels, Pacinian corpuscles (pressure), arrector pili muscles
🌡️ 3. Hypodermis (Subcutaneous Tissue) – The Insulating Layer
- Deepest layer of the skin
- Composed of loose connective tissue and adipose tissue
- Functions:
- Provides insulation and shock absorption
- Stores energy (fat)
- Anchors skin to underlying muscles and organs
- Contains large blood vessels and nerves
🌟 Functions of the Skin
- Protection – Against UV rays, microbes, chemicals, and physical trauma
- Sensation – Touch, pressure, pain, temperature via sensory receptors
- Thermoregulation – Sweat production, blood vessel dilation/constriction
- Vitamin D synthesis – In response to UV radiation
- Immune defense – Langerhans cells and intact barrier
- Excretion – Sweat glands eliminate salts, urea, and waste
- Absorption – Lipid-soluble substances (e.g., topical medications)
🩺 Clinical Relevance
- Burn classification:
- 1st-degree: Epidermis only
- 2nd-degree: Epidermis + part of dermis
- 3rd-degree: Full-thickness (epidermis + dermis + possibly hypodermis)
- Skin disorders: Psoriasis, eczema, dermatitis, skin cancers
- Pressure ulcers: Occur due to prolonged pressure affecting blood supply to dermis/hypodermis
- Injections:
- Intradermal: Into dermis (e.g., Mantoux test)
- Subcutaneous: Into hypodermis (e.g., insulin, heparin)
🧠 Quick Recap Mnemonic:
“Every Dog Has Super Skin”
→ Epidermis – Dermis – Hypodermis – Sensation – Sweat
👁️🧠 Anatomy of the Human Eye – The Organ of Sight
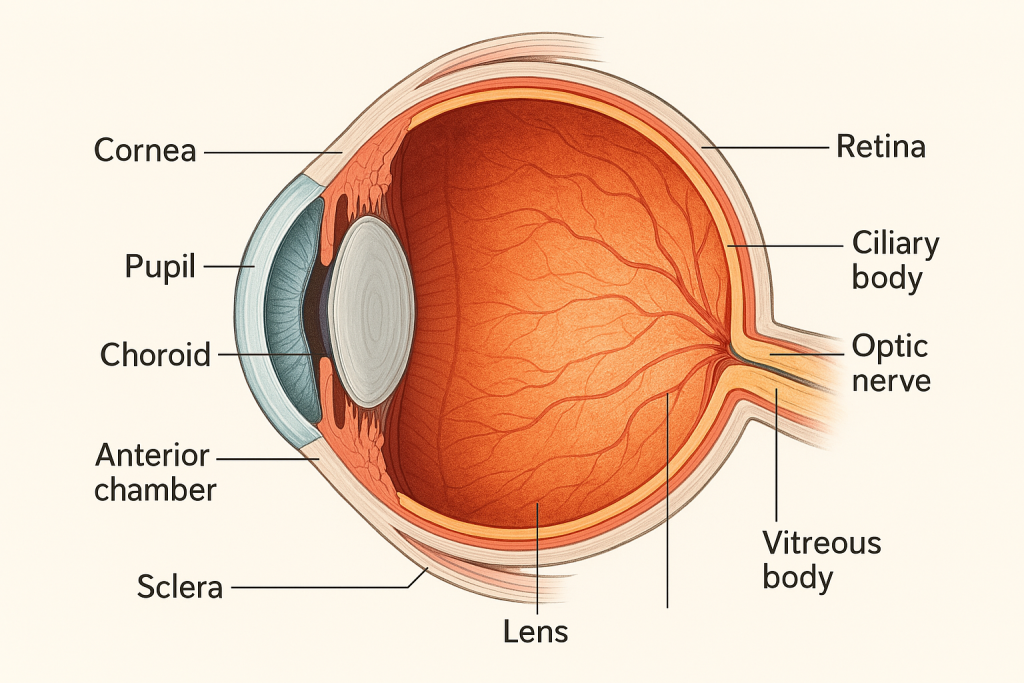
The human eye is a complex, spherical sensory organ that captures light and transforms it into electrical signals that are interpreted by the brain as vision. It is a precise optical system and a part of the nervous system, protected and supported by accessory structures.
📍 Location and General Description
- Situated in the bony orbit of the skull
- Maintained in position by six extraocular muscles, fatty tissue, and connective support
- Approximately 2.5 cm in diameter
- Weight: ~7.5 grams
🧱👁️ 1. Fibrous Tunic (Outer Layer of the Eye)
The fibrous tunic is the outermost protective layer of the eyeball. It provides shape, support, and mechanical protection, and serves as an attachment site for extraocular muscles. This layer is avascular (contains no blood vessels) and is made up of dense connective tissue.
It has two main parts:
🔹 A. Sclera – “The White of the Eye”
📍 Location & Structure
- Forms the posterior 5/6 of the outer layer
- Thick, opaque, white tissue
- Composed of collagen and elastic fibers
🔧 Functions
- Maintains the shape of the eyeball (important for proper vision)
- Acts as a protective outer shell
- Provides attachment for 6 extraocular muscles that move the eye
- Helps resist internal pressure from fluids
🧠 Features
- Covered externally by episclera (a thin vascular connective tissue)
- Internally lined by suprachoroid lamina, in contact with the choroid
- Pierced posteriorly by the optic nerve
🩺 Clinical Note
- Scleritis: Inflammation of the sclera, often painful and associated with autoimmune disease
- Blue sclera: Seen in conditions like osteogenesis imperfecta
🔸 B. Cornea – “The Clear Window of the Eye”
📍 Location & Structure
- Forms the anterior 1/6 of the fibrous tunic
- Transparent, dome-shaped structure
- Composed of five microscopic layers:
- Epithelium (outermost) – protective barrier
- Bowman’s layer
- Stroma – makes up ~90% of corneal thickness
- Descemet’s membrane
- Endothelium (innermost) – pumps out excess fluid
💧 Avascular but Rich in Nerve Endings
- Nourished by diffusion from:
- Aqueous humor
- Tear film
- Capillaries at the limbus (cornea-sclera junction)
🔧 Functions
- Main refractive surface of the eye (bends light toward the retina)
- Provides a smooth, clear surface for light to pass through
- Protects the inner eye from dust, germs, and injury
🧠 Features
- Highly sensitive to pain and touch
- Transparent due to its nonvascularity and regular arrangement of collagen fibers
🩺 Clinical Note
- Corneal abrasion: Scratch on the surface epithelium – painful, heals quickly
- Keratitis: Inflammation of the cornea
- Corneal ulcer: Infection leading to tissue damage
- LASIK surgery: Reshapes the cornea to correct refractive errors
📍 Junction Between Sclera and Cornea: The Limbus
- Also called the corneoscleral junction
- Important site for aqueous humor drainage
- Contains the Canal of Schlemm, which plays a role in intraocular pressure regulation
🧠 Summary – Fibrous Tunic at a Glance
| Part | Coverage | Function | Special Features |
|---|---|---|---|
| Sclera | Posterior 5/6 | Shape, protection, muscle anchor | White, opaque, tough connective tissue |
| Cornea | Anterior 1/6 | Refraction, barrier function | Transparent, highly innervated, no blood vessels |
🩸👁️ 2. Vascular Tunic (Middle Layer / Uvea)
The vascular tunic, also known as the uvea, is the middle layer of the eyeball. It is rich in blood vessels and pigment, providing nutrients, oxygen, and light absorption for the inner layers of the eye.
