Anatomy-B.sc-Unit-8-Renal System
🧠 Structure of the Kidney
📍 Basic Overview
| Feature | Description |
|---|---|
| Location | Retroperitoneal space (between T12–L3 vertebrae) |
| Number | Two (left is slightly higher than the right due to liver on the right side) |
| Shape | Bean-shaped |
| Size | ~10–12 cm (length), 5–7 cm (width), 2.5–4 cm (thickness) |
| Weight | ~120–170 grams in adults |
| Color | Reddish-brown |
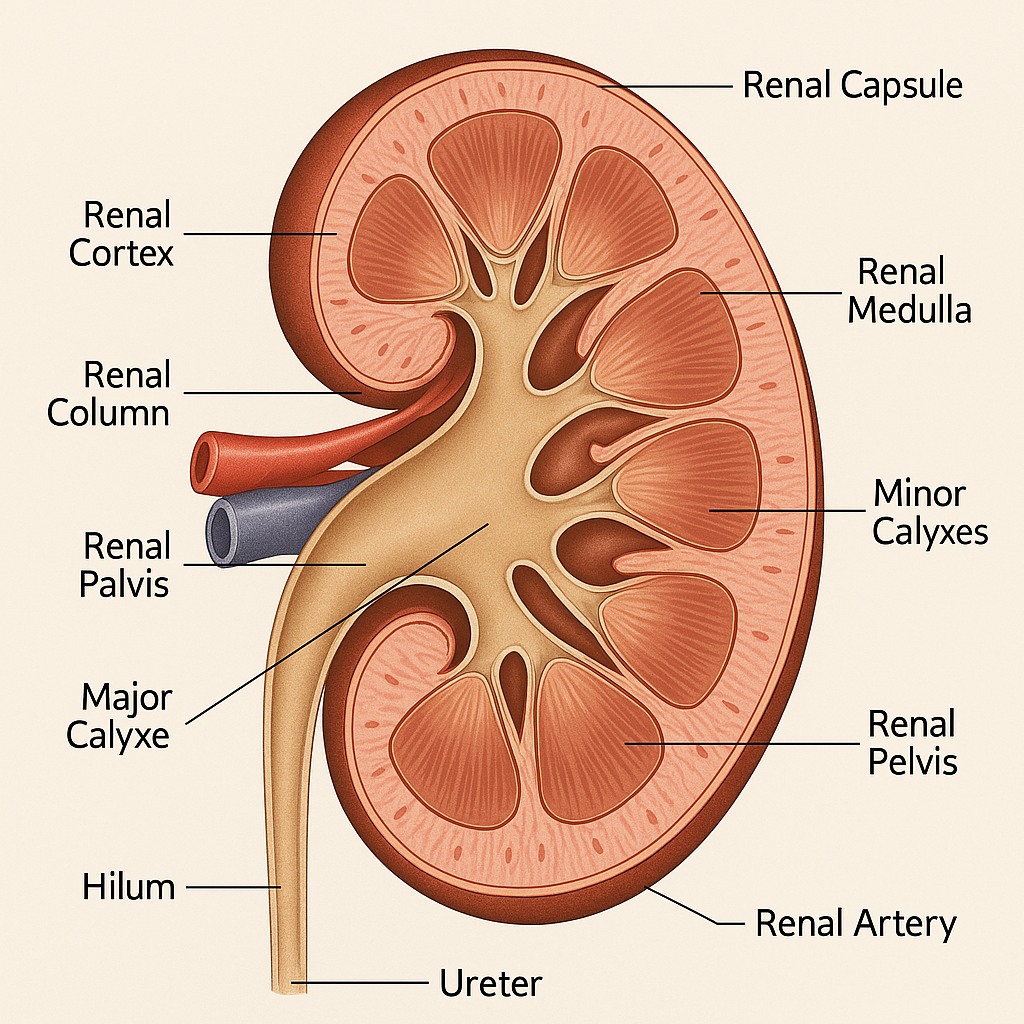
🔍 External Structure of the Kidney
- Renal Capsule
- A tough, fibrous connective tissue membrane.
- Protects against trauma and infections.
- Adipose Capsule (Perirenal fat)
- A layer of fatty tissue around the kidney.
- Provides cushioning and insulation.
- Renal Fascia (Gerota’s Fascia)
- A dense outermost layer anchoring the kidney to surrounding organs.
- Hilum of Kidney
- Medial concave border where structures enter/exit:
- Renal artery (in)
- Renal vein (out)
- Ureter (out)
- Lymphatics and nerves
- Medial concave border where structures enter/exit:
🧬 Internal Structure (Longitudinal Section)
The kidney is divided into three main internal regions:
1. Renal Cortex
- Outer layer (~1 cm thick).
