Anatomy-B.sc-Unit-9-The Reproductive system
🧬 STRUCTURE OF MALE REPRODUCTIVE ORGANS
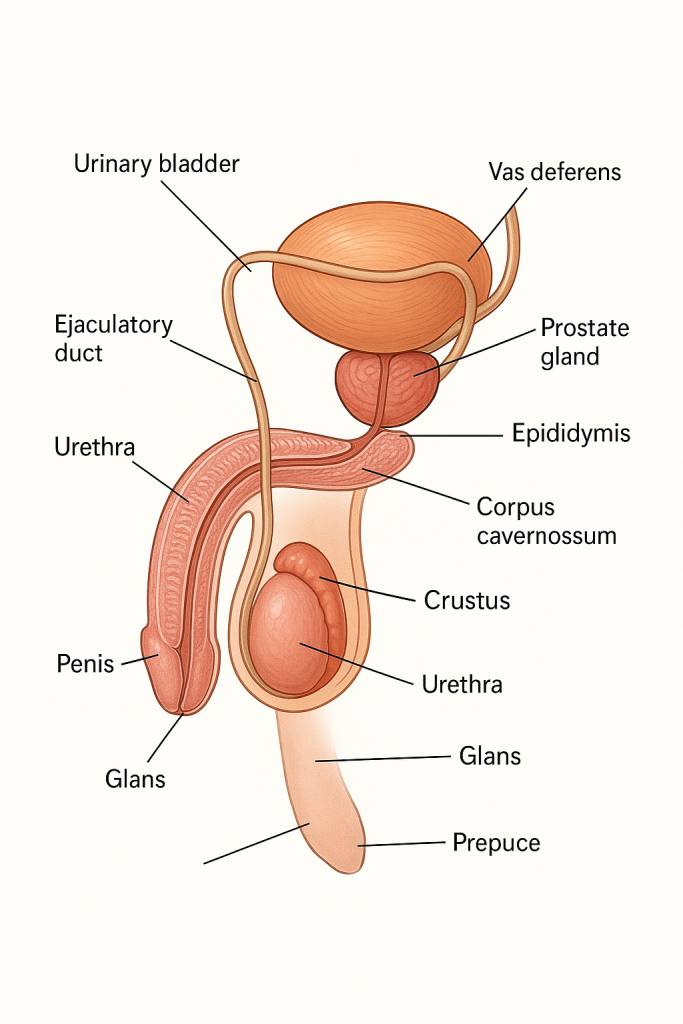
The male reproductive system is designed to produce, nourish, transport, and deliver sperm for reproduction. It consists of both external and internal organs, as well as various glands and ducts, each playing a vital role in spermatogenesis, hormone secretion, and ejaculation.
🧔♂️ I. EXTERNAL MALE REPRODUCTIVE ORGANS
1. Penis
The penis is the external copulatory organ that also serves as a conduit for urine and semen.
🔹 Structure:
- Composed of three cylindrical masses of erectile tissue:
- Two corpora cavernosa (dorsal side)
- One corpus spongiosum (ventral side), which surrounds the urethra and expands at the tip to form the glans penis.
- Covered by skin and a thin fibrous sheath called Buck’s fascia.
- The glans penis is covered by a retractable fold of skin known as the prepuce or foreskin (removed during circumcision in some cultures).
- The external urethral meatus is the opening at the tip of the glans for expelling semen or urine.
🔹 Function:
- Delivers sperm into the female reproductive tract during intercourse.
- Passage of urine from the bladder to outside the body.
2. Scrotum
The scrotum is a sac of skin and superficial fascia that houses the testes, epididymis, and part of the spermatic cord.
🔹 Features:
- Divided into two compartments by a median septum.
- Contains dartos muscle (smooth muscle) and cremaster muscle (skeletal muscle) that contract to regulate testicular temperature for optimal sperm production (~2–3°C below body temperature).
🔹 Function:
- Protects and maintains the testes at a cooler temperature necessary for spermatogenesis.