This layer lies between the fibrous tunic (sclera and cornea) and the inner nervous tunic (retina), and it is composed of three continuous parts:
🔸 A. Choroid – The Nourishing Layer
📍 Location
- Lies between the sclera and retina
- Extends from the optic disc at the back to the ciliary body in the front
🔬 Structure
- Darkly pigmented, vascular membrane
- Contains melanocytes, loose connective tissue, and many capillaries
- Has four layers microscopically, including Bruch’s membrane (next to the retina)
⚙️ Functions
- Supplies oxygen and nutrients to the outer layers of the retina (esp. photoreceptors)
- The melanin pigment absorbs stray light to prevent internal light reflection and glare
- Assists in thermoregulation of the retina
🩺 Clinical Relevance:
- Choroiditis: Inflammation, often part of uveitis
- Choroidal neovascularization: Seen in age-related macular degeneration
🟡 B. Ciliary Body – The Focus Controller & Fluid Producer
📍 Location
- Extends from the choroid to the base of the iris
- Forms a ring around the lens
🔬 Structure
- Composed of:
- Ciliary muscle: smooth muscle
- Ciliary processes: finger-like projections
- Suspensory ligaments (zonular fibers): connect to the lens
⚙️ Functions
- Accommodation:
- Ciliary muscle contracts → lens becomes thicker → focuses on near objects
- Ciliary muscle relaxes → lens flattens → focuses on distant objects
- Aqueous Humor Production:
- Ciliary processes secrete aqueous humor into the posterior chamber
- Maintains intraocular pressure and nourishes avascular structures like the lens and cornea
🩺 Clinical Relevance:
- Cyclitis: Inflammation of the ciliary body
- Glaucoma: Overproduction or blocked drainage of aqueous humor increases pressure
- Presbyopia: Age-related loss of ciliary muscle elasticity → difficulty focusing on near objects
🔵 C. Iris – The Light Regulator (Colored Part of the Eye)
📍 Location
- Lies in front of the lens and behind the cornea
- Forms a flat, ring-shaped structure with a central opening (the pupil)
🔬 Structure
- Composed of pigmented cells, blood vessels, and two sets of smooth muscles:
- Sphincter pupillae (circular): constricts pupil (parasympathetic control)
- Dilator pupillae (radial): dilates pupil (sympathetic control)
- The color of the iris depends on the amount and type of melanin:
- High melanin = brown eyes
- Low melanin = blue/green eyes
⚙️ Functions
- Regulates the diameter of the pupil and thus the amount of light entering the eye
- Protects retina from excessive light
- Helps enhance contrast and visual sharpness
🩺 Clinical Relevance:
- Iritis: Inflammation, often painful and light-sensitive
- Anisocoria: Unequal pupil sizes – may indicate neurological problem
- Mydriasis: Pupil dilation (e.g., from drugs or trauma)
- Miosis: Pupil constriction (e.g., opioid effect)
📌 Uvea Summary Table
| Part | Location | Main Function |
|---|---|---|
| Choroid | Between sclera and retina | Nourishes outer retina; light absorption |
| Ciliary Body | Ring between choroid and iris | Accommodation; aqueous humor secretion |
| Iris | Front of eye, around pupil | Controls pupil size and light entry |
🧠 Mnemonic to Remember Uvea Parts:
🔹 “CIC” – Choroid, Iris, Ciliary body
Or
🔹 “I See Clearly” → Iris, Sclera (connects), Ciliary body
👁️🧠 3. Nervous Tunic (Inner Layer of the Eye) – The Retina
The nervous tunic, also known as the retina, is the innermost and most crucial layer of the eyeball, responsible for receiving visual images and transmitting them to the brain. It contains specialized photoreceptor cells that convert light energy into electrical impulses, which are carried by the optic nerve to the visual cortex.
📍 Location & General Features
- Lies between the choroid (middle layer) and the vitreous body
- It is attached firmly at two points:
- Optic disc (where the optic nerve exits)
- Ora serrata (anterior edge of the retina)
- Thin, delicate, transparent neural tissue
🔬 Microscopic Layers of the Retina
The retina consists of 10 distinct layers, but they can be functionally grouped into three major layers:
🔹 1. Photoreceptor Layer
- Contains two types of light-sensitive cells:
- Rods – ~120 million, for dim light (night vision) and peripheral vision
- Cones – ~6 million, for color vision, fine detail, and daylight (bright light)
- Rods are concentrated in the periphery
- Cones are concentrated in the fovea centralis
🔹 2. Bipolar Cell Layer
- Transmits signals from photoreceptors to ganglion cells
- Acts as a relay center in the retinal pathway
🔹 3. Ganglion Cell Layer
- Axons from these cells bundle together to form the optic nerve (CN II)
- These carry visual signals to the brain’s occipital lobe
🧱 Other Supporting Cells in Retina:
- Horizontal cells: Integrate signals between photoreceptors
- Amacrine cells: Modify signals between bipolar and ganglion cells
- Müller cells: Provide structural and metabolic support
🌟 Specialized Areas of the Retina
🔸 A. Macula Lutea
- Small, yellowish central area of retina
- Responsible for sharp central vision
- Rich in cones
🔸 B. Fovea Centralis
- Center of the macula
- Contains only cones, no rods
- Area of maximum visual acuity
🔸 C. Optic Disc (Blind Spot)
- Point where optic nerve exits the eye
- No photoreceptors present → insensitive to light
- Appears pale on fundus examination
💧 Retinal Pigmented Epithelium (RPE)
- Lies just outside the photoreceptor layer
- Absorbs stray light to enhance image clarity
- Helps in nutrient transport, waste removal, and photoreceptor maintenance
🧠 Function of the Retina
- Phototransduction: Converts light into electrical impulses
- Signals pass through:
- Photoreceptors (rods & cones)
- Bipolar cells
- Ganglion cells
- Optic nerve
- Brain (visual cortex in occipital lobe)
🩺 Clinical Relevance
| Condition | Involvement |
|---|---|
| Retinal detachment | Separation of retina from choroid |
| Diabetic retinopathy | Damage to retinal blood vessels |
| Macular degeneration | Degeneration of the fovea |
| Retinitis pigmentosa | Genetic loss of photoreceptors |
| Glaucoma | Ganglion cell death due to pressure |
| Papilledema | Swelling of optic disc due to ↑ ICP |
✅
- Retina = inner sensory layer of the eye
- Contains rods (night vision) and cones (color vision)
- Key areas: macula, fovea, optic disc
- Converts light into neural signals → sent to optic nerve → brain
👁️✨ Internal Structures of the Eye – The Optical Apparatus
The internal structures of the eye work collectively to refract (bend) and focus light rays onto the retina, facilitating clear and sharp vision.
🔍 1. Lens
- A biconvex, transparent, avascular structure located behind the iris and in front of the vitreous humor
- Held in place by zonular fibers (suspensory ligaments) attached to the ciliary body
- Composed of a capsule, epithelial layer, and lens fibers (crystalline proteins)
- Capable of changing shape to focus on near or distant objects (accommodation)
🔁 Accommodation Mechanism:
- For near objects: ciliary muscles contract, tension on ligaments decreases → lens thickens
- For distant objects: ciliary muscles relax, tension increases → lens flattens
🩺 Clinical Insight:
- Cataract: Opacification of the lens causing blurred vision
- Presbyopia: Age-related stiffness of the lens → impaired near vision
🔍 2. Chambers and Fluids
📌 A. Anterior Chamber
- Space between the cornea and iris
- Filled with aqueous humor
📌 B. Posterior Chamber
- Space between the iris and lens
- Also filled with aqueous humor
📌 C. Vitreous Chamber (Vitreous Cavity)
- Located behind the lens and in front of the retina
- Filled with vitreous humor, a gel-like, transparent substance
- Maintains intraocular pressure
- Supports the retina by pressing it against the choroid
- Allows light transmission to the retina
🩺 Clinical Insight:
- Posterior vitreous detachment can lead to floaters and possible retinal tear/detachment
💧🔁 Aqueous Humor Circulation – The Intraocular Fluid System
Aqueous humor is a clear, nutrient-rich fluid secreted by the ciliary processes. It provides:
- Nourishment to avascular structures (cornea, lens)
- Maintenance of intraocular pressure (IOP)
- Removal of waste products
🔄 Flow Pathway of Aqueous Humor:
- Produced by ciliary processes (in the posterior chamber)
- Flows through the pupil into the anterior chamber
- Drains via:
- Trabecular meshwork → into Canal of Schlemm
- Then into episcleral veins
⛔ Disruption in this pathway causes raised IOP, leading to glaucoma, which can result in optic nerve damage and irreversible blindness.
🩺 Clinical Types:
- Open-angle glaucoma: gradual clogging of trabecular meshwork
- Closed-angle glaucoma: iris blocks drainage angle — acute emergency
🧴👁️ Accessory Structures of the Eye – Protection & Function Enhancers
These are external structures that protect the eyeball, aid in vision, and maintain eye health.
🟤 A. Eyelids (Palpebrae)
- Upper and lower folds of skin, lined internally by conjunctiva
- Contain orbicularis oculi (closes eye) and levator palpebrae superioris (opens upper lid)
- Protect from injury, light, dust and spread tear film
🩺 Clinical Note:
- Ptosis: drooping eyelid (e.g., CN III palsy or Horner’s syndrome)
🟣 B. Conjunctiva
- Transparent mucous membrane
- Palpebral conjunctiva: lines inner eyelids
- Bulbar conjunctiva: covers anterior sclera
- Helps lubricate the eye and provides immune protection
🩺 Clinical Note:
- Conjunctivitis (pink eye): due to infection or allergy
🔵 C. Lacrimal Apparatus
Includes:
- Lacrimal gland: located superolaterally; secretes tears (reflex, basal, emotional)
- Lacrimal ducts: distribute tears across the eye
- Lacrimal puncta → canaliculi → sac → nasolacrimal duct → drains tears into nasal cavity
💧 Tears contain: water, salts, mucus, and lysozyme (antibacterial enzyme)
🟢 D. Extraocular Muscles (6 total)
| Muscle | Movement | Nerve Supply |
|---|---|---|
| Superior rectus | Elevation | CN III (Oculomotor) |
| Inferior rectus | Depression | CN III |
| Medial rectus | Adduction (inward) | CN III |
| Lateral rectus | Abduction (outward) | CN VI (Abducens) |
| Superior oblique | Depression + Intorsion | CN IV (Trochlear) |
| Inferior oblique | Elevation + Extorsion | CN III |
🩺 Mnemonic:
“LR6 SO4, all the rest 3”
(Lateral rectus = CN 6; Superior oblique = CN 4; others = CN 3)
🔌🧠 Nerve Supply of the Eye – Vision, Sensation, and Movement
The eye is innervated by sensory, motor, and autonomic (involuntary) nerves.