- Contains:
- Renal corpuscles (glomeruli + Bowman’s capsule)
- Proximal and distal convoluted tubules
- Peritubular capillaries
- Function: Site of initial blood filtration (glomerular filtration).
2. Renal Medulla
- Inner portion made up of 8–18 renal pyramids.
- The base faces the cortex; the apex (renal papilla) drains into a minor calyx.
- Between pyramids: Renal columns (cortical extensions).
- Function: Urine concentration, reabsorption, and electrolyte regulation.
3. Renal Pelvis & Calyces
- Renal pelvis: Funnel-like collecting chamber at the center.
- Divides into:
- Major calyces (2–3)
- Minor calyces (8–18)
- Function: Collect urine and drain it into the ureter.
🌟 Nephron – The Structural and Functional Unit
Each kidney contains approximately 1–1.5 million nephrons, responsible for urine formation.
🔬 Parts of a Nephron:
1. Renal Corpuscle
- Located in the cortex.
- Components:
- Glomerulus – A tuft of capillaries.
- Bowman’s capsule – Double-layered epithelial cup that encases the glomerulus.
- Function: Filtration of blood.
2. Renal Tubule
- Begins after Bowman’s capsule.
- Components:
- Proximal Convoluted Tubule (PCT) – Reabsorbs ~65–70% of filtrate (water, glucose, Na⁺, Cl⁻).
- Loop of Henle – U-shaped; has descending and ascending limbs:
- Descending: Reabsorbs water.
- Ascending: Reabsorbs Na⁺, K⁺, Cl⁻ (impermeable to water).
- Distal Convoluted Tubule (DCT) – Secretion of ions (H⁺, K⁺) and hormone-regulated reabsorption.
- Collecting Duct – Final site of water reabsorption; responsive to ADH and aldosterone.
🔄 Blood Supply of the Kidney
Arterial Pathway:
- Renal artery → segmental arteries → interlobar arteries → arcuate arteries → interlobular (cortical radiate) arteries → afferent arteriole → glomerulus → efferent arteriole
Venous Drainage:
- Efferent arteriole → peritubular capillaries/vasa recta → interlobular veins → arcuate veins → interlobar veins → renal vein → inferior vena cava
💡 Note: The vasa recta (in juxtamedullary nephrons) help maintain the medullary osmotic gradient essential for urine concentration.
💦 Flow of Urine Through the Kidney
Nephron → Collecting duct → Renal papilla → Minor calyx → Major calyx → Renal pelvis → Ureter → Urinary bladder → Urethra
🔁 Functions of the Kidney (Linked to Structure)
| Structure | Function |
|---|---|
| Glomerulus | Filtration of blood |
| PCT | Reabsorption of nutrients and electrolytes |
| Loop of Henle | Creates a concentration gradient |
| DCT | Secretion of ions; fine-tunes salt balance |
| Collecting duct | Water reabsorption, regulated by ADH |
| Calyces & Renal pelvis | Transport and collection of urine |
⚠️ Clinical Correlation
| Condition | Affected Structure | Clinical Significance |
|---|---|---|
| Glomerulonephritis | Glomerulus | Proteinuria, hematuria |
| Pyelonephritis | Renal pelvis and calyces | Infection, inflammation |
| Kidney stones (Calculi) | Renal pelvis/ureter | Obstruction, severe pain |
| Renal failure | Nephrons | Waste accumulation, dialysis may be needed |
| Hydronephrosis | Renal pelvis/calyces | Back pressure due to urine retention |