🧬 II. INTERNAL MALE REPRODUCTIVE ORGANS
1. Testes (Singular: Testis)
The testes are paired oval organs, each about 4–5 cm long, located in the scrotum and suspended by the spermatic cords.
🔹 Coverings:
- Surrounded by several layers including:
- Tunica vaginalis (outer serous layer)
- Tunica albuginea (thick fibrous capsule)
🔹 Internal Structure:
- Divided into 200–300 lobules, each containing:
- Seminiferous tubules – tightly coiled tubes where spermatogenesis occurs.
- Interstitial (Leydig) cells – located in spaces between tubules; secrete testosterone.
- Sertoli cells – support and nourish developing sperm cells and form the blood-testis barrier.
🔹 Function:
- Production of spermatozoa (sperm cells)
- Secretion of testosterone, the primary male sex hormone
2. Epididymis
A comma-shaped, coiled tube attached to the posterior surface of each testis.
🔹 Divided into:
- Head – receives sperm from seminiferous tubules via efferent ducts.
- Body and tail – where sperm mature and are stored.
🔹 Function:
- Maturation and storage of sperm
- Provides motility and functional capacity to sperm
- Moves sperm to vas deferens during ejaculation
3. Vas Deferens (Ductus Deferens)
A muscular tube (~45 cm long) that carries sperm from the epididymis to the ejaculatory duct.
🔹 Path:
- Travels through the spermatic cord, enters the inguinal canal, and loops around the urinary bladder.
🔹 Function:
- Transports mature sperm via peristaltic contractions during ejaculation
4. Ejaculatory Ducts
Formed by the union of the vas deferens and the ducts of the seminal vesicles, these short ducts (~2 cm) pass through the prostate gland and open into the prostatic urethra.
🔹 Function:
- Passage of sperm and seminal fluid into the urethra before ejaculation.
5. Urethra
A common passage for urine and semen, it runs through the penis and is divided into:
- Prostatic urethra – within the prostate gland
- Membranous urethra – within the urogenital diaphragm
- Spongy (penile) urethra – through the corpus spongiosum
🔹 Function:
- Conveys semen and urine out of the body (at different times)
🧪 ACCESSORY SEX GLANDS
1. Seminal Vesicles
These are paired, sac-like glands located posterior to the bladder and above the prostate.
🔹 Secretion:
- Produces 60–70% of semen volume, including:
- Fructose (nourishes sperm)
- Prostaglandins (stimulate female contractions)
- Alkaline fluid (neutralizes vaginal acidity)
2. Prostate Gland
A walnut-sized gland located below the bladder and surrounding the prostatic urethra.
🔹 Secretion:
- Contributes 25–30% of semen, including:
- Citrate (nutrient)
- Enzymes (liquefy semen)
- Prostate-specific antigen (PSA)
🔹 Function:
- Enhances sperm motility and longevity
3. Bulbourethral (Cowper’s) Glands
Small pea-sized glands located near the base of the penis, inferior to the prostate.
🔹 Secretion:
- Releases clear, alkaline mucus into the urethra during sexual arousal
🔹 Function:
- Lubricates urethra and neutralizes residual acidic urine to protect sperm
🧠 Hormonal Regulation of Male Reproductive Function
- Hypothalamus secretes GnRH → stimulates anterior pituitary to release:
- FSH – stimulates spermatogenesis (via Sertoli cells)
- LH – stimulates testosterone production (via Leydig cells)
- Testosterone promotes development of secondary sexual characteristics, libido, and sperm production
💡 Clinical Note: Importance in Nursing and Healthcare
- Nurses and clinicians assess male reproductive organs for:
- Testicular torsion, varicocele, or hydrocele
- Erectile dysfunction
- Infertility evaluation
- Benign prostatic hyperplasia (BPH) and prostate cancer
- Sexually transmitted infections (STIs)
- Testicular self-examination (TSE) is taught for early detection of testicular cancer.