🧠 A. Sensory Nerves
- Optic Nerve (CN II):
- Carries visual signals from the retina to the occipital lobe
- Formed by axons of retinal ganglion cells
- Ophthalmic Division of Trigeminal Nerve (CN V1):
- Sensory to cornea, conjunctiva, lacrimal gland, and eyelids
🧠 B. Motor Nerves (for Eye Movement)
- Oculomotor Nerve (CN III):
- Innervates 4/6 extraocular muscles + levator palpebrae + ciliary & sphincter pupillae muscles
- Trochlear Nerve (CN IV):
- Controls superior oblique
- Abducens Nerve (CN VI):
- Controls lateral rectus
🧠 C. Autonomic Nervous System (Involuntary Control)
🔸 Parasympathetic (via CN III):
- Constricts pupil (miosis) via sphincter pupillae
- Contracts ciliary muscle for near vision
🔸 Sympathetic:
- Dilates pupil (mydriasis) via dilator pupillae
- Elevates eyelid slightly via superior tarsal muscle
🩺 Clinical Correlation:
- Horner’s syndrome: Ptosis, miosis, anhidrosis (due to sympathetic disruption)
- Oculomotor palsy: Drooping eyelid, dilated pupil, eye deviates “down and out”
🧠 Final Review Chart
| System | Key Role |
|---|---|
| Internal Structures | Focus light, support retina, maintain eye shape |
| Aqueous Humor | Nourish cornea/lens, maintain pressure, drain waste |
| Accessory Structures | Protect, move, lubricate, support eye function |
| Nerve Supply | Vision, sensation, movement, autonomic responses |
👂🧠 Anatomy of the Human Ear – The Organ of Hearing and Balance
The ear serves two essential functions:
- Hearing (auditory function)
- Balance (equilibrium or vestibular function)
The ear is anatomically divided into three main regions:
✅ 1. External Ear
✅ 2. Middle Ear
✅ 3. Inner Ear
👂🔍 External Ear – Structure and Function
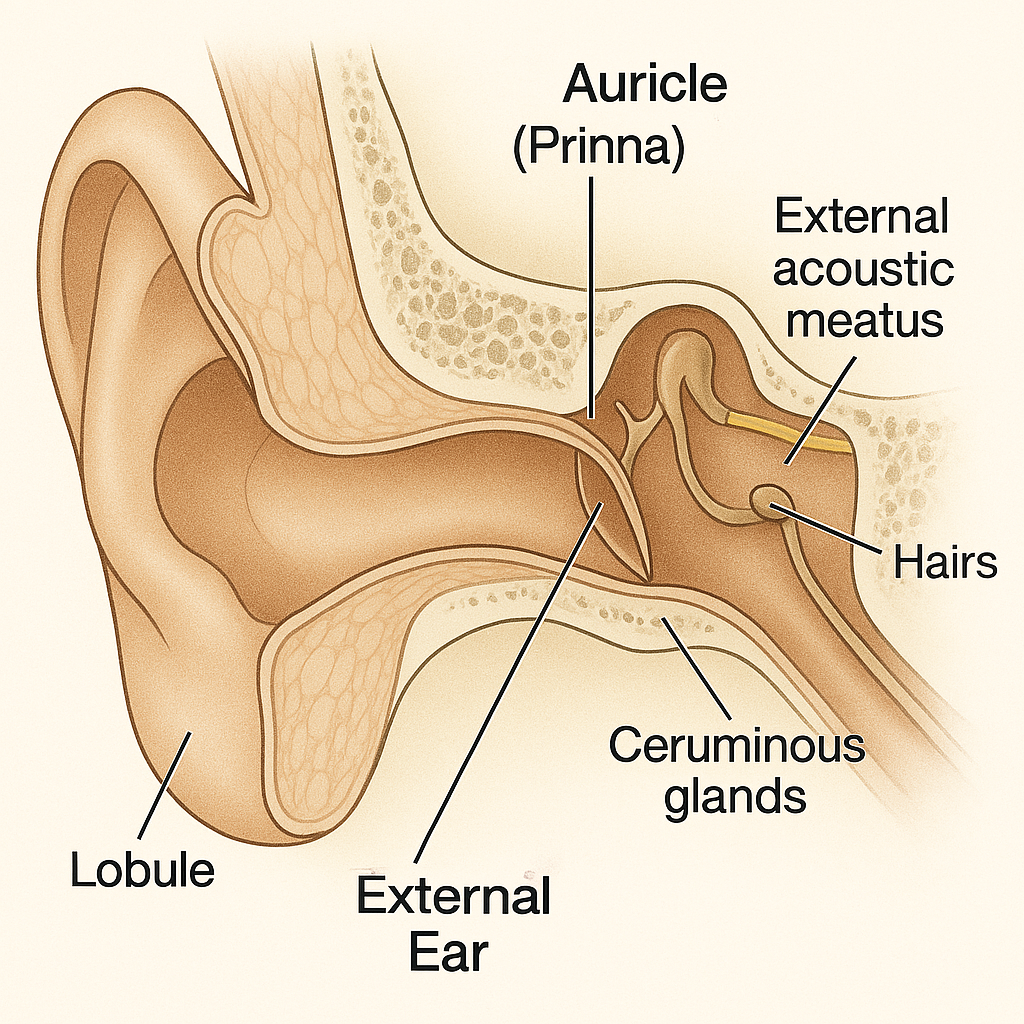
The external ear is the outermost portion of the ear that is visible externally and functions to collect and direct sound waves into the ear canal toward the tympanic membrane (eardrum).
It consists of three main components:
🔹 1. Auricle (Pinna)
📍 Structure
- A cartilaginous, funnel-shaped structure covered by skin
- Made of elastic cartilage except for the earlobe (lobule), which is soft and fatty
- Numerous grooves and ridges provide structural complexity
🧠 Parts of the Auricle:
- Helix: the outer rim
- Antihelix: a curved prominence parallel to the helix
- Tragus: small projection in front of the external auditory canal
- Antitragus: opposite the tragus, separated by intertragic notch
- Concha: deep cavity leading to the ear canal
- Lobule (earlobe): lower, soft portion with rich blood supply
🔧 Function
- Acts like a satellite dish, collecting sound waves and funneling them toward the ear canal
- Its unique shape helps to localize sound direction
🔹 2. External Auditory Canal (External Acoustic Meatus)
📍 Structure
- A slightly S-shaped tube, ~2.5 cm long
- Extends from the concha of auricle to the tympanic membrane
- Composed of:
- Outer 1/3: cartilaginous portion (lined with skin, hair follicles, and ceruminous glands)
- Inner 2/3: bony portion (within the temporal bone)
💧 Ceruminous Glands:
- Modified sweat glands that produce cerumen (earwax)
- Cerumen + hair trap dust, debris, and microbes
🔧 Function
- Conducts sound vibrations to the eardrum
- Protects deeper structures by:
- Maintaining an acidic environment (prevents microbial growth)
- Self-cleaning via migration of epithelial cells
🔹 3. Tympanic Membrane (Eardrum)
🟡 Though technically a boundary between the external and middle ear, it is often included in the external ear for anatomical teaching.
📍 Structure
- Thin, cone-shaped semi-transparent membrane
- Made up of three layers:
- Outer layer – continuous with skin of the canal
- Middle layer – fibrous connective tissue
- Inner layer – continuous with mucosa of middle ear
- It is anchored to the bony canal by the tympanic ring
🔧 Function
- Vibrates in response to incoming sound waves
- Transmits mechanical energy to malleus (ear ossicle) in the middle ear
🩺 Clinical Relevance
| Condition | Description |
|---|---|
| Otitis externa | Infection of the external ear canal (swimmer’s ear); redness, itching, pain |
| Impacted cerumen | Excessive earwax can block sound and cause hearing loss |
| Tympanic membrane perforation | Tear in the eardrum due to trauma, infection, or pressure changes (barotrauma) |
| Congenital malformations | Abnormal development of auricle or canal → may affect hearing |
🧠 Innervation (Nerve Supply)
- Auriculotemporal nerve (branch of CN V3 – mandibular nerve)
- Great auricular nerve (from cervical plexus)
- Auricular branch of the vagus nerve (Arnold’s nerve) – may cause cough reflex when cleaning ears!
