ENGLISH-endocrine disorder (part-4)(deepali)(UPLOAD)
Explain the management of patients with the hepatic disorder :
1) explain/define the jaundice (Define jaundice.)
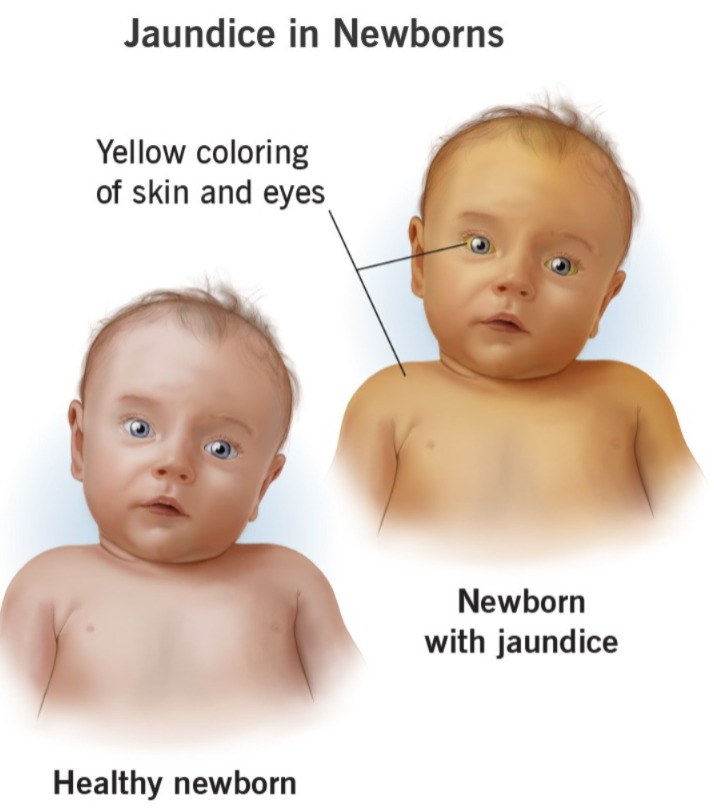
- => Jaundice is also called icterus.
- => Jaundice is not a disease but it is seen as a sign of disease after many diseases.
- => Jaundice is a condition in which the skin, mucous membrane, and sclera of the body become yellow in color due to an increase in the amount of bilirubin in the body. It is called jaundice.
- => Jaundice occurs when the amount of bilirubin in the body increases above 2.5 mg/dl. The condition of jaundice is seen.
- (Note:=normal bilirubin level is 0.3 to 1.0 mg/dl.)
- ( In jaundice := level of bilirubin is exced 2.5 mg/dl)
- { direct/unconjugated/fat soluable bilirubin level is 0.1 -0.3 mg/dl.}
- { indirect/conjugated / water soluable billirubin level is 0.2-0.8mg/dl.}
- => Bilirubin is a natural product that is released as a byproduct of the breakdown of red blood cells and is excreted out of the body by the liver.
- => The condition of jaundice arises when the amount of conjugated bilirubin is not excreted from the body by the liver using the biliary system and the bilirubin accumulates in the body, due to which the condition of jaundice arises.
2)explain the type of jaundice. (Describe the types of jaundice.)

There are four types of jaundice in total:=
types:=
- 1)hemolytic jaundice,
- 2)obstructive jaundice,
- 3)hepatocellular jaundice ( Hepatocellular jaundice)
- 4) hereditary jaundice
1)hemolytic jaundice,
- => HEMO MEANS:= “BLOOD,”
- => LYTIC MEANS:= “BREAKDOWN OF CELL”
- => “HEMO LYTIC MEANS := “BREAKDOWN OF RED BLOOD CELL”
- => Hemolytic jaundice is also called pre hepatic jaundice.
- => In this jaundice, the level of bilirubin is raised due to excessive breakdown of red blood cells.
=>some common causes of hemolytic jaundice are:
- Sickle cell anemia,
- Transfusion reaction,
- Malaria,
- Thalassemia,
- Autoimmune disorder.
2) Obstructive jaundice ( Obstructive jaundice) ,
- =>Obstructive jaundice is called extra hepatic type of jaundice.
- => Obstructive jaundice occurs when there is bile duct blockage and bilirubin is not excreted from the liver and remains in the liver.
- => Therefore it is called cholestatic jaundice because due to obstruction of bile duct, bilirubin cannot be excreted from the liver. No.
- => Obstructive jaundice causes extreme levels of itching in the body because salt builds up in the body.
Some of the common causes of obstructive jaundice :=
- Due to carcinoma in the gallbladder and bile duct,
- Gallstones in the biliary system stones) due to the presence of,
- Infection and inflammation.
3) Hepatocellular jaundice (Hepatocellular jaundice)
- => Hepatocellular jaundice is called the most common type of jaundice.
- => Hepatocellular jaundice occurs when the liver cells are damaged for any reason, due to which the liver is unable to excrete bilirubin from the body and due to this, bilirubin increases in the blood.
Hepatocellular jaundice is mainly
- Liver failure,
- Liver disease,
- Liver cancer,
- Hepatitis,
- Viruses such as,
- Yellow fever,
- Epstein Barr virus, caused by certain types of drugs.
4)Hereditary jaundice (Hereditary jaundice)
- => Hereditary jaundice is mainly seen in any person from his family in a hereditary way.
- => Hereditary jaundice is mainly due to impairment in bilirubin metabolism from birth itself, which causes excessive accumulation of bilirubin in the body.
- => It mainly occurs when excessive production of bilirubin or It occurs due to the body not being able to excrete it.
1) Dubin/Johnson syndrome
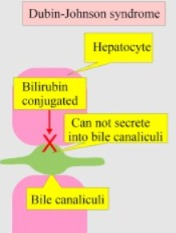
- => This is an inherited disorder.
- => In this jaundice, the level of conjugated bilirubin increases in the liver.
2)Gilbert’s syndrome
- => Gilbert’s syndrome is an inherited condition that is mainly caused by benign conditions in which the level of bilirubin increases to a mild level.
3) Rotor’s syndrome
- => This is an inherited disease in which intermittent jaundice is seen.
3)explain the causes/Etiology of jaundice. Explain the causes of jaundice
- Due to excessive amount of bilirubin in the body.
- Due to any abnormality of liver cells.
- Due to blockage of bile duct.
- Due to inflammation in liver and bile duct.
These are some common conditions that can cause jaundice
1)pre hepatic cause (before bile is made in liver)
- => Due to the destruction of red blood cells,
- => Conditions in which red blood cells break down such as:=
•Malaria,
•Sickle cell anemia,
•Thalassemia,
•Glucose 6 phosphate,
•Drugs and other toxins,
•Autoimmune disorders.
2)hepatic ( the problem arising in the liver)
- => Hepatic jaundice is mainly seen when there is an inability of the liver to produce the condition of jaundice.
- => Due to hepatitis (alcoholic or viral),
=> Cirrhosis of the liver,
=> Due to certain types of drugs,
=> Gilbert’s syndrome,
=> Cancer
3)post -hepatic jaundice ( after bile has been made in the liver)
- => This is mainly seen due to any obstruction.
- => Due to gallstones.
- => Due to cancer.
- => Due to stricture of the bile duct.
- => Cholangitis.
- =>pancreatitis.
4)explain the Clinical manifestation/sign and symptoms of jaundice. Explain the Clinical manifestation/sign and symptoms of jaundice
- A yellowish discolouration of the skin, membrane and sclera is seen in the body.
- Stool appears light colored.
- yellowish brown colored urine.
- Itchy skin.
- Fatigue.
- Abdominal pain.
- nausea.
- Vomiting.
- Fever.
- Weakness.
- Loss of appetite.
- Headache.
- Confusion.
- Swelling in the legs and abdomen.
- Loss of appetite. feel.
5)Explain the diagnostic evaluation of jaundice. Write the diagnostic evaluation of jaundice
- History taking and physical examination.
- blood test.
- Complete blood count test.
- liver function test.
- urinalysis.
- Liver Biopsy.
- Imaging studying.
- ct scan.
- MRI.
- abdomonal ultrasonography.
- hepatitis A,B,c test.
6)explain the management of jaundice. (Write the management of jaundice)
- Provide intravenous fluids to the patient to prevent dehydration.
- Provide antiemetic medicine if the patient is experiencing nausea and vomiting.
- Provide analgesic medicine if the patient is experiencing pain.
- Provide antibiotic medicine if the patient has any bacterial infection.
- Provide antiviral medicine to the patient.
- Provide blood transfusion when the patient needs it.
- Provide chemotherapy and radiation therapy to the patient.
- Provide phototherapy if there is a newborn.
- Provide steroids and immunoglobulin to the patient.
- Provide the patient with a high carbohydrate and low protein diet.
- Provide nutritional supplementation to the patient.
- Provide vitamin K injection to prevent bleeding.
- Any drugs, toxic chemicals, and alcohol can cause jaundice, so avoid these things.
7) Explain the surgical management of patients with jaundice. Explain the surgical management of a patient with jaundice.
- If there is a cancer condition, then surgical treatment is required.
- If the condition of jaundice is due to obstruction of the bile duct, then it should be opened surgically.
- Many times, liver transplantation is also required.
- If the patient has gallstones, then surgery to remove them is required. To do.
- If the patient has hemolytic jaundice, then provide him with medication and give him treatment.
8)explain nursing management of patients with jaundice. Write the nursing management of a patient with jaundice.
- Advise the patient to drink plenty of fluids.
- Ask the patient to take adequate rest.
- Tell the patient to avoid things like coffee, alcohol, junk food, soda drinks, etc.
- Encourage the patient to eat fruits and vegetables Tell.
- Avoid foods that contain preservatives.
- Ask the patient to avoid meat and animal fats.
- Tell the patient not to take dairy products like cheese, milk, etc.
- Ask the patient not to take fats like ghee, butter, cream, oil for 2 weeks.
- According to the patient’s condition, soybeans, Egg,. Dale, Milk should be provided in small quantities.
- Ask the patient to take carbohydrate-rich food like roti, bread, boiled potato etc. in small quantities.
- Take medicine as prescribed by the health care personnel.
1)Explain/define the hepatic cirrhosis (Hepatic cirrhosis definition.)
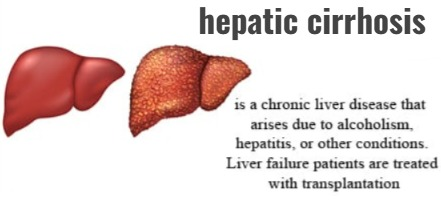
- => Hepatic cirrhosis is a chronic, degenerative disease in which normal liver cells are damaged and fibrous scar tissues form in the liver.
- => Scar tissues form instead of healthy liver tissues, which blocks blood flow to the liver and prevents the liver from functioning properly, leading to liver failure.
- => Liver is distorted, hardened and lumpy.
2) Explain the classification of hepatic cirrhosis. (Describe the classification of hepatic cirrhosis.
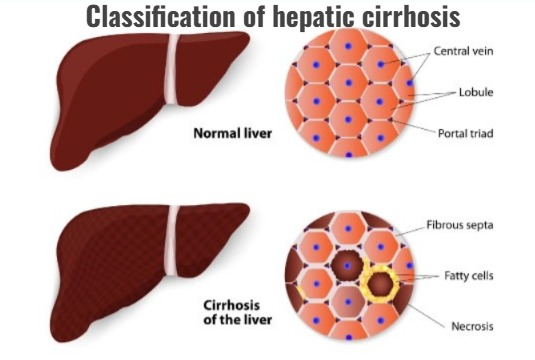
- 1) Alcoholic cirrhosis
- 2)Post necrotic cirrhosis (Post necrotic cirrhosis)
- 3)Billiary cirrhosis (Biliary cirrhosis)
1)Alcoholic cirrhosis (Alcoholic cirrhosis)
- => Alcoholic cirrhosis is called Laennec’s cirrhosis and is the most common type of cirrhosis.
- => This cirrhosis is mainly caused by hepatitis C and chronic alcohol use.
- => In this, the liver is damaged mainly due to malnutrition and chronic alcohol consumption.
- => In this type of cirrhosis, fibrous tissues form around the portal area and central veins.
2) Post necrotic cirrhosis
- => Post necrotic cirrhosis is mainly caused by any toxic agent, and viral hepatitis.
- => This causes liver cell damage, which is called post-necrosis cirrhosis.
- => Post-necrosis cirrhosis is seen in 10-30% of patients.
3)Billiary cirrhosis (Biliary cirrhosis)
- => Biliary cirrhosis is a chronic disease. Which is mainly seen due to inflammation of the bile duct in the liver.
- => In biliary cirrhosis, fibrous tissue and scar formation occurs around the bile duct of the liver.
- => This causes chronic obstruction of the bile duct
3)explain the Etiology of hepatic cirrhosis.Explain the causes of hepatic cirrhosis
- Due to long-term alcohol consumption.
- Due to chronic hepatitis.
- Due to obesity.
- Due to Wilson’s disease.
- Due to cystic fibrosis.
- Bile duct blockage Due to.
- Autoimmune hepatitis.
- Toxic hepatitis.
- Chronic congestive heart failure.
- Non-alcoholic fatty liver disease.
- Biliary atresia.
- In the gallbladder Due to surgery.
- Due to glycogen storage disease.
- Due to alpha 1 antitrypsin deficiency.
- Due to galactosemia.
4)explain the Clinical manifestation/sign and symptoms of hepatic cirrhosis. Describe the symptoms and signs of hepatic cirrhosis
early stage:=
- Weight loss,
- Fatigue,
- Liver enlargement,
- nausea,
- vomiting,
- vascular spider (vascular spider: = in this superficial capillaries are dilated and red dots are seen)
- palmer erythema.
- ankle heel.
- intense itching.
late stage:=
- Symptoms (Acities := abnormal collection of fluid in to the abdominal cavity.)
- Jaundice,
- Light colored stool,
- Yellowish bright colored urine,
- brushing and bleeding,
- distended vein in abdomen
later stage:=
- Brain function is lost.
- The liver removes toxic materials from the blood Cannot remove.
- Mental disturbance.
- Poor concentration.
- Slurred speech.
- Atrexis
- Flapping and hand tremors are seen.
- Loss of motor control occurs in some parts of the body.
- Involuntary flapping movements of the hands are seen.
5)explain the diagnostic evaluation of hepatic cirrhosis. Write a diagnostic evaluation of hepatic cirrhosis.
- History taking and physical examination.
- assess blood test.
- ct scan.
- MRI.
- LFT (SGPT ,SGOT Test).
- ultrasonography.
- Liver Biopsy.
- esophago gastroduodeno scopy.
6) Explain the management of hepatic cirrhosis. (Write the management of hepatic cirrhosis.)
- Tell the patient to take a nutritious diet.
- Provide adequate amount of nutrition to the person with hepatic cirrhosis.
- Provide a sodium restricted diet if the patient develops ascites.
- Provide vitamin and mineral supplements to the patient. To do.
- If the patient has fluid retention, provide a potassium sparing diuretic (ex:= sporonolectone).
- Give the patient oral antibiotic medicine to treat the infection.
- If the hepatic cirrhosis is caused by alcohol, stop drinking alcohol.
- If the hepatic cirrhosis is caused by a viral infection, provide the patient with antiviral medicine.
- If the patient has autoimmune hepatitis, then provide steroid medicine to the patient.
- If the patient has esophageal varices, then provide vasopressin to the patient.
