BSC SEM 3 UNIT 9 ADULT HEALTH NURSING 1
UNIT 9 Nursing management of patients with disorders of Integumentary system
🧬 Review of Anatomy and Physiology of the Skin
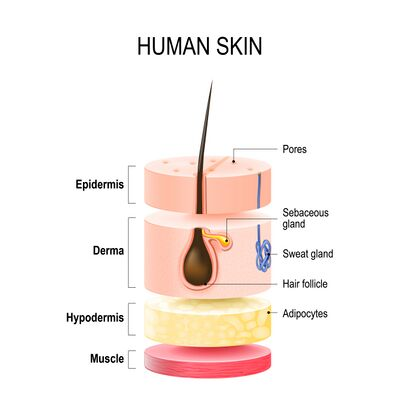
📌 Definition:
The skin is the largest organ of the human body. It serves as a protective barrier between the internal organs and the external environment and plays vital roles in temperature regulation, sensory reception, immune defense, and vitamin D synthesis.
🧱 ANATOMY OF THE SKIN:
The skin is made up of three main layers:
1️⃣ Epidermis (Outer Layer)
- Avascular (contains no blood vessels)
- Composed of stratified squamous epithelial cells
- Provides a protective barrier against environmental damage
📍 Layers of Epidermis (from inner to outer):
- Stratum basale (germinativum) – deepest layer; site of cell division and melanin production
- Stratum spinosum – provides strength and flexibility
- Stratum granulosum – contains keratohyalin granules for keratin formation
- Stratum lucidum – present only in thick skin (palms, soles)
- Stratum corneum – outermost, made of dead keratinized cells for waterproof protection
🔬 Cell Types in Epidermis:
- Keratinocytes – produce keratin for strength and waterproofing
- Melanocytes – produce melanin pigment (skin color and UV protection)
- Langerhans cells – immune defense
- Merkel cells – touch sensation
2️⃣ Dermis (Middle Layer)
- Thickest skin layer
- Made of connective tissue, collagen, and elastin fibers
- Provides strength, elasticity, and nourishment to the epidermis
- Highly vascularized and innervated
📍 Divided into:
- Papillary layer – contains capillaries, pain and touch receptors
- Reticular layer – contains sweat glands, sebaceous glands, hair follicles, blood vessels, and nerves
🩺 Structures in the Dermis:
- Blood vessels – regulate temperature and nourish skin
- Nerve endings – detect pressure, temperature, pain, and vibration
- Hair follicles – produce hair and support thermoregulation
- Sebaceous glands – secrete sebum for lubrication
- Sweat glands:
- Eccrine – thermoregulation (present all over body)
- Apocrine – located in axillae, groin; activated during puberty
3️⃣ Hypodermis / Subcutaneous Tissue (Inner Layer)
- Composed of loose connective tissue and fat cells (adipose tissue)
- Functions:
- Acts as insulation and shock absorber
- Stores energy in fat form
- Anchors skin to underlying muscles and bones
⚙️ PHYSIOLOGY OF THE SKIN:
The skin performs multiple essential functions to maintain homeostasis and protect the body.
✅ 1. Protection
- Barrier against mechanical, chemical, microbial, and UV damage
- Prevents water loss
✅ 2. Thermoregulation
- Sweat glands cool the body via evaporation
- Blood vessel dilation/constriction regulates heat loss or retention
- Hair assists in insulating heat
✅ 3. Sensation
- Contains specialized nerve receptors for:
- Touch (Merkel discs, Meissner’s corpuscles)
- Pain (free nerve endings)
- Pressure and vibration (Pacinian corpuscles)
- Temperature (Ruffini and Krause endings)
✅ 4. Metabolism (Vitamin D Synthesis)
- Exposure to UVB rays converts skin cholesterol to vitamin D3, essential for calcium absorption
✅ 5. Excretion
- Minor excretion of salt, water, and urea through sweat
✅ 6. Immune Function
- Langerhans cells in epidermis initiate immune responses
- Acts as a first line of defense against pathogens
✅ 7. Absorption
- Certain medications (e.g., topical creams, nicotine patches) can be absorbed through the skin
🩺 Nursing Assessment of Patients with Integumentary System Disorders
🎯 Purpose of Assessment:
- Identify skin abnormalities
- Monitor for infection, inflammation, allergies, pressure injuries, wounds
- Detect systemic diseases with skin manifestations (e.g., diabetes, lupus)
- Guide interventions and patient education
🗂️ I. Health History (Subjective Data)
Begin with interviewing the patient to obtain relevant personal, family, and lifestyle information:
✅ A. Chief Complaints:
- Itching (pruritus)
- Pain, burning, or tenderness
- Rash, redness, discoloration
- Dryness or scaling
- Blistering, ulcers, swelling
- Lesions or moles that changed in size, shape, or color
- Hair loss, nail changes
- Excessive sweating or dryness
✅ B. Past Medical History:
- Previous or chronic skin conditions: eczema, psoriasis, dermatitis, acne, vitiligo
- History of allergies or hypersensitivities
- Previous hospitalizations or surgeries related to the skin
- Any autoimmune disorders (e.g., lupus) or metabolic diseases (e.g., diabetes)
✅ C. Family History:
- Hereditary conditions: psoriasis, skin cancer, alopecia
- Atopic history (eczema, hay fever, asthma)
✅ D. Lifestyle and Environmental Factors:
- Sun exposure history (risk for melanoma)
- Occupational exposure to chemicals or irritants
- Hygiene practices
- Cosmetic or skin products used
- Dietary habits
- Smoking, alcohol, and substance use
- Recent travel (to rule out endemic skin infections)
🧍♀️ II. Physical Examination (Objective Data)
Use inspection and palpation to assess the skin, hair, nails, and associated symptoms.
✅ A. Skin Inspection:
Assess color, integrity, lesions, and texture.
| Aspect | What to Assess |
|---|---|
| Color | Pallor, cyanosis, erythema, jaundice, hyperpigmentation, hypopigmentation |
| Moisture | Dryness, oiliness, excessive sweating |
| Temperature | Warmth, coolness (use dorsum of hand to assess) |
| Texture | Roughness, smoothness, thickness, thinness |
| Turgor | Skin elasticity (pinch test on forearm) — ↓ in dehydration or aging |
| Lesions | Location, size, shape, color, elevation, drainage, and pattern |
| Wound presence | Pressure injuries, diabetic ulcers, surgical wounds — stage and document clearly |
✅ B. Lesion Assessment (if present):
- Type: macule, papule, vesicle, pustule, plaque, ulcer
- Number: single, multiple
- Distribution: localized, generalized, symmetrical, dermatomal
- Arrangement: linear, clustered, annular, targetoid
- Color and border: pigmented, erythematous, well-defined, irregular
- Drainage: serous, purulent, bloody
- Pain or tenderness: on palpation
✅ C. Hair Assessment:
- Distribution, texture, oiliness
- Hair loss patterns (alopecia), dandruff, lice/nits
- Color changes or brittleness
- Scalp condition (dry, scaly, inflamed)
✅ D. Nail Assessment:
- Color (pale, cyanotic, yellow)
- Shape (clubbing in chronic hypoxia, spooning in anemia)
- Texture and thickness
- Nail bed capillary refill (normal <2 seconds)
- Presence of fungal infections or lesions around nails
🧾 III. Special Considerations During Assessment:
- Use the Braden Scale to assess pressure injury risk
- Be culturally sensitive (e.g., skin tone variations in dark-skinned individuals)
- Be mindful of psychosocial effects — body image issues, emotional distress
- Use gloves when assessing open wounds or infected areas
📊 Documentation Tips:
- Use standard terminology (e.g., macular rash, stage II ulcer)
- Describe lesions or wounds accurately with dimensions (in cm)
- Document patient’s response (e.g., “pain 6/10 on pressure ulcer site”)
- Note progress or regression during each shift/visit
🩺 History and Physical Assessment of Patients with Integumentary System Disorders
🧾 I. Health History (Subjective Assessment)
The health history focuses on collecting relevant information from the patient about current symptoms, past conditions, lifestyle, and risk factors affecting the skin, hair, and nails.
✅ A. Presenting Complaints (Chief Concerns):
Ask the patient about:
- Rash, redness, swelling, or discoloration
- Itching (pruritus)
- Pain, burning, tingling, or stinging
- Dryness or peeling of skin
- Wounds, ulcers, or sores that won’t heal
- Lesions, bumps, or moles that have changed in size, shape, or color
- Nail discoloration or thickening
- Hair loss or unusual hair growth
- Excessive sweating (hyperhidrosis) or dry skin (xerosis)
📌 Ask about onset, location, duration, pattern, progression, and relieving/aggravating factors.
✅ B. Past Medical and Surgical History:
- History of chronic skin conditions: eczema, psoriasis, acne, dermatitis, vitiligo
- Autoimmune diseases: lupus, scleroderma
- Infectious diseases: fungal infections, scabies, shingles
- Diabetes mellitus or peripheral vascular disease (delayed healing, diabetic foot ulcers)
- Previous skin injuries, burns, surgeries, scars, or tattoos
✅ C. Medication History:
- Current and past medications (especially steroids, antibiotics, chemotherapeutics)
- Use of topical products: creams, ointments, lotions
- Any known drug allergies (e.g., to sulfa, penicillin, iodine)
✅ D. Family History:
- Hereditary skin conditions: psoriasis, vitiligo, albinism, eczema
- Skin cancers (melanoma, basal cell carcinoma) in the family
✅ E. Lifestyle and Environmental Factors:
- Sun exposure habits and use of sunscreen
- Occupational exposure to chemicals, allergens, UV light
- Personal hygiene routine
- Smoking, alcohol, or drug use
- Nutritional status (deficiencies can affect skin health)
- Recent travel or contact with infected individuals or animals
✅ F. Psychosocial Impact:
- How the skin problem affects the patient emotionally, socially, or mentally
- Issues with body image, confidence, or depression related to chronic skin issues
🔍 II. Physical Assessment (Objective Data)
A systematic inspection and palpation of the skin, scalp, nails, and mucous membranes is performed.
✅ A. Skin Assessment:
🔸 Color:
- Normal, pale (anemia), cyanotic (hypoxia), flushed (fever), jaundiced (liver disease), hyperpigmented, or hypopigmented areas
🔸 Lesions:
- Note type (macule, papule, pustule, ulcer, plaque, vesicle), location, size, color, shape, and distribution
- Look for signs of infection (redness, heat, pus), allergic reaction, or trauma
🔸 Moisture:
- Dryness, sweating, or oiliness
🔸 Temperature:
- Use the back of your hand to check if skin is warm, cool, or hot (inflammation or infection)
🔸 Texture and Thickness:
- Rough, smooth, scaly, thin or thickened areas
🔸 Turgor (Elasticity):
- Pinch skin on the forearm or chest; delayed return = dehydration or aging
🔸 Edema or Swelling:
- Check for pitting edema, firmness, or inflammation
✅ B. Hair Assessment:
- Distribution: Even or patchy hair loss (alopecia)
- Texture: Coarse, fine, brittle, oily, or dry
- Color: Normal or unusual (e.g., greying, discoloration)
- Scalp: Check for lesions, dandruff, scaling, parasites (lice)
✅ C. Nail Assessment:
- Color: Pale (anemia), cyanotic, yellow (fungal infection)
- Shape: Clubbing (chronic hypoxia), spooning (koilonychia in iron deficiency)
- Texture: Brittle, thickened, or ridged nails
- Capillary refill: Normal <2 seconds
- Presence of infection or inflammation around the nail bed
✅ D. Mucous Membranes & Pressure Points:
- Check lips, oral cavity, conjunctiva for hydration, ulcers, or pigmentation
- Inspect bony prominences for early signs of pressure injury (redness, warmth, tenderness)
📝 Documentation Tips:
- Use accurate, objective descriptions (e.g., “2 cm round erythematous lesion with central crust”)
- Document location, size (in cm), shape, color, drainage, odor
- Describe patient’s subjective complaints along with visible findings
- Use tools like Braden Scale for risk of pressure ulcers
🩺 Dermatitis
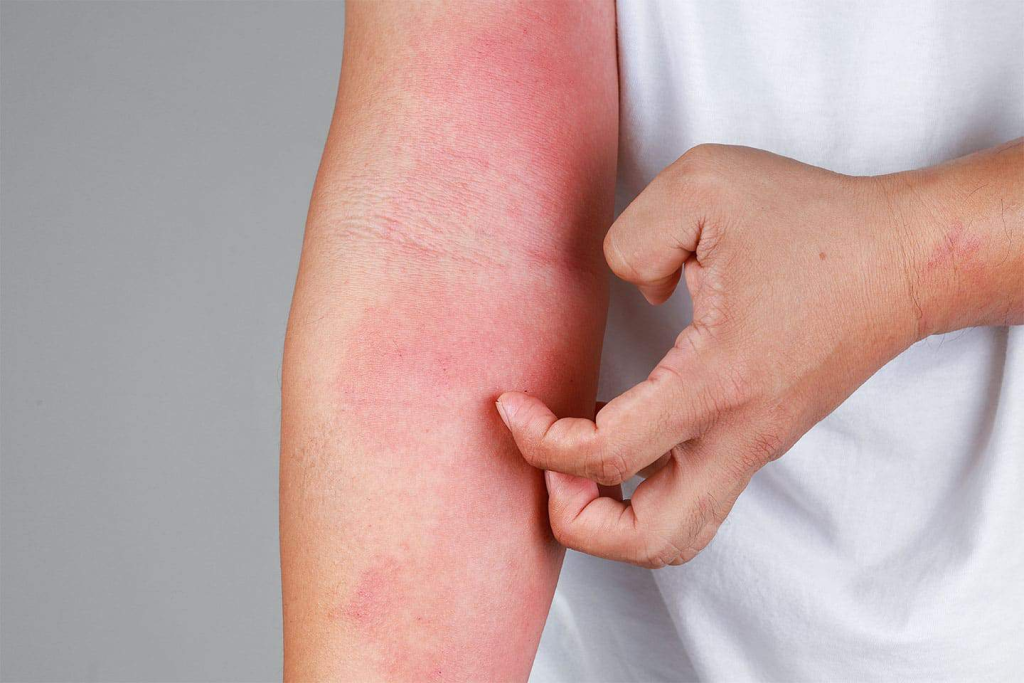
📌 Definition and Causes
✅ Definition:
Dermatitis is a general term for inflammation of the skin, characterized by redness (erythema), swelling, itching (pruritus), and sometimes blistering, oozing, scaling, or thickening of the skin.
It is not a specific disease, but rather a broad classification of inflammatory skin conditions caused by allergens, irritants, infections, or immune reactions.
🔍 Dermatitis can be acute (sudden onset) or chronic (long-standing and recurring).
🧬 Causes of Dermatitis:
The causes vary depending on the type of dermatitis but generally include:
🟠 1. Allergic Reactions:
- Contact with allergens (e.g., poison ivy, nickel, cosmetics, fragrances)
- Immune system reacts with Type IV hypersensitivity
🔵 2. Irritants:
- Direct skin damage from chemicals, detergents, solvents, soaps, or cleaning products
🟢 3. Genetic Factors:
- Family history of atopic conditions (eczema, asthma, hay fever)
- Common in atopic dermatitis
🟣 4. Infections:
- Bacterial (e.g., impetiginized eczema)
- Fungal (e.g., seborrheic dermatitis)
- Viral (e.g., herpetic eczema)
🟡 5. Environmental Triggers:
- Heat, cold, humidity, sweating
- Sun exposure (photodermatitis)
🔴 6. Stress and Hormonal Factors:
- Emotional stress can trigger or worsen dermatitis
- Hormonal changes (e.g., puberty, menstruation)
⚫ 7. Autoimmune and Systemic Disorders:
- E.g., Stasis dermatitis from poor circulation
- Contact dermatitis due to delayed-type immune response
🔢 Types of Dermatitis
Dermatitis is broadly classified based on its cause, appearance, and pathophysiology. Below are the major types:
1️⃣ Atopic Dermatitis (Eczema)
🧬 A chronic, relapsing, allergic skin condition, often starting in childhood
- Cause: Genetic + environmental (allergens, irritants, stress)
- Associated with: Asthma, allergic rhinitis (hay fever)
- Common sites: Face, neck, elbows, knees, flexural areas
- Symptoms: Dry, itchy skin; redness; lichenification (thickening); scratching
2️⃣ Contact Dermatitis
🌿 Inflammatory reaction caused by direct contact with an allergen or irritant
🔸 A. Irritant Contact Dermatitis
- Cause: Soaps, acids, detergents, solvents
- Occurs in anyone, not immune-mediated
- Symptoms: Burning, stinging, dryness, cracking
🔸 B. Allergic Contact Dermatitis
- Cause: Nickel, latex, cosmetics, poison ivy
- Delayed hypersensitivity (Type IV reaction)
- Symptoms: Redness, swelling, vesicles, oozing
3️⃣ Seborrheic Dermatitis
🧴 Chronic dermatitis in sebaceous (oil-producing) areas
- Cause: Overgrowth of Malassezia yeast + oily skin
- Common sites: Scalp, face, behind ears, chest
- Symptoms: Greasy, yellowish scales; dandruff; mild itching
- Common in infants (cradle cap) and adults
4️⃣ Nummular Dermatitis
💧 Coin-shaped, scaly, itchy plaques
- Cause: Unknown; associated with dry skin, environmental changes
- Often appears in older adults
- Common on arms, legs, back, and buttocks
5️⃣ Stasis Dermatitis
🦵Occurs in lower legs due to poor venous circulation
- Cause: Chronic venous insufficiency
- Symptoms: Redness, scaling, edema, ulcers, brownish discoloration
- Often seen in elderly or immobile patients
6️⃣ Dyshidrotic Dermatitis
💦 Involves small blisters (vesicles) on hands and feet
- Cause: Stress, sweating, allergies
- Symptoms: Intense itching, burning, peeling
- Blisters may rupture → pain and secondary infection
7️⃣ Perioral Dermatitis
💋 Occurs around the mouth, nose, or eyes
- Cause: Overuse of topical steroids, cosmetics, fluoride toothpaste
- Symptoms: Redness, papules, burning, scaling
- Seen mostly in young women
8️⃣ Photodermatitis
☀️ Skin inflammation due to sunlight (UV radiation)
- Cause: Sun exposure + photosensitizing agents (e.g., tetracyclines, perfumes)
- Symptoms: Redness, swelling, blisters in sun-exposed areas
9️⃣ Neurodermatitis (Lichen Simplex Chronicus)
🔁 Chronic itch-scratch cycle causes thickened, leathery skin
- Cause: Repeated scratching due to stress, eczema, or unknown triggers
- Symptoms: Dry, scaly patches; thickened skin; intense itch
1️⃣0️⃣ Autoimmune Dermatitis (e.g., Dermatitis Herpetiformis)
🧪 Associated with celiac disease and gluten sensitivity
- Cause: Autoimmune reaction to gluten
- Symptoms: Itchy, burning blisters on elbows, knees, buttocks
🔬 Pathophysiology of Dermatitis (Type-wise Explanation)
1️⃣ Atopic Dermatitis (Eczema)
- Genetic predisposition + immune dysregulation lead to:
- Impaired skin barrier function (↓ filaggrin protein)
- Increased trans-epidermal water loss → dry, itchy skin
- Exposure to allergens or irritants → triggers Th2-dominant immune response
- Result: Chronic inflammation, itching, redness, and skin thickening (lichenification)
2️⃣ Contact Dermatitis
🔸 A. Irritant Contact Dermatitis
- Direct chemical or physical damage to skin from irritants (e.g., acids, soaps)
- Causes local inflammation without immune involvement
- Releases proinflammatory cytokines → redness, swelling, and skin breakdown
🔸 B. Allergic Contact Dermatitis
- Type IV delayed-type hypersensitivity reaction
- Allergen binds to skin proteins → processed by Langerhans cells → presented to T-cells
- On re-exposure, memory T-cells trigger inflammation and blistering
3️⃣ Seborrheic Dermatitis
- Involves overactive sebaceous glands + overgrowth of Malassezia yeast
- Yeast metabolites trigger inflammatory response in genetically predisposed individuals
- Leads to erythema, scaling, and itching in oily areas like scalp and face
4️⃣ Nummular Dermatitis
- Often associated with dry skin (xerosis)
- Skin barrier dysfunction allows irritants and allergens to enter
- Activates immune cells → localized circular plaques with inflammation and scaling
5️⃣ Stasis Dermatitis
- Results from chronic venous insufficiency in lower extremities
- Poor circulation leads to venous hypertension → leakage of blood and plasma into skin
- Iron deposits (hemosiderin) and inflammation result in discoloration, thickening, and ulcers
6️⃣ Dyshidrotic Dermatitis
- Likely involves abnormal sweat gland function or stress-triggered immune response
- Leads to intraepidermal vesicle formation filled with clear fluid
- Often worsened by excessive sweating, allergens, or metal exposure (e.g., nickel)
7️⃣ Perioral Dermatitis
- Triggered by topical steroid use, fluoride toothpaste, or cosmetics
- These agents disrupt skin flora and induce inflammation around mouth/nose
- Histology shows follicular inflammation and papular eruptions
8️⃣ Photodermatitis
- UV radiation reacts with photosensitizing chemicals on the skin
- Forms free radicals that damage skin cells and DNA
- Leads to immune-mediated inflammation in sun-exposed areas
9️⃣ Neurodermatitis (Lichen Simplex Chronicus)
- Triggered by chronic scratching or rubbing of the skin
- Repetitive trauma → epidermal hyperplasia (thickened skin) and nerve ending proliferation
- Causes intensified itching and cycle of itch → scratch → more itch
🔟 Dermatitis Herpetiformis
- Autoimmune response triggered by gluten ingestion
- IgA antibodies deposit in dermal papillae of the skin
- Activates complement system → neutrophil recruitment → vesicle formation
- Extremely itchy, blistering rash linked to celiac disease
✅ Common Final Pathway in Most Types of Dermatitis:
- Skin barrier dysfunction → allergen/irritant entry
- Immune system activation (T-cell mediated or cytokine-driven)
- Inflammation → erythema, edema, pruritus, vesiculation or scaling
🔍 Signs & Symptoms and Diagnosis of Dermatitis
✅ GENERAL SIGNS & SYMPTOMS (Common to Most Types)
Most forms of dermatitis share a basic set of skin-related symptoms due to inflammation and immune response:
| ⚠️ Symptom | 📝 Description |
|---|---|
| Erythema | Redness due to vasodilation and inflammation |
| Pruritus (Itching) | Most common symptom, can be severe and lead to scratching |
| Edema | Swelling of the skin or surrounding tissues |
| Dryness / Scaling | Flaky, dry skin; often seen in chronic dermatitis |
| Vesicles / Blisters | Fluid-filled lesions, especially in acute types |
| Crusting / Oozing | Common when vesicles rupture |
| Lichenification | Thickened, leathery skin from chronic rubbing/scratching |
| Pigmentation changes | Darkening (hyperpigmentation) or lightening (hypopigmentation) |
🔷 TYPE-SPECIFIC SIGNS & SYMPTOMS
1️⃣ Atopic Dermatitis
- Dry, itchy, inflamed skin (especially in flexural areas)
- Red patches with thickening and scaling
- Lichenification from chronic scratching
- Common in infants and children
- Often associated with asthma and allergic rhinitis
2️⃣ Contact Dermatitis
- Localized rash or irritation where skin touched irritant/allergen
- May appear as blisters, redness, or dry cracked skin
- Allergic type may appear 48–72 hours after exposure
3️⃣ Seborrheic Dermatitis
- Greasy yellow scales and dandruff-like flakes
- Affects scalp, eyebrows, nose creases, chest
- Mild itching and redness
- Common in infants (“cradle cap”) and adults
4️⃣ Nummular Dermatitis
- Coin-shaped (nummular) plaques on limbs or trunk
- Intensely itchy and dry
- May ooze or crust in acute stage
5️⃣ Stasis Dermatitis
- Found on lower legs
- Red-brown pigmentation, itching, edema
- May develop ulcers, particularly near ankles
6️⃣ Dyshidrotic Dermatitis
- Small, deep vesicles (blisters) on palms, fingers, or soles
- Intense burning or itching
- Scaling and cracking after blister rupture
7️⃣ Perioral Dermatitis
- Red papules or pustules around mouth, nose, or eyes
- Tingling or burning sensation
- Often caused by topical steroids or cosmetics
8️⃣ Photodermatitis
