ENGLISH-unit-8-respiratory disorder-PART-3-UPLOAD
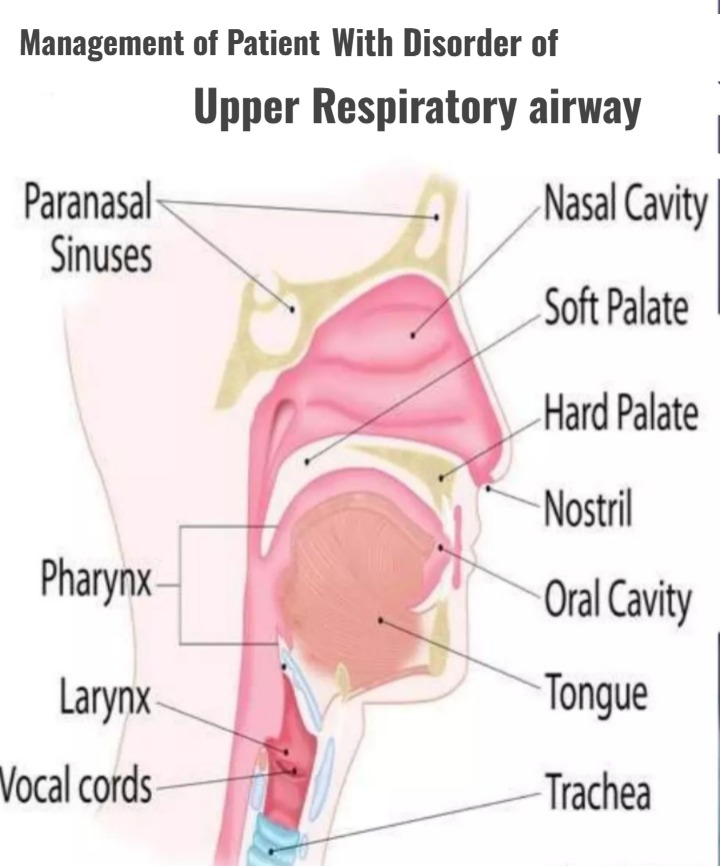
Management of Patient With Disorder of Upper Respiratory airway:
Define obstruction of upper airway:
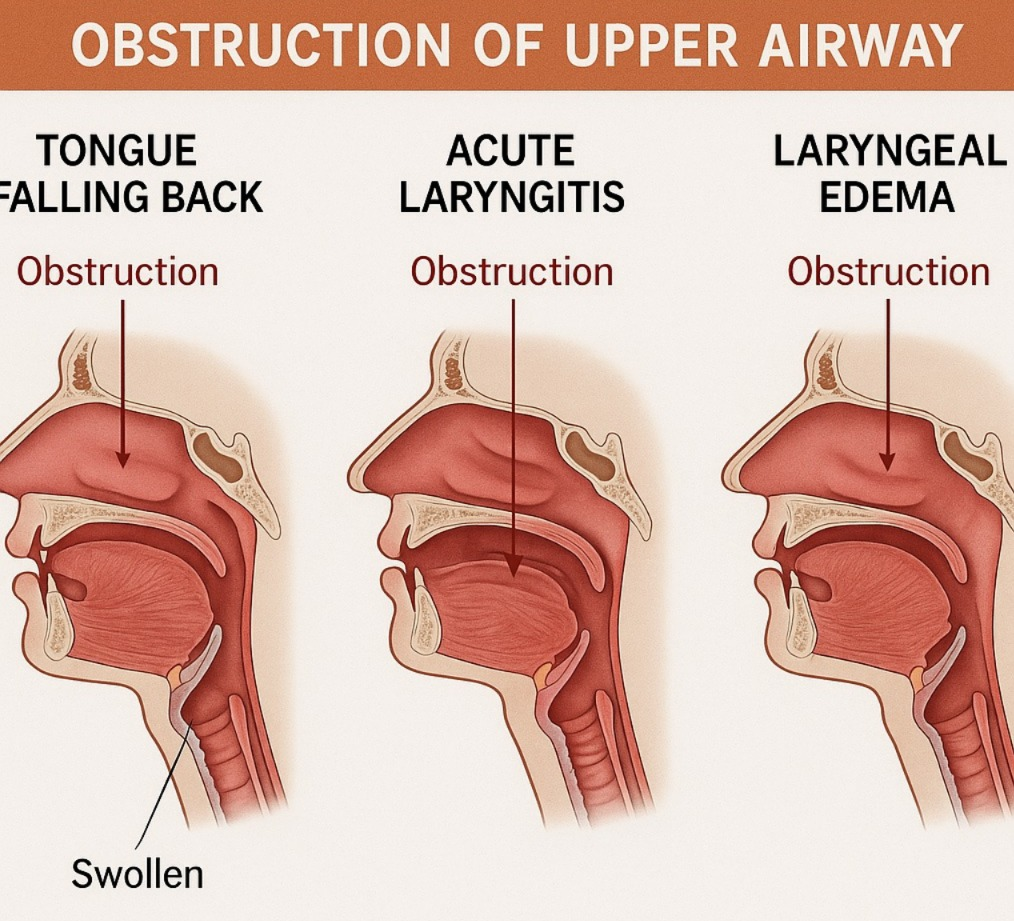
- This is a life threatening emergency. In which the upper airway becomes obstructed, causing the respiratory passage to become blocked, which obstructs the free flow of the airway.
Write causes of upper airway obstruction:
- Foreign object: Inhaling or ingesting a foreign object. Which blocks the airway such as food pieces, toys or small items
- Infection:Epiglottitis as well as infection in the larynx and pharynx cause edema and spasms there. Due to which airway blockage occurs.
- Trauma: Obstruction in the upper airway is seen due to injury to the face and neck. Such as fractures and dislocations
- Allergic reaction: Severe allergic reactions cause swelling in the airways, which leads to obstruction.
- Tumor: Abnormal growth and tumor formation in the upper airways cause blockage of the air passages.
Write clinical manifestations of upper airway obstruction:
The main sign of upper airway obstruction is choking .
- choking (Choking) : The universal sign for choking is ‘hand clutches to the throat’ i.e. the person clutches their throat during choking.
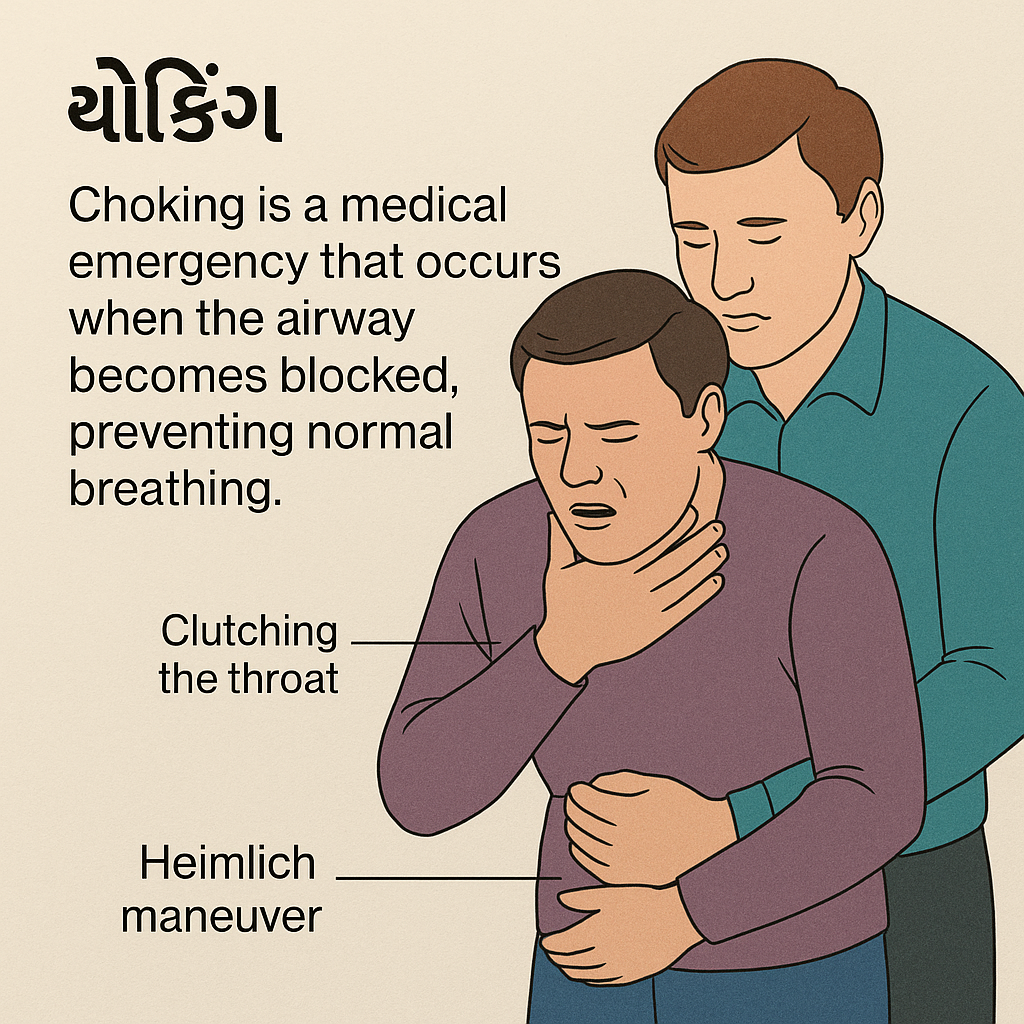
- Difficulty in breathing
- Cuffing or gagging
- Cyanosis
- Distress
- Restlessness
- Difficulty in speaking
- Aphonia
- Respiratory distress and death
Write management of upper airway obstruction:
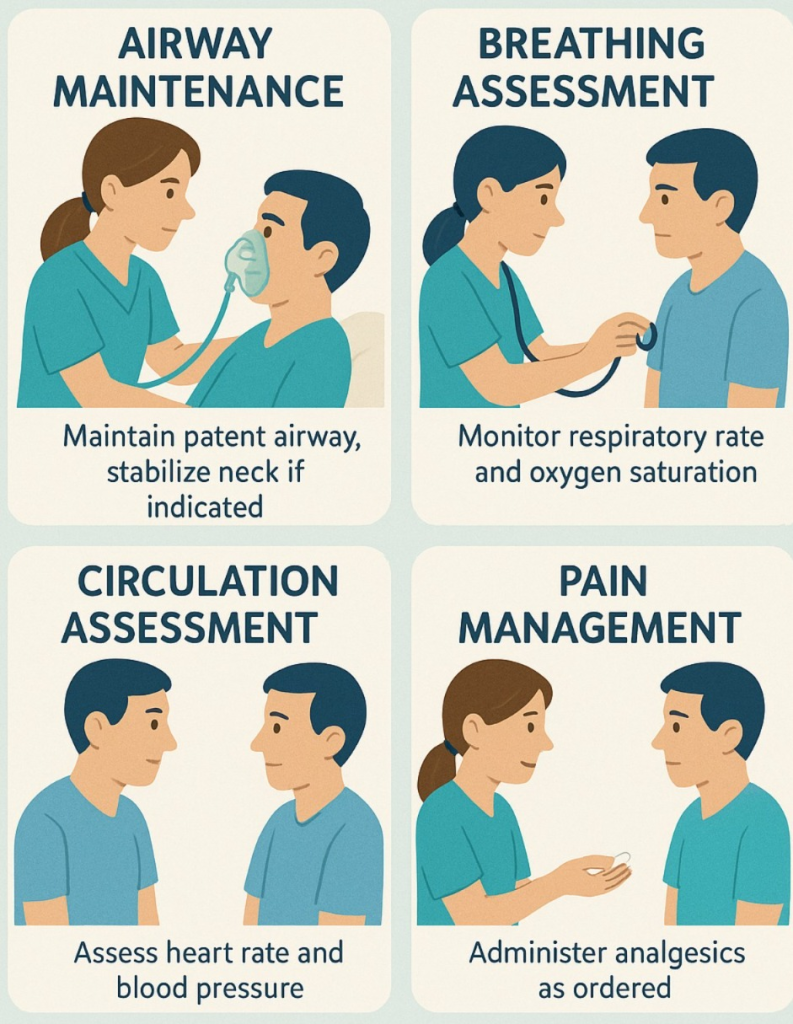
- Assessment: Assess the severity of the obstruction. Check for signs of respiratory distress.
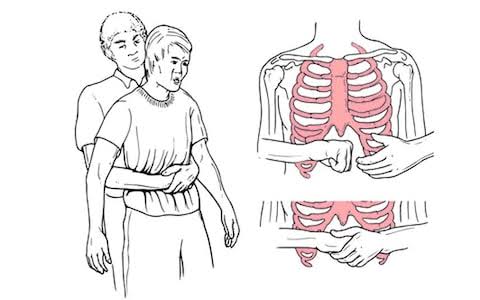
- Clear the Airway: Perform Heilmich Maneuvers to clear the airway.
Heilmich Maneuver in Adults and Children:
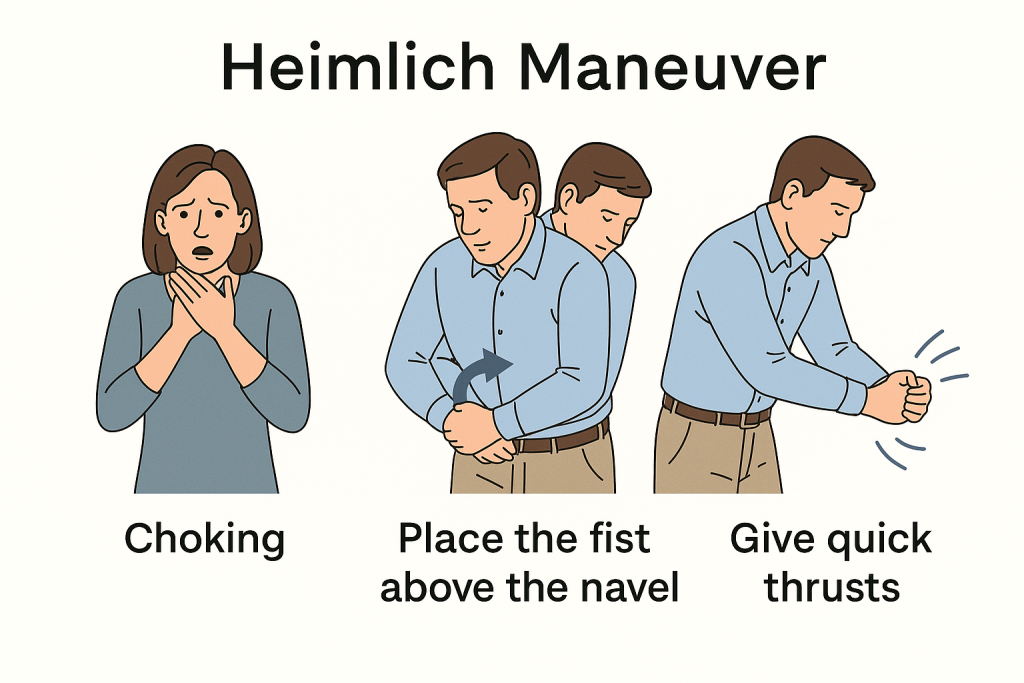
- Stand behind the adult patient. Keep one foot slightly in front of the other for balance.
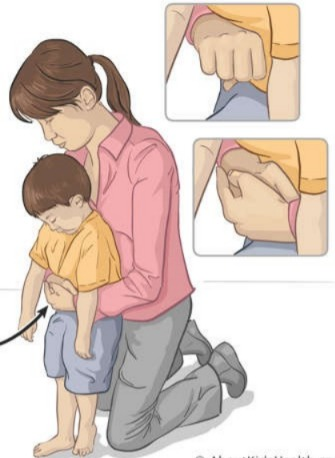
- If there is a child, sit behind him with his legs bent at the knees.
- Hold the arm next to the patient’s waist. Then make a fist with one hand and place the thumb side of the fist against the person’s abdomen, above the navel and below the ribs.
- With the help of the other hand, grab the fist and provide rapid upward thrusts into the abdomen.
- Provide repeated thrusts if the object has not yet come out.
- Apply a little less pressure to the child.
- Provide chest thrusts to the patient if the patient is pregnant and the arm is not around the stomach. To place the hand on the breastbone in chest thrusts and provide thrusts.
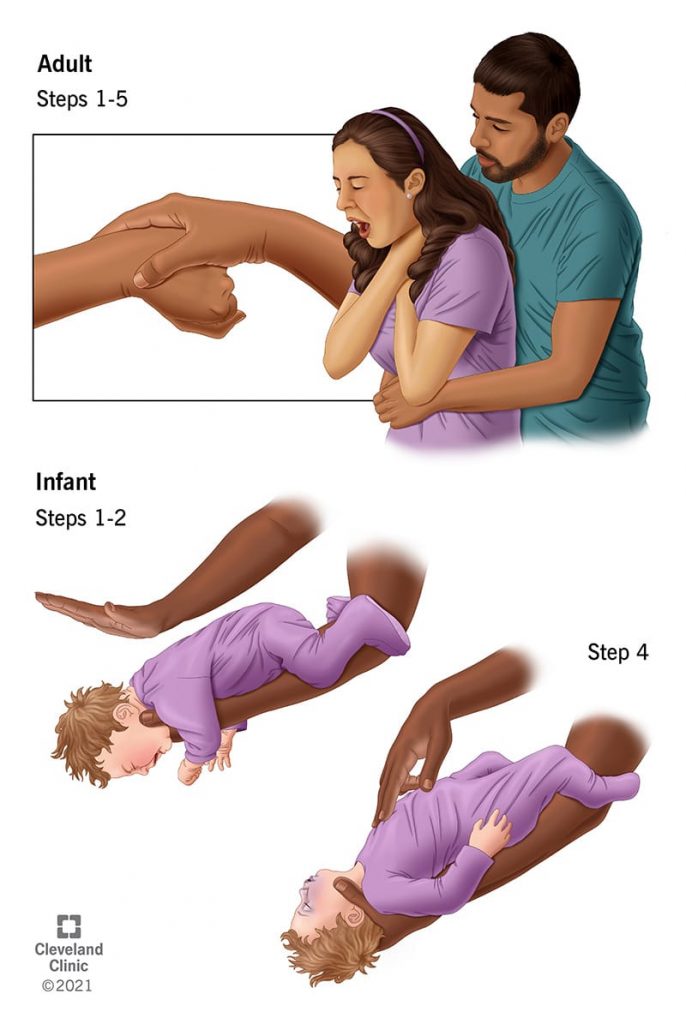
To provide back blow to the newborn and infant.
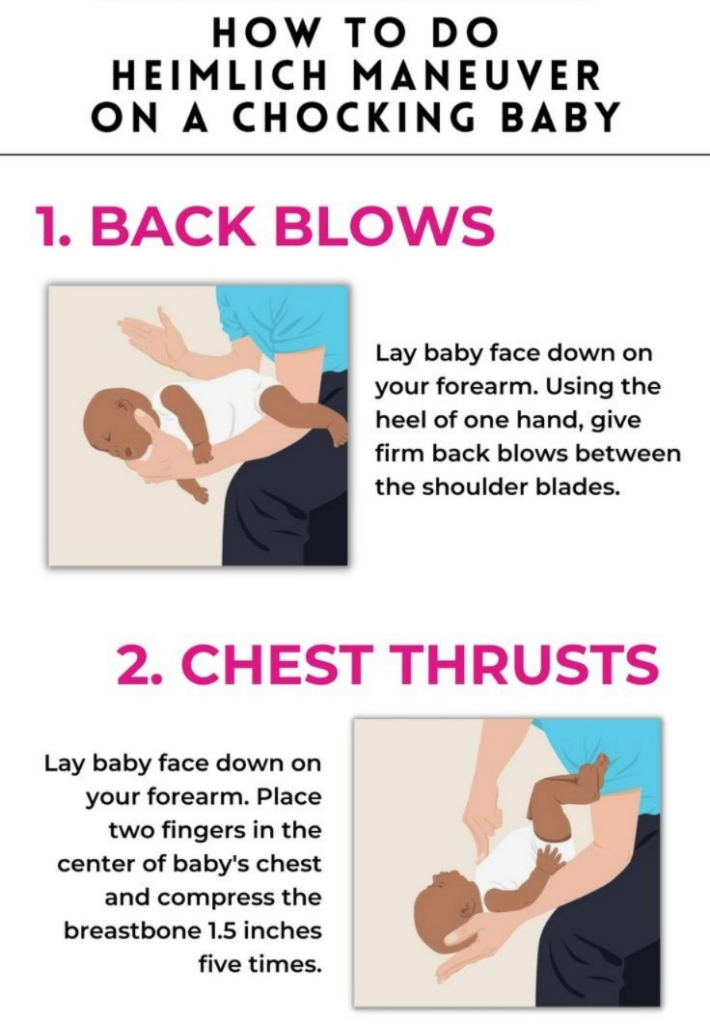
- In which the baby is placed in the forearm and gripped by the hand and given five black blows.
- Open the airway: If the patient is conscious and has difficulty breathing, ask the patient to forcefully expel the phlegm so that the obstruction is released. Go.
- Call for help: If the obstruction does not clear and the patient’s condition worsens, call emergency services.
- Oxygen therapy: If oxygen is unavailable, provide supplemental oxygen to improve oxygen levels.
Define Epistaxis:
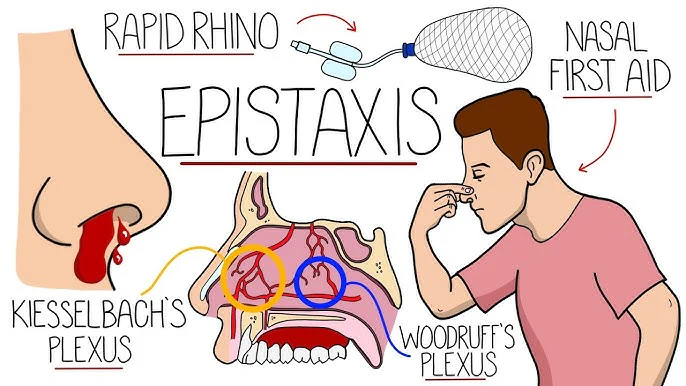
- Epistaxis means nose bleed or nasal hemorrhage
- Bleeding from the nostril or nasal cavity is known as epistaxis due to rupture of vessels in any area of the mucous membrane in the nose.
Type of epistaxis:
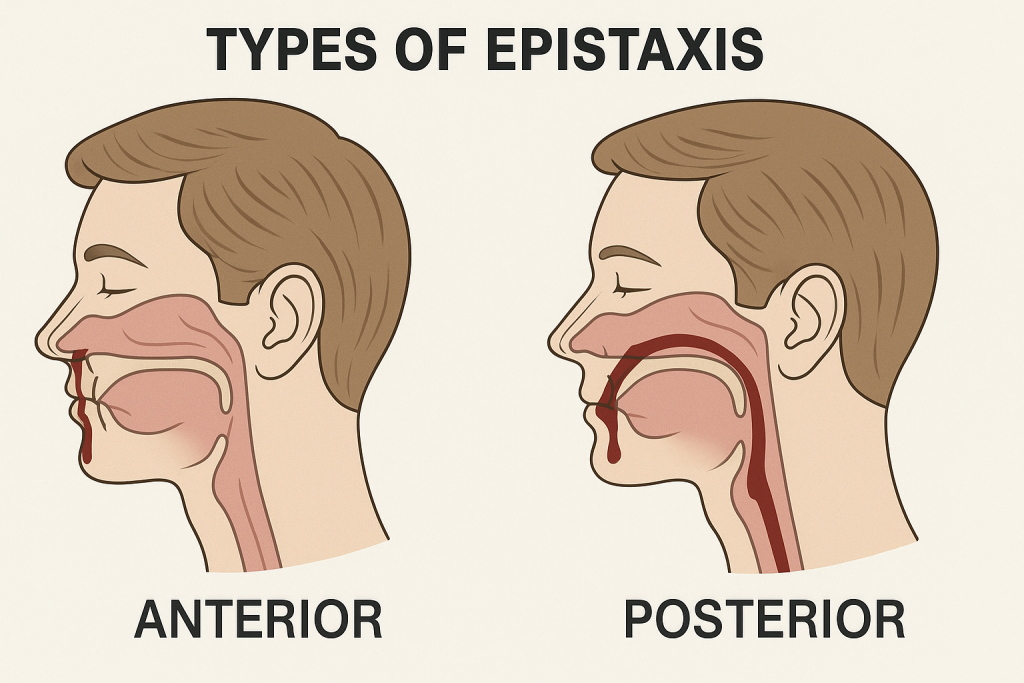
Epistaxis or nosebleed is divided into two types based on its location.

