Anatomy-B.sc-unit-5-Endocrine
🧠🩺 Major Endocrine Glands – The Body’s Chemical Messengers
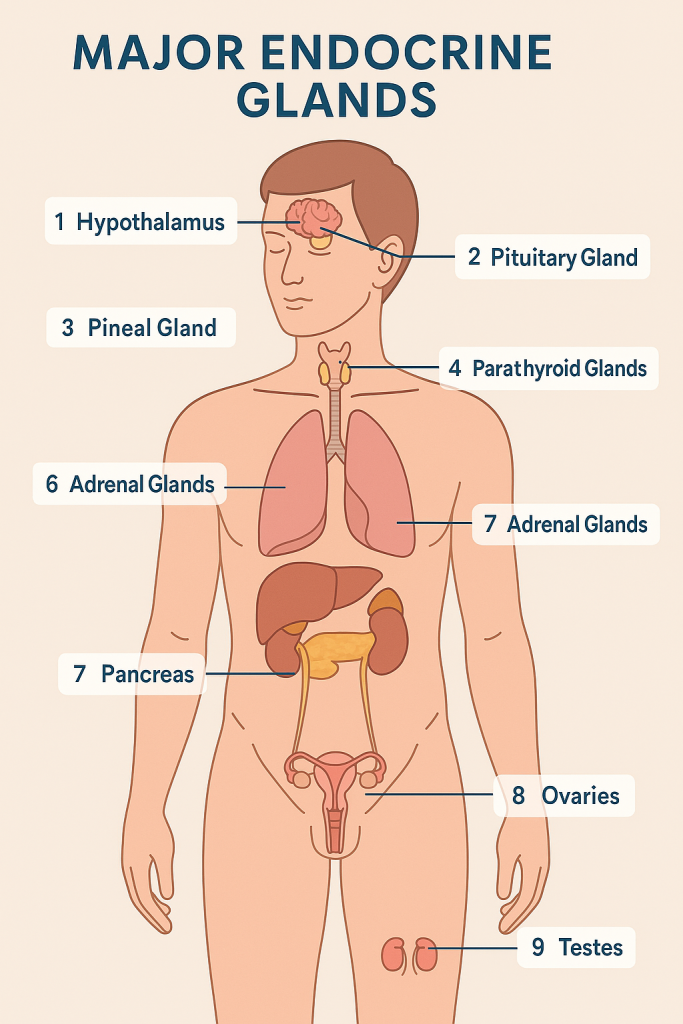
The endocrine system is a network of glands that secrete hormones directly into the bloodstream to regulate body functions like metabolism, growth, reproduction, and mood.
Hormones = Chemical messengers
Endocrine glands = Hormone-producing factories
🗺️ List of Major Endocrine Glands
| 🔢 | Gland Name | Location | Primary Hormones | Function |
|---|---|---|---|---|
| 1️⃣ | Hypothalamus | Brain (below thalamus) | Releasing/inhibiting hormones | Controls pituitary gland; links nervous & endocrine |
| 2️⃣ | Pituitary Gland | Base of brain (in sella turcica) | GH, TSH, ACTH, FSH, LH, Prolactin, ADH, Oxytocin | Master gland – controls other endocrine glands |
| 3️⃣ | Pineal Gland | Center of brain (epithalamus) | Melatonin | Regulates sleep-wake cycle (circadian rhythm) |
| 4️⃣ | Thyroid Gland | Neck (in front of trachea) | T3, T4, Calcitonin | Regulates metabolism, growth, and calcium balance |
| 5️⃣ | Parathyroid Glands | 4 small glands behind thyroid | Parathyroid hormone (PTH) | Increases blood calcium levels |
| 6️⃣ | Adrenal Glands | On top of kidneys | Cortisol, Adrenaline, Aldosterone | Stress response, BP regulation, salt balance |
| 7️⃣ | Pancreas (endocrine part) | Behind stomach (dual function) | Insulin, Glucagon, Somatostatin | Regulates blood sugar levels |
| 8️⃣ | Ovaries (females) | Pelvic cavity | Estrogen, Progesterone | Regulates female reproduction and secondary traits |
| 9️⃣ | Testes (males) | Scrotum | Testosterone | Regulates sperm production and male traits |
🔄 Other Important Hormone-Secreting Organs (Secondary endocrine function)
- Kidneys – Erythropoietin (EPO), Renin
- Heart – Atrial Natriuretic Peptide (ANP)
- Thymus – Thymosin (immune development)
- Placenta (during pregnancy) – hCG, estrogen, progesterone
🧠 Mnemonic to Remember Major Endocrine Glands
👉 “How Proud People Take Perfect Actions Proving Overall Triumph”
- H: Hypothalamus
- P: Pituitary
- P: Pineal
- T: Thyroid
- P: Parathyroid
- A: Adrenal
- P: Pancreas
- O: Ovaries
- T: Testes
🧠 Structure of the Hypothalamus – Master Regulator of the Body
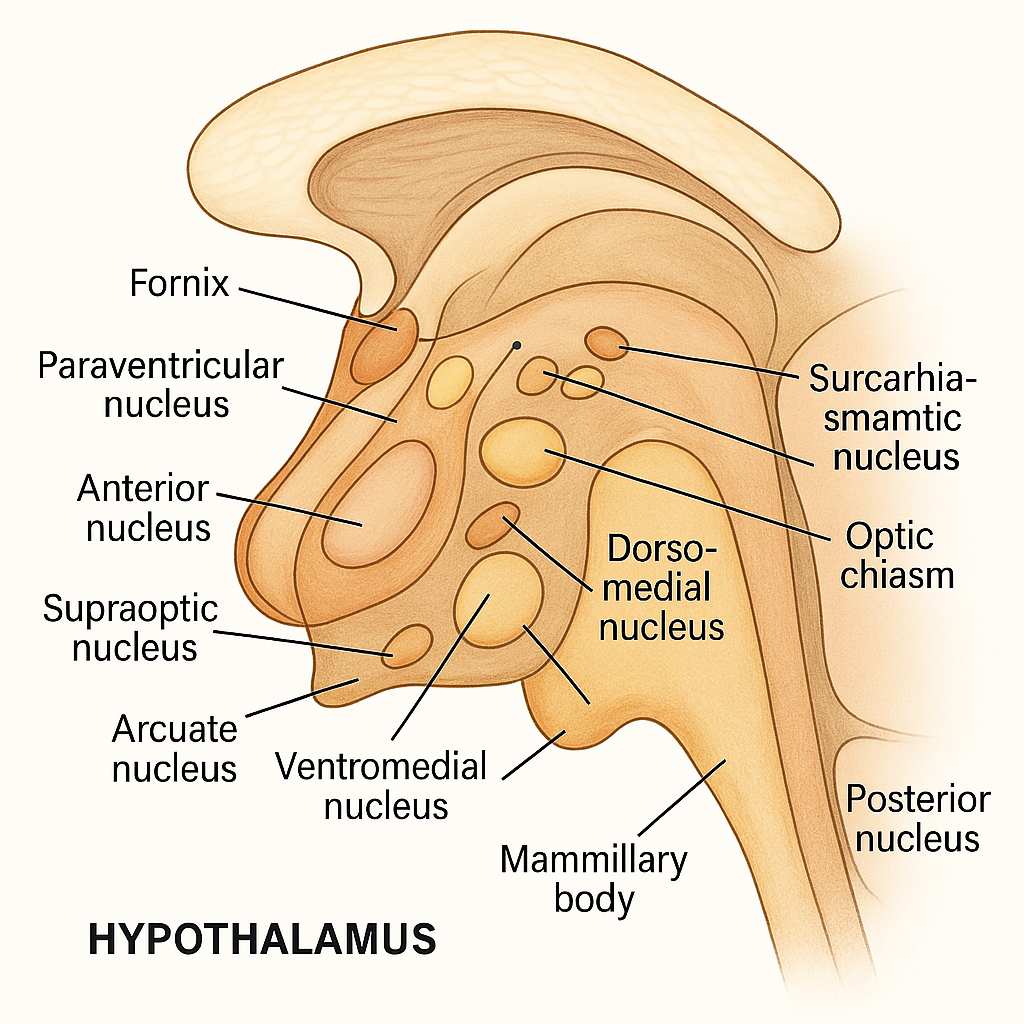
The hypothalamus is a small, cone-shaped structure in the brain, located just below the thalamus and above the pituitary gland. Despite its small size, it plays a huge role in maintaining homeostasis — the internal balance of the body — by controlling hormones, autonomic functions, and behavioral responses.
🔍 Anatomical Location & Structure
The hypothalamus forms the floor and lower walls of the third ventricle in the brain. It lies just above the optic chiasm, beneath the thalamus, and connects directly to the pituitary gland through a stalk called the infundibulum.
