ENGLISH-endocrine disorder (deepali) (part-2)(UPLOAD)
Definition:
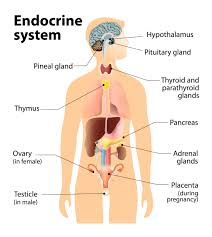
1) Give the full form of DM. Define the DM. (Give full form of DM and define DM.)

- Full form of DM IS DIABETES MALLITUS.( The full form of DM is Diabetes Mellitus).
- Diabetes Mellitus is a chronic metabolic disorder in which there is impairment in the metabolism of carbohydrates, proteins, and lipids. Mainly the metabolism of carbohydrates is altered.
- Diabetes is a condition in which the blood glucose level of a person’s body increases (Hyperglycemia).
- It mainly occurs if the body is not able to produce enough insulin or the cells do not respond to insulin in an adequate amount, therefore the metabolism of glucose cannot be normal, which causes a condition like diabetes mellitus.
IN DIABETES MALLITUS 3 ‘P’ SYMPTOMS

- P : POLYURIA ( FREQUENT URINATION : Frequent urination.),
- P: POLYDYPSIA ( INCREASED THIRST : Increased thirst.),
- P: POLYPHAGIA ( INCREASE HUNGER : Increased hunger. )
2) Define hypoglycemia

- Hypoglycemia is a condition in which the blood glucose level is lower than the normal level. This condition is called hypoglycemia.
- Normal blood glucose level is 60- 120 mg/dl.
- In hypoglycemia blood glucose level is less than 60 mg/dl
3) Define hyperglycemia or diabetic ketoacidosis (DKA). (Define hyperglycemia and diabetic ketoacidosis.)
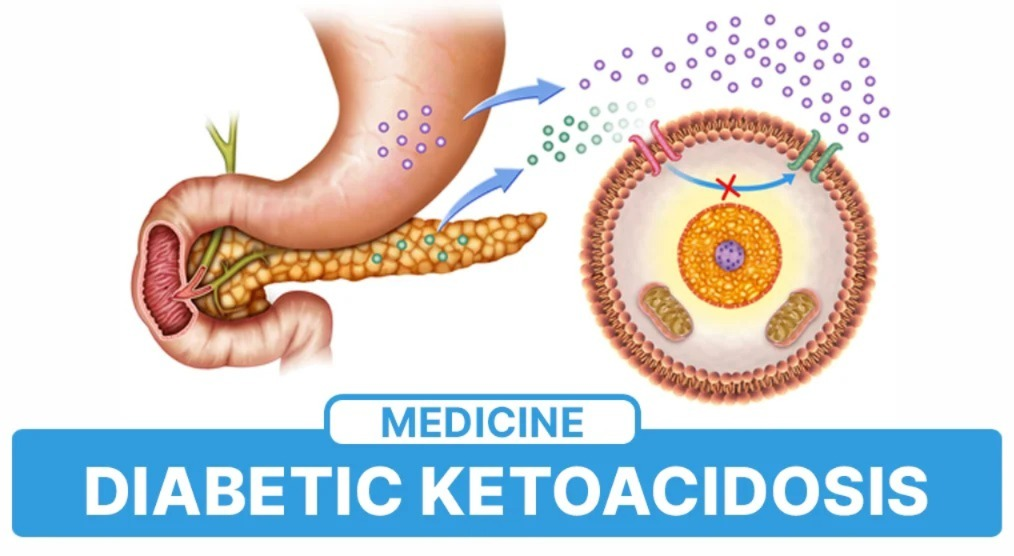
- Hyperglycemia is a condition in which the blood glucose level increases above the normal body glucose level.
- Diabetic ketoacidosis is a life-threatening complication of diabetes mellitus.
- Diabetic ketoacidosis is mainly caused by the absence of insulin or insufficient insulin in the body.
- It causes the metabolism of carbohydrates, proteins, and fats to be disrupted. Impairment is seen in the mother. In this condition, due to the absence of insulin, fat is metabolized instead of glucose and excess ketone bodies are released into the blood as waste, which damages the brain in the body.
- Diabetic ketoacidosis is an emergency condition that should be treated immediately.
- Normal blood glucose level is 60- 120mg / dl.
- In hyperglycemia blood glucose level is greater than 125 mg / dl.
4) Define Diabetic Nephropathy. (Define diabetic nephropathy.)
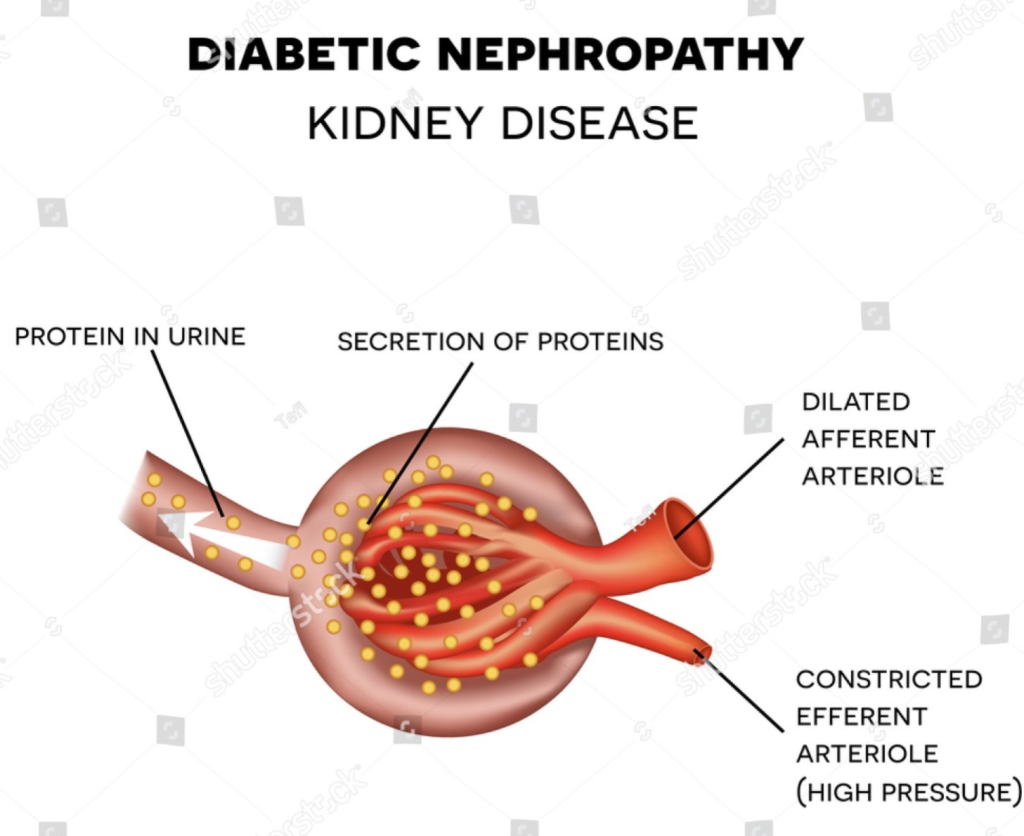
- Diabetic nephropathy or renal disease is mainly caused by diabetes. It is seen as a complication of microvascular changes due to which changes are mainly seen in the kidneys.
5) Define diabetic Neuropathies. (Define diabetic neuropathy.)
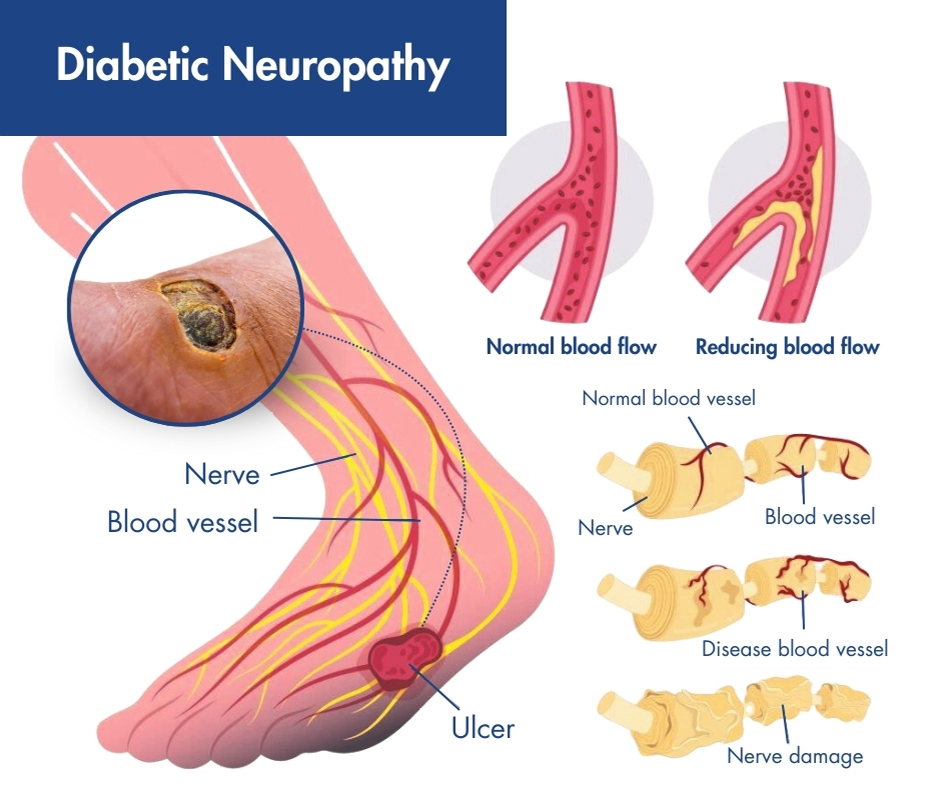
- Diabetic neuropathy is a group of diseases in which all types of nerves are affected such as anatomical nerves, spinal nerves, motor nerves etc. and this problem mainly depends on the affected nerve cell location.
- Diabetic neuropathy is a complication of diabetes that affects the nervous system.
6) Define Hypothyroidism.
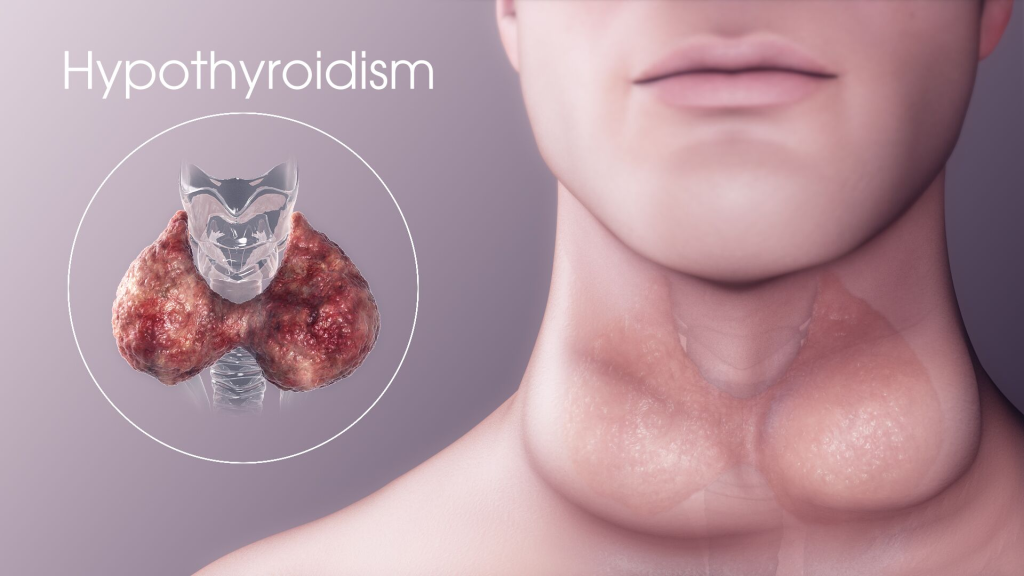
- Hypothyroidism is a condition in which the level of thyroid hormone in the body is lower than normal.
7) Define hyperthyroidism.
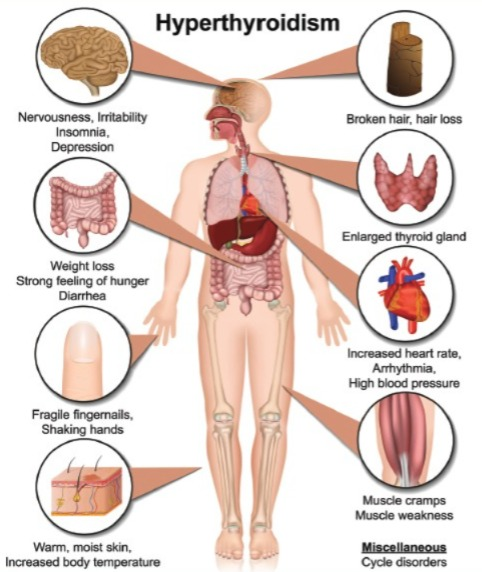
- Hyperthyroidism is a condition in which the amount of thyroid hormone in the body increases above normal.
8) Define Thyroid cancer. (Define thyroid cancer.)
- The thyroid gland is located in the neck.
- The abnormal and uncontrolled growth of cells in the thyroid gland and the formation of tumor-like structures is called thyroid cancer.