🧠 Mnemonic for Kidney Structures (from outer to inner):
“Certain Mice Prefer Cheese Made Particularly Savory Compared to Rotten Pie”
→ Capsule → Medulla → Pyramids → Columns → Minor calyx → Pelvis → Segmentals → Calyx (major) → Renal artery/vein → Pelvis
🚰 Structure of Ureters
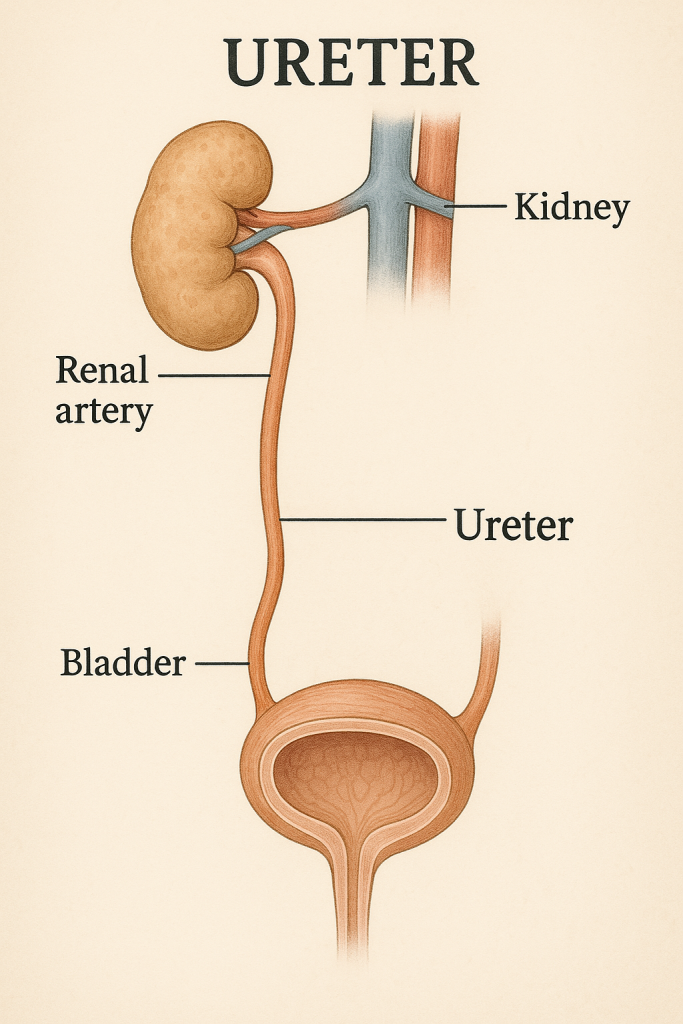
📍 Basic Overview
| Feature | Description |
|---|---|
| Number | Two (one from each kidney) |
| Length | ~25–30 cm |
| Diameter | ~3–5 mm (can vary at constriction sites) |
| Location | Retroperitoneal (behind the peritoneum) |
| Function | Transport of urine from renal pelvis to urinary bladder through peristaltic movements |
🧠 Course of the Ureters
The ureters are divided into three parts based on anatomical location:
1. Abdominal Part
- Extends from the renal pelvis (L1 level) to the pelvic brim.
- Lies on the psoas major muscle.
- Crossed by gonadal vessels and colon (right by ascending colon; left by descending colon).
2. Pelvic Part
- Enters the pelvic cavity.
- In males: passes behind ductus deferens.
- In females: passes under the uterine artery (“water under the bridge“).
3. Intramural (Intravesical) Part
- Shortest part.
- Enters the bladder obliquely through the bladder wall.
- Prevents backflow (vesicoureteral reflux) during micturition.
🔍 Histological Structure (Layers of Ureter Wall)
From inner to outer, the ureter wall is made of three layers:
1. Mucosa (Inner Layer)
- Lined by transitional epithelium (urothelium).
- Has longitudinal folds, allowing expansion.
- Forms a protective barrier against urine toxicity.
2. Muscularis (Middle Layer)
- Smooth muscle responsible for peristalsis.
- Arrangement:
- Upper 2/3: Inner longitudinal & outer circular muscle layers.
- Lower 1/3 (near bladder): Adds an outer longitudinal layer (three layers total).
- Function: Pushes urine downward into the bladder.
3. Adventitia (Outer Layer)
- Connective tissue layer.
- Contains blood vessels, lymphatics, and autonomic nerves.
- Anchors ureter to surrounding tissues.
🚨 Sites of Physiological Narrowing (Ureter Constrictions)
These are common sites for ureteric obstruction (e.g., kidney stones):
- Pelvi-ureteric junction (PUJ) – Where renal pelvis becomes ureter.
- Pelvic brim – Where ureter crosses the iliac vessels.
- Vesico-ureteric junction (VUJ) – Where ureter enters the bladder wall.
🔎 Clinical Tip: Stones are most likely to lodge at these sites.
🧠 Nerve Supply
- Sympathetic: T10–L2 segments – causes vasoconstriction and reduces peristalsis.
- Parasympathetic: S2–S4 (pelvic splanchnic nerves) – enhances peristalsis.
- Sensory fibers carry pain (ureteric colic) via T11–L2 dermatomes → pain radiates from flank to groin.
❤️ Blood Supply of Ureters
The ureter receives segmental blood supply along its course:
| Ureter Part | Arterial Supply From: |
|---|---|
| Upper third | Renal artery |
| Middle third | Gonadal artery, common iliac artery |
| Lower third | Internal iliac artery branches (e.g., uterine, vesical) |
🔄 Venous drainage parallels the arteries.
