ENGLISH-UNIT-8-Respiratory disorder-part-02-UPLOAD
Assessment of respiratory function (Assessment of respiratory functions):
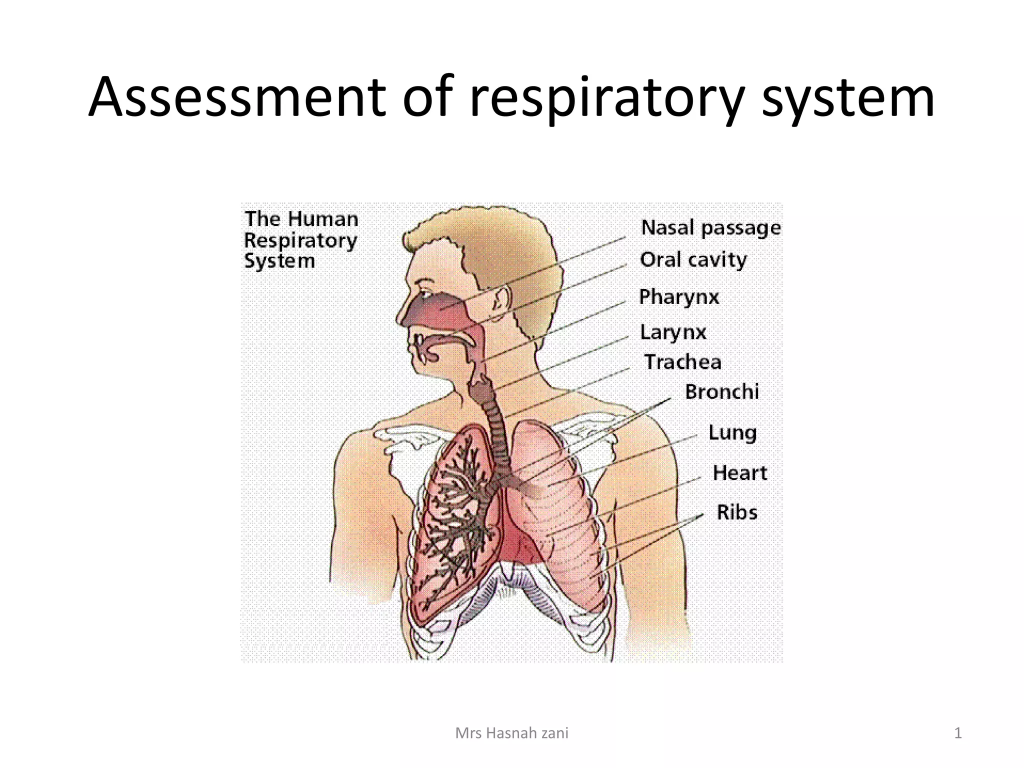
Health history (subjective data) :

- Health history includes present health history, past health history, past surgical history, personal history, family history and occupational history.
Present health history / chief complaint (Present health history / chief complaint) :

- Ask the patient about their current complaints.
- Ask the patient about their current complaints.
- Ask the patient whether they have breathing difficulties, chest pain, or coughing.
- If the patient has these symptoms, ask about their duration, severity, intensity, and associated factors.
- Such as when and in what position does the breathing difficulties occur?
- Ask whether any kind of sound is heard while breathing.
- Ask which side of the chest is the pain and whether this pain radiates or not. (If there is a cardiac-related problem, then the pain radiates. While if there is a respiratory-related problem, the pain does not radiate.)
- Ask whether there is sputum production.
- If there is production, know its quality and quantity.
- To know what color the sputum is.
- To know whether there is blood in the sputum.
- To ask how long the sputum has been present.
Past health history:

- Ask the patient if he has had any such symptoms in the previous years.
- Find out if the patient has had conditions like TB, whooping cough, diphtheria, Covid 19 in the previous years.
- Find out if the patient has been admitted to the hospital in the past.
- Collect information about childhood diseases and immunizations.
Past surgical history:

- To know whether the patient has undergone any type of surgery in the previous years.
Personal history :

- Ask the patient if he has any allergies.
- Find out if the patient smokes.
- If there is a smoking history, find out how long he has been smoking and how many times he smokes throughout the day.
- Know whether he is taking any kind of medicine.
- To know if there is a history of alcohol.
Family history:

- Collect the patient’s family history.
- To know whether anyone in the family has respiratory diseases or allergies. Such as asthma, emphysema, cystic fibrosis
- To know whether there are any other diseases.
- To know whether anyone in the family smokes.
Occupational history:

- Collect the patient’s occupational history.
- For example, to know what work the patient does.
- If someone works in an industry or factory, to know whether they use protective equipment or not.
- Respiratory tract infections are more common in people working in mining, refining, manufacturing, construction, stone making, cotton and textile industries. Such as silicosis, asthma, asbestosis
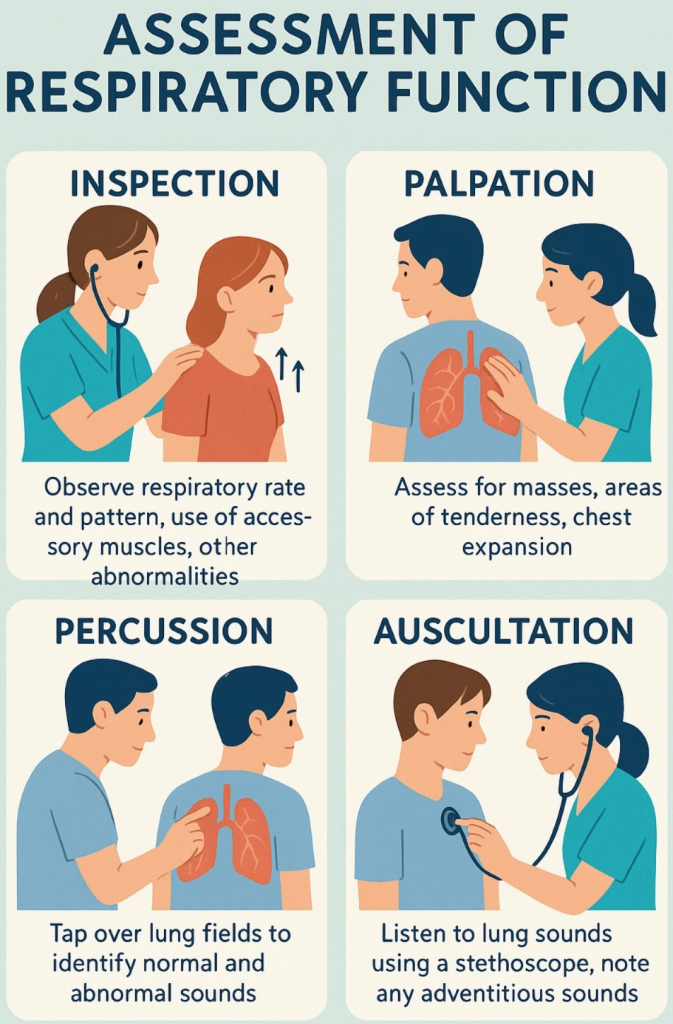
Physical examination (Physical Examination) / objective data (Objective Data):

- Respiratory assessment mainly includes the head, chest, extremities, fingers and toes.
- Inspection, palpation, percussion and auscultation methods are used in respiratory examination.
- Use adequate lighting and maintain a cool and comfortable environment during the examination.
- Keep a sputum mug with you during the examination. This allows the patient’s sputum to also be examined.
Inspection:
Skin inspection:
- skin and Check the color of the mucous membrane.
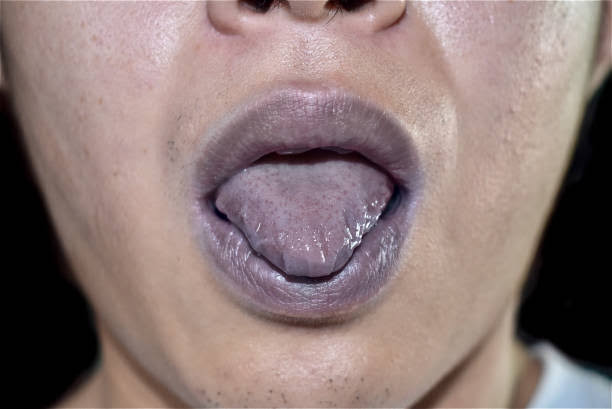
- Check whether cyanosis is present in the conjunctiva, lips, and tongue.
- Cyanosis is mainly seen due to the condition of hypoxia, i.e. the condition of deoxygenated hemoglobin is present.
- Cyanosis seen in the lips, gums, and tongue is known as ‘Central cyanosis’.
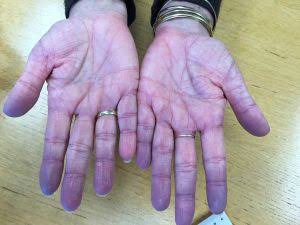
- Cyanosis seen in the fingers and toes is known as ‘Peripheral cyanosis’ .
Thoracic inspection:

- Examine the patient’s breathing pattern and rhythm. Also check the effort for breathing.
- Check whether there is any restriction while breathing. In addition, check whether the accessory muscles are used while breathing. (If restriction is seen during inspiration and if it is asymmetrical, it indicates a block in the respiratory branch)
- Examine whether there is any asymmetrical bulging during breathing.
- Check whether there is any bulging in the intercostal space during expiration. (If found, it indicates obstruction of expiratory flow)
- Examine the chest for symmetry, shape, and deformity.
- Check whether the chest has a normal shape or a barrel, pigeon, or funnel shape.
👉🏻 For your knowledge :
- The shape of the chest in a normal healthy person is elliptical.
- In a normal healthy person, the anterior posterior diameter is 1 while the lateral diameter is 2.
- In a normal healthy person, the ratio of anterior posterior to transverse diameter is 1:2.
Barrel chest:
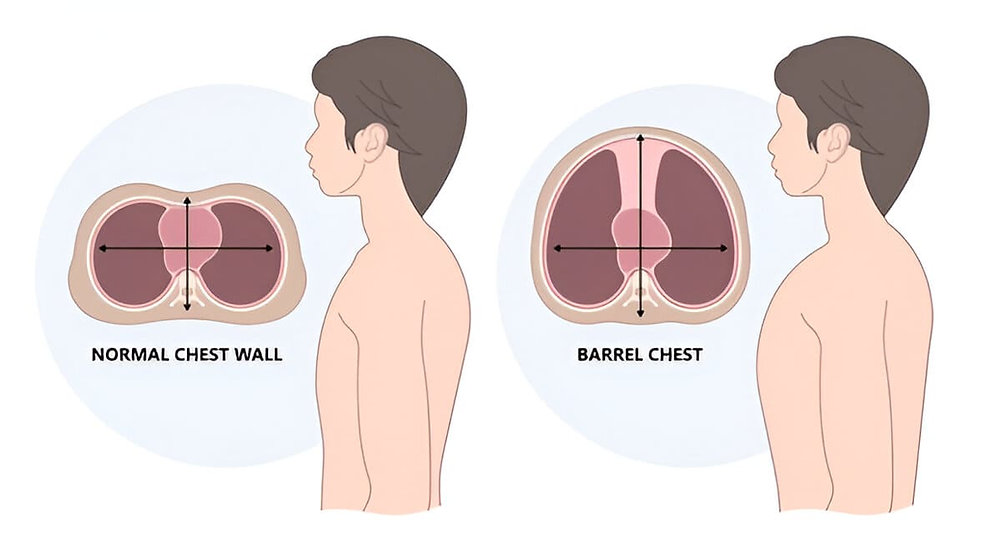
- Barrel chest is caused by over-inflation of the lungs. Due to the decrease in elasticity of the alveoli, they appear swollen. Due to which they appear as a round bulging chest and look like a Barrel chest.
- In barrel chest, the anterior posterior diameter increases to 2. Hence, the ratio of anterior posterior diameter to lateral diameter is 1:1.
- Barrel chest is seen in patients with COPD and emphysema.
Pigeon chest:
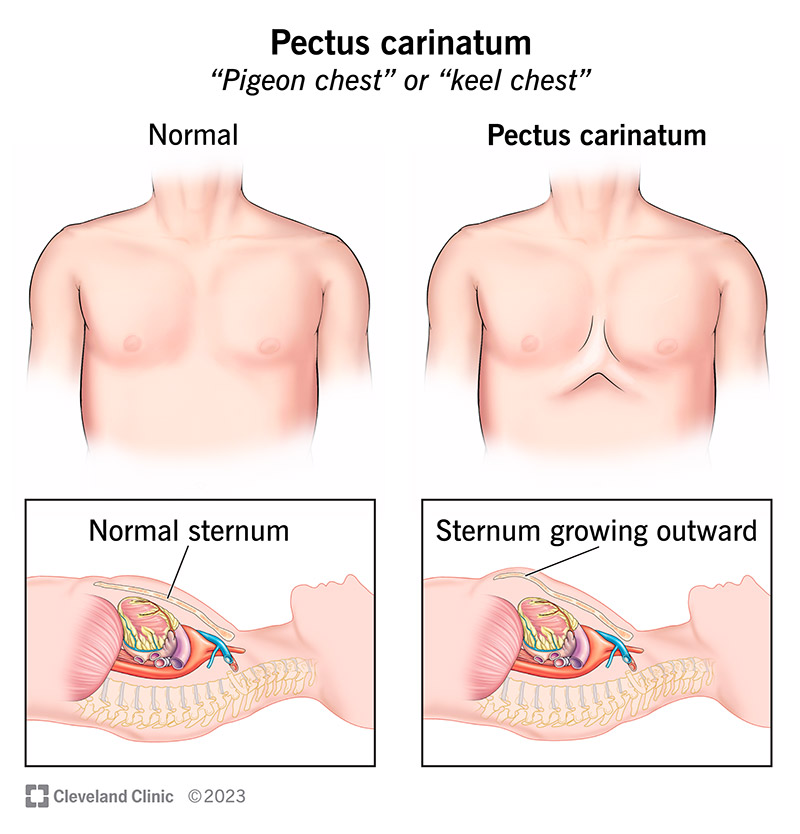
- Pigeon chest is also known as ‘Pectus carinatum’.
- In which pectus means chest and carinatum means keel of a boat.
- Pectus carinatum is a deformity of the chest wall in which there is an overgrowth of cartilage between the sternum and ribs, causing the sternum and ribs to protrude outward.
- This results in an increase in anterior posterior diameter.
Funnel chest:
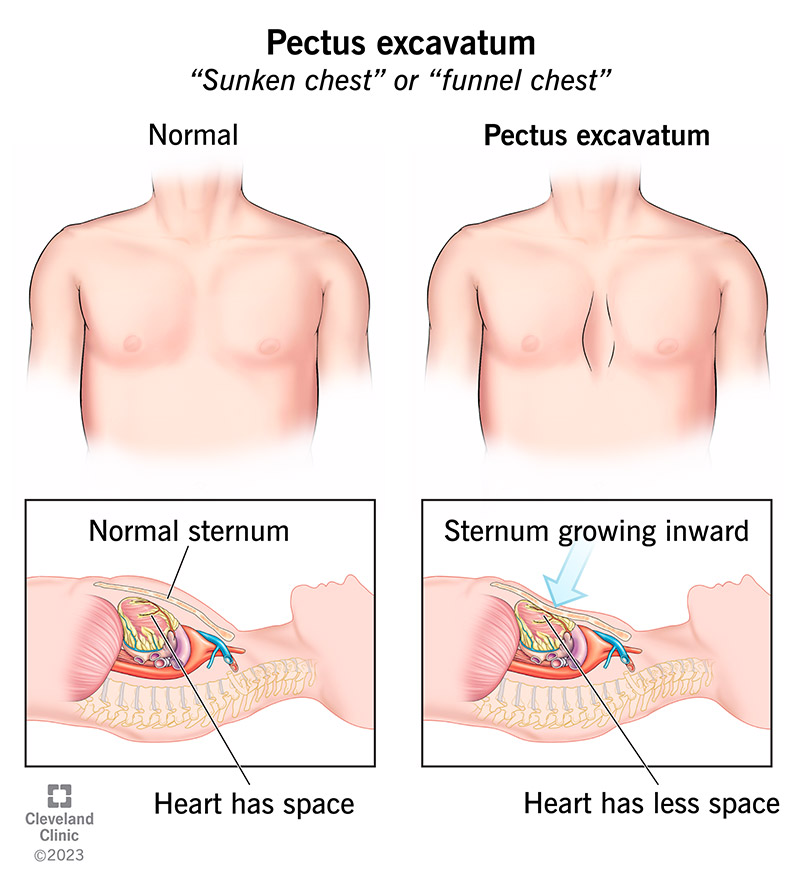
- Funnel chest is also known as ‘Pectus excavatum’, ‘sagged chest’ and ‘cobbler’s chest’.
Where pectus means chest, and excavatum means pit. - Pectus excavatum is an abnormal congenital condition. In which the sternum is pulled inward, that is, the sternum is seen depressed and grows inward.
- A decrease in the anterior posterior diameter is seen in the funnel chest.
Inspection of finger & toes (Inspection of Fingers and Toes):
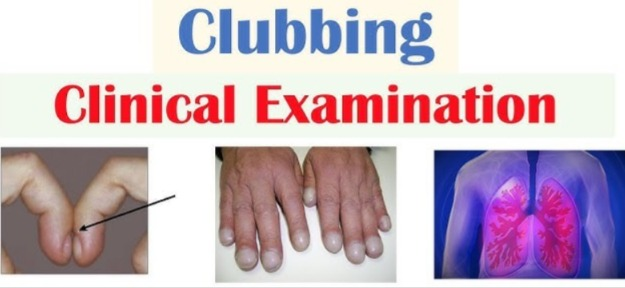
- Check whether clubbing is present in the fingers and toes.
- Check for cyanosis in the fingers and toes.
👉🏻 For your knowledge Clubbing of finger (Clubbing of finger):
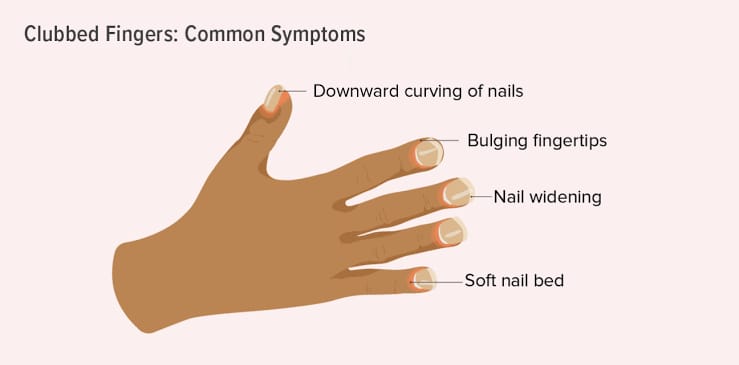
- In clubbing of the finger, the nail is found to be abnormal and round in shape (like a spoon).
- Clubbing of the finger is a sign of heart and lung disease that indicates chronic hypoxic conditions, i.e. low levels of oxygen in body tissues or organs such as chronic lung infection, chronic lung malignancy
- A Schmarroth window test is performed to check whether clubbing is present in the finger or not.
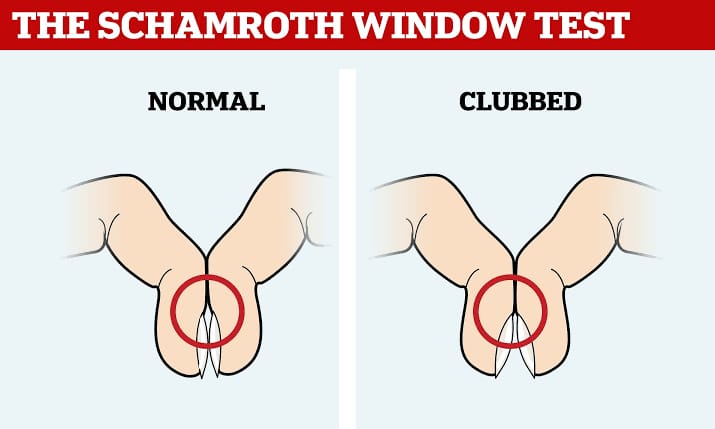
Scharmroth window test:
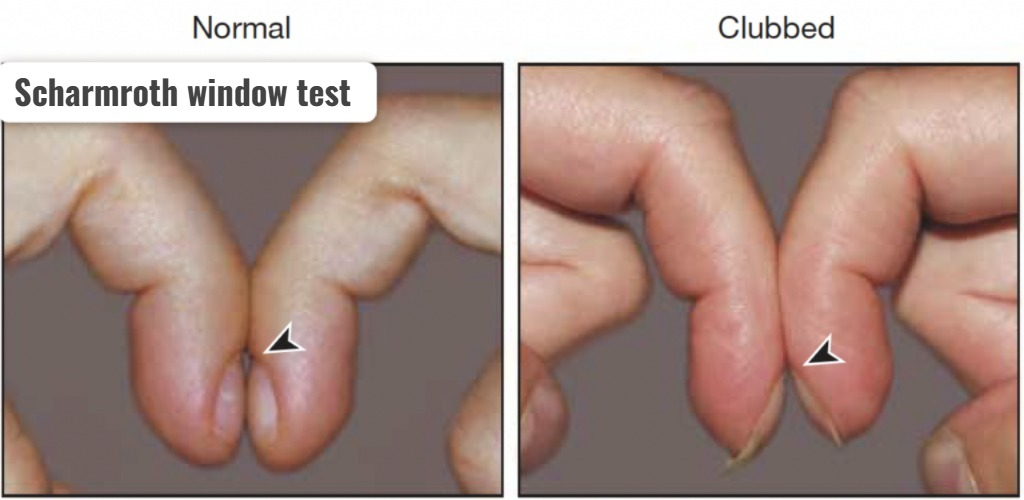
- The Scharmroth window test is used to confirm whether clubbing is present in the finger or not.
- In the Scharmroth window test, the nail beds of each finger of both hands are held together as shown in the picture and a diamond shape is checked to see if there is a diamond shape between the nail beds.
- If a diamond shape is seen between the nail beds, it is normal, while if there is no space between the nail beds, it indicates clubbing.
Palpation (palpation):
- Thoracic palpation involves palpating the thoracic area.
- In which the front and back of the chest are Palpation is performed for tenderness, deformity, and abnormal movement.
- In addition, the area is palpated for pain, lesions, respiratory expansion, and fremitus.
for your knowledge
Tactile fremitus:
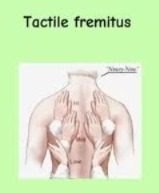
- Tactile fremitus is a palpation technique used to assess the vibrations transmitted to the chest due to speech. In which the health care personnel places their hand in the area as shown in the image and asks the patient to speak and feels the vibration in the chest area.
- If there is an increase in fremitus, it indicates a condition like pneumonia, but if there is a decrease in fremitus, it indicates a condition like pleural effusion.
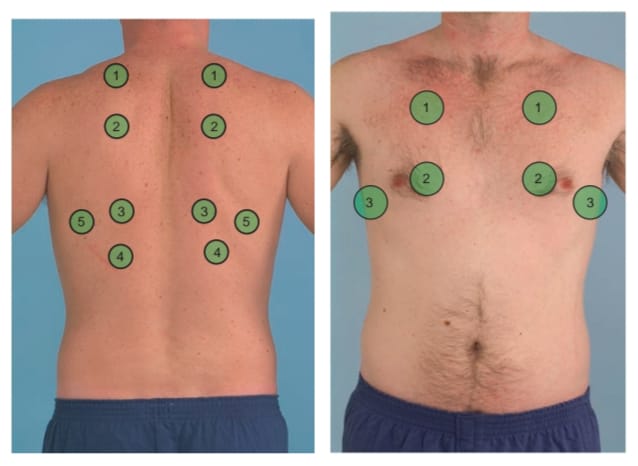
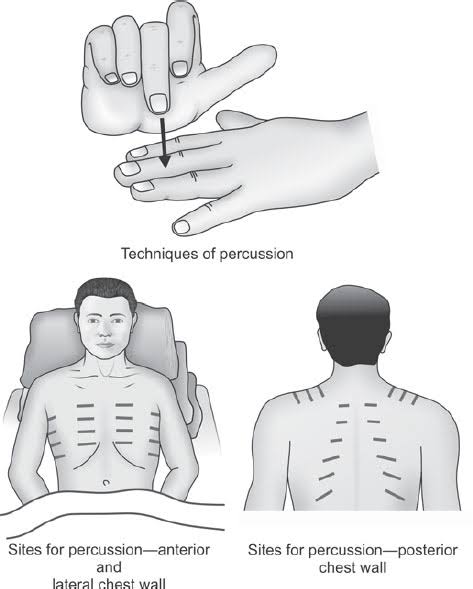
Percussion:

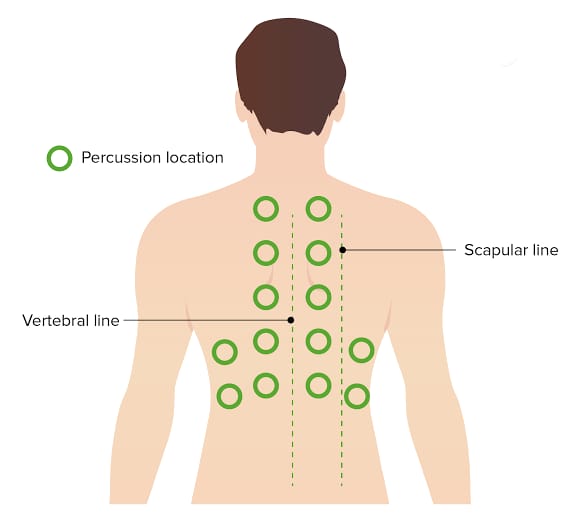
- Respiratory percussion involves tapping the chest to assess the underlying structures to check for air, fluid, or solids present.
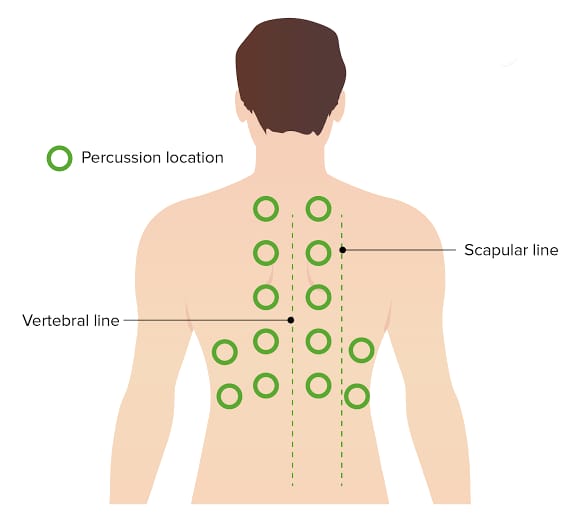
- In which the anterior and posterior chest is tapped side to side and top to bottom and the sounds heard through it are noted.
- In addition, respiratory excursion is noted in respiratory percussion.
- Respiratory percussion is useful for identifying changes in lung density and diagnosing conditions such as pneumonia and pleural effusion.
for your knowledge
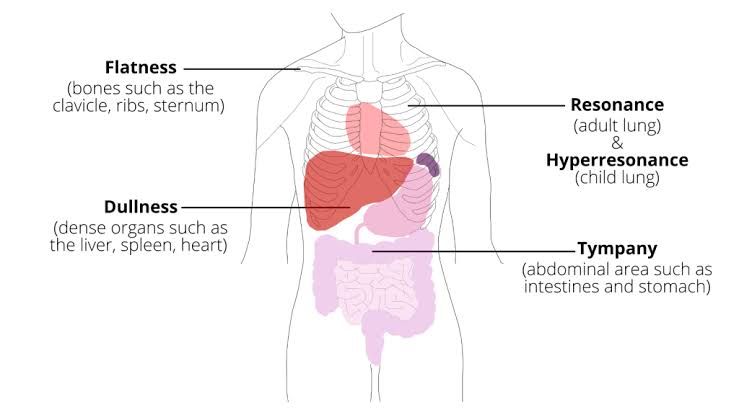
• Resonance sound :
- Resonance is a low pitch sound. Which is mainly heard in airy areas. Such as in the thoracic cavity (Lungs)
• Dull sound:
- A dull sound is heard in areas with fluid. Such as heart, liver, spleen
• Flat sound:
- Flat sound is heard in solid areas. Such as bone, muscles
• Tympanic sound (tympanic Sound:
- A tympanic sound is a hollow, drum-like sound that is heard in an area with a bloated stomach, i.e. an area with air pressure.
Hyperresonance sound:
- Hyperresonance sounds are heard when the thoracic cavity is filled with excessive air. Such as the condition of pneumothorax
- When a dull sound is heard in the thoracic cavity, it indicates that fluid has accumulated in the thoracic cavity.
Auscultation:
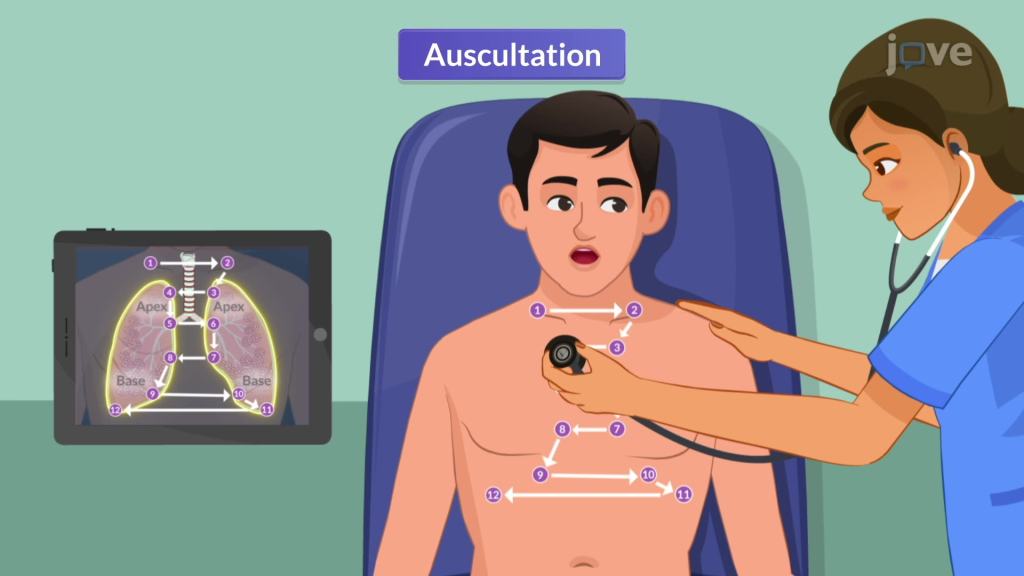
- Auscultation involves listening to lung sounds with the help of a stethoscope.
- Auscultation is performed by expert staff.
- Using a stethoscope, the characteristics of normal lung sounds such as location, quality, intensity are noted.
- Auscultation also involves listening to any abnormal lung sounds. To do.
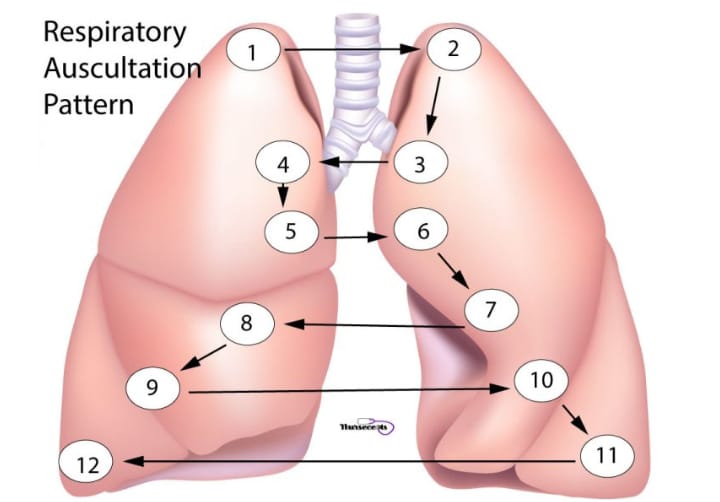
- In auscultation, lung sounds are auscultated on the anterior and posterior sides of the chest with the help of the diaphragm. The chest is auscultated as shown in the picture below.
- Sounds are noted during both inspiration and expiration. In between, the patient is given rest so that the condition of hyperventilation can be prevented.
- Thus, abnormal sounds are detected with the help of auscultation.
- In addition, voice sounds (bronchophony, egophony) are also noted in auscultation.
Normal lung sound:
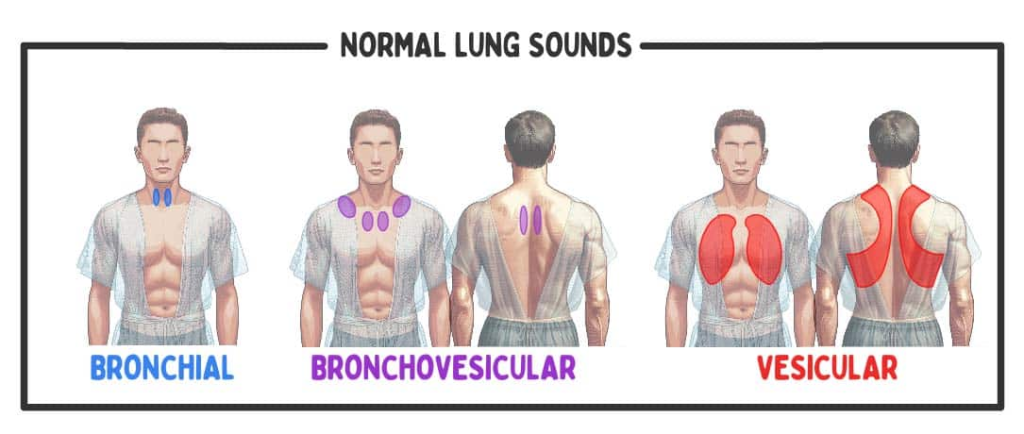
- Bronchial sound, vesicular sound and broncho-vesicular sound are normal lung sounds.
Bronchial sound:
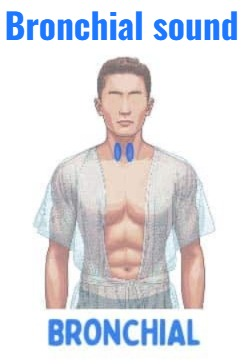
- Bronchial is a normal high-pitched hollow or tubular sound.
- Heared in the trachea.
- In which the expiratory time is longer than the inspiratory time.
Vesicular sound:
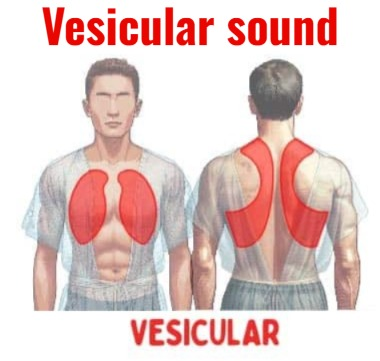
- Vesicular is a normal low-pitched soft sound. Which is heard in the entire lung.
- In which the inspiratory time is longer than the expiratory time.
Bronchovesicular sound:
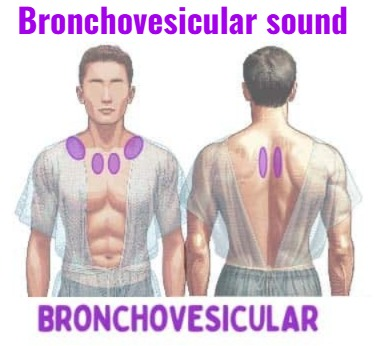
- Broncho-vesicular is a normal medium pitch sound in which the inspiratory and expiratory times are similar.
Abnormal lung sound:
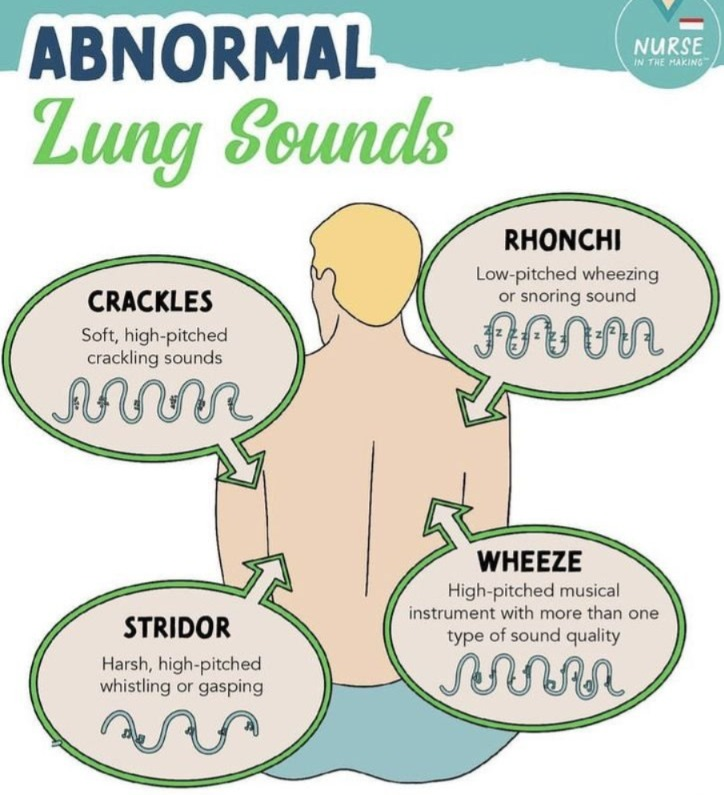
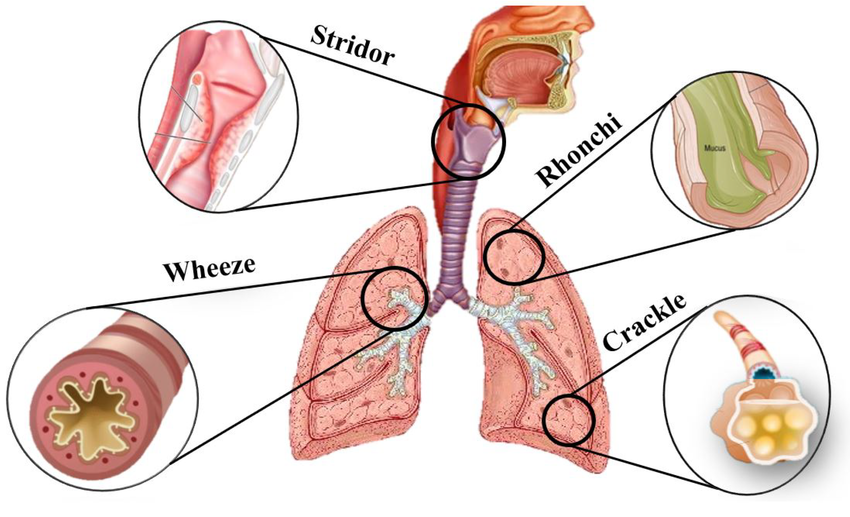
Wheezing sound:

- Wheezing is a high-pitched (High-Pitch) musical sound. Wheezing sound occurs when the airway – i.e. breathing passage – becomes narrowed or partially obstructed. Wheezing is a sound that occurs only during expiration (breathing out).