- Rash in sun-exposed areas
- Redness, blistering, swelling, peeling
- Triggered by sun + medications or chemicals
9️⃣ Neurodermatitis
- One or more thick, scaly patches from constant scratching
- Very itchy, especially during stress or at night
- Localized (e.g., back of neck, arms, legs)
🔟 Dermatitis Herpetiformis
- Itchy, grouped vesicles on elbows, knees, back, or buttocks
- Linked to gluten sensitivity
- Burning sensation and risk of excoriation due to scratching
🧪 DIAGNOSIS OF DERMATITIS
✅ 1. Clinical Examination
- Diagnosis often based on history and visual inspection
- Assessment of pattern, distribution, and morphology of skin lesions
✅ 2. Patch Testing
- Used for suspected Allergic Contact Dermatitis
- Identifies specific allergens causing delayed hypersensitivity
✅ 3. Skin Biopsy
- May be used to:
- Differentiate types of dermatitis
- Rule out psoriasis, fungal infection, or skin cancer
✅ 4. Blood Tests
- IgE levels: Often elevated in Atopic Dermatitis
- Celiac antibody panel: For suspected Dermatitis Herpetiformis
✅ 5. Skin Scraping or Culture
- To rule out fungal infections or secondary bacterial infections
💊 Medical Management of Dermatitis
🎯 Goals of Treatment:
- Relieve itching and inflammation
- Restore skin barrier function
- Eliminate or avoid triggering factors
- Prevent infection and recurrence
🧾 General Treatment Approaches for All Types:
✅ 1. Topical Corticosteroids
First-line for reducing inflammation, redness, and itching
- Examples: Hydrocortisone, Betamethasone, Clobetasol
- Mild steroids for face and children; stronger ones for thick plaques
- Used in short courses to avoid skin thinning and side effects
✅ 2. Topical Emollients & Moisturizers
Help hydrate skin and repair the barrier
- Apply multiple times daily, especially after bathing
- Examples: petroleum jelly, urea-based creams, ceramide-rich lotions
✅ 3. Antihistamines
To relieve itching and help with sleep
- Oral options: Cetirizine, Loratadine (non-sedating), Diphenhydramine (sedating)
- May reduce scratching and inflammation
✅ 4. Antibiotics (Topical or Oral)
Used if secondary bacterial infection is present (e.g., Staphylococcus)
- Topical: Mupirocin or Fusidic acid
- Oral: Amoxicillin-clavulanate, Cephalexin, or Clindamycin
✅ 5. Antifungal Agents
For seborrheic dermatitis or fungal superinfections
- Topical: Ketoconazole, Clotrimazole
- Oral: Fluconazole, Itraconazole for resistant cases
✅ 6. Immunomodulators
For steroid-resistant or long-term control
- Topical Tacrolimus (Protopic) or Pimecrolimus (Elidel)
- Useful for atopic dermatitis, especially in sensitive areas (face, eyelids)
✅ 7. Phototherapy (UV Light Therapy)
For chronic or widespread dermatitis unresponsive to topical treatment
- Types: UVB, PUVA therapy
- Reduces inflammation and itching
✅ 8. Systemic Corticosteroids (Short-term)
For severe flare-ups
- Example: Prednisolone
- Should be tapered off gradually
- Not for long-term use due to side effects
✅ 9. Biologics (Advanced Therapy)
Used in moderate-to-severe atopic dermatitis
- Example: Dupilumab (IL-4 receptor blocker)
- Given by injection under specialist care
📋 Type-Specific Management
| 🧪 Type | 💊 Specific Treatment Highlights |
|---|---|
| Atopic Dermatitis | Moisturizers + topical steroids + antihistamines. Severe: immunosuppressants (e.g., cyclosporine) or biologics |
| Contact Dermatitis | Identify & eliminate trigger. Use mild topical steroids and emollients |
| Seborrheic Dermatitis | Antifungal shampoos (ketoconazole, selenium sulfide), mild corticosteroids for flares |
| Stasis Dermatitis | Elevation, compression stockings, topical steroids, wound care for ulcers |
| Dyshidrotic Dermatitis | Cool compresses, strong topical steroids, drying agents (e.g., Domeboro) |
| Perioral Dermatitis | Stop steroids, use topical metronidazole or oral tetracyclines |
| Photodermatitis | Avoid sun, use sunscreens, treat flares with steroids and antihistamines |
| Neurodermatitis | Break itch-scratch cycle: strong topical steroids, antihistamines, behavior therapy |
| Dermatitis Herpetiformis | Gluten-free diet, Dapsone for rapid symptom control |
🛠️ Surgical Management of Dermatitis
🔍 Overview:
Surgery is not a first-line treatment for any type of dermatitis. However, surgical intervention may be considered in the following situations:
✅ 1. Incision and Drainage (I&D) of Secondary Infections
- Indicated when:
- A localized abscess or pustule forms due to bacterial superinfection (commonly Staphylococcus aureus)
- Topical or oral antibiotics fail to resolve the infection
- Procedure:
- Local anesthesia is used
- The lesion is opened, and pus or fluid is drained
- Followed by wound cleaning, dressing, and antibiotic coverage
✅ 2. Debridement of Infected or Necrotic Tissue
- Indicated in:
- Chronic stasis dermatitis with ulcers
- Lichenified lesions with secondary infection
- Dermatitis with necrotic skin or tissue breakdown
- Procedure:
- Surgical debridement (removal of dead tissue) to promote healing
- May use scalpel, curette, or enzymatic agents
- Requires sterile technique and often wound care follow-up
✅ 3. Skin Biopsy
- Indicated for:
- Unclear diagnosis (to differentiate from psoriasis, lupus, fungal infections, skin cancers)
- Unusual or non-healing dermatitis
- Suspected autoimmune dermatitis (e.g., dermatitis herpetiformis)
- Procedure:
- Punch biopsy or excisional biopsy under local anesthesia
- Tissue sent to pathology for histopathological examination
✅ 4. Laser Therapy (in Selected Cases)
- Used for chronic lichenified or hypertrophic lesions
- May help reduce pigmentation changes or vascular dilation post-inflammation
- Rarely used unless dermatitis causes cosmetic disfigurement
✅ 5. Skin Grafting (Rare)
- Only in severe cases of dermatitis with non-healing ulcers or extensive tissue damage
- Especially in stasis dermatitis with large venous ulcers
- Requires multidisciplinary wound care and vascular support
⚠️ Note:
- Surgical interventions are supportive or diagnostic, not curative
- The mainstay of dermatitis treatment remains medical and nursing management
🩺 Nursing Management of Dermatitis
🎯 Nursing Goals:
- Relieve itching and inflammation
- Promote skin healing
- Prevent infection and recurrence
- Educate the patient about trigger avoidance and skin care
- Support psychological and emotional well-being
🗂️ I. Nursing Assessment
✅ Subjective Data:
- Ask about itching, burning, pain, or skin sensitivity
- Note history of allergies, past skin disorders, family history of eczema or dermatitis
- Inquire about exposure to triggers (e.g., soaps, detergents, metals, cosmetics, food, weather changes)
✅ Objective Data:
- Inspect skin for:
- Redness (erythema), rash, swelling, dryness
- Vesicles, oozing, crusting, scaling
- Scratches or excoriations from itching
- Signs of infection (pus, warmth, odor)
- Assess location, distribution, and type of lesion
🧾 II. Nursing Interventions
🔹 1. Skin Care and Comfort Measures:
- Apply prescribed topical medications: corticosteroids, antibiotics, antifungals
- Use cool compresses or oatmeal baths to soothe itching
- Keep skin clean and moisturized using unscented emollients
- Encourage gentle pat-drying after bathing (no rubbing)
- Trim fingernails short to prevent skin damage from scratching
- Use hypoallergenic soap and laundry products
- Dress the patient in soft, breathable clothing (e.g., cotton)
🔹 2. Infection Prevention:
- Maintain skin hygiene and wound care
- Monitor for signs of secondary bacterial infection: warmth, redness, swelling, pus
- Use aseptic technique when applying dressings
- Educate on avoiding scratching or breaking blisters
- Apply barrier creams for patients at risk of moisture-related dermatitis (e.g., incontinence)
🔹 3. Medication Administration and Monitoring:
- Administer:
- Antihistamines for itching (e.g., cetirizine, diphenhydramine)
- Oral antibiotics if infection is present
- Topical or systemic corticosteroids as ordered
- Monitor for side effects of steroids (skin thinning, increased blood sugar with systemic use)
- Document effectiveness of medications
🔹 4. Patient and Family Education:
- Educate on:
- Avoiding known triggers (chemicals, allergens, fabrics, heat, stress)
- Proper use and timing of topical medications
- Importance of moisturizing daily
- When to seek help (fever, spreading redness, yellow drainage)
- Encourage allergy testing if contact or atopic dermatitis is suspected
- Teach about lifestyle adjustments: reducing stress, dietary changes if applicable
🔹 5. Psychosocial Support:
- Address concerns about appearance, body image, and social embarrassment
- Encourage participation in support groups (especially for chronic cases like eczema or psoriasis)
- Support coping strategies for stress-related dermatitis
📊 III. Evaluation (Expected Outcomes):
✅ Patient reports reduction in itching and discomfort
✅ Skin lesions heal without infection or scarring
✅ Patient demonstrates correct use of medications and skin care practices
✅ Patient identifies and avoids triggers
✅ Maintains intact, healthy skin and stable emotional well-being
⚠️ COMPLICATIONS OF DERMATITIS
If untreated, poorly managed, or frequently recurrent, dermatitis can lead to various complications:
🔴 1. Secondary Bacterial Infections
- Scratching leads to breaks in skin → entry of Staphylococcus or Streptococcus
- Results in impetigo, cellulitis, or abscess formation
- May require antibiotics or incision & drainage
🟠 2. Chronic Lichenification
- Repeated scratching causes skin to thicken, darken, and become leathery
- Often seen in chronic atopic or neurodermatitis
🟡 3. Skin Atrophy
- Prolonged use of topical corticosteroids may cause thinning of skin, visible blood vessels, or stretch marks
🟢 4. Pigment Changes
- After healing, lesions may leave hyperpigmentation (dark spots) or hypopigmentation (light spots)
- More noticeable in dark-skinned individuals
🔵 5. Sleep Disturbances
- Constant itching and discomfort may cause insomnia, irritability, and fatigue
🟣 6. Psychological Impact
- Visible rashes can cause low self-esteem, embarrassment, and anxiety or depression
- Especially significant in adolescents or chronic cases
⚫ 7. Ulceration & Scarring
- Common in stasis dermatitis or infected dyshidrotic dermatitis
- Deep ulcers may lead to scars or long-term skin damage
📌 KEY POINTS ON DERMATITIS
✅ Definition: Dermatitis is inflammation of the skin, characterized by redness, itching, swelling, and lesions.
✅ Main Causes:
- Allergens, irritants, infections, genetics, autoimmune factors, and stress
✅ Common Types:
- Atopic, Contact, Seborrheic, Dyshidrotic, Nummular, Stasis, Neurodermatitis, Photodermatitis, Perioral
✅ Signs & Symptoms:
- Erythema, pruritus, vesicles, scaling, oozing, crusting, skin thickening
✅ Diagnosis:
- Clinical examination
- Patch testing (for allergies)
- Skin biopsy (if unclear or chronic)
- Blood tests (e.g., IgE, celiac panel for dermatitis herpetiformis)
✅ Medical Management:
- Topical corticosteroids, moisturizers, antihistamines, antibiotics/antifungals, immunomodulators, phototherapy
✅ Surgical Management (rare):
- I&D, debridement, skin biopsy, or wound care in severe/complicated cases
✅ Nursing Care:
- Promote comfort, prevent infection, teach trigger avoidance, support mental well-being
✅ Complications:
- Infection, lichenification, pigmentation changes, scarring, emotional distress
🧬 Dermatoses (Skin Diseases)
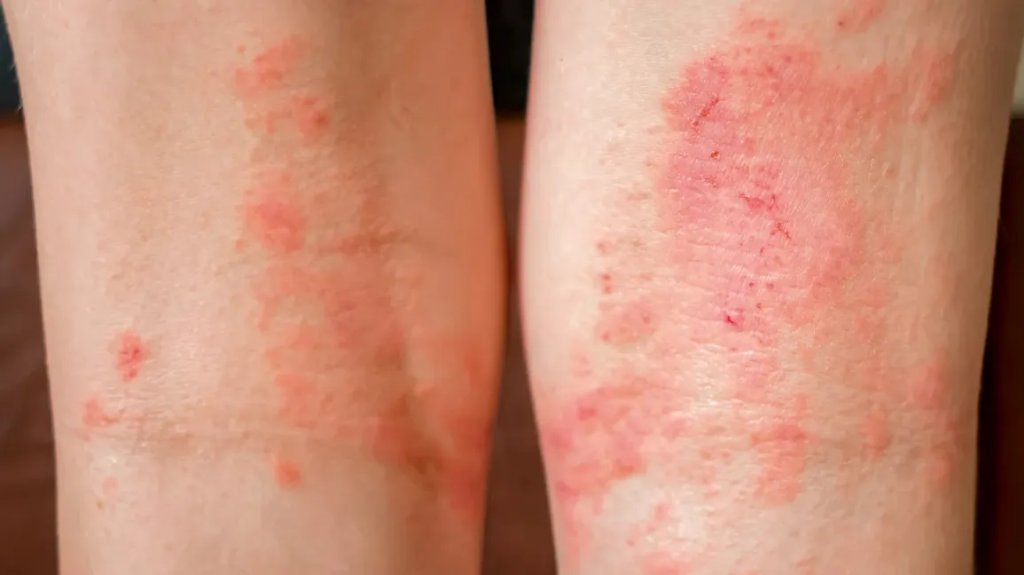
📌 Definition, Causes, and Types (Infectious & Non-Infectious)
✅ Definition:
Dermatoses (plural of dermatosis) refer to any abnormal skin condition or disease that affects the epidermis, dermis, or subcutaneous tissues. It is a broad, non-specific term used to describe various inflammatory, infectious, allergic, autoimmune, or neoplastic skin disorders.
🧾 Dermatosis ≠ dermatitis (dermatitis is just one type of dermatosis)
🔍 Causes of Dermatoses:
Dermatoses may result from:
| ⚠️ Cause | 📝 Examples |
|---|---|
| Infections | Bacteria, viruses, fungi, parasites |
| Allergies | Contact with allergens, food, environmental triggers |
| Autoimmune diseases | Lupus, psoriasis, pemphigus |
| Environmental factors | Sunlight, humidity, irritants, heat |
| Genetic predisposition | Atopic dermatitis, ichthyosis |
| Systemic illness | Diabetes, liver or kidney disease |
| Nutritional deficiencies | Pellagra (niacin), scurvy (vitamin C) |
| Drugs and chemicals | Reactions to medications or topical agents |
| Psychogenic factors | Stress-induced itching or lichen simplex |
🔬 TYPES OF DERMATOSES
Dermatoses are broadly divided into two categories:
🦠 I. Infectious Dermatoses
Skin diseases caused by microorganisms (bacteria, fungi, viruses, parasites)
✅ A. Bacterial Dermatoses
- Impetigo – superficial infection (Staph/Strep) with honey-colored crusts
- Cellulitis – deep skin infection with redness, warmth, swelling
- Erysipelas – superficial streptococcal skin infection with raised borders
- Folliculitis – infection of hair follicles
- Furuncle/Carbuncle – deeper abscesses
✅ B. Fungal Dermatoses
- Tinea (ringworm) – dermatophyte infection of skin, nails, or scalp
- Candidiasis – yeast infection, commonly in skin folds or mucosa
- Pityriasis versicolor – superficial fungal infection causing discoloration
✅ C. Viral Dermatoses
- Herpes simplex – grouped vesicles, usually around lips/genitals
- Herpes zoster (shingles) – reactivation of varicella-zoster virus
- Warts (verruca) – caused by HPV
- Molluscum contagiosum – dome-shaped viral lesions in children/adults
✅ D. Parasitic Dermatoses
- Scabies – caused by Sarcoptes scabiei, intensely itchy rash with burrows
- Pediculosis (lice) – lice infestation of scalp, body, or pubic area
- Leishmaniasis – parasitic infection causing ulcerative skin lesions
🚫 II. Non-Infectious Dermatoses
Skin conditions not caused by microorganisms, but by inflammation, immune disorders, allergens, or systemic disease
✅ A. Inflammatory/Allergic Dermatoses
- Atopic dermatitis – chronic, itchy eczema seen in children/adults
- Contact dermatitis – allergic/irritant response to substances
- Urticaria (hives) – red, itchy wheals due to allergens or medications
- Erythema multiforme – immune reaction with target lesions
✅ B. Autoimmune Dermatoses
- Psoriasis – chronic scaly plaques due to immune overactivity
- Lichen planus – itchy, purple, flat-topped papules
- Pemphigus vulgaris – life-threatening blistering disease
- Bullous pemphigoid – autoimmune blisters in elderly
✅ C. Genetic or Metabolic Dermatoses
- Vitiligo – loss of skin pigment due to melanocyte destruction
- Ichthyosis – inherited dry, scaly skin
- Porphyria cutanea tarda – blistering disorder due to liver enzyme defect
✅ D. Neoplastic Dermatoses
- Basal cell carcinoma, squamous cell carcinoma, melanoma
- Skin manifestations of internal cancers (e.g., paraneoplastic dermatoses)
🔬 PATHOPHYSIOLOGY OF DERMATOSES
The pathophysiology of dermatoses varies by the underlying cause (infectious vs non-infectious), but most share common pathways involving inflammation, immune response, or tissue damage.
✅ A. Infectious Dermatoses
- Bacterial:
- Bacteria invade the epidermis/dermis through breaks in the skin (cuts, insect bites)
- Immune cells (neutrophils/macrophages) respond → pus formation, redness, warmth, swelling
- Toxins may cause tissue necrosis or systemic symptoms
- Fungal:
- Dermatophytes, yeasts (like Candida) digest keratin in skin/hair/nails
- Cause inflammation, scaling, itching, and discoloration
- Immunocompromised patients are at higher risk
- Viral:
- Viruses infect epidermal cells, leading to vesicle or wart formation
- Herpes viruses (HSV, VZV) can remain dormant and reactivate later
- Local immune response causes inflammation and pain
- Parasitic:
- Parasites like mites or lice burrow into or live on the skin
- Trigger hypersensitivity reactions, intense itching, excoriation
✅ B. Non-Infectious Dermatoses
- Inflammatory/Allergic:
- Triggered by allergens or irritants → activate T-cells and mast cells
- Leads to histamine release, vasodilation, and inflammatory cell infiltration
- Autoimmune:
- The immune system attacks the skin’s own cells (e.g., basal cells, keratinocytes)
- Causes blistering, scaling, pigment loss, or plaques (as in psoriasis, vitiligo)
- Genetic/Metabolic:
- Mutations lead to abnormal keratinization (ichthyosis) or pigment production (albinism)
- In metabolic dermatoses, toxins or deficient enzymes cause skin sensitivity and fragility
🚨 SIGNS & SYMPTOMS OF DERMATOSES
| 🩹 Symptom | 🔍 Description |
|---|---|
| Itching (pruritus) | Common in both infectious (e.g., scabies, tinea) and allergic types (eczema) |
| Redness (erythema) | Due to vasodilation in inflamed skin |
| Rash/Lesions | Papules, pustules, plaques, vesicles, macules depending on cause |
| Pain or burning | Seen in viral infections (herpes) or infected lesions |
| Swelling (edema) | Often accompanies infection or hypersensitivity |
| Discoloration | Hypo/hyperpigmentation in vitiligo, post-inflammatory states |
| Crusting/oozing | Due to vesicle rupture or secondary infection |
| Thickening/scaling | Seen in psoriasis, lichen simplex, ichthyosis |
| Ulcers or blisters | Autoimmune dermatoses (pemphigus, bullous pemphigoid), stasis ulcers |
| Nail/hair changes | Brittle nails, hair thinning or loss in fungal and autoimmune skin diseases |
📍 Lesions may be localized or generalized, symmetrical or asymmetrical, acute or chronic.
🧪 DIAGNOSIS OF DERMATOSES
✅ 1. Clinical Examination
- Visual inspection: type, shape, color, distribution of lesions
- History-taking: onset, duration, progression, exposure history, associated symptoms
- Examine hair, nails, mucous membranes
✅ 2. Laboratory Tests & Diagnostic Tools
| 🧪 Test | 💡 Purpose |
|---|---|
| Skin scrapings (KOH test) | Diagnose fungal infections (e.g., tinea, candidiasis) |
| Tzanck smear | Identifies multinucleated cells in viral infections (e.g., herpes simplex) |
| Gram stain & culture | For bacterial identification (e.g., impetigo, cellulitis) |
| Skin biopsy | For autoimmune, neoplastic, or unclear dermatoses |
| Patch testing | Identifies contact allergens in allergic dermatitis |
| Dermoscopy | Non-invasive tool for pigmented lesions (e.g., melanoma vs benign mole) |
| Blood tests | IgE (atopic eczema), ANA (lupus), antibodies (pemphigus, dermatitis herpetiformis) |
| Wood’s lamp examination | Detects fungal infections or pigment changes under UV light |
💊🛠️ Medical and Surgical Management of Dermatoses
💊 MEDICAL MANAGEMENT
Medical treatment depends on the cause, type, severity, and location of the dermatosis. Here’s a breakdown:
🦠 A. Management of Infectious Dermatoses
| 🧪 Type | 💊 Treatment |
|---|---|
| Bacterial | – Topical antibiotics (e.g., mupirocin, fusidic acid) |
markdownCopyEdit - Oral antibiotics (e.g., **cephalexin**, **amoxicillin-clavulanate**) for cellulitis, abscesses
- Maintain hygiene, wound care |
| Fungal | – Topical antifungals (e.g., clotrimazole, ketoconazole)
– Oral antifungals (e.g., fluconazole, terbinafine) for extensive tinea or nail infections
– Dry the skin thoroughly to prevent recurrence | | Viral | – Antivirals (e.g., acyclovir, valacyclovir) for herpes simplex/zoster
– Cryotherapy or salicylic acid for warts
– Molluscum contagiosum may resolve on its own | | Parasitic | – Permethrin 5% cream or ivermectin for scabies
– Malathion or permethrin lotion for pediculosis (lice)
– Antiprotozoal drugs (e.g., amphotericin B) for leishmaniasis |
🚫 B. Management of Non-Infectious Dermatoses
| 🧬 Condition Type | 💊 Treatment |
|---|---|
| Allergic/Inflammatory | – Topical corticosteroids (e.g., hydrocortisone, betamethasone) |
markdownCopyEdit - **Antihistamines** for itching
- Emollients and moisturizers
- **Avoid allergens/irritants** |
| Autoimmune | – Systemic corticosteroids (e.g., prednisolone)
– Immunosuppressants (e.g., methotrexate, azathioprine)
– Biologics (e.g., dupilumab for atopic dermatitis, infliximab for psoriasis)
– Topical immunomodulators (e.g., tacrolimus, pimecrolimus) | | Psoriasis | – Topical treatments (coal tar, salicylic acid)
– Phototherapy (UVB)
– Systemic: methotrexate, cyclosporine, biologics | | Pigmentary Disorders (e.g., vitiligo) | – Topical steroids or tacrolimus
– PUVA therapy (psoralen + UVA)
– Cosmetic camouflage products |
🧠 Supportive Therapies:
- Moisturizers/emollients to restore skin barrier
- Antiseptics (e.g., chlorhexidine) for wound cleansing
- Zinc oxide or calamine lotion for soothing itchy skin
- Psychological support for visible or chronic dermatoses (e.g., psoriasis, vitiligo)
🛠️ SURGICAL MANAGEMENT
Surgical treatment is not routine for dermatoses but may be needed in specific or complicated cases.