- Provide laxative medicine to the patient.
- Provide medicine to the patient that improves blood flow to the kidney.
- If the patient has any complications If there is, treat it.
- When complications are not treated, liver transplantation should be performed.
7) Explain the nursing management of patients with endocrine disorder. Write the nursing management of a person with endocrine disorder.
1)Altered nutrition less than body requirement related to loss of appetite.
improving nutritional status of the patient.
- Assess the dietary intake and nutritional status of the patient.
- Provide the patient with high protein, high calorie, and supplementary Provide vitamins A, D, E, K and folic acid.
- Instruct the patient to eat small and frequent meals.
- Instruct the patient to maintain adequate oral hygiene.
- Provide anti-emetic medicine if the patient has conditions such as nausea and vomiting.
2) fluid volume excess related to disease condition.
maintain the fluid volume of the patient.
- History taking and physical examination.
- assess blood test.
- ct scan.
- MRI.
- LFT (SGPT ,SGOT Test).
- ultrasonography.
- Liver Biopsy.
- esophago gastroduodeno scopy.
6) Explain the management of hepatic cirrhosis. (Write the management of hepatic cirrhosis.)
- Tell the patient to take a nutritious diet.
- Provide adequate amount of nutrition to the person with hepatic cirrhosis.
- Provide a sodium restricted diet if the patient develops ascites.
- Provide vitamin and mineral supplements to the patient. To do.
- If the patient has fluid retention, provide a potassium sparing diuretic (ex:= sporonolectone).
- Give the patient oral antibiotic medicine to treat the infection.
- If the hepatic cirrhosis is caused by alcohol, stop drinking alcohol.
- If the hepatic cirrhosis is caused by a viral infection, provide the patient with antiviral medicine.
- If the patient has autoimmune hepatitis, then provide steroid medicine to the patient.
- If the patient has esophageal varices, then provide vasopressin to the patient.
- Provide laxative medicine to the patient.
- Provide medicine to the patient that improves blood flow to the kidney.
- If the patient has any complications If there is, treat it.
- When complications are not treated, liver transplantation should be performed.
7) Explain the nursing management of patients with endocrine disorder. Write the nursing management of a person with endocrine disorder.
1)Altered nutrition less than body requirement related to loss of appetite.
improving nutritional status of the patient.
- Assess the dietary intake and nutritional status of the patient.
- Provide the patient with high protein, high calorie, and supplementary Provide vitamins A, D, E, K and folic acid.
- Instruct the patient to eat small and frequent meals.
- Instruct the patient to maintain adequate oral hygiene.
- Provide anti-emetic medicine if the patient has conditions such as nausea and vomiting.
2) fluid volume excess related to disease condition.
maintain the fluid volume of the patient.
- Maintain the patient’s intake-output chart.
- Monitor the patient’s blood pressure.
- Monitor the patient’s respiratory status.
- Assess the patient’s peripheral area for conditions similar to those seen in the ankle.
- Monitor the patient’s serum electrolyte levels.
3)Activity intolerance related to generalised body weakness.
maintain of rest and comfort of the patient.
- Assess the patient’s activity level.
- Ask the patient to take adequate rest.
- Provide a comfortable position to the patient.
- Instruct the patient to take a high protein and high calorie diet.
- Provide oxygen to the patient.
- Instruct the patient to exercise.
- Instruct the patient to do small amounts of daily routine activity.
4)Risk for Impaired skin integrity related to decies condition.
maintaining skin integrity of the patient .
- Assess the patient’s skin integrity.
- Frequently change the patient’s position.
- Do not use irritating soap.
- Massage the patient’s back every two hours.
- Instruct the patient to use a comfort device.
5)knowledge deficit related to disease condition and treatment.
providing knowledge to the patient.
- Assess the knowledge level of the patient.
- Provide complete information about the disease to the patient and his family members.
- Provide education on nutrition and rest to the patient.
- Ask the patient to avoid alcohol.
- Ask the patient and his family members to clear all doubts.
- If Ask the patient to report any complications immediately.
1) Define/explain portal hypertension. Define portal hypertension.
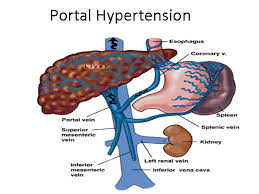
- => Portal hypertension is a vascular disease.
- => Hypertension or high blood pressure is a disease in which the pressure of the blood against the wall of the vessels increases.
- => The condition when blood pressure increases in the portal veins and their branches is called portal hypertension.
- => •••{ About the portal vein := Portal veins are large blood vessels that transmit blood from the abdominal organs (digestive system) to the liver. }•••
- => Portal hypertension is mainly seen due to liver cirrhosis or any other liver disease condition.
- => In portal hypertension, the portal pressure gradient is greater than 12 mmHg (portal pressure gradient:= the difference between the pressure in the portal vein and the hepatic vein.).
- => Portal hypertension causes conditions such as esophageal varices and ascites.
- ••{ meaning of varices := Varicose veins are a condition that occurs due to portal hypertension in which the veins in the lower part of the esophagus become enlarged and swollen. }•••.
- => •••{ Acities ( Ascites:= . Ascites is mainly seen due to portal hypertension and liver cirrhosis in which fluid collects in the abdominal area causing the abdominal area to become swollen and enlarged. )}•••.
2)explain the Etiology/cause of portal hypertension. Explain the etiology/cause of portal hypertension
prehepatic cause:=
1) thrombosis of the portal vein
- => The condition of portal hypertension is caused by blood clots in the portal vein, which obstructs blood flow.
2) Thrombosis of the splenic vein (Thrombosis of the splenic vein.
- => Obstruction is seen due to blood clot in the splenic vein, due to which the condition of portal hypertension is seen.
3) Congenital atresia or stenosis
- => Atresia => Atresia means the tubular structure in the body is absent from birth.
- stenosis (stenosis) := Stenosis means the narrowing of the tubular structure of the body.
4)massive spleenomegaly (massive spleenomegaly)
- => If there is only spleenomegaly, the length of the spleen is 12 to 20 cm.
- => But massive splenomegaly is when the length of the spleen increases beyond 20 centimeters, leading to the condition of portal hypertension.
5) Atriovenous fistula
- => Due to abnormal connection between the artery and vein.
6) Compression by tumor
- => Due to the formation of abnormal tumors, pressure increases on body parts, which also causes the condition of portal hypertension.
hepatic cause (Hepatic cause)
1)Liver cirrhosis (Liver cirrhosis)
- => In the condition of liver cirrhosis, fibrous scar tissues are formed in place of normal tissues of the liver, due to which blood flow is impaired and the condition of portal hypertension is seen.
2) Schistosomiasis
- => Schistosomiasis is a type of parasitic infection. This disease mainly converts the tissues of the liver into fibrous and scar tissues, due to which blood flow impairment is observed and a condition of portal hypertension occurs.
3) Alcoholic liver cirrhosis (Alcoholic liver cirrhosis)
- => In this condition, liver cirrhosis is seen due to long-term alcohol consumption and due to this, portal hypertension is seen.
4) Hepatic veno-occlusion disease
- => In this condition, hepatic vein occlusion is seen and due to this, the condition of portal hypertension is seen.
5)cytotoxic deug (cytotoxic drug)
- => Some types of drugs cause liver cell damage and due to this, impairment in blood flow and condition of portal hypertension are seen.
post hepatic cause (Post Hepatic Cause)
1) Hepatic vein thrombosis/Budd chiary syndrome (Hepatic vein thrombosis/Budd chiary syndrome)
- => In this, the hepatic vein is occluded, due to which blood flow impairment occurs and the condition of portal hypertension is seen.
2) Congestive cardiac failure
- => Due to heart failure, pressure is seen in the hepatic vein. Due to this, the condition of portal hypertension is seen.
3) Constrictive pericarditis
- => Due to thickening and hardening of the pericardium layer of the heart, the heart cannot function properly, resulting in blood flow impairment.
4) Right side heart failure
- => Due to right side heart failure, the right ventricle cannot pump adequate amount of blood to the lungs, which causes back flow of blood and increases pressure in the veins, resulting in the condition of portal hypertension.
3) Explain the Clinical manifestation/sign and symptoms of portal hypertension.
- Abdominal Pain,
- Abdominal girth increases,
- Gastro intestinal bleeding,
- Rapid weight gain,
- Ascities ( fluid is collection in to the abdomen area) ,
- Variecous veins,
- Variecous veins,
- Difficulty breathing,
- black, terry stool or blood in the stool (maleana),
- discomfort due to enlarged abdomen,
- blood in vomiting (hemetemesis),
- distended veins in the abdominal area becoming visible,
- Low platelet count,
- Fluid and electrolyte imbalance,
- Jaundice ( jaundice := serum billirubin is greater than 2.5 mg/dl),
- Hepatic encephalopathy ( hepatic encephalopathy := hepatic encephalopathy is a disturbance mainly seen in the central nervous system (CNS) and is caused by hepatic insufficiency. ),
- spinder angiomata swelling ( Abnormal dilatation of any vascular vessels beneath the skin result in red spot .) ,
- umbilical hernia, ( abnormal budge that can be seen at the umbilicus area. ),
- gynecomastia ( gynecomastea := enlargement of man’s Breast due to Hormonal imbalance or Hormonal therapy.) ,
- feeling tired,
- feeling weak,
- feeling weak,
- pruritus ( itching),
- increased irritability,
- altered sleep patterns,
- caput medusae (capute medusae: = veins around the umbilicus that are dilated.),
4)explain the diagnostic evaluation of portal hypertension. Write a diagnostic evaluation of portal hypertension.
- history taking and physical examination.
- x rays,
- endoscopic examination,
- ct scan,
- MRI,
- Abdominal ultrasound,
- assess the abdominal girth,
- liver function test
5) Explain the management of portal hypertension. Write the management of portal hypertension
1)Dietary modifications
- => The patient has fluid retention in the condition of portal hypertension, so to prevent fluid retention, the patient should be told to avoid sodium.
- Ex:= table salt, salty food, salted butter and margarine.
2)medication/ drug therapy (Medication / Drug Therapy)
- => Provide beta blocker medicine to the patient.
Ex:=nadolol and propranolol, - =>provide lactulose to the patient for treat the hepatic encephalopathy .
- => Provide anti-emetic medicine to the patient.
- => Provide vitamin K to prevent gastro intestinal bleeding.
- => Provide diuretic medicine to the patient.
3)Endoscopy therapy
=> Endoscopic therapy is considered the first-line treatment for variceal bleeding, and includes
- 1) bending.
- 2) sclerotherapy.
1) banding
- => In the banding procedure, a rubber band is used to block the blood vessel.
2) Sclerotherapy
- => Sclerotherapy is mainly used when banding procedures cannot be used.
- =>In sclerotherapy, a sclerosant solution is injected into the bleeding varicose veins, causing a scar to form at the bleeding site.
4)Life style changes
- => Ask the patient to maintain good nutritional habits.
- => Provide education to the patient to avoid alcohol intake.
- => Ask the patient not to use over the counter drugs.
- => Tell the patient to take adequate bed rest.
5) Transjugular intrahepatic portosystemic shunt (TIPS := Trans Jugular Intrahepatic Portosystemic Shunt)
- => In this procedure, a stent (tubular device) is placed in the middle of the liver.
- => This stent connects the hepatic vein to the portal vein.
- => This procedure reroutes the impaired blood flow in the liver, which corrects the abnormal pressure of the blood in the veins and treats the condition of portal hypertension.
6)Distal spleenorenal shunt (DSRS := Distal Splenorenal Shunt)
- => Distal splenic renal shunt is a surgical procedure in which the splenic vein is detached from the portal vein and attached to the left kidney.
- => This surgery reduces the pressure in the varices and controls the build-up caused by portal hypertension.
- => This is mainly done in patients who have good liver function.
7) Devascularization
- => This is a surgical procedure in which bleeding varices are removed.
- => This procedure is mainly done when Tips and surgical shunt procedures have not been successful.
8) Paracentesis (paracentesis)
- => This is a procedure in which fluid accumulated in the abdominal cavity due to ascites is removed.
9)Liver transplantation
- => This mainly occurs when end-stage liver disease is present.
8)Nursing management of patients with portal hypertension . Write the nursing management of patients with portal hypertension
Nursing management Nursing assessment
- Patient’s vital signs To assess the sine.
- Measure the patient’s abdominal girth.
- Do an integrated assessment of the patient’s skin.
- Assess whether the patient has any abnormalities or discolouration in his skin.
- Ask whether the patient has consumed alcohol.
- Is the patient taking any over the counter drugs? Ask whether the patient uses it or not.
- Ask about the patient’s eating pattern.
Nursing diagnosis
1)ineffective breathing pattern related to restriction of thoracic expansion secondary to the ascities , abdominal distension.
improve respiratory status of the client:=
- Assess the patient’s respiratory rate.
- Provide the patient with a comfortable position.
- Provide reassurance to the client.
- Ask the client to do deep breathing.
- Change the patient’s position every two hours To do.
2) Imbalance nutritional status less than body requirement related to abdominal distention.
improve the nutritional level:=
- Assess the nutritional status of the patient.
- Assess the patient’s likes and dislikes of food.
- Ask the patient to maintain oral hygiene.
- Provide a conductive environment for the patient.
- Give the patient a high carbohydrate and low sodium diet. Provide a nutritious diet.
- Instruct the patient to eat small and frequent amounts of food.
- Serve food to the patient in an attractive manner.
- Advise the patient not to consume alcohol.
- Provide anti-emetic medicine if the patient has conditions such as vomiting or nausea.
3)Impaired skin integrity related to oedema.
improve the skin integrity of the client.
- Assess the patient’s skin integrity.
- Ask the patient to maintain skin hygiene.
- Make the patient wear a clean cotton cloth Tell.
- Tell the patient to keep fingernails short.
- Tell the patient not to use dry shampoo.
- Tell the patient to apply an emollient.
- Tell the patient to do range of motion exercises.
- Tell the patient to follow a sodium restricted diet.
- Assess the patient’s skin every 4 to 8 hours.
4) Activity intolerance related to fatigue and lethargy.
enhance the activity level of the client.
- Assess the patient’s activity level.
- Instruct the patient to perform small amounts of daily routine activity.
- Instruct the patient to take bed rest.
- Instruct the patient to take rest between activities.
- Provide the patient with prescribed vitamin supplementation.
5) Disturbed body image related to changes in approach, role function.
improve the self esteem and body image of the patient.
- Assess the patient’s coping ability.
- Provide information to the client about the disease condition and the changes that occur due to it.
- Provide reassurance to the client.
- The patient’s Involve his family members in the care.
- Clear all the doubts of the patient.
- Do not give false reassurance to the patient and his family members.
1)explain / define the Acities . Define ascites.
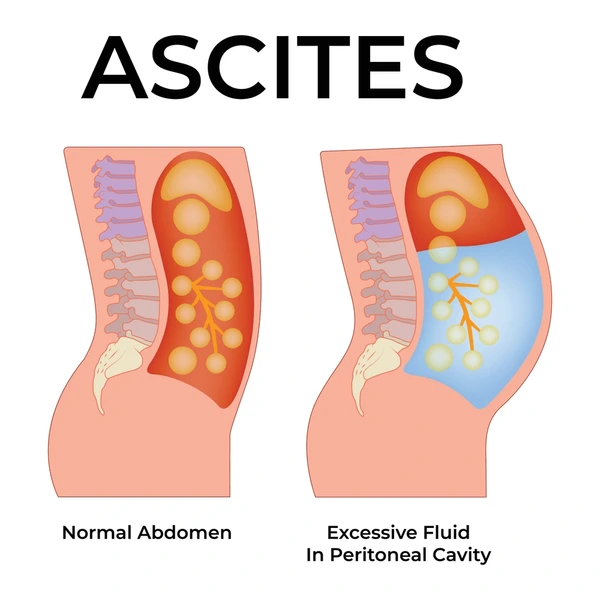
- => Ascites is a condition in which serous fluid accumulates in the abdominal cavity.