Stridor (Stider):
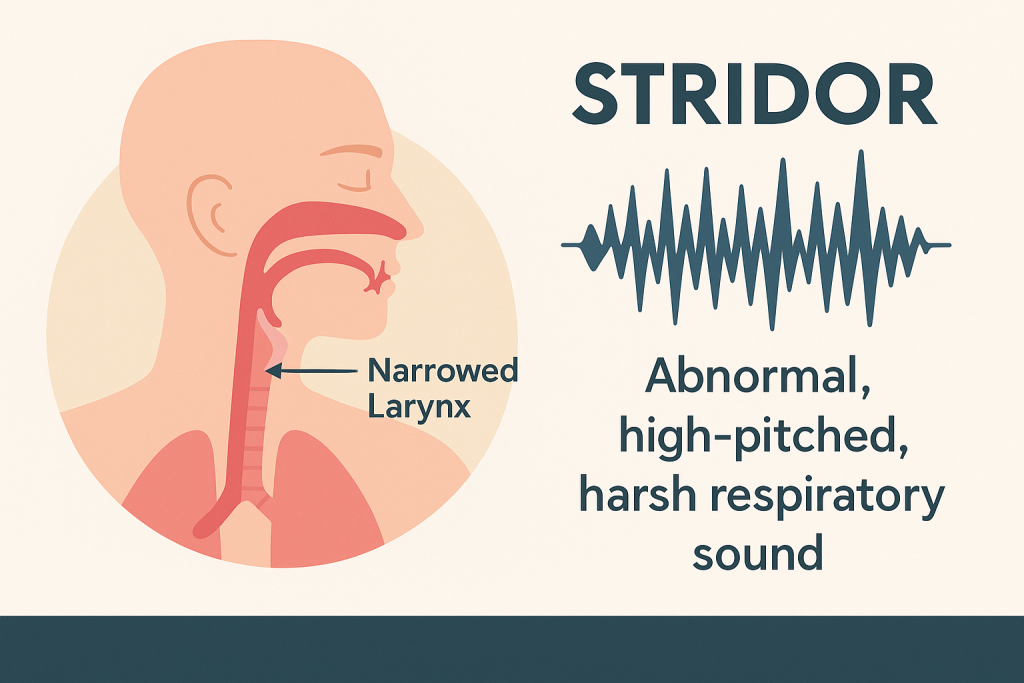
- Stridor is an abnormally high-pitched (High-pitched) breathing sound, usually heard during inspiration. This sound is produced when the upper airway – especially the larynx or trachea – becomes narrowed or obstructed.
- That is, Stridor = Inspiratory high-pitched harsh sound due to upper airway obstruction.
Pleural friction rub:

- Pleural Friction Rub is an abnormal respiratory sound that occurs when the Pleural Membranes – the outer layers of the lungs (the parietal and visceral pleura) – rub against each other.
- Normally, a small amount of lubricated pleural fluid (Pleural Fluid), which prevents friction.
But when inflammation occurs, this layer becomes rough and produces a grinding sound when breathing in or out, and a grating and cracking sound is heard. Which is called Pleural Friction Rub.
Rhonchi :
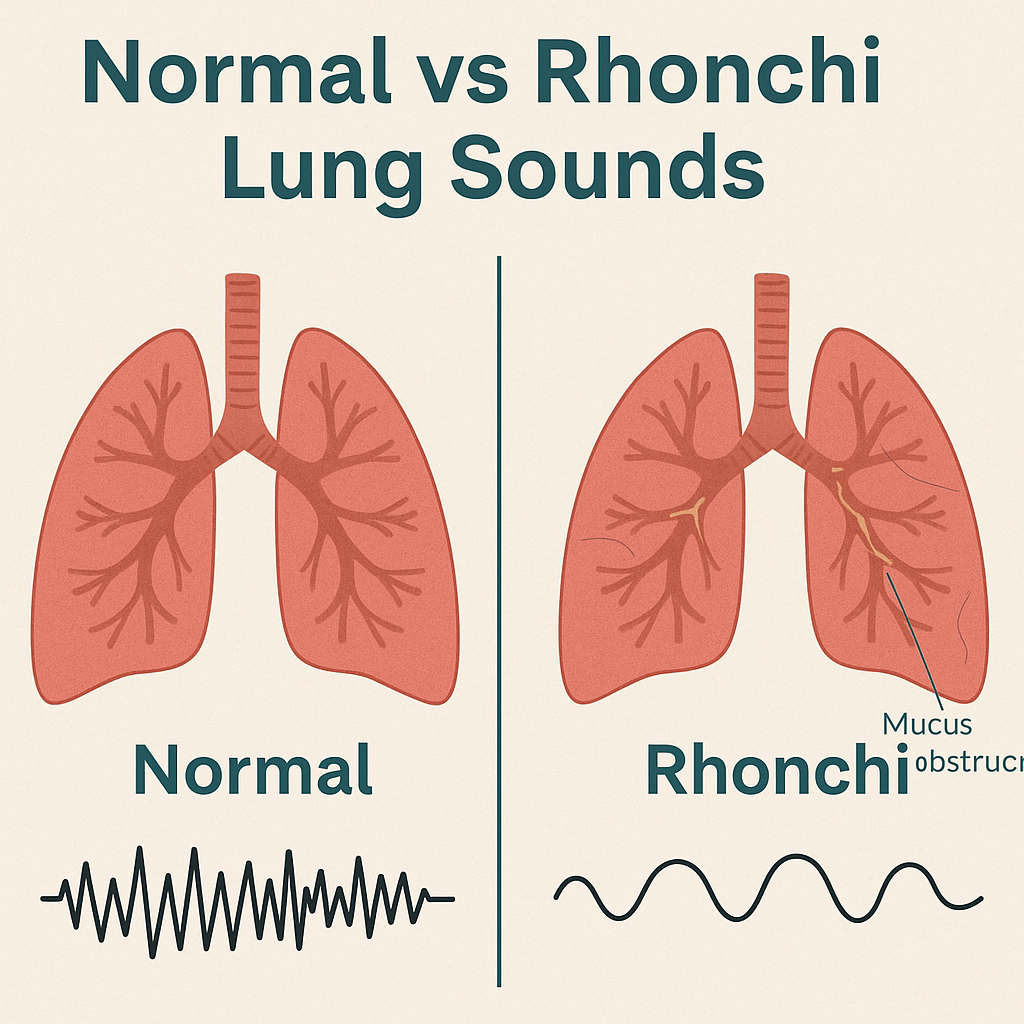
- Rhonchi is an abnormal continuous breath sound, which is usually low-pitched and snoring / gurgling-like.
- This sound is most often caused by the blockage of the airway with mucus or other secretions, especially In the Large Bronchi. Which is usually heard during expiration, sometimes also during inspiration.
Fine crackles:
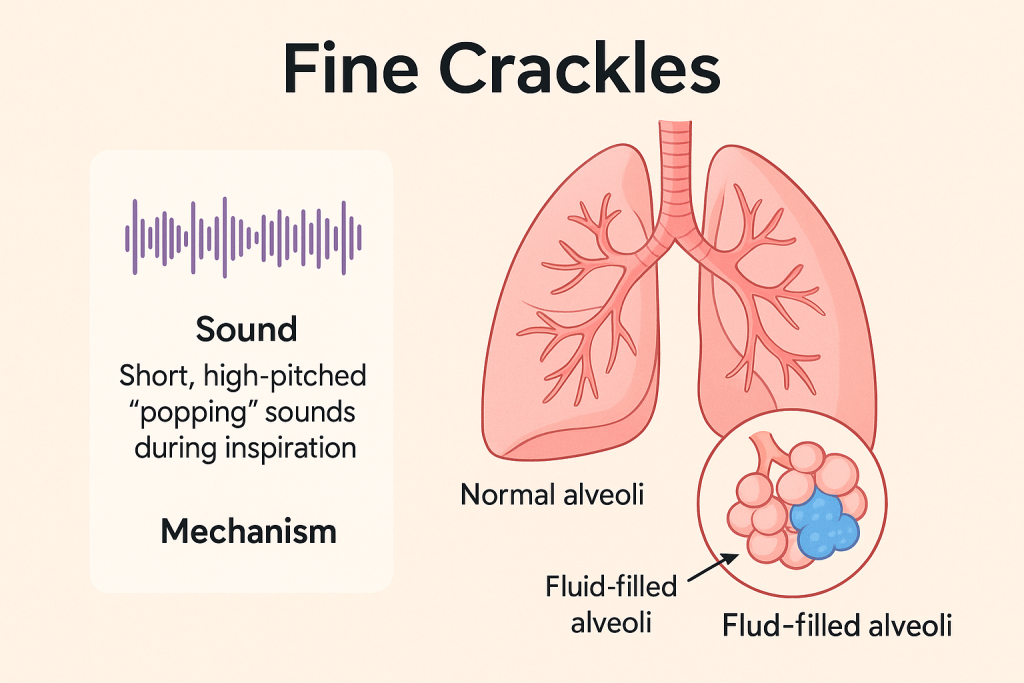
- Fine Crackles are a type of abnormal discontinuous breath sound, which is heard as a Short, Soft, High-pitched Popping or Crackling sound.
- This sound is usually heard during inspiration, especially at the bases of the lungs.
It indicates that the small airways or alveoli of the lungs are Fluid or collapsed air spaces are exposed in the lungs.
Coarse crackles:

- Coarse Crackles are a type of Abnormal Breath Sounds that are Long, Loud and Low-pitched “Bubbling or Gurgling Sound”.
- This sound is usually heard during both inspiration and expiration and is caused by Mucus or Fluid accumulation in the Larger Airways of the Lungs. is.
Diagnostic evaluation:
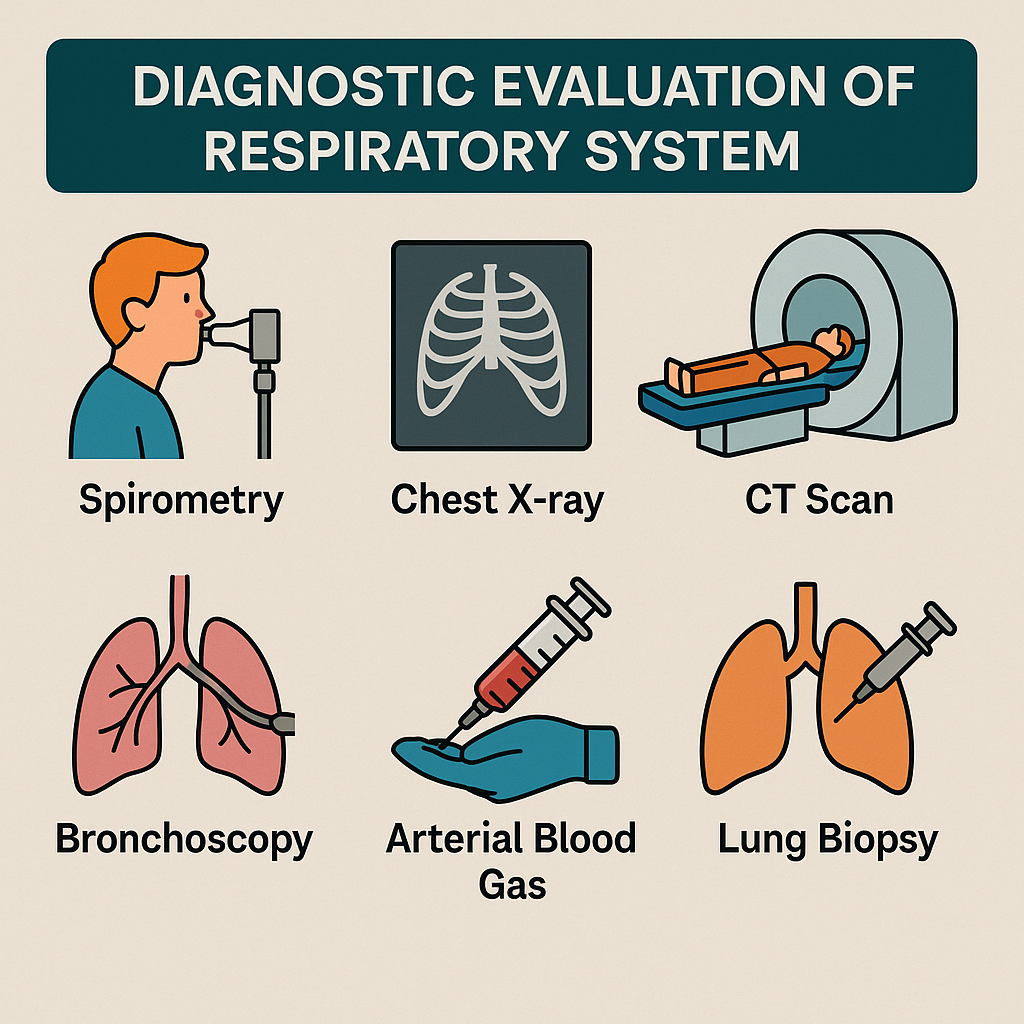
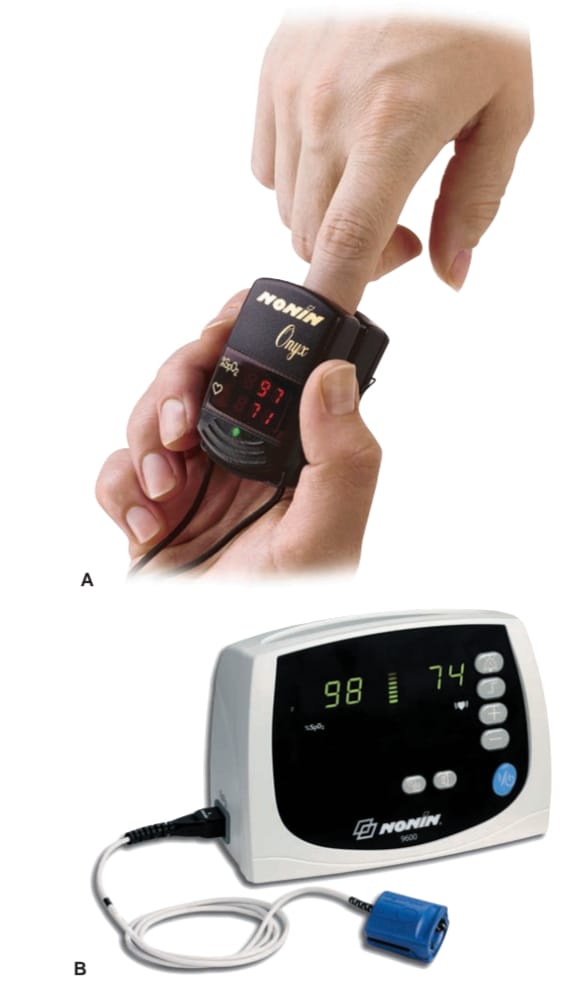
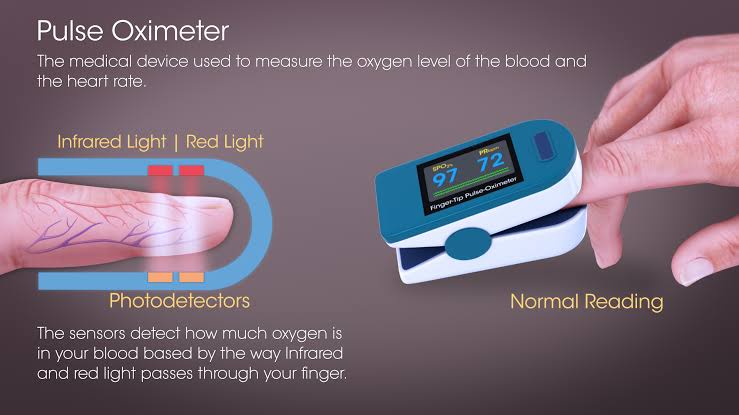
Pulse oximetry:

- Pulse oximetry is also known as an ‘oxygen saturation test’.
- Pulse oximetry is a It is a quick, non-invasive technique that monitors oxygen saturation linked to hemoglobin.
- Pulse oximetry uses a pulse oximeter. Which is a type of electronic device.
- This device has a light emitting diode installed which passes light of two specific wavelengths (infrared light and red light) mostly on the finger tip. One of these lights measures the amount of oxygenated hemoglobin while the other light measures the amount of deoxygenated hemoglobin and finally shows the amount of oxygenated hemoglobin.
- The pulse oximeter is placed on the finger, toes, foot, ear and nose and the SpO2 level is checked.
- Normal spo2 levels are between 95-100%. If the spo2 level is less than 85%, it indicates that sufficient oxygen is not reaching the cells and tissues.
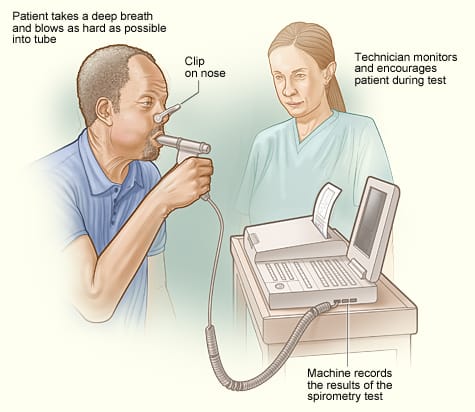
Spirometry:
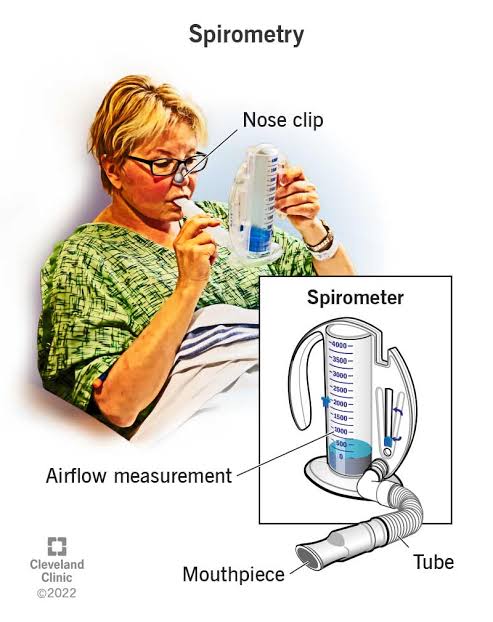
- Spirometry is a type of lung function test that measures the amount of air we inhale and exhale, as well as the rate (flow) at which we inhale and exhale.
- A spirometry test uses a spirometer instrument to which a mouthpiece is connected through a tube, and through this mouthpiece the patient is asked to inhale and exhale air, and the changes in the spirometer are observed.
- The nose is clipped while performing this test.
- Spirometry can be used to assess respiratory conditions such as asthma and COPD.
Pulmonary function test:
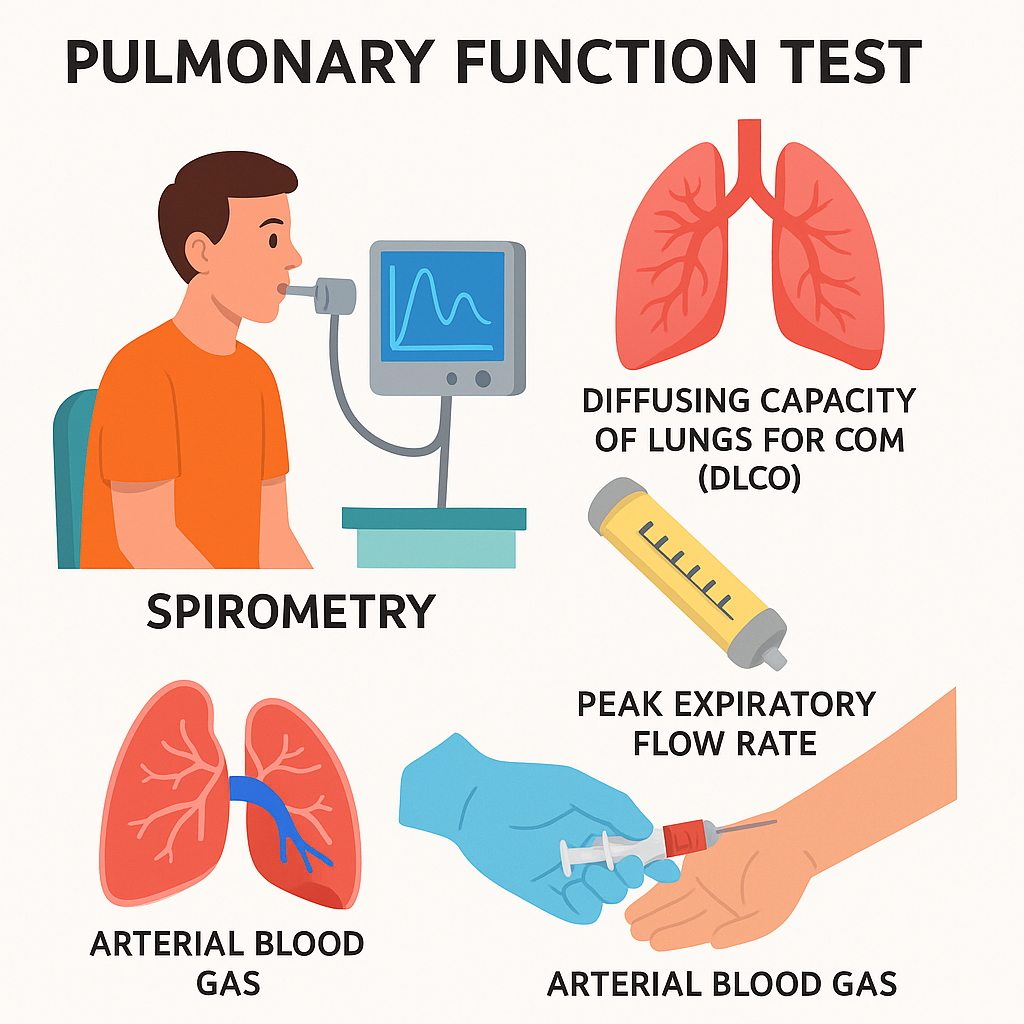
- Pulmonary function tests are a group of tests that measure how well the lungs work.
- These include spirometry, lung diffusion tests, lung volume tests, and exercise tests.
- Pulmonary function tests measure lung volume, capacity, Measures flow rate and gas exchange.
- Pulmonary function tests are used to diagnose certain types of lung disease. Like asthma, emphysema
Arterial blood gas analysis (ABGs):
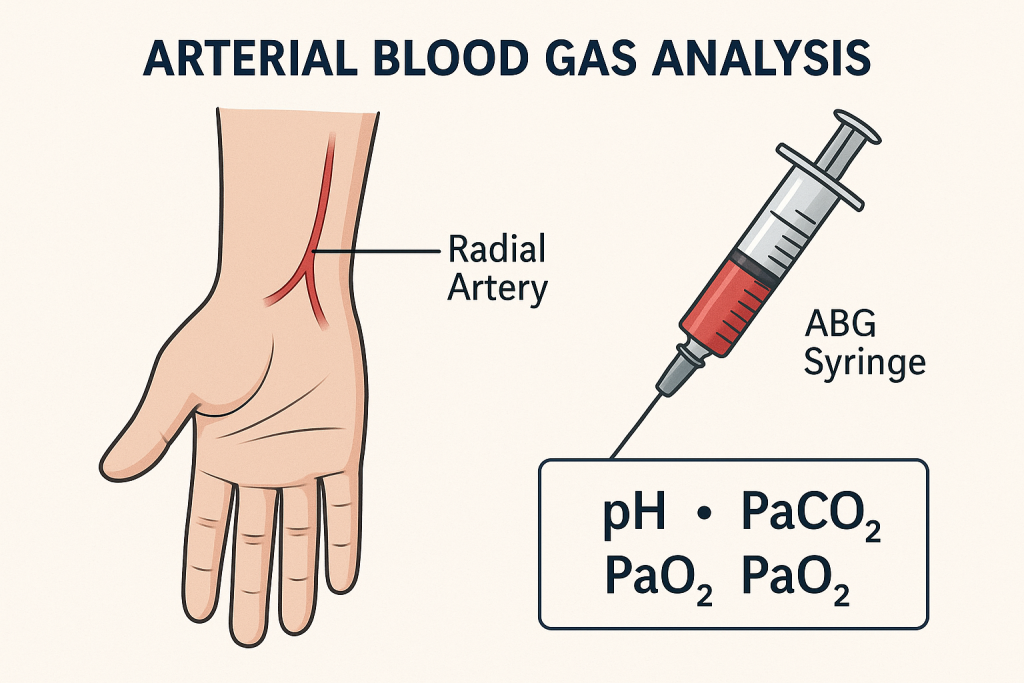
- Arterial blood gas analysis is an important It is a diagnostic method. It measures the levels of oxygen and carbon dioxide in the blood, as well as blood pH and blood bicarbonate levels.
- In which blood is mainly collected from the radial artery by expert health care personnel, in addition, blood is often collected from the brachial or femoral artery. (Blood is not collected from a vein)
- This test measures the lungs’ capacity to dissolve oxygen in the blood and remove carbon dioxide from the blood.
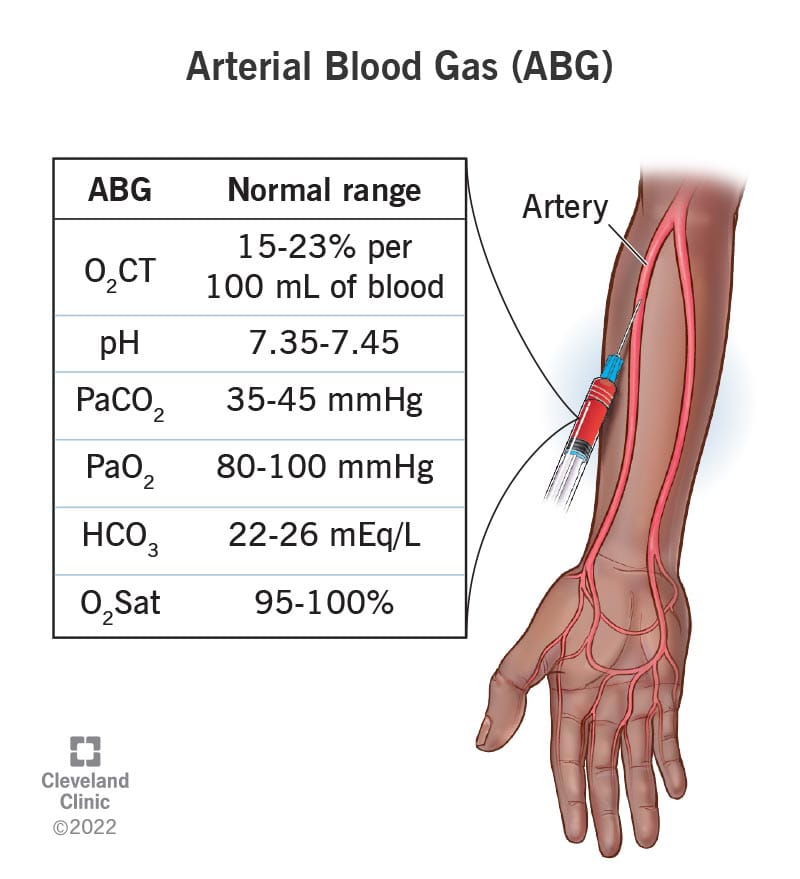
- Before this test, the Allen test is performed, which is used to check the patency of the arteries supplying blood to the hand (radial and ulnar arteries). Normal value of ABGs (Normal value of ABGs)
partial pressure of oxygen – Pao2
• 75 – 100 mmHg
Partial pressure of carbon dioxide – Paco2
• 35 – 45 mmHg
PH : 7.35 – 7.45
Bicarbonate – Hco3-
• 22 – 26 mEq/L
Oxygen content – O2CT
• 15 – 23% per 100 ml of blood
Oxygen saturation
• 95 – 100%
- Abnormal ABGs values indicate respiratory and metabolic disorders.
Culture:
- Cultural tests include blood culture and sputum culture. So that it can be identified which type of microorganism it contains
Sputum studies:

- Sputum study involves the study of sputum (mucus cough) to identify bacteria, viruses, and abnormal cells present in the sputum. Sputum study can be used to identify conditions like pneumonia and tuberculosis.
Imaging studies:
- Imaging studies are performed to evaluate anatomical structures.
- These include X-rays, CT scans, M. R. I., angiography, and ventilation perfusion lung scans.
Chest x-ray:
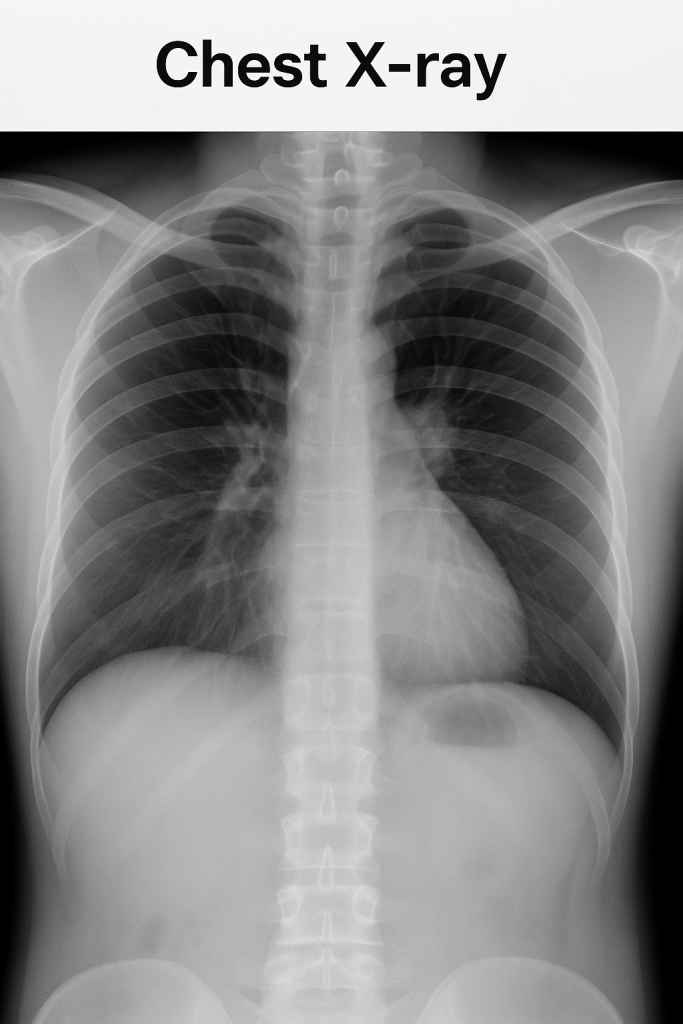
- A chest X-ray uses a small amount of X-rays to create a 2D image of the area and can visualize bones and tumors.
- It mainly takes an anterior-posterior and lateral side view.
- Before taking the X-ray, the patient is asked to inhale fully so that the lungs can be visualized well.
- X-rays can be used to identify pneumonia, lung cancer, tumors, foreign bodies, and rib fractures.
CT-scan:
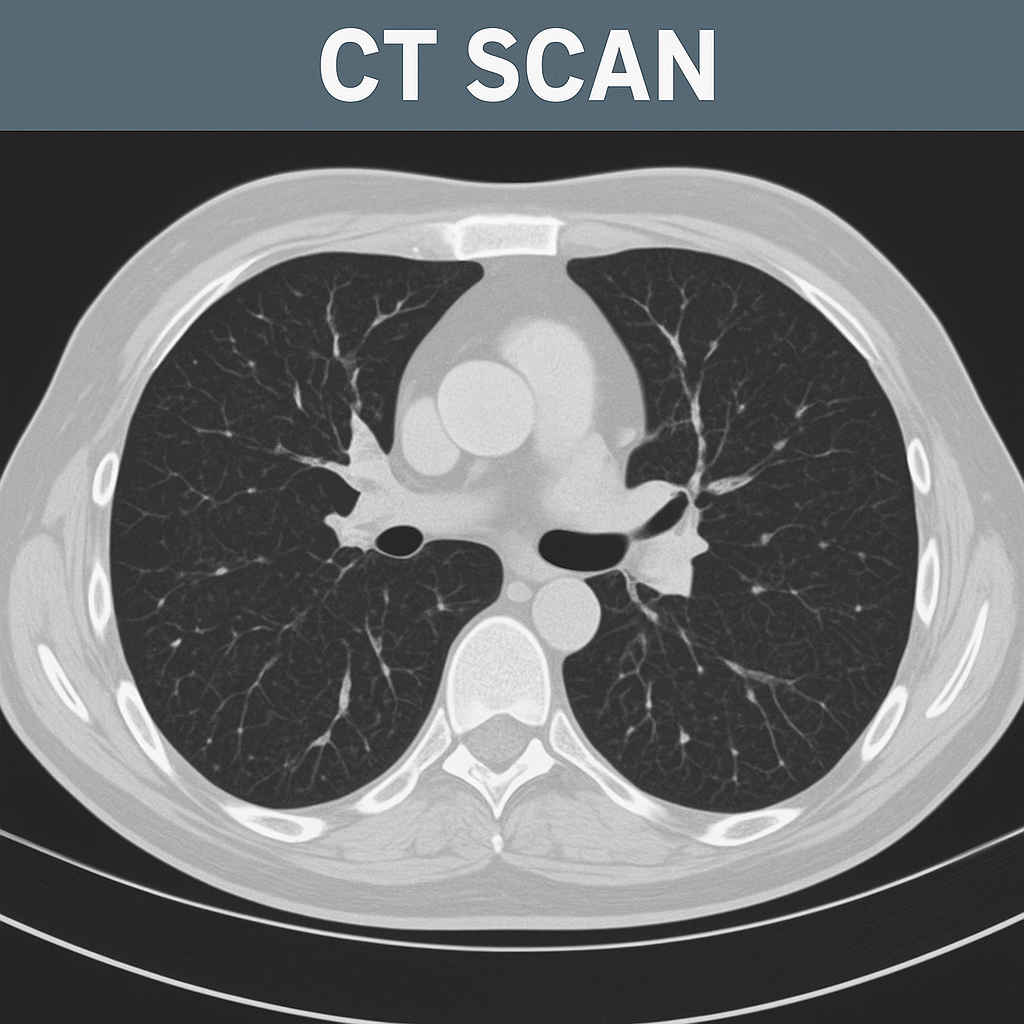
- A CT scan is an imaging study that provides more detailed information than an X-ray and provides a 3D image.
- A CT scan takes X-rays from different angles of the body and uses a computer to create a cross-sectional picture of the body.
- A CT scan can help determine the condition of organs and soft tissues.
- A CT scan can identify lung cancer, pulmonary embolism, and infection.
MRI:
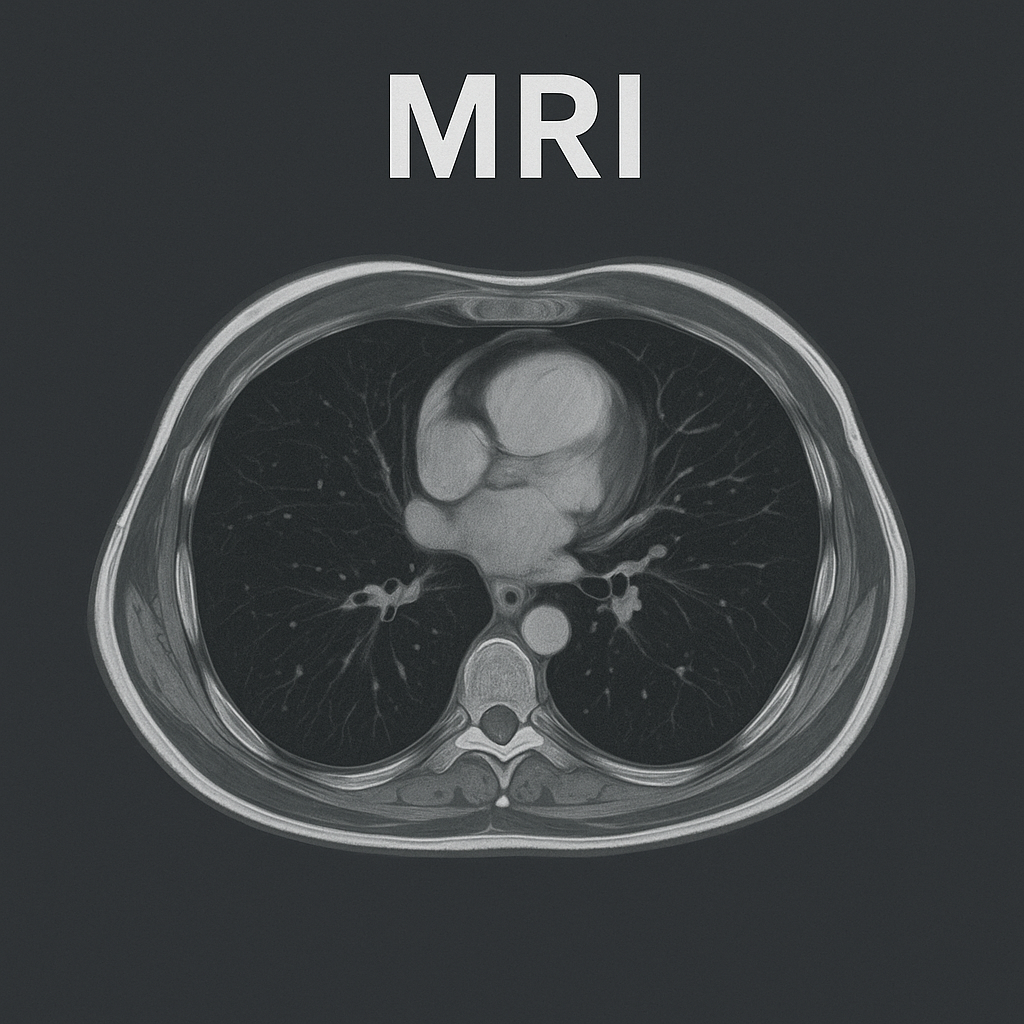
- MRI – Magnetic Resonance Imaging
- MRI uses powerful magnets and radio waves to create a cross-sectional image of a given area.
- MRI provides detailed information about the heart, lungs, and blood vessels.
- MRI can detect pulmonary nodules, fibrosis, pleural disease, and vascular abnormalities.
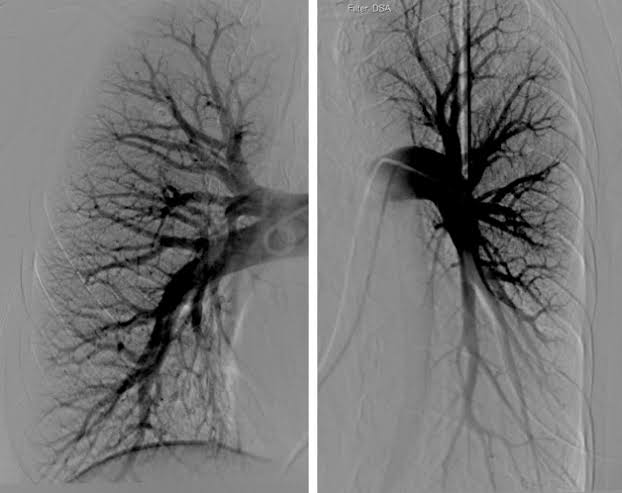
Pulmonary angiography Angiography):
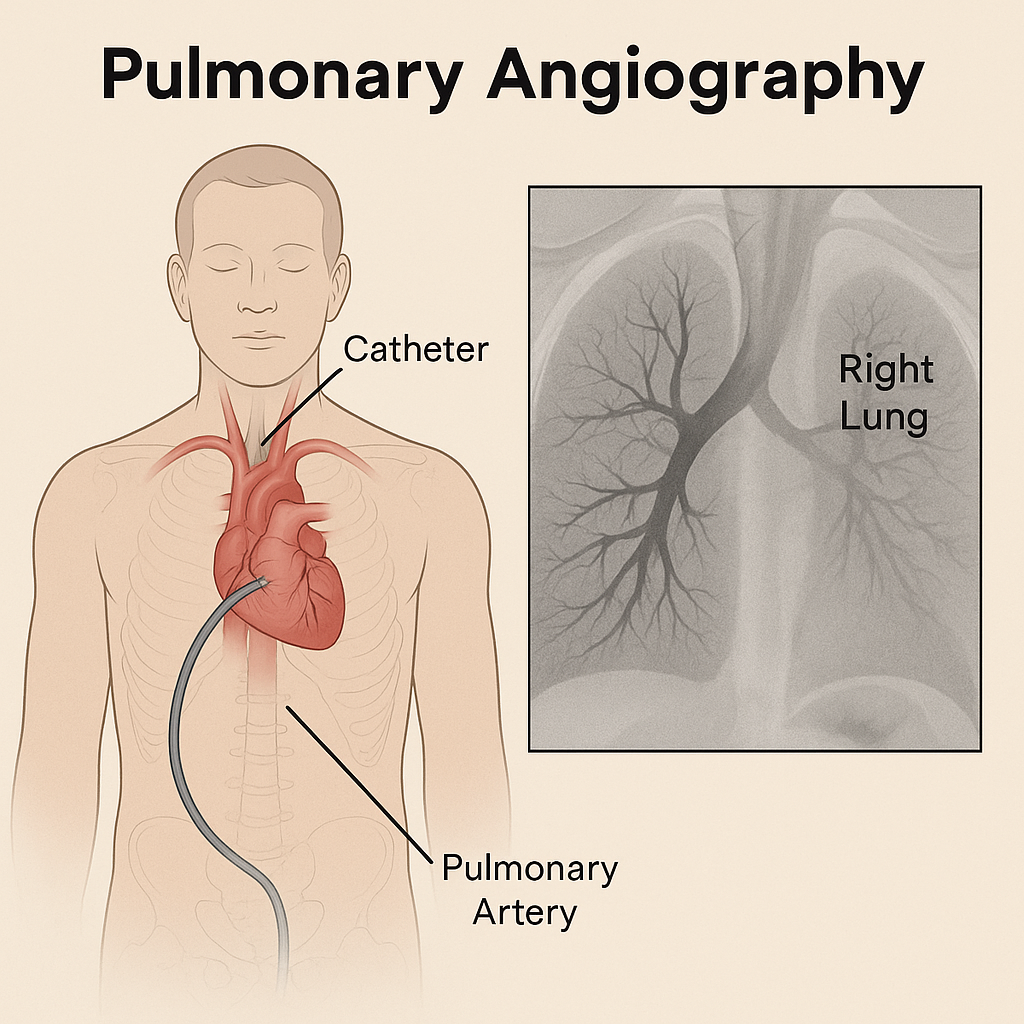
- This is an invasive fluoroscopic procedure that can be used to visualize the pulmonary veins and pulmonary arteries. is.
- In which contrast dye is injected into the femoral artery or pulmonary artery with the help of a catheter and the pulmonary vessels are visualized and studied.
- With the help of pulmonary angiography, pulmonary embolism, pulmonary vascular, pulmonary hypertension and abnormalities of the pulmonary vascular tree can be detected and pulmonary blood flow, blockage, pressure and abnormalities are evaluated.
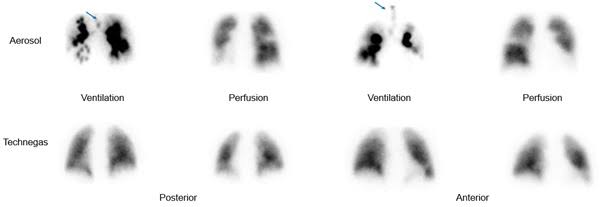
Ventilation perfusion lung scan:
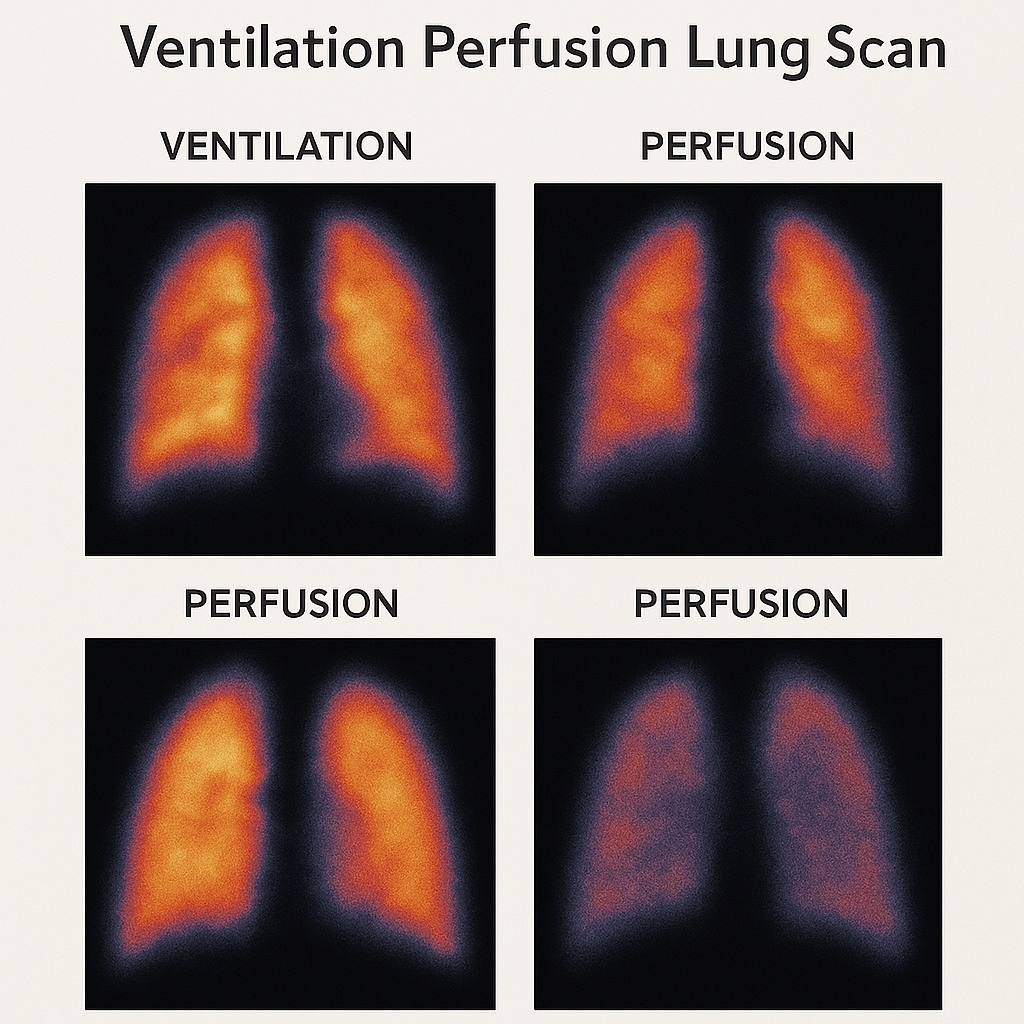
- A ventilation perfusion lung scan is a nuclear medicine test that evaluates the air flow and blood flow of the lungs.
- In which radioactive Substances are inhaled and used to measure air flow. Similarly, radioactive substances are administered intravenously to measure blood flow.
Endoscopic procedure:
- Endoscopic procedures involve direct inspection and examination of organs using an endoscope.
- Endoscopic procedures include bronchoscopy and thoracoscopy.
Bronchoscopy:

- Bronchoscopy involves the direct inspection and examination of the larynx, trachea, bronchi, and bronchioles using a bronchoscope.
- In which a bronchoscope is inserted into the airway through the nose or sometimes the mouth and the organ is visualized through the light and small camera in the bronchoscope and the secretions and tumors present in it are identified.
- In addition, secretions and foreign bodies present in the trachea-bronchial tree can be removed.
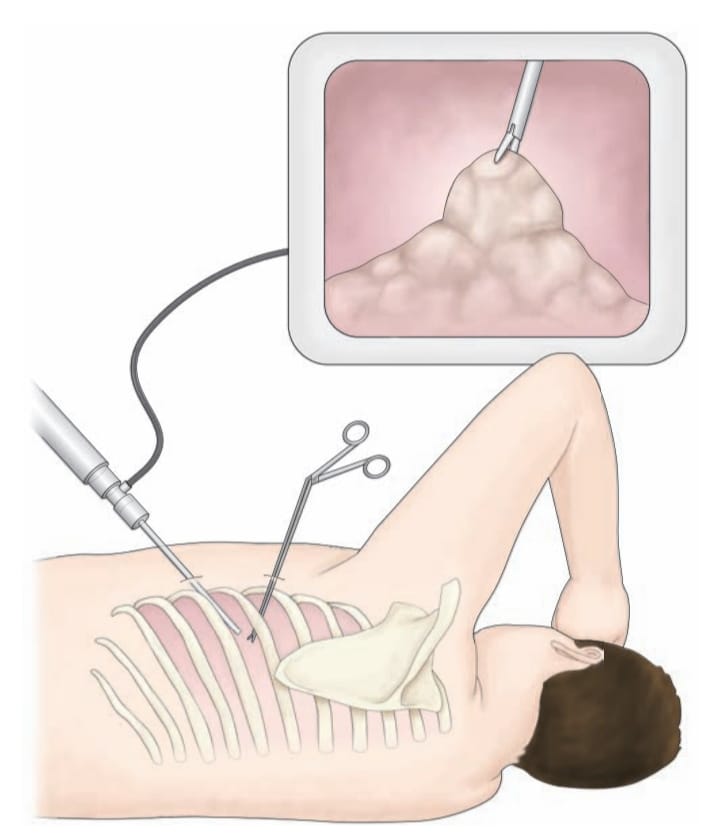
Thoracoscopy:
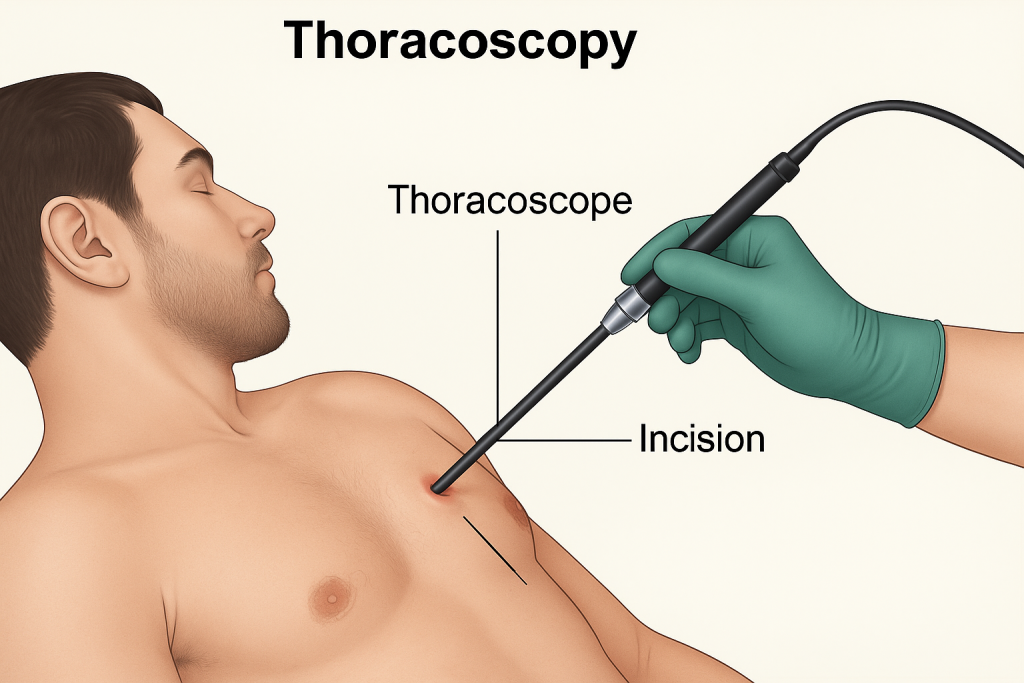
- Thoracoscopy is a diagnostic procedure in which the pleural cavity is examined with the help of an endoscope.
- In this procedure, a small incision is made in the chest wall and through this incision, an endoscope is inserted into the pleural cavity and a direct examination of that area is done.
- This specialized endoscope has a narrowing tube and the thoracic area is visualized through the camera and light in it.
- Thoracoscopy can be used to diagnose pleural effusion, pleural disease and staging of tumors. In addition, biopsies are also collected using thoracoscopy.
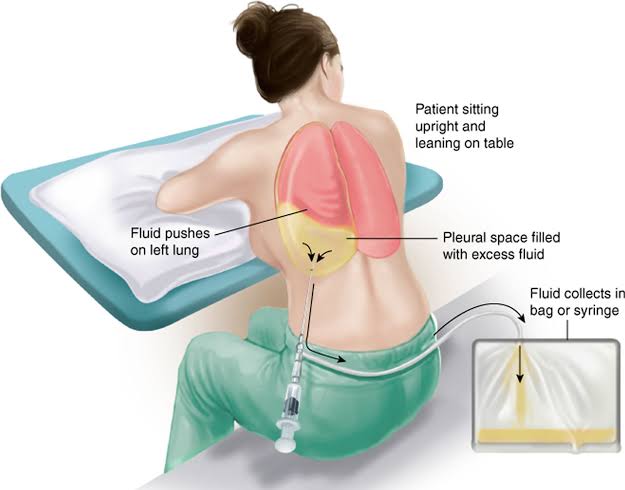
Thoracocentesis:
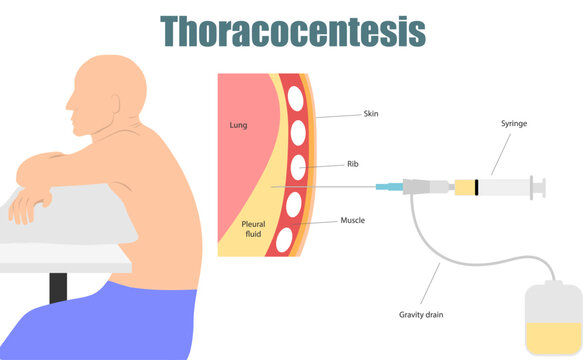
- Thoracocentesis is a diagnostic and therapeutic procedure.
- In which fluid is aspirated from the pleural space between the lung and the chest wall using a needle or plastic catheter and this pleural fluid is analyzed.
- Normally, a small amount of pleural fluid is present in the pleural space. If present in large quantities, it indicates a disease condition.
- The pleural fluid is studied for Gram stain culture and sensitivity, acid fast sensitivity and culture, differential cell count, cytology pH, specific gravity and total protein.
- This procedure is performed under the guidance of ultrasound.
Biopsy:
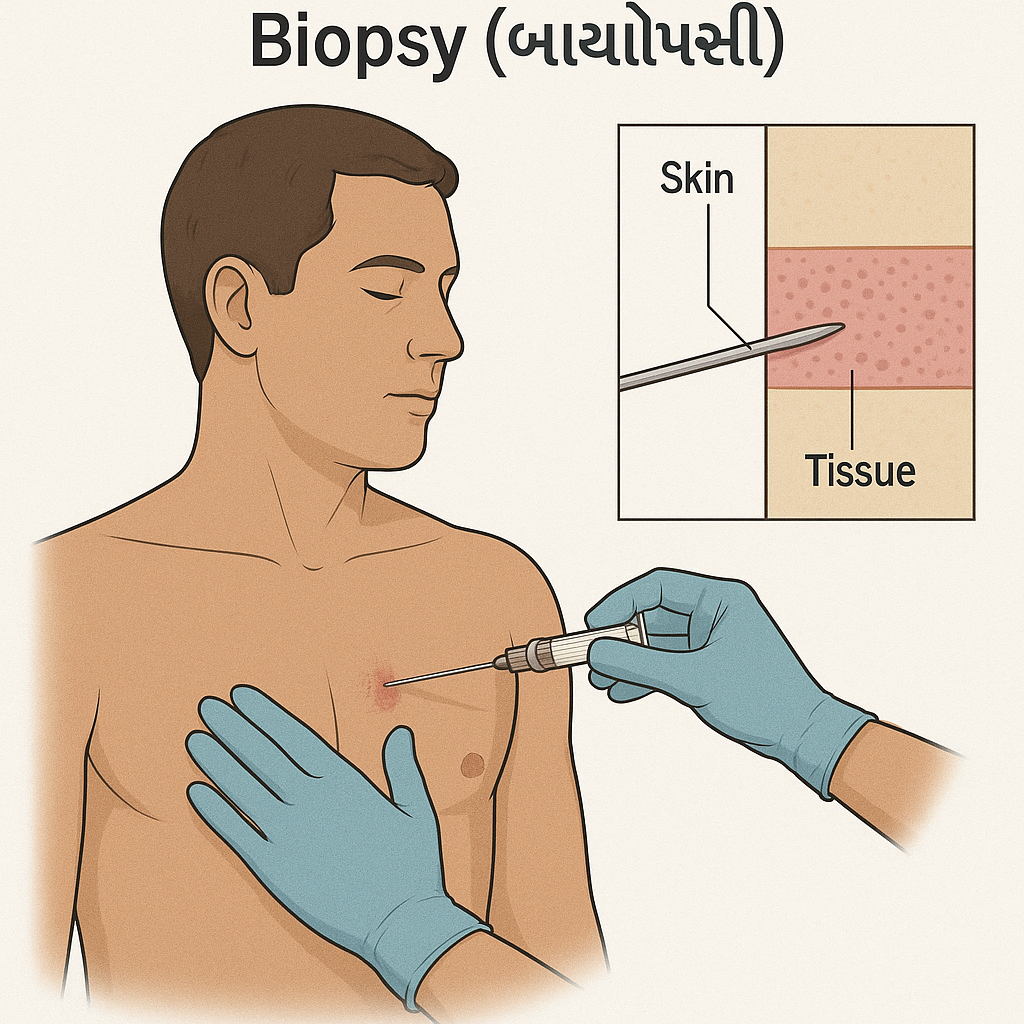
- In a biopsy, a small sample of tissue is collected from the suspected area and examined microscopically. So that it can be identified whether malignancy is present or not.
Pleural biopsy:
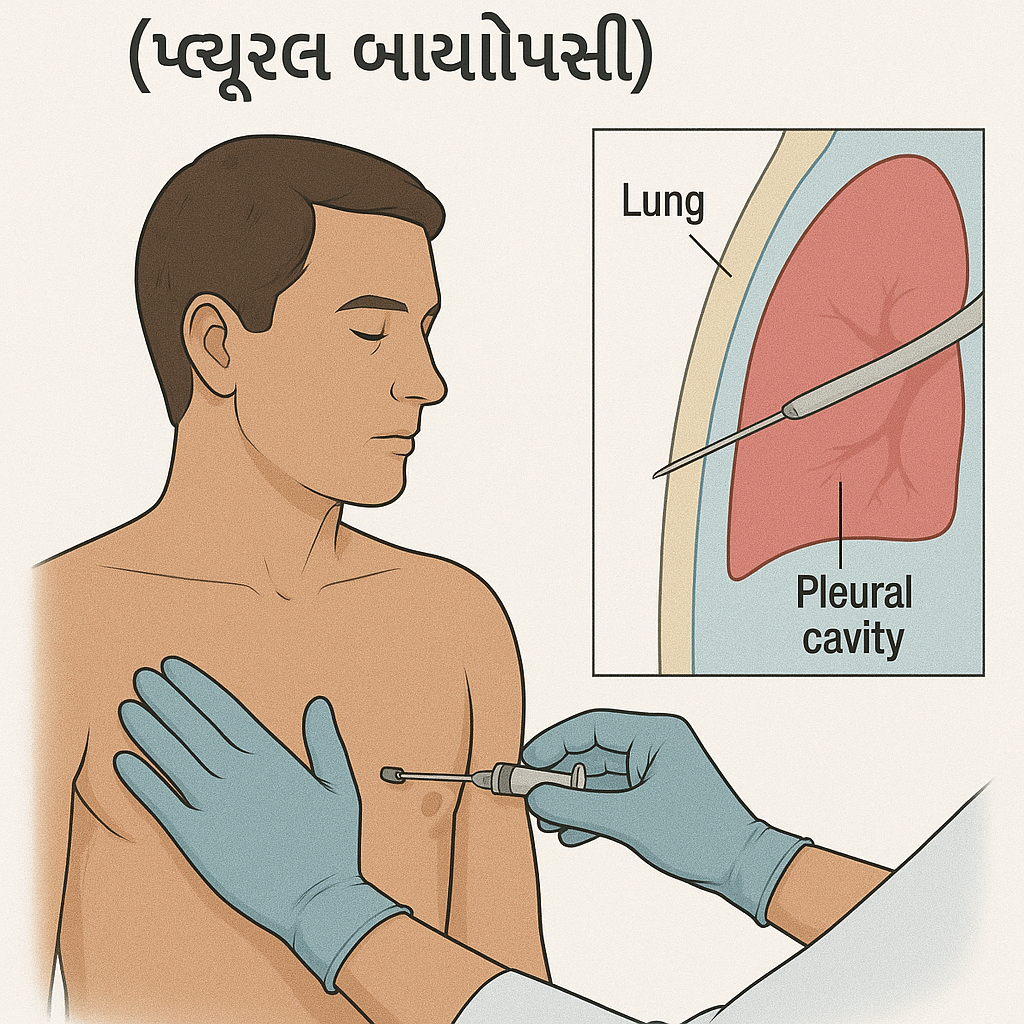
- A pleural biopsy involves collecting a small sample of tissue from the pleura.
(The thin membrane that lines the lungs and chest cavity is called the pleura). - A pleural biopsy is collected using a needle biopsy or thoracoscopy.
Lung biopsy:
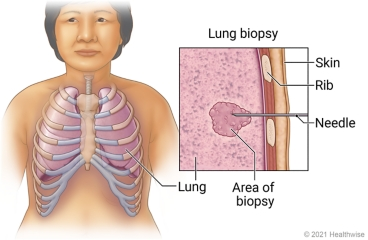
- A lung biopsy involves collecting a sample of lung tissue from the lungs and examining it. So that lung cancer, lung infection and disease can be identified.
Different methods are used to collect lung biopsy:
- Bronchoscopic biopsy
- Open lung biopsy
- Mediastinoscopy
- Needle biopsy