✅ 1. Incision and Drainage (I&D)
- For abscesses or furuncles that are fluctuant
- Performed under local anesthesia
- Followed by antibiotics and dressing care
✅ 2. Skin Biopsy
- For diagnosis of unclear or persistent dermatoses (e.g., psoriasis, lupus, pemphigus)
- Types: punch biopsy, shave biopsy, or excisional biopsy
✅ 3. Cryotherapy or Electrocautery
- Used to remove warts, molluscum, or seborrheic keratoses
- Involves freezing or burning off lesions
✅ 4. Surgical Excision
- For neoplastic dermatoses like:
- Basal cell carcinoma
- Squamous cell carcinoma
- Melanoma
- Ensures complete lesion removal with clear margins
✅ 5. Skin Grafting or Flap Surgery
- For chronic ulcers, necrotic lesions, or post-debridement wounds (e.g., in stasis dermatitis)
- Helps restore integrity and function of damaged skin
✅ 6. Laser Therapy
- For vascular dermatoses, psoriasis plaques, or cosmetic scar reduction
- Also used in pigment correction (e.g., vitiligo, birthmarks)
🩺 Nursing Management of Dermatoses
🎯 Nursing Objectives:
- Relieve discomfort, itching, and pain
- Prevent or control infection and spread
- Promote healing of skin lesions
- Educate the patient on trigger avoidance and skincare
- Address emotional and psychosocial concerns
🗂️ I. Assessment (Subjective and Objective)
✅ Subjective Data:
- Complaint of itching, burning, pain, or skin tightness
- Past history of allergies, infections, or autoimmune disease
- Exposure to irritants, allergens, new medications, or travel
- Impact on daily life, self-image, and mood
✅ Objective Data:
- Inspect skin for:
- Lesion type (macules, papules, vesicles, pustules, plaques, ulcers)
- Distribution and location
- Presence of scaling, crusting, oozing, bleeding
- Signs of infection (redness, warmth, pus, odor)
- Assess hair, nails, and mucous membranes
- Monitor vital signs (fever may suggest systemic infection)
🧾 II. Nursing Interventions
🔹 1. Skin Care and Symptom Relief
- Apply topical medications (antibiotics, antifungals, corticosteroids) as prescribed
- Use cool compresses, calamine lotion, or colloidal oatmeal baths to relieve itching
- Keep affected area clean and dry
- Avoid friction, tight clothing, and scratching
- Encourage use of moisturizers or emollients after bathing
🔹 2. Infection Prevention
- Use gloves during dressing changes or handling infected lesions
- Maintain aseptic technique for wound care
- Monitor for secondary infections (swelling, pus, fever)
- Isolate patients with highly contagious dermatoses (e.g., scabies, impetigo) if needed
- Educate on hand hygiene and hygiene of personal items
🔹 3. Medication Administration
- Administer:
- Oral antihistamines (e.g., cetirizine, diphenhydramine) for pruritus
- Systemic antibiotics, antivirals, antifungals, corticosteroids if prescribed
- Observe for side effects: GI upset, drowsiness, allergic reactions
- Reinforce adherence to treatment regimen, especially in chronic dermatoses
🔹 4. Patient and Family Education
- Instruct patient to:
- Avoid known triggers (e.g., allergens, irritants, food, weather)
- Use hypoallergenic soaps and mild detergents
- Avoid self-medicating or overuse of topical steroids
- Perform proper skin hygiene without over-washing
- Avoid scratching or picking at lesions to prevent infection or scarring
- Educate family if the condition is contagious (e.g., scabies, fungal infections)
🔹 5. Psychosocial Support
- Address body image issues and self-esteem concerns
- Support coping with chronic conditions (e.g., psoriasis, vitiligo)
- Encourage support groups or counseling if needed
- Promote compliance by building trust and involving the patient in care
📊 III. Evaluation (Expected Outcomes):
✅ Skin lesions reduce in size, redness, and discomfort
✅ Patient reports less itching, better sleep, and improved mood
✅ No signs of secondary infection or complication
✅ Patient adheres to treatment, hygiene, and lifestyle advice
✅ Emotional needs are addressed; patient is confident and reassured
⚠️ COMPLICATIONS OF DERMATOSES
If dermatoses are not identified, treated, or controlled properly, they may lead to the following complications:
🦠 1. Secondary Bacterial Infections
- Occur due to scratching, poor hygiene, or improper treatment
- Common organisms: Staphylococcus aureus, Streptococcus pyogenes
- May result in cellulitis, abscess, impetigo, or sepsis in severe cases
🧱 2. Lichenification (Skin Thickening)
- Repeated scratching or rubbing leads to thickened, leathery skin
- Seen in chronic eczema, neurodermatitis
🎯 3. Hyperpigmentation or Hypopigmentation
- Healing skin may leave dark spots (post-inflammatory hyperpigmentation)
- Light spots may occur in vitiligo or after severe inflammation
🔁 4. Chronicity and Recurrence
- Chronic dermatoses (e.g., psoriasis, atopic dermatitis) have repeated flare-ups
- Can affect quality of life, sleep, work, and emotional well-being
🔥 5. Psychological Impact
- Embarrassment, anxiety, depression, or social withdrawal due to visible lesions
- Especially in adolescents or those with facial/body involvement
🧬 6. Scarring and Ulceration
- Improper treatment of infected or autoimmune dermatoses (e.g., bullous pemphigoid) can lead to permanent scars or ulcers
🧪 7. Drug Side Effects
- Long-term use of topical steroids may cause:
- Skin thinning (atrophy)
- Stretch marks
- Steroid-induced acne or perioral dermatitis
- Systemic immunosuppressants may lead to infection risk
📌 KEY POINTS ON DERMATOSES
✅ Definition: Dermatoses are any non-specific skin diseases, which may be infectious or non-infectious
✅ Common Causes:
- Infections (bacterial, viral, fungal, parasitic)
- Allergens, irritants, autoimmune conditions
- Genetic and metabolic disorders
✅ Signs & Symptoms:
- Itching, redness, lesions (e.g., papules, pustules, plaques)
- Dryness, scaling, blisters, or ulcers
- Localized or generalized skin involvement
✅ Diagnosis:
- Based on history, physical exam, and tests like:
- KOH mount, biopsy, Gram stain, patch testing, antibody screening
✅ Medical Treatment:
- Topical agents: corticosteroids, antibiotics, antifungals
- Systemic therapy: antihistamines, antibiotics, antivirals, immunosuppressants
- Biologics and phototherapy for chronic cases
✅ Surgical Treatment (if needed):
- Incision & drainage, biopsy, excision, cryotherapy, or skin grafts in selected cases
✅ Nursing Management:
- Skin care, infection control, medication adherence
- Trigger avoidance, hygiene, emotional support
✅ Complications:
- Infection, scarring, pigment changes, chronic skin thickening, emotional distress
🧴 Acne (Acne Vulgaris)
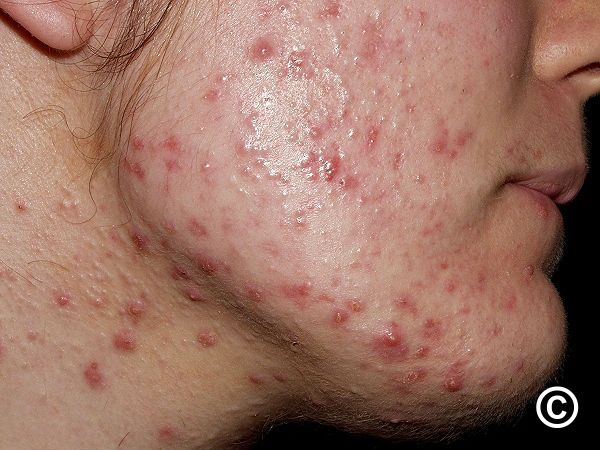
📌 Definition and Causes
✅ Definition:
Acne is a chronic inflammatory skin disorder of the pilosebaceous unit (hair follicle + sebaceous gland), characterized by the formation of comedones (blackheads and whiteheads), papules, pustules, nodules, and cysts. It primarily affects adolescents but can occur at any age.
🔍 Most commonly appears on the face, chest, shoulders, and back, where sebaceous glands are most active.
🔍 Causes of Acne:
Acne is a multifactorial condition involving several interrelated mechanisms:
🔹 1. Increased Sebum Production
- Triggered by hormones (especially androgens during puberty)
- Sebaceous glands enlarge and produce excess oil
🔹 2. Follicular Hyperkeratinization
- Dead skin cells clump together and block the hair follicle opening
- Leads to formation of comedones (open = blackhead, closed = whitehead)
🔹 3. Bacterial Colonization
- Cutibacterium acnes (formerly Propionibacterium acnes) colonizes the blocked follicles
- Breaks down sebum into irritating fatty acids → inflammation
🔹 4. Inflammatory Response
- Immune system responds to bacteria and blockage → causes red, swollen papules, pustules, or nodules
🔹 5. Hormonal Factors
- Puberty, menstrual cycle, PCOS, or use of androgenic steroids increase acne risk
🔹 6. Other Contributing Factors
| ⚠️ Factor | 📝 Details |
|---|---|
| Genetic predisposition | Family history of acne increases risk |
| Stress | Increases cortisol and worsens inflammation |
| Diet | High glycemic index foods, dairy, or chocolate may aggravate acne in some |
| Medications | Steroids, lithium, phenytoin, isoniazid |
| Cosmetics | Oil-based or comedogenic products can block pores |
| Environmental | Humidity, sweat, and pollution may exacerbate acne |
🔢 Types of Acne (Acne Vulgaris)
📌 Based on Lesion Type, Severity, and Special Conditions
🔷 I. Based on Lesion Type
1️⃣ Non-Inflammatory Acne
- Characterized by comedones (no redness or swelling)
🔹 Types:
- Open comedones (blackheads):
- Hair follicles plugged with sebum + dead cells
- Surface remains open and oxidizes → dark appearance
- Closed comedones (whiteheads):
- Follicle plugged but covered by skin
- Appears as small, skin-colored bumps
2️⃣ Inflammatory Acne
- Characterized by redness, swelling, and pain due to immune response and bacterial activity
🔹 Types:
- Papules: Small, red, tender bumps
- Pustules: Similar to papules, but filled with pus (yellow/white center)
- Nodules: Large, painful, solid lumps deep within the skin
- Cysts: Deep, pus-filled, inflamed lesions; may scar
🔶 II. Based on Severity
| 💢 Severity | 🩺 Description |
|---|---|
| Mild | Few comedones, occasional papules/pustules, no scarring |
| Moderate | More widespread comedones, papules, and pustules |
| Severe | Multiple inflamed nodules, cysts, possible scarring |
🔵 III. Special Types of Acne
✅ 1. Acne Conglobata
- Severe, chronic, disfiguring acne
- Numerous nodules, abscesses, and cysts interconnected under the skin
- Often leads to deep scarring
- More common in males and may be associated with steroid abuse
✅ 2. Acne Fulminans
- Sudden, severe ulcerative acne with systemic symptoms (fever, joint pain)
- Occurs mainly in young males
- May be a hypersensitivity reaction
- Requires systemic steroids and antibiotics
✅ 3. Acne Mechanica
- Triggered by heat, friction, or pressure on the skin
- Common in athletes (e.g., from helmets, straps, backpacks)
- Appears as papules or pustules on pressure areas
✅ 4. Acne Cosmetica
- Caused by comedogenic cosmetic products
- Common in women; lesions are usually non-inflammatory
- Usually affects forehead, cheeks, and chin
✅ 5. Hormonal Acne
- Seen in teenagers, adult women, or PCOS patients
- Worsens before menstruation
- Commonly located on jawline, chin, and neck
- May need hormonal therapy (e.g., OCPs, anti-androgens)
✅ 6. Drug-Induced Acne
- Caused by medications such as:
- Steroids (steroid acne)
- Isoniazid, lithium, phenytoin
- Typically monomorphic (lesions look similar), often sudden onset
🧬 Pathophysiology of Acne (All Types)
✅ Overview of Acne Pathophysiology
All types of acne share a common core mechanism, which involves the pilosebaceous unit (hair follicle + sebaceous gland). Acne begins with blockage and inflammation of this unit due to multiple interacting factors:
🔄 Step-by-Step Mechanism (Common to All Types):
- ↑ Sebum Production
- Stimulated by androgens during puberty or hormonal imbalance
- Sebaceous glands secrete excess oil
- Follicular Hyperkeratinization
- Increased turnover of skin cells in the follicle
- Cells stick together and block the follicular opening → comedone formation
- Bacterial Colonization
- Cutibacterium acnes (formerly Propionibacterium acnes) thrives in sebum-rich environment
- Produces enzymes and pro-inflammatory factors
- Inflammation
- Body responds with immune cells → swelling, redness, pus formation
- Deep inflammation leads to nodules or cysts
🔬 Type-wise Pathophysiology
1️⃣ Non-Inflammatory Acne (Comedonal Acne)
- No immune or bacterial involvement
- Hyperkeratinization + sebum retention → clogged follicle
- Open comedones (blackheads): pore remains open, sebum oxidizes
- Closed comedones (whiteheads): follicle is blocked with no air exposure
2️⃣ Inflammatory Acne (Papules, Pustules, Nodules, Cysts)
- Blocked follicles are colonized by C. acnes
- Bacterial enzymes break down sebum into inflammatory fatty acids
- Immune system recruits neutrophils, macrophages → leads to:
- Papules: early inflammation
- Pustules: pus-filled inflammatory lesion
- Nodules: deeper dermal inflammation
- Cysts: fluid-filled deep lesions, can rupture → scarring
3️⃣ Acne Conglobata
- Severe form with interconnected nodules and cysts
- Results from intense immune response, possible genetic predisposition
- May involve systemic symptoms and extensive tissue destruction
4️⃣ Acne Fulminans
- Sudden, explosive onset of nodules/ulcers with systemic inflammation
- Caused by hypersensitive immune reaction to C. acnes
- Leads to necrosis, ulceration, fever, arthralgia
- Often associated with use of androgens or in adolescent males
5️⃣ Acne Mechanica
- Triggered by repetitive friction, heat, or pressure (e.g., helmets, sports gear)
- Causes mechanical blockage of follicles → inflammation
- Exacerbates underlying acne or creates new lesions
6️⃣ Acne Cosmetica
- Caused by comedogenic substances in skin or hair products
- Blocks follicles and prevents normal oil flow
- Leads to non-inflammatory microcomedones or whiteheads
7️⃣ Hormonal Acne
- Excess androgens (puberty, PCOS, stress, medications) → increased sebum
- Affects chin, jawline, and neck
- Cyclical flares (often before menstruation)
- Resistant to standard treatment; may need hormonal therapy
8️⃣ Drug-Induced Acne
- Caused by certain medications (e.g., steroids, lithium, phenytoin)
- Drugs alter skin’s immune or hormonal balance → follicular plugging and inflammation
- Lesions often look monomorphic (same size/type) and appear suddenly
🔁 Key Inflammatory Pathways Involved:
- IL-1, TNF-α, and IL-8: drive immune cell recruitment
- Lipase enzymes from C. acnes: break down sebum → fatty acids
- Toll-like receptors (TLRs): recognize bacterial components → activate inflammation
🔍 Signs & Symptoms and Diagnosis of Acne
✅ Signs and Symptoms of Acne
Acne presents with different types of lesions based on severity and skin response. Symptoms typically affect areas with high sebaceous (oil) gland density: face, chest, shoulders, upper back.
🔷 A. Types of Acne Lesions
| 💠 Lesion Type | 📝 Description |
|---|---|
| Open comedones | Blackheads – open pores filled with oxidized sebum and keratin |
| Closed comedones | Whiteheads – clogged pores beneath the skin surface |
| Papules | Small, red, tender bumps without pus |
| Pustules | Papules filled with pus (white/yellow center) |
| Nodules | Large, painful, solid lumps under the skin |
| Cysts | Deep, pus-filled lesions; soft and painful; may scar |
🔶 B. Associated Symptoms
- Oily skin (seborrhea)
- Itching or tenderness in inflamed areas
- Pain in deeper nodules or cysts
- Scarring or pigmentation (especially in darker skin types)
- Psychosocial effects: anxiety, embarrassment, low self-esteem (especially in adolescents)
📍 Common Sites of Acne:
- Face (forehead, cheeks, chin, jawline)
- Back (bacne)
- Chest
- Shoulders and upper arms
- Neck and jawline (especially in hormonal acne)
🧪 Diagnosis of Acne
Diagnosis is primarily clinical — based on visual inspection and history.
✅ 1. History-Taking
- Onset, duration, and progression of acne
- Menstrual cycle-related flares (hormonal acne)
- Use of cosmetics, topical products, or medications
- Family history of acne or scarring
- Presence of stress, diet patterns, or endocrine disorders (e.g., PCOS)
✅ 2. Physical Examination
- Evaluate type and distribution of lesions: comedones, pustules, nodules, cysts
- Check for post-inflammatory pigmentation, scars, or excoriations
- Look for signs of acne conglobata or fulminans in severe cases
✅ 3. Grading the Severity (for treatment planning)
- Mild: mostly comedones ± few papules
- Moderate: comedones, papules, and pustules
- Severe: nodules, cysts, abscesses, or scarring
✅ 4. Investigations (if indicated):
🔹 Hormonal Workup (for females with hormonal acne or irregular periods):
- Serum testosterone, DHEAS, LH/FSH, prolactin
- Pelvic ultrasound (for polycystic ovarian syndrome – PCOS)
🔹 Skin Swab or Culture:
- Rarely needed, unless:
- Suspecting secondary infection
- Treatment resistance or atypical lesions
🔹 Biopsy (very rare):
- Done if acne-like lesions are suspicious for other skin disorders (e.g., lupus, folliculitis)
💊 Medical Management of Acne
🎯 Goals of Treatment:
- Reduce sebaceous gland activity
- Decrease bacterial colonization (Cutibacterium acnes)
- Prevent comedone formation and reduce inflammation
- Prevent scarring and improve skin appearance
✅ I. Topical Therapy (First-line for Mild to Moderate Acne)
| 💠 Category | 💊 Examples | 🔍 Mechanism of Action |
|---|---|---|
| Keratolytics / Retinoids | Tretinoin, Adapalene, Tazarotene | Normalize keratinization, unclog pores |
| Antibiotics | Clindamycin, Erythromycin | Inhibit C. acnes and reduce inflammation |
| Antibacterials | Benzoyl peroxide | Kills bacteria and prevents resistance when combined with antibiotics |
| Combination creams | Clindamycin + Benzoyl peroxide, Adapalene + BPO | Broad-spectrum and effective for papulopustular acne |
⚠️ Note: Start with low concentrations to avoid irritation.
✅ II. Systemic Therapy (For Moderate to Severe Acne)
🔹 1. Oral Antibiotics
- Used in: Moderate to severe inflammatory acne
- Common drugs:
- Doxycycline (most preferred)
- Minocycline
- Azithromycin or Erythromycin (for those intolerant to tetracyclines)
- Limit use to 3–6 months to reduce resistance
- Always combine with topical benzoyl peroxide to prevent bacterial resistance
🔹 2. Hormonal Therapy (for Females with Hormonal Acne)
| 🌸 Drug | 🧬 Effect |
|---|---|
| Combined oral contraceptives (OCPs) | Regulate androgens, reduce sebum production |
| Anti-androgens (Spironolactone) | Blocks androgen receptors in sebaceous glands |
| Cyproterone acetate (in some OCPs) | Suppresses sebum via androgen inhibition |
🚺 Especially useful in women with acne along jawline/chin, PCOS, or premenstrual flares.
🔹 3. Oral Isotretinoin (Accutane)
- Indicated for:
- Severe nodulocystic or recalcitrant acne
- Acne with scarring or failure of other therapies
- Mechanism:
- Reduces sebum production, normalizes keratinization, and has anti-inflammatory effects
- The only treatment that targets all four acne pathways
- Monitoring Required:
- Liver function tests (LFTs)
- Lipid profile
- Pregnancy test (before and during treatment) – contraindicated in pregnancy (Category X)
- Educate on dry skin, cheilitis, photosensitivity, mood changes
🧴 III. Supportive Skin Care Measures
- Use non-comedogenic (oil-free) moisturizers and sunscreens
- Avoid harsh scrubbing, oily products, or squeezing pimples
- Wash face twice daily with mild cleanser
- Maintain hydration and balanced diet
🔄 Treatment Based on Acne Severity
| 🧪 Severity | 💊 Treatment Approach |
|---|---|
| Mild | Topical retinoid ± benzoyl peroxide |
| Moderate | Topical retinoid + topical antibiotic or oral antibiotic + BPO |
| Severe | Oral isotretinoin or hormonal therapy (females) |
🛠️ Surgical / Procedural Management of Acne
Surgical or dermatological procedures are adjuncts to medical therapy and are useful in:
- Severe acne,
- Acne scars, or
- Cases not fully responding to topical/systemic treatments.