The hypothalamus is composed of a group of nuclei — clusters of nerve cells — that are divided into anterior, middle, and posterior regions, based on their location.
🧠 Functional Areas of the Hypothalamus
- Anterior (supraoptic) region
This includes important nuclei like the supraoptic, paraventricular, and suprachiasmatic nuclei. These regulate:- Body temperature (cooling)
- Circadian rhythms (sleep-wake cycle)
- Secretion of hormones like ADH (vasopressin) and oxytocin
- Middle (tuberal) region
Located in the central part of the hypothalamus, this region contains the arcuate, ventromedial, and dorsomedial nuclei. These are crucial for:- Controlling hunger and satiety
- Regulating the release of pituitary hormones like growth hormone, FSH, and LH
- Emotional behavior
- Posterior (mammillary) region
This area includes the mammillary bodies and other nuclei responsible for:- Memory processing
- Arousal and alertness
- Increasing body temperature (heating)
- Activating the sympathetic nervous system
🧬 Hypothalamus and Hormone Control
The hypothalamus acts as a bridge between the nervous system and the endocrine system. It produces releasing and inhibiting hormones that travel to the anterior pituitary gland, telling it when to release or stop releasing hormones.
Some of the key hormones controlled by the hypothalamus include:
- TRH (thyrotropin-releasing hormone)
- CRH (corticotropin-releasing hormone)
- GnRH (gonadotropin-releasing hormone)
- GHRH and Somatostatin (growth hormone regulators)
- Dopamine, which inhibits prolactin secretion
The hypothalamus also directly produces ADH and oxytocin, which are stored and released by the posterior pituitary.
🧠 Other Key Functions
- Temperature regulation: The anterior part helps cool the body, while the posterior part helps increase heat.
- Appetite and satiety: The lateral hypothalamus triggers hunger, and the ventromedial nucleus signals fullness.
- Circadian rhythms: The suprachiasmatic nucleus responds to light from the eyes to control sleep-wake cycles.
- Autonomic control: The hypothalamus controls heart rate, blood pressure, digestion, and stress responses.
- Emotional behavior: Works with the limbic system to influence emotions like fear, rage, and pleasure.
🌙🧠 Structure of the Pineal Gland – The Timekeeper of the Brain
🌙🧠 Structure of the Pineal Gland – The Timekeeper of the Brain
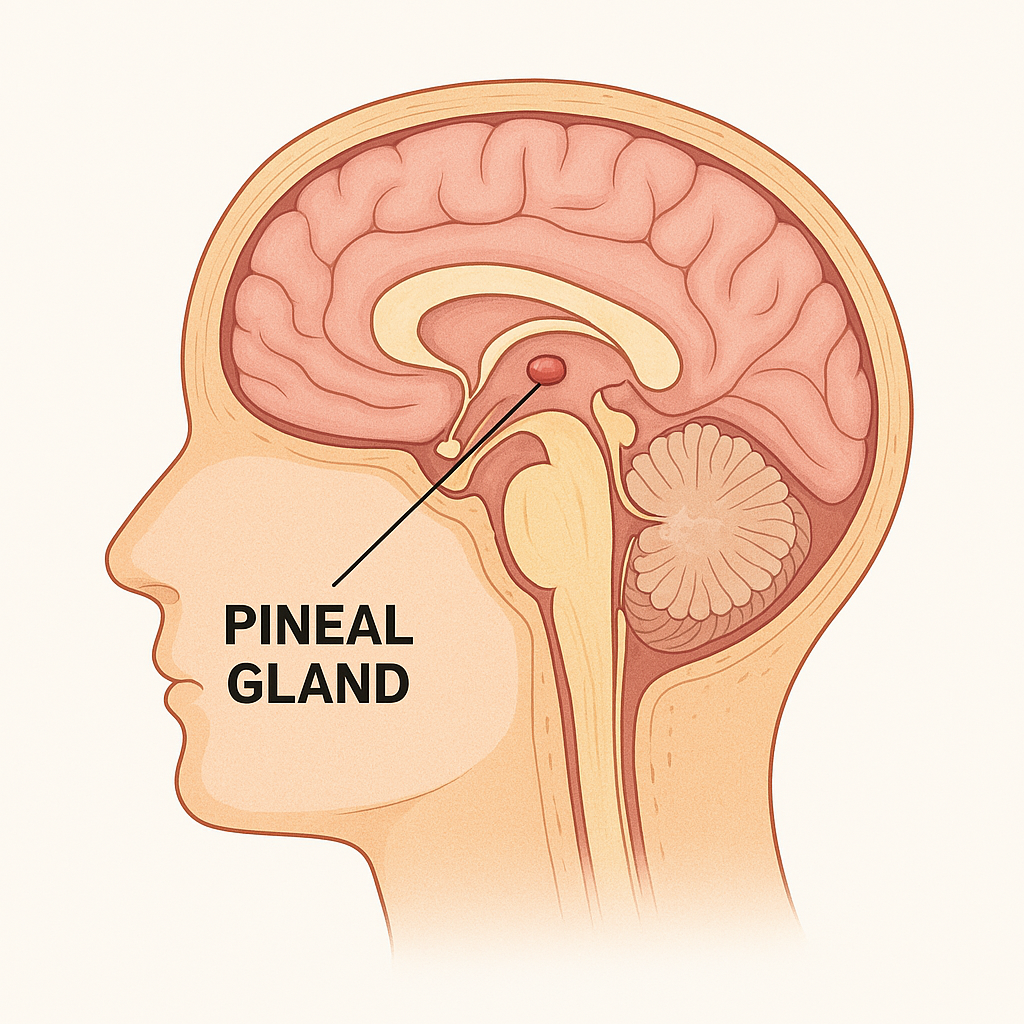
The pineal gland, also known as the epiphysis cerebri, is a small, pea-shaped endocrine gland nestled deep in the brain. Though tiny in size, it plays a big role in regulating circadian rhythms — the body’s internal clock that governs the sleep-wake cycle.
📍 Anatomical Location
The pineal gland is located in the center of the brain, tucked in a groove between the two hemispheres, where the two halves of the thalamus join. It sits just above the superior colliculi, and posterior to the third ventricle, attached to the roof of the diencephalon by a stalk called the pineal stalk.
Despite being near the brain’s midline, the pineal gland is not paired — it is a single, midline structure.
🧠 Gross Structure
- Shape & Size: Resembles a tiny pine cone (hence the name), about 5–8 mm long and weighs ~100 mg in adults.
- Color: Reddish-gray in youth, but becomes calcified with age (this is why it often appears white on X-rays and CT scans).
- Covering: It is surrounded by a thin capsule derived from the pia mater, the innermost meningeal layer.
🔬 Histological Structure
The pineal gland is made up of two main types of cells:
- Pinealocytes
- These are the main functional cells of the pineal gland.
- They are large, pale-staining cells with irregular nuclei.
- Their main function is to synthesize and secrete melatonin, the hormone that regulates sleep.
- Glial Cells (interstitial cells)
- These are supporting cells, similar to astrocytes in the brain.
- They help maintain the structure and protect the pinealocytes.
Another interesting feature is the presence of “brain sand” or corpora arenacea, which are calcium deposits that increase with age. These have no known function but help locate the pineal gland radiologically.
🌙 Functions of the Pineal Gland
- The primary role of the pineal gland is to secrete melatonin, a hormone that:
- Regulates sleep-wake cycles (circadian rhythm)
- Influences puberty onset and reproductive hormones
- Acts as an antioxidant and immunomodulator
Melatonin secretion is inhibited by light and stimulated by darkness, which is why it’s often called the “hormone of darkness.” This rhythm is controlled through a connection between the retina and the suprachiasmatic nucleus (SCN) of the hypothalamus.
🔄 Neural Connections
- The pineal gland does not have a direct connection to the hypothalamus through blood vessels (like other endocrine glands).
- Instead, it receives indirect neural input from the sympathetic nervous system, which is activated by signals from the SCN.
- The signal pathway: Retina → SCN → Spinal cord → Superior cervical ganglion → Pineal gland
🩺 Clinical Significance
- Disturbances in sleep: Linked to abnormal melatonin production or pineal tumors
- Pinealomas: Rare tumors that may lead to precocious puberty or obstructive hydrocephalus
- Calcification: Normal with age, but excessive early calcification may be linked to psychiatric or sleep disorders
- Jet lag and shift work: Disrupt melatonin cycles and impact sleep health
🧠 Fun Fact:
The philosopher Descartes called the pineal gland the “seat of the soul” because of its unique central position and solitary structure in the brain.