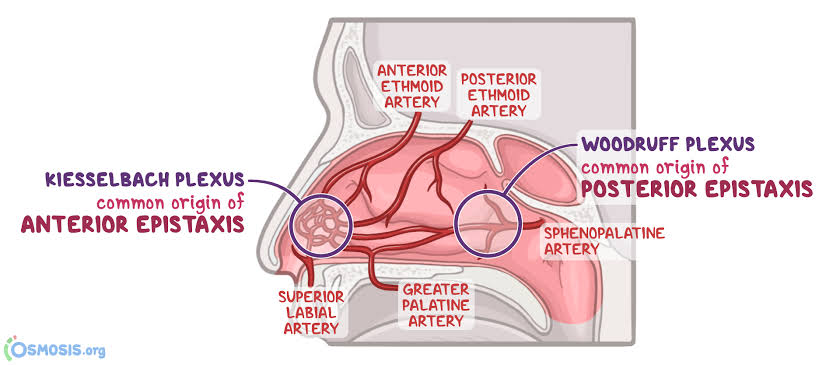
Anterior Epistaxis :
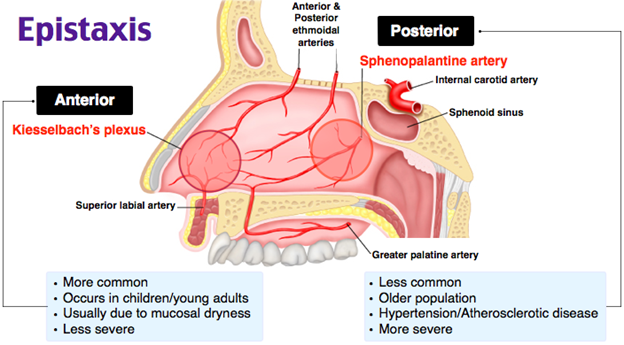
- Anterior epistaxis involves bleeding from blood vessels in the front part of the nose. This area is known as the Klesselbach Plexus. Anterior epistaxis is the most common type, with bleeding occurring from the nostrils. It can be managed by applying gentle pressure or nasal packing.
Posterior Epistaxis:
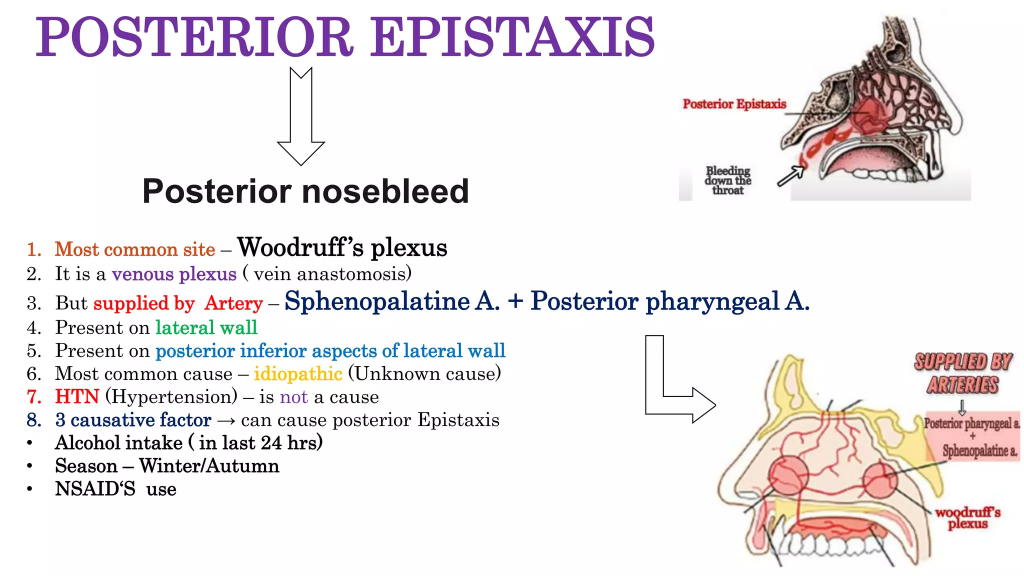
- Posterior epistaxis is bleeding from the back part of the nose or the deeper nasal cavity. That is, bleeding is seen from the area containing the sphenopalatine artery. That area is known as the Woodruff Plexus. Posterior epistaxis is less common but is a challenging form to control. In which bleeding is seen from the nostril and blood drains into the throat, hence blood is seen in the sputum. Management of posterior epistaxis requires surgical procedures.
Write causes of epistaxis:
- Nasal trauma (most common cause)
- Nasal infection
- Nasal Irritant
- Dry air
- Allergies
- Underlying medication (heparin, warfarin)
Explain pathophysiology of epistaxis:
Due to etiological factors
|
Inflammation occurs in the vessels of the mucous membrane in the nose.
|
This causes the vessels to rupture.
|
Which leads to nose bleeds.
Explain sign & symptoms of epistaxis (Explain sign and symptoms of epistaxis):
- Bleeding from the nose (nose bleed)
- Blood dripping from the nostrils
- Presence of blood clot
- Mouth bleed
- Tachycardia
- Headache
- Diagnosis
- Fainting
How to diagnose epistaxis:
- History Collection
- Physical Examination
- Nasal Endoscopy
- X-ray
- CT Scan
- Angiography
- Biopsy
Write medical management of epistaxis:
Pressure :
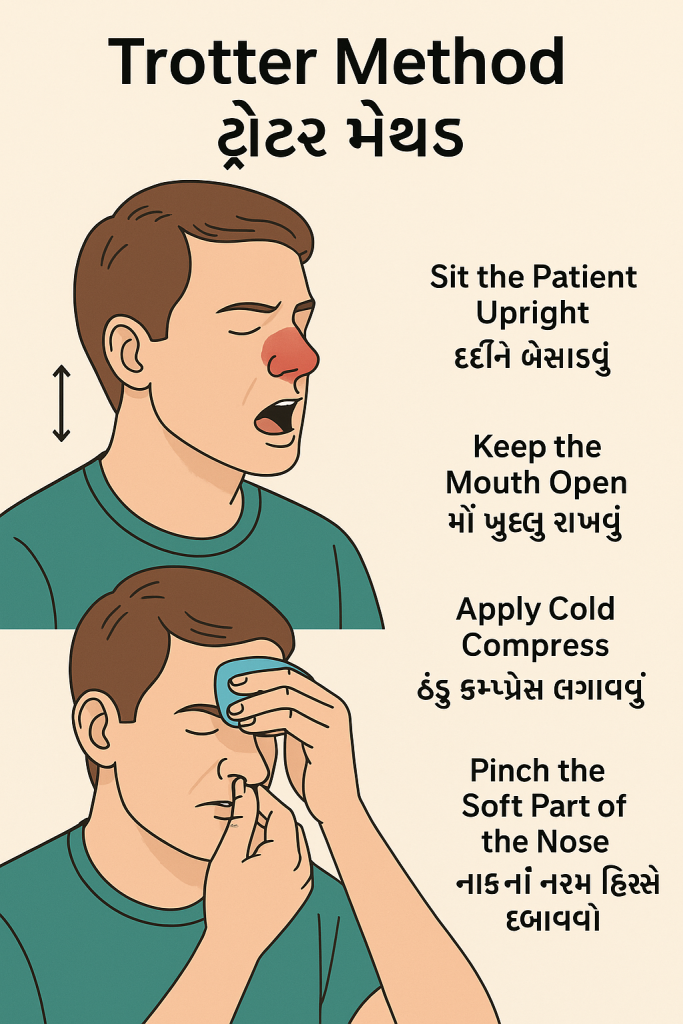
- Pressure is applied to the soft part of the nose, i.e. the nose is pinched with the thumb and index finger for 10 to 15 minutes and breathing is done through the mouth. This method is called Trotter Method. During this method, the patient is given a sitting or semi-fowler position.
Ice pack :
- Applying an ice pack or cold compress to the bridge of the nose can constrict blood vessels and reduce bleeding.
Nasal spray:
- Use an over-the-counter saline nasal spray or decongestant. Which helps blood vessels shrink.
Topical Medicine:
- Use petroleum jelly as a topical agent. Which moisturizes the nasal mucosa and protects the nasal mucosa.
Write surgical management of epistaxis:
Surgical management is performed to control bleeding when medical management fails to control nosebleeds. The following surgical methods are used in it.
Cauterization :
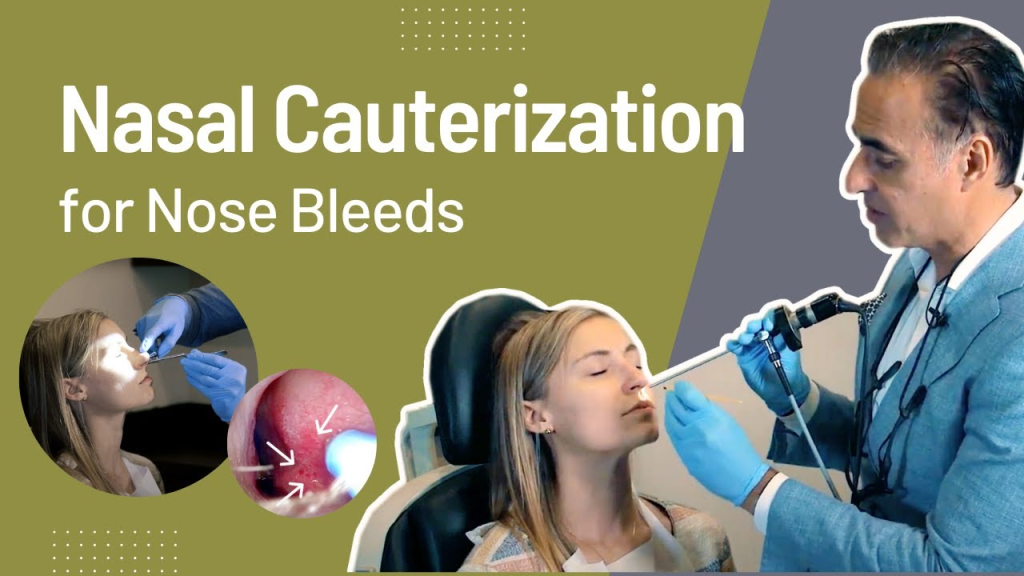
- Cauterization involves sealing bleeding blood vessels using heat, electricity, or chemicals. In which silver nitrate is mostly used as a chemical.
Nasal packing:
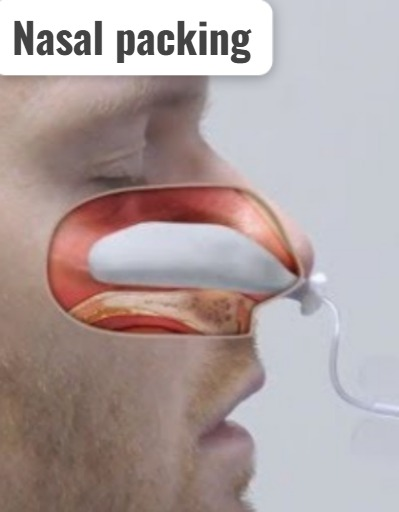
In nasal packing, gauze or a special balloon is inserted into the nasal cavity and pressure is applied to the blocked point to stop the blockage. Nasal packing includes anterior and posterior nasal packing.
Ligation:
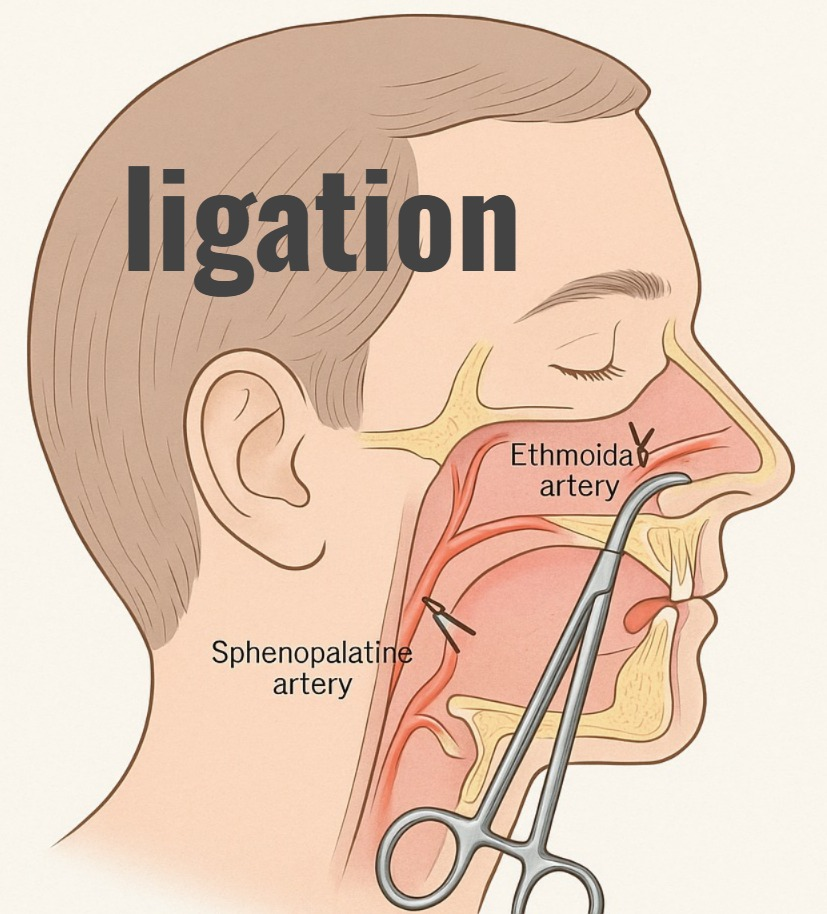
In ligation, blood vessels are ligated or tied to stop the building.
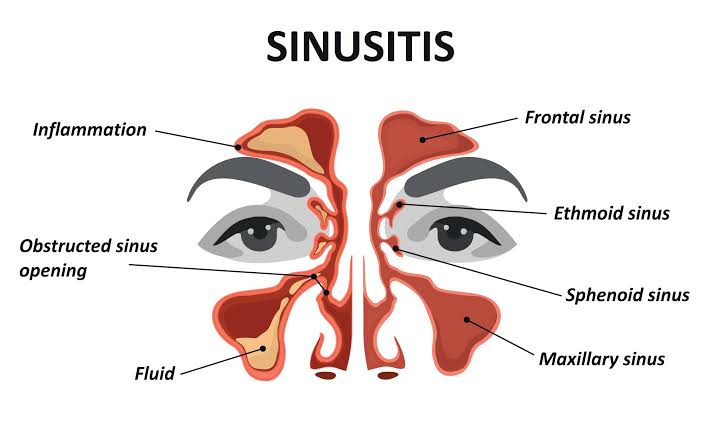
Define sinusitis:
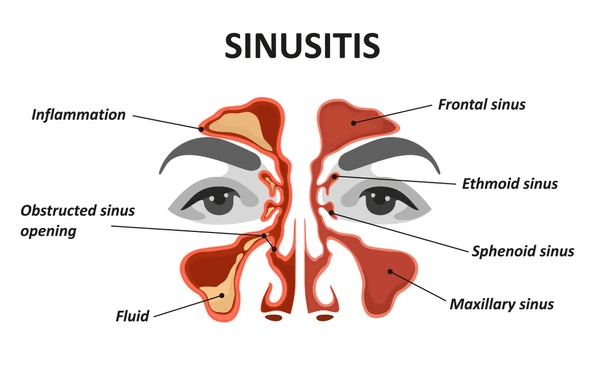
- Infection and inflammation of the sinuses Known as sinusitis. Sinuses are air-filled cavities located in the face and skull.
Write causes of sinusitis:
- Viral infection
- Bacterial infection
- Allergies
- Nasal polyps
- Structural problem (deviated nasal septum)
- Immune system disorder
Risk factor:
- Changes in the Temperature and Air
- Swimming
- Smoking
- Driving
Classification of sinusitis:
Sinusitis is classified on the basis of its duration and severity as follows.
On the basis of duration:
1) Acute Sinusities: Acute sinusitis has four stages. Symptoms of sinusitis are seen for a period of less than 12 weeks. Which is mainly caused by bacterial or viral infections. In which facial pain, nasal congestion, nasal discharge and fatigue are seen.
2) Subacute sinusitis (SubAcute Sinusities): In subacute sinusitis, symptoms of sinusitis are seen for 4 to 12 weeks. It has symptoms similar to acute sinusitis but is less severe.
3) Chronic sinusitis (Chronic Sinusities) : In chronic sinusitis, symptoms of sinusitis are seen for a period of 12 weeks or more. Chronic sinusitis is caused by persistent inflammation, recurrent infection, allergies or structural issues.
4) Recurrent Sinusitis (Recurrent Sinusities) : If multiple episodes of acute sinusitis are seen within a year, it is known as recurrent sinusitis.
On the basis of location:
1) Maxillary sinusitis:
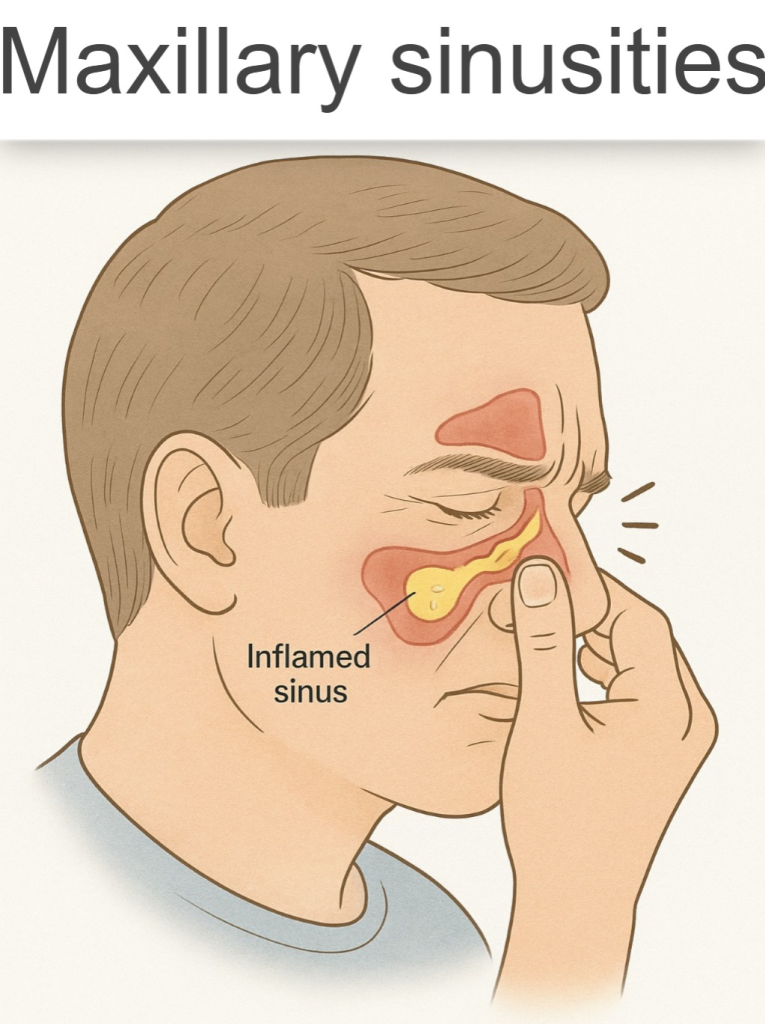
- Maxillary sinusitis is inflammation of the maxillary sinuses, which are located in the cheekbone. Maxillary sinusitis is the most common type of sinusitis.
2) Frontal Sinusities:

- In frontal sinusitis, inflammation is seen in the frontal sinuses. Which is located behind the forehead and forms a frontal headache.
3) Ethmoid sinusitis:
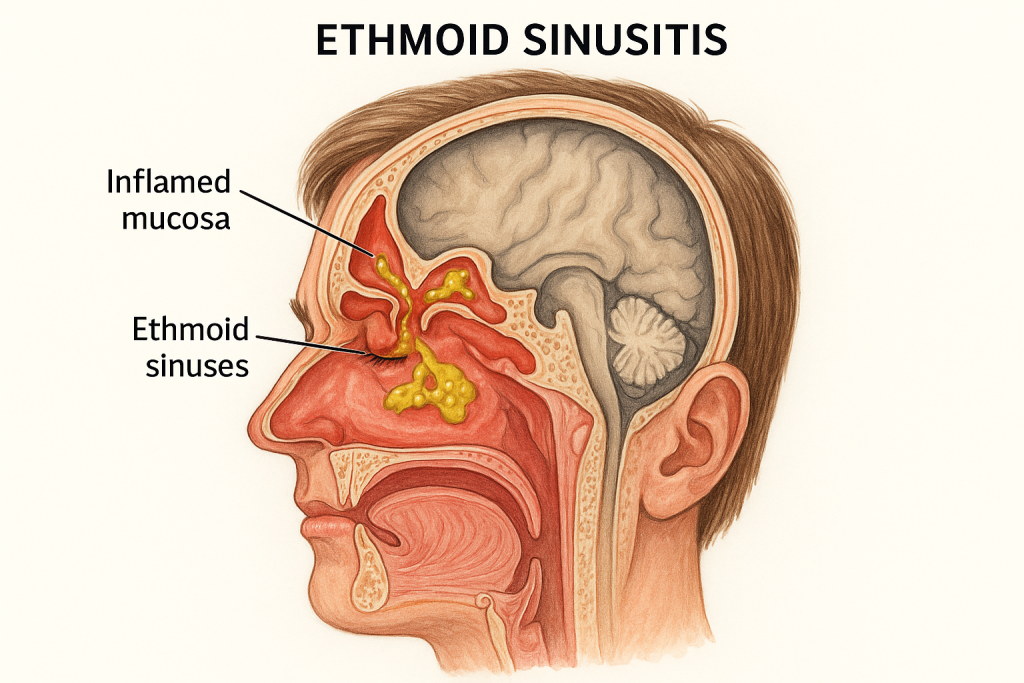
- Ethmoid sinusitis is inflammation of the ethmoid sinus, which is located between the eyes. And it causes pain and pressure around the eye.
4) Sphenoid sinusitis:
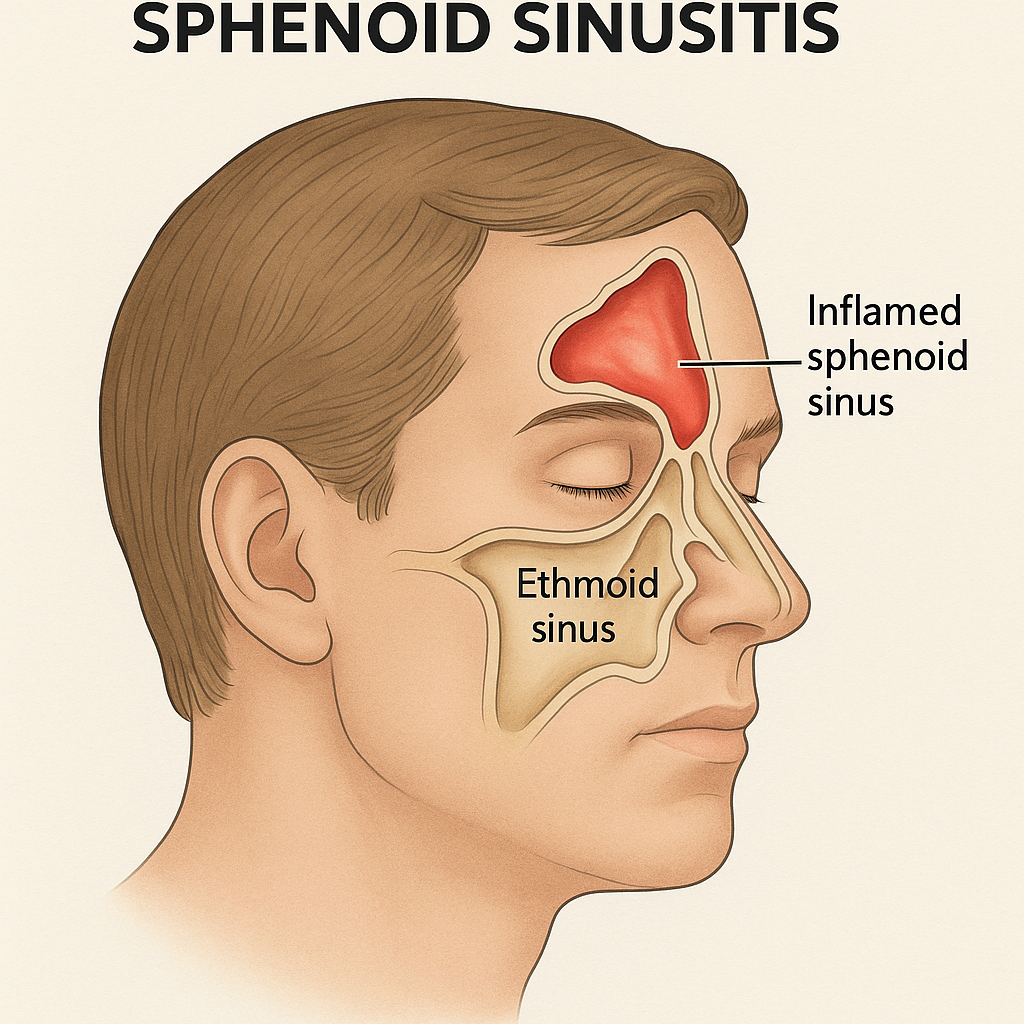
- Sphenoid sinusitis is inflammation of the sphenoid sinus. It is located behind the ethmoid sinus and deep in the skull. Which causes earache, headache and neck pain.
Write clinical manifestations of sinusitis:
- Clinical signs are seen depending on the type of sinusitis and its severity.
- Facial pain and pressure: Pain is seen in the eye, forehead, nose and cheek area. is.
- Nasal congestion: Blockage and stuffiness are seen in the nasal passages.
- Nasal discharge: Thick discolored mucus discharge is seen.
- Reduced sense of smell and taste
- Cough
- Sore throat
- Fatigue
- Fever
- Headache
- Toothache
- Ear pressure or fullness
- Halitosis
- Vertigo
- Blurred vision
Write diagnostic evaluation of sinusitis
- History collection
- Physical examination
- X-ray
- CT scan
- Endoscopy
- Rhinoscopy
Write medical management of sinusitis:
- To reduce nasal congestion, give a nasal spray or oral decongestant. This can promote drainage. Do not use nasal decongestant sprays for a long time. Because it causes rebound congestion.
Saline nasal irrigation:
- Using saline solution to flush out the nasal passages helps clear mucus and reduces inflammation and promotes drainage.
Nasal corticosteroid:
- Use nasal corticosteroids to reduce inflammation of the nasal passages and sinuses and to relieve symptoms of congestion.
Antibiotic:
- If sinusitis is caused by a bacterial infection, then antibiotic drugs should be provided to treat it.
Pain relievers:
- Provide over-the-counter medications acetaminophen and ibuprofen to relieve facial pain, headaches, and earaches.
Mucolytics:
- Provide mucolytic drugs to thin and loosen mucus so that sinus drainage can improve.
Write surgical management of sinusitis:
Surgical management is performed when medical management fails. The following common surgical procedures are performed for the management of sinusitis.
Functional Endoscopy Sinus Surgery (FESS):
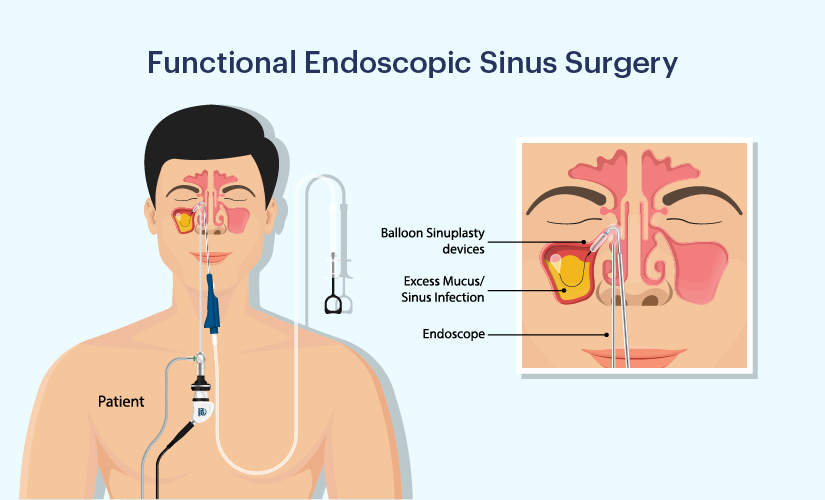
- FESS is the most common surgical procedure used to treat chronic sinusitis. It involves inserting a thin, flexible tube called an endoscope and attaching a camera to it. This allows the sinuses to be visualized. This endoscope is introduced into the nasal cavity through the nostril and obstructions such as nasal polyps, scar tissue and bony growths are removed and the opening of the sinuses is widened.
Image Guided Surgery (Image Guided Surgery) :
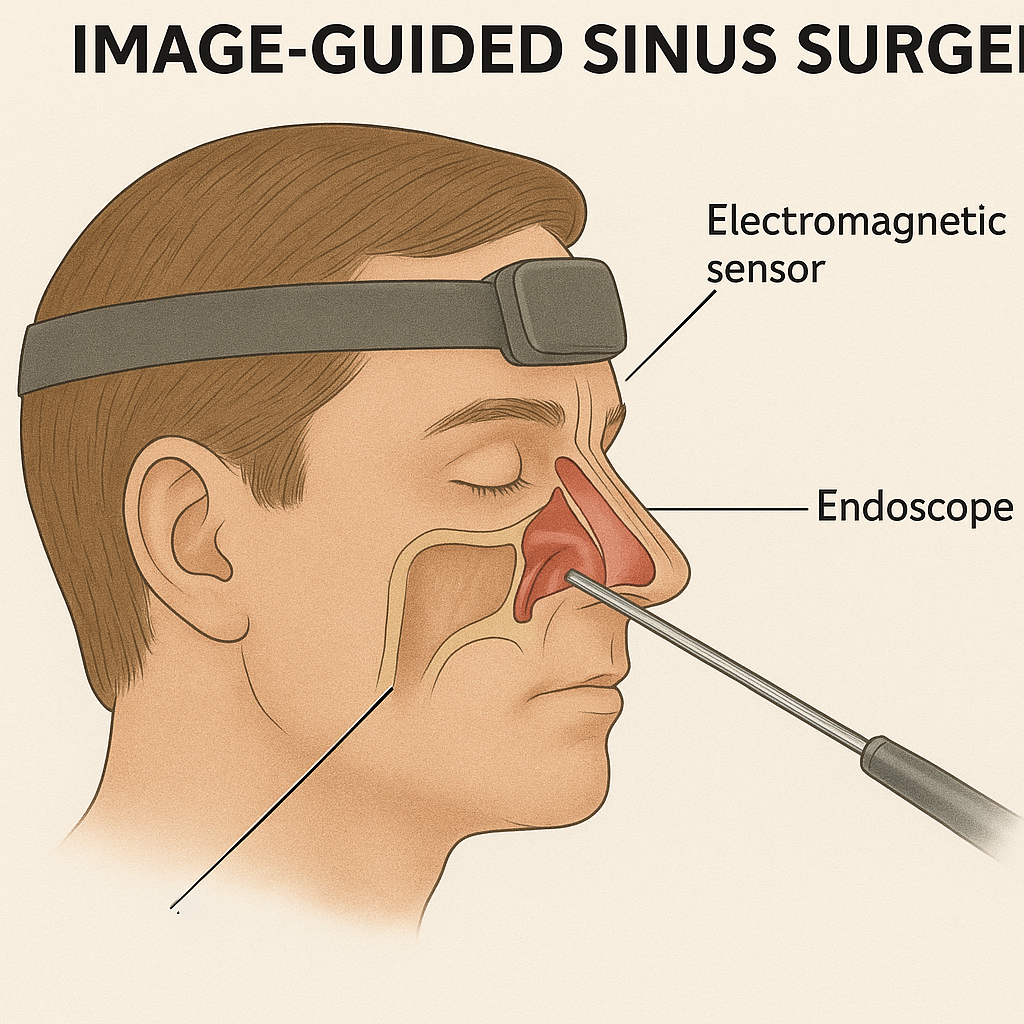
- Image-guided surgery is performed when the anatomy is found to be distorted due to previous surgery or other disease. In which the location is decided and surgery is performed using a CT scan or other image-guided method.
Balloon sinuplasty (Balloon sinuplasty) :
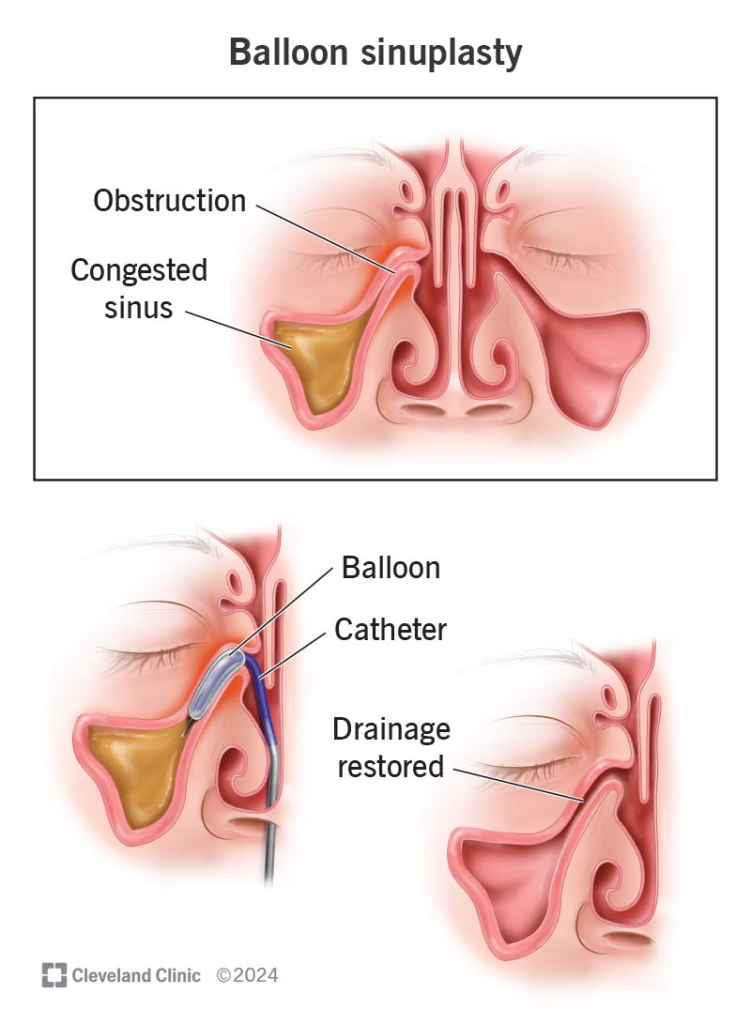
- This is a minimally invasive procedure in which a small flexible balloon catheter is inserted into the inflamed sinus and the balloon is inflated there, dilating and expanding the opening of the sinus.
Cardwell Luck Operation (Cardwell Luck Operation) :
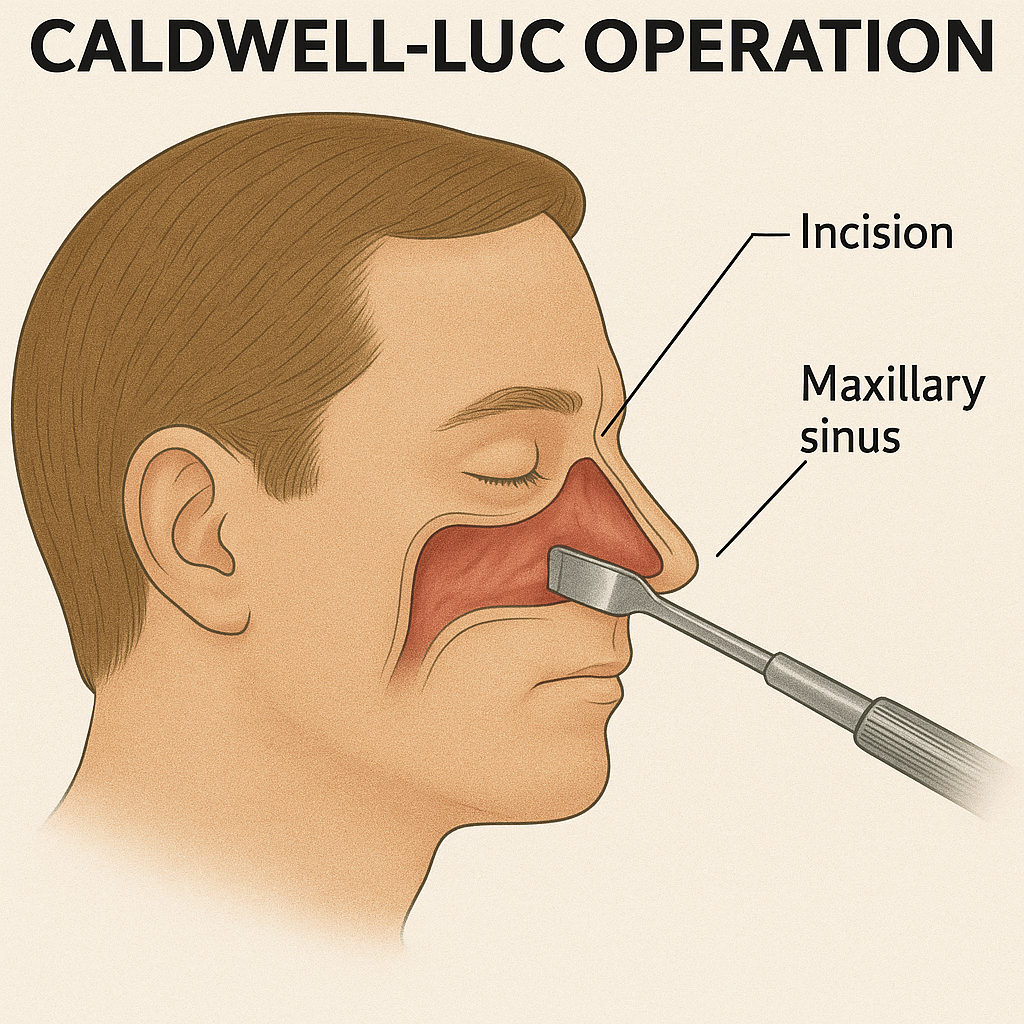
- Cardwell Lock operation is mainly performed for the treatment of chronic maxillary sinusitis. In which a large window is created in the maxillary sinus to improve drainage.
Sinus irrigation:
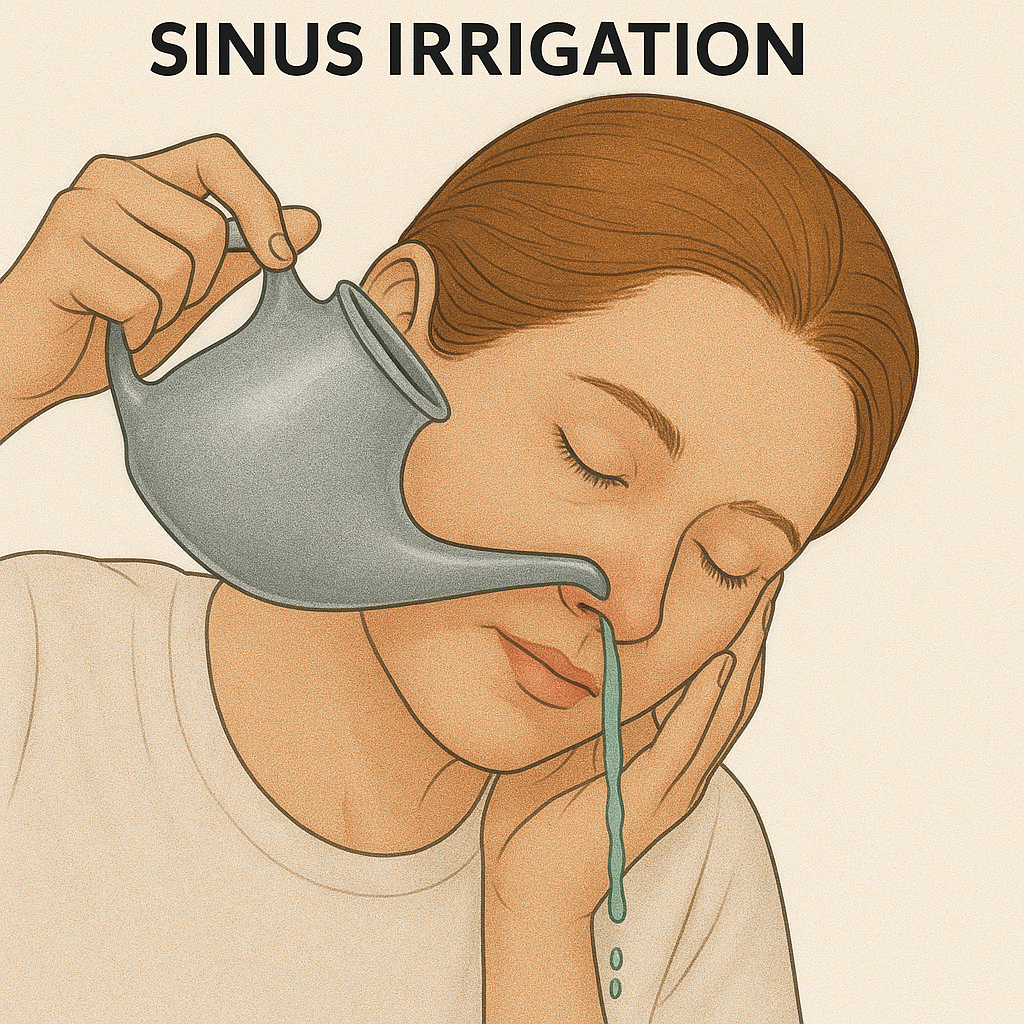
- In some cases, surgical management involves placement of a sinus irrigation device such as a sinus stent or irrigation tube to promote drainage and reduce the risk of inflammation and infection.
Ethmoidectomy, Maxillary Antrostomy, Sphenoidotomy:
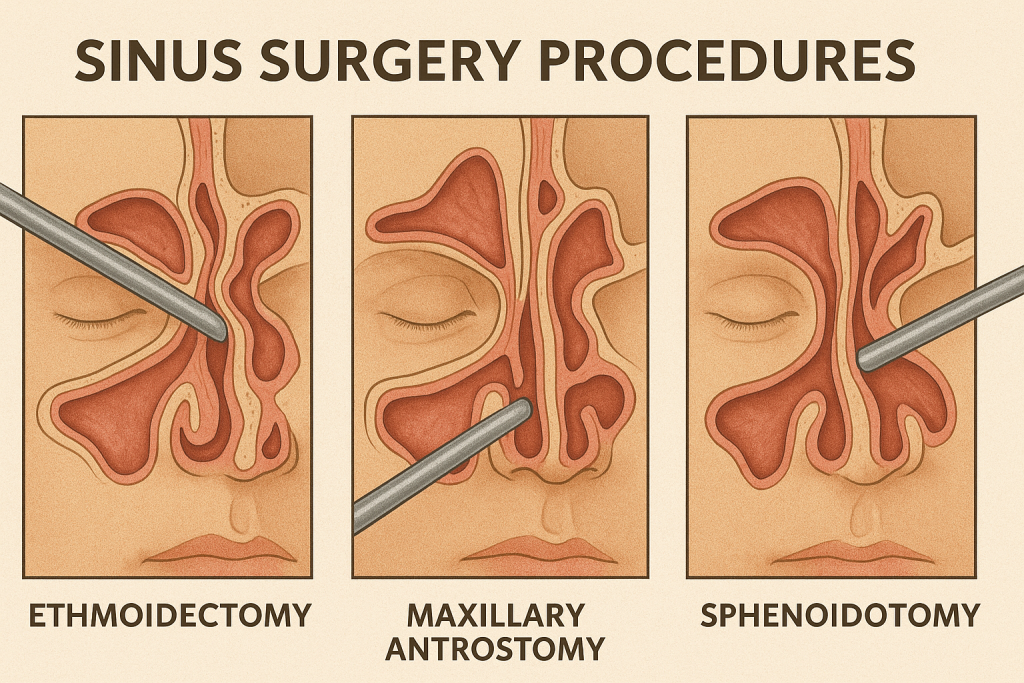
- This is a specific procedure that targets the ethmoid, maxillary and sphenoid sinuses to open them, remove abnormal tissue and improve drainage
Define pharyngitis
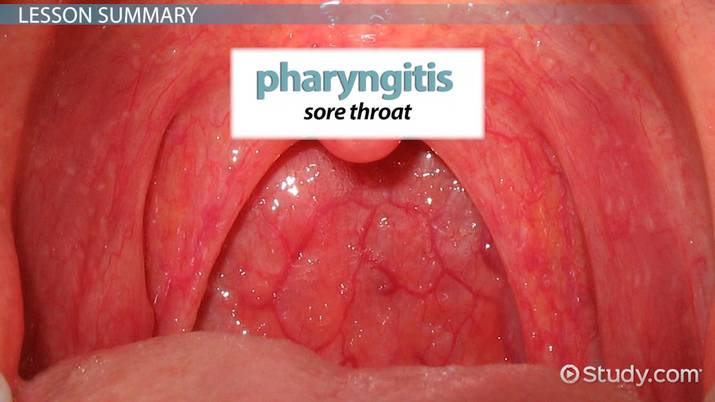
- Infection and inflammation of the pharynx is known as pharyngitis.
- Which is Also known as ‘Sore Throat’.
Write causes of pharyngitis (right cause of pharyngitis):
Bacterial infection:
- Pharyngitis is caused by group A streptococcus bacteria.
Viral infection:
- Viruses like common cold virus, influenza virus, Epstein Barr virus are responsible for causing pharyngitis.
Allergies:
- Irritation and inflammation are seen in the throat area due to contact with allergens.
Environmental Factor:
- Pharyngitis can be caused by exposure to smoke, dry air, and pollutants.
Irritant:
- Pharyngitis can be caused by exposure to strong chemicals and fumes.
Gastroesophageal reflux disease:
- Backflow of stomach acid into the throat can cause irritation and pharyngitis.
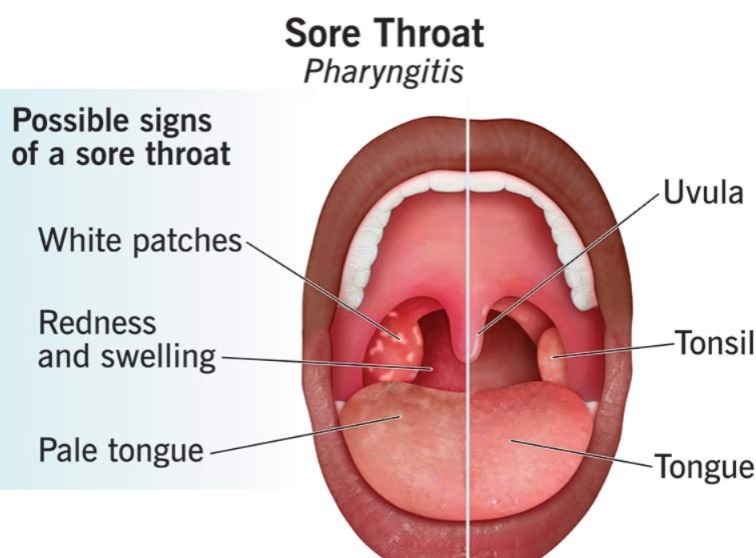
Explain sign & symptoms seen in pharyngitis (Explain sign & Symptoms seen in pharyngitis)
- Sore throat
- Throat pain
- Redness and swelling
- Dysphagia
- Hacking cough
- Fever
- Headache
- Discomfort
- Malass
Write diagnostic evaluation of pharyngitis
- History Collection
- Physical Examination
- Complete Blood Count
- Throat Culture
Write management of pharyngitis
Antibiotic: Use antibiotic medicine to treat bacterial infections. Such as penicillin, azithromycin
Antiviral: Use antiviral medicine to treat viral infections. Such as acyclovir
Corticosteroids : Use corticosteroid drugs to control inflammation.
Pain relievers : Use over-the-counter drugs such as acetaminophen and ibuprofen to relieve pain. Which relieves pain and reduces body temperature.
Throat lozenges: Throat lozenges relieve throat irritation.
Hydration: Intake plenty of fluids to maintain hydration.
Warm salt water Gargle: Gargle with warm salt water. This will relieve throat discomfort.
Avoid irritants: Avoid irritants such as smoking, pollutants, etc.
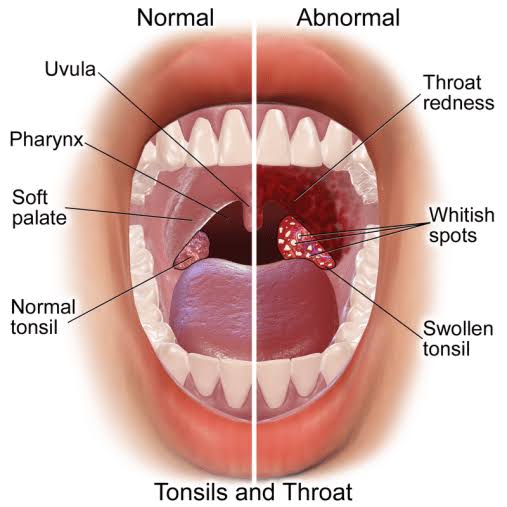
Define Tonsillitis:
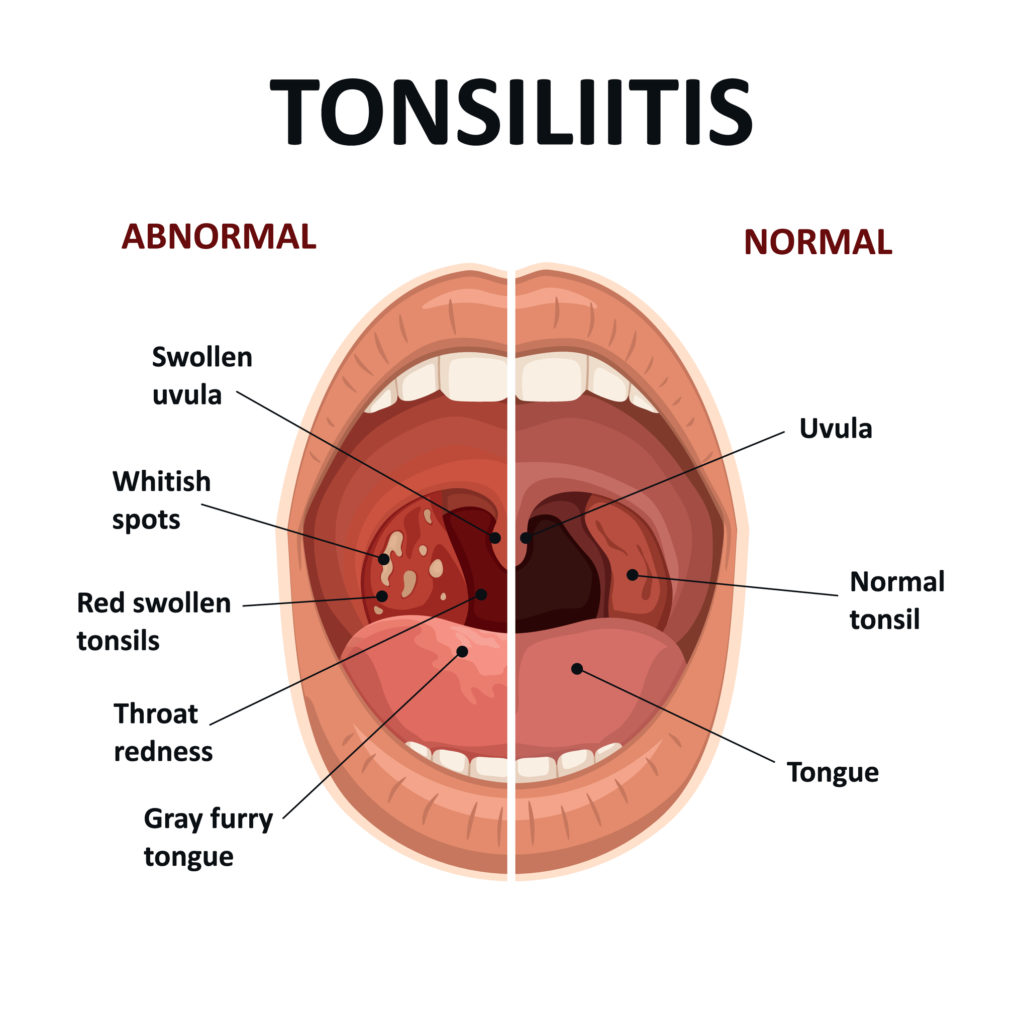
- Infection and inflammation of the tonsils is known as tonsillitis. It is mainly caused by bacterial and viral infections.
- (Tonsils are small masses of tissue located on the side of the throat that filter and kill foreign bodies that enter through the nose and mouth)
Write causes of tonsillitis (Write causes of tonsillitis):
- Tonsillitis is mainly caused by bacterial and viral infections. In which tonsillitis is mainly caused by Group A Streptococcus bacteria. Common viruses include influenza virus, herpes simplex virus, cytomegalovirus, adenovirus, and Epstein-Barr virus.
Explain pathophysiology of tonsillitis:
Etiological factors
|
Bacteria and viruses enter the body through the nose and mouth.
|
They are filtered by the tonsils located there.
|
White blood cells are the ones that fight bacteria And surrounds the virus and fights with it.
|
This causes an increase in body temperature. Due to which fever is seen.
|
The tonsils become inflamed and painful.
|
The condition of tonsillitis is seen.
Explain sign & symptoms seen in tonsillitis (Explain sign and symptoms seen in tonsillitis)
- Swelling seen in the throat
- Sore throat and throat pain
- White and yellow colored patches seen on the tonsils
- Dysphagia (difficulty in swallowing)
- Swelling of the lymph nodes in the neck
- Referred pain in the ear (ipsilateral ear)
- Bad breath and foul smelling (halitosis)
- Fever
- Headache
- Chills
- malaise
- discomfort
- fatigue
How to diagnose tonsilitis (How to diagnose tonsillitis):
- History Collection
- Physical Examination
- Complete Blood Count
- Throat Culture (Rapid Strip Test)
Write medical management of tonsillitis (Write medical management of tonsillitis) Tonsillitis)
- Antibiotics: If tonsillitis is caused by a bacterial infection, then antibiotic drugs should be given to treat it.
- Pain relievers:Provide analgesic medicine to relieve pain.
- Corticosteroid: In selected cases, corticosteroid drugs are given to reduce inflammation.
- Antipyretic: Use antipyretic drugs to reduce fever.
- Fluid: Provide plenty of fluids to the patient. So that dehydration can be prevented.
- Rest : Provide adequate rest to the patient.
Write surgical management of tonsillitis:
Tonsillectomy (Tonsilectomy) :