✅ 1. Comedone Extraction (Manual Extraction)
- Used for: Non-inflammatory acne (open and closed comedones)
- Procedure:
- Done with a sterile comedone extractor
- Pressure is applied to remove blackheads or whiteheads
- Reduces cosmetic concerns and prevents inflammation if done properly
- Not advised for inflamed pustules or cysts
✅ 2. Intralesional Corticosteroid Injections
- Used for: Large, painful nodules or cysts
- Drug: Triamcinolone acetonide injected directly into the lesion
- Reduces inflammation, swelling, and pain rapidly
- Prevents scarring and speeds up healing
- Often used in nodulocystic or hormonal acne flares
✅ 3. Chemical Peels
- Used for: Post-acne pigmentation, superficial scars, and comedonal acne
- Agents used:
- Salicylic acid (beta hydroxy acid) – comedolytic
- Glycolic acid or Lactic acid – improves skin tone and texture
- Peels help in removing dead skin, unclogging pores, and promoting collagen production
✅ 4. Laser and Light Therapies
- Used for: Inflammatory acne, oil gland reduction, and scar improvement
- Common types:
- Blue light therapy – kills C. acnes bacteria
- Intense Pulsed Light (IPL) – reduces redness and pigment
- Fractional CO₂ laser – resurfaces skin and reduces scars
⚠️ These treatments are usually done in multiple sessions and may need topical numbing.
✅ 5. Acne Scar Revision Procedures
For post-acne scarring, the following minor surgical options are used:
| Procedure | Use |
|---|---|
| Microneedling (Dermaroller) | Stimulates collagen for shallow acne scars |
| Subcision | Breaks fibrous bands under depressed scars |
| Punch excision | Removes deep, pitted scars |
| Laser resurfacing | Evens out skin texture and stimulates healing |
| Dermabrasion/Microdermabrasion | Physical exfoliation of superficial scars |
| Fillers | For shallow, atrophic scars (e.g., hyaluronic acid) |
✅ 6. Drainage and Surgical Excision
- Used in severe, painful cysts or abscesses
- Procedure:
- Sterile incision and drainage (I&D) under local anesthesia
- May be followed by oral antibiotics and dressing care
- Reserved for resistant or infected lesions
🧠 Important Considerations:
- All procedures must be performed by qualified dermatologists or trained professionals
- Post-procedure care is crucial to avoid infections or pigmentation
- Sun protection is a must after chemical peels or laser therapies
- Not suitable for patients with active infections or keloid tendencies
🩺 Nursing Management of Acne
🎯 Goals of Nursing Care:
- Alleviate inflammation, pain, and discomfort
- Promote healing of acne lesions
- Prevent infection, scarring, and recurrence
- Provide emotional support for body image concerns
- Educate patients on skin care, medication adherence, and trigger avoidance
🗂️ I. Nursing Assessment
✅ Subjective Data:
- Complaints of pain, itching, burning, or sensitivity
- Onset, duration, progression, and location of acne
- History of:
- Cosmetic use, hormonal issues, family history, stress
- Medications or recent lifestyle changes
- Menstrual irregularities (in females)
✅ Objective Data:
- Inspect for:
- Type of lesions: comedones, papules, pustules, nodules, cysts
- Distribution: face, chest, back, shoulders
- Scarring, pigmentation, or signs of secondary infection
- Assess for psychological impact: embarrassment, anxiety, low self-esteem
🧾 II. Nursing Interventions
🔹 1. Skin Care and Hygiene Education
- Advise gentle face washing twice daily with mild cleanser
- Avoid scrubbing, harsh soaps, or frequent washing
- Recommend non-comedogenic (oil-free) skin care and makeup products
- Instruct patient not to squeeze or pick lesions — prevents scarring and infection
🔹 2. Medication Administration and Monitoring
- Administer topical/oral medications as prescribed:
- Retinoids, antibiotics, benzoyl peroxide, hormonal therapy, isotretinoin
- Teach proper application of topical treatments:
- Apply to entire affected area, not just individual lesions
- Warn about initial irritation or dryness
- Monitor for side effects:
- Oral antibiotics → GI upset
- Retinoids → photosensitivity, skin peeling
- Isotretinoin → mood changes, dry skin, teratogenicity
🔹 3. Infection Prevention
- Maintain clean linens and towels
- Teach patients to avoid sharing personal items
- Educate on recognizing signs of secondary infection (redness, pus, warmth)
🔹 4. Psychosocial Support
- Provide a non-judgmental, supportive approach
- Discuss emotional and social concerns related to acne
- Refer to a counselor or support group if body image distress is significant
- Reinforce that acne is treatable and help them stay positive during therapy
🔹 5. Diet and Lifestyle Counseling
- Encourage a balanced, low-glycemic diet
- Reduce processed foods, dairy, and sugary items (if patient reports correlation)
- Encourage stress-reduction techniques (yoga, sleep hygiene, exercise)
🔹 6. Monitoring and Follow-up
- Track progress during follow-up visits
- Evaluate response to medications and adjust if necessary
- Reinforce long-term adherence even after improvement
- Counsel on sun protection, especially if using retinoids or after procedures
📊 III. Evaluation (Expected Outcomes)
✅ Reduction in acne lesions and inflammation
✅ Improved skin appearance and patient satisfaction
✅ Patient verbalizes understanding of medications and skin care
✅ No signs of secondary infection or scarring
✅ Better emotional and psychological well-being
⚠️ Complications of Acne
If untreated, poorly managed, or in severe cases, acne can lead to both physical and psychological complications:
✅ A. Physical Complications
| 🔥 Complication | 📝 Description |
|---|---|
| Scarring | Depressed (ice-pick, boxcar, rolling) or hypertrophic/keloid scars after cystic acne |
| Post-inflammatory hyperpigmentation | Dark spots left after acne heals; more common in darker skin tones |
| Post-inflammatory hypopigmentation | Light spots where acne was inflamed; seen in healing stage |
| Secondary bacterial infection | Especially from squeezing or picking lesions; may lead to cellulitis or abscess |
| Sebaceous hyperplasia | Enlarged oil glands after chronic inflammation |
| Acne fulminans | Rare, severe, ulcerative acne with systemic symptoms (fever, joint pain) |
| Chronicity/recurrence | Recurrent flares despite treatment, often hormonal or medication-related |
✅ B. Psychological Complications
- Depression or anxiety due to facial disfigurement
- Social withdrawal, low self-esteem, poor body image
- Increased risk of emotional stress, especially in adolescents and young adults
📌 Key Points Summary of Acne (Acne Vulgaris)
✅ Definition: A chronic inflammatory disorder of the pilosebaceous unit involving comedones, papules, pustules, nodules, or cysts
✅ Common Sites: Face, chest, shoulders, back
✅ Causes:
- ↑ Sebum (androgens)
- Follicular plugging
- C. acnes bacteria
- Inflammation
- Genetics, diet, stress, cosmetics, hormones
✅ Types:
- Non-inflammatory: blackheads, whiteheads
- Inflammatory: papules, pustules, nodules, cysts
- Special types: hormonal, cosmetic, mechanical, drug-induced, conglobata
✅ Diagnosis:
- Clinical examination
- Hormonal tests for suspected PCOS
- Graded by severity: mild, moderate, severe
✅ Medical Treatment:
- Topicals: retinoids, benzoyl peroxide, clindamycin
- Systemic: antibiotics, isotretinoin, hormonal therapy (OCPs, spironolactone)
- Supportive: cleansers, moisturizers, sun protection
✅ Surgical/Procedural:
- Comedone extraction, chemical peels, laser therapy, intralesional steroids
- Scar treatments: microneedling, subcision, fillers
✅ Nursing Care:
- Education on skin care and triggers
- Medication adherence
- Psychological support
- Infection prevention
✅ Complications:
- Scarring, pigmentation changes
- Infection, psychosocial distress, recurrence
🌿 Allergies

📌 Definition and Causes
✅ Definition:
An allergy is an abnormal immune response to a substance (called an allergen) that is harmless to most people. The immune system overreacts, producing histamine and other chemicals, leading to inflammation and allergy symptoms.
🔬 It is a hypersensitivity reaction, usually of Type I (immediate hypersensitivity), mediated by IgE antibodies.
🧠 Key Concept:
In allergies, the immune system treats a non-harmful substance (like dust or pollen) as a threat, triggering a reaction.
🔍 Causes of Allergies (Common Allergens)
Allergens can be inhaled, ingested, injected, or come into skin contact.
🏠 1. Environmental Allergens (Airborne)
- Pollen (grass, trees, weeds) – causes seasonal allergic rhinitis (hay fever)
- Dust mites – common indoor trigger
- Mold spores – thrive in damp environments
- Animal dander (skin flakes, saliva, urine of pets)
- Cockroach debris
🍤 2. Food Allergens
- Milk, eggs, peanuts, tree nuts, shellfish, wheat, soy
- Can cause hives, vomiting, anaphylaxis in sensitive individuals
💊 3. Drug Allergens
- Penicillin, sulfa drugs, NSAIDs, anticonvulsants, vaccines
- Can cause rashes, itching, or life-threatening anaphylaxis
🌼 4. Insect Venoms
- Bee, wasp, hornet, or ant stings
- Can lead to localized swelling or systemic allergic reaction
🧴 5. Contact Allergens
- Nickel, latex, fragrances, dyes, soaps, plants (e.g., poison ivy)
- Cause allergic contact dermatitis
🔁 6. Occupational Allergens
- Chemical fumes, industrial dust, latex gloves
- Seen in healthcare workers, hairdressers, lab technicians, and farmers
🔢 Types of Allergies
Allergies can be classified into clinical types based on how allergens enter the body, and what systems they affect. Most are IgE-mediated hypersensitivity reactions (Type I).
🌬️ 1. Respiratory Allergies (Inhaled Allergens)
🔹 A. Allergic Rhinitis (Hay Fever)
- Triggered by: Pollen, dust mites, pet dander, mold
- Symptoms: Sneezing, nasal congestion, runny nose, itchy eyes/throat, postnasal drip
- Can be seasonal (pollen) or perennial (indoor allergens)
🔹 B. Allergic Asthma
- Triggered by: Inhaled allergens like dust mites, mold, pollen, animal dander
- Involves bronchospasm, airway inflammation, and mucus production
- Symptoms: Wheezing, coughing, breathlessness, chest tightness
🍽️ 2. Food Allergies
- Triggered by: Peanuts, tree nuts, eggs, milk, wheat, soy, shellfish, fish
- Immune system reacts to specific proteins in food
- Symptoms:
- Mild: Hives, itching, vomiting
- Severe: Swelling of lips, throat, anaphylaxis
- Most common in children, but may persist or develop in adults
💊 3. Drug Allergies (Medication Allergies)
- Triggered by: Penicillin, sulfa drugs, NSAIDs (e.g., aspirin), anticonvulsants, vaccines
- Symptoms:
- Mild: Rash, hives, itching
- Moderate: Angioedema (swelling)
- Severe: Anaphylaxis, Stevens-Johnson Syndrome
📌 Note: Not all drug reactions are true allergies—some are side effects or intolerances
🐝 4. Insect Sting Allergies
- Triggered by: Bee, wasp, hornet, ant stings
- Reaction to venom proteins
- Symptoms:
- Local: Redness, swelling, pain at sting site
- Systemic: Urticaria, dizziness, throat swelling, anaphylaxis
🧴 5. Skin Allergies (Contact and Urticaria)
🔹 A. Contact Dermatitis (Type IV delayed hypersensitivity)
- Triggered by: Nickel, latex, cosmetics, soaps, poison ivy
- Not IgE-mediated; caused by T-cell immune reaction
- Symptoms: Redness, itching, blistering, swelling where contact occurred
🔹 B. Urticaria (Hives) and Angioedema
- Triggered by: Foods, medications, cold, heat, pressure, stress
- Urticaria: Superficial raised red itchy wheals
- Angioedema: Deeper swelling (lips, face, tongue, eyelids)
🌡️ 6. Anaphylaxis (Severe Systemic Allergy)
- Life-threatening allergic reaction involving multiple organs
- Common triggers: Food, insect stings, medications
- Symptoms:
- Swelling of lips/tongue, difficulty breathing
- Drop in blood pressure (shock)
- Dizziness, collapse
- Requires immediate treatment: epinephrine injection (EpiPen)
⚙️ 7. Occupational Allergies
- Seen in professionals exposed to chemicals, latex, hair dyes, dust, or animal proteins
- Examples:
- Latex allergy in healthcare workers
- Asthma in bakers (flour dust)
- Contact dermatitis in hairdressers or cleaners
🧬 8. Allergic Reactions due to Immune Conditions
- Atopic Dermatitis (Eczema): Chronic itchy inflammation of skin
- Eosinophilic Esophagitis: Food allergy causing inflammation of the esophagus
- Allergic Conjunctivitis: Itchy, watery, red eyes due to airborne allergens
🧬 Pathophysiology of Allergies
Allergic reactions are hypersensitivity responses of the immune system to substances that are usually harmless (called allergens). The most common allergic response is Type I Hypersensitivity, which is IgE-mediated and occurs rapidly after exposure.
🔄 Step-by-Step Pathophysiology (Type I Hypersensitivity)
✅ 1. First Exposure (Sensitization Phase)
- The allergen (e.g., pollen, food protein, dust mite) enters the body via skin, inhalation, ingestion, or injection.
- It is recognized by antigen-presenting cells (APCs), which process the allergen and present it to T-helper cells (Th2 type).
- Th2 cells stimulate B lymphocytes to produce IgE antibodies specific to the allergen.
- The produced IgE antibodies bind to receptors (FcεRI) on the surface of mast cells and basophils, primarily in the skin, lungs, and mucosa.
🧠 The person is now sensitized to that allergen — no reaction yet, but the immune system is primed.
✅ 2. Re-Exposure (Activation Phase)
- Upon re-exposure to the same allergen:
- The allergen cross-links with the IgE antibodies on mast cells/basophils.
- This causes degranulation — the mast cells release histamine, leukotrienes, prostaglandins, and cytokines.
✅ 3. Inflammatory Response (Effector Phase)
These chemical mediators cause the classic allergic symptoms:
| 🧪 Mediator | 💥 Effects |
|---|---|
| Histamine | Vasodilation → redness & swelling, increased permeability → edema, smooth muscle contraction → bronchospasm, increased mucus secretion |
| Leukotrienes & Prostaglandins | Prolonged inflammation, bronchoconstriction, mucus production |
| Cytokines (e.g., IL-4, IL-5) | Attract eosinophils, promote IgE production, sustain inflammation |
📊 Resulting Allergic Reactions:
- Localized reactions:
- Sneezing, nasal congestion (allergic rhinitis)
- Asthma (bronchoconstriction)
- Hives, itching (urticaria)
- Vomiting or diarrhea (food allergy)
- Systemic reactions:
- Anaphylaxis → severe hypotension, airway narrowing, life-threatening
🚫 Other Types of Hypersensitivity Involved in Allergies
| 🔢 Type | 📋 Mechanism | 🧾 Examples |
|---|---|---|
| Type I | IgE-mediated, immediate | Asthma, hay fever, anaphylaxis |
| Type II | IgG/IgM-mediated cytotoxic (less common) | Drug-induced hemolysis |
| Type III | Immune complex-mediated | Serum sickness, Arthus reaction |
| Type IV | Delayed-type, T-cell-mediated | Contact dermatitis, TB skin test |
🔍 Signs and Symptoms & Diagnosis of Allergies
✅ I. Signs and Symptoms of Allergies
Allergic reactions vary in severity and depend on the type of allergen, route of exposure, and individual sensitivity. Symptoms may be localized, systemic, mild, or life-threatening.
🔷 1. Respiratory Allergies
➤ Allergic Rhinitis (Hay Fever):
- Sneezing
- Runny or congested nose
- Itchy eyes, nose, throat
- Watery or red eyes
- Postnasal drip
- Fatigue (due to poor sleep)
➤ Allergic Asthma:
- Wheezing
- Shortness of breath
- Chest tightness
- Cough (especially at night or early morning)
🍽️ 2. Food Allergies
- Itching or tingling in the mouth
- Swelling of lips, tongue, or throat
- Hives, redness, or eczema
- Abdominal pain, vomiting, diarrhea
- Difficulty breathing or anaphylaxis
💊 3. Drug Allergies
- Skin rash or hives
- Itching or fever
- Swelling of face or extremities
- Anaphylaxis (severe cases)
🐝 4. Insect Sting Allergies
- Local: Redness, swelling, pain at sting site
- Systemic: Hives, difficulty breathing, dizziness, drop in BP → anaphylaxis
🧴 5. Skin Allergies
➤ Urticaria (Hives):
- Raised, red, itchy welts
- Often migratory and vary in shape/size
➤ Contact Dermatitis:
- Redness, itching, blisters at site of contact
- Often delayed (24–48 hours post-exposure)
⚠️ 6. Anaphylaxis (Severe Allergic Reaction)
🛑 Life-threatening emergency!
- Rapid onset (minutes to hours)
- Swelling of face, tongue, and airway
- Difficulty breathing, wheezing
- Rapid heartbeat, low BP
- Skin rash or hives
- Confusion or loss of consciousness
- Needs IM epinephrine (EpiPen) immediately
✅ II. Diagnosis of Allergies
Allergy diagnosis is based on clinical history, physical examination, and specialized tests to identify the specific allergen.
🔹 1. Detailed History
- Onset, duration, and type of symptoms
- Timing in relation to food, drugs, seasons, or exposure
- Family history of allergies, asthma, or eczema
- Past allergic reactions (mild or severe)
- Occupational and lifestyle factors
🔹 2. Physical Examination
- Skin: rash, hives, eczema
- Respiratory: wheezing, nasal congestion, watery eyes
- GI signs in food allergy: bloating, cramps, vomiting
🔹 3. Allergy Testing Methods
| 🧪 Test | 🔍 Purpose & Notes |
|---|---|
| Skin Prick Test (SPT) | Identifies immediate-type (IgE-mediated) reactions to allergens |
| Intradermal Test | Used for drug or insect allergy testing
– More sensitive than SPT but higher risk of reaction
| Patch Testing | Detects delayed hypersensitivity (e.g., contact dermatitis)
– Applied to the back and left for 48–72 hrs
| Blood Tests (RAST / ImmunoCAP) | Measures specific IgE antibodies in serum
– Used when skin tests are contraindicated (e.g., eczema, antihistamine use)
| Total Serum IgE Levels | May be elevated in allergic patients but not specific
| Elimination Diet | Useful in food allergy – remove and reintroduce suspected foods
| Oral Food Challenge | Gold standard for diagnosing food allergies
– Done under medical supervision due to risk of anaphylaxis
| Spirometry or Peak Flow | Assesses lung function in allergic asthma patients
💊 Medical Management of Allergies
🎯 Goals of Treatment:
- Relieve symptoms (itching, sneezing, wheezing, rashes)
- Prevent allergic reactions from recurring
- Control inflammation and immune response
- Desensitize the immune system (in select cases)
✅ I. Avoidance of Allergens (First Step)
- Identify and eliminate exposure to known allergens:
- Dust, pollens, animal dander
- Trigger foods, drugs, insect stings
- Use hypoallergenic products, wear protective clothing, or switch medications
✅ II. Pharmacological Treatment
🟢 1. Antihistamines (Most Common First-Line Drugs)
| 💊 Examples | 💡 Use |
|---|---|
| Cetirizine, Loratadine, Fexofenadine (non-sedating) | Allergic rhinitis, urticaria, mild food/drug allergies |
| Diphenhydramine, Hydroxyzine (sedating) | Severe itching, nighttime use |
🧠 Block H1 histamine receptors to reduce sneezing, itching, hives, and watery eyes
🟡 2. Corticosteroids
| 💊 Form | 📋 Use |
|---|---|
| Topical: Hydrocortisone, Betamethasone | Eczema, contact dermatitis, skin rashes |
| Nasal sprays: Fluticasone, Mometasone | Allergic rhinitis – reduce nasal swelling |
| Oral/IV: Prednisone, Methylprednisolone | Severe allergic reactions, asthma, anaphylaxis (supportive) |
🔬 Suppress inflammation and immune response
🔴 3. Epinephrine (Adrenaline) – Emergency Use
- Drug of choice for Anaphylaxis
- Given intramuscularly (IM) (e.g., EpiPen 0.3 mg for adults, 0.15 mg for children)
- Action:
- Bronchodilation (opens airways)
- Vasoconstriction (raises BP)
- Stops life-threatening allergic shock
🛑 Always followed by IV fluids, oxygen, antihistamines, and corticosteroids in hospital
🔵 4. Decongestants
- Examples: Pseudoephedrine, Oxymetazoline nasal spray
- Used for nasal congestion in allergic rhinitis
- Avoid long-term use → risk of rebound congestion
🟣 5. Leukotriene Receptor Antagonists
- Example: Montelukast
- Used in: Allergic asthma, allergic rhinitis
- Blocks leukotrienes that cause bronchoconstriction and inflammation
🟤 6. Mast Cell Stabilizers
- Examples: Cromolyn sodium (nasal spray or eye drops)
- Prevent mast cell degranulation → used prophylactically for allergic rhinitis or conjunctivitis
- Safe in children and pregnancy
⚪ 7. Immunotherapy (Allergy Shots or Sublingual Tablets)
- Used for: Severe allergic rhinitis, insect sting allergy, mild asthma
- Gradual exposure to allergen → develops tolerance
- Given as:
- Subcutaneous injections (over months to years)
- Sublingual tablets (e.g., for grass or ragweed allergies)
💡 Reduces long-term dependency on medications
📋 Supportive Measures
- Cool compresses or calamine lotion for skin allergies
- Saline nasal rinses for allergic rhinitis
- Avoid intense activity during pollen seasons (for asthma)
- Maintain hydration, air purification, and environmental hygiene
🩺 Nursing Management of Allergies
🎯 Objectives:
- Relieve symptoms and prevent complications
- Monitor and respond to acute allergic reactions
- Educate the patient on allergen avoidance, medications, and emergency response
- Support the patient’s physical and emotional well-being
🗂️ I. Nursing Assessment
✅ Subjective Data:
- History of allergen exposure (food, dust, drugs, stings, etc.)
- Reports of:
- Sneezing, itching, rash, swelling
- Breathing difficulty, abdominal pain, dizziness
- Family or personal history of allergies, asthma, or eczema
✅ Objective Data:
- Observe for:
- Skin changes: hives, rashes, redness
- Respiratory signs: wheezing, stridor, cough, cyanosis
- GI symptoms: vomiting, cramps, diarrhea
- Anaphylaxis signs: low BP, rapid pulse, altered consciousness
🧾 II. Nursing Interventions
🔹 1. Monitor and Manage Symptoms
- Monitor vital signs, respiratory status, and oxygen saturation
- Assess for progression of rash, swelling, or breathing difficulty
- Administer prescribed medications:
- Antihistamines for itching or hives
- Corticosteroids to reduce inflammation
- Bronchodilators for asthma symptoms
- Epinephrine IM if anaphylaxis occurs
🔹 2. Emergency Response for Anaphylaxis
- Position patient flat with legs elevated (unless breathing is impaired)
- Administer IM epinephrine immediately (EpiPen or injection)
- Provide oxygen therapy and start IV fluids if needed
- Prepare for intubation or advanced airway management if airway is compromised
- Stay with patient and monitor closely until stabilized
🔹 3. Patient Education
- Teach the patient:
- To identify and avoid known allergens
- Proper use of prescribed medications (e.g., antihistamines, inhalers, nasal sprays)
- To always carry an EpiPen if at risk for anaphylaxis
- Early signs of allergic reaction and when to seek emergency care
- Importance of wearing a medical alert bracelet
📘 Also educate family members or caregivers in the use of an epinephrine auto-injector.