The pineal gland, also known as the epiphysis cerebri, is a small, pea-shaped endocrine gland nestled deep in the brain. Though tiny in size, it plays a big role in regulating circadian rhythms — the body’s internal clock that governs the sleep-wake cycle.
📍 Anatomical Location
The pineal gland is located in the center of the brain, tucked in a groove between the two hemispheres, where the two halves of the thalamus join. It sits just above the superior colliculi, and posterior to the third ventricle, attached to the roof of the diencephalon by a stalk called the pineal stalk.
Despite being near the brain’s midline, the pineal gland is not paired — it is a single, midline structure.
🧠 Gross Structure
- Shape & Size: Resembles a tiny pine cone (hence the name), about 5–8 mm long and weighs ~100 mg in adults.
- Color: Reddish-gray in youth, but becomes calcified with age (this is why it often appears white on X-rays and CT scans).
- Covering: It is surrounded by a thin capsule derived from the pia mater, the innermost meningeal layer.
🔬 Histological Structure
The pineal gland is made up of two main types of cells:
- Pinealocytes
- These are the main functional cells of the pineal gland.
- They are large, pale-staining cells with irregular nuclei.
- Their main function is to synthesize and secrete melatonin, the hormone that regulates sleep.
- Glial Cells (interstitial cells)
- These are supporting cells, similar to astrocytes in the brain.
- They help maintain the structure and protect the pinealocytes.
Another interesting feature is the presence of “brain sand” or corpora arenacea, which are calcium deposits that increase with age. These have no known function but help locate the pineal gland radiologically.
🌙 Functions of the Pineal Gland
- The primary role of the pineal gland is to secrete melatonin, a hormone that:
- Regulates sleep-wake cycles (circadian rhythm)
- Influences puberty onset and reproductive hormones
- Acts as an antioxidant and immunomodulator
Melatonin secretion is inhibited by light and stimulated by darkness, which is why it’s often called the “hormone of darkness.” This rhythm is controlled through a connection between the retina and the suprachiasmatic nucleus (SCN) of the hypothalamus.
🔄 Neural Connections
- The pineal gland does not have a direct connection to the hypothalamus through blood vessels (like other endocrine glands).
- Instead, it receives indirect neural input from the sympathetic nervous system, which is activated by signals from the SCN.
- The signal pathway: Retina → SCN → Spinal cord → Superior cervical ganglion → Pineal gland
🩺 Clinical Significance
- Disturbances in sleep: Linked to abnormal melatonin production or pineal tumors
- Pinealomas: Rare tumors that may lead to precocious puberty or obstructive hydrocephalus
- Calcification: Normal with age, but excessive early calcification may be linked to psychiatric or sleep disorders
- Jet lag and shift work: Disrupt melatonin cycles and impact sleep health
🧠 Fun Fact:
The philosopher Descartes called the pineal gland the “seat of the soul” because of its unique central position and solitary structure in the brain.
🦋 Structure of the Thyroid Gland – The Metabolism Regulator
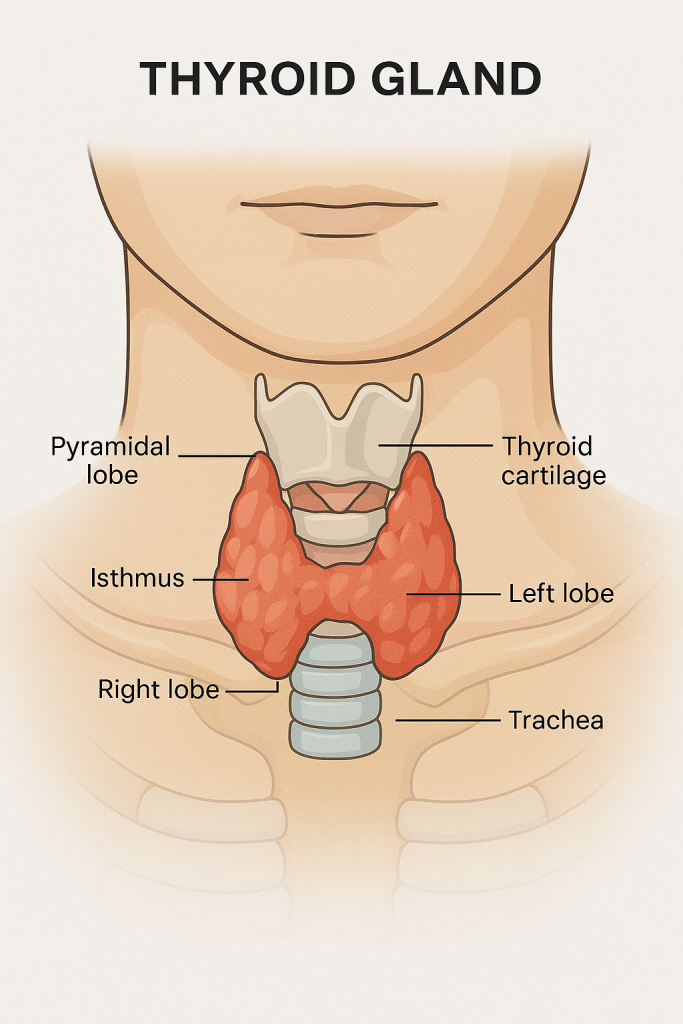
The thyroid gland is a butterfly-shaped, highly vascular endocrine gland located in the anterior neck, just below the larynx (voice box), and in front of the trachea (windpipe). It plays a vital role in controlling the body’s metabolism, growth, and development by secreting hormones like thyroxine (T₄), triiodothyronine (T₃), and calcitonin.
📍 Anatomical Location
The thyroid gland is situated at the level of the C5 to T1 vertebrae, resting on the anterior and lateral sides of the trachea. It is enclosed in a fibrous capsule and covered externally by pretracheal fascia, which is part of the deep cervical fascia of the neck.
🦋 Gross Anatomy of the Thyroid Gland
The thyroid has:
1. Two lateral lobes:
- One on each side of the trachea
- Extend from the oblique line of the thyroid cartilage down to the 6th tracheal ring
- These lobes lie over the carotid arteries and jugular veins
2. Isthmus:
- A thin band of glandular tissue that connects the two lobes
- Lies over the 2nd to 4th tracheal rings
3. Pyramidal lobe (in some people):
- An extension from the isthmus or one lobe
- Remnant of the thyroglossal duct from embryological development
🔬 Microscopic (Histological) Structure
The thyroid gland is made up of many lobules, and each lobule contains numerous follicles. These follicular structures are the functional and structural units of the gland.
🧪 Thyroid follicles:
- Spherical structures lined with a single layer of cuboidal epithelial cells
- The center of each follicle is filled with colloid, a protein-rich substance containing thyroglobulin, the precursor of thyroid hormones (T₃ and T₄)
- Follicular cells absorb iodine and convert it into thyroid hormones
🧬 Two main types of cells in the thyroid:
- Follicular cells (or thyrocytes):
- Line the follicles
- Produce and secrete T₃ (triiodothyronine) and T₄ (thyroxine)
- These hormones regulate basal metabolic rate, growth, temperature, and energy production
- Parafollicular cells (also called C cells):
- Located in between follicles
- Secrete calcitonin, a hormone that helps lower blood calcium levels by inhibiting bone resorption
🩸 Blood Supply of the Thyroid Gland
The thyroid is one of the most richly vascularized organs in the body.