9) Define hyperparathyroidism :
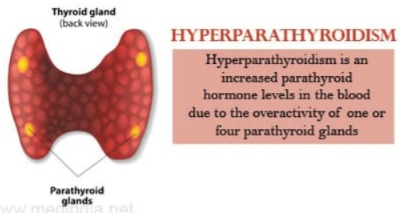
- There are four parathyroid glands in the neck of a human being.
- These glands are oval in shape.
- Which produces parathyroid hormone, which is a hormone that maintains the level of calcium in the blood.
- But when this parathyroid gland secretes too much parathyroid hormone into the body and blood stream, the condition of hyperparathyroidism occurs. is.
10) Define hypoparathyroidism
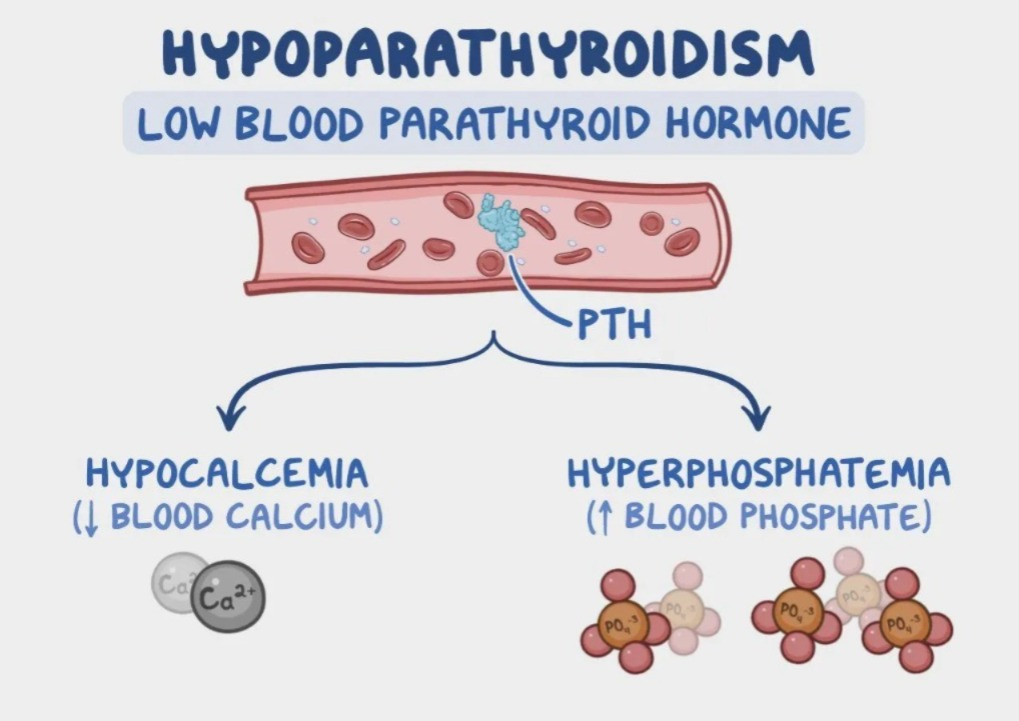
- Hypoparathyroidism is a disorder of the parathyroid gland.
- Hypoparathyroidism is caused by a deficiency of parathyroid hormone.
- Due to this, the amount of phosphate in the blood is elevated and the amount of calcium is low.
11) Define thyroiditis
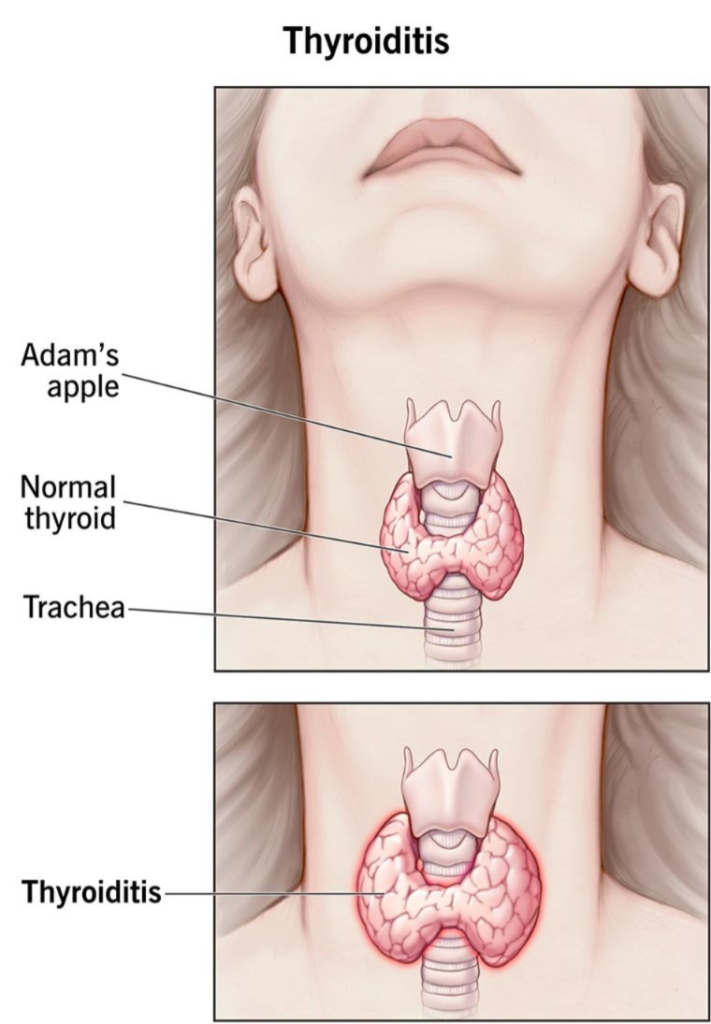
- Infection and inflammation of the thyroid gland is called thyroiditis.
- acute suppurative painful thyroiditis.
- subacute thyroiditis.
- Chronic thyroiditis (Hashimoto’s disease).
- lymphocytic. Etc. are its types.
12) Define Addition’s disease.
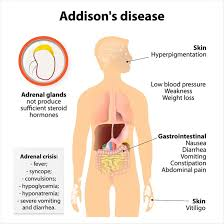
- Addison’s disease is a rare but chronic disease.
- It is caused by adrenal gland insufficiency, mainly due to inadequate secretion of adrenal gland hormones (glucocorticoids/mineralocorticoids).
13) Define Chusing’s syndrome.
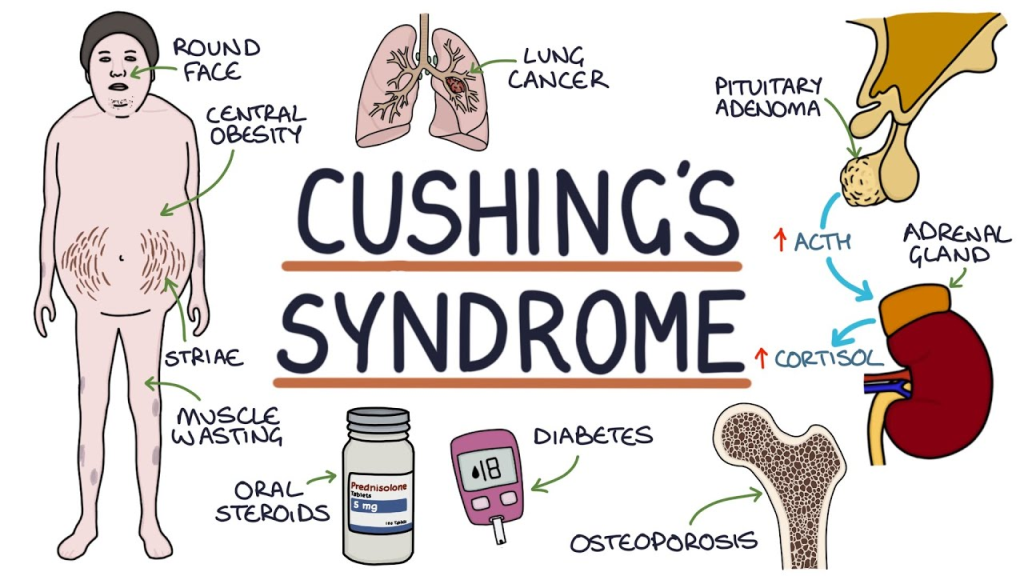
- Cushing’s syndrome is a It is an endocrine disorder.
- Which is mainly caused by excessive secretion of the adrenal gland.
14) Define Pheochromocytoma. (Define pheochromocytoma.)
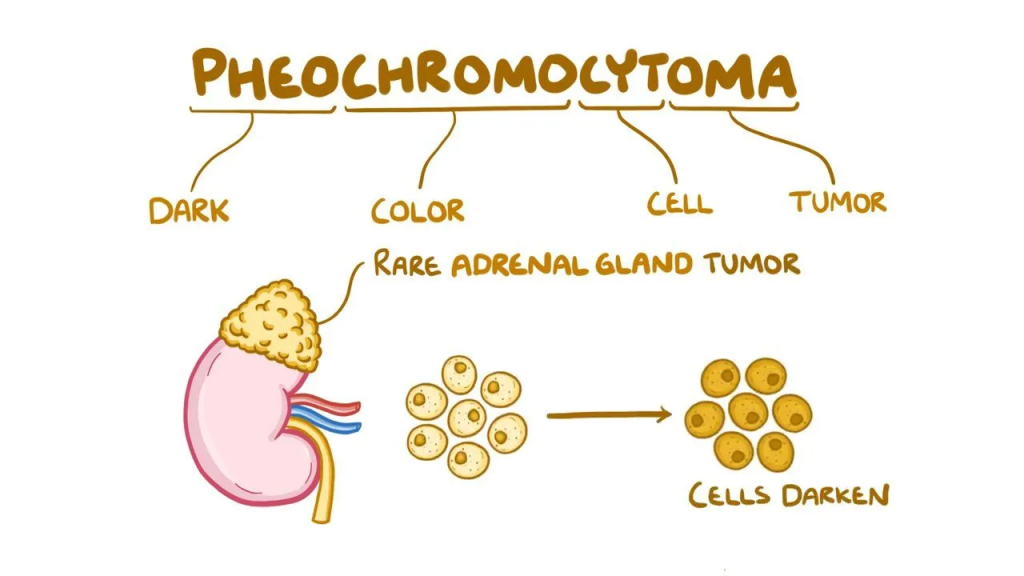
- Pheochromocytomas are a type of tumor in the adrenal gland. It is a tumor.
- It causes excessive amounts of epinephrine and norepinephrine hormones to be released, which elevates heart rate, metabolism, and blood pressure.
15) Define diabetes insipidus.
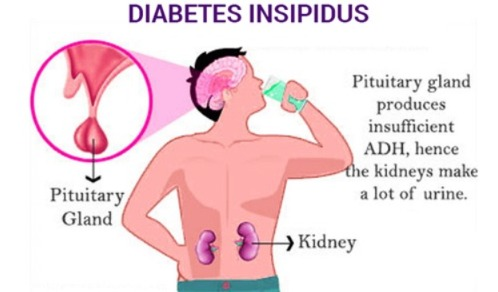
- Diabetes insipidus is caused by a disorder of the posterior lobe of the pituitary gland.
- Vasopressin (Antidiuretic hormone) is secreted in low amounts. Due to this, conditions like Polydipsia and Polyuria are seen and excessive amounts of urine are excreted from the body.
16) Define Hypopituitarism.
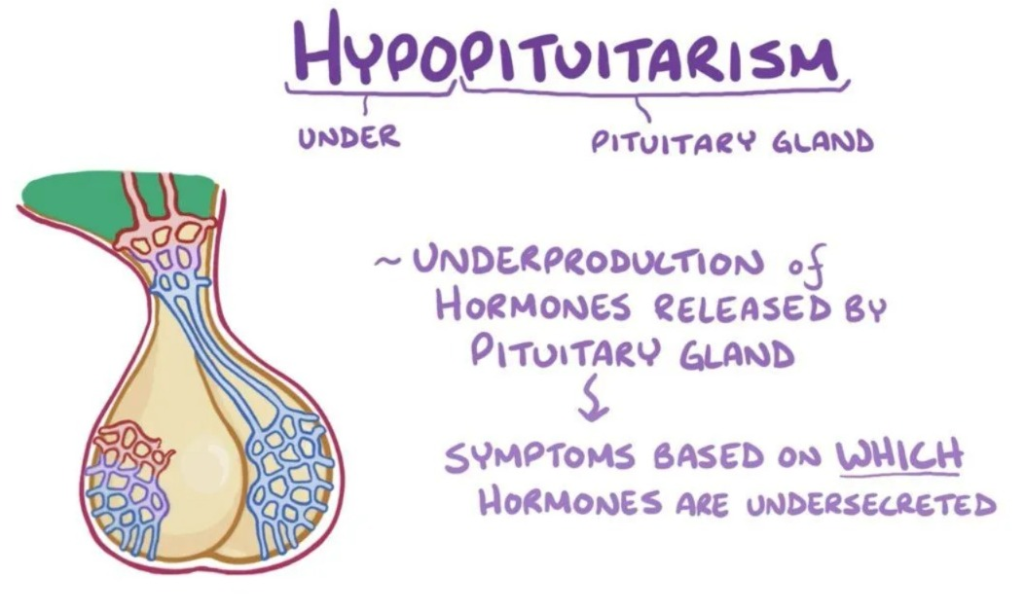
- Hypopituitarism is a condition in which the pituitary gland does not secrete enough of its hormones.