🔹 4. Skin and Environmental Care
- For skin allergies: apply cool compresses, use hypoallergenic moisturizers
- Advise using unscented soaps and laundry detergents
- Educate on dust mite control: encase pillows/mattresses, wash linens in hot water
- Use HEPA filters, avoid pets if allergic, limit outdoor exposure during high pollen seasons
🔹 5. Emotional and Psychosocial Support
- Reassure and calm the patient, especially during acute reactions
- Address anxiety and fear related to repeated or severe allergic episodes
- Refer to allergy support groups if needed
- Encourage compliance with long-term treatments (e.g., immunotherapy)
📊 III. Evaluation (Expected Outcomes)
✅ Allergic symptoms are relieved or controlled
✅ No progression to severe or systemic reaction
✅ Patient understands medications and emergency precautions
✅ Patient successfully avoids allergens and uses preventive strategies
✅ Improved emotional confidence and safety awareness
⚠️ Complications of Allergies
If not properly identified and managed, allergies can lead to various physical and psychological complications:
✅ A. Physical Complications
| 🚨 Complication | 📝 Description |
|---|---|
| Anaphylaxis | Life-threatening systemic allergic reaction; causes airway obstruction, shock, and requires immediate epinephrine administration |
| Asthma exacerbation | Allergens can trigger or worsen asthma attacks → severe breathing difficulty |
| Chronic sinusitis or ear infections | Common in long-standing allergic rhinitis |
| Eczema worsening | Allergens worsen atopic dermatitis and lead to itching, secondary infections |
| Food allergy reactions | Can cause vomiting, diarrhea, dehydration, or anaphylaxis |
| Secondary bacterial infections | Scratching itchy skin may break the barrier and lead to infections |
| Medication side effects | Incorrect or prolonged use of antihistamines or steroids can lead to unwanted effects like drowsiness, GI upset, or immunosuppression |
✅ B. Psychological and Social Impact
- Anxiety or fear about potential exposure (especially with food or drug allergies)
- Social limitations in school, travel, or work
- Poor self-esteem or isolation due to skin or breathing issues
- In children: behavioral issues, sleep disturbances, poor concentration
📌 Key Points Summary: Allergies
✅ Definition: Allergies are abnormal immune responses to harmless substances (allergens) due to IgE-mediated hypersensitivity (Type I)
✅ Common Allergens:
- Airborne: dust, pollen, mold, dander
- Food: milk, eggs, nuts, shellfish
- Drugs: penicillin, sulfa, NSAIDs
- Stings: bees, wasps
- Contact: latex, nickel, cosmetics
✅ Types of Allergies:
- Allergic rhinitis, asthma, eczema, urticaria, food allergy, drug allergy, contact dermatitis, anaphylaxis
✅ Pathophysiology:
- Allergen exposure → IgE formation → binds to mast cells → re-exposure causes mast cell degranulation → histamine & chemical release → inflammation
✅ Signs & Symptoms:
- Sneezing, wheezing, itching, hives, swelling, GI upset, breathing difficulty, low BP (in anaphylaxis)
✅ Diagnosis:
- History, skin prick test, IgE testing, patch test, food challenge, spirometry (for asthma)
✅ Medical Management:
- Avoid allergens, use antihistamines, steroids, bronchodilators, epinephrine, and immunotherapy
✅ Nursing Management:
- Symptom monitoring, medication administration, emergency care, patient education, allergen control, emotional support
✅ Complications:
- Anaphylaxis, chronic symptoms, secondary infections, psychological impact
🌿 Eczema (Atopic Dermatitis)
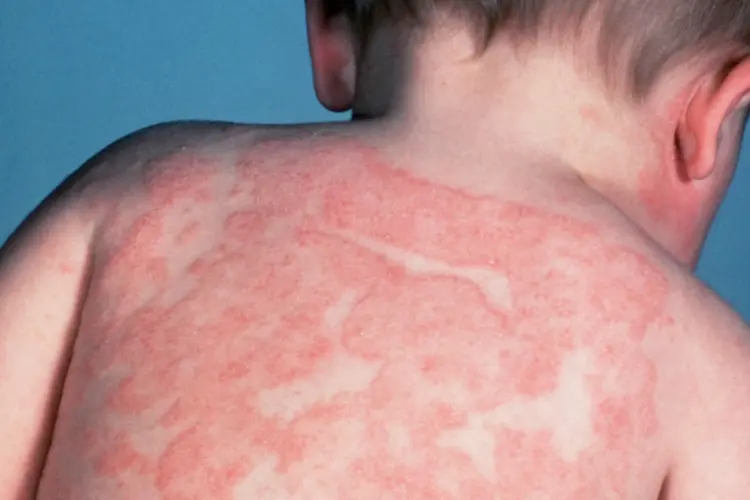
📘 Definition, Causes, Types, Pathophysiology, Signs & Symptoms, Diagnosis, Management, Complications, and Key Points
✅ Definition:
Eczema, also known as Atopic Dermatitis, is a chronic, relapsing inflammatory skin condition characterized by dry, itchy, red, and inflamed skin, often with crusting or lichenification. It is commonly seen in children but can persist or begin in adulthood.
🔬 It is associated with immune dysregulation and a defective skin barrier.
🔍 Causes of Eczema:
Eczema results from a combination of genetic, environmental, and immunologic factors:
| 🧬 Cause | 📝 Details |
|---|---|
| Genetic predisposition | Family history of eczema, asthma, or allergic rhinitis (atopic triad) |
| Allergens | Dust mites, pollen, animal dander, foods (e.g., eggs, milk) |
| Irritants | Soaps, detergents, perfumes, rough fabrics |
| Microbial | Staphylococcus aureus colonization, viruses |
| Climate and Weather | Cold, dry air or excessive sweating |
| Emotional Stress | Stress can worsen or trigger flare-ups |
🔢 Types of Eczema:
| 📌 Type | 💡 Description |
|---|---|
| Atopic Dermatitis | Most common; chronic, itchy, allergic in nature; begins in childhood |
| Contact Dermatitis | Caused by irritants (soaps) or allergens (nickel, latex) |
| Dyshidrotic Eczema | Small, itchy blisters on hands and feet |
| Nummular Eczema | Coin-shaped patches of irritated skin |
| Seborrheic Dermatitis | Affects oily areas (scalp, face); causes scaling and redness |
| Stasis Dermatitis | Occurs on lower legs due to poor circulation |
🧬 Pathophysiology of Eczema:
- Skin barrier dysfunction (↓ filaggrin protein) → ↑ transepidermal water loss
- Entry of allergens and irritants → stimulates immune cells
- Th2-dominant immune response → ↑ IgE production
- Mast cell degranulation → release of histamine → itching
- Scratching causes further skin damage, inflammation, and secondary infections
🚨 Signs & Symptoms of Eczema:
| 🔍 Symptom | 📝 Details |
|---|---|
| Itching (pruritus) | Most prominent feature; often severe |
| Red, inflamed patches | Common on cheeks, arms, legs, hands, neck |
| Dryness & scaling | Skin feels rough, flaky, and cracked |
| Vesicles or oozing | In acute phases; may crust and scab over |
| Lichenification | Thickened, leathery skin from chronic scratching |
| Hyperpigmentation | May occur post-inflammation, especially in darker skin tones |
🧪 Diagnosis of Eczema:
- Clinical diagnosis based on appearance, history, and chronicity
- No specific blood test, but the following may support:
- ↑ IgE levels (not always present)
- Skin prick test (to identify allergens)
- Patch testing (for contact dermatitis)
- Skin biopsy (rare; to rule out psoriasis, fungal infections)
💊 Medical Management of Eczema:
🔹 1. Topical Treatments:
- Moisturizers (emollients): Use frequently to restore barrier
- Topical corticosteroids: Hydrocortisone, betamethasone for inflammation
- Topical calcineurin inhibitors: Tacrolimus, pimecrolimus (for face/folds)
- Antibiotic creams: Mupirocin for secondary infection
🔹 2. Oral Medications:
- Antihistamines: Cetirizine, loratadine to reduce itching
- Oral antibiotics: If infected (e.g., cephalexin, amoxicillin)
- Oral steroids (short course): For severe flare-ups
- Immunosuppressants: Cyclosporine, methotrexate (in resistant cases)
- Biologics: Dupilumab (in severe atopic dermatitis)
🛠️ Surgical Management:
➡️ Generally not required, but in complicated or infected eczema, the following may be used:
- Incision and drainage (I&D) for infected abscesses
- Wound debridement if secondary infection leads to tissue damage
- Skin biopsy for unclear or persistent lesions
🩺 Nursing Management of Eczema:
- Assess lesion type, location, severity, and triggers
- Educate on:
- Regular use of moisturizers
- Avoiding known triggers (soaps, dust, allergens)
- Importance of not scratching – keep nails short
- Proper application of topical treatments
- Apply cool compresses to relieve itching
- Monitor for infection signs (pus, fever, worsening redness)
- Provide psychological support for appearance-related concerns
- Instruct on clothing: soft, breathable fabrics (e.g., cotton)
⚠️ Complications of Eczema:
- Secondary infections (bacterial, viral – e.g., impetigo, eczema herpeticum)
- Sleep disturbances from itching
- Pigmentation changes (hyper/hypopigmentation)
- Thickening or scarring of skin
- Psychosocial effects (low self-esteem, anxiety, social withdrawal)
📌 Key Points Summary:
✅ Eczema = chronic inflammatory skin disorder, common in children
✅ Caused by genetic + environmental factors
✅ Itching, redness, dryness, and thickened skin are classic features
✅ Diagnosed clinically, supported by allergy tests if needed
✅ Treatment: Moisturizers, topical steroids, antihistamines, immunomodulators
✅ Nursing care includes trigger avoidance, skin care, education, and infection monitoring
✅ Can lead to infection, sleep issues, or emotional distress
🧬 Pemphigus
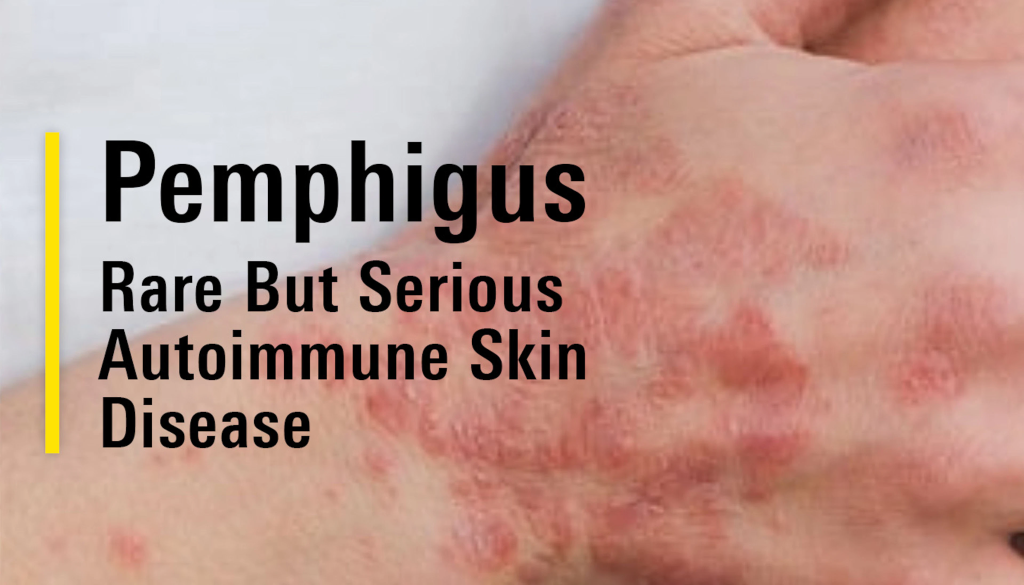
📘 Definition and Causes
✅ Definition:
Pemphigus is a rare, chronic, autoimmune blistering disorder of the skin and mucous membranes, characterized by the formation of flaccid blisters and erosions due to loss of cohesion between epidermal cells (a process called acantholysis).
🧠 In pemphigus, the body produces autoantibodies against desmogleins, which are proteins essential for cell-to-cell adhesion in the skin.
🔍 Key Characteristics:
- Superficial, easily ruptured blisters
- Painful erosions (especially in the mouth and genitals)
- Positive Nikolsky’s sign: Gentle pressure on skin causes epidermal separation
- Often starts in oral mucosa, then spreads to skin
🔎 Causes of Pemphigus:
Pemphigus is primarily autoimmune in origin, but several triggers may initiate or worsen the disease.
🔹 1. Autoimmune Response (Primary Cause)
- The body produces IgG autoantibodies against:
- Desmoglein 3 (in mucosal pemphigus)
- Desmoglein 1 & 3 (in skin + mucosal pemphigus vulgaris)
🔹 2. Genetic Predisposition
- Associated with certain HLA genes (e.g., HLA-DR4, HLA-DR14)
- Seen more commonly in people of Mediterranean, Jewish, and Indian descent
🔹 3. Drug-Induced Pemphigus
Some medications can trigger pemphigus in susceptible individuals:
- Penicillamine
- Captopril (ACE inhibitor)
- Rifampicin
- NSAIDs
- Phenobarbital
🔹 4. Environmental Factors (Rare)
- Exposure to UV radiation, certain chemicals, or infections may act as triggers
- Higher prevalence in certain endemic regions (e.g., Brazil – fogo selvagem, a form of pemphigus foliaceus)
🔢 Types of Pemphigus
Pemphigus is classified based on the depth of blistering and the specific target of autoantibodies.
✅ 1. Pemphigus Vulgaris (PV)
- Most common and most severe type
- Autoantibodies target desmoglein 3 (oral mucosa) ± desmoglein 1 (skin)
- Affects both mucous membranes and skin
- Flaccid blisters rupture easily → painful erosions
- Starts in the mouth, then may spread to skin
🧪 Nikolsky’s sign: Positive
🔍 Tzanck smear: Acantholytic cells
✅ 2. Pemphigus Foliaceus (PF)
- Milder and more superficial form
- Autoantibodies target desmoglein 1 (found in superficial epidermis)
- No mucosal involvement
- Blisters are superficial, fragile, often presenting as crusty erosions and scales
- Often involves face, scalp, and trunk
🧠 Common in endemic areas of Brazil (“fogo selvagem”)
✅ 3. Pemphigus Vegetans
- A rare variant of pemphigus vulgaris
- Characterized by vegetating plaques (thick, warty overgrowths)
- Seen in axillae, groin, and skin folds
- Slower in onset and progression
- May be misdiagnosed as fungal infection or psoriasis
✅ 4. Paraneoplastic Pemphigus (PNP)
- Associated with underlying malignancy (e.g., non-Hodgkin lymphoma, chronic lymphocytic leukemia)
- Severe mucosal erosions and polymorphic skin lesions
- Resistant to treatment and may involve lungs (bronchiolitis obliterans)
🧬 Autoantibodies target multiple antigens, not just desmogleins
✅ 5. IgA Pemphigus
- Rare form with IgA autoantibodies instead of IgG
- Blisters arranged in annular or grouped (clustered) patterns
- Responds better to dapsone than steroids
- Often misdiagnosed as dermatitis herpetiformis
✅ 6. Drug-Induced Pemphigus
- Triggered by drugs like penicillamine, captopril, or rifampicin
- Can mimic either pemphigus vulgaris or foliaceus
- Usually resolves after withdrawal of the offending drug
🧬 Pathophysiology of Pemphigus (All Types)
Pemphigus is a group of autoimmune blistering disorders that affect the epidermis and mucous membranes, caused by autoantibodies against desmogleins, which are cadherin-type adhesion molecules in the skin.
When these antibodies disrupt desmoglein function, keratinocytes lose adhesion, leading to a process called acantholysis — separation of skin cells — causing blister formation.
🔄 General Mechanism (Common to All Types)
- Trigger (genetic predisposition, drug, infection, or cancer in paraneoplastic pemphigus)
- Autoimmune activation – production of IgG (or IgA) autoantibodies
- Target – antibodies attack desmogleins (DSG1 or DSG3) in desmosomes
- Desmosomal disruption – loss of adhesion between epidermal cells (acantholysis)
- Blister formation – intraepidermal, flaccid blisters that rupture easily
- Inflammatory response – release of cytokines → further skin damage and erosion
📘 Type-wise Pathophysiology
✅ 1. Pemphigus Vulgaris (PV)
- Autoantibodies: IgG against desmoglein 3 (oral mucosa) and sometimes desmoglein 1 (skin)
- Affects deep epidermis (suprabasal layer)
- Leads to flaccid bullae and erosions, especially on mucous membranes and skin
- Blisters rupture easily due to fragile epidermal adhesion
🧪 Histology: Suprabasal clefting and “row of tombstones” appearance of basal cells
✅ 2. Pemphigus Foliaceus (PF)
- Autoantibodies: IgG against desmoglein 1 (expressed in superficial epidermis)
- No mucosal involvement, as Dsg1 is not present in mucosa
- Affects upper epidermis (subcorneal layer)
- Causes shallow erosions, scaling, and crusts rather than deep blisters
🧪 Histology: Acantholysis in the superficial epidermis
✅ 3. Pemphigus Vegetans
- Variant of PV
- Same autoantibodies (Dsg3 ± Dsg1)
- Exaggerated inflammatory response causes hyperplasia and vegetating plaques
- Found in moist, intertriginous areas (groin, axilla)
🧪 Histology: Suprabasal clefting + epidermal hyperplasia
✅ 4. Paraneoplastic Pemphigus (PNP)
- Autoantibodies against multiple antigens:
- Desmogleins 1 and 3
- Plakins (envoplakin, periplakin)
- Desmoplakin, BP230, plectin
- Associated with malignancies (esp. lymphoma, leukemia)
- Causes severe mucocutaneous blistering, polymorphic skin eruptions, and pulmonary involvement (bronchiolitis obliterans)
🧪 Histology: Interface dermatitis, necrotic keratinocytes, and acantholysis
✅ 5. IgA Pemphigus
- Autoantibodies of IgA class target desmocollin 1 or other desmosomal components
- Results in neutrophilic pustules and intraepidermal cleavage
- Pathology differs from PV/PF due to IgA-mediated neutrophilic activation
🧪 Histology: Intraepidermal pustules and neutrophilic infiltrates
✅ 6. Drug-Induced Pemphigus
- Medications (e.g., penicillamine, captopril) act as haptens, modifying keratinocyte antigens
- Induce IgG autoantibodies similar to PV or PF
- Usually resolves on drug withdrawal
🧪 Histology and immunofluorescence similar to the type it mimics (PV or PF)
🔍 Signs & Symptoms and Diagnosis of Pemphigus
✅ I. Signs and Symptoms of Pemphigus (All Types)
The clinical presentation of pemphigus depends on the type and depth of blistering, but most forms involve flaccid blisters, erosions, and painful mucosal involvement.
🔷 1. Pemphigus Vulgaris (PV)
- Most common and severe type
- Initial symptom: painful oral ulcers or mucosal erosions (seen in >90% of cases)
- Flaccid skin blisters on normal or erythematous base
- Blisters rupture easily, leaving raw, painful erosions
- Positive Nikolsky’s sign: gentle pressure shears off the skin
- Slow healing; new lesions appear as old ones heal
- May affect scalp, face, chest, axilla, groin
🔷 2. Pemphigus Foliaceus (PF)
- No mucosal involvement
- Presents with superficial blisters that rapidly break down into scaling, crusting, and erosions
- Common sites: face, scalp, upper chest, and back
- Lesions may resemble seborrheic dermatitis or psoriasis
🔷 3. Pemphigus Vegetans
- Characterized by thickened, warty (vegetating) plaques
- Occurs in moist areas like groin, axillae, or under breasts
- May be associated with foul-smelling discharge
🔷 4. Paraneoplastic Pemphigus (PNP)
- Severe, painful mucosal erosions: mouth, lips, eyes, pharynx
- Polymorphic skin lesions: blisters, erythema multiforme–like, or lichenoid rashes
- Associated with systemic symptoms: weight loss, fever, and underlying malignancy
- Can involve lungs → dyspnea (bronchiolitis obliterans)
🔷 5. IgA Pemphigus
- Annular or clustered pustules, often itchy
- Resembles subcorneal pustular dermatosis
- Involves trunk, proximal limbs, and may be misdiagnosed as dermatitis or psoriasis
🔷 6. Drug-Induced Pemphigus
- Similar to PV or PF in symptoms
- Usually develops weeks to months after drug exposure
- May resolve after discontinuing the drug
✅ II. Diagnosis of Pemphigus
Diagnosis is confirmed by clinical features, histopathology, and immunological testing.
🔬 1. Clinical Examination
- Nikolsky’s Sign: Positive in PV and PF — gentle lateral pressure causes skin to peel
- Asboe-Hansen Sign: Extension of a blister when pressure is applied
- Look for: flaccid bullae, oral ulcers, raw erosions, and crusting
🧪 2. Tzanck Smear
- Scraping from the base of the lesion shows acantholytic cells (rounded keratinocytes with large nuclei)
- Quick bedside test, but not definitive
🔬 3. Skin Biopsy
- Histopathology from edge of a fresh blister
- Findings:
- Suprabasal acantholysis in PV
- Subcorneal clefting in PF
- Neutrophilic pustules in IgA pemphigus
- Interface dermatitis in PNP
💡 4. Direct Immunofluorescence (DIF)
- Gold standard for pemphigus
- Skin biopsy shows intercellular IgG deposition in a “chicken wire” or “fishnet” pattern
- In IgA pemphigus: IgA deposits instead of IgG
🧪 5. Indirect Immunofluorescence / ELISA
- Blood test to detect circulating autoantibodies (anti-desmoglein 1 and 3)
- Helps assess disease severity and monitor response to treatment
📋 6. Additional Investigations (if Paraneoplastic Pemphigus suspected)
- CT scan, chest X-ray, or PET-CT to look for underlying malignancy
- Lung function tests if respiratory symptoms are present
💊 Medical Management of Pemphigus
Pemphigus, being an autoimmune blistering disorder, requires immunosuppressive and anti-inflammatory treatment to control disease activity, prevent new blister formation, and promote healing.