- => In this, the fluid increases to more than 25 ml.
- => The accumulation of serous fluid in the abdominal cavity causes the abdominal cavity to enlarge and swell.
2)explain the Etiology of Ascites. Explain the causes of Ascites
- Liver cirrhosis (liver cirrhosis)
- Heart failure,
- Portal hypertension,
- Constrictive pericarditis,
- hepatic venous occlusion:=Budd chiary syndrome or veno occlusive disease.
- Due to infection.
- Hypoalbu neminemia( hypoalbunemia := decrease serum protiene levels).
- Pericarditis ( infection and inflammation of pericardium layer of heart).
- Cancer.
- Nephrotic syndrome.
In hereditary angioedema (hereditary angioedema := Hereditary angioedema is a hereditary disorder in which fluid collects on the outside of blood vessels, impairing the normal flow of blood and lymph, and causing swelling in the face, hands, and extremities due to accumulation of fluid.
Due to poor nutrition.
Renal dialysis.
3) Explain the pathophysiology of Ascites. (Write the pathophysiology of Ascites. )
- => When the amount of aldosterone in the body increases.
- => Then the damaged hepatocytes (liver cells) cannot metabolize aldosterone.
- => Due to this, the amount of sodium in the body increases.
- => This increase in the amount of sodium in the body causes accumulation of water in the body and due to this, ascites and edema are seen in the body.
4)explain the Clinical manifestation/ sign and symptoms of Ascites.
- Abdominal distension.
- Abdominal pain.
- Weight gain.
- Portal hypertension.
- Swelling in the legs and ankles.
- Brushing.
- Swelling in the legs.
- Gynecomastea ( gynecomastea := enlargement of the man’s Breast tissues. Encephalopathy ( encepalopathy := When the liver is not functioning properly, ammonia accumulates in the body and brain function is impaired due to this).
- Fatigue and weakness.
- Heart failure.
- Hypokalemia ( hypokalemia := low level of pottasium in to the blood)
4) Explain the diagnostic evaluation of Ascites. Write the diagnostic evaluation of ascites
- history taking and physical examination.
- complete blood count (CBC test).
- Assess the electrolyte level. #check the liver enzyme.
- protein level.
- CT scan.
- Albumin and cell counts.
- culture, gram stain, cytopathology.
- Abdominal ultrasound.
- Albumin and cell count.
- Serum Acidity Albumin gradient (SAAG).
- Ultrasound.
- Ct scan of abdomen.
5) Explain the management of Ascites. (Write the management of Ascites)
- Provide the patient with a salt restricted diet.
- Provide albumin intravenously to the patient.
- Provide diuretic medicine to the patient (ex:= sporonolectone).
- Remove fluid from the patient’s abdominal area by paracentesis.
6)explain the management of Acities. (Write the management of ascites)
- Check the patient’s daily abdominal girth.
- Maintain the patient’s intake output chart.
- Maintain the patient’s fluid and electrolyte balance.
- Check the patient’s daily weight.
- Ask the patient to follow a low-restriction diet.
- Check the patient’s vital signs.
- Monitor the patient’s respitory status.
- Assess the effectiveness of the treatment given to the patient.
- Provide the prescribed medicine to the patient.
- To check the patient’s vital signs when performing paracentesis.
1)explain/define hepatic encephalopathy. Define hepatic encephalopathy.

- => Hepatic means ” “of the liver “
- => Encephalopathy means “A Disorder of the brain”.
- {“Hepatic Encephalopathy means := Disturbance in the central nervous system function because of hepatic insufficiency.( If there is any impairment in the function of the central nervous system due to hepatic insufficiency, it is called hepatic encephalopathy.) }
- => Hepatic encephalopathy is a condition in which any impairment in the function of the central nervous system due to hepatic insufficiency is called hepatic encephalopathy.
- => Hepatic encephalopathy is an impairment of brain function. It mainly occurs when the liver is unable to remove toxic substances from the body due to any abnormality in the liver and when these toxic substances accumulate in the body, a condition called hepatic encephalopathy occurs.
2)explain the causes/Etiology of hepatic encephalopathy. Give the cause of hepatic encephalopathy.
- Due to any liver disease.
- Cirrhosis of liver.
- Hepatitis ( hepatitis :=infection and inflammation of the liver),
- Liver cancer,
- Portal Hypertension,
- Alkalosis,
- Potassium deficiency.
- narcotics.
- Viral infection.
- Renal failure,
- Electrolyte abnormalities,
factore precipitating hepatic encephalopathy.
1)disorder that increase the protien.
- Gastro intestinal bleeding.
- Due to high protein diet.
2)metabolic stress:=
- diuretic drugs,
- dehydration,
- renal failure,
- electrolyte imbalance especially hypokalemia.
3)Non specific cerebral depressants:=
- Alcohol,
- Sedative,
- Analgesic,
Other factors :=
- Increase the sensitivity of GABA (Gamma Aminobutairic Acid),
- increase the circulating level of endogenous benzodiazepanes.
3) Explain the risk factor of the hepatic encephalopathy. Name the risk factors of hepatic encephalopathy.
- Due to dehydration,
- Due to too much protein intake,
- Electrolyte Abnormalities,
- Intestinal stomach, or
- Due to bleeding from the esophagus.
-
- Due to infection.
-
- Due to kidney problems.
-
- Due to low oxygen levels in the body.
-
- Due to the use of medications that suppress the central nervous system.
4)explain the pathophysiology of the hepatic encephalopathy. Explain the pathophysiology of the hepatic encephalopathy:=
=> Due to any etiological factor.
|
\/
=> Since the liver cells are damaged, they cannot convert toxic substances such as ammonia into urea in the body.
|
\/
=> Due to this, ammonia accumulates in the body.
|
\/
=> The level of this ammonia increases in the blood.
|
\/
=> Due to the increase in the level of ammonia in the blood, ammonia enters the blood stream.
|
\/
=> Due to this, the permeability of the blood increases and it crosses the blood brain barrier.
|
\/
=> Therefore, ammonia reaches the brain and damages the brain and alters the function of the brain.
|
\/
It causes
=> hepatic encephalopathy
5)explain the Clinical manifestation/sign and symptoms of hepatic encephalopathy. Describe the symptoms and signs of hepatic encephalopathy.
-
- Asterixis ( Asterixis := “Flapping tremor”) ,
-
- Disturbance in sleep patterns.
-
- Restlessness.
-
- Mental confusion.
-
- Insomnia ( Insomnia) coming).
-
- Apathy ( lack of feelings and emotions),
-
- Drowsiness,
-
- Confusion,
-
- Foul smelling breath,
-
- Sluggish movement to be,
-
- concentration to be poor,
-
- disorientation,
-
- behavior to be in appropriate.
-
- judgement to be poor.
-
- slurred speech to be.
-
- attention to be decreased.
-
- Childish behaviour,
-
- Being aggressive,
6) Explain the diagnostic evaluation of hepatic encephalopathy. Write the diagnostic evaluation of hepatic encephalopathy.
- History taking and physical examination.
- Elevated blood ammonia level.
- hypokalemia.
- assess the albumin level.
- assess the bilirubin level.
- electroencephalogram( EEG).
- Assess the prothrombin time.
- cerebrospinal fluid examination (SCF examination).
- ct scan.
- Complete blood count.
- erythrocyte sedimentation rate.
- Assess the electrolyte level.
- assess the liver function test (LFT).
- assess the Renal function test (RFT).
7) Explain the management of hepatic encephalopathy. Write the management of hepatic encephalopathy.
management
- Hospitalize the patient.
- Maintain the patient’s airway, circulation and breathing.
- Provide intravenous fluids to the patient.
- Maintain the patient’s fluid and electrolyte balance normal.
- Do not allow the patient to take a protein-rich diet. Telling.
- Tell the patient to take a glucose-rich diet.
- Provide the patient with a solution of lactolose to reduce constipation.
- Provide the patient with antibiotic medicine.
- Ex:= neomycin,
- Rigaximine,
- Ampiccilline,
- Metronidazole.
- The patient should avoid sedative and tranquilizer medicines.
- The patient should avoid ammonium-containing medicines.
- The patient should avoid Prevent bleeding in the gastrointestinal tract.
8) Explain the nursing management of patients with the hepatic encephalopathy. Write the nursing management of a patient with hepatic encephalopathy#
# Nursing diagnosis #
1)Impaired nutritional level less than body requirement related to Anorexia.
2)Impaired skin integrity related to oedema.
3)Activity intolerance related to fatigue.
4)Risk for injury related to diminished perception.
# nursing interventions #
- Monitor the patient’s intake output chart.
- Monitor the patient’s daily weight.
- Monitor the patient’s fluid balance.
- Monitor the patient’s vital signs.
- Frequently monitor the patient’s central venous pressure.
- Provide the patient with prescribed medicine.
- Ask the patient to take adequate rest.
- Provide the patient with comfort and a quiet atmosphere.
- Take care of the patient’s skin.
- Ask the patient to take a low protein diet.
- Prevent the patient from injury Use appropriate safety measures.
- Monitor the patient’s level of consciousness.
- Monitor the patient’s intake-output chart and monitor electrolyte balance.
- Perform laboratory investigations of the patient.
- Ask the patient to stop drinking alcohol.
- Ask the patient to take complete bed rest.
- Ask the patient to take adequate nutrition.
- Ask the patient to take proper diet.
- Ask the patient to avoid hepatotoxic drugs.
- Provide psychological support to the patient.
explain/define hepatitis. describe hepatitis.
=> Hepatitis is a condition in which the liver is infected and inflamed.
=> Viral hepatitis is mainly caused by
••>Hepatitis A virous,
••>Hepatitis B virous,
••> Hepatitis c virous,
••> Hepatitis D virous,
••>Hepatitis E virous.
•••> Epstein bar virous virus,
•••> Yellow fever virous,
•••> Rubella virus,
•••> Herpes simplex,
•••> Varicella virus,
•••> Adeno virus
All these viruses also cause hepatitis.
=> Hepatitis viruses enter the liver and multiply there, then damage the liver and cause inflammation and necrosis of hepatocytes.
=> When the hepatitis virus enters the body, its signs and symptoms are seen in three phases (3 phases).
- 1) Pre icterus phase ( prodromal phase .)
- 2) Icterus phase ( icterus phase)
- 3) Convalescent phase. ( Convulsant phase)
★★★••••>
1)pre icterus phase ( prodromal phase .) ( Preicterus phase or prodromal phase)
- => This phase lasts for one to two weeks (1 to 2 weeks).
- => In this phase, the patient experiences flu-like symptoms.
Such as,
=> Fatigue,
=> Loss of appetite,
=> Body aches,
=> Nausea,
=> Vomiting,
=> Diarrhea,
and
=> Constipation.
2)Icterus phase (Icterus phase)
- => The icterus phase begins five to ten days (5-10 days) after coming into contact with the hepatitis virus and signs and symptoms appear.
- => This phase lasts from two to six weeks.
- => In this phase, the level of bilirubin increases in the body, due to which the skin and mucous membrane of the body becomes yellowish in colour.
- => In this phase, the condition of jaundice is seen.
- => In this phase, itching/pruritus occurs due to bile salt deposition in the patient’s skin.
- => In this phase, the stool is light brown and clay colored due to the bile not being excreted through the normal fecal pathway.
3) Convalescent phase. (Convalescent phase)
- => Convalescent phase occurs after the icterus phase.
- => This phase can last for a few weeks and even months.
- => In this phase, signs and symptoms gradually improve.
1) Explain/define hepatitis A. (Define hepatitis A.)
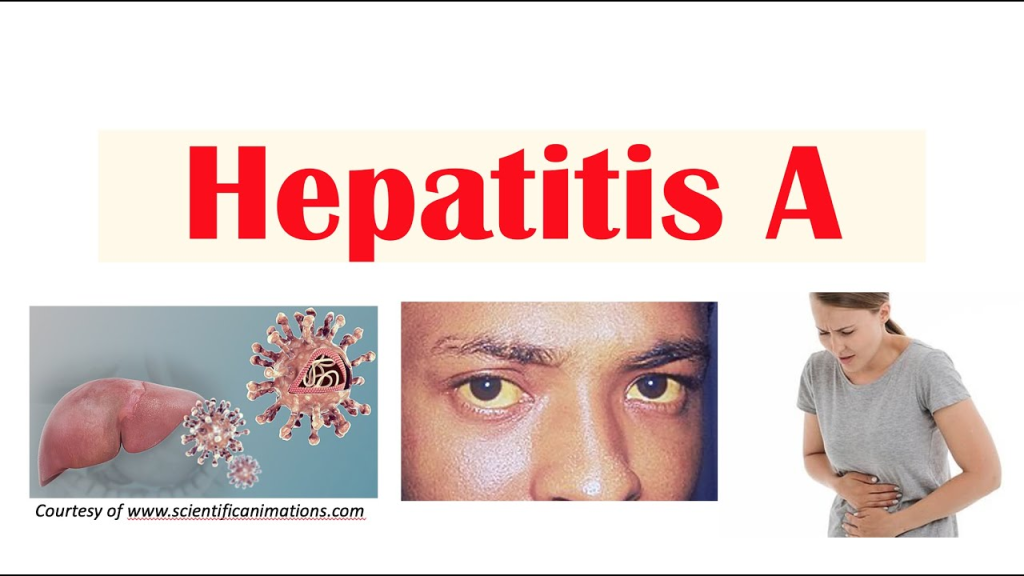
- => Hepatitis A is a viral infection that causes infection or inflammation of the liver
- =>It is mainly caused by an RNA virus.
- => Hepatitis A is mainly transmitted through the feco-oral route.
- => It is mainly transmitted through food or liquid contaminated with the hepatitis A virus.
- => Hepatitis A virus is mainly transmitted by a person who is infected with the hepatitis A virus and does not wash their hands properly after a bowel movement and when that person prepares food.
- => The incubation period of hepatitis A is between 15 and 50 days. And the average is 30 days.
- => Hepatitis A virus can be latent for four to eight weeks.
2)explain the Etiology/ cause of Hepatitis A disease. Explain the causes of Hepatitis A
1)contaminated food or water
- => Transmitted through food and food materials prepared by an infected person.
2)Person to person contact
- => Due to direct contact with any infected person or contact with their things.
3) Due to poor sanitation.
4) Due to poor hygiene.
5) Due to overcrowding.
6) Due to not washing hands properly after bowel movement.
7) Drinking contaminated water To do.
8) Eating undercooked shellfish.
9) Due to blood transfusion.
10) Having oral or anal sex with a person who has hepatitis A.
11) Reusing contaminated needles.
3)Explain the Clinical manifestation/sign and symptoms of hepatitis A virous. Write the symptoms and signs of Hepatitis A virus:=
- In this, the patient experiences flu-like symptoms.
- Upper respiratory track infection.
- Low grade fever.
- No appetite (anorexia).