🩸 Blood Supply
- Posterior auricular artery and superficial temporal artery
- Veins drain into the external jugular vein
✅ Summary
| Part | Structure | Function |
|---|---|---|
| Auricle (Pinna) | Cartilage + skin | Collects sound |
| Auditory Canal | Cartilage + bony tube | Channels sound; produces cerumen |
| Tympanic Membrane | Thin trilaminar membrane | Vibrates to transmit sound to ossicles |
🦴👂 Middle Ear (Tympanic Cavity) – Structure and Function
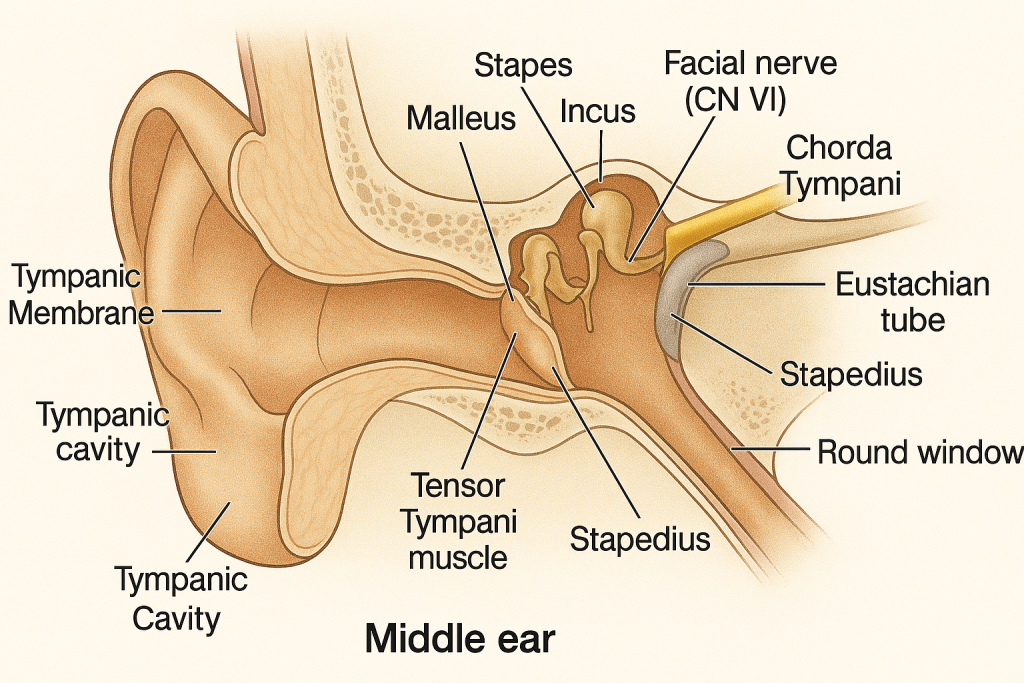
The middle ear is an air-filled cavity located within the petrous part of the temporal bone, situated between the external ear and the inner ear. It functions as a mechanical amplifier, transmitting sound vibrations from the eardrum to the inner ear.
🧱 Boundaries of the Middle Ear
The middle ear cavity is shaped like a box and has six walls:
| Wall | Location | Key Features |
|---|---|---|
| Lateral wall | Outer boundary | Formed by the tympanic membrane (eardrum) |
| Medial wall | Inner boundary | Contains oval window, round window, and promontory (overlying cochlea) |
| Anterior wall | Faces carotid artery | Opening for the Eustachian (auditory) tube |
| Posterior wall | Towards mastoid | Leads to mastoid air cells (via aditus) |
| Roof | Tegmen tympani (bony) | Separates middle ear from cranial cavity |
| Floor | Thin bone above jugular bulb | Separates ear from internal jugular vein |
🔸 Main Components of the Middle Ear
1️⃣ Tympanic Membrane (Eardrum)
- Though part of the external ear anatomically, functionally it belongs to the middle ear.
- It vibrates when sound waves hit it and transmits the energy to the ossicles.
2️⃣ Auditory Ossicles (Ear Bones)
The three smallest bones in the human body, which form a chain from the tympanic membrane to the inner ear:
a) Malleus (“hammer”)
- Handle attached to tympanic membrane
- Head articulates with the incus
b) Incus (“anvil”)
- Intermediate bone; articulates with both malleus and stapes
c) Stapes (“stirrup”)
- Footplate fits into the oval window (fenestra vestibuli)
- Transmits vibrations to the fluid-filled cochlea of the inner ear
⚙️ Function of Ossicles
- Amplify sound vibrations ~20x from air (low impedance) to fluid (high impedance)
- Transform sound waves into mechanical energy for the cochlea
3️⃣ Eustachian Tube (Pharyngotympanic Tube)
- Connects middle ear to the nasopharynx
- Lined with mucous membrane and opens during swallowing or yawning
- Equalizes pressure on both sides of the eardrum, preventing rupture
🩺 Clinical note:
- In children, the Eustachian tube is shorter and more horizontal, increasing the risk of otitis media
4️⃣ Middle Ear Muscles
These tiny muscles regulate sound transmission:
a) Tensor Tympani Muscle
- Originates from the auditory tube and inserts on the malleus
- Contracts in response to loud sounds → tightens tympanic membrane → reduces vibration
b) Stapedius Muscle
- Smallest skeletal muscle in the body
- Attaches to stapes
- Dampens excessive vibrations (especially from one’s own voice)
- Innervated by Facial Nerve (CN VII)
🩺 Clinical note:
- Loss of stapedius reflex (e.g., in Bell’s palsy) may cause hyperacusis (sensitivity to sound)
5️⃣ Windows of the Middle Ear
a) Oval Window
- Covered by the footplate of stapes
- Transmits vibrations to the inner ear (cochlea)
b) Round Window
- Covered by a membrane
- Acts as a pressure release valve, allowing fluid displacement within cochlea
🔌 Nerve Relations in the Middle Ear
- Facial Nerve (CN VII):
- Passes through the facial canal, giving rise to the nerve to stapedius and chorda tympani (taste from anterior 2/3 tongue)
- Tympanic Plexus:
- Formed by Glossopharyngeal Nerve (CN IX) → provides sensory innervation to middle ear mucosa
🩺 Clinical Relevance
| Condition | Description |
|---|---|
| Otitis media | Infection of middle ear (common in children) |
| Barotrauma | Pressure difference injury (e.g., during flights or diving) |
| Cholesteatoma | Abnormal skin growth in middle ear; destructive if untreated |
| Otosclerosis | Stapes fixation due to bone overgrowth → conductive deafness |
| Mastoiditis | Infection spreading to mastoid air cells |
✅ Summary Table
| Structure | Function |
|---|---|
| Tympanic membrane | Receives sound and vibrates |
| Ossicles (M-I-S) | Amplify and transmit vibrations to the cochlea |
| Eustachian tube | Equalizes pressure between middle ear and pharynx |
| Stapedius & Tensor Tympani | Protect inner ear from loud sounds |
| Oval & round windows | Interface between middle and inner ear |
🧠👂 Inner Ear (Labyrinth) – Structure and Function
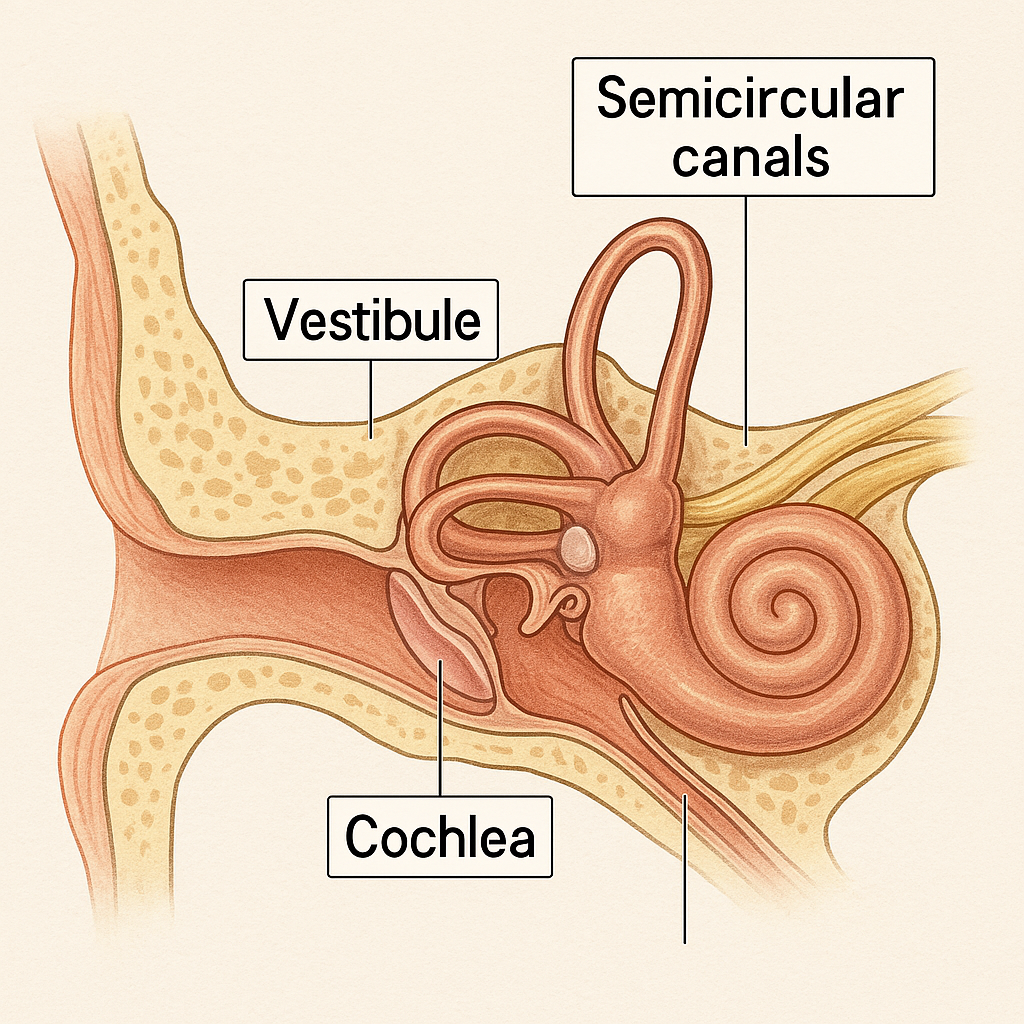
The inner ear is a complex, fluid-filled structure housed in the petrous part of the temporal bone. It serves two main functions:
- Hearing via the cochlea
- Balance (equilibrium) via the vestibular system (vestibule and semicircular canals)
🧱 Structural Overview
The inner ear has two main parts:
- Bony labyrinth – a system of hollow, rigid, bone-encased canals
- Membranous labyrinth – a delicate, fluid-filled membrane suspended within the bony labyrinth
Both contain fluids:
- Perilymph: fills the space between the bony and membranous labyrinths (like CSF)
- Endolymph: fills the membranous labyrinth (rich in potassium, like intracellular fluid)
🔄 Three Major Divisions of the Inner Ear
🔊 1. Cochlea – Hearing Apparatus
📍 Structure:
- Snail-shaped spiral canal (~2.5 turns)
- Bony cochlea contains three parallel fluid-filled chambers:
- Scala vestibuli (perilymph)
- Scala media (cochlear duct) – contains endolymph and houses the Organ of Corti
- Scala tympani (perilymph)
🧬 Organ of Corti:
- Located on the basilar membrane inside the cochlear duct
- Contains hair cells (mechanoreceptors) with stereocilia
- Hair cells synapse with the cochlear nerve fibers (CN VIII)
- When sound-induced vibrations move the basilar membrane, hair cells bend, triggering nerve impulses
⚙️ Function:
- Converts mechanical vibrations into electrical nerve signals → sent to the auditory cortex via the cochlear branch of the vestibulocochlear nerve (CN VIII)
🌀 2. Vestibule – Static Balance & Linear Acceleration
📍 Structure:
- Central part of the bony labyrinth
- Contains two sac-like structures of the membranous labyrinth:
- Utricle
- Saccule
Each contains a macula: a patch of hair cells covered by a gelatinous membrane with embedded otoliths (calcium crystals).