- Arterial supply:
- Superior thyroid artery (from external carotid artery)
- Inferior thyroid artery (from thyrocervical trunk of subclavian artery)
- Occasionally, thyroid ima artery (a variant artery from brachiocephalic trunk)
- Venous drainage:
- Superior, middle, and inferior thyroid veins
- Drain into the internal jugular and brachiocephalic veins
🧠 Nerve Supply
Though the thyroid gland itself has no direct role in nerve activity, its surgical relevance is high because of nearby nerves:
- External branch of the superior laryngeal nerve (at risk during thyroidectomy)
- Recurrent laryngeal nerve (critical for vocal cord movement)
🩺 Clinical Relevance
- Goiter: Enlargement of the thyroid, due to iodine deficiency or hormonal imbalance
- Hypothyroidism: Underactive thyroid; symptoms include fatigue, weight gain, cold intolerance
- Hyperthyroidism: Overactive thyroid; symptoms include weight loss, heat intolerance, irritability
- Thyroid nodules: Lumps within the gland; may be benign or malignant
- Thyroidectomy: Surgical removal of the gland, often performed in cancer or large goiters
- Thyroid storm: Life-threatening hyperthyroid crisis
🦴🧠 Structure of the Parathyroid Glands – The Calcium Controllers
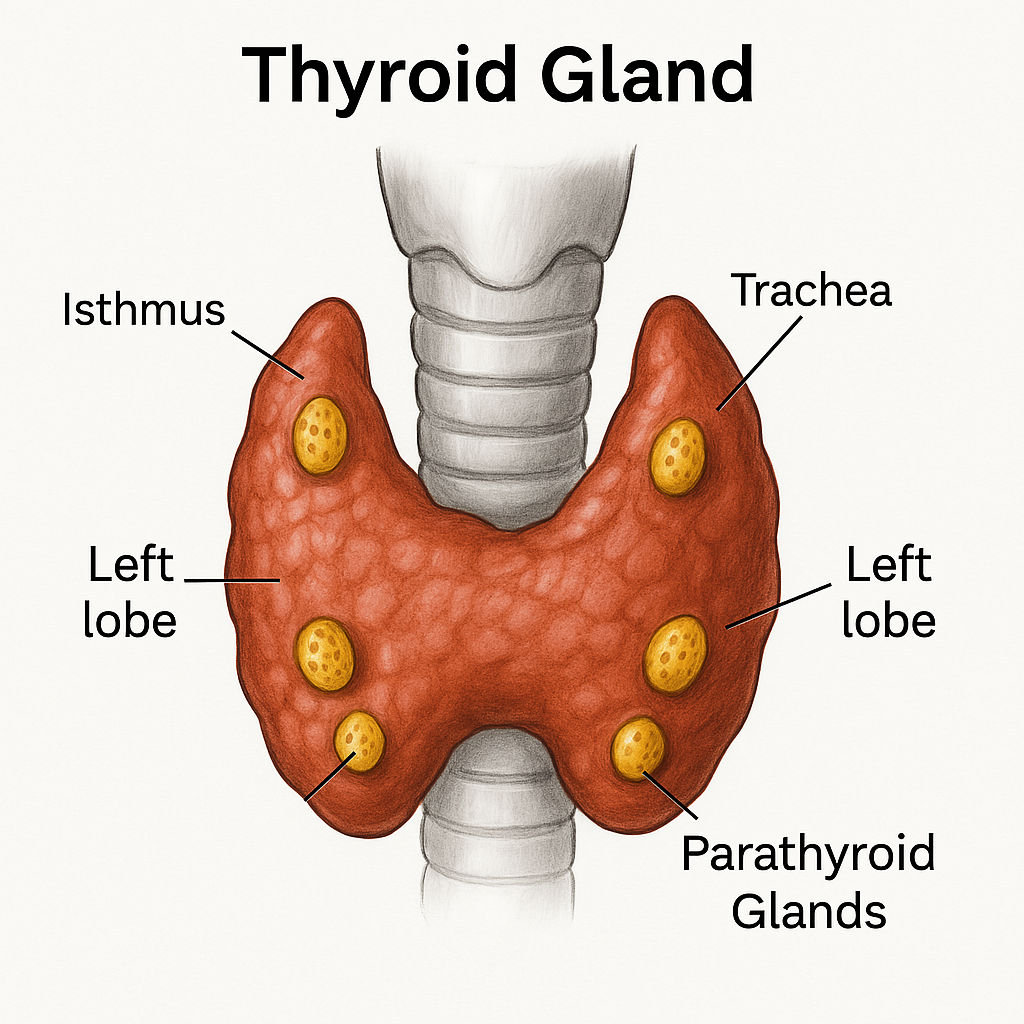
The parathyroid glands are small, pea-sized endocrine glands located on the back of the thyroid gland. Despite their size, they are essential for regulating calcium and phosphate balance, which is critical for bone health, nerve conduction, and muscle function.
📍 Anatomical Location
- There are typically four parathyroid glands:
- Two superior (upper)
- Two inferior (lower)
- They are embedded in the posterior surface of the thyroid gland within the capsule of the thyroid but are functionally separate from it.
- In some people, there may be more (supernumerary) or fewer glands, or they may be ectopically located (e.g., in the thymus or near the carotid sheath).
🔬 Microscopic (Histological) Structure
Each parathyroid gland is surrounded by a thin connective tissue capsule that extends inward to form septa, which divide the gland into lobules.
The parathyroid tissue is composed of two main types of cells:
1. Chief Cells (Principal Cells)
- Most abundant cell type
- Small, pale-staining with round nuclei
- Primary producers of parathyroid hormone (PTH)
- PTH increases blood calcium levels by:
- Stimulating bone resorption (osteoclast activation)
- Increasing calcium reabsorption in kidneys
- Promoting activation of Vitamin D, enhancing calcium absorption in intestines
2. Oxyphil Cells
- Larger, less numerous, appear after puberty
- Unknown function, but rich in mitochondria
- May play a role in supporting chief cells or PTH production under stress or disease
🩸 Blood Supply of the Parathyroid Glands
- Mainly supplied by the inferior thyroid artery
- Sometimes receive blood from the superior thyroid artery, thyroidea ima artery, or anastomotic branches
- Venous drainage is via the thyroid veins, eventually into the internal jugular vein
🧠 Nerve Supply
- Innervated by autonomic nerves from the cervical sympathetic chain
- However, parathyroid hormone secretion is primarily regulated by blood calcium levels, not by nerve signals
🧬 Functional Role of the Parathyroid Glands
Their sole and crucial function is to maintain calcium homeostasis. They do this through the secretion of parathyroid hormone (PTH) in response to low serum calcium levels.
When calcium levels drop:
- PTH is released
- This leads to:
- Increased calcium reabsorption from bones
- Decreased excretion of calcium by kidneys
- Increased absorption from intestines (via Vitamin D activation)
🩺 Clinical Relevance
- Hyperparathyroidism (Overactivity)
- Caused by tumor or hyperplasia of the glands
- Leads to high blood calcium levels, bone weakening, kidney stones
- Mnemonic: “Bones, stones, groans, and moans”
- Hypoparathyroidism (Underactivity)
- Can occur after thyroidectomy
- Causes low calcium, leading to muscle cramps, spasms, tetany
- Parathyroidectomy
- Surgical removal is done in cases of parathyroid tumors or severe hyperparathyroidism
🧠 Summary
- Location: Posterior surface of thyroid gland
- Number: Usually four
- Main cells: Chief cells (PTH producers), Oxyphil cells
- Hormone: Parathyroid hormone (PTH)
- Main function: Regulate blood calcium and phosphate levels
🧠🛡️ Structure of the Thymus Gland – The Immune System Trainer
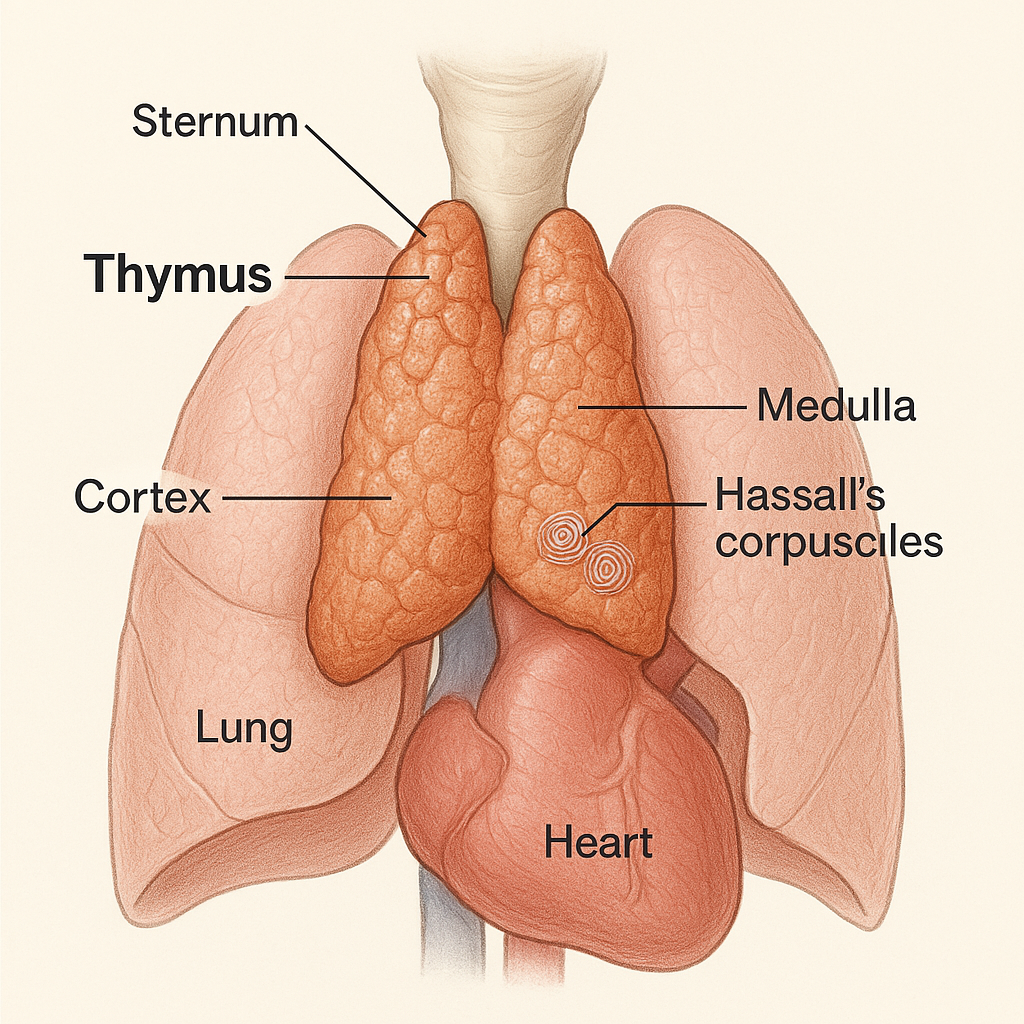
The thymus gland is a specialized primary lymphoid organ of the immune system. It plays a crucial role during early life by producing and maturing T-lymphocytes (T cells), which are vital for adaptive immunity.