🎯 Goals of Treatment:
- Stop the formation of new blisters
- Promote healing of existing lesions
- Prevent secondary infection
- Reduce disease relapses and improve quality of life
✅ I. First-Line Therapy (Systemic Corticosteroids)
🔹 Oral Prednisolone
- Initial dose: 1–2 mg/kg/day (for moderate to severe pemphigus)
- High-dose steroids are often needed to control the disease quickly
- Once controlled, dose is tapered gradually over weeks/months
🔹 IV Methylprednisolone (Pulse Therapy)
- Given in severe or rapidly progressing cases or when oral route is not feasible
- Dose: 500–1000 mg/day IV for 3 consecutive days
⚠️ Long-term steroid use requires monitoring for side effects (osteoporosis, diabetes, infections, hypertension, cataracts)
✅ II. Steroid-Sparing Immunosuppressants (Adjuvant Therapy)
Used to reduce steroid dependency and maintain remission
| 💊 Drug | 💡 Use |
|---|---|
| Azathioprine | Commonly used with corticosteroids |
| Mycophenolate mofetil | Alternative to azathioprine |
| Cyclophosphamide | Used in resistant or severe cases |
| Methotrexate | Occasionally used in mild disease |
✅ III. Biologic Therapy (For Refractory Cases)
🔹 Rituximab (Anti-CD20 monoclonal antibody)
- Targets B-cells that produce autoantibodies
- Now considered first-line in many guidelines for moderate to severe pemphigus
- Given as IV infusions on days 1 and 15, sometimes with maintenance doses
- Often combined with corticosteroids
✅ IV. Adjunctive/Supportive Medications
| 💊 Drug/Measure | 📝 Purpose |
|---|---|
| Antibiotics (topical/oral) | Prevent or treat secondary bacterial infections |
| Antifungals | For candidiasis due to steroid use |
| Antivirals | In immunosuppressed patients if herpes or shingles suspected |
| Calcium/Vitamin D | Prevent steroid-induced osteoporosis |
| Proton Pump Inhibitors | Protect stomach lining from steroid irritation |
| Analgesics | Relieve pain from erosions and ulcers |
✅ V. Topical Treatments (for Mild or Localized Lesions)
- Topical corticosteroids: e.g., clobetasol or betamethasone
- Antiseptic mouthwashes (e.g., chlorhexidine) for oral lesions
- Barrier creams or emollients to soothe inflamed skin
- Wound dressings to protect eroded or infected areas
📌 Special Considerations for Paraneoplastic Pemphigus (PNP)
- Requires treatment of underlying malignancy
- Often resistant to conventional pemphigus therapy
- May need aggressive immunosuppression and cancer-directed therapy
🛠️ Surgical Management of Pemphigus
📌 General Note:
Pemphigus is an autoimmune condition, and thus, surgery is not a primary treatment modality. However, surgical interventions may be required in specific situations to manage complications or aid in supportive care.
✅ When Surgical Intervention Is Considered:
🔹 1. Wound Care and Debridement
- Indicated for:
- Extensive skin erosions with crusting
- Secondary bacterial infections
- Necrotic tissue in chronic, non-healing ulcers
- Procedure:
- Gentle debridement of necrotic skin under sterile conditions
- Aseptic dressing changes post-debridement
- May be done in an outpatient or minor OT setting
🔹 2. Biopsy for Diagnosis
- Punch or incisional skin biopsy is essential for:
- Histopathology
- Direct immunofluorescence (DIF)
- Taken from the edge of a fresh lesion (not ulcerated area)
🔹 3. Management of Superinfected Lesions or Abscesses
- If a blister site becomes secondarily infected and forms an abscess:
- Incision and drainage (I&D) may be required
- Followed by antibiotics and sterile dressings
🔹 4. Surgical Management of Underlying Malignancy (in Paraneoplastic Pemphigus)
- In cases of PNP, surgery may be needed to:
- Remove the underlying tumor (e.g., lymphoma, thymoma)
- Often part of oncological management, which may improve skin symptoms indirectly
🔹 5. Cosmetic or Reconstructive Surgery (Rare)
- Considered in long-term survivors with:
- Severe scarring or disfigurement
- Chronic non-healing erosions or skin contractures
⚠️ These are typically done after the disease is in remission and well-controlled.
⚠️ Surgical Risks in Pemphigus Patients:
- Poor wound healing due to immunosuppressive therapy
- High infection risk
- Skin fragility makes surgical handling more difficult
- Post-op corticosteroid adjustment may be required to prevent flare-up
🩺 Nursing Management of Pemphigus
🎯 Objectives of Nursing Care:
- Promote skin and mucosal healing
- Prevent and manage infection
- Alleviate pain and discomfort
- Support emotional well-being
- Ensure adherence to treatment and prevention of complications
🗂️ I. Assessment
✅ Subjective Data:
- Burning, pain, or itching over skin or mouth
- Difficulty eating, swallowing, or speaking due to oral lesions
- Fatigue, depression, or fear about appearance
✅ Objective Data:
- Presence of flaccid blisters, erosions, and crusting
- Mucosal involvement: oral, nasal, genital, conjunctival ulcers
- Signs of secondary infection: redness, pus, foul odor
- Monitor vitals: temperature (infection), BP (for steroid effects)
🧾 II. Nursing Interventions
🔹 1. Skin Integrity and Wound Care
- Handle the patient very gently — skin is fragile
- Apply topical medications and non-adherent dressings
- Use saline or antiseptic solutions for wound cleansing
- Turn and reposition patient frequently to avoid pressure sores
- Keep nails short and advise against scratching
🔹 2. Infection Prevention
- Maintain strict aseptic technique during dressing changes
- Observe for fever, pus, spreading redness
- Administer antibiotics as prescribed
- Encourage good hand hygiene for patient and caregivers
🔹 3. Oral and Mucosal Care
- Use soft toothbrush or swab sticks for oral hygiene
- Encourage cool liquids, soft foods to avoid mucosal trauma
- Provide mouth rinses (e.g., chlorhexidine)
- Apply topical anesthetics before meals if needed
🔹 4. Nutrition and Hydration Support
- Monitor nutritional status (especially with oral involvement)
- Offer high-protein, high-calorie, soft/blended meals
- Maintain adequate fluid intake
- Consider enteral feeding if oral intake is severely compromised
🔹 5. Medication Administration
- Administer steroids, immunosuppressants, and analgesics as prescribed
- Monitor for side effects of corticosteroids:
- Hyperglycemia, mood swings, infections, GI bleeding
- Provide gastroprotective agents (e.g., PPIs)
- Ensure adherence to the full course of therapy
🔹 6. Pain and Comfort Management
- Use analgesics appropriately
- Apply cool compresses for relief
- Provide calm, quiet environment to reduce stress
🔹 7. Emotional and Psychosocial Support
- Provide emotional support for body image issues
- Educate patient and family about the chronic nature of the disease
- Refer to support groups or counseling if needed
- Address fear of relapse, especially during steroid tapering
🔹 8. Health Education and Discharge Planning
- Teach patient to:
- Recognize signs of flare-ups and infection
- Avoid skin trauma and harsh soaps/chemicals
- Maintain regular follow-ups and medication compliance
- Encourage stress management and a healthy lifestyle
📊 III. Evaluation (Expected Outcomes)
✅ Wounds and mucosal lesions begin to heal
✅ No signs of new blister formation
✅ Patient remains infection-free
✅ Pain is effectively managed
✅ Patient and family demonstrate understanding of disease and treatment
✅ Emotional needs are addressed; patient has improved quality of life
⚠️ Complications of Pemphigus
If left untreated or poorly managed, pemphigus can lead to serious, even life-threatening consequences:
✅ 1. Secondary Skin Infections
- Most common complication
- Blisters and erosions act as portals for bacterial, viral, or fungal infections
- Can lead to cellulitis, sepsis, or impetigo
✅ 2. Fluid and Electrolyte Imbalance
- Due to extensive weeping wounds and erosions
- Risk of dehydration, hyponatremia, and hypovolemia
✅ 3. Nutritional Deficiencies
- Painful oral ulcers impair chewing and swallowing
- Leads to weight loss, protein-energy malnutrition, and vitamin deficiencies
✅ 4. Steroid-Related Complications
- Cushingoid features: moon face, buffalo hump
- Hyperglycemia, hypertension, osteoporosis, peptic ulcers
- Immunosuppression → increased risk of infections
✅ 5. Eye Involvement (Paraneoplastic Pemphigus)
- Can lead to conjunctivitis, corneal scarring, or even blindness
✅ 6. Respiratory Complications
- Seen in Paraneoplastic Pemphigus
- May develop bronchiolitis obliterans, a serious lung disease with poor prognosis
✅ 7. Psychological Impact
- Chronic illness and skin disfigurement → depression, anxiety, low self-esteem
- May cause social isolation and reduced quality of life
📌 Key Points Summary: Pemphigus
✅ Pemphigus is a chronic autoimmune blistering disorder
✅ Caused by IgG autoantibodies against desmogleins (1 and/or 3) → leads to acantholysis
✅ Pemphigus vulgaris is the most common and involves oral and skin lesions
✅ Pemphigus foliaceus is superficial and lacks mucosal involvement
✅ Paraneoplastic pemphigus is severe and associated with malignancy
✅ Classic signs: flaccid bullae, erosions, positive Nikolsky’s sign
✅ Diagnosed with Tzanck smear, skin biopsy, and direct immunofluorescence
✅ Treated with corticosteroids, immunosuppressants, rituximab, and supportive care
✅ Nursing care focuses on wound care, infection prevention, oral hygiene, nutrition, and emotional support
✅ Major complications include infection, steroid toxicity, dehydration, and psychosocial distress
🌿 Psoriasis
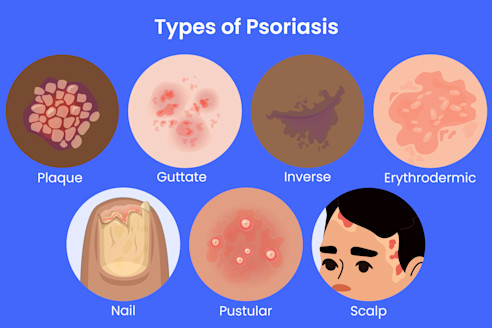
📘 Definition, Causes, and Types
✅ Definition:
Psoriasis is a chronic, autoimmune, inflammatory skin disorder characterized by accelerated proliferation of skin cells, leading to the formation of thick, red, scaly plaques. It is non-infectious and follows a relapsing-remitting course.
🔬 It results from an immune-mediated attack on the skin, especially involving T-cells and cytokines (like TNF-α, IL-17, and IL-23).
🔍 Causes and Risk Factors of Psoriasis:
Psoriasis is multifactorial, with both genetic and environmental contributors.
🔹 1. Genetic Factors
- Family history of psoriasis (seen in ~30% of cases)
- Linked to genes like HLA-Cw6
🔹 2. Immune Dysfunction
- Autoimmune process involving hyperactivation of T-cells
- Causes inflammation and rapid skin turnover
🔹 3. Environmental Triggers
| ⚠️ Trigger | 📝 Description |
|---|---|
| Infections | Streptococcal throat infection (esp. in guttate psoriasis) |
| Stress | Worsens flare-ups |
| Injury to skin | Koebner phenomenon – new lesions form at trauma sites |
| Medications | Lithium, beta-blockers, antimalarials, NSAIDs |
| Weather | Cold, dry weather aggravates psoriasis |
| Smoking & Alcohol | Increases severity and flare frequency |
| Hormonal changes | Puberty or menopause may influence onset |
🔢 Types of Psoriasis
Psoriasis can present in various clinical forms:
✅ 1. Plaque Psoriasis (Psoriasis Vulgaris) – Most Common
- Thick, red plaques with silvery-white scales
- Common on elbows, knees, scalp, and lower back
- Often symmetrical
✅ 2. Guttate Psoriasis
- Small, drop-like red lesions with fine scales
- Commonly appears after streptococcal infection
- Mostly seen in children and young adults
✅ 3. Inverse (Flexural) Psoriasis
- Occurs in skin folds: armpits, groin, under breasts
- Smooth, shiny, red patches without scales
- Can be confused with fungal infections
✅ 4. Pustular Psoriasis
- White pustules surrounded by red skin
- Can be localized (palms/soles) or generalized (life-threatening)
- May be triggered by sudden withdrawal of steroids
✅ 5. Erythrodermic Psoriasis
- Widespread redness and scaling over most of the body
- Medical emergency due to risk of fluid loss, infection, and hypothermia
- Often triggered by abrupt discontinuation of psoriasis treatment
✅ 6. Nail Psoriasis
- Causes pitting, ridging, onycholysis (nail separation), discoloration
- Often associated with psoriatic arthritis
✅ 7. Psoriatic Arthritis
- Inflammation of joints associated with skin psoriasis
- May involve small or large joints, causing pain, swelling, and deformity
- Up to 30% of psoriasis patients may develop joint symptoms
🧬 Pathophysiology of Psoriasis
Psoriasis is a chronic, immune-mediated inflammatory skin disease involving hyperproliferation of keratinocytes and abnormal immune system activation.
🔄 Step-by-Step Pathophysiology:
- Trigger or genetic predisposition activates immune system
- T-cells (especially Th1 and Th17) become abnormally activated
- These T-cells migrate to the skin and release inflammatory cytokines:
- TNF-α, IL-17, IL-23
- These cytokines stimulate:
- Keratinocyte proliferation → rapid skin cell turnover (3–5 days instead of 28)
- Inflammation → redness and swelling
- Angiogenesis → increased blood flow to affected areas
- Accumulated immature skin cells form thick plaques with scaling
🧠 The entire process results in the formation of red, raised, itchy, scaly plaques
👀 Signs and Symptoms of Psoriasis
✅ 1. Skin Lesions (Most Common Presentation)
| 📌 Feature | 💡 Description |
|---|---|
| Plaques | Raised, well-demarcated, red patches with silvery-white scales |
| Symmetrical distribution | Typically affects elbows, knees, scalp, back, and buttocks |
| Itching or burning | Especially during flare-ups |
| Auspitz Sign | Pinpoint bleeding when scales are scraped off |
| Koebner Phenomenon | New lesions at the site of trauma (scratches, cuts) |
✅ 2. Nail Changes (in Nail Psoriasis)
- Pitting (tiny depressions)
- Onycholysis (nail lifting from the nail bed)
- Discoloration, thickening, ridging
- Subungual hyperkeratosis (scaling under the nail)
✅ 3. Joint Involvement (Psoriatic Arthritis)
- Pain, swelling, and stiffness in joints
- Can affect fingers (sausage digits), wrists, knees, and spine
- Morning stiffness lasting more than 30 minutes
- Joint deformities in severe, long-standing cases
✅ 4. Systemic Features (in severe forms)
- Fever, chills, malaise in erythrodermic psoriasis
- Risk of dehydration, sepsis, and electrolyte imbalance
🧪 Diagnosis of Psoriasis
Diagnosis is mostly clinical, supported by history and sometimes laboratory or histological tests.
✅ 1. Clinical Examination
- Inspection of skin, scalp, nails, and joints
- Note location, shape, and scaling of lesions
- Check for Koebner phenomenon, Auspitz sign, nail changes
✅ 2. Skin Biopsy (if uncertain)
- Confirms diagnosis when atypical
- Histopathology shows:
- Parakeratosis (nuclei in stratum corneum)
- Acanthosis (epidermal thickening)
- Munro microabscesses (neutrophils in stratum corneum)
✅ 3. Blood Tests (for systemic/severe cases)
- ESR and CRP may be elevated (inflammation markers)
- Uric acid levels may be raised
- HLA-B27 may be positive in psoriatic arthritis
✅ 4. Joint Imaging (if arthritis present)
- X-rays or MRI to detect joint damage in psoriatic arthritis
- Early signs: joint space narrowing, erosions
💊 Medical Management of Psoriasis
Treatment is based on the type, severity, site of involvement, and patient response. The goals are to:
- Control inflammation and scaling
- Relieve itching and discomfort
- Prevent flare-ups and complications
- Improve quality of life
✅ I. Topical Therapies
➡️ First-line for mild to moderate psoriasis
| 💊 Drug | 📋 Action |
|---|---|
| Topical corticosteroids (e.g., betamethasone, clobetasol) | Anti-inflammatory; reduces redness and swelling |
| Vitamin D analogues (e.g., calcipotriol, calcitriol) | Slows skin cell proliferation |
| Coal tar | Reduces itching and scaling; used in plaque psoriasis |
| Salicylic acid | Keratolytic; softens and removes scales |
| Topical calcineurin inhibitors (e.g., tacrolimus) | Especially useful on face or flexural areas |
Apply moisturizers/emollients regularly to maintain skin hydration.
✅ II. Phototherapy
➡️ Used in moderate to severe cases or when topical treatments fail
| 💡 Type | 💬 Details |
|---|---|
| UVB phototherapy | Narrowband UVB is most effective; done 2–3 times/week |
| PUVA (Psoralen + UVA) | Psoralen taken orally or topically before UVA exposure |
| Excimer laser | Targeted UV light for small, stubborn lesions |
⚠️ Monitor for side effects like burning, pigmentation changes, and long-term skin cancer risk.
✅ III. Systemic Medications
➡️ Reserved for moderate to severe or resistant psoriasis
| 💊 Drug | 📝 Function & Notes |
|---|---|
| Methotrexate | Inhibits rapid skin cell division; also treats psoriatic arthritis |
| Cyclosporine | Suppresses T-cell activity; effective but nephrotoxic if prolonged |
| Acitretin (retinoid) | Regulates keratinocyte differentiation; avoid in women of childbearing age |
| Apremilast | PDE-4 inhibitor; reduces inflammation with fewer side effects |
| Biologics (e.g., infliximab, adalimumab, secukinumab) | Target specific immune pathways (TNF-α, IL-17, IL-23); very effective for severe psoriasis and psoriatic arthritis |
📌 Regular liver, kidney, and CBC monitoring is required for systemic therapy.
🛠️ Surgical Management of Psoriasis
Psoriasis is typically managed medically, but surgery is rarely needed. Surgical options may be considered in specific situations:
✅ 1. Nail Psoriasis
- Partial or complete nail avulsion (removal of the nail)
- Used in painful or severely damaged nails
- Combined with topical therapy or intralesional steroids
✅ 2. Psoriatic Arthritis
- Joint surgery (e.g., synovectomy or joint replacement) may be needed in:
- Severe joint deformities
- Loss of mobility or chronic pain unresponsive to drugs
✅ 3. Cosmetic or Corrective Procedures
- In patients with disfiguring plaques or scars, dermatologic surgical procedures may be offered after disease stabilization
⚠️ Important Surgical Considerations:
- Psoriatic skin is fragile and inflamed — take precautions during handling
- Use gentle techniques and monitor wound healing
- Risk of Koebner phenomenon (new lesions forming at trauma/surgical sites)
🩺 Nursing Management of Psoriasis
🎯 Goals of Nursing Care:
- Promote symptom relief and skin healing
- Prevent infection and flare-ups
- Support emotional well-being and self-image
- Enhance treatment compliance and patient education
- Maintain joint mobility (in psoriatic arthritis)
🗂️ I. Nursing Assessment
✅ Subjective Data:
- Complaints of itching, pain, burning, or tightness of skin
- History of stress, infection, medication use, family history
- Reported difficulty with daily activities, sleep, or social interaction
✅ Objective Data:
- Location and type of lesions (plaques, scaling, pustules, redness)
- Presence of nail changes or joint swelling/stiffness
- Signs of secondary infection (redness, pus, warmth, fever)
🧾 II. Nursing Interventions
🔹 1. Skin Care and Lesion Management
- Apply prescribed topical medications (e.g., corticosteroids, vitamin D analogues)
- Keep skin clean, moisturized, and protected
- Use lukewarm water and mild, non-irritating soaps
- Avoid scratching – trim nails, suggest soft cotton gloves at night
- Use occlusive dressings over thick plaques (if prescribed)
🔹 2. Infection Prevention
- Monitor for signs of skin infection: increased redness, pain, or pus
- Educate on hand hygiene and skin protection
- Use aseptic technique for dressing changes
- Administer antibiotics if ordered
🔹 3. Itch and Discomfort Relief
- Provide antihistamines (as prescribed) to relieve itching
- Suggest cool compresses or oatmeal baths
- Encourage use of soft clothing and avoiding irritating fabrics
🔹 4. Psychosocial and Emotional Support
- Offer emotional reassurance to reduce anxiety, depression, or social withdrawal
- Encourage open discussion about body image concerns
- Refer to support groups, counseling, or dermatological rehabilitation services
- Promote self-care confidence and independence
🔹 5. Patient Education
Educate the patient and family on:
- Nature of disease: chronic, not contagious, may relapse
- Importance of regular treatment and follow-up
- Identifying and avoiding triggers (stress, infection, smoking, alcohol, cold weather)
- Proper use of topical, oral, or injectable medications
- Maintaining hydration and healthy diet
🔹 6. Joint Care (if Psoriatic Arthritis is present)
- Encourage range of motion exercises to maintain flexibility
- Teach joint protection techniques
- Monitor for joint deformities, pain, and swelling
- Coordinate with physiotherapy if needed
📊 III. Evaluation (Expected Outcomes)
✅ Skin lesions reduce or heal without secondary infection
✅ Patient verbalizes understanding of condition and treatment
✅ Itching and pain are relieved
✅ Patient shows confidence and self-care in managing disease
✅ No signs of complications or flare-ups
⚠️ Complications of Psoriasis
Although psoriasis is primarily a skin disorder, it can lead to significant systemic, psychological, and functional complications if not well-managed.
✅ A. Dermatologic Complications
| 💢 Complication | 📝 Description |
|---|---|
| Secondary skin infections | Scratching or skin barrier breakdown → cellulitis, impetigo |
| Erythrodermic psoriasis | Severe, life-threatening → widespread redness, dehydration, electrolyte loss |
| Pustular psoriasis | Can lead to systemic toxicity (fever, malaise, leukocytosis) |
| Koebner phenomenon | New lesions develop at trauma sites (e.g., cuts, scratches) |
✅ B. Systemic Complications
| ⚠️ Complication | 📋 Details |
|---|---|
| Psoriatic arthritis | Inflammatory joint disease in up to 30% of cases → joint deformity, disability |
| Cardiovascular disease | Increased risk of hypertension, stroke, and heart disease due to chronic inflammation |
| Metabolic syndrome | Higher incidence of obesity, insulin resistance, dyslipidemia |
| Eye involvement | Uveitis, conjunctivitis in psoriatic arthritis |
✅ C. Psychological and Quality-of-Life Complications
- Depression and anxiety due to chronic disfigurement and social stigma
- Sleep disturbances from itching and discomfort
- Social withdrawal, embarrassment, and poor self-image
- May lead to non-adherence to treatment
📌 Key Points Summary: Psoriasis
✅ Psoriasis is a chronic autoimmune skin condition characterized by rapid skin cell turnover and inflammation.
✅ Most common type: Plaque psoriasis – red plaques with silvery-white scales, commonly on elbows, knees, scalp.
✅ Other types: Guttate, inverse, pustular, erythrodermic, nail psoriasis, and psoriatic arthritis.
✅ Causes/triggers include genetic predisposition, infections, stress, trauma, certain drugs, and cold weather.
✅ Pathophysiology: T-cell–mediated immune response → cytokine release (TNF-α, IL-17) → keratinocyte hyperproliferation.
✅ Diagnosed clinically and confirmed by skin biopsy if needed.
✅ Treatment includes:
- Topical agents (steroids, vitamin D analogues)
- Phototherapy
- Systemic drugs (methotrexate, cyclosporine, biologics)
✅ Nursing care includes skin care, infection prevention, patient education, and psychosocial support.
✅ Complications include infection, joint deformities, erythroderma, and emotional distress.
🧬 Malignant Melanoma
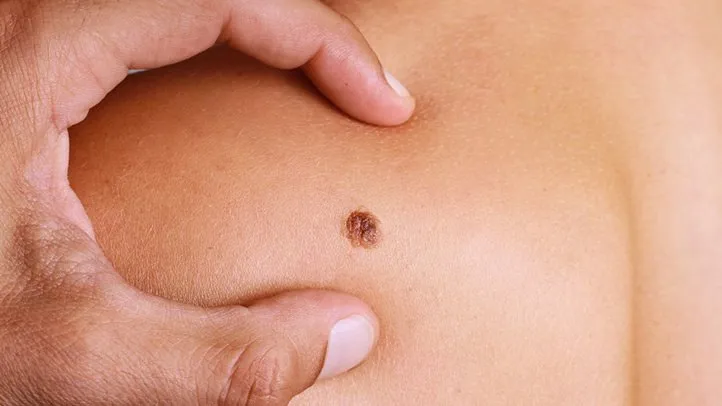
✅ Definition:
Malignant melanoma is a highly aggressive, life-threatening skin cancer that originates from melanocytes, the pigment-producing cells in the basal layer of the epidermis. It is characterized by uncontrolled melanocyte proliferation, with a high potential to invade locally and metastasize early.