⚙️ Function:
- Detects linear acceleration and gravity (e.g., head tilting, moving forward/backward)
- Sends signals to the brain via the vestibular nerve (CN VIII)
🔁 3. Semicircular Canals – Dynamic (Rotational) Balance
📍 Structure:
- Three looped canals:
- Anterior, Posterior, and Lateral (horizontal)
- Positioned at right angles to detect movement in all 3 dimensions
- Each canal has an enlarged area called the ampulla, which contains the crista ampullaris
🧬 Crista Ampullaris:
- Contains hair cells with stereocilia embedded in a gelatinous structure called the cupula
- When the head rotates, endolymph lags behind, bending the cupula → stimulates hair cells → sends impulse via vestibular nerve
⚙️ Function:
- Detects rotational (angular) movement of the head
🔌 Nerve Supply
The Vestibulocochlear Nerve (CN VIII) has two branches:
- Cochlear nerve – carries hearing signals from cochlea
- Vestibular nerve – carries balance information from semicircular canals, utricle, and saccule
These enter the brainstem at the pons-medulla junction and relay to the auditory cortex or cerebellum.
🩺 Clinical Relevance
| Condition | Description |
|---|---|
| Sensorineural hearing loss | Damage to cochlea or CN VIII |
| Meniere’s disease | Excess endolymph → vertigo, tinnitus, hearing loss |
| Labyrinthitis | Inflammation of inner ear → dizziness, nausea |
| Vestibular neuritis | Viral infection of vestibular nerve → sudden vertigo |
| Benign Paroxysmal Positional Vertigo (BPPV) | Otoliths displaced into semicircular canals → brief vertigo |
✅ Summary Table
| Part | Structure | Function |
|---|---|---|
| Cochlea | Organ of Corti with hair cells | Hearing |
| Vestibule | Utricle + Saccule with macula | Linear acceleration and gravity |
| Semicircular Canals | 3 canals with crista ampullaris | Rotational balance |
| CN VIII | Cochlear + Vestibular branches | Transmits sound and balance signals |
👃🧠 Anatomy of the Nose – The Organ of Smell and Airway Gateway
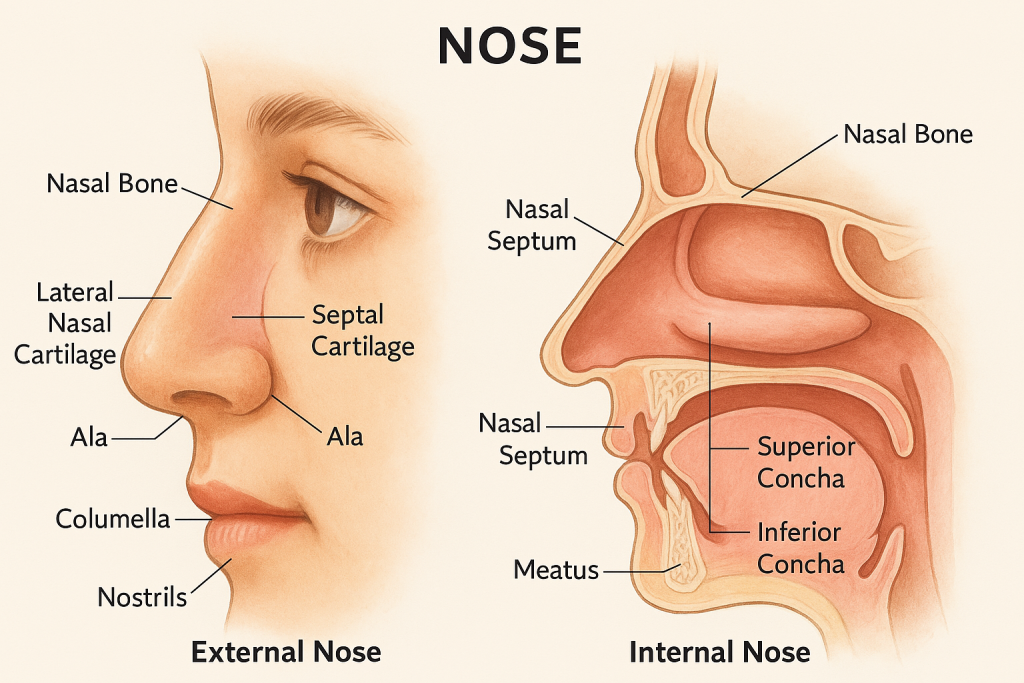
The nose is a vital component of the respiratory system and the olfactory (smell) system. It serves as the entry point for air, filters and humidifies it, and houses sensory receptors for the sense of smell.
🔄 Main Divisions of the Nose
The nose is anatomically divided into two parts:
✅ 1. External Nose
✅ 2. Internal Nose (Nasal Cavity)
🔹 1. External Nose
📍 Structure:
- Pyramidal shape, projecting from the face
- Made of bones, cartilage, muscles, and skin
🧱 Skeletal Framework:
A. Bony Part:
- Nasal bones (bridge of nose)
- Frontal process of maxilla
- Nasal part of frontal bone
B. Cartilaginous Part:
- Lateral nasal cartilages
- Septal cartilage (midline divider)
- Alar cartilages (surround nostrils)
✨ Features:
- Nostrils (nares): external openings leading to nasal cavity
- Columella: soft tissue between nostrils
- Alae: lateral, wing-like flaps of the nostrils
⚙️ Function:
- Allows inhalation/exhalation of air
- Provides initial filtering, warming, and humidification
- Involved in facial expression and aesthetics
🔸 2. Internal Nose (Nasal Cavity)
A large, air-filled space behind the external nose, divided into right and left halves by the nasal septum.
