ENGLISH-MSN 1 UNIT 13 CONNECTIVE TISSUE AND COLLAGEN DISORDERS(UPLOAD)
CONNECTIVE TISSUE AND COLLAGEN DISORDERS:
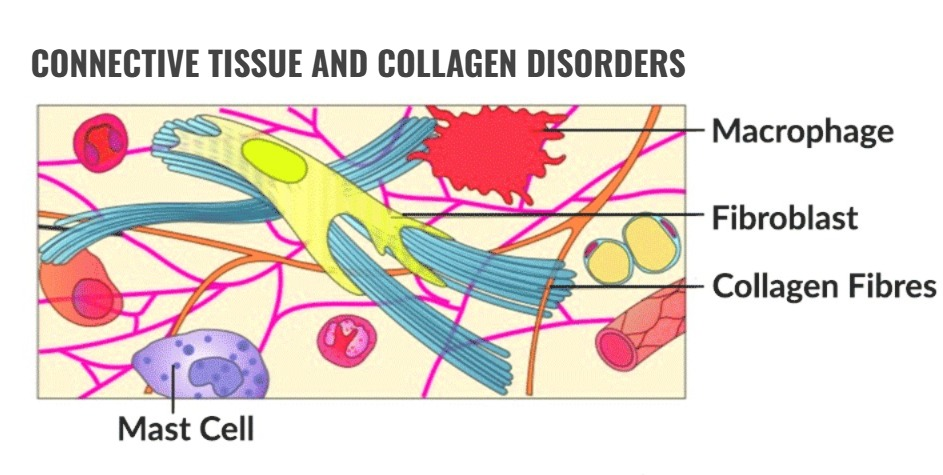
Define Rheumatoid Arthritis.
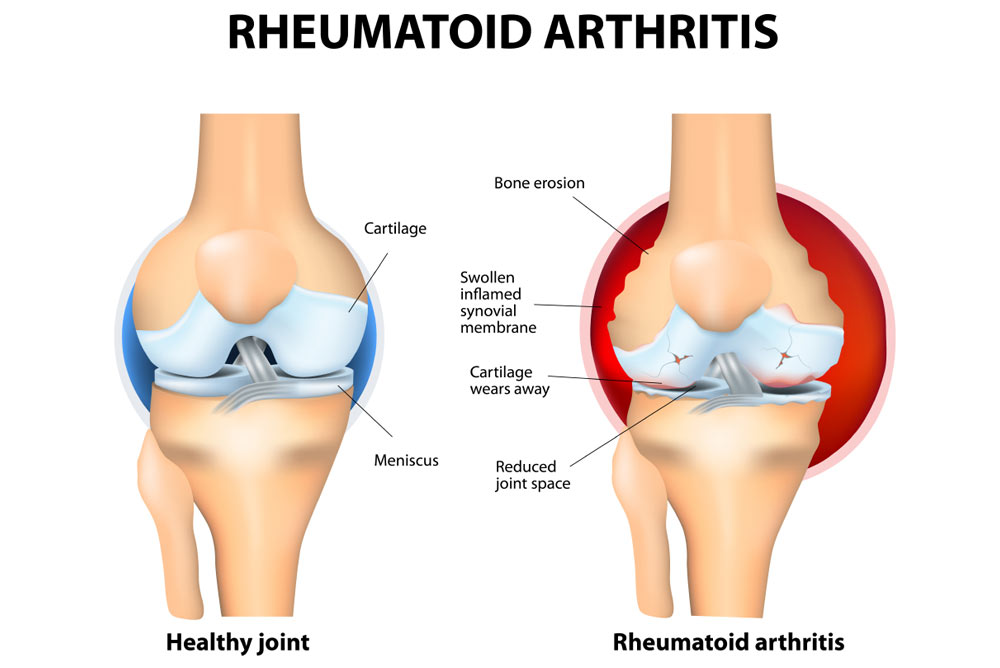
- Rheumatoid Arthritis is a chronic, systemic, autoimmune connective tissue disorder that causes inflammation of the tissues that line the synovial membrane around the joints, along with destruction and proliferation of synovial members, resulting in joint destruction, ankylosis (stiffness of the joint) and deformity (physical deformity).
- In autoimmune disease, the body’s immune system produces antibodies against normal cells and damages normal cells. This is called autoimmune disease. Joint pain, stiffness, and immobility occur.
- Rheumatoid arthritis also affects other organs of the body, including the skin, eyes, lungs, and blood vessels.
Explain Etiology of Rheumatoid Arthritis (Causes of Rheumatoid Arthritis):
- The exact cause of rheumatoid arthritis is unknown.
- Due to genetic factors (if a parent has this disease, there is a possibility of it in their child),
- Due to stress.
- Sex: women are more likely to develop Rheumatoid Arthritis.
- Due to any infectious agent.
- Age is mainly from 30 Between the ages of 60 and 80.
- Due to environmental factors.
- Due to family history.
- Due to hormonal effects.
- Due to long-term smoking.
- Due to metabolic and biochemical abnormalities.
- Due to any bacterial, fungal, viral infection.
- Due to immunological response.
Explain the Stages of Rheumatoid Arthritis (Explain the Stages of Rheumatoid Arthritis).
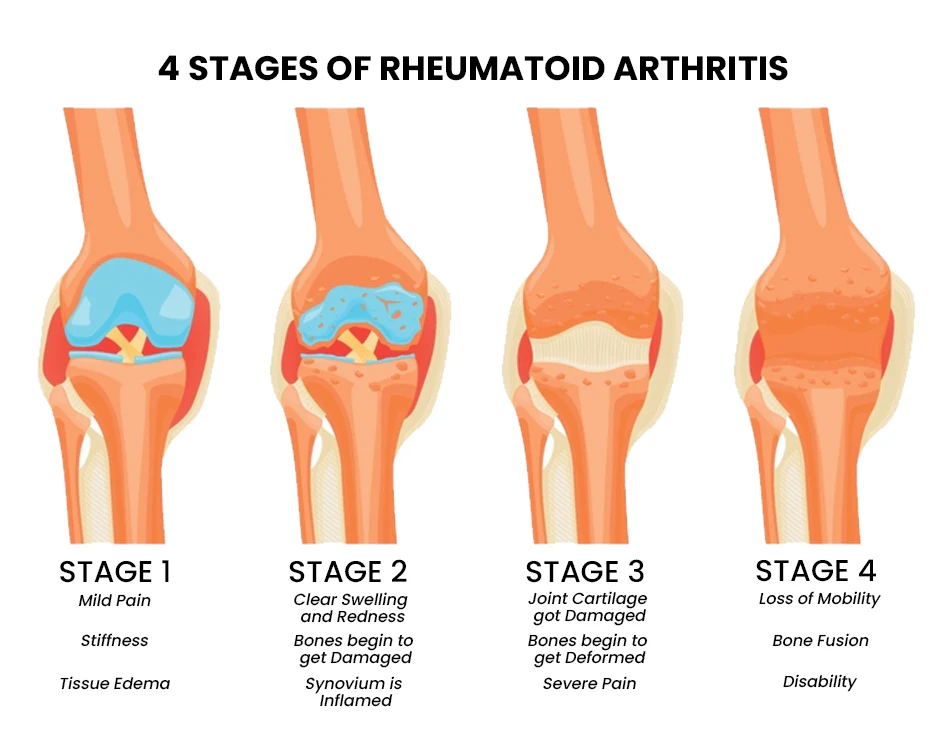
1) Synovitis,
2) Pannus formation,
3) Fibrous tissues Ankylosis,
4) Bony Ankylosis.