- Indigestion (indiagetion:= indigestion).
- nausea,
- vomiting,
- diarrhea,
- clay colored stool,
- Heart burn (heart burn).
- Jaundice (jaundice:= yellow discolouration of the skin and mucous membrane).
- Weakness to come.
- Headache.
- Feel tired.
- generalised weakness.
- stomach cramps.
- The patient may develop strong sense of cigarette smoking.
4)explain the diagnostic evaluation of hepatitis A virous.
- Tell the patient not to drink alcohol.
- Tell the patient not to eat fatty foods.
- Tell the patient to maintain personal hygiene.
- Tell the patient to wash their hands frequently.
- Tell the patient to avoid unprotected sex.
- Instruct the patient to take a nutritional diet.
- Provide intravenous glucose to the patient.
- Maintain the patient’s body weight.
- Instruct the patient to take adequate bed rest.
- Instruct the patient to avoid physical activity.
- Instruct the patient to take small Ask to do activity in the amount.
- If the patient is experiencing nausea and vomiting, provide antiemetic medicine.
6)Explain the Nursing management of the patient with the hepatitis A. (Write the nursing management of the patient with hepatitis A.)
- Frequently monitor the patient’s vital signs.
- Monitor the patient’s daily weight.
- Frequently assess the patient’s stool.
- Provide the patient with frequent oral fluids.
- Provide the patient with intravenous fluids.
- Monitor the patient’s intake-output chart.
- Monitor the patient’s nutritional status.
- Ask the patient to eat in a sitting position.
- Provide the patient with small, free dietary supplements.
- Maintain the patient’s oral hygiene.
- Provide oral care to the patient.
- Instruct the patient to eat small and frequent amounts of food.
- Provide a calm and quiet environment for the patient while eating.
- Instruct the patient to get adequate rest.
- Monitor the patient’s daily intake output chart.
- Properly provide oxygen to the patient.
1)explain/define hepatitis B . (Describe hepatitis B:=
- => Hepatitis B is also called serum hepatitis.
- => Hepatitis B is mainly transmitted by the hepatitis B virus.
- => Hepatitis B virus is mainly found in the blood, saliva, semen, and vaginal secretions of an infected person.
- => Hepatitis B virus creates infection and inflammation in the liver which is called a severe form of infection (life threatening condition).
- => Hepatitis B virus is a life-long infection due to this
- •••>Liver cirrhosis (scarring),
- •••>Liver failure (liver failure),
- •••>Liver cancer (liver cancer) ••••>Death can also occur.
- => Hepatitis B •••>Acute (Acute := rapidly developing) and •••>Chronic (Cronic:=long lasting) forms are found.
- => The incubation period of hepatitis B is from one to six months (1 to 6 months).
- => Hepatitis B is mainly transmitted by the hepatitis B virus which is mainly present in blood, semen, and other body fluids.
2)explain the Etiology/cause of hepatitis B. (Explain the etiology/cause of hepatitis B)
- Caused by the hepatitis B virus.
- Transmitted through the blood, saliva, semen, vaginal secretions, etc. of an infected person is.
- Unprotected Sexually contact
- By sharing an infected needle.
- Mother to child transmission.
- Intravenous drug users.
- Health care workers. People who have frequent blood transfusions.
- From sexual contact with an infected person.
- From sexual contact with multiple partners.
- From Indra Venus drug abuse.
- From repeated exposure to blood.
- From sharing toothbrushes and razors.
- A patient undergoing dialysis.
- A person undergoing tattooing.
- Any medical procedure that is repeated.
3)explain the sign and symptoms/clinical manifestation of the hepatitis B virus.
- Hepatitis B virus occurs after contact with the virus
- It occurs after 12 weeks (range 9-21 weeks).
- Jaundice (jaundice:= yellowish of the skin and the sclera)
- Fever.
- Loss of appetite.
- Respiratory symptoms may occur.
- Abdominal discomfort.
- Rashes.
- Abdominal pain.
- nausea.
- vomiting.
- Generalized pain To occur.
- Weakness.
- Dark yellow urine.
- Liver is tender, enlarged.
- Clay coloured stools.
- Lethargy.
- spleen Is also enlarge and palpable in a few patient.
4) Explain the diagnostic evaluation of hepatitis B viral. (Write diagnostic evaluation of hepatitis B.)
- History taking and physical examination.
- assess the albumin level.
- assess the liver function test.
- assess the prothrombin time.
- assess about the presence of antibody HBsAG ( anti -HBs).
- antibody to hepatitis B core antigen (Anti-HBc).
- hepatitis B surface antigen (HBsAG).
- hepatitis E surface
- Antigen (HBeAG).
5) Explain the management of hepatitis B viral. (Write the management of Hepatitis B virus.)
medical management
- If the patient has acute hepatitis, then his/her lifestyle should be modified.
- Ask the patient to take proper bed rest.
- Ask the patient to take adequate fluids.
- Advise the patient to take a nutritional diet.
- If the patient has a condition of chronic hepatitis, tell him to avoid alcohol.
- Tell the patient to avoid over the counter (over the counter) medicine.
- Provide interferon-alpha medication to the patient who has a condition of chronic hepatitis B.
- Interferon- alpha increases the activity of the body’s immune system and impairs the reproduction of the hepatitis B virus.
- Interferon- alpha tablets are taken daily or three times a week for six months.
- Provide lamivudine and adenovir medicine to the patient.
- Tell the patient to take adequate bed rest.
- Provide adequate fluid to the patient.
- If the patient has a severe condition, perform liver transplantation.
Explain the nursing management of the patient with the hepatitis B virus. (Write the nursing management of a patient with Hepatitis B.)
- Maintain the patient’s skin integrity.
- Provide good skin care to the patient.
- Instruct the patient not to use irritating soaps.
- Instruct the patient to apply an emollient.
- Ask the patient to keep finger nails.
- Assess the patient for any bleeding.
- If the patient is itching, provide medication to reduce it.
- Frequently change the patient’s position to prevent pressure ulcers.
- Assess the patient for any neurological signs and symptoms.
- Provide the patient with a quiet and comfortable environment.
- If the patient is experiencing any bleeding, ask him to report it immediately.
- Monitor the patient’s prothrombin time and bleeding time and administer vitamin K.
- Do not perform any procedure that may cause trauma to the patient.
- Do not expose the patient to any needle stick. Take proper care to avoid injury.
6)Explain the prevention of occurrence of hepatitis B. (Write the prevention of hepatitis B.)
- To prevent hepatitis B, take the hepatitis B vaccine properly.
- Properly screen the donated blood.
- Use disposable series- needles.
- Instruct the patient to maintain good personal hygiene.
- Disinfect the working area daily.
- Wear gloves when working with any body fluid.
- Health care personnel and high-risk individuals should be vaccinated against hepatitis B. Say.
- => A total of three doses of Hepatitis B are taken.
- => After one month of taking the first dose, the second dose (2nd dose) is taken and then the 3rd dose of hepatitis B is taken six months after that dose.
- If you have come into contact with the hepatitis B virus due to any needle stick injury, get vaccinated immediately.
- Avoid sexual contact with a person who has acute or chronic hepatitis.
- Use a barrier method as a contraceptive during sexual activity.
- Do not share personal items such as toothbrushes and razors.
- Do not use any needles that have not been disinfected and use disposable series and needles.
- Avoid contact with the body fluids of an infected person.
1)explain the hepatitis c virus. (Describe hepatitis C virus.)
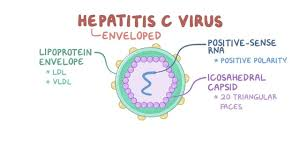
- => Hepatitis C is an infection and inflammation of the liver and is mainly caused by the hepatitis C virus.
- => Hepatitis C is a viral infection caused by the hepatitis C virus, an RNA virus that belongs to the Flaviviridae family of viruses.
- => Hepatitis C was first identified in 1989.
- => Hepatitis C is spread primarily through direct contact with the blood of an infected person.
- => Hepatitis C ( C ) is different from hepatitis A ( A ) and B ( B ).
- => The incubation period of hepatitis C is 15 -160 days.
2)explain the Etiology/cause of hepatitis c virous.
- Because of hepatitis C virus,
- Because of dialysis for a long time,
- Regularly working with blood.
- Having unprotected sexual activity with someone who has hepatitis C infection.
- Coming into contact with any body fluid of someone who has hepatitis C infection.
- Having any needle stick injury.
- Having a blood transfusion.
- Due to tattooing with any infected instrument.
- Due to any accidental needle stick injury.
- Due to any organ transfusion.
- Due to sharing personal items such as toothbrushes and razors.
- Due to giving birth to a child by a mother who has Hepatitis C infection.
- In people who are sexually active.
- In people who have multiple partners.
- Health care personnel.
3)explain the Clinical manifestation/sign and symptoms of hepatitis c virous. (Tell the symptoms and signs of a person with Hepatitis C)
- Liver failure,
- Cirrhosis of liver,
- Abdominal pain (Right upper abdomen),
- Abdominal swelling (Due to fluid collection in to the abdomen its called Ascites. ),
- Jaundice ( jaundice := yellowish discolouration of the skin , mucous membrane and sclera of the eyes. ),
- Dark urine and pale and clay-coloured stools.
- Building up in the oesophagus and stomach.
- Dark urine.
- Fatigue.
- Itching Coming.
- Muscle and joint pain.
- Fever.
- Loss of appetite.
- nausea .
- vomiting .
- Liver cancer.
4) Explain the diagnostic evaluation of the patient with hepatitis c viral. Write a diagnostic evaluation of a patient with hepatitis C.
- history tacking and physical examination.
- assess the liver function test.
- assess EIA( enzyme immunoassay) to detect the hepatitis c antibody.
- hepatitis c genotype.
- assess albumin level.
- assess liver function test.
- assess the prothrombin time.
- Liver Biopsy.
5) Explain the management of the hepatitis c virus. Explain the management of a patient with hepatitis C.
- Provide antiviral medicine to the patient to treat hepatitis C virus
- Ex:= pegylated interferon alfa and ribavirin.
- Instruct the patient to maintain good hand washing technique.
- Instruct the patient to follow strict aseptic technique.
- Follow strict aseptic technique when visiting a person who has an infection.
- Provide education to the patient not to scratch the area that is itching.
- If the patient experiences abdominal discomfort, extreme fatigue, skin rashes, fever, and vomiting, notify the doctor immediately.
- Provide education to the patient that tattoos and skin piercings can also cause hepatitis B. Transmission of hepatitis C can occur.
- Provide education to the patient that they should not donate blood after being infected with hepatitis C.
- Instruct the patient to take rest between activities.
- Instruct the patient to come for regular checkups.
- Avoid sexual activity with someone who is infected with hepatitis C.
- The patient should Advise the use of barrier methods of contraception during sexual activity.
1) Explain/define hepatitis D.
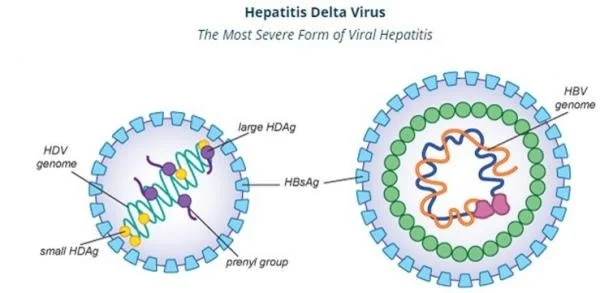
- => Hepatitis D is also called delta virus.
- => Hepatitis D is an infection and inflammation of the liver that occurs mainly due to the hepatitis D virus.
- => Hepatitis D is a viral infection caused by the hepatitis D virus.
- => Hepatitis D is also called a satellite infection because hepatitis D is mainly found in people who have hepatitis B.
- => Hepatitis D can exacerbate the severity of hepatitis B and cause more liver damage.
- It is mainly transmitted through contact with infected blood.
2) Explain the etiology/cause of hepatitis D viral. Explain the causes of Hepatitis D virus.
- Due to contact with infected blood and body fluids.
- In persons who have Hepatitis B.
- Due to sharing needles, syringes, and personal utensils (like toothbrush, razor) of an infected person.
- Sexual activity with an infected person Due to.
- Unprotected sexual activity.
- Intra venous drug users.
- Direct contact with the blood of an infected person.
- Birth of a baby by an infected mother.
- Previous hepatitis B infection.
- Due to receiving blood transfusion.
3) explain the Clinical manifestation/sign and symptoms of the hepatitis D .
1)Flu like symptoms:=
- Fatigue,
- Weakness,
- Muscle pain,
- Fever, 2)Jaundice
- Yellowish discolouration of the skin, mucous membrane and sclera is observed due to accumulation of bilirubin in the body. 3)Abdominal pain
- Pain and discomfort in the upper right quadrant of the abdomen due to inflammation of the liver. 4)Dark urine
- Due to the buildup of bilirubin in the body, the urine is seen as dark in colour. 5)Pale or clay colour stool
- Due to the failure of bilirubin to be excreted from the body, the stool is seen as pale and clay in colour. 6)Nausea and vomiting
- People with hepatitis D often experience nausea and vomiting. 7)Loss of appetite
- A person does not feel hungry due to hepatitis D. 8)Joint pain
- A person experiences joint pain due to the disease.
- 9) Confusion.
- 10) Itching.
- 11) Fever.
5) Explain the diagnostic evaluation of hepatitis D viral. (Write a diagnostic evaluation of a patient with hepatitis D.)
- history taking and physical examination.
- liver biopsy.
- blood test.
- liver function test.
- liver enzyme.
- Abdominal ultrasound.
- anti delta agent antibody test.
6) Explain the management of the patient with the hepatitis D. Write the management of a patient with Hepatitis D
medical management
- Provide antiviral medication to the patient.
Ex:=tenoflovir, Entecavir.
- Provide the patient with interferon-alpha medication.
- Monitor the patient’s liver function test regularly.
- Advise the patient to take an adequate nutritional diet.
- If the patient has a condition of nausea and vomiting Administer antiemetic medicine.
- If the patient’s condition is very severe, then liver transplantation should be done.
- Provide the patient with vaccines.
- Tell the patient to avoid alcohol as it impairs liver function.
- Tell them to avoid drugs that alter liver function or damage liver cells.
- Tell the patient to take high carbohydrate foods like bread, jam, whits, biscuits, rice, vegetables…
1) explain/ define hepatitis E . Describe Hepatitis E ( E )
- => Hepatitis E is a viral infection that is transmitted by the hepatitis E virus.
- => Hepatitis E is an infection and inflammation of the liver and is mainly transmitted by the hepatitis E virus.
- => Hepatitis E was mainly discovered in the 1990s.
- => Hepatitis E is mainly transmitted through the feco-oral route, i.e. through contaminated/infected food or water.
- => The incubation period of hepatitis E is from two to nine weeks (2 to 9 weeks).
- => Hepatitis E is self-limited but it affects pregnant women more severely. It can also cause abortion and intrauterine death in pregnant women.
2)explain Etiology/cause of hepatitis E . (Explain the cause of hepatitis E.)
Hepatitis E is caused by the virus. genotypes:=1,2,3,4
- Genotype := 1,2 are associated with the human infection.
- Genotype:=3,4 are associated with the animal infection.
- Due to contaminated food and water intake.
- Poor sanitation Due to.
- Poor hygienic conditions.
- Low socio-economic conditions.
- During the third trimester of pregnancy.
- In international travelers.