📍 Anatomical Location
- The thymus is located in the anterior part of the superior mediastinum, extending into the anterior mediastinum.
- It lies behind the sternum and in front of the heart, above the pericardium, and between the lungs.
- In infants and children, it is relatively large and prominent, but it begins to shrink (involute) after puberty and is replaced by fatty tissue in adults.
🧠 Gross Structure
The thymus is:
- Bilobed (consists of right and left lobes)
- Encapsulated by a thin connective tissue membrane
- Internally divided into lobules by extensions of the capsule called septa
Each lobule consists of two distinct regions:
1. Cortex (outer zone):
- Densely packed with immature T cells (also called thymocytes)
- Contains epithelial cells, macrophages, and dendritic cells
- Site for T-cell maturation and selection
2. Medulla (inner zone):
- Contains fewer, more mature T cells
- Rich in epithelial cells
- Contains unique structures called Hassall’s corpuscles — concentric arrangements of epithelial cells with a central keratinized core; their function is not fully understood but may help in T-cell tolerance
🔬 Histological Features
- Cortex: Stains darker under the microscope due to high density of thymocytes
- Medulla: Lighter staining with fewer lymphocytes
- Hassall’s corpuscles: Key histological marker unique to the thymus
- The gland is lobulated, and each lobule has its own cortex and medulla
🔄 Blood-Thymus Barrier
- Present in the cortex to prevent immature T cells from exposure to antigens in the blood during development
- Composed of capillary endothelial cells, epithelial reticular cells, and macrophages
This barrier ensures controlled environment for T-cell maturation and protects them from premature antigenic exposure.
🧬 Function of the Thymus
The primary function of the thymus is to:
- Produce and mature T-lymphocytes, which are essential for cell-mediated immunity
- Educate T cells to distinguish self from non-self antigens
- T cells that fail to recognize self are destroyed (positive selection)
- T cells that attack self-antigens are eliminated (negative selection)
- Only about 2–5% of T cells survive and are released into circulation
🩺 Clinical Relevance
- Thymic Hyperplasia: Enlargement of the thymus, can be seen in autoimmune diseases like myasthenia gravis
- Thymoma: Tumor of thymic epithelial cells, can be benign or malignant
- DiGeorge Syndrome: Congenital absence or underdevelopment of thymus → leads to T-cell immunodeficiency
- Thymectomy: Surgical removal of the thymus, sometimes used in treating myasthenia gravis
🧠 Summary Points
- Type: Primary lymphoid organ
- Location: Superior and anterior mediastinum
- Structure: Bilobed, lobulated; has cortex and medulla
- Cells: Thymocytes, epithelial cells, dendritic cells, macrophages
- Special Features: Hassall’s corpuscles, blood-thymus barrier
- Function: Maturation and education of T cells (adaptive immunity)
- Changes with Age: Active in children; atrophies after puberty
🩺🧠 Structure of the Pancreas – Dual Gland of Digestion and Hormones
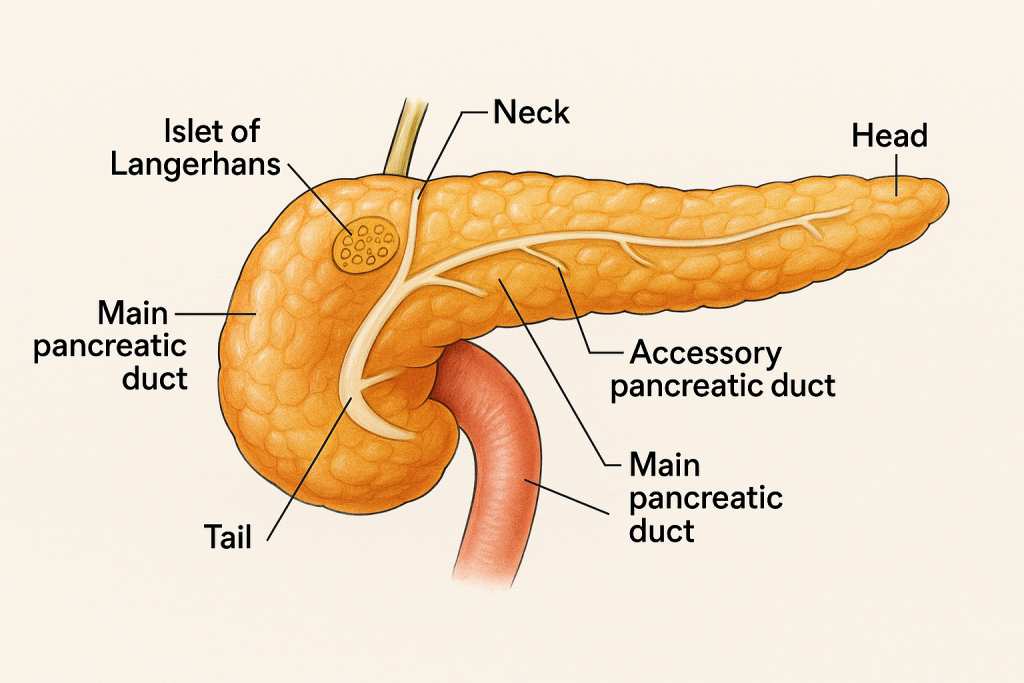
The pancreas is a soft, elongated, retroperitoneal organ located in the upper abdomen, behind the stomach. It functions as both an exocrine gland (producing digestive enzymes) and an endocrine gland (producing hormones that regulate blood sugar).
📍 Anatomical Location and External Structure
- Lies horizontally across the posterior abdominal wall at the level of L1–L2 vertebrae
- Positioned behind the stomach and in close relation to the duodenum and spleen
- The pancreas is divided into four main parts:
1. Head
- Nestled in the curve of the duodenum
- Connected to the duodenum via the main pancreatic duct (duct of Wirsung) and often the accessory duct (duct of Santorini)
2. Neck
- Short region between the head and body
- Lies anterior to the superior mesenteric vessels
3. Body
- Elongated central portion that extends to the left across the aorta and vertebral column
- Lies behind the stomach
4. Tail
- Tapered end of the pancreas that touches the spleen
- Only part that is intraperitoneal
🔬 Internal (Microscopic) Structure
The pancreas has two distinct functional parts:
🧪 1. Exocrine Component (~98%)
- Composed of serous acini (clusters of secretory cells)
- These cells secrete:
- Digestive enzymes: amylase, lipase, proteases (e.g., trypsinogen)
- Bicarbonate-rich fluid: neutralizes stomach acid
- Enzymes are delivered to the duodenum via the pancreatic duct system
➤ Ducts:
- Main pancreatic duct (Duct of Wirsung): Runs the length of the pancreas and joins the common bile duct, opening into the duodenum at the major duodenal papilla
- Accessory duct (Duct of Santorini): May drain into the duodenum independently (present in ~40% people)
🧬 2. Endocrine Component (~2%) – Islets of Langerhans
Scattered clusters of pale-staining cells within the pancreas. They produce and secrete hormones directly into the bloodstream, which regulate glucose metabolism and other functions.
Main Cell Types:
- Alpha (α) cells: Secrete glucagon → raises blood glucose
- Beta (β) cells: Secrete insulin → lowers blood glucose
- Delta (δ) cells: Secrete somatostatin → inhibits both insulin & glucagon
- PP (F) cells: Secrete pancreatic polypeptide → regulates pancreatic secretions
These islets are more concentrated in the tail of the pancreas.
