ENGLISH-msn-2-oncology-Part-02
Oncology

♦ What is Oncology?

Oncology is a branch of medicine that deals with the diagnosis and treatment of cancer. A person who is involved in the practice of Oncology is called an oncologist.

Oncology is formed with the words ONKOS : BULK, MASS : TUMOR, LOGY MEANING : STUDY OF is.

There are three main branches of Oncology:
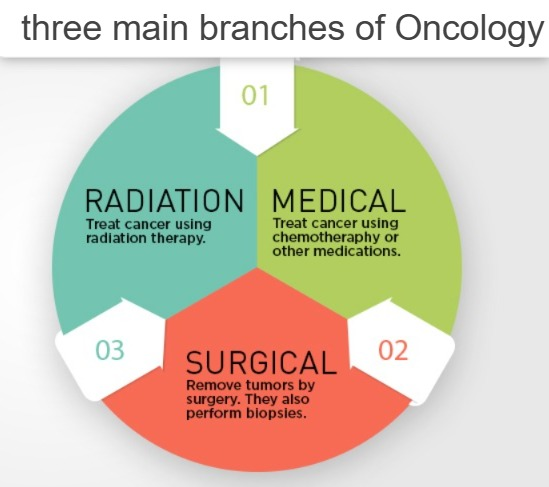
1) Medical oncology: In this, treatment begins with drugs and chemotherapy.
2) Surgical oncology: In this, cancer is treated through biopsy, any surgery, and surgical resection of any tumor, etc.
3) Radiation oncology: In this, cancer is treated through therapeutic radiation.
♦ DEFINE CANCER OR WHAT IS CANCER (केंसर इत्ने की) :
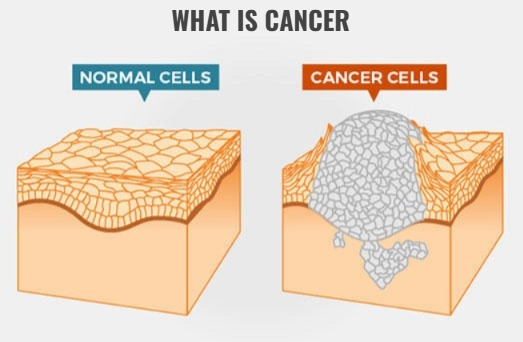
Cancer is a group of diseases in which cells grow uncontrollably and can invade nearby tissues and spread throughout the body. Cancer is a disease in which cells grow uncontrollably and multiply, and can spread to nearby areas and even to the entire body. Cancer cells spread throughout the body through the blood and lymphatic system. Cancer is not a single disease but a group of about 100 cancers. Cancer is named after the part of the body where it occurs or not. Cancer is named after the part where it occurs.
♦ EXPLAIN STRUCTURE OR CHARACTERISTICS OF NORMAL CELLS.:
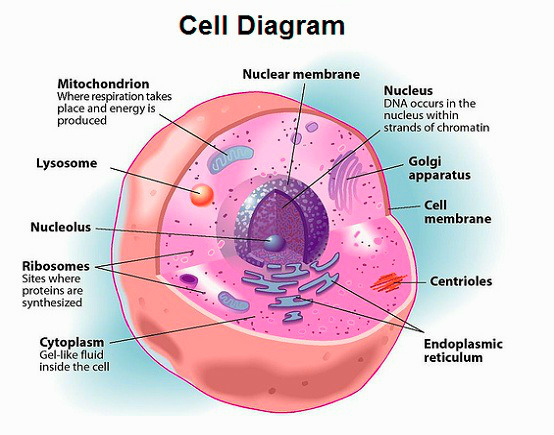
- 1) Mitotic division results in the formation of two daughter cells.
- 2) In this, the shape, size, and arrangement of the daughter cell are the same as the original cell.
- 3) In this, the cell is formed for any specific function.
- 4) It does not invade and enter the blood circulation and lymphatic circulation.
- 5) In this, the division of the cell stops. When it comes into contact with any other cell, it has the characteristics of contact inhibition.
- 6) These cells cannot spread to other parts of the body.
♦ EXPLAIN STRUCTURE OR CHARACTERISTICS OF ABNORMAL CELLS. (Explain the structure and characteristics of abnormal cells – cancerous cells or malignant cells)
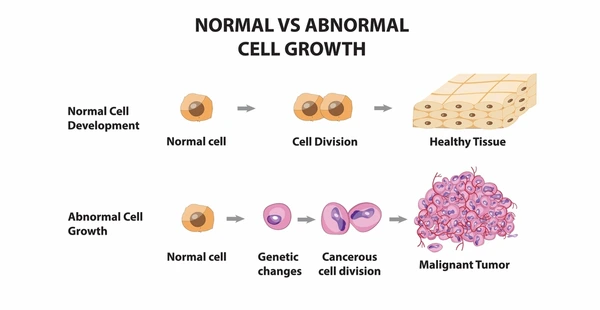
- 1) In this, many daughter cells are produced due to cell division and they do not even look like the parent cell.
- 2) In this, the cell grows rapidly
- 3) In this, the daughter CELL is different from the normal CELL in shape, size and appearance.
- 4) This CELL is not produced for a specific purpose but its abnormal growth occurs.
- 5) This CELL travels in the blood, lymphatic circulation and other systems of the body.
- 6) It does not have the characteristics of contact inhibition, so the CELL continues to grow abnormally and forms a tumor-like structure.
- 7) In this, abnormal CELLs spread to other organs in the body and grow.
♦ What are the Different between Benign tumor or Malignant tumor ? What is the difference between a benign tumor and a malignant tumor (cancerous tumor)?
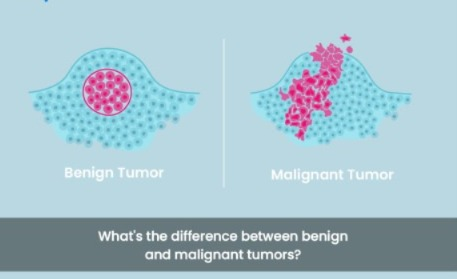
Benign tumor (Benign tumor) :-
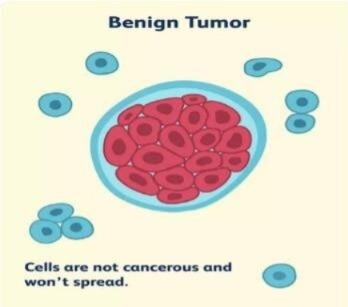
1) CELL feature: In this, CELL growth occurs and forms a tumor-like structure but this tumor is not cancerous.
2) CELL growth rate: In this, the growth of CELL occurs slowly.
3) Tissue damage: In this, the tissue is damaged to a small extent.
4) Metastasis: The tumor of CELL remains in the same place where it was formed and does not go to another place.
5) General effect : This benign tumor is less harmful when it does not put any pressure on the circulation.
6) treatment and follow up: After this tumor is surgically removed, no follow-up is required.
7) severity: Since this tumor is localized, it does not affect vital organs too much.
Malignant tumor:-
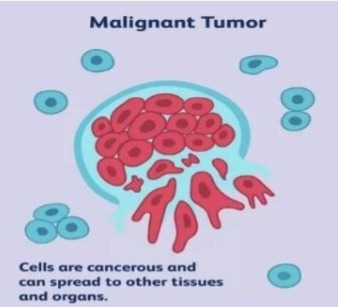
1) CELL features: Thus. The tissue is undifferentiated and often has some resemblance to normal cells of the tissue and malignant cells grow from it.
2)GROWTH rate: These cells grow very quickly.
3)Tissue damage:This causes a lot of damage to the tissue and causes tissue necrosis.
4) Metastasis: This tumor can spread to nearby organs and distant organs.
5)General effect: This is very harmful because it also damages the normal shell.
6)Treatment and follow up: After surgical removal of this tumor, chemotherapy and radiation therapy are required.
7)Severity: This tumor is not controllable and this tumor leads to death.
Cancer (Cancer):
Cancer is a very serious disease in which cells grow abnormally and form a tumor-like structure and this tumor spreads to other parts of the body and even there, the organs of the body Function ulter thus cancer is a very dangerous disease.
Etiology and risk factors:

Etiology (Etiology):
1) Age: The chances of getting cancer increase with age because as you get older, the body’s immune system gets weaker and due to this, diseases like cancer occur.
2) Gender:
In male: Prostate, lung, gastrointestinal tract, bladder etc.
In females: Breast cancer, colon ,lung, uterus are the most common cancerous site in females.
3)Race: Black community has a higher chance of getting cancer than white community.
4)Genetic / hereditary: People who have hereditary cancer have a higher chance of getting cancer in their sons or daughters than the general population.
5)Immunological Factor: When the body’s immune system is weakened, there are chances of getting cancer because the immune system is not strong enough to fight against cancerous cells and due to this, cancer-like conditions occur.
6)Psychological factors: People who take too much stress increase the level of hormones and the body’s immune system is altered. And due to this, cancer-like conditions occur.
7)Hormonal factor:
Endogenous: In this, there are changes in the body’s hormones and due to this, cancer of organs like breast, uterus and prostate gland occurs.
Exogenous : In this, due to taking any type of oral contraceptives, there is an imbalance in hormones and due to this, cancer occurs in the body.
External risk factor: External factors include any type of chemical, radiation, virus, tobacco and alcohol, obesity, and excessive exposure to sunlight.
1) Chemical carcinogens: In this, cancer can occur in the body due to contact with certain types of chemicals.
Example: asbestos, arsenic, chemical therapy.
2) Radiation therapy: In this, there is a higher chance of skin cancer due to the thinning of the ozone layer due to ultraviolet rays of sunlight.
3) Viruses: Certain types of viruses lead to cancer in humans.
Example: Epstein barr virus is linked with ->Lymphoma,
Herpes simplex,
Cytomegalovirus,
human papillomavirus type 16-18 ,
HIV virus.
4)Diet: Certain types of food and substances added to food cause cancer of the gastrointestinal tract. Low fiber diet causes colon cancer Smoked and processed meat causes liver cancer. Excessive fat, alcohol, food contain nitrate, high calories in diet also cause cancer.
5)tobacco: Tobacco and smoking cause cancers like mouth cancer, esophagus cancer, esophageal cancer, and lung cancer, oral cancer etc.
6)Alcohol use: Alcohol consumption causes cancer of the oral cavity, larynx, esophagus etc.
7)Recreational drug use:This reduces the body’s immunity. Marijuana smoke is more dangerous because of this, it can cause lung Cancer occurs.
8)Obesity: Excess body fat causes hormone-related cancers.
9)sun exposure: Excessive exposure to sunlight causes skin cancer.
Chemical agent : Aromatic amyl, Different type of dyes,arsenic, benzene,zinc,wood dust, polyvinyl chloride. Chemical substances like etc. also cause cancer.
Classification of cancer cell:
1)GRADDING ,
2)STAGGING,
3)T.N.M .
(T=TUMOR, N=NODE, M=METASTASIS).
GRADDING (grading):