🧱 Boundaries of the Nasal Cavity:
| Wall | Structures |
|---|---|
| Roof | Nasal bones, frontal bone, cribriform plate of ethmoid |
| Floor | Hard palate (maxilla + palatine bones) |
| Medial wall | Nasal septum (cartilage + vomer + perpendicular plate) |
| Lateral wall | Maxilla, ethmoid, inferior concha, palatine bone |
🔸 Important Internal Structures:
A. Nasal Septum
- Divides cavity into right and left
- Made of:
- Septal cartilage (anterior)
- Perpendicular plate of ethmoid (superior)
- Vomer (inferior)
B. Nasal Conchae (Turbinates)
- Three scroll-like bony projections on lateral wall:
- Superior, Middle, Inferior
- Beneath each is a groove called meatus (superior, middle, inferior)
⚙️ Function of Conchae:
- Increase surface area of nasal mucosa
- Warm, moisten, and filter inspired air
- Guide airflow for olfaction and drainage
🌬️ Functions of the Nose
- Respiration – filters, warms, and humidifies air
- Olfaction (Smell) – via olfactory epithelium in upper nasal cavity
- Filtration – nose hairs (vibrissae) and mucous trap dust/pathogens
- Resonance – contributes to voice quality
- Drainage – receives drainage from:
- Paranasal sinuses
- Nasolacrimal duct (tears) into inferior meatus
🔌 Nerve Supply
🧠 Sensory Innervation:
- Olfactory nerve (CN I) – smell sensation from upper nasal mucosa
- Trigeminal nerve (CN V):
- V1 (ophthalmic) → anterior/superior nasal cavity
- V2 (maxillary) → posterior/inferior cavity
✨ Autonomic Innervation:
- Parasympathetic: increases mucus secretion
- Sympathetic: reduces blood flow, decongests nasal mucosa
🩸 Blood Supply
- Kiesselbach’s plexus: vascular network in anterior septum, common nosebleed site
Arteries:
- Facial artery
- Sphenopalatine artery (main)
- Ethmoidal arteries (anterior & posterior)
🩺 Clinical Relevance
| Condition | Description |
|---|---|
| Nasal polyps | Benign mucosal overgrowths, can block airflow |
| Deviated nasal septum | Misalignment of septum, causing obstruction and sinus issues |
| Epistaxis | Nosebleed (common in Little’s area/Kiesselbach’s plexus) |
| Rhinitis | Inflammation/allergy causing nasal congestion |
| Sinusitis | Infection/inflammation of paranasal sinuses |
✅ Summary
| Part | Main Features | Function |
|---|---|---|
| External Nose | Bones + cartilage + nostrils | Directs airflow, smell, facial feature |
| Nasal Septum | Divides cavity, guides air | Supports airflow, filters |
| Conchae & Meatuses | Scroll-shaped bones + grooves | Humidify, filter, increase surface area |
| Olfactory Area | Roof of nasal cavity | Detects smell |
| Paranasal Sinuses | Air-filled cavities around nose | Lighten skull, voice resonance, mucus |
👅🧠 Structure of the Tongue – Organ of Taste, Speech, and Swallowing
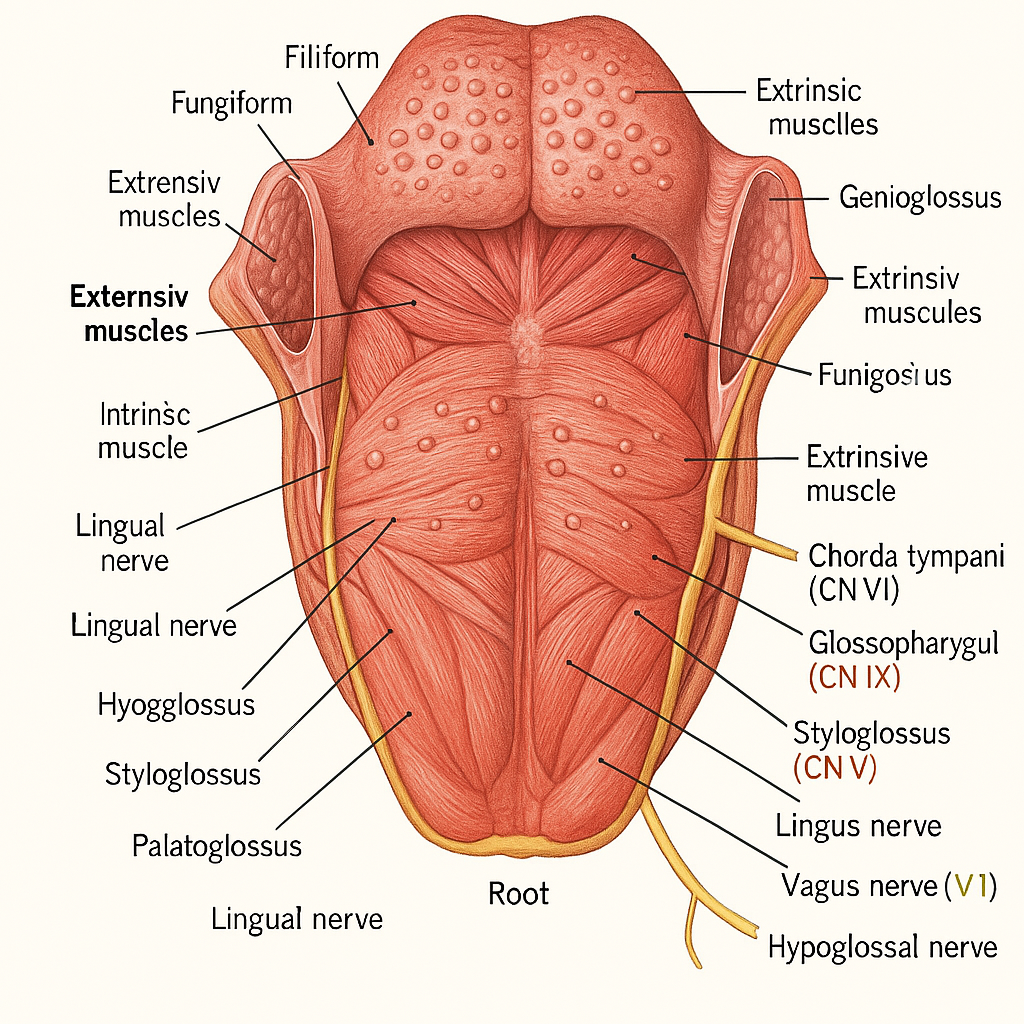
The tongue is a muscular organ located in the oral cavity, playing essential roles in:
- Taste perception
- Speech articulation
- Swallowing (deglutition)
- Food manipulation and mastication
🔍 Divisions of the Tongue
The tongue is divided into three anatomical regions:
1. Apex (Tip)
- Most anterior and mobile part
- Involved in delicate movements for speech and taste
2. Body
- Anterior 2/3 of the tongue (oral part)
- Lies in the oral cavity
- Involved in taste, chewing, and speech
3. Root (Base or Posterior 1/3)
- Lies in the oropharynx
- Anchored to the hyoid bone and mandible
- Involved in swallowing and immune function
📌 Surfaces of the Tongue
🔸 Dorsal Surface (Top)
- Divided by a V-shaped sulcus terminalis:
- Anterior 2/3 (oral part): contains papillae
- Posterior 1/3 (pharyngeal part): contains lingual tonsils
🔸 Ventral Surface (Bottom)
- Smooth and richly vascular
- Contains:
- Lingual frenulum: mucosal fold that anchors tongue to floor of the mouth
- Sublingual caruncles: openings of submandibular ducts (saliva)
🔍 Tongue Papillae (Taste and Texture)
The dorsum of the tongue (top surface) contains four types of papillae:
| Type | Shape & Features | Function |
|---|---|---|
| Filiform | Thin, cone-shaped (most numerous) | Provide friction; no taste buds |
| Fungiform | Mushroom-shaped; scattered across tip/sides | Contain taste buds |
| Circumvallate | Large, round; arranged in a V-shape near sulcus terminalis | Contain many taste buds |
| Foliate | Leaf-like folds on lateral edges | Contain taste buds (especially in children) |
🧬 Muscles of the Tongue
The tongue is made entirely of skeletal muscle. It has:
🔹 Intrinsic Muscles (within the tongue)
- Change the shape of the tongue (e.g., curling, flattening, narrowing)
- Includes: superior longitudinal, inferior longitudinal, transverse, vertical
🔹 Extrinsic Muscles (attach tongue to bone)
- Move the tongue in different directions
- Include:
- Genioglossus – protrudes tongue
- Hyoglossus – depresses tongue
- Styloglossus – elevates and retracts tongue
- Palatoglossus – elevates posterior tongue (also part of soft palate)
🧠 Nerve Supply of the Tongue
📌 Motor Supply:
- All tongue muscles are supplied by the Hypoglossal Nerve (CN XII)
- Except Palatoglossus, supplied by Vagus Nerve (CN X)
📌 Sensory Supply:
| Region | General Sensation | Taste Sensation |
|---|---|---|
| Anterior 2/3 (oral part) | Lingual nerve (branch of CN V3) | Chorda tympani (branch of CN VII) |
| Posterior 1/3 (pharyngeal part) | Glossopharyngeal nerve (CN IX) | Glossopharyngeal nerve (CN IX) |
| Base of tongue (epiglottis) | Vagus nerve (CN X) | Vagus nerve (CN X) |
💧 Blood Supply
- Lingual artery (branch of external carotid artery)
- Venous drainage via lingual vein → internal jugular vein
🧠 Lymphatic Drainage
- Tip of tongue → submental nodes
- Lateral anterior tongue → submandibular nodes
- Posterior tongue → deep cervical nodes
- Important: Cancers of the tongue often metastasize to submandibular or deep cervical lymph nodes
🩺 Clinical Relevance
| Condition | Description |
|---|---|
| Glossitis | Inflammation of the tongue (e.g., due to B12 deficiency) |
| Tongue tie (ankyloglossia) | Shortened frenulum restricts movement (speech/breastfeeding issues) |
| Leukoplakia | White patches, possibly precancerous |
| Oral cancers | Common at lateral border of tongue; tobacco is a major risk |
| Hypoglossal nerve palsy | Tongue deviates toward affected side on protrusion |
✅ Summary Table
| Feature | Details |
|---|---|
| Regions | Tip, body (oral part), root (pharyngeal part) |
| Surface | Dorsal (with papillae), ventral (smooth) |
| Muscles | Intrinsic (shape), Extrinsic (movement) |
| Taste buds | On fungiform, foliate, circumvallate papillae |
| Motor nerve | CN XII (except Palatoglossus – CN X) |
| Taste nerves | CN VII, IX, X |
| Blood supply | Lingual artery and vein |
👁️👂👅👃🖐️ The Sensory Organs – Applications & Implications in Nursing Practice
🔍 Introduction
The five special sensory organs — eyes, ears, nose, tongue, and skin — are essential for perceiving the external environment. They provide sensory input that helps the body maintain homeostasis, avoid danger, communicate, and enjoy life.