17) Define Acromegaly.
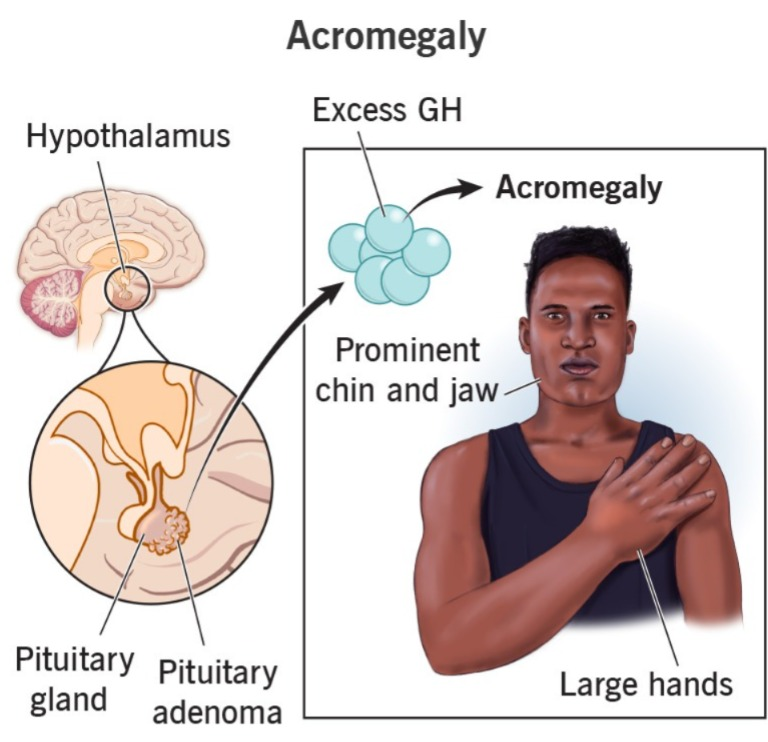
- Acromegaly is a long-term condition in which excessive amounts of growth hormone are secreted, causing enlargement of body tissues and organs.
17) Define Gigantism. Do.)
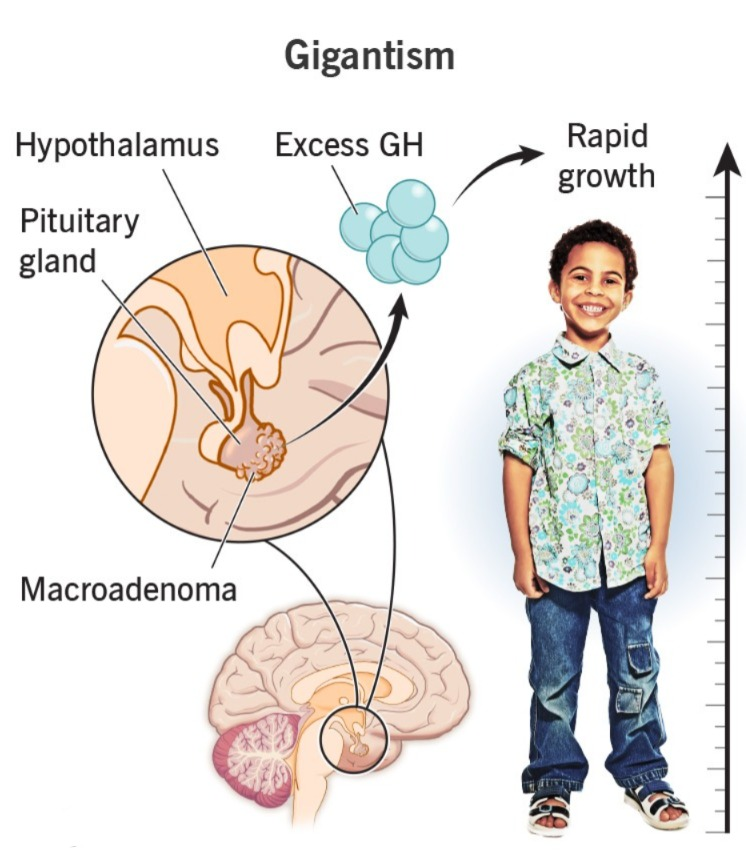
- Gigantism is an abnormally increased body growth rate. It is mainly caused by excessive secretion of growth hormone during childhood. It is seen in children due to excessive secretion of growth hormone before the growth plate of the bone closes.
18) Define pituitary gland tumor. (Define Pituitary Gland Tumor.)
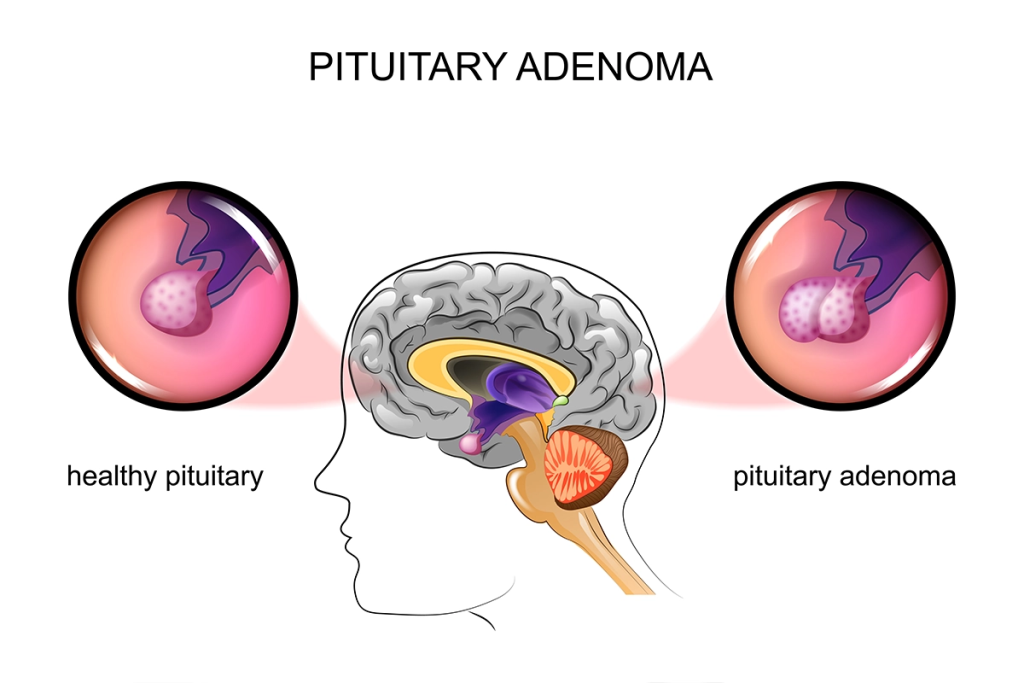
A pituitary gland tumor is a condition in which there is abnormal and uncontrolled cell growth. It occurs in the pituitary gland and causes the formation of tumors, which causes disturbances in its function.
1) Explain the diabetes malitus.
- Diabetes is a chronic metabolic disorder. In which there is impairment of carbohydrate, protein and lipid metabolism. Changes are mainly seen in the metabolism of carbohydrates.
- Diabetes is a group of metabolic disorders in which a person’s blood sugar level is high. This is mainly seen when the insulin secretion in the body is less than normal and there is any impairment in the action of insulin, resulting in high blood sugar levels in the body.
The “3 P” syndrome is seen in diabetes mellitus.

- 1) P : polyuria (frequent urination),
- 2) P : polydypsia (increase thirst),
- 3) P : polyphagia (increase hunger).
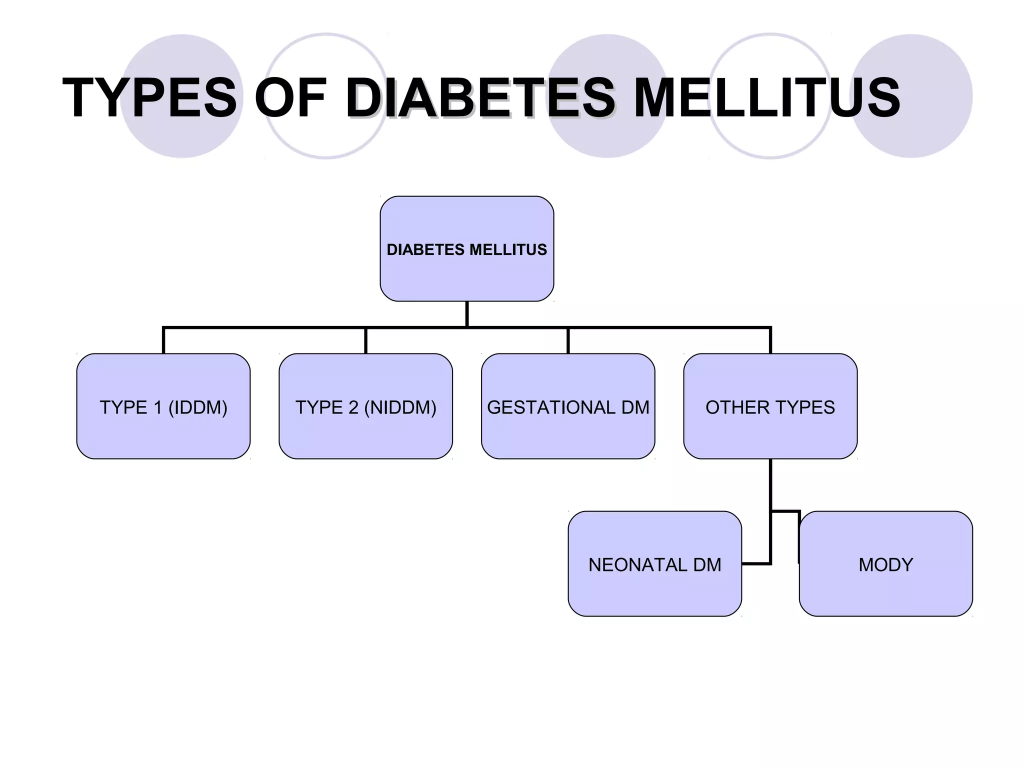
2) Explain the type of diabetes mellitus. Explain the types of diabetes mellitus.
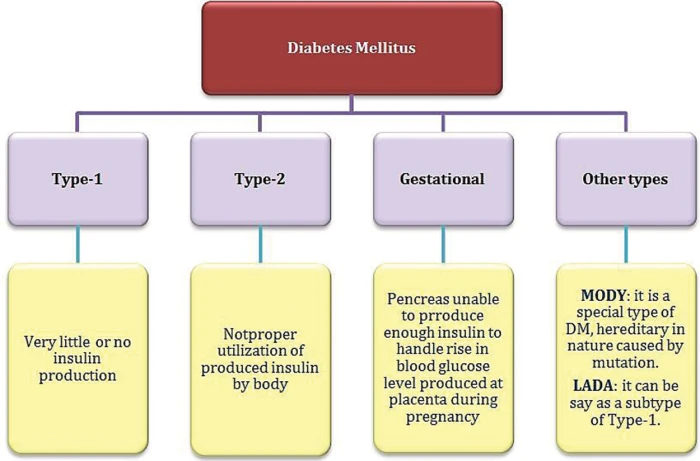
There are mainly four types of diabetes.
- Type:=1 ( IDDM )insulin dependent diabetes malitus( Insulin Dependent Diabetes Malitus).
- Type:=2 ( NIDDM ) Non Insulin Dependent Diabetes Malitus( Non Insulin Dependent Diabetes Malitus).
- Type:=3 diabetes mallitus associated other diseases conditions( Diabetes Malitis Associated Other Disease Condition).
- Type:=4 GDM ( gestational diabetes malitus:= gestational diabetes malitus )
Type:=1 ( IDDM ) insulin dependent diabetes mellitus.
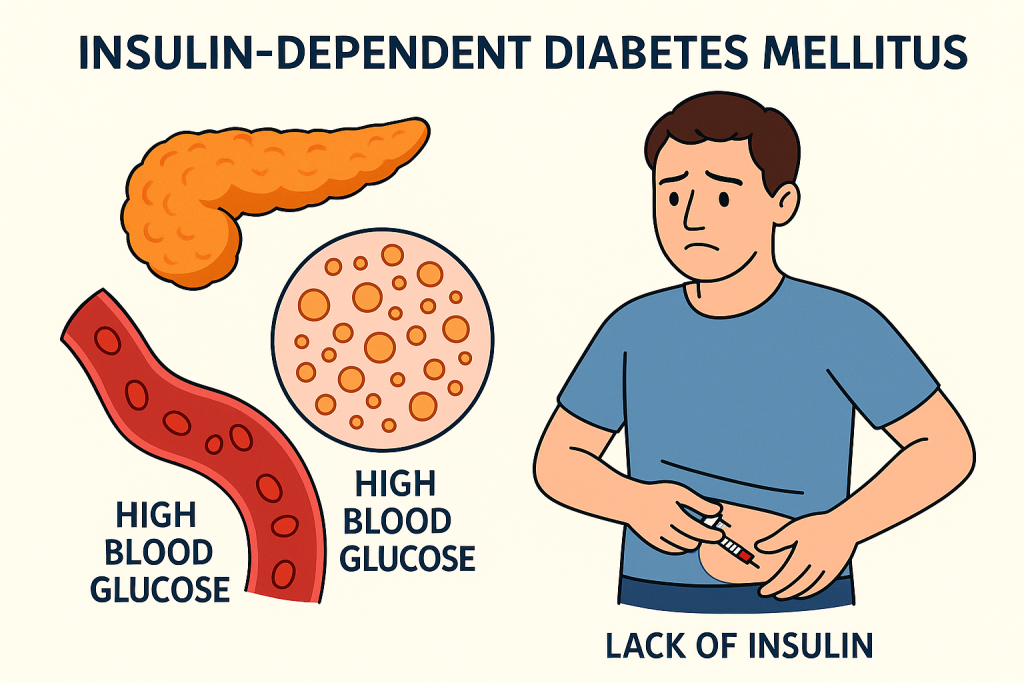
- This is a type of diabetes mellitus in which the pancreatic beta cells in the body, which are responsible for producing insulin, are destroyed due to any reason or autoimmune disease, resulting in a total deficiency of insulin.