- In people who live in areas where there is an outbreak of hepatitis E.
- A person who has had sexual activity with an infected person.
- Due to unprotected sexual activity.
3) Explain clinical manifestation/sign and symptoms of the hepatitis E. Explain the symptoms and signs of a patient with hepatitis E.
- Weakness,
- Fatigue,
- Fever,
- Muscle pain,
- nausea,
- vomiting,
- No appetite (anorexia),
- Abdominal pain,
- Pain in the right upper quadrant of the abdomen.
- Jaundice (jaundice: = yellowish discoloration of the skin, mucous membranes, and sclera).
- Dark urine due to bilirubin.
- Pale and passing of clay-colored stool.
- Enlargement of the liver (hepatomegaly).
- Itching due to accumulation of bullirubin in the skin,
- Weakness,
- malaise,
- joint pain,
- Muscle pain,
- Weight loss.
4)Explain the diagnostic evaluation of the hepatitis E. Write the diagnostic evaluation of hepatitis E.
- History taking and physical examination.
- Assess the blood test of the patient.
- Anti-HEv igG antibody test.
- Anti-HEV igM
- Antibody test.
- assess the liver function test.
- assess the serological test.
- Assess the stool examination.
- Assess the imaging study.
- assess the hepatitis A,
- hepatitis B, hepatitis c test.
5) Explain the management of the patient with hepatitis E virus. Write the management of the patient with hepatitis E.
explain the medical management of the patient with the hepatitis E .
- There is no specific treatment for hepatitis E but it subsides on its own.
- The patient should be advised to take a nutritious diet.
- The patient should be advised to take a nutritious diet.
- The patient should be advised to take a nutritious diet. Antiemetic medicine should be given to treat the condition of vomiting.
- Provide the patient with high carbohydrate foods such as bread, jam, wheat, biscuits, rice, vegetables, and potatoes.
- Ask the patient to maintain good hygienic condition.
- Avoid eating uncooked food.
- Do not drink contaminated water. To do.
Nursing management
- Take a complete health history and physical examination of the patient.
- Ask the patient about any signs and symptoms of hepatitis.
- Instruct the patient to take short breaks from activities.
- Assess the patient’s working ability.
- Provide the patient with work and a quiet environment. Provide.
- Provide the patient with a high-calorie diet.
- Monitor the patient’s intake output chart.
- Serve food to the patient in an attractive manner.
- Provide a relaxing environment for the patient.
- Instruct the patient to maintain oral hygiene.
- Ask the patient to avoid alcohol.
- Ask the patient to avoid carbonated drinks.
- Ask the patient to adopt proper hand washing techniques.
- Ask the patient to maintain personal hygiene.
- Ask the patient to avoid unprotected sexual activity.
- Avoid sexual activity with someone who is infected.
- Use a barrier method as a contraceptive during sexual activities.
- Provide education to the patient on proper skin care.
- Ask the patient to bathe with warm water. Avoid using hot water as it increases skin dryness.
- Have the patient use an alcohol-based soap. Avoid it.
- Ask the patient to apply emollient properly.
- Ask the patient to keep his fingernails short.
- Provide proper back care if the patient is bed ridden.
1)explain/define liver cyst. (Define liver cyst.)
- => Liver cysts are also called hepatic cysts.
- => Liver cysts and hepatic cysts are round, thin, and sac-like structures that are irregularly located in the tissues of the liver.
- => The size of liver cysts ranges from a (two millimeters) to 2 mm (two centimeters).
- => A liver cyst is a fluid-filled sac that is located in the tissues of the liver.
- => The most common size of a liver cyst is up to two centimeters (2 cm).
- => A cyst is a cyst that is surrounded mainly by liver tissue and is either empty or contains a semi-fluid substance.
2) Explain the Etiology/cause of the liver cyst. Explain the causes of liver cyst.
- Liver cysts are also present at birth due to any developmental abnormality.
- Polycystic liver disease.
- Parasitic infection.
- Any injury or trauma.
- Liver cancer.
- Congenital hepatic fibrosis
- This is a hereditary disorder in which the bile ducts are irregularly shaped along with scar tissues and it and renal function are also impaired.
caroli’s disease
- Carolis disease is mainly caused by recurrent inflammation of the bile duct and the formation of stones in it and dilatation of the intrahepatic bile duct.
choledochal cyst
- Congenital abnormality of the bile duct.
- Due to congenital hepatic fibrosis.
- Due to echinococcus infection.
3) Explain the Clinical manifestation/ sign and symptoms of the hepatic cyst. Explain the signs and symptoms of hepatic cyst.
- Swelling and discomfort in the upper part of the abdomen.
- Abdominal pain.
- Nausea.
- Digestive problems.
- Shoulder pain.
- Liver enlargement.
- Bile duct infection and blockage.
- Jaundice (yellowish discolouration of the skin, mucous membrane and sclera).
- Heaviness and fullness in the abdomen.
- A mass-like structure in the abdomen.
4) Explain the diagnostic evaluation of the liver cyst. Write diagnostic evaluation of liver cyst
- History taking and physical examination.
- abdominal ultrasound,
- ct scan,
- MRI,
- Biopsy of the affected part,
- blood test,
- liver function test,
5) Explain the management of the liver cyst. Write the management of liver cyst.
- In the treatment of liver cyst, the cyst is aspirated and the cyst is surgically removed.
- To prevent the cyst from recurring, the affected area is also removed.
- Provide antibiotic medication to the patient.
- If the patient is in pain, provide him with analgesic medicine. To do.
Explain the nursing management of the patient with the liver cyst. Write the nursing management of a patient with liver cyst.
- Continuously monitor the patient.
- Monitor the patient’s vital signs.
- Assess the patient’s pain level.
- Provide analgesic medicine if the patient is in pain.
- Assess the patient for any complications such as jaundice, nausea,
- Vomiting or not.
- Monitor the patient’s intake output chart.
- Maintain the patient’s hydration status.
- Provide complete information about the disease to the patient.
- Provide psychological support to the patient.
- Relieve the patient’s anxiety.
- Assess the patient for any complications after cyst removal.
explain / define liver cancer (liver cancer) Describe.)
Introduction:=
- => Liver cancer arises in the liver and is called hepatocellular carcinoma.
- =>This cancer arises in the cells of the liver.
- => It involves abnormal and uncontrolled growth of cells and formation of a tumor and this tumor can be malignant (cancerous) or benign (non-cancerous).
- =>This cancer is also called hepatoma.
2)explain Etiology / cause of the patient with the liver cancer. State the causes of patients with liver cancer:=
- certain type of liver disease:=cirrhosis,
- hepatitis B viral,
- hepatitis c viral,
- Diabetes,
- Obesity,
- Aflatoxin:=
- Birth control pills,
- Tobacco use,
- vinyl chloride,
- Anabolic steroids,
- Arsenic,
- Cytological drug,
- use of steroids.
3) Explain the clinical/manifestation sign and symptoms of the patient with the liver cancer.:=
- Pain occurs in the right side of the abdomen and this pain is transferred to the back side and shoulder.
- The right side of the abdomen becomes swollen.
- A lump appears in the abdomen.
- The liver only enlarges.
- Weight decreases.
- malaise occurs.
- I don’t feel hungry and my abdomen feels very bloated after eating a little.
- I feel extremely tired.
- The eyes, skin and whole body become yellowish.
- nausea,
- vomiting,
- fever,
- fluid retention (acities),
- liver damage,
- Metabolic disturbance,
- splenomegaly,
- Hepatic encephalopathies,
- Jaundice( Jaundice),
- esophageal varies (the esophagus becomes enlarged).
- Abdominal distension.
4) Explain the diagnostic evaluation of the patient with the liver cancer. Write the diagnostic evaluation of a patient with liver cancer:=
- History tacking and physical examination,
- Hepatological investigation,
- ->( AFT := Alpha feto protien),
- ->blood test,
- ->liver function test,
- ->Albumin alkaline Phosphate,
- ->Prothrombin time,
- X Ray,
- ultrasonography,
- ct scanning,
- MRI,
- Laproscopy,
- Biopsy,
- hepatitis b test,
- hepatitis c test
5) Explain medical management of the liver cancer. Write the management of liver cancer:=
- chemotherapy,
- Radiation therapy,
- Ablation therapy,
- Immunotherapy,
- Biotherapy,
6) Explain surgical management of liver cancer. Write the surgical management of liver cancer:=
- Surgical resection,
- liver transplantation.
7) complication:=
- Malnutrition,
- Biliary obstruction,
- sepsis,
- liver abscesses,
- Metastasis.
8)explain the Nursing management of the patient with the liver cancer: =Write the Nursing management of the patient with liver cancer:=
Nursing assessment:=
- Assess the patient’s pain level.
- Assess the patient’s coping ability.
- The patient’s To check vital signs.
- Check the patient’s skin turgor and see if there is any condition in the heel.
- Check the patient’s dietary condition.
- Assess the patient’s activity level and sleep pattern.
- Assess the patient’s chemotherapy, radiotherapy, and immunotherapy side effects.
Nursing diagnosis
1)pain related to liver enlargement.
Nursing interventions:=
Controlling pain:=
- To the patient Provide analgesic medications.
- Provide mind diversionary therapy to the patient
- Monitor the patient for any signs of drug toxicity.
- Provide guided imagery to the patient.
- Instruct the patient to exercise moderately.
- Provide comfort measures to the patient To do.
2)Altered nutrition less than body requirement related to disease and side effects of chemotherapy.
Using interventions:=
Improving nutritional status:=
- Tell the patient to eat small amounts of food.
- Tell the patient to take supplementary drugs.
- Give the patient food that he likes to eat.
- Know the patient’s likes and dislikes.
- Give the patient food that is high in calories.
- Do not keep things with bad smells near the patient while he is eating.
3)fluid level excess related to oedema.
Nursing interventions:=
Relieving excess fluid volume:=
- Check the patient’s vital signs.
- Check the patient’s intake output.
- Do not give the patient sodium-rich food.
- Give the patient fluids as prescribed.
- Give the patient diuretic medicine.
- Maintain the patient’s potassium level.
- Provide albumin and protein supplementation to the patient.
- Check the patient’s abdominal girth daily.
- Check the patient’s weight. If there is weight gain, it indicates fluid retention.
- Get the patient’s laboratory tests done.
- Prepare the patient and his family members for surgery.
- Clear all the doubts of the patient and family members.
- Provide psychological support to the patient and his family members.
4) Discomfort related to disease condition.
5) Altered sleeping pattern related to pain.
6) Activity intolerance related to weakness.
7)Risk for infection related to bone marrow depression secondary to chemotherapy.
1)Explain/ define liver abscesses. Describe liver abscess
- => Liver abscess is a condition in which pus collects in the liver tissue due to any type of infection, it is called liver abscess.
- =>Due to this abscess, the pressure on the healthy liver tissue increases,
- => Due to this, the healthy liver tissue is also killed, after which this infection enters the bloodstream and creates a very extreme level of infection in the bloodstream.
- => When any infection occurs in the gastrointestinal tract (GI track) or the biliary track, the infection reaches the liver through the biliary system, the portal system, and the lymphatic system. After that, it destroys the normal cells of the liver and causes necrosis.
- => Then, these necrotic cells of the liver cause the formation of an abscess/pus in the liver.
2)explain the type of the liver Abscesses. Name the type of liver abscess:=
- 1)pyogenic liver abscesses,
- 2)Amoebic liver Abscesses,
- 3)Fungal Abscess
1)Pyogenic liver Abscesses,
=> Pyogenic liver abscess is mainly caused by infection.
Like:=
=> bacterial infection
=> Parasitic infection
•••> Pyogenic liver abscess is the most common type of liver abscess.
2)Amoebic liver Abscesses,
=> Amoebic liver abscess is caused by microscopic organisms called Amebas and Entamoeba histolytica.
=> Thus, amoebic liver abscess is caused by these microscopic organisms.
3) Fungal Abscess
=> Fungal abscesses are mainly caused by fungal microorganisms.
Ex:= most common fungus is candida albicans ( Candida albicans).
3)explain the Etiology/ cause of the liver Abscesses. Give the causes of liver abscess:=
- Due to immune deficiency,
- Abdominal infections such as appendicitis
- ( Appendicitis),
( Diverticulitis), and perforated bowel. - Diabetes mellitus.
- Due to blood infection.
- Due to infected hepatic cyst.
- Due to infection of bile duct (cholengitis).
- Due to metastatic liver tumor and cancer.
- Due to endoscopy of bile draining tube.
- Any liver trauma Due to.
- Amoebic dysentery (Decentry:= severe diarrhea present of blood and mucous in to the feces. ) Due to.
- Bacterial infection.
4) Explain the Clinical manifestation/ sign and symptoms of the liver Abscesses. Explain the clinical manifestations/ signs and symptoms of the liver abscesses.
- Pain in the right upper quadrant of the abdomen.
- Fever.
- Feeling cold.
- nausea,
- vomiting.
- Profuse sweating.
- Weight loss.
- Right side chest pain.
- Jaundice.
- Weakness.
- Abdominal pain.
- Anemia.
- Dark urine occur.
- Passing pale and clay colored stools.
- Hepatomegaly ( hepatomegaly := enlargement of the liver) .
- Joint pain.
- Sepsis and shock.
- Loss of appetite.
- Extreme fatigue Feeling.
- General discomfort.
- Itching.
5) Explain the Diagnostic evaluation of the patient with the liver Abscesses.
- history tacking and physical examination.
- blood culture.
- abdominal ct scan.
- ultrasound of the abdomen.
- aspiration of the liver Abscesses.
- billirubin blood test.
- liver biopsy.
- billirubin blood test.
- liver function test.
- blood culture for bacteria.
- complete blood count test.
- liver function test.
- white blood cell count.
6) Explain the management of the patient with the liver abscesses. Write the management of a patient with liver abscess
- Treatment depends on the cause of the abscess.
- Provide chemotherapy to the patient.
- Provide antibiotic medicine to the patient.
Ex:=
- Aminoglycoside,
- Amikacine,
- Gentamycine,
- Clindamycin,
- Piparacillin-
- tazobactam,
- Metronidazole.
- Aspiration of abscess through needle to the patient.
- do percutaneous drainage and aspiration of the abscess.
7) Explain the nursing management of patients with liver abscesses. Explain the nursing management of a patient with liver abscess.
Nursing assessment
- Assess the patient’s vital signs.
- Perform a thorough physical examination of the patient.
- Assess the patient for any signs and symptoms of liver abscess.
- Asking about the patient’s eating habits.
- Assessing whether the patient has a condition like jaundice.
Nursing diagnosis
1)hyperthermia related to disease condition and infection.
maintaining body temperature of the patient
- Monitor the patient’s body temperature.
- Assess the patient’s vital signs.
- Provide ventilation to the patient in the room.
- Provide cold compression to the patient.
- Provide sponge bath to the patient.
- Give the patient antipyretic medicine.
- Provide intravenous fluid to the patient.
2)Acute pain related to pus formation in to the liver.
Relieving Abdominal pain.
- Assess the patient’s pain level.
- Ask the patient to do deep breathing exercises.
- Provide the patient with mind diversionary therapy.
- Apply cold compression to the area of pain.
- Instruct the patient to eat frequent but small amounts of food.
- The patient Advise the patient to take a soft diet.
- Provide analgesic medicine to the patient to relieve pain.
- Provide antacid medicine to the patient.
3)Impaired nutritional status less than body requirement related to abdominal pain.