🩺 STRUCTURE OF THE BREAST
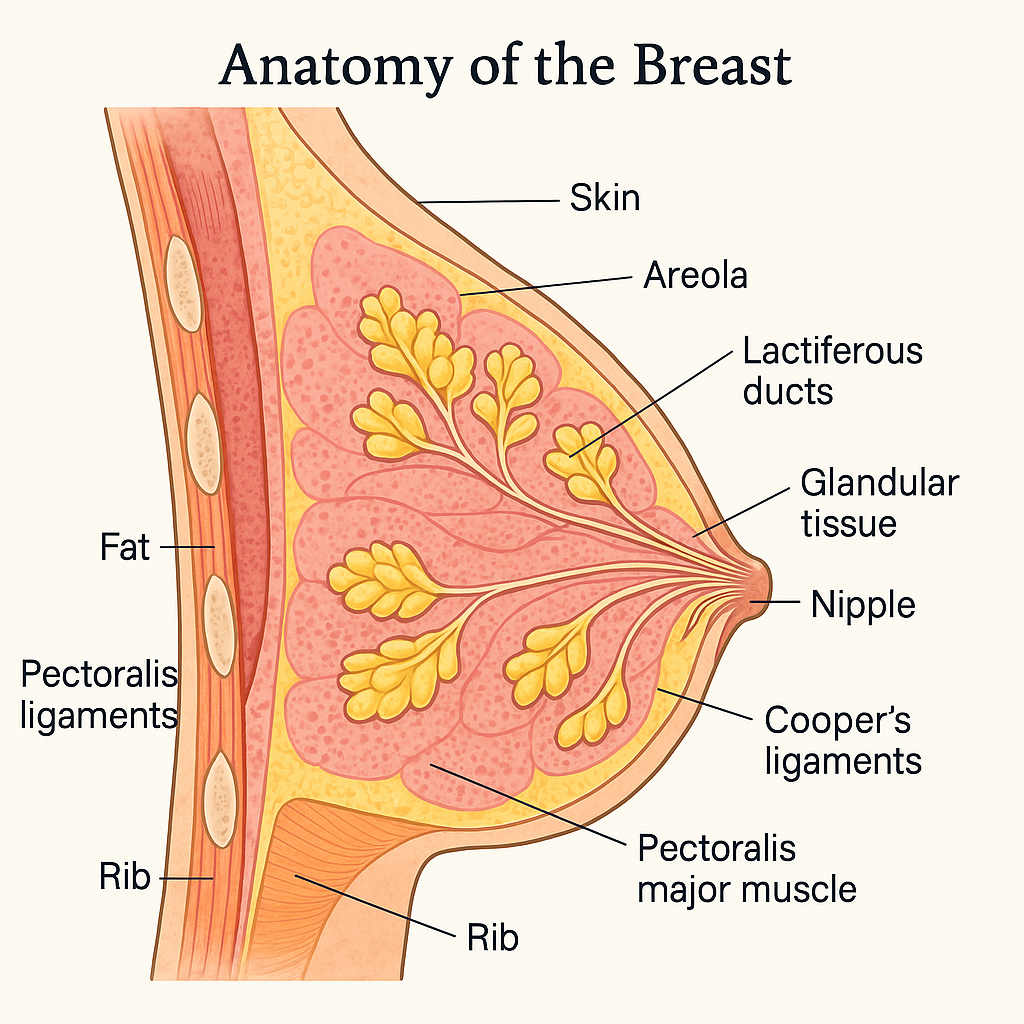
The breast is a paired, modified sweat gland that forms a key component of the female reproductive and endocrine systems. Its primary biological function is milk production (lactation), though it also has significant aesthetic, cultural, and psychological importance.
Breasts are present in both sexes, but in females, they are more developed and functionally active, particularly during puberty, pregnancy, and lactation.
📌 I. Location and External Structure
- Each breast lies in the superficial fascia of the anterior chest wall, extending from the 2nd to the 6th ribs vertically, and from the sternum to the mid-axillary line horizontally.
- Lies over: Pectoralis major and serratus anterior muscles.
- The breast is firmly attached to the overlying skin and the underlying fascia via suspensory ligaments (Cooper’s ligaments).