🔬 Though less common than basal or squamous cell carcinoma, it causes the majority of skin cancer–related deaths.
🔍 Causes and Risk Factors:
| 🧪 Cause/Risk Factor | 💡 Explanation |
|---|---|
| Ultraviolet (UV) exposure | Excessive sun or tanning bed use → DNA damage in melanocytes |
| Fair skin | Less melanin → higher UV sensitivity |
| Moles (nevi) | Multiple or atypical moles increase risk |
| Family history | Genetic mutations (e.g., CDKN2A, BRAF) |
| Previous skin cancers | History of melanoma or other skin cancers |
| Immunosuppression | Transplant recipients, HIV patients |
| Genetic syndromes | Xeroderma pigmentosum, familial atypical mole syndrome |
🔢 Types of Malignant Melanoma:
| 🔹 Type | 📝 Description |
|---|---|
| Superficial Spreading Melanoma | Most common (~70%); slow horizontal growth; often on trunk or limbs |
| Nodular Melanoma | Second most common; fast-growing; aggressive vertical growth phase |
| Lentigo Maligna Melanoma | Occurs on sun-exposed skin in elderly; slow progression |
| Acral Lentiginous Melanoma | Common in palms, soles, and under nails; more common in darker skin tones |
| Amelanotic Melanoma | Rare; lacks pigment, making it harder to diagnose early |
🧬 Pathophysiology:
- DNA damage (often due to UV radiation) causes genetic mutations in melanocytes.
- These mutations (e.g., BRAF, NRAS) result in uncontrolled cell proliferation.
- Melanocytes grow abnormally, first radially (horizontally) within the epidermis.
- As the disease progresses, it grows vertically into deeper dermis and blood vessels.
- Early lymphatic and hematogenous spread → metastasis to lungs, liver, brain, bones
- Immune evasion allows tumor progression despite body’s defense mechanisms.
👀 Signs and Symptoms:
🔹 Use the ABCDE Rule to recognize melanoma:
| 🔤 Acronym | 📝 What to Look For |
|---|---|
| A – Asymmetry | One half doesn’t match the other |
| B – Border | Irregular, scalloped, or poorly defined edges |
| C – Color | Multiple colors or uneven distribution |
| D – Diameter | Greater than 6 mm (pencil eraser size) |
| E – Evolving | Changes in size, shape, color, or symptoms (itching/bleeding) |
🔹 Other Symptoms:
- New mole or growth
- Bleeding or ulceration of an existing mole
- Non-healing lesion
- Lymph node swelling (if metastasized)
🧪 Diagnosis:
| 🔬 Test | 💡 Purpose |
|---|---|
| Dermatoscopy | Visual inspection of skin lesion with magnification |
| Skin biopsy (excisional preferred) | Histological confirmation |
| Sentinel lymph node biopsy | Check for early metastasis |
| CT/MRI/PET scan | Staging and detection of distant metastasis |
| Blood tests (e.g., LDH) | Elevated levels may indicate metastasis |
🔬 Histopathology: Confirms melanoma subtype and depth (Breslow thickness, Clark level)
💊 Medical Management:
| 💊 Modality | 📋 Details |
|---|---|
| Targeted therapy | BRAF mutation-positive: vemurafenib, dabrafenib |
| Immunotherapy | Immune checkpoint inhibitors: nivolumab, pembrolizumab, ipilimumab |
| Chemotherapy | Limited role (e.g., dacarbazine); used in advanced/metastatic cases |
| Radiotherapy | Palliative for brain or bone metastasis |
🌟 Immunotherapy has significantly improved survival in metastatic melanoma.
🛠️ Surgical Management:
| ✂️ Procedure | 📝 Purpose |
|---|---|
| Wide local excision | Primary treatment of localized melanoma |
| Sentinel lymph node dissection | To assess spread in regional lymph nodes |
| Lymphadenectomy | Removal of affected lymph nodes |
| Metastasectomy | Removal of distant metastatic lesions in select cases |
| Skin graft/flap reconstruction | In large excisions |
🩺 Nursing Management:
🔹 Pre-operative & Post-operative Care
- Monitor vital signs, surgical site, and wound healing
- Educate patient on wound care and follow-up
- Support pain management and mobility
🔹 Skin Care and Observation
- Perform regular skin checks
- Teach self-examination using ABCDE criteria
🔹 Emotional and Psychological Support
- Address fear of recurrence or metastasis
- Provide counseling/referral to oncology support groups
- Encourage open communication and body image acceptance
🔹 Patient Education
- Importance of sun protection (SPF ≥30, clothing, shade)
- Avoid tanning beds and direct sunlight
- Teach early signs of recurrence or new lesions
⚠️ Complications:
| ❗ Complication | 💬 Description |
|---|---|
| Local recurrence | Cancer may reappear at or near the original site |
| Metastasis | Spread to lymph nodes, lungs, brain, liver, bones |
| Lymphedema | Post lymph node removal |
| Disfigurement | Post-surgical scarring |
| Immune-related adverse effects | Due to immunotherapy (colitis, hepatitis, pneumonitis) |
📌 Key Points Summary:
✅ Malignant melanoma = deadliest skin cancer, arises from melanocytes
✅ Risk factors: UV exposure, fair skin, family history, multiple nevi
✅ Types: Superficial spreading, nodular, lentigo maligna, acral lentiginous
✅ Use ABCDE rule for clinical detection
✅ Diagnosis: Biopsy, imaging, node biopsy
✅ Treated by surgical excision, immunotherapy, targeted therapy
✅ Nursing care includes wound care, psychological support, and sun safety education
✅ Watch for recurrence, metastasis, and treatment-related side effects
🧑🦲 Alopecia
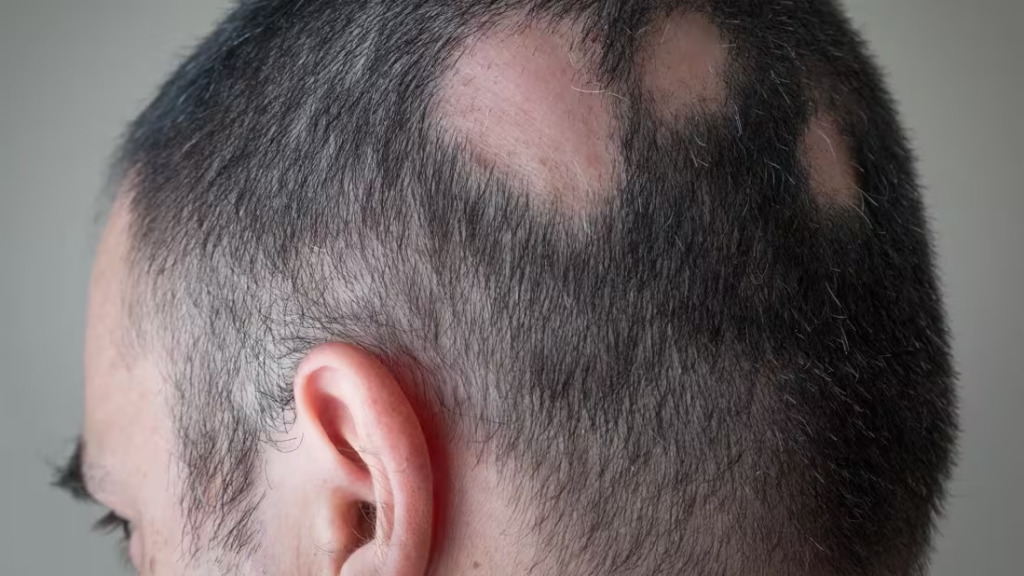
📘 Definition and Causes
✅ Definition:
Alopecia is a general medical term for hair loss from the scalp or body, which can be temporary or permanent, partial or complete, and caused by a variety of underlying conditions.
🔬 It can affect the hair follicles, the immune system, or the hormonal balance, and may result in thinning, patchy loss, or complete baldness.
🔍 Causes of Alopecia:
Alopecia can result from genetic, autoimmune, hormonal, infectious, nutritional, or drug-related factors. Causes may be primary (directly affecting hair follicles) or secondary (due to systemic conditions or damage).
🔹 1. Genetic Causes
- Androgenetic Alopecia (male/female pattern baldness)
- Most common cause
- Inherited sensitivity of hair follicles to dihydrotestosterone (DHT)
- Gradual thinning and receding hairline in males; diffuse thinning in females
🔹 2. Autoimmune Causes
- Alopecia Areata
- Immune system attacks hair follicles, leading to round patches of hair loss
- May progress to total scalp loss (Alopecia Totalis) or complete body hair loss (Alopecia Universalis)
🔹 3. Hormonal Causes
- Thyroid disorders (hypo-/hyperthyroidism)
- Polycystic ovarian syndrome (PCOS)
- Postpartum hormonal shifts
- Menopause or andropause
🔹 4. Physical or Emotional Stress
- Telogen Effluvium
- Triggered by illness, surgery, trauma, or severe stress
- Causes sudden, diffuse hair shedding due to more follicles entering the resting phase (telogen)
🔹 5. Nutritional Deficiencies
- Lack of protein, iron, zinc, vitamin D, or B-complex vitamins
- Seen in malnutrition, crash dieting, eating disorders
🔹 6. Drug-Induced Alopecia
- Medications that interfere with hair growth:
- Chemotherapy
- Beta-blockers, anticoagulants, retinoids, antidepressants, antithyroid drugs
🔹 7. Infections
- Fungal infections (Tinea capitis) – especially in children
- Bacterial folliculitis
- Syphilis, HIV/AIDS
🔹 8. Mechanical or Traumatic Causes
- Traction alopecia: due to tight hairstyles (braids, ponytails)
- Trichotillomania: psychological condition involving hair pulling
- Burns, scars, or radiation therapy
🔢 Types of Alopecia
Alopecia is classified based on cause, pattern, and extent of hair loss.
✅ I. Non-Scarring (Non-Cicatricial) Alopecia
In these types, the hair follicles are not permanently destroyed, and hair regrowth is often possible.
🔹 1. Androgenetic Alopecia (Male/Female Pattern Baldness)
- Most common type
- Genetically inherited, hormone-sensitive hair follicles
- Males: receding hairline, crown thinning
- Females: diffuse thinning over the crown with frontal hairline preservation
🔹 2. Alopecia Areata
- Autoimmune disorder where T-cells attack hair follicles
- Round or oval patches of hair loss on scalp or body
- Subtypes:
- Alopecia totalis: complete scalp hair loss
- Alopecia universalis: complete body hair loss
- Ophiasis pattern: band-like loss at sides/back of scalp
🔹 3. Telogen Effluvium
- Temporary, diffuse hair shedding
- Triggered by stress, surgery, illness, childbirth, or crash dieting
- Hair shifts prematurely from growth phase (anagen) to shedding phase (telogen)
🔹 4. Anagen Effluvium
- Sudden hair loss during the growth phase
- Caused by chemotherapy, radiation, or toxins
- Hair loss is rapid and usually reversible after cessation of trigger
🔹 5. Traction Alopecia
- Due to prolonged tension from hairstyles (tight braids, buns, ponytails)
- Common in individuals with tight hairstyles or frequent styling
- Reversible if diagnosed early
🔹 6. Trichotillomania
- Psychiatric condition involving compulsive hair pulling
- Hair loss is patchy, with hairs of varying lengths
- More common in children and adolescents
✅ II. Scarring (Cicatricial) Alopecia
In these types, inflammation destroys the hair follicles permanently, leading to irreversible hair loss and scarring of the scalp.
🔹 1. Lichen Planopilaris
- Autoimmune condition; type of lichen planus affecting the scalp
- Redness, scaling, follicular plugging, and permanent patchy hair loss
🔹 2. Discoid Lupus Erythematosus (DLE)
- Chronic form of cutaneous lupus
- Red, scaly patches that cause scarring, pigment changes, and permanent hair loss
🔹 3. Central Centrifugal Cicatricial Alopecia (CCCA)
- Progressive hair loss starting at the crown and spreading outward
- More common in African descent, often associated with hair styling and chemical use
🔹 4. Folliculitis Decalvans
- Chronic bacterial infection of the hair follicles
- Presents with pustules, crusts, and eventual scarring hair loss
🔹 5. Frontal Fibrosing Alopecia
- Type of lichen planopilaris
- Causes receding hairline, often with eyebrow loss
- Affects mostly postmenopausal women
🧬 Pathophysiology of Alopecia
Alopecia arises from disruption of the normal hair growth cycle, inflammation, autoimmunity, or physical damage to hair follicles. The underlying mechanism varies based on the type of alopecia.
✅ Normal Hair Growth Cycle
- Anagen (growth phase) – 85–90% of scalp hair; lasts 2–6 years
- Catagen (transitional phase) – lasts 1–2 weeks
- Telogen (resting/shedding phase) – 10–15% of hair at a time; lasts 2–4 months
- After telogen, new anagen hair pushes old hair out.
🔁 Basic Pathological Mechanisms in Alopecia
🔹 1. Androgenetic Alopecia (AGA)
- Dihydrotestosterone (DHT) binds to androgen receptors in scalp follicles
- Leads to miniaturization of hair follicles → shorter anagen phase → thinner and shorter hair
- Eventually results in follicular atrophy and baldness in genetically predisposed individuals
🔹 2. Alopecia Areata (Autoimmune)
- T-lymphocytes (especially CD8+ cells) attack hair follicles (an immune-privileged site)
- Causes premature shift from anagen to telogen phase
- Follicle remains intact → potential for regrowth if inflammation is controlled
- Associated with other autoimmune diseases (thyroiditis, vitiligo)
🔹 3. Telogen Effluvium
- Sudden physiologic or emotional stress (e.g., illness, surgery, childbirth)
- Triggers massive shift of anagen hairs into telogen phase
- Results in diffuse shedding approximately 2–3 months after the event
- Hair follicles are not destroyed; recovery is often spontaneous
🔹 4. Anagen Effluvium
- Caused by cytotoxic agents (e.g., chemotherapy, radiation)
- Disrupts rapidly dividing matrix cells in anagen follicles
- Hair shaft narrows and breaks → rapid and diffuse hair loss
- Follicle remains intact → regrowth possible after trigger is removed
🔹 5. Traction Alopecia
- Chronic tension on hair (tight hairstyles) damages follicles mechanically
- Prolonged traction causes follicular inflammation and miniaturization
- May progress to scarring and irreversible loss if not treated early
🔹 6. Cicatricial (Scarring) Alopecia
- Chronic inflammation, infection, or autoimmune damage destroys the follicular stem cells and sebaceous glands
- Results in permanent loss of hair follicles and scar formation
- Common causes: Lichen planopilaris, Discoid lupus, Folliculitis decalvans
⚠️ Summary of Pathophysiologic Differences
| ⚙️ Type | 🔬 Pathology |
|---|---|
| Androgenetic | DHT → follicle miniaturization |
| Alopecia areata | Autoimmune T-cell attack |
| Telogen effluvium | Stress-induced early telogen shift |
| Anagen effluvium | Toxic damage to hair matrix cells |
| Traction alopecia | Physical tension and follicle injury |
| Scarring alopecia | Destruction of follicles by inflammation → fibrosis |
👀 Signs and Symptoms of Alopecia
The presentation of alopecia varies based on its type, cause, and chronicity. Hair loss may be patchy, diffuse, or complete, and may involve the scalp, body hair, eyebrows, or eyelashes.
✅ Common Signs & Symptoms Across Types:
| 🔍 Symptom | 💡 Description |
|---|---|
| Visible hair loss | Patches or widespread thinning on the scalp or body |
| Hair thinning | Often noticed in androgenetic alopecia (diffuse in females, receding in males) |
| Bald patches | Typically seen in alopecia areata – round, smooth areas |
| Scalp changes | May show redness, scaling, pustules (in infections or scarring alopecia) |
| Itching or burning | May occur in scarring alopecia, fungal infections, dermatitis |
| Hair breakage | In traction alopecia or trichotillomania |
| Exclamation mark hairs | Narrowed hairs seen at the margins of alopecia areata patches |
| Nail changes (in alopecia areata) | Nail pitting, ridges, or trachyonychia (rough nails) |
🔍 Type-specific Clinical Clues:
| 🧪 Type of Alopecia | 📝 Key Features |
|---|---|
| Androgenetic alopecia | Gradual thinning; male: frontal/crown; female: central scalp |
| Alopecia areata | Sudden onset of smooth, round bald patches; may regrow or worsen |
| Telogen effluvium | Diffuse hair shedding 2–3 months after stressor |
| Anagen effluvium | Sudden, widespread loss during chemotherapy or radiation |
| Scarring alopecia | Hair loss with redness, pustules, scarring, or skin atrophy |
| Trichotillomania | Broken hairs of different lengths; often irregular patches |
| Tinea capitis | Patchy hair loss with scaling, black dots, possible lymphadenopathy |
🧪 Diagnosis of Alopecia
Diagnosis is primarily clinical, supported by history, examination, and tests to identify the type and cause.
✅ 1. History Taking
- Onset, duration, and pattern of hair loss
- Recent illness, emotional or physical stress
- Medications, diet, hair care practices
- Family history of baldness or autoimmune disease
- Any associated symptoms (itching, scaling, systemic signs)
✅ 2. Physical Examination
- Pattern of hair loss (diffuse vs. patchy)
- Examine scalp, nails, eyebrows, eyelashes, body hair
- Look for signs of inflammation: erythema, scaling, pustules
- Hair pull test: gently pull 30–60 hairs from scalp
- >6 hairs coming out = positive (suggests active shedding)
✅ 3. Trichoscopy (Dermatoscopy of Hair and Scalp)
- Non-invasive magnified scalp examination
- Helps differentiate:
- Alopecia areata: yellow dots, exclamation mark hairs
- Androgenetic alopecia: hair diameter variability
- Scarring alopecia: absence of follicular openings
✅ 4. Scalp Biopsy
- Useful in scarring alopecia or unclear cases
- Shows inflammation, scarring, miniaturization, or follicle destruction
✅ 5. Blood Tests (as indicated)
| 🧪 Test | 💡 Indications |
|---|---|
| Thyroid profile (TSH, T3, T4) | For thyroid-related hair loss |
| CBC, iron studies | For anemia or iron deficiency |
| Vitamin B12, D levels | Nutritional hair loss |
| ANA, ESR, CRP | Autoimmune screening |
| Hormonal panel (LH, FSH, testosterone, prolactin) | If PCOS or androgen excess suspected in females |
✅ 6. Fungal Culture / KOH Scraping
- Performed in suspected tinea capitis or scalp infections
👀 Signs and Symptoms of Alopecia
The presentation of alopecia varies based on its type, cause, and chronicity. Hair loss may be patchy, diffuse, or complete, and may involve the scalp, body hair, eyebrows, or eyelashes.
✅ Common Signs & Symptoms Across Types:
| 🔍 Symptom | 💡 Description |
|---|---|
| Visible hair loss | Patches or widespread thinning on the scalp or body |
| Hair thinning | Often noticed in androgenetic alopecia (diffuse in females, receding in males) |
| Bald patches | Typically seen in alopecia areata – round, smooth areas |
| Scalp changes | May show redness, scaling, pustules (in infections or scarring alopecia) |
| Itching or burning | May occur in scarring alopecia, fungal infections, dermatitis |
| Hair breakage | In traction alopecia or trichotillomania |
| Exclamation mark hairs | Narrowed hairs seen at the margins of alopecia areata patches |
| Nail changes (in alopecia areata) | Nail pitting, ridges, or trachyonychia (rough nails) |
🔍 Type-specific Clinical Clues:
| 🧪 Type of Alopecia | 📝 Key Features |
|---|---|
| Androgenetic alopecia | Gradual thinning; male: frontal/crown; female: central scalp |
| Alopecia areata | Sudden onset of smooth, round bald patches; may regrow or worsen |
| Telogen effluvium | Diffuse hair shedding 2–3 months after stressor |
| Anagen effluvium | Sudden, widespread loss during chemotherapy or radiation |
| Scarring alopecia | Hair loss with redness, pustules, scarring, or skin atrophy |
| Trichotillomania | Broken hairs of different lengths; often irregular patches |
| Tinea capitis | Patchy hair loss with scaling, black dots, possible lymphadenopathy |
🧪 Diagnosis of Alopecia
Diagnosis is primarily clinical, supported by history, examination, and tests to identify the type and cause.
✅ 1. History Taking
- Onset, duration, and pattern of hair loss
- Recent illness, emotional or physical stress
- Medications, diet, hair care practices
- Family history of baldness or autoimmune disease
- Any associated symptoms (itching, scaling, systemic signs)
✅ 2. Physical Examination
- Pattern of hair loss (diffuse vs. patchy)
- Examine scalp, nails, eyebrows, eyelashes, body hair
- Look for signs of inflammation: erythema, scaling, pustules
- Hair pull test: gently pull 30–60 hairs from scalp
- >6 hairs coming out = positive (suggests active shedding)
✅ 3. Trichoscopy (Dermatoscopy of Hair and Scalp)
- Non-invasive magnified scalp examination
- Helps differentiate:
- Alopecia areata: yellow dots, exclamation mark hairs
- Androgenetic alopecia: hair diameter variability
- Scarring alopecia: absence of follicular openings
✅ 4. Scalp Biopsy
- Useful in scarring alopecia or unclear cases
- Shows inflammation, scarring, miniaturization, or follicle destruction
✅ 5. Blood Tests (as indicated)
| 🧪 Test | 💡 Indications |
|---|---|
| Thyroid profile (TSH, T3, T4) | For thyroid-related hair loss |
| CBC, iron studies | For anemia or iron deficiency |
| Vitamin B12, D levels | Nutritional hair loss |
| ANA, ESR, CRP | Autoimmune screening |
| Hormonal panel (LH, FSH, testosterone, prolactin) | If PCOS or androgen excess suspected in females |
✅ 6. Fungal Culture / KOH Scraping
- Performed in suspected tinea capitis or scalp infections
💊 Medical Management of Alopecia
Management depends on the type of alopecia, its cause, extent, and the patient’s age, gender, and preferences. Treatments aim to slow progression, stimulate regrowth, and manage underlying triggers.