- In this, due to a total deficiency of insulin, insulin is taken through injection.
- This type of diabetes is mainly seen before the age of 30.
Type:=2 ( NIDDM ) Non insulin dependent diabetes mellitus.

- Type 2 diabetes is mainly caused by insulin resistance or insulin deficiency, in which the pancreatic cells produce adequate amounts of insulin, but the body cells cannot use it properly, which causes the blood sugar level to rise.
- This type of diabetes is mainly caused by eating a proper diet, exercising, and making lifestyle changes. This type of diabetes can be prevented by making changes and increasing physical activity.
- This type of diabetes is mainly seen after the age of 30. Therefore, it is also called adult onset diabetes mellitus.
- If diabetes is not treated in the above way, then oral hypoglycemic agents are also taken.
Type:=3 diabetes mellitus associated other diseases conditions.
- Diabetes is also seen in the body due to any other disease. Its symptoms depend on the disease condition.
Type:=4 GDM ( gestational diabetes malitus (gestational diabetes malitus )
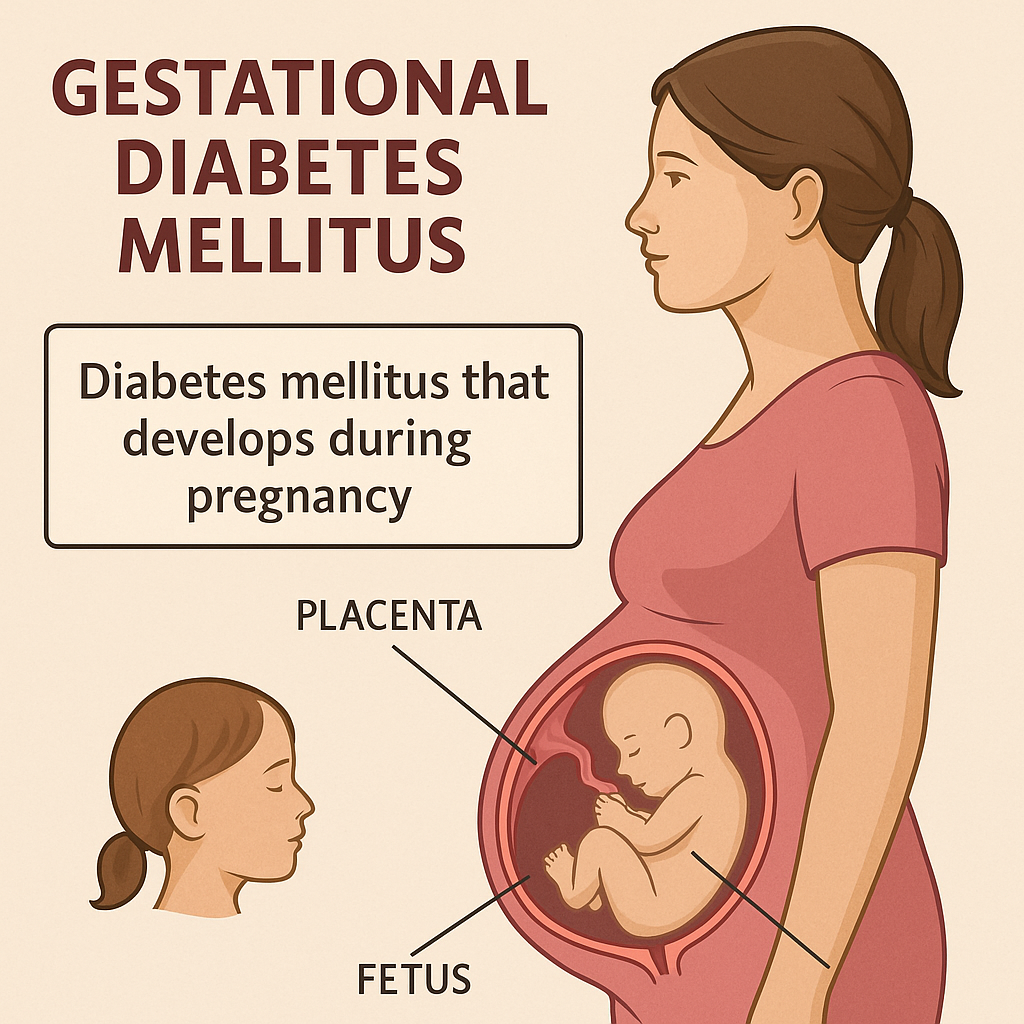
- This type of diabetes is mainly seen in women and even in those women, diabetes mellitus is seen during pregnancy due to glucose intolerance.
explain the Etiology of diabetes malitus.Explain the causes of diabetes malitus.
- inherited,
- environmental factor,
- Stress
- Genetic factor,
- Environmental factor,
- Obesity,
- diabetes from the other diseases conditions..
- during pregnancy Hormonal imbalance.
- Due to insulin deficiency.
- Despite insulin, cells become resistant to insulin.
- Due to excessive sugar intake.
- Due to sedentary lifestyle.
- Because of excess cholesterol in the body.
explain Clinical manifestation/sign and symptoms.
- 1) polyuria ( increase urine output),
- 2) polydipsia ( increase thirst),
- 3) polyphagia ( increase appetite)
- Fatigue (fatigue).
- weakness (weakness).
- Visual Changes (difficulty seeing).
- tingling and numbness on hands and feet.
- Dry skin.
- Sore that heals slowly.
- Frequent infections.
- Nausea.
- Vomiting.
- Decrease wound healing.
- Weight loss.
- abdominal pain.
Explain diagnostic evaluation (Write a diagnostic evaluation.)
History tacking and physical examination.
1) Fasting blood sugar (FBS)
- This test is done without eating or drinking anything for at least eight hours.
- The normal value of sugar in the blood should be less than 110 mg/dl (milligrams per deciliter).
- If the fasting blood glucose level is more than 125 mg/dl (milligrams per deciliter), then it is diagnosed as diabetes.
2)Random blood sugar ( RBS )
- In this, the sample can be taken at any time and there is no need to do any preparation.
- If the random blood glucose is more than 200mg/dl milligram per deciliter, then it is indicated as diabetes.
3)PP2bs( post prandial blood sugar )
- This test is done 2 hours after taking a full meal.
- Usually the blood glucose level reaches the peak level of glucose in the blood two hours after the meal, but if any smoking or drinking of caffeine is done, then alteration is seen in it.
3)glycosylated HB .
- In this, how much amount of glucose is present in the blood? This test is done to assess the amount of glucose attached to the molecule.
4) Glycosylated Albumin:
- Glucose is usually attached to albumin, so glycosylated albumin is used to assess average glucose levels.
5) Oral glucose tolerance test.(gtt)
- In this, the patient is provided with 150 mg of carbohydrate for three days.
- Then the patient’s fasting blood glucose level is checked.
- Then the client is given 75 grams of glucose to drink and then the patient’s glucose tolerance level is checked.
7)ketonuria :
- If ketones are present in the urine, it indicates that the body is using fat as a source of energy.
8) Proteinuria:
- If protein is present in the urine, it indicates that protein is being used as a major source of energy.
- 9)serum lipid profile.
- 10)serum BUN.
- 11)serum creatinine. etc. are tested.
3) Explain the management of diabetes malitus.
overall principle of management
- To eliminate the symptoms of hyperglycemia.
- To reduce microvascular and macrovascular complications of diabetes mellitus.
- To reduce blood glucose levels.
- The patient can achieve a normal lifestyle as much as possible.
- The patient can reduce blood glucose levels using education, dietary management, exercise, and pharmacological therapy.
patient education
- Provide appropriate health education to the patient and their family members.
- Teach how to self-monitor glucose.
- Teach how to monitor urine ketones if type 1 diabetes mellitus is present. (Urine examination)
- Teach the patient how to administer insulin.
- Teach the management of hypoglycemia.
- Provide education to the patient about foot and skin care.
- Teach the management of diabetes before, during, and after exercise.
- Patient’s life Providing education about style modification.
dietary management
aim of dietary management
- To reduce the symptoms of hyperglycemia.
- To reduce the symptoms of hypoglycemia that occur when hyperglycemia is treated.
- Reduce the overall blood glucose level of the body.
- Avoid diets that increase blood glucose levels.
- If the patient is obese, ask him to lose weight.
- Make the patient have regular food intake.
- Tell the patient not to take excess sugar.
- Advise the patient to eat a diet that contains adequate amounts of protein, carbohydrates, and fat.
dietary management
- The main goal of dietary management is to improve metabolic control in the diabetic client.
- Improve the patient’s blood glucose level and lipid levels To do.
- Create a daily food intake plan for the patient.
- Create a plan for the patient’s weight management.
- Provide adequate nutrition for the patient.
- A person’s lifestyle and habits play an important role in controlling and managing their disease.
- A balanced nutritional diet is very important for all patients. It is important.
- Asking the patient to increase protein intake in their diet, excessive protein intake increases renal function. And the glomerular filtration rate increases.
- Maintain the level of fat in the patient’s diet Maintain the daily cholesterol level in the diet and limit saturated fat and cholesterol.
- Provide carbohydrates according to the patient’s body requirement.
- Instruct the patient to take adequate amount of carbohydrates so that the energy requirement of the body can be maintained.
for type :1 diabetes special diet management includes
- Breakfast should be taken half or 1 hour after taking the morning insulin dose.
- Then a small amount of carbohydrates should be taken after three hours.
- Lunch should be taken four to five hours after taking the morning insulin.
- Foods that are sweet and contain sugar should not be consumed such as cakes, ice cream, jams, etc.
- Check the patient’s blood glucose level regularly.
- Be particular about amount, distribution and timing of nutrition.
- Carbohydrates should be taken in small amounts before exercise.
- The patient should be asked to check the amount of glucose, ketones and albumin in the urine and all these substances It is seen during fasting.
- Calorie restriction for obese clients.
Exercise:
- Advise the patient to do regular exercise to prevent and control his disease condition.
- Ask him to walk regularly.
- Ask him to ride a bicycle regularly.
- Ask him to swim.
- Take adequate amount of carbohydrates before and after exercise Explain the pharmacological management. It is responsible for maintaining blood glucose levels. It is used in the administration of insulin and oral hypoglycemic drugs. It is absorbed faster when insulin is given on the abdomen. When given on the arm and leg, its absorption decreases.
Time, course
1)Rapid acting insulin:=
- Ex:=Humalog.
- Its onset is within 10 to 15 minutes.
2)short acting insulin:=
- It is called regular insulin or R insulin or zinc crystalline insulin (czi).
- Its onset is 30 minutes.
3)Intermediate acting insulin:=
- It is also called regular R insulin (R insulin).
- And its onset period is after 3 to 4 hours and the patient needs to take food during this period.
4)Long acting insulin:=
- Ultra lente insulin or peakless insulin.
- Its onset time is 6-8 hours and its action lasts for 20 to 30 hours.
insulin dosage
- The starting dose of insulin is 0.5 units/kg/day is.
- Insulin is 2/3 dose in the morning and 1/3 dose in the evening.
- This dose can be increased or decreased based on food intake, exercise, and illness.
insulin pump therapy
- Use of small portable pumps It is used to administer insulin and its needle has to be changed daily.
combine therapy
The patient is provided with oral insulin.
oral antidiabetic agent:
- 1)sulfonyle uria,
- 2)meglitinides,
- 3)thiazolidinediones,
- 4)bigunides,
- 5)alpha glucoside inhibitor.
This therapy is mainly given to patients with type 2 diabetes.
patient teaching about insulin administration
Proper teaching should be provided to the patient for proper administration of insulin because if insulin is not administered properly, tissue damage or conditions like insulin shock can occur.
1)insulin preparation:=
Insulin has to be prepared in a unit. It is present in a vial and contains 100 units of insulin per milliliter.
2) Insulin syringe:=
Insulin capacity has a series of 0.25,0.30,0.50, 1ml and 2ml and according to the capacity of the patient there is a long needle and a short needle. If there is an obese patient then a long needle is used.
3) insulin storage:=
Insulin is stored in the refrigerator at 36°F to 86°F and should not be stored for more than 30 days.
4)insulin preparation and injection.
Before taking insulin in a series, the vial should be rolled properly between the hands and brought to room temperature before administration.