Nurses must understand the structure and function of each sense organ to provide holistic care, recognize early signs of disorders, and ensure patient comfort, safety, and education.
🧠 Five Main Sensory Organs and Their Clinical Applications
👁️ 1. Eyes (Organ of Vision)
➤ Functions:
- Detects light, color, shapes
- Enables perception of distance and motion
➤ Nursing Implications:
- Assessment: Visual acuity (Snellen chart), pupil reaction, eye movement
- Care of blind/partially sighted patients: Orientation, mobility support
- Medication administration: Eye drops/ointments → use sterile technique
- Postoperative care: Cataract, glaucoma, retinal surgeries
- Patient education: Avoid rubbing, report floaters/flashes, control diabetes/hypertension
🩺 Common Conditions: Cataract, Glaucoma, Diabetic Retinopathy, Conjunctivitis
👂 2. Ears (Organ of Hearing and Balance)
➤ Functions:
- Hearing (via cochlea)
- Balance and spatial orientation (via semicircular canals)
➤ Nursing Implications:
- Hearing assessments: Whisper test, audiometry
- Assistive devices: Support with hearing aids
- Ear hygiene: Safe cleaning, avoid cotton buds
- Care during infections: Otitis media/externa → monitor for fever, discharge
- Patient education: Protect ears from loud noise, use prescribed drops properly
🩺 Common Conditions: Hearing loss, Tinnitus, Vertigo, Meniere’s disease, Otitis media
👃 3. Nose (Organ of Smell)
➤ Functions:
- Olfaction (smell)
- First line of defense (filters air)
- Enhances taste perception
➤ Nursing Implications:
- Monitoring airway patency
- Observation for infection: Rhinitis, sinusitis
- Smell testing: Anosmia can indicate neurodegeneration (e.g., Parkinson’s)
- Nasal medication: Use correct technique for sprays/drops
- Post-surgery care: Septoplasty or nasal packing care
🩺 Common Conditions: Deviated septum, Sinusitis, Anosmia, Nasal polyps, Epistaxis
👅 4. Tongue (Organ of Taste)
➤ Functions:
- Taste perception (sweet, salty, bitter, sour, umami)
- Assists speech, swallowing, chewing
➤ Nursing Implications:
- Taste changes: May occur due to medications, infections, or nutritional deficiencies
- Oral hygiene care: Especially in unconscious or ventilated patients
- Nutrition monitoring: Altered taste → reduced appetite
- Tongue inspection: For ulcers, coatings, tongue-tie, cancers
🩺 Common Conditions: Glossitis, Oral thrush, Leukoplakia, Taste disorders
✋ 5. Skin (Organ of Touch)
➤ Functions:
- Tactile sensation (touch, pressure, pain, temperature)
- Protection from infection, dehydration
- Thermoregulation, vitamin D synthesis
➤ Nursing Implications:
- Skin integrity: Prevent and manage pressure ulcers
- Sensation testing: Monofilament for diabetic patients
- Temperature regulation: Monitor in post-op or critical care settings
- Skin care: Hydration, hygiene, wound care
🩺 Common Conditions: Burns, Pressure ulcers, Dermatitis, Diabetic neuropathy
📚 Applications in Holistic Nursing Care
✅ 1. Sensory Impairment Assessment
- Early detection of visual, hearing, or tactile loss
- Use of assessment tools like Snellen chart, audiometry, two-point discrimination
✅ 2. Risk Prevention
- Prevent injuries in vision-impaired or sensory-deficient patients
- Remove environmental hazards (e.g., clutter, sharp objects)
✅ 3. Patient Communication
- Adapt communication for hearing-impaired (use of gestures, writing)
- Speak clearly and directly; ensure patient comprehension
✅ 4. Sensory Stimulation
- Use appropriate stimuli in ICU or long-term care (radio, touch therapy)
- Prevent sensory deprivation or overload
✅ 5. Education and Rehabilitation
- Teach correct use of aids (glasses, hearing devices)
- Guide families in providing support at home
🧠 Common Nursing Diagnoses Related to Sensory Organs
- Disturbed sensory perception (visual/auditory/tactile/gustatory)
- Risk for injury (related to sensory deficits)
- Impaired verbal communication
- Impaired oral mucous membrane
- Acute/chronic pain (ear, eye, skin, etc.)
✅ Summary Table
| Organ | Function | Key Nursing Focus |
|---|---|---|
| Eyes | Vision | Safety, medication, post-op care |
| Ears | Hearing, balance | Hearing aid care, infection, vertigo management |
| Nose | Smell, airway filter | Nasal meds, infection, neuro check (smell loss) |
| Tongue | Taste, speech | Oral hygiene, nutrition, taste changes |
| Skin | Touch, protection | Ulcer prevention, hygiene, neuropathy checks |
🦴 Structure of Bone – Gross and Microscopic Anatomy
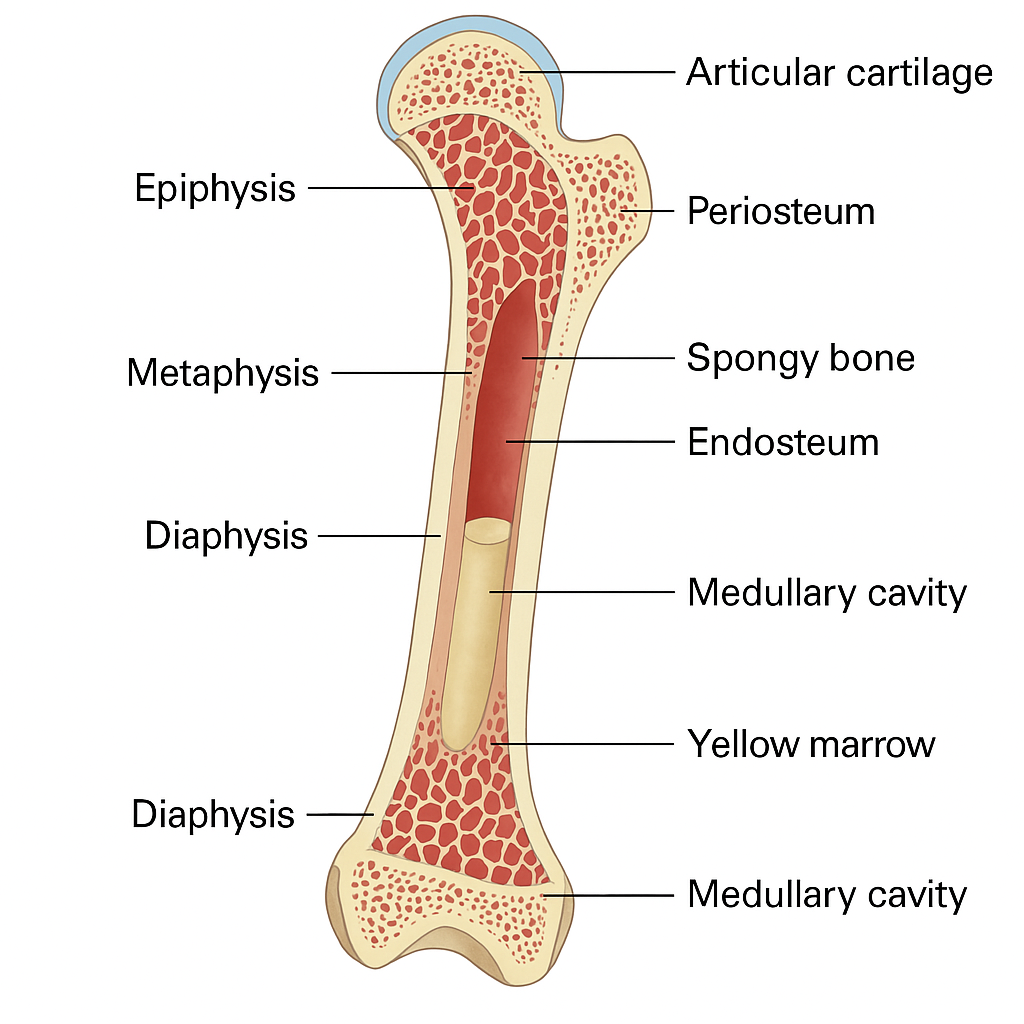
📌 I. Gross Structure of Bone (Macroscopic Anatomy)
Bones are organs made of osseous tissue, blood vessels, bone marrow, nerves, and connective tissue. Let’s take the example of a long bone (e.g., femur) to understand the structure:
1. Diaphysis (Shaft)
- The long, cylindrical middle portion of the bone
- Composed of thick compact bone
- Encloses the medullary (marrow) cavity, which contains:
- Yellow marrow (fat storage in adults)
- Red marrow in children
2. Epiphyses (Ends of Bone)
- Expanded ends of the bone (proximal and distal)
- Composed mostly of spongy (cancellous) bone
- Contains red marrow (site of blood cell production)
- Covered by articular (hyaline) cartilage → smooth, reduces friction at joints
3. Metaphysis
- Region between diaphysis and epiphysis
- In growing children, contains the epiphyseal plate (growth plate)
- In adults, becomes the epiphyseal line
4. Periosteum
- Tough, fibrous membrane covering the outer surface of bones (except joints)
- Has two layers:
- Outer fibrous layer: dense connective tissue
- Inner osteogenic layer: contains osteoblasts and osteoclasts
- Rich in nerves and blood vessels
- Function: Bone growth, repair, and serves as an attachment point for muscles, tendons, and ligaments
5. Endosteum
- Thin membrane lining the internal surfaces (medullary cavity, Haversian canals)
- Contains osteoblasts and osteoclasts
6. Medullary Cavity (Marrow Cavity)
- Central cavity in diaphysis
- Contains:
- Red marrow in children (hematopoietic)
- Yellow marrow in adults (fat storage)
🔬 II. Microscopic Structure of Bone (Histology)
Bone tissue is of two types:
✅ Compact bone (dense)
✅ Spongy bone (cancellous)
🔹 A. Compact Bone
Highly organized, strong, and forms the outer layer of bones.
