ENGLISH-Unit-12-neurological Disorder(part-5)(UPLOADED)
Explain/Define Spinal cord injury. (Define Spinal Cord Injury.)
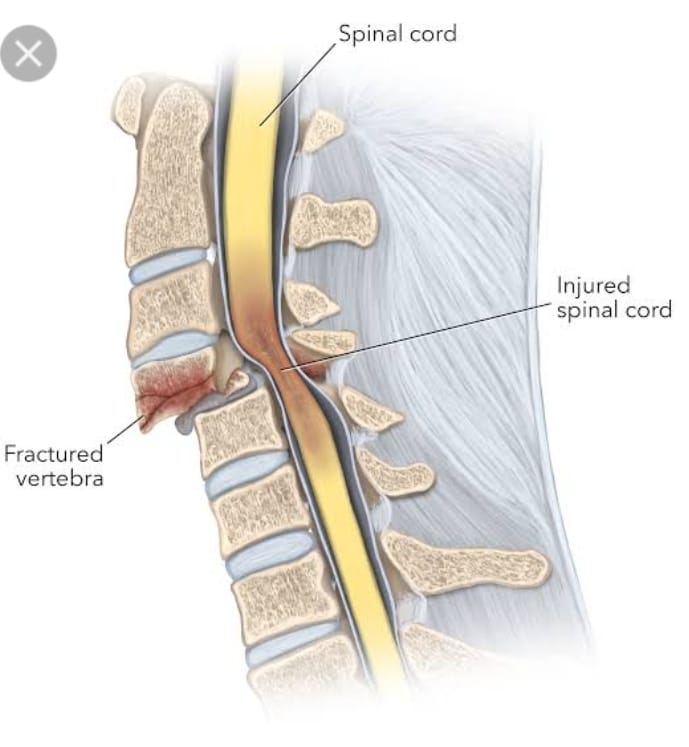
- The spinal cord is a part of the central nervous system. Which works to control the functions of the body.
- Spinal cord injury is a condition in which there is trauma to the spinal cord and the spinal cord is damaged, causing loss of sensation and reduced mobility.
- When there is a sudden injury or trauma to the spinal cord, the function of the spinal cord is temporarily and permanently changed.
- When the spinal cord is injured, the spinal cord can fracture or the vertebrae in the spinal cord can also become dislocated. This condition is called spinal cord injury.
Explain the Etiology/ cause of the spinal cord injury. (Give reasons for spinal cord injury)
- Due to trauma.
- Due to fall down.
- Due to gun shot.
- Road Traffic Accident ( R.T.A.).
- Due to infection.
- Due to inflammation in the spinal cord.
- Due to tumor in the spinal cord.
- Ex:=
Meningiomas, (Meningiomas,)
Ependymomas, (Ependymomas,)
Astrocytomas, (Astrocytomas,) - Due to falling from a great height.
- Due to electric shock.
- Due to motor vehicle accident.
- Due to ischemia.
- Due to developmental disorder.
- Due to neurodegenerative disease.
- Due to multiple sclerosis.
- Due to stroke.
- Due to inflammation.
Explain the classification of the spinal cord injury. (Explain the classification of spinal cord injury.)
A) Indicate Complete :=
- In complete spinal cord injury, motor and sensory function are not preserved and sacral segments S4 and S5 are involved.
B) indicates incomplete:
- In incomplete spinal cord injury below the neurological level, only sensory function is preserved, but motor function is not preserved, and sacral segments S4 and S5 are involved.
c) indicates Normal:
- In this, mainly sensory and motor scores are normal. In this, mainly spinal cord injury is present but motor and sensory function are normal.
Explain the Clinical manifestation/ sign and symptoms of the patient with the spinal cord injury. (Describe the symptoms and signs of spinal cord injury.)
- Paralysis.
- Loss of sensation.
- Breathing difficulty.
- Changes in bowel and bladder function.
- Limb movement loss.
- Difficulty in walking.
- Symptoms mainly depend on the injury to the spinal region.
1) Cervical ( Neck) injury:=
- Affect the Arm ,legs and middle part of the body. (Affects hands, feet and middle part of the body.)
- Breathing difficulty.
- Loss of normal bowel and bladder control.
- Numbness.
- Sensory change. (Sensory changes.)
- Spasticity (increased muscle tone). Spasticity (increased muscle tone).
2) Thoracic/ chest level / injury. (Thoracic / Chest level / Injury.)
- Loss of normal bowel and bladder control.
- Numbness. is.)
- Sensory changes occur.(Sensory changes happen.)
- Spasticity (increased muscle tone).
- weakness.(Weakness.)
- Paralysis.(Paralysis.)
3) Lumber Sacral ( Lower back injury) (Lumber Sacral ( Lower back injury)
- Loss of normal bowel and bladder control.
- Numbness.
- Pain.
- Sensory change.
- Coming to Wickness.
- becoming paralyzed.
Explain the types of the spinal cord injury. (Explain the type of spinal cord injury.)
There are two main types of spinal cord injuries. (There are two main types of spinal cord injuries.) (Is.)
- 1) Complete (Complete),
- 2) Incomplete (Incomplete)
1) Complete (Complete) Spinal cord injury is again of three types.
A) Paraplegia (Paraplegia) , Paraplegia is mainly caused by injury to T1- L5.
In it, the upper body can function fully but the impairment is mainly seen in the lower legs.
B) Hemiplegia (Hemiplegia) Hemiplegia is a half-body paralysis.
C) Quadriplegia (Quadriplegia) Quadriplegia is also called tetraplegia.
Quadriplegia There is involvement of upper two limbs and lower limbs.

2) Incomplete (Incomplete) spinal cord injury It has 3 types again.
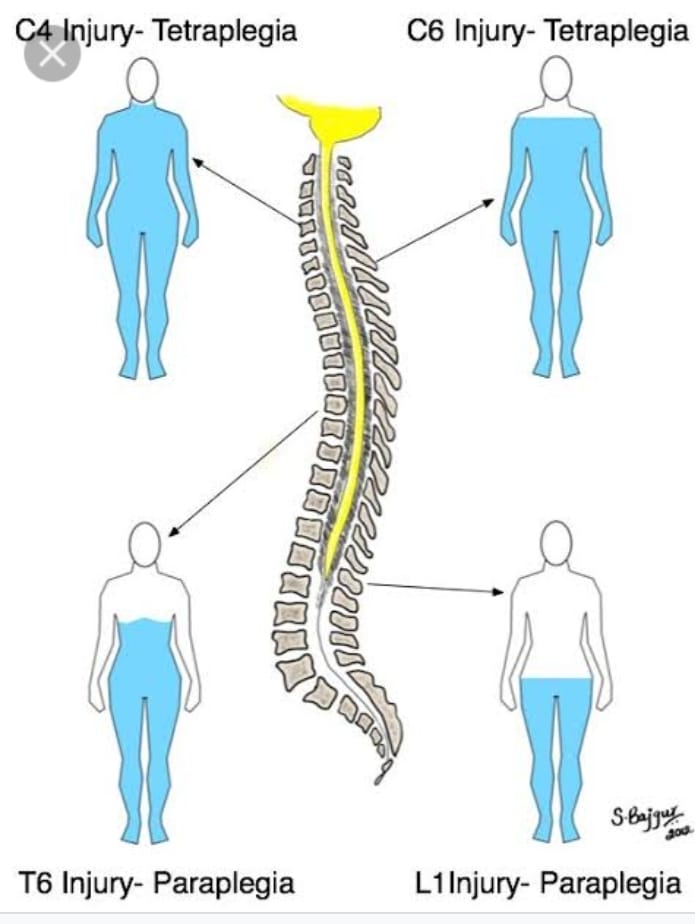
A) Central cord syndrome
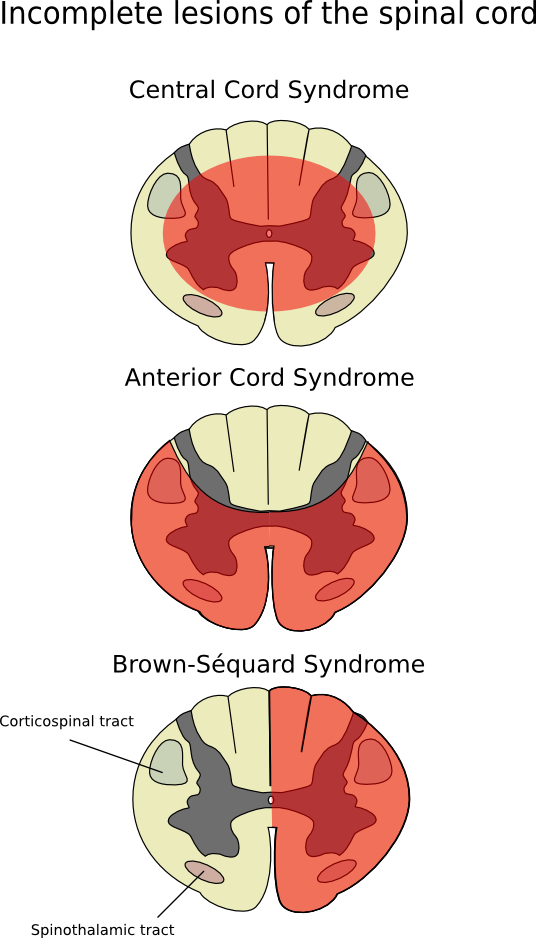
Cause := This is mainly due to injury and edema in the cervical area.
Characteristic:=
In this, motor deficit is seen in the upper extremities. Sensory loss in the upper extremities varies.
B) Anterior cord syndrome
Cause:= This is mainly caused by injury and lesion in the anterior spinal artery.
Characteristic:=
Loss of pain,
- Temperature increase .
- Impaired motor and sensory function.
- poor prognosis.
C) Broed Sequard syndrome
Cause:=
In this, the lesion is mainly due to transverse hemisection of the cord. It is mainly caused by knife, missile injury, fracture.
Characteristic:=
-
- ipsilateral paralysis. (Ipsilateral paralysis.)
-
- Contralateral loss of pain and temperature
Explain the Diagnostic evaluation of the spinal cord injury.
-
- History tacking and physical examination. (History taking and physical examination.)
-
- X ray. ( X ray.)
-
- Ct scan. (CT scan.)
-
- MRI. (MRI.)
-
- CBC ( Hb, RBC, WBC. ).
-
- Arterial blood gas Analysis. (Arterial blood gas analysis.)
-
- myelogram. (Myelogram)
-
- Urodynamic Studies. (Urodynamic Studies.)
Explain the Treatment of the Spinal Cord injury. (Write the treatment of the spinal cord injury.)
Respiratory management:=
-
- Provide adequate amount of oxygen to the patient. (Provide adequate ventilatory support to the patient.)
-
- Provide adequate ventilatory support to the patient. (Provide adequate ventilatory support to the patient.)
Pharmacological management:=
-
- Provide corticosteroid medication to the patient.
-
- Ex:= Dexamethasone, Methyl prednisolone,
Immobilization:=
-
- Provide spinal traction to the patient.
-
- Provide special bed to the patient.
-
- Properly perform surgery on the patient.
Explain the Nursing management of patients with Spinal Cord Injury
-
- Oxygenate the patient properly. (Oxygenate the patient properly.)
-
- Assess the patient’s respiratory rate and depth properly.
-
- Keeping the patient’s airway properly patent. (Keep the patient’s airway properly patent.)
-
- Advise the patient to perform range of motion exercises. (Advise the patient to do range of motion exercises.)
-
- To provide proper special bed to the patient.. (Provide proper special bed to the patient.)
-
- Properly assess the patient’s skin integrity. (Properly assess the patient’s skin integrity.)
-
- Change the patient’s position every two hours. (Change the patient’s position every two hours.)
-
- Properly assess the patient’s bowel and bladder function. (Properly assess the patient’s bowel and bladder function.)
-
- Provide adequate amount of fluid to the patient. (Provide adequate amount of fluid to the patient.)
-
- Provide the patient with a high fiber and high protein diet. (Provide the patient with a high-fiber and high-protein diet.)
Explain / Define the Paraplegia. (Define Paraplegia.)
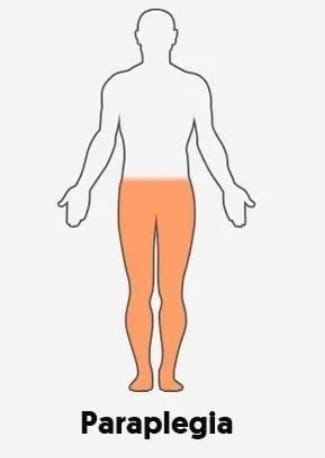
-
- Paraplegia is a condition that Mainly due to injury to the spinal cord, the motor and sensory function of the lower extremities is impaired, i.e. the lower extremities are paralyzed, due to which the lower extremities (lower legs) cannot work properly and there is difficulty in walking and running. This condition is called paraplegia.
-
- Paraplegia is mainly seen due to any impairment in the thoracic, lumbar or sacral region of the spinal cord.
Explain the Etiology/cause of the Paraplegia.
-
- Due to spinal injury.
-
- due to stroke.
-
- Due to spinal tumor.
-
- Due to brain tumor.
-
- Due to ischemia.
-
- Diabetes-related nerve damage.
-
- Due to spina bifida.
-
- Due to cerebral palsy.
-
- Due to multiple sclerosis.
-
- Falls .
-
- Accident.
-
- Due to brain infection.
Explain the Clinical manifestation/ sign and symptoms of the patient with the Paraplegia. (Describe the symptoms and signs of a patient with paraplegia.)
-
- Moment loss.
-
- Loss of sensation.
-
- Loss of bowel and bladder control.
-
- Muscle stiffness.
-
- Tingling and burning sensation. (Tingling and burning sensation.)
-
- Muscle spasms.
-
- Reflexes change.
Explain the Diagnostic evaluation of the patient with the Paraplegia.
-
- history tacking and physical examination.
-
- Neurological examination.
-
- imaging studies.
-
- X ray.
-
- Ct scan.
-
- MRI. (MRI.)
-
- Electromyography.
-
- Blood test.
Explain the medical management of the patient with the Paraplegia. (Explain the medical management of a patient with paraplegia.)
-
- Properly immobilize the patient’s spinal cord.
-
- Provide analgesic medication if the patient is in pain.
-
- Provide muscle relaxant medication to the patient.
-
- Provide physical therapy to the patient. To do.
-
- Provide the patient with an assistive device.
-
- Manage the patient’s bowel and bladder function.
-
- Advise the patient to prevent complications.
-
- Advise the patient to have regular follow-up.
Explain the Nursing management of patients with the Paraplegia.
-
- Assess the patient’s neurological status.
-
- Properly assess the patient’s skin integrity.
-
- Properly assess the patient’s bowel and bladder function.
-
- Properly assess the patient’s respiratory status.
-
- Properly assess the patient’s skin care Do.
-
- Properly assess the patient’s skin hygiene.
-
- Advise the patient to exercise properly.
-
- Advise the patient to exercise the bowel and bladder properly.
-
- Provide the patient with proper respiratory support.
- If the patient is in pain, administer analgesics. Provide medicine.
- Provide proper psychological support to the patient.
- Provide complete information to the patient about his disease, causes of the disease, its symptoms and signs and its treatment.
- Provide adequate treatment to the patient to prevent any further complications.
Explain/Define the Hemiplegia. (Define hemiplegia.)
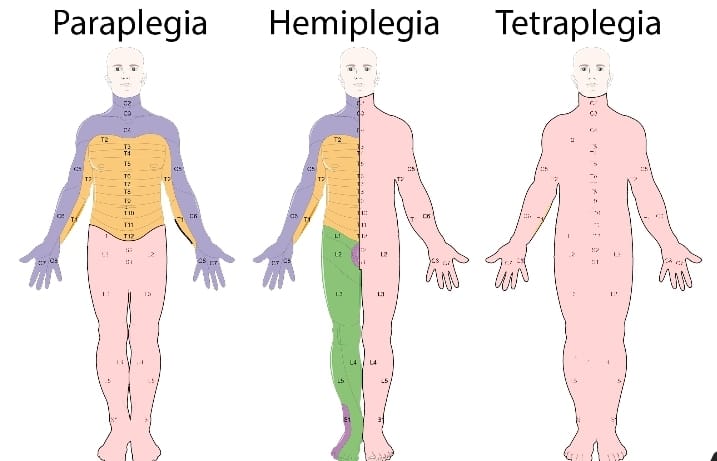
- Hemiplegia is a word derived from “Greek” Hemiplegia is a condition in which half of the body is paralyzed, either completely or partially, mainly on the right or left side of the body, due to any illness, injury, or disease in the brain or spinal cord. Hemiplegia is a condition in which half of the body is paralyzed, either completely or partially, mainly on the right or left side of the body, due to any illness, injury, or disease in the brain or spinal cord. –>
- (Hemiplagia Means:= Paralysis of the Half part of the body.)
Explain the Classification of the Hemiplegia. (Describe the classification of hemiplegia.)
There are a total of five types of hemiplegia.
-
- 1) Facial hemiplegia,
-
- 2) Spinal hemiplegia,
-
- 3) Contralateral hemiplegia,
–>
-
- 4) Spastic hemiplegia,
-
- 5) Alternating hemiplegia of childhood.
1) Facial hemiplegia,
-
- Facial means related to ” Face”
-
- In this type, paralysis occurs on one side of the facial muscles.
-
- And half of the facial muscles cannot work properly.
2) Spinal hemiplegia,
-
- Spinal hemiplegia is called Brown Sequard syndrome. In this type, if one half of the spinal cord is damaged, then one half of the body is paralyzed, it is called spinal hemiplegia.
-
- In this type, if the spinal cord is damaged on the right side, then the body on the right side becomes paralyzed and if the spinal cord is damaged on the left side, then the left body becomes paralyzed.
3) Contralateral hemiplegia,
-
- Contralateral hemiplegia means opposite side paralysis.
-
- This type of hemiplegia is mainly seen due to brain damage. In this type, if the right side of the brain is damaged, paralysis occurs in the left body and if the left brain is damaged, paralysis occurs in the right body side.
4) Spastic hemiplegia,
-
- This is a type of hemiplegia in which the muscles of half the body side become spastic and contracted for a long time.
5) Alternating Hemiplegia of Childhood.
-
- Alternating hemiplegia is mainly seen in children 18 months or older.
-
- It mainly involves more than one episode of hemiplegia that affects one side of the body. is.
Explain the Etiology / Cause of the Hemiplegia. (Give reasons for hemiplegia.)
-
- Due to brain injury.
-
- Due to cerebral hemorrhage.
-
- Stroke.
-
- Due to diabetic neuropathy.
-
- Due to brain infection.
-
- Due to meningitis.
-
- Due to encephalitis.
-
- Neoplastic (due to glioma-meningioma).
-
- Due to congenital defect.
-
- Due to injury to the spinal cord.
-
- Due to demyelinating disease.
-
- Due to brain cancer.
-
- Due to brain tumor.
-
- Due to neurological disorder.
-
- Due to psychological disorder.
Explain the Clinical manifestation/ Sign and symptoms of the patient with the Hemiplegia.
-
- Muscle weakness and paralysis.
-
- Motor function impairment.
-
- Difficulty in walking, talking, working.
-
- Changes in reflexes.
-
- Difficulty in coordination.
-
- Sensory changes.
-
- Changes in posture.
-
- Difficulty in speech and swallowing.
-
- Emotional and psychological impact.
-
- Loss of motor function.
-
- Weakness and stiffness on one side of the body.
-
- Difficulty in grasping any object.
Explain the Diagnostic evaluation of the patient with the Hemiplegia. (Describe the diagnostic evaluation of a patient with hemiplegia.)
-
- History tacking and physical examination
-
- Blood test.
-
- CT scan.
-
- MRI.
-
- Electro myography.
-
- Electroencephalography.
-
- Cerebral Angiography.
Explain the Medical management of the patient with the Hemiplegia. (Explain the medical management of a hemiplegic patient.)
-
- Properly treat the patient for the reasons due to which hemiplegia has arisen.
-
- If the patient has hemiplegia due to any infection, then provide him with antibiotic medication.Ex:= Amoxicillin, Flucloxacillin.
-
- If the patient has any viral infection, then provide him with antiviral medicine.Ex:= Acyclovir, Fumciclovir.
-
- If the patient has any coagulation disorder, then provide anticoagulant medication. Ex:= Warfarin , Heparin.
-
- If the patient has any plasmotic disorder then provide the patient with antispasmodic medicine. Ex:= Dicyclomine, Bellaclonma.
-
- Provide Chemotherapy drugs properly to the patient.
-
- Provide rehabilitation therapy properly to the patient.
-
- Provide physical therapy, occupational therapy, psychotherapy properly to the patient.
Explain the Nursing management of patients with the Hemiplegia.
-
- Provide the patient with proper orthostatic splints, casts, braces.
-
- If the patient’s muscles are overactive, provide Botox injections to the muscles.
-
- Provide the patient with a walker, wheelchair.
-
- Provide the patient with analgesic medicine for pain management.
–>
-
- Assess the patient for any other complications.
-
- Provide proper nutritional support to the patient.
-
- Provide proper psychological support to the patient.
-
- Provide proper medication to the patient.
-
- Advise the patient on proper range of motion exercises.
-
- Properly assess the patient for any side effects.
Explain/Define the Quadriplegia. (Define quadriplegia.)
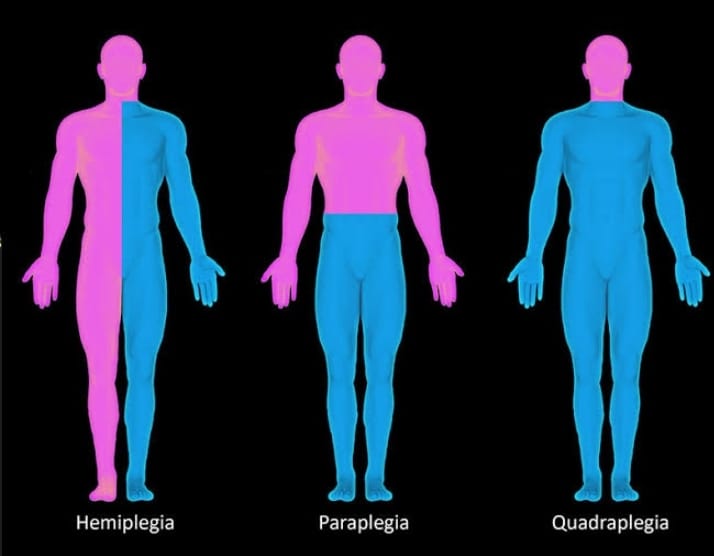
-
- Quadriplegia is also called tetraplegia Quadriplegia is a condition in which there is impairment and paralysis of motor and sensory function in four limbs, namely Upper Extremities (Hand), Lower Extremities (foot) and trunk. Quadriplegia is a condition in which there is impairment and paralysis in motor and sensory function in four limbs, namely Upper Extremities (Hand), Lower Extremities (foot) and trunk. Quadriplegia is a condition in which there is impairment and paralysis in motor and sensory function in four limbs, namely Upper Extremities (Hand), Lower Extremities (foot) and trunk. Quadriplegia is a condition in which there is impairment and paralysis in motor and sensory function in four limbs, namely Upper Extremities (Hand), Lower Extremities (Foot), and Trunk. Quadriplegia is a condition in which there is impairment and paralysis in motor and sensory function (Tell the cause of quadriplegia.)
-
-
- Due to spinal cord damage.
-
-
-
- Due to traumatic injury.
-
-
-
- Falls from the height.
-
-
-
- Due to spinal cord injury.
-
-
-
- Motor vehicle accident Due to.
-
-
-
- Due to certain types of medicine.
-
-
-
- Due to lack of blood supply.
-
-
-
- Due to neurological disorders.
-
-
-
- Due to a traumatic injury.
-
-
-
- Due to autoimmune disorders.
-
-
-
- Cerebral palsy Because of.
-
-
-
- Spinal bifida ( Spina bifida).
-
Explain the types of the Quadriplegia. (Tell the type of quadriplegia.)
There are two types of quadriplegia.
-
-
- 1) Complete Quadriplegia (Complete Quadriplegia),
-
-
-
- 2) Incomplete Quadriplegia (Incomplete Quadriplegia)
-
1) Complete Quadriplagia (Complete Quadriplegia),
-
-
- In complete quadriplegia, motor and sensory function are completely lost. And the person’s voluntary muscle control is impaired. And the person has a total loss of sensation in the lower limb and upper limb, which is called complete quadriplegia.
-
2) Incomplete Quadriplegia
- In incomplete quadriplegia, a person’s motor and sensory function are partially impaired.
- In incomplete quadriplegia, the person has limited voluntary muscle control and some sensation. A person who has a limited amount of muscle control is called incomplete quadriplegia.
Explain the Clinical manifestation/ Sign and symptoms of the patient with the Quadriplegia. (Symptoms and description of quadriplegia Vada patient.)
- Loss of motor function.
- Loss of sensory function.
- Spasticity, muscle stiffness.
- No involuntary muscle spasms.
- Muscles Reflux is impaired.
- Respiratory complications.
- Balance and coordination are impaired.
- Loss of bowel and bladder function.
- Emotional and psychological problems.
- Development of pressure ulcers.
- Muscle stiffness.
- Difficulty walking.
- Loss of bladder control.
- Tingling and numbness.
- Loss of movement.
- Loss of sensation.
- Loss of sensation.
- Autonomic dysreflexia occurs.
Explain the Diagnostic evaluation of the patient with the Quadriplegia. (Describe the diagnostic evaluation of a quadriplegia patient.)
- history taking and physical examination.
- Neurological examination.
- Imaging studies.
- X rays.
- Ct scan.
- MRI.
- Electromyography ( EMG ).
- Laboratory tests.
- Urodynamic testing.
- Autonomic function testing.
- Blood tests.
- Lumbar Puncture .
Explain the medical management of the patient with the Quadriplegia.
- Properly provide oxygen to the patient.
- Properly provide anti-inflammatory drugs to the patient.
- Properly administer cold saline to the patient accurately.
- Properly immobilize the patient.
- If the patient has any spinal cord injury Stabilize it properly.
- If the patient is in pain, provide analgesic medicine.
- If the patient has any infection, provide antibiotic medicine.
- Provide proper skin care to the patient to prevent pressure ulcers from developing.
- Provide proper nutritional support to the patient.
- Provide proper orthopedic care to the patient.
- Provide proper rehabilitation services to the patient.
- Provide proper psychological support to the patient.
Explain the Nursing management of patients with the Quadriplegia. (Explain the nursing management of a quadriplegia Vada patient.)
- Properly assess the patient.
- Properly provide skin care to the patient.
- Properly provide respiratory support to the patient.
- Properly assess the patient’s bowel and bladder function.
- Provide the patient with proper assistive devices.
- Provide the patient with analgesic medicine for pain management.
- Provide the patient with proper psychological support.
- Provide the patient with proper education.
- Advise the patient to exercise properly.
- Provide the patient with proper functioning and a comfortable environment.
Explain/ Define Meningitis.
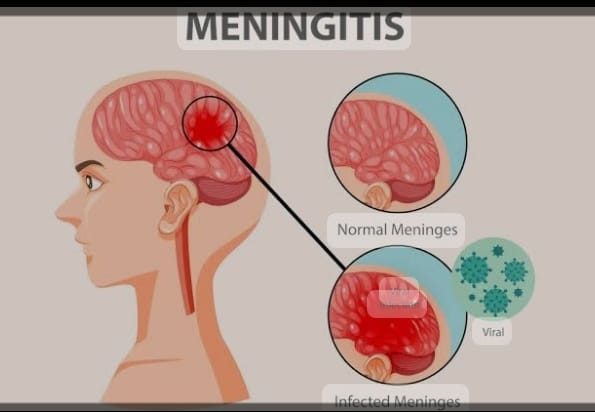
- Meninges:= Meninges are the protective membranes of the brain and spinal cord that cover the brain and spinal cord.
- These meninges have three other layers.
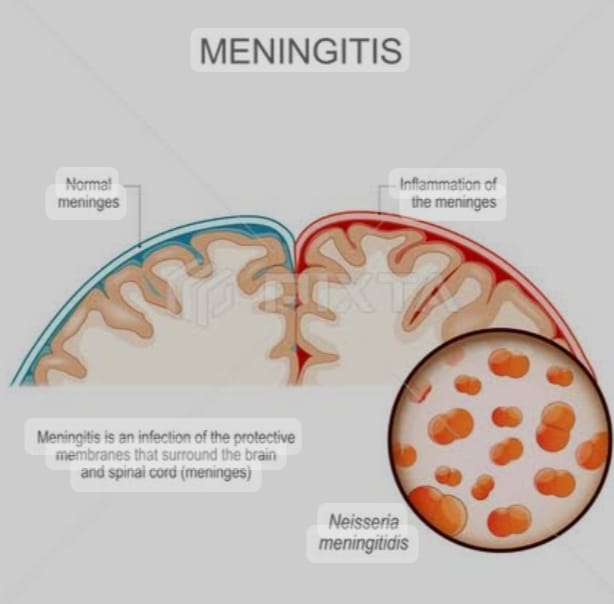
- 1) Duramater (outer most layer),
- 2) Arachnoid mater (intermidiate layer),
- 3) Pia mater (Innermost layer)
Thus, there are three layers of meninges that cover and protect the brain and spinal cord.
Meningitis:= Infection and inflammation of the meninges layer that should be cover to the brain and Spinal cord }
{ Meningitis:= infection and inflammation of the Meninges layer that should be cover to the brain and Spinal cord }
Explain the Etiology/ cause of the meningitis. (Please state the cause of meningitis.)
Due to bacterial infection.
- Ex:=
- Mycobacterium Tuberculosis,
- Streptococcus pneumoniae,
- Neisseria Meningitidis,
- Haemophilus influenzae,
- Listeria monocytogenes.
Due to viral infection.
- Mumps,
- Herpis simplex virous,
- Epstain barr virous,
- Varicella-zoster virous ,
- Measles,
- Influenza.
Caused by fungal infection.
- Candida, Systemic Lupus Erythematosus ( SLE ) Due to,
- Some types of medication.
- Head injury.
- Trauma to the head and spinal cord.
- Cancer.
- Tobacco use.
- Immune system impairment Due to.
- Due to overcrowding.
- Due to brain surgery.
Explain the Clinical manifestation/ sign and symptoms of the patient with the Meningitis. (Tell the symptoms and signs of meningitis.)

- Headache,
- Very high Fever,
- Maintenance status altered.
- Confusion.
- Consciousness altered.
- Vomiting.
- Photophobia ( An Inability to tolerate light).
- Irritability.
- Drowsiness.
- Confusion.
- Altered consciousness.
- Vomiting.
- Sign of meningeal irritation.
- Nuchal rigidity ( Neck Stiffness).
- Headache.
- Alternate mental status.
- Stun.
- Joint pain.
- Muscle ache.
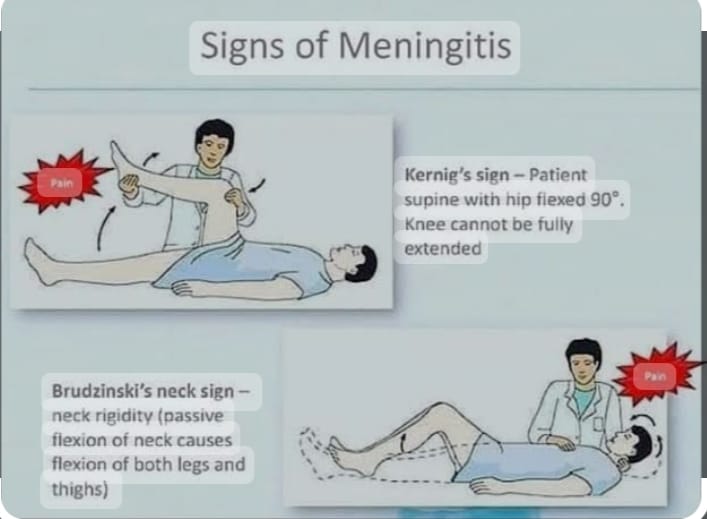
Positive Brudzinski Sign:=
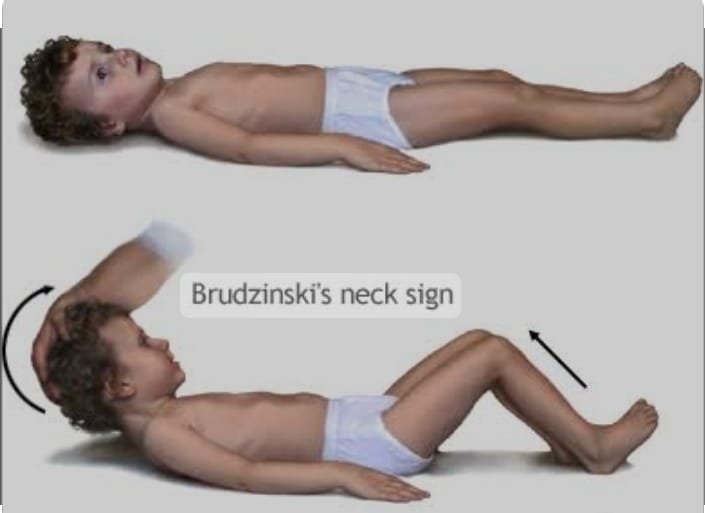
- In Brudzinski sign, when the patient is provided with a supine position and his neck is flexed towards the chest, his hip and ankle automatically flex, which is called Brudzinski sign.
Kerning sign:= ( Kerning sign)
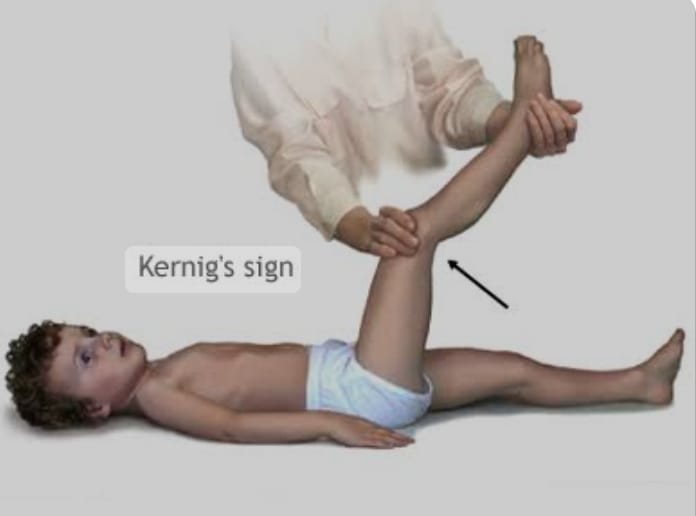
- In Kerning sign, when the patient is provided with supine position and then the patient’s knee and hip are flexed, if the patient feels pain when the knee is extended again, it is called Kerning sign.
- K:= Knee,
- E:= Extention
- R:= Resistense
- That is, the patient feels pain when the knee is directly extended.
Explain the diagnostic evaluation of the patient with the Meningitis. (Describe the diagnostic evaluation of a patient with meningitis.)
- History taking and physical examination.
- Blood culture.
- Lumbar puncture.
- Chest X-ray.
- CSF examination.
- ct scan.
- Gram stain.
- CSF culture.
- MRI test.
Explain the Management of the patient with the Meningitis. (Explain the Management of the patient with Meningitis.)
- Provide antibiotic medicine if the patient has any bacterial infection. Ex:= Rifampicin, Cefotaxime, Vancomycin.
- If the patient has any viral infection, then provide antiviral medicine.
- If the patient is in pain, then provide analgesic medicine. Ex:= Acetaminophen, NSAID ( Non steroidal anti inflammatory drug).
- Provide intravenous fluid to the patient.
- If the patient has a fever, give antipyretic medicine.
- If the patient has a fever, give anticonvulsant medication.
- The patient Continuous close monitoring.
- Continuous close monitoring of the patient’s vital signs.
- Provide corticosteroid medicine if the patient is experiencing inflammation.
- If the patient has a condition of meningitis, keep him properly isolated.
- Properly monitor the patient’s hydration status.
- Provide proper nutritional support to the patient.
- Provide proper intravenous fluids to the patient.
Explain the Nursing management of patients with the Meningitis. Explain the nursing management of a patient with meningitis.
- Properly assess the patient.
- Continuously monitor the patient’s vital signs.
- Properly assess the patient’s hydration status.
- Maintain the patient’s fluid and electrolyte levels properly.
- Provide analgesic medicine if the patient is in pain.
- Properly assess the patient’s neurological status.
- Provide anticonvulsant medicine if the patient is having seizures.
- Provide proper nutritional support to the patient.
- Provide proper psychological support to the patient.
- Provide proper education to the patient about his/her disease, its causes, and its symptoms and signs.
- Continuously monitor the patient’s intake output.
- Continuously monitor the patient’s vital signs and neurological status.
- Continuously monitor the patient’s level of consciousness.
- The patient Advise the patient to take medicine regularly.
- Advise the patient to take regular follow-up.
- Provide proper psychological support to the patient.
Define/Explain Encephalitis. (Define encephalitis.)
- When there is infection and inflammation in the brain, it The condition is called encephalitis. Encephalitis is a condition that causes infection and inflammation in the white and gray matter of the brain and mainly affects the cerebrum, brain stem and cerebellum.
- Encephalitis is caused by any viral infection, bacterial infection and allergic condition.
- The condition of encephalitis is mainly seen in young and old age people.
Explain the Etiology/cause of the patient with the Encephalitis. (Give reasons for encephalitis.)
Due to bacteria.
- Ex:=Mycobacterium Tuberculosis , Streptococcus,
- Due to viral infection.
- Ex:= Herpes Simplex Virus,
- Ex:= Herpes Simplex Virus,
- Epstein Barr virus,
- Varicella-zoster virus,
- Enteroviruses (polio virus and coxsackie virus),
- Arabovirus,
- Arthropod-borne virus,
- Tick-borne virus,
- mumps,Measles and rubella ( MMR )
- Rabies viral .
Due to parasitic infection.
- Ex:= Roundworm, Cysticercosis, Toxoplasmosis.
- Due to weakened immune system.
- Due to fungal infection.
- Ex:= Aspergillus Species, Cryptococcus neoformans,
- Due to autoimmune diseases,
- Due to any allergic conditions.
Explain the types of the Encephalitis . (Tell the type of encephalitis.)
- There are a total of six types of encephalitis.
1) Infectious encephalitis,
2) Postinfectious encephalitis,
3) Autoimmune encephalitis,
4) Japanese encephalitis,
5) Allergic encephalitis,
6) Chronic encephalitis
- A) Subacute sclerosing panencephalitis
- B) Progressive multifocal leukodystrophy ( PML )
1) Infectious encephalitis,
- Infectious encephalitis is caused by any type of infection. The condition of infectious encephalitis arises due to microorganisms such as bacteria, viruses, fungi, parasites, etc.
2) Postinfectious encephalitis,
- Postinfectious encephalitis is the condition of infectious encephalitis that arises after a period of two to three weeks after the initial infection. Postinfectious encephalitis is any viral infection. It is also seen as a complication of vaccination of infection.
3) Autoimmune encephalitis,
- In autoimmune encephalitis, if our body’s immune system itself damages our brain, it is called autoimmune encephalitis. In this condition, our body’s antibodies cross the blood-brain barrier and then damage the brain tissue and cause encephalitis. It is called autoimmune encephalitis.
4) Japanese encephalitis,
- Japanese encephalitis is mainly spread by mosquitoes. This condition is mainly seen in south, east, Asia, the far east and the Pacific islands. And this condition is more common in people who do farming.
5) Allergic encephalitis ,
- Allergic encephalitis is mainly caused by any allergic reaction.
6) Chronic Encephalitis
- Chronic encephalitis develops slowly and gradually over several months. If the condition of encephalitis is present for a long period of time, it is called chronic encephalitis.
- The condition of chronic encephalitis is mainly seen in patients with HIV when their immunity is down.
- There are two other types of chronic encephalitis.
A) Subacute sclerosing panencephalitis
Subacute sclerosing panencephalitis inflammation is seen as a complication of measles infection.
B) Progressive multifocal leukodystrophy ( PML )
Progressive multifocal leukodystrophy ( PML ) is mainly seen due to inflammation of john Cunningham virous ( JC virous ) ( John Cunningham virus ).
Explain the Clinical manifestation/ sign and symptoms of the patient with the Encephalitis. (Tell the symptoms and signs of a patient with encephalitis.)
- Fever,
- Headache,
- Confusion and altered mental status,
- Stunting,
- Neurological deficit.
- Behavioral changes.
- Nausea and vomiting.
- Stiff neck.
- Photophobia ( Sensitivity to bright lights).
- Hallucinations ( Falls Sensory Perception ).
- Speech and language difficulties.
- Motor disturbances.
- Body pain.
- Seizures.
- Aphasia ( Inability in Speaking).
- Aphagia ( Inability in Swallowing).
- Disorientation.
- Joint pain.
- Loss of sensation in some parts of the body.
- Changes in personality and behavior.
- Muscle weakness.
- Vision may be partially or totally lost.
- Eye movement may be lost.
- Involuntary loss of face, arm, and legs.
- Anxiety.
- Unusual behavior may occur.
- Delusion:= believing things that are obviously untrue.
Explain the Diagnostic evaluation of the patient with the Encephalitis. (Explain the diagnostic evaluation of the patient with Encephalitis.)
- History taking and physical examination.
- Brain MRI.
- CT scan.
- Brain biopsy.
- Culture of the Cerebro spinal fluid ( CSF ).
- Serology test.
- Lumber puncture.
- CSF Examination.
- PCR Test (Polymerase Chain Reaction).
Explain the medical management of the patient with the Encephalitis. (Describe the medical management of a patient with encephalitis.)
- Provide proper supportive care to the patient.
- Advise the patient to take proper rest.
- Advise the patient to take proper nutrition.
- Advise the patient to take proper fluids.
- If the patient has a viral infection, then give antiviral medicine. Ex:=Acyclovir ( Zovirax) , Foscavir (foscarnet).
- Provide the patient with proper anti-inflammatory drugs. Ex:= Acetaminophen, Ibuprofen, Naproxen.
- If the patient has a bacterial infection, then give antibiotic medicine to the patient.
- If the patient has any parasitic infection, then give antiparasitic medicine.
- If the patient has a seizure condition, provide anticonvulsant medicine.
- Provide proper supportive care to the patient.
- Provide analgesic medicine if the patient has any pain condition.
- Monitor the neurological status of the patient.
- Monitor the mental status and level of consciousness of the patient.
- Provide proper rehabilitation services to the patient.
- Provide proper psychological support to the patient.
- Provide proper oxygen to the patient.
- Provide proper intravenous fluids to the patient.
Explain the Nursing management of patients with the Encephalitis. (Explain the nursing management of a patient with encephalitis.)
- Properly provide comprehensive care to the patient.
- Properly assess the patient.
- Properly assess the patient’s neurological status, mental status and level of consciousness.
- Properly assess the patient’s vital signs.
- Continuously monitor the patient’s fluid and electrolyte levels.
- Continuously monitor the patient’s electrolyte levels.
- If the patient has a seizure condition, provide anticonvulsant medicine.
- If the patient has a viral infection, provide antiviral medicine.
- If the patient has any bacterial infection, provide antibiotic medicine.
- If the patient has any fungal infection, provide antifungal medicine.
- If the patient has any parasitic infection, provide antiparasitic medicine.
- Provide proper respiratory support to the patient.
- Provide proper nutritional support to the patient.
- Maintain proper hydration status of the patient.
- Assess the patient properly if any complication occurs.
- Provide proper education to the patient and his family members.
- Provide emotional support to the patient.
- Monitor the patient’s vital signs frequently.
- Monitor the patient’s intake output chart properly.
- Monitor the patient’s vital signs properly.
- Monitor the patient’s neurological status closely.
- Keep the patient’s airway properly patent.
- Provide the patient with a calm and comfortable environment.
- Keep the patient away from noisy environments.
- Monitor the patient’s skin integrity properly.
- Advise the patient to do proper range of motion exercises.
- Provide the patient with proper standard precautions and isolation.
- Provide the patient with proper antipyretic medication.
- Provide the patient with proper psychological support.
- Advise the patient to take proper medication.
- Advise the patient to follow up regularly.
Define/ Explain Brain Abscess.
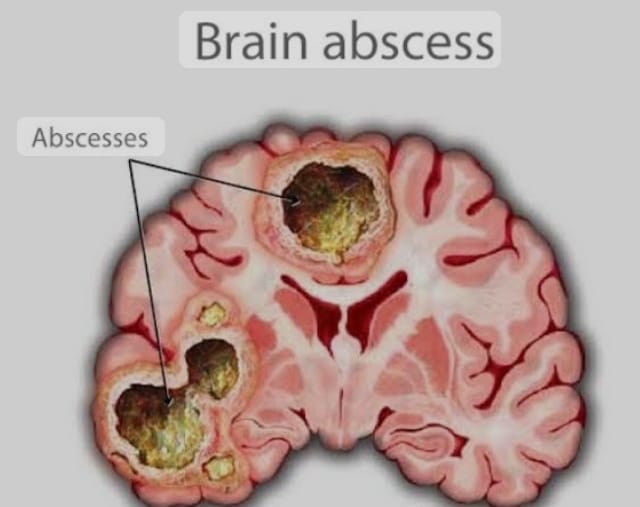
- A brain abscess is a bacterial brain infection. It is also called a cerebral abscess. In this condition, bacteria reach the brain. The bacteria then create an infection in the brain.
- When an infection occurs in the brain and the body responds to it, inflammation occurs in the brain. Due to this inflammation, pus forms in the brain. This condition is called a brain abscess.
- Infection occurs due to any bacterial or other microorganism in the brain tissue. Due to this infection, inflammation occurs in the brain. Due to this inflammation, pus forms in the brain. Due to this pus formation, the pus converts into an abscess and the condition of brain abscess arises. है.
Explain the Etiology/ cause of the patient with the Brain Abscess.
- Explain the cause of the brain abscess.
- Due to bacterial infection.
- Due to fungal infection.
- Caused by parasitic infection.
- Caused by direct trauma and injury.
- Caused by blood stream infection.
- Caused by compromised immune system.
- Caused by ear infection.
- Caused by dental abscess.
- Infection of the paranasal sinuses.
- Infection of the lungs, heart and kidneys.
- Penetrating injury.
- Chronic disease.
- Taking immune system suppressive drugs.
- Any fungal infection Because of.
Explain the clinical manifestation/sign and symptoms of the patient with the brain abscess. (Describe the symptoms and signs of a patient with brain abscess.)
- Headache,
- Fever,
- Neurological impairment.
- Altered mental status.
- Nausea and vomiting.
- Seizure.
- Visual disturbances.
- Difficulty in speaking.
- Difficulty in swallowing.
- Personality changes.
- Increased intracranial pressure in the skull.
- If the abscess occurs in the cerebellum, the person loses balance. is.
- If the abscess occurs in the frontal lobe of the brain, memory loss occurs, attention span is shortened, and speech disorders occur.
- If the abscess occurs in the temporal lobe, vision is partially lost.
- Confusion occurs.
- Seizures occur.
- Irritability occurs.
- Drowsiness.
- Loss of sensation.
- Loss of coordination.
- Decreased movement.
- Language difficulties.
- Weakness.
- Loss of muscle function.
- Stiff neck.
Explain the diagnostic evaluation of the patient with the brain abscess. (Describe the diagnostic evaluation of a patient with brain abscess.)
- history taking and physical examination.
- ct scan.
- MRI.
- Blood culture.
- Chest and Skull x rays.
- Complete Blood Count.
- Electroencephalogram ( EEG ),
- Needle Biopsy,
- Lumbar Puncture,
Explain the medical management of the patient with the Brain Abscess. (Explain the medical management of a patient with brain abscess.)
- Properly provide antibiotic medicine to the patient. Ex:= Penicillin, Metronidazole .
- Provide corticosteroid medicine to the patient properly.
- If the patient is in pain, provide analgesic medicine.
- If the patient has fever, provide antipyretic medicine.
- If the patient has seizures If necessary, provide antiepileptic medicine.
- Continuously monitor the patient’s vital signs.
- Properly assess the patient’s neurological status.
Explain the Surgical management of patients with the Brain Abscess. (Explain the Surgical Management of Patients with Brain Abscess.)
- In the case of brain abscess, the abscess is surgically drained.
- The abscess is properly aspirated.
- The brain abscess is surgically opened and the infectious material is removed.
- The brain abscess is removed using CT scan and MRI.
Explain the Nursing management of patients with the Brain Abscess. (Explain the nursing management of a patient with brain abscess.)
- Properly assess the patient’s neurological status.
- Properly assess the patient’s vital signs.
- Properly assess the patient’s pupillary response and motor response.
- Inspect the patient for any signs and symptoms of increased intracranial pressure such as Assess for headache, altered mental status, and any changes in vital signs.
- Monitor the patient’s vital signs regularly.
- Provide analgesic medicine if the patient is in pain.
- Provide antiepileptic medicine if the patient is having seizures.
- Provide antibiotic medicine if the patient has any infection.
- Properly assess the patient’s fluid and electrolyte levels.
- Provide proper nutritional support to the patient.
- Provide proper psychological support to the patient.
- Provide complete information to the patient about their disease, its causes, its symptoms and signs, and its treatment.
- Provide the patient with any other Assess whether there are complications.
- Advise the patient to take regular medication.
- Advise the patient to take proper follow-up.
- Provide the patient with proper work and a comfortable environment.
- Advise the patient to take regular follow-up
Define/Explain Multiple Sclerosis. (Define Multiple Sclerosis.)
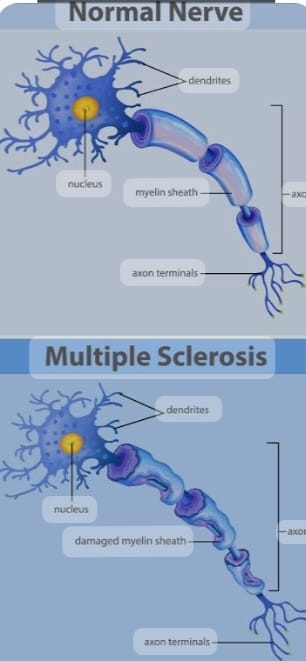
- Multiple Sclerosis The abbreviation is also called MS. Multiple sclerosis is a type of autoimmune disease in which the myelin sheath over the neurons of the brain and spinal cord is degenerative, demyelinating, scarring and its destruction.
- Due to this, neurons cannot function properly, due to which electrical impulses are not transmitted properly and body functions are impaired.
- In multiple sclerosis, neurological symptoms are also seen due to destruction of the myelin sheath. Symptoms such as fatigue, weakness, numbness and tingling sensation, impairment in balance and coordination are seen.
- This disease is mainly seen in young adults and more in females.
Explain the Etiology/ cause of the Multiple sclerosis. (Explain the cause of Multiple Sclerosis.)
- Due to genetic factors.
- Due to environmental factors.
- Due to viral infections.
- Due to low vitamin D.
- Due to smoking.
- Due to genetic and environmental factors.
- Due to a history of the disease in family members.
- Due to smoking.
- Environmental exposure to pollution, toxins,
Explain the types of the Multiple sclerosis. (Tell the types of multiple sclerosis.)
There are a total of four types of multiple sclerosis.
- 1) Relapsing Remitting Multiple Sclerosis; (RRMS) ,
- 2) Primary Progressive Multiple Sclerosis (PPMS),
- 3) Secondary Progressive Multiple Sclerosis (SPMS),
- 4) Progressive Relapsing Multiple Sclerosis (PRMS).
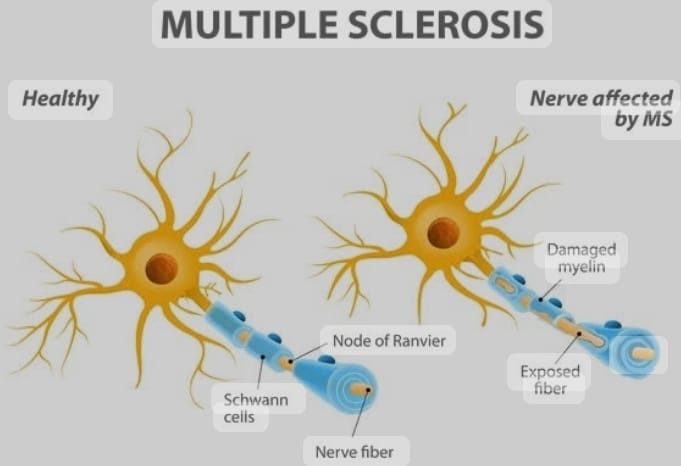
1) Relapsing Remitting Multiple Sclerosis; ( RRMS) ,
- Relapsing remitting multiple sclerosis is the most common form of multiple sclerosis. In this type, a person gets multiple sclerosis, then recovers and the person experiences attacks of multiple sclerosis again.
2) Primary Progressive Multiple Sclerosis (PPMS),
- In primary progressive multiple sclerosis, after a person gets the disease, there is continuous progression of the disease. This type of multiple sclerosis is mainly seen after 40 years.
3) Secondary Progressive Multiple Sclerosis ( SPMS ),
- In this type, initially there will be Relapsing-Remitting Attacks. But after two to three attacks, the disease starts to progress continuously. If the patient does not receive proper treatment for relapsing remitting multiple sclerosis, it can be transmitted to secondary progressive multiple sclerosis.
4) Progressive Relapsing Multiple Sclerosis (PRMS).
- Progressive relapsing multiple sclerosis is characterized by continuous progression after its onset.
Explain the Clinical manifestation/ sign and symptoms of the patient with the Multiple Sclerosis .
- Numbness and tingling sensation.
- Burning sensation.
- Weakness and paralysis.
- Muscle stiffness and spasticity.
- Tremor and involuntary muscle movements.
- Visual disturbances.
- Blurred vision.
- Loss of color vision.
- Double vision (Diplopia).
- Difficulty in balance and coordination (Ataxia).
- Dizziness.
- Fatigue
- Impairment in concentration.
- Changes in mood.
- Bowel and bladder dysfunction.
- Sexual dysfunction.
- Pain and sensory disturbances.
- difficulty in speech and Swallowing.
- Involuntary eye movements.
- Mood alterations.
- Weakness and numbness in one or both extremities.
Explain the Diagnostic evaluation of the patient with the Multiple Sclerosis. (Describe the diagnostic evaluation of a patient with multiple sclerosis.)
- History tacking and physical examination.
- history tacking and physical examination.
- Ct scan.
- M.R.I.
- PET test.
- C.S.F.Analysis.
- Neuro psychological testing.
- Evoked potential.
- Neurological studies.
- Blood tests.
Explain the medical management of the patient with the Multiple Sclerosis . (Write the medical management of the patient with the Multiple Sclerosis.)
Disease modifying therapy.
- Disease modifying therapy is the main treatment for relapsing remitting multiple sclerosis and secondary progressive multiple sclerosis.
- These medications reduce inflammation, suppress the disease, and prevent the disease from relapsing.
- Ex:=
- Interferan beta,
- Glatirmate Acitate,
- Dimythyle fumarate,
- Fingolimod,
- Teriflunomide,
- Ocrelizumab.etc.
- Provide proper symptomatic treatment to the patient.
- Provide physical therapy and occupational therapy to the patient.
- Provide antispasmodic medicine to the patient if the patient has muscle stiffness.
- Provide antidepressant medicine if the patient has a condition of depression.
- Provide anticholinergic medicine to the patient.
- Provide proper physical therapy and speech therapy to the patient.
- Properly provide corticosteroid medicine if the patient has an inflammatory condition.
- Properly monitor the patient.
- Properly provide rehabilitation to the patient. To do.
- Advise the patient to adopt healthy lifestyle habits.
- Advise the patient to take regular exercise, a balanced diet, adequate sleep, and to reduce stress.
- Advise the patient to avoid smoking and alcohol.
- Provide proper bowel and bladder training to the patient.
Explain the Nursing management of patients with the Multiple Sclerosis. (Explain the nursing management of a multiple sclerosis patient.)
- Properly assess the patient.
- Properly assess the patient’s physical, psychological, neurological, and cognitive status.
- Properly assess the patient’s symptoms.
- Properly administer medication to the patient. Advise the patient to exercise properly.
- Provide proper psychological support to the patient.
- Advise the patient to exercise properly.
- Advise the patient to take proper rest.
- Provide proper muscle relaxant medicine to the patient.
- Advise the patient to exercise frequently to Advise the patient to change positions.
- Advise the patient to maintain proper aseptic technique.
- Advise the patient to provide proper skin care.
- Provide proper corticosteroids medicine to reduce edema and inflammation in the patient’s body.
- Advise the patient to make proper lifestyle modifications.
- Advise the patient to take proper follow-up.
- Advise the patient to take proper medication.
- Provide the patient with a properly calm and conformable environment.
Define/Explain Myasthenia Gravis . (Define Myasthenia Gravis.)
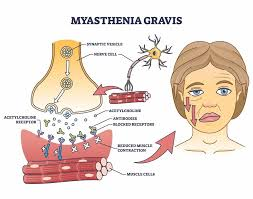
- Myasthenia Gravis is a compound word.
- Mys:= Muscles ,
Aisthesis:= Sensation. - Myasthenia Gravis is a chronic autoimmune disorder. MG (Myesthenia Gravis) disease mainly affects the neuromuscular junction and in Myesthenia Gravis, the chronic progressive neuromuscular junction gets damaged and the muscles get weak.
- In Myasthenia Gravis, an inappropriate antibody is produced in the patient’s body and this antibody is Ach receptor (Acetylecoline) receptor) and this antibody blocks the Ach Receptor and due to this the number of Ach receptors decreases and its function also gets impaired. And the nerve impulses cannot be transmitted properly and the muscles of the body become weak and the voluntary muscle control of the body gets impaired. And due to this, weakness and fatigue occur in the muscles.
Explain the Etiology/ Cause of the patient with the Myasthenia Gravis. (Tell the cause of myasthenia gravis in patients.)
- The exact cause of myasthenia gravis is unknown.
- Due to a tumor in the thymus gland.
- Due to an abnormality of the thyroid gland.
- Autoimmune attack: = thyrotoxicosis, rheumatoid arthritis,
- Systemetic Lupus erythematosus,
- Myesthenia Crisis,
- Due to Acetylecoline Deficiency.
- Due to Abnormalities in Thyroid Gland.
- Due to Environmental Factors.
- Due to Genetic Factors.
Explain the clinical manifestation/sign and symptoms of the patient with the Myesthenia Gravis.
- Muscle weakness,
- Ptosis ( Drooping of the eye lids),
- Diplopia ( Double vision ),
- Facial muscle weakness.
- Mask – like facial expressions.
- Voice changes to happen.
- Arm,Hands,
- Weakness in fingers, legs and neck.
- Dysphagia (difficulty in swallowing),
- Dysarthia (Weakness in the muscles of the mouth and throat can cause Slurred Speech),
- Feel tired,
- Respiratory impairment.
- Facial weakness.
- Weakness in the extremities.
- Breathing difficulty.
- Swallowing difficulty.
- Talking difficulty.
- Speech becomes impaired.
- Shortness of breath.
- Double vision.
- Weakness in legs and hands.
- Facial paralysis.

Explain the diagnostic evaluation of the patient with the Myasthenia Gravis. (Describe the diagnostic evaluation of a patient with myasthenia gravis.)
- History tacking and physical examination.
- Ct scan.
- MRI.
- Repetitive nerve Stimulation.
- Single fiber electromyography
- ( EMG).
- Pulmonary function test.
- Endophonium test.
- Neurological examination.
Explain the medical management of the patient with the Myasthenia Gravis. (Describe the medical management of a patient with myasthenia gravis.)
1) Cholinesterase inhibitor:=
Ex:= pyridostigmine
is the first-line treatment for myasthenia gravis.
This medicine prevents the breakdown of acetylcholine, which increases muscle concentration and neuromuscular transmission.
2) Immuno suppressive therapy:=
Individuals with moderate to severe MG who do not respond to cholinesterase inhibitor medications should be given immunosuppressive medications.
Ex:=
corticosteroids, (corticosteroids)
Azathioprine, (azathioprine,)
Methotrexate, (methotrexate,)
Mycophenolate mofetil. (Mycophenolate mofetil.)
3) Monoclonal antibody:=
Properly provide monoclonal antibody to the patient.
4) Intravenous immunoglobulin and plasma exchange ( Plasmaphresis )
This medicine decreases the circulating antibodies in acute exacerbations or myasthenia gravis.
5) Thymectomy:=
In this, the thymus gland is removed.
6) Supportive therapy:=
Provide proper supportive therapy to the patient To do.
7) Regular Monitoring:
Monitor the patient regularly.
8) Lifestyle monitor:
Give advice to the patient to make proper lifestyle modifications.
Explain the Nursing management of patients with the Myesthenia Gravis. (Explain the nursing management of a patient with myasthenia gravis.)
-
- Properly assess the patient.
-
- Properly assess the patient’s neurological status.
-
- Properly provide respiratory support to the patient.
-
- Advise the patient to do physical activity properly.
-
- Provide proper nutritional support to the patient.
-
- Provide proper psychological support to the patient.
-
- Keep the patient’s airway properly patent.
-
- Properly assess the patient’s fluid and electrolyte levels.
-
- Provide proper nutritional support to the patient.
-
- Provide proper psychological support to the patient.
-
- Provide proper calm and comfortable environment to the patient.
Explain/ Define Guillain Barre Syndrome. Explain/Define Guillain Barre Syndrome.
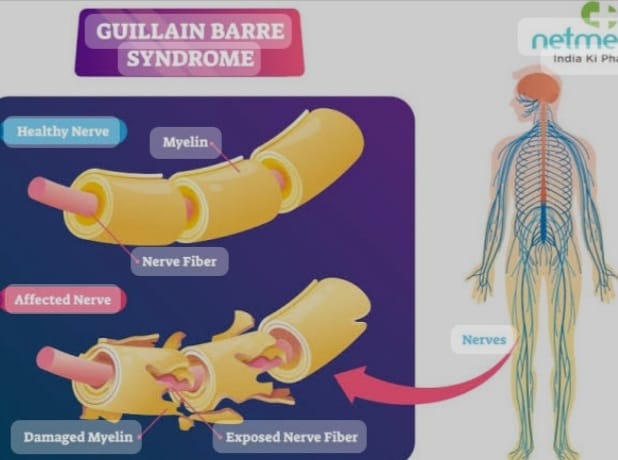
-
- Guillain Barre Syndrome is named after George’s Guillian, Jan Alexander Bare And Strohl. Guillain Barre Syndrome was first described in 1916.
-
- Guillain Barre Syndrome is an acute Also called inflammatory polyneuropathy or polyradiculoneuritis.
-
- Guillain Barre Syndrome is also called G.B. Syndrome.
-
- Guillain Barre Syndrome affects the peripheral nervous system (which affects the cranial nerves and spinal nerves.)
-
- Guillain Barre Syndrome is an autoimmune disorder. It is a disorder in which the body’s immune system affects the peripheral nervous system and spinal nerves.
-
- In this condition, the swan cell is damaged. Due to the damage to the swan cell, the neuron is demyelinated, damaged and destroyed, due to which the transmission of the nerve is disturbed and the transmission of nerve impulses cannot take place. Therefore, the nerve impulses cannot be transmitted between one neuron and another. So this is called Guillain Barre Syndrome disease.
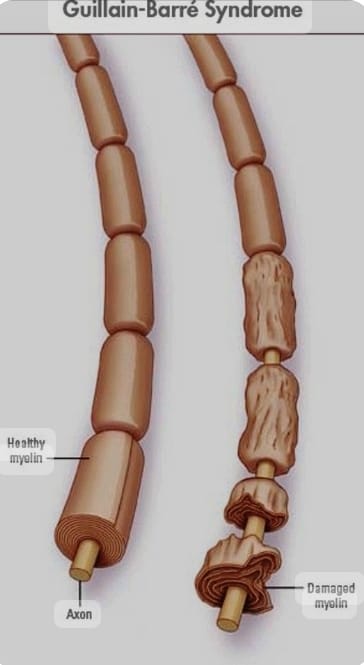
Explain the Etiology/ Cause of the Guillian Barr Syndrome. (Give the cause of Guillain-Barré syndrome.)
- Exact causes are unknown.
- Lung infection and gastrointestinal infection.
- Campylobacterium jejuni.
- Cytomegalovirus.
- Due to the Epstein Barr virus.
- Zika virus.
- Due to swine flu infection.
- Due to general surgery and epidural anesthesia.
- Due to certain types of autoimmune diseases.
- Due to certain types of medications like:= Thrombolytic and immunosuppressive.
Explain the Classification of the patient with the Guillian bare syndrome. Explain the classification of Guillain Barre syndrome.
There are 6 classifications of Guillain Barre syndrome.
- 1) Acute Inflammatory Demyelinating Polyneuropathy (AIDP),
- 2)Miller Fisher Syndrome ( MFS ),
- 3) Acute Motor Axonal Neuropathy ( AMAN ),
- 4) Acute Motor Sensory Axonal Neuropathy ( AMSAN ),
- 5) Acute Panautonomic Neuropathy ( APN ),
- 6) Bickerstaff Brainstem Encephalitis ( BBE ).
1)Acute inflammatory demyelinating polyneuropathy (AIDP),
- This acute inflammatory demyelinating polyneuropathy is the most common form and subtype of Guillain-Barré syndrome. This is mainly due to the autoimmune response, which is mainly directed against the dog’s own cells.
2)Miller Fisher Syndrome (MFS),
- Miller Fisher Syndrome is a rare variant of Guillain-Barré Syndrome. In this, descending paralysis mainly occurs. It mainly affects the eye muscles first. And the Triad such as, Opthelmoplagia, Ataxia (Loss of the Muscles Control), and Areflexia (Absence of the deep tendon Reflexes) is seen. In this type, Anti – GQ1b antibodies are found in 90% of cases.
3) Acute motor axonal neuropathy (AMAN), (Acute motor axonal neuropathy (AMAN),
- In this type, the motor nodes of Ranvier It is mainly an autoimmune response that occurs directly in the exoplasm of the peripheral nerve. This type is seasonal and recovery is also rapid, in this case Anti-GD3 antibodies are not seen.
4) Acute Motor Sensory Axonal Neuropathy (AMSAN)
- This is similar to AMAN But there is severe axonal damage to the sensory nerve as well. This type responds directly to the peripheral nerve, just like AMAN. Recovery is slow and incomplete.
5) Acute Pantonomic Neuropathy (APN), (Acute Pantonomic Neuropathy ( APN ),
- This is a rare variant type of GBS. It also involves encephalopathy. This type has a high mortality rate due to cardiovascular involvement.
- This patient has impaired sweating, lack of tear formation, photophobia, dryness of nasal mucosa, itching or peeling Symptoms like Skin, Nausea, Dysphagia, constipation, Lethargy, Fatigue, are seen.
6) Bickerstaff brainstem encephalitis (BBE).
- This is a further variant of Guillain-Barré Syndrome.
- This mainly Ophthalmoplegia, ataxia, consciousness disturbance, hyperreflexia, and Babinski sign are seen. BBE is a severe initial presentation and its prognosis is good.
Explain the Clinical manifestation/ sign and symptoms of the patient with the Guillian bare syndrome.
- Weakness in the muscles.
- Tingling and numbness.
- Areflexia ( Deminised and Absense of the deep tendon Reflexes).
- Pain.
- Blood pressure fluctuation.
- Heart rate abnormality.
- Sweating disturbance Occur.
- Bowel and bladder function disturbances.
- Respiratory function impairment.
- Difficulty in swallowing (Dysphagia).
- Facial weakness.
- Double vision (Diplopia).
- Difficulty in speaking (Dysarthia).
- Progressive muscle weakness in both arms, legs, and face.
- Reflexes in the lower extremities are diminished.
- Tingling sensation in the arms and legs.
- Standingness and muscle pain.
- An uncoordinated moment.
- Muscle spasms.
- Palpitations.
- Changes in heart rate.
- Cardiac arrhythmias.
- Difficulty with eye movement, facial movement, speaking, chewing, and swallowing.
Explain the Diagnostic evaluation of the patient with the Guillian bare syndrome.
- History tacking and physical examination. (History taking and physical examination)
- Laboratory test . (Blood test.)
- Cytomegalo virus test (CMV), (Cytomegalo virus test ( CMV),
- Epstein Barr Virus (EBV) Test, (Epstein Barr Virus ( EBV) Test,)
- Cerebro spinal fluid analysis,
- Electro Physiological Test,
- Electro Physiological Test,
- Electromyography (EMG),
- Imaging studies. (MRI test.)
- Autoimmune function test.
- Pulmonary function test (PFT test).
- Nerve conduction velocity test.
Explain the medical management of the patient with the Guillian bare syndrome. (Explain the medical management of the Guillain Barre syndrome.)
- Provide proper supportive care to the patient.
- Properly monitor the patient closely.
- Properly support the patient. Provide care.
- Properly monitor the patient’s vitals.
- Properly provide respiratory support to the patient.
- Provide intravenous immunoglobulin to the patient.
- Properly perform Plasmaphresis (in this process, plasma is removed from the patient’s body, its antibodies are removed, and then the plasma is replaced back into the patient’s body.) is.
- Provide proper mechanical ventilation to the patient.
- Provide analgesia if the patient is in pain.
- Provide proper therapy and rehabilitation therapy to the patient.
- Provide proper nutritional support to the patient.
- Provide proper psychological Provide support.
Explain the Nursing management of patients with the Guillian bare syndrome. (Explain the Nursing Management of Guillain Barre Syndrome.)
- Provide proper respiratory support to the patient.
- Properly assess the patient.
- Properly assess the patient’s vital signs.
- Properly provide respiratory support to the patient.
- Advise the patient to perform proper range of motion exercises.
- Provide proper nutritional support to the patient.
- Properly manage the patient’s pain.
- Provide proper psychological support to the patient.
- Provide proper education to the patient.
- Provide proper rehabilitation to the patient.
- Provide proper mechanical ventilation to the patient.
- Advise the patient to perform proper deep breathing and cuffing exercises.
- Advise the patient to perform proper active range of motion exercises.
- Advise the patient to consume a high-calorie, high-protein diet.
- Advise the patient to consume adequate fluid intake. Give.
- Advise the patient to take proper medicine.
- Advise the patient to take proper follow-up.
- Provide the patient with a properly calm and comfortable environment.
1) Define/ Explain Parkinson’s Disease. Define Parkinson’s disease.

- Parkinson’s disease is a chronic, progressive, neurological disorder in which the muscles No control, movement, and balance are disturbed. Parkinson’s disease is a slow, progressive neurological movement disorder that can also result in disability. Parkinson’s disease is a type of movement disorder. In which a person’s muscle movement is altered.
- Parkinson’s disease was first described in 1817 by London surgeon James Parkinson.
- Parkinson’s disease has 3 main cardinal signs.
- 1) Tremor ( Tremor: = Shaking),
- 2) Muscles Rigidity ( Muscles Rigidity:=stiffness),
- 3) Bradykinesia
••>
1) Tremor (tremor:=shaking),
- In fingers, hands, feet, etc. Voluntary movement is observed. Tremor is mainly observed when the person is in the resting stage. But it is not observed when the person is on a task. Tremor occurs when a person is excited, tense and stressed.
2) Muscles Rigidity (Muscles Rigidity:=Stiffness),
- In this, stiffness occurs in the limbs and trunk. This stiffness increases during movement. Rigidity causes pain and ache in the muscles.
3) Bradykinesia
- Bradykinesia is a slowness of voluntary movement. Sometimes there is difficulty in movement, due to stiffness in facial muscles in bradykinesia, a “Mask-Like” appearance is seen.
- Thus, the cardinal signs of Parkinson’s disease are Tremor, Muscles Rigidity and Bradykinesia.
2) Explain the Etiology/ cause of the Parkinson’s. Explain the causes of Parkinson’s disease.
- Due to genetic factors.
- Due to environmental factors.
- Due to destruction of nerve cells that produce dopamine.
- Due to genetic factors.
- Due to family history.
- Due to genetic factors.
- Due to atherosclerosis.
- Due to viral infection.
- Due to head trauma.
- Due to chronic use of antipsychotic drugs.
- Due to dopamine deficiency in the substantia nigra of the brain Due to.
- Environmental factors.
- Use of antipsychotic drugs.
3) Explain the Clinical manifestation/ sign and symptoms of the patient with the Parkinson’s Disease. Describe the symptoms and signs of a patient with Parkinson’s disease.
- Tremors,
- Muscle rigidity,
- Bradykinesia,
- Postural instability,
- Difficulty in speech and swallowing.
- Sleep disturbances.
- Mood and cognitive changes.
- Constipation.
- Memory loss.
- Swallowing difficulties.
- Speech problems.
- Depression.
- Anxiety.
- Stress.
- Confusion.
- Memory loss.
- Dementia.
- Diminished sense of smell Occur.
- Increased sweating.
- Male erectile dysfunction.
- Skin problems.
- Impairment in speech.
- Urinary frequency and urgency.
- Loss of spontaneous movement Occurrence.
- Auditory and Visual Hallucination Occurrence.
4) Explain the Diagnostic evaluation of the patient with the Parkinson’s Disease. Explain the diagnostic evaluation of the patient with Parkinson’s Disease.
- history tacking and physical examination.
- CSF Examination.
- MRI (Magnetic Resonance Imaging).
- PET (Positron Emission Tomography).
- Neurological Examination.
- CSF culture.
5) Explain the medical management of the patient with the Parkinson’s Disease. Explain the medical management of the patient with Parkinson’s Disease.
1) Provide antiparkinsonian medication to the patient.
- Ex:= Levodopa and Carbodopa.
2) Provide the patient with Dopamine Agonist medication.
- Ex:= Pergolide,
- Apomorphine ( Apokyn).
This type of medicine works to increase Dopamine in the brain.
3) Provide the patient with Monoamine Oxidase B inhibitor medicine. To do.
- Ex:= Selegiline,
- Rasagiline ( Azilect).
This type of medicine prevents the breakdown of dopamine.
4) Provide the patient with catechol O-methyltransferase inhibitors medicine.
- This type of medicine increases the effects of carbidopa and levodopa and works by blocking the enzyme that breaks down levodopa.
5) Provide the patient with anticholinergic medicine.
- This type of medicine is used to control tremors and rigidity in the muscles due to Parkinson’s disease.
- Ex:= Benztropine ( Cognitine),
Trihexyphenidyl
,Cycrimine,
Procyclidine,
6) Provide Antiviral therapy to the patient.
7) Provide proper physical therapy to the patient.
8) Advise the patient to do proper range of motion exercises.
9) Provide proper speech therapy to the patient to improve speaking and swallowing. The problem can be reduced.
6) Explain the Surgical management of patients with the Cerebro Parkinson’s Disease. Explain the surgical management of patients with Parkinson’s Disease.
1) Deep Brain Stimulation
- Deep brain stimulation is a surgical procedure to treat Parkinson’s disease. In this procedure, electrodes are placed in the deep part of the brain and these electrodes block the nerve pathways in the brain that are responsible for tremors, due to which the tremor is reduced.
2) Stereotatic Procedure.
- Thalamotomy Localise:= In this, a specific group of cells mainly in the thalamus is destroyed.
- Pallidotomy:= In this procedure, the globus pallidus in the brain is surgically removed. Destruction is done.
3) Neural Transplantation
- In this procedure, the adrenal medulla is surgically implanted and this procedure is mainly done to reestablish the release of dopamine.
7) Explain the Nursing management of patients with the Parkinson’s Disease. Explain the nursing management of a patient with Parkinson’s disease.
- Properly assess the patient.
- Provide complete information to the patient and his family members about the cause, symptoms and signs of Parkinson’s disease and its treatment.
- Advise the patient to take proper medication.
- Provide proper nutritional support to the patient Provide support.
- Provide proper speech therapy and swallowing therapy to the patient.
- Provide proper psychological support to the patient.
- Advise the patient to do proper physical exercises such as walking, cycling, swimming.
- Advise the patient to take a proper bath with lukewarm water so that the muscles can relax properly.
- Advise the patient to take proper rest.
- Advise the patient to walk properly.
- Advise the patient to take food intake in small and frequent amounts.
- Monitor the patient’s daily weight.
- Provide the patient with a properly calm and comfortable environment.
1) Define/Explain Alzheimer’s Diseases. Define Alzheimer’s disease.
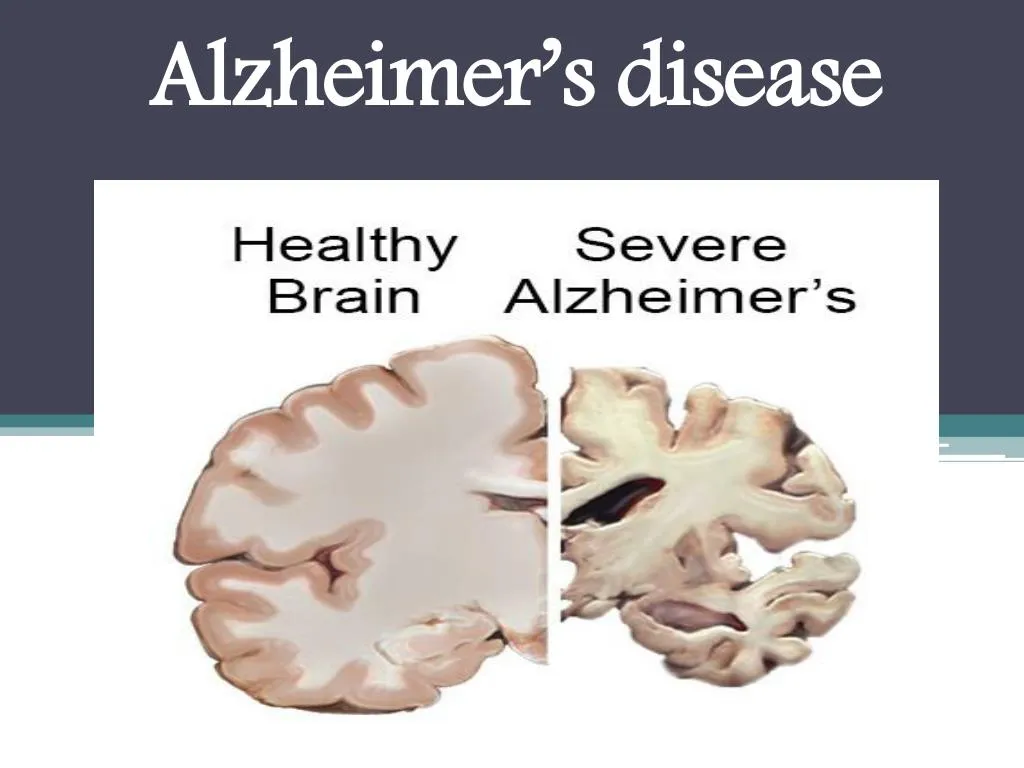
- Alzheimer’s disease is a progressive neurological disorder. Alzheimer’s The disease is also called senile dementia of the Alzheimer’s type (SDAT).
- Alzheimer’s is the most common form of dementia (the inability to remember anything, whether short-term or long-term).
Alzheimer’s disease causes impairment in a person’s memory, judgment, language, cognitive function, and daily living activities. In Alzheimer’s dementia, brain cells are first destroyed, which leads to mental disorders. - Alzheimer’s disease primarily affects older adults. It causes impairment in a person’s memory, cognitive function, behavior, and daily routine activities. In this disease, mainly due to the accumulation of protein in the brain, the brain cells are first destroyed, due to which the neural pathway breaks down and mental disorders are seen in the person.
2) Explain the Etiology/ cause of the patient with the Alzhimer’s Disease. Explain the cause of the Alzheimer’s Disease.
- Due to genetic factors
- Chromosome 1,14,19 and 21.
- Age above the 65 year’s.
- Due to brain changes.
- Environmental factors.
- Head injury Due to.
- Exposure to certain toxins.
- Lifestyle factors.
- Low physical activity.
- Poor diet.
- Smoking.
- Family history Due to.
- Viral infection.
- Smoking.
- Coronary artery disease.
- Myocardial infarction.
- Immune system impairment.
- Exposure to environmental toxins Due to getting into.
- Due to high blood pressure.
- Due to elevated blood cholesterol levels.
- Due to Down syndrome (People with trisomy 21).
- Due to vascular factor.
3) Explain the 7 stage of the patient with the Alzheimer’s Diseases. Explain the seven stages of Alzheimer’s disease in a patient..
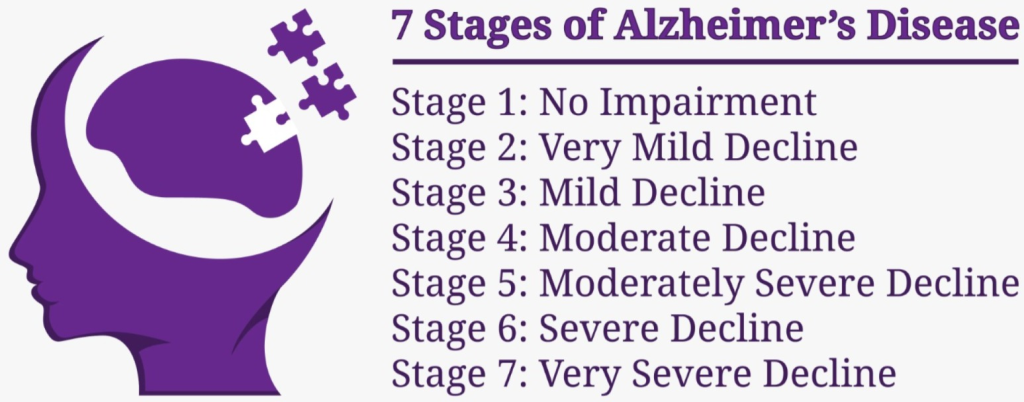
1) No Cognitive impairment.
- In this stage, the person does not experience any symptoms. In this stage, the person’s cognitive, behavioral and intellectual function is not impaired and the person can perform his daily routine activities properly.
2) Very mild Cognitive decline:=
- In this stage, the person experiences minor impairment in his memory and cognitive function. In this stage, the person does not remember his name properly and these changes can be noticed by the person’s family members and friends.
3) Mild Cognitive Decline (Early stage Alzheimer’s):=
- In this stage, the symptoms of the person are more noticeable. In this stage, the person has problems remembering anything that happened recently and finding the right words. But in this stage, a person can do his daily routine activities properly by applying some remedies.
4) Moderate Cognitine Decline(Mild to moderate Alzhimer’s):=
- In this stage, a person’s cognitive decline is very high. In this stage, the person has to struggle with any task such as managing finances, remembering recent events, communicating, performing complex activities.
- In this stage, changes also occur in the personality and behavior of the person. Such as irritability, social withdrawal, anxiety, etc. are seen.
- But the person can perform daily routine activities with some amount of guidance.
5) Moderately severe Cognitive decline ( Moderate Alzhimer’s)
- In this stage, the person requires a greater amount of assistance in performing their daily routine activities. In this stage, the person has difficulty dressing, bathing, and using the toilet independently. In this stage, the person’s memory is lost to a greater extent. The person’s personal history is also forgotten and the person is disoriented to time, place, and person.
6) Severe Cognitive Decline ( Moderately severe to severe Alzhimer’s )
- In this stage, the person experiences profound cognitive decline and the person has extensive difficulty in daily routine activities. Assistance is needed. In this stage, the person cannot even recognize his family members and friends. Behavioral changes such as agitation, aggression, or wandering are seen in the person. And the person has difficulty controlling physical activities such as walking and movement.
7) Very severe Cognitive decline (severe Alzhimer’s)
- In this stage, the person’s cognitive and functional impairment becomes severe. In this stage, the person also has impairment in communication and the person is bedridden. In this stage, the person needs constant care to perform all activities such as eating, toileting, personal hygiene, etc. Assistance is required in activities. In this stage, the person cannot perform any activity on his own and is persistently dependent on others.
4) Explain the Clinical manifestation/ sign and symptoms of the patient with the Alzhimer’s Disease.
- Memory loss.
- Difficulty in solving tasks.
- Confusion.
- Disorientation in time, place and person.
- Changes in mood and behavior To be.
- Language problems.
- Judgement is decreased.
- Impairment in solving tasks.
A. Stage 1 ( Duration of disease 1 – 3 years)
- Mild memory impairment.
- Difficulty in new learning.
- Personality: Occasional irritability.
- Sadness.
- Diffusion.
- The person cannot remember properly.
B.Stage 2( Duration of disease 2 – 10 years):=
- Moderate memory impairment.
- Recent and remote things are not remembered properly.
- Spatial disorientation.
- Speaking impairment.
- Personality changes.
- Changes in sleep patterns.
- Delirium.
- Motor system:= restlessness, pacing.
C Stage 3 ( Duration of disease 8 – 12 years)
- In this, cognitive function is severely impaired.
- Rigidity in the limbs.
- Flexion posture.
- Urinary and fecal incontinence.
- Increased irritability.
- Difficulty swallowing.
- Weight loss.
- Loss of appetite.
- Direct infection.
- Short-term and long-term
- Memory loss.
- Unresponsiveness.
5) Explain the Warning sign of Alzheimer’s Disease. Tell the warning signs of Alzheimer’s disease.
- Memory loss,
- Changes in mood and behavior.
- Difficulty performing familiar tasks.
- Changes in personality.
- In time, place, and person Disorientation.
- Misplacing things.
- Problems with language.
- Poor and decreased judgment.
- Problems with abstract thinking.
- Loss of initiative.
6) Explain the diagnostic evaluation of the patient with Alzheimer’s disease. Explain the diagnostic evaluation of a patient with Alzheimer’s disease.
- history taking and physical examination.
- cognitive assessment.
- neuropsychological test.
- laboratory test.
- brain imaging.
- Magnetic Resonance Imaging ( MRI ).
- Computed Tomography ( CT SCAN).
- Positron Emission Tomography ( PET Test).
- Cerebro Spinal Fluid Analysis ( C.S.F.Analysis).
- Genetic Testing.
- Electroencephalogram.
- Single photon emission computed tomography (SPECT).
- Mini mental status examination.
- Complete blood count test.
- Erythrocyte sedimentation rate (ESR) testing.
7) Explain the medical management of the patient with the Alzhimer’s Dieseas. Explain the medical management of the patient with Alzheimer’s Disease.
- The aim of treatment for Alzheimer’s disease is to alleviate symptoms, slow the progression of the disease, and improve quality of life.
1) Provide the patient with cholinesterase inhibitor medication.
- Cholinesterase inhibitor medication is It is considered the first line treatment for treating cognitive impairment in Alzheimer’s disease.
Ex:=
Donezepil ,
Rivastigmine,
Galantamine,
Memantadine. - These medications work to improve cognitive function and prevent behavioral changes and any changes in the individual.
2) Neuroleptics Drugs:=
- This type of medicine is provided to relieve some symptoms caused by Alzheimer’s disease such as anger, depression, anxiety, sleep disturbances, etc.
3) Memory enhancing drug:=
- Memory enhancing drugs are provided to improve memory and cognitive function.
- Ex:=
- Acytykcholine precursors ( choline, lecithin and),
- Anticholinestrase agent ( Physostigmine).
4) Provide the patient with antipsychotic drugs.
- Antipsychotic drugs are mainly used as important medicines to treat agitation, confusion, hallucinations, delusions.
- Ex:=
Haloperidol,
Thioridazine .
5) Provide the patient with Antidepressant medication.
Antidepressant medicine is mainly used to treat depression.
- Ex:= Tricyclic antidepressant,
- Nortriptyline and desipramine.
6) Provide the patient with antioxidant medicine.
7) Provide the patient with non-steroidal anti-inflammatory drugs (NSAIDs).
Ex:=
Ibuprofen,
Sulindac,
Indomethacin.
8) Advise the patient to exercise properly.
9) Advise the patient to consume foods rich in vitamin C, vitamin E, and beta-carotene and vegetables. Give.
10) Advise the patient to consume a low fat diet.
11) Advise the patient to maintain normal blood pressure.
12) Provide the patient with proper work and a comfortable environment.
13) Provide the patient with proper aromatherapy, massage and music therapy.
14) Advise the patient to make proper behavioral modifications.
8) Explain the Nursing management of patients with the Alzhimer’s Dieseas. Explain the Nursing Management of Patients with Alzheimer’s Disease.
- Properly assess the patient.
- Properly assess the patient’s cognitive function, physical health, nutritional status.
- Properly provide the patient with a safe and supportive environment.
- Keep all hazardous things away from the patient.
- Properly Advise on meditation, massage, and exercise.
- Advise the patient to take medication properly.
- Advise the patient to set an alarm for work.
- Advise the patient to label the things he needs.
- Provide the patient with a proper work and comfortable environment.
- Properly monitor the patient.
- Advise the patient to properly consume nutritious food.
- Advise the patient to properly maintain his/her personal hygiene.
- Provide the patient with a properly supportive environment.
- Advise the patient to properly take medication.
- Advise the patient to follow up properly.
1) Define/ explain the Trigiminal Neuralgia. Define trigeminal neuralgia.
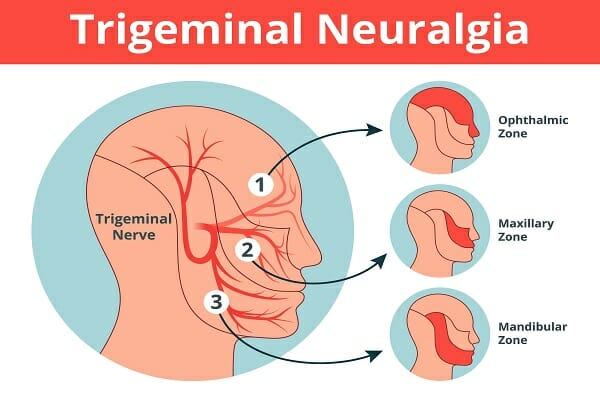
- Trigeminal neuralgia is a type of nerve disorder. This disease is characterized by stabbing and electric Shock-like pain occurs in the face.
- Trigeminal neuralgia is also known as “suicide disease” because the condition causes severe pain that cannot be easily controlled.
- Trigeminal neuralgia involves the fifth cranial nerve (trigeminal). And the most severe pain occurs in that part of the face.
- Another name for trigeminal neuralgia is Tik doulourex.
The Trigeminal nerve has three main branches :
- Ophthalmic branch (V1) – forehead, eyes, scalp
- Maxillary branch (V2) – cheek, upper lip, upper teeth
- Mandibular branch (V3) – jaw, lower lip, lower teeth
2) Explain the Etiology/cause of the patient with the Trigiminal Neuralgia. Give the causes of trigeminal neuralgia.
- Due to compression in the trigeminal nerve.
- Due to multiple sclerosis.
- Age := more common above the 50 years.
- Due to nerve injury and trauma.
- Due to genetic factors.
- Due to other medical conditions.
- Due to stroking the face.
- Due to brushing the teeth.
- Due to talking.
- Drinking.
3) Explain the Clinical manifestation/ sign and symptoms of the patient with the Trigiminal Neuralgia.
- Facial pain.
- Pain is felt on one or both sides of the face.
- Pain occurs during facial movements.
- Sudden, electrical shock-like ,Stabbing pain.
- Pain in the lips, eyes, nose, scalp and forehead.
- Pain in daily routine.
- Psychosocial impact.
- Sleep disturbance.
4) Explain the Diagnostic evaluation of the patient with the Trigiminal Neuralgia. Write a diagnostic evaluation of a patient with trigeminal neuralgia.
- history taking and physical examination.
- Neurological examination.
- Blood test.
- MRI test.
- CT scan.
- Electrophysiological Test.
- Laboratory Test.
5) Explain the medical management of the patient with the Trigiminal Neuralgia. Explain the medical management of a patient with trigeminal neuralgia.
- If the patient is having seizures, then give anticonvulsant medicine.
Ex:=
carbamazepine,
Oxcarbazepine,
Gabapentin, - Provide muscle relaxant medicine to the patient.
- Ex:= Baclofen
- Provide the patient with tricyclic antidepressant medicine.
- Provide the patient with NSAID group medicine.
- Provide steroid medicine if the patient has an inflammatory condition.
- Provide the patient with botulinum toxin injection when no other treatment is working properly.
6) Explain the surgical management of patients with the Trigiminal Neuralgia. Write the surgical management of patients with the Trigiminal Neuralgia.
1) Microvascular Decomposition:=
- Microvascular decompression is a classic and most effective surgical procedure. This procedure is performed to reduce the pressure in the trigeminal nerve.
2) Gamma knife Radiosurgery :=
- Gamma knife radiosurgery is a non-invasive procedure. In this procedure, a highly focused beam of radiation is directed directly at the trigeminal nerve. Due to this, pain is reduced.
3) Radiofrequency ( RF) Rhizotomy ( Thermo coagulation)
- This is an outpatient procedure. In this procedure, a needle is inserted into the gasserian ganglion. Through which electric current is passed and heating is provided, which causes a lesion in the ganglion.
4) Rhizotomy:=
- In this procedure, a part of the trigeminal nerve at the base of the brain is cut.
5) Balloon Compression:=
- In balloon compression, a catheter with a balloon attached is advanced to the trigeminal nerve and pressure is applied to the trigeminal nerve, which blocks the nerve signal.
7) Explain the Nursing management of patients with the Trigiminal Neuralgia. Explain the nursing management of a patient with trigeminal neuralgia.
- Properly assess the patient.
- Properly assess the patient’s pain.
- Properly take comfort measures for the patient.
- Properly provide psychological support to the patient.
- Provide proper nutritional support to the patient.
- Provide proper safety measures to the patient.
- Provide complete information to the patient about his disease, its causes, and signs and symptoms.
- Advise the patient to avoid very hot and very cold foods.
- Advise the patient to take small and frequent amounts of food. Giving advice.
- Giving advice to the patient to maintain proper oral hygiene.
- Properly explaining the procedure to the patient and his family members.
- Providing analgesic medicine if the patient is in pain.
- Providing proper work and a comfortable environment for the patient.
- Patient Advise the patient to take medication regularly.
- Advise the patient to take proper follow-up.
1) Explain/ Define Bell’s palsy. Define Bell’s Palsy.
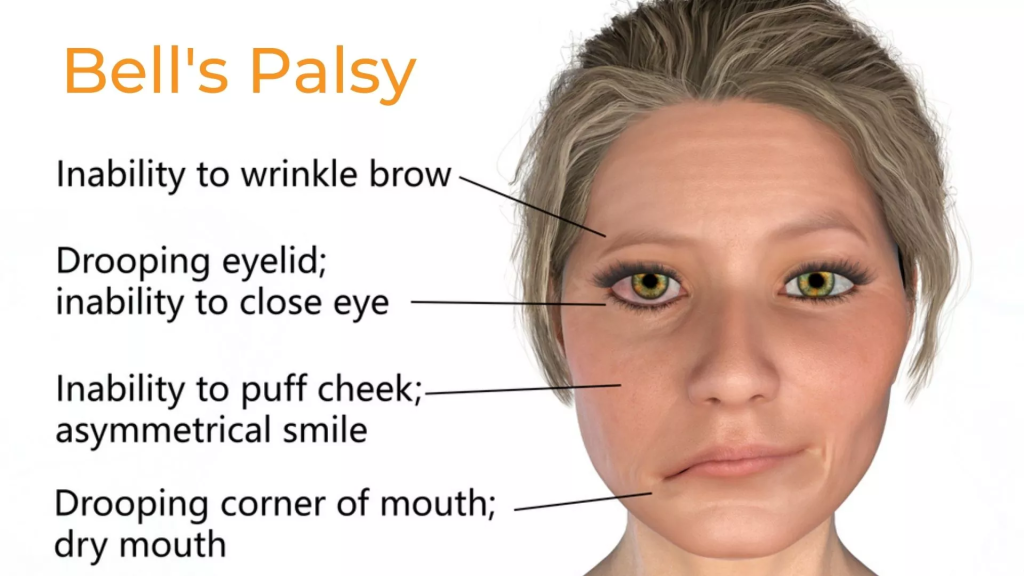
- Bell’s Palsy is a condition in which the seventh cranial nerve, i.e. Facial nerve (vii cranial nerve := Facial nerve) dysfunction occurs. Due to this, the facial muscles of the affected side of the face cannot work properly and due to damage to this facial nerve, the muscles of that side of the face become weak and paralyzed.
- Facial palsy is characterized by idiopathic unilateral (one-sided) facial nerve paralysis. Due to this paralysis, there is difficulty in opening and closing the eyes of the affected side of the face. Drooling (dripping of saliva from the corner of the mouth) occurs in the face of the affected side. And the facial muscles cannot work properly.
- Bell’s palsy is mainly seen between the ages of 15 and 60. This disease was described by Scottish Anatomist Charles Bell’s.
2) Explain the Etiology/ cause of the patient with the Bell’s palsy. Explain the cause of Bell’s palsy.
- The exact cause of Bell’s palsy is unknown.
- Due to inflammation and swelling in the facial nerve.
- Due to viral infection.
- Ex:=
Herpes simplex virus (HSV).
Herpes zoster virus.
Epstein Barr virus. - Due to autoimmune response.
- Due to environmental factors.
- Due to genetic conditions.
- Due to brain tumors.
- Stroke.
- Hiv infection.
- Middle ear infection Because of.
- Lyme disease.
- Sarcoidosis.
3) Explain the clinical manifestation/ sign and symptoms of the patient with the Bell’s palsy. Describe the symptoms and signs of a patient with Bell’s Palsy.
- Facial weakness and paralysis.
- Difficulty opening and closing the eyes.
- Drooling (dripping of saliva from the corners of the mouth).
- Difficulty eating and speaking.
- The sense of taste is altered.
- Twitching and spasms in facial muscles.
- Facial expression is impaired.
- Eyes and mouth become dry.
- Headache.
- Difficulty in talking.
4) Explain the diagnostic evaluation of the patient with the Bell’s palsy. Explain the diagnostic evaluation of a patient with Bell’s palsy.
- history taking and physical examination.
- Ct scan.
- MRI (Magnetic Resonance Imaging).
- Electromyography (EMG).
- Nerve conduction test .
5) Explain the medical management of the patient with Bell’s palsy. Explain the medical management of a patient with Bell’s palsy.
- Properly provide corticosteroid medicine to the patient.
- Ex:=
prednisone - Properly provide antiviral drug to the patient.
- Ex:=
Acyclovir,
Valacyclovir. - Provide proper eye care to the patient.
- Provide proper analgesic medicine to the patient for pain management.
- Ex:= Acetaminophen,
Ibuprofen. - Provide proper physical therapy to the patient.
- Provide proper medication to the patient.
- Properly provide botulinum toxin injection to the patient.
- Properly provide a well-balanced diet to the patient.
- Properly provide medicine to the patient.
6) Explain the nursing management of patients with Bell’s palsy. Explain the nursing management of Bell’s Palsy patient.
- Provide proper education to the patient.
- Provide complete information to the patient about his disease, its causes, its symptoms and signs, and its treatment.
- Provide proper eye care to the patient.
- The patient Advise on proper facial muscle exercise.
- Provide proper emotional support to the patient.
- Provide proper analgesic medicine for the patient’s pain management.
- Provide proper nutritional support to the patient.
- Advise the patient to take medicine regularly.
- Advise the patient to follow up properly.
1) Explain/ Define Peripheral Neuropathies. Define peripheral neuropathies.
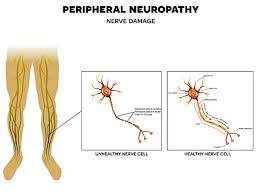
- Peripheral neuropathy is a group of disorders in which the peripheral nerves are damaged. Peripheral nerves are nerves that are present outside the brain and spinal cord. Which provides communication between the brain and other parts of the body such as muscles, skin, internal organs and blood vessels etc.
- If there is involvement of a single nerve in the nerve damage, it is called mononeuropathy.
- If there is involvement of multiple nerves in the nerve damage, it is called multifocal neuropathies.
- And
- If there is involvement of many nerves in the nerve damage, it is called Polyneuropathy.
- Peripheral neuropathy causes pain, tingling, numbness, and burning sensation in the hands and feet.
2) Explain the Etiology/ cause of the patient with the Peripheral Neuropathies. Explain the cause of peripheral neuropathy.
- Due to diabetes.
- Due to infection.
- Herpes simplex virus,
Varicella zoster virus,
Lyme disease,
Hepatitis c . - Due to autoimmune disorder.
- Ex:= Rheumatoid arthritis,
Guillian bare syndrome,
Sjogran syndrome, - Due to exposure to toxic substances.
- Ex:= chemotherapy drugs,
Heavy metal (lead, mercury),
Alcohol. - Due to genetic factors.
- Due to trauma and injury.
- Due to accident.
- Due to fall down.
- Due to sports injury.
- Due to nutritional deficiency.
- Ex:= deficiency of vitaminB12 ,Folate, Thiamin.
- Due to vascular disorder.
- Singles (post herpetic neuralgia).
- Due to metabolic and endocrine disorders.
- Ex:= Diabetes mellitus,
- Due to alcoholism.
- Due to vascular damage and blood diseases.
- Due to inherited disorders.
- Ex:= Amyloid Polyneuropathy,
- Charcot- Marie- Tooth disease.
- Due to cancer therapy.
- Ex:= Vincristine ( Oncovin,Vincasar),
3) Explain the Clinical manifestation/ sign and symptoms of the patient with the Peripheral Neuropathies. Explain the symptoms and signs of the patient with Peripheral Neuropathies.
- Tingling and numbness sensation in the hands and feet.
- Weakness in the hands and feet.
- Pain.
- Extreme sensitivity even to light touch.
- Decreased coordination.
- Painful cramps.
- Bone degeneration and changes in skin, hair and nails.
- Bowel and bladder problems.
- Changes in blood pressure.
- Sharp pain.
- Extreme pain in the extremities.
4) Explain the Diagnostic evaluation of the patient with the Peripheral Neuropathies. Explain the diagnostic evaluation of the patient with peripheral neuropathy.
- History taking and physical examination.
- Electroencephalography (EEG).
- Electromyography (EMG).
- Blood tests.
- Imaging studies.
- CT scan.
- MRI.
- Nerve conduction velocity studies (NCV) studies.
- Spinal tap.
- Nerve biopsy.
- Skin biopsy.
5) Explain the management of the patient with the Peripheral Neuropathies. Explain the management of the patient with peripheral neuropathy.
- If the patient is in pain, provide analgesic medicine.
- Ex:= Acetaminophen,
Ibuprofen. - Provide the patient with antidepressant medicine.
- Ex:= tricyclic Antidepressant,
( Amitriptyline), - Selective Seretonine Reuptake inhibitor ( Duloxetine),
- This medicine works to reduce neuropathic pain and improve mood.
- Advise the patient to exercise properly.
- Advise the patient to make lifestyle modifications.
- Advise the patient to eat a nutritious diet.
- Provide immunosuppressive medication to the patient.
- Ex:=
Prednisone ,
Cyclosporine,
Azathioprine, - Provide antiseizure medicine to the patient.
- Provide proper supporting device to the patient.
- Hand and foot braces,
Orthopedic shoes, - Advise the patient to make lifestyle modifications.
- Advise the patient to take proper medication.
- Advise the patient to take proper regular follow-up.
1.Explain/ define Brain Tumor =
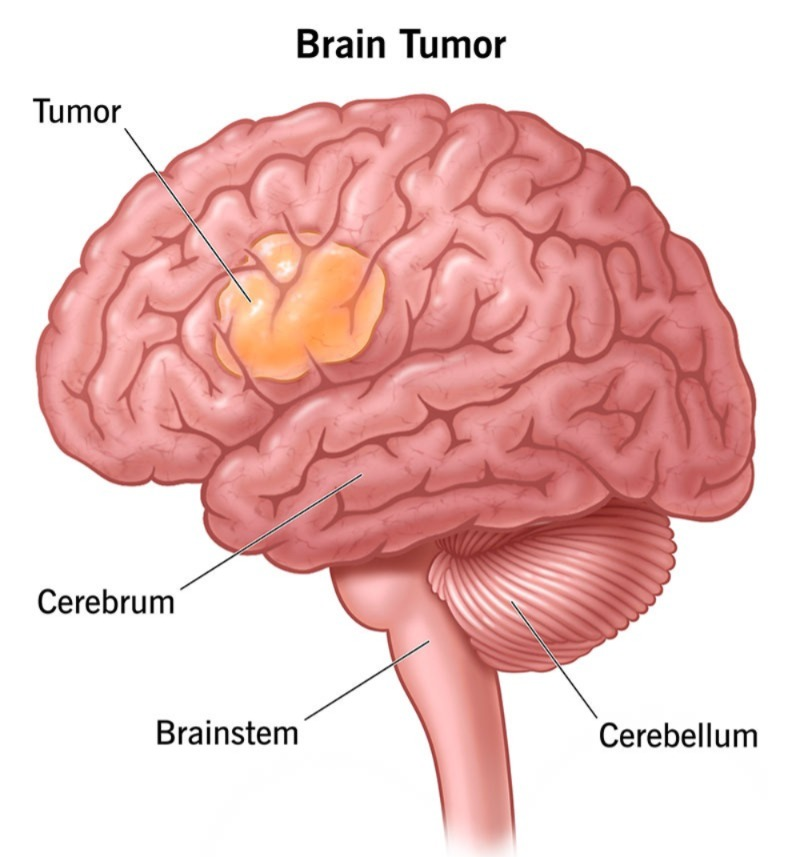
- In a brain 🧠 tumor, abnormal growth of cells occurs in the brain and forms a tumor.
This tumor can be malignant or benign. - In a brain tumor, abnormal and uncontrolled division of cells occurs in the brain and cell growth occurs and it forms a tumor.
- These tumors are found in the brain, lymphatic tissue, blood, intracranial nerves, pituitary gland, pineal gland And it can be in any other organ of the body and transfer to the brain and affect the brain.
- This tumor can be in the junction of the gray matter and white matter of the brain.
2)Explain Brain tumor classification / type. State the classification of brain tumors.
1) Primary Brain 🧠 tumor,
2) secondary Brain 🧠 tumor,
1) Primary Brain tumor:=
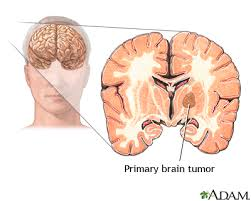
- Primary brain tumors are made up of cells and structures of the brain itself.
A)Intracerebral tumor:=
- Most common Primary brain tumors are gliomas that arise from glial cells.
There are many types of gliomas, such as:
- Astrocytoma (in astrocytes),
- Brain stem glioma (brain stem glioma),
- Ependymoma ( in ependymo),
- oligodendroglioma ( in oligodendroglio)
- Medulloblastoma ( in medulloblasto).
2) tumor arising from supporting structures (tumor that arises from the supporting structures of the brain):=
- Menengioma ( in meningioma),
- schwannoma ( schwanoma),
- germ cell tumor of the brain,
- pineal region tumor,
- Angioma.
2)secondary Brain 🧠 tumor:=
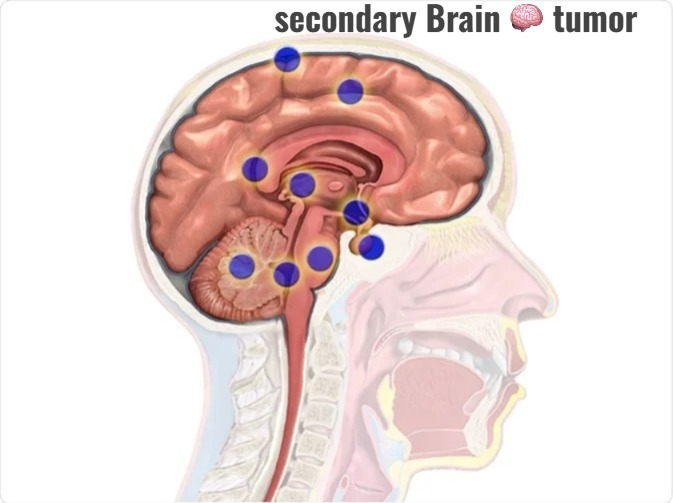
- This secondary brain tumor develops from a structure outside the brain and it is transferred to the brain (i.e. metastasis) and the tumor develops in the brain, it is called secondary brain tumor.
- The most common organ like
🧠 brain,
🫁 lung,
Brest,
Kidney. - Tumors from all these parts of the body metastasize and transfer to the brain and there the tumor grows to a greater extent, which results in cancer. is.
3) Explain the Etiology of the brain tumor.
3) Explain the clinical manifestation / Sign and symptoms of the patient with the brain Tumor. Give the symptoms and signs of brain tumor. 4) Explain the diagnostic evaluation of the patient with the brain tumor. Explain the diagnostic evaluation of a patient with brain tumor. 4) Explainthe Management of the patient with the brain tumor . Explain the management of a patient with brain tumor. Antineoplastic agent:= A)alkylating agent, #COMPLICATION := Nursing management := Nursing assessment := 1) Check the patient’s level of consciousness. 2) Perform a neurological examination of the patient. 3) Check the patient’s pain level. 4) Check the patient’s nutritional status. 5) Check the patient’s skin integrity. 6) Check if the patient has a condition like tics or weakness or seizures. 7) Check the patient’s activity level. 8) Check the patient’s vital signs. Nursing diagnosis:= 1) Pain related to mass in Brain, nerve compression. Nursing interventions:= Reliving pain . 2)Risk of injury related to gait disturbance . Nursing interventions:= Prevention of *injury:= 3) Anxiety related to disease condition . Nursing interventions:= Reliving Anxiety:= 4) Activity intolerance related*to weakness or fatigue . Nursing interventions := Promoting activity level:= 5) Altered nutrition status less than body requirement related to nausea and vomiting. Nursing interventions:= improve nutrition status of client:= 6)ineffective family coping related to clients disease and prognosis . Nursing interventions:= Reassure the family coping. 1) Explain the Spinal Cord Tumor. Define spinal cord tumor. 2) Type of spinal cord tumor. Name the types of spinal cord tumors. 1)primary spinal cord tumor:= 2)secondary spinal cord tumor:= ## type:= 1) intramedullary tumor ( intramedullary tumor). 2) intradural extramedullary tumor ( intradural extramedullary tumor) Tumor ) 3) extradural spinal tumor ( Extradural Spinal Tumor) 4)secondary bone cancer ( Secondary Bone Cancer) 1) intramedullary tumor ( Intramedullary Tumor):= 2) Intradural extramedullary tumor.( Intradural extramedullary tumor) := This tumor mainly arises from the dura but is located outside the spinal cord, so it is called an intradural extramedullary tumor. This is mainly inside the covering of the spinal cord but is located outside the spinal cord itself. Ex:= 2)schwannomas (schwannomas) 3) extradural spinal tumor (extradural spinal tumor) := Extradural spinal tumor is mainly metastasized but it arises from the vertebra itself. This mainly starts from the bone of the spine itself. Ex:= benign tumor includes:= 1) Chordomas (Chordomas) 2) osteomas (osteomas) ##malignant tumor includes:= 1) chordosarcomas (cordosarcomas) 2) fibrosarcomas ( Fibrosarcomas) 4)Secondary bone cancer (Secondary bone cancer) . This cancer mainly spreads to the spinal cord from other parts of the body. This is called secondary bone cancer. This cancer mainly occurs in the lungs, breast, lymphoma, prostate cancer, and myeloma. Myeloma is a plasma cell cancer that mainly It affects the vertebrae. 2) Explain The Etiology/ causeof the patient with the Spinal cord tumor. Write the causes of spinal cord tumor:= 3)explain clinical manifestation/sign and symptoms of the patient with the tumor. Describe the symptoms and signs of spinal cord tumor. 4) explain The diagnostic evaluation of the patient with the spinal cord tumor. Write the diagnostic evaluation of the patient with the spinal cord tumor. 5) Explain the management of spinal tumor. Write the management of spinal tumor. ## medical management ## surgery:= ## explain the nursing management ## 1) Explain/Define Huntington’s disease. Define Huntington’s disease. 2) Explain the Etiology/ cause of the patient with the Huntington’s disease. Give the causes of Huntington’s disease. 3) Explain the clinical manifestation/ sign and symptoms of the patient with Huntington’s disease. Describe the symptoms and signs of a patient with Huntington’s disease. 4) Explain the diagnostic evaluation of the patient with Huntington’s disease. Explain the diagnostic evaluation of a patient with Huntington’s disease. 5) Explain the medical management of the patient with Huntington’s disease. Explain the medical management of a patient with Huntington’s disease. 6) Explain the Nursing management of patients with the Huntington’s disease. Explain the nursing management of a patient with Huntington’s disease. 1) Explain/Define Muscular Dystrophy. Define muscular dystrophy. 2) Explain the types/ Classification of the Muscular Dystrophy. State the types and classification of muscular dystrophy. There are a total of nine types of muscular dystrophy. 1) Duchenne Muscular Dystrophy (DMD) Sign and symptoms: 2) Backer Muscular Dystrophy Sign and symptoms:= 3) Myotonic Muscles Dystrophy Signs and symptoms:= 4) Conginital Muscular Dystrophy (Congenital Muscular Dystrophy) Sign and symptoms:= 5) Facio Scapulo Humoral Muscular Dystrophy (Facio Scapulo Humoral Muscular Dystrophy) Sign and symptoms:= 6) Limb Girdle Muscular Dystrophy 7) Oropharyngeal Muscular Dystrophy Signs and symptoms:= 8) Distal Muscular Dystrophy 9) Emery Dreifuss Muscular Dystrophy Sign and symptoms:= 3) Explain the Etiology/cause of the patient with the Muscular Dystrophy. Explain the causes of Muscular Dystrophy in patients. 4) Explain the Clinical manifestation/ sign and symptoms of the patient with the Muscular Dystrophy. Describe the symptoms and signs of a patient with muscular dystrophy. 5) Explain the Diagnostic evaluation of the patient with the Muscular Dystrophy. Explain the diagnostic evaluation of muscular dystrophy. 6) Explain the medical management of the patient with the Muscular Dystrophy. Explain the medical management of the patient with the Muscular Dystrophy. 7) Explain the Nursing management of patients with the Muscular Dystrophy. Explain the nursing management of a patient with muscular dystrophy. 1) Explain/Define the Spinal disk Herniation. Define spinal disc herniation. 2) Explain the Etiology/ cause of the patient with the Spinal disk Herniation. Explain the cause of the spinal disk herniation. 3) Explain the Classification of the Spinal disk Herniation. Explain the classification of spinal disc herniation. There are three types of spinal disc herniation. 1) Cervical disk Herniation ( Cervical Disk Herniation) 2) Thoracic disk Herniation ( Thoracic Disk Herniation) , 3) Lumber disk Herniation ( Lumbar Disk Herniation) ••> 1) Cervical disk Herniation ( Cervical Disk Herniation) 2) Thoracic disk Herniation 3) Lumbar disk herniation 4) Explain the clinical manifestation/sign and symptoms of the patient with the Spinal disk Herniation. Describe the symptoms and signs of spinal disc herniation. 5) Explain the Diagnostic evaluation of the patient with the Herniation of intervertebral Disc. Explain the diagnostic evaluation of intervertebral disc herniation. 6) Explain the medical management of the patient with the Herniation of the Spinal disk. Explain the medical management of spinal disc herniation. 7) Explain the surgical management of patients with the herniation of the intervention disk. Explain the surgical management of spinal disc herniation. 1) Chemonucleolysis 2) Discectomy / Microdiscectomy 3) IDET ( intradiscal Electrothermal therapy ) 4) Lamibectomy 5) Hemilaminectomy 6) (Lumber Fusion ) Lumbar Fusion:= 8) Explain the Nursing management of patients with the Spinal disk Herniation. Explain the Nursing management of patients with Spinal disk Herniation.
( Single Photo Emission Computer Tomography),
( Corticosteroid treatment),
(Craniotomy:=
craniotomy)
( Chemotherapy),
B)Nitrosureas,
C)Antimetabolites,
D)Anti tumor antibiotics,
E)Hormonal agents.
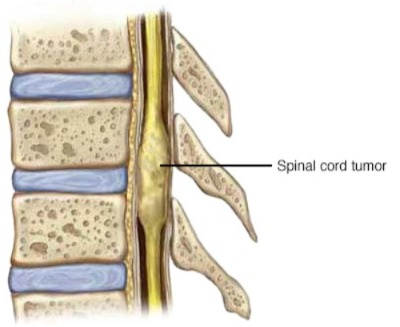
1)meningiomas (meningiomas)
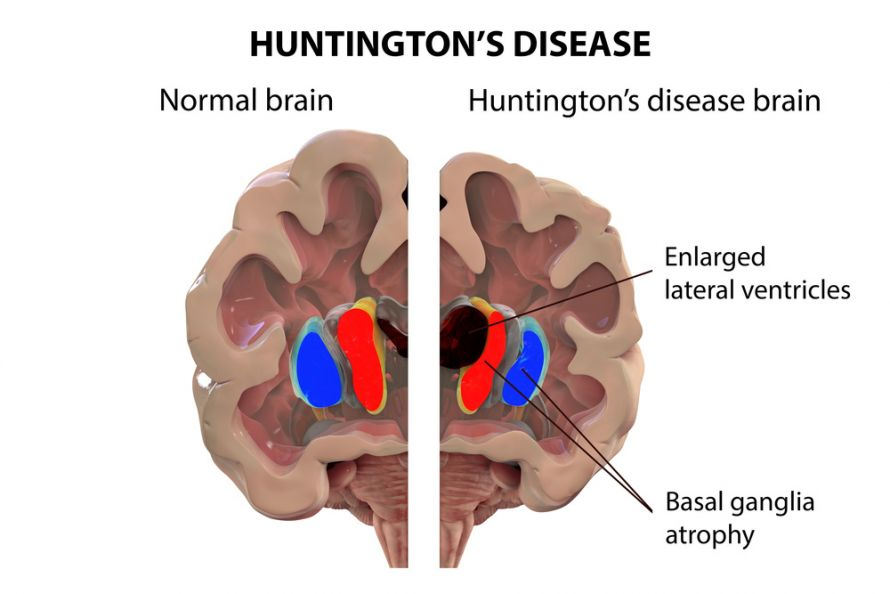
Esitalopram,( Lexapro)
Fluoxitine
( Prozac, Sarafem),
Sertaline ( Zoloft).
Valporic Acid,
Divalproex,
Lamotrigine.
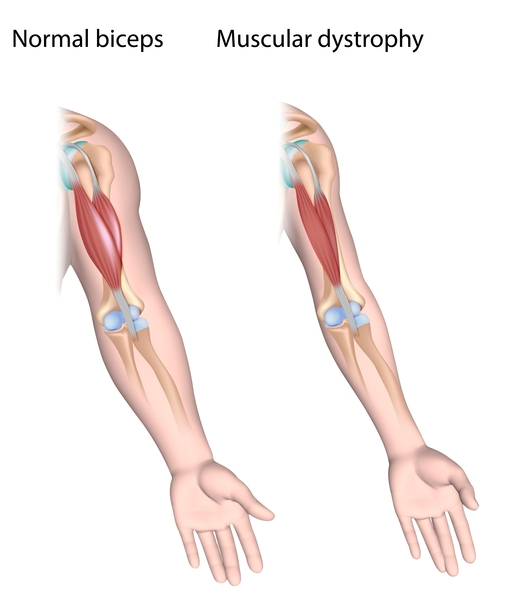
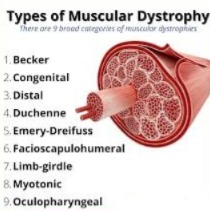
Bracing, Orthopedic surgery etc.
Ex:= prednisone.
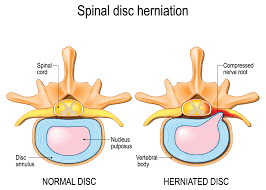
Ex:=
Ibuprofen,
Naproxen.