🩸 Blood Supply of the Pancreas
- Arteries: Derived from branches of:
- Celiac trunk (via splenic artery)
- Superior mesenteric artery (via pancreaticoduodenal branches)
- Veins: Drain into the portal vein
🧠 Dual Function Summary
| Function | Type | Secretes | Target |
|---|---|---|---|
| Endocrine | Hormonal | Insulin, glucagon, somatostatin, PP | Bloodstream (systemic) |
| Exocrine | Digestive | Enzymes and bicarbonate | Duodenum (via ducts) |
🩺 Clinical Relevance
- Diabetes Mellitus: Due to dysfunction or loss of beta cells (insulin deficiency)
- Pancreatitis: Inflammation of the pancreas, often due to alcoholism or gallstones
- Pancreatic cancer: Often arises from the head of the pancreas; late detection is common
- Cystic fibrosis: Thick secretions block pancreatic ducts → malabsorption
🧠 Key Facts to Remember
- The pancreas is both endocrine and exocrine
- Islets of Langerhans are responsible for hormone secretion
- It is retroperitoneal, except for the tail
- Connected closely to duodenum, spleen, and bile ducts
🧠🩺 Structure of the Adrenal (Suprarenal) Glands – The Stress & Salt Controllers
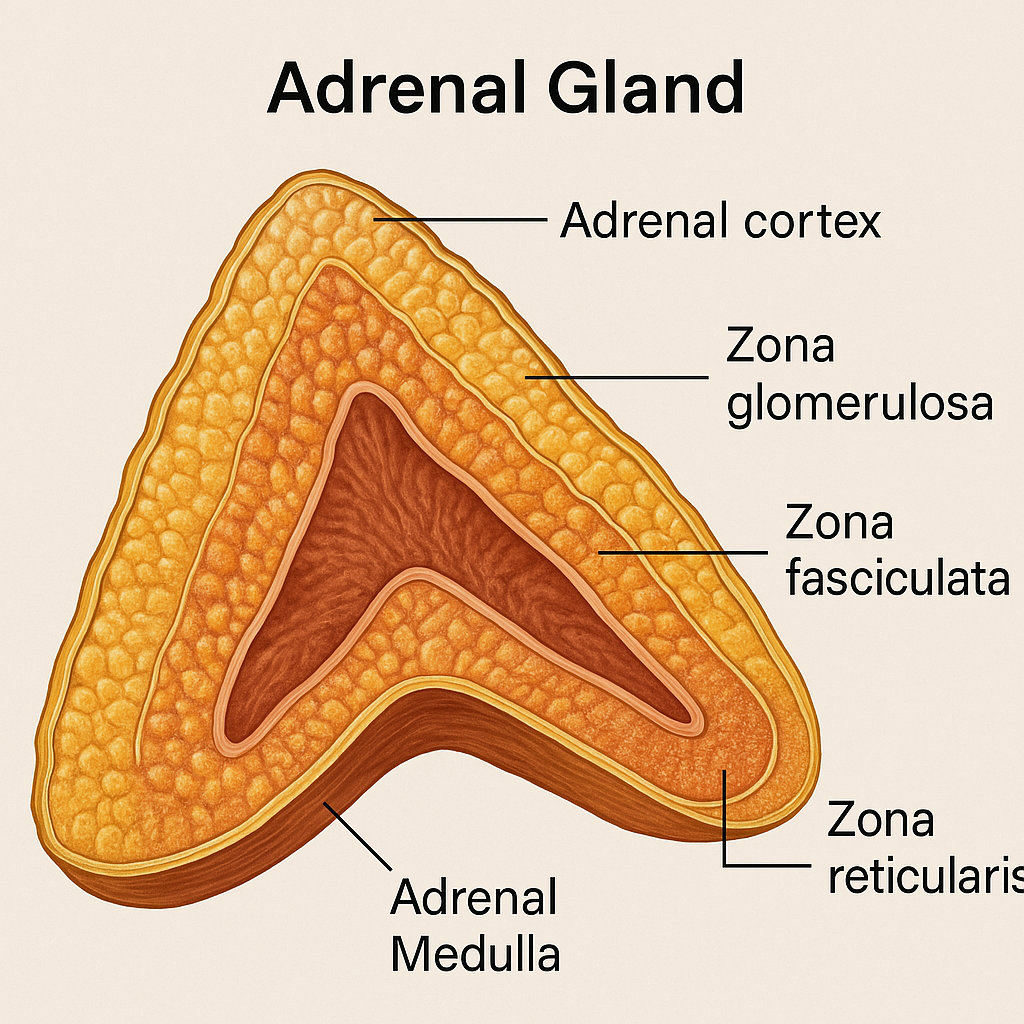
The adrenal glands, also called suprarenal glands, are paired endocrine organs that sit on top of each kidney like small caps. Despite their small size, they play a huge role in stress response, metabolism, electrolyte balance, and sex hormone production.
📍 Anatomical Location
- Located above each kidney in the retroperitoneal space of the upper abdomen.
- The right adrenal gland is pyramidal in shape, lies behind the inferior vena cava.
- The left adrenal gland is crescent-shaped, lies behind the stomach and pancreas.
- Each gland is enclosed in a fibrous capsule and surrounded by perirenal fat.
🧠 Gross Structure
The adrenal gland has two distinct regions, both in structure and function:
🔸 1. Adrenal Cortex (Outer layer – 80–90% of the gland)
The cortex is yellowish due to cholesterol and lipid content, and is divided into three concentric zones, each producing different types of steroid hormones:
a) Zona Glomerulosa (outermost)
- Cells arranged in rounded clusters
- Secretes mineralocorticoids, mainly aldosterone
- Function: Regulates sodium and potassium balance; affects blood pressure
b) Zona Fasciculata (middle and largest zone)
- Cells arranged in long cords
- Secretes glucocorticoids, mainly cortisol
- Function: Controls metabolism, immune response, and stress adaptation
c) Zona Reticularis (innermost cortical zone)
- Cells form a branching network
- Secretes androgens (sex hormones like DHEA)
- Function: Contributes to secondary sexual characteristics, especially in females
🔹 2. Adrenal Medulla (Inner core – 10–20% of the gland)
- Derived from neural crest cells (same origin as sympathetic neurons)
- Composed of chromaffin cells, which are modified postganglionic sympathetic neurons
- Secretes catecholamines:
- Adrenaline (epinephrine) – ~80%
- Noradrenaline (norepinephrine) – ~20%
- These hormones prepare the body for the “fight or flight” response:
- Increase heart rate, blood pressure, blood glucose
- Dilate bronchi and pupils
- Divert blood flow to muscles
🩸 Blood Supply
The adrenal glands have a rich blood supply from three sources:
- Superior adrenal artery – from inferior phrenic artery
- Middle adrenal artery – from abdominal aorta
- Inferior adrenal artery – from renal artery
Venous drainage:
- Right adrenal vein → directly into inferior vena cava
- Left adrenal vein → drains into left renal vein
This ensures rapid hormone distribution during stress.