A =Anaplasia
(In this case, the cell does not look like its parent cell but is different.)
Grade 1:
This grade is called low grade malignancy. Cells are similar to normal parent cells. It have <25%Anaplasia cell.
Grade 2:
It has low to moderate degree Malignant cells. Some cells are normal and some cells are cancerous. It has 25 to 50 % Anaplasia cell.
Grade 3:
It has moderate to high grade cell malignancy. It has 50 to 75% Anaplasia cells.
Grade 4 :
This has high grade malignancy and all the cells are malignant. It has >75% Anaplasia cells.
Staging:
Stage (0): No abnormal cells are seen in this because the abnormal cells are only in the first layer of cells.
Stage 1: In this, the cancer is only in the primary cell site.
Stage 1 (a): In this, the cancerous cells are present in small quantities and are visible under a microscope.
Stage 1 (b): In this, the cancerous cells are present in large quantities.
Stage 2: In this, the cancer spreads to nearby areas.
Stage 2 (a):In this, the cancer spreads to the primary area.
stage 2 (b):In this, the cancer spreads to tissues and organs.
stage 3:In this, the cancer spreads to nearby areas.
stage 4: In this, the cancer spreads to other parts of the body.
Stage 4 (a): In this, the cancer spreads to nearby body parts.
Stage 4 (b): In this, the cancer spreads to other organs and tissues of the body.
classification on the basis of TNM (TUMOR, NODE AND METASTASIS):

1)T : TUMOR: This depends on the size of the tumor and its extension. Tx: The tumor cannot be evaluated in this. To : In this, some cells are abnormal but no signs of a tumor are seen.
T1234: In this, the size of the tumor and its expansion are like the primary tumor.
2)N : NODE : In this, it depends on how much lymph node is involved.
Nx: In this, there are cancerous cells in the lymph node. Evaluation cannot be done.
N1: In this, metastasis of cancerous cells is seen in the area and region near the lymph node.
N2: In this, the cancerous cells are between N1 and N3, that is, they do not spread to all tissues.
N3: In this, the cancerous cells spread to many areas of the lymph node.
3)M : METASTASIS: In this, the cancerous cells spread to another part of the body. M1: In this, metastasis of the cells is not seen. M2: In this, the cancerous cell has spread to another part of the body (organ).
Detection of cancer: >History taking, >Physical examination, >Laboratory investigation.
History taking: In this, a complete assessment of the patient is done in which the patient is asked about any current or past surgical history or whether any family member has signs and symptoms of cancer.
Physical examination: When we do a physical examination, we look for The patient may experience
Anorexia: (anorexia: loss of appetite). weight loss: (weight loss: weight loss).
Anemia (anemia: low blood volume).
weakness (weakness: weakness).
Fatigue (Fatigue: Feeling tired).
pain (Pain: Pain). etc. To see if the patient has signs and symptoms.
1) lymphadenopathy (lymphadenopathy), 2) suspicious mole (suspicious mole), 3) Breast mass (breast mass), 4) Thyroid mass (thyroid mass), 5) Prostate enlargement (prostate enlargement), 6) oral leukoplakia (oral leukoplakia: white sores in the mouth) Thus, the patient may see such signs. To see if it is or not.
Laboratory test:
1)Phosphate specific antigen: This is a laboratory test for the detection of prostate gland cancer.
2)complete blood count (cbc): This test is done to see if there is a condition like anemia or not and if there is anemia then colon cancer can be detected.
3)stool test (blood in stool): If blood is found in the stool then it may be the cause of colon rectal cancer.
4) Biopsy: If there is any abnormal cell growth, a small piece of that cell is taken and it is examined microscopically in the laboratory and cancer is detected.
This biopsy can be taken from organs like the liver, kidney, spleen, lungs, breast etc. and cancer can be detected.
5) Cytological study: This diagnostic test uses a smear similar to a pap smear and can be taken mainly from the cervix and oral cavity.
6) Ultrasound test: This test uses high frequency sound waves and ultrasound is mostly used to detect abdominal, pelvic and breast cancer.
7) MRI (magnetic resonance imaging): This test is done to see if there is any cancer of the central nervous system, spine, head and musculoskeletal system etc.
8) Radiological study: X-ray is done to see if there is bone cancer and cancer of any hollow organ. Chest x-ray is done to detect lung cancer. Mammography is done to detect breast cancer. Contrast media is used to detect cancers of the bone, gastrointestinal system, urinary system, etc.
9) CT SCAN (COMPUTED TOMOGRAPHY): CT scan provides a 3-dimensional, cross sectional, computerized picture of the body. CT scan accurately shows the size and location of any tumor. CT scan shows the differentiation between malignant and non-malignant.
10) Nuclear imaging procedure: This test is done to detect cancer of organs like brain, kidney, liver, lungs, pericardium (outer layer of heart) and bone etc.
11) PET test (positron emission tomography): This test is done to detect cancer of organs like lungs, colon, breast, bone, brain etc.
Other test: Blood test, urine test, pap smear test, Afp (alpha photo protein for liver cancer) etc test used for detection of cancer.
Prevention of cancer (Prevention of Cancer):

1)Primary prevention:

It is done to reduce risk factors.
OBJECTIVE: 1) To strengthen healthy lifestyle. 2) To reduce weakness. 3) To reduce the risk factors of cancer.
Influencing factors of carcinogenesis:
Diet: Fatty, alpha toxin, non antioxidant, smoky, uncooked raw food.
★Smoking and drinking,
★viral infection,
★parasite,
★chemical agents,
★ultraviolet rays,
★x-ray,
★Obesity,
★polluted environment,
★lack of exercise,
★Limited to health care services.
prevention of cancer:

1) Eat green leafy vegetables.
2) Consume fiber-rich foods.
3) Take vitamin A and vitamin C.
4) Improve the quality of your lifestyle.
5) Exercise daily.
6) Reduce fatty foods in your diet.
7) Reduce the intake of sugary foods.
8) Use medical facilities properly.
9) Avoid things that are responsible for causing cancer such as tobacco, cigarette smoking, sedentary lifestyle, stress, fatty and spicy food and many other things that are responsible for cancer.
10) Avoid alcohol.
11) Avoid excessive sun exposure.
12) Avoid excessive exposure to X-rays and ultraviolet rays.
13) Provide health education to people about the causes of cancer and also provide health education to prevent it.
14) Tell people to work a little bit and not to lead a sedentary life.
15) Tell people to get regular health check-ups.
2) Secondary prevention (secondary prevention):

This secondary prevention includes early diagnosis and prompt treatment, which requires early screening for cancer. is.
objective: 1) early diagnosis and investigation of Abnormality. 2) assessment of the risk group. 3) Cancer screening and early detection.
THE WARNING SIGN OF CANCER:

CAUTION :

C: CHANGE IN BOWEL AND BLADDER HABIT, In this, there is a change in the color of the stool, its size and its shape. ex: Diarrhea, constipation. In this, blood is present in the urine and stool.
A: A SORE WHICH DOES NOT HEAL, In this, there is no healing in any type of sore. ★more bigger, ★more pain full, ★start bleeding from the sore.
U : UNUSUAL DISCHARGE AND BLEEDING, Blood comes in urine and stool. ★Discharge comes from any part of the body such as nipple, Penis.
T: THICKENING OF LUMP IN BREAST AND OTHER BODY PARTS, Jay.Ray When breast self examination is done, a lump, mass in the breast is seen. Lumps can be found on any part of the body.
I : INDIGESTION AND DIFFICULTY IN SWALLOWING , In this, there is pressure on the throat and chest and due to this there is difficulty in swallowing. If even a little is eaten, the stomach feels very bloated.
O : OBVIOUS CHANGE IN MOLE, Use THE ABCD RULE ,
A: ASYMMETRY See if the mole looks the same from all parts or different.
B: Border See if the border is sharp or rough.
C: color See what kind of color is seen in the mole.
D: Diameter The diameter of this mole is larger than an eraser, i.e. larger than 6 mm.
N:=NAGGING , COUGH SORENESS .
See if there is a change in voice, see how long the phlegm has been coming,
See if there is blood in the phlegm.
Ask the patient about all these cancer warnings.
Assessment of the patient’s health Do (Assessing the patient’s health):

>tacking history (asking the patient about their history),
>family and personal history of cancer, (asking whether anyone has a history of a disease like cancer).
>tobacco use and alcohol consumption, (asking whether the person consumes tobacco and alcohol)
>occupation (asking about his/her occupation),
>Medication (asking about medication).
Encourage the client for early detection of cancer:

MAMMOGRAPHY (mammography) :
- Mammography is an examination of the breast.
- >Mammography should be done once in 3 years in the age group of 20-30 years. >All women over the age of 40 years should have mammography done every year. Every woman should do breast self-examination after the age of 20.
- If there is any abnormality in the breast, immediately inform the health care worker and if any lump, mass or size, symmetrical abnormality is found in the breast, immediately inform the health care professional or health care personnel.
- If anyone in the family has a history of breast cancer, daughters should take the advice of a health care member.
colon and rectal cancer (colon and rectal cancer) :
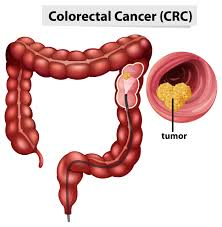
After the age of 50, every man and woman is at risk of developing colorectal cancer. So after the age of 50, the following tests should be done.
1) FECAL OCCULT BLOOD TEST (FOBT) should be done every year.
2) (FIT) FECAL IMMUNOLOGICAL TEST should be done every year.
3) FLEXIBLE SIGMOIDOSCOPY should be done every five years.
4) Colonoscopy should be done every 10 years.
5) DOUBLE CONTRAST BARIUM ENEMA TEST should be done every 5 years Should.
6) CT COLONOGRAPHY should be done every five years.
7) Stool DNA test.
CERVICAL CANCER (Cervical Cancer) :
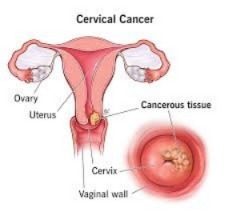
1)Every woman should get screened for cervical cancer every 3 years after vaginal intercourse.
2)After the age of 30 years, women should get screened for cervical cancer every 3 years. If 3 Pap smear tests are normal, she should continue to have a Pap smear test every two to three (2-3) years.
3) If a woman has a risk factor such as Diethylstilbestrol exposure, HIV infection, Or a weakened immune system due to organ transplantation, Chronic steroid use, such women should have a pap smear test every year.
4) If a woman is over 70 years of age and has had 3 negative pap smears, she should be examined every 10 years.
5) Endometrial cancer (uterine) If a woman has had a total hysterectomy, she does not need to have a pap smear test.
6) If a woman has a history of colon or rectal cancer, she should have a pap smear test.
TERTIARY PREVENTION (Tertiary Prevention) :

In TERTIARY prevention Tertiary care is used to prevent metastasis of abnormal cells, provide treatment for cancer, cure it, perform rehabilitation, and provide palliative care. Prevention is done.
The following treatment are useful for cancerous patients:
- RADIATION THERAPY (Radiation Therapy)
- CHEMOTHERAPY (chemo therapy)
- GENE THERAPY
- BIOTHERAPY
- BONE MARROW TRANSPLANTATION Transplantation)
1) RADIATION THERAPY (Radiation Therapy)