5)route and site of insulin administration:=
Route:=subcutaneous,
Site:= abdomen,
Back of arm,
Upper part of buttock,
Side of the thighs.
procedure of administration:=
1) Using your left hand, stabilize the skin of the abdomen between your thumb and finger.
2) Insert the insulin syringe into the skin at a 90° angle.
3) Then push the plunger so that the insulin is injected.
4) Then remove the syringe from the skin and apply cotton to the injection site for a few seconds.
5) Then properly discard the syringe To do.
surgical management
Surgical management depends on the severity of the disease and the clinical condition. In which pancreas transplantation can be done.
nursing management of Diabetes malitus
1)Impaired nutritional status more than body requirement related to intake excess of activity expenditure.
- The primary goal of a diet plan is to control glucose levels, so assess the patient’s glucose level, and the patient’s lifestyle, cultural background, Assess activity level, dietary habits and food preferences.
- Instruct the patient to eat adequate amounts of food and to have snacks in between.
- Arrange extra meals before the patient engages in physical activity.
- Administer insulin as ordered by the doctor.
2)imbalance fluid volume related to increased stress hormone as evidenced by polyuria.
- Assess the patient’s intake output chart.
- Ask the patient to take oral fluids.
- Provide intravenous fluids to the patient as needed.
- Check the patient’s serum electrolyte levels.
- Check the patient’s vital signs.
3)Activity intolerance related to weakness as evidenced by limited activities.
- Assess the patient’s activity level.
- Plan the patient’s activity.
- Provide the patient with analgesic medicine before resuming activity.
- Instruct the patient to rest between activities.
- Provide the patient with carbohydrate and protein rich food. To do.
- Provide the prescribed medicine to the patient.
4)knowledge deficit related to cause and disease as evidence by asking questions.
- Assess the patient’s knowledge level.
- Provide education to the patient about the diabetic diet To do.
- Provide education to the patient about foot and nail care.
- Provide education to the patient to cover their feet with soft shoes.
- Provide education to the patient about safe and self-administration of insulin.
- 5)fear related to insulin injection.
- Monitor the patient’s blood glucose level.
- Provide education to the patient about self-administration of insulin.
- Provide education to the patient about complications of insulin therapy.
- Provide education to the patient about signs and symptoms of hyperglycemia and hypoglycemia.
1) Explain the hypoglycemia. (Describe hypoglycemia.)

- Hypo means:= decrease/reduce.
- Glycemia means glucose level in blood.
- Hypoglycemia:= means reduce glucose level in blood.
- Hypoglycemia means reduce / decrease glucose level in blood such as glucose level is less than 50-60 mg/dl.
- Normal blood glucose level Is 60-120mg/dl.
- In hypoglycemia blood glucose level is less than 50- 60 mg/dl.
2) Explain the etiology of hypoglycemia. (Write the causes of hypoglycemia.)
- Mostly due to taking insulin.
- oral hypoglycemic agent.
- due to consuming less food.
- due to doing too much physical activity and exercise.
- due to delayed consumption of meals.
Explain the clinical manifestation/sign and symptoms of hypoglycemia.
in mild hypoglycemia:
- Paspiration (sweating).
- Tachycardia (increased heart rate).
- palpitations.
- Nervousness.
- Air hunger (breathing difficulties).
in moderate hypoglycemia :
Due to the decrease in blood glucose level, the function of brain cells decreases, due to which impairment is seen in the central nervous system.
- Becoming nervous,
- Unable to concentrate.
- Memory loss.
- Restlessness.
- Feeling of numbness in the lips and tongue.
- Headache.
- memory lapse.
- Double vision or blurred vision.
- irritational behaviour.
- drowsiness.
- loss of orientation etc. symptoms are seen.
in severe hypoglycemia :
- In severe hypoglycemia, the central nervous system is severely impaired, so the patient needs another person for his treatment.
- The patient is seen semiconscious or fully unconscious.
- Behavior becomes disoriented.
- Stumbling.
- Drawing.
- Difficulty sleeping.
Explain the diagnostic evaluation :
- History taking and physical examination.
- Monitoring blood glucose level.
- autonomic neuropathy assessment.
- vision check up
- vision examination.
Explain the medical management
- In conscious patient to take simple glucose. Check RBS
- In an unconscious patient, provide intramuscular or subcutaneous glucagon injection which stimulates the liver and glucose is released.
- Provide 50% dextrose solutions intravenously 25-50ml.
- Tell the patient not to eat high calorie, high fat, desert food, cookies, cakes, ice cream etc.
Explain the nursing management
- Provide education to the patient to avoid high calorie, high fat and dessert foods.
- Routinely examine the patient’s blood glucose level.
- Provide health education to the patient and his family members.
- Provide education to the patient to eat in adequate amounts.
- Instruct the patient to take adequate amount of snacks.
- Check blood glucose levels regularly.
- Provide family members with explanations about the signs and symptoms of hypoglycemia, its causes, and its management.
1) Define hyperglycemia.
- hyper means := increase/high.
- Glycemia means:=glucose level in blood dose).
- Hyperglycemia means:=high glucose level in blood.
- Hyperglycemia is also known as diabetic ketoacidosis ( DKA) .
- Hyperglycemia is also known as diabetic ketoacidosis.
- Diabetic ketoacidosis ( DKA) is a life threatening condition of diabetes mellitus ( DM ).
- DKA is mainly caused by the absence or inadequate amount of insulin.
- It causes disturbances in the metabolism of carbohydrates, proteins and fats, which are considered emergency conditions that require immediate treatment.
Explain the Etiology/cause of hyperglycemia ( diabetic ketoacidosis) . Causes of hyperglycemia Write.
- Hyperglycemia is mainly caused by low glucose utilization by the cells and high glucose production by the liver.
- Insulin deficiency or absence.
- decrease or missed dose of insulin.
- undiagnosed diabetes mellitus.
- acidosis.
explain the pathophysiology of hyperglycemia.
When the amount of insulin in the human being body is low or absent, the utilization of glucose does not occur by the muscles, fat and liver and the production of glucose occurs in a very high amount by the liver.
|
\/
The utilization of glucose in the body is not Due to this, the level of glucose in the body (blood) increases.
|
\/
Result in( retinopathy:= blurred vision),
polyuria( increase urine output),
Dehydration due to excessive urine excrete from the body.
weakness,
headache,
polydypsia.
explain the Clinical manifestation/.sign and symptoms of hyperglycemia. Write the signs and symptoms of hyperglycemia.
- polyuria ( increase urination),
- polydypsia ( Increase thirst),
- faint appearance,
- faint appearance,
- fatigue
- headache
- acetone breath( fruity odor),
- low blood pressure,
- orthostatic hypotension (orthostatic hypotension: when the patient suddenly gets up from a lying position to a standing position, the patient feels dizzy, which is seen due to a sudden decrease in blood pressure, it is called orthostatic hypotension)
- Pulse becomes weak.
- kussmaul breathing (air hunger : difficulty breathing),
- loss of appetite,
- nausea,
- vomiting,
- abdominal pain.
- Changes in mental status.
explain the diagnostic evaluation (write the diagnostic evolution.)
- history taking and physical examination.
- monitoring blood glucose level is greater than 300mg/dl.
- low blood pH level<7.30.
- hyponatremia.
- BuN assessment.
- Nitrogen and hematocrit level.
- renal insufficiency (disruptions in kidney function)
Explain medical management )
- Restore hemodynamic status.
- Treat dehydration.
- Maintain electrolyte balance.
- Treat acidosis.
fluid therapy
- If the patient is dehydrated, provide 0.9% intravenous normal saline.
- Continuously provide the patient with fluids until the patient’s dehydration is treated.
- Continuously monitor the patient’s blood glucose level.
Restoring electrolyte
- Maintain the patient’s electrolyte level due to excessive urine output.
complication
- Fluid overload.
- Pulmonary edema.
- Heart failure.
- Hypokalemia.
- Hyperglycemia.
- Ketoacidosis.
- In cerebral AD.
- Hypoglycemia.
Nursing management
- Normalizing blood glucose levels in the management of hyperglycemia.
- Patient education about the five components To provide.
A)Nutritional therapy,
B)Exercise,
C)Monitoring,
D)Pharmacological therapy,
E)Education.
1)fluid volume deficit related to osmotic diuresis.
- Check the patient’s intake output.
- Monitor the patient’s temperature.
- Monitor the patient’s skin color and moisture.
- Check the patient’s skin turgor and mucous membrane.
- Instruct the patient to increase fluid intake.
2) Impaired nutritional status related to disease condition.
- Monitor the patient’s nutritional status.
- Assess the patient for signs and symptoms of hyperglycemia.
- Ask the patient to take food frequently.
3)Impaired skin integrity related to decrease sensation and circulation to lower extremity .
- Assess the patient’s legs and hands to see if their temperature is increased.
- Patient’s skin integrity Assess.
- Check the patient’s skin moisture and whether there is any abnormality in the skin.
4)Activity intolerance related to poor glucose control.
- Advise the patient to assess blood glucose levels before and after exercise.
- The patient Advise or do regular exercise.
- Provide education to the patient that if the blood glucose level is more than 250 mg/d, then exercise should be avoided.
5)Risk for hypoglycemia related to effect of insulin inability to eat.
- Provide patient education or closely monitor blood glucose levels.
- Provide patient with adequate insulin.
- Check patient for signs and symptoms of hypoglycemia.
6) Ineffective management of therapeutic regimen related to lack of knowledge about exercise.
- Check the client’s current knowledge level.
- Check the patient’s blood glucose level regularly.
- Provide education to the patient on insulin administration.
Explain the prevention
- Provide patient education on adequate fluid intake.
- Continuously monitor patient’s blood glucose level.
- Take small amounts of carbohydrates at frequent intervals.
- Provide patient education on self-insulin administration.
- Instruct the patient to eat small amounts of food.
- Instruct the patient to drink extra fluids.
explain the definition of diabetic neuropathies. (Define diabetic nephropathy.)
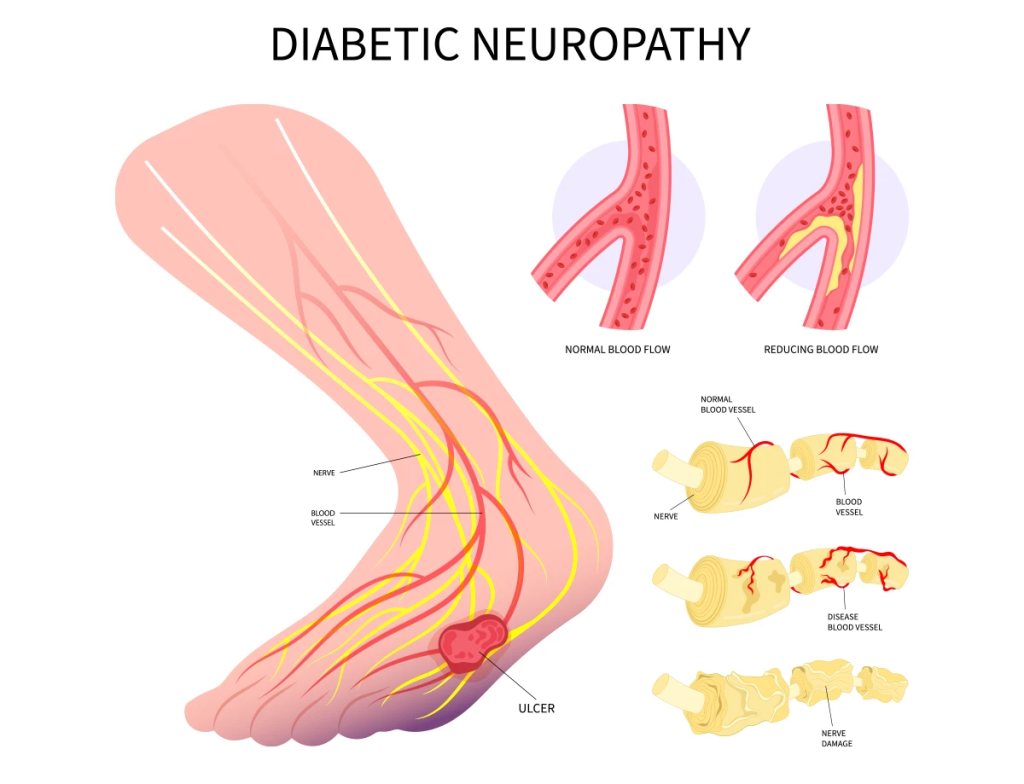
- Diabetic nephropathy is a It is a complication in which renal impairment is seen due to diabetes and renal lesions are seen in it.
Explain Etiology (Explain the cause)
- Due to increased cholesterol levels.
- Due to smoking.
- Increase in blood pressure Because of.
- Due to diabetes.
Explainthe clinical manifestation/sign and symptoms
- Renal failure,
- nocturnal diarrhea,
- Hypoglycemia.
- Congestive heart failure.
Explain diagnostic evaluation (Diagnostic Evaluation write.)
- History taking and physical examination.
- urine examination.
- assess the blood urea nitrogen level.
- Hypertension.
Explain the medical management (Explain the medical management.)
- The blood glucose level of the body Maintain.
- And be careful not to develop any of the following conditions.