🧫 Lymphatic Drainage
- Upper ureter: Lateral aortic (lumbar) nodes
- Middle ureter: Common iliac nodes
- Lower ureter: External and internal iliac nodes
💉 Clinical Correlations
| Condition | Relevance to Ureter |
|---|---|
| Ureteric Calculus | Painful obstruction at constriction sites |
| Ureteric injury in surgery | Common during hysterectomy or pelvic operations |
| Vesicoureteral reflux | Defective intravesical angle – urine flows backward |
| Ureterocele | Ballooning at the distal ureter – may obstruct flow |
| Infections (ureteritis) | Often part of ascending urinary tract infections (UTIs) |
🧠 Mnemonic to Remember Ureter Constrictions:
“PUJ, Brim, Bladder”
→ Pelvi-Ureteric Junction, Pelvic Brim, Vesico-Bladder Junction
🧠 STRUCTURE OF THE URINARY BLADDER
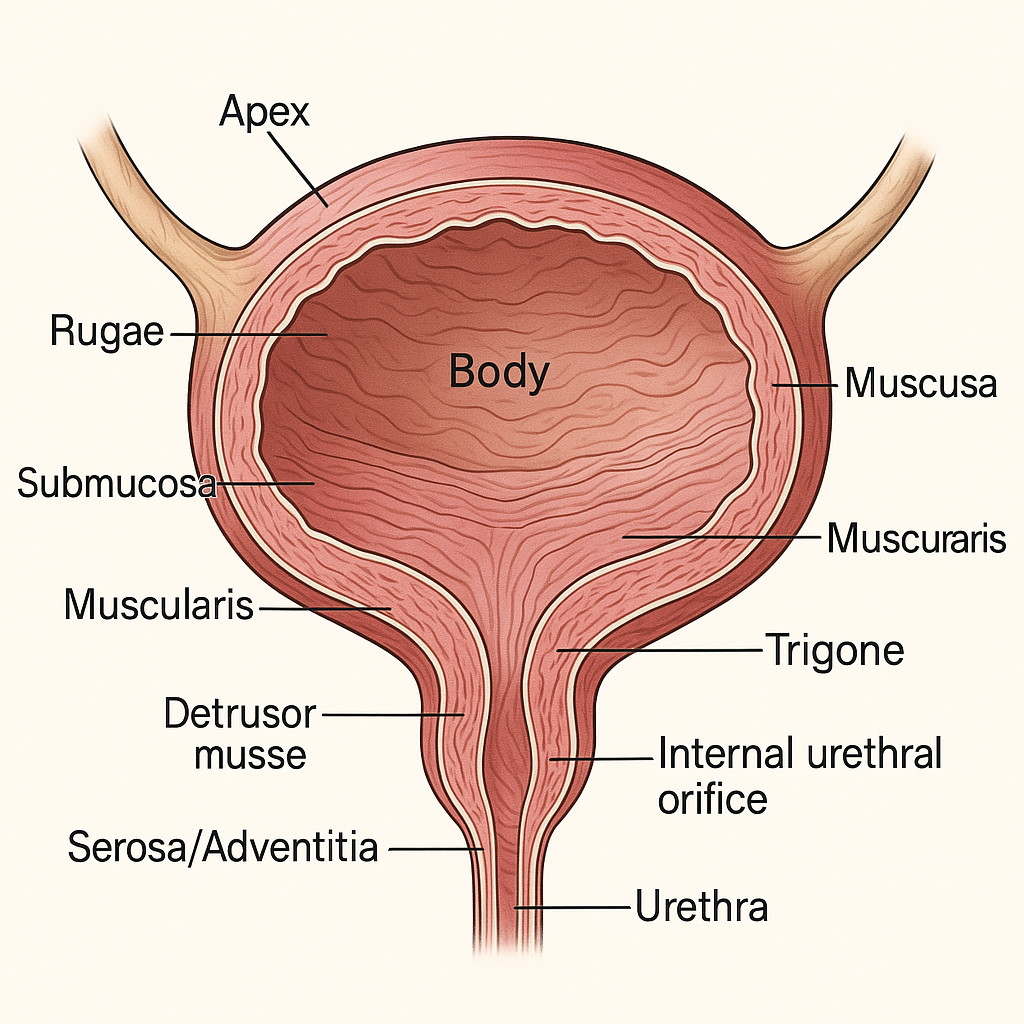
📍 1. Location and Position
🔹 In Males:
- Lies anterior to the rectum, superior to the prostate gland.
- Separated from the rectum by the rectovesical pouch.
- The bladder neck is closely related to the prostate.
🔹 In Females:
- Lies anterior to the uterus and upper vagina.
- Separated from the uterus by the uterovesical pouch.
- Supported by the pubocervical ligament.
🏗️ 2. Gross Anatomy
| Structure | Description |
|---|---|
| Shape | Empty: Tetrahedral; Full: Ovoid |
| Size | Varies with age and bladder fullness |
| Capacity | Average adult capacity: 400–600 mL Urge to void typically felt at 150–300 mL |
| Position when full | May rise above the pubic symphysis and become palpable in the suprapubic region |
| Surface | – Superior surface: covered by peritoneum – Inferolateral surfaces: related to the pelvic floor muscles – Posterior surface (base): faces rectum (male) or vagina (female) |
🔸 Four Anatomical Parts:
- Apex: Anterior tip; connected to median umbilical ligament (urachus remnant).