Ionizing radiation is used in radiation therapy. Abnormal cellular growth is prevented using radiation. This radiation therapy damages cancerous cells and causes them to necrosis.
purpose:
1) Primary (Primary): Primary purpose is only for the treatment and cure of cancer. Example : hodgkin’s disease, skin cancer, Prostate Cancer, cancer of cervix.
2) Adjuvant : This is used only in preoperative and postoperative conditions and is used with chemotherapy.
3) palliative: This is used in any emergency condition such as superior vena cava compression (superior vena cava) and spinal cord compression.etc
4) Prophylactic purpose (Prophylactic Purpose): This radiation therapy is given only in the suspected area.
Action of radiation therapy (radiation therapy action):
1)Normal cell: Radiation therapy affects normal cells, but normal cells have the capacity to regrow. Therefore, radiation therapy does not cause problems in normal cells.
2)Abnormal cell ( Abnormal cell ): X-ray and gamma rays destroy the genes of cancerous cells and do not allow them to grow.
type of radiation therapy (Types of radiation therapy):
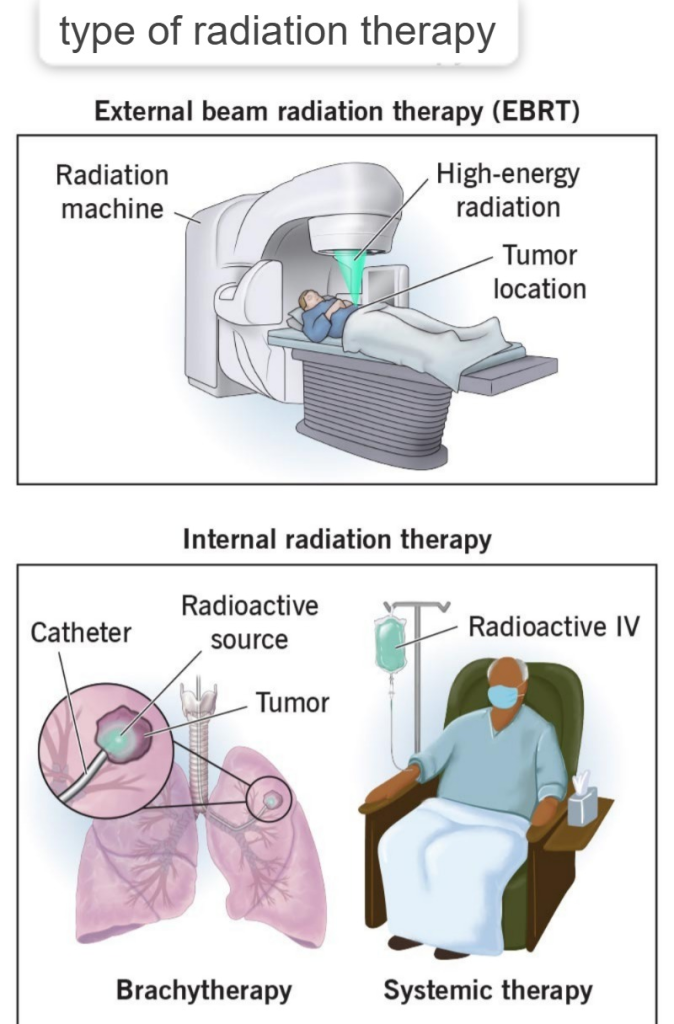
1) External : telly therapy,
2) Internal : brachytherapy : A) shield (shield), B) unshield (unshield).
1) External therapy: telly therapy:
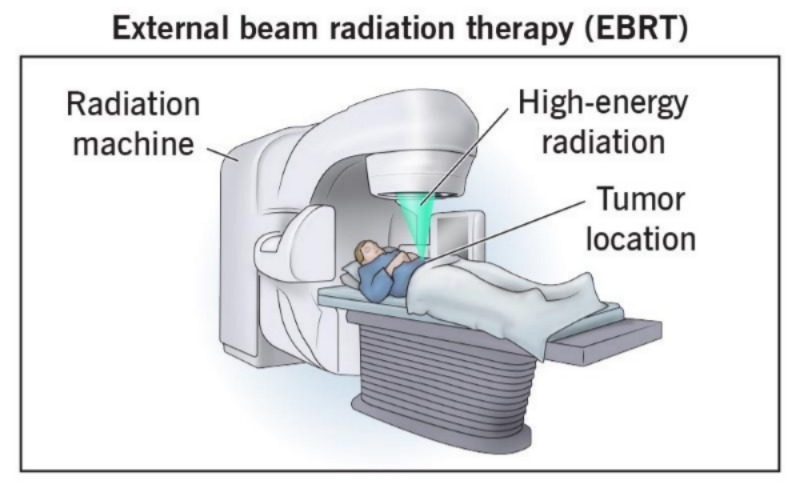
In this therapy, X-rays and gamma rays are applied directly to the cancerous cells. And the most common advantage of this is that this therapy affects the maximum depth area of the cell. It does not only affect the upper surface area, it goes deep inside and destroys the cancer.
2) Internal therapy: brachytherapy:
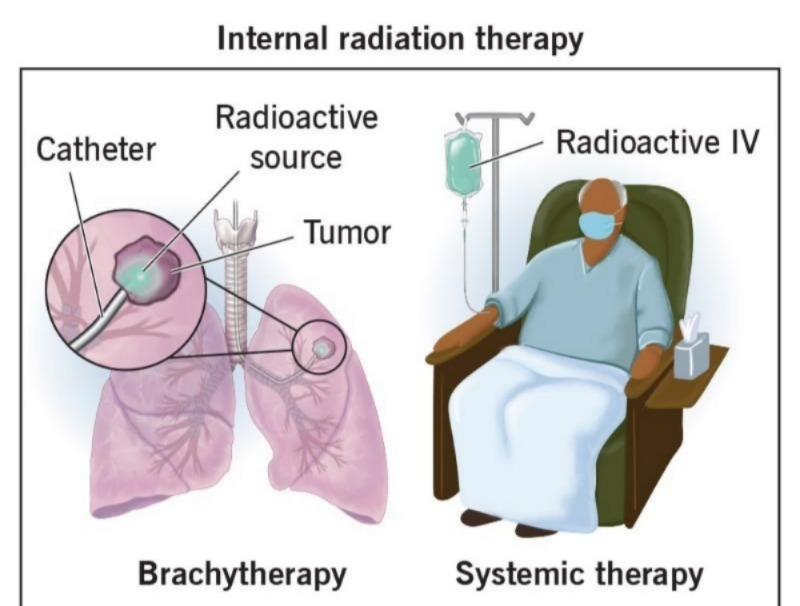
In this, radiation therapy is implanted directly inside the cell.
It have two types:
1) Sealed ( Shielded ) : In this, radiation therapy is provided to the abnormal cells using a needle, tube and applicator.
2) Unsealed ( Unshielded ) :In this, radiation is provided in the form of tablets and injections.
safety standards of radiation therapy:

Distance (Distance): When providing radiation therapy, health care personal should stay away from the patient’s bed. It is not necessary to stand near the patient’s bed continuously when providing radiation therapy.
Time (Time): When providing radiation therapy to a patient, they can work next to the patient for a maximum of 30 minutes.
Shield : When providing radiation therapy, health care personal should use a protective shield and cover all parts of the body.
When providing radiation therapy, health care personal should use a dosimeter that determines the dose of radiation.
A separate private room should be kept for health care personal in which they can wear personal protective equipment.
Children and pregnant women are at risk when we provide radiation therapy. Should be kept away from.
side effect :
- vomiting
- Nausea
- Diarrhea
- Dysphagia (difficulty in swallowing)
- fatigue (fatigue),
- weakness (weakness),
- stomatitis (inflammation of the mucous membrane of the mouth),
- loss of appetite (loss of appetite),
- leukoplakia (decreased WBC count), Increase the risk of infection (increases the risk of infection),
- Body ache (body ache),
- Alopecia (hair loss)
Nursing management of radiation therapy:
- Explain radiation therapy to the patient.
- Explain the equipment needed and the procedure time to the patient.
- Tell the patient that his relatives should visit him less while he is receiving radiation therapy.
- Insertion of a catheter to MT the bladder.
- Put the patient on a low salt diet Give.
- Give the patient an antidiarrheal agent.
- Assess the patient’s skin integrity.
- See if the patient has hair loss or skin shedding.
- Assess the patient’s oral mucosa.
- Assess whether the patient has conditions such as nausea, vomiting, diarrhea. Check.
- Check whether the patient has anemia or any blood abnormality.
- Check whether the patient has fatigue, malaise and body ache.
- Instruct the patient not to use any kind of ointments and lotions or powders.
- Tell the patient to maintain oral cavity hygiene and not to brush in an irritating manner.
- Tell the patient not to come into contact with sunlight.
- Tell the patient and his family members that Jay.Ray While providing radiation therapy, stay away from the patient and maintain contact by telephone.
2) Chemotherapy:

Chemotherapy is the treatment of cancer using chemicals.
chemo : chemical ,Therapy : treatment.

In this, tablets and injections are used to treat cancer.
purpose of chemotherapy (Purpose of chemotherapy):

curative : In this to cure cancer.
control : This has the purpose of controlling cancer.
palliative : It aims to reduce symptoms.
Drugs which are used in chemotherapy:

1)Group : Alkylating Agent (Alkylating Agent)
Example : cisplatin,
Action : This drug disrupts the DNA of cancerous cells.
Responsibilities : Corticosteroids should not be used while taking this drug. It is a contraindication.
2)Group: Antimetabolites agent (Antimetabolites agent)
Example : fluorouracil (fluorouracil).
Action : This drug prevents the DNA of cancerous cells from forming.
Nursing responsibilities : While giving this drug, the patient should also be given folic acid tablets.
3)Group : Mitosis inhibitor agents.
Example : vincristine, Vinblastine,
Action : It inhibits Mitosis of malignant cell mass.
Nursing responsibilities: provide palliative care.
4) Group : Hormonal agents (Antiestrogen)
Example: tamoxifen.
Action : In this Malignant cell’s hormone level is altered.
Nursing responsibilities : Provide palliative care to the patient.
5) Radiation therapy (Radiological sodium and iodine)
Action : inhibited the malignant cell growth.
Nursing responsibilities : To ensure that the patient is exposed to radiation with minimal side effects.
6) Group : Antibiotic
Example : Bleomycin
Action : Antimicrobial agent.
Nursing responsibilities : Do not give live vaccines to the patient.
Route of drug administration : Oral, Intramuscular, Intravenous, Interactivity,Intrathecal,Intraarterial,Subconscious, Applied topically.
common side effect of chemotherapy :

1) Skin : Anemia, hyperpigmentation, photosensitivity.
2) Blood : Bone Marrow suppression, Anemia, Leukopenia, Thrombocytopenia.
3) GI tract : nausea, vomiting, constipation, diarrhea, ulcer.
4) Genitourinary system : Nephrotoxicity, Cystitis, Weight loss, Fluid loss, Weakness.
Nursing management:
- Check the patient’s vital signs.
- Isolate the patient.
- Tell the patient to maintain his/her personal hygiene.
- Give the patient a well-balanced diet.
- Check the patient’s culture and sensitivity.
- Advise the patient to Toe Physical Examination.
- Check the patient’s bleeding time, clotting time, and platelet count.
- Prevent the patient from bleeding.
- Keep the patient as erect as possible while giving injections and catheterization.
- Tell the patient to avoid alcohol and smoking.
- Give the patient a meal that he likes.
- Food should be calorie rich, high protein, high fiber, vitamin C and provide all vitamins.
- Tell the patient to maintain his oral hygiene.
- Give the patient an antiemetic to prevent vomiting.
- See if the patient has hair loss.
- Cut the patient’s hair before treatment.
- Lubricate the patient’s scalp with vitamins A and D.
- Tell the patient to keep doing some activity.
- Tell the patient to keep his will power strong.
- Tell the patient to express his feelings honestly.
- Provide psychological support to the patient.
- Check the patient’s fluid and electrolyte levels.
- Provide chemotherapy to the patient.
- Clear all doubts of the patient and his relatives.
BIOTHERAPY (biotherapy):