1) Synovitis:
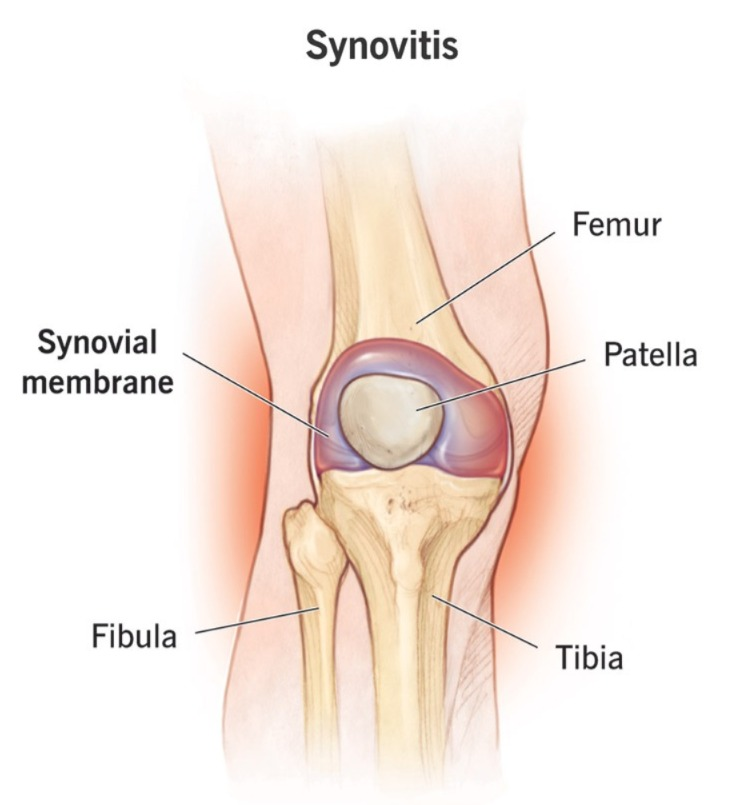
- In the synovitis stage, when an infection occurs in the body, the infection affects the synovial membrane of the joint and due to this, the synovial members become infected and inflamed, causing synovitis and an increase in synovial fluid.
2) Pannus formation:
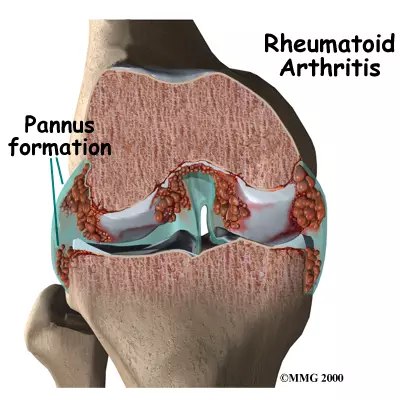
- In this, the synovial fluid gets invaded and it becomes very thick and this fluid increases around the capsule of the joint.
3) Fibrous tissues Ankylosis (Fibrous tissues) Ankylosis):
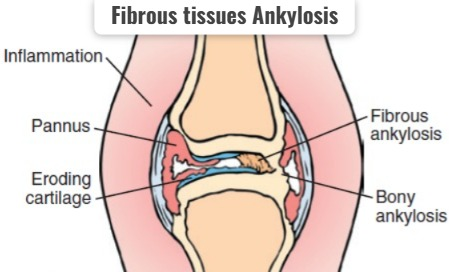
- In this, the synovial fluid increases a lot and it becomes stiff and it gets stuck around the joint and forms a hard structure. does the formation of .
4)Bony Ankylosis:
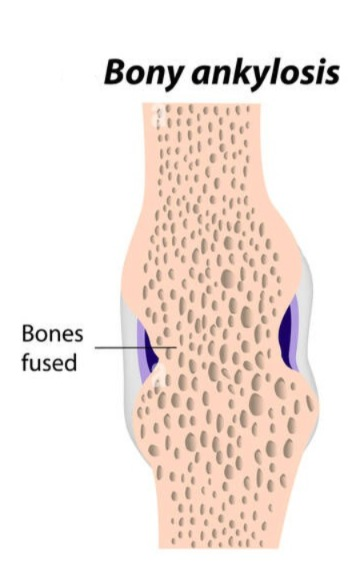
- In this, fibrous tissue forms a very hard structure and forms a bone-like formation and due to this the joint becomes immobilized and stiffness occurs in it.
Due to any etiological factor.
|
\/
Infection of the synovial membrane occurs.
|
\/
Inflammation of the synovial members occurs.
|
\/
Synovial fluid is secreted from the synovial members This fluid progresses and accumulates in the bone.
|
\/
Then the bone becomes very hard and stiff which immobilizes the bone.
|
\/
Rheumatoid arthritis .
Explain Clinical Manifestation/ sign and symptoms :
- The affected joint becomes red and warm.
- The joints become swollen and stiff and tender.
- Joint pain occurs.
- Morning stiffness occurs in the joints.
- Arthritis occurs in more than three bones.
- Joint becomes swollen ( sponge like ).
- Arthritis occurs in the joints of the hands.
- Firm bumps of tissues under the skin on Arms.
- Rheumatoid nodules form.
- Rh factor positive.
- Fluid accumulation occurs in the ankles.
- The joint loses its range of motion and becomes deformed.
- Muscular Atrophy around the affected joint.