- hypertension,
- urinary track infections,
- nephrotoxin substances,
- low sodium diet.
treatment :
- Dialysis in which the kidney function is altered and waste cannot be removed, so the waste is removed from the body by dialysis.
1)explain the diabetic neuropathies.
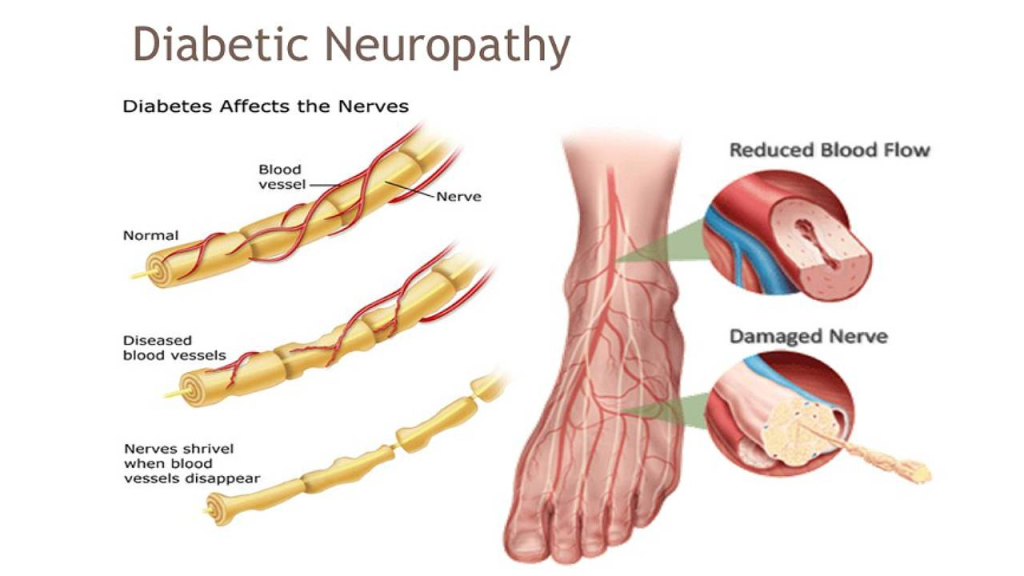
- Diabetic neuropathy is a group of diseases in which all types of nerves are involved such as autonomic, spinal nerve, sensory, motor nerve etc., leading to alterations in nerve function. is.
- The signs and symptoms depend on the location and type of nerve.
2) Explain the Etiology (Explain the cause.)
- Due to essential fatty acid abnormality.
- Due to polymerase activation .
- Oxidative stress.
- Protein kinase c activation.
- poly pathway activation.
Explain the Clinical manifestation/sign and symptoms
- Tingling sensation.
- burning sensation.
- Numbness in feet .
- decrease sensation of touch, decrease sensation of pain and temperature.
Explain the management
- Provide insulin therapy to the patient.
- Assess the patient’s blood glucose level.
- Assess lower extremity pain.
- Provide analgesic medicine to the patient.
1) Explain the Diabetic foot.
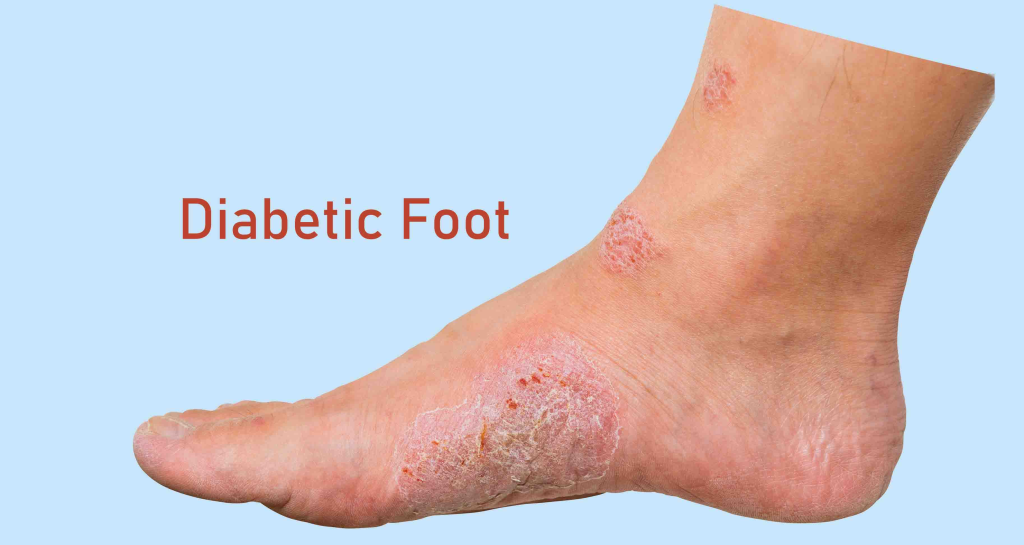
- This is a complication of uncontrolled diabetes in the foot, in which ulcers, infections or inflammation are seen in the foot.
Causes
1)Neuropathy:=
In this, there is a loss of pain sensation and in the skin Dryness and fissures are seen.
2)Poor vascular disease:=
- Poor blood circulation in the legs leads to impairment in wound healing.
- Due to this, gangrene formation is seen.
3)immunocompromise :=
- In this body W.B.C. Due to the low level of WBC, the bacteria cannot be fought and due to this, abnormalities are seen in the foot.
- Tissues injury in foot .
- formation of fissure.
- Drainage, swelling, Redness and gangrene formation in foot.
Explain the management
- Tell the patient to take continuous bed rest.
- Provide antibiotic medicine to the patient
- Continuously maintain the patient’s blood glucose level.
- Give the patient an adequate amount of antibiotic medicine.
- Care for the patient’s feet, checking for cuts, blisters, soreness.
- Tell the patient to take proper foot care.
- Provide education to the patient to keep the feet dry.
- Wear comfortable shoes.
- Seek advice from a doctor for foot care.
- Seek to see a doctor immediately if there is any cut, soreness, blister on the foot.
1) Define hypothyroidism. (Define hypothyroidism.)
- Hypothyroidism is a disorder of the endocrine gland in which the thyroid gland The gland does not secrete adequate amounts of thyroid hormone.
- In hypothyroidism, thyroid hormone is secreted in inadequate amounts, causing normal body functions to be altered.
- Hypo means:= less
- Thyroidism:= thyroid hormone.
hypothyroidism :
- means inadequate secretion of thyroid hormone from the thyroid gland.
- Conginital hypothyroidism it’s called critinism.
2)explain the Etiology of hypothyroidism.
- Autoimmune thyroiditis.
- If any patient has a pre-existing condition of hypothyroidism.
- Radiation therapy.
- medication that has lithium and iodine compound.
- Due to iodine deficiency.
- Congenital problem.
- Thyroid dysgenesis.
- exposure to goitrogens.
explain the Classification (Describe classification)
1)primary or thyroidal hypothyroidism.
- This type is mainly seen due to dysfunction of the thyroid gland itself.
- Due to dysfunction of the thyroid gland itself.
2)Central hypothyroidism.
- This type is caused by dysfunction of the hypothalamus and pituitary gland.
3)pituitary or secondary hypothyroidism. ( Pituitary or secondary hypothyroidism)
- This type is seen only due to dysfunction of the pituitary gland.
4) Hypothalamic or tertiary hypothyroidism. (Hypothalamic or tertiary hypothyroidism.)
- This type is caused by dysfunction of the hypothalamus.
5)congenital hypothyroidism. (Congenital hypothyroidism).
- If a person is born with a problem in the thyroid gland, it is called cretinism.
6) Myxedema
- Myxedema is a form of hypothyroidism. There is a more serious complication. In this, the patient experiences swelling in their soft tissues. If the brain and consciousness level are altered in this condition, it is called coma in hyperthyroidism or thyroid crisis.
- In hyperthyroidism, mucopolysaccharides accumulate in the subcutaneous tissue.
Explain the Clinical manifestation/sign and symptoms of hypothyroidism.
- Hair loss.
- Brittle nails.
- Dry skin.
- Numbness and tingling of finger.
- Depending on voice.
- Disturbance in menstrual cycle.
- loss of libido.
- menstrual disturbances.
- subnormal temperature and pulse.
- patient gains weight.
- skin thickness.
- face becomes less expressive.
- patient becomes irritable and fatigued is.
- The patient’s speech slows down.
- tongue enlarges hand and feet increase in size.
- Deafness is seen.
- Complaint of constipation is seen.
- inadequate ventilation.
- pleural effusion.
- Respiratory muscles become weak.
- Serum cholesterol levels increase and coronary artery disease is seen.
- Myxedema coma.
- Fatigue.
Explain the diagnostic evaluation :
- History taking and physical examination.
- Serum T3,T4 and Tsh level assessment (test is done in fasting).
- Radioisotope based thyroid scanning.
3) Explain the management of hypothyroidism.
Explain the medical management :
- To restore normal metabolic function, the missing hormone is replaced.
- synthyroid, levothyroid.
- If there is a condition of severe hypothyroidism, then to monitor vital functions, arterial blood gases, pulse Monitor oxygen saturation by oximetry.
- Administer fluids to the patient.
- Provide hormonal therapy to the patient.
- Avoid applying external heat as it increases oxygen requirements.
Explain the nursing management
Nursing management
Nursing assessment
- Monitoring the patient’s vital signs.
- Assessing the client’s eating pattern and dietary pattern.
- Assess the patient’s alcohol consumption and smoking.
- Assess the patient’s consumption of lithium or iodine containing drugs.
- Assess the patient’s symptoms of hypothyroidism.
Nursing diagnosis
- 1) Activity intolerance related to lethargy and weakness.
- 2) Disturbance body image related to edema.
- 3) Hyperthermia or hypothermia related to decreased metabolism.
- 4) Impaired nutritional less than body requirement related to disease condition.
- 5)Impaired bowel elimination constipation related to disease.
- 6)ineffective therapeutic regimen related to ignorance about disease and treatment.
Nursing management
- Ask the patient to do some amount of daily routine activity.
- Ask the patient to maintain personal hygiene.
- Ask the patient to do regular physical activity.
- Monitor the patient’s vital signs.
- Check the patient’s cognitive level.
- If the patient feels excessively cold, provide him with a black cat.
- Provide emotional support to the patient.
- Inform the patient and his family members about the disease.
- Encourage the patient to eat a moderate amount of food.
- Clear all the doubts of the patient and provide him with psychological support.
1)define hyperthyroidism.

- Hyper means: excessive
- Thyroidism means: thyroid hormone.
- hyperthyroidism means : excessive secretion of thyroid hormone in the blood from the thyroid gland.
- hyperthyroidism means : excessive secretion of thyroid hormone in the blood from the thyroid gland is called hyperthyroidism.
2) Explain the Etiology
- Due to infection,
- Emotional grief,
- stress,
- Excessive ingestion of thyroid hormone.
- pituitary adenomas.
- autoimmune disorder thyroiditis.
- toxic adenomas.
- chronic lymphocytic thyroiditis.
- grave disease.
- iodine induced hyperthyroidism.
explain the Clinical manifestation/ sign and symptoms
- Nervousness,
- Emotionally hyperexcited,
- The person cannot sit still,
- palpitation,
- rapid pulse,
- heat intolerance,
- skin flushing.
- tremor.
- exophthalmos( bulging eyes).
- excessive hunger but weight loss.
- muscular fatigue and weakness.
- ( amenorrhea) Amenorrhea,
- Increased pulse rate.
- Osteoporosis.
- Fatigue.
- Tachycardia,
- dysrhythmias,
- Pulse rate increases.
Explain the diagnostic evaluation
- History taking and physical examination.
- thyroid scan.
- inspection,
- palpation,
- percussion,
- palpation.
- blood exam
- radiological exam
Explain the management of hyperthyroidism (Write the management of hyperthyroidism.)
medical management
- The goal of medical management of hyperthyroidism is to reduce the hyperactivity of the thyroid gland.
pharmacological therapy
- Medications in pharmacological management Provide a medication that reduces hyperactivity of the thyroid gland and reduces hormone release.
- Ex: propylethiouracil, Tapazole.
Radioactive iodine therapy:
- The goal of radioactive iodine therapy is to The cells of the thyroid gland are to be destroyed and this therapy is provided for a week or one month.
Adjuctive therapy:
In this therapy, the patient is provided with iodine and iodine compound mixed in milk and fruit juice.
explain the surgical management
thyroidectomy
- (surgically removal of whole thyroid gland parts) if other measures fail.
explain the nursing management of hyperthyroidism
explain nursing assessment
- Monitor the patient’s vital signs.
- Continuously measure the patient’s body weight.
- Check the patient’s activity level.
- Assess the patient’s food habits.
- Assess whether the patient is an alcoholic or a smoker.
- Assess the patient’s hand for any tremors or skin flushing.
- Assess the patient’s emotional status.
- Assess menstrual history if female.
explain the nursing diagnosis
1)Impaired nutritional status more than body requirement related to high metabolic rate.
maintain nutritional status
- Assess the nutritional status of the patient.
- Make enquiries about the patient’s dietary habits and the foods the patient likes.
- Plan a proper diet menu for the client.
- Provide a high calorie diet to the patient.
- Provide the patient with a diet in small amounts but at frequent intervals.
- Provide the patient with a high calorie diet.
- Serve food to the patient in an attractive manner.