- improve nutritional status of the patient.
- Assess the nutritional status of the patient.
- Gain information from the patient about the foods the patient likes and dislikes.
- Maintain the patient’s oral hygiene.
- Provide the patient with small but frequent amounts of food.
- Provide the patient with a high protein and Provide high carbohydrate food.
- Provide food to the patient in an attractive way.
- Keep food utensils properly cleaned.
4)Activity intolerance related to fatigue, malaise and weakness.
promote Activity level of the patient.
- Assess the patient’s activity level.
- Change the patient’s position every two hours.
- Instruct the patient to do some daily routine activities.
- Instruct the patient to take rest between activities.
- Instruct the patient to do some range of motion exercises.
- Provide the patient with the prescribed vitamin supplement.
5)Impaired knowledge of the patient related to disease condition.
promote knowledge level of the client.
- Assess the patient’s knowledge level.
- Assess the patient’s anxiety level.
- Provide the patient with information about their condition, its cause, and its treatment.
- Instruct the patient to avoid alcohol.
- Provide the patient with information about surgical management.
- Provide the patient with information about the patient’s antibiotic medication.
- To clear all the doubts of the patient.
- To provide complete information about his treatment to the patient.
1)Define/explain liver failure. Define liver failure.
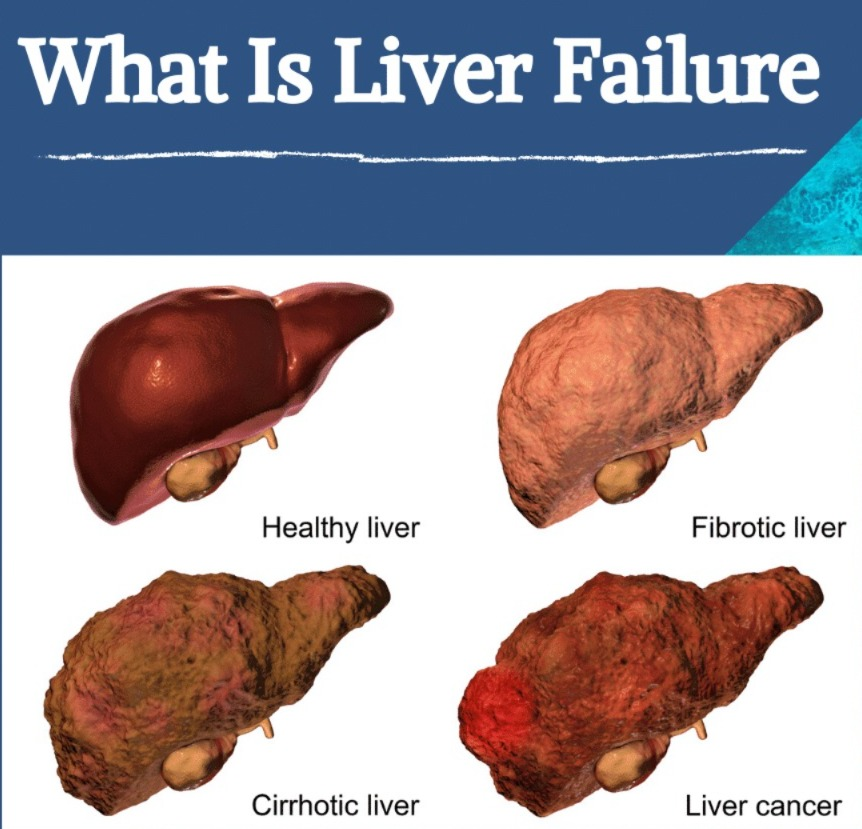
- => Liver failure is a condition in which the liver is severely damaged and due to this the liver cannot perform its vital functions.
- => The liver performs many vital functions such as detoxification, metabolism and protein formation which is responsible for blood clotting, due to liver failure all these functions become impaired.
- => The condition of liver failure is mainly caused by any disease condition of the liver.
- => Liver failure is a very life threatening condition, it occurs in two forms
- => 1) Acute liver failure which occurs within 48 hours,
- And 2) Chronic liver failure which occurs gradually over many months and years is called chronic liver failure.
2) Explain the Classification of the liver failure. Explain the classification of liver failure.
- 1)fulminant hepatic failure (FHF Fulminant Hepatic Failure)
- 2)late onset hepatic failure (Lat Onset Hepatic Failure)
- 3)chronic decompensated hepatic failure. Chronic Decompensated Hepatic Failure
1) Fulminant hepatic failure (FHF Fulminant hepatic failure)
- => This type of hepatic failure is seen within eight weeks (8 weeks) of the onset of any disease condition.
2)late onset hepatic failure (late onset hepatic failure)
- => This type of hepatic failure is seen within 8 to 26 weeks of the onset of any disease condition.
3)chronic decompensated hepatic failure. (Chronic Decompensated Hepatic Failure)
- => This type of hepatic failure occurs within six months.
explain type of hepatic failure.
- 1)Acute hepatic failure (Acute hepatic failure).
- 2) Chronic hepatic failure (Chronic hepatic failure)
1)Acute hepatic failure.
- => In this type, liver dysfunction occurs within a week.
- => This type of hepatic failure can be caused by many reasons such as any ••>infection,
••>viral hepatitis,
••>drug toxicity,
••>acute fatty liver in pregnancy. - => This type of hepatic failure requires immediate medical attention because it progresses rapidly and can create a life-threatening condition.
2) chronic hepatic failure (chronic hepatic failure)
- => This type of liver failure is progressive and gradual and progresses over many months and years.
- => This type of liver failure is caused by
••>chronic liver disease,
••> liver cirrhosis,
••>chronic alcohol consumption,
••> Due to viral hepatitis, ••>Non-alcoholic fatty liver disease
The condition of chronic liver failure is seen.
3)explain the Etiology/cause of hepatic failure. Give the reasons for hepatic failure#
- Due to viral infection,
- Hepatitis B,
- Hepatitis C,
- Prolonged alcohol consumption,
- Liver cirrhosis,
- Due to taking some kind of toxic drug.
- Ex:=acetaminophen,
- Hepatitis A, B and C,
- Due to reaction to some kind of medication,
- Ingestion of any poisonous and mushroom,
- Hepatocellular carcinoma.
- Metastatic carcinoma.
- Autoimmune disease condition.
- Genetic disorder.
- Any other liver disease.
4)explain the Clinical manifestation/sign and symptoms of the hepatic failure. Explain the clinical manifestation/sign and symptoms of the hepatic failure.
- nausea,
- loss of appetite,
- jaundice (yellowish discolouration of the,skin, mucous membrane, and sclera),
- fatigue,
- diarrhea,
- pain in the upper right part of the abdomen Pain.
- Acities ( Accumulation of the fluid in to the abdominal cavity. ),
- Difficulty concentrating.
- Confusion.
- Drowsiness.
- Bleeding easily.
- Abdominal pain occur.
- Swelling.
- Constant itching of the skin.
- Darkening of the urine color.
- Pale-clay color stool.
- Palmar erythematosus.
- Scratch marks appear.
- Gynecomastia ( gynecomastea := enlargement of man’s Breas ttissues),
- Anemia,
- Coma,
- Hepatocellular carcinoma.
5)explain the diagnostic evaluation of the hepatic failure. Write a diagnostic evaluation of hepatic failure#
- history taking and physical examination,
- blood test,
- imaging test,
- liver tissue biopsy,
- Doppler ultrasound,
- ct scan,
- MRI,
- electroencephalography.
- Examination of the liver tissue.
- liver function test.
- Complete blood count test.
- Coagulation study.
- ultrasound.
- metabolic test.
- autoimmune marker test.
- Assess Ammonia level.
6) Explain the management of the patient with the hepatic failure. Write the management of a patient with hepatic failure#
1)medication to reverse poisoning:=
- Liver failure is mainly caused by overdose of acetaminophen and mushrooms, so to prevent its adverse effects, antidotes such as
- Provide agents that are poisonous Neutralizes the agent.
2)Relieving excess fluid in the brain:=
- => In cerebral ED, it is mainly caused by liver failure, so to reduce this pressure, provide osmotic diuretic mannitol, which prevents fluid buildup in the brain, so provide the patient with intravenous mannitol (0.5-1g/kg or 50-100g).
3)screening of the infection:=
- => Collect blood and urine samples of the patient and assess whether there is any infection or not and if there is a condition of infection, provide antibiotic medicine to the patient.
4)prevention severe bleeding:=
- => A person who develops a condition of liver failure has a high chance of bleeding from the gastrointestinal tract, so to prevent that bleeding, the patient should be provided with meditation or if the patient has lost a lot of blood, then the patient should be given a blood transfusion.
5)liver transplantation:=
- => Liver failure is an irreversible condition, so in this condition, the damaged liver is removed from the patient’s body and a healthy liver is transplanted into the patient’s body.
explain the nursing management of the patient with the hepatic failure. Write the nursing management of a patient with hepatic failure.
improve the nutritional status of the patient:=
- Assess the nutritional status of the patient.
- Provide the patient with small and frequent amounts of food.
- Provide mouth care to the patient. Provide.
- Tell the patient to reduce sodium intake.
- Provide food to the patient through parenteral route.
- Provide antiemetic medicine if the patient has nausea and vomiting.
- Provide high calorie food to the patient.
- Provide vitamin and Provide mineral supplements.
2)Maintain adequate fluid volume.
- Frequently monitor the patient’s vital signs.
- Monitor the patient’s daily weight.
- Maintain the patient’s intake output chart Do.
- Record the patient’s abdominal mass.
- Assess the patient for any conditions such as peripheral edema.
- Instruct the patient to restrict sodium.
- Maintain the patient’s electrolyte levels.
- Assess the patient for any bleeding or hemorrhage symptoms.
3)improve Respiratory status:=
- Assess the patient’s respiratory rate and depth.
- Analyze the patient’s arterial blood gas.
- Assess the patient’s hemoglobin and hematocrit level.
- Keep the patient’s head elevated.
- Ask the patient to do deep breathing exercises.
- Provide oxygen to the patient.
1)Define/explain the pancreatitis. (Define pancreatitis.)
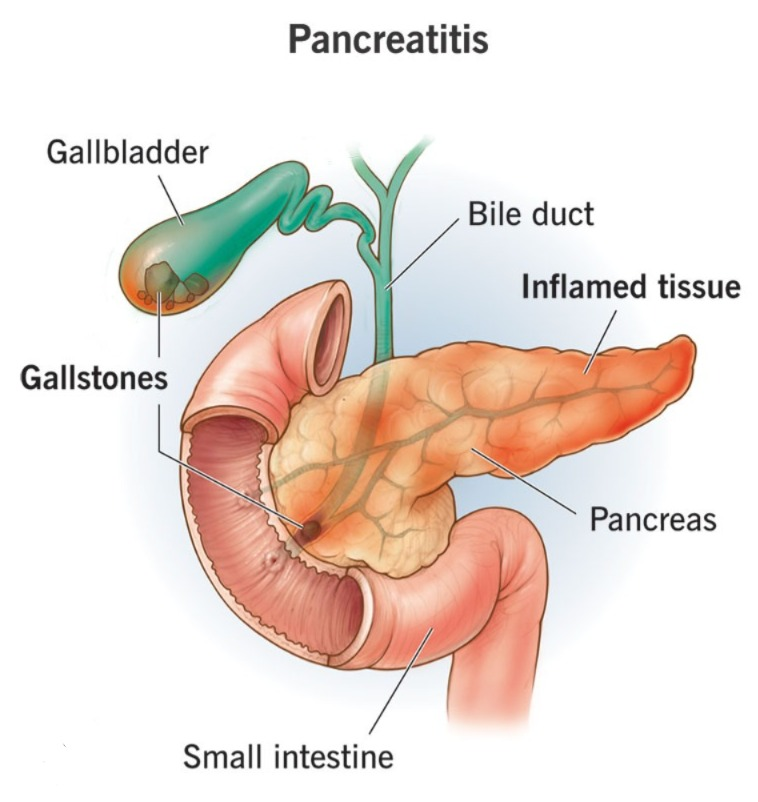
- =>Pancreatitis is an infection and inflammation of the pancreas. is.
- => The pancreas is a gland located behind the stomach that releases insulin, glucagon, and many digestive enzymes that help in the digestion and absorption of food.
=> There are two types of the pancreatitis.
- 1)Acute pancreatitis.
- 2) cronic pancreatitis
1) Define/explain Acute pancreatitis. (Define acute pancreatitis.)
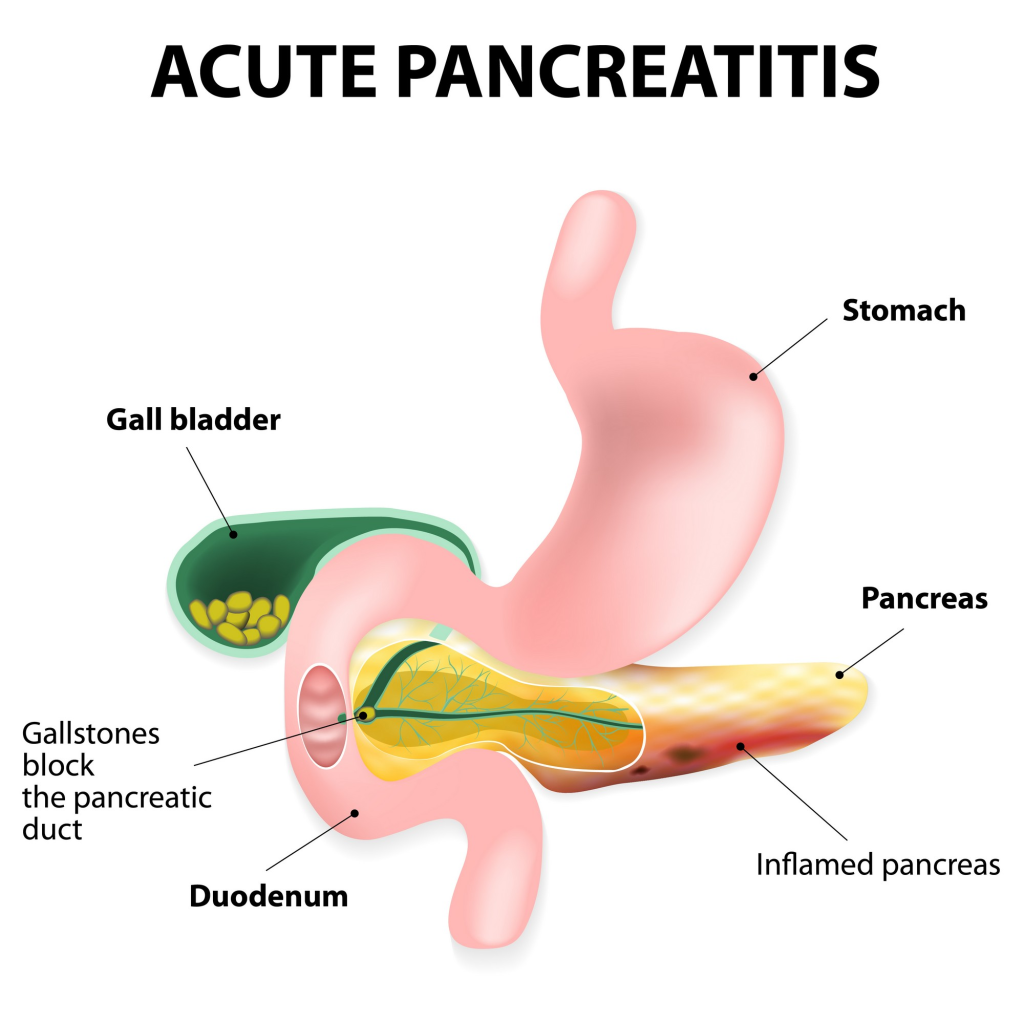
- =>Acute pancreatitis is a condition In which there is infection and inflammation of the pancreas and it resolves within a few days and it creates serious complications.