🧠 Nerve Supply
- Sympathetic nerve fibers (from thoracic splanchnic nerves)
- Directly stimulate chromaffin cells of the adrenal medulla to release catecholamines
🧬 Functional Summary
| Region | Hormone Secreted | Function |
|---|---|---|
| Zona glomerulosa | Aldosterone | Regulates Na⁺, K⁺, water → affects blood pressure |
| Zona fasciculata | Cortisol | Stress response, metabolism, anti-inflammatory |
| Zona reticularis | Androgens (e.g., DHEA) | Sex characteristics, especially in females |
| Adrenal medulla | Epinephrine, Norepinephrine | Fight-or-flight response |
🩺 Clinical Significance
- Addison’s disease: Adrenal insufficiency (↓ cortisol & aldosterone)
- Cushing’s syndrome: Excess cortisol (e.g., from adrenal tumor)
- Pheochromocytoma: Tumor of adrenal medulla → ↑ catecholamines → hypertension
- Congenital adrenal hyperplasia (CAH): Genetic enzyme defects → hormonal imbalance
- Conn’s syndrome: Excess aldosterone → high BP and low potassium
🧬🩺 Structure of the Ovaries – The Female Reproductive Glands
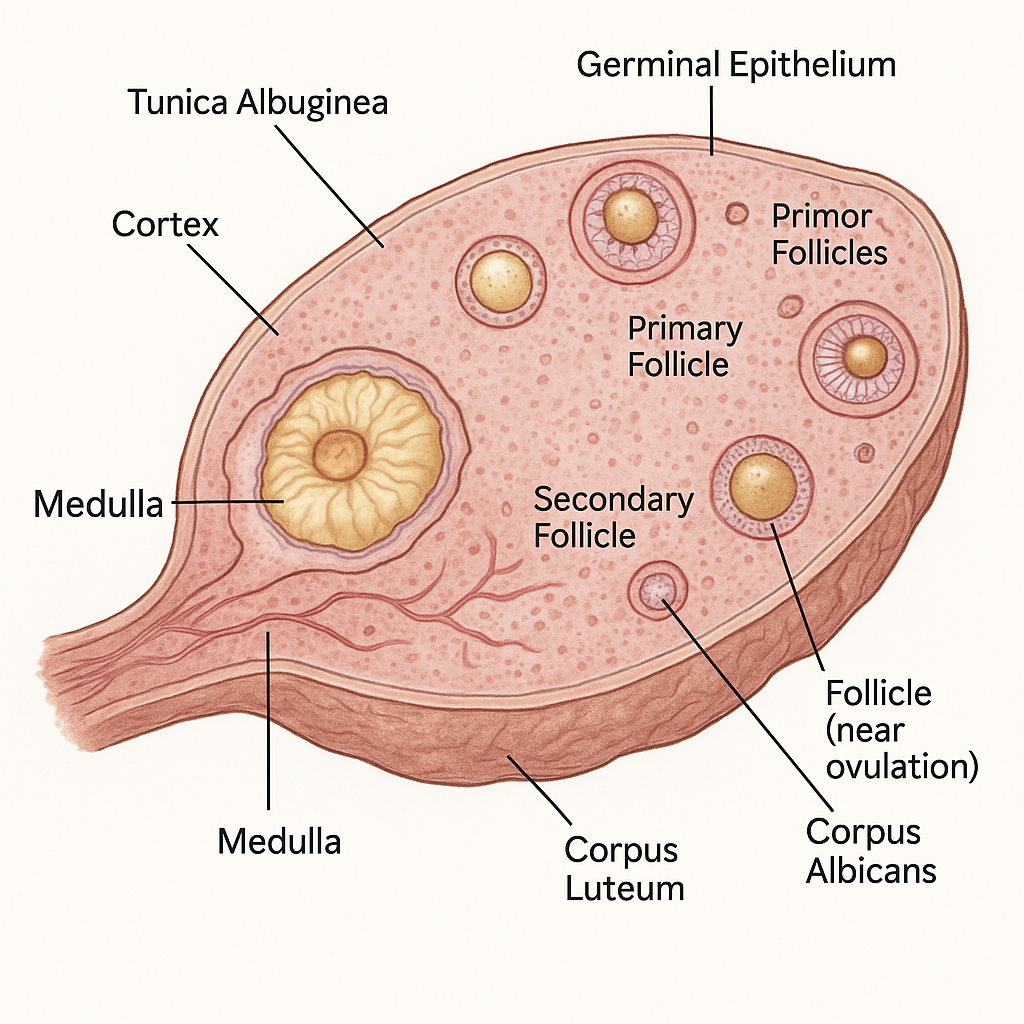
The ovaries are the female gonads, functioning as both reproductive organs and endocrine glands. They are responsible for producing female gametes (ova) and secreting vital sex hormones such as estrogen, progesterone, inhibin, and small amounts of androgens.
📍 Anatomical Location
- Located in the pelvic cavity, on either side of the uterus
- Positioned posterior to the broad ligament of the uterus, attached by the mesovarium
- Each ovary is about 3–5 cm long, 1.5–3 cm wide, and 1–1.5 cm thick
- Connected to the uterus by the ovarian ligament
- Suspended by the suspensory ligament of the ovary, which contains the ovarian artery, vein, lymphatics, and nerves
🧠 Gross Structure of the Ovary
Each ovary is almond-shaped and has the following external features:
1. Outer Surface
- Covered by a germinal epithelium (simple cuboidal epithelium), which is misnamed because ova don’t originate from it
- Beneath this is a dense connective tissue capsule called the tunica albuginea
2. Two Main Regions
A. Cortex (Outer Region)
- Contains ovarian follicles at various stages of development
- Surrounded by stroma, a connective tissue matrix
- Also contains interstitial cells and hormone-secreting cells
- Site of folliculogenesis (maturation of eggs)
- Contains corpus luteum and corpus albicans (post-ovulation structures)
B. Medulla (Inner Region)
- Central part containing loose connective tissue
- Richly supplied with blood vessels, lymphatics, and nerves
- No follicles are present here
🧬 Ovarian Follicles (Cortical Structures)
The cortex contains follicles in different stages:
- Primordial follicles: Resting, immature follicles (most abundant)
- Primary and secondary follicles: Begin to develop under hormonal influence
- Graafian (mature) follicle: Fully mature, ready to release an egg (ovulation)
- Corpus luteum: Temporary glandular structure that secretes progesterone after ovulation
- Corpus albicans: Fibrotic remnant of a degenerated corpus luteum
🌸 Endocrine Function of the Ovary
The ovaries act as endocrine glands by producing hormones critical to the menstrual cycle, reproduction, and secondary sexual characteristics:
1. Estrogen
- Secreted by developing follicles and corpus luteum
- Stimulates:
- Growth of uterine lining
- Development of female secondary sexual characteristics (breasts, fat distribution)
- Regulation of menstrual cycle
2. Progesterone
- Secreted by the corpus luteum after ovulation
- Prepares the endometrium for possible implantation
- Maintains pregnancy in early stages
3. Inhibin
- Inhibits FSH production from the anterior pituitary
- Regulates the rate of follicular development
4. Relaxin (during pregnancy)
- Relaxes uterine muscles and pubic ligaments
- Prepares body for childbirth
🩸 Blood Supply
- Ovarian artery: Direct branch from abdominal aorta
- Ovarian vein:
- Right vein drains into inferior vena cava
- Left vein drains into left renal vein
🧠 Clinical Relevance
- Ovarian cysts: Fluid-filled sacs in the ovary; may be functional or pathological
- Polycystic Ovary Syndrome (PCOS): Hormonal imbalance with multiple cysts, irregular cycles, infertility
- Ovarian failure: Leads to menopause; estrogen and progesterone levels drop
- Ovarian cancer: Often asymptomatic in early stages; may present with abdominal bloating or pelvic pain
🧠 Key Facts to Remember
- Dual role: Gamete (ova) production + hormone secretion
- Cortex = functional zone, Medulla = supportive core
- Follicles mature in the cortex; the corpus luteum forms post-ovulation
- Estrogen = promotes growth; Progesterone = maintains uterine readiness
🧬🧪 Structure of the Testes – The Male Reproductive and Hormonal Glands
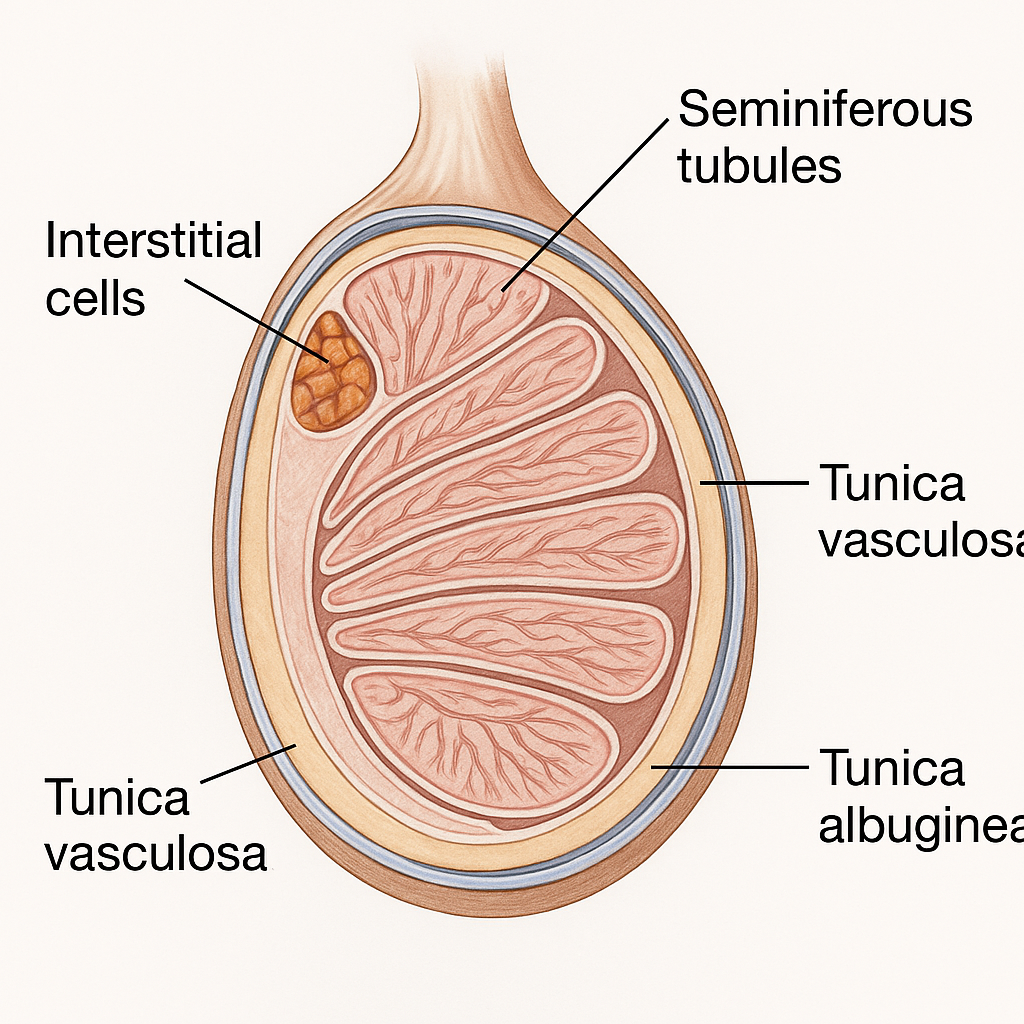
The testes (singular: testis) are the male gonads – paired oval-shaped organs responsible for the production of sperm (spermatogenesis) and the male sex hormone testosterone. They function as both exocrine glands (secreting sperm) and endocrine glands (secreting hormones into the blood).
