ENGLISH-unit-7-msn-1- Management of patient undergoing surgery-UPLOAD
Management of patient undergoing surgery (Management of patient undergoing surgery):

Peri Operative Nursing:

Introduction (Introduction):
- Perioperative Nursing is a specialized field of nursing in which care is provided to patients during the three main stages of surgery: Preoperative, Intraoperative, and Postoperative.
- The main aim of this nursing method is to ensure complete physical and mental comfort, safety, and effective treatment for the patient. The nurse’s function is not only to provide technological knowledge, but also to be a dedicated associate in the entire surgical process of the patient.
Three Phases of Peri Operative Period:
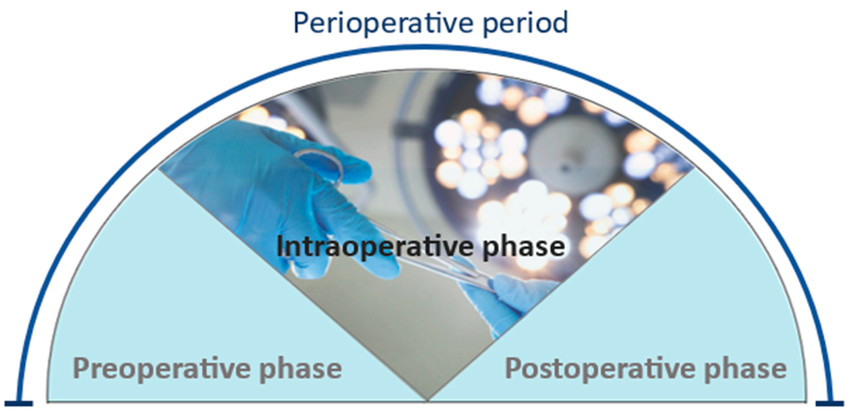
1.Preoperative Phase:
- This stage is the period in which the patient is selected for surgery and taken to the Operation Theater.
- Nurse Collects details like patient’s medical history, allergies and previous surgical experience. Evaluates laboratory reports, imaging and other diagnostic tests.
- Also, the nurse conducts a physical and psychological assessment of the patient, so that he can be fully prepared for the surgery. The patient is explained about anesthesia and educated about how the surgery is to be performed.
- Finally, informed consent is obtained from the patient and the NPO Pre-operative instructions such as (NPO – Nil Per Os) are explained.
2.Intraoperative Phase:
- This stage begins when the patient enters the operation theater and remains until the surgery is completed.
- The nurse maintains a sterile environment in the operating room and prepares all the instruments and machinery required for the surgery. The patient is positioned properly so that no skin, nerve or muscular injury occurs.
- The circulating nurse coordinates the processes inside and outside the operating room. Scrub Nurses work on sterile fields and handle instruments.
- The patient’s vital signs such as blood pressure, heart rate, oxygen saturation, etc. are continuously monitored. The nurse coordinates with the anesthesia team and continuously monitors the patient’s condition.
3. Postoperative Phase:
- This stage begins after the surgery is complete and continues until the patient has completely recovered.
- After surgery, the patient is taken to the Post Anesthesia Care Unit (Post Anesthesia Care Unit – PACU) or Recovery Room. There, nurses monitor vital signs, administer necessary medication for pain management, and perform wound care.
- The incision site is checked and observed for any signs of infection. It helps to mobilize the patient so that the risks like bedsores, thrombosis can be reduced.
- Then the nurse provides proper education to the patient and his family members for discharge instructions, medicine, diet and follow-up.
Role of Peri Operative Nurse:
- The perioperative nurse is responsible for the holistic care of the patient. Initially, the nurse conducts a detailed assessment of the patient. Then, a care plan is prepared, taking into account the patient’s physical, mental, and medical needs.
- The nurse implements the plan and evaluates its results.
- The perioperative nurse maintains effective communication with the patient, family, and health care team.
- The nurse also works as an advocate for the patient’s rights and safety. Proper and timely documentation of all care activities also falls under the responsibility of the nurse.
Importance of Peri Operative Nursing:
- Perioperative nursing is very important for the success and safety of the patient’s surgical study.
- It prepares the patient physically and mentally, reduces risks during surgery, and helps in faster recovery during the subsequent recovery.
- The patient receives quality care through pain management, infection prevention, and clinical monitoring.
- As well as Psychological support is also provided to strengthen the patient’s morale and self-confidence.
- Perioperative nursing is not just a nursing method that provides care during surgery, but a service with a broad, scientific and humanistic perspective.
- The contribution of perioperative nurses to the holistic health of the patient is important. A nurse is not just a caregiver – she acts as an educator, ally, and a safety net for the patient.
- Perioperative nursing is extremely effective and essential in improving the patient’s quality of life and improving surgical outcomes.
Pre-operative Assessment of Patient:

Introduction:
- Preoperative assessment That is, evaluating the patient’s complete medical condition before the operation. The main aim of this process is to ensure that no complications arise during or after the surgery and that the patient has a safe and successful surgery. This assessment is done through a multidisciplinary approach involving a surgeon, anesthesiologist, nurse and other medical staff.
1. Medical History:
- It is important to know the patient’s complete medical history. This includes the following:
- Potential chronic diseases such as heart disease, hypertension, diabetes mellitus, asthma, kidney disorder.
- Previous surgery and reactions to anesthesia.
- Current medications, vitamins, herbal supplements.
- Allergies – especially to medications, Latex or food allergy.
2. Physical Examination:
- The patient’s complete body is examined
- In which special attention is paid to:
- vital signs: Blood Pressure, Pulse Rate (Pulse Rate), Respiratory Rate and Temperature.
- Heart and Lung Function
- Airway Assessment: Especially necessary for anesthesia.
3.Laboratory and Diagnostic Tests:
- Blood Tests: CBC (Complete Blood Count), RFT (Renal Function Test), LFT (Liver Function Test), Blood Sugar Level.
- Urine Analysis
- Electrolytes
- ECG (ECG – Electrocardiogram)
- X-ray Chest (X-ray Chest)
- Echocardiography, Stress Test – if needed.
4. Anesthesia Risk Evaluation:
- The patient’s suitability for anesthesia is assessed by the anesthesiologist. It uses the ASA Classification which measures surgical risk according to the patient’s health status.
5. Medication Management:
- Where necessary, specific medications such as blood thinners, insulin, etc. need to be stopped or adjusted before surgery.
6. Counseling and Informed Consent:
- Patients are given complete information about their illness, the surgery to be performed, the possible risks, and the follow-up. Later, informed consent is taken, which is very essential from a medical point of view.
7.Nutritional and Psychological Assessment:
- Nutritional status is observed – especially if the patient is malnourished.
- It is also necessary to check whether the patient is psychologically ready for surgery or not.
8.Special Considerations:
- Special care needs to be taken for Pediatric, Pregnant Women, Geriatric Patients.
- In special cases like Organ Transplant or Oncological Surgery, advance assessment may be necessary. is.
- Pre-operative assessment is an essential step for the success of surgery. It is not just a formality, but an important basis for saving the patient’s life. It is essential for every member of the medical team to understand and implement this process so that the patient can have a safe and successful surgery.
Pre-Operative Assessment of Patient:
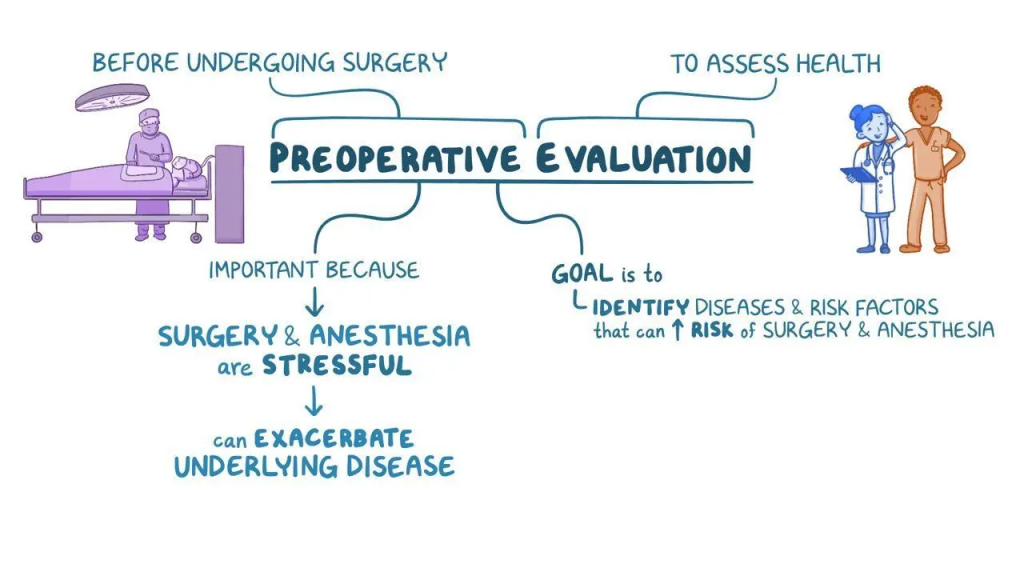
Meaning:

- Pre-operative assessment is the assessment of the patient’s health status, body systems, psychological condition before surgery. Pre-operative assessment is the assessment of the patient’s health status, body systems, psychological condition and social background Background) function to perform a comprehensive evaluation.
- Its main aim is to ensure that the patient is physically and mentally ready for surgery and to prevent complications during or after surgery.
1) Subjective Data:

- Subjective data is verbal information obtained directly from the patient.
- It includes information on chief complaint, present illness, duration, severity, relieving and aggravating factors.
- Whether the patient has a history of previous surgery, complications during anesthesia, allergies, or blood transfusions. Ask.
- It is important to know about the patient’s daily routine habits such as smoking, alcohol intake, sleep pattern and dietary habits.
2) Psychosocial Assessment:

- Evaluate the patient’s psychological state and social support system.
- Check whether the patient has fear, anxiety, or depression regarding the surgery.
- The support of the patient’s family or caregiver is also important.
- If necessary So, to prepare the patient mentally for the surgery by giving counseling.
3) Past Health History:

- Get details of previously occurring chronic diseases such as hypertension, diabetes mellitus, coronary artery disease, asthma, tuberculosis, seizure disorder, thyroid dysfunction, bleeding disorder, etc.
- If there has been any previous hospitalization or previous surgery, record its nature and outcome.
4) Family Health History:

- Ask about a family history of illnesses such as hypertension, diabetes, asthma, heart disease, bleeding disorder, cancer, anesthesia reaction, or malignant hyperthermia.
5) Medications:

- Write the details of all the medications the patient is currently taking:
- Antihypertensives (antihypertensives), Antidiabetic drugs (antidiabetic), Anticoagulants (anticoagulants), corticosteroids (corticosteroids), Antidepressants (antidepressants), Antibiotics (Antibiotic).
- Record the dose, frequency, and last dose timing of medications. If there is a drug allergy, write it down clearly.
6) Assessment of Body Systems:
a) Cardiovascular Assessment:
- Assess the patient’s heart rate, rhythm, blood pressure, jugular venous pressure, and edema.
- Perform ECG and echocardiography if necessary.
- Ask about history of chest pain, palpitation, and orthopnea.
b) Respiratory System (Respiratory System):

- Respiratory rate (Respiratory rate), oxygen saturation (SpO₂), breath sounds (Breath sound), cough (Cough), sputum (Sputum) and dyspnea should be assessed.
- Chest X-ray and Pulmonary Function Test (PFT) should be performed as required.
c) Nervous System:
Check level of consciousness, orientation, cranial nerves, motor and sensory function, and reflexes.
Note if there is a seizure disorder or neurological deficit.
d) Urinary System (Urinary System):
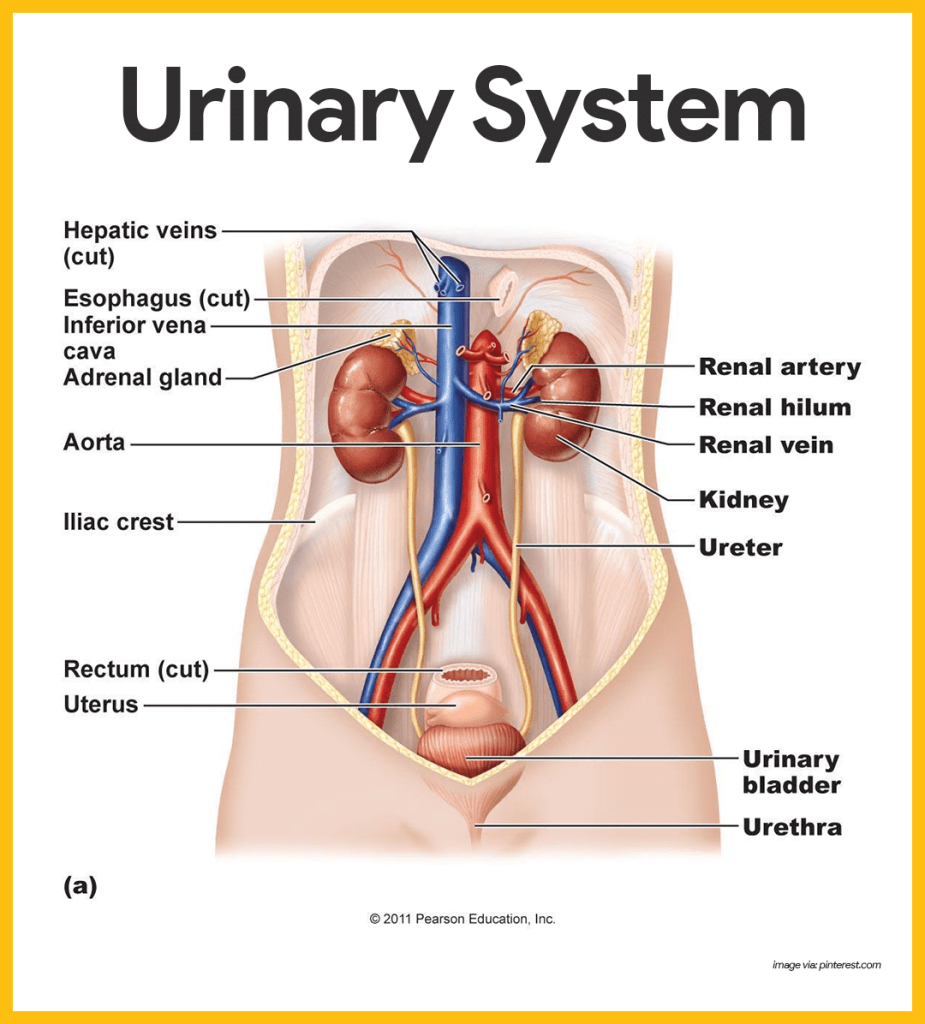
- Urine output, color, frequency, dysuria or hematuria (Hematuria) to look for.
- Ask for a history of urinary tract infection.
e) Renal Function Test:
- Serum creatinine, Blood Urea Nitrogen : BUN and electrolytes.
- It shows the filtration capacity of the kidneys.
f) Hepatic System:
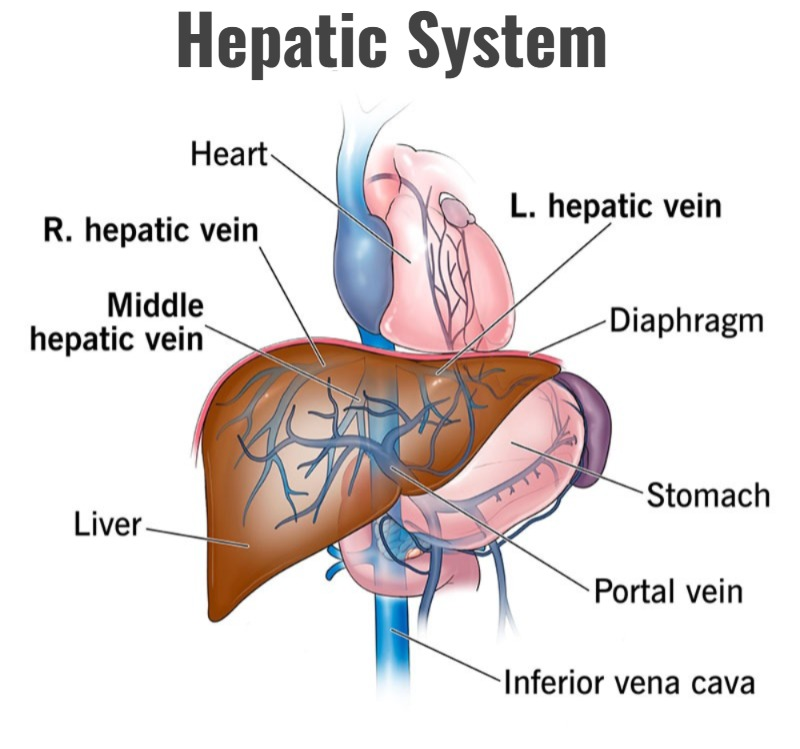
- Look for symptoms like jaundice, itching, ascites, hepatomegaly.
- Alcohol consumption Ask for a history of alcohol consumption and hepatitis.
g) Liver Function Test : LFT (Liver Function Test):
- To check AST (AST), ALT (ALT), ALP (ALP), bilirubin (bilirubin), albumin (albumin), prothrombin time – PT (prothrombin time) and INR (INR).
- These show the functional ability and coagulation ability of liver cells.
h) Integumentary System:
- Skin integrity Check for integrity, rash, ulcer, pressure sore.
- Choosing the right place for IV line or incision site.
i) Musculoskeletal System:
- To check joint mobility, deformity, stiffness and contracture.
- To perform proper evaluation for positioning.
j) Endocrine System:
- Check for diabetes mellitus, thyroid disorder, adrenal insufficiency.
- Get blood glucose and thyroid function test done.
k) Immune System:

- Check recent infection, fever, immunosuppressive drugs and vaccination status.
l) Nutritional Status:

- Body Mass Index – Assess BMI, weight loss, serum albumin, and dietary habits.
- Malnutrition slows wound healing.
7) Common Pre-Operative Diagnostic Tests:

- Complete Blood Count CBC (Complete Blood Count)
- Blood Group & Cross-Match (Blood Group and Cross-Match)
- Blood Sugar Test (Blood Sugar Test)
- Serum Electrolytes (Serum Electrolytes)
- Renal Function Test : RFT (Renal Function Test)
- Liver Function Test : LFT (Liver Function Test)
- Chest X-ray (Chest X-ray)
- Electrocardiogram : ECG
- Coagulation Profile : PT, aPTT, INR
- Urine Analysis
- Arterial Blood Gas : ABG
- Pregnancy Test
8) Additional Pre-Operative Preparation:
- Nil per oral : NPO (Nil per oral) : Stop eating and drinking before surgery.
- Informed consent : Obtain consent from patient and family members.
- Pre-operative medications : anxiolytics, anticholinergics, antibiotics.
- Skin preparation – antiseptic cleaning (Antiseptic cleaning).
- IV line – keeping venous access ready.
- Thromboprophylaxis – measures to prevent deep vein thrombosis.
Pre-operative assessment is a systematic and comprehensive evaluation before surgery that involves observing the patient’s physical status, psychological state, nutritional balance, and systemic function.
It The aim is to make the patient safe for surgery, prevent complications and improve post-operative recovery.
Pre Operative Care:

- Preoperative care is the preparation and management done before surgery.
- Patients are admitted to the hospital to treat different physical conditions and different situations that require surgical intervention. The nurse is responsible for completing preoperative care and implementing the doctor’s orders, recording the care provided.
- Preoperative care consists of several components that are performed in the hospital before surgery. Many surgical procedures do not require admission.
- Reducing and correcting physiological and psychological problems that, if not corrected, can have an impact during surgery.
Providing surgery-related information to the patient (Giving surgery related information to the patient):

Giving demonstration and instruction of some post-operative exercises to the patient
- Physical Preparation
- Psychological preparation
- Physiological preparation
- Pre-medication
- Legal and Ethical Considerations Consideration)
- Operative preparation
The above preparations are done in pre-operative care.
Physical Preparation:

Physical Assessment in Physical Preparation
Medical History (Medical history):
- Take a history of any past medical conditions such as diabetes, hypertension, asthma, TB, myocardial infarction etc.
- Get information about any previous surgery.
- Get detailed information about any drug allergies.
General Examination (General Examination):
- Do a physical examination, including checking and recording vital signs.
Drug and alcohol use:
- A physical examination should be conducted to determine if there is a history of alcoholism. To know whether he/she is using any drugs or not.
Nutritional and fluid status:
- Assess and checks the nutritional status of the patient, looking for signs of obesity, weight loss, malnutrition, etc. If nutritional deficiency is found, correct it before surgery.
Respiratory status:
- Assess respiratory status as ventilation is potentially compromised during surgical treatment
- If the patient has a respiratory infection, the surgery is postponed.
- If the patient has a history of smoking, then it should be stopped one month before the surgery because it affects the course of the surgery.
Cardiovascular status:
- When preparing a patient for surgery The goal is that the cardiovascular system should function properly so that the whole body gets oxygen, fluid, and nutrition.
- If blood pressure is uncontrolled, surgery is postponed.
Hepatic and renal function:
- Before surgery, check whether the liver and urinary system are functioning well or not because of the medications, anesthetic agents, body waste and toxins that are being removed. Therefore, if this system works properly, it can remove waste.
Endocrine function:
- If the patient has diabetes, then he/she is at risk of hypoglycemia during surgery and glucose levels need to be checked frequently before, during and after surgery.
- Before surgery, check whether there are any diseases related to the endocrine system.
- Do bowel clearance if lower gastrointestinal tract surgery is involved.
- Sleeping on the night before surgery may be given to some patients.
- Prepare the skin before surgery. Order on S, clean it through a special shop and remove the hair from the surgical area.
To perform preoperative laboratory and diagnostic investigation:
Laboratory and diagnostic tests:
- Complete Blood Count CBC (Complete Blood Count CBC) Count)
- Blood Group & Cross-Match (Blood Group and Cross-Match)
- Blood Sugar Test (Blood Sugar Test)
- Serum Electrolytes (Serum Electrolytes)
- Renal Function Test : RFT (Renal Function Test)
- Liver Function Test : LFT (Liver Function Test)
- Chest X-ray (Chest X-ray)
- Electrocardiogram : ECG
- Coagulation Profile : PT, aPTT, INR
- Urine Analysis
- Arterial Blood Gas : ABG
- Pregnancy Test
Psychological preparation:

- Surgery related patients have anxiety and fear
- The patient should express his emotions with family members so that he feels good and his anxiety is relieved.
- Provide psychological support to the patient and his family members.
- Sometimes the surgery is postponed if the patient feels too insecure.
- The surgical procedure is not for the patient And explain to their family members so that we can reduce their fear.
- Spiritual belief plays an important role in coping with anxiety
Pre-medication:
- Anesthesia is administered in pre-operative care, it is administered using aseptic technique is.
Anti-emetic drug:
- Anti-emetic drug is given to prevent aspiration. For example, ondansetron
Sedative drug:
- Sedative drugs such as diazepam are given before surgery to prevent muscle hyperactivity.
- Intravenous fluids are given as per the doctor’s order.
- Prophylactic antibiotics are given.
- Antihypertensive drugs such as propranolol are given if needed.
- Also provide other prescribed medications such as diuretics, cardiac drugs, and current medication for the patient.
- Record the medications given.
Pre-operative preparation:
When the patient is ready for the operation, the surgeon orders pre-operative preparation. If it is an elective operation, then give the pre-operative order a day before.
Identify the patient and remove his hair from the surgical side, before the operation, and give a complete bath with antiseptic soap and Savlon the day before the surgery.
- Relieve anxiety
- Give enema for bowel care
- Do a pre-anesthetic checkup
- Take a pre-operative concert
Legal and ethical:

Informed consent (consent):
- Return consent from the patient or their guardian for surgery is a vital portion of preoperative care. According to the law, the physician who performs the procedure explains to the patient the risk factors and benefits of the surgery, as well as other treatment options.
- When the patient signs the consent form, the nurse acts as a witness. It is important that the patient understands what the surgeon has explained. Sometimes, the patient is asked to explain what was explained to him/her, which can be used to gauge how much the patient understood.
- If a patient is mentally impaired, heavily sedated, or in a critical condition, he/she is not legally able to give a consent form, so in such a situation, his/her spouse, adult child, or adult sibling signs the consent form.
- If the patient is under 18 years of age, his/her parents Signature in concert form.
Pre operative teaching:
- In operative teaching, explain to the patient about the pre-operative period, surgery time, and post-operative. Preparing for surgery in the pre-operative period.
- Explain to the patient how to prepare the day before surgery, e.g. giving an enema before surgery.
- Explain to the patient why they should not drink or eat for 8 to 12 hours before surgery, because there is a chance of vomiting aspirating due to the effects of anesthesia.
- Ask the patient to take a bath in the morning, remove all jewelry, makeup, eye glasses, dentures, etc. before going to the operation room.
- In operative teaching, explain to the patient about the pre-operative period, surgery time, and post-operative. Preparing for surgery in the pre-operative period.
- Explain to the patient how to prepare the day before surgery, e.g. giving an enema before surgery.
- Explain to the patient why they should not drink or eat for 8 to 12 hours before surgery, because there is a chance of vomiting aspirating due to the effects of anesthesia.
- Ask the patient to take a bath in the morning, remove all jewelry, makeup, eye glasses, dentures, etc. before going to the operation room.
- Explain the setup of the operation theater and recovery room to the patient. Asking his staff members to wear scrubs and masks.
- Telling the patient that after surgery he will be transferred to the recovery room and will be closely monitored there. Oxygen masks, blood pressure cuffs, and other monitoring equipment are attached there.
- Instructing the patient that breathing exercises can prevent complications.
- Pain management is a primary concern after surgery. Tell the patient to inform the medical staff when he or she feels pain, check his or her pain level using a pain scale, and use pain control methods based on that. Such as comfort positions, mind diversional therapy, music therapy, etc.
Immediately Before Surgery:
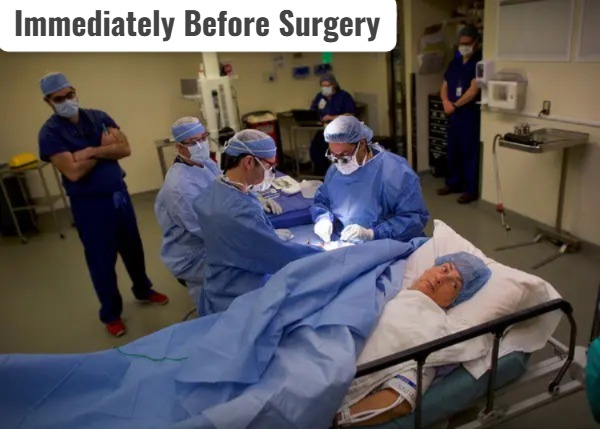
Definition:
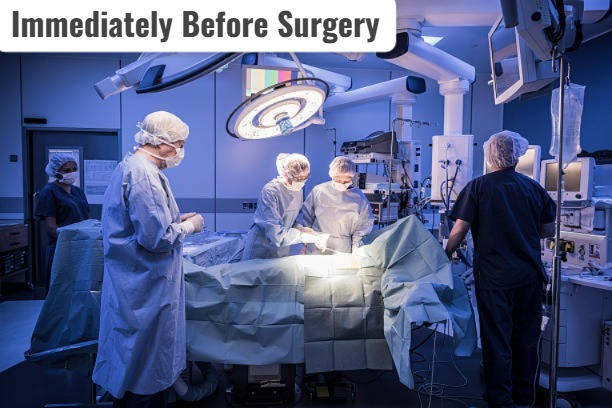
- Immediately before surgery means the period immediately before the start of surgery, in which final verification, assessment and preparation are done to completely prepare the patient.
- The purpose of this stage is to ensure that the patient is completely prepared for surgery physically, mentally and medically, and that no errors or complications occur.
1) Verification of Patient Identity:
- Completely verify the patient’s name, age, hospital ID, procedure and surgical site.
- Check whether the identification band is properly attached to the hand.
- Consent form signed and properly filled in Ensure that it is filled in the correct way.
2) Preoperative Checklist:
- Check the following in the preoperative checklist:
- All investigations reports are available or not.
- Vital signs: temperature, pulse, respiration, blood pressure.
- Allergies or hypersensitivity are clearly stated.
- All jewelry, dentures, contact lenses, and nail polish are removed.
3) Confirmation of Surgical Site and Procedure (Conformation of Surgical Site and Procedure):
- Check whether the surgical site is marked correctly by the surgeon.
- Verbally confirm the procedure name and site with the patient and the surgical team.
- Follow the time-out procedure as per the WHO Surgical Safety Checklist.
4) Preoperative Medication Administration:
- Giving the patient preoperative medications as ordered by the physician, such as –
- Anxiolytics – to reduce anxiety.
- Anticholinergics – to reduce secretion.
- Antibiotics – to prevent infection.
- Record the time and dose after giving the medication.
5) Vital Signs Monitoring:
To recheck the patient’s vital signs:
- Temperature
- Pulse
- Respiration
- Blood pressure
- Oxygen saturation – SpO₂
- Any reading If abnormal, inform the surgeon and anesthesiologist immediately.
6) Bowel and Bladder Preparation:
- If ordered by the physician, perform an enema or bowel cleansing.
- The patient should void before surgery. Ask to void so that the bladder remains empty.
- Indwelling catheter may be inserted if necessary.
7) Removal of Personal Items:
- Remove the patient’s jewelry, watch, ring, necklace, hairpins, contact lenses, nail polish, and dentures.
- Give all personal items to the patient’s relative and keep a record.
8) Skin Preparation:
- Clean the patient’s surgical area with an antiseptic solution.
- If necessary, perform shaving with sterile technique.
- Keep the skin clean and dry.
9) IV Line and Fluids:
- Insert an IV line into the patient.
- Start IV fluids such as Normal saline or Ringer lactate as ordered by the physician.
- Check the IV site for leakage (leakage) or redness.
10) Pre-Anesthetic Preparation:
- Evaluate the patient’s airway.
- Remove dentures and loose teeth.
- Complete the pre-anesthetic checklist.
- Ensure that oxygen supply, suction apparatus, and anesthesia machine are functional.
11) Psychosocial Support:
- Positively reassure the patient that the surgery will be safe.
- Give reassurance to reduce anxiety and fear.
- Behave with the patient sympathetically.
12) Transfer to Operation Theatre:
- Safely move the patient onto the stretcher.
- Maintain the patient’s privacy.
- Carry the identification slip and case file.
- Handover the patient to the OT nurse.
- Immediately before surgery Final verification of every aspect of the patient is done: identification, consent, vitals, medication, skin preparation, and transfer. Proper care at this stage can prevent complications during surgery and ensure the safety and comfort of the patient. Intraoperative care:
Intraoperative care:
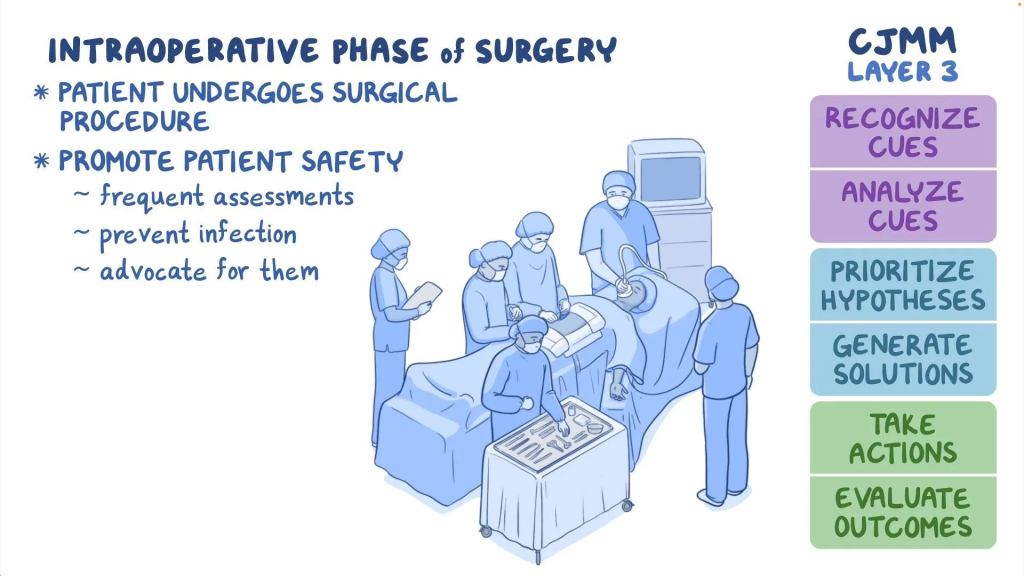
Definition:
- Intraoperative care is the comprehensive, safe, aseptic, and continuous nursing care provided to a patient during surgery, from incision to wound closure.
- Its purpose is to keep the patient safe under anesthesia, prevent infection, and position the patient properly. To do this, maintain vital signs and ensure that no complications occur during surgery.
- The purpose of intraoperative care is to maintain patient safety. Some goals include maintaining hemostasis during the procedure, maintaining strict sterile technique during the procedure to minimize cross-infection, and checking that the patient is secure on the operating table.
1) Preparation in Operation Theatre:

- Operation theatre should be clean, sterile and all instruments should be ready.
- Keep sterile instruments, drapes, suture material and medications ready.
- Anesthesia machine Check the anesthesia machine, suction apparatus and oxygen supply.
- Emergency drugs: adrenaline, atropine, epinephrine etc. should be available.
2) Patient Identification and Positioning:

- Assess patient identification by checking name, age, procedure, and consent.
- Provide appropriate position: such as supine, prone, lithotomy, or lateral position.
- Provide padding for patient safety to prevent pressure sores or nerve injury.
3) Maintenance of Aseptic Technique:

- Scrubbing, gowning and gloving should be done properly.
- Clean the patient’s surgical site with an antiseptic solution and apply sterile drapes.
- Maintain a sterile field during the operation and avoid contact with non-sterile objects.
4) Administration of Anesthesia:
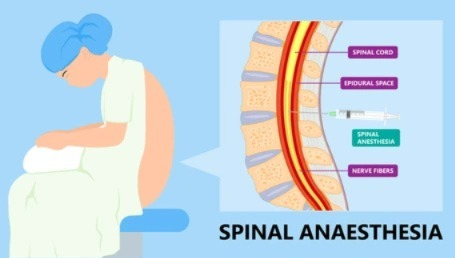
- General by Anesthesiologist General anesthesia, regional anesthesia, or local anesthesia are administered.
- Continuous monitoring of the patient’s airway, breathing, and circulation.
- Oxygen, IV fluids, and monitoring devices should be properly functional.
5) Monitoring of Vital Signs (Monitoring of vital signs):
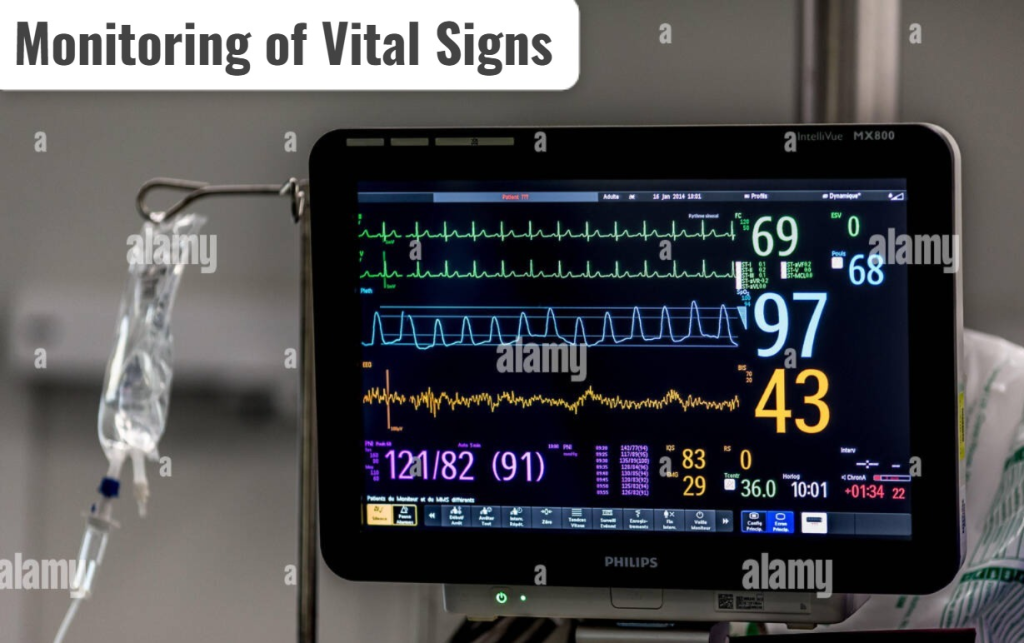
- Continuous monitoring of the patient’s vital signs:
- Pulse rate
- Blood pressure
- Respiratory rate
- Oxygen saturation : SpO₂
- Temperature
- Electrocardiogram : ECG
If any value is found abnormal, immediately inform the surgeon and anesthesia team.
6) Fluid and Electrolyte Balance:
- Give the patient the necessary IV fluids: normal saline, Ringer lactate, etc.
- If there is blood loss during surgery, prepare for blood transfusion.
- Measure urine output to evaluate kidney function.
7) Documentation and Sponge/Instrument Count:
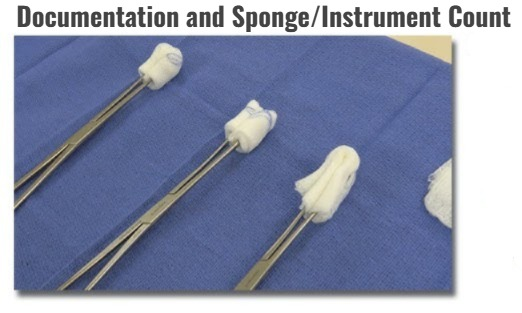
- Do sponge count and instrument count before and after surgery and record it.
- Every medication, fluid Keep a record of fluid and blood.
- If any adverse event occurs, note it immediately.
8) Maintaining Body Temperature:
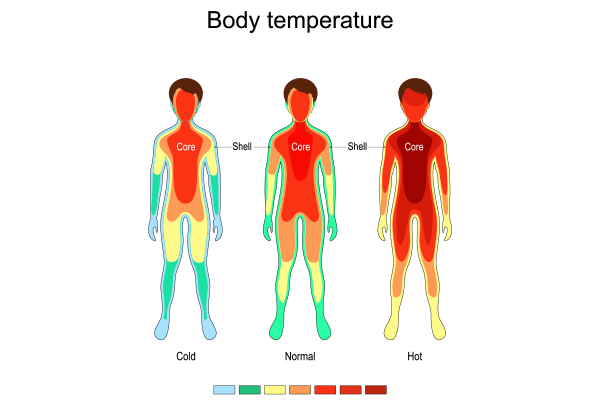
- To prevent hypothermia during surgery, use a warming blanket or warmed IV fluids.
- Continuous monitoring of body temperature.
9) Prevention of Complications:

- Avoid hemorrhage or excessive bleeding.
- Timely diagnose conditions such as hypoxia, hypotension, arrhythmia.
- Proper padding should be used to prevent positioning injury and nerve compression.
10) Transfer to Recovery Room:
- After the surgery is complete, the patient is transferred to the anesthesia recovery room or post-anesthesia care unit – PACU.
- Assess the patient’s airway, vital signs, IV line, and wound site.
- Documentation Complete the documentation and handover.
Intraoperative care is an important phase for patient safety, physiological stability, and surgical success.
During it, aseptic precautions, vital monitoring, anesthesia care, instrument safety, and documentation should be followed very carefully.
Good intraoperative care can prevent infection, hemorrhage, and complications, and the patient can be safely taken into the recovery phase.
Surgical team:
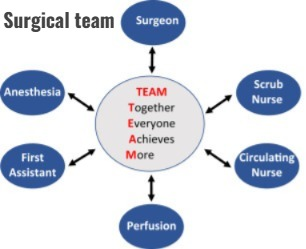
Definition:
- A surgical team is a professional health care team that works together to ensure the safety, treatment, and successful operation of a patient during surgery.
- Each member of the surgical team has a specific role and responsibility to provide the patient with comprehensive, coordinated, and safe surgical care. Coordinated and safe surgical care.
Main Members of Surgical Team:

1) Surgeon:
- The surgeon is the main member who performs surgery.
- He is responsible for the preoperative evaluation, operative procedure, and postoperative management of the patient.
- The surgeon ensures that the appropriate surgical method is selected for the patient and that aseptic technique is maintained during the operation.
2) Assistant Surgeon:
- The assistant surgeon helps the main surgeon during surgery.
- He helps with retraction, suction, tissue handling and suturing.
- When necessary, the assistant surgeon also performs some procedures independently but under the observation of the surgeon.
3) Anesthesiologist / Nurse Anesthetist Anaesthetist):
- This member provides anesthesia to patients before, during, and after surgery.
- Responsible for airway management, oxygenation, ventilation and vital signs monitoring of the patient.
- Immediately manages any complications that may arise during anesthesia.
4) Scrub Nurse / Scrub Technician:

- The scrub nurse wears sterile clothing and provides sterile instruments, suture materials, and supplies to the surgeon.
- She is responsible for instrument count and sponge count.
- Scrub nurse plays an important role in maintaining aseptic field.
5) Circulating Nurse:
- Circulating nurse works outside the sterile field.
- She is responsible for the overall management of the OT (Operation Theatre). (Overall Management).
- Provides the sterile team with the necessary instrument, specimen or medication.
- Performs documentation and sponge/instrument count verification.
6) Operating Room Technician:
- This member checks whether all the equipment, suction, light and table in the OT are functioning properly.
- Prevents cleaning and sterilization of the OT before and after the operation.
7) Surgical Orderly / Ward Boy:

- Bringing and moving the patient to the OT on a stretcher.
- Positioning (Positioning) Helping with OT cleaning and post-operative transfer.
- Helping with OT cleaning and post-operative transfer.
8) Post-Anesthesia Care Nurse:
- After the surgery is complete, the patient is taken to the recovery room or post-anesthesia care unit (PACU).
- There, he monitors the patient’s vital signs, airway, consciousness, and wound dressing.
- Observes side effects or complications of anesthesia.
Main Objectives of Surgical Team:
- Maintain patient safety and comfort.
- Follow aseptic technique.
- Work as a team by maintaining effective communication.
- Monitoring vital signs during the operation.
- Completing documentation properly.
A surgical team is a multidisciplinary group in which surgeons, anesthesiologists, nurses, and technicians function in a coordinated manner.
The roles of each member are complementary to each other, which makes the surgery successful, safe, and effective.
Good coordination and aseptic discipline are the greatest strengths of a surgical team, which ensure patient safety and ensures recovery.
Anesthesia:

Definition:
- Anesthesia is a medical process in which a temporary loss of sensation or loss of consciousness is produced in a patient using anesthetic agents or medications to prevent pain, stress, and discomfort during surgery, diagnostic, or therapeutic procedures.
- The main purpose of anesthesia is to make the patient pain-free, relaxed, and physiologically stable. (Physiologically stable) so that surgery can be performed safely.
1) Purpose of Anesthesia:
- Analgesia: Keeping the patient free from pain.
- Amnesia: Removing the memory of events that occurred during surgery.
- Muscle relaxation: Relaxing the muscles necessary for surgery.
- Control of reflexes (Reflex control): Controlling the body’s reflex actions.
- Maintenance of homeostasis: Keeping the body’s physiological functions stable.
2) Types of Anesthesia:
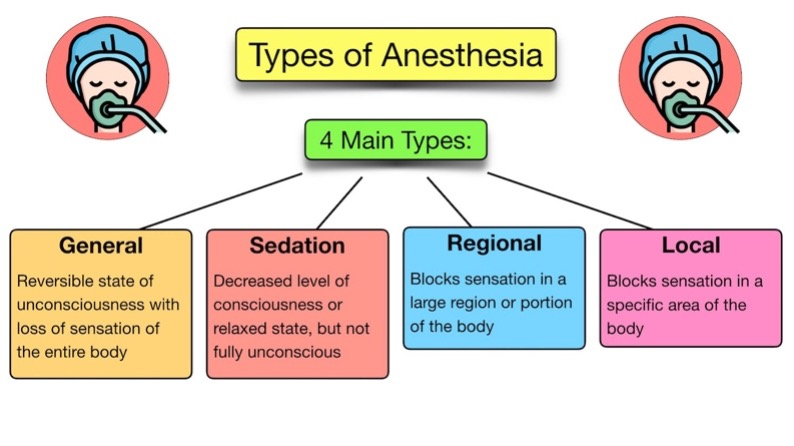
a) General Anesthesia:

- The patient is made completely unconscious.
- The patient loses awareness and sensation.
- Anesthetic drugs are inhalational agents or intravenous drugs (Intravenous drugs) are given by.
Used for : major surgeries.
- Examples: Propofol, Thiopental, Isoflurane, Nitrous oxide.
- Benefits : Complete pain control of the body is available and is suitable for long surgeries.
- Limitations: Nausea, vomiting or drowsiness may occur after anesthesia and special monitoring of the airway and breathing is required.
b) Regional Anesthesia:

- Sensation is blocked in a specific area of the body.
- The patient remains alert but the area being operated on becomes sensationless.
Types:
Spinal anesthesia:
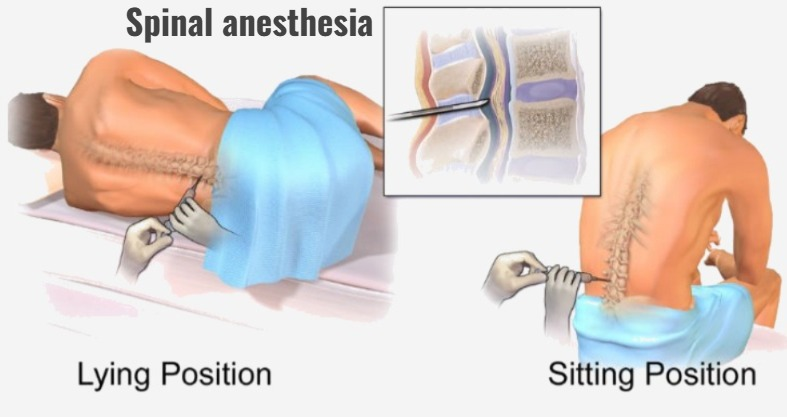
- Drug is given into the subarachnoid space of the spinal canal.
Commonly used for:
- lower abdominal, pelvic and lower limb surgeries.
Epidural anesthesia:
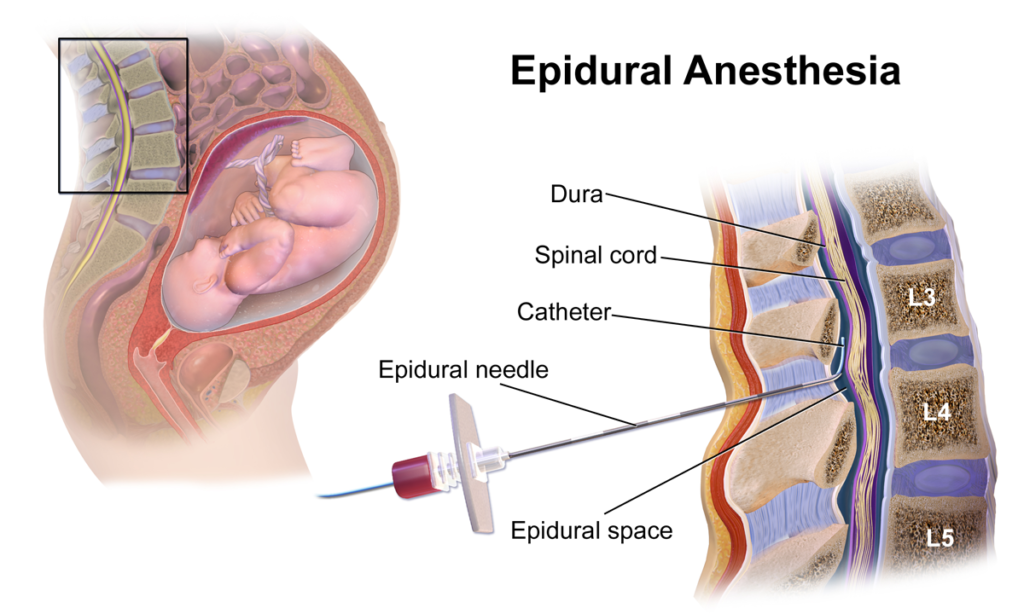
- Drug is given into the epidural space.
Commonly used for: obstetric procedures and prolonged surgeries.
Nerve block: Injecting a drug near a specific nerve to numb the area.
Example: Brachial plexus block, Femoral block.
c) Local Anesthesia:
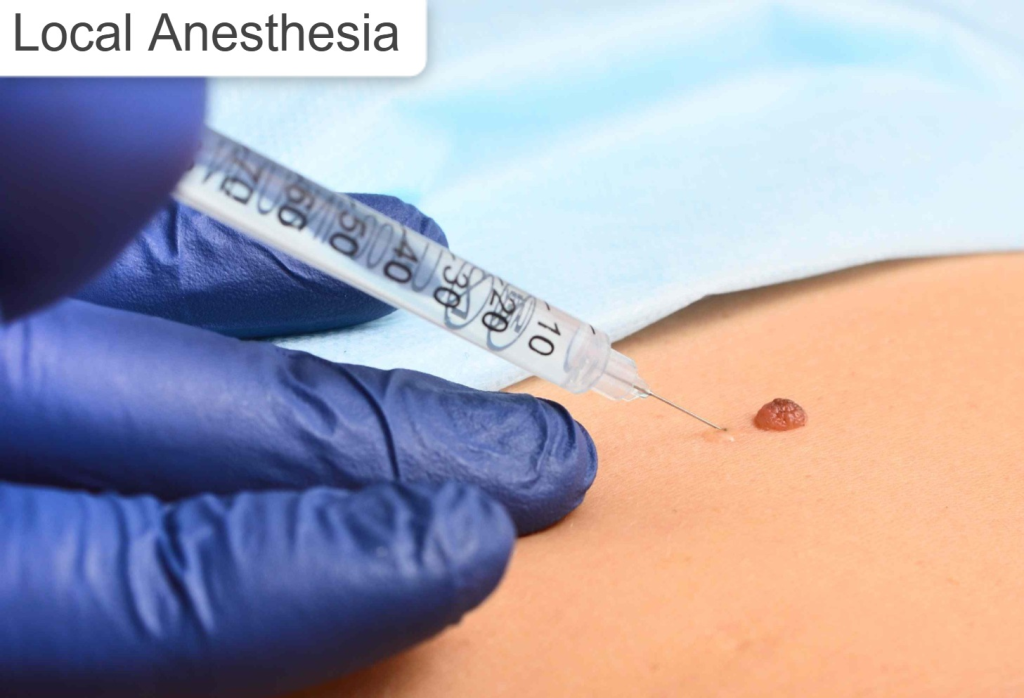
- Temporary numbness arises in a small area of the body.
Used for :
minor procedures:wound suturing, tooth extraction.
Examples: Lignocaine, Bupivacaine.
Benefits: Recovery is faster and sedation is not required.
Limitations: Only effective in small areas and may cause anxiety in patients.
d) Sedation:

- The patient is made calm and sleepy.
- Pain perception is reduced but complete unconsciousness does not occur.
Used for: short diagnostic procedures such as endoscopy.
Examples: Midazolam, Diazepam.
3) Stages of Anesthesia (Stages of General Anesthesia):

Induction:
- Inducing unconsciousness by administering an anesthetic drug, securing the airway, and monitoring vital signs.
Maintenance:
- Maintain anesthesia depth during surgery, administer oxygen, anesthetic gas, and IV agents.
Emergence:
- After surgery is complete, discontinue anesthesia, gradually awaken the patient, and monitor vital signs.
4) Pre-Anesthetic Preparation:
- Before administering anesthesia, the patient is completely examined by the anesthesiologist.
- Pre-anesthetic evaluation: The patient’s medical history, allergy, and medication. Check.
- NPO status: Do not give food or water before surgery to prevent aspiration.
- IV line: Put the patient on an IV line and start fluids.
- Monitoring devices: Put ECG, BP, SpO₂ on.
- Informed consent: Get permission for anesthesia.
5) Role of Nurse During Anesthesia:
- Nurses play an important role in maintaining patient safety during anesthesia.
- Continuously monitor the patient’s vital signs.
- Check the oxygen supply, suction apparatus, and anesthesia machine.
- Keep emergency drugs ready.
- Maintain communication between the surgeon and the anesthesiologist.
- Keep documentation accurate.
- Keep the patient in a safe position so that no injury occurs.
6) Complications of Anesthesia:
a) Minor complications:
- Nausea and vomiting
- Drowsiness
- Sore throat
- Mild hypotension Hypotension)
b) Major complications:
- Respiratory depression: Decreased breathing rate.
- Cardiac arrest: Heart rate stops.
- Anaphylaxis: Allergic reaction.
- Malignant hyperthermia: Sudden increase in temperature.
- Aspiration: Aspiration of stomach contents into the lungs.
7) Post-Anesthetic Care:
- After the surgery is completed, the patient is moved to the recovery room or post-anesthesia care unit – PACU (Post Anesthesia Care Unit).
- Check the patient’s airway, breathing and circulation.
- Continuously monitor vital signs – BP, Pulse, Respiration, SpO₂.
- Give analgesics for pain control.
- Give antiemetic drugs for nausea or vomiting.
- Complete documentation and report to the surgeon.
8) Commonly Used Drugs in Anesthesia:
Various types of drugs are used in anesthesia:
- Induction agents such as Propofol, Thiopental and Ketamine : to make the patient unconscious.
- Inhalational agents such as Isoflurane, Sevoflurane and Nitrous oxide : to maintain anesthesia.
- Muscle relaxants such as Succinylcholine and Vecuronium: to achieve muscle relaxation.
- Analgesics such as Fentanyl and Morphine: to relieve pain.
- Reversal agents (Reversal agents) such as Neostigmine and Glycopyrrolate: To reverse the effects of muscle relaxants.
- Antiemetics such as Ondansetron: To prevent nausea and vomiting after surgery.
Anesthesia is an important medical process that keeps the patient pain-free and relaxed during a surgical or diagnostic procedure.
Its different types – General, Regional, Local and Sedation anesthesia – are selected according to the type, duration of the surgery and the health of the patient.
While administering anesthesia, the main task of both the anesthesiologist and the nursing team is to maintain the patient’s safety, airway and vital signs.
Proper pre-anesthetic preparation, dose calculation and post-anesthetic care ensure the safety of the patient and the success of the surgery.
Post Operative Care:

Introduction:

- Post Operative Care refers to all types of medical and physical care provided to a patient after surgery. This time is life-long important because without proper care, there is a high chance of infection, bleeding, pain, or complications. The main aim is to ensure proper recovery of the patient.
Key Components of Post Operative Care:
1. Vital Signs Monitoring:
- After surgery, it is necessary to regularly check vital signs, i.e. BP (Blood Pressure), Pulse Rate, Respiratory Rate, and Body Temperature. Hence, any complication can be identified in advance.
2. Pain Management:
- Medications like analgesics and opioids are used to reduce the severity of post-operative pain. It is important to give medications by measuring the pain score so that the patient feels comfortable.
3. Wound Care:
- Regular cleaning and dressing of the wound after surgery is necessary. Sterile technique has to be adopted so that infection does not occur. Daily inspection of the risk and immediate monitoring if any symptoms like redness or pus are seen.
4.Fluid and Electrolyte Balance:
- Water and IV fluids are given into the body during or after surgery. Continuously monitor the levels of sodium, potassium, chloride, etc.
5.Respiratory Care:
- Use spirometry, deep breathing exercises, and incentive spirometer to prevent lung infections. Especially necessary in patients who have difficulty breathing after anesthesia.
6. Ambulation and Physical Activity:
- The patient should be encouraged to get out of bed and walk as soon as possible. Prolonged lying down can lead to conditions like Deep Vein Thrombosis (DVT) and Pulmonary Embolism.
7.Nutritional Support:
- Nutrition is most important after surgery. Initially, a clear liquid diet is given, followed by a soft diet and then a normal diet. Providing proper nutrition for the body’s energy needs and wound healing.
8.Mental and Psychological Support:
- Some patients experience anxiety, depression, or delirium after surgery. For this, their counseling and supportive therapy are necessary.
9. Medication Management:
- It is important to follow the medications given after surgery: such as antibiotics, analgesics, anticoagulants, etc. at the proper time and in the proper amount.
10. Discharge Planning and Follow-Up:
- When the patient is discharged, provide clear information about what care to take at home, when to take which medicine, and when to have a follow-up visit.
- Post Operative Care is not just a medical procedure but a process of bringing the patient back to a normal lifestyle. Proper monitoring, pain control, prevention of infection, and mental corporation make the patient’s health rehabilitation possible. It is essential for every medical staff and family member to understand this care and implement it properly.
Postoperative Care for the Patient:

- Post-surgery care means all the medical and helpful measures required for the complete recovery of the patient. During this period, it is extremely important to keep a close eye on the patient’s condition and prevent complications like infection, bleeding, and pain.
1. Monitoring of Vital Signs:
- Regular monitoring of temperature, pulse, blood pressure, and respiratory rate is necessary.
- If any abnormality is found in this amount, immediate medical intervention becomes necessary.
2. Pain Management:
- Medications like analgesics can be given to the patient to relieve pain.
- Morphine or other opioid medications are given depending on the severity of the pain.
- It is necessary to monitor the patient’s pain score.
3. Wound Wound Care:
- Regular dressing of the surgical site is very important.
- Antiseptic is used to prevent infection.
- If redness, swelling, or discharge is observed in the wound, immediately inform the medical personnel.
4.Fluid and Electrolyte Balance:
- The patient is given IV fluids. (IV) Therapy provides the necessary fluids.
- It is necessary to monitor the levels of electrolytes like Sodium, Potassium, Chloride.
5. Mobilization:
- Keeping the patient lying down for a long time can cause problems like thrombosis. It is necessary to get the patient seated as soon as possible and ask them to walk slowly. 6. Postoperative Diet Management: Initially, a clear liquid diet is given. –>
- If nausea, vomiting or bloating is observed, the diet is changed.
7.Respiratory Care:
- Lying for a long time The patient is likely to get an infection in the lungs.
- It is useful to ask him to cough and do spirometry.
- Deep breathing exercises are also important.
8. Psychological Support:
- After surgery, the patient experiences depression and anxiety.
- Family support and counseling prove to be very helpful.
9.Drug Therapy:
- Antibiotics, pain Timely administration of medicines like painkillers, anti-emetics.
- All medicines must be given according to the dose, route and time.
10. Discharge Planning and Follow-up:
- Provide complete information about wound care, medications, and follow-up to the patient before discharge.
- It is important to be present for timely medical check-ups.
- Taking care of the patient after surgery is as important for his recovery as the surgery itself. With proper monitoring, medication, wound care, diet, and mental support, the patient’s health can be improved quickly and safely.
Complications After Surgery:

- Various types of complications can occur in a patient after surgery. These complications are usually caused by lack of proper post-operative care, infection, anesthesia reaction, blood loss or deterioration of the patient’s physical condition.
1) Hemorrhage
Definition:
- The loss of blood, either internally or externally, after surgery is called hemorrhage. If bleeding is excessive, the patient may go into shock.
Signs and Symptoms:
- Pallor – Yellowish color of the face
- Tachycardia – Increased heart rate
- Hypotension (Hypotension) – Low blood pressure
- Restlessness
- Cold clammy skin
Management:
- Control blood loss
- Monitor vital signs.
- Give intravenous (IV) fluids and blood transfusions
- Notify surgeon immediately
2) Shock (Shock)
Definition:
- Shock is a life-threatening condition caused by decreased blood volume, infection, or anesthesia reactions.
Signs and Symptoms (Symptoms):
- Rapid Pulse
- Low Blood Pressure
- Cold & Pale Skin
- Oliguria (decreased urine output)
Management:
- Lay down the patient in the supine position
- Give oxygen
- Give intravenous (IV) fluids
- Give vasopressor drugs as ordered by the doctor
3) Infection:
Definition:
- Infection occurs due to bacterial contamination at the surgical site.
Signs and Symptoms:
- Redness, swelling, and pain at the incision site
- Fever
- Purulent discharge
Management (Management):
- Strictly follow aseptic technique
- Give antibiotics
- Change dressings regularly
- Monitor vital signs
4) Wound Dehiscence:
Definition:
- This condition occurs when the suture of a wound breaks or the incision site opens due to excessive tension.
Signs and Symptoms:
- Incision site opening
- Serosanguinous Discharge
- Pain and Fever
5.Deep Vein Thrombosis (DVT):
Definition:
- If a post-operative patient remains on bed rest for a long time, a blood clot forms in the lower limb vein.
Signs and Symptoms:
- Calf Pain
- Swelling
- Increased local temperature
Management:
- Early Mobilization
- Anticoagulant Therapy
- Leg Elevation
- Elastic Stockings
6) Pulmonary Complications:
Types:
- Atelectasis
- Pneumonia
- Pulmonary Embolism
Signs and Symptoms:
- Shortness of Breath
- Cough
- Fever
- Chest Pain
Management:
- Doing Deep Breathing Exercise
- Doing Incentive Spirometry
- Early Ambulation
- Giving Oxygen Therapy
7) Urinary Retention:
Definition:
- Inability to pass urine due to anesthesia or nerve impairment.
Management (Management):
- Bladder Training
- Warm Compress
- Catheterization if necessary
8) Nausea and Vomiting Vomiting):
Causes:
- Caused by anesthesia, pain, medication or gastric irritation.
Management:
- Giving Anti-emetic Drugs
- Introducing Food Slowly
- Keeping the Patient in a Comfortable Position
To Prevent Post-Operative Complications –
Careful Post-Operative Care
Aseptic Technique
Early Early Mobilization
Vital Sign Monitoring
and Doctor Ordered Medication
Timely nursing intervention and teamwork make patient recovery safe and immediate.