✅ 1. Androgenetic Alopecia (Male/Female Pattern Baldness)
| 💊 Treatment | 📝 Details |
|---|---|
| Minoxidil (Topical) | OTC solution/foam (2% for women, 5% for men); prolongs anagen phase |
| Finasteride (Oral) | 1 mg/day for men; inhibits DHT production; not used in women of childbearing age |
| Spironolactone | Anti-androgen; often used in female androgenetic alopecia |
| Dutasteride | More potent than finasteride; used in resistant cases |
| Low-level laser therapy | FDA-approved; stimulates follicle activity (home-use devices available) |
✅ 2. Alopecia Areata (Autoimmune)
| 💊 Treatment | 📝 Details |
|---|---|
| Intralesional corticosteroids | Triamcinolone acetonide injected into patches |
| Topical corticosteroids | Potent steroids (e.g., clobetasol) applied to affected areas |
| Topical immunotherapy | Agents like diphencyprone (DPCP) to induce contact dermatitis and restart hair growth |
| Systemic steroids | Used in extensive or rapidly progressing cases |
| Immunosuppressants | Methotrexate, cyclosporine in severe cases |
| JAK inhibitors | Newer oral drugs (e.g., tofacitinib, baricitinib) for refractory alopecia areata |
✅ 3. Telogen Effluvium
- Usually self-limiting (hair regrows in 3–6 months)
- Identify and remove the trigger (stress, illness, hormone changes)
- Provide reassurance and nutritional support
- Use topical minoxidil if recovery is delayed
✅ 4. Anagen Effluvium (Chemo-induced)
- Hair usually regrows after cessation of chemotherapy/radiation
- Cold caps/scalp cooling during chemo may reduce severity
- Minoxidil may aid regrowth
✅ 5. Nutritional or Hormonal Alopecia
- Treat underlying deficiencies:
- Iron, Vitamin D, B12, zinc supplements
- Treat hormonal imbalances (e.g., thyroid replacement, anti-androgens for PCOS)
✅ 6. Fungal and Infectious Alopecia
- Topical or oral antifungals (e.g., terbinafine, griseofulvin) for tinea capitis
- Antibiotics for bacterial folliculitis
✅ 7. Trichotillomania (Psychological Hair Pulling)
- Cognitive Behavioral Therapy (CBT)
- SSRIs (e.g., fluoxetine) for associated anxiety or OCD
🛠️ Surgical Management of Alopecia
Surgery is considered in permanent hair loss or cosmetic cases unresponsive to medical therapy.
✅ 1. Hair Transplantation (Hair Restoration Surgery)
🔹 Types:
- FUT (Follicular Unit Transplantation): Strip of scalp is removed and follicles are implanted
- FUE (Follicular Unit Extraction): Individual follicles are extracted and transplanted
🔹 Indications:
- Androgenetic alopecia (main indication)
- Stable scarring alopecia after inflammation has stopped
⚠️ Not suitable for active alopecia areata or unstable scarring alopecia
✅ 2. Scalp Reduction / Flap Surgery
- In large bald areas, the scalp is surgically stretched and repositioned
- Rarely used now due to the success of FUE/FUT techniques
✅ 3. Scalp Micropigmentation / Cosmetic Camouflage
- Tattooing technique that gives the illusion of thicker hair
- Used for cosmetic satisfaction, especially in male baldness
✅ 4. Wigs and Hair Prostheses
- Offered as non-surgical cosmetic alternatives for extensive or irreversible alopecia
- Useful for alopecia universalis, chemotherapy-induced loss, or scarring alopecia
🩺 Nursing Management of Alopecia
🎯 Goals of Nursing Care:
- Identify the type and cause of hair loss
- Promote emotional support and self-esteem
- Encourage adherence to medical treatment
- Prevent further hair loss by reducing contributing factors
- Provide education and counseling for lifestyle, nutrition, and hair care
🗂️ I. Nursing Assessment
✅ Subjective Data:
- Complaints of hair thinning, hair fall, patchy loss
- Emotional expression: distress, embarrassment, anxiety
- History of:
- Recent illness, medication, or stress
- Hair care habits (tight hairstyles, chemical use)
- Family history of baldness or autoimmune conditions
✅ Objective Data:
- Pattern and location of hair loss (diffuse, patchy, total)
- Presence of scalp scaling, redness, pustules, scarring
- Associated nail or skin changes
- Hair pull test (performed by physician) may be observed
🧾 II. Nursing Interventions
🔹 1. Promote Scalp and Hair Health
- Encourage gentle hair care:
- Use mild shampoos
- Avoid tight hairstyles, frequent brushing, and heat styling
- Advise against scratching or pulling hair
- Monitor for scalp infections or inflammation
🔹 2. Assist with Medication Compliance
- Educate on proper use of:
- Topical minoxidil
- Steroid creams or injections (if prescribed)
- Oral medications (finasteride, immunosuppressants)
- Emphasize regular application and patience (results may take weeks/months)
- Watch for side effects and report adverse reactions
🔹 3. Nutritional Counseling
- Assess dietary habits and screen for deficiencies
- Promote high-protein, iron-rich foods
- Encourage supplementation if prescribed (iron, vitamin D, B12, zinc)
🔹 4. Support Psychological Well-being
- Provide a non-judgmental environment for patients to express concerns
- Offer counseling or psychiatric referral (especially in alopecia areata, trichotillomania)
- Promote use of cosmetic options: wigs, scarves, hats, or scalp micropigmentation
- Encourage participation in support groups
🔹 5. Patient Education
- Explain the nature and course of alopecia
- Emphasize that many forms are temporary and treatable
- Educate on:
- Avoiding triggers (e.g., stress, trauma, heat, chemicals)
- Sun protection for exposed scalp
- Monitoring for changes in hair patterns
🔹 6. Monitoring and Follow-Up
- Track progress of hair regrowth
- Assess for signs of treatment response or complications
- Schedule follow-ups for medication titration or specialist consultation (dermatologist, endocrinologist, psychiatrist)
📊 III. Evaluation (Expected Outcomes)
✅ Patient reports reduction in hair loss
✅ Patient expresses improved self-esteem and emotional adaptation
✅ Scalp remains free of infection or irritation
✅ Patient demonstrates understanding of treatment and compliance
✅ Nutritional needs are being met
✅ Patient utilizes coping mechanisms and/or cosmetic aids if needed
⚠️ Complications of Alopecia
Although alopecia is non-life-threatening, it can have significant emotional, psychological, dermatologic, and systemic implications, especially when untreated or mismanaged.
✅ A. Psychological & Social Complications
| ❗ Complication | 📋 Details |
|---|---|
| Low self-esteem and body image issues | Common in both genders; may lead to withdrawal or embarrassment |
| Depression and anxiety | Especially in alopecia areata and female pattern baldness |
| Social isolation | Fear of judgment, bullying, or public appearances |
| Quality of life reduction | Daily stress related to appearance and hair grooming |
✅ B. Physical Complications
| 🧬 Complication | 💡 Details |
|---|---|
| Scalp infections | In cases of open follicles, poor hygiene, or tinea capitis |
| Permanent scarring | Seen in cicatricial alopecia if inflammation destroys follicles |
| Sunburn or skin damage | Due to loss of hair protection on scalp/eyebrows |
| Progression of underlying illness | E.g., thyroid disease, lupus, iron deficiency, if left undiagnosed |
✅ C. Treatment-Related Complications
| 💊 Issue | ⚠️ Concern |
|---|---|
| Topical irritants (e.g., minoxidil) | Redness, itching, or dermatitis |
| Steroid overuse | Thinning of skin, systemic side effects |
| Oral immunosuppressants | Risk of infection, liver/kidney toxicity |
| Psychotropic drugs | Side effects like drowsiness, mood changes in trichotillomania |
📌 Key Points Summary: Alopecia
✅ Alopecia = Hair loss condition affecting scalp/body due to genetic, autoimmune, hormonal, nutritional, psychological, or physical causes
✅ Types include:
- Androgenetic alopecia – genetic pattern baldness
- Alopecia areata – autoimmune patchy loss
- Telogen effluvium – stress-triggered shedding
- Scarring alopecia – permanent follicle destruction
- Trichotillomania – compulsive hair pulling
✅ Diagnosis: clinical exam, trichoscopy, blood tests, scalp biopsy
✅ Medical management: minoxidil, finasteride, corticosteroids, immunotherapy, nutritional correction, and counseling
✅ Surgical options: hair transplant (FUE/FUT), scalp micropigmentation, wigs
✅ Nursing role: scalp care, medication support, psychological counseling, nutrition guidance, and education
✅ Complications include psychological distress, scarring, infections, and treatment side effects…
🌿 Special Therapies for Integumentary System Disorders
(For conditions like eczema, psoriasis, burns, dermatitis, ulcers, acne, skin cancers, and more)
✅ 1. Phototherapy (Light Therapy)
🔹 Types:
- UVB (Narrowband) – for psoriasis, vitiligo, eczema
- PUVA (Psoralen + UVA) – for chronic plaque psoriasis, lichen planus
- Blue light therapy – for acne vulgaris
🔹 Mechanism:
- Slows down keratinocyte proliferation
- Modulates immune response and inflammation
🔹 Nursing Considerations:
- Protect eyes with UV goggles
- Monitor for burns, erythema, dryness
- Ensure consistent skin exposure times
- Educate patient on phototoxicity with PUVA
✅ 2. Topical Therapies
Widely used in eczema, psoriasis, acne, dermatitis, fungal infections, ulcers
| 💊 Type | 📋 Examples & Use |
|---|---|
| Corticosteroids | Hydrocortisone, clobetasol – reduce inflammation & itching |
| Keratolytics | Salicylic acid, urea – remove scales (psoriasis, calluses) |
| Antibiotics | Mupirocin – for localized bacterial skin infections |
| Antifungals | Clotrimazole, ketoconazole – for tinea, candidiasis |
| Moisturizers/Emollients | Prevent dryness, restore barrier (eczema, ichthyosis) |
| Calcineurin Inhibitors | Tacrolimus – for sensitive areas in eczema |
| Vitamin D analogs | Calcipotriol – used in psoriasis |
| Retinoids | Tretinoin, adapalene – for acne and hyperpigmentation |
✅ 3. Systemic Drug Therapy
Used for moderate-to-severe or refractory skin conditions
🔹 Immunosuppressants:
- Methotrexate, cyclosporine → psoriasis, pemphigus, lichen planus
🔹 Biologics:
- Adalimumab, secukinumab, dupilumab → target specific immune pathways in psoriasis, eczema, urticaria
🔹 Retinoids:
- Isotretinoin → severe acne (monitor liver function, pregnancy prevention)
🔹 Antihistamines:
- Cetirizine, hydroxyzine → relieve itching in urticaria, eczema
🔹 Antibiotics & Antifungals:
- Used in infected wounds, cellulitis, impetigo, tinea
🔍 Monitor CBC, LFTs, kidney function as per drug requirements
✅ 4. Surgical Therapies
🔹 Types:
- Excision or Mohs surgery – skin cancers
- Debridement – burns, ulcers
- Skin grafting or flaps – after trauma or burns
- Laser surgery – for scars, tattoos, vascular lesions
🔹 Nursing Role:
- Wound dressing, pain management
- Pre/post-op care
- Educating patient on graft site hygiene and movement restrictions
✅ 5. Wound Care Therapies
🔹 Types:
- Negative Pressure Wound Therapy (NPWT/VAC) – improves healing in chronic ulcers, burns
- Hydrocolloid and alginate dressings – absorb exudate and support moist healing
- Honey dressing / collagen dressing – for infected wounds or diabetic ulcers
🔹 Principles:
- Keep wound moist, protected, infection-free
- Encourage granulation tissue formation
✅ 6. Cryotherapy
- Involves freezing abnormal skin cells using liquid nitrogen
- Used in warts, actinic keratosis, skin tags, basal cell carcinoma
⚠️ May cause temporary pain, blistering, or hypopigmentation
✅ 7. Chemical Peels
- Use of chemical agents (like glycolic acid, salicylic acid) to exfoliate damaged skin layers
- Commonly used for acne scars, melasma, pigmentation
Requires proper skin preparation and aftercare to avoid burns or infections
✅ 8. Psychotherapy/Counseling
- Vital for patients with alopecia, vitiligo, severe acne, psoriasis
- Helps manage body image issues, anxiety, depression
Referrals to mental health professionals or support groups as needed
✅ 9. Nutritional and Lifestyle Therapy
- Encourage diets rich in vitamins A, C, E, zinc, omega-3 fatty acids
- Avoid trigger foods in eczema, acne, urticaria
- Encourage hydration, sun protection, gentle skincare routine
✅ 10. Complementary Therapies
| 🌿 Type | 💡 Uses |
|---|---|
| Aloe vera | Soothing agent for burns, eczema |
| Turmeric (curcumin) | Anti-inflammatory properties |
| Tea tree oil | Antifungal and acne treatment |
| Oatmeal baths | Itch relief in eczema, dermatitis |
| Ayurveda/Homeopathy | Popular in chronic conditions (used with caution) |
⚠️ Always assess for skin sensitivity or allergies before recommending herbal treatments.
🌿 Alternative Therapies for Integumentary System Disorders
These therapies are used alongside conventional treatments to enhance skin healing, reduce inflammation, and promote well-being in conditions such as eczema, psoriasis, acne, burns, ulcers, dermatitis, and hair loss.
✅ 1. Herbal Therapies
🌱 Common Herbs Used:
| 🌿 Herb | 💡 Uses |
|---|---|
| Aloe vera | Soothes burns, eczema, sunburns; anti-inflammatory & hydrating |
| Neem (Azadirachta indica) | Antibacterial; used in acne, eczema, fungal infections |
| Turmeric (Curcumin) | Anti-inflammatory and antioxidant; used in psoriasis, acne |
| Tea Tree Oil | Antimicrobial and antifungal; used in acne, dandruff, fungal infections |
| Calendula (Marigold) | Wound healing and soothing; helpful in dermatitis, ulcers |
| Chamomile | Calms skin inflammation, helps in eczema and rashes |
⚠️ Always perform a patch test to prevent allergic reactions.
✅ 2. Ayurveda
🔹 Principles:
- Based on three doshas (Vata, Pitta, Kapha) and their balance
- Skin diseases are believed to result from toxic buildup (ama) and imbalance in doshas
🔹 Common Therapies:
| 🌿 Ayurvedic Remedy | 💡 Application |
|---|---|
| Neem & Turmeric pastes | For acne, eczema, infections |
| Triphala | Detoxifier; improves skin glow |
| Kumkumadi oil | Skin brightening and anti-aging |
| Manjistha (Rubia cordifolia) | Blood purifier for psoriasis, dermatitis |
| Abhyanga (herbal oil massage) | Nourishes skin, improves circulation |
| Panchakarma detox | Used in chronic skin disorders |
✅ 3. Homeopathy
Used for chronic skin conditions like psoriasis, eczema, urticaria, alopecia areata.
⚕️ Common Remedies:
- Sulphur – for dry, itchy skin
- Graphites – for oozing eczema
- Arsenicum album – for burning rashes
- Natrum muriaticum – for acne and hair loss
- Sepia – for hormonal skin issues (e.g., melasma)
⚠️ Requires individualized constitutional assessment by a trained homeopath.
✅ 4. Acupuncture and Acupressure
- Based on Traditional Chinese Medicine (TCM)
- Stimulates specific acupoints to improve Qi (energy) and blood flow
💡 Uses:
- Reduces stress-related flare-ups in psoriasis or eczema
- Helps in chronic urticaria and alopecia areata
- May assist in pain relief for skin ulcerations and scars
✅ 5. Aromatherapy
Uses essential oils to promote skin healing and emotional well-being.
🌸 Common Oils:
| 🌼 Oil | 💡 Effect |
|---|---|
| Lavender oil | Calms skin and mind; promotes wound healing |
| Chamomile oil | Anti-inflammatory and soothing |
| Rose oil | Improves complexion and skin hydration |
| Frankincense oil | Scar healing and anti-aging |
| Tea tree oil | Antibacterial for acne |
⚠️ Always dilute with carrier oils (like coconut or almond oil) to avoid irritation.
✅ 6. Dietary and Nutritional Therapies
Certain skin conditions improve with anti-inflammatory and antioxidant-rich diets.
🍎 Key Nutrients:
- Omega-3 fatty acids (from flaxseed, walnuts, fish oil) – reduce inflammation
- Vitamin A – skin regeneration (carrots, sweet potatoes)
- Vitamin C and E – antioxidants for healing
- Zinc and selenium – support skin barrier and repair
- Probiotics – improve skin-gut health (eczema, acne)
Encourage hydration, avoid processed foods, dairy (in acne), or gluten (in psoriasis, if sensitive)
✅ 7. Yoga and Stress Management
- Yoga, pranayama (breathing exercises), and meditation help reduce:
- Stress-induced flare-ups (psoriasis, eczema, urticaria)
- Hormonal acne and autoimmune reactions
Regular yoga and mindfulness practices improve skin tone, immunity, and healing.
✅ 8. Natural Topical Packs and Baths
| 🧖 Remedy | 💡 Use |
|---|---|
| Oatmeal bath | Relieves itching in eczema, dermatitis |
| Multani mitti (Fuller’s Earth) | Oil control and acne treatment |
| Sandalwood paste | Cooling and anti-inflammatory |
| Cucumber and honey mask | Skin hydration and soothing |
✅ 9. Lifestyle Modifications
- Avoid harsh soaps, detergents, and hot water baths
- Use cotton clothing for eczema and urticaria patients
- Encourage daily exercise and sun protection
- Sleep hygiene: Skin regenerates best during proper sleep cycles
📌 Summary Table
| 💠 Alternative Therapy | 📝 Benefits |
|---|---|
| Herbal / Ayurveda | Natural anti-inflammatory, skin healing |
| Homeopathy | Individualized care for chronic skin diseases |
| Acupuncture | Balances energy, reduces flares |
| Aromatherapy | Skin and emotional healing |
| Nutritional support | Anti-inflammatory & antioxidant protection |
| Yoga & meditation | Stress control, immune balance |
| Natural packs/baths | Soothing relief, detox, hydration |
💊 Drugs Used in the Treatment of Integumentary System Disorders
Integumentary system disorders include conditions like eczema, psoriasis, acne, dermatitis, fungal/bacterial infections, alopecia, burns, ulcers, urticaria, and skin cancers. Treatment is based on underlying cause, severity, site, and patient’s response.
✅ 1. Topical Corticosteroids
🔹 Examples:
- Hydrocortisone (mild)
- Betamethasone, Clobetasol (potent)
🔹 Uses:
- Eczema, psoriasis, dermatitis, allergic reactions
🔹 Action:
- Reduces inflammation, itching, and redness
🔹 Nursing Note:
- Use sparingly, especially on face/folds
- Risk of skin thinning, depigmentation, or tachyphylaxis with prolonged use
✅ 2. Antifungal Agents
🔹 Topical: Clotrimazole, Miconazole, Ketoconazole
🔹 Oral: Fluconazole, Terbinafine, Griseofulvin
🔹 Uses:
- Tinea infections, candidiasis, seborrheic dermatitis
🔹 Action:
- Disrupts fungal cell membrane → kills fungus
🔹 Nursing Note:
- Educate on completing full course
- Monitor liver function for oral agents
✅ 3. Antibiotics
🔹 Topical: Mupirocin, Fusidic acid
🔹 Oral: Doxycycline, Amoxicillin, Erythromycin, Cephalexin
🔹 Uses:
- Impetigo, cellulitis, folliculitis, infected wounds or ulcers
🔹 Action:
- Kills or inhibits bacterial growth
🔹 Nursing Note:
- Monitor for allergies, resistance, and GI upset
- Ensure wound hygiene with topical use
✅ 4. Antiviral Drugs
🔹 Examples: Acyclovir, Valacyclovir
🔹 Uses:
- Herpes simplex, Herpes zoster (shingles)
🔹 Action:
- Inhibits viral replication
🔹 Nursing Note:
- Initiate early for best effectiveness
- Monitor hydration and renal function
✅ 5. Antihistamines
🔹 Examples: Cetirizine, Loratadine, Diphenhydramine, Hydroxyzine
🔹 Uses:
- Urticaria, eczema, dermatitis, insect bites, allergic skin reactions
🔹 Action:
- Blocks histamine receptors, reducing itching and swelling
🔹 Nursing Note:
- Warn about drowsiness (especially with older generation antihistamines)
- Encourage hydration
✅ 6. Retinoids (Vitamin A Derivatives)
🔹 Topical: Tretinoin, Adapalene
🔹 Oral: Isotretinoin (for severe acne)
🔹 Uses:
- Acne, psoriasis, keratosis pilaris, aging skin
🔹 Action:
- Promotes cell turnover, reduces oil production, unclogs pores
🔹 Nursing Note:
- Causes photosensitivity → advise sunscreen use
- Isotretinoin is teratogenic → requires pregnancy testing and contraception
✅ 7. Immunosuppressants
🔹 Examples: Methotrexate, Cyclosporine, Azathioprine
🔹 Uses:
- Psoriasis, pemphigus, eczema (severe cases)
🔹 Action:
- Suppresses immune-mediated skin inflammation
🔹 Nursing Note:
- Monitor CBC, LFT, kidney function
- Educate on infection prevention during therapy
✅ 8. Calcineurin Inhibitors (Topical Immunomodulators)
🔹 Examples: Tacrolimus, Pimecrolimus
🔹 Uses:
- Atopic dermatitis, eczema (especially in sensitive areas like face or folds)
🔹 Action:
- Inhibits T-cell activation, reducing inflammation
🔹 Nursing Note:
- Avoid sun exposure
- Used as steroid-sparing agents
✅ 9. Biologics
🔹 Examples:
- Adalimumab, Secukinumab, Ustekinumab, Dupilumab
🔹 Uses:
- Severe psoriasis, atopic dermatitis, urticaria, hidradenitis suppurativa
🔹 Action:
- Target specific immune molecules (e.g., TNF-α, IL-17, IL-23)
🔹 Nursing Note:
- Given via subcutaneous injection
- Monitor for infections, TB testing, and autoimmune reactions
✅ 10. Moisturizers and Emollients
🔹 Examples: Paraffin, petroleum jelly, ceramide creams
🔹 Uses:
- Eczema, dry skin, ichthyosis, burns
🔹 Action:
- Restores skin barrier, prevents moisture loss
🔹 Nursing Note:
- Apply after bathing and as needed throughout the day
- Encourage regular use to prevent flare-ups
✅ 11. Wound Healing Agents
| 💊 Example | 💡 Use |
|---|---|
| Silver sulfadiazine | Burns, ulcers – antibacterial and soothing |
| Collagen dressings | Chronic wounds, diabetic ulcers |
| Zinc oxide ointment | Diaper rash, pressure ulcers |
Monitor for allergic reactions and signs of infection
✅ 12. Chemotherapy Agents (for Skin Cancers)
| 💊 Drug | 📋 Use |
|---|---|
| 5-Fluorouracil (5-FU) | Topical for actinic keratosis, basal cell carcinoma |
| Imiquimod | Immunomodulator for warts and superficial skin cancers |
| Vismodegib, Cemiplimab | For advanced basal/squamous cell carcinoma |
✅ 13. Miscellaneous
| 💊 Drug | 💡 Use |
|---|---|
| Dapsone | Acne, leprosy, dermatitis herpetiformis |
| Colchicine | Hidradenitis suppurativa |
| Thalidomide | Severe skin conditions (with caution due to teratogenicity) |
📌 Key Nursing Considerations for All Skin Drugs:
- Perform skin assessment before and after therapy
- Teach patient how to apply topicals properly
- Monitor for side effects and allergic reactions
- Educate on photoprotection and hydration
- Encourage treatment adherence for best outcomes
- Support emotional care in chronic skin conditions