Biotherapy uses the biological response modifier (BRM) calmette guerin and stimulates the body’s natural immune system to fight and destroy cancerous cells.
There are three categories of biotherapy:

1) Non specific,
2) monoclonal antibody,
3) cytokines (cytokines).
1) Non specific:In non specific, we use non specific agents like Bacillus Calmette Guerin and Coryne bacterium parvum which stimulate the body’s immune system to produce antibodies to fight against any antigen that enters the body.
2) Monoclonal antibody : In this method, the same antibody made to fight any cancerous cell in the body is introduced into the body and used to fight the cancerous cell.
3) Cytokines: In cytokines, antibodies are made from the body’s healthy immune system and are entered into the patient’s body, due to which they can fight and destroy the cancerous tumor.
>It has four types: interferon (interferon)
>interleukin (interleukin)
>colony stimulating factor (colony simulating factor)
>tumor necrosis factor (tumor necrosis factor)
Gene therapy (gene therapy) :
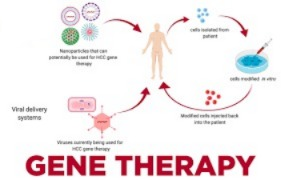
- A gene is a functional unit.
- In genetics, a normal gene is inserted into an organism, causing a genetic defect. Corrected.
AIM:
Gene therapy is a permanent therapy. Because in it, the permanent gene is changed and the genetic material of the cancerous cell is changed.
Indication:
1) cancer,
2) Infectious disease,
3) inherited disorder, genetic disorder.
ex: thalassemia, Hemophilia
process of gene therapy ( Process of Gene Therapy ) :
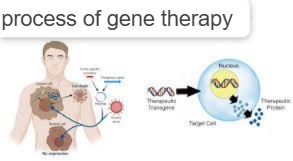
Gene therapy involves copying abnormal cells. Then the abnormal cells are removed from the patient’s body and normal ones are inserted into his body.
Method of gene therapy:
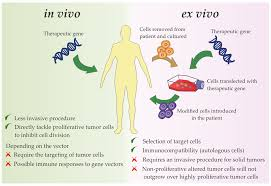
★Ex vivo,
★In vivo.
Ex vivo: In this, the target gene is taken out of the patient’s body and the abnormal cell is inactivated and reintroduced into the patient’s body. Only some of the cells are developed in to Ex vivo like : Lymphocytes, Hepatocytes.
In vivo : In this method, the healthy gene is directly inserted into the patient’s body. Through vector (virus), through non-vector
Through vector: In this method, a virus is used to extract its gene and introduce the healthy gene into it, after which it is administered intravenously to the patient’s body. In which: Edino virus, Retrovirus, Herpes virus etc.
Non vector : In this, the organ or artificial chromosomes are directly entered.
Advantage: This gene therapy is a permanent therapy. Because in it, a normal gene is inserted with an abnormal gene. And if gene therapy is used, then no other therapy is needed, or any other treatment is not needed. And if ovum and sperm are used in this gene therapy, then genetic disorders can be reduced.
Disadvantages: If any infectious virus is used in this gene therapy, the chances of infection in the body increase. This is not useful for all diseases. This process is quite expensive.
immune response: The patient’s body shows an immune response when any foreign body enters.
Bone Marrow transplantation (Bone Marrow Transplantation) :
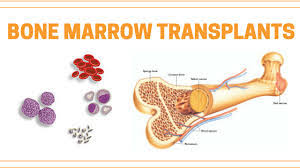
In bone marrow transplantation, cells are collected from the marrow of the patient and from the donor and healthy cells are administered back into the patient’s body for therapeutic purposes.
Indication: Oncology disorder like leukemia, Lymphoma.
Haematological disorder: Anemia, Aplastic Anemia, Sickle cell Anemia .
Type of bone marrow transplant (Type of bone marrow transplant):
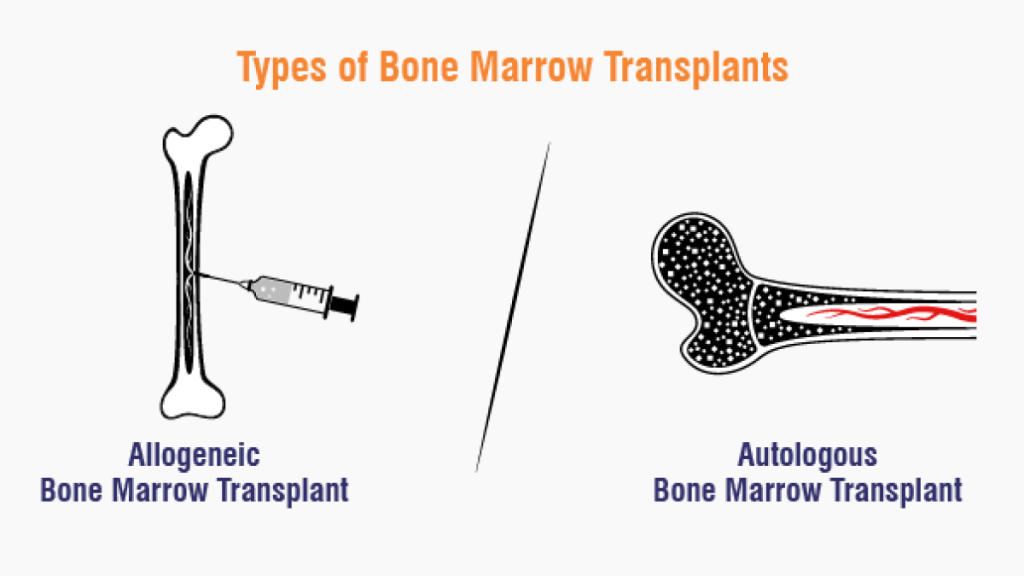
1) Autologous, 2) Allogeneic, 3) Syngenic.
1) Autologous (Autologous):
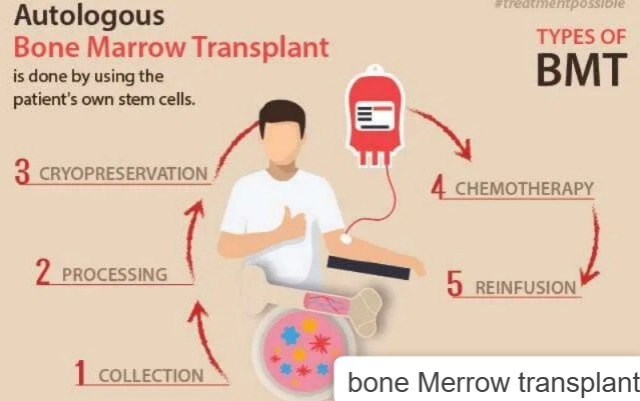
This is a procedure in which the patient’s healthy bone marrow is taken from the patient’s own bone marrow. Stem cells are collected from the patient. Then chemotherapy and radiation therapy are provided to the patient and after that it is confirmed that almost all the cancerous cells have been destroyed. Healthy stem cells are then inserted into the patient’s body.
2) Allogeneic:
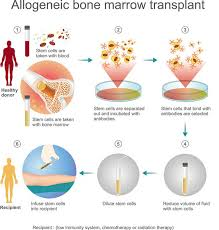
This is a procedure in which stem cells are taken from the healthy bone marrow of the patient’s parents or siblings and are transplanted into the patient’s body.
3) Syngenic:
In this, stem cells are taken from twins and there is a high chance of matching this bone marrow, after which it is inserted into the patient’s body.
PROCEDURE:
-> Bone Marrow transplant is done in the operation theatre through a central line.
-> The time for this depends on the severity of the patient’s cancer condition.
-> It takes a minimum of 30 minutes and a maximum of 4 (four) hours.
-> When bone marrow is transplanted, it causes a burning sensation.
->Complete bone marrow transplantation is only complete when the patient’s body starts producing healthy cells.
Nursing management (Nursing management):
- >Prepare the patient physically and psychologically.
- >Explain the procedure to the patient and his family members.
- >The patient and his family members should be told about its risks, its benefits and its return consent.
- >Keep the patient isolated.
- >Restrict entry to visitors.
- >To see if the patient is having any side effects of chemotherapy and radiotherapy during this time.
- >To view the patient’s intake output.
- >To check the patient’s vital signs.
- >To administer IV fluid (i.v. fluid) to the patient.
- >To maintain strict aseptic technique.
- >To administer prescribed medicine Blood component To do.
- >Provide psychological support to the patient.
- >Tell the patient and his family members about coping abilities.
- >After bone marrow transplantation, dressing the central line properly.
- >After bone marrow transplantation, check for any type of infection.
- >The patient and his Tell family members about regular follow-up.
complications (complications ) :
- -> Hematopoietic : Infection, nosocomial infection, Anemia.
- ->Gastrointestinal Tract: Nausea, Vomiting, Diarrhea.
- -> Renal and Genitourinary: Renal failure, Hemorrhagic Cystitis,
- -> Hepatic: Hepatomegaly, Bilirubinemia, Coagulopathy disorder.
- -> Pulmonary : Bacterial Pneumonia, Fungal infection, TB toxoplasmosis, Pulmonary, fibrosis.
Nursing management of patient with the cancer:

1)Nursing Assessment:
-> Assess the patient’s pain level.
-> Check the patient’s vital signs.
-> Check the patient’s urine output.
-> Check if the patient has any scratches on the body.
-> Assess the patient’s skin integrity.
-> Ask if the patient has hair loss.
-> Observe the patient for bleeding from the oral cavity and observe oral hygiene.
-> Ask about the patient’s bowel and bladder habits, i.e., ask about conditions such as diarrhea or vomiting.
Nursing diagnosis (Nursing Diagnosis):
1) Chronic pain related to cancerous conditions as evidenced by verbalisation with the client.
Relieving pain:
1) Assess the patient’s pain level.
2) Position the patient in a comfortable position.
3) Involve the family in the patient’s care.
4) Provide the patient with mind diversionary therapy.
5) Provide the patient with work and a kind environment.
6) Provide the patient with analgesics.
2) self care deficit related to disease condition As evidenced by observation of the client condition.
Nursing intervention:
1) Provide the patient with a clean and comfortable environment to work in.
2) Provide the patient with a clean and wrinkle-free bed.
3) Change the patient’s bedsheet and clothes daily.
4) Maintain the patient’s personal hygiene.
5) Involve the patient in the care.
6) Wash hands thoroughly before serving food.
3) Impaired tissue percussion related to disease condition as evidenced by pinching the skin of the patient .
Nursing interventions:
1) Check the patient’s tissue integrity and skin turgor.
2) Observe the patient’s skin side for bleeding.
3) Tell the patient to maintain his oral hygiene.
4) Instruct the patient not to brush in an irritating manner.
5) Instruct the patient not to scratch the area of skin exposed to radiation.
6) Instruct the patient to wear loose clothing.
4) Disturbed body image related to chemotherapy as evidenced by observing the hair loss of the client.
Nursing interventions: Manage hair fall :
1) How to maintain rapport with the patient and describe their feelings with them.
2) Talk to the patient very politely.
3) Talk to the patient about their coping abilities as they are experiencing hair loss.
4) Tell the patient that hair loss is common while undergoing therapy, so there is no need to panic.
5) Tell the patient that hair will grow back normally after the treatment is completed.
5) Impaired nutritional status pattern less than body requirement related to nausea and vomiting.
Nursing interventions: Managing diet :
1) Provide the patient with a comfortable and functional environment.
2) Avoid creating an environment that smells bad when the patient eats.
3) Provide the patient with a high-calorie and high-protein diet.
4) Encourage the patient to drink plenty of fluids.
5) Encourage the patient to drink plenty of fluids. Tell the patient to eat small and frequent meals.
6) Give the patient a meal that he/she likes.
6) Activity intolerance is related to weakness as evidenced by observing the activity level of the client.
Nursing interventions: Promoting activity level
1) Assess the patient’s activity level.
2) Involve the patient in daily routine activities.
3) Ask the patient to take short breaks between activities.
4) Tell the patient to do some exercise and yoga.
5) Tell the patient to do meditation.
7) High risk of infection related to bone marrow depression secondary to chemotherapy.
Nursing Interventions : Prevention from infection:
1) Provide a clean environment to the patient.
2) Minimize the number of visitors near the patient.
3) Ask the patient to wear clean clothes.
4) Check the patient’s vital signs.
5) Ask the patient to wear a mask when going out.
6) Give the patient a high protein diet.
7) Give the patient prescribed medicine.
surgery of cancer ( Surgery of cancer ) :
Following type of surgery are used to remove cancer tumor :
1) Electrosurgery :
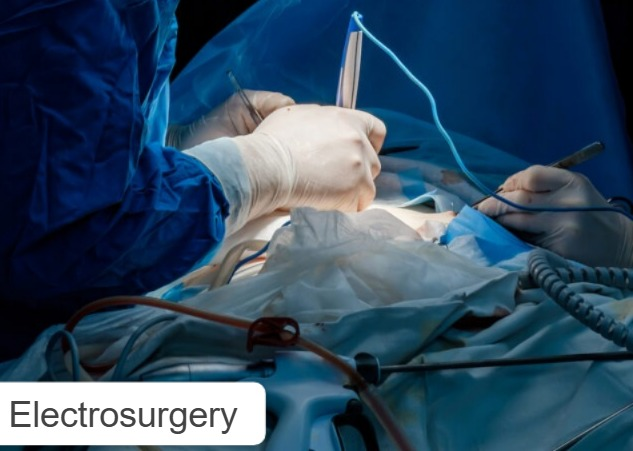
In this, electric current is used to dissolve the tumor.
2) Cryosurgery :
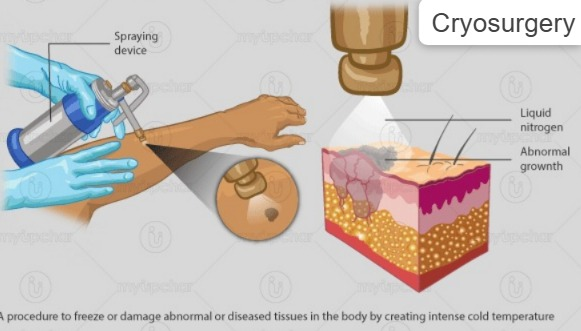
In this, cancerous cells and tumors are destroyed using liquid nitrogen.
3) Laser surgery (Laser beam): In this, the tumor is destroyed using a laser beam.
4) Ectomy: In this, an incision is made on the side of the tumor and the entire tumor is removed.
Surgery has three main aim (There are three main aims of surgery):
1) curative, 2) palliative, 3) Reconstruction.
1)Curative: In this aim, the entire tumor is removed.
2)Palliative: In this, only the cancerous cells are removed.
3)Reconstructive: In our reconstructive type, any therapeutic modalities such as chemotherapy and radiation therapy are performed at the same time as any reconstructive or cosmetic surgery. Example: plastic surgery.
preoperative and postoperative nursing management:
preoperative:
- Provide psychological support to the patient.
- Try to remove the fear of the operation from the patient’s mind.
- Prepare the patient physically and psychologically for surgery.
- Explain all the information about the surgery to the patient and his relatives.
- Tell the patient about reconstructive surgery.
- Give the patient a high protein, high vitamin E, D, and iron-rich diet.
- Give the patient an intravenous (i.v.) route before surgery. Give fluid.
- Provide blood transfusion if the patient needs it.
- Prepare the patient’s operation area.
- Shave the patient’s body area properly.
- After shaving, clean the area with spirit and savlon.
- Keep necessary medicines and blood ready for the patient.
- To conduct all laboratory investigations of the patient.
- To check the patient’s vital signs.
post operative :
- To check the patient’s vital signs after the operation.
- To monitor the patient’s blood pressure properly.
- To keep the patient under close observation.
- Check the patient for conditions such as shock, collapse, and hemorrhage.
- Ask the patient to do deep breathing exercises after surgery.
- Check the area from which the graft is to be taken for any pain, redness, swelling, or infection.
- Properly position the patient after surgery.
- Operation Dress the side properly.
- If the patient is in severe pain, provide him with analgesics.
- Check the drainage tube and dress it properly.
- Give antibiotics to prevent infection.
- Check the skin side for any redness, swelling, and inflammation.
- Give the patient antibiotics Provide inflammatory drugs.
- Instruct the patient and his family members to take proper follow-up.
PALLIATIVE CARE:

INTRODUCTION: Palliative care is provided to alleviate the symptoms of the patient.
- This is not for the cure of the patient but is provided to the patient who is dying or terminally ill.
- This palliative care improves the patient’s quality of life during death time. does.
- Palliative care is provided by trained nurses, doctors, and family members.
- Palliative care also involves family members and friends.
- Psychiatric, (Psychiatric) Councillor (Counselor), Social worker (Social worker), Spiritual worker, And Doctor are also involved.
- Palliative care involves health care personnel as well as family members and friends in the care of the patient.
Goal of palliative care:
- To relieve the patient’s pain and other symptoms.
- To improve the patient’s emotional status, mental status, and spiritual status.
- To support both the patient and his family members.
- To provide psychological support to the patient.
Services provided:
- To improve the psychological, spiritual and coping abilities of the patient when they are in the last stages of their life.
- To relieve the patient’s pain and symptoms.
- To teach the patient and their family members how to care for the patient.
- To provide the patient with the necessary Hospice care is provided to provide drugs and equipment.
- Thus, palliative care is provided to a patient who is in the last stage of his life to relieve the symptoms of his disease.
Hospice care:

home and hospital care of patients:

INTRODUCTION : This care is provided to a patient who is ill for a long time and has been undergoing treatment in the hospital for a long time, in such a situation, he should be provided with a comfortable stay at his home with his family members and friends etc. The patient is treated while staying in the environment. In hospice care, a home-like environment is created around the patient.
service setting:

Home,
Hospice hospital’s,
Hospice home ,
Hospital
In all these areas, family members and friends are involved and care is provided to the patient. In this, the family members as well as the hospital’s health care personnel are also involved in the patient’s care.
BENEFITS :
- In this, the patient gets treatment in a family-oriented environment.
- In such an environment, the patient gets work and a comfortable environment.
- The patient gets support from his family and friends during his illness.
- The patient’s mental health remains good in such an environment.
- The patient stays at home and gets treatment instead of living in an uncomfortable environment like a hospital.
care provider:
->All hospitals are staffed with trained professionals.
->physicians,
->Specially trained nurses,
->Social worker,
->Family members,
->friends
Thus, hospice care is the treatment of the patient in a home-like environment in the patient’s home or hospital, which is called hospice care.
WRITE IN DETAIL ABOUT VARIOUS CANCER AND ITS MANAGEMENT.
1) Lung cancer:
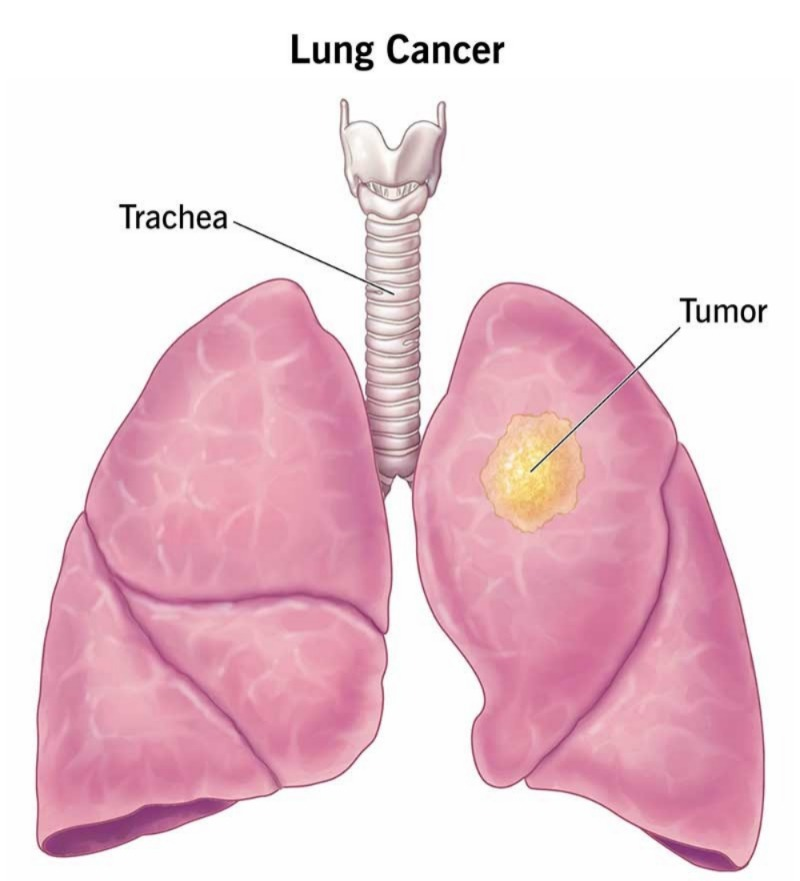
Definition:
Lung cancer can arise from any part of the body. About 90% of people with lung cancer have lung cancer. 95 percent of cancers arise from epithelial cells, and most often they arise from the bronchi and bronchioles of the lungs. For this reason, lung cancer is called bronchogenic cancer or bronchogenic carcinoma. Cancer mainly originates from the pleura (it’s called mesotheliomas) but sometimes it originates from the tissues of the lungs. Wherever cancer occurs in the body or if a cancer tumor develops, the lungs are the main place where it metastasizes from one place to another.
Etiological Factor ( etiological factor ):
- Cigarette smoking ( cigarette smoking 🚬),
- Passive smoking,
- Tobacco use,
- Hereditary and Environmental Factors.
- History of lungs 🫁 cancer,
- Air pollution,
- Occupational carcinogens,
- Asbestos fiber,
- Radon ⛽ gas,
- Nutritional deficiency
clinical manifestation / sign and symptoms :
- Cough,
- Dyspnea (difficulty in breathing),
- Wheezing,
- Chest pain,
- Excessive sputum production,
- Hemoptysis (Hemoptysis) (Hemoptysis: Blood in the phlegm),
- Dysphagia (Dysphagia: Difficulty swallowing),
- Nausea,
- Vomiting,
- Headache,
- Weight loss,
- Fatigue,
- Anorexia (anorexia:= loss of appetite),
- Weakness,
- Blurred vision,
- Seizures (seizure).
Diagnosis evaluation (Diagnostic evaluation):
- History taking and physical examination,
- X Ray,
- Computed tomography (CT scan),
- Magnetic resonance imaging (MRI),
- Positron emission tomography (PET),
- Biopsy,
- Psychological examination (Cytological examination),
- Pulmonary function test (PFT),
- Bronchoscopy (Bronchoscopy: Visualization of the bronchi through a bronchoscope).
Management:
- 1)Radiation therapy (Radiation therapy),
- 2)Chemotherapy,
- 3)Bronchoscopy,
- 5)Airway stuntenning.
complication (complication ) :
- 1.Superior vena cava syndrome,
- 2)Hypocalcemia (low calcium levels),
- 4) Spinal cord compression,
- 5) Pulmonary 🫁 scarring.
Nursing management (nursing management ):
Nursing assessment:
- 1) Check the patient’s vital signs.
- 2) Check the patient’s intake output.
- 3) Check the patient’s pain level.
- 4) Check the patient’s eating pattern.
- 5) Check whether the patient has any complications.
- 6) Check the patient’s anxiety level and coping ability.
- 7) Check the patient’s blood investigations.
- 8) Perform a physical examination of the patient.
Nursing Diagnosis :
1) Impaired breathing pattern related to compromised respiration.
Nursing interventions:
Improving breathing patterns:
- Elevate the patient’s head.
- Teach the patient breathing exercises.
- Give nebulization to the patient.
- Ask the patient to cough up phlegm on their own.
- Give oxygen to the patient.
- Ask the patient to get enough sleep and how to keep his head slightly low while sleeping.
- Give the patient a fowler position.
2) Impaired nutritional pattern less than body requirement related to nausea and vomiting.
Nursing interventions:
Improving nutritional status:
- How to make the patient eat small amounts of food.
- Tell the patient to eat high calorie and high protein rich food.
- Give prescribed vitamin supplementation.
- Advise to take a soft and liquid diet.
- Administer fluids through an intravenous route to those who are unable to eat on their own.
3) Pain related to abnormal cell growth.
Nursing interventions:
controlling pain:
- Assess the patient’s pain level.
- Give the patient the prescribed analgesic medication.
- Ask the patient about his anxiety level, depression level, and whether he is getting enough 😴 sleep.
- Tell the patient’s family member to take proper care of his family member.
4) Anxiety, fear, related to therapeutic regimen and prognosis.
Nursing interventions :
Minimise anxiety:
- Check the patient’s anxiety level.
- Ask the patient to describe his feelings.
- Tell the patient that his body pain is caused by cancer, so ask him for
coping mechanisms. - Give the patient N.S.A.I.D. ( N.S.A.I.D.)s group or any other type of Analgesic Provide.
- Tell the patient about proper cope up mechanism.
BRAIN TUMOR (Brain Tumor):
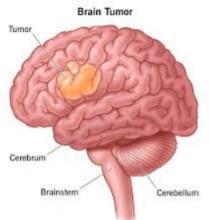
INTRODUCTION / DEFINITION ( Definition ):
Brain 🧠 Tumor is the abnormal growth of cells in the brain and forms a tumor. This tumor can be malignant or benign. In brain tumors, abnormal and uncontrolled cell division and growth of cells occurs in the brain and it forms a tumor. These tumors are in the brain, lymphatic tissue, blood, intracranial nerves, pituitary gland, pineal gland and in any other organ of the body and are transferred to the brain and affect the brain. These tumors can be in the junction of gray matter and white matter of the brain.
classification / type (classification / type):
- 1)Primary Brain tumor,
- 2)secondary Brain tumor,
1) Primary Brain tumor: Primary brain tumors are made up of cells and structures of the brain itself.
A) Intracerebral tumor: The most common primary brain tumor is gliomas, which arise from glial cells.
There are many types of gliomas like :
Astrocytoma (in astrocytes),
Brain stem glioma (brain stem glioma),
Ependymoma (in ependymoma),
oligodendroglioma (in oligodendroglioma)
Medulloblastoma (in medulloblastoma).
B) tumor arising from supporting structures (tumor arising from supporting structures of the brain):
Meningioma (in meninges),
schwannoma (schwannoma),
germ cell tumor of the brain,
pineal region tumor,Angioma.
2)secondary Brain 🧠 tumor ( ): This secondary Brain tumor develops from a structure outside the Brain and it transfers (i.e. metastasis) to the Brain and the tumor develops in the Brain is called Secondary Brain Tumor. The most common organ like 🧠 brain, lung, Brest, Kidney.
Tumors from all these parts of the body metastasize and transfer to the Brain. And that’s where the tumor grows excessively, which results in cancer.
Etiology :
- being male (being male),
- Race,
- Age (Age) ,
- Family history (Family history),
- Inherited,
- Occupational (occupational),
- Nutritional factor,
- Radiation (Radiation),
- H. I. V. HIV infection,
- Cigarette smoking,
- Use of hair dyes,
- Head trauma,
- Dietary exposure to such factors as nitrates.
clinical manifestation (symptoms and signs ):
- Headache,
- Gait disturbance (difficulty in walking),
- memory loss (not remembering),
- visual disturbance,
- personality disturbance,
- confusion,
- seizure,
- weakness,
- paralysis.
Diagnostic evaluation ( Diagnostic evaluation ) :
- History taking and physical examination (history taking and physical examination),
- Computed tomography (ct scan),
- Magnetic resonance imaging (MRI),
- Angiogram,
- X Ray (X Ray),
- Positron emission tomography (PET positron emissions tomography),
- Single Photo Emission Computer Tomography (SPECT)
Management:
1)corticosteroids treatment,
2) Palliative treatment (palliative treatment),
3)Radiation therapy (radiation therapy),
4)surgery (craniotomy) 5)Chemotherapy,
Antineoplastic agent (antineoplastic agent):
- A)alkylating agent,
- B)Nitrosoureas,
- C)Antimetabolites,
- D) Antitumor antibiotics,
- E) Hormonal agents.
COMPLICATION ( Complications ):
- Learning difficulty (learning difficulty: difficulty in learning),
- memory difficulty (memory difficulty: difficulty in remembering),
- walking and talking difficulty (walking and talking difficulty: difficulty in moving and speaking),
- Visual difficulty (visual difficulty: difficulty in seeing),
- Hydrocephalus ( Hydrocephalus : Collection of cerebrospinal fluid in the brain),
- Bleeding in Brain ( Bleeding in Brain : Bleeding from the head) etc.
Nursing management (Nursing Management ): &
Nursing assessment :
- 1) Check the patient’s level of consciousness.
- 2) Perform a neurological examination of the patient.
- 3) Check the patient’s pain level.
- 4) Check the patient’s nutritional status To do.
- 5) Check the patient’s skin integrity.
- 6) Check whether the patient has a condition such as phlegm or weakness or seizures.
- 7) Check the patient’s activity level.
- 8) Check the patient’s vital signs.
Nursing diagnosis ( Nursing Diagnosis ):
1) pain related to mass in Brain, nerve compression.
Nursing interventions: Reliving pain
- Patient prescribed Analgesic Give medicine.
- Provide mind diversion therapy to the patient.
- If the patient has photophobia, keep him in a completely dark room and wear dark glasses.
- Tell the patient to rest.
- Provide the patient with the prescribed analgesic.
2) Risk of injury related to gait disturbance .
Nursing interventions: Prevention of injury:
- If the patient’s intracranial pressure has increased, report it to the physician.
- Maintain the patient’s position properly.
- Maintain the patient’s intake output To do.
- To see whether the patient is affected by the pharmacological treatment.
- To ambulate the patient.
- To provide the patient with a side rail in the bed.
3) Anxiety related to disease conditions.
Nursing interventions: Relieving Anxiety:
- Giving reassurance to the patient.
- Ask the patient to describe his feelings.
- Ask the patient to clear all his doubts.
- Ask the patient to do a little exercise.
- Spending some time with the patient.
- Tell the patient to improve his/her coping abilities.
- Tell the patient to engage in mind diversional therapy.
4) Activity intolerance related to weakness or fatigue.
Nursing interventions : Promoting activity level:
- Patient’s Maintain personal hygiene.
- Ask the patient to do daily routine activities.
- Keep the necessary things near him.
- Ask the patient to do some exercise.
5) Altered nutrition status less than body requirement related to nausea and vomiting.
Nursing interventions: improve nutrition status of client:
- Maintain oral hygiene of the patient.
- Do not keep any bad smelling items near the patient while he is eating.
- Give the patient only the things he likes to eat.
- What the patient likes and dislikes Keep in mind to eat like this.
- Provide proper position to the patient.
- Provide proper fluid to the patient.
- Check the patient’s weight daily.
6)ineffective family coping related to clients disease and prognosis .
Nursing interventions: Reassure the family coping:
- Giving reassurance to family members.
- Involving family members in coping mechanisms.
- Providing psychological support to the family and the patient.