Ulnar Deviation:
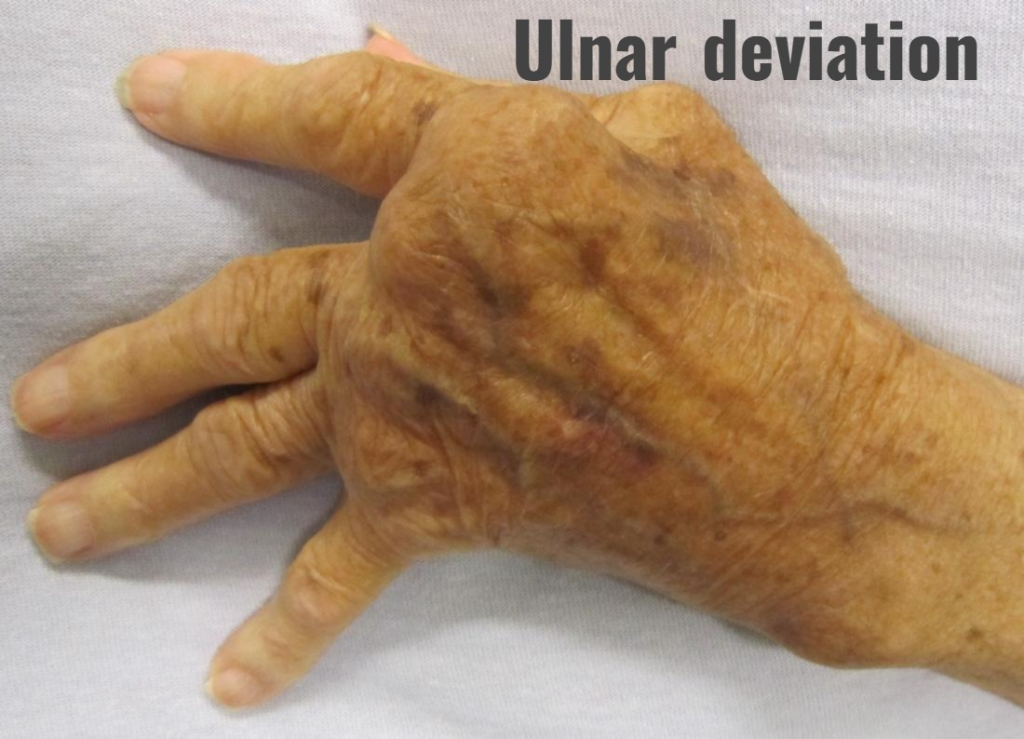
In this, the finger deviates towards the ulnar surface.
Swan Neck Deformity:
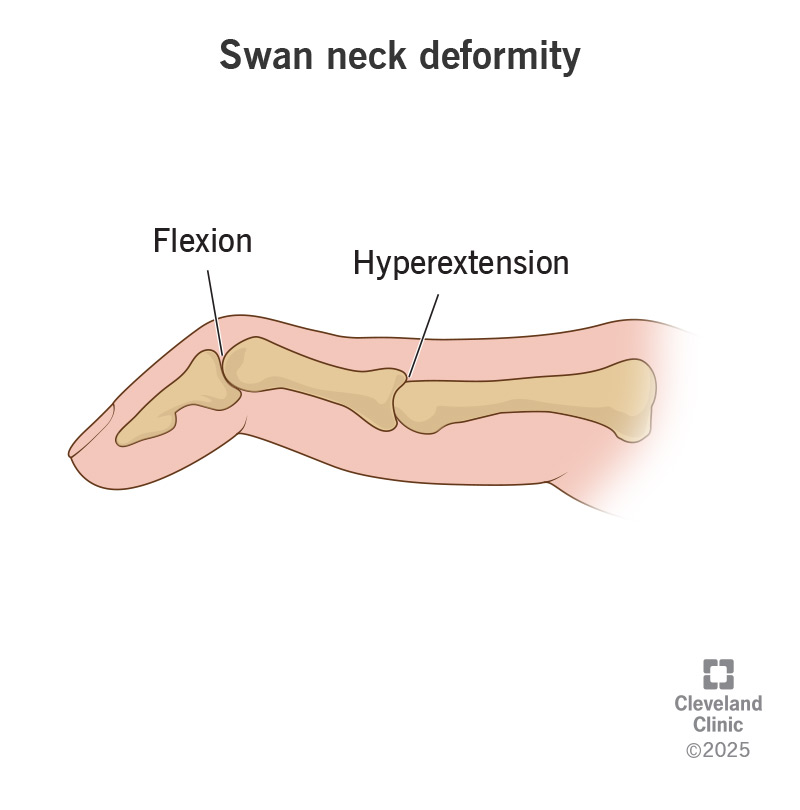
In this the finger becomes a swan sap.
Buterine Deformity (Buterine deformity):
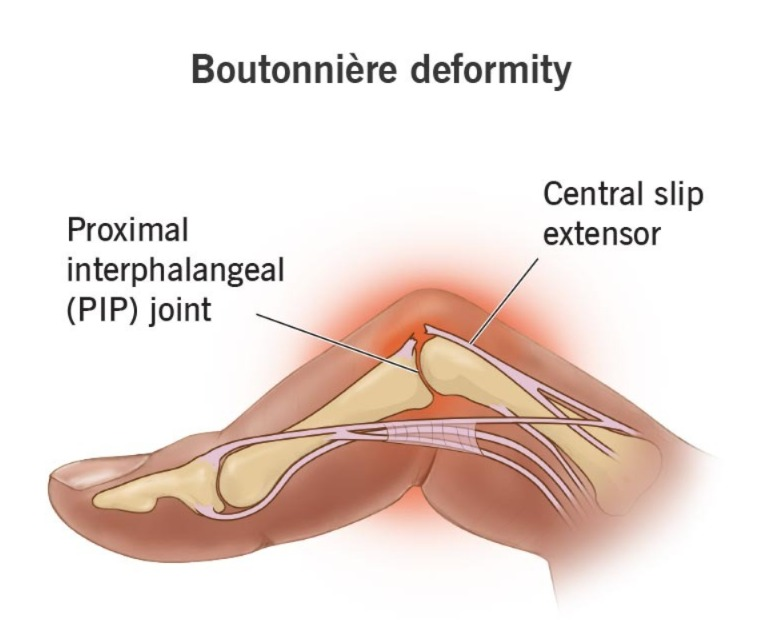
Ama, finger is bent.
- knock knee.
- Difficulty in sleeping.
- Numbness and tingling sensation.
- Burning sensation in hand and foot.
- Module formation within the skin.
- Burning sensation in the eyes.
- Itching and discharge.
- Dry mouth and eyes.
- Chest pain.
- Weakness.
- Trouble breathing.
- Fatigue.
- Loss of appetite. Feeling.
- Weight loss.
- Low grade fever.
- Malaise.
- Depression.
- Lymphadenopathy.
- Inflammation of blood vessels.
- Multiple organ involvement (pericarditis, osteoporosis, anemia, subcutaneous nodules, vasculities, neuropathy, fibrotic lung disease).
Explain Diagnostic Evaluation (Write a diagnostic evaluation):
- history tacking and physical examination (History Taking and Physical Examination).
- Rheumatoid factor test: RA positive (Rheumatoid factor test).
- Antinuclear Antibody test (Antinuclear Antibody Test).
- Erythrocyte sedimentation rate (ESR).
- C-reactive protein (CRP test).
- complete blood count test (Complete blood count).
- comprehensive metabolic panel (to monitor kidney and liver function).
- synovial fluid analysis (synovial fluid changes from transparent to milky, cloudy, and dark yellow fluid).
- Arthroscopic examination (Anthroscopic examination) .
- X Ray ( X Ray ) .
- joint Ultrasound ( Joint Ultrasound ) .
- MRI (M.R.I.) .
Explain the management of rheumatoid arthritis (Write the management of rheumatoid arthritis):
Medical Management (Medical Management):
1) NSAID (NON STEROIDAL ANTI INFLAMMATORY DRUG):
This medicine is used to relieve pain and inflammation.
Ex: ibuprofen,
Naproxen sodium.
2) DMARDs ( Disease modifying Antirheumatic Drugs):
These are mainly given in conditions such as moderate to severe Rheumatoid Arthritis.
Ex: imuran,
Anti malarial medication,
Panicillamine and methotrexate.
3) Antimalarial medication :
This medicine mainly uses hydroxychloroquine along with methotrexate. is.
4)Corticosteroid (Corticosteroid) :
Corticosteroid is used to relieve inflammation.
5)Biological agent (Biological agent) :
Tnf-a antagonist targets B cells, T cells.
- Biological agent મા actemra,
- Rituxan,
- Remicade,
- Enbrel,
- Kindred નો સમાવેશ થાય છે.
- Kindred is included.
6) Immunosupressants:
The immune system in rheumatoid arthritis is suppressed. In arthritis, this medication weakens the immune system or .
Ex: Azathioprine (imuran, azasan),
Cyclosporine.
7) tumor necrosis factor a :
This medicine inhibits the inflammatory chemical that is tumor necrosis factor.
Explain Surgical management:
1) Joint fusion :
In this, the joint is surgically fused to stabilize the joint.
2) Synovectomy:
In this, the joint lining is removed.
This is mainly used to remove the inflamed tissues that are causing pain.
Synovectomy is mainly used to reduce swelling and slow down joint damage.
3) Tendon repairs:
The tendons around the joint that are inflamed and damaged cause loss of tendons, so the surgeon repairs the tendons around the joint and keeps it stable.
4) Total joint replacement:
In joint replacement, the surgeon removes the damaged joint part and inserts a prosthesis made of metal or plastic in its place.
Explain nursing management:
- Assess the patient’s pain level.
- Assess whether the patient has morning stiffness.
- Provide the patient with a comfortable position.
- Encourage the patient to engage in non-pharmacological management.
Such as yoga, relaxation techniques, guided imaginary, and rhythmic breathing. - Advise the patient for hot and cold applications.
- Provide the patient with prescribed medicine.
- Instruct the patient to rest between activities.
- Instruct the patient to rest frequently.
- Instruct the patient to engage in physical activities such as walking, swimming etc.
- Ask the patient to use an assistive device.
- Ask the patient to verbalize his/her feelings.
- Provide the patient with complete education about the disease and its treatment.
- Ask the patient to maintain strict aseptic technique.
- Provide the patient with education on self Participate in care activities.
- Encourage the patient to join self-help groups and support groups.
Define systemic lupus erythematosus:
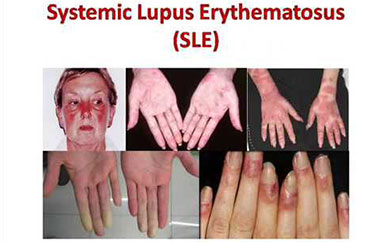
- Systemic lupus erythematosus is a chronic inflammatory, autoimmune, multisystem disorder.
- In which the body’s immune system mistakenly attacks its own tissues. Due to which a large amount of inflammation and tissue damage is observed.
- Systemic lupus erythematosus mainly affects the skin, joints, kidneys, blood cells, brain, heart, lungs.
Write causes and risk factors of systemic lupus erythematous (Write causes of systemic lupus erythematosus)
- The exact cause of systemic lupus erythematosus is unknown. However, it is thought to be caused by genetic, hormonal, and environmental factors.
Write sign and symptoms of systemic lupus erythematosus (Write sign and symptoms of systemic lupus erythematosus)
- Skin rash: Butterfly shaped rash across the cheek and nose
- Joint pain and swelling
- Fatigue
- Tiredness
- Photo sensitivity
- Fever
- Hair Loss
- Kidney Problems
- Swelling in Legs and Feet
- High Blood Pressure
- Raynaud’s Phenomenon
- Mouth Sores
- Chest Pain
- Headache
- Diarrhea
- Seizures
- Memory Loss
- Enlargement of Lymph Nodes
- Anemia
- Low White Blood Cells Blood Cells
- Low Platelet Count
Write diagnostic evaluation of systemic lupus erythematosus
- History Collection
- Physical Examination
- Blood test (antinuclear antibody (ANA) test, anti-dsDNA, anti-Smith antibody)
- Urine test (check for kidney involvement)
- Biopsy (in some cases)
Write management of systemic lupus erythematosus (Write management of systemic lupus erythematosus) erythematosus)
✓ Medication :
- Non-steroidal anti-inflammatory drugs: Non-steroidal anti-inflammatory drugs are given to relieve inflammation and pain.
- Antimalarial drugs: Antimalarial drugs such as Use hydroxychloroquine.
- Corticosteroid: Use corticosteroid drugs such as prednisolone to reduce inflammation.
- Immunosuppression: Use immunosuppression drugs such as methotrexate to suppress immunity.
- Biologics: Biologics are used when all other treatments fail. Targets specific parts of the immune system.
✓ Lifestyle Changes :
- Regular Exercise: Exercise regularly. Which maintains joint flexibility and muscle strength.
- Healthy Diet: Advise the patient to consume a healthy and well-balanced diet.
- Sun Protection: Use sun screen and protective clothes to protect from the sun.
- Stress Management: Use yoga, meditation and relaxation techniques for stress management.
- Avoid Smoking: Avoid smoking. To do.
Define scleroderma
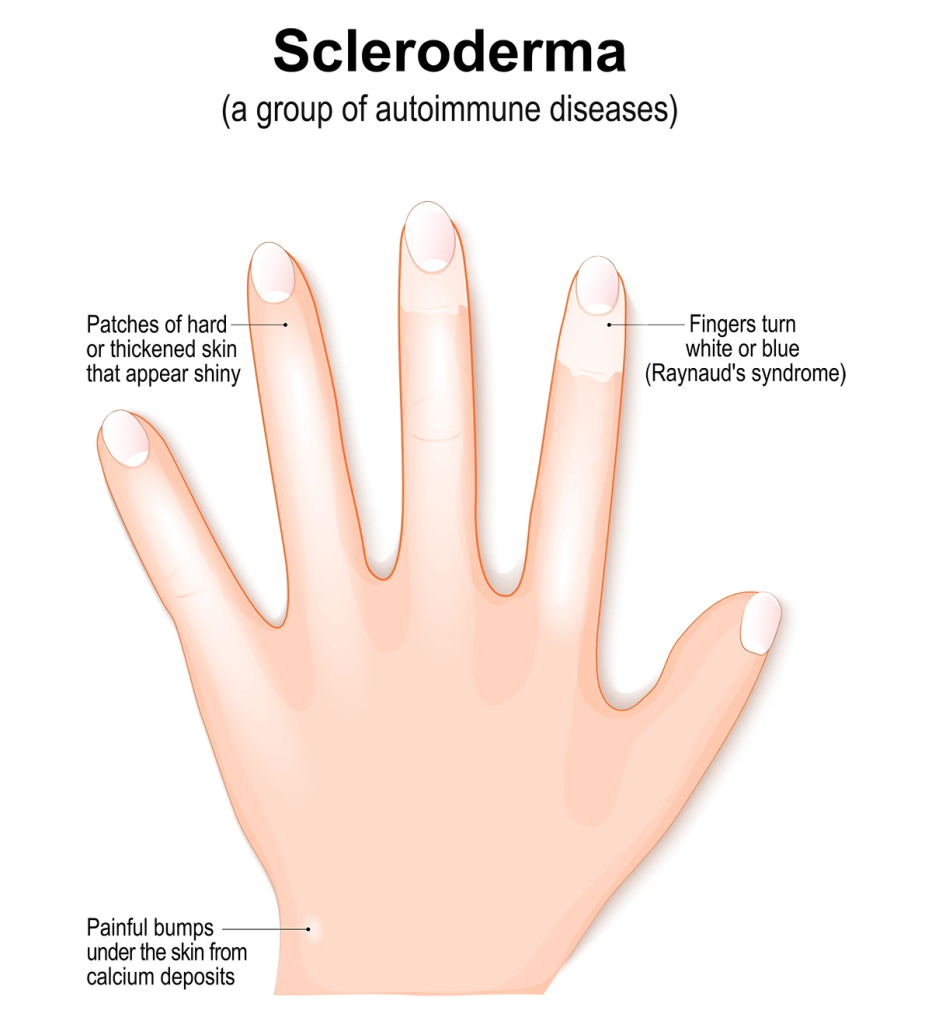
- Scleroderma is also known as ‘systemic sclerosis’ and ‘CREST syndrome’ .
- Scleroderma is a chronic autoimmune condition characterized by excessive collagen production, which causes hardening and tightening of the skin and connective tissue.
- Scleroderma is mainly seen between the ages of 30 and 50. It also affects women more.
Write causes of scleroderma
- The exact cause of scleroderma is unknown. But it is seen due to genetic, environmental and immunological factors.
- Genetic factors (genetic predisposition)
- Autoimmunity (body mistakenly attacks its own tissue)
- Environmental factors (exposure to toxins, chemicals – silica, dust, vinyl chloride bleomycin, aromatic hydrocarbons)
- Hormonal factors (Hormonal Imbalance)
Write sign and symptoms of scleroderma
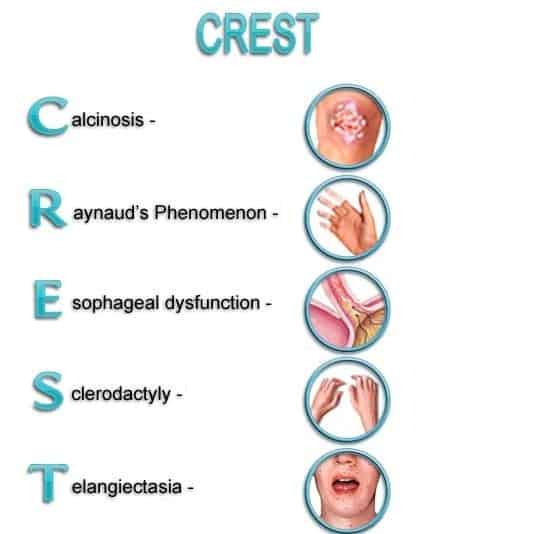
- Calchinosis : Deposition of calcium in skin
- Raynaud’s phenomenon : Abnormal blood flow during contact with stress and cold
- Esophageal dysfunction : Difficulty in swallowing
- Sclerodactyly : Tightening of skin on the fingers and toes
- Telangiectasia : Red spots on hand, forearm, palm, face
- Swelling and puffiness
- Shiny skin
- Ulcers and Sores
- Joint Pain and Stiffness
- Muscle Weakness
- Shortness of Breath
- Irregular Heart Beat
- Fatigue
Write diagnostic evaluation of scleroderma
- History Collection
- Physical Examination
- Blood Tests (ANA-Antinuclear Antibody, ACA-Anticentromere Antibody, anti-scI-70 – Antitopoisomerase I Antibody)
- Skin biopsy
- Electrocardiogram
- Pulmonary function test
- X-ray
- Urine analysis
Write management of scleroderma
- Immunosuppressant: Use immunosuppressant drugs such as methotrexate, cyclophosphamide to suppress immunity.
- Corticosteroid: Use corticosteroid drugs to reduce inflammation.
- Calcium channel blocker: Use calcium channel blocker for the treatment of Raynaud’s phenomenon and to control high blood pressure. Such as nifedipine
- Antacid (H2 blocker): Use proton pump inhibitor or H2 blocker to manage gastroesophageal reflux disease.
- Pain management: Use analgesic, non-steroidal anti-inflammatory medicine to relieve pain.
- Skin care: Keep the skin moisturized regularly. So that the skin remains soft and hydrated. Protect the skin from trauma and avoid exposing the skin to extreme temperatures.
- Physical therapy: Use range of motion exercises and stretching exercises to maintain joint flexibility and prevent contractures.
- Pulmonary rehabilitation: Lung involvement is seen in some cases. Hence, arrange a pulmonary rehabilitation program. This includes providing education on deep breathing exercises, techniques to improve respiratory function, lung health, etc.
- Heart health management: Regularly monitor heart function. Take prescribed medicine to manage high blood pressure and arrhythmia. To arrange a cardiac rehabilitation program.
Define polymyositis
- Polymyositis is a rare autoimmune condition in which inflammation occurs in many connective tissues and muscle fibers. Which causes muscle weakness.
- Which affects the skeletal muscles on the sides of the body.
Write causes of polymyositis
- The exact cause of polymyositis is unknown, but it is believed to be a combination of genetic factors, infectious agents, and environmental factors. It is believed to be caused by triggers and certain drugs.
- Muscle weakness (predominant symptom)
- Weakness is seen especially in the muscles near the trunk. Such as shoulder, hip, thigh, upper arm
- Muscle pain and stiffness
- Tenderness
- Difficulty in rising from a seated position
- Joint pain
- Difficulty in swallowing
- Skin Rash
- Fever
- Unintentional Weight Loss
- Irregular Heart Rhythm
Write sign and symptoms of polymyositis
Write diagnostic test for polymyositis
- History Collection
- Physical Examination
- Blood Test (Muscle Enzyme-Creatine Kinase, Aldolase)
- Electromyography
- Muscle Biopsy
- CT scan
- MRI
- Pulmonary function test
- Swallowing study
Write management of polymyositis
- Corticosteroid: Corticosteroid drugs are given to reduce inflammation and muscle weakness. Such as prednisone
- Immunosuppressive drugs: Immunosuppressive drugs are given along with corticosteroids to suppress immunity. E.g. Methotrexate, mycophenolate
- Intravenous immunoglobulin: Intravenous immunoglobulin is given to some patients when no response is seen to other treatments.
- Biologic agents: Biological agents are given in refractory cases and when other treatments cannot be tolerated. For example, Rituximab
- Physiotherapy: Exercises to improve flexibility, strength, and function of muscles.
- Speech therapy: Providing speech therapy to patients with swallowing difficulties. Because speech therapy improves swallowing function.
Osteoarthritis:
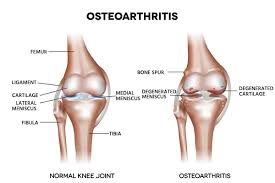
- Osteoarthritis is a chronic, noninflammatory, and slowly progressive disorder that causes deterioration of articular cartilage. Osteoarthritis mainly affects the hip bone and knee bone.
- Osteoarthritis is also called degenerative joint disease. It is a slow, progressive, noninflammatory disorder that mainly affects mobile joints, particularly articulation joints.
- Osteoarthritis is caused by the breakdown of the cartilage around the joint.
Types of Osteoarthritis
1)Primary Osteoarthritis:
- Primary Osteoarthritis is mainly seen in elderly people and mainly in women.
- Osteoarthritis is seen due to trauma, hereditary, obesity, age etc.
2)Secondary Osteoarthritis:
- Secondary osteoarthritis can occur at any age. It is mainly caused by any prior injury, repeated strain or sprain, joint dislocation, fracture, inflammation, congenital dislocation of hip, Disorder of nervous system, Use of corticosteroids etc.
Etiology:
- Due to older age, more common in women,
- Due to genetic factors,
- Due to excess weight,
- Due to obesity,
- Due to septic arthritis,
- Trauma Due to,
- due to strenuous and repetitive exercise,
- due to joint injury,
- due to decreased estrogen levels.
- due to increased parathyroid hormone.
- due to metabolic diseases such as diabetes, gout, and other hormonal disorders.
clinical manifestation/ sign and symptoms:
- Joint pain,
- Joint stiffness,
- Pain increases with activity and decreases with rest.
- Stiffness in the joints in the morning.
- parestheia(tingling and numbness sensation),
- swelling,
- weakness in the muscles,
- Bony deformity,
- swelling in the joints (warmth, effusion, synovial thickening).
- Tenderness and soreness in the joint.
- Back pain.
- Reduced flexibility of the joint.
- Reduced range of motion in the affected joint.
- Crapitus (a sound made by friction between two bones).
- Swelling in the bone.
- grating sensation.
diagnostic evaluation:
- History taking and physical examination
- X Ray,
- ct scan,
- MRI,
- Blood test,
- analysis of synovial fluid,
- erythrocyte sedimentation rate (ESR Test),
- Radionuclide imagine.
management of Osteoarthritis:
- If the patient is in pain, provide him with analgesic medicine.
- Ex: acetaminophen
- Provide medicine to relieve inflammation and pain.
- Ex:=NSAID( Non steroidal anti inflammatory drug),
- Ibruprofen,
- Naproxen.
- Tramadol.
- Cox 2 inhibitor drug.etc.
- Reduce proper weight to avoid stress on the joints.
- Do proper exercise. Exercise increases joint movement and muscle strength in the muscles around the joints.
- Do simple exercises like swimming and walking, i.e. on a flat surface. This is because these exercises are less stressful on the joints.
- Telling the patient to take proper nutrition, get proper sleep and reduce stress, which improves well-being.
- Telling the patient with dementia to lose weight.
- Losing weight reduces stress on the knee joint, hip joint and spine, and pain is also relieved.
- When the patient’s pain When the level increases excessively, it is also necessary to manage the patient surgically.
- Using supportive devices such as splints, shoes, due to which the pain level is reduced.
- Using supportive assistive devices, due to which the pressure on the joint is reduced and it is mainly used to stabilize the ligament and reduce the pain level.
- Glucosamine and chondroitin: This is mainly used to reduce the pain in a person who has a condition of osteoarthritis.
- Provide hot and cold applications to the patient.
- Providing hot therapy reduces joint stiffness and should be provided mainly two to three times throughout the day.
- Cold therapy is mainly used to reduce swelling and cold applications should not be applied for more than 20 minutes.
surgical management of Osteoarthritis:
1)Osteotomy:
- In osteotomy, the bone is cut from above and below and the weight is reduced, due to which the pain level is reduced.
2) Joint fusion:
- In joint fusion, the damaged joint is removed and the two bones are fused and this is mainly done where joint replacement is not effective.
3)Arthroscopy:
- In arthroscopy, the damaged cartilage is mainly cleaned and the tissues are repaired.
4)joint replacement:
- In joint replacement, the surgeon removes the damaged joint surface and replaces it with a plastic or metal device called a prosthesis.
nursing management (nursing Management):
- Assess the patient’s pain level.
- Measure the location of the patient’s pain and its intensity using a pain scale.
- Provide the patient with hot or cold applications.
- Ask the patient to change positions frequently and to assume a comfortable position.
- Ensure the patient takes complete rest Tell.
- Tell the patient to take the prescribed analgesic medicine.
- Provide the patient with a comfortable mattress, pillow, and proper rest.
- Tell the patient to maintain good body mechanics while walking, sitting, moving, or lifting anything.
- Instruct the patient to use devices such as splints, braces, traction, etc. properly. Tell.
- Tell the patient to take complete rest.
- Tell the patient to take the analgesic medicine prescribed by the doctor.
- Tell the patient to adopt stress management techniques.
- Provide education to the patient or reduce activities that increase the pain level.
- Provide hot and cold applications to the patient To do.
- Provide education to the patient to maintain correct posture and body mechanism.
- Ask the patient to roll a towel and then rest by keeping it at neck level.
- Ask the patient to reduce weight.
- Ask the patient to do as much activity as possible.
- To do range of motion exercises for the patient Give advice.
- Provide education to the patient to get adequate rest, sleep and nutrients.
- Check the patient’s joint site for inflammation.
- Assess the patient’s range of motion of the affected joint.
- Ask the patient to do range of motion exercises.
- Provide a safe environment for the patient For example, raise the chair, use high grip and tub and toilet, the use of mobility aids/wheelchair rescue.
- Provide assistance to the patient in active and passive exercise.
- Advise the patient to do early ambulation by use of assisting device like crutches, walker and canes.
- Provide education to the patient to exercise.
- Advise the patient to use assistive device.
- Ask the patient to maintain a comfortable position.
- Ask the patient to maintain proper posture.
- If the patient is obese, ask him to lose weight.
- Ask the patient to take the prescribed medicine.
- Advise the patient to make lifestyle modifications.
Define ankylosing spondylitis
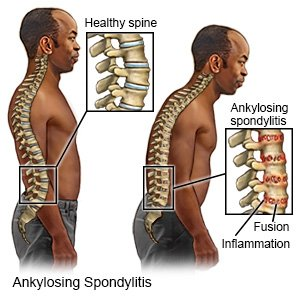
- Ankylosing spondylitis is also known as ‘Bechterew’s disease.
- Ankylosing spondylitis is a chronic inflammatory disorder. Which mainly affects the axial skeleton.
- Ankylosing spondylitis is a type of inflammatory arthritis that mainly affects the spine and large joints (sacroiliac joints).
Write causes and risk factors of ankylosing spondylitis (Write causes and risk factors of ankylosing spondylitis)
- The exact cause of ankylosing spondylitis is unknown. But it is believed to be caused by genetic factors.
- Such people have the HLA-B27 antigen present.
- Ankylosing spondylitis is mainly found in men and develops in late adolescence or early adulthood.
Write sign and symptoms of ankylosing spondylitis (Write sign and symptoms of ankylosing spondylitis) Spondylitis)
- Chronic back pain and stiffness
- Pain typically starts in the lower back and buttocks
- Reduces flexibility of spine
- Stiffness and loss of flexibility of spine
- Difficulty in bending and twisting the spine
- Kyphosis and stooped posture
- Pain and swelling in other joints
- Sacroiliitis (inflammation in sacroiliac joint)
- Peripheral arthritis
- Enthesitis (inflammation at the site of tendon And ligaments attach the bone
- Chest pain
- Uveitis
- Iritis
- Fever
- Fatigue
- Weight loss
Write diagnostic evaluation of ankylosing spondylitis
- History Collection
- Physical Examination
- X-ray
- CT scan
- MRI
- HLA-B27 testing
- Inflammatory markers (CRP, ESR)
Write management of ankylosing spondylitis
✓ Pharmacological Management :
Nonsteroidal Anti-Inflammatory Drugs :
-
- Use nonsteroidal anti-inflammatory drugs to reduce pain and inflammation. Such as ibuprofen, diclofenac
Tumor necrosis factor inhibitor :
- In cases where NSAIDs are ineffective, use tumor necrosis factor inhibitors. Which reduce inflammation and prevent disease progression. Ex. Infliximab, Golimumab,
Interleukin 17 (IL-17) Inhibitors:
- Interleukin 17 inhibitors are given in cases where patients do not respond to tumor necrosis factor inhibitors.
Corticosteroids:
- Intraarticular and topical corticosteroids are used to reduce inflammation and suppress immunity.
✓ Surgical intervention :
Joint replacement surgery :
- Severe Joint replacement surgery is performed in cases where the joint is significantly damaged.
Spinal Surgery:
- Spinal surgery is rarely performed to correct spinal deformities and fractures.
✓ Physical Therapy and Exercise :
Physical Therapy :
- Maintaining posture, flexibility, and mobility is a curricular part of the management of AS. Therefore, tailor-made exercises should be performed that strengthen the back and abdominal muscles and improve posture.
Exercises:
- Perform activities like swimming, walking, and stretching regularly. Which improves spinal mobility and reduces stiffness.
✓ Lifestyle Modification:
Postural Training:
- Provide training to the patient to maintain good posture and make the patient aware about it. Especially while sitting, standing and sleeping.
Smoking session:
- Smoking increases symptoms, so smoking should be avoided.
Healthy diet:
- Healthy Eat a balanced diet to maintain weight and reduce joint strain.
Define fibromyalgia
- Fibromyalgia is also known as a pain syndrome.
- Fibromyalgia is a chronic disorder characterized by widespread musculoskeletal pain, fatigue, sleep issues, and mood disturbances.
Write causes of fibromyalgia
- The exact cause of fibromyalgia is unknown but is thought to be a combination of genetic, environmental, and psychological factors, including:
- Abnormality in pain processing in the central nervous system
- Neurotransmitter imbalance
- Genetic abnormality
- Physical Or emotional trauma
- Hormonal changes
Write sign and symptoms seen in fibromyalgia
- Widespread musculoskeletal pain
- Aching, burning or stabbing pain throughout the body
- Fatigue
- Persistent tiredness
- Sleep disturbances
- Cognitive difficulties (problems in memory, concentration, attention)
- Anxiety
- Mood swings
- Multiple tender points (such as back of head, top of shoulder, chest, hip, knee, outer elbow)
- Numbness and tingling sensation in hand and foot
- Headache
- Digestive problems (irritable bowel syndrome, hypoglycemia)
Write diagnostic evaluation of fibromyalgia
- History Collection
- Physical Examination
- Widespread Pain Index (WPI)
- Symptom Severity Scale (SSS)
Write management of fibromyalgia
- Pain relievers: Use over-the-counter pain medicine acetaminophen or nonsteroidal anti-inflammatory drugs to relieve pain.
- Antidepressants: Use of antidepressant drugs duloxetine, amitriptyline. Which relieve pain, improve sleep and eliminate symptoms of depression and anxiety associated with fibromyalgia.
- Muscle relaxants: Muscle relaxants are useful in eliminating muscle spasms.
- Physical therapy: Stretching exercises, low impact aerobic exercises and strength training. Which can improve muscle flexibility and strength.
- Cognitive Behavioral Therapy: Cognitive behavioral therapy is useful for helping individuals develop coping strategies, change negative thought patterns, and manage anxiety.
Define gout
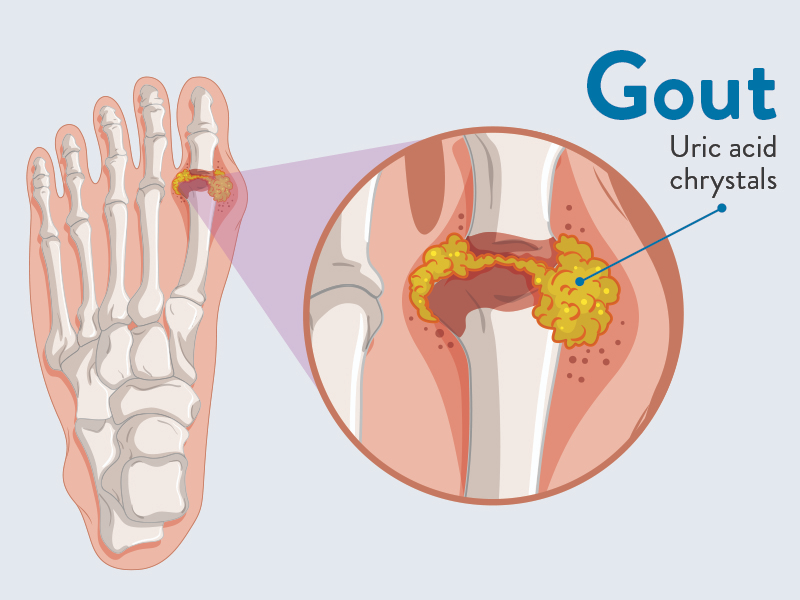
- Gout is also known as ‘gouty arthritis’.
- Gout is a type of arthritis characterized by recurrent attacks of inflammatory arthritis.
- In this condition, the level of uric acid in the blood increases, which leads to the formation of urate crystals. These urate crystals are deposited in the joints, causing pain and inflammation. Gout mainly affects the big toe, but other joints can also be affected. Uric acid is a waste product of purine metabolism and is excreted by the kidneys.
Write type of gout:
There are two types of gout:
1) Primary gout
2) Secondary gout
1) Primary Gout :
- Primary gout is seen to be inherited. In which there is an error in the metabolism of purine due to which overproduction of uric acid is seen and uric acid levels increase and uric acid retention is seen.
2) Secondary gout:
- Secondary gout is mainly seen due to some other disease condition or due to some medicine. Such as chronic renal failure, diabetic ketoacidosis, hemolytic anemia. Medicines like cyclosporine, ethambutol
Write causes of gout
- Alcohol consumption
- Regular intake of seafood, red meat
- Obesity
- Chronic Kidney Disease
- Hemolytic Anemia
- Hypertension
- Diabetes Mellitus
- Diabetic Ketoacidosis
- Malignancy
- Metabolic syndrome
- Cyclosporin
- Salicylate
- Diuretic
Write sign and symptoms of gout
- Severe joint pain: Sudden and severe joint pain may occur. In which the big toe (gout) is mainly affected, besides the ankle, knee, elbow, wrist and finger joints are also affected.
- Lingering discomfort: Even after the pain subsides, discomfort is observed in the joint for a few days and weeks.
- Inflammation and redness: The affected joint appears swollen and red and feels warm to the touch.
- Limited range of motion: Due to pain and swelling in the affected joint, its mobility is reduced.
- Toffee Formation: In cases of chronic gout, urate crystals are deposited under the skin and form a lump-like structure known as a toffee. These toffees are painless but become inflamed during a gout attack.
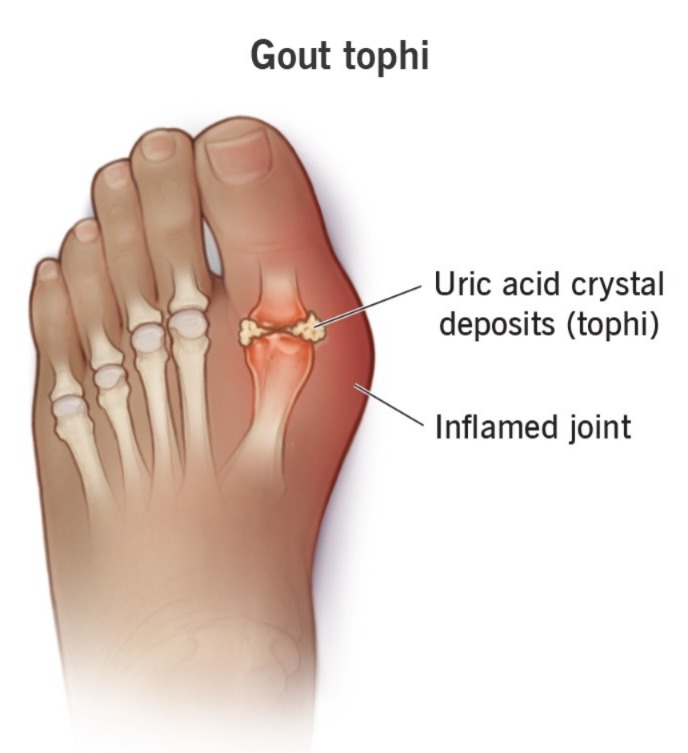
- Fever and Malaise: Some patients experience fever during a severe attack of gout.
Write diagnostic evaluation of gout
- History Collection
- Physical Examination
- Serum Uric Acid Level
- Joint Fluid Analysis
- X-Rays
- Erythrocyte Sedimentation Rate
- Kidney Function Test
Write management of gout
✓ Acute gout attack management :
Non-steroidal anti-inflammatory drug :
- NSAID is the drug of choice for the treatment of acute gout attack. Ex. Ibuprofen, Naproxen
Colchicine :
- Colchicine is an antigout agent that is used to reduce the symptoms of inflammation caused by uric acid crystals. Colchicine is mainly taken when a gout attack has set in.
Corticosteroids:
- Corticosteroid drugs are used in cases where NSAIDs and colchicine are ineffective or contraindicated. Ex. Prednisolone. Corticosteroids are administered orally or directly into the joint.
✓ Uric acid lowering agent:
- Xanthine oxidase inhibitor: Xanthine oxidase inhibitor is used to reduce the production of uric acid. Ex. Allopurinol, Febuxostat
- Uricosuric Agents: Uricosuric agents excrete uric acid through urine and decrease the level of uric acid in the blood. Ex. Probenecid
- Recombinant uricase: In severe cases, recombinant uricase is used to break down uric acid.
✓ Lifestyle Modification:
- Avoid a purine-rich diet. Such as red meat, seafood, alcohol
- Use low-fat dairy products and vegetables in the diet.
- Intake plenty of fluids. So that uric acid can be diluted and crystal formation can be prevented.
- Maintain a healthy weight so that gout attacks can be reduced.