- Body: Central, largest portion; receives ureters.
- Fundus (Base): Posterior aspect; faces backward and downward.
- Neck: Lowest and most fixed part; continuous with the urethra; contains internal urethral orifice.
🔬 3. Histological Layers (Wall Structure)
The bladder wall consists of four main layers, each with specialized functions:
🔹 a. Mucosa (Inner lining)
- Made of transitional epithelium (urothelium):
- Unique to urinary tract organs.
- Allows stretching and recoil without damage.
- Rugae: Folds that allow expansion; disappear when bladder is full.
- Trigone:
- Smooth triangular area between the two ureteric orifices and the internal urethral orifice.
- Lacks rugae.
- Highly sensitive to stretch; involved in signaling micturition reflex.
🔹 b. Submucosa
- Layer of loose connective tissue containing:
- Blood vessels
- Lymphatics
- Nerve plexuses
- Supports mucosa and helps in nutrient exchange.
🔹 c. Muscularis (Detrusor Muscle)
- Three poorly defined layers of smooth muscle:
- Inner longitudinal
- Middle circular (thicker, helps form internal sphincter at neck)
- Outer longitudinal
- Function: Contracts to expel urine during micturition.
- Innervated by autonomic nervous system.
🔹 d. Serosa/Adventitia (Outer Layer)
- Superior surface: Covered by serosa (peritoneum).
- Inferior and lateral surfaces: Covered by adventitia (connective tissue).
- Anchors bladder to surrounding structures.
⚙️ 4. Ureteric and Urethral Openings
- Ureteric Orifices (2): Located at the posterior angles of the trigone; guarded by a flap-like mucosal valve to prevent reflux.
- Internal Urethral Orifice (1): Located at the inferior angle of trigone; leads to urethra.
- Trigone: Triangle formed by the above three orifices; smooth and non-distensible.
🧠 5. Nerve Supply (Autonomic + Somatic)
| System | Nerve Roots | Action |
|---|---|---|
| Parasympathetic | Pelvic splanchnic nerves (S2–S4) | Stimulates detrusor contraction and relaxation of internal sphincter → urination |
| Sympathetic | T11–L2 | Relaxes detrusor and contracts internal sphincter → urine storage |
| Somatic (voluntary) | Pudendal nerve (S2–S4) | Controls external urethral sphincter |
Micturition reflex: Coordinated by the pontine micturition center in the brainstem and spinal cord reflexes.
💉 6. Blood Supply
🔸 Arterial Supply:
- Superior vesical artery (from umbilical artery)
- Inferior vesical artery (male)
- Vaginal artery (female)
- Obturator and inferior gluteal arteries (contribute collateral branches)
🔸 Venous Drainage:
- Vesical venous plexus
- Drains into internal iliac veins
🌐 7. Lymphatic Drainage
- Primarily drains to:
- External iliac nodes
- Internal iliac nodes
- Sacral lymph nodes
🧪 8. Microscopic Features of Urothelium
- Basal cells: Cuboidal, regenerative.
- Intermediate cells: Pear-shaped, 2–3 layers.
- Superficial (umbrella) cells: Large, dome-shaped, protective, and impermeable to urine.
🧩 9. Developmental & Embryological Origin
- The bladder develops from the upper part of the urogenital sinus (endodermal origin).
- The trigone develops from the mesonephric ducts (mesodermal origin).
