ENGLISH-Unit-12-neurological Disorder (part-3)(UOLOAD)
Explain/ Define the Increase intracranial pressure.
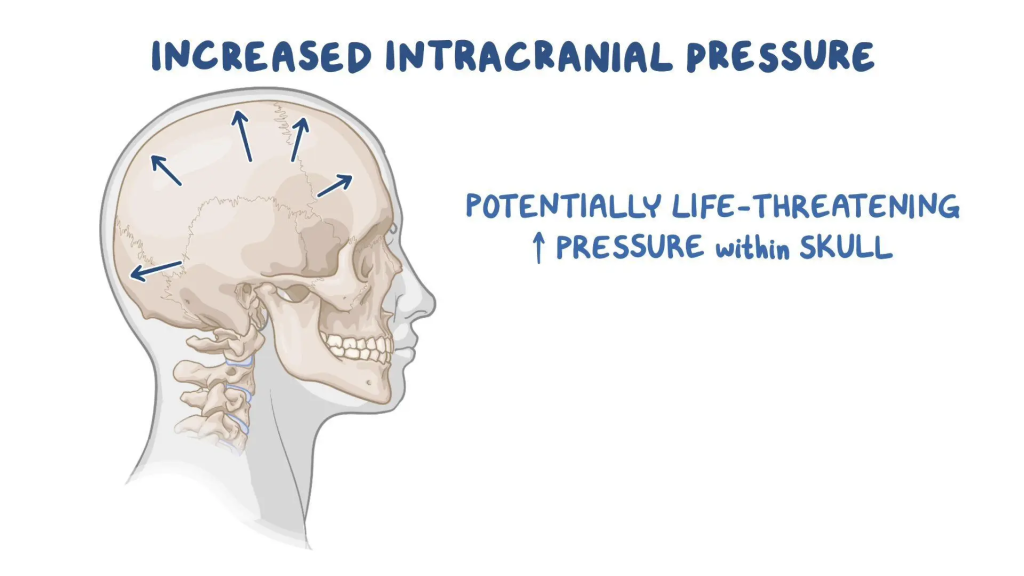
- Intracranial pressure is the pressure that is felt inside the skull and brain tissues due to CSF.
- Increased intracranial pressure means when the intracranial pressure in the cranial cavity is elevated compared to the normal intracranial pressure, it is called increased intracranial pressure.
- Normal intracranial pressure is 5 – 15 mmhg.
- Normal intracranial pressure is 5 – 15 mmhg.
- In increased intracranial pressure in the cranial cavity is > 15 mmhg.
- if pressure into the cranial cavity is > 15 mmhg its known as a increase intracranial pressure.
- Temporary intracranial pressure increases due to coughing, sneezing, straining, bending forward, vomiting.
Explain the Etiology/ cause of the increase intracranial pressure.
- Due to infection,
- Due to tumor,
- Due to stroke,
- Due to aneurysm,
- Due to epilepsy,
- Due to seizure,
- Due to hydrocephalus Due to,
- Hypertensive brain injury.
- Hypoxemia.
- Meningitis.
- Head injury.
- Brain abscess.
- Encephalitis Due to.
- Due to intracranial hemorrhage.
Explain the Clinical manifestation/ sign and symptoms of the patient with the increase intracranial pressure.
- Changes in the level of consciousness.
- The patient’s level of consciousness decreases.
- The patient’s pupillary reflex is absent.
- The patient loses bowel and bladder control.
- Headache.
- Nausea.
- Vomiting.
- The patient’s blood pressure increases.
- The patient’s respiratory pattern changes.
- The patient’s body temperature increases.
- The patient’s mental ability decreases.
- Confusion.
- Double vision.
- Seizure.
- Loss of consciousness.
- Coma.
- Abnormal flexion and extension of the patient.
- Blurred vision. Come.
- Diplopia.
- Abnormal eye movement.
Explain the Diagnostic evaluation of the increased intracranial pressure.
- History tacking and physical examination.
- Lumbar puncture.
- CT scan.
- M .R .I scan.
- PET scan.
- Transcranial dropper.
- Cerebral angiography.
- Neurological assessment.
- Vital sign assessment.
- Pupillary changes assessment.
- Properly assess the patient.
- Properly assess the patient’s vital signs.
- Assess the patient’s neurological status.
- Elevate the patient’s bed to a 30° angle.
- Properly provide oxygen if the patient has respiratory difficulty.
- Provide ventilatory support to the patient through mechanical ventilation.
- Properly measure and provide intravenous fluid to prevent the condition of fluid overload from arising in the patient’s body.
- Give the patient loop and osmotic diuretic medicine.
Explain the medical management of the patient with the increased intracranial pressure.
Ex:=inj. lasix ( frusemide), Inj.mannitol.
- Provide corticosteroids medicine to the patient.
Ex:= Dexamethasone.
- Provide anticonvulsant medicine to the patient.
Ex:= phenytoin.
- Providing antacid medicine to the patient.
Ex:= Ranitidine, Pantoprazole.
- Give the patient sedation and paralysis drugs such as Morphone, Propofol, Vecuronium.
- Give the patient sedation and paralysis drugs such as Morphone, Propofol, Vecuronium.
- Provide inotopic drugs and intravenous fluids to maintain the patient’s blood pressure.
- Provide the patient with nasogastric fitting.
- Properly drain the patient Provide parenteral nutrition.
- If the patient is in pain, provide medication to properly manage the pain.
- Properly monitor the patient closely.
Explain the Surgical management of patients with the increased intracranial pressure.
1) Ventriculostomy:=
- In ventriculostomy, a special type of catheter is inserted into the lateral ventricles to drain the cerebro spinal fluid.
2) Craniotomy:=
- If hematoma and tumor are present, then craniotomy is performed है.
Explain the Nursing management of patients with the increased intracranial pressure.
- Do a neurological assessment of the patient.
- Properly assess the patient using the Glass Coma Scale (GCS).
- Continuously monitor the patient’s vital signs.
- Properly assess the patient’s vital signs including blood pressure, respiratory status, temperature, heart rate.
- Properly elevate the patient’s head at a 30° angle.
- Advise the patient to avoid activities that increase intracranial pressure.
- The patient Provide proper oxygen and ventilation.
- Properly monitor the patient’s fluid and electrolyte levels.
- Properly provide antiepileptic medicine if the patient has a seizure condition.
- Properly position the patient and provide comfort measures.
- Maintain the patient’s body temperature normal.
- Keep the patient’s neck in a neutral position.
- Provide a quiet environment for the patient.
- Do not restrain the patient as this plays an important role in increasing intracranial pressure.
- Keep the patient’s airway properly patent.
- Provide chest physiotherapy and postural drainage to remove secretions.
- Properly maintain the patient’s body fluid and electrolyte balance.
- Properly provide antibiotic medication to the patient to prevent infection.
- Maintain strict aseptic technique when performing nursing activities to prevent infection.
- Advise the patient to follow up properly.
- Properly Giving advice on taking medication.
Explain/Define the intracranial surgery. Define intracranial surgery.
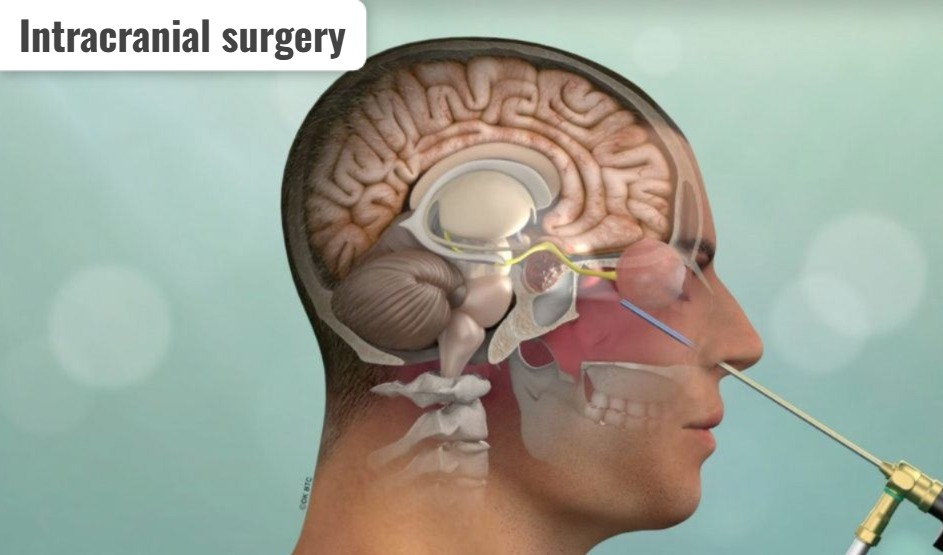
- Intracranial surgery is a surgical procedure that is performed in the cranial cavity.
- In this type of surgery, any type of surgical procedure is performed in the brain.
- Intracranial surgery is performed for different purposes.
- Intracranial surgery is performed to remove tumors, vascular abnormalities, structural problems, etc.
Burr Hole surgery:=
- Burr hole surgery is a type of neurological procedure in which a small hole is made in the skull, usually using a specialized drill called a burr.
- This surgical procedure is used to access the brain and treat a variety of neurological conditions.
- Burr hole surgery is also performed to remove blood and fluid from the brain.
Craniotomy:
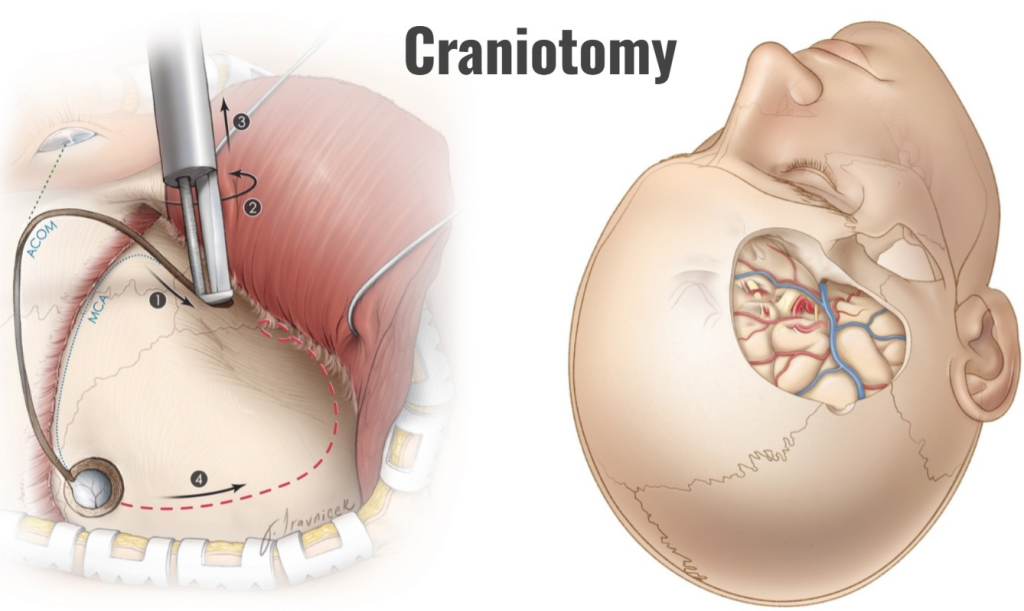
- A craniotomy is a surgical procedure in which a small section of the skull bone is surgically removed, primarily to gain access to the intracranial compartment. But in this procedure, the bone flap that is removed is mainly replaced in its position after the operation.
Craniectomy (craniectomy) :=
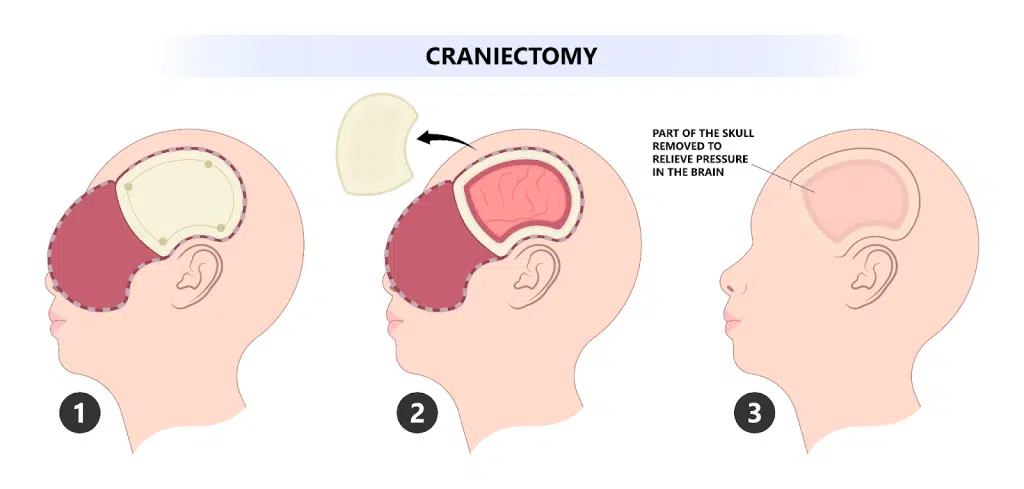
- In craniectomy, the bone flap is removed but not replaced.
Explain the indication of the intracranial surgery.
- Due to having a brain tumor.
- Due to vascular abnormality.
- Due to cerebral aneurysm.
- Due to traumatic brain injury.
- Due to the condition of epilepsy.
- Due to intracranial hemorrhage. Due to.
- Due to hydrocephalus.
- Due to cranial nerve disorders.
- Due to meningiomas.
- Due to functional neurosurgery.
- Due to intracranial infection.
- Skull fracture Due to.
- Due to hematoma.
Explain the pre operative teaching to the patient and family.
- Properly assess the patient’s blood test.
- Patient’s Perform proper radiological tests.
- Explain the complete procedure to the patient, including the estimated length of anesthesia and procedure, and the recovery period.
- Provide the patient with complete information about post-operative procedures such as dressings, catheters, ET tubes, intravenous fluids, and pain management.
- Properly obtain consent before performing surgery.
- Prepare the operative area Prepare properly.
- Properly monitor the patient’s vital signs.
Explain the post operative management of the patient with the intracranial surgery.
- Assess the patient’s neurological status every 30 minutes for the first 24-48 hours.
- Assess the patient’s vital signs frequently.
- The patient’s bed is 30 Keep the patient’s neck elevated at a 45 degree angle.
- Keep the patient’s neck in a neutral position.
- Advise the patient to prevent head movement.
- Keep the patient away from painful stimuli.
- Take measures to prevent the patient from constipation.
- The patient Do not restrain.
- Provide analgesic medicine if the patient is in pain.
- Check the patient’s drainage and follow strict sterile technique.
- Properly suction the patient.
- Monitor the patient’s fluid and electrolyte balance.
- Monitor the patient’s nutritional status. Do.
- If the patient is conscious, provide oral fluids.
- Advise the patient to do range of motion exercises.
- If the patient has a seizure condition, keep the side rails up.
- Advise the patient to maintain proper personal hygiene.
- Properly wash the patient Provide rehabilitation therapy, Like:= Speech therapy, Physical therapy etc.
- Provide proper psychological support to the patient and his family members.
Explain/ Define headache. (Define a headache.)

- A headache is a pain in the head. Which mainly causes pain above the eyes and ears, behind the head (occipital) and back of the upper neck.
- Headache is also called cephalalgia.
- The word cephalalgia comes from the Greek. “Kephale meaning ” HEAD”, Algos meaning” PAIN “
- Cephalalgia meaning head pain.
- Headache means discomfort in the head, neck and scalp.
- Headache is the most common complaint seen in people and the severity, intensity and duration of headache also differ from person to person.
Explain the Etiology/ cause of the of the Headache. (Explain the cause of the headache)
Tension headache
- Muscle tension,
- Due to stress.
Migraine
- Genetics,
- Neurological factors,
- Triggers (due to changes in food),
- Lack of sleep,
- Environmental
- Simulation),
Cluster Headache
- Due to hypothalamic activation, vasodilation.
- Due to intracranial infection,
- Due to head injury,
- Due to bacterial and viral meningitis,
- Acute systemic Due to infection,
- Due to severe hypertension,
- Due to intracranial tumors,
- Acute and chronic diseases of the eye, ear, nose and throat.
- Headaches are seen due to various reasons such as fever, anxiety, working for long hours, getting less sleep, etc.
Explain the Classification of the Headache.
Headache is mainly divided into three categories.
- 1) Primary Headache,
- 2) Secondary Headache,
- 3) Cranial Neuralgia, Facial Pain and Other Headaches
1) Primary Headache,
- Primary headaches involve 1) Migraine, 2) Tension headache and 3) Cluster headache.
2) Secondary Headache,
- Secondary headaches are mainly caused by any structural problem in the head and neck.
3) Cranial Neuralgia, Facial Pain and Other Headaches
- Cranial neuralgia means that if a headache occurs due to inflammation of the nerves in the head and neck or a problem in its structure, it is called cranial neuralgia.
- In this type, headaches occur due to different reasons.
- Thus, there are mainly three classifications of headache.
Primary Headache
A) Explain/Define Migraine Headache.

- 20% of all headaches are migraines.
- Migraine is mainly caused by the constriction of blood vessels in the head and neck, which prevents proper blood flow to the head.
- Migraine headaches can occur on one side of the head or on both sides of the head.
- Migraine-type headaches are more common in females than males.
- Migraine is mainly caused by anatomical and nervous system dysfunction.
Explain the Etiology/ cause of the migraine headache.
- Due to genetic factors,
- Neuro transmitter imbalance Due to,
- Vascular changes,
- Hormonal fluctuations,
- Environmental stimuli,
- Family history of migraine.
- Prolonged muscle tension and stress.
- Due to alcohol use,
- Due to smoking,
- Due to tobacco consumption,
- Due to insufficient sleep,
- For women := menstrual period and use of oral contraceptives.
Explain the Classification of the migraine.
1) Migraine with the aura (classic migraine)
- This classic migraine is characterized by a headache and visual disturbances, motor function and sensory function disturbances. In this, symptoms are mainly seen for a few minutes and even hours.
2) Migraine without aura (common migraine)
- Moderate to severe pulsating headache pain is seen in this type of migraine.
- This type of pain is mainly seen on one side of the head.
- It has other symptoms like nausea, vomiting, photophobia ( Sensitivity to light)
- Phonophonia ( Sensitivity to sound) is seen.
Explain the Clinical manifestation/ sign and symptoms of the patient with the .Migraine Headache.
- Headache.
- Quality := Thrombosing pulsating pain,
- Location := Usually on one side of the head, but sometimes pain is seen on both sides.
Intensity:= Moderate to severe. - Headache is accompanied by nausea, vomiting, dizziness and visual disturbances.
- Photophobia (Sensitivity to light),
- Phonophobia (Sensitivity to sound),
- Osmophobia (smell sensitivity)
- Sensitivity to light and noise.
- Paresthesia (abnormal sensation).
- Diplopia and blurred vision Occur.
- Irritability.
- Restlessness.
- Fatigue.
- Changes in mood.
Explain the management of the patient with the migraine headache. (Describe the management of a patient with migraine headache.)
- If the patient is in pain, provide analgesic medicine.
- Like:= Acetaminophen, Ibuprofen, Aspirine.
- If the patient has an inflammatory condition, provide triptans group medicine.
Ex:=sumatriptan, Rizatriptan, - If the patient is in pain, provide analgesic medicine. If there is a condition of vomiting, provide antiemetic medicine to the patient.
- Provide the patient with a properly quiet and dark room.
- Advise the patient to make proper lifestyle modifications such as avoiding caffeine rich foods.
- Advise the patient to get regular sleep.
- Maintain the patient’s hydration status properly.
- If the patient has a condition of stress, then advise him to do proper meditation, yoga.
- Advise the patient to do regular exercise.
- If the patient has severe migraine, then the patient should be given beta blockers, calcium channel blockers,
- Provide anti-depression medicine, anti-convulsive medicine.
- If If the patient has a chronic migraine condition, provide botulinum toxin injection.
- Advise the patient to avoid smoking.
- Advise the patient to avoid tyramine rich food.
B) Explain / Define tension Headache. (Define tension headache.)
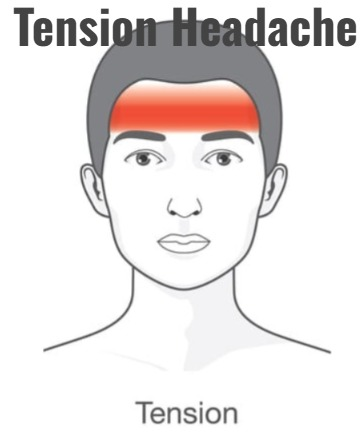
- Tension headache is the most common type of primary headache.
- This type of headache is mainly caused by contraction of the head and neck muscles.
- Tension headaches are also seen due to emotional crises and intense worry.
- This type of headache is also seen mainly in people who have depression and anxiety.
Explain the etiology/cause of the tension headache. (Tell the reasons for tension headaches.)
- Due to muscles contraction.
- Due to stress and anxiety.
- Due to environmental factors.
- Due to sleep pattern disturbance.
- Eye strain.
- Due to tobacco and alcohol use.
- Due to hormonal changes.
- Due to excessive caffeine intake.
- Excessive smoking.
- Due to nasal congestion.
- Due to sinus infection.
Explain the clinical manifestation/sign and symptoms of the patient with the tension headache. ( State the symptoms and signs of tension headache.)
- Headache.
- Muscle tenderness.
- Sensitivity to light and sound.
- Muscle tightening.
- Feeling of pain in the head and neck To be.
Explain the diagnostic evaluation of the patient with the tension headache. (Describe the diagnostic evaluation of a patient with tension headache.)
- history taking and physical examination.
- Neurological examination.
- CT scan.
- MRI.
- Blood test.
Explain the management of the patient with the tension headache. (Describe the management of a patient with tension headache.)
- Advise the patient to get adequate sleep.
- Advise the patient to take a balanced diet.
- Advise the patient to exercise regularly.
- Advise the patient to take stress relaxation techniques.
- Advise the patient for muscle relaxation.
- Provide non-steroidal anti-inflammatory drugs to relieve the patient’s pain.
- Advise the patient for muscle relaxant techniques.
- Provide proper psychological support to the patient.
C). Explain/Define cluster headache. (Define cluster header.)
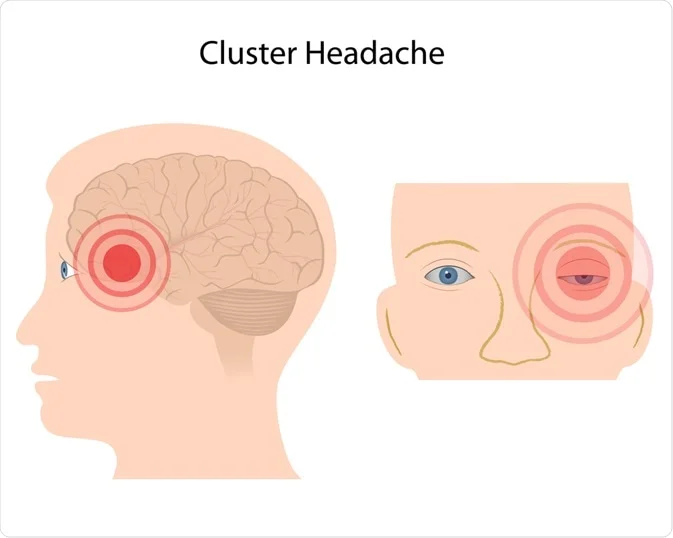
- A cluster headache is a one-sided headache that can also be accompanied by tearing in the eyes and stuffiness.
- A cluster headache is a chronic and repeated headache.
- A cluster headache can last from a few minutes to a few hours.
- But cluster headaches can last from 45 to 90 minutes.
- A cluster headache is a The most common type is painful headache.
Explain the Etiology/cause of the cluster headache.
- Hypothalamic involvement.
- Due to vascular changes.
- Neurotransmitter imbalance Due to.
- Due to genetic factors.
- Due to taking certain medicines.
- Due to interruption in normal sleep patterns.
- Due to imbalance of certain hormones.
- Due to alcohol and cigarette smoking.
- High Due to altitude.
- Due to cocaine consumption.
Explain the Clinical manifestation/ sign and symptoms of the patient with the cluster headache. (Describe the symptoms and signs of a patient with cluster headache.)
- Severe pain.
- Eyelid tearing, redness and drooping.
- Nasal congestion.
- Restlessness.
- Severe sudden, Burning, throbbing, and steady headache.
- Pain and cluster headaches are short-lived, usually lasting 30 to 90 minutes.
- Swelling around the eyes.
- Rhinorrhea (runny nose)
- Red and flushed face.
Explain the Diagnostic evaluation of the patient with the cluster headache.
- history tacking and physical examination.
- imaging studies.
- CT scan.
- M. R.I.
- Blood test.
Explain the management of the patient with the cluster headache. (Describe the management of a patient with cluster headache.)
- Provide the patient with adequate amount of oxygen.
- Provide the patient with sumatriptan medication.
- Provide the patient with verapamil, lithium, divalproex sodium, prednisone, and ergotamine tartrate medication to prevent cluster headache.
- Provide the patient with proper work and comfortable environment Provide.
- Provide proper psychological support to the patient.
- Provide a calm and comfortable environment to the patient.
- Provide proper mind diversional therapy to the patient.
2). Explain/Define secondary headache. (Define secondary headache.)
- Secondary headaches are mainly caused by any structural problem in the head and neck.
- Overall, headaches are mainly caused by sinus infections, head injuries, medication side effects, bleeding in the brain, tumors, meningitis, and encephalitis.
Explain the etiology/cause of the secondary headache. (Tell the cause of secondary headache.)
- Due to infection,
- Due to trauma,
- Due to vascular disorder,
- Due to medication overuse,
- Due to structural issues.
- Due to metabolic disorders.
- Due to inflammatory conditions.
- Due to exposure.
- Due to neurological disorders.
- Due to endocrine disorders.
Explain the clinical manifestation / sign and symptoms of the patient with the secondary headache. ( State the symptoms and signs of a patient with a headache.)
- Headache has different qualities such as severity, location, type etc.
- The patient may experience different neurological symptoms such as dizziness, visual disturbances, weakness.
- The frequency and duration of headaches are different.
- Fever Come.
- Sinus congestion.
- Joint pain.
- Neurological disorders.
- Fatigue.
- Weight loss.
- Appetite changes.
- Nausea and vomiting.
- Photophobia.
- Stiff neck.
- Fever.
- Changes in vision.
- Altered mental status.
- Occurrence.
- Facial pain.
- Slip disturbance.
- Hormonal changes.
Explain the Diagnostic evaluation of the patient with the secondary headache. (Describe the diagnostic evaluation of a patient with secondary headache.)
- history taking and physical examination.
- Blood test.
- Imaging studies.
- CT scan.
- MRI.
- Lumbar Puncture .
- Electroencephalogram.
- Hormonal Tests.
- Allergy Testing.
- Medication History Review.
- Eye Examination.
Explain the management of the patient with the secondary headache. (Describe the management of a patient with secondary headache.)
- If the patient has an infection, provide antibiotic medicine.
- Provide analgesic medicine to the patient for pain management.
- Provide antiepileptic medication to the patient.
- Anti-inflammatory to reduce the patient’s inflammation Provide.
- Provide corticosteroid medicine to reduce the patient’s inflammation.
- Advise the patient to make lifestyle modifications.
- Provide physical therapy to the patient.
- Advise the patient to have regular follow-up.
- Provide proper Provide medication.
- Provide the patient with work and a comfortable environment.
Explain/Define seizures. (Define seizures.)

- Seizures are a condition in which the electrical activity of the brain becomes uncontrolled. Seizures
- Seizures are a condition in which uncontrolled electrical activity occurs in the brain, which is called seizures.
- If uncontrolled electrical activity occurs in the brain, the normal function of the brain is impaired and due to this, a particular situation arises, which is called seizures. is.
Explain/ Define the epilepsy(Define epilepsy)
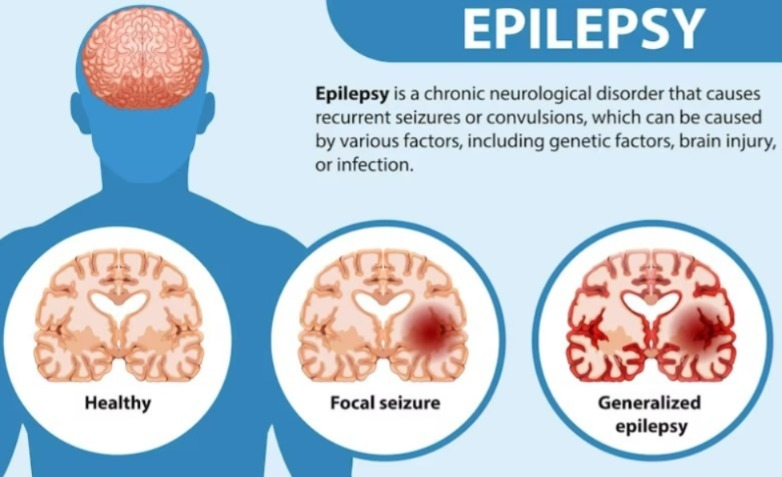
- If a person has frequent episodes of seizures, then that condition converts to epilepsy.
- Epilepsy is a mental abnormality in which the electrical impulses of neurons in a person’s brain are greatly disturbed, due to which abnormal electrical activity is seen in the neurons and the condition of epilepsy occurs, due to which jerking moments arise in the body.
Explain the Etiology/ cause of the seizures. (Explain the Etiology/ cause of the seizures.)
- Due to genetic factors.
- Due to head trauma.
- Due to brain tumor.
- Stroke .
- Due to alcohol withdrawal.
- Due to brain infection.ex:= meningitis.
- Due to drug abuse and withdrawal.
- Due to hypoglycemia.
- Due to hypoxia.
- Due to dehydration.
- Due to fever.
- Due to high blood pressure.
- Due to septicemia.
- Due to diabetes mellitus.
- Due to electric shock.
- Due to birth injury.
- Due to developmental disorder.
- Due to traumatic brain injury.
- Due to brain tumor.
- Due to exposure to any poisonous substance, Ex:= lead, carbon monoxide.
Explain the Classification of the seizures.
Seizures are mainly classified into three types.
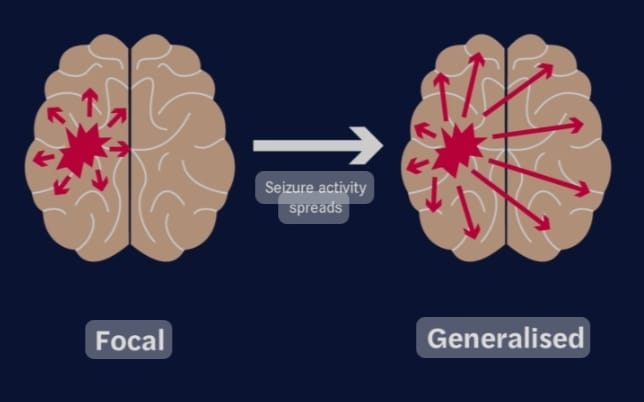
- A) General seizures (general seizures)
- B) Partial or focal onset seizures. (Partial and focal onset seizures.)
- C) Psychogenic seizures
A) General seizures
There are six more types of general seizures.
- 1) Tonic-clonic seizure.
- 2) Absent seizure.
- 3) Myoclonic seizure.
- 4) Tonic seizure.
- 5) Atonic seizure.
- 6) Clonic seizure.
B) Partial or focal onset seizures.
There are two more types of partial and focal onset seizures.
- 1) Simple focal seizure.
- 2) Complex focal seizure.
C) Psychogenic seizures ( Psychogenic seizures)
A) General seizures (General seizures)
- There are six types of generalized seizures.
- In generalized seizures, both the hemispheres of the brain, i.e. the right and left hemispheres, are involved, i.e. uncontrolled electrical discharges occur in both the hemispheres of the brain.
- In this type of seizure, the patient becomes unconscious.
- These seizures last from a few seconds to a few minutes.
1) Tonic – clonic seizures.
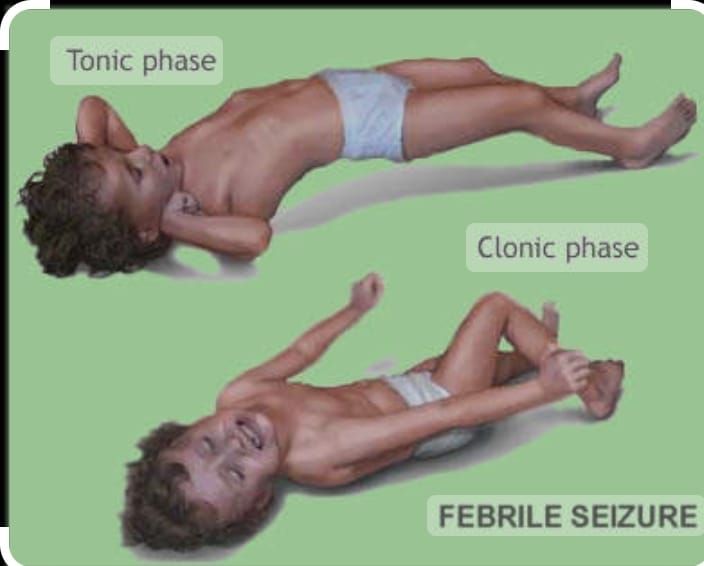
- Tonic clonic seizures are also called grandmother seizures.
- In this seizure, the patient’s consciousness is completely lost. And the patient also falls to the ground.
- In the tonic stage, the patient’s muscles stiffen and muscle tone increases.
- In the clonic phase, the patient’s muscle tone is lost.
2) Absence seizure.

- Absence seizures are also called petitmal seizures.
- This type of seizure is mainly seen in children.
- These seizures are seen only for a few seconds.
- In these seizures, the patient experiences episodes lasting only a few seconds and the patient does not even realize that he has any kind of issue.
3) Myoclonic seizures.

- Myoclonic seizures involve the muscles and involve excessive jerking movements of the body. Therefore, in myoclonic seizures, excessive jerking of the body is observed.
4) Tonic seizures.
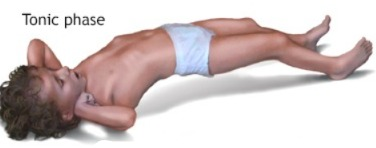
- In this seizure, muscle tone suddenly increases and the body becomes stiff and muscle tone increases greatly.
5) Atonic seizure.
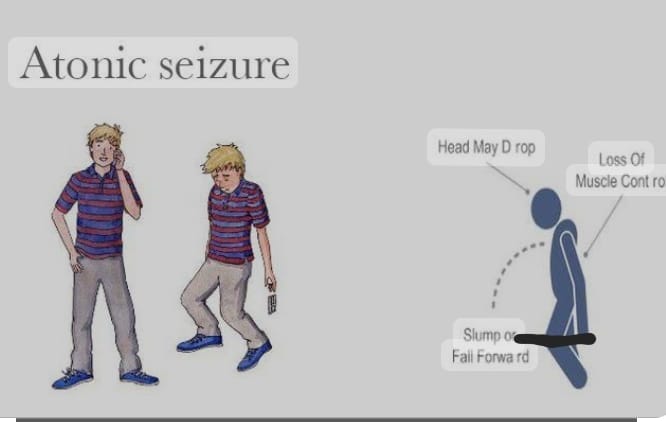
- In this seizure, muscle tone is lost, so a drop attack is seen in this, that is, the patient falls down because in this seizure, the patient’s muscle tone suddenly stops. In this seizure, the patient suddenly regains consciousness after having a drop attack. In this seizure, the patient is at high risk of head injury.
6) Clonic seizure.
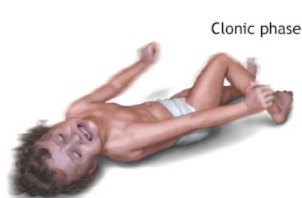
- In this seizure, the patient’s muscle tone is suddenly lost. In this, the person appears unconscious and his muscle tone is also lost. In this seizure, jerking moment of the limb and jerking moment of the extremities are seen.
B) Partial or focal onset seizures. (Partial and Focal Onset Seizures.)
- These seizures are also called partial focal seizures and partial seizures.
- These seizures involve one side of the hemisphere.
- Therefore, whatever body activity is regulated by the involved hemisphere, the affection is seen.
- There are two types of partial and focal onset seizures.
1) Simple focal seizure.
- In this type of seizure, the patient feels conscious but experiences unusual feelings and sensations.
- In this type of seizure, the person may feel very happy, very angry, or Feelings of sudden sadness or nausea occur suddenly and without any reason.
This seizure involves only one hemisphere, so the person feels things that are not there in reality.
2) Complex focal seizure.
- In this seizure, the patient’s level of consciousness is altered or lost.
- In this seizure, the person experiences a dream-like experience.
- In this type of seizure, the person does not even remember the work properly. It is called complex focal seizure.
C) Psychogenic seizures
- These seizures are also called pseudo seizures.
- These seizures are mainly seen due to psychiatric conditions.
In these seizures, the person feels like he is having a seizure but it is not actually happening.
Explain the Clinical manifestation/ sign and symptoms of seizure.
- Temporary confusion.
- Uncontrolled jerking of the arms and legs.
- Loss of consciousness.
- Loss of awareness.
- Temporary confusion is observed.
- In the body Numbness.
- Loss of memory.
- Visual changes.
- Dizziness.
- Tingling sensation in the chest.
Explain the Diagnostic evaluation of the patient with the seizures. (Describe the diagnostic evaluation of a patient with seizures.)
- History taking and physical examination.
- Blood test.
- Lumbar puncture.
- Electroencephalogram.
- Computerized tomography (CT) scan).
- Magnetic resonance imaging ( MRI ).
- Positron emission tomography ( PET test).
- Single photo emission computerized tomography ( SPECT ).
- Neuropsychological tests.
- Brain mapping.
Explain the medical management of the patient with the seizures .
If the patient has a condition of seizures, then provide anticonvulsant medication.
1) Provide Phenytoin sodium medication to the patient.
If the patient has partial and generalized seizures, then phenytoin Provide medication.
This medication is mainly used when there is a condition of cardiac dysrhythmia or some types of nerve pain.
2) Provide carbamazepine medication to the patient.
Carbamazepine is mainly used for partial and generalized seizures.
Carbamazepine decreases synaptic transmission in the central nervous system.
3) Administer valporic acid medication to the patient.
Valporic acid is used for partial and generalized seizures.
Valporic acid increases GABA.
4) Ethosuxamide := This medication is mainly used for absence seizures.
5) Diazepam = Diazepam medication mainly works as a sedative. Which is mainly used in generalized seizures (Absence, Atonic, Myoclonic).
Explain the Surgical management of patients with seizures. (Explain the surgical management of Caesarean section patient.)
- Surgery is mainly performed for patients who have suffered from any intracranial tumor, cyst, abscess and vascular abnormality.
1) Resective and palliative operations:=
- If the electrical activity inside the brain increases To treat the signs and symptoms of a stroke, the part of the brain that is causing the increased electrical activity is resected.
2) Temporal Lobectomy:
- If the seizure is mainly caused by the temporal lobes, then the temporal lobe is removed.
3) Corpus Callosum.
- If the seizure is caused by the corpus callosum, then the affected part is removed.
4) Extratemporal resection
- In this, if the seizure is mainly caused by the temporal lobe, then the temporal lobe is resected.
5) Hemispherectomy :=
- If the seizure is caused by any hemisphere, then its part is removed.
Explain the Nursing management of patients with the seizures. (Explain the nursing management of a patient with Caesarean section.)
- Maintain a properly safe environment to prevent the patient from injury.
- Keep the side rails up to prevent the patient from injury.
- Do not put anything in the patient’s mouth.
- If the patient is wearing anything around his neck, loosen it.
- Do not provide restraint to the patient, which may prevent injury.
- Provide a small pillow under the patient’s head.
- If the patient is vomiting, take proper care to prevent aspiration.
- Keep suction readily available.
- Keep the patient’s airway patent, which may allow for proper breathing. Can.
- Advise the patient to take proper bed rest.
- Advise the patient to take a special ketogenic diet, which mainly keeps the amount of carbohydrates low and provides a high amount of fiber, minerals, and protein.
- Provide the patient with intravenous fluids.
- Provide oxygen therapy to the patient.
- Provide the patient with proper work and a comfortable environment.
- Advise the patient to take medication properly.
Explain/ Define status epilepticus. (Define status epilepticus.)
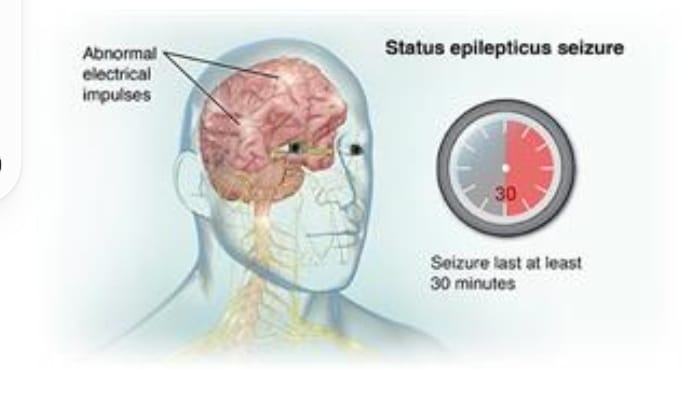
- Status epilepticus is a medical emergency. In which continuous, prolonged, recurrent seizures are seen.
- If the patient experiences prolonged, continuous and repetitive seizures i.e. seizures lasting more than 5 minutes without any gap between them, then it is called status epilepticus.
Explain the Etiology/ cause of the patient with the status epilepticus. (Explain the cause of the patient with status epilepticus.)
- Due to brain injury.
- Due to infection.
- Due to metabolic imbalance.
- Due to drug withdrawal.
- Due to stroke.
- Due to certain types of medication.
- Due to sudden anticonvulsant drug withdrawal.
- Due to any infection in the central nervous system.
- Encephalitis,
- Meningitis,
- Due to conditions of hypoxia.
- Any type of psychiatric Because of the condition.
Explain the clinical manifestation/sign and symptoms of the patient with the status epilepticus. (Describe the symptoms and signs of a patient with status epilepticus.)
- Prolonged and repetitive seizures.
- Loss of consciousness.
- Convulsions.
- Muscle rigidity.
- Changes in breathing pattern Occur.
- Altered mental status.
- Confusion.
- Behavior changes.
- Loss of bowel and bladder control.
Explain the Diagnostic evaluation of the patient with the status epilepticus. Explain the diagnostic evaluation of an epileptic patient.)
- History tacking and physical examination.
- Electroencephalogram.
- Blood test.
- Imaging studies. Computed tomography (CT scan).
- Magnetic resonance Imaging ( MRI ).
- Lumbar Puncture.
- Complete Blood Count ( CBC Test).
- Serum Electrolyte Test .
- Assess calcium level.
- Assess the Megnesium level.
- Assess the Creatinine level.
- Assess the Blood Urea Nitrogen ( BUN ) Level.
- Assess the Liver Function Test ( LFT ).
- Assess the Arterial Blood Gas Analysis ( ABG Level).
- Urine Test.
Explain the medical management of the patient with the status epilepticus. (Describe the medical management of a patient with status epilepticus.)
- Provide the patient with anti-epileptic drugs. Ex:= Phenytoin sodium,
- Provide the patient with sedative medication. Ex:= Diazepam.
- Continuously monitor the patient’s vital signs.
- Keep the patient’s airway properly patent.
- Continuously monitor the patient.
- Advise the patient to modify their lifestyle.
- Provide a properly safe environment for the patient. To do.
Explain the nursing management of patients with status epilepticus. (Explain the nursing management of a patient with status epilepticus.)
- Continuously monitor the patient’s vital signs.
- Keep the patient’s airway properly patent.
- Properly provide oxygen to the patient.
- Properly document the type of seizures the patient has and how long they last.
- Properly provide medication to the patient.
- Properly provide safety measures to the patient.
- Properly provide information to the patient and his family members about the patient’s condition.
- Properly provide emotional support to the patient and his family members.
- Other health care for the patient’s care Collaborate properly with personnel.
- Provide a properly safe environment to the patient.
- Provide a properly working and comfortable environment to the patient.
- Advise the patient to take medication properly.
- Advise the patient to follow up regularly.