- Monitor the client’s daily weight.
2) altered body temperature related to high metabolic rate.
maintain normal body temperature:
- Monitor the patient’s vital signs.
- Maintain the patient’s personal hygiene.
- Provide the patient with adequate amounts of fluid.
- Ask the patient to wear clean clothes.
- Maintain adequate ventilation in the room.
3)activity intolerance related to fatigue and weakness and high metabolic rate.
maintain activity level:=
- Ask the client to do indoor activities.
- The client is nervous and cannot sit still. Ask him to rest for an adequate amount of time.
- Ask the client to reduce physical exertion.
- Provide reassurance to the client.
4)altered sleep pattern related to disease condition.
enhancing sleep :=
- Assess the client’s sleeping habits.
- Provide the client with an environment that improves sleeping.
- Provide the client with nutritional requirements before sleeping.
- Tell the client to pray or read a book before going to bed.
5)Impaired knowledge level related to disease condition.
provide knowledge:=
- Assess the patient’s learning level and understanding level.
- Ask the client to clear all doubts.
- Ask the patient to adopt coping strategies.
- Provide the patient with information about the disease condition and its treatment.
- Assist the patient in following the therapeutic regiment Say.
- Provide the patient with the prescribed medicine.
- Encourage the patient to have frequent blood testing.
- Monitor for any side effects of the anti-thyroid drug.
- And hyperthyroidism also increases the metabolic rate.
1)Define thyroid cancer. (Define thyroid cancer.)
-
- The thyroid is a gland located in the neck.
-
- In thyroid cancer, the cells of the thyroid gland grow abnormally and uncontrollably, forming a tumor-like formation.
-
- Which can be benign or malignant. If the tumor is malignant, it results in thyroid cancer.
2)explain the Classification of thyroid gland cancer. Explain the classification of thyroid gland cancer
-
- 1) Anaplastic carcinoma ( Anaplastic carcinoma)
-
- 2) Follicular carcinoma ( Follicular carcinoma)
-
- 3) Medullary carcinoma ( Medullary carcinoma)
-
- 4) Papillary carcinoma ( Papillary carcinoma) carcinoma)
1) Anaplastic carcinoma
-
- (it also called giant or spindle cell)
-
- This is the most dangerous type of thyroid cancer that occurs rarely and spreads very quickly.
2) Follicular carcinoma (Follicular carcinoma)
-
- Follicular carcinoma is the second most common cancer.
-
- This is mainly caused by inadequate secretion of iodine.
-
- It has a good prognosis and is more aggressive than papillary cancer.
-
- Follicular carcinoma does not spread to lymph nodes but spreads to other organs.
-
- Like lungs or brain.
3) Medullary carcinoma (Medullary carcinoma)
- Medullary carcinoma is a non-thyroid cell cancer.
- This type of thyroid cancer, which is mainly present in the thyroid gland, is mainly seen in family members.
- This cancer mainly develops from the C cells of the thyroid gland.
4) Papillary carcinoma ( Papillary carcinoma)
- Papillary carcinoma is the most common type of thyroid cancer.
- About 80 percent of cases are papillary carcinoma.
- Papillary carcinoma is slow growing.
- Papillary carcinoma grows from follicular cells and It affects one or both lobes of the thyroid gland.
- This type of cancer spreads to the lymph nodes in the neck but has a good prognosis.
explain the Etiology of thyroid cancer.
- Due to radiation therapy to the neck in childhood.
- Due to chronic goiter.
- Due to family history.
- Due to iodine deficiency.
- Due to thyroiditis.
- Due to older age.
- Food source contaminated with radioactivity.
- Radioactive iodine concentration in the thyroid gland.
explain the Clinical manifestation/sign and symptoms of thyroid cancer (Explain the Clinical manifestation/sign and symptoms of thyroid cancer.)
- A lump-like feeling in the neck and it grows rapidly.
- Pain in the front of the neck and it radiates to the ear.
- There is a change in the voice.
- There is difficulty in swallowing.
- There is difficulty in breathing.
- Cough.
- Enlargement of the thyroid gland.
- Swelling in the neck.
explain the diagnostic evaluation of thyroid cancer (Write a diagnostic evaluation of thyroid cancer.)
- history taking and physical examination .
- calcitonin blood test.
- laryngoscopy.
- thyroid biopsy.
- Thyroid scan.
- TSH,T3,T4 test.
- Ultrasound of thyroid gland.
- Thyroid function test.
- Biopsy
- CT SCAN.
- MRI.
- Radioactive iodine uptake studies.
- Thyroid suppression test.
explain the management of thyroid cancer (Write the management of thyroid cancer.)
- Treatment of thyroid cancer depends on the type of thyroid cancer.
surgery
- thyroidectomy.
- external beam radiation therapy.
- chemotherapy
- Ex:=urambicil and sysplastin.
- Hormonal therapy.
- thyroid replacement therapy.
- Thyroxine therapy.
explain the nursing management
- 1)Acute pain related to pressure/Swelling of the tumor nodule.
- 2) ineffective Airway clearance related to obstruction due to tumor mass pressure/laryngeal spasm.
- 3) Impaired verbal communication related to injury to vocal cord.
- 4) Anxiety related to concern about cancer, upcoming surgery.
- 5) Knowledge deficit related to cancer and its treatment.
Nursing interventions
- Assess the patient’s respiratory rate, depth and breathing pattern.
- Auscultate the patient’s breath sounds.
- Assess whether the patient has a condition of cyanosis.
- Assess the patient’s anxiety level and ask him to gain coping skills.
- Check the color and amount of phlegm by suctioning from the trachea and mouth.
- Ask the patient to take high protein and carbohydrate rich food.
- Ask the patient to take a high calorie diet so that the patient can gain an adequate amount of weight.
- Properly assess the patient’s dressing side.
- Properly measure the patient’s vital signs.
- If the patient is experiencing excessive pain, provide the patient with analgesic medicine.
- Properly support the patient’s head.
- Provide a comfortable position for the patient.
- Provide the patient with a semi-fowler position and keep the head elevated by supporting it with a pillow.
- Provide intravenous fluids to the patient.
- Assess the patient for any difficulty swallowing.
- Provide steam inhalation to the patient.
- Keep the patient’s room well ventilated to ensure proper breathing.
complication
- Injury to the voice box.
- Hoarseness after thyroid surgery.
- low calcium level (due to removal of parathyroid gland).
- spread of the cancer to the lungs,bones,or other part of body.
1)Define hyperparathyroidism.
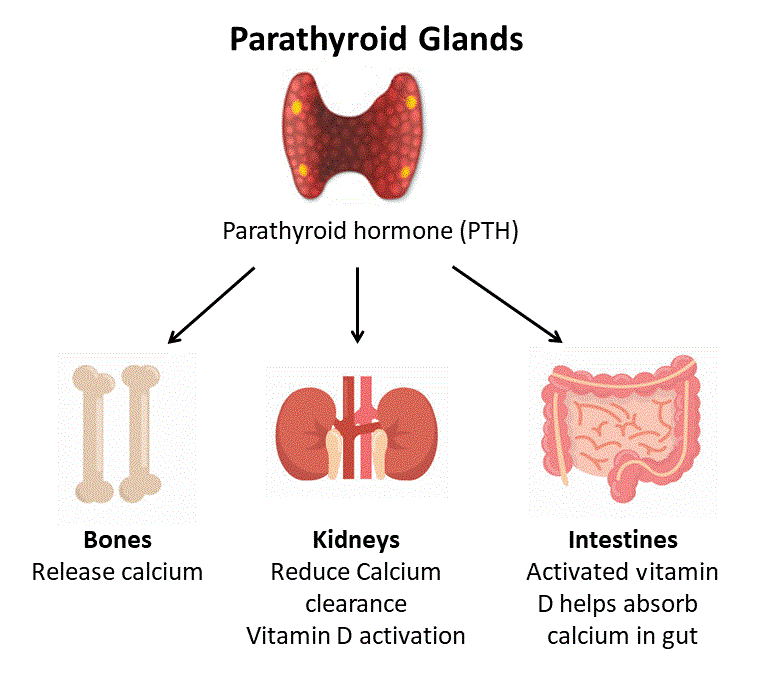
- Parathyroid glands are located at the back of the neck.
- Parathyroid glands are oval in shape and have four.
- Parathyroid glands secrete parathyroid hormone.
- This is due to the overactivity of more than one parathyroid gland, which causes parathyroid hormone to be secreted in excessive amounts into the bloodstream, which causes the condition of hyperparathyroidism to arise in the body. is.
Hyper: excessive , parathyroidism: parathyroid hormone
hyperparathyroidism :
- Excessive excretion of parathyroid hormone from the parathyroid gland.
- Excessive secretion of parathyroid hormone from the parathyroid gland into the blood stream is called hyperparathyroidism.
Explain the type of hyperparathyroidism
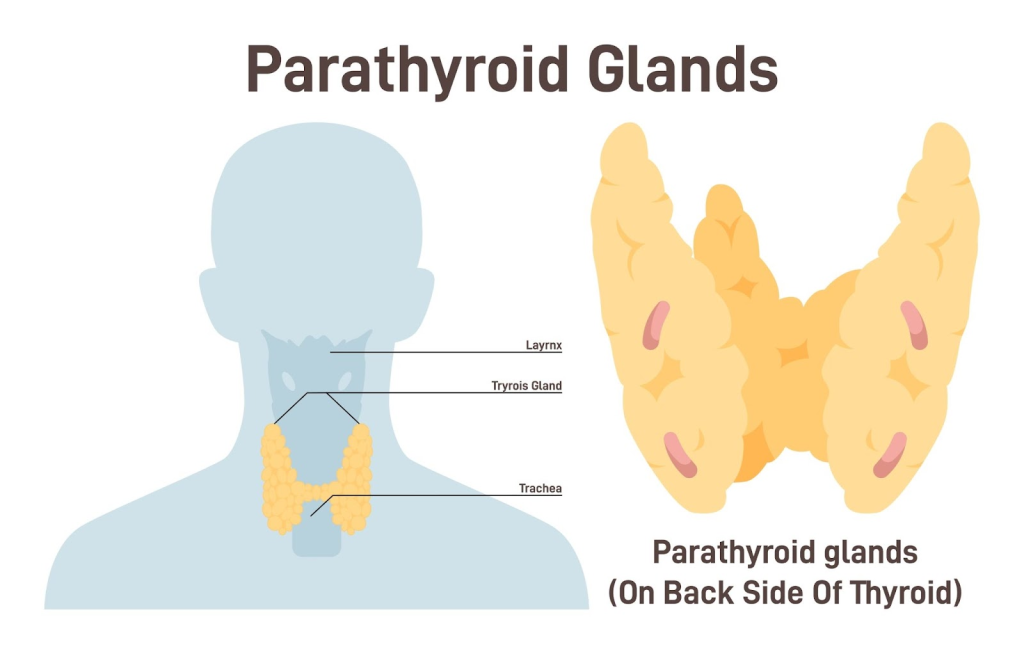
1)Primary hyperparathyroidism.
- Primary parathyroidism is mainly caused by any abnormality in one or four parathyroid glands.
2)Secondary hyperparathyroidism
1)cause of primary hyperparathyroidism
- Due to any non-cancerous growth on the gland.
- Due to enlargement of more than one parathyroid gland.
- rare cause is cancerous tumor.
2)Secondary hyperparathyroidism .
- Due to severe calcium deficiency.
- Due to serum vitamin D deficiency.
- Due to chronic kidney failure.
- No metabolic abnormality Because of.
explain the risk factor (Explain the risk factor)
- Menopause, Prolong and Severe Calcium and Vitamin D Deficiency.
- Due to Radiation Therapy.
- Due to Lithium.
explain the Clinical manifestation/sign and symptoms
- Fatigue.
- Weakness in muscles.
- Nausea and vomiting.
- Hypertension.
- Cardiac dysrhythmias.
- Bone fragility.
- Kidney stones.
- Excessive urination.
- Abdominal pain.
- Weakness.
- Depression.
- Pain in bones and joints.
- The patient complains frequently of illness.
- Nausea, vomiting, and loss of appetite.
- Irritability.
- Neurosis or psychosis.
- Demineralization of bones.
- Skeletal pain.
- Tenderness in the back and joints.
explain the diagnostic evaluation (write a diagnostic evaluation.)
- history taking and physical examination.
- blood test,
- urine test,
- ultrasound,
- bone mineral density test,
- imaging test of kidney,
- X Ray,
- CT scan,
- MRI,
- Sestambin scan,
Explain the management
treatment
surgery
- parathyroidectomy.
- The damaged part of the parathyroid gland is removed.
explain the medical management
Provide adequate diet and medication .
- Assess the nutritional status of the patient.
- If the patient has peptic ulcer, provide antacid medicine.
- Take measures to improve the patient’s appetite.
- Tell the patient to drink plenty of fluids.
maintain hydration level.
- Instruct the patient to take adequate amount of fluid daily.
- Check the patient for signs and symptoms of renal calculi such as abdominal pain and hematuria.
- Avoid thiazide diuretics as these diuretic medicines cause calcium retention in the body, which increases serum calcium levels in the body.
- If the patient develops a condition of dehydration, then immediately Physician and report.
improve mobility level
- Ask the patient to do activities as much as possible.