⚠️ 10. Clinical Correlations
| Condition | Description |
|---|---|
| Urinary tract infection (UTI) | Infection of bladder lining (cystitis), more common in females |
| Neurogenic bladder | Bladder dysfunction due to spinal cord or nerve injury |
| Bladder calculi | Stones formed in stagnant urine |
| Bladder cancer | Usually arises from transitional epithelium |
| Bladder rupture | Can occur with pelvic trauma; may lead to urine extravasation |
| Detrusor overactivity | Common cause of urge incontinence |
| Cystocele | Herniation of bladder into vagina due to pelvic floor weakness |
🌟 STRUCTURE OF THE URETHRA
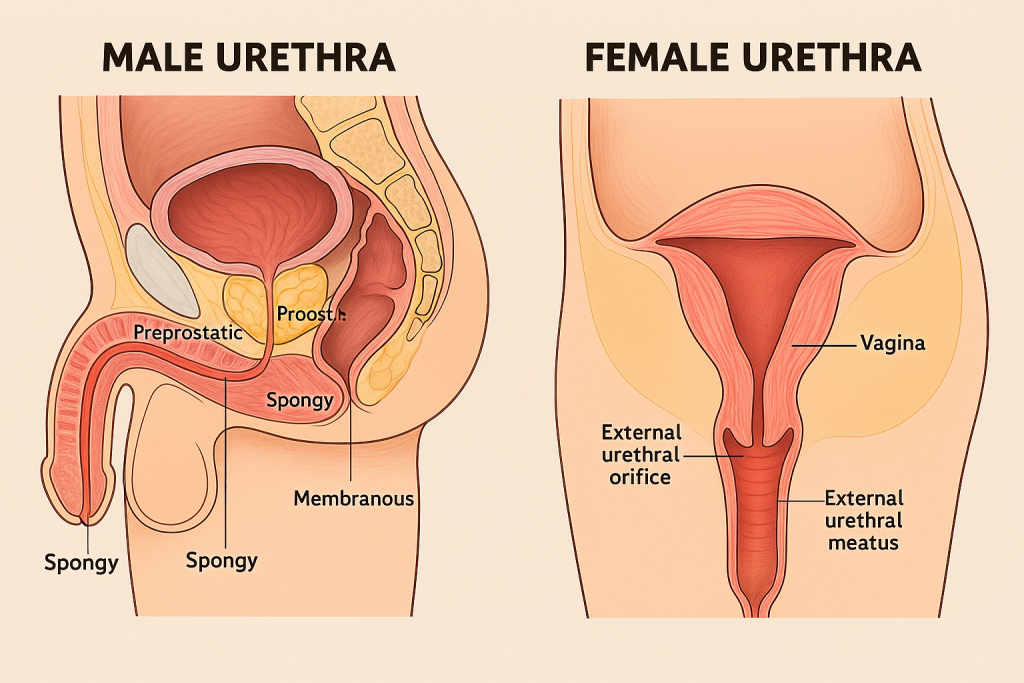
📌 Introduction
The urethra is a fibromuscular tube that serves as the final passage through which urine exits the urinary bladder and leaves the body. While it performs a single function in females — excreting urine, in males, it plays a dual role: conducting both urine and semen (during ejaculation). Although simple in function, the urethra has a complex anatomical and histological design tailored to its role in each sex.
👩⚕️ Female Urethra – Short, Straight & Urinary Only
The female urethra is relatively short, measuring approximately 4 centimeters in length and about 6 millimeters in diameter. It begins at the internal urethral orifice at the neck of the bladder and runs a slightly curved, anterior-inferior path to open into the external urethral meatus, which lies in the vestibule of the vulva, between the clitoris and vaginal opening.
The short length of the female urethra makes catheterization easier but also predisposes women to urinary tract infections (UTIs) due to the proximity of the urethral opening to the anus and vagina.
The wall of the female urethra consists of three key layers:
- The mucosal layer is made up of transitional epithelium near the bladder, which gradually changes to pseudostratified or stratified columnar epithelium, and finally to stratified squamous epithelium near the urethral opening, which is adapted to resist friction.
- The submucosal layer contains rich venous plexuses and elastic tissue, allowing expansion and helping seal the urethra during times of increased abdominal pressure.
- The muscular layer has an inner longitudinal and outer circular smooth muscle, reinforced externally by striated muscle fibers that form the external urethral sphincter, giving voluntary control over urination.
Special glands called paraurethral glands or Skene’s glands, homologous to the male prostate, open near the external urethral meatus and may contribute to lubrication.
👨⚕️ Male Urethra – Long, Curved & Dual-Purpose
The male urethra is significantly longer than its female counterpart, typically around 18 to 20 centimeters in length. It carries both urine from the bladder and sperm/semen from the reproductive tract, making it part of both the urinary and reproductive systems.
The male urethra is divided into four anatomical segments, each with specific features and functions:
- Preprostatic (Intramural) Urethra:
This short segment, approximately 1 cm in length, begins at the internal urethral orifice in the bladder neck. It is surrounded by the internal urethral sphincter, composed of smooth muscle fibers under involuntary control, which plays a vital role in preventing retrograde ejaculation into the bladder. - Prostatic Urethra:
Measuring around 3–4 cm, this portion runs through the prostate gland. It receives secretions from the prostatic ducts, the ejaculatory ducts, and the prostatic utricle (a vestigial remnant of the Müllerian duct). The urethral crest, a longitudinal ridge on the posterior wall, contains the seminal colliculus, where these ducts open. This section has a wider lumen and is lined mainly by transitional epithelium. - Membranous Urethra:
This is the shortest and narrowest part of the urethra (about 1–1.5 cm), passing through the urogenital diaphragm. It is surrounded by the external urethral sphincter, a band of voluntary striated muscle under control of the pudendal nerve (S2–S4), which allows conscious control over urination. - Spongy (Penile) Urethra:
The longest segment (~15 cm), it runs through the corpus spongiosum of the penis and terminates at the external urethral meatus at the tip of the glans. This part is lined by pseudostratified columnar epithelium, which transitions to stratified squamous epithelium distally. Along its length, it receives mucus from the glands of Littre, and just before it enters the penile bulb, it receives secretions from the bulbourethral (Cowper’s) glands, which lubricate and neutralize acidic urine before ejaculation.