- Communicating with the patient and his family members.
- Clearing all doubts of the patient and his family members To do.
- If the patient is unconscious, provide care.
ORAL CANCER (Oral Cancer):
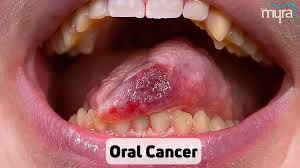
INTRODUCTION ( Introduction ) :
Oral cancer is a cancer of the mouth and throat. In this cancer, the cells of the mouth grow uncontrollably and abnormally, forming a tumor. Oral cancer can develop in any part of the mouth. Like: Oropharynx (Oropharynx),
- Lips (Lips : Lips)
- Tongue (Tongue : Tongue)
- Hard and soft palates (Hard and soft palates: Palate),
- Salivary gland (Salivary glands : Salivary gland),
- lining of cheeks,
- floor of mouth ,
- gums,
- teeth.
- Cancer can develop in any part of the oral cavity.
Etiology :
- Tobacco ( ટોબેકો ),
- Alcohol (અલ્કોહોલ),
- Exposure to ultraviolet rays (એસ્પોસ્પોસ્ટો ટુ અલ્ટોવોલેટ રેઇસ ),
- chronic irritation at the lining of mouth (મૂથ નિ લેનિ લેનિ માઉથ નિ લેનિ લેનિંગમે Chronic irritation,
- Sun Exposure,
- A person history of Head and neck cancer.
- Diet low in fruits and vegetables.
- mouthwash with high Alcohol.
- Human papilloma virus.
- Immune system suppression.
- Age above 35 years.
- Gender/Sex: both man and women equally occur.
- Gender/Sex: both man and women equally occur.
clinical manifestation (symptoms and signs ):
- A sore in the mouth which does not heal (a sore that does not heal or becomes silvery and keeps growing).
- pain (pain).
- A lump on the mouth, lip or in the throat (a lump develops in the lips, throat and cheeks).
- A persistent white and red patch on the gums, toung (a persistent white and red patch on the tongue).
- tonsil or lining of the mouth. (a white and red patch on the mouth, tongue, gums, tonsils and lining of the mouth).
- Bleeding from the mouth (bleeding from the mouth).
- Bad breath (halitosis).
- Hoarseness or other change in the voice (change in voice).
- Difficulty chewing and moving the jaw or tongue (difficulty chewing).
- Painful swallowing (difficulty swallowing or pain when swallowing).
- Weight loss (weight loss).
- Swelling of jaw (swelling of the jaw).
- pain in one ear without hearing loss (pain in one ear).
- A lump or mass in the neck (a lump or mass in the neck).
- voice change (change in voice).
Diagnostic evaluation:
- History taking and physical examination,
- Biopsy,
- Cytological test,
- X-ray,
- CT scan,
- MRI scan,
- Toludine blue test,
- Oral exfoliative cytology.
Management:
- 1)Radiation therapy,
- 2)Chemotherapy,
Surgery:
- a)primary tumor resection,
- B)Mandibularectomy,
- C)Maxillectomy,
- D)Moh’s micrograph surgery.
- E)laryngectomy,
- F)Radical neck dissection,
- G)plastic surgery.
Nursing management:
- Assess the patient’s pain level.
- Provide the patient with Fowler and semi-Fowler positions.
- Give oral suction to the patient.
- Check the patient’s body temperature.
- Check the patient’s vital signs.
- Check the patient’s weight.
- Prepare the patient for chemotherapy and radiation therapy.
- Ask the patient to maintain oral hygiene.
- Provide the patient with a high-calorie diet.
- Tell the patient to avoid tobacco, smoking, and alcohol.
- Tell the patient to eat a healthy diet every day.
- Explain to the patient what the side effects of chemotherapy and radiation therapy are.
- Explain to the patient what the side effects of using tobacco or cigarettes are.
- Provide emotional support to the patient.
- Provide psychological support to the patient and his family members.
- Providing a comfortable environment for the patient and the work.
Esophagus cancer:
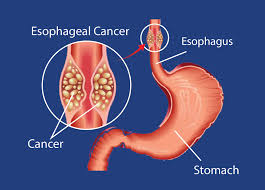
This is cancer of the esophagus and it involves the lining of the esophagus and its muscles and lymph nodes and the development of cancer.
Etiology :
- 1)Gender more in men.
- 2)Race Esophageal cancer in African and American races Cancer occurs more frequently.
- 3)Age: It occurs more in people after the age of 50.
- 4)Use of Alcohol and tobacco,
- 5)GERD (Gastero esophageal reflux disease),
- 6)Hot, spicy dietary intake (due to excessive spicy fried food),
- 7)Exposure to niterosomine in food/Environments.
clinical manifestation (symptoms and signs):
- Dysphagia (difficulty swallowing),
- feeling of lump in throat (feeling of lump in throat),
- painfully and difficulty in swallowing,
- Regurgitation of undigested food ( undigested food comes back into the mouth),
- loss of appetite ( loss of appetite),
- loss of weight ( weight loss),
Diagnostic evaluation ( Evaluation):
- History tacking and physical examination,
- X Ray,
- Computed Tomography (Ct scan),
- Magnetic Resonance Imaging (MRI),
- PET (Positron Emissive Tomography),
Management:
1)Radiation therapy,
2)Chemotherapy,
3)Phototherapy,
4)De bulking surgery (De bulking surgery)
Nursing management:
- Patient’s vital To check the sign.
- Provide emotional support to the patient.
- Maintain hygienic conditions.
- Give the patient high-calorie and high-protein rich food.
- Meet all the needs of the patient.
- When giving chemotherapy and radiation therapy to the patient To see if he has any kind of side effects.
- To see if the patient has any kind of adverse effects.
- To maintain the nutritional status of the patient.
- To maintain the fluid level of the patient.
- To clear all the doubts of the patient and his family members.
- To provide support to the patient and his family Provide psychological support to members.
cancer of stomach:
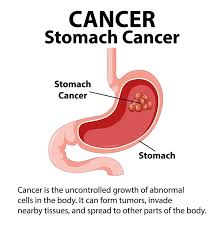
Introduction ( Introduction ):
Stomach cancer is also called gastric cancer. It develops in any part of the stomach and is characterized by abnormal and uncontrolled growth of the lining of the stomach and the formation of tumor and mass-like structures. These tumors can be both benign (non-cancerous) and malignant (cancerous). About 85% of stomach cancers are adenocarcinomas and occur mainly in the lining (mucosa) of the stomach. About 40% of stomach cancers occur in the lower part of the stomach (pylorus). 40%: Most cases occur in the middle part of the stomach (body). 15%: Most cases occur in the upper part of the stomach (cardia) and this stomach cancer metastasizes, i.e. transfers and spreads to other parts of the body such as the liver, lungs, bone, and brain. And mainly it spreads to the periosteum i.e. the abdominal cavity.
Etiology:
- Age: Seen after the age of 40.
- Gender: More common in men than women.
- Region: More common in Japanese people is.
- Diet: It can also be caused by not eating enough fruits and vegetables.
- Smoking (smoking),
- Alcohol (alcohol),
- Hereditary factors,
- chronic infection in the stomach (due to long-term infection in the stomach),
- Stomach surgery,
- H.pylorus infection(Helico bacterium pylori ),
- High consumption of red meat 🍖, (due to eating too much meat),
- Pernicious Anemia (due to vitamin B 12 deficiency),
- Gasteric ulcer (gastric ulcer),
- Hereditary (hereditary),
- Obecity (obesity),
- Hormonal factore, Etc.
clinical manifestation (symptoms and signs):
- Pain in the stomach area.
- Difficulty swallowing.
- Nausea and vomiting.
- Weight loss.
- A little The stomach feels very bloated even after eating.
- There is blood in vomiting (hemetemesis).
- There is blood in the stool. ( hematochezia),
- Gastrointestinal bleeding,
- Conditions like indigestion (Indiagetion) and gas (heart burn) occur.
- Anorexia ( loss of appetite:= loss of appetite),
- Diarrhea ( loss watery stool),
- Constipation (difficulty in passing stool),
- fatigue (feels tired).
- Iron deficiency Anemia.
Diagnosis evaluation ( Diagnostic evaluation ):
- History tacking and physical examination,
- Biopsy,
- Endoscopy,
- ultrasound
- X Ray ( X Ray ),
- ct scan ( Computed Tomography ),
- MRI ( Magnetic Resonance Imaging ),
Management ( Management ):
- chemotherapy ( chemotherapy ),
- Radiation therapy ( radiation therapy ),
- gastrectomy ( gastrectomy ),
- Total gastrectomy ( total gastrectomy ),
- sub total gastrectomy ( subtotal gastrectomy )
- esophageal gastrectomy
- Billiroth :- I ( gasteroduodenostomy) ,
- Billroth:=II
Nursing management :
- Check the patient’s vital signs every 15 minutes.
- Check the patient’s blood pressure every 15 minutes.
- Set up two intravenous lines for the patient and prepare a blood transfusion.
- Give the patient oxygen.
- To check bowel sounds.
- Check whether the patient is vomiting and diarrhea.
- Catheterize the patient to check urine intake output.
- Check the patient’s skin color.
- Maintain the patient’s intake output chart.
- Put the patient in the fowler position to prevent aspiration of mucus. For.
- Insertion of naso-gastric tube (N.g tube) in the patient.
- Start feeding the patient with a clear liquid diet.
preoperative and postoperative nursing management (pre-operative and post-operative nursing management):
Preoperative nursing management (Preoperative Nursing Management):
- Provide psychological support to the patient.
- Explain the procedure to the patient and his family members.
- Set up an intravenous line for the patient.
- Catheterize the patient.
- Maintain the patient’s intake output chart.
- Set up blood transfusion for the patient.
- Get all the laboratory investigations done for the patient.
- Administer oxygen to the patient.
- Proper shaving of the part of the patient that is the operation part.
- Clean or paint the patient on the operation side with Savlon and spirit.
- Prepare the patient mentally and physically for surgery.
- Check the patient’s vital signs.
- Provide psychological support to the patient and his family members.
post operative nursing management (Post Operative Nursing Management) :
- Close observation of the patient after the operation.
- Check the patient’s vital signs every 15 minutes.
- Give the patient intravenous fluids through the parenteral route Provide fluids.
- Check the patient’s bowel sounds.
- Give the patient proper antibiotics.
- Provide psychological support to the patient.
- Advise the patient’s family members to ensure that the patient does not do too much hard work.
- Tell the patient to rest.
- Provide the patient with work and a comfortable environment.
- Maintain the patient’s nutritional and food status balance.
- Instruct the patient to do small amounts of activity.
liver cancer (liver cancer):
Introduction:
Liver cancer occurs in the liver. It is called hepatocellular carcinoma. This Cancer arises in the cells of the liver. It is characterized by abnormal and uncontrolled growth of cells and the formation of a tumor. This tumor can be malignant (cancerous) or benign (non-cancerous). This cancer is also called hepatoma.
Etiology:
- certain type of liver disease: cirrhosis,
- hepatitis B viral,
- hepatitis c viral,
- Diabetes,
- Obesity,
- Aflatoxin:
- Birth control pills,
- Tobacco use,
- vinyl chloride,
- Anabolic steroids,
- Arsenic,
- Cytological drug,
- use of steroids.
clinical manifestation (symptoms and signs):
- abdomen Pain occurs in the right side and this pain is transferred to the back side and shoulder.
- The right side of the abdomen becomes swollen.
- A lump appears in the abdomen.
- The liver It only enlarges.
- Weight decreases.
- malaise occurs.
- I don’t feel hungry and my abdomen feels very bloated after eating a little.
- I feel extremely tired.
- The eyes, skin and whole body become yellowish.
- nausea,
- vomiting,
- fever,
- fluid retention (acities),
- liver damage,