- Ask the patient to walk in small amounts.
- Bed rest reduces the calcium level in the body and renal Calculus formation is reduced.
- Provide oral phosphate to the patient which reduces the amount of calcium in the body.
provide health education
- Properly raise awareness in the patient.
- Calcium phosphorus of the patient Maintain balance.
- Monitor the patient closely.
- Ask the nurse to follow up the patient properly.
- Ask the patient to take maximum food.
Nursing management
Nursing assessment
- Monitor the patient’s vital signs.
- Assess the patient for any symptoms of hyperparathyroidism.
- Assess the patient’s dietary habits, alcohol, and smoking habits.
- Complete physical examination of the patient To do.
- To assess the patient’s pain in terms of its quality, intensity, duration and other factors.
pre operative Nursing diagnosis
- 1)Activity intolerance related to fatigue and weakness.
- 2)Impaired nutritional status less than body requirement related to nausea and vomiting.
- 3) Discomfort related to bone pain.
- 4) Disturbed sleeping pattern related to pain and psychosis.
- 5) Anxiety related to disease and surgery.
pre operative nursing interventions.
1)Promote activity level.
- Assess the client’s activity level.
- Create a nursing care plan for the patient.
- Ask the patient to provide rest between activities.
- Ask the patient to take a balanced diet.
- Instruct the patient to drink adequate amounts of fluid.
- Provide the patient with supplementary vitamins.
2)maintain nutritional status.
- Assess the nutritional status of the client.
- Assess the patient’s eating habits.
- Provide the patient with small amounts of food frequently.
- To maintain oral hygiene for the patient Tell.
- Tell the patient to take a balanced diet.
- Tell the patient to take a soft and balanced diet.
- Maintain the patient’s intake output chart.
3)Promote comfort level.
- Assess the patient’s pain level.
- Provide the patient with a comfortable position.
- Provide the patient with diversional therapy.
- Ask the patient to do range of motion exercises.
- Provide the patient with comfort devices such as pillows, cushions, heat therapy.
4)Promote sleep.
- Assess the patient’s sleeping habits.
- Provide a conductive environment for the patient.
- Maintain the patient’s personal hygiene.
- Provide analgesic medicine to the patient To do.
- Ask the patient to read any book before sleeping.
Post-operative Nursing interventions
- 1)ineffective Airway clearance related to post anesthesia effect.
- 2)ineffective gas changes related to post operative bed rest.
- 3) fluid volume deficit related to post operative bed rest.
- 4)Risk for infection related to post surgery hospitalization.
Nursing interventions:
1)keep airway patent.
- Assess the patient’s respiratory status and breathing sounds.
- Provide the patient with a Fowler position.
- Encourage the patient to do deep breathing exercises.
- Instruct the patient to perform oral and endocrine suctioning.
- Check the patient’s pulse oximetry.
2)improving breathing pattern.
- Assess the patient’s respiratory rate.
- Provide the patient with a Fowler position.
- Ask the patient for deep breathing exercises.
- Advise the patient to do steam inhalation, physiotherapy and Provide incentive spirometry.
- Instruct the patient to drink plenty of fluids.
3)Maintain fluid and electrolyte balance.
- Monitor the patient’s vital signs.
- Provide the patient with intravenous fluids.
- Instruct the patient to maintain strict aseptic technique.
- Maintain the patient’s intake output chart.
4)prevent occurrence of infections:
- Monitor the patient’s vital signs.
- Instruct the patient to wash his hands.
- Instruct the patient to maintain aseptic technique.
- Provide the patient with a clean and neat environment.
- Ask the patient to wear a clean cotton cloth.
- Provide plenty of fluid to the patient.
- Give the patient the prescribed medicine.
- Monitor the patient for any complications.
1)explain the hypoparathyroidism. (Define hypoparathyroidism.)
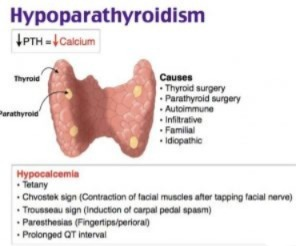
- Hypoparathyroidism is an endocrine disorder of the parathyroid gland. is.
- In hypoparathyroidism, inadequate (low) amount of parathyroid hormone is secreted from the parathyroid gland, which is called hypoparathyroidism.
- Hypoparathyroidism is a condition in which the amount of phosphate in the blood is elevated and the amount of calcium is decreased.
2)explain Etiology. (Explain the reason)
- If the parathyroid gland has been removed due to cancer.
- Due to an excessive amount of iron.
- Due to an excessive amount of aluminum in the diet.
- Infraction of parathyroid gland.
- Grave Diseases.
- Hazimoto’s thyroiditis.
- Magnesium deficiency due to alcoholism.
explain the Clinical manifestation/sign and symptoms.(Write the signs and symptoms.)
- In the neuromuscular system Irritability.
- numbness and tingling sensation in extremities.
- Stiffness in hands and feet.
- Broncho spasm.
- Difficulty swallowing.
- Photophobia.
- Shock.
explain the diagnostic evaluation
- History taking and physical examination.
- blood test.
- examine serum calcium level.
explain the management
medical management
- Immediately after thyroidectomy, calcium gluconate should be administered intravenously.
- To treat hypoparathyroidism Administer parathyroid hormone via parenteral route.
- Provide anti-conversion drug to the patient.
- Environment should be noise free and low light.
- If the patient is in respiratory distress, tracheostomy followed by mechanical ventilation and bronchodilating medicine should be provided.
- Advise the patient to consume food with high calcium and low phosphorus (milk, milk products, eggs) yolk).
- Provide aluminum hydroxide gel to the patient.
explain the nursing management
nursing assessment
- Monitor the patient’s vital signs To do.
- Assess the patient’s dietary habits.
- Assess the patient’s fluid intake.
- Perform a neuromuscular examination of the patient.
- Assess whether the patient has any behavioral changes such as anxiety, irritability, etc.
- Observe seizure activity.
nursing diagnosis
- 1) Risk of injury related to tetany, Seizures.
- 2) Anxiety related to disease, treatment.
- 3)Impaired nutritional pattern less than body requirement related to dysphagia.
- 4) Activity intolerance related to weakness, photophobia.
- 5) Knowledge deficit related to disease condition, treatment, self care, prognosis and discharge needs.
Nursing interventions
reduce the risk of injury.
- Monitor the patient’s vital signs.
- Assess whether the patient has numbness, tingling sensation or not.
- Do not restrain the patient if he is having a seizure.
- Keep the patient’s side rails up.
- Monitor the patient’s serum calcium level.
- Administer anticonvulsant medication to control seizures.
2)Relieve anxiety.
- Monitor the patient’s anxiety level.
- Explain all the information, whatever it is.
- Reduce external stimuli and provide a calm environment.
- Provide the patient with mind diversional therapy.
- Provide the patient with anti-anxiety drugs.
3)Maintain stable weight by reducing malnutrition.
- Monitor the patient’s food intake level.
- Ask the patient to take adequate amount of meal.
- Ask the patient to take high calorie food that is easily digested.
- Provide the patient with high calorie, high protein and carbohydrate rich food.
- Maintain the patient’s intake output chart.
4)improved ability to participate in desired activities.
- Monitor the patient’s vital signs and assess the client’s activity level.
- List the patient for tachypnea, dyspnea, pallor, cyanosis.
- Provide the patient with a calm environment.
- Provide the patient with bed rest and restrict excessive activity.
- Give the patient antacids and provide anti-anxiety agents.
enhancing knowledge.
- Assess the patient’s knowledge about the disease and its treatment.
- Provide the patient with knowledge about drug therapy and its side effects.
- Balance the patient Provide nutritional diet.
- Plan the patient’s nutritional menu.
- Ask the patient to have regular follow-up.
1)Define/explain thyroiditis.
- => The thyroid gland is a small butterfly-shaped gland located in the front part of the neck.
- => The thyroid gland is located in the inferior (bottom) part of the cricoid cartilage.
- => The thyroid gland releases hormones (T3, T4) into the bloodstream, which play an important role in the body’s growth and metabolism.
- => This infection and inflammation in the thyroid gland is called thyroiditis.
- =>( inflammation of the thyroid gland its called Thyroiditis.)
2)explain the types of thyroiditis.
- 1)Acute suppurative thyroiditis ( Acute suppurative thyroiditis)
- 2)subacute or lymphatic thyroiditis.( Subacute or lymphatic thyroiditis )
- 3)chronic thyroiditis ( HASHIMOTO’S DISEASE) ( Chronic thyroiditis/ Hashimoto’s disease)
- 4)lymphocytic/silent or Painless thyroiditis.( Lymphocytic Silent or Painless Thyroiditis)
1)Acute suppurative thyroiditis
- => This type of thyroiditis is mainly seen due to a bacterial invasion.
- => Acute thyroiditis is mainly seen up to one month.
2)subacute or lymphatic thyroiditis. ( Subacute or lymphatic thyroiditis )
- Subacute and lymphatic thyroiditis
- Quervain’s thyroiditis,
- Granulomatous thyroiditis,
- giant cell thyroiditis
Also known as.
=> In subacute thyroiditis, the patient’s thyroiditis condition lasts for three to four months.
3)chronic thyroiditis ( HASHIMOTO’S DISEASE) ( Chronic thyroiditis/ Hashimoto’s disease)
- => Chronic thyroiditis is called Hashimoto’s thyroiditis.
- => Chronic thyroiditis is a long-term inflammatory disorder.
- => Chronic thyroiditis is seen in the patient for up to 1 year (12 to 18 months).
4)lymphocytic/silent or Painless thyroiditis. (Lymphocytic/Silent or Painless Thyroiditis)
- => This type of thyroiditis is mainly seen in women during the post-partum period.
3)explain the causes/Etiology of thyroiditis .(Explain the causes of thyroiditis)
1)Acute suppurative thyroiditis:=
- Due to bacterial infection:=
- Staphylococcus bacteria ( staphylococcus bacteria)
- Streptococcus bacteria ( Streptococcus bacteria)
- pneumococcus pneumonia ( pneumococcus pneumonia),
Due to fungal infection:
- aspergillus ( Aspergillus),
- candida ( Candida),
- histoplasma ( Histoplasma),
=> This is mainly seen in women between the ages of 20 and 40, as well as in children and older people.
2) Subacute thyroiditis:=
- Due to viral infection,
- Due to autoimmune abnormality.,
- Due to genetic condition,
- Due to mycobacterial infection.
- Due to taking certain types of drugs.
- These types Thyroiditis is mainly seen in women aged 40 to 50 years.
3)chronic thyroiditis:=
- Due to autoimmune disorders.
- Due to genetic abnormalities.
- This type of thyroiditis is mainly It is more common in women aged 20 to 50 years.
4)explain the Clinical manifestation/diagnostic evaluation of thyroiditis.
1)Acute thyroiditis:=
- In this, in both the front parts of the neck Pain occurs and this pain radiates to the ear and mandibles.
- Bacterial toxicity,
- Fever,
- Sweating,
- Feeling cold,
- Sore throat,
- hoarseness,
- difficulty swallowing,
2)subacute lymphocytic thyroiditis:=
- The thyroid gland becomes swollen and inflamed.
- pain in the neck,
- Fever,
- Fatigue,
- Loss of appetite :=Anorexia,
3)subacute Granulomatous thyroiditis:=
- Neck pain occur,
- Pain in the neck radiating to the ear and mandible.
- Muscle pain.
- sore throat,
- Thyrotoxicosis (high level of thyroid hormone in blood for any cause),
4)chronic thyroiditis:=
- Enlargement of the thyroid gland.
- Difficulty swallowing.
- Respiratory distress.
- Fatigue.
- Low energy.
- Joint and muscle pain.
- Changes in voice.
5)explain the diagnostic evaluation of thyroiditis. (Write the diagnostic evaluation of thyroiditis.)
- History taking and physical examination,
- blood culture,
- needle aspiration,
- thyroid ultrasound,
- thyroid stimulating hormone level assessment.
- T3, (triiodothyronin),
- T4 (thyroxine) level assessment.
- needle aspiration.
6) Explain the management of thyroiditis. (Write management of thyroiditis)
- 1) Acute pain related to post operative tissue damage.
- 2)imbalance nutritional status less than body requirement related to hyper metabolic rate and impaired utilization and storage of nutrients.
- 3) Impaired skin integrity related to surgical incision.
Nursing management
- Assess the nutritional status of the patient.
- Assess the amount of nutrition the patient is taking in.
- Assess whether the patient has any difficulty swallowing.
- Administer antiemetic medicine if the patient is experiencing nausea and vomiting.
- Provide the patient with adequate fluid to maintain the patient’s hydration status.
- Check the patient’s weight daily.
- Assess the patient’s respiratory status every one to two hours.
- Assess the patient’s pain level.
- Provide the patient with a semi-fowler’s position.
- The dressing should be clean and dry to prevent infection.
- Encourage the patient to do diversional activities to improve their coping abilities.
- Check the patient’s vital signs every 15 minutes during the post-operative period.
- Check the patient’s dressing during the post-operative period.
- Is the patient bleeding? Check if the patient has signs and symptoms of hypocalcemia. Check the patient’s calcium, magnesium, and phosphate levels. Assess the patient for any restlessness, agitation, and tachycardia. Monitor the patient’s thyroid function levels. –>