🧠 Sphincters and Control of Micturition
The internal urethral sphincter is present only in males and is composed of smooth muscle fibers. It is involuntarily controlled by the sympathetic nervous system and plays a key role during ejaculation by preventing the backward flow of semen into the bladder.
The external urethral sphincter, present in both sexes, is composed of skeletal muscle and provides voluntary control over urination. It is innervated by the pudendal nerve, allowing conscious regulation of micturition.
🩸 Blood and Nerve Supply
The urethra’s blood supply comes from branches of the internal pudendal artery, the inferior vesical artery, and in females, also from the vaginal artery. Venous drainage corresponds to the arterial supply and flows into the internal pudendal vein.
Nerve supply includes:
- Somatic fibers from the pudendal nerve that control voluntary sphincters.
- Autonomic fibers from the pelvic plexus, including sympathetic (T11–L2) and parasympathetic (S2–S4) innervation, which coordinate relaxation and contraction of the bladder and urethra during urination.
🌐 Lymphatic Drainage
- The proximal urethra (in both sexes) drains into the internal iliac lymph nodes.
- The distal urethra (especially in males) drains into the deep and superficial inguinal lymph nodes.
⚠️ Clinical Correlations
Understanding urethral anatomy is essential in diagnosing and managing several common and serious conditions:
- Urethritis is inflammation of the urethra, commonly caused by sexually transmitted infections (e.g., gonorrhea, chlamydia).
- Urethral strictures occur due to scarring from infection, trauma, or catheterization, leading to urinary obstruction.
- Urinary incontinence often results from weakened sphincter muscles or nerve damage.
- Hypospadias is a congenital condition in males where the urethral opening is on the underside of the penis.
- Catheter-related injuries, especially in males, can occur if anatomical curvature and segments are not carefully navigated.
- Urethral carcinoma, though rare, can affect the urethral epithelium, with squamous cell carcinoma more common in females.
🎯
The urethra, though narrow and often overlooked, plays a crucial role in both urinary and reproductive physiology. Its structure varies significantly between males and females, both in length and function. With a delicate balance of muscle control, epithelial transitions, and strategic glandular input, the urethra is a finely tuned organ whose disorders can significantly affect quality of life.
🩺 The Renal (Urinary) System: Application and Implications in Nursing
🔍
The renal system, also known as the urinary system, plays a fundamental role in maintaining physiological homeostasis. It is essential not only for waste elimination, but also for regulating fluid balance, electrolyte composition, acid-base equilibrium, blood pressure, and erythropoiesis. In nursing practice, a deep understanding of the renal system enables effective patient assessment, intervention, and care planning, especially in critical care, medical-surgical units, geriatrics, and nephrology settings.
🧠 Anatomy and Physiology: A Nursing Perspective
The renal system comprises two kidneys, two ureters, one urinary bladder, and one urethra. Each component contributes to the formation, transport, storage, and elimination of urine.
✨ Major Functions of the Renal System:
- Filtration of blood to remove waste products (urea, creatinine, toxins)
- Regulation of fluid balance through selective reabsorption and secretion
- Electrolyte regulation, especially sodium, potassium, calcium, and phosphate
- Acid-base balance via H⁺ ion secretion and bicarbonate retention
- Regulation of blood pressure via the renin-angiotensin-aldosterone system (RAAS)
- Erythropoietin production for stimulation of red blood cell formation
- Activation of vitamin D into its active form (calcitriol), essential for calcium absorption
🧾 Application in Nursing Practice
1. Comprehensive Assessment of Renal Function
A nurse’s ability to recognize early signs of renal dysfunction is critical. Assessment includes:
- Intake and output (I&O) charting – helps detect fluid imbalance or renal failure.
- Urine examination – monitoring color, clarity, odor, volume, and abnormalities such as hematuria, proteinuria, or sediment.
- Signs of fluid overload – including edema, hypertension, jugular vein distension, shortness of breath.
- Signs of fluid deficit – such as dry mucous membranes, hypotension, tachycardia, low urine output.
- Palpation and percussion – assessing for bladder distention or costovertebral angle tenderness (suggestive of infection or stones).
- Daily weight monitoring – most accurate indicator of fluid retention.
2. Nurse’s Role in Diagnostic Procedures
Nurses are instrumental in preparation, monitoring, and post-procedure care for diagnostic tests such as:
- Urinalysis (U/A) – reveals infection, protein, glucose, ketones, or blood in urine.
- 24-hour urine collection – assesses creatinine clearance and proteinuria.
- Blood tests – including BUN, serum creatinine, GFR, and electrolyte levels.
- Renal ultrasound, CT scan, or MRI – assess structural abnormalities.