- Metabolic disturbance,
- splenomegaly,
- Hepatic encephalopathies,
- Jaundice,
- esophageal varices (the opening of the esophagus is enlarged).
- Abdominal distension.
Diagnostic evaluation ( Diagnostic evaluation ):
- History tacking and physical examination (History Taking and Physical Examination),
- Hepatological investigation (Hepatological Investigation),
- AFT : Alpha feto protein (AFT: Alpha Feto Protein),
- blood test (blood test),
- liver function test (liver function test),
- Albumin alkaline Phosphate(albumin alkaline phosphate),
- Prothrombin time (prothrombin time),
- X Ray (X-ray),
- ultrasonography (ultrasonography),
- ct scan (CT scan),
- MRI (M. R. I.),
- Laproscopy (Laproscopy) ,
- Biopsy (Biopsy),
- hepatitis b test (Hepatitis B test),
- hepatitis c test (Hepatitis C test)
Management:
- Radiation therapy,
- Chemotherapy,
- Ablationtherapy,
- Immunotherapy,
- Biotherapy
surgical management:
- Surgical resection,
- liver transplantation ( liver transplantation).
complication :
- Malnutrition ( Malnutrition),
- Biliary obstruction ( Biliary obstruction),
- sepsis ( Sepsis),
- liver abscesses ( Liver abscess),
- Metastasis ( Metastasis) ).
Nursing management:
Nursing assessment:
- Assess the patient’s pain level.
- Assess the patient’s coping ability.
- Check the patient’s vital signs.
- Check the patient’s skin turgor and see if there is any condition in the heel.
- Check the patient’s dietary condition.
- Assess the patient’s activity level and sleep pattern.
- Assess the patient’s activity level and sleep pattern.
- Assess the patient’s chemotherapy, radiotherapy, and immunotherapy side effects.
Nursing diagnosis:
1) pain related to liver enlargement.
Nursing interventions:
Controlling pain:
- Provide analgesic medications to the patient.
- Provide mind diversional therapy to the patient*.
- Observe the patient for any signs of drug toxicity.
- Guide the patient Provide imagery.
- Ask the patient to exercise in small amounts.
- Provide comfort measures to the patient.
2)Altered nutrition less than body requirement related to disease and side effects of chemotherapy.
Nursing interventions:
Improving nutritional status:
- Tell the patient to eat small amounts of food.
- Tell the patient to take supplementary drugs.
- Give the patient food that he likes to eat.
- Know the patient’s likes and dislikes.
- Give the patient high-calorie food.
- Do not keep things with bad smell near the patient while he is eating.
3)fluid level excess related to oedema.
Nursing interventions:
Relieving excess fluid volume:
- Check the patient’s vital signs.
- Check the patient’s intake output.
- Do not give the patient sodium-rich food.
- Give the patient fluids as prescribed.
- Give the patient diuretic medicine.
- Maintain the patient’s potassium level To do.
- Provide albumin and protein supplementation to the patient.
- Check the patient’s abdominal girth daily.
- Check the patient’s weight. If there is weight gain, it indicates fluid retention.
- Conduct laboratory tests of the patient.
- Prepare the patient and his family members for surgery.
- Clear all doubts of the patient and family members.
- Provide psychological support to the patient and his family members.
4) Discomfort related to disease condition.
5) Altered sleeping pattern related to pain.
6) Activity intolerance related to weakness.
7)Risk for infection related to bone marrow depression secondary to chemotherapy.
LEUKEMIA CANCER:
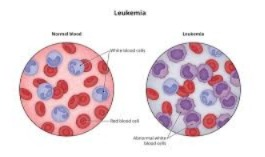
The word Leukemia comes from the Greek word leukos.
Leukemia means “leukos : white ” Aimia : blood ”
Leukemia is a type of cancer of the bone marrow and blood system.
Leukemia is a type of cancer of the blood and bone marrow,
Leukemia is a type of cancer of the blood and bone marrow, where the body produces abnormal white blood cells. These cells don’t function properly and can crowd out healthy blood cells, leading to serious health issues. (Increase the risk of infection: The chances of infection in the body increase.) lack of red blood cell ( result in fatigue, weakness, and Anemia : Low blood pressure causes fatigue, weakness, and anemia). lack of normal platelet count production ( Increase the risk of bleeding: Low blood pressure causes the blood to clot.)
classification ( classification ):
- A) Acute leukemia,
- B) Chronic leukemia .
A)Acute leukemia: In this, blood cells are formed very quickly and immediate treatment of this Acute leukemia is very important because in this, blood cells It grows rapidly. It forms and results in cancer.
B)Chronic leukemia: In this leukemia, there is an excess of abnormal white blood cells, which form and it takes months and years for this to happen. But these cells It grows faster than normal cells and due to this, many white blood cells are formed.
Other classification:
- 1) ALL (Acute lymphocytic leukemia),
- 2) CLL ( Chronic lymphocytic leukemia),
- 3) AML ( Acute myelogenous leukemia),
- 4) CML ( Chronic myelogenious leukemia),
- 5) HCL ( hairy cell leukemia).
1) Acute lymphocytic leukemia: This is very common in young children and adults, especially after 65 years of age.
2) Chronic lymphocytic leukemia: This is more common in people after 55 years of age and sometimes even in children.
3) Acute myelogenious leukemia: This leukemia is more common in adults than in children. And it is mainly seen in men more than women.
4) Chronic Myelogeneous leukemia : This is mainly seen in adults.
5) Hairy cell leukemia: This leukemia is curative and can be easily treated.
Etiology :
- Due to excessive contact with radiation.
- Due to working with certain types of chemicals.
- atomic 💣bomb explosions.
- X Ray,
- smocking,
- chemotherapy,
- inherited disorder,
- Human t cell leukemia viral type,
- family history.
clinical manifestation (symptoms and signs):
- Difficulty breathing,
- Weight loss,
- Fever,
- Frequent infections,
- Pain in bones and joints,
- Pain when touching bones and joints,
- Feeling tired,
- Weakness,
- Loss of appetite,
- Swelling of lymph nodes Swelling in the spleen,
- Swelling of the spleen,
- Night sweats,
- Excessive bleeding,
- Purple patches on the skin,
- Headache,
- Confusion,
- Looking pale,
- nausea,
- seizure,
- vomiting,
Diagnostic evaluation:
- History taking and physical examination,
- blood test,
- Biopsy,
- other findings,
- lumber puncture,
- Radiography,
- ct scan ,
- MRI.
Management:
- chemotherapy,
- Radiation therapy,
- Stem cell therapy,
- biotherapy,
- Bone Merrow transplantation.
Nursing management:
Nursing diagnosis
1) High risk of infection related to Neutropenia.
Nursing interventions:
- Wash hands properly before visiting the patient.
- Refrain from visitors with communicable diseases from visiting the patient.
- Keep the patient in isolation.
- Bathe the patient properly.
- Tell the patient to maintain oral hygiene.
- Do not take any suppositories, enemas, or rectal temperatures.
- Take the prescribed analgesics and antibiotics Provide medications.
- Check for any infection where the intravenous line is inserted.
- Check the patient for any fungal or viral infection.
2)High risk of bleeding related to bone marrow suppression.
Nursing interventions : Prevent bleeding
- Do not administer aspirin or any aspirin-containing products to the patient.
- Do not give the patient an intramuscular injection.
- Have the patient have a clean toothbrush Give to brush.
- Do not insert rectal suppositories into the patient.
- Do not insert a urinary catheter.
- When suctioning, Avoid trauma to the oral mucosa.
- Change the patient’s position frequently to prevent bed sores.
- Do not over-inflate the BP cuff.
3) Fluid volume definitely related to less intake.
Nursing interventions : maintain electrolyte and fluid balance:
- Maintain the patient’s intake-output chart every day.
- Check the patient’s weight every day.
- Check the patient for any signs of dehydration or fluid overload.
- Get lab investigations done.
- Give the patient intravenous fluids fluid Provide.
4)Discomfort related to pain.
Relief from pain:
- Give the patient a cold sponge.
- Change the patient’s bed linen and towels daily.
- Provide the patient with gentle massage.
- Use acetaminophen to reduce fever.
- Provide anal sex to the patient.
- Make a proper environment for proper sleep.
5)Activity intolerance related to weakness.
Nursing interventions: improve activity level of client.
- Tell the patient to maintain a balance between work and rest.
- Tell the patient to do proper exercise.
- Tell the patient to sit in a comfortable chair or bed.
- Tell the patient to do some activity.
6) altered nutrition less than body requirement related to Anorexia, vomiting secondary to side effect of chemotherapy.
Maintain adequate nutrition.
- Provide analgesic and antipyretic medicine to the patient.
- Maintain oral care of the patient.
- Feed the patient in small and frequent amounts.
- Check the patient’s weight daily.
- Provide fluids to the patient through an intravenous line.
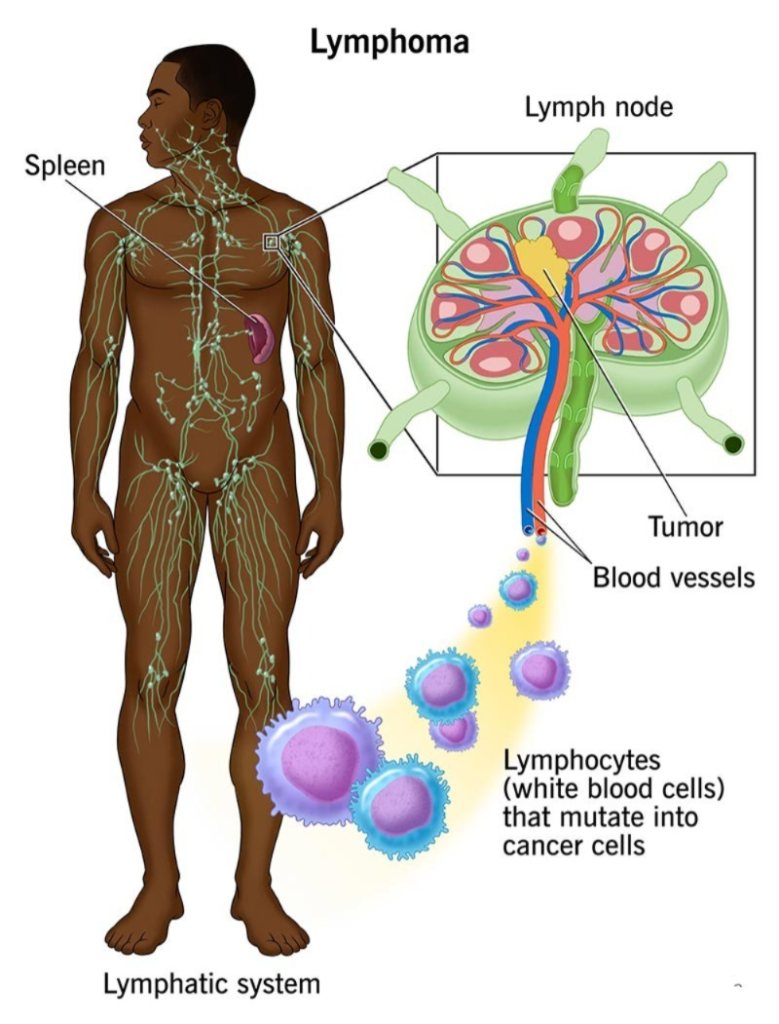
Lymphoma ( Hodkings disease) :
introduction (Introduction) :
This involves abnormal and uncontrolled growth of cells and the formation of tumors. This tumor is cancerous and causes cancer-like disease in the lymphatic system. It is mainly in the lymphatic system. Along with this, the spleen and lymph nodes are also involved.
Etiology:
- Age: peak at 20 years above or 50 years above.
- Gender: It is mainly more common in men.
- carcinogenesis,
- cytotoxic drug,
- other body parts cancer,
- other disease condition.
clinical manifestation (symptoms and signs):
- Enlargement of lymph node,
- Node is firm and painless,
- pruritus,
- severe pain,
- fever without chills,
- fever without chills,
- Weight loss ( weight loss ),
- night sweat ( night sweat ),
- mild Anemia ( mild anemia ),
- Dysapnia ( difficulty breathing ),
- Cough ( cough ),
- jaundice ( jaundice ),
- Abdominal pain ( Abdominal pain ),
- Bone pain ( Bone pain )
Diagnostic evaluation ( Diagnostic evaluation ) :
- lymph node Biopsy,
- presents of” B”symptoms: like ( Presence of B symptoms )
- Fever without chills,
- Excessive weight loss,
- Night sweat ( Night sweats )
- X Ray ( X Ray ),
- ct scan ( CT scan ),
- PET test ( prositron Emissions tomography : Positron Emission Tomography ),
- Laboratory test ( Laboratory test),
- Bone Merrow Biopsy (Bonemarrow Biopsy),
- Bone scane ( Bone Scane ).
Management ( Management ):
- Combination ABVD:
- A:=achiamycin,
- B:=Bliomycine ,
- v:=Vinblastine,
- D:=Dacrabazine.
- Combination of abvd is standard treatment.
General nursing management ( Nursing Management ):
- Explaining the disease condition.
- See its benefits and its limitations.
- Check the patient’s vital signs.
- Prescribe the patient Provide the treatment done.
- Provide an environment where the patient can do some amount of activity on his own.
- Maintain the patient’s hygienic condition.
- Take care that the patient does not get infected.
- Provide the patient with a well-balanced diet.
- If there is any kind of oncological emergency Report to the physician.
- Provide psychological support to the patient and his family members.
- Clear all doubts of the patient and his family members.

FOR UNLOCK 🔓 FULL COURSE NOW. MORE DETAILS CALL US OR WATSAPP ON- 8485976407
For unlocking the full course 🔓 or for more information, contact or whatsapp the following number.-
8485976407