- Tonsillectomy is performed in patients with recurrent or chronic tonsillitis, i.e. Tonsils are surgically removed.
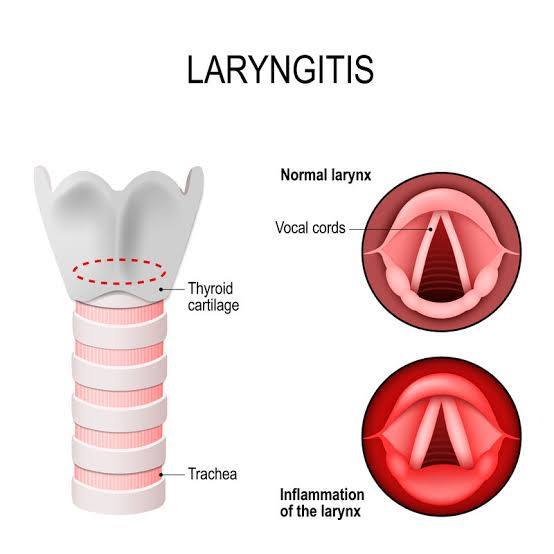
Define Laryngitis:
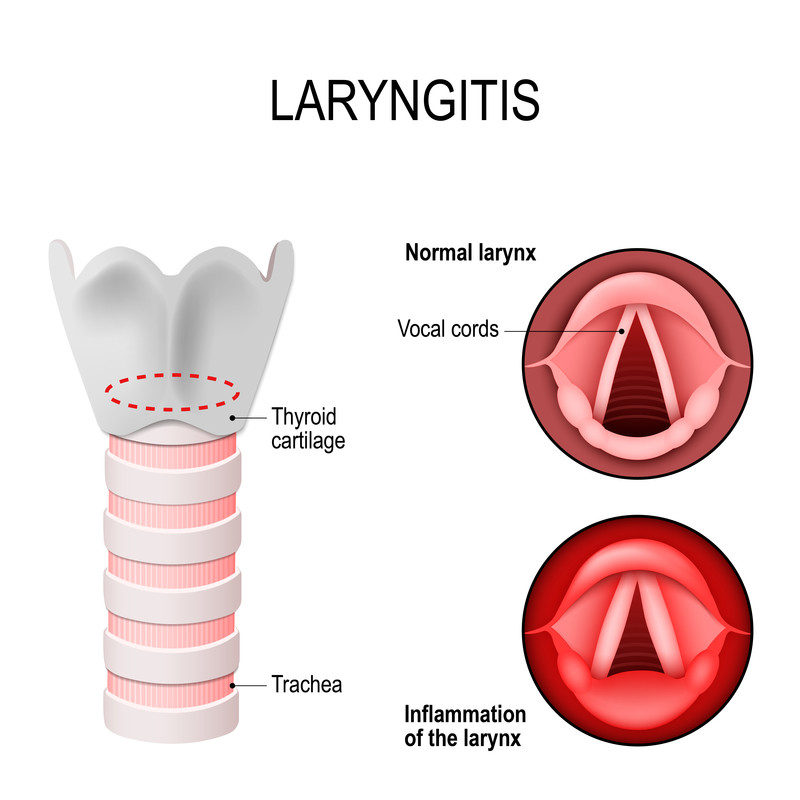
- Infection and inflammation of the larynx (voice box) is known as laryngitis Comes.
Write etiological factor of laryngitis:
- Bacterial Infection: Laryngitis is caused by bacteria such as Streptococcus.
- Viral Infection: Laryngitis is also caused by viruses that cause the common cold and flu.
- Excessive Train: Excessive training of the vocal cords (by speaking loudly for a long time) can cause laryngitis.
- Irritants: Exposure to irritants such as smoke, strong fumes, and chemicals can cause laryngitis.
- Acid Reflex
- Allergies
- Respiratory Infection
- Inhalation of Toxic Substances
Explain sign & symptoms seen in laryngitis (Explain sign and symptoms seen in laryngitis):
- Horsiness
- Dry cough
- Sore throat
- Throat pain
- Dysphagia (difficulty in swallowing)
- Aphonia (Loss of Voice)
- Fever
- Fatigue
- Malass
- Discomfort
Write medical management of laryngitis (Right Medical Management of Laryngitis):
Use antibiotic medicine to treat bacterial infections. Such as penicillin, azithromycin
- Antiviral: Use antiviral medicine to treat viral infections. Such as acyclovir
- Corticosteroids: Use corticosteroid drugs to control inflammation.
- Pain relievers: Use over-the-counter drugs such as acetaminophen and ibuprofen to relieve pain. Which relieves pain and reduces body temperature.
- Throat lozenges: Throat lozenges relieve throat irritation.
- Hydration: Intake plenty of fluids to maintain hydration.
- Warm salt water gargle: Gargle with warm salt water. So that throat discomfort is relieved.
- Avoid Irritants:Avoid irritants such as smoking, pollutants, etc.
- Resting the Voice:Advise the patient not to talk too much and speak only when necessary.
- Voice Therapy: Voice therapy is provided in some cases to make the voice more effective.
- Hydration: Ask the patient to take fluids so that the vocal cords remain hydrated.
Define deviated nasal septum:
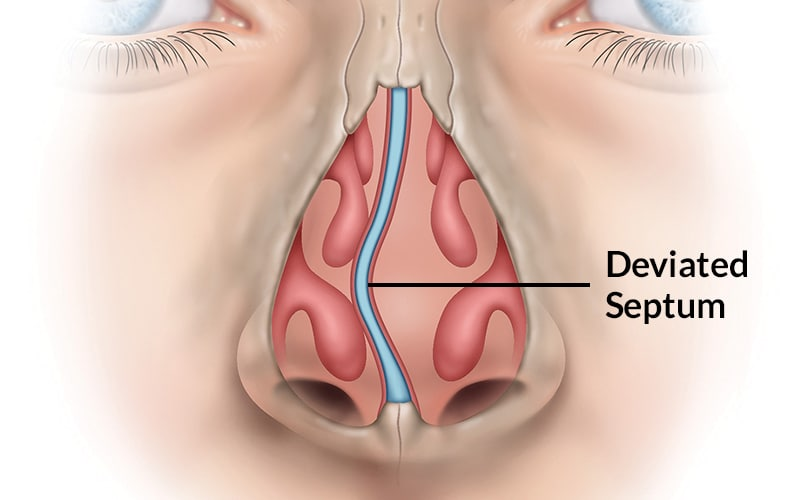
- The septum between the nostrils, which is normally thin and straight, deviates and protrudes from the midline, causing nasal obstruction and breathing difficulty.
Write causes of deviated nasal septum (right cause of deviated nasal septum):
- A deviated nasal septum is congenital and acquired.
- Congenital factors include birth defects or genetic predisposition.
- Acquired factors include nasal trauma.
Types of deviated nasal septum (Types of deviated nasal septum):
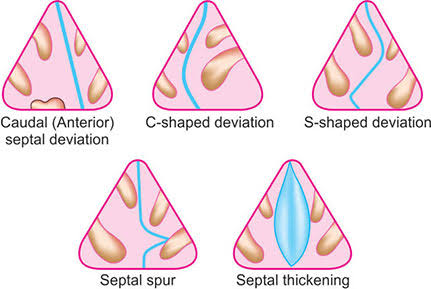
- Anterior or Caudal Dislocation :
In anterior dislocation, the front portion of the septum is deviated. Which can be visualized by external examination.
- ‘C’ Shape Deviation :
In ‘C’ shape deviation, the septum is seen to be deviated convexly on one side like the letter ‘c’.
- ‘S’ Shape Deviation :
In ‘S’ shape deviation, the septum is seen deviated like the letter ‘s’ on the convex side.
- Septal spur :
Spur a It is a shelf-like projection that is located near the junction of bone and cartilage. This spur is dislocated towards the lateral wall.
- Septal thickening :
In some cases of nasal trauma, nasal septum thickening is seen due to hematoma and excess fibrosis.
Write sign and symptoms of deviated nasal septum right sign & Symptoms of Deviated Nasal Septum)
- Difficulty in Breathing
- Noisy Breathing
- Nasal Congestion
- Recurrent Sinus Infection
- Headache
- Post Nasal Drip
- Nose Bleed
- Snoring
Wirte medical management of deviated nasal septum
- Nasal decongestant : Use nasal decongestant sprays and drops to reduce nasal congestion.
- Nasal corticosteroid : Use nasal corticosteroid sprays to reduce inflammation and swelling of the nasal passages.
- Antihistamine : If If nasal congestion and inflammation are observed due to allergies, antihistamine drugs should be provided.
- Saline nasal irrigation: Use saline nasal irrigation regularly. Which helps clear the nasal passages and relieve congestion.
- Nasal dilators: Use external nasal dilators such as adhesive strips that widen the nasal passages to improve airflow.
- Avoiding allergens: Minimize contact with allergens. So that nasal symptoms can be relieved.
Wirte surgical management of deviated nasal septum
Submucous resection-SMR (submucous resection):
- Submucous resection is a surgical procedure commonly used to treat a deviated nasal septum. In which the submucous tissue in the nasal septum is removed and repositioned.
Septoplasty (Septoplasty):
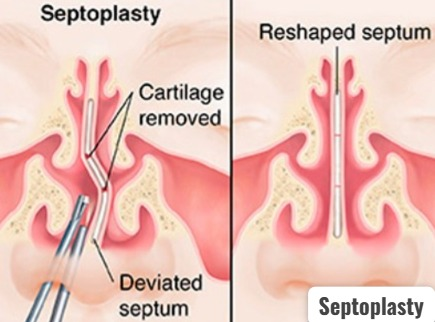
- Septoplasty is a surgical procedure in which a deviated septum, cartilage, and bone are reshaped and repositioned. So that nasal airflow can be improved and breathing difficulties can be eliminated.
Rhinoplasty (Rhinoplasty):
Rhinoplasty is a cosmetic surgery that involves reshaping and resizing the nose, i.e., reconstruction of the nose. So that the appearance of the nose can be improved and breathing issues can be solved.
MANAGEMENT OF PATIENT WITH DISORDERS OF THE CHEST AND LOWER RESPIRSTORY TRACK (Management of Patient with Disorder of Chest and Lower Respiratory Track):
Define lung abscess:
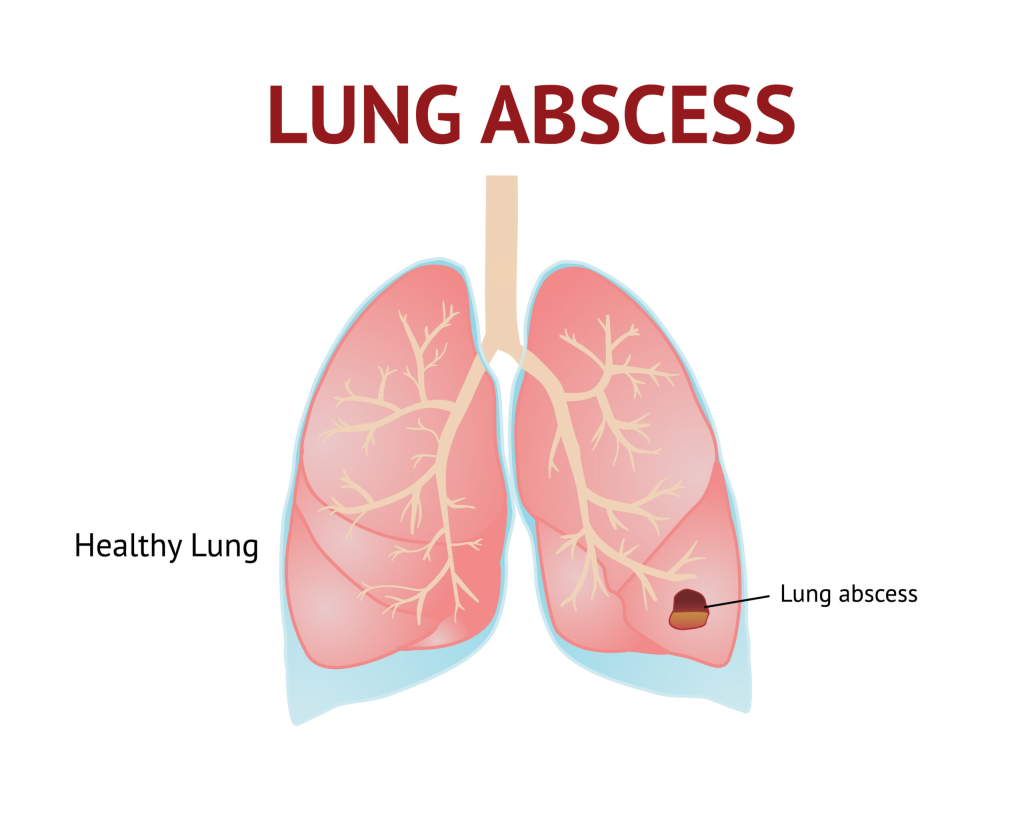
- In lung abscess, a pus-filled cavity is seen in the lung parenchyma and inflammation is seen in the surrounding tissue and necrosis is seen in it.
OR
- Lung Abscess is a Localized Collection of Pus in the Lung Tissue. Which is caused by Tissue Destruction and Necrosis due to Infection.
- This is usually caused by Bacterial Infection or Aspiration of Oropharyngeal Contents.
Write causes of lung abscess:
- Bacterial Infection: Lung abscess is most often caused by bacterial infection. Streptococcus pneumoniae, Klebsiella pneumoniae, Staphylococcus aureus are found to be caused by bacteria.
- Foreign body inhalation
- Foreign body aspiration
- Trauma
- Tuberculosis
- COPD
- Chronic Lung Disease
Write clinical manifestations of lung abscess:
- Persistent cough
- Blood in sputum
- Foul smelling in Sputum
- Chest Pain
- Dypsonia
- Shortness of Breath
- Fever
- Chills
- Weakness
- Diapharesis
- Cyanosis
Write diagnostic evaluation of lung abscess:
- History Collection
- Physical Examination
- X-ray
- CT scan
- M. R. I
- Sputum culture
- Complete blood count
- C-reactive protein
- Erythrocyte sedimentation rate
- Biopsy
Write management of lung abscess:
Antibiotic therapy:
- Use broad-spectrum antibiotics (amoxicillin, clindamycin) to treat bacterial infections.
Oxygen Therapy:
- Provide supplemental oxygen if needed.
Percutaneous Drainage:
- If the abscess is large and antibiotics fail to treat it Drainage is necessary. Percutaneous drainage should be performed under CT scan.
Supportive Care :
- Supportive care includes pain management, oxygen therapy, hydration levels, etc.
Treat Underline Condition :
- Treating the underlined condition associated with lung abscess.
Surgery:
- Performing pulmonary resection (lobectomy) in severe cases.
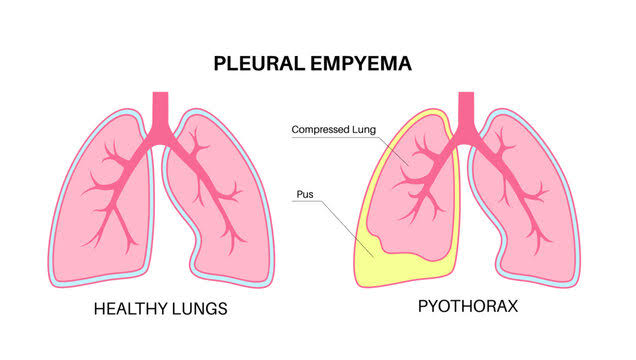
Define Empyema:

- Abnormal pus collection seen in pleural cavity is known as Empyema. Empyema is also known as ‘Pyothorax’ and ‘Purulent Pleuritis’ .
- Empyema is mainly seen as a complication of pneumonia and lung abscess.
Stage of Empyema empyema):

i) Exudative stage :
- The exudative stage is the early stage of empyema. In which sterile serous fluid accumulates in the pleural space.
ii) Fibropurulent stage:
- In this stage, the pleural fluid becomes purulent (pus-like) and the fibrous septa form pockets with localized pus.
iii) Organizing stage:
- This is the last stage of empyema. In which fibrin and pus organize in the pleural space and form a thick pleural pellicle.
Write causes of empyema
- Bacterial Infection (Streptococcus pneumoniae)
- Viral Infection
- Fungal Infection
- Pneumonia
- Tuberculosis
- Lung Abscess
- Trauma
- Chest wound
- Chest surgery
Risk factor:
- Smoking
- Alcoholism
- Immunosuppression
Write clinical manifestations of Empyema
- Shortness of breath
- Chest Tightness
- Chest pain
- Persistent cough
- Fever
- Chills
- Weakness
- Fatigue
- Night Sweat
- Anorexia
- Weight Loss
Write diagnostic evaluation of Empyema
- History Collection
- Physical Examination
- X-ray
- CT Scan
- Ultra Sound
- Sputum Analysis
- Thoracocentesis
- Blood Test
Write management of Empyema
Antibiotics :
- Provide antibiotics to treat bacterial infections.
Pain relievers:
- Provide analgesic drugs to relieve pain.
Antipyretic:
- Provide antipyretic drugs to reduce fever.
Mucolytics:
- Provide mucolytic drugs to break up and clear mucus.
Thoracocentesis :
- Thoracocentesis involves inserting a needle directly into the pleural cavity to aspirate pus or fluid.
Chest Tube Drainage :
- In chest tube drainage, a chest tube (thoracostomy tube) is placed in the pleural space and the pus present there is drained.
Fibrinolytic therapy:
- In cases of fibropurulent empyema, a fibrinolytic agent such as plasminogen activator is instilled into the pleural space. Which breaks down fibrin and helps in drainage.
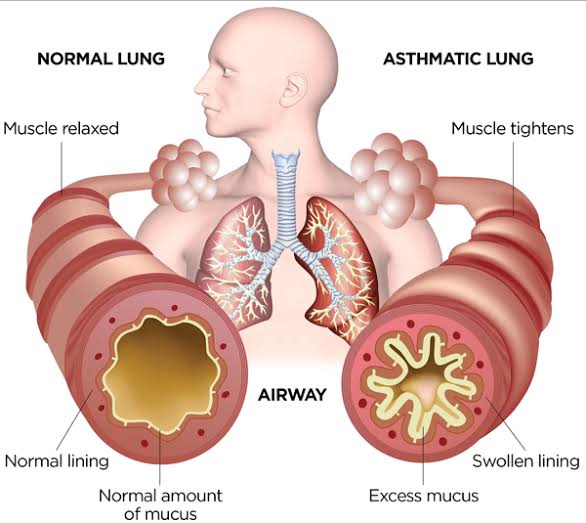
Bronchial asthma :

- Asthma is a chronic inflammatory respiratory disease. It is a disorder in which the airways become hyperresponsive to certain stimuli, causing them to become inflamed and narrowed, and airway obstruction due to mucus production.
- Asthma differs from COPD in that it is a reversible process.
Write causes of asthma
- Genetic factors
- Family history
- Respiratory infections
- Environmental factors : Exposure to allergens, air pollutants (Dust, Chemical)
- Occupational Factor
- Chronic Smoking
Explain pathophysiology of asthma:
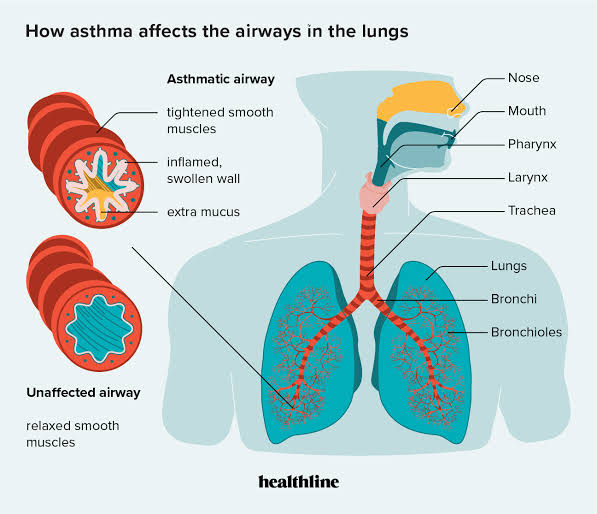
Due to etiological factors
|
Airway hyperresponsiveness occurs.
|
This causes inflammation in the airways.
|
Which causes hypersecretion of mucus, contraction of airway muscles and swelling of bronchial membranes.
|
Which causes airway narrowing
|
Which causes cough, chest tightness, shortness of breath and wheezing sound.
Write diagnostic evaluation of asthma:
- History collection
- Physical examination
- Pulmonary Function Test
- Spirometer
- Peak Expiratory Flow Measurement
- Fractional Exhaled Nitric Oxide Test
- Pulse Oximetry
- Chest X-ray
- CT Scan
- Sputum Analysis
- Blood Test
- Complete Blood Count
- ABGs Analysis
- Allergy Testing
Write medical management of asthma:
Controller medication:
- Controller medication is used to control symptoms.
Inhaled corticosteroids:
- These medications are most effective for long-term control of asthma. They reduce airway inflammation and decrease mucus production. Examples include budesonide, beclomethasone. In addition, long-acting beta agonists are also inhaled along with it.
Long-acting beta agonists:
- These bronchodilators drugs are used to dilate the bronchi. For example salmeterol
Leukotriene modifiers:
- Leukotriene modifiers block the action of leukotrienes, which are inflammatory molecules in asthma. This reduces airway inflammation and prevents symptoms. For example, Montelukast.
Mast cell stabilizers:
- Mast cell stabilizers inhibit the inflammatory chemicals released from mast cells in the airways, thereby relieving asthma symptoms. For example, Nedocromil
Biological therapy :
- Biological medications are used in cases of severe asthma. For example, monoclonal antibodies targeting IgE Quick relief medications :
- Quick relief medications are used to quickly relieve symptoms. In which short-acting beta agonists and oral corticosteroid drugs are used.
Short-acting beta agonists:
- Short-acting beta agonists are used to quickly relieve the condition of bronchospasm and improve airflow during an asthma attack. For example salbutamol and levalbuterol
Oral corticosteroids:
- In severe conditions, oral corticosteroids such as prednisolone, methylprednisolone are given to quickly reduce airway inflammation.
Spacer Device :
- This device is used with a metered dose inhaler. So that the medicine delivered to the lungs can be improved.
Write nursing management of asthma
Impaired gas exchange related to altered oxygen supply, obstruction of airway
Improve Gas Exchange (Improve Gas Exchange):
- Monitor vital signs.
- Assess respiratory rate, rhythm, and breathing pattern.
- Assess breath sounds and chest movement.
- Monitor pulse oximetry and arterial blood gas values.
- Provide the patient with a Fowler position and monitor his/her activity. Restrict.
- Explain and encourage the patient about deep breathing and cuffing exercises.
- Provide the patient with knowledge about pursed lip breathing and diaphragmatic breathing.
- Encourage the patient to expectorate phlegm if secretions are present.
- Provide oxygen therapy if the SpO2 level is low.
- Provide nebulization to the patient.
- Administer the medicine (bronchodilator) prescribed by the doctor.
- Maintain records and reports.
Ineffective airway clearance related to obstruction from narrowed lumen Maintain a patent airway
Maintaining a patent airway:
- Monitor vital signs.
- Assess respiratory rate, rhythm, and breathing pattern.
- Assess breath sounds and chest movement.
- Monitor pulse oximetry and arterial blood gas values.
- Provide the patient with a Fowler position and restrict his/her activity.
- Explain and encourage the patient about deep breathing and cuffing exercises.
- Provide the patient with knowledge about pursed lip breathing and diaphragmatic breathing.
- Encourage the patient to expectorate phlegm if secretions are present.
- If the SpO2 level is low, provide oxygen therapy.
- Provide nebulization to the patient.
- Administer the medicine (bronchodilator) prescribed by the doctor.
- Maintain records and reports.
Ineffective breathing pattern related to bronchospasm
Improving breathing patterns
- Monitor vital signs.
- Assess respiratory rate, rhythm, and breathing patterns.
- Assess breath sounds and chest movement.
- Assess breath sounds and chest movement.
- Monitor pulse oximetry and arterial blood gas values.
- Provide the patient with a Fowler position and restrict his/her activity.
- Explain and encourage the patient to do deep breathing and cuffing exercises.
- Provide the patient with knowledge about pursed lip breathing and diaphragmatic breathing.
- If secretions are present Encourage the patient to expectorate.
- Provide oxygen therapy if the SpO2 level is low.
- Provide nebulization to the patient.
- Administer the medicine (bronchodilator) prescribed by the doctor.
- Maintain records and reports.
Anxiety related to disease condition, hospitalization
Reduce Anxiety
- Assess the patient’s condition.
- Pay attention to the patient’s psychological needs and listen carefully to the patient.
- Encourage the patient to express his/her feelings, discomfort and anxiety.
- Solve all the doubts and queries of the patient.
- Provide the patient with knowledge about his/her condition and treatment so that his/her anxiety is removed and the patient becomes confident.
- Provide psychological support to the patient.
- Provide the patient with mind diversionary therapy and recreational therapy To do.
Activity intolerance related to fatigue, dyspnea
Enhanced activity level
- Assess the patient’s condition.
- Check the patient’s activity level.
- Provide bed rest to the patient initially.
- Then gradually encourage the patient to do range of motion exercises.
- Assist the patient with his/her activities.
- Provide the patient with rest between 2 activities.
- Check whether the patient has any breathing difficulty during the activity.
- If breathing difficulty is observed, stop the patient’s activity and provide rest.
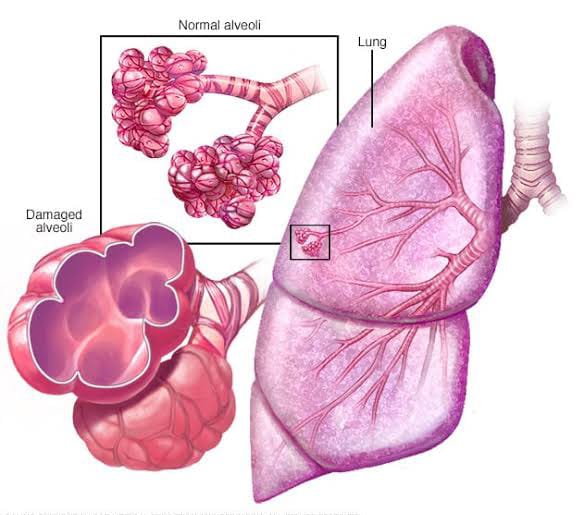
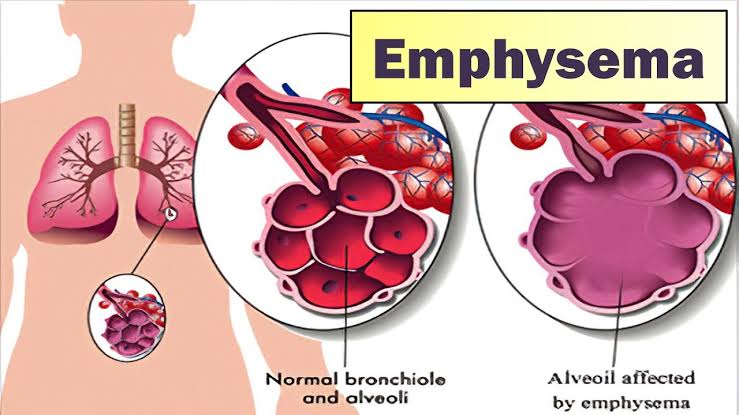
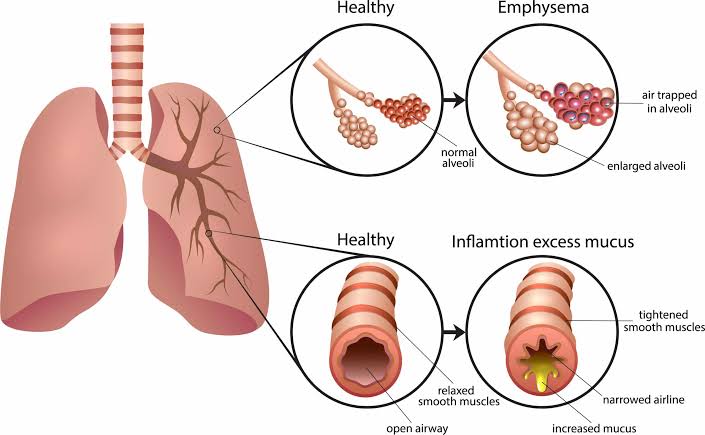
Define Emphysema:
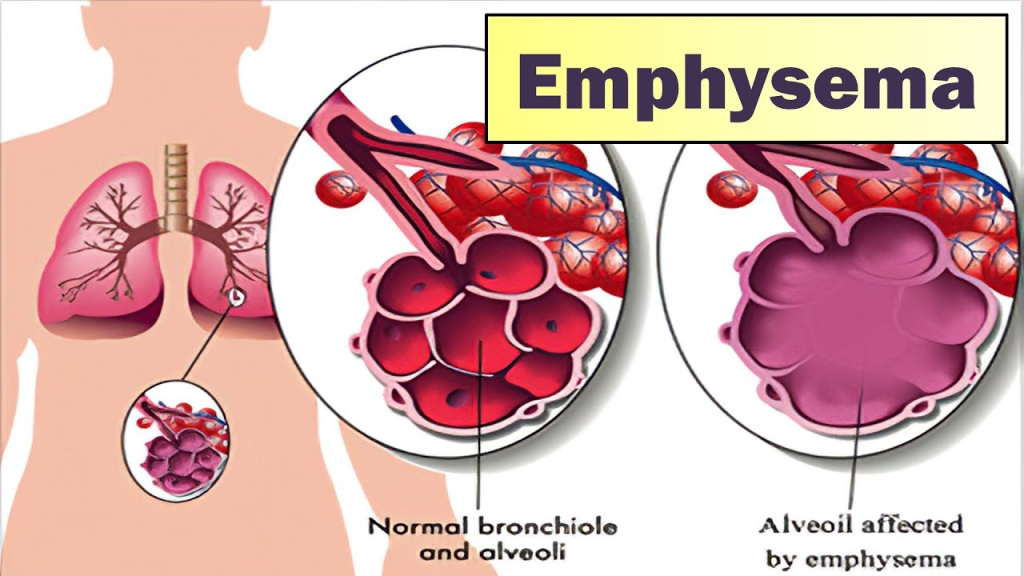
- Emphysema is a Greek word meaning ‘Inflation’ .
- Emphysema is a chronic lung disease. In which overdistension and overinflation are seen in the air sacs (alveoli) of the terminal bronchioles in the lungs and the air sacs are gradually damaged.Due to which shortness of breath is seen.
- Emphysema is also known as ‘Pink Puffer’.

Write causes of emphysema:
- Tobacco Smoke
- Secondhand Smoker
- Air Pollution
- Exposure to Dust, Chemicals, Fumes
- Alpha One Antitrypsin Deficiency
- Genetic Factors
Explain pathophysiology of emphysema
Due to etiological factors
|
Hyperinflation is observed in the alveoli.
|
Due to which destruction is observed in the wall of the alveoli capillary.
|
This causes the elasticity of the alveoli to be lost, in addition to this, the gas exchange capacity of the alveoli is lost.
|
In the alveoli Air trapping occurs.
|
The condition of emphysema is seen.
Write sign & symptoms seen in emphysema:
- Shortness of breath
- Chronic cough
- Wheezing sound
- Chest tightness
- Barrel chest
- Decrease exercise tolerance
- Hypoxia
- Hypercapnia
- Cyanosis
- Frequent respiratory infections
- Fatigue
- Diaphragm
- Weight loss
Write diagnostic evaluation of emphysema
- History Collection
- Physical Examination
- Pulmonary Function Test
- X-ray
- CT scan
- MRI
- Alpha antitrypsin test
- Electrocardiogram
- Complete blood count
- Exercise tolerance test
Write medical management of emphysema
Bronchodilators:
- Provide bronchodilators to relieve bronchial spasm and relax the muscles around the airways. Bronchodilators relax the muscles around the airways and relieve spasms.
Inhaled corticosteroids:
- Inhaled corticosteroid drugs to reduce airway inflammation.
Mucolytics :
- Provide mucolytics drugs to thin mucus and clear it from the lungs.
Antibiotics :
- Provide antibiotic drugs to prevent bacterial infections To do.
Oxygen therapy :
- Provide supplemental oxygen to improve blood oxygen levels.
Write surgical management of emphysema:
Bullectomy :
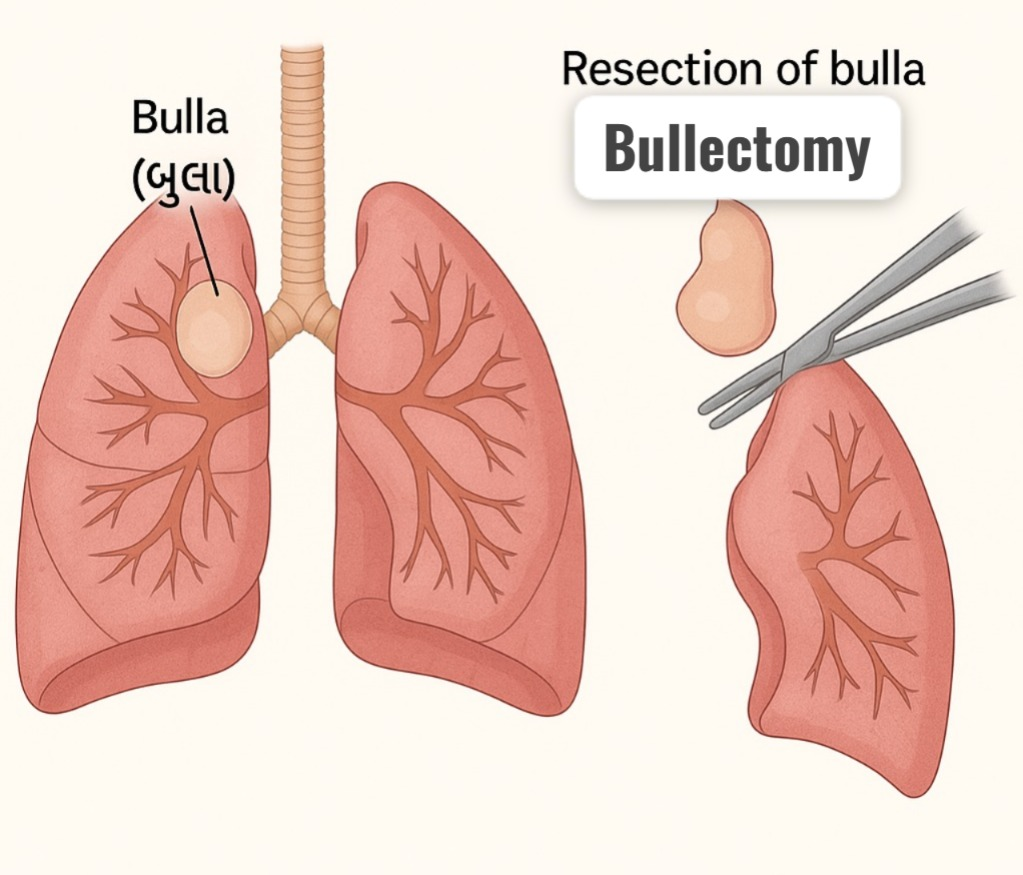
- Bullectomy involves removing the affected bulla (air field space). So that the compression on healthy lung tissue can be removed.
Lung volume reduction surgery (LVRS/Lung volume reduction surgery) :
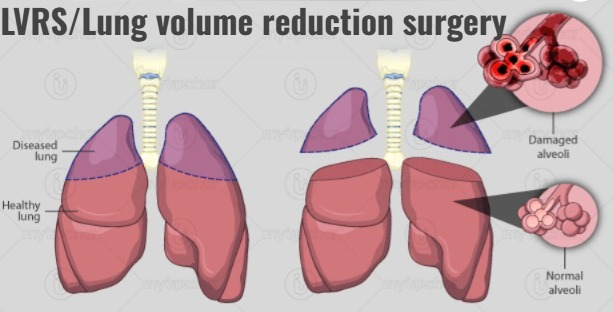
- Damaged lung porson is removed in LVRS. So that the patient can function well in the lung.
Lung transplantation :

- In more severe cases where lung function is significantly compromised, lung transplantation is the treatment. In which lungs provided by a donor are replaced with the affected lungs.
Write nursing management of emphysema
- Monitor vital signs.
- Assess respiratory rate, rhythm, and breathing pattern.
- Assess breath sounds and chest movement To do.
- Monitor pulse oximetry and arterial blood gas values.
- Provide the patient with a Fowler position and restrict his/her activity.
- Explain and encourage the patient about deep breathing and cuffing exercises.
- Provide the patient with knowledge about pursed lip breathing and diaphragmatic breathing.
- If secretions are present, encourage the patient to expectorate.
- If SpO2 levels are low, provide oxygen therapy.
- Provide nebulization to the patient.
- Administer the medicine (bronchodilator) prescribed by the doctor.
- Maintain records and reports.
Write complications of emphysema
- Chronic obstructive pulmonary disease
- Pneumonia
- Pneumothorax
- Atelektasis
- Recurrent respiratory tract infection
- Respiratory failure
- Respiratory acidosis
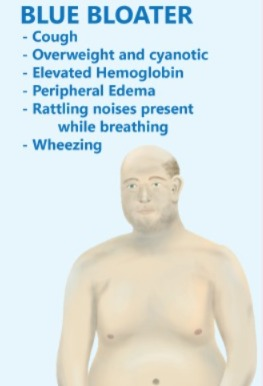
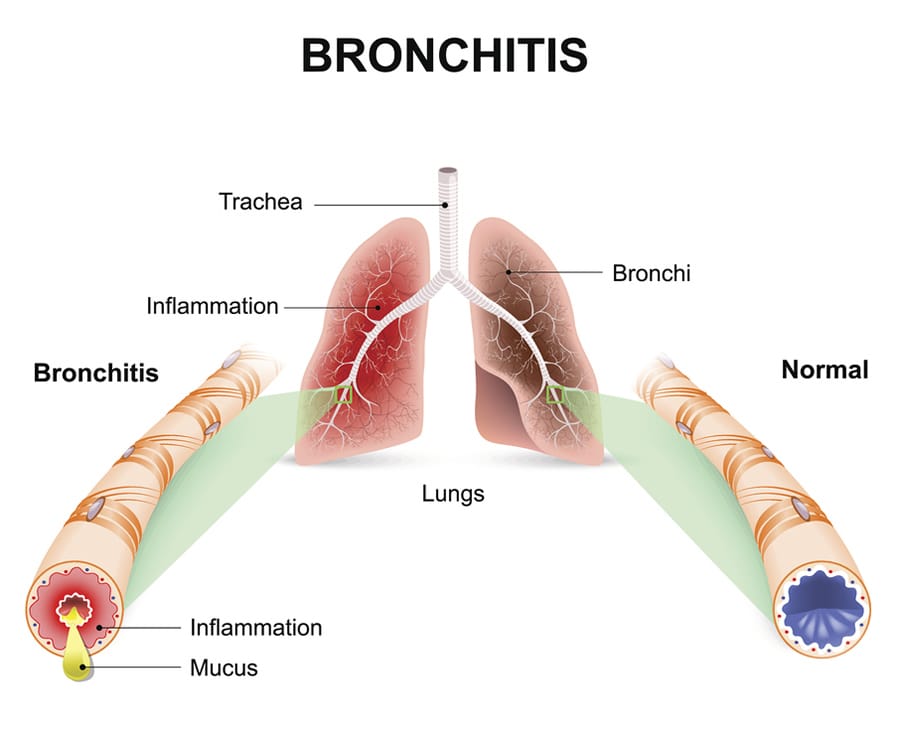
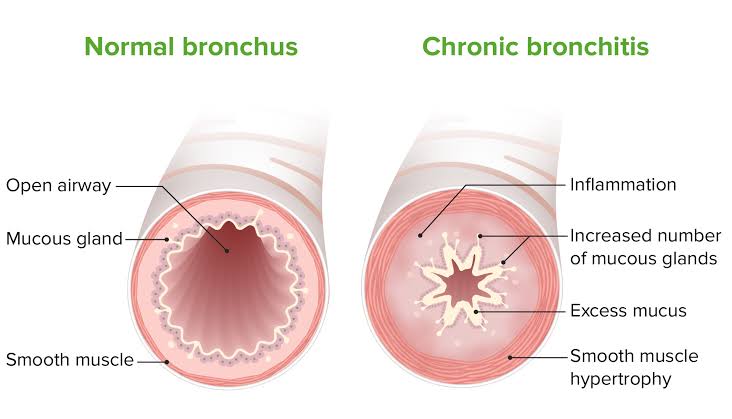
Define bronchitis:

- Inflammation of the bronchi and bronchioles tubes is known as bronchitis. Bronchitis is also known as ‘Blue Bloater’.
Write causes of bronchitis:
- Viruses: Rhinovirus, Influenza Virus, Parainfluenza Virus
- Bacteria: Mycoplasma pneumoniae, Bordetella Pertussis
- Smoking
- Air pollution
- Exposure to chemical fumes
- Contact to allergens
- Weak immune system
Explain pathophysiology of bronchitis
Due to etiological factors
|
Hyperplasia is seen in the mucus glands.
|
Due to which there is an increase in goblet cells and an increase in mucus production.
|
The function of cilia occurs
|
Due to which the bronchial lumen becomes narrow and limitation in air flow is seen.
|
The condition of bronchitis is seen.
Write clinical manifestations of bronchitis
- Shortness of breath
- Runny and stuffy nose
- Chest congestion
- Wheezing sound
- Yellow or green mucus production
- Chest tightness
- Diaphragm
- Low grade fever
- Fatigue
- Clubing
Write diagnostic evaluation of bronchitis:
- History collection
- Physical examination
- X-ray
- CT scan
- Sputum culture
- Blood test
Write management of bronchitis
Broncho dilators :
- Provide bronchodilators drugs to relax respiratory muscles and dilate bronchi.
Antibiotics:
- Provide antibiotic drugs to treat bacterial infections.
Cough Expectorant :
- Provide a cough expectorant drug to help expel phlegm.
Nasal Decongestant :
- Provide nasal decongestants to relieve congestion.
Rest and Hydration:
- Get adequate rest and plenty of fluid intake.
Avoid irritants :
- Avoid contact with irritants.
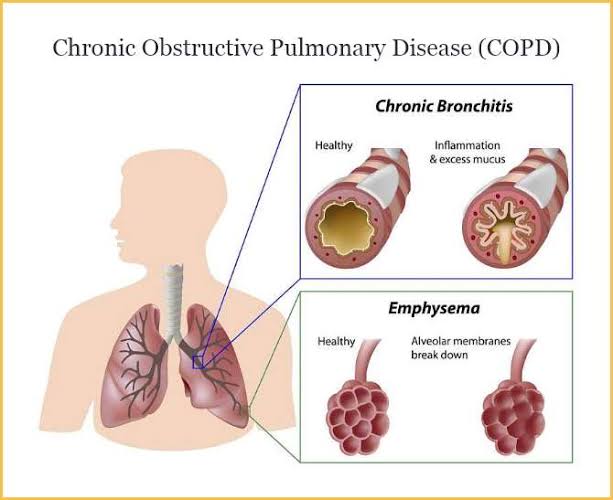
Define chronic obstructive pulmonary disease (Define Chronic Obstructive Pulmonary Disease):
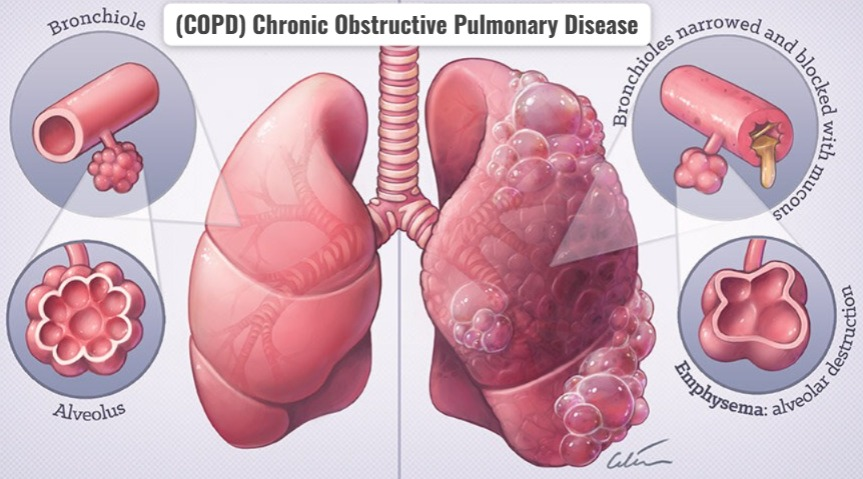
- Chronic Obstructive Pulmonary Disease (COPD) is a Respiratory disease. In which airflow is obstructed due to chronic bronchitis and emphysema.
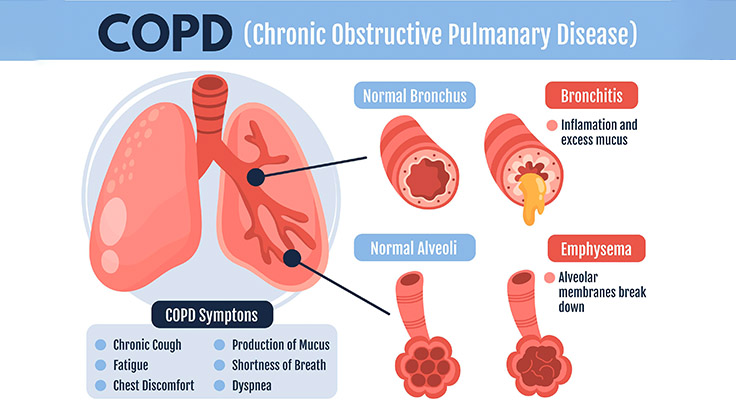
Write causes of chronic obstructive pulmonary disease
- Smoking
- Second-hand smoker
- Environmental factors
- Occupational Factor
- Genetic Factor (Deficiency of Alpha One Antitypsin)
- Exposure to Pollutants
Write clinical manifestations of chronic obstructive pulmonary disease
- Chronic cough
- Shortness of breath
- Wheezing
- Chest Tightness
- Chest pain
- Barrel chest
- Excessive mucus production
- Frequent respiratory infections
- Cyanosis
- Clubing
- Fatigue
- Weight Loss
Write diagnostic evaluation of chronic obstructive pulmonary disease
- History Collection
- Physical Examination
- X-ray
- CT Scan
- Spirometry
- Pulmonary Function Test
- Arterial Blood Gas Analysis
- Sputum Analysis
- Blood Test
- The most important intervention for the management of COPD is to stop smoking. Which slows the progression of the disease and reduces its frequency and severity.
- To relax the muscles around the airways and increase airflow Use short-acting bronchodilators (albuterol) and long-acting bronchodilators (salmeterol) to improve.
- Give inhaled corticosteroids to reduce airway inflammation. For example budesonide, fluticasone
- Use of phosphodiesterase 4 inhibitors in patients with severe COPD and chronic bronchitis. Which reduces inflammation and prevents exacerbations.
Write management of chronic obstructive pulmonary disease
Smoking Cessation :

Medication:
Bronchodilators:
Inhaled corticosteroids:
Phosphodiesterase 4 inhibitors:
Mucolytic drug:
- Using mucolytic drugs to thin mucus and clear it from the airways.
Pulmonary Rehabilitation:
- This comprehensive program includes exercise training, education, nutritional, and psychological support. So that the quality of life can be improved.
Oxygen therapy:
- Provide supplemental oxygen to improve oxygen levels.
Lifestyle modification:
- Lifestyle modification should include regular exercise, a healthy diet, avoiding environmental pollutants and respiratory irritants.
Write nursing management of chronic obstructive pulmonary disease
Impaired gas exchange related to pulmonary obstruction as evidenced by hypoxia, hypercapnia, cynosis, abnormal ABG
Improve gas exchange
- Monitor vital signs.
- Assess respiratory rate, rhythm, and breathing pattern.
- Breath Assess sound and chest movement.
- Monitor pulse oximetry and arterial blood gas values.
- Provide the patient with a Fowler position and restrict his/her activity.
- Explain and encourage the patient to do deep breathing and cuffing exercises.
- Provide the patient with knowledge about pursed lip breathing and diaphragmatic breathing.
- If secretions are present, encourage the patient to expectorate.
- If SpO2 levels are low, provide oxygen therapy.
- Provide nebulization to the patient.
- Administer the medicine (bronchodilator) prescribed by the doctor.
- Maintain records and reports.
Ineffective airway clearance related to bronchoconstriction, increased mucus production
Maintain a patent airway
- Monitor vital signs.
- Assess respiratory rate, rhythm, and breathing pattern.
- Assess breath sounds and chest movement.
- Monitor pulse oximetry and arterial blood gas values.
- Provide the patient with a Fowler position and restrict their activity. To do.
- Explain and encourage the patient about deep breathing and cuffing exercises.
- Provide the patient with knowledge about pursed lip breathing and diaphragmatic breathing.
- Encourage the patient to expectorate phlegm if secretions are present.
- Provide oxygen therapy if the SpO2 level is low.
- Provide nebulization to the patient.
- Administer the medicine (bronchodilator) prescribed by the doctor.
- Maintain records and reports.
Ineffective breathing patterns related to shortness of breath, mucous production
- Monitor vital signs.
- Assess respiratory rate, rhythm, and breathing pattern.
- Assess breath sounds and chest movement.
- Monitor pulse oximetry and arterial blood gas values.
- Provide the patient with a Fowler position and restrict their activity. To do.
- Explain and encourage the patient about deep breathing and cuffing exercises.
- Provide the patient with knowledge about pursed lip breathing and diaphragmatic breathing.
- Encourage the patient to expectorate phlegm if secretions are present.
- Provide oxygen therapy if the SpO2 level is low.
- Provide nebulization to the patient.
- Administer the medicine (bronchodilator) prescribed by the doctor.
- Maintain records and reports.
Ineffective breathing patterns related to shortness of breath, mucous production
Improve breathing patterns (Improving breathing patterns)
- Monitor vital signs.
- Assess respiratory rate, rhythm, and breathing pattern.
- Assess breath sounds and chest movement.
- Monitor pulse oximetry and arterial blood gas values.
- Provide the patient with a Fowler position and restrict his/her activity.
- Explain and encourage the patient about deep breathing and cuffing exercises.
- Provide the patient with knowledge about pursed lip breathing and diaphragmatic breathing.
- Encourage the patient to expectorate phlegm if secretions are present.
- If the SpO2 level is low So provide oxygen therapy.
- Provide nebulization to the patient.
- Administer the medicine (bronchodilator) prescribed by the doctor.
- Maintain records and reports.
Knowledge deficit related to disease condition and it’s prognosis
Improve Knowledge Level
- Assess the patient’s condition.
- Assess the patient’s knowledge of the disease condition and its treatment.
- Provide the patient with knowledge about the disease condition and its prognosis.
- In a way that the patient can understand Providing knowledge in language.
- To resolve patient doubts and concerns.
Anxiety related to disease condition, hospitilisation
Reduce anxiety
- Assess the patient’s condition.
- Pay attention to the patient’s psychological needs and listen carefully to the patient.
- Encourage the patient to express his feelings, discomfort and anxiety.
- Resolve all the patient’s doubts and queries.
- Educate the patient about his condition and Provide knowledge about the treatment so that his anxiety is removed and the patient becomes confident.
- Provide psychological support to the patient.
- Provide mind diversionary therapy and recreational therapy to the patient.
Activity intolerance related to fatigue, dyspnea
Enhance activity level
- Assess the patient’s condition.
- Check the patient’s activity level.
- Provide bed rest to the patient initially.
- Then gradually encourage the patient to do range of motion exercises.
- Assist the patient with his/her activity.
- Provide rest to the patient between 2 activities.
- Check whether the patient has any breathing difficulty during the activity.
- If breathing difficulty is found, stop the patient’s activity and provide rest.
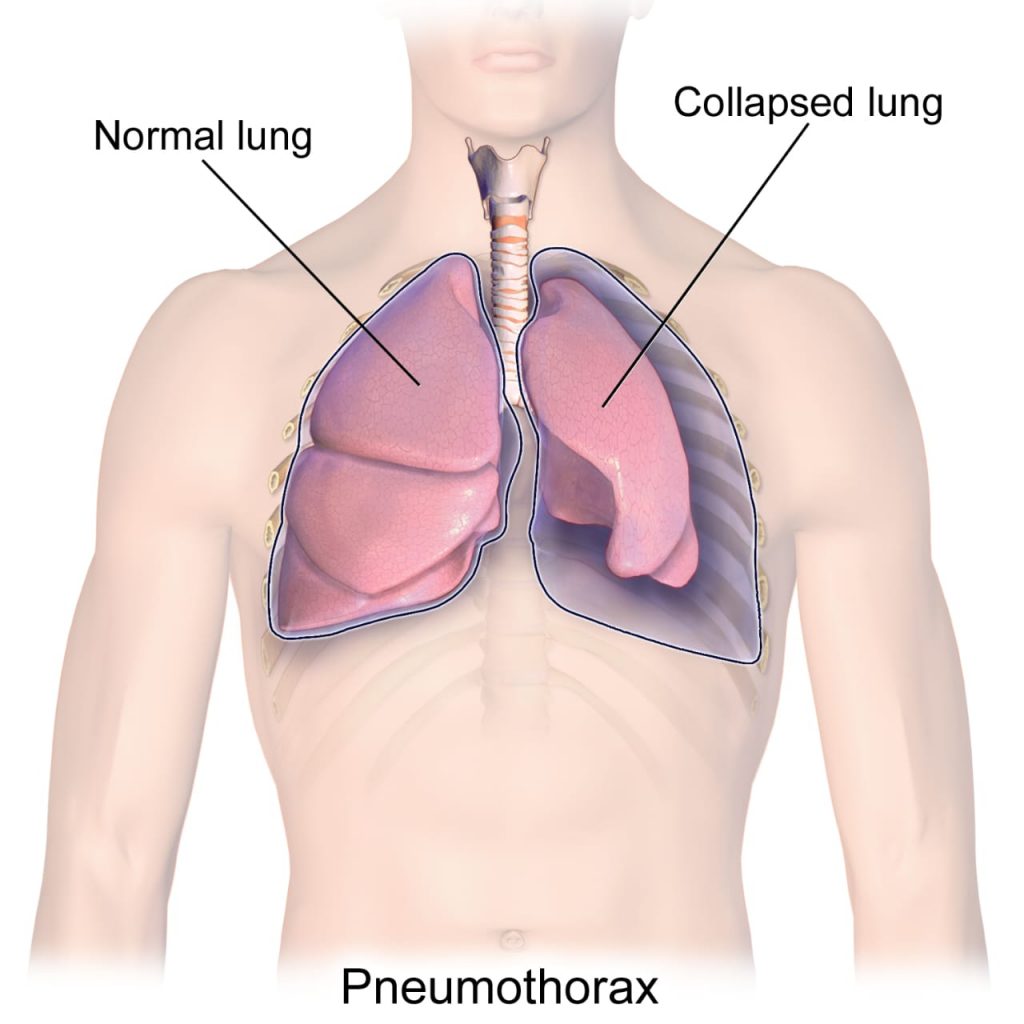
Define Pneumothorax:
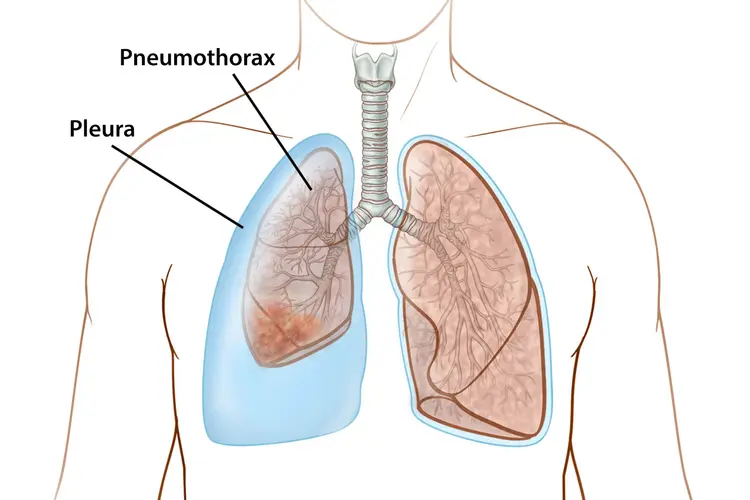
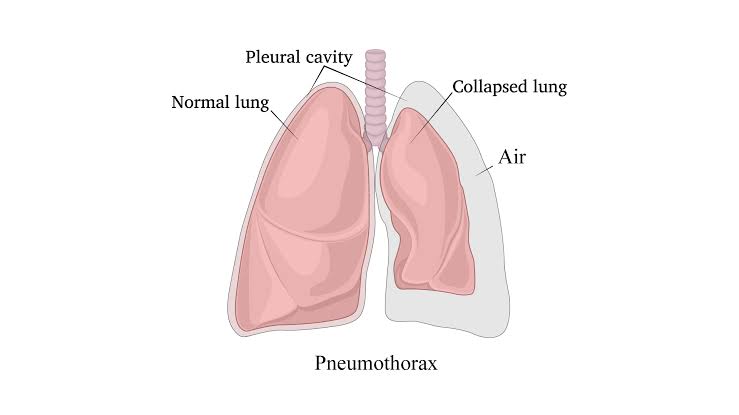
- Pneumothorax is a medical condition. In which air or gas leakage is seen in the pleural cavity, due to which the lung is seen to collapse.
OR
- Pneumothorax means filling the Pleural Cavity – that is, between the Membranes Covering the Lungs (Visceral and Parietal Pleura) – with Air or Gas, due to which Part or Entire Lung Collapse.
- This condition can occur Spontaneous, Traumatic, or as a complication of Disease or Medical Procedure.
Write causes of pneumothorax:
- Chest Trauma (Rib Fracture)
- Lung Disease (COPD, Cystic Fibrosis)
- Medical Procedure
- Spontaneous
Write clinical manifestations of Pneumothorax (Right Clinical Manifestation of Pneumothorax):
- Sudden Sharp Chest Pain
- Shortness of Breath
- Rapid Breathing
- Chest Tightness
- Cyanosis
- Rapid Heart Rate
Write Diagnostic Evaluation of Pneumothorax
- History Collection
- Physical Examination
- Ex Ray
- CT Scan
- Ultrasound
- ABG Analysis
Write management of Pneumothorax:
Needle Insufflation:
- In needle insufflation, a hollow needle attached to a flexible tube (catheter) is inserted into the air field space. is inserted. The needle is then removed and a syringe is attached to the catheter and the air is removed.
Chest tube insertion:
- In chest tube insertion, a flexible chest tube is inserted into the air field space and a one-way valve is attached to it, which continuously removes air from the chest cavity.
Surgery :
- Surgery is required in some cases. In which a small incision is made and all the air is removed.
Define Pneumonia:
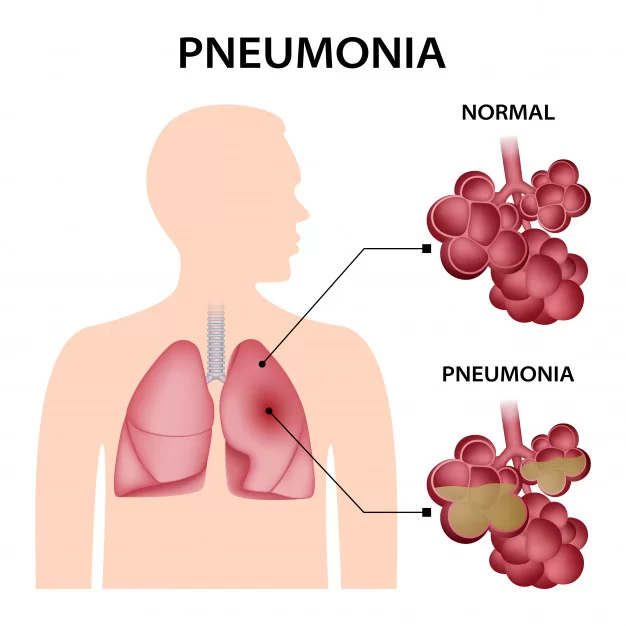
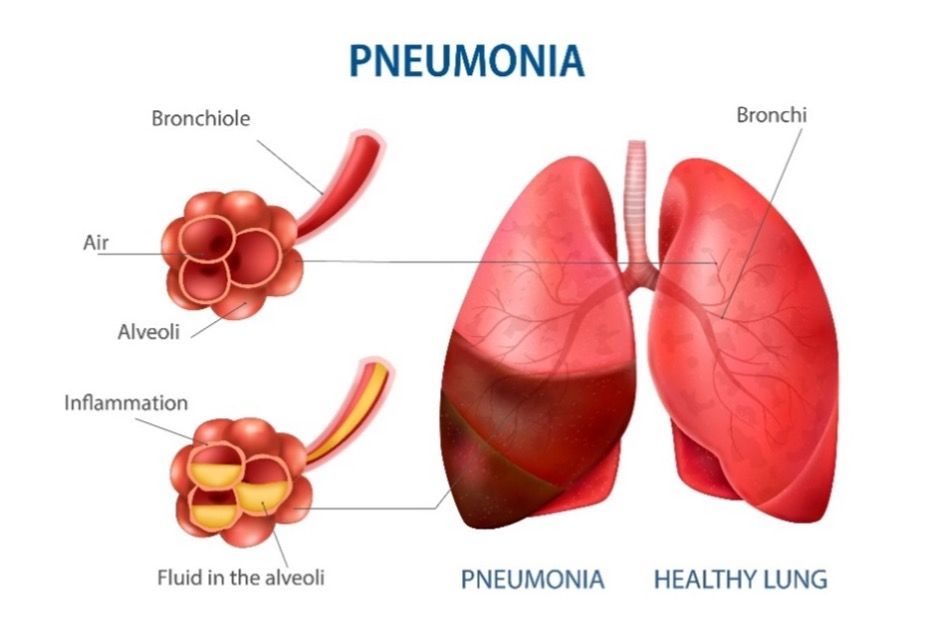
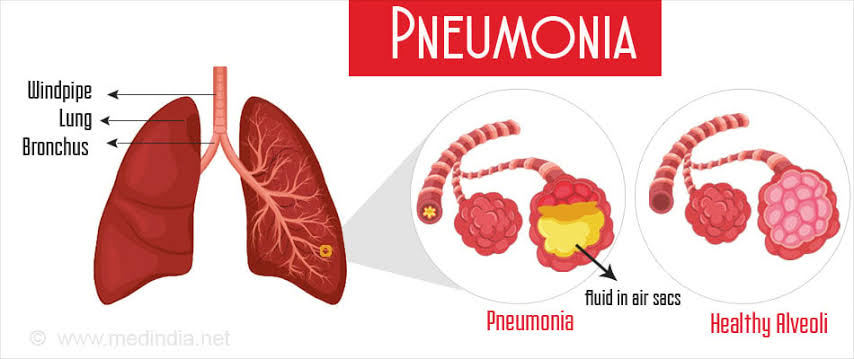
- Inflammation of the lung parenchyma (alveoli) is known as pneumonia, which occurs due to bacterial, viral, or fungal infections. In which the air sac fills with fluid or pus and becomes solid.
Write classification of pneumonia:
Pneumonia is classified on the basis of its cause, anatomical structure and its severity.
On the basis of Etiological factors (On the basis of etiological factor) :

Bacterial Pneumonia :
- Pneumonia caused by bacterial infection is known as bacterial pneumonia. Pneumonia is caused by Streptococcus pneumoniae, Mycoplasma pneumoniae and Haemophilus influenzae bacteria.
Viral Pneumonia:
- Pneumonia caused by a viral infection is known as viral pneumonia. Viruses such as influenza, coronavirus, adenovirus, and respiratory syncytial virus are responsible for causing pneumonia.
Fungal Pneumonia:
- Pneumonia caused by fungal infection is known as fungal pneumonia.
On the Basis of Anatomical Structure:

Pneumonia is classified based on the anatomical structure as follows :
Lobar pneumonia (Lobar pneumonia) :
- Lobar pneumonia is an infection in one or more lobes of the lung.
Broncho pneumonia (Broncho pneumonia) :
- In bronchopneumonia, infection is seen in the bronchi in addition to many lobes.
Interstitial pneumonia (Interstitial pneumonia):
- In interstitial pneumonia, the interstitial tissue and alveolar septa become infected.
On the Basis of Broad Classification:

Community Acquired Pneumonia:
- Pneumonia that occurs in the community is called community acquired pneumonia.
Hospital Acquired Pneumonia:
- Pneumonia that occurs after 48 hours of hospitalization is called hospital acquired pneumonia.
Ventilator Associated Pneumonia:
- Pneumonia that occurs due to endotracheal intubation or mechanical ventilation is called ventilator associated pneumonia.
Aspiration pneumonia :
- Pneumonia caused by aspiration of endogenous or exogenous substances is called aspiration pneumonia.
Write causes of Pneumonia
- Bacterial Infection
- Viral Infection
- Fungal Infection
- Aspiration of Gastric Contents
- Inhalation of Chemical Substances and Fumes
Write clinical manifestations of pneumonia:
- Productive cough (green and yellow color)
- Blood in sputum
- Shortness of breath
- Chest pain
- Cyanosis
- Orthopnea
- Tachypnea
- Fever
- Dehydration
- Malaysia
- Confusion
- Sweating
- Nausea
- Vomiting
- Diarrhea
- Anorexia
Write diagnostic evaluation of pneumonia
- History Collection
- Physical Examination
- Pulmonary Function Test
- X-Ray
- CT Scan
- Sputum Culture
- Complete Blood Count
- C-Reactive Protein
- Blood Culture
- Pulse Oximetry
- Arterial Blood Gas Analysis
Write management of pneumonia :
Antibiotic therapy:
- Providing antibiotic drugs to treat bacterial pneumonia.
Antiviral drugs:
- Give antiviral drugs to treat viral pneumonia.
Fever Management:
- Provide the over-the-counter medicine acetaminophen to reduce fever.
Pain relievers :
- Provide analgesic drugs to reduce chest pain.
Oxygen therapy :
- Provide supplemental oxygen to maintain oxygen levels.
Cough Expectorant :
- Provide a cough expectorant to thin and expel phlegm.
Rest and Fluid :
- Provide adequate rest to the patient. Also maintain hydration levels.
Write Nursing Management of Pneumonia:
Ineffective airway clearance related to broncho constriction and increased mucus production
Maintain a patent airway.
- Monitor vital signs.
- Assess respiratory rate, rhythm, and breathing pattern.
- Assess breath sounds and chest movement.
- Monitor pulse oximetry and arterial blood gas values.
- Provide the patient with a Fowler position and restrict their activity. To do.
- Explain and encourage the patient about deep breathing and cuffing exercises.
- Provide the patient with knowledge about pursed lip breathing and diaphragmatic breathing.
- Encourage the patient to expectorate phlegm if secretions are present.
- Provide oxygen therapy if the SpO2 level is low.
- Provide nebulization to the patient.
- Administer the medicine (bronchodilator) prescribed by the doctor.
- Maintain records and reports.
Impaired gas exchange related to decrease ventilation
Improve gas Exchange
- Monitor vital signs.
- Assess respiratory rate, rhythm, and breathing pattern.
- Assess breath sounds and chest movement.
- Monitor pulse oximetry and arterial blood gas values.
- Assess patient’s Fowler Provide position and restrict activity.
- Explain and encourage the patient to do deep breathing and cuffing exercises.
- Provide knowledge about pursed lip breathing and diaphragmatic breathing to the patient.
- Encourage the patient to expectorate phlegm if secretions are present.
- Provide oxygen therapy if SpO2 levels are low To do.
- Provide nebulization to the patient.
- Administer the medicine (bronchodilator) prescribed by the doctor.
- Maintain records and reports.
Infective breathing pattern related to chest pain
- Monitor vital signs.
- Assess respiratory rate, rhythm, and breathing pattern.
- Assess breath sounds and chest movement.
- Monitor pulse oximetry and arterial blood gas values.
- Provide the patient with a Fowler position and restrict his/her activities.
- Explain and encourage the patient about deep breathing and cuffing exercises.
- Provide the patient with knowledge about pursed lip breathing and diaphragmatic breathing.
- Encourage the patient to expectorate phlegm if secretions are present.
- Provide oxygen therapy if the SpO2 level is low.
- Provide nebulization to the patient.
- Administer the medicine (bronchodilator) prescribed by the doctor.
- Maintain records and reports.
Write complication of pneumonia:
- Respiratory Failure
- Sepsis
- Lung Abscess
- Pleural Effusion
- Atelectasis
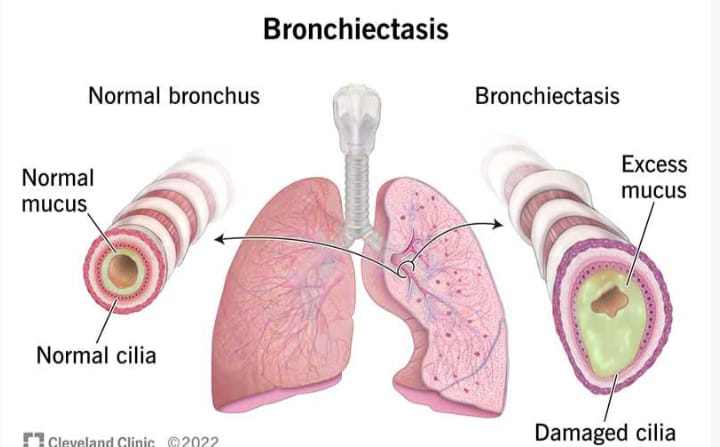
Define Bronchiectasis:

- Bronchiectasis is a chronic respiratory condition characterized by abnormal and irreversible dilation, inflammation, and thickening of the bronchi and bronchioles. As a result, mucus accumulates in it and the mucus is not cleared properly from the airways, which leads to recurrent respiratory infections.
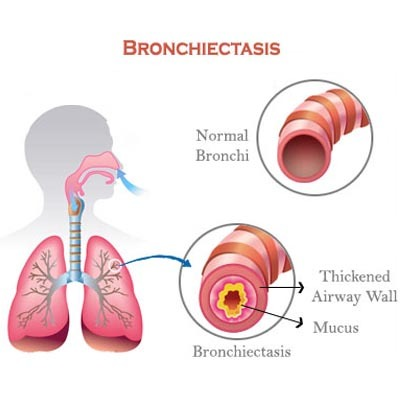
Write causes of bronchiectasis:
- Infection (previous respiratory infection such as pneumonia, tuberculosis)
- Genetic disorder (cystic fibrosis)
- Immune system disorder (rheumatoid arthritis, inflammatory bowel disease)
- Autoimmune condition
- Allergic bronchopulmonary aspergillosis
- Environmental factor
Write clinical manifestations of bronchiectasis:
- Chronic cough
- Excessive sputum production
- Blood in sputum
- Shortness of breath
- Wheezing
- Chest pain
- Recurrent respiratory infection
- Clubbing of finger
- Weight loss
- Fatigue
- Weakness
Write diagnostic evaluation of bronchiectasis (Right Diagnostic Evaluation of Bronchiectasis)
- History Collection
- Physical Examination
- X-ray
- CT Scan
- Pulmonary Function Test
- Sputum culture
- Bronchoscopy
Write medical management of bronchiectasis
Bronchodilators :
- Administer bronchodilators drugs to relax airway muscles and dilate bronchi.
Antibiotics:
- Provide antibiotic drugs to treat bacterial infections.
Expectorant and Mucolytics :
- Provide expectorant and mucolytic drugs to thin and expel mucus.
Airway Clearance Techniques :
- Airway clearance techniques such as chest physiotherapy, postural drainage
Write surgical management of bronchiectasis:
- In severe cases, severely damaged lung tissue is surgically removed.
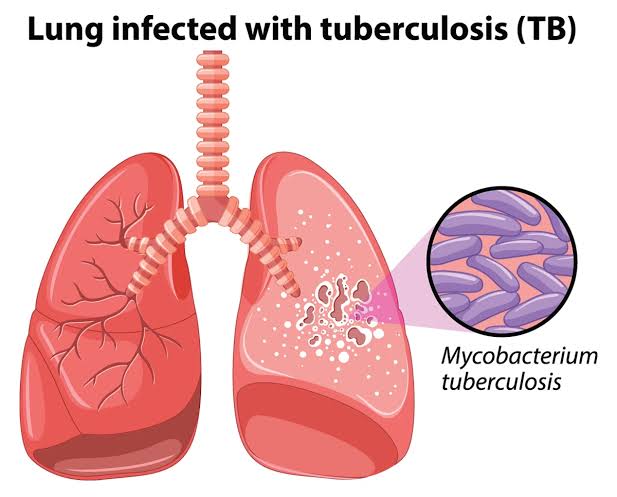
Define pulmonary tuberculosis:
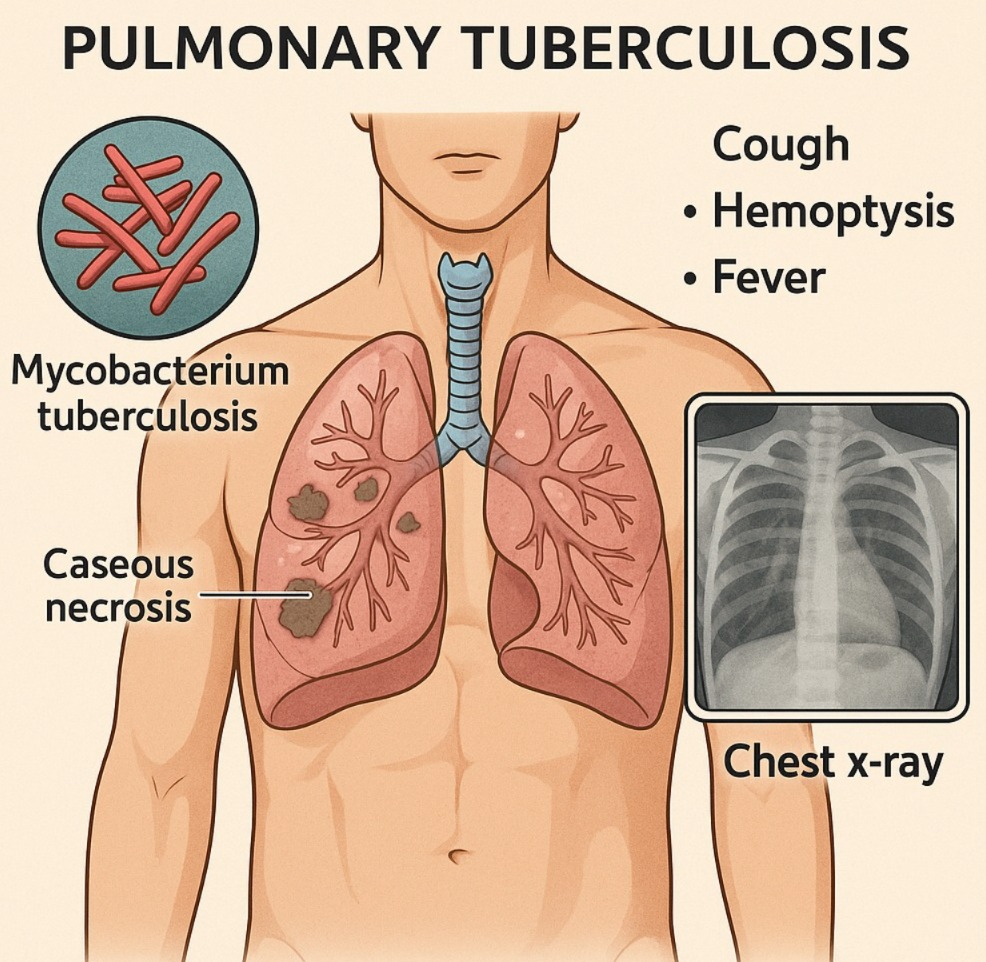
- Pulmonary tuberculosis is a serious infection caused by the bacterium Mycobacterium tuberculosis that mainly affects the lungs but can also spread to other areas of the body. Pulmonary tuberculosis is spread through the air, that is, by coming into contact with an infected person coughing or sneezing.
Write risk factor of pulmonary tuberculosis:
- Close contact with an active tuberculosis patient
- Weak immune system (HIV, Organ transplantation, cancer, corticosteroid therapy)
- Age
- Substance abuse
- Living in overcrowded areas
- Malnutrition
- Chronic health conditions
Write clinical manifestations of pulmonary tuberculosis:
- Persistent cough (coughing for more than three weeks)
- Blood in sputum
- Chest pain
- Fever
- Fatigue
- Night sweats
- Loss of appetite
- Weight loss
- Shortness of breath
Write diagnostic evaluation of pulmonary tuberculosis (Right Diagnostic Evaluation of Pulmonary Tuberculosis):
- History Collection
- Physical Examination
- Tuberculin Skin Test
- X Ray
- Sputum Test
- Blood test
Write management of pulmonary tuberculosis:
Antibiotic therapy:
- Pulmonary Tuberculosis is treated with a combination of antibiotics, including isoniazid, rifampin, ethambutol, and pyrazinamide. This medicine is given for a course of six to nine months.
Directly Observed Treatment Short Course (DOTs):
- In DOTs therapy, TB patients are supervised by a health care provider. The patient takes regular medicine and its effectiveness is observed. So that it can be known whether the patient has completed the full course of treatment or not.
Isolation :
- TB positive patients are isolated. Because TB is a contagious disease and it spreads through the air. Therefore, the patient is isolated to prevent it from spreading.
Nutritional support:
- Provide adequate nutrition to the patient with TB so that his immune system can be improved and weight can be gained.
Education and Counseling:
- Provide education and counseling to the patient about tuberculosis. Explaining infection control measures to the patient and his family members.
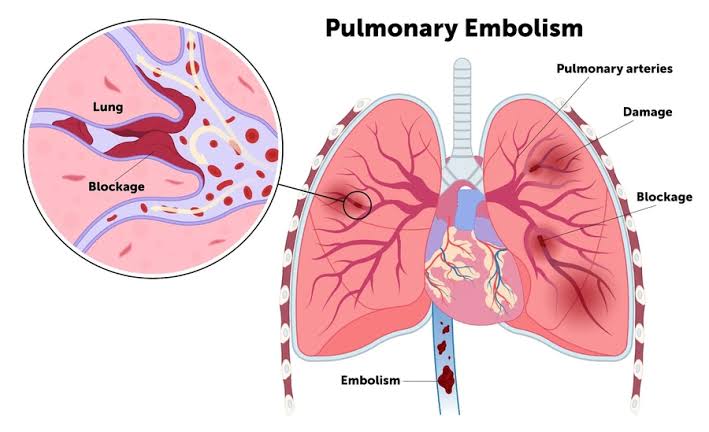
Define pulmonary embolisms:
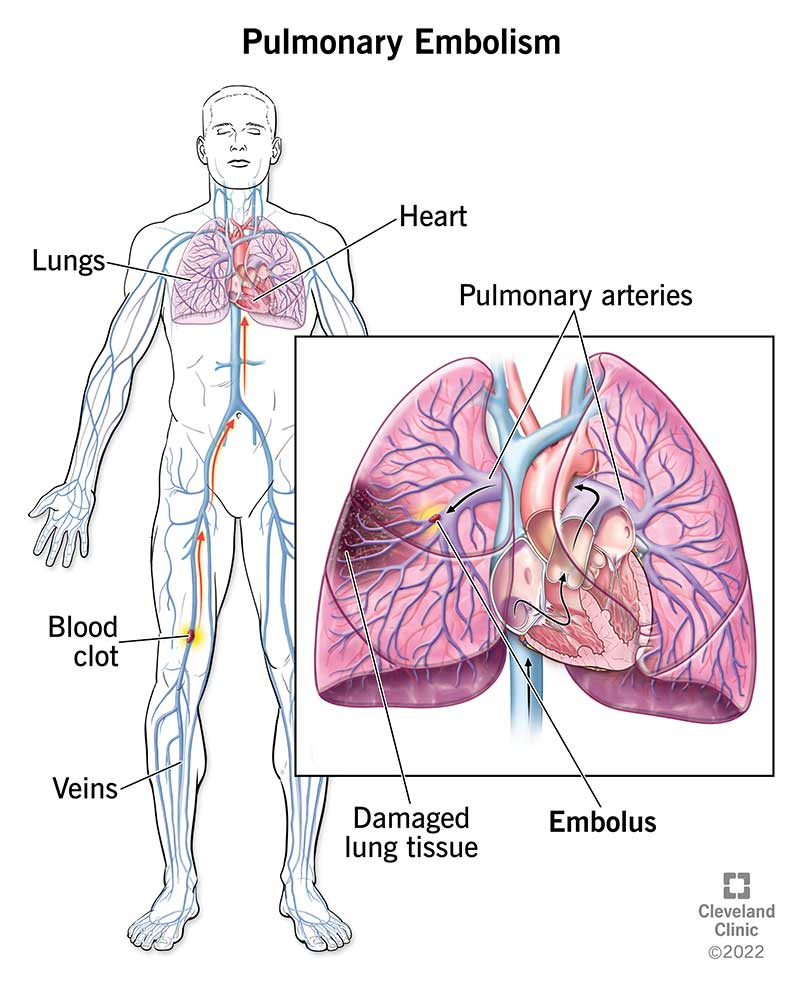
- Pulmonary embolism is a condition in which a blood clot (a blood clot) blocks one or more of the pulmonary arteries. Obstruction and blockage are caused by thrombus (blood clot). This thrombus originates from the vascular system or right heart and travels to the pulmonary artery.
Write cause of pulmonary embolism:
- Deep vein thrombosis
- Hypercoagulation
- Venous Stasis
Risk factor:
- Trauma and Injury
- Surgery
- Prolonged Immobilization
- Heart Failure
- Heart Disease
- Hormonal Factors
- Advance Age
- Obesity
Write sign & symptoms seen in pulmonary embolism:
- Rapid onset of dyspnea
- Shortness of breath
- Pleuritic chest pain
- Tachycardia
- Diapharesis
- Blood in Cough (Hemoptysis)
- Cyanosis
- Fever
- Fanning
- Calf & Pain
Write diagnostic evaluation of pulmonary embolism:
- History Collection
- Physical Examination
- Chest X-ray
- Ultrasound
- Magnetic Resonance Imaging
- Pulmonary Angiography
- Ventilation perfusion scan
- D dimer test
- Electrocardiogram
Write management of pulmonary embolisms:
Anticoagulant therapy :
-
- Providing anticoagulant drugs for the treatment of pulmonary embolism. These prevent the formation of blood clots and help dissolve the clots. Administer heparin, low molecular weight heparin medicine as anticoagulant drug.
Thrombolytic therapy :
-
- Provide thrombolytic therapy to rapidly dissolve clots in life-threatening and emergency conditions. Which breaks down the clot. For example, tissue plasminogen activator (tPA)
Inferior vena cava filter:
-
- Inferior vena cava filters are used when anticoagulant therapy is contraindicated or ineffective. In which an inferior vena cava filter is placed, which prevents the clot in the lower area of the body from traveling to the lungs and getting deposited in the filter there.
Supplemental oxygen:
-
- Provide supplemental oxygen to maintain adequate oxygen levels.
Emblemectomy :
-
- In an embolectomy, the clot (embolism) is surgically removed.
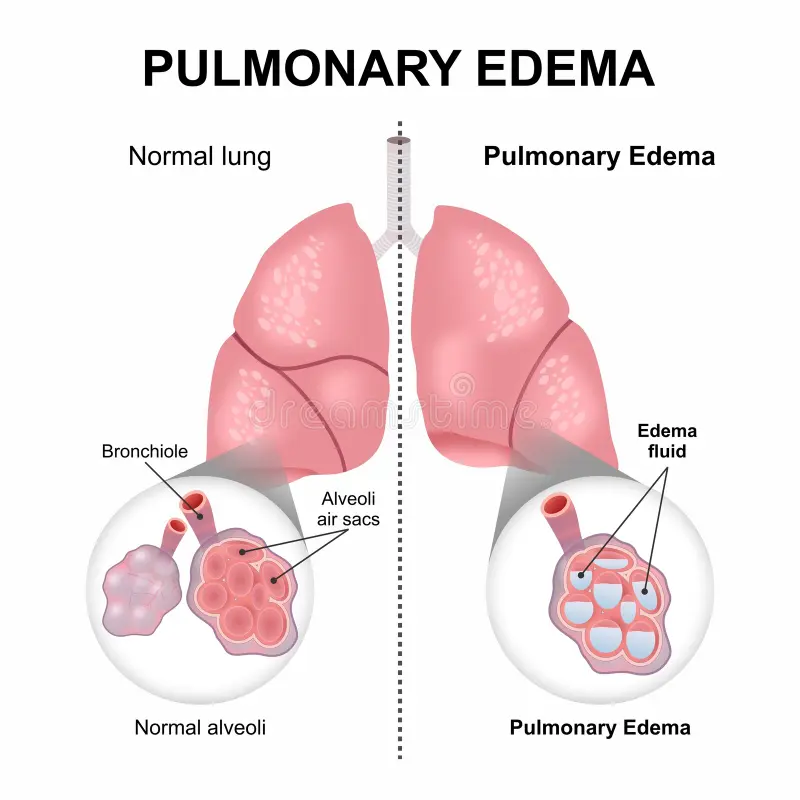
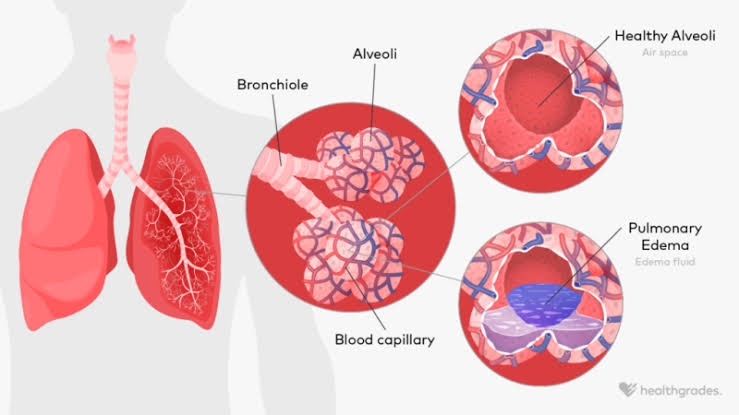
Define pulmonary edema:
-
- Pulmonary edema is a condition in which fluid accumulates or builds up around the lungs and this fluid collects in the air sacs, causing difficulty in breathing.
Write causes of pulmonary edema (right cause of pulmonary edema):
- Congestive Heart Failure
- Renal Failure
- Acute Kidney Injury
- Exposure to Certain Toxins and Drugs
- Heart Disease
- Acute Respiratory Distress Syndrome
- Near drowning
Explain sign & symptoms seen in pulmonary edema (Explain sign and symptoms seen in pulmonary edema):
- Shortness of breath
- Rapid breathing
- Persistent cough and frothy mucus
- Blood in cough
- Wheezing
- Feeling like suffocation
- Chest tightness and pain
- Fatigue
- Restlessness
- Increased heart rate
- Swelling in legs
Write diagnostic evaluation of pulmonary edema:
- History collection
- Physical examination
- Chest X-ray
- Echocardiogram
- Electrocardiogram
- Complete Blood Count
- Arterial Blood Gas Analysis
- Brain Natriuretic Peptide
- Basic Metabolic Panel
Write management of pulmonary edema:
Oxygen therapy:
- Provide supplemental oxygen to improve oxygen levels.
Diuretic :
- Provide diuretic medicine such as frusemide, which prevents fluid overload and reduces pulmonary congestion. Diuretics increase urine output and remove excess fluid from the body.
Vasodilators:
- Administering a vasodilator drug such as nitroglycerin or nitroprusside to reduce the load on the heart and decrease the load on cardiac output. Which dilates blood vessels and improves cardiac output.
Inotropic agent:
- Giving an inotropic agent to improve myocardial contractility. Such as dobutamine
Positioning :
- Elevate the patient’s head from the bed and provide the patient with an upright sitting position. So that lung expansion and venous return can be improved.
Fluid Retraction :
- Fluid retraction in conditions of fluid overload to prevent pulmonary congestion.
Treat underlying cause:
- Identify and treat the cause of pulmonary edema.
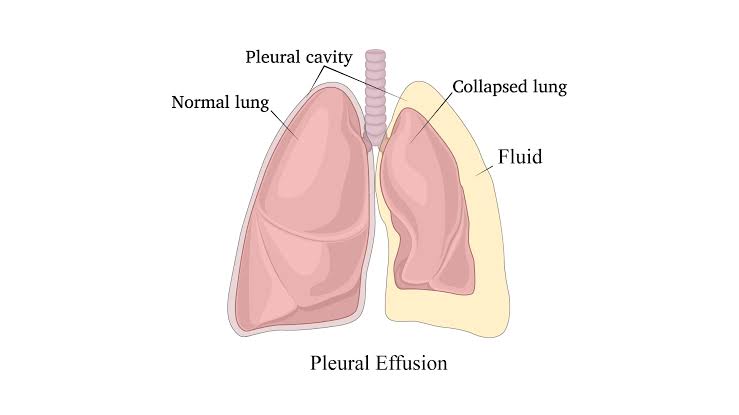
Define Pleural Effusion:
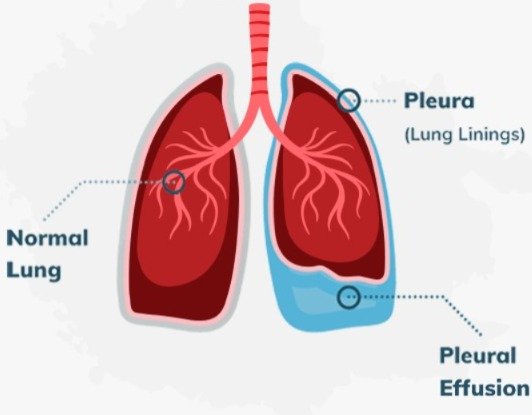
- Abnormal fluid collection in the pleural cavity is known as pleural effusion.
Write causes of pleural effusion:
- Congestive heart Failure
- Pneumonia
- Pulmonary embolism
- Cancer
- Liver disease
- Kidney disease
- Tuberculosis
- Autoimmune Disease
Write clinical manifestations of pleural effusion:
- Shortness of breath
- Chest pain
- Dry Cough
- Reduces chest expansion
- Dullness to percussion
- Decreases breath sound
- Pleuritic pain
- Fever
- Fatigue
Write diagnostic evaluation of pleural effusion:
- History collection
- Physical examination
- X-ray
- CT-scan
- Ultrasound
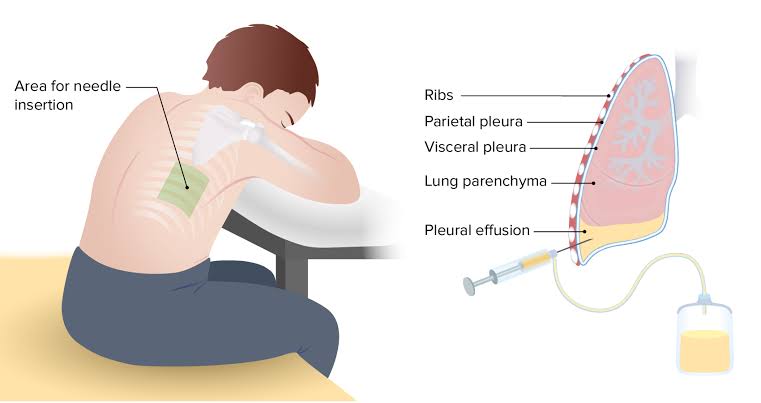
- Thoracocentesis
- Pleurodesis
- Pleural Fluid Analysis
- Pleural Biopsy
Write medical management of pleural effusion
Diuretic :
- If pleural effusion is caused by congestive heart failure or fluid overload, then diuretic drugs should be given to treat it.
Antibiotic :
- Providing antibiotic drugs to treat bacterial infections.
Anti-inflammatory medication :
- If pleural effusion is due to autoimmune disease or inflammatory condition, anti-inflammatory medication or corticosteroid drug should be provided to treat it.
Chemotherapy & Radiation Therapy:
- If pleural effusion is caused by cancer, chemotherapy and radiation therapy should be provided to treat the cancer.
Pain Relievers:
- Provide pain relievers to relieve pain. Such as ibuprofen
Antipyretic:
- Provide antipyretic drugs to reduce fever.
Oxygen therapy:
- Provide supplemental oxygen to improve oxygen levels.
Write surgical management of pleural effusion:
Video-assisted thoracic surgery (VATS/Video Assisted Thoracic Surgery) :
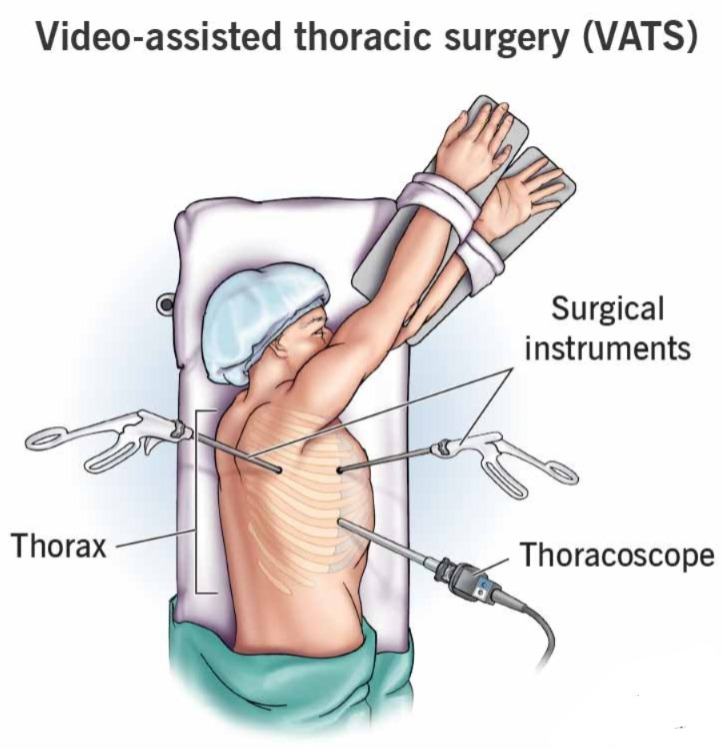
- This is a minimally invasive procedure. In which a small incision is made on the chest wall and a thoracoscope is inserted and with its help, fluid is drained and a biopsy is collected from the abnormal tissue.
Pleurodesis:
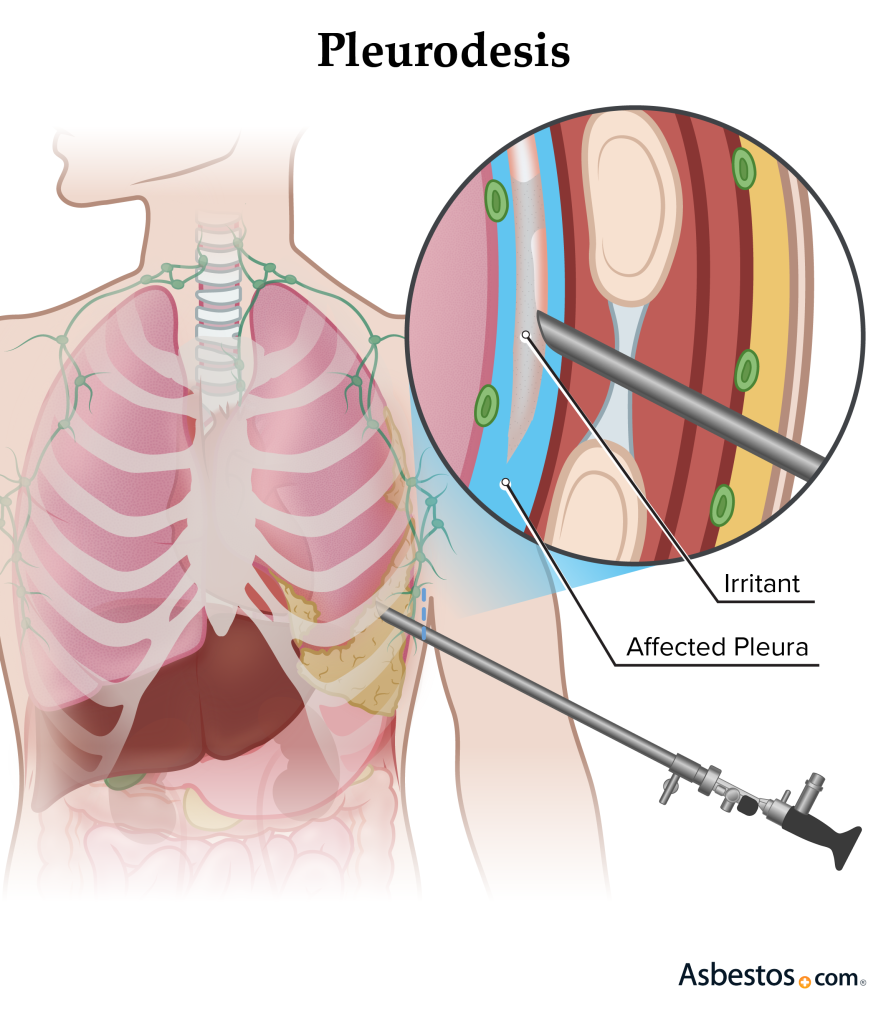
- Pleurodesis is a procedure in which adhesion is created between the two layers of the pleura and further fluid accumulation is prevented. In which a sclerosing agent is instilled into the pleural space during thoracoscopy, which causes the formation of adhesions.
Pleurectomy :
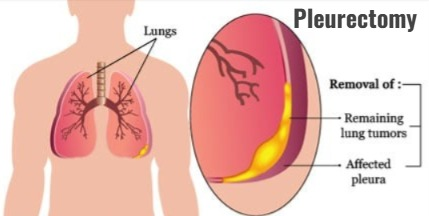
- In a pleurectomy procedure, the parietal pleura and visceral pleura are surgically removed. So that fluid accumulation between them can be prevented.
Pleural catheter placement:
- In pleural catheter placement, a small tube is inserted into the pleural space through the chest wall, with the help of which the fluid is continuously drained.
Write complications of pleural effusion:
- Pneumothorax
- Empyema
- Pleural thickening
- Atelectasis
- Respiratory Failure
- Pulmonary Hypertension
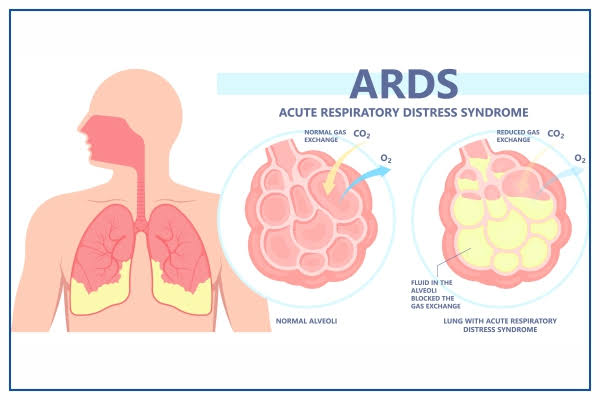
Define acute respiratory distress syndrome:
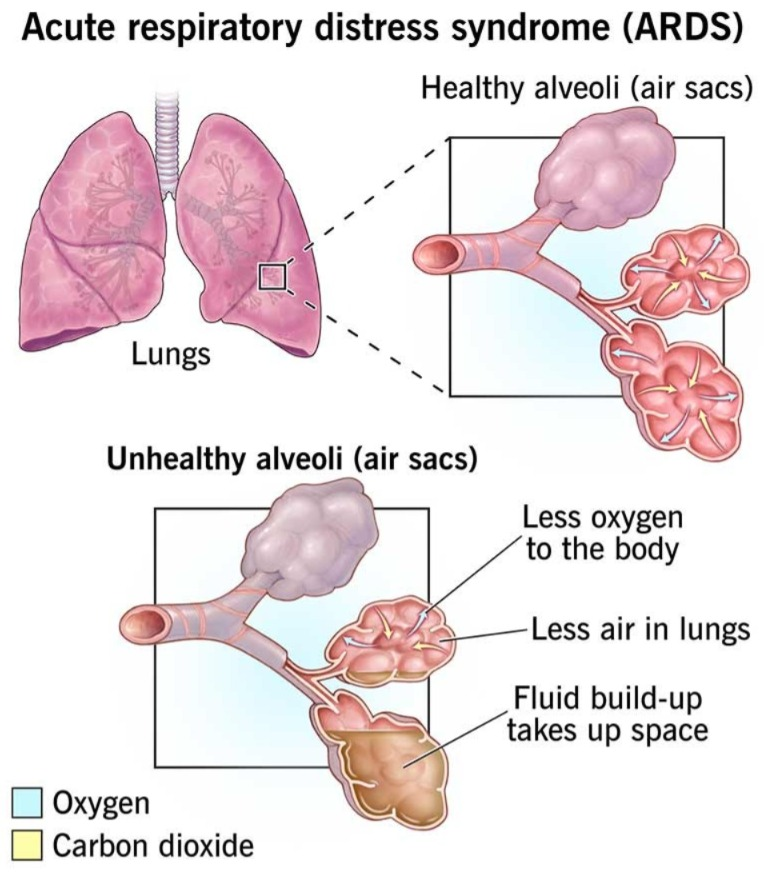
- This is a life-threatening, severe lung condition. In which fluid builds up in the tiny and elastic air sacs in the lungs, so that the air sacs cannot transport oxygen and the oxygen level in the blood decreases.
Write causes of acute respiratory distress syndrome:
- Infection
- Pneumonia
- Tuberculosis
- Sepsis
- COVID 19
- Inhalation of Harmful Substances
- Trauma – Direct Injury to the Lungs
- Pancreatitis
- Drug overdose (cocaine, opioids)
- Drowning
Write clinical manifestations of acute respiratory distress syndrome:
- Difficulty in breathing
- Rapid breathing
- Hypoxemia
- Hypoxia
- Cyanosis
- Cough
- Frothy secretion
- Fatigue and weakness
- Confusion
- Altered mental status
Write diagnostic evaluation of acute respiratory distress syndrome:
- History Collection
- Physical Examination
- X-ray
- CT Scan
- Echocardiogram
- Electrocardiogram
- Pulse oximeter
Write management of acute respiratory distress syndrome:
Mechanical ventilation:
- Mechanical ventilation to support breathing Provide ventilation.
Oxygen therapy:
- Provide supplemental oxygen to maintain oxygen levels.
Fluid management:
- Fluid management should be performed to prevent fluid overload and pulmonary edema from developing in patients with ARDS.
Pharmacotherapy:
- Giving antibiotics to treat infection. In addition, in some cases, corticosteroids and neuromuscular blocking agents should be provided.
Positioning:
- Provide the patient with a prone position. So that lung perfusion and ventilation can be improved.
Nutritional Support :
- Provide adequate nutrition to patients with ARDS to promote healing and recovery.
Treatment of underlying cause :
- Identify and treat the underlying cause of ARDS.
Supportive Care:
- Close monitoring of vital signs, electrolytes, and organ function. Pain management, sedation, and stress relief.
Write complications of acute respiratory distress syndrome:
- Blood clot
- Deep vein thrombosis
- Collapsed lung
- Confusion
- Multiple Organ Failure
- Muscle Weakness
- Lung Fibrosis
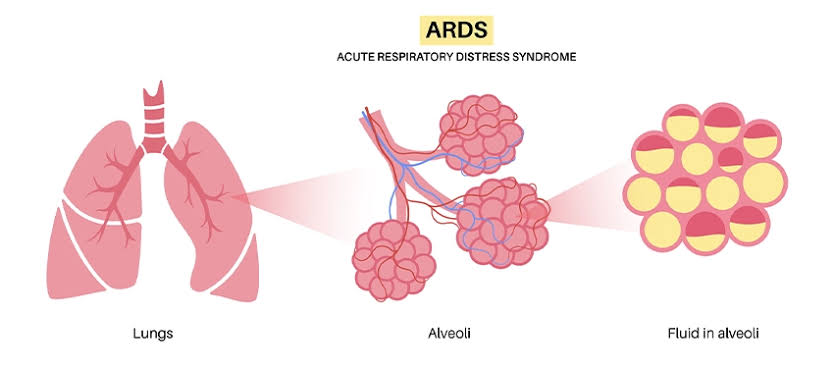
Define SARS:

- SARS means Severe Acute Respiratory Syndrome. This is a viral respiratory illness caused by the SARS-associated coronavirus (SARS-CoV).
Write clinical manifestations of SARS:
- Fever
- Cough
- Shortness of Breath
- Chills
- Muscle
- Headache
- Loss of appetite
- Sore throat
- Fatigue
- Malasses
- In severe cases, pneumonia and respiratory failure may also occur.
Write diagnostic evaluation of SARS:
- History collection
- Physical examination
- RT-PCR
- Serology (ELISA)
- X-ray
- CT scan
- Complete blood count
- Blood culture
- Sputum culture
Write management of SARS:
Supportive care:
- Supplemental oxygen or mechanical ventilation should be used if necessary. In addition, provide adequate hydration and nutrition to the patient.
Infection control measures:
- Isolate SARS patients to prevent them from spreading to other people. Use personal protective equipment when dealing with patients with SARS.
Antiviral therapy:
Since SARS is caused by a virus, antiviral drugs should be used to treat it.
Alternate Therapies in Respiratory System Disorder:
1.Introduction:
- Respiratory System Disorder refers to diseases of the respiratory system such as asthma, bronchitis, tuberculosis, pneumonia, and chronic obstructive pulmonary disease (COPD).
- These diseases are characterized by difficulty breathing, cough, heaviness in the chest, and oxygen deficiency. In this disease, the use of alternative therapies along with medical treatment proves helpful for disease control and recovery.
2. Yoga Therapy:
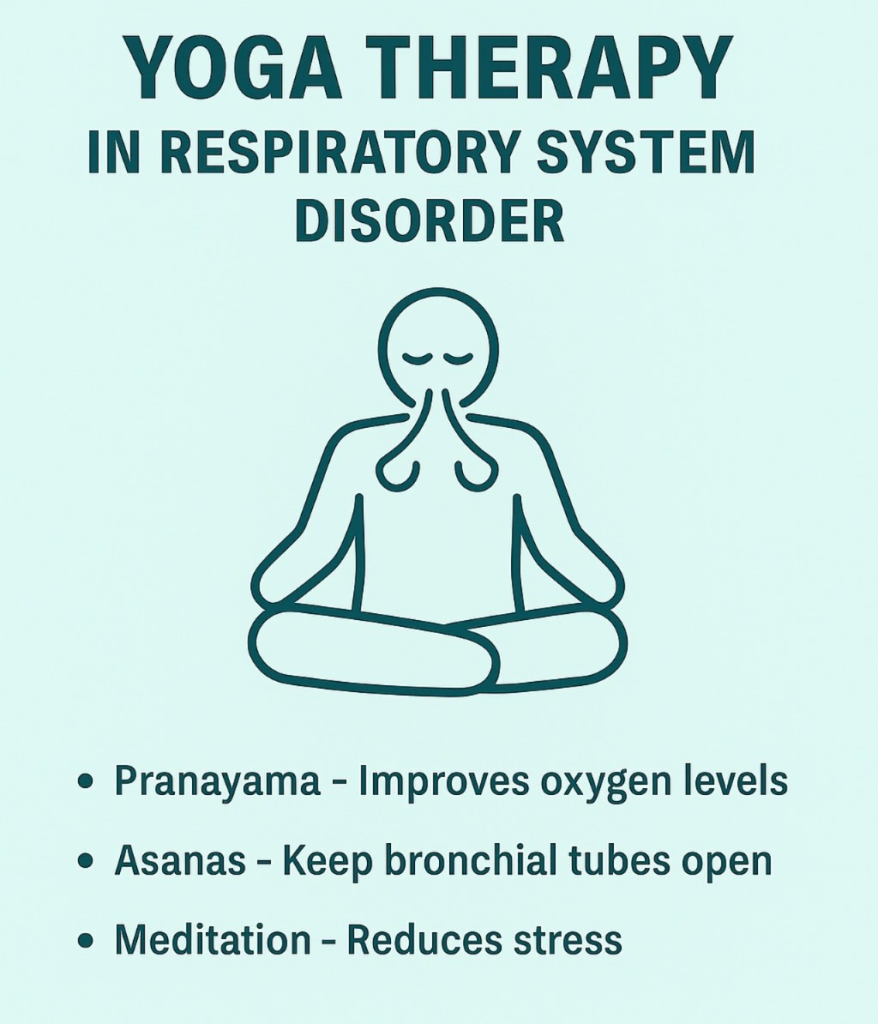
- Yoga strengthens the respiratory system and improves the ability of the lungs.
Pranayama:
- Oxygen levels improve through Anulom Vilom, Kapalbhati, Bhramari.
Asanas :
- Bhujangasana, Tadasana, Matsyasana, and Shavasana (Shavasana) keeps the bronchial tubes open and lung function improves.
Meditation:
- Reduces stress which is important in asthma or COPD.
3.Physiotherapy:
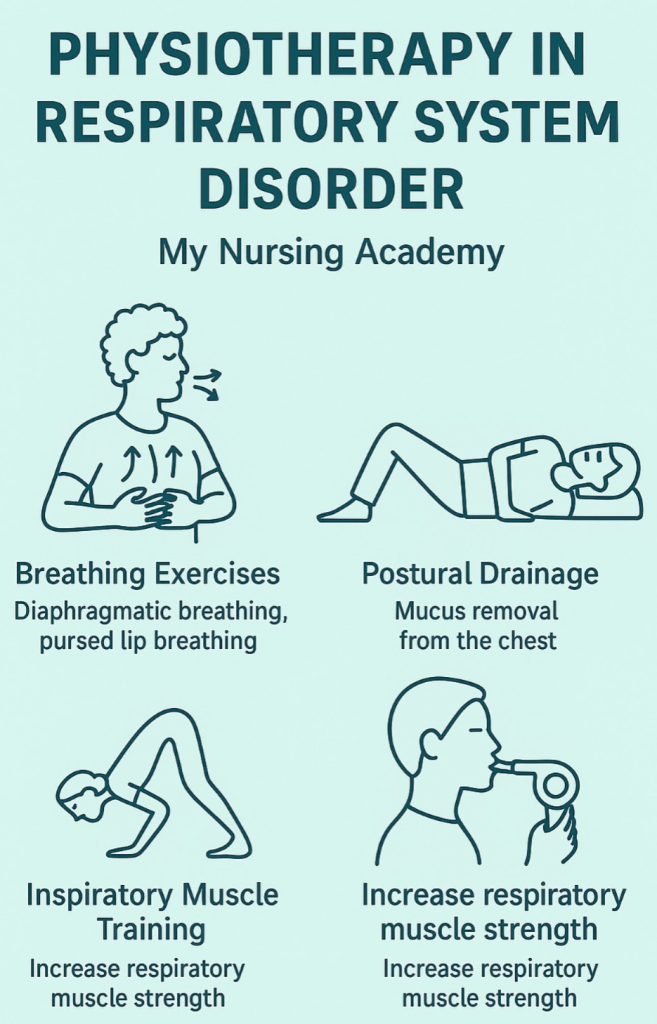
- Physiotherapy is very effective for patients with respiratory system disorders.
Breathing Exercises:
- Diaphragmatic Breathing, Pursed Lip Breathing control breathing.
Postural Drainage :
- Helpful in removing secretions (mucus) from the chest.
Inspiratory Muscle Training :
- Increases the muscle strength of the lungs.
4.Aromatherapy:
- Aromatherapy uses natural essential oils.
- Eucalyptus Oil and Peppermint Oil clean the breathing tube and reduce inflammation.
- Lavender or Tea Tree Oil has antimicrobial effects.
- Used through inhalation or steam therapy.
5. Acupuncture:
- Acupuncture is a Chinese treatment method in which needles are inserted at specific points on the body to improve energy flow.
- Breathway obstructions are relieved by applying pressure to the Lung Meridian. Reduces.
- Diseases like Asthma, Allergic Bronchitis are relieved.
6. Naturopathy:
- Naturopathy is based on natural healing.
Hydrotherapy :
- Steam Therapy with hot water removes phlegm.
Herbal Remedies:
- Tulsi, Ginger, Turmeric, Honey are used for anti-inflammatory and antimicrobial effects.
Sunbath and Proper Diet:
- A diet rich in vitamins C and E strengthens the respiratory system.
7.Homeopathy:
- Homeopathy depends on individual symptoms.
Arsenicum Album :
- For shortness of breath and anxiety.
Bryonia :
- For dry cough and chest pain.
Ipecacuanha :
- For difficulty breathing with cough.
8. Music Therapy (Music Therapy):

- Music Therapy Reduces Stress, Improves Breathing Rhythm and is helpful in increasing oxygenation.
- Slow and Pure Music improves heart rate and respiratory rate.
- Alternative therapies like yoga, physiotherapy, aromatherapy, acupuncture and naturopathy are helpful in treating respiratory system disorders along with medical treatment.
These therapies are helpful in improving the functioning of the respiratory system, immunity and mental balance.