Common nursing diagnosis & care for respiratory disorders :

1.Impaired gas exchange related to bronchospasm
Improve gas exchange:
(Improve gas exchange)
- Monitor vital signs.
- Assess respiratory rate, rhythm, and breathing pattern.
- Breath sounds and chest movement Assess.
- Monitor pulse oximetry and arterial blood gas values.
- Provide the patient with a Fowler position and restrict his/her activity.
- Explain and encourage the patient to do deep breathing and cuffing exercises.
- Provide the patient with knowledge about pursed lip breathing and diaphragmatic breathing.
- If secretions are present, encourage the patient to expectorate.
- If SpO2 levels are low, provide oxygen therapy.
- Provide nebulization to the patient.
- Administer the medicine (bronchodilator) prescribed by the doctor.
- Maintain records and reports.
2.Ineffective airway clearance related to bronchoconstriction, increased mucus production as evidenced by hypoxia, hypercapnia, abnormal ABG
Maintain patent airway:
(maintaining airway patent)
- Monitor vital signs.
- Provide knowledge about pursed lip breathing and diaphragmatic breathing to the patient.
- Encourage the patient to expectorate if secretions are present.
- Provide oxygen therapy if SpO2 levels are low.
- Assess respiratory rate, rhythm, and breathing pattern To do.
- Assess breath sounds and chest movement.
- Monitor pulse oximetry and arterial blood gas values.
- Provide the patient with a Fowler position and restrict his/her activity.
- Explain and encourage the patient to do deep breathing and cuffing exercises.
- The patient Provide nebulization.
- Administer prescribed medicine (bronchodilator) by the doctor.
- Maintain records and reports.
3.Ineffective breathing patterns related to shortness of breath, mucous production, bronchospasm.
Improve breathing patterns:
(Improve breathing patterns)
- Monitor vital signs.
- Monitor pulse oximetry and arterial blood gas values.
- Provide the patient with a Fowler position and restrict his/her activity.
- Explain and encourage the patient to do deep breathing and cuffing exercises.
- Give the patient a pursed lip Provide knowledge about breathing and diaphragmatic breathing.
- Encourage the patient to expectorate phlegm if secretions are present.
- Assess respiratory rate, rhythm, and breathing pattern.
- Assess breath sounds and chest movement.
- Provide oxygen therapy if SpO2 levels are low.
- Provide nebulization to the patient.
- Administer the medicine (bronchodilator) prescribed by the doctor.
- Maintain records and reports.
4.Acute pain related to inflammatory condition of lung
Relieve Pain
(relieving pain)
- Pain Assess the level.
- Assess the location, duration, and intensity of the pain.
- Assess the factors that trigger the pain.
- Provide the patient with a comfortable position.
- Provide the patient with warm moist compression.
- Provide the patient with mind diversional therapy. So that the patient’s attention is diverted from the pain.
- Advise the patient about relaxation therapy.
- Administer the prescribed analgesic medicine.
5.Knowledge deficit related to disease condition and it’s prognosis
Improve knowledge level
(Improving knowledge level)
- Assess the patient’s condition.
- Assess the patient’s knowledge about the disease condition and its treatment.
- Provide the patient with knowledge about the disease condition and its prognosis.
- Provide knowledge in a language that the patient can understand.
- Resolve the patient’s doubts and concerns.
6.Anxiety related to disease condition and hospitalization.
Reduce Anxiety
(relieving anxiety)
- Assess the patient’s condition.
- Pay attention to the patient’s psychological needs and listen carefully to the patient.
- Encourage the patient to express his feelings, discomfort and anxiety.
- Resolve all the patient’s doubts and queries.
- Educate the patient about his condition and Provide knowledge about the treatment so that his anxiety is removed and the patient becomes confident.
- Provide psychological support to the patient.
- Provide mind diversionary therapy and recreational therapy to the patient.
7.Activity intolerance related to fatigue and dyspnea.
Enhanced activity level
(Increase activity level)
- Assess the patient’s condition.
- Check the patient’s activity level.
- Provide education to the patient to take rest initially.
- Then gradually encourage the patient to do range of motion exercises.
- Assist the patient with his/her activities.
- Encourage the patient to take rest between activities Provide education for
- Check whether the patient experiences any breathing difficulty during activity.
- If breathing difficulty is observed, stop the patient’s activity and provide education to take rest.