📍 Anatomical Location
- The testes are located in the scrotal sac, which hangs outside the body cavity.
- This cooler environment (2–3°C below body temperature) is essential for sperm production.
- Each testis is suspended by the spermatic cord, which contains the vas deferens, blood vessels, lymphatics, and nerves.
🧠 Gross Structure of the Testes
Each testis is:
- Roughly 4–5 cm long and 2.5–3 cm wide
- Surrounded by three protective layers:
- Tunica vaginalis – outermost serous membrane (derived from peritoneum)
- Tunica albuginea – thick fibrous capsule under the tunica vaginalis
- Tunica vasculosa – inner layer with blood vessels
The tunica albuginea projects inward to form septa, dividing the testis into about 250–300 lobules.
🔬 Microscopic (Internal) Structure
Each lobule contains:
1. Seminiferous Tubules
- Coiled structures within each lobule
- Site of spermatogenesis (sperm production)
- Lined by germinal epithelium, which contains two key cell types:
- Spermatogenic cells – develop into mature sperm
- Sertoli cells (sustentacular cells) – support and nourish developing sperm, form the blood-testis barrier, and secrete inhibin
2. Interstitial Cells (Leydig Cells)
- Located between seminiferous tubules
- Produce the male hormone testosterone
- Stimulated by LH (Luteinizing Hormone) from the pituitary gland
🧬 Endocrine Function of the Testes
The Leydig cells are responsible for the endocrine function of the testes. They secrete:
➤ Testosterone
- Essential for:
- Development of male reproductive organs
- Appearance of secondary sexual characteristics (deep voice, facial hair)
- Sperm maturation
- Libido (sex drive) and muscle mass
➤ Inhibin (secreted by Sertoli cells)
- Inhibits FSH (Follicle Stimulating Hormone) to regulate sperm production
🔁 Sperm Pathway from Seminiferous Tubules
- Seminiferous tubules
- Straight tubules (tubuli recti)
- Rete testis (network of tubules in the mediastinum)
- Efferent ductules
- Epididymis → where sperm matures and is stored
- Vas deferens → carries sperm to ejaculatory ducts
🩸 Blood Supply and Lymphatics
- Testicular artery: from the abdominal aorta
- Pampiniform plexus of veins: regulates temperature and drains into testicular vein
- Lymphatic drainage: to lumbar (para-aortic) lymph nodes
🧠 Nerve Supply
- Derived from the sympathetic fibers (testicular plexus)
- Also has sensory innervation from genitofemoral and ilioinguinal nerves
🩺 Clinical Relevance
- Cryptorchidism: Undescended testis at birth → infertility risk
- Orchitis: Inflammation, often viral (e.g., mumps)
- Testicular torsion: Twisting of the spermatic cord → emergency
- Testicular cancer: Common in young males (15–35 years)
- Varicocele: Enlarged veins in pampiniform plexus → infertility
✅ Quick Summary Points
- Dual role: Exocrine (sperm) + Endocrine (testosterone)
- Seminiferous tubules = sperm production site
- Leydig cells = testosterone producers
- Sertoli cells = support and secrete inhibin
- Surrounded by three protective layers
- Sperm exits via the epididymis and vas deferens
🧠🩺 The Endocrine System – Applications and Implications in Nursing Practice
The endocrine system consists of ductless glands that secrete hormones directly into the bloodstream to regulate growth, metabolism, reproduction, fluid balance, and stress response. Understanding this system is crucial in nursing for assessment, diagnosis, medication management, and patient education.
🧬 Applications of Endocrine Knowledge in Nursing
1. Assessment and Monitoring
Nurses frequently monitor patients for signs and symptoms of hormonal imbalances, such as:
- Weight gain/loss
- Changes in energy level or mood
- Menstrual irregularities
- Temperature sensitivity
- Excessive thirst or urination
These observations help identify disorders like:
- Diabetes mellitus
- Thyroid disorders
- Cushing’s syndrome
- Addison’s disease
2. Administration of Hormonal Therapies
Nurses play a key role in administering, monitoring, and educating patients on hormone-based treatments:
- Insulin for diabetes
- Thyroxine (T4) for hypothyroidism
- Steroids for adrenal insufficiency
- Oral contraceptives or hormone replacement therapy
3. Blood Glucose Monitoring and Management
- Frequent monitoring using glucometers
- Managing hypoglycemia/hyperglycemia
- Educating patients on diet, exercise, insulin use
- Preventing complications like diabetic ketoacidosis (DKA)
4. Fluid and Electrolyte Balance
Many endocrine disorders affect fluid/electrolyte regulation:
- SIADH: fluid overload → need fluid restriction
- Diabetes insipidus: excessive urine loss → IV fluids and desmopressin
- Nurses monitor intake-output, serum sodium, urine osmolality, etc.
5. Nursing Care in Endocrine Emergencies
- Thyroid storm, myxedema coma, DKA, and adrenal crisis require:
- Close monitoring of vital signs
- Rapid intervention
- Administering IV medications, oxygen, electrolyte replacement
- Preparing for intensive care transfer
6. Nutritional and Lifestyle Counseling
- Educating patients with diabetes on low glycemic diet, carbohydrate counting
- Teaching thyroid patients about iodine intake
- Supporting weight management and exercise plans in metabolic syndrome
7. Psychological Support
Hormonal imbalances often affect mental health:
- Mood swings, depression, anxiety (e.g., hypothyroidism, menopause)
- Nurses assess emotional well-being and provide support or referrals
💉 Common Nursing Diagnoses Related to Endocrine Disorders
- Risk for unstable blood glucose level
- Deficient fluid volume or Excess fluid volume
- Altered body image (Cushing’s, acromegaly)
- Risk for injury (osteoporosis from hormone loss)
- Imbalanced nutrition: more or less than body requirements
- Fatigue and activity intolerance
🧠 Clinical Implications: System-Based View
| Gland | Disorder | Nursing Focus |
|---|---|---|
| Pituitary | Acromegaly, DI, SIADH | I&O charting, neuro checks, hormone replacement |
| Thyroid | Hypo/Hyperthyroidism | Vital signs, weight, cardiac monitoring |
| Parathyroid | Hypo/Hyperparathyroidism | Calcium monitoring, fall prevention |
| Adrenal | Addison’s, Cushing’s | Corticosteroid care, infection risk, skin care |
| Pancreas | Diabetes mellitus | Insulin management, foot care, glucose monitoring |
| Gonads | Menopause, infertility | Hormonal therapy support, reproductive education |
🩺 Key Roles of Nurses in Endocrine Care
- Patient education: explaining medications, monitoring, diet, and self-care
- Pre- and post-operative care: for gland removal (e.g., thyroidectomy)
- Collaborating with endocrine teams: doctors, dietitians, and psychologists
- Monitoring lab values: glucose, TSH, cortisol, electrolytes
- Promoting self-management: especially in chronic diseases like diabetes
📚
- The endocrine system impacts nearly every organ system
- Nurses must be vigilant in recognizing symptoms, managing hormone therapies, and educating patients
- Endocrine care involves holistic nursing: physical, emotional, nutritional, and lifestyle dimensions