➤ Structural Unit: Osteon (Haversian System)
Each osteon consists of:
| Part | Function |
|---|---|
| Haversian canal | Central canal with blood vessels and nerves |
| Lamellae | Concentric rings of calcified matrix |
| Lacunae | Small spaces between lamellae; contain osteocytes |
| Canaliculi | Tiny canals connecting lacunae; allow nutrient/waste exchange |
| Volkmann’s canals | Perpendicular canals connecting osteons; carry vessels and nerves |
🔹 B. Spongy Bone (Cancellous Bone)
- Found in epiphyses, flat bones, vertebrae, etc.
- Made of trabeculae (lattice of thin bone plates)
- Spaces between trabeculae are filled with red bone marrow
- Lighter and less dense than compact bone
- No osteons – nutrients diffuse through canaliculi from marrow spaces
🧬 Types of Bone Cells
| Cell | Function |
|---|---|
| Osteoblasts | Build new bone matrix (bone-forming cells) |
| Osteocytes | Mature bone cells that maintain the matrix |
| Osteoclasts | Break down bone matrix (bone-resorbing cells) |
| Osteoprogenitor cells | Stem cells that differentiate into osteoblasts |
🧪 Bone Matrix Composition
| Component | Function |
|---|---|
| Organic matrix (35%) | Collagen fibers (strength + flexibility) |
| Inorganic salts (65%) | Calcium phosphate crystals (bone hardness) |
🩺 Clinical Correlation
| Condition | Involvement |
|---|---|
| Fractures | Break in continuity of compact/spongy bone |
| Osteoporosis | Loss of bone density, especially in trabecular bone |
| Osteomalacia/Rickets | Poor mineralization due to vitamin D deficiency |
| Bone cancer | May originate in marrow (leukemia) or bone matrix |
✅ Summary Table
| Feature | Details |
|---|---|
| Gross Parts | Diaphysis, epiphysis, metaphysis, periosteum |
| Compact bone | Dense outer layer; contains osteons |
| Spongy bone | Lattice-like; contains red marrow |
| Bone cells | Osteoblasts, osteocytes, osteoclasts |
| Marrow types | Red (hematopoiesis), Yellow (fat storage) |
🦴✨ Classification of Bones: Types, Structure & Clinical Relevance
The human skeleton is composed of 206 bones, and each bone is classified based on its shape, internal structure, and function. Understanding these types helps in identifying bone behavior during growth, movement, trauma, or disease.
🧠 Overview: Why Do We Classify Bones by Shape?
- To understand mechanical function
- To determine locations of hematopoiesis
- To identify fracture risks and clinical relevance
- To aid in radiographic interpretation
🧱 The 5 Main Types of Bones
🔹 1. Long Bones
📍 Characteristics:
- Longer than they are wide
- Have a central shaft (diaphysis) and two expanded ends (epiphyses)
- Mostly compact bone in the shaft and spongy bone at the ends
- Medullary cavity contains marrow
🧬 Structure:
- Diaphysis: provides strength and weight-bearing
- Epiphysis: contains red marrow for hematopoiesis
- Metaphysis: contains the growth plate in children
📘 Examples:
- Upper limb: humerus, radius, ulna, metacarpals, phalanges
- Lower limb: femur, tibia, fibula, metatarsals, phalanges
- Clavicle is also classified as a long bone
🩺 Clinical Importance:
- Fracture-prone in trauma (e.g., femoral neck fractures)
- Bone marrow biopsy in children often taken from long bones
- Common site of osteomyelitis in growing bones (metaphysis)
🔸 2. Short Bones
📍 Characteristics:
- Cuboidal or box-like in shape
- Length ≈ Width ≈ Height
- Core made of spongy bone, surrounded by a thin compact bone shell
- Provide support and stability, allow limited motion
📘 Examples:
- Carpal bones (wrist)
- Tarsal bones (ankle)
🩺 Clinical Importance:
- Wrist fractures (e.g., scaphoid) can disrupt blood supply → risk of avascular necrosis
- Common site for sprain injuries
🔹 3. Flat Bones
📍 Characteristics:
- Thin, flat, and often slightly curved
- Composed of two layers of compact bone with spongy bone (diploë) in between
- Offer broad surface area for muscle attachment
- Provide protection to underlying organs
📘 Examples:
- Skull bones (frontal, parietal, occipital)
- Sternum
- Ribs
- Scapula
🩺 Clinical Importance:
- Skull fractures can lead to intracranial injuries
- Sternum is used for bone marrow biopsy
- Flat bones are major sites for red marrow in adults (hematopoiesis)
🔸 4. Irregular Bones
📍 Characteristics:
- Complex shapes that don’t fit into other categories
- Often contain notches, ridges, or projections
- Made of spongy bone inside, covered by a thin compact bone shell
- Protect nervous tissue or serve multiple muscle attachments
📘 Examples:
- Vertebrae
- Sacrum and coccyx
- Pelvic bones (ilium, ischium, pubis)
- Mandible
- Certain skull bones (ethmoid, sphenoid)
🩺 Clinical Importance:
- Vertebral fractures common in osteoporosis
- Pelvic fractures are life-threatening due to vascular proximity
- Base of skull (ethmoid/sphenoid) fractures → CSF leaks
🔹 5. Sesamoid Bones
📍 Characteristics:
- Small, round bones embedded within tendons
- Develop in areas of friction, stress, and tension
- Act to:
- Protect the tendon
- Alter the direction of muscle pull
- Increase mechanical efficiency of muscles
📘 Examples:
- Patella (largest sesamoid bone)
- Sesamoids in the tendons of the big toe and thumb
🩺 Clinical Importance:
- Sesamoiditis: inflammation common in dancers/athletes
- Patellar fractures affect knee extension
- Can be mistaken for fracture on X-rays
🧪 Rare Types of Bones (Additional Classifications)
| Type | Description | Examples |
|---|---|---|
| Pneumatic bones | Contain air-filled spaces (sinuses) | Ethmoid, sphenoid, maxilla |
| Accessory bones | Extra bones due to incomplete fusion during development | Sutural bones in skull, Os trigonum |
📚 Comprehensive Summary Table
| Type of Bone | Shape | Location/Examples | Function |
|---|---|---|---|
| Long | Elongated shaft and ends | Femur, humerus, tibia, radius, phalanges | Support, movement, marrow production |
| Short | Cube-shaped | Carpals, tarsals | Stability with limited motion |
| Flat | Thin, flat, often curved | Skull, sternum, ribs, scapula | Protection, muscle attachment |
| Irregular | Complex, non-uniform shape | Vertebrae, pelvis, mandible, ethmoid | Protect nervous system, muscle support |
| Sesamoid | Small, rounded, in tendons | Patella, under big toe/thumb tendons | Reduce friction, improve leverage |
🧠 Mnemonic to Remember Bone Types
“Long Short Flat Irregular Sesamoid”
Think: “Lovers Should Find Interesting Souls” 😊
🩺 Nursing and Clinical Implications
- Knowing bone types helps:
- Understand fracture mechanics and healing
- Choose biopsy or injection sites (e.g., flat bones like sternum or iliac crest)
- Monitor high-risk areas for degeneration, infections, or metastasis
- Crucial for:
- Orthopedic care
- Physiotherapy
- Radiographic assessments
- Post-trauma evaluation