- => Acute pancreatitis is an infection and inflammation of the pancreas that occurs within a week.
- => Acute pancreatitis is a life-threatening condition and can cause severe complications.
2) Explain the Etiology/cause of the acute pancreatitis.
- Gallstones ( gall stones := cholilithiasis:= a hardened deposit of digestive fluid that can form into the gall bladder.).
- Billiary tract disease.
- Cholelithiasis := ( inflammation of the bile duct) due to ( cholangitis ) := ( inflammation of the bile duct).
- Prolonged alcohol intake.
- Some types Due to taking medication.
- Due to any bacterial and viral infection.
- Due to trauma.
- Due to any surgery of the pancreatic duct.
- Due to metabolic disorders.
- Hereditary.
- Pancreas Due to surgery.
- Any severe injury to the abdominal area.
- Using any oral contraceptive medicine.
- Due to abnormal structure of the pancreas.
- Using any corticosteroids.
- Complications of cystic fibrosis Due to.
- Peptic ulcer ( A sore that can develop in the lining of the esophagus, stomach and intestine. ) due to.
- Excessive amount of lipids in the blood.
- Pancreatic duct blockage.
- Injury to the pancreas due to any accident.
3) Explain the sign and symptoms/clinical manifestation of the pancreatitis. (Tell the symptoms and signs of creatitis.)
- Abdominal pain.
- abdomen is swollen or tender.
- Back pain.
- nausea.
- vomiting.
- Fever.
- Epigastric pain.
- Increased heart rate.
- Abdomen becomes rigid and boared.
- Gasean abdominal fullness.
- Brushing around the umbilicus.
- Hypotension and go into shock.
- Jaundice.
- Mild confusion.
- Dehydration.
- Low blood pressure.
- Acute renal failure.
- Clay colored stool.
- Respiratory distress.
- Indication.
- Hypocalcemia.
- Hyperglycemia.
- Myocardial depression.
- Skin rashes and sores.
- Respiratory distress.
4)explain the diagnostic evaluation of the patient with the acute pancreatitis. Write the diagnostic evaluation of the patient with acute pancreatitis.
- History taking and physical examination.
- blood test.
- assess the laboratory test.
- assess the serum amylase and lipase level.
- assess the urinary amylase level.
- assess the Wbc count.
- assess the calcium level.
- assess the glucose level.
- assess the complete blood count test.
- abdominal ultrasound.
- x rays.
- ct scan.
- MRI.
- MRCP (Magnetic resonance cholangiopancreatography.).
- assess the peritoneal fluids shows increase in the level of pancreatic enzyme.
- Stool Examination.
5) Explain the medical management of the patient with acute pancreatitis. (Write the medical management of a patient with acute pancreatitis.)
- Provide total parental fluid through the patient’s intravenous line.
- Give the patient antibiotic medicine if there is an infection.
- Do nasogastric suction if the patient has nausea, vomiting and abdominal distension.
- If the patient is in pain Provide analgesic medicine.
- If the patient is vomiting, provide antiemetic medicine.
- If the patient is acidotic, provide sodium bicarbonate.
- If the patient has blood loss, perform blood transfusion.
- Provide adequate amount of intravenous fluid to the patient.
- If the patient is unable to take oral food and fluids, give him/her nasogastric fluids.
surgery
- placement of biliary drains in the pancreatic duct.
- surgical removal of the pancreas.
Explain the Nursing management of patients with the acute pancreatitis.Explain the Nursing management of patients with the acute pancreatitis.
- Monitoring the cardiovascular and respiratory systems for problems.
- Providing a calm and comfortable environment to the patient.
1) Define/explain chronic pancreatitis. Describe chronic pancreatitis.
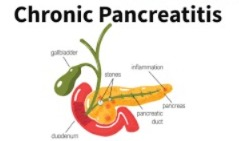
- => Chronic pancreatitis is a gradual and long-term infection and inflammation of the pancreas, which causes permanent damage to the pancreas.
- => This condition of the pancreas develops gradually in which ••>There is ongoing inflammation of the pancreas, ••>Scarring of pancreatic tissue, and ••>Impairment in the function of the pancreas occurs.
- => Chronic pancreatitis is a condition in which the pancreas gradually becomes infected and inflamed and does not heal and reaches a state of permanent pancreatic damage. It is called chronic pancreatitis.
- => Chronic pancreatitis takes many years to develop but is estimated to last 10 years or more.
2) Explain the Etiology/cause of chronic pancreatitis. Give the causes of chronic pancreatitis.
- Due to long-term alcohol intake.
- Hereditary.
- Due to hypercalcemia.
- Due to blockage of pancreatic duct.
- Due to cystic fibrosis.
- Due to the use of certain types of medication.
- Due to hyperparathyroidism.
- Due to certain types of autoimmune conditions.
- Due to an increase in the amount of lipids in the body.
3) explain the Clinical manifestation/sign and symptoms of the cronic pancreatitis.Tell the symptoms and signs of chronic pancreatitis#
- Pain in the upper abdominal area.
- Vomiting with pain.
- Weight loss.
- Loss of appetite.
- Abdominal bloating.
- Abdominal cramps. To be.
- diarrhea.
- diabetes mellitus.
- malabsorption.
- flatulence (flatulence).
- smelly and greasy feaceas ( stools).
- pale or clay colour stool.
4) Explain the diagnostic evaluation of the chronic pancreatitis. Write a diagnostic evaluation of chronic pancreatitis.
- history taking and physical examination.
- ultrasound.
- X rays.
- ct scan.
- glucose tolerance test.
- ERCP ( Endoscopic retrograde cholangio pancreatography ) for analysing the composition of juice.
- blood, urin and stool test.
5)explain the management of the patient with the cronic pancreatitis . क्रोनी पां Write medical management.
1)Maintain adequate nutritional status of the patient.
- => Do not provide fluid and food orally to the patient.
- => Provide fluid through the patient’s intravenous line.
- => If the patient is vomiting, insert a tube from the nose into the stomach to remove fluid and air.
- => If the patient is experiencing continuous weight loss, provide nasogastric feeding to the patient.
2)advise the patient about stopping drinking and smoking.
- => Advise the patient to stop alcohol.
- => Advise the patient to avoid smoking.
3)Advice about dietary modifications:=
- => The pancreas plays an important role in digestion, so now, due to pancreatic disease, instead of taking large amounts of food three times a day, the patient should be asked to take small but frequent amounts of food.
- Tell the patient to avoid fatty foods.
4)control pain of the patient:=
- Patient’s pain level is in different amounts, if the patient is experiencing mild level of pain then paracetamol should be provided and if the patient is experiencing severe pain then drugs like morphine should also be provided.
- => Due to the disease condition of the pancreas, the pancreas cannot release the enzyme, so the patient should be provided with insulin as a replacement.
surgical management
1)endoscopy surgery:=
- => In this surgery, a narrow, hollow flexible tube is inserted into the digestive system under ultrasound guidance.
- =>This device has a small deflated balloon at the tip of an endoscope.
- => When the balloon reaches the duct, it is inflated, widening the duct.
- => Then a stent is placed in it so that the duct does not narrow again.
2)Pancreas Resection:
- => In this procedure, the head of the pancreas is surgically removed.
- => This procedure not only reduces pain but also reduces the pressure on the duct.
#beger procedure
- => In this procedure, the inflamed head of the pancreas is resected.
#Frey procedures
- => The Frey procedure is mainly performed when it is determined that the pain is caused by inflammation of the head of the pancreas as well as blockage of the duct.
- => In this procedure, the head of the pancreas is surgically removed and the duct is decompressed and connected directly to the intestine.
#PPPD ( pylorus – sparing pancreaticoduodenectomy)
- => In this procedure, the gallbladder, duct, and head of the pancreas are surgically removed.
- => This is mainly done when there is severe chronic pain, in which the head of the inflamed pancreas and the blocked duct are removed.
- => This procedure is a very effective procedure for reducing pain.
- => But this procedure increases the chances of infection and internal bleeding.
3) Pancreatectomy
#partial pancreactomy
- => In partial pancreatectomy, some body parts of the pancreas are removed, mainly the pancreas body and tail.
#total pancreactomy (Total Pancreatectomy)
- => In total pancreatectomy, the entire pancreas is removed, so the patient has to rely on continuous medical treatment to perform some of the body’s vital functions of the pancreas.
## explain the nursing management of patients with the chronic pancreatitis. Write the nursing management of patients with chronic pancreatitis#
- Provide analgesic medicine to relieve the patient’s pain. Ex:=meperidine.
- Avoid oral fluids and provide total parenteral nutrition to the patient.
- Provide mind diversanal therapy to relieve the patient’s discomfort.
- Ask the patient to maintain his oral hygiene.
- Ask the patient to take frequent bed rest.
- Give the patient intra Provide fluids and electrolytes through the venous route.
- Check the side of the wound that is being drained for any infection or inflammation.
- Provide the patient with a semi-fowler position to improve breathing patterns.
- Encourage deep breathing exercises to improve breathing patterns.
- Avoid heavy lifting of the patient Say.
- Continuously monitor the patient’s vital signs.
- Monitor the patient’s abdominal girth daily.
- Carefully monitor the patient for any abnormal signs and symptoms of the neurological, cardiovascular and respiratory systems.
- Provide psychological support to the patient.
- Provide a calm and comfortable environment to the patient.
- Clear all doubts of the patient and his family members and do not give him false assurance.
1)Define/explain pancreatic cancer. Define pancreatic cancer.
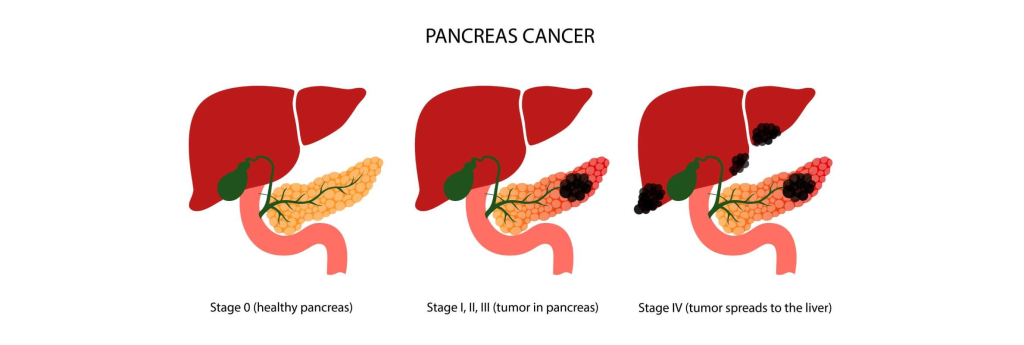
- => Pancreatic carcinoma is called cancer of the pancreas.
- => In pancreatic cancer, there is abnormal and uncontrolled growth of pancreatic cells and the formation of a tumor.
- => This pancreatic tumor is most common in the head and body of the pancreas.
- => Pancreatic cancer spreads rapidly and mainly spreads to the stomach, gallbladder, and duodenum, and can also spread to the lymphatic system and distal organs.
2)explain the types of pancreatic tumor. State the type of pancreatic tumor.
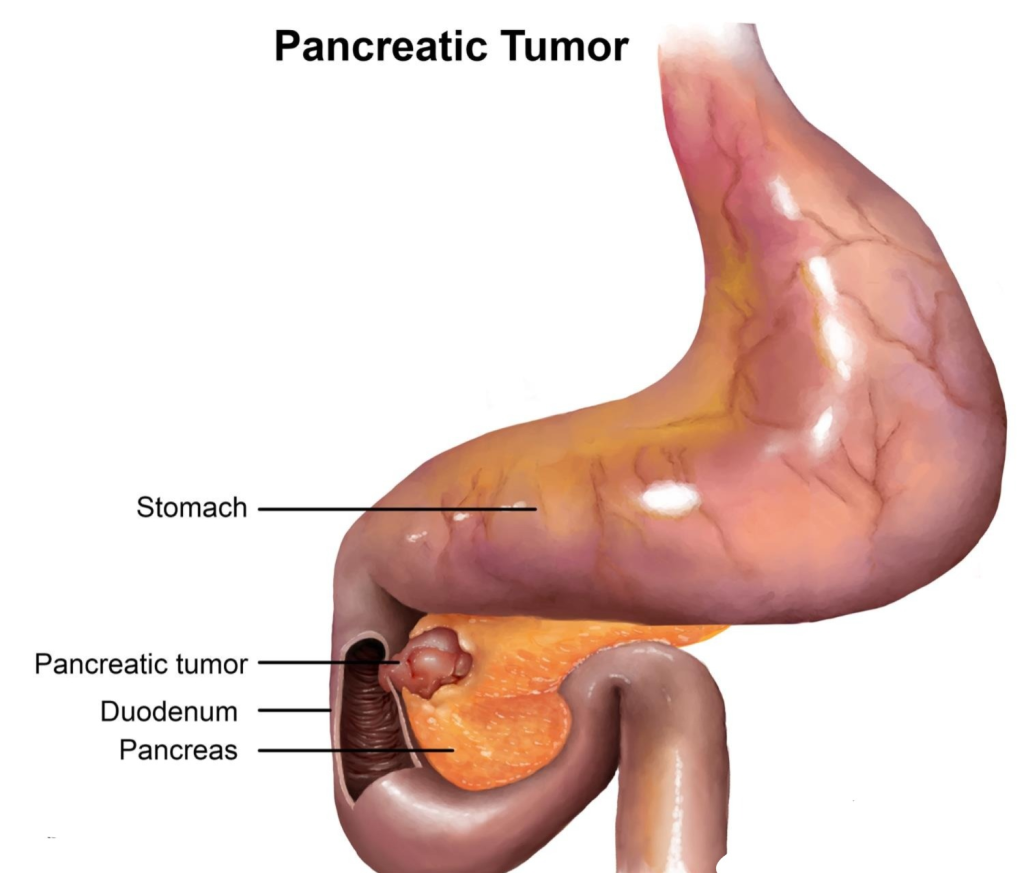
••> There are two types of pancreatic tumors.
1)exocrine tumor
( Exocrine tumor) ,
2)endocrine tumor
( Endocrine tumor)
1)exocrine tumor/pancreatic edinocarcinoma. ( Exocrine tumor/ Pancreatic adenocarcinoma) ,
- => Exocrine tumor is the most common type of pancreatic cancer.
- => In this cancer, cancer is found in the part of the pancreatic gland that secretes digestive enzymes.
- => Most exocrine pancreatic tumors are malignant (cancerous).
- =>example of exocrine gland tumor is:= Adenocarcinoma ( adenocarcinoma)
2)endocrine tumor/pancreatic neuroendocrine tumor ( endocrine tumor/ pancreatic endocrine tumor)
=> The cells of the pancreas that secrete hormones are called the endocrine portion.
=>Tumors that develop in this endocrine portion are called endocrine tumors/pancreatic neuroendocrine tumors, and these endocrine tumors are also called islet cell tumors.