- Cystoscopy – visualization of the bladder; nurses monitor for bleeding, infection post-procedure.
- Renal biopsy – nurses assist in pre-procedure preparation, monitor for bleeding, and enforce strict bed rest afterward.
3. Medication Management and Monitoring
The kidneys are involved in metabolizing and excreting drugs, making renal function a key consideration for safe medication administration. Nurses must:
- Review renal function tests before administering nephrotoxic drugs (e.g., aminoglycosides, vancomycin, NSAIDs, contrast media).
- Adjust doses in patients with renal impairment.
- Monitor side effects of diuretics (loop, thiazide, potassium-sparing) including hypokalemia or hyperkalemia.
- Educate patients on fluid restrictions and electrolyte control.
- Encourage adherence to prescribed phosphate binders or sodium bicarbonate in CKD patients.
4. Clinical Care in Common Renal Conditions
a) Urinary Tract Infections (UTIs)
Nurses are often the first to detect early UTI symptoms like burning sensation, urgency, frequency, cloudy urine, or lower abdominal pain. Nursing interventions include:
- Promoting perineal hygiene and adequate hydration
- Timely collection of urine cultures
- Administering antibiotics as prescribed
- Monitoring for complications like pyelonephritis, especially in the elderly
b) Chronic Kidney Disease (CKD)
CKD is a progressive and irreversible condition. Nurses play a central role in:
- Monitoring for uremia symptoms: fatigue, confusion, nausea
- Managing fluid restrictions and sodium/potassium-controlled diets
- Monitoring for anemia, bone disease, and cardiovascular risks
- Educating patients about dialysis, transplant eligibility, and psychosocial support
c) Acute Kidney Injury (AKI)
AKI is sudden and reversible with prompt intervention. Nursing priorities include:
- Early detection of oliguria, azotemia, and electrolyte imbalances
- Preventing further renal insult by reviewing medications and maintaining hydration
- Monitoring blood pressure, I&O, daily weight, and mental status
- Collaborating in fluid and electrolyte replacement therapies
d) Nephrolithiasis (Kidney Stones)
Nurses manage:
- Pain relief using prescribed analgesics and antispasmodics
- Encouraging fluid intake to facilitate stone passage
- Straining urine to collect stones for analysis
- Preparing patients for lithotripsy or stone removal surgery if needed
e) Urinary Incontinence and Retention
Incontinence impacts physical and emotional well-being. Nursing interventions include:
- Behavioral therapies: bladder training, scheduled voiding
- Pelvic floor exercises (Kegels)
- Catheterization for retention: intermittent or indwelling, with infection prevention
- Preventing skin breakdown, ensuring privacy and dignity
5. Catheter Care and Infection Control
Nurses are responsible for urinary catheter insertion, maintenance, and removal. Key principles include:
- Strict adherence to aseptic technique during insertion
- Daily assessment for catheter necessity to prevent CAUTI
- Securing the catheter to prevent urethral trauma
- Ensuring free urine flow, regular emptying of drainage bag, and hygiene care
6. Dialysis Care and Nursing Responsibilities
a) Hemodialysis
- Monitor vascular access site (AV fistula or graft) for thrill/bruit
- Prevent infection and protect access arm (no BP or IVs)
- Monitor for hypotension, cramps, or bleeding
- Support patient emotionally and physically before, during, and after sessions
b) Peritoneal Dialysis
- Maintain strict aseptic technique during exchanges
- Monitor dialysate clarity, input/output, and signs of peritonitis
- Educate patient/family on self-care technique and infection prevention
7. Health Education and Counseling
Nurses play an essential role in educating renal patients:
- Dietary advice: limit salt, potassium, phosphorus, and protein as required
- Encourage adequate hydration (unless contraindicated)
- Inform about warning signs: changes in urination, fatigue, swelling, confusion
- Encourage medication adherence and regular follow-ups
- Support smoking cessation, alcohol reduction, and BP control
- Prepare patients and families for dialysis or transplant journey
8. Psychosocial and Holistic Support
Renal disease, especially CKD or end-stage renal disease (ESRD), affects emotional, social, and financial aspects of life. Nurses must:
- Provide psychological support, addressing anxiety, depression, or denial
- Refer to support groups, counselors, and social workers
- Support patients in adjusting to lifestyle modifications, dialysis schedules, or body image changes
- Promote holistic care that includes spiritual and cultural needs
✅
The renal system is a cornerstone of body regulation, and its dysfunction can have widespread effects on multiple organs. For nurses, understanding the renal system is not only a theoretical requirement but a clinical necessity. From basic assessments to complex dialysis management, nursing care in renal health demands knowledge, precision, empathy, and advocacy. By applying renal concepts to nursing practice, nurses can ensure early detection, safe intervention, and comprehensive support to patients with renal conditions, ultimately improving outcomes and quality of life.