🔹 External Features:
- Nipple (Papilla)
- Located roughly at the level of the 4th intercostal space (in nulliparous females).
- Contains 15–20 tiny openings (lactiferous duct orifices).
- Composed of smooth muscle fibers, enabling erection in response to stimuli.
- Areola
- Circular, pigmented area surrounding the nipple.
- Contains sebaceous glands (Montgomery’s tubercles) which secrete lubricating fluid during lactation.
- The pigmentation darkens during pregnancy.
🧬 II. Internal Structure of the Breast
The breast is made up of glandular, fibrous (supportive), and fatty (adipose) tissue.
🔸 A. Glandular Tissue (Mammary Glands)
- Divided into 15–20 lobes, each opening into a lactiferous duct.
- Each lobe contains multiple lobules, which consist of alveoli (acini) — the milk-secreting units.
- Myoepithelial cells surrounding the alveoli help expel milk into ducts under the influence of oxytocin.
- Milk travels through lactiferous ducts → stored in lactiferous sinuses → exits through the nipple.
Key Hormonal Influence:
- Estrogen: Promotes ductal growth
- Progesterone: Stimulates lobulo-alveolar development
- Prolactin: Stimulates milk synthesis
- Oxytocin: Causes milk ejection (let-down reflex)
🔸 B. Fibrous Tissue (Stroma)
- Provides structural support.
- Includes Cooper’s ligaments, which anchor the skin to the chest wall fascia.
- These ligaments divide the breast into compartments and are responsible for breast contour.
- Loss of elasticity in these ligaments can lead to breast ptosis (drooping).
🔸 C. Fatty (Adipose) Tissue
- Fills the spaces between lobes and ducts.
- Determines the size and shape of the breast.
- The amount of fat varies among individuals and with age, hormonal status, and nutritional state.
💉 III. Blood Supply
- Arterial Supply:
- Internal thoracic (mammary) artery
- Lateral thoracic artery (branch of axillary artery)
- Thoracoacromial artery
- Posterior intercostal arteries
- Venous Drainage:
- Accompanies arteries; drains into axillary vein, internal thoracic vein, and intercostal veins.
🌐 IV. Lymphatic Drainage
Lymphatic drainage is clinically important due to the high incidence of breast cancer metastasizing via lymphatics.
- Major Drainage (75%): To axillary lymph nodes (especially the anterior/pectoral group).
- Other routes:
- Internal mammary (parasternal) lymph nodes
- Supraclavicular nodes
- Contralateral breast (rare but significant)
Sentinel lymph node biopsy is performed in breast cancer to check for early metastasis.
🧠 V. Nerve Supply
- Supplied by intercostal nerves (T3–T5).
- Sensory innervation to the skin, areola, and nipple.
- Hormonal regulation of milk production and ejection is neuroendocrine, not purely neural.
🤰 VI. Changes During Life Stages
🔸 Puberty:
- Breasts enlarge due to estrogen and growth hormone.
- Ducts elongate, fat accumulates.
🔸 Menstrual Cycle:
- Glandular tissue may swell before menstruation under hormonal influence, causing tenderness.
🔸 Pregnancy:
- Breasts enlarge; ducts and lobules proliferate.
- Areola darkens, Montgomery glands enlarge.
- Colostrum may be secreted in late pregnancy.
🔸 Lactation:
- Fully functional for milk production post-delivery due to prolactin and oxytocin.
🔸 Menopause:
- Involution of glandular tissue; breasts may become softer, smaller, and more fatty.
⚠️ VII. Clinical Relevance in Nursing & Healthcare
Nurses play a vital role in:
- Breast health education: Teaching self-breast examination (SBE)
- Screening and early detection: Assisting in clinical breast exams, mammography
- Recognizing signs of:
- Mastitis
- Fibrocystic changes
- Breast cancer (lumps, dimpling, nipple changes)
- Galactorrhea (abnormal milk secretion)
- Supporting:
- Breastfeeding mothers
- Post-operative mastectomy care
- Body image concerns and cancer survivorship