=> These endocrine pancreatic tumors are rare.
=> there are subtypes of islet cell tumor that are named according to the type of hormone secreting cells they originate from:=
1)Glucogonomas (Glucogonomas)
- => This type of tumor arises from the cells that secrete glucagon.
2) Insulinomas
- => This tumor arises from the cells of the pancreas that produce insulin.
3) Somatostatinomas
- => This tumor arises from the cells of the pancreas that release the hormone somatostatin.
4)Gastrinomas
- => Gastrinomas are tumors that arise from cells that release the hormone gastrin.
5)Vipnomas (vasoactive intestinal peptide)
- => A pancreatic mass tumor arises from a cell that releases vasoactive intestinal peptide.
3)Explain the stages of the pancreatic tumor. Write the stages of pancreatic tumor.
1)stage 1:=
- => In this stage, the cancer is confined to the pancreas.
2)stage:=2
- => In this stage, the cancer in the pancreas has spread to nearby tissues, organs, and lymph nodes.
3)Stage:3:=
- => In this stage, the cancer in the pancreas has spread to the blood vessels and lymph nodes.
4)stage:=4
- => In this stage, the cancer spreads to the distal parts such as the liver, lungs and the lining of the abdominal organs.
4)explain the Etiology/cause of pancreatic cancer. Explain the causes of pancreatic cancer.
- The exact cause is unknown.
- Smoking.
- Due to advanced age.
- Due to overweight.
- Male sex.
- Due to chronic pancreatitis.
- Due to diabetes mellitus.
- Due to a family history of pancreatic cancer.
- due to surgery for a peptic ulcer.
- due to occupational exposure to carcinogens.
- diet high in meat, cholesterol, fried food, and nitrosomide.
- family history of genetic syndrome that can increase cancer risk including,
- •> BRCA 2 Gene mutation,
•>Peutz jeghers syndrome,
•>Lynch syndrome,
•>Familial atypical mole-malignant malinonoma (FAMMM).
5) Explain clinical manifestation/sign and symptoms of pancreatic cancer. Write the signs and symptoms of pancreatic cancer.
- Pain in the upper abdominal area.
- Abdominal distension.
- Jaundice.
- nausea,
- vomiting,
- Loss of appetite,
- Indigestion,
- Fever,
- Feeling cold,
- Itching,
- Weakness Coming,
- Passing pale and gray colored stools.
- Steatorrhea (= excess fat in stool),
- Bone pain,
- Darkening of the color of the urine,
- Difficulty in sleeping.
6) Explain the diagnostic evaluation of pancreatic cancer. Write a diagnostic evaluation of pancreatic cancer.
- history taking and physical examination.
- routine blood tests,
- liver function test,
- angiogram,
- endoscopic
- Ultrasound,
- Barium swallow,
- Pancreatic biopsy,
- MRI,
- Computed tomography (ct scan),
- Percutaneous transhepatic cholangiogtaphy,
- Positron emission tomography,
7)explain the management of pancreatic cancer. Write the management of pancreatic cancer.
## surgery##
- In surgery, all parts of the pancreas are removed.
1) Pancreatoduodenectomy (pancreatoduodenectomy) )
- => In this surgery, the duodenum (duodenam:=the initial part of the small intestine), the head of the pancreas, and the gallbladder are removed.
- => Then the remaining pancreas, bile duct, and stomach are joined to the intestine.
- => The remaining bile duct is then attached directly to the small intestine so that pancreatic juice and bile can flow directly into the intestine.
2)Distal pancreatectomy
- => In this surgery, only the body and tail of the pancreas are removed.
- => In most cases, the spleen is also removed.
- => This surgery is mainly used to remove tumors in the body and tail of the pancreas.
- => This procedure is mainly used to treat islet cell and neuroendocrine tumors.
3)Total pancreactomy
- => In this procedure, the entire pancreas and along with it the spleen are removed.
- => This surgery is mainly used to remove tumors in the head and body of the pancreas.
- => Palliative surgery is used when pancreatic cancer cannot be removed.
- => In this surgery, the common bile duct and duodenum are bypassed.
2) Chemotherapy
- => Chemotherapy uses medicine to destroy abnormal cells.
- Ex:=gemcitabine,
Flurouracil,
Capacitabine.
3)Radiation therapy (radiation therapy)
- => Radiotherapy uses high energy gamma rays to destroy abnormal cells.
4)Target therapy
- => Targeted therapy uses medicine to inhibit the growth and multiplication of abnormal cells.
5) Dietary management
- => Adequate dietary management plays a very important role in cancer.
- => Ask the patient to eat small and frequent amounts of food.
- => Ask the patient to eat soft, light, and easily digestible food.
- => Provide nutritional supplements to the patient.
- => Ask the patient to avoid high fat.
- => Tell the patient to avoid alcohol and smoking.
##Nursing management of the patient with pancreatic cancer. Write the nursing management of the patient with pancreatic cancer#
- Assess the patient’s pain level.
- Assess the patient’s condition of jaundice.
- Assess the patient’s itching in the body.
- Assess the patient’s urine.
- Assess the patient’s vital signs.
- Assess the patient’s prothrombin time.
- Report immediately if the patient has abdominal distension, shock, or blood in the stool.
- Monitor the secretion drained through the nasogastric tube.
- Maintain the patency of the nasogastric tube.
- Provide nutritional supplementation to the patient.
- Provide the patient with a low-fat, high-carbohydrate, and high-protein diet.
- Instruct the patient to eat small, frequent meals.
- Provide the patient with a semi-fowler position to improve proper breathing.
- Provide the patient with pancreatic enzyme supplements.
- Provide psychological support to the patient.
- Ask the patient and his family members to explain his feelings.
define/explain cholecystitis.
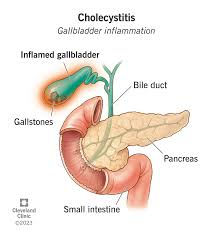
=> Inflammation and swelling of the gallbladder is called cholecystitis.
=> There are also two types of cholecystitis.
1)Acute cholecystitis (acute cholecystitis),
- => The onset of acute cholecystitis is sudden.
2)chronic cholecystitis (chronic cholecystitis).
- => Chronic cholecystitis occurs progressively and gradually.
##other types of cholecystitis:=
1)Calculous cholecystitis (calculous cholecystitis)
- => In this condition, the outflow of bile is impaired due to stones in the gallbladder.
- => Due to this, bile remains in the gallbladder and due to this, chemical reactions are observed.
- => Due to this, the blood vessels in the gallbladder are compressed and the vascular supply is compromised.
- => This ultimately leads to gangrene formation and perforation.
2)Acaculaous cholecystitis (Accalculous cholecystitis)
- => Acalculous cholecystitis is not caused by any gallstone but by any major surgical procedure, severe trauma, any bacterial infection and multiple blood transfusions which cause obstruction of the cystic duct.
2)explain Etiology/cause of the cholecystitis.
- Gallstone,
- Block of cystic duct Due to,
- ischemia,
- due to obesity disorder,
- due to infection by any microorganism.
- due to any allergic reaction.
3) explain the Clinical manifestation/sign and symptoms of colycystitis. State the symptoms and signs of cholecystitis#
- Abdominal pain,
- Abdominal tenderness,
- nausea,
- vomiting,
- Indigestion,
- Low grade fever,
- Jaundice,
- Abdominal fullness and bloating.
- Clay coloured stool.
4)explain the diagnostic evaluation of the cholecystitis. Write a diagnostic evaluation of cholecystitis#
- history tacking and physical examination.
- abdominal ultrasound,
- ct scan,
- x rays,
- colecystogram,
- gallbladder radionuclide scane.
- blood test.
5) Explain the management of the patient with the cholecystitis. Write the management of the patient with cholecystitis.
- Provide intravenous fluid to the patient.
- Provide intravenous fluid to the patient.
- If the patient is experiencing nausea and vomiting, provide antiemetic medicine.
- Maintain the patient’s fluid and electrolyte balance.
- If the patient is experiencing pain, provide analgesic medicine.
- If the patient has any infection, provide antibiotic medicine.
- Ex:=pipperacilline,
- Ampicillin,
- Metronidazole,
- Cifalosporine,
- Ciprofloxacine,
- surgery includes removal of the gall bladder ( cholecystectomy).
- ( ERCP:= Endoscopic retrograde cholangio pancreatography. )
- => This procedure is mainly used to remove stones in the common bile duct and open the bile duct to drain them.
1) Define/explain cholelithiasis. Define cholethiasis.
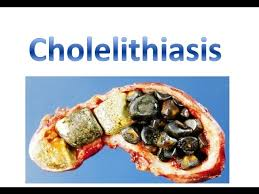
- => Cholelithiasis is a condition in which stones (hard deposits/calculi) of solid composition form in the gallbladder.
2) Explain the type of gall stones.
1) Cholesterol stone (cholesterol stone)
- => Cholesterol stones are the most common type of stone
- =>Which mainly forms due to the presence of too much cholesterol in the bile.
2) Pigment stone ( Pigment stone)
- => Pigment stones are mainly formed due to excessive amount of bile in the gall bladder.
- => Pigment stones dissolve and can be surgically removed.
2) Explain the Etiology/cause of cholilithiasis. Give the causes of cholelithiasis.
- Due to inadequate removal of bile from the gallbladder during pregnancy.
- Due to infection in the biliary tract.
- Liver cirrhosis.
- Due to sickle cell anemia and chronic hemolytic anemia.
- Diabetes mellitus.
- Due to obesity.
- Due to overweight.
- Due to bone marrow transplantation.
- Intravenous nutritional.
- Obesity.
- Inflammatory bowel Diseases.
- Due to some types of medication.
3)explain the Clinical manifestation/sign and symptoms of cholilithiasis. Write the signs and symptoms of cholelithiasis.
- Pain in the upper abdomen.
- Abdominal swelling.
- Abdominal bloating.
- Abdominal tenderness.
- Gallbladder Distended.
- Gallbladder infected and inflamed.
- clay coloured stool.
- Fever.
- Feeling cold.
- Loss of appetite.
- nausea without vomiting.
- Sweating.
- Indigestion.
- Jaundice.
4) Explain the diagnostic evaluation of the patient with the cholelithiasis. Write a diagnostic evaluation of a patient with cholelithiasis.
- history taking and physical examination.
- Abdominal ultrasound.
- abdominal x rays.
- endoscopic ultrasound.
- colecystography.
- blood test .
- Endoscopic retrograde cholangiopancreatography( ERCP).
- percutaneous transhepatic cholangiogram (PTCA).
- cholecystography.
- Murphy sign.
5)Explain the management of the patient with cholelithiasis. Write the management of a patient with cholelithiasis.
- Tell the patient to take a low fat diet.
- If the patient is bleeding, has itching in the body, jaundice, then administer vitamin K to the patient.
- If the patient is in pain, then provide analgesic medicine.
- If the patient is If there is spasmodic pain, provide antispasmodic medicine and anticholinergic medicine.
- If the patient has a condition of nausea and vomiting, provide antiemetic medicine.
- Provide intravenous fluid to the patient.
- Provide antibiotic medicine to the patient.
- If the patient has a condition of severe jaundice, provide cholestyramide medicine. To be done.
- Provide urodeoxycholic acid (UDCA) and chenodeoxycholic acid (CDCA) to the patient to dissolve cholesterol.
- # done dissolution therapy:=
- => In this dissolution therapy, mono octane or methyl tertiary butyl is administered directly into the gallbladder by inserting a tube or catheter and the stone present in the gallbladder is dissolved.
- The stone is removed through instrumentation.
- Do extra corporeal shock wave lithotripsy.
- Do intracorporeal lithotripsy.
## explain the surgical management ##
1)elecro leproscopy cholecystectomy ( Electro laparoscopy cholecystectomy).
2)minicholecystectomy ( Minicholecystectomy).
3) surgical choledocholecystectomy ( Surgical choledocholecystectomy).
4)percutaneous cholecystectomy ( Percutaneous cholecystectomy) Cholecystectomy).
##Nursing management ##
##Nursing assessment ##
- Assess the patient’s pain level.
- Assess the patient’s level of consciousness and activity level To do.
- Assess the patient’s anxiety level.
- Assess the patient’s respiratory status and nutritional status.
- Monitor the patient’s vital signs.
## Nursing management ##
- Assess the patient’s pain level.
- Advise the patient on deep breathing techniques.
- Provide analgesic medicine to the patient.
- Assess the patient’s respiratory rate, depth and breath sounds.
- Report immediately if the patient is experiencing abdominal pain, nausea and vomiting Do.
- Advise the patient to maintain a low-fat and high-protein diet.
- Monitor the patient’s vital signs regularly.
- Assess the patency of the patient’s intravenous line.
- If the patient requires a blood transfusion, cross-match.
- The patient has signs and symptoms of any infection. To assess whether or not.
- Monitor the patient’s vital signs.
- Ask the patient to do deep breathing exercises.
- Maintain the patient’s intake output chart.
- If the patient is in pain
- Provide analgesic medicine.
- Advise the patient to continue exercising.
1)explain/define choledocolithiasis.

- => Choledocholithiasis is a condition in which gallstones are present in the common bile duct. It is called choledocholithiasis.
- => Gallstones are mainly formed in the gallbladder, then they pass from the gallbladder into the common bile duct and cystic duct and then they obstruct the common bile duct.
2)explain the Etiology/cause of choledocolithiasis. Explain the Etiology/cause of choledocolithiasis
- Because of gallstones.
- Due to obesity.
- Due to stasis in the gallbladder.
- Due to gallbladder dysfunction.
- Due to certain types of medication.
- Hereditary.
- Due to obesity.
- Billiary stasis Cause.
- Due to any inflammation.
- Due to any infection.
3) explain the sign and symptoms/clinical manifestation of choledocolithiasis. Pain in the upper part of the abdomen.
- obstructive jaundice
- dark urine.
- fever.
- clay-colored stool.
- pruritus.
- Nozia.
- Vomiting.
- loss of appetite.
- Bleeding.
- Steatorrhea (presence of the fat into the stool).
4) Explain the diagnostic evaluation of choledocholithiasis. Write the diagnostic evolution of choledocholithiasis.
- history tacking and physical examination.
- Abdominal ultrasound.
- Endoscopic ultrasound.
- Endoscopic retrograde cholangiography ( ERCP).
- Percutaneous transhepatic cholangiography ( PTCA).
- x rays.
- Ct scan.
- MRI.
- Complete blood count.
- liver function test.
- assess pancreatic enzyme level.
- Assess the bilirubin level.
5)explain the treatment of choledocolithiasis. Write the treatment of choledocolithiasis.
1) Billiary Endoscopic sphincterotomy ( BES)
- => This is mainly used to remove stones in the bile duct.
2)lethotropsy can be done.
3)Do cholecystectomy
- => Cholecystectomy is performed when stones are present in the gallbladder and bile duct.
4)Billiary stents
- => When surgery is not possible, biliary stenting is used to open the occlusion so that adequate drainage can occur.
Nursing management
- Advise the patient to engage in moderate amounts of physical activity.
- Advise the patient to consume fiber-rich foods.
- Advise the patient to follow a low-fat diet.
- A low-fat diet reduces the risk of stone formation.
- Monitor the patient’s vital signs.
- Assess the patient for any signs of dehydration.
- Monitor the patient’s intake output.
- Apply moisturizer after bathing to prevent itching.
- Keep nails short to prevent scratching.
- Instruct the patient to avoid bathing